The Influence of Socio-Economic Factors on Diet and Active Lifestyle in the Spanish Female Population
Abstract
1. Introduction
2. Materials and Methods
2.1. Subjects
- −
- population between 18 and 45 years of age
- −
- of Spanish nationality
- −
- resident in Spain
- −
- of female sex
- −
- respondents who had a chronic illness that could affect their diet.
- −
- respondents who, at the time of the survey, were in a situation that temporarily deregulated their usual diet: hospitalization, prison admission, etc.
2.2. Ethical Approval
2.3. Instruments and Variables
2.4. Data Collection
- Personal social networks (LinkedIn, Twitter, Facebook).
- Chain mails and WhatsApp messages.
- Mailing to different establishments throughout Spain, selected because of the heterogeneous public (pharmacies, clinics, etc.).
- An Instagram account @elretonutricional was created and used specifically to disseminate the survey, from which several professionals and influencers were contacted.
2.5. Healthy Nutrition Index
2.6. Statistical Analysis
3. Results
- −
- Sample size: 14.784 valid surveys.
- −
- Age: 53.49% (7.908 people) aged between 18 and 30 years old and 46.51% aged between 31 and 45 years old (6.876 people). Mean = 30.41, Mode = 23, Median = 30.
- −
- Level of studies: 30.56% (4.518) with basic education (No studies, Primary school, Vocational training or Secondary School) and 69.44% (10.266 respondents) with higher education (Degree, Master’s, or Doctorate).
- −
