Preoperative Nutrition-Based Interventions in Children Undergoing Cardiac Surgeries—A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Eligibility Criteria
2.2. Search Strategy
2.3. Data Collection and Management
2.4. Risk of Bias Assessment
2.5. Data Analysis
3. Results
3.1. Study Selection
3.2. Study Characteristics
3.2.1. Interventional Studies
3.2.2. Observational Studies
3.3. Risk of Bias
3.4. Effects of Any Modified Fatty Acid Emulsion
3.4.1. Enteral DHA in Sunflower Oil vs. Sunflower Oil Only
Efficacy
Safety
- Postoperative sepsis and severe sepsis, in both the intention-to-treat (ITT; RR = 0.67, 95%CI, 0.34 to 1.30; and RR = 0.89, 95% CI, 0.51 to 1.56, respectively; n = 55) and per-protocol (PP; RR = 0.38, 95% CI, 0.12 to 1.15; RR = 0.28, 95% CI, 0.03 to 2.26, respectively; n = 34) analyses;
- Any postoperative organ dysfunction, including: respiratory (RR = 0.19; 95% CI, 0.03 to 1.4), cardiovascular (RR = 0.28; 95% CI, 0.03 to 2.26), hematological (RR = 0.16; 95% CI, 0.01 to 2.87), hepatic (RR = 0.37; 95% CI, 0.02 to 8.55), and renal dysfunctions (RR = 0.16; 95% CI, 0.01 to 2.87);
- Vomiting events in the ICU (RR = 1.13, 95% CI, 0.18 to 7.09; n = 34);
- Mortality in either the ITT analysis (RR = 0.21; 0.03 to 1.66; n = 55) or in the PP analysis (RR = 0.37; 0.02 to 8.55; n = 34); none of the deaths were related to DHA administration [21].
3.4.2. Intravenous 50% MCT, 40% LCT and 10% Fish Oil Emulsion (MCT/LCT/Fish Oil) vs. Fully LCT Emulsion
Efficacy
- Mean duration of the ICU stay (MD = −7.4 days, 95% CI, −10.86 to −3.94);
- Mean duration of mechanical ventilation (MD = −2.1 days, 95% CI, −2.86 to −1.34);
- Mean length of hospital stay (MD = −5.1 days, 95% CI, −8.77 to −1.43) [22].
Safety
3.4.3. High-Dose Cholecalciferol vs. Usual Care/No Intervention
Efficacy
Safety
Compliance
3.4.4. Effect of Human Milk Fortifier vs. Placebo in Breastfed Infants
Efficacy
Safety
3.4.5. Effects of Preoperative Nutrition-Based Protocols
Efficacy of Preoperative Trophic Breast Milk Feeds
- Efficacy
- Safety
A 2-Week vs. 1-Week Preoperative Nutrition Support
- Efficacy of the 2-week vs. 1-week preoperative nutrition support
- A shorter mean length of ICU stay (MD = 36.5 h, 95% CI, −44.61 to −28.39) [16];
- A shorter mean hospital length of stay (MD = −40.9 days, 95%CI, −65.26 to −16.54) [16];
- A shorter mean duration of postoperative mechanical ventilation was found (MD = −14.0 h, 95% CI, −17.95 to −10.05) [16];
- A higher mean postoperative feeding volume intake, measured before discharge (MD = 7.53 mL/feed, 95%CI, 0.99 to 14.07) [16].
- Other feeding-related outcomes, including: day of enteral feeding initiation (RR = 1.33, 95% CI, 0.88 to 2.0 3, and RR = 1.00, 95% CI, 0.34 to 2.93, for day 1 and 2, respectively), route of feeding (oral: RR = 1.42, 95% CI, 0.95 to 2.12, vs. oral and nasogastric tube: RR = 0.38, 95% CI, 0.12 to 1.21), and feeding frequency (every 2 h: RR = 1.19, 95% CI, 0.93 to 1.51, vs. every 3 h: RR = 0.25, 95% CI, 0.03 to 2.05) [16];
- The proportion of children with successful extubation (RR = 1.05, 95% CI, 0.92 to 1.2), early extubation (≤48 h) (RR = 1.2, 95% CI, 0.9 to 1.61), late extubation (>48 h) (RR = 0.33, 95% CI, 0.04 to 2.94), and reintubation (RR = 0.5, 95%CI, 0.05 to 5.08) [16].
