Effects of Levocarnitine on Brachial-Ankle Pulse Wave Velocity in Hemodialysis Patients: A Randomized Controlled Trial
Abstract
:1. Introduction
2. Methods
2.1. Patients and Study Protocol
2.2. Study Evaluations
2.3. HD Procedure
2.4. Statistical Analysis
3. Results
3.1. Baseline Demographic and Clinical Data
| l-carnitine Group (n = 88) | Control Group (n = 88) | p Value | |
|---|---|---|---|
| Male/female | 63/25 | 65/23 | NS |
| Age (years) | 67 ± 11 | 68 ± 10 | NS |
| Duration of dialysis (months) | 54 ± 50 | 52 ± 50 | NS |
| Diabetes mellitus (%) | 54.5 | 52.3 | NS |
| Smoker (%) | 15.9 | 13.6 | NS |
| Medication | |||
| Antihypertensive agents (%) | 75 | 77.2 | NS |
| Statins (%) | 35.2 | 37.5 | NS |
| Kt/V | 1.32 ± 0.16 | 1.32 ± 0.17 | NS |
| Hemoglobin (g/dL) | 11.0 ± 0.9 | 11.1 ± 1.0 | NS |
| BUN (mg/dL) | 56.3 ± 13.6 | 57.7 ± 10.7 | NS |
| Creatinine (mg/dL) | 9.57 ± 2.93 | 9.21 ± 2.20 | NS |
| Uric acid (mg/dL) | 6.9 ± 1.1 | 6.7 ± 0.8 | NS |
| Sodium (mEq/L) | 142 ± 4 | 142 ± 2 | NS |
| Potassium (mEq/L) | 4.8 ± 0.7 | 4.9 ± 0.5 | NS |
| Corrected Ca (mg/dL) | 9.1 ± 0.6 | 9.0 ± 0.6 | NS |
| Phosphate (mg/dL) | 5.0 ± 1.0 | 5.0 ± 1.4 | NS |
| Total protein (g/dL) | 6.8 ± 0.5 | 6.7 ± 0.6 | NS |
| Albumin (g/dL) | 3.8 ± 0.4 | 3.7 ± 0.5 | NS |
| Intact PTH (pg/mL) | 158 ± 120 | 164 ± 116 | NS |
| Total cholesterol (mg/dL) | 158 ± 35 | 161 ± 29 | NS |
| LDL cholesterol (mg/dL) | 88 ± 26 | 90 ± 25 | NS |
| Triglycerides (mg/dL) | 126 ± 67 | 115 ± 65 | NS |
| Hs-CRP (mg/dL) | 0.45 ± 0.86 | 0.56 ± 0.81 | NS |
| β2-microglobulin (mg/L) | 23.8 ± 6.2 | 24.2 ± 8.3 | NS |
| Ferritin (ng/mL) | 119 ± 116 | 112 ± 130 | NS |
| TSAT (%) | 34.5 ± 13.4 | 33.0 ± 9.8 | NS |
| Total carnitine (μmol/L) | 41.1 ± 10.8 | 38.1 ± 8.3 | NS |
| Free carnitine (μmol/L) | 26.7 ± 7.6 | 23.9 ± 6.3 | NS |
| Acyl carnitine (μmol/L) | 14.9 ± 4.8 | 14.3 ± 3.6 | NS |
| Acyl/free carnitine | 0.59 ± 0.25 | 0.62 ± 0.16 | NS |
3.2. Effects of l-Carnitine Supplementation on Clinical Variables
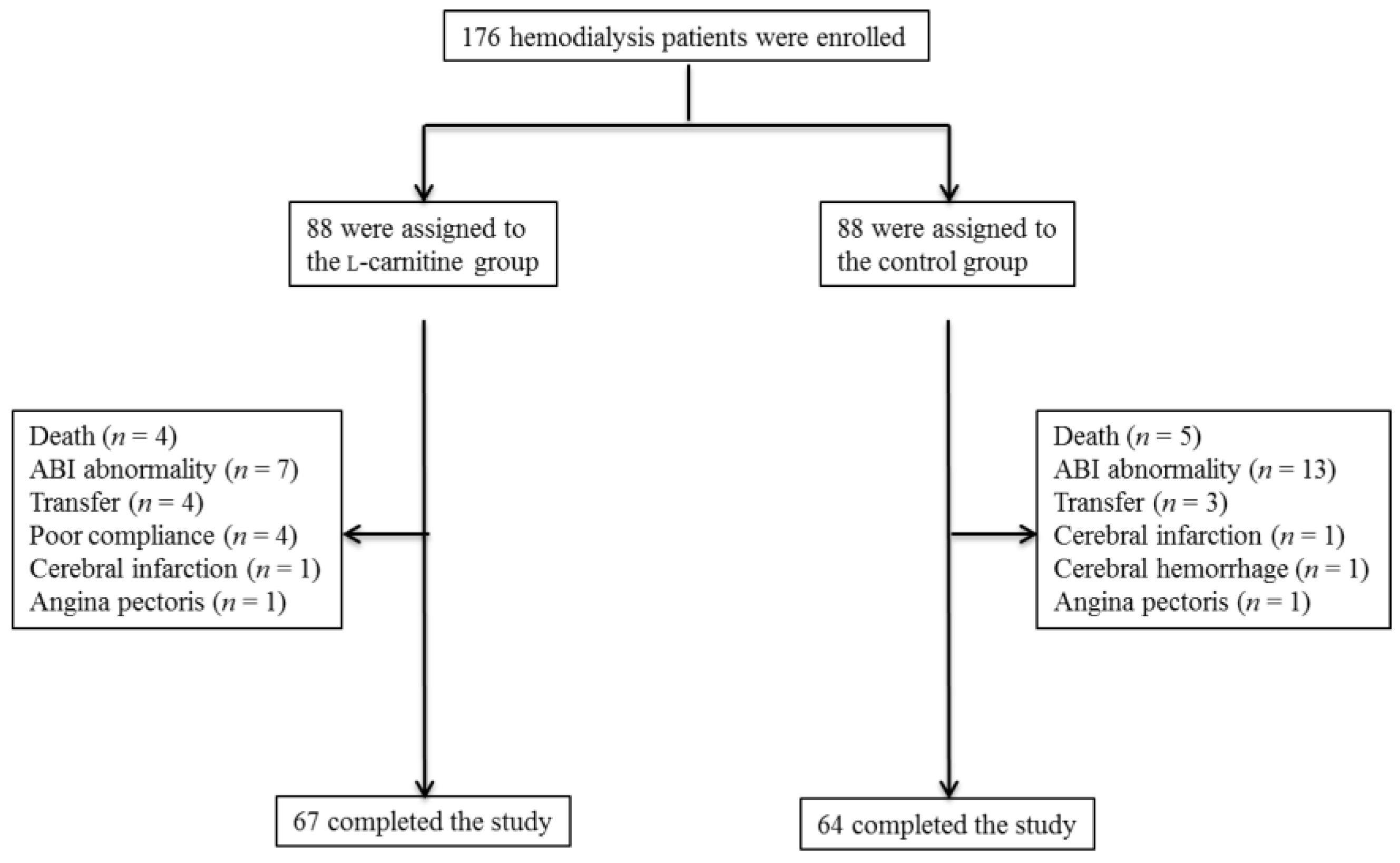
| l-carnitine Group (n = 67) | Control Group (n = 64) | |||||
|---|---|---|---|---|---|---|
| Baseline | 12 Months | p Value | Baseline | 12 Months | p Value | |
| Hemoglobin (g/dL) | 10.9 ± 0.9 | 11.0 ± 0.8 | NS | 10.9 ± 0.9 | 10.9 ± 1.0 | NS |
