Gluten-Free Diet in Children: An Approach to a Nutritionally Adequate and Balanced Diet
Abstract
:1. Introduction
| Gluten-Free Cereals | Gluten Containing Cereals |
|---|---|
| Cereals and minor cereals | Wheat Barley Rye Kamut Malt Triticale |
| Corn | |
| Rice | |
| Sorghum | |
| Oats * | |
| Teff | |
| Millet | |
| Pseudo-cereals | |
| Amaranth | |
| Quinoa | |
| Buckwheat | |
| Vegetable foods |  |
| Vegetables | |
| Fruits | |
| Nuts | |
| Other plant foods | All foods produced with any of the gluten containing cereals mentioned above. Numerous foods available in supermarkets and grocery stores, including meat products, sweets and beer, contain gluten. |
| Potatoes | |
| Tapioca | |
| Soybean | |
| Vegetable oils | |
| Animal foods | |
| Dairy products | |
| Egg | |
| Meat | |
| Fish |
1.1. Macronutrients
1.2. Micronutrients and Minerals
1.3. Dietary Fiber
2. Nutritional Imbalances in Children with Celiac Disease Following a GFD
| Common Nutrient Deficiencies in Subjects with Celiac Disease | |||
|---|---|---|---|
| At Diagnosis | GFD | GFD Products | Long-Term GFD |
| Calorie/protein | |||
| Fiber | Fiber | Fiber | Fiber |
| Iron | Iron | Iron | |
| Calcium | Calcium | ||
| Vitamin D | Vitamin D | ||
| Magnesium | Magnesium | ||
| Zinc | |||
| Folate, niacin, vitamin B12 | Folate, niacin, vitamin B12 | Folate, niacin, vitamin B12 | Folate, niacin, vitamin B12 |
| Riboflavin | Riboflavin | Riboflavin | Riboflavin |
3. Effects of Gluten-Free Diet on Anthropometric Parameters
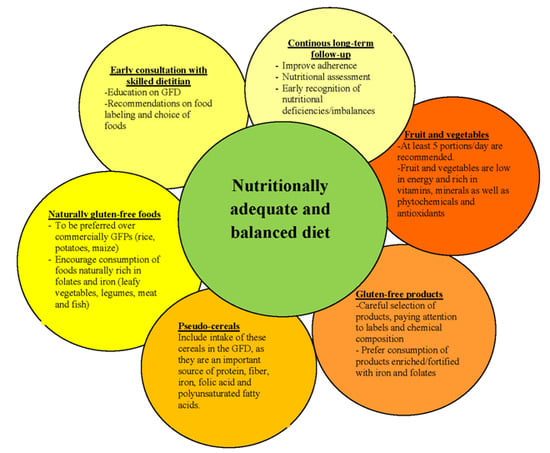
4. Dietary Advices for a Nutritionally Adequate and Balanced Diet in Children with Celiac Disease
4.1. Education and Compliance
4.2. Dietary Intake
4.3. Gluten-Free Foods
4.4. Pseudo-Cereals and Minor-Cereals
| Nutritional Characteristics of Amaranth, Buckwheat and Quinoa |
|---|
| High fiber content, 7–10 g/100 g, approximately the same as wheat fiber 9.5 g/100 g. |
| High protein content, 10.9%–15.2% of dry mass vs. 11.7% of dry mass in wheat. |
| High quality amino acids: lysine, arginine, histidine, methionine and cysteine. |
| Source of unsaturated fatty acids, in particular, α-linolenic acid. |
| High content of folic acid: quinoa and amaranth, 78.1 µg/100 g and 102 µg/100 g, respectively, vs. 40 µg/100 g in wheat. |
| Source of vitamins: B2, B6, riboflavin, vitamin C and E. |
| Source of minerals: the content is twice as high as in other cereals. |
4.5. Oats
4.6. Vitamins and Minerals
4.7. Nutritional Follow-Up