Efficacy of a 1-Month Preoperative Nutrition Support vs. No Support
Effects of Any Preoperative Feeding vs. No Feeding
- Effectiveness
- Safety
Effectiveness of Meeting Versus Not Meeting Center-Recommended Preoperative Caloric Intake Requirements (Cohort Study)
Preoperative Fortified vs. Unfortified Nutrition
- Effectiveness
- Safety
3.4.6. Preoperative Exclusive Human Milk and Direct Breastfeeding
3.5. Quality of Evidence
4. Discussion
4.1. Summary
4.2. Comparison with Other Systematic Reviews
4.3. Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| BDG | Bidirectional Glenn |
| BMI | Body mass index |
| CHD | Congenital heart disease |
| CI | Confidence interval |
| CS-AKI | Cardiac surgery-associated acute kidney injury |
| DHA | Docosahexaenoic acid |
| ERAS | Enhanced recovery after surgery |
| GER | Gastroesophageal reflux |
| GRADE | Grading of Recommendations, Assessment, Development, and Evaluation |
| HMF | Human milk fortifier |
| HR | Hazard ratio |
| ICU | Intensive care unit |
| ITT | Intention-to-treat |
| IV | Intravenous |
| LCT | Long-chain triglycerides |
| MD | Mean difference |
| MCT | Medium-chain triglycerides |
| MV | Mechanical ventilation |
| n | Number of participants |
| ND | No difference |
| NEC | Necrotizing enterocolitis |
| NeoC3 | Neonatal Cardiac Care Collaborative |
| NOS | Newcastle–Ottawa Scale |
| OR | Odds ratio |
| PP | Per-protocol |
| PRISMA | Preferred Reporting Items for Systematic Reviews and Meta-Analyses |
| RCT | Randomized controlled trial |
| RoB 2 | Revised Cochrane risk-of-bias tool for randomized trials |
| RR | Risk ratio |
| SD | Standard deviation |
| STRONG | Screening Tool for Risk on Nutritional Status and Growth |
References
- Diao, J.; Chen, L.; Wei, J.; Shu, J.; Li, Y.; Li, J.; Zhang, S.; Wang, T.; Qin, J. Prevalence of Malnutrition in Children with Congenital Heart Disease: A Systematic Review and Meta-Analysis. J. Pediatr. 2022, 242, 39–47.e4. [Google Scholar] [CrossRef] [PubMed]
- Abbas, Q.; Ali, H.; Ahuja, A.K.; Bhatti, O.A.; Ladak, S.; Khan, I.; Rehman, A.; Mohsin, S.; Shah, I.; Ilyas, A.; et al. Preoperative nutrition status in children with congenital heart disease and its impact on postoperative outcomes: A systematic review and meta-analysis. Sci. Rep. 2025, 15, 25738. [Google Scholar] [CrossRef]
- Ljungqvist, O.; Scott, M.; Fearon, K.C. Enhanced Recovery After Surgery: A Review. JAMA Surg. 2017, 152, 292–298. [Google Scholar] [CrossRef] [PubMed]
- Lau, C.S.; Chamberlain, R.S. Enhanced Recovery After Surgery Programs Improve Patient Outcomes and Recovery: A Meta-analysis. World J. Surg. 2017, 41, 899–913. [Google Scholar] [CrossRef]
- Hidayah, B.A.; Toh, Z.A.; Cheng, L.J.; Syahzarin, B.D.; Zhu, Y.; Pölkki, T.; He, H.; Mali, V.P. Enhanced recovery after surgery in children undergoing abdominal surgery: Meta-analysis. BJS Open 2023, 7, zrac147. [Google Scholar] [CrossRef] [PubMed]
- Practice Guidelines for Preoperative Fasting and the Use of Pharmacologic Agents to Reduce the Risk of Pulmonary Aspiration: Application to Healthy Patients Undergoing Elective Procedures: An Updated Report by the American Society of Anesthesiologists Task Force on Preoperative Fasting and the Use of Pharmacologic Agents to Reduce the Risk of Pulmonary Aspiration. Anesthesiology 2017, 126, 376–393.
