An Assessment of the Impact of Fortification of Staples and Condiments on Micronutrient Intake in Young Vietnamese Children
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Sampling
2.2. Food Consumption Analysis
2.3. Socioeconomic Status
2.4. Proposed Fortification Strategy
| Food vehicle | Standards |
|---|---|
| Wheat flour | 40 mg/kg of iron as NaFeEDTA; 50 mg/kg of zinc and 5 mg/kg of folic acid |
| Rice | 40 mg/kg of iron as micronized ferrous pyrophosphate; 5 mg/kg of zinc and 0.5 mg/kg of folic acid |
| Vegetable oil | 75 IU of retinyl palmitate per gram of vegetable oil |
| Sauces | 2.5 mg of iron as NaFeEDTA per 10 mL of sauces |
2.5. Statistical Analysis
2.6. Ethical Issues
3. Results
| n | Energy (Kcal) | Protein (g) | carbohydrates (g) | Lipid (g) | Iron (mg) | Zinc (mg) | Vitamin A (µg retinol activity equivalent) | Vitamin B1 (mg) | Vitamin B2 (mg) | |
|---|---|---|---|---|---|---|---|---|---|---|
| Total | 415 | 871.2 (617.9; 1199.3) | 33.1 (22.0; 45.0) | 140.7 (101.3; 199.9) | 15.4 (8.2; 23.8) | 4.8 (3.1; 7.4) | 4.3 (3.0; 6.2) | 182.8 (40.0; 387.9) | 0.5 (0.3; 0.7) | 0.3 (0.2; 0.5) |
| Sex | ||||||||||
| Boy | 212 | 884.2 (642.5; 1229.3) | 34.7 (22.7; 46.0) | 144.8 (103.5; 217.7) | 16.3 (8.5; 23.8) | 4.9 (3.2; 7.3) | 4.5 (3.1; 6.5) | 177.8 (40.3; 383.8) | 0.5 (0.3; 0.7) | 0.3 (0.2; 0.5) |
| Girl | 203 | 830.3 (601.0; 1126.4) | 32.3 (21.5; 44.8) | 131.7 (97.3; 185.8) | 14.3 (7.3; 23.8) | 4.7 (2.9; 7.4) | 4.2 (2.9; 6.1) | 190.7 (37.1; 397.3) | 0.5 (0.3; 0.7) | 0.4 (0.2; 0.6) |
| p 2 | p = 0.090 | p = 0.373 | p = 0.127 | p = 0.179 | p = 0.592 | p = 0.113 | p = 0.837 | p = 0.392 | p = 0.476 | |
| Age groups (month) | ||||||||||
| (6–11.9) | 48 | 597.8 (327.4; 871.0) | 22.7 (11.3; 36.0) | 69.6 (37.8; 110.6) | 11.5 (3.8; 21.6) | 3.0 (1.6; 4.1) | 3.0 (1.7; 6.1) | 57.7 (4.5; 224.1) | 0.3 (0.1; 0.7) | 0.2 (0.1; 0.4) |
| (12–23.9) | 97 | 760.7 (555.5; 1143.2) | 27.2 (17.8; 40.9) | 111.8 (82.3; 202.5) | 14.9 (7.8; 23.4) | 3.8 (2.4; 5.5) | 4.0 (2.4; 5.7) | 174.6 (49.4; 284.9) | 0.4 (0.2; 0.8) | 0.3 (0.1; 0.5) |
| (24–35.9) | 94 | 883.2 (647.0; 1173.8) | 34.7 (21.6; 45.5) | 148.4 (117.0; 189.8) | 14.4 (8.2; 25.7) | 5.3 (3.6; 8.3) | 4.1 (2.9; 6.2) | 174.4 (39.5; 430.7) | 0.4 (0.3; 0.7) | 0.3 (0.2; 0.6) |