| Nutritional Follow-Up | |
|---|---|
| When? | How? |
| Diagnosis 6 months post commencement of GFD Annually post diagnosis | Accurate dietary history |
| Evaluation of nutritional status | |
| Anthropometric parameters, (weight, height, BMI) | |
| Physical examination (attention to signs of malnutrition) | |
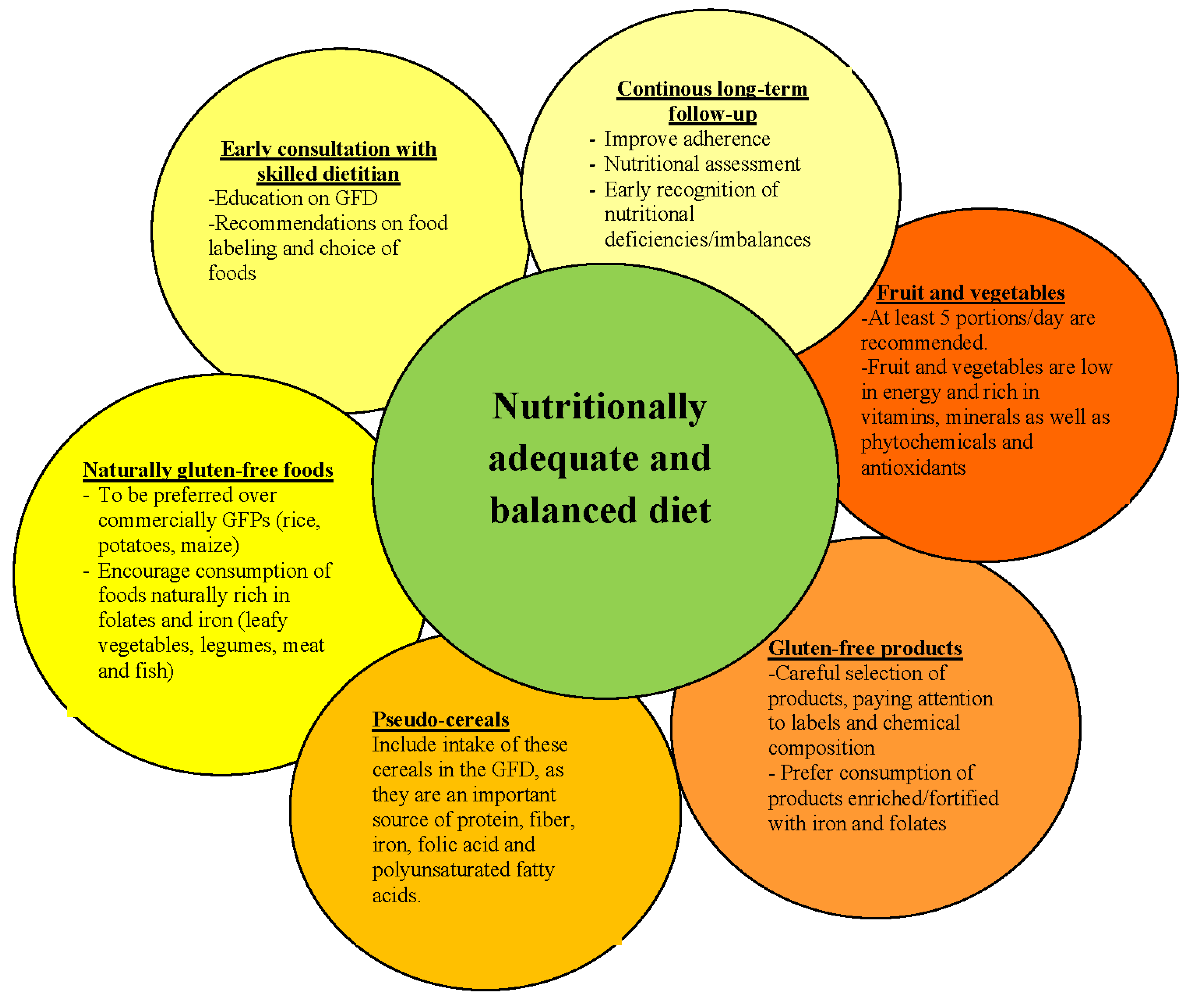
5. Conclusions
Conflicts of Interest
References
- Sjöström, H.; Lundin, K.E.; Molberg, O.; Körner, R.; McAdam, S.N.; Anthonsen, D.; Quarsten, H.; Norén, O.; Roepstorff, P.; Thorsby, E.; et al. Identification of a gliadin T-cell epitope in celiac disease: General importance of gliadin deaminidation for intestinal T cell recognition. Scand. J. Immunol. 1998, 48, 111–115. [Google Scholar] [CrossRef]
- Maiuri, L.; Ciacci, C.; Ricciardelli, I.; Vacca, L.; Raia, V.; Auricchio, S.; Picard, J.; Osman, M.; Quarantino, S.; Londei, M. Association between innate response to gliadin and activation of pathogenic T cells in coeliac disease. Lancet 2003, 362, 30–37. [Google Scholar] [CrossRef]
- Mowat, A.M. Coeliac disease—A meeting point for genetics, immunology and protein chemistry. Lancet 2003, 361, 1290–1292. [Google Scholar] [CrossRef]
- Ciacci, C.; Cirillo, M.; Cavallaro, R.; Mazzacca, G. Long-term follow-up of celiac adults on gluten-free diet: Prevalence and correlates of intestinal damage. Digestion 2002, 66, 178–185. [Google Scholar] [CrossRef]
- Alvarez-Jubete, L.; Arendt, E.K.; Gallagher, E. Nutritive value and chemical composition of pseudocereals as gluten-free ingredients. Int. J. Food Sci. Nutr. 2009, 60, 240–257. [Google Scholar] [CrossRef]
- Vega-Gàlvez, A.; Miranda, M.; Vergara, J.; Uribe, E.; Puente, L.; Martìnez, E.A. Nutrition facts and functional potential of quinoa (Chenopodium quinoa willd.), an ancient Andean grain: A review. J. Sci. Food Agric. 2010, 90, 2541–2547. [Google Scholar] [CrossRef]
- Thompson, T. Thiamin, riboflavin, and niacin contents of the gluten-free diet: Is there cause for concern? J. Am. Diet. Assoc. 1999, 99, 858–862. [Google Scholar] [CrossRef]
- Thompson, T. Folate, iron, and dietary fiber contents of the gluten-free die. J. Am. Diet. Assoc. 2000, 100, 1389–1396. [Google Scholar] [CrossRef]
- Hallert, C.; Grant, C.; Grehn, S.; Grännö, C.; Hultén, S.; Midhagen, G.; Strön, M.; Svensson, H.; Valdimarsson, T. Evidence of poor vitamin status in celiac patients on a gluten-free diet for 10 years. Aliment. Pharmacol. Ther. 2002, 16, 1333–1339. [Google Scholar] [CrossRef]