- Frykholm, P.; Disma, N.; Andersson, H.; Beck, C.; Bouvet, L.; Cercueil, E.; Elliott, E.; Hofmann, J.; Isserman, R.; Klaucane, A.; et al. Pre-operative fasting in children: A guideline from the European Society of Anaesthesiology and Intensive Care. Eur. J. Anaesthesiol. 2022, 39, 4–25. [Google Scholar] [CrossRef]
- Mehta, N.M.; Skillman, H.E.; Irving, S.Y.; Coss-Bu, J.A.; Vermilyea, S.; Farrington, E.A.; McKeever, L.; Hall, A.M.; Goday, P.S.; Braunschweig, C. Guidelines for the Provision and Assessment of Nutrition Support Therapy in the Pediatric Critically Ill Patient: Society of Critical Care Medicine and American Society for Parenteral and Enteral Nutrition. JPEN J. Parenter. Enter. Nutr. 2017, 41, 706–742. [Google Scholar] [CrossRef]
- Kołodziej, M.; Skulimowska, J. A Systematic Review of Clinical Practice Guidelines on the Management of Malnutrition in Children with Congenital Heart Disease. Nutrients 2024, 16, 2778. [Google Scholar] [CrossRef]
- Raval, M.V.; Brockel, M.A.; Kolaček, S.; Simpson, K.E.; Spoede, E.; Starr, K.N.P.; Wulf, K.L. Key Strategies for Optimizing Pediatric Perioperative Nutrition-Insight from a Multidisciplinary Expert Panel. Nutrients 2023, 15, 1270. [Google Scholar] [CrossRef]
- Weimann, A.; Bezmarevic, M.; Braga, M.; Correia, M.; Funk-Debleds, P.; Gianotti, L.; Gillis, C.; Hübner, M.; Inciong, J.F.B.; Jahit, M.S.; et al. ESPEN guideline on clinical nutrition in surgery—Update 2025. Clin. Nutr. 2025, 53, 222–261. [Google Scholar] [CrossRef] [PubMed]
- Page, M.J.; Moher, D.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. PRISMA 2020 explanation and elaboration: Updated guidance and exemplars for reporting systematic reviews. BMJ 2021, 372, n160. [Google Scholar] [CrossRef]
- Higgins, J.P.T.; Thomas, J.; Chandler, J.; Cumpston, M.; Li, T.; Page, M.; Welch, V.; Flemyng, E. Cochrane Handbook for Systematic Reviews of Interventions Version 6.4 (Updated August 2023). Cochrane. 2023. Available online: www.training.cochrane.org/handbook (accessed on 20 December 2025).
- Sterne, J.A.C.; Savović, J.; Page, M.J.; Elbers, R.G.; Blencowe, N.S.; Boutron, I.; Cates, C.J.; Cheng, H.Y.; Corbett, M.S.; Eldridge, S.M.; et al. RoB 2: A revised tool for assessing risk of bias in randomised trials. BMJ 2019, 366, l4898. [Google Scholar] [CrossRef]
- Hozo, S.P.; Djulbegovic, B.; Hozo, I. Estimating the mean and variance from the median, range, and the size of a sample. BMC Med. Res. Methodol. 2005, 5, 13. [Google Scholar] [CrossRef]
- El-Ganzoury, M.M.; El-Farrash, R.A.; Ahmed, G.F.; Hassan, S.I.; Barakat, N.M. Perioperative nutritional prehabilitation in malnourished children with congenital heart disease: A randomized controlled trial. Nutrition 2021, 84, 111027. [Google Scholar] [CrossRef]
- Lin, Y.F.; Lin, W.H.; Lin, S.H.; Zhang, Q.L.; Chen, Q.; Zheng, Y.R. Using Human Milk Fortifiers to Improve the Preoperative Nutritional Status of Infants With Non-restricted Ventricular Septal Defect. Front. Pediatr. 2022, 10, 900012. [Google Scholar] [CrossRef] [PubMed]
- Zyblewski, S.C.; Nietert, P.J.; Graham, E.M.; Taylor, S.N.; Atz, A.M.; Wagner, C.L. Randomized Clinical Trial of Preoperative Feeding to Evaluate Intestinal Barrier Function in Neonates Requiring Cardiac Surgery. J. Pediatr. 2015, 167, 47–51.e1. [Google Scholar] [CrossRef]
- Xu, L.P.; Lin, S.H.; Zhang, Q.L.; Zheng, Y.; Lin, G. Short-Term Nutritional Support Improves The Preoperative Nutritional Status of Infants With Non-Restrictive Ventricular Septal Defect: A Prospective Controlled Study. Heart Surg. Forum 2022, 25, E745–E749. [Google Scholar] [CrossRef]
- Schünemann, H.; Brożek, J.; Guyatt, G.; Oxman, A. (Eds.) GRADE Handbook for Grading Quality of Evidence and Strength of Recommendations; Updated October 2013; The GRADE Working Group: Hamilton, ON, Canada, 2013; Available online: http://guidelinedevelopment.org/handbook (accessed on 20 December 2025).