| BUN (mg/dL) | 55.2 ± 12.7 | 55.7 ± 14.5 | NS | 56.9 ± 12.7 | 57.8 ± 13.1 | NS |
| Creatinine (mg/dL) | 9.58 ± 2.52 | 9.48 ± 2.70 | NS | 9.49 ± 2.60 | 9.36 ± 2.40 | NS |
| Uric acid (mg/dL) | 7.0 ± 1.2 | 6.9 ± 1.1 | NS | 6.9 ± 1.0 | 6.9 ± 1.1 | NS |
| Sodium (mEq/L) | 142 ± 4 | 142 ± 4 | NS | 142 ± 4 | 142 ± 4 | NS |
| Potassium (mEq/L) | 4.7 ± 0.7 | 4.7 ± 0.7 | NS | 4.7 ± 0.6 | 4.8 ± 0.6 | NS |
| Corrected Ca (mg/dL) | 9.0 ± 0.6 | 9.0 ± 0.7 | NS | 8.9 ± 0.8 | 8.9 ± 0.7 | NS |
| Phosphate (mg/dL) | 5.1 ± 1.0 | 5.2 ± 1.3 | NS | 5.2 ± 1.1 | 5.1 ± 1.0 | NS |
| Total protein (g/dL) | 6.8 ± 0.5 | 6.7 ± 0.5 | NS | 6.7 ± 0.5 | 6.7 ± 0.5 | NS |
| Albumin (g/dL) | 3.8 ± 0.4 | 3.7 ± 0.4 | NS | 3.7 ± 0.4 | 3.7 ± 0.4 | NS |
| AST (IU/L) | 15 ± 9 | 15 ± 9 | NS | 14 ± 11 | 14 ± 9 | NS |
| ALT (IU/L) | 12 ± 8 | 12 ± 8 | NS | 11 ± 6 | 12 ± 8 | NS |
| Total cholesterol (mg/dL) | 160 ± 36 | 154 ± 31 | NS | 163 ± 34 | 160 ± 32 | NS |
| LDL cholesterol (mg/dL) | 89 ± 26 | 85 ± 22 | NS | 90 ± 26 | 88 ± 25 | NS |
| Triglycerides (mg/dL) | 127 ± 64 | 135 ± 74 | NS | 116 ± 64 | 118 ± 54 | NS |
| Hs-CRP (mg/dL) | 0.19 ± 0.20 | 0.16 ± 0.18 | NS | 0.21 ± 0.23 | 0.20 ± 0.20 | NS |
| Ferritin (ng/mL) | 123 ± 123 | 115 ± 103 | NS | 111 ± 70 | 104 ± 68 | NS |
| TSAT (%) | 30.5 ± 9.3 | 28.8 ± 10.2 | NS | 29.3 ± 11.0 | 29.4 ± 10.7 | NS |
| β2-microglobulin (mg/L) | 27.4 ± 8.7 | 26.6 ± 8.4 | NS | 27.6 ± 6.8 | 27.1 ± 5.7 | NS |
| Intact PTH (pg/mL) | 153 ± 88 | 150 ± 92 | NS | 147 ± 80 | 141 ± 82 | NS |
| ERI | 9.75 ± 9.02 | 6.39 ± 5.52 | <0.01 | 10.7 ± 10.8 | 9.83 ± 10.4 | NS |
| l-carnitine Group (n = 67) | Control Group (n = 64) | |||||
|---|---|---|---|---|---|---|
| Baseline | 12 Months | p Value | Baseline | 12 Months | p Value | |
| Total carnitine (μmol/L) | 42.0 ± 11.0 | 243.1 ± 87.4 * | <0.0001 | 40.2 ± 9.7 | 49.9 ± 9.5 | NS |
| Free carnitine (μmol/L) | 27.0 ± 7.8 | 157.6 ± 54.8 * | <0.0001 | 25.9 ± 6.9 | 25.6 ± 6.7 | NS |
| Acyl carnitine (μmol/L) | 15.0 ± 5.0 | 85.6 ± 38.3 * | <0.0001 | 14.2 ± 4.5 | 14.3 ± 4.5 | NS |
| Acyl/free ratio | 0.59 ± 0.27 | 0.54 ± 0.17 | <0.05 | 0.56 ± 0.17 | 0.58 ± 0.19 | NS |
3.3. Effects of l-Carnitine Supplementation on baPWV
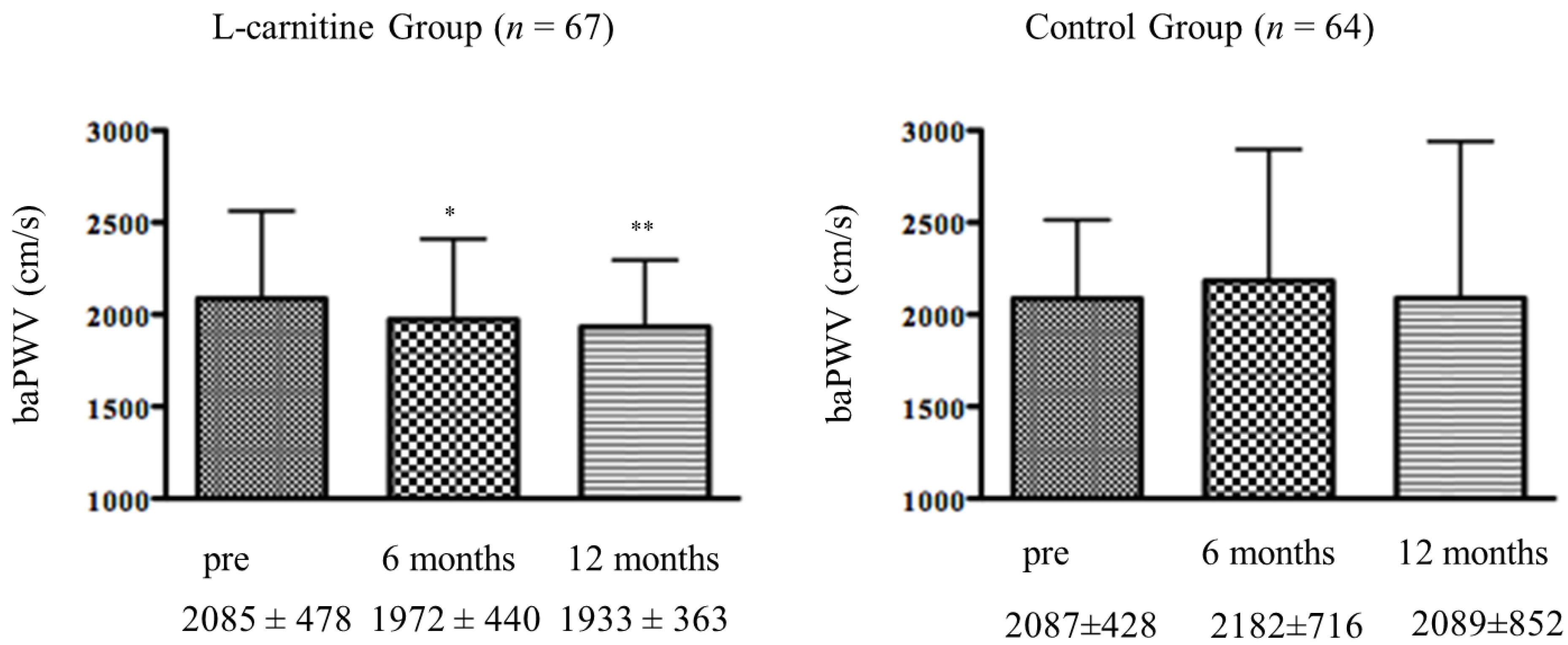
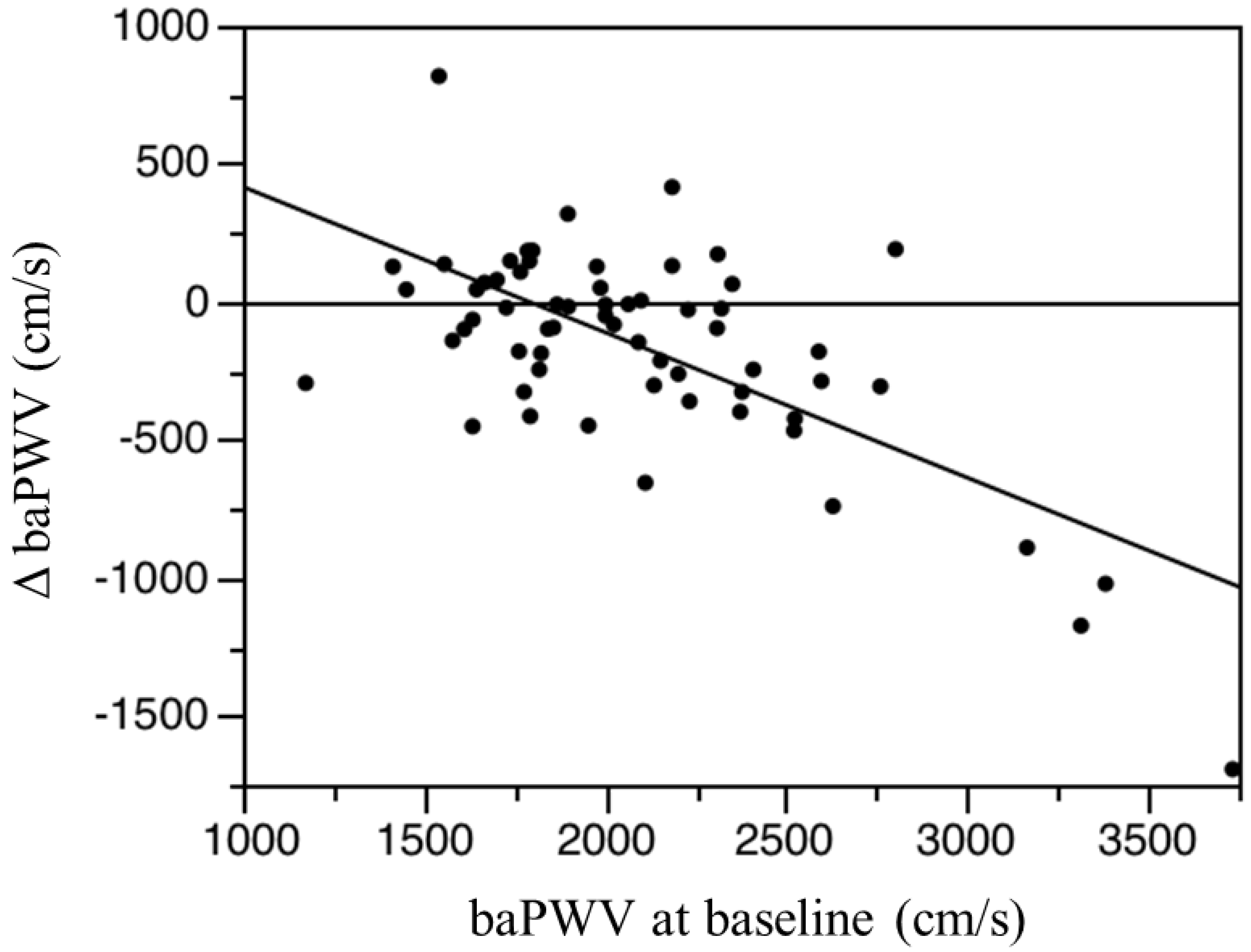