| (36–59.9) | 176 | 957.9 (732.5; 1269.2) | 35.6 (25.6; 48.5) | 159.1 (118.6; 225.4) | 16.3 (9.8; 23.7) | 5.9 (4.2; 8.6) | 4.7 (3.6; 7.0) | 220.2 (78.1; 448.6) | 0.6 (0.3; 0.8) | 0.4 (0.2; 0.6) |
| p 2 | p < 0.001 | p < 0.001 | p < 0.001 | p = 0.159 | p < 0.001 | p < 0.001 | p < 0.001 | p < 0.01 | p < 0.001 | |
| Category socioeconomic | ||||||||||
| Extremely poor | 100 | 733.8 (578.0; 1039.7) | 23.4 (17.9; 35.5) | 139.3 (103.5; 192.6) | 9.4 (3.0; 19.7) | 3.9 (2.7; 5.8) | 3.5 (2.2; 4.9) | 121.8 (3.0; 273.5) | 0.3 (0.2; 0.6) | 0.2 (0.1; 0.4) |
| Poor | 70 | 990.0 (737.8; 1225.0) | 36.6 (25.5; 47.0) | 161.1 (119.0; 250.8) | 16.3 (11.6; 22.6) | 5.4 (3.7; 7.2) | 4.7 (3.5; 6.6) | 199.9 (73.9; 449.4) | 0.6 (0.3; 0.8) | 0.4 (0.2; 0.6) |
| Intermediate low | 60 | 883.2 (608.5; 1176.4) | 34.8 (22.1; 48.0) | 136.3 (101.4; 188.4) | 16.2 (8.6; 26.8) | 4.9 (2.7; 8.0) | 4.6 (2.9; 6.4) | 153.7 (32.9; 350.4) | 0.5 (0.3; 0.8) | 0.4 (0.1; 0.6) |
| Intermediate high | 75 | 833.1 (551.7; 1247.3) | 34.8 (23.5; 47.4) | 132.7 (80.4; 173.3) | 18.5 (8.9; 28.7) | 5.0 (2.9; 8.2) | 4.5 (2.9; 6.9) | 259.9 (103.2; 430.7) | 0.6 (0.3; 0.8) | 0.4 (0.2; 0.6) |
| Wealthy | 110 | 900.7 (686.3; 1248.0) | 36.3 (25.4; 48.6) | 134.9 (99.2; 214.0) | 16.4 (10.0; 26.1) | 5.1 (3.8; 8.1) | 4.8 (3.3; 6.4) | 186.7 (59.9; 430.3) | 0.5 (0.3; 0.7) | 0.4 (0.2; 0.6) |
| p 2 | p < 0.01 | p < 0.001 | p = 0.148 | p < 0.001 | p < 0.01 | p < 0.01 | p < 0.001 | p < 0.01 | p < 0.001 | |
| Areas | ||||||||||
| Rural | 223 | 916.7 (613.7; 1199.3) | 32.8 (21.5; 44.1) | 151.4 (99.9; 201.0) | 16.1 (8.5; 23.6) | 5.0 (3.2; 7.4) | 4.3 (3.1; 6.4) | 177.5(32.4; 372.0) | 0.5 (0.3; 0.7) | 0.3 (0.2; 0.5) |
| Urban | 192 | 804.2 (625.5; 1209.0) | 34.4 (22.4; 47.1) | 132.9 (102.0; 197.4) | 14.7 (8.0; 24.7) | 4.7 (3.1; 7.3) | 4.4 (2.9; 6.2) | 183.3 (53.0; 401.0) | 0.5 (0.3; 0.8) | 0.3 (0.2; 0.6) |
| p 2 | p = 0.363 | p = 0.396 | p = 0.354 | p = 0.768 | p = 0.988 | p = 0.868 | p = 0.308 | p = 0.671 | p = 0.271 |
| n | Rice | Wheat flour | Vegetable oil | Sauces | |
|---|---|---|---|---|---|
| Socioeconomic status | |||||
| Extremely poor | 100 | 100.0% | 19.0% | 18.0% | 47.0% |
| Poor | 70 | 100.0% | 15.7% | 34.3% | 54.3% |
| Intermediate low | 60 | 96.7% | 20.0% | 41.7% | 50.0% |
| Intermediate high | 75 | 97.3% | 12.0% | 45.3% | 50.7% |
| Wealthy | 110 | 96.4% | 15.5% | 52.7% | 52.7% |