- Segura, M.E.; Rosell, C.M. Chemical composition and starch digestibility of different gluten-free breads. Plant Foods Hum. Nutr. 2011, 3, 224–230. [Google Scholar] [CrossRef]
- Jenkins, D.J.; Thorne, M.J.; Wolever, T.M.; Jenkins, A.L.; Rao, A.V.; Thompson, L.U. The effect of starch-protein interaction in wheat on the glycaemic response and rate of in vitro digestion. Am. J. Clin. Nutr. 1987, 45, 946–951. [Google Scholar]
- Berti, C.; Riso, P.; Monti, L.D.; Porrini, M. In vitro starch digestibility and in vivo glucose response of gluten-free foods and their gluten counterparts. Eur. J. Nutr. 2004, 43, 198–204. [Google Scholar]
- Caponio, F.; Summo, C.; Clodoveo, M.L.; Pasqualone, A. Evaluation of the nutritional quality of the lipid fraction of gluten-free biscuits. Eur. Food Res. Technol. 2008, 223, 135–139. [Google Scholar]
- Thompson, T.; Dennis, M.; Higgins, L.A.; Lee, A.R.; Sharrett, M.K. Gluten-free diet survey: Are Americans with celiac disease consuming recommended amounts of fibre, iron, calcium and grain food? J. Hum. Nutr. Diet. 2005, 18, 163–169. [Google Scholar] [CrossRef]
- Wild, D.; Robins, G.G.; Burley, V.J.; Howdle, P.D. Evidence of high sugar intake and low fiber and mineral intake in the gluten–free diet. Aliment. Pharmacol. Ther. 2010, 32, 573–581. [Google Scholar] [CrossRef]
- Kemppainen, T.; Uusitupa, M.; Janatuinen, E.; Järvinen, R.; Julkunen, R.; Pikkarainen, P. Intakes of nutrients and nutritional status in celiac patients. Scand. J. Gastroenterol. 1995, 30, 575–579. [Google Scholar] [CrossRef]
- Kinsey, L.; Burden, S.T.; Bannerman, E. A dietary survey to determine if patients with celiac disease are meeting current healthy eating guidelines and how their diet compares to that of British general population. Eur. J. Clin. Nutr. 2008, 62, 1333–1342. [Google Scholar] [CrossRef]
- Bardella, M.T.; Fredella, C.; Prampolini, L.; Molteni, N.; Giunta, A.M.; Bianchi, P.A. Body composition and dietary intakes in adult celiac disease patients consuming a strict gluten-free diet. Am. J. Clin. Nutr. 2000, 72, 937–939. [Google Scholar]
- Jameson, S. Coeliac, insulin-like growth factor, bone mineral density, and zinc. Scand. J. Gastroenterol. 2000, 35, 894–896. [Google Scholar] [CrossRef]
- Kupper, C. Dietary guidelines and implementation for celiac disease. Gastroenterology 2005, 128, S121–S127. [Google Scholar] [CrossRef]