| l-carnitine Group (n = 67) | Control Group (n = 64) | |||||||
|---|---|---|---|---|---|---|---|---|
| Baseline | 12 Months | 6 Months | p Value | Baseline | 12 Months | 6 Months | p Value | |
| SBP (mmHg) | 151 ± 25 | 149 ± 23 | 149 ± 18 | NS | 150 ± 18 | 151 ± 20 | 147 ± 22 | NS |
| DBP (mmHg) | 82 ± 14 | 81 ± 12 | 81 ± 11 | NS | 78 ± 13 | 81 ± 11 | 82 ± 14 | NS |
| MAP (mmHg) | 114 ± 19 | 114 ± 17 | 113 ± 14 | NS | 113 ± 16 | 114 ± 18 | 112 ± 16 | NS |
| HR (bpm) | 73 ± 12 | 73 ± 11 | 74 ± 11 | NS | 71 ± 10 | 74 ± 21 | 71 ± 14 | NS |
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Ahmad, S. l-carnitine in dialysis patients. Semin. Dial. 2001, 14, 209–217. [Google Scholar] [PubMed]
- Evans, A.M.; Faull, R.J.; Nation, R.L.; Prasad, S.; Elias, T.; Reuter, S.E.; Fornasini, G. Impact of hemodialysis on endogenous plasma and muscle carnitine levels in patients with end-stage renal disease. Kidney Int. 2004, 66, 1527–1534. [Google Scholar] [CrossRef] [PubMed]
- Eknoyan, G.; Latos, D.L.; Lindberg, J. Practice recommendation for the use of l-carnitine in dialysis-related carnitine disorder. National Kidney Foundation Carnitine Consensus Conference. Am. J. Kidney Dis. 2003, 41, 868–876. [Google Scholar] [CrossRef] [PubMed]
- Fornasini, G.; Upton, R.N.; Evans, A.M. A pharmacokinetics model for l-carnitine in patients receiving hemodialysis. Br. J. Clin. Pharmacol. 2007, 64, 335–345. [Google Scholar] [CrossRef] [PubMed]
- Peluso, G.; Barbarisi, A.; Savica, V.; Reda, E.; Nicolai, R.; Benatti, P.; Valvani, M. Carnitine: An osmolyte that plays a metabolic role. J. Cell. Biochem. 2000, 80, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Schreiber, B. Levocarnitine and dialysis: A review. Nutr. Clin. Pract. 2005, 20, 218–243. [Google Scholar] [CrossRef] [PubMed]
- Matera, M.; Bellinghieri, G.; Costantino, G.; Santoro, D.; Calvani, M.; Savica, V. History of l-carnitine: Implications for renal disease. J. Ren. Nutr. 2003, 13, 2–14. [Google Scholar] [CrossRef] [PubMed]
- Stenvinkel, P.; Heimburger, O.; Lindholm, B.; Kaysen, G.A.; Bergström, J. Are there two types of malnutrition in chronic renal failure? Evidence for relationships between malnutrition, inflammation and atherosclerosis (MIA syndrome). Nephrol. Dial. Transplant. 2000, 15, 653–960. [Google Scholar]