- Bernabe-Garcia, M.; Lopez-Alarcon, M.; Villegas-Silva, R.; Mancilla-Ramirez, J.; Rodriguez-Cruz, M.; Maldonado-Hernandez, J.; Chavez-Rueda, K.A.; Blanco-Favela, F.; Espinoza-Garcia, L.; Lagunes-Salazar, S. Beneficial Effects of Enteral Docosahexaenoic Acid on the Markers of Inflammation and Clinical Outcomes of Neonates Undergoing Cardiovascular Surgery: An Intervention Study. Ann. Nutr. Metab. 2016, 69, 15–23. [Google Scholar] [CrossRef] [PubMed]
- Larsen, B.M.; Goonewardene, L.A.; Joffe, A.R.; Van Aerde, J.E.; Field, C.J.; Olstad, D.L.; Clandinin, M.T. Pre-treatment with an intravenous lipid emulsion containing fish oil (eicosapentaenoic and docosahexaenoic acid) decreases inflammatory markers after open-heart surgery in infants: A randomized, controlled trial. Clin. Nutr. 2012, 31, 322–329. [Google Scholar] [CrossRef]
- McNally, J.D.; O’Hearn, K.; Fergusson, D.A.; Lougheed, J.; Doherty, D.R.; Maharajh, G.; Weiler, H.; Jones, G.; Khamessan, A.; Redpath, S.; et al. Prevention of post-cardiac surgery vitamin D deficiency in children with congenital heart disease: A pilot feasibility dose evaluation randomized controlled trial. Pilot Feasibility Stud. 2020, 6, 159. [Google Scholar] [CrossRef]
- Jelveh-Moghaddam, H.; Fani, K.; Hekmat, M.; Azari, A.A. The effects of Vitamin D3 in pediatric patients undergoing congenital heart surgery. J. Cell. Mol. Anesth. 2020, 5, 66–73. [Google Scholar]
- Sahu, M.K.; Bipin, C.; Niraghatam, H.V.; Karanjkar, A.; Singh, S.P.; Rajashekar, P.; Ramakrishnan, L.; Devagourou, V.; Upadhyay, A.D.; Choudhary, S.K. Vitamin D Deficiency and Its Response to Supplementation as Stoss Therapy in Children with Cyanotic Congenital Heart Disease Undergoing Open Heart Surgery. J. Card. Crit. Care 2019, 3, 17–23. [Google Scholar] [CrossRef]
- Bertrandt, R.A.; Gist, K.; Hasson, D.; Zang, H.; Reichle, G.; Krawczeski, C.; Winlaw, D.; Bailly, D.; Goldstein, S.; Selewski, D.; et al. Cardiac Surgery-Associated Acute Kidney Injury in Neonates Undergoing the Norwood Operation: Retrospective Analysis of the Multicenter Neonatal and Pediatric Heart and Renal Outcomes Network Dataset, 2015–2018. Pediatr. Crit. Care Med. 2024, 25, e246–e257. [Google Scholar] [CrossRef]
- Dabbagh, A.; Miller, S.; McCulloch, M.; Rosenthal, G.; Conaway, M.; White, S. Preoperative Oral Feeding in Infants with Congenital Heart Disease Within the First Month of Life is Associated with a Higher Likelihood of Freedom From Tube Feeding at Time of Postoperative Discharge. Pediatr. Cardiol. 2025, 47, 221–228. [Google Scholar] [CrossRef]
- Elgersma, K.M.; Wolfson, J.; Fulkerson, J.A.; Georgieff, M.K.; Looman, W.S.; Spatz, D.L.; Shah, K.M.; Uzark, K.; McKechnie, A.C. Human Milk Feeding and Direct Breastfeeding Improve Outcomes for Infants With Single Ventricle Congenital Heart Disease: Propensity Score-Matched Analysis of the NPC-QIC Registry. J. Am. Heart Assoc. 2023, 12, e030756. [Google Scholar] [CrossRef]
- Menon, S.C.; McCandless, R.T.; Mack, G.K.; Lambert, L.M.; McFadden, M.; Williams, R.V.; Minich, L.L. Clinical outcomes and resource use for infants with hypoplastic left heart syndrome during bidirectional Glenn: Summary from the Joint Council for Congenital Heart Disease National Pediatric Cardiology Quality Improvement Collaborative registry. Pediatr. Cardiol. 2013, 34, 143–148. [Google Scholar] [CrossRef] [PubMed]