| p 1 | p < 0.05 | ns | p < 0.001 | ns | |
| Sex | |||||
| Boys | 212 | 100.0% | 16.5% | 41.5% | 52.4% |
| Girls | 203 | 96.6% | 16.3% | 35.0% | 49.3% |
| p 1 | p < 0.05 | ns | ns | ns | |
| Age groups (month) | |||||
| (6–11.9) | 48 | 91.7% | 4.2% | 45.8% | 62.5% |
| (12–23.9) | 97 | 100.0% | 17.5% | 28.9% | 47.4% |
| (24–35.9) | 94 | 96.8% | 9.6% | 38.3% | 42.6% |
| (36–59.9) | 176 | 100.0% | 22.7% | 41.5% | 54.0% |
| p 1 | p < 0.05 | p < 0.01 | ns | ns | |
| Areas | |||||
| Rural | 223 | 100.0% | 18.8% | 33.6% | 51.1% |
| Urban | 192 | 96.9% | 13.5% | 43.8% | 50.5% |
| p 1 | p < 0.05 | ns | p < 0.05 | ns | |
| Total population | 415 | 98.6% | 16.4% | 38.3% | 50.8% |
| n | Rice | n | Wheat flour | n | Vegetable oil | n | Sauces | |
|---|---|---|---|---|---|---|---|---|
| Total | 408 | 170.0 (110.0; 250.0) | 68 | 43.0 (14.3; 76.0) | 159 | 6.0 (3.0; 10.0) | 211 | 4.0 (2.0; 9.0) |
| Sex | ||||||||
| Boy | 212 | 180.0 (120.0; 263.0) | 35 | 50.0 (15.0; 80.0) | 88 | 6.0 (3.0; 10.0) | 111 | 4.0 (2.0; 8.0) |
| Girl | 196 | 157.0 (104.0; 240.0) | 33 | 35.0 (12.5; 75.5) | 71 | 6.0 (3.0; 9.0) | 100 | 4.5 (2.5; 9.0) |
| p 2 | p = 0.150 | p = 0.507 | p = 0.583 | p = 0.926 | ||||
| Category socioeconomic | ||||||||
| Extremely poor | 100 | 165.0 (111.8; 243.0) | 19 | 50.0 (14.0; 76.0) | 18 | 5.0 (3.0; 9.8) | 47 | 4.0 (2.0; 7.0) |
| Poor | 70 | 204.4 (126.0; 295.0) | 11 | 40.0 (12.0; 110.0) | 24 | 6.5 (4.0; 11.5) | 38 | 5.0 (2.0; 10.5) |
| Intermediate low | 58 | 170.0 (117.8; 254.0) | 12 | 45.0 (15.6; 92.8) | 25 | 5.0 (3.0; 9.0) | 30 | 6.0 (2.0; 8.3) |
| Intermediate high | 73 | 150.0 (100.0; 219.0) | 9 | 35.0 (12.0; 51.5) | 34 | 6.0 (4.0; 9.3) | 38 | 5.0 (3.0; 9.0) |
| Wealthy | 106 | 164.0 (108.8; 247.8) | 17 | 50.0 (18.5; 67.5) | 58 | 5.5 (3.0; 10.6) | 58 | 4.0 (2.0; 9.5) |
| p 2 | p = 0.168 | p = 0.813 | p = 0.661 | p = 0.683 | ||||
| Age groups (month) | ||||||||
| (6–11.9) | 44 | 70.0 (47.5; 120.0) | 2 | 6.0 (6.0; 6.0) | 22 | 5.5 (2.0; 15.0) | 30 | 2.5 (2.0; 7.5) |
| (12–23.9) | 97 | 125.0 (93.5; 250.0) | 17 | 40.0 (16.0; 75.5) | 28 | 6.0 (3.3; 13.2) | 46 | 4.0 (2.0; 6.0) |
| (24–35.9) | 91 | 185.0 (124.0; 230.0) | 9 | 50.0 (23.5; 88.8) | 36 | 5.5 (4.0; 9.8) | 40 | 3.5 (1.6; 8.8) |
| (36–59.9) | 176 | 195.0 (136.5; 284.5) | 40 | 47.0 (12.8; 84.5) | 73 | 6.0 (3.0; 9.0) | 95 | 5.0 (3.0; 10.0) |