- Kalantar-Zadeh, K.; Block, G.; McAllister, C.J.; Humphreys, M.H.; Kopple, J.D. Appetite and inflammation, nutrition, anemia, and clinical outcome in hemodialysis patients. Am. J. Clin. Nutr. 2004, 80, 299–307. [Google Scholar] [PubMed]
- Stenvinkel, P. Inflammation in end-stage renal failure: Could it be treated? Nephrol. Dial. Transplant. 2002, 17, 33–38. [Google Scholar] [CrossRef] [PubMed]
- Stenvinkel, P.; Yeun, J.Y. Role of inflammation in malnutrition and atherosclerosis in chronic renal failure. In Kopple and Massry’s Nutritional Management of Renal Disease, 2nd ed.; Kopple, J.D., Massry, S.G., Eds.; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2004; pp. 199–212. [Google Scholar]
- Horl, W.H. Oxidative stress. In Kopple and Massry’s Nutritional Management of Renal Disease, 2nd ed.; Kopple, J.D., Massry, S.G., Eds.; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2004; pp. 99–110. [Google Scholar]
- Jacobs, P.; Glorieux, G.; Vanholder, R. Interleukin/cytokine profiles in haemodialysis and in continuous peritoneal dialysis. Nephrol. Dial. Transplant. 2004, 19, v41–v45. [Google Scholar] [CrossRef] [PubMed]
- Savica, V.; Santoro, D.; Mazzaglia, G.; Ciolino, F.; Monardo, P.; Calvani, M.; Bellinghieri, G.; Kopple, J.D. l-carnitine infusions may suppress serum C-reactive protein and improve nutritional status in maintenance hemodialysis patients. J. Ren. Nutr. 2005, 15, 225–230. [Google Scholar] [CrossRef] [PubMed]
- Duranay, M.; Akay, H.; Yilmaz, F.M.; Sens, M.; Tekeli, N.; Yucel, D. Effects of l-carnitine infusions on inflammatory and nutritional markers in haemodialysis patients. Nephrol. Dial. Transplant. 2006, 21, 3211–3214. [Google Scholar] [CrossRef] [PubMed]
- Shakeri, A.; Tabibi, H.; Hedayati, M. Effects of l-carnitine supplement on serum inflammatory cytokines, C-reactive protein, lipoprotein(a), and oxidative stress in hemodialysis patients with Lp(a) hyperlipoproteinemia. Hemodial. Int. 2010, 14, 498–504. [Google Scholar] [CrossRef] [PubMed]
- Tabibi, H.; Hakeshzadeh, F.; Hedayati, M.; Malakoutian, T. Effects of l-carnitine supplement on serum amyloid A and vascular inflammation markers in hemodialysis patients: A randomized controlled trial. J. Ren. Nutr. 2011, 21, 485–491. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, M.; Ueda, S.; Misaki, H.; Sugiyama, N.; Matsumoto, K.; Matsuo, N.; Murao, S. Carnitine determination by an enzymatic cycling method with carnitine dehydrogenase. Clin. Chem. 1994, 40, 817–821. [Google Scholar] [PubMed]