- Income level: 51.86% (6.974 respondents) with a low purchasing power (less than EUR 2200 per month for the family nucleus) and 48.14% (6.473 people) with a medium-high purchasing power.
4. Discussion
Study Strengths and Weaknesses
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
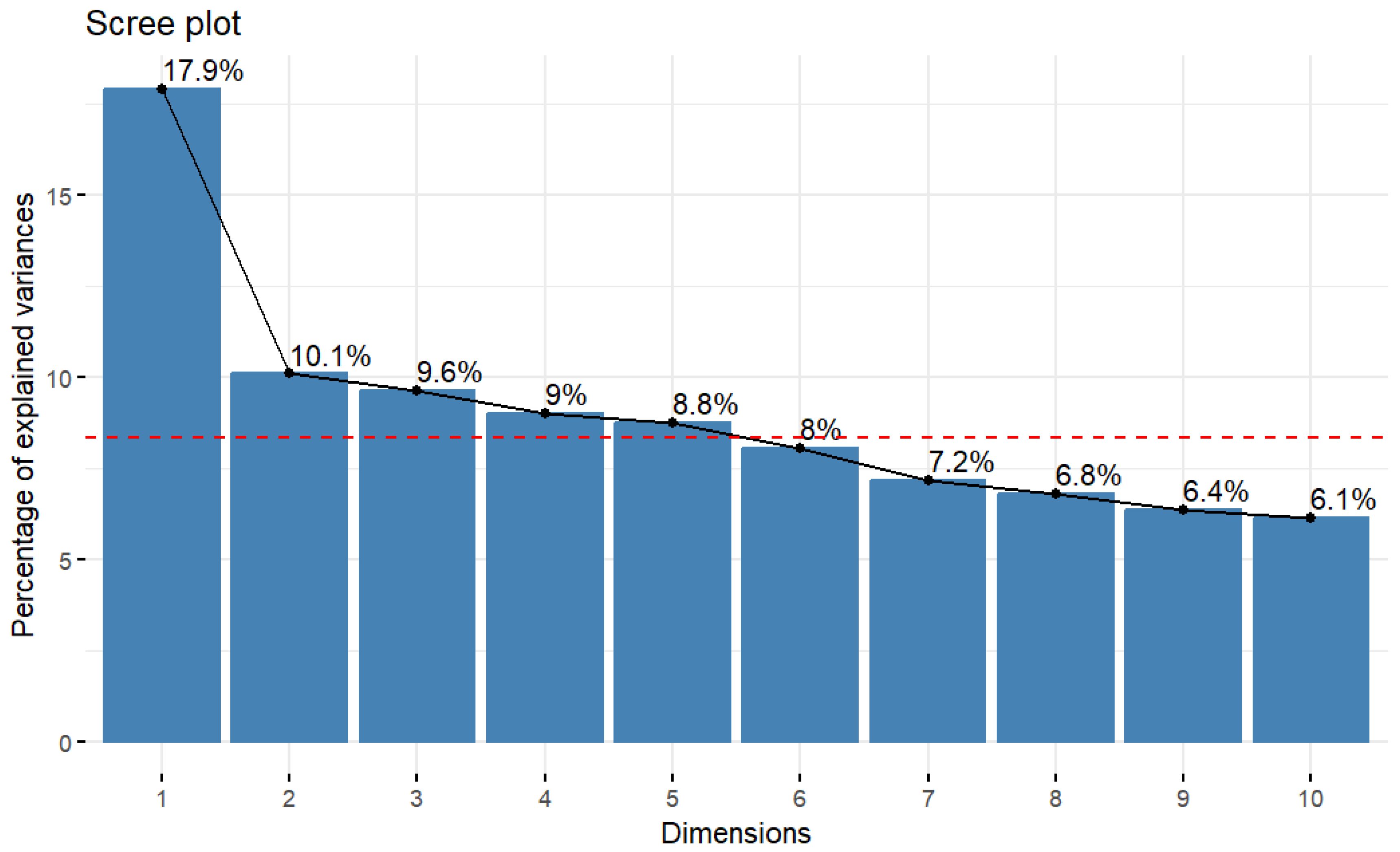
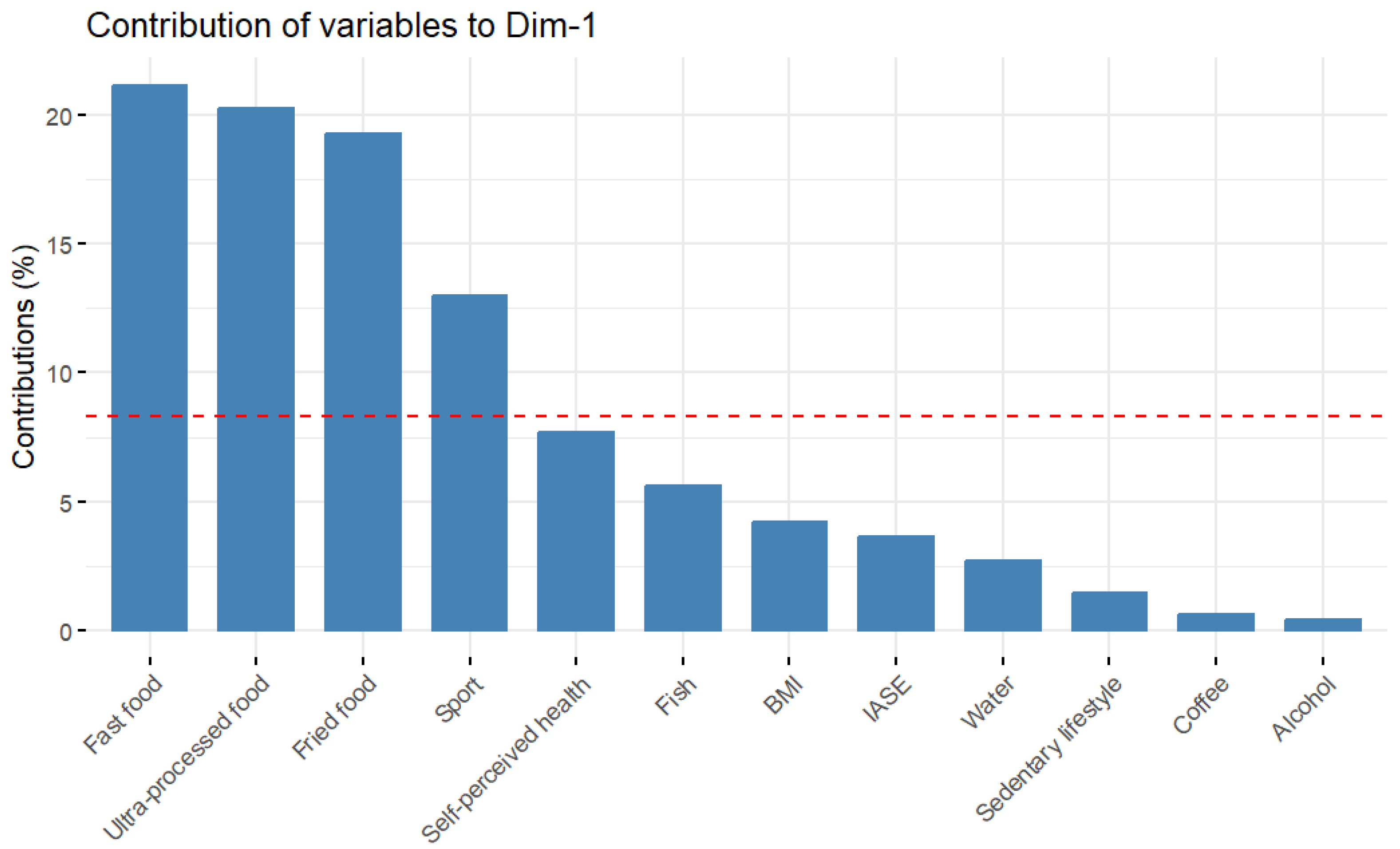
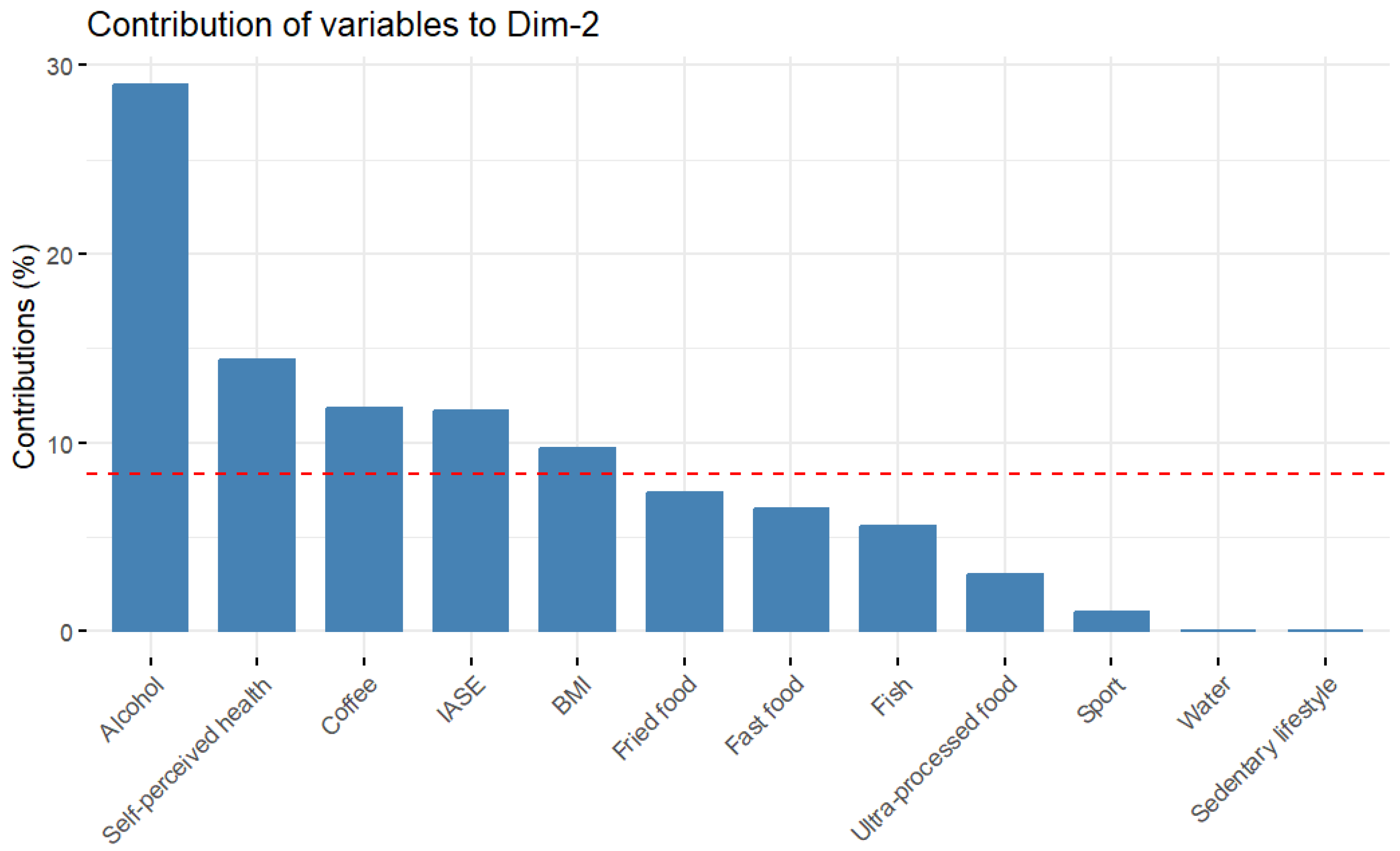
Appendix B
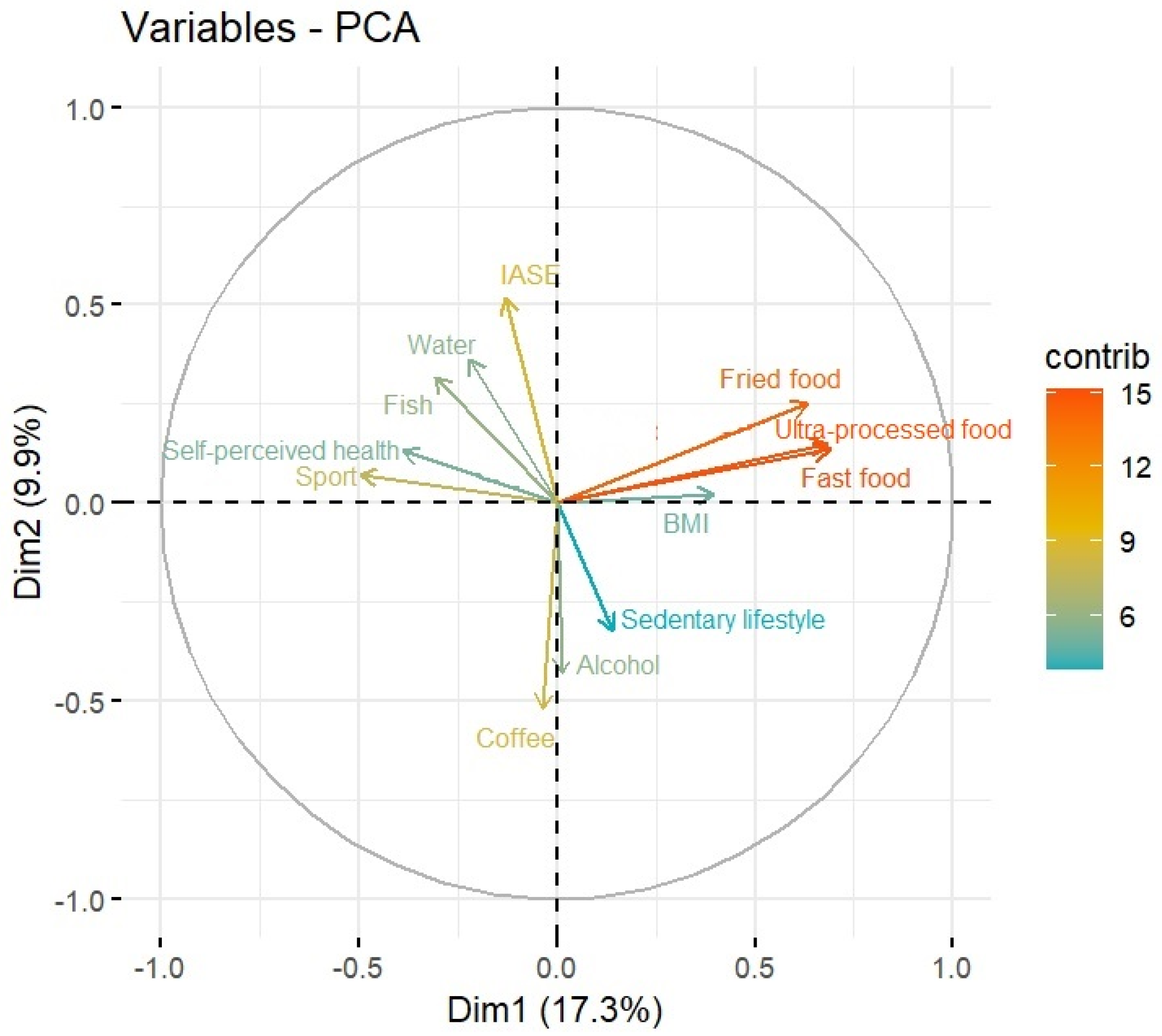
References
- Hooper, L.; Summerbell, C.D.; Thompson, R.; Sills, D.; Roberts, F.G.; Moore, H.; Davey Smith, G. Reduced or Modified Dietary Fat for Preventing Cardiovascular Disease. Cochrane Database Syst. Rev. 2011. [Google Scholar] [CrossRef]
- Robles-Agudo, F.; Sanz-Segovia, F.; López-Arrieta, J.M.; Beltran De La Ascension, M. Diet and Cancer. Rev. Esp. Geriatr. Gerontol. 2005, 40, 184–194. [Google Scholar] [CrossRef]
- Rakhra, V.; Galappaththy, S.L.; Bulchandani, S.; Cabandugama, P.K. Obesity and the Western Diet: How We Got Here. Mo. Med. 2020, 117, 536. [Google Scholar]
- Fung, T.T.; Willett, W.C.; Stampfer, M.J.; Manson, J.A.E.; Hu, F.B. Dietary Patterns and the Risk of Coronary Heart Disease in Women. Arch. Intern. Med. 2001, 161, 1857–1862. [Google Scholar] [CrossRef]
- Hu, F.B.; Rimm, E.B.; Stampfer, M.J.; Ascherio, A.; Spiegelman, D.; Willett, C.W. Prospective Study of Major Dietary Patterns and Risk of Coronary Heart Disease in Men. Am. J. Clin. Nutr. 2000, 72, 912–921. [Google Scholar] [CrossRef]
- Gil, Á.; de Victoria, E.M.; Olza, J. Indicators for the Evaluation of Diet Quality. Nutr. Hosp. 2015, 31 (Suppl. 3), 128–144. [Google Scholar] [CrossRef]