- Murray, S.E.; Zimmerman, D.; Patel, S.S. Preoperative Feeding Fortification Among Infants with Congenital Heart Disease is Associated with Higher Growth Velocity in the First 30 Days Post-repair and Lower BMI Percentile for Age at 10 Years: A Retrospective Cohort Study. Pediatr. Cardiol. 2025, 46, 394–400. [Google Scholar] [CrossRef]
- Scahill, C.J.; Graham, E.M.; Atz, A.M.; Bradley, S.M.; Kavarana, M.N.; Zyblewski, S.C. Preoperative Feeding Neonates With Cardiac Disease. World J. Pediatr. Congenit. Heart Surg. 2017, 8, 62–68. [Google Scholar] [CrossRef]
- Toms, R.; Jackson, K.W.; Dabal, R.J.; Reebals, C.H.; Alten, J.A. Preoperative trophic feeds in neonates with hypoplastic left heart syndrome. Congenit. Heart Dis. 2015, 10, 36–42. [Google Scholar] [CrossRef]
- Zacharias, P.; Blinci, J.; Shenoy, R.; Lee, J.; Singh, Y. Impact of the Pre-Operative Standardized Nutritional Protocol in Infants with Congenital Heart Disease (CHD). J. Cardiovasc. Dev. Dis. 2025, 12, 166. [Google Scholar] [CrossRef]
- Venna, A.; Reid, K.; Davis, S.; Gai, J.; d’Udekem, Y.; Clauss, S. Preoperative Feeding in Single Ventricle Neonates is Predictive of Shorter Time to Goal Feed. Congenit. Heart Dis. 2022, 17, 505–518. [Google Scholar] [CrossRef]
- Iliopoulos, I.; Burke, R.; Hannan, R.; Bolivar, J.; Cooper, D.S.; Zafar, F.; Rossi, A. Preoperative Intubation and Lack of Enteral Nutrition are Associated with Prolonged Stay After Arterial Switch Operation. Pediatr. Cardiol. 2016, 37, 1078–1084. [Google Scholar] [CrossRef]
- Kataria-Hale, J.; Osborne, S.W.; Hair, A.; Hagan, J.; Pammi, M. Preoperative Feeds in Ductal-Dependent Cardiac Disease: A Systematic Review and Meta-analysis. Hosp. Pediatr. 2019, 9, 998–1006. [Google Scholar] [CrossRef] [PubMed]
- Bell, D.; Suna, J.; Marathe, S.P.; Perumal, G.; Betts, K.S.; Venugopal, P.; Alphonso, N.; QPCR Group. Feeding Neonates and Infants Prior to Surgery for Congenital Heart Defects: Systematic Review and Meta-Analysis. Children 2022, 9, 1856. [Google Scholar] [CrossRef] [PubMed]
- Mills, K.I.; Kim, J.H.; Fogg, K.; Goldshtrom, N.; Graham, E.M.; Kataria-Hale, J.; Osborne, S.W.; Figueroa, M. Nutritional Considerations for the Neonate With Congenital Heart Disease. Pediatrics 2022, 150, e2022056415G. [Google Scholar] [CrossRef]
- Silva-Gburek, J.; May, K.; Walvoord, B.; Lozano, C.; Coss-Bu, J.A. Perioperative Nutrition in Pediatric Patients with Congenital Heart Disease and Heart Failure. Nutrients 2025, 17, 3609. [Google Scholar] [CrossRef]
- Szentirmay, L.S.; Heywood, A.; James-Nunez, K.; Trivedi, A.; Dalrymple, H. Preoperative enteral nutrition in neonates with congenital heart disease: A review of literature. J. Neonatal Nurs. 2025, 31, 101667. [Google Scholar] [CrossRef]
- Vandenbroucke, J.P.; von Elm, E.; Altman, D.G.; Gøtzsche, P.C.; Mulrow, C.D.; Pocock, S.J.; Poole, C.; Schlesselman, J.J.; Egger, M.; STROBE Initiative. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE): Explanation and elaboration. Int. J. Surg. 2014, 12, 1500–1524. [Google Scholar] [CrossRef]
- European Medicines Agency (EMA). Guideline on Registry-Based Studies. EMA/426390/2021. 22 October 2021. Available online: https://www.ema.europa.eu/en/documents/scientific-guideline/guideline-registry-based-studies_en.pdf (accessed on 20 December 2025).