| p 2 | p < 0.001 | p = 0.150 | p = 0.864 | p < 0.05 | ||||
| Areas | ||||||||
| Rural | 223 | 175.0 (105.0; 270.0) | 42 | 47.5 (19.5; 81.9) | 75 | 6.0 (3.0; 15.0) | 114 | 5.0 (2.0; 11.3) |
| Urban | 186 | 167.5 (114.8; 247.8) | 26 | 35.0 (12.0; 71.3) | 84 | 5.0 (3.0; 9.0) | 97 | 4.0 (2.0; 7.0) |
| p 2 | p = 0.883 | p = 0.167 | p < 0.05 | p = 0.196 |
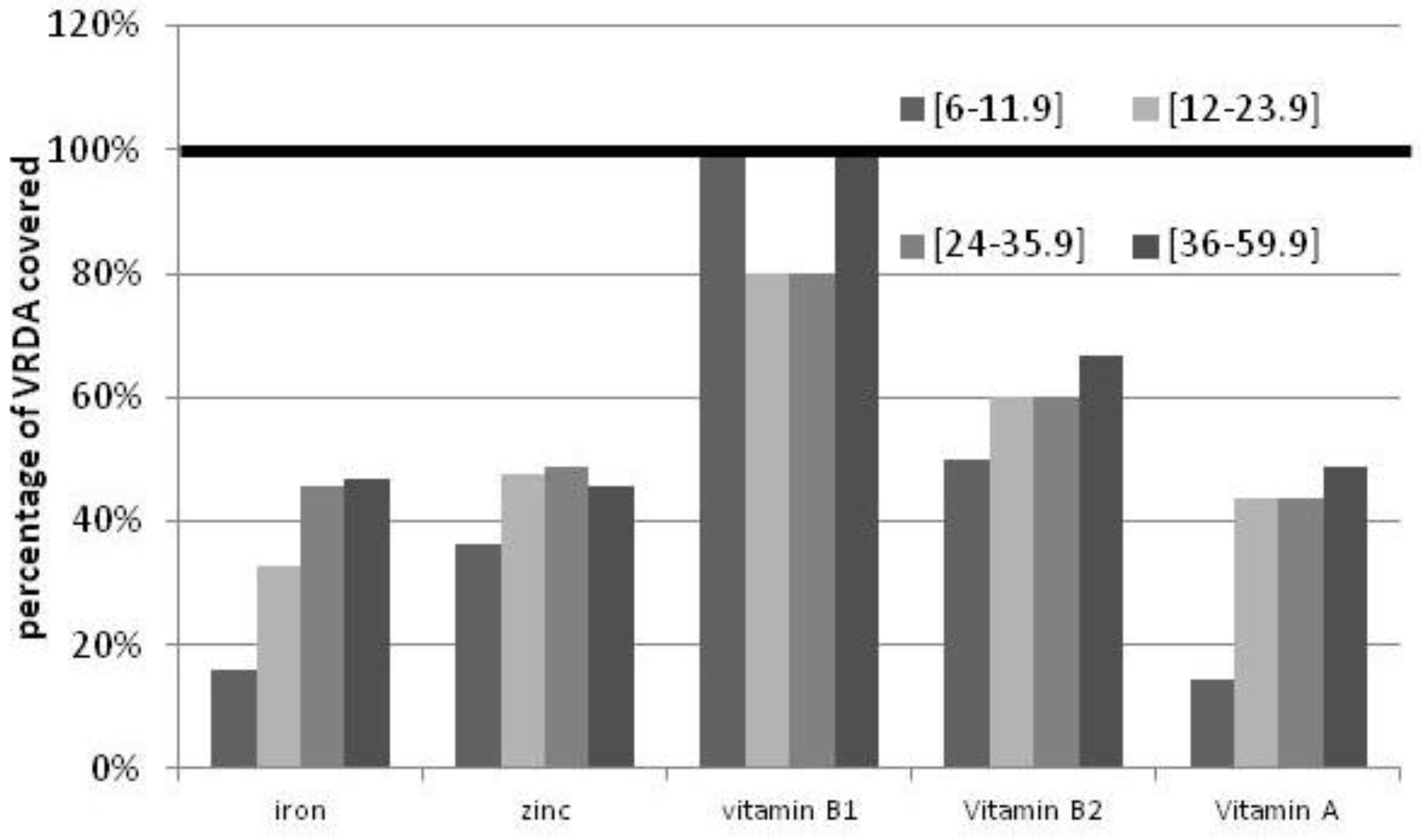
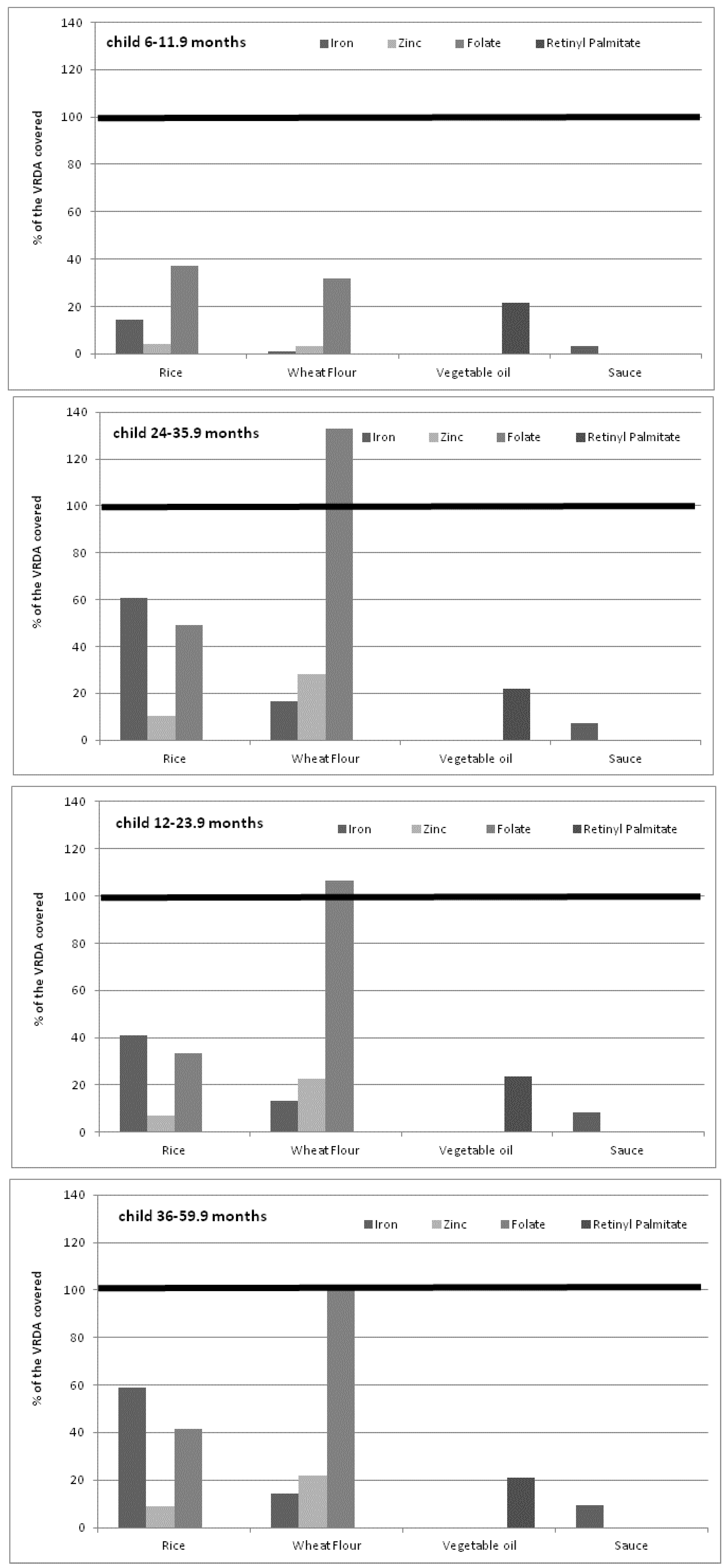
| Nutrient contribution per child from individual food fortification | ||||||||
|---|---|---|---|---|---|---|---|---|
| Age groups | Fortified wheat flour | Fortified sauces | Fortified vegetable oil | Fortified rice | ||||
| Iron (mg/day) | Zinc (mg/day) | Folate (µg/day) | Iron (mg/day) | Retinyl palmitate (µg RAE/day) | Iron (mg/day) | Zinc (mg/day) | Folate (µg/day) | |
| (6–11.9) | 0.2 (0.2–0.2) | 0.3 (0.3–0.3) | 26 (26–26) | 0.6 (0.5–1.8) | 86.6 (31.5–236.3) | 2.7 (1.8–4.6) | 0.3 (0.2–0.6) | 30 (20–51) |
| (12–23.9) | 1.5 (0.6–2.9) | 1.9 (0.8–3.6) | 170 (68–321) | 1.0 (0.5–1.4) | 94.5 (52.0–207.9) | 4.8 (3.6–9.5) | 0.6 (0.4–1.2) | 53 (40–106) |
| (24–35.9) | 1.9 (0.9–3.4) | 2.4 (1.1–4.2) | 213 (100–377) | 0.8 (0.4–2.1) | 86.6 (63.0–154.4) | 7.0 (4.7–8.7) | 0.9 (0.6–1.1) | 79 (53–98) |
| (36–59.9) | 1.8 (0.5–3.2) | 2.2 (0.6–4.0) | 200 (54–359) | 1.2 (0.7–2.4) | 94.5 (47.3–141.8) | 7.4 (5.2–10.8) | 0.9 (0.6–1.4) | 83 (58–121) |
4. Discussion
4.1. Vegetable Oil Fortification: A Solution for Additional Vitamin A Intake and Possibly Vitamin D Intake
4.2. Rice and Sauces Fortification to Increase Zinc, Iron and Folate Intakes
4.3. Wheat Flour Fortification to Increase Zinc, Iron and Folate Intakes: A Possibility but Not a Priority
4.4. Limitations of the Study
5. Conclusions
Acknowledgments
Conflict of Interest
References
- Black, R.E.; Allen, L.H.; Bhutta, Z.A.; Caulfield, L.E.; de Onis, M.; Ezzati, M.; Mathers, C.; Rivera, J. Maternal and child undernutrition: Global and regional exposures and health consequences. Lancet 2008, 371, 243–260. [Google Scholar]
- Victora, C.G.; Adair, L.; Fall, C.; Hallal, P.C.; Martorell, R.; Richter, L.; Sachdev, H.S. Maternal and child undernutrition: Consequences for adult health and human capital. Lancet 2008, 371, 340–357. [Google Scholar]