- Pem, D.; Jeewon, R. Fruit and Vegetable Intake: Benefits and Progress of Nutrition Education Interventions-Narrative Review Article. Iran. J. Public Health 2015, 44, 1309. [Google Scholar]
- Slavin, J.L.; Lloyd, B. Health Benefits of Fruits and Vegetables. Adv. Nutr. 2012, 3, 506. [Google Scholar] [CrossRef]
- Elizabeth, L.; Machado, P.; Zinöcker, M.; Baker, P.; Lawrence, M. Ultra-Processed Foods and Health Outcomes: A Narrative Review. Nutrients 2020, 12, 1955. [Google Scholar] [CrossRef]
- Rico-Campà, A.; Martínez-González, M.A.; Alvarez-Alvarez, I.; De Deus Mendonça, R.; De La Fuente-Arrillaga, C.; Gómez-Donoso, C.; Bes-Rastrollo, M. Association between Consumption of Ultra-Processed Foods and All Cause Mortality: SUN Prospective Cohort Study. BMJ 2019, 365, l1949. [Google Scholar] [CrossRef]
- Marti, A. Ultra-Processed Foods Are Not “Real Food” but Really Affect Your Health. Nutrients 2019, 11, 1902. [Google Scholar] [CrossRef]
- Salinas, C.J.; Vio del, R.F. Promoción de La Salud En Chile. Rev. Chil. Nutr. 2002, 29, 164–173. [Google Scholar] [CrossRef]
- Boraita, R.J.; Alsina, D.A.; Ibort, E.G.; Torres, J.M.D. Quality of Life Related to Health and Habits: Differences between Adolescents in Rural and Urban Environments. An. Pediatría (Engl. Ed.) 2022, 96, 196–202. [Google Scholar] [CrossRef]
- Gavala-González, J.; Torres-Perez, A.; Gálvez-Fernández, I.; Fernández-García, J.C. Lifestyle and Self-Perceived Quality of Life in Sports Students: A Case Study. Int. J. Environ. Res. Public Health 2022, 19, 1598. [Google Scholar] [CrossRef] [PubMed]