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef]



| Autor (Year) | Selection (0–4) | Comparability (0–2) | Outcome (0–3) | Overall (0–9) |
|---|---|---|---|---|
| Bertrandt 2024 [26] | ★★★ | ★ | ★★★ | 7 |
| Zacharias 2025 [33] | ★ | ★★★ | 5 | |
| Venna 2022 [34] | ★★★★ | ★ | ★★★ | 9 |
| Toms 2015 [32] | ★★★ | ★★★ | 6 | |
| Scahill 2017 [31] | ★★★★ | ★ | ★★★ | 9 |
| Murray 2025 [30] | ★★★ | ★ | ★★★ | 7 |
| Menon 2013 [29] | ★★★★ | ★ | ★★★ | 9 |
| Elgersma 2023 [28] | ★★★★ | ★ | ★★★ | 8 |
| Dabbagh 2025 [27] | ★★★★ | ★ | ★★★ | 9 |
| Intervention/Exposure vs. Comparator | Number of Studies and Participants (n) | Efficacy/Effectiveness | Safety |
|---|---|---|---|
| Intravenous 50% MCT, 40% LCT and 10% fish oil vs fully LCT emulsion [22] | 1 RCT, n = 32 | ↓ ICU stay ↓ Hospital stay ↓ MV | Sepsis—ND |
| Enteral DHA in sunflower oil vs sunflower oil only [21] | 1 RCT, n = 34 | ↓ ICU stay | Intraoperative bleeding—ND Postoperative sepsis—ND Bleeding—ND Severe sepsis—ND Organ dysfunctions—ND Vomiting at ICU—ND Mortality—ND |
| High-dose vitamin D vs usual care/no intervention [23,24,25] | 2 RCTs, n = 101 | ICU stay—ND (2 RCTs, n = 101) MV—ND (2 RCTs, n = 101) ↓ Hospital stay (1 RCT, n = 41) ↑ MV (1 non-RCT, n = 60) | Adverse events—ND (2 RCT, n = 101) Mortality ND (2 RCT, n = 101) Need for inotropes ND (1 RCT, n = 41) |
| Human milk fortifier vs placebo [17] | 1 RCT, n = 58 | ↑ Albumins and Prealbumins ↑ STRONG Kids score Hemoglobin ND | Preoperative adverse events—ND No NEC No death |
| Preoperative trophic breast milk feeding vs no enteral feeding [18] | 1 RCT, n = 27 | Postoperative feeding intolerance ND Nasogastric tube dependence | Postoperative NEC—ND GER medication—ND Mortality—ND |
| Preoperative nutrition support 2 weeks vs 1 week [16] | 1 RCT, n = 40 | ↓ ICU stay ↓ Hospital stay ↓ MV ↑ Postoperative feeding intake other feeding related outcomes—ND ↑ Weight z-score pre- and postoperatively Height z-score—inconsistent Albumins—ND Hemoglobulin—ND | Sepsis—ND Successful extubation—ND Feeding-related adverse events ND |
| 1-month preoperative nutrition support vs no support [19] | 1 RCT, n = 80 | ↓ ICU and hospital stay ↓ Preoperative STRONG Kids Score ↑ Albumins, Prealbumins and Hemoglobulin | Not reported |