- Mariani, P.; Viti, M.G.; Montuori, M.; La Vecchia, A.; Cipolletta, E.; Calvani, L.; Bonamico, M. The gluten-free diet: A nutritional risk factor for adolescents with celiac disease? J. Pediatr. Gastroenterol. Nutr. 1998, 27, 519–523. [Google Scholar]
- Hopman, E.G.; Le Cessie, S.; von Blomberg, B.M.; Mearin, M.L. Nutritional management of the gluten-free diet in young people with coeliac disease in The Netherlands. J. Paediatr. Gastroenterol. Nutr. 2006, 43, 102–108. [Google Scholar] [CrossRef]
- Öhlund, K.; Olsson, C.; Hernell, O.; Öhlund, L. Dietary shortcomings in children on a gluten-free diet. J. Hum. Nutr. Diet. 2010, 23, 294–300. [Google Scholar] [CrossRef]
- Zuccotti, G.; Fabiano, V.; Dilillo, D.; Picca, M.; Cravidi, C.; Brambilla, P. Intakes of nutrients in Italian children with celiac disease and the role of commercially available gluten-free products. J. Hum. Nutr. Diet. 2013, 26, 436–444. [Google Scholar] [CrossRef]
- Ferrara, P.; Cicala, M.; Tiberi, E.; Spadaccio, C.; Marcella, L.; Gatto, A.; Calzolari, P.; Castelluccio, G. High fat consumption in children with celiac disease. Acta Gastroenterol. Belg. 2009, 72, 296–300. [Google Scholar]
- Barera, G.; Mora, S.; Brambilla, P.; Ricotti, A.; Menni, L.; Beccio, S.; Bianchi, C. Body composition in children with celiac disease and the efffects of a gluten-free diet: A prospective case-control study. Am. J. Clin. Nutr. 2000, 72, 71–75. [Google Scholar]
- Cheng, J.; Brar, P.S.; Lee, A.R.; Green, P.H. Body mass index in celiac disease: Beneficial effect of a gluten-free diet. J. Clin. Gastroenterol. 2010, 44, 267–271. [Google Scholar] [CrossRef]
- Radlović, N.; Mladenović, M.; Leković, Z.; Zivanović, D.; Brdar, R.; Radlović, V.; Ristić, D.; Pavlović, M.; Stojsić, Z.; Vuletić, B.; et al. Effect of gluten-free diet on the growth and nutritional status of children with coeliac disease. Srp. Arh. Celok. Lek. 2009, 137, 632–637. [Google Scholar] [CrossRef]
- Venkatasubramani, N.; Telega, G.; Werlin, S.L. Obesity in pediatric celiac disease. J. Pediatr. Gastroenterol. Nutr. 2010, 51, 295–297. [Google Scholar]
- Brambilla, P.; Picca, M.; Dilillo, D.; Meneghin, F.; Cravidi, C.; Tischer, M.C.; Vivaldo, T.; Bedogni, G.; Zuccotti, G.V. Changes of body mass index in celiac children on a gluten-free diet. Nutr. Metab. Cardiovasc. Dis. 2013, 23, 177–182. [Google Scholar] [CrossRef]
- Kabbani, T.A.; Goldberg, A.; Kelly, C.P.; Pallav, K.; Tariq, S.; Peer, A.; Hasen, J.; Dennis, M.; Leffler, D.A. Body mass index and the risk of obesity in coeliac disease treated with gluten-free diet. Aliment. Pharmacol. Ther. 2012, 35, 723–729. [Google Scholar] [CrossRef]