- Park, J.H.; Moon, J.H.; Kim, H.J.; Kong, M.H.; Oh, Y.H. Sedentary Lifestyle: Overview of Updated Evidence of Potential Health Risks. Korean J. Fam. Med. 2020, 41, 365. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.; Son, J.S.; Eum, Y.H.; Kang, O.L. Association of Sedentary Time and Physical Activity with the 10-Year Risk of Cardiovascular Disease: Korea National Health and Nutrition Examination Survey 2014–2017. Korean J. Fam. Med. 2020, 41, 374–380. [Google Scholar] [CrossRef]
- Ellingson, L.D.; Meyer, J.D.; Shook, R.P.; Dixon, P.M.; Hand, G.A.; Wirth, M.D.; Paluch, A.E.; Burgess, S.; Hebert, J.R.; Blair, S.N. Changes in Sedentary Time Are Associated with Changes in Mental Wellbeing over 1 year in Young Adults. Prev. Med. Rep. 2018, 11, 274. [Google Scholar] [CrossRef]
- Hoare, E.; Milton, K.; Foster, C.; Allender, S. The Associations between Sedentary Behaviour and Mental Health among Adolescents: A Systematic Review. Int. J. Behav. Nutr. Phys. Act. 2016, 13, 108. [Google Scholar] [CrossRef]
- Warburton, D.E.R.; Nicol, C.W.; Bredin, S.S.D. Health Benefits of Physical Activity: The Evidence. Can. Med. Assoc. J. 2006, 174, 801. [Google Scholar] [CrossRef]
- Patel, A.V.; Bernstein, L.; Deka, A.; Feigelson, H.S.; Campbell, P.T.; Gapstur, S.M.; Colditz, G.A.; Thun, M.J. Leisure Time Spent Sitting in Relation to Total Mortality in a Prospective Cohort of US Adults. Am. J. Epidemiol. 2010, 172, 419–429. [Google Scholar] [CrossRef]
- Pinckard, K.; Baskin, K.K.; Stanford, K.I. Effects of Exercise to Improve Cardiovascular Health. Front. Cardiovasc. Med. 2019, 6, 69. [Google Scholar] [CrossRef] [PubMed]