- World Health Organization (WHO), Global Prevalence of Vitamin A Deficiency in Populations at Risk 1995–2005; WHO: Geneva, Switzerland, 2009.
- Sanghvi, T.; van Ameringen, M.; Baker, J.; Fiedler, J.; Borwankar, R.; Phillips, M.; Houston, R.; Ross, J.; Heymann, H.; Dary, O. Vitamin and mineral deficiencies technical situation analysis: A report for the ten year strategy for the reduction of vitamin and mineral deficiencies. Food Nutr. Bull. 2007, 28, S160–S219. [Google Scholar]
- Fischer Walker, C.L.; Ezzati, M.; Black, R.E. Global and regional child mortality and burden of disease attributable to zinc deficiency. Eur. J. Clin. Nutr. 2009, 63, 591–597. [Google Scholar]
- Nga, T.T.; Winichagoon, P.; Dijkhuizen, M.A.; Khan, N.C.; Wasantwisut, E.; Furr, H.; Wieringa, F.T. Multi-micronutrient-fortified biscuits decreased prevalence of anemia and improved micronutrient status and effectiveness of deworming in rural Vietnamese school children. J. Nutr. 2009, 139, 1013–1021. [Google Scholar] [CrossRef]
- Lien do, T.K.; Nhung, B.T.; Khan, N.C.; Hop le, T.; Nga, N.T.; Hung, N.T.; Kiers, J.; Shigeru, Y.; te Biesebeke, R. Impact of milk consumption on performance and health of primary school children in rural vietnam. Asia Pac. J. Clin. Nutr. 2009, 18, 326–334. [Google Scholar]
- Nhien, N.V.; Khan, N.C.; Ninh, N.X. Micronutrient deficiencies and anemia among preschool children in rural Vietnam. Asia Pac. J. Clin. Nutr. 2008, 17, 48–55. [Google Scholar]
- Laillou, A.; Pham, T.V.; Tran, N.T.; Le, H.T.; Wieringa, F.; Rohner, F.; Fortin, S.; Le, M.B.; Tran do, T.; Moench-Pfanner, R.; et al. Micronutrient deficits are still public health issues among women and young children in vietnam. PLoS One 2012, 7, e34906. [Google Scholar]
- Young Child Nutrition Working Group: Formulation Subgroup. Formulations for fortified complementary foods and supplements: Review of successful products for improving the nutritional status of infants and young children. Food Nutr. Bull. 2009, 30, S239–S255.
- Nguyen, P.H.; Menon, P.; Ruel, M.; Hajeebhoy, N. A situational review of infant and young child feeding practices and interventions in Viet Nam. Asia Pac. J. Clin. Nutr. 2011, 20, 359–374. [Google Scholar]
- Ministry of Health, Plan of Action for Infant and Young Child Feeding Period 2006–2010; Ministry of Health: Hanoi, Vietnam, 2006.