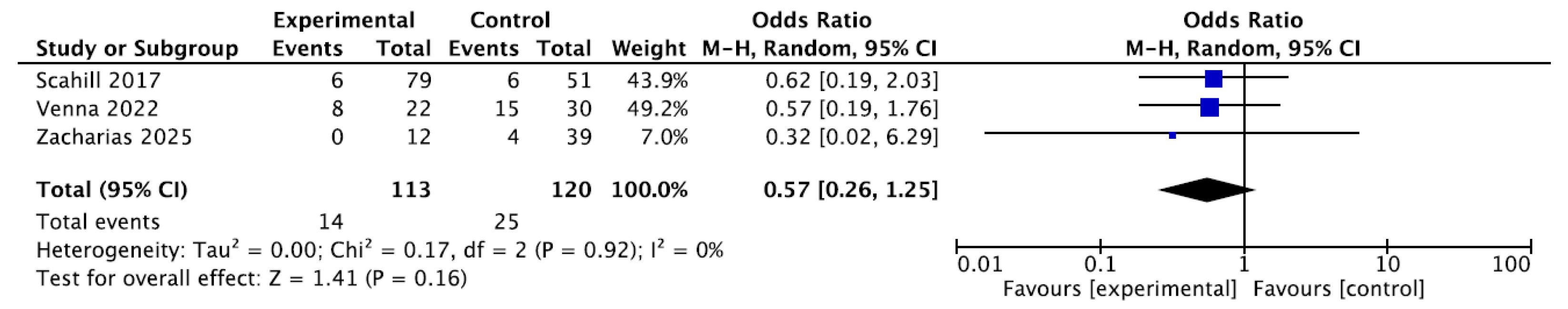
| Any preoperative feeding vs no feeding [26,27,31,32,33,34,35] | 7 studies, n = 917 | ICU stay—ND (3 studies, n = 226) ↓ Hospital stay (4 studies, n = 278) ↓ Days to achieve full feeds postoperatively (3 studies, n = 138) MV duration—inconsistent results (2 studies, n = 175) Postoperative weight z-score—ND (2 studies, n = 181) ↑ Albumins (1 study, n = 45) ↑ Children on full feeding (1 study, n = 235) | ↓ CS-AKI (1 study, n = 347) NEC—ND (3 studies, n = 232), Postoperative infection rate—ND (1 study, n = 45) Mortality risk—ND (2 studies, n = 97) |
| Achieved vs not achieved center-recommended pre-operative caloric intake requirements [29] | 1 study, n = 160 | ↑ Postoperative hospital stay | Not reported |
| Preoperative fortified nutrition (≥22 kcal/oz) vs unfortified nutrition (20 kcal/oz) [30] | 1 study, n = 84 | ↑ ICU stay ↑ Hospital stay ↓ Postoperative weight MV duration—ND BMI-for-age percentiles at 5 and 10 years | Surgical site infection risk—ND |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Stróżyk, A.; Halicki, P.; Kołodziej, M.; Horvath, A.; Buczyński, M.; Pietrzak, R. Preoperative Nutrition-Based Interventions in Children Undergoing Cardiac Surgeries—A Systematic Review and Meta-Analysis. Nutrients 2026, 18, 544. https://doi.org/10.3390/nu18030544
Stróżyk A, Halicki P, Kołodziej M, Horvath A, Buczyński M, Pietrzak R. Preoperative Nutrition-Based Interventions in Children Undergoing Cardiac Surgeries—A Systematic Review and Meta-Analysis. Nutrients. 2026; 18(3):544. https://doi.org/10.3390/nu18030544
Chicago/Turabian StyleStróżyk, Agata, Piotr Halicki, Maciej Kołodziej, Andrea Horvath, Michał Buczyński, and Radosław Pietrzak. 2026. "Preoperative Nutrition-Based Interventions in Children Undergoing Cardiac Surgeries—A Systematic Review and Meta-Analysis" Nutrients 18, no. 3: 544. https://doi.org/10.3390/nu18030544
APA StyleStróżyk, A., Halicki, P., Kołodziej, M., Horvath, A., Buczyński, M., & Pietrzak, R. (2026). Preoperative Nutrition-Based Interventions in Children Undergoing Cardiac Surgeries—A Systematic Review and Meta-Analysis. Nutrients, 18(3), 544. https://doi.org/10.3390/nu18030544