- Craft, L.L.; Perna, F.M. The Benefits of Exercise for the Clinically Depressed. Prim. Care Companion J. Clin. Psychiatry 2004, 6, 104. [Google Scholar] [CrossRef]
- Dolezal, B.A.; Neufeld, E.V.; Boland, D.M.; Martin, J.L.; Cooper, C.B. Interrelationship between Sleep and Exercise: A Systematic Review. Adv. Prev. Med. 2017, 2017, 1364387. [Google Scholar] [CrossRef] [PubMed]
- Sotos-Prieto, M.; Ortolá, R.; Ruiz-Canela, M.; Garcia-Esquinas, E.; Martínez-Gómez, D.; Lopez-Garcia, E.; Martínez-González, M.Á.; Rodriguez-Artalejo, F. Association between the Mediterranean Lifestyle, Metabolic Syndrome and Mortality: A Whole-Country Cohort in Spain. Cardiovasc. Diabetol. 2021, 20, 5. [Google Scholar] [CrossRef] [PubMed]
- Garrido, Á.A.; Monserrat Hernández, M.; Carlos, J.; Olmos, C. Healthy Eating in the Spanish University Community: A Case Study. Nutrients 2023, 15, 2053. [Google Scholar] [CrossRef]
- Romero, I.; Díez, J.; Del Cura, I.; Franco, M.; Gullón, P. Diet Quality Changes by Educational Level among Adults in Spain from 2017 to 2021. Nutrients 2023, 15, 858. [Google Scholar] [CrossRef]
- Guasch-Ferré, M.; Willett, W.C. The Mediterranean Diet and Health: A Comprehensive Overview. J. Intern. Med. 2021, 290, 549–566. [Google Scholar] [CrossRef]
- Estadísticos Estatales por Comunidades Autónomas TOMO, Las Personas Mayores En España. Available online: https://imserso.es/documents/20123/0/112017001_informe-2016-persona.pdf/e01282c2-cdce-f7ce-bd30-dd627eabc230 (accessed on 28 June 2023).