- National Institute of NutritionGeneral Statistic OfficeThe Progress of Malnutrition Reduction among Children under 5 Years old and Their Mothers. Impact of Nutritional Intervention Programmes in Vietnam 1999–2004; Statistical Publishing House: Hanoi, Vietnam, 2005.
- Sazawal, S.; Dhingra, U.; Dhingra, P.; Hiremath, G.; Sarkar, A.; Dutta, A.; Menon, V.P.; Black, R.E. Micronutrient fortified milk improves iron status, anemia and growth among children 1–4 years: A double masked, randomized, controlled trial. PLoS One 2010, 5, e12167. [Google Scholar]
- Rivera, J.A.; Shamah, T.; Villalpando, S.; Monterrubio, E. Effectiveness of a large-scale iron-fortified milk distribution program on anemia and iron deficiency in low-income young children in Mexico. Am. J. Clin. Nutr. 2010, 91, 431–439. [Google Scholar]
- Semba, R.D.; Moench-Pfanner, R.; Sun, K.; de Pee, S.; Akhter, N.; Rah, J.H.; Campbell, A.A.; Badham, J.; Bloem, M.W.; Kraemer, K. Iron-fortified milk and noodle consumption is associated with lower risk of anemia among children aged 6–59 mo in Indonesia. Am. J. Clin. Nutr. 2010, 92, 170–176. [Google Scholar]
- Thuy, P.V.; Berger, J.; Davidsson, L.; Khan, N.C.; Lam, N.T.; Cook, J.D.; Hurrell, R.F.; Khoi, H.H. Regular consumption of nafeedta-fortified fish sauce improves iron status and reduces the prevalence of anemia in anemic Vietnamese women. Am. J. Clin. Nutr. 2003, 78, 284–290. [Google Scholar]
- Van Thuy, P.; Berger, J.; Nakanishi, Y.; Khan, N.C.; Lynch, S.; Dixon, P. The use of nafeedta-fortified fish sauce is an effective tool for controlling iron deficiency in women of childbearing age in rural Vietnam. J. Nutr. 2005, 135, 2596–2601. [Google Scholar]
- Ministry of Health (MOH), Circular for Issuing National Technical Regulations for Micronutrients Fortified Foods; MOH: Hanoi, Vietnam, 2011; 18.
- Vietnam FAIRS Country Report 2008; GAIN Report No. VM8057; Global Agriculture Information Network (GAIN): Hanoi, Vietnam, 2008. Available online: http://www.fas.usda.gov/gainfiles/200809/146295727.pdf (accessed on 21 August 2012).
- FTA Research & Consultant, Staple and Condiment Market Survey; Global Alliance for Improved Nutrition (GAIN): Ho Chi Minh, Vietnam, 2010.
- Kyritsi, A.; Tzia, C.; Karathanos, V.T. Vitamin fortified rice grain using spraying and soaking methods. LWT Food Sci. Technol. 2011, 44, 312–320. [Google Scholar] [CrossRef]
- Prom-u-thai, C.; Rerkasem, B.; Fukai, S.; Huang, L. Iron fortification and parboiled rice quality: Appearance, cooking quality and sensory attributes. J. Sci. Food Agric. 2009, 89, 2565–2571. [Google Scholar] [CrossRef]
- Yoo, J.; Alavi, S.; Adhikari, K.; Haub, M.D.; Aberle, R.A.; Huber, G. Rice-shaped extruded kernels: Physical, sensory and nutritional properties. Int. J. Food Prop. 2011. [Google Scholar]
- Li, Y.O.; Diosady, L.L.; Jankowski, S. Folic acid stability in the presence of various formulation components including iron compounds in fortified extruded ultra rice® over prolonged storage at 40 °C and 60% relative humidity (RH). Int. J. Food Sci. Technol. 2011, 46, 379–385. [Google Scholar] [CrossRef]
- Bagni, U.V.; Baiao, M.R.; Santos, M.M.; Luiz, R.R.; Veiga, G.V. Effect of weekly rice fortification with iron on anemia prevalence and hemoglobin concentration among children attending public daycare centers in Rio de Janeiro, Brazil (in Portuguese). Cad. Saude Publica 2009, 25, 291–302. [Google Scholar] [CrossRef]
- Beinner, M.A.; Velasquez-Meléndez, G.; Pessoa, M.C.; Greiner, T. Iron-fortified rice is as efficacious as supplemental iron drops in infants and young children. J. Nutr. 2010, 140, 49–53. [Google Scholar] [CrossRef]
- Angeles-Agdeppa, I.; Saises, M.; Capanzana, M.; Juneja, L.R.; Sakaguchi, N. Pilot-scale commercialization of iron-fortified rice: Effects on anemia status. Food Nutr. Bull. 2011, 32, 3–12. [Google Scholar]
- Radhika, M.S.; Nair, K.M.; Kumar, R.H.; Rao, M.V.; Ravinder, P.; Reddy, C.G.; Brahmam, G.N. Micronized ferric pyrophosphate supplied through extruded rice kernels improves body iron stores in children: A double-blind, randomized, placebo-controlled midday meal feeding trial in Indian schoolchildre. Am. J. Clin. Nutr. 2011, 94, 1202–1210. [Google Scholar] [CrossRef]
- Le Hung, Q.; de Vries, P.J.; Giao, P.T.; Binh, T.Q.; Nam, N.V.; Kager, P.A. Anemia, malaria and hookworm infections in a Vietnamese ethnic minority. Southeast Asian J. Trop. Med. Public Health 2005, 36, 816–821. [Google Scholar]
- Dop, M.C.; Le, B.M.; Laillou, A.; Sénémaud, B.; Nguyen, C.K.; Khoi, H.H. Validation of the 24-hour Recall against the Weighing Method at Household Level-Advantage of Comparing Methods on the Same and Separate Days: A Case Study from Vietnam. In Proceedings of Fourth International Conference on Dietary Assessment Methods, Tucson, AZ, USA, 17–20 September 2000.