- Reuter, S.; Faull, R.J.; Ranieri, E.; Evans, A.M. Endogenous plasma carnitine pool composition and response to erythropoietin treatment in chronic haemodialysis patients. Nephrol. Dial. Transplant. 2009, 24, 990–996. [Google Scholar] [CrossRef] [PubMed]
- Foley, R.N.; Parfrey, P.S.; Sarnak, M.J. Epidemiology of cardiovascular disease in chronic renal disease. J. Am. Soc. Nephrol. 1998, 9, S16–S23. [Google Scholar] [PubMed]
- Iseki, K.; Fukiyama, K. The Okinawa Dialysis Study Group. Long-term prognosis and incidence of acute myocardial infarction in patients on chronic hemodialysis. Am. J. Kidney Dis. 2000, 36, 820–825. [Google Scholar] [CrossRef] [PubMed]
- Iseki, K.; Fukiyama, K. The Okinawa Dialysis Study Group. Clinical demographics and long-term prognosis after stroke in patients on chronic haemodialysis. Nephrol. Dial. Transplant. 2000, 15, 1808–1813. [Google Scholar] [CrossRef] [PubMed]
- Nishizawa, Y.; Shoji, T.; Ishimura, E.; Inaba, M.; Morii, H. Paradox of risk factors for cardiovascular mortality in uremia: Is a higher cholesterol level better for atherosclerosis in uremia? Am. J. Kidney Dis. 2001, 38, S4–S7. [Google Scholar] [CrossRef] [PubMed]
- Dossa, C.D.; Shepard, A.D.; Amos, A.M.; Kupin, W.L.; Reddy, D.J.; Elliott, J.P.; Wilczwski, J.M.; Ernst, C.B. Results of lower extremity in patients with end-stage renal disease. J. Vasc. Surg. 1994, 20, 14–19. [Google Scholar] [CrossRef] [PubMed]
- Aulivola, B.; Hile, C.N.; Hamdan, A.D.; Sheahan, M.G.; Veraldi, J.R.; Skillman, J.J.; Campbell, D.R.; Scovell, S.D.; LoGerfo, F.W.; Pomposelli, F.B., Jr. Major lower extremity amputation. Arch. Surg. 2004, 139, 395–399. [Google Scholar] [CrossRef] [PubMed]
- Rocco, M.V.; Soucie, J.M.; Reboussin, D.M.; McClellan, W.M. Risk factors for hospital utilization in chronic dialysis patients. J. Am. Soc. Nephrol. 1996, 7, 889–896. [Google Scholar] [PubMed]
- Koch, M.; Trapp, R.; Kulas, W.; Grabensee, B. Critical limb ischemia as a main cause of death in patients with end-stage renal disease: A single-centre study. Nephrol. Dial. Transplant. 2004, 19, 2547–2452. [Google Scholar] [CrossRef] [PubMed]