- Mussida, C.; Patimo, R. Women’s Family Care Responsibilities, Employment and Health: A Tale of Two Countries. J. Fam. Econ. Issues 2021, 42, 489. [Google Scholar] [CrossRef]
- Allshouse, A.; Pavlovic, J.; Santoro, N. Menstrual Cycle Hormone Changes Associated with Reproductive Aging and How They May Relate to Symptoms. Obstet. Gynecol. Clin. N. Am. 2018, 45, 613. [Google Scholar] [CrossRef]
- Kumar, P.; Magon, N. Hormones in Pregnancy. Niger. Med. J. 2012, 53, 179. [Google Scholar] [CrossRef]
- Kundakovic, M.; Rocks, D. Sex Hormone Fluctuation and Increased Female Risk for Depression and Anxiety Disorders: From Clinical Evidence to Molecular Mechanisms. Front. Neuroendocrinol. 2022, 66, 101010. [Google Scholar] [CrossRef] [PubMed]
- Marques, A.; Bordado, J.; Peralta, M.; Gouveia, E.R.; Tesler, R.; Demetriou, Y.; Gomez Baya, D. Cross-Sectional and Prospective Relationship between Physical Activity and Depression Symptoms. Sci. Rep. 2020, 10, 16114. [Google Scholar] [CrossRef] [PubMed]
- Relative Validity and Reproducibility of a Diet History Questionnaire in Spain. I. Foods. EPIC Group of Spain. European Prospective Investigation into Cancer and Nutrition. Int. J. Epidemiol. 1997, 26 (Suppl. 1), S91–S99. [CrossRef]
- DÍaz, B.M.; Molina-Recio, G.; Romero-Saldaña, M.; Sánchez, J.R.; Taberné, C.A.; Blanco, C.A.; Molina-Luque, R.; De La Iglesia, J.M. Validation (in Spanish) of the Mini Nutritional Assessment Survey to Assess the Nutritional Status of Patients over 65 Years of Age. Fam. Pract. 2019, 36, 172–178. [Google Scholar] [CrossRef]
- Martínez-García, A.; Trescastro-López, E.M.; Galiana-Sánchez, M.E.; Llorens-Ivorra, C.; Pereyra-Zamora, P. Cultural Adaptation and Evaluation of the Perceived Nutrition Environment Measures Survey to the Mediterranean Spanish Context (NEMS-P-MED). Nutrients 2020, 12, 3257. [Google Scholar] [CrossRef]
- Norte Navarro, A.I.; Ortiz Moncada, R. Quality of the Spanish Diet According to the Healthy Eating Index. Nutr. Hosp. 2011, 26, 330–336. [Google Scholar]
- Grupo Colaborativo de la Sociedad Española de Nutrición Comunitaria (SENC). Guías Alimentarias Para La Población Española; La Nueva Pirámide de La Alimentación Saludable. Nutr. Hosp. 2016, 33, 1–48. [Google Scholar]
- Fuhrman, J. The Hidden Dangers of Fast and Processed Food. Am. J. Lifestyle Med. 2018, 12, 375. [Google Scholar] [CrossRef]
- Pagliai, G.; Dinu, M.; Madarena, M.P.; Bonaccio, M.; Iacoviello, L.; Sofi, F. Consumption of Ultra-Processed Foods and Health Status: A Systematic Review and Meta-Analysis. Br. J. Nutr. 2021, 125, 308–318. [Google Scholar] [CrossRef]
- Maldonado-Pereira, L.; Barnaba, C.; de Los Campos, G.; Medina-Meza, I.G. Evaluation of the Nutritional Quality of Ultra-Processed Foods (Ready to Eat + Fast Food): Fatty Acids, Sugar, and Sodium. J. Food Sci. 2022, 87, 3659–3676. [Google Scholar] [CrossRef]
- Moore, L.V.; Diez Roux, A.V.; Nettleton, J.A.; Jacobs, D.R.; Franco, M. Fast-Food Consumption, Diet Quality, and Neighborhood Exposure to Fast Food: The Multi-Ethnic Study of Atherosclerosis. Am. J. Epidemiol. 2009, 170, 29. [Google Scholar] [CrossRef]
- Tengiz, Z.M.; Oraman, Y. The Evaluation of the Students’ Attitudes and Behavior towards Fast Food Consumption. In Proceedings of the Foodbalt 2019: 13th Baltic Conference on Food Science and Technology: Food. Nutrition, Jelgava, Latvia, 2–3 May 2019; pp. 232–237. [Google Scholar] [CrossRef]