- Rustein, S.O.; Johnson, K. The DHS Wealth Index; DHS Comperative Reports No. 6; ORC Macro: Calverton, MD, USA, 2004.
- Rutstein, S. The DHS wealth index: Approaches for rural and urban areas. Available online: http://www.iywg.org/ar/popline/dhs-wealth-index-approaches-rural-and-urban-areas (accessed on 15 February 2012).
- World Health Organization, Recommendations on Wheat and Maize Flour Fortification. Meeting Report: Interim Consensus Statement; WHO: Geneva, Switzerland, 2009.
- Chavasit, V.; Nopburabutr, P.; Kongkachuichai, R. Combating iodine and iron deficiencies through the double fortification of fish sauce, mixed fish sauce, and salt brine. Food Nutr. Bull. 2003, 24, 200–207. [Google Scholar]
- Ministry of HealthNational Institute of NutritionGeneral Nutrition Survey; Medical Publishing House: Hanoi, Vietnam, 2000.
- Thuy, P.V.; Nga, T.T. Vietnam National Micronutrient Survey, 2010; National Institute of Nutrition: Hanoi, Vietnam, 2011. [Google Scholar]
- Khan, N.C.; Hoan, P.V. Vietnam recommended dietary allowances 2007. Asia Pac. J. Clin. Nutr. 2008, 17, S409–S415. [Google Scholar]
- Allen, L.; de Benoist, B.; Dray, O.; Hurrell, R. Guidelines on Food Fortification with Micronutrients; World Health Organization: Geneva, Switzerland, 2006. [Google Scholar]
- Ministry of Public HealthNational Institute of NutritionNutritive Composition Table of Vietnamese Food; Medical Publishing House: Hanoi, Vietnam, 2000.
- West, K.P.J.; Darnton-Hill, I. Vitamin A Deficiency. In Nutrition and Health in Developing Countries, 2nd ed; Humana Press: New York, NY, USA, 2008; pp. 377–433. [Google Scholar]
- Phuong, H.; Menon, P.; Ruel, M.; Hajeebhoy, N. A situational review of infant and young child feeding practices and interventions in Viet Nam. Asia Pac. J. Clin. Nutr. 2011, 20, 359–374. [Google Scholar]
- Bruyeron, O.; Denizeau, M.; Berger, J.; Treche, S. Marketing complementary foods and supplements in Burkina Faso, Madagascar, and Vietnam: Lessons learned from the Nutridev program. Food Nutr. Bull. 2010, 31, S154–S167. [Google Scholar]
- Garcia-Casal, M.N.; Layrisse, M.; Solano, L.; Baron, M.A.; Arguello, F.; Llovera, D.; Ramirez, J.; Leets, I.; Tropper, E. Vitamin A and beta-carotene can improve nonheme iron absorption from rice, wheat and corn by humans. J. Nutr. 1998, 128, 646–650. [Google Scholar]
- Dary, O.; Mora, J.O. Food fortification to reduce vitamin A deficiency: International vitamin A consultative group recommendations. J. Nutr. 2002, 132, 2927S–2933S. [Google Scholar]
- United Nations Economic and Social Commission for Asia and the Pacific (ESCAP). Rising Food Prices and Inflation in the Asia-Pacific Region: Causes, Impact and Policy Response; MPDD policy briefs No. 7. March 2011. Available online: http://www.unescap.org/pdd/publications/me_brief/mpdd-pb-7.pdf (accessed on 11 January 2012).