- Valletta, E.; Fornaro, M.; Cipolli, M.; Conte, S.; Bissolo, F.; Danchielli, C. Celiac disease and obesity: Need for nutritional follow-up after diagnosis. Eur. J. Clin. Nutr. 2010, 64, 1371–1372. [Google Scholar] [CrossRef]
- Roma, E.; Roubani, A.; Kolia, E.; Panayiotou, J.; Zellos, A.; Syriopoulou, V.P. Dietary compliance and life style of children with celiac disease. J. Hum. Nutr. Diet. 2010, 23, 176–182. [Google Scholar] [CrossRef]
- Charalampopoulos, D.; Panayiotou, J.; Chouliaras, G.; Zellos, A.; Kyritsi, E.; Roma, E. Determinants of adherence to gluten-free diet in Greek children with celiac disease: A cross-sectional study. Eur. J. Clin. Nutr. 2013, 67, 615–619. [Google Scholar] [CrossRef]
- Codex Alimentarius Commission. Draft Revised Codex Standard for Foods for Special Dietary Use for Persons Intolerant to Gluten Joint FAO/WHO Food Standards Programme; WHO: Geneva, Switzerland, 2007. [Google Scholar]
- Dyner, L.; Drago, S.R.; PiÑeiro, A.; Sànchez, H.; Gonzàlez, R.; Villaamil, E.; Valencia, M.E. Composition and potential contribution of iron, calcium and zinc of bread and pasta made with wheat and amaranth flours. Arch. Latinoam. Nutr. 2007, 57, 69–77. [Google Scholar]
- Ötles, S.; Cagindi, Ö. Cereal based functional foods and nutraceuticals. Acta Sci. Pol. Technol. Aliment. 2006, 5, 107–112. [Google Scholar]
- Gorinstein, S.; Pawelzik, E.; Delgado-Licon, E.; Haruenkit, R.; Weisz, M.; Trakhtenberg, S. Characterization of pseudocereal and cereal proteins by protein and amino acid analyses. J. Sci. Food Agric. 2002, 82, 886–891. [Google Scholar] [CrossRef]
- Abdel-Aal, E.S.M.; Hucl, P. Amino acid composition and in vitro protein digestibility of selected ancient wheats and their products. J. Food Comp. Anal. 2002, 15, 737–747. [Google Scholar] [CrossRef]
- Yànez, E.; Zacarìas, I.; Granger, D.; Vàsquez, M.; Estèvez, A.M. Chemical and nutritional characterization of amaranthus (Amaranthus cruentus). Arch. Latinoam. Nutr. 1994, 44, 57–62. [Google Scholar]
- Adeyeye, A.; Ajewole, K. Chemical composition and fatty acid profiles of cereals in Nigeria. Food Chem. 1992, 44, 41–44. [Google Scholar] [CrossRef]
- Coulter, L.; Lorenz, K. Quinoa-composition, nutritional value, food applications. Lebensm. WissTechnol. 1990, 23, 203–207. [Google Scholar]