- Stender, S.; Dyerberg, J.; Astrup, A. Fast Food: Unfriendly and Unhealthy. Int. J. Obes. 2007, 31, 887–890. [Google Scholar] [CrossRef]
- Cahill, L.E.; Pan, A.; Chiuve, S.E.; Sun, Q.; Willett, W.C.; Hu, F.B.; Rimm, E.B. Fried-Food Consumption and Risk of Type 2 Diabetes and Coronary Artery Disease: A Prospective Study in 2 Cohorts of US Women and Men. Am. J. Clin. Nutr. 2014, 100, 667–675. [Google Scholar] [CrossRef]
- Gadiraju, T.V.; Patel, Y.; Gaziano, J.M.; Djoussé, L. Fried Food Consumption and Cardiovascular Health: A Review of Current Evidence. Nutrients 2015, 7, 8424–8430. [Google Scholar] [CrossRef] [PubMed]
- Mendivil, C.O. Fish Consumption: A Review of Its Effects on Metabolic and Hormonal Health. Nutr. Metab. Insights 2021, 3, 14. [Google Scholar] [CrossRef] [PubMed]
- Dighriri, I.M.; Alsubaie, A.M.; Hakami, F.M.; Hamithi, D.M.; Alshekh, M.M.; Khobrani, F.A.; Dalak, F.E.; Hakami, A.A.; Alsueaadi, E.H.; Alsaawi, L.S.; et al. Effects of Omega-3 Polyunsaturated Fatty Acids on Brain Functions: A Systematic Review. Cureus 2022, 14, e30091. [Google Scholar] [CrossRef] [PubMed]
- Zhang, A.C.; Singh, S.; Craig, J.P.; Downie, L.E. Omega-3 Fatty Acids and Eye Health: Opinions and Self-Reported Practice Behaviors of Optometrists in Australia and New Zealand. Nutrients 2020, 12, 1179. [Google Scholar] [CrossRef] [PubMed]
- Grosso, G.; Galvano, F.; Marventano, S.; Malaguarnera, M.; Bucolo, C.; Drago, F.; Caraci, F. Omega-3 Fatty Acids and Depression: Scientific Evidence and Biological Mechanisms. Oxid. Med. Cell. Longev. 2014, 2014, 313570. [Google Scholar] [CrossRef]
- Stenholm, S.; Vahtera, J.; Kawachi, I.; Pentti, J.; Halonen, J.I.; Westerlund, H.; Razak, F.; Subramanian, S.V.; Kivimäki, M. Patterns of Weight Gain in Middle-Aged and Older US Adults, 1992–2010. Epidemiology 2015, 26, 165–168. [Google Scholar] [CrossRef]
- Tao, X.; Jiang, A.; Yin, L.; Li, Y.; Tao, F.; Hu, H. Body Mass Index and Age at Natural Menopause: A Meta-Analysis. Menopause 2015, 22, 469–474. [Google Scholar] [CrossRef]
- Dagmar, S.; Erik, S.; Karel, F.; Aleš, S. Gender Differences in Physical Activity, Sedentary Behavior and BMI in the Liberec Region: The IPAQ Study in 2002–2009. J. Hum. Kinet. 2011, 28, 123. [Google Scholar] [CrossRef]
- O’Donoghue, G.; Perchoux, C.; Mensah, K.; Lakerveld, J.; Van Der Ploeg, H.; Bernaards, C.; Chastin, S.F.M.; Simon, C.; O’Gorman, D.; Nazare, J.A. A Systematic Review of Correlates of Sedentary Behaviour in Adults Aged 18-65 Years: A Socio-Ecological Approach. BMC Public Health 2016, 16, 163. [Google Scholar] [CrossRef]
- García-Mendizábal, M.J.; Carrasco, J.M.; Pérez-Gmez, B.; Aragonés, N.; Guallar-Castilln, P.; Rodríguez-Artalejo, F.; Lpez-Abente, G.; Pollán, M. Role of Educational Level in the Relationship between Body Mass Index (BMI) and Health-Related Quality of Life (HRQL) among Rural Spanish Women. BMC Public Health 2009, 9, 120. [Google Scholar] [CrossRef]
- Rippin, H.L.; Hutchinson, J.; Greenwood, D.C.; Jewell, J.; Breda, J.J.; Martin, A.; Rippin, D.M.; Schindler, K.; Rust, P.; Fagt, S.; et al. Inequalities in Education and National Income Are Associated with Poorer Diet: Pooled Analysis of Individual Participant Data across 12 European Countries. PLoS ONE 2020, 15, e0232447. [Google Scholar] [CrossRef]
- Azizi Fard, N.; De Francisci Morales, G.; Mejova, Y.; Schifanella, R. On the Interplay between Educational Attainment and Nutrition: A Spatially-Aware Perspective. EPJ Data Sci. 2021, 10, 18. [Google Scholar] [CrossRef]