- Bloem, M.W.; Semba, R.D.; Kraemer, K. Castel gandolfo workshop: An introduction to the impact of climate change, the economic crisis, and the increase in the food prices on malnutrition. J. Nutr. 2010, 140, 132S–135S. [Google Scholar] [CrossRef]
- West, K.P., Jr.; Mehra, S. Vitamin A intake and status in populations facing economic stress. J. Nutr. 2010, 140, 201S–207S. [Google Scholar] [CrossRef]
- Pereira, S.M.; Begum, A. Prevention of vitamin A deficiency. Am. J. Clin. Nutr. 1969, 22, 858–862. [Google Scholar]
- Perlas, L.A.; Florentino, R.F.; Fuertes, R.T.; Madriaga, J.R.; Cheong, R.L.; Desnacido, J.A.; Marcos, J.M.; Cabrera, M.I. Vitamin A status of filipino preschool children given a massive oral dose. Southeast Asian J. Trop. Med. Public Health 1996, 27, 785–791. [Google Scholar]
- Arroyave, G.; Mejia, L.A.; Aguilar, J.R. The effect of vitamin A fortification of sugar on the serum vitamin A levels of preschool Guatemalan children: A longitudinal evaluation. Am. J. Clin. Nutr. 1981, 34, 41–49. [Google Scholar]
- Muhilal; Permeisih, D.; Idjradinata, Y.R.; Muherdiyantiningsih; Karyadi, D. Vitamin A-fortified monosodium glutamate and health, growth, and survival of children: A controlled field trial. Am. J. Clin. Nutr. 1988, 48, 1271–1276. [Google Scholar]
- Favaro, R.; Ferreira, J.; Desai, I.; de Oliveira, J.D. Studies on fortification of refined soybean oil with all-trans retinyl palmitate in Brazil: Stability during cooking and storage. J. Food Comp. Anal. 1991, 4, 237–244. [Google Scholar] [CrossRef]
- Pettifor, J.M. Nutritional rickets: Deficiency of vitamin D, calcium, or both? A. J. Clin. Nutr. 2004, 80, 1725S–1729S. [Google Scholar]
- Laillou, A.; Wieringa, F.; Nga, T.T.; Thuy, P.V.; Mai, L.B.; Fortin, S.; Hop, L.T.; Moench-Pfanner, R.; Berger, J. Calcium and Vitamin D Deficiency among Rural and Urban Vietnamese Preschool Children and Women of Reproductive Age. In World Summit of Nutrition; World Public Health Association: Rio De Janeiro, Brazil, 2012. [Google Scholar]
- Holick, M.F.; Chen, T.C. Vitamin D deficiency: A worldwide problem with health consequences. Am. J. Clin. Nutr. 2008, 87, 1080S–1086S. [Google Scholar]
- Beard, J. Recent evidence from human and animal studies regarding iron status and infant development. J. Nutr. 2007, 137, 524S–530S. [Google Scholar]
- Lozoff, B.; Beard, J.; Connor, J.; Barbara, F.; Georgieff, M.; Schallert, T. Long-lasting neural and behavioral effects of iron deficiency in infancy. Nutr. Rev. 2006, 64 discussion S72-S91, S34–S43. [Google Scholar] [CrossRef]
- Moretti, D.; Zimmermann, M.B.; Muthayya, S.; Thankachan, P.; Lee, T.C.; Kurpad, A.V.; Hurrell, R.F. Extruded rice fortified with micronized ground ferric pyrophosphate reduces iron deficiency in Indian schoolchildren: A double-blind randomized controlled trial. Am. J. Clin. Nutr. 2006, 84, 822–829. [Google Scholar]
- MacPhail, A.P.; Patel, R.C.; Bothwell, T.H.; Lamparelli, R.D. EDTA and the absorption of iron from food. Am. J. Clin. Nutr. 1994, 59, 644–648. [Google Scholar]
- Brown, K.H.; Hambidge, K.M.; Ranum, P. Zinc fortification of cereal flours: Current recommendations and research needs. Food Nutr. Bull. 2010, 31, 62S–74S. [Google Scholar]
- Joseph, M.; Beesabathuni, K.; Matthias, D. Enhancing the iron content of milled rice with path’s ultra rice® technology. Available online: http://www.path.org/publications/files/TS_ur_enh_iron_pos.pdf (accessed on 19 February 2012).
- National Institute of NutritionUnited Nations International Children’s Emergency Fund (UNICEF)A Review of the Nutrition Situation in Vietnam 2009–2010; United Nations International Children’s Emergency Fund: Hanoi, Vietnam, 2011.
© 2012 by the authors; licensee MDPI, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Laillou, A.; Mai, L.B.; Hop, L.T.; Khan, N.C.; Panagides, D.; Wieringa, F.; Berger, J.; Moench-Pfanner, R. An Assessment of the Impact of Fortification of Staples and Condiments on Micronutrient Intake in Young Vietnamese Children. Nutrients 2012, 4, 1151-1170. https://doi.org/10.3390/nu4091151
Laillou A, Mai LB, Hop LT, Khan NC, Panagides D, Wieringa F, Berger J, Moench-Pfanner R. An Assessment of the Impact of Fortification of Staples and Condiments on Micronutrient Intake in Young Vietnamese Children. Nutrients. 2012; 4(9):1151-1170. https://doi.org/10.3390/nu4091151
Chicago/Turabian StyleLaillou, Arnaud, Le Bach Mai, Le Thi Hop, Nguyen Cong Khan, Dora Panagides, Frank Wieringa, Jacques Berger, and Regina Moench-Pfanner. 2012. "An Assessment of the Impact of Fortification of Staples and Condiments on Micronutrient Intake in Young Vietnamese Children" Nutrients 4, no. 9: 1151-1170. https://doi.org/10.3390/nu4091151
APA StyleLaillou, A., Mai, L. B., Hop, L. T., Khan, N. C., Panagides, D., Wieringa, F., Berger, J., & Moench-Pfanner, R. (2012). An Assessment of the Impact of Fortification of Staples and Condiments on Micronutrient Intake in Young Vietnamese Children. Nutrients, 4(9), 1151-1170. https://doi.org/10.3390/nu4091151