- Barrett, B.J.; Parfrey, P.S.; Morgan, J.; Barré, P.; Fine, A.; Goldstein, M.B.; Handa, S.P.; Jindal, K.K.; Kjellstrand, C.M.; Levin, A.; et al. Prediction of early death in end-stage renal disease patients starting dialysis. Am. J. Kidney Dis. 1997, 29, 214–222. [Google Scholar] [CrossRef] [PubMed]
- Chertow, G.M.; Normand, S.L.; Silva, L.R.; McNeil, B.J. Survival after acute myocardial infarction in patients with end-stage renal disease: Results from the cooperative cardiovascular project. Am. J. Kidney Dis. 2000, 35, 1044–1051. [Google Scholar] [CrossRef] [PubMed]
- Kitahara, T.; Ono, K.; Tsuchida, A.; Kawai, H.; Shinohara, M.; Ishii, Y.; Koyanagi, H.; Noguchi, T.; Matsumoto, T.; Sekihara, T.; et al. Impact of brachial-ankle pulse wave velocity and ankle-brachial blood pressure index on mortality in hemodialysis patients. Am. J. Kidney Dis. 2005, 46, 688–696. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, M.; Ishii, H.; Aoyama, T.; Takahashi, H.; Toriyama, T.; Kasuga, H.; Takeshita, K.; Yoshikawa, D.; Amano, T.; Murohara, T. Ankle brachial pressure index but not brachial-ankle pulse wave velocity is a strong predictor of systemic atherosclerotic morbidity and mortality in patients on maintenance hemodialysis. Atherosclerosis 2011, 219, 643–647. [Google Scholar] [CrossRef] [PubMed]
- Japanese Society for Dialysis Therapy. Japanese society for dialysis therapy guidelines for management of cardiovascular diseases in patients on chronic hemodialysis. Ther. Apher. Dail. 2012, 16, 387–435. [Google Scholar]
- Tomiyma, H.; Yamashina, A.; Arai, T.; Hirose, K.; Koji, Y.; Chikamori, T.; Hori, S.; Yamamoto, Y.; Doba, N.; Hinohara, S. Influence of age and gender on result of noninvasive brachial-ankle pulse wave velocity measurement—A survey of 12517 subjects. Atherosclosis 2003, 166, 302–309. [Google Scholar]
- Locatelli, F.; Canaud, B.; Eckardt, K.U.; Stenvinkel, P.; Wanner, C.; Zoccali, C. Oxidative stress in endstage renal disease: An emerging threat to patient outcome. Nephrol. Dial. Transplant. 2003, 18, 1272–1280. [Google Scholar] [CrossRef] [PubMed]