- Stevens, L.; Rashid, M. Gluten-free and regular foods: A cost comparison. Can. J. Diet. Pract. Res. 2008, 69, 147–150. [Google Scholar] [CrossRef]
- Hoffenberg, E.J.; Haas, J.; Drescher, A.; Barnhurst, R.; Osberg, I.; Bao, F.; Eisenbarth, G. A trial of oats in children with newly diagnosed celiac disease. J. Pediatr. 2000, 137, 361–366. [Google Scholar] [CrossRef]
- Höberg, L.; Laurin, P.; Faith-Magnusson, K.; Grant, C.; Grodzinsky, E.; Jansson, G.; Ascher, H.; Browaldh, L.; Hammersjö, J.A.; Lindberg, E.; et al. Oats to children with newly diagnosed celiac disease: A randomized double-blind study. Gut 2004, 53, 649–654. [Google Scholar] [CrossRef]
- Sadiq Butt, M.; Tahir-Nadeem, M.; Khan, M.K.; Shabir, R.; Butt, M.S. Oat: Unique among the cereals. Eur. J. Nutr. 2008, 47, 68–79. [Google Scholar] [CrossRef]
- Størsund, S.; Hulthèn, L.R.; Lenner, R.A. Beneficial effects of oats in the gluten-free diet of adults with special reference to nutrient status, symptoms and subjective experiences. Br. J. Nutr. 2003, 90, 101–107. [Google Scholar] [CrossRef]
- Lee, A.R.; Ng, D.L.; Dave, E.; Ciaccio, E.J.; Green, P.H. The effect of substituting alternative grains in the diet on the nutritional profile of the gluten-free diet. J. Hum. Nutr. Diet. 2009, 22, 359–363. [Google Scholar] [CrossRef]
- Stevenson, D.E.; Hurst, R.D. Polyphenolic phytochemicals—Just antioxidants or much more? Cell Mol. Life Sci. 2007, 64, 2900–2916. [Google Scholar] [CrossRef]
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Penagini, F.; Dilillo, D.; Meneghin, F.; Mameli, C.; Fabiano, V.; Zuccotti, G.V. Gluten-Free Diet in Children: An Approach to a Nutritionally Adequate and Balanced Diet. Nutrients 2013, 5, 4553-4565. https://doi.org/10.3390/nu5114553
Penagini F, Dilillo D, Meneghin F, Mameli C, Fabiano V, Zuccotti GV. Gluten-Free Diet in Children: An Approach to a Nutritionally Adequate and Balanced Diet. Nutrients. 2013; 5(11):4553-4565. https://doi.org/10.3390/nu5114553
Chicago/Turabian StylePenagini, Francesca, Dario Dilillo, Fabio Meneghin, Chiara Mameli, Valentina Fabiano, and Gian Vincenzo Zuccotti. 2013. "Gluten-Free Diet in Children: An Approach to a Nutritionally Adequate and Balanced Diet" Nutrients 5, no. 11: 4553-4565. https://doi.org/10.3390/nu5114553
APA StylePenagini, F., Dilillo, D., Meneghin, F., Mameli, C., Fabiano, V., & Zuccotti, G. V. (2013). Gluten-Free Diet in Children: An Approach to a Nutritionally Adequate and Balanced Diet. Nutrients, 5(11), 4553-4565. https://doi.org/10.3390/nu5114553