- Bueno, R.; Sotomayor, M.A.; Perez-Gurrero, C.; Gomez-Amores, L.; Vazquez, C.M.; Herrera, M.D. l-carnitine and propionyl-l-carnitine improve endothelial dysfunction in spontaneously hypertensive rats: Different participation of NO and COX-products. Life Sci. 2005, 77, 2082–2097. [Google Scholar] [CrossRef] [PubMed]
- Miguel-Crrasco, J.L.; Mate, A.; Monserrat, M.T.; Arias, J.L.; Aramburu, O.; Vazquez, C.M. The role of inflammatory markers in the cardioprotective effect of l-carnitine in l-NAME-induced hypertension. Am. J. Hypertens. 2008, 21, 1231–1237. [Google Scholar] [CrossRef] [PubMed]
- Pertosa, G.; Grandaliano, G.; Simone, S.; Soccio, M.; Schena, F.P. Inflammation and carnitine in hemodialysis patients. J. Ren. Nutr. 2005, 15, 8–12. [Google Scholar] [CrossRef] [PubMed]
- Savica, V.; Calvani, M.; Benatti, P.; Santoro, D.; Monardo, P.; Peluso, G.; Bellinghieri, G. Carnitine system in uremic patients: Molecular and clinical aspects. Semin. Nephrol. 2004, 24, 464–468. [Google Scholar] [CrossRef] [PubMed]
- Bellinghieri, G.; Santoro, D.; Calvani, M.; Savica, V. Role of carnitine in modulating acute-phase protein synthesis in hemodialysis patients. J. Ren. Nutr. 2005, 15, 13–17. [Google Scholar] [CrossRef] [PubMed]
- Abe, M.; Okada, K.; Soma, M.; Matsumoto, K. Relationship between insulin resistance and erythropoietin responsiveness in hemodialysis patients. Clin. Nephrol. 2011, 75, 49–58. [Google Scholar] [PubMed]
- Abe, M.; Okada, K.; Maruyama, T.; Maruyama, N.; Matsumoto, K.; Soma, M. Relationship between erythropoietin responsiveness, insulin resistance, and malnutrition-inflammation-atherosclerosis (MIA) syndrome in hemodialysis patients with diabetes. Int. J. Artif. Organs 2011, 34, 16–25. [Google Scholar] [CrossRef] [PubMed]
- Reuter, A.E.; Faull, R.J.; Evans, A.M. l-carnitine supplementation in the dialysis population: Are Australian patients missing out? Nephrology 2008, 13, 3–16. [Google Scholar] [PubMed]
- Yamagishi, S. Advanced glycation end products and receptor-oxidative stress system in diabetic vascular complications. Ther. Aphel. Dial. 2009, 13, 534–539. [Google Scholar] [CrossRef]
- Furuya, R.; Kumagai, H.; Miyata, T.; Fukasawa, H.; Isobe, S.; Kinoshita, N.; Hishida, A. High plasma pentosidine level is accompanied with cardiovascular events in hemodialysis patients. Clin. Exp. Nephrol. 2012, 16, 421–426. [Google Scholar] [CrossRef] [PubMed]
- Rajasekar, P.; Anuradha, C.V. l-carnitine inhibits protein glycation in vitro and in vivo: Evidence for a role in diabetic management. Acta Diabetol. 2007, 44, 83–90. [Google Scholar] [CrossRef] [PubMed]
- Fukami, K.; Yamagishi, S.; Sakai, K.; Kaida, Y.; Adachi, T.; Ando, R.; Okuda, S. Potential inhibitory effects of l-carnitine supplementation on tissue advanced glycation end products in patients with hemodialysis. Rejuvenation Res. 2013, 16, 460–466. [Google Scholar] [CrossRef] [PubMed]
- Van Es, A.; Henny, F.C.; Kooistra, M.P.; Lobatto, S.; Scholte, H.R. Amelioration of cardiac function by l-carnitine administration in patients on hemodialysis. Contrib. Nephrol. 1992, 98, 28–35. [Google Scholar] [PubMed]
- Sayed-Ahmed, M.M.; Khattab, M.M.; Gad, M.Z.; Mostafa, N. l-carnitine prevents the progression of atherosclerotic lesions in hypercholesterolaemic rabbits. Pharmacol. Res. 2001, 44, 235–242. [Google Scholar] [CrossRef] [PubMed]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Higuchi, T.; Abe, M.; Yamazaki, T.; Mizuno, M.; Okawa, E.; Ando, H.; Oikawa, O.; Okada, K.; Kikuchi, F.; Soma, M. Effects of Levocarnitine on Brachial-Ankle Pulse Wave Velocity in Hemodialysis Patients: A Randomized Controlled Trial. Nutrients 2014, 6, 5992-6004. https://doi.org/10.3390/nu6125992
Higuchi T, Abe M, Yamazaki T, Mizuno M, Okawa E, Ando H, Oikawa O, Okada K, Kikuchi F, Soma M. Effects of Levocarnitine on Brachial-Ankle Pulse Wave Velocity in Hemodialysis Patients: A Randomized Controlled Trial. Nutrients. 2014; 6(12):5992-6004. https://doi.org/10.3390/nu6125992
Chicago/Turabian StyleHiguchi, Terumi, Masanori Abe, Toshio Yamazaki, Mari Mizuno, Erina Okawa, Hideyuki Ando, Osamu Oikawa, Kazuyoshi Okada, Fumito Kikuchi, and Masayoshi Soma. 2014. "Effects of Levocarnitine on Brachial-Ankle Pulse Wave Velocity in Hemodialysis Patients: A Randomized Controlled Trial" Nutrients 6, no. 12: 5992-6004. https://doi.org/10.3390/nu6125992
APA StyleHiguchi, T., Abe, M., Yamazaki, T., Mizuno, M., Okawa, E., Ando, H., Oikawa, O., Okada, K., Kikuchi, F., & Soma, M. (2014). Effects of Levocarnitine on Brachial-Ankle Pulse Wave Velocity in Hemodialysis Patients: A Randomized Controlled Trial. Nutrients, 6(12), 5992-6004. https://doi.org/10.3390/nu6125992