- Miller, L.M.S.; Cassady, D.L. The Effects of Nutrition Knowledge on Food Label Use. A Review of the Literature. Appetite 2015, 92, 207–216. [Google Scholar] [CrossRef]
- Ohri-Vachaspati, P.; Deweese, R.S.; Acciai, F.; Delia, D.; Tulloch, D.; Tong, D.; Lorts, C.; Yedidia, M. Healthy Food Access in Low-Income High-Minority Communities: A Longitudinal Assessment-2009–2017. Int. J. Environ. Res. Public Health 2019, 16, 2354. [Google Scholar] [CrossRef]
- Rao, M.; Afshin, A.; Singh, G.; Mozaffarian, D. Do Healthier Foods and Diet Patterns Cost More than Less Healthy Options? A Systematic Review and Meta-Analysis. BMJ Open 2013, 3, e004277. [Google Scholar] [CrossRef]
- Hilmers, A.; Hilmers, D.C.; Dave, J. Neighborhood Disparities in Access to Healthy Foods and Their Effects on Environmental Justice. Am. J. Public Health 2012, 102, 1644. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Global Recommendations on Physical Activity for Health; WHO Library Cat: Geneva, Switzerland, 2010; pp. 1–58. [Google Scholar]
- Serra Majem, L.; Ortiz Andrellucchi, A.; Serra Majem, L.; Ortiz Andrellucchi, A. La Dieta Mediterránea Como Ejemplo de Una Alimentación y Nutrición Sostenibles: Enfoque Multidisciplinar. Nutr. Hosp. 2018, 35, 96–101. [Google Scholar] [CrossRef] [PubMed]
- French, M.T.; Norton, E.C.; Fang, H.; Maclean, J.C. Alcohol Consumption and Body Weight. Health Econ. 2010, 19, 814–832. [Google Scholar] [CrossRef] [PubMed]
- INE. Encuesta Nacional de Salud, 2011–2012; Ministerio de Sanidad, Servicios Sociales e Igualdad, Gobierno de España: Madrid, Spain, 2012. [Google Scholar]

| Variables of Study | |||
|---|---|---|---|
| General Data | Nutrition Habits | Physical Activity | Social Habits |
| Sex | Number of meals per day | Daily sitting time | Number of nights out |
| Age | Breakfast | Frequency of intense sport | Number of hours of sleep |
| Place of birth | Number of glasses of water | Duration of intense sport | Quality of sleep |
| Place of residence | Frequency of fruit consumption | Frequency of moderate sport | Sleep result |
| Size of municipality | Frequency of vegetable consumption | Duration of moderate sport | Ease of falling asleep |
| Work | Frequency of consumption of white and blue fish | Reason for lack of physical activity | Tobacco addiction |
| Level of education | Frequency of consumption of white and red meat | Frequency of alcohol consumption | |
| Income level | Frequency of consumption of legumes | Quantity of alcohol consumed | |
| Weight | Frequency of consumption of dairy products | Frequency of excessive alcohol consumption | |
| Height | Frequency of cereal consumption | ||
| Self-perceived level of health | Frequency of fast food consumption | ||
| Illnesses requiring special diet | Frequency of consumption of fried food | ||
| Symptoms of eating disorders | Frequency of ultra-processed food consumption | ||
| Usual residence | Frequency of soft drinks consumption | ||
| Origin survey | Frequency of fruit juice consumption | ||
| Frequency of consumption of coffee or energy drinks | |||
| Drinks to accompany meals | |||
| Special diet | |||
| Mean ± SD or n (%) | |||
|---|---|---|---|
| AGE | 18–30 years | 31–45 years | p-value * |
| Body mass index (BMI) | 22.78 ± 4.00 | 24.06 ± 4.52 | 4.06 × 10−71 |
| Healthy eating index (IASE) | 53.19 ± 9.70 | 54.43 ± 9.84 | 1.0686 × 10−15 |
| Self-perceived health | 3.78 ± 0.81 | 3.80 ± 0.83 | 0.0151 |
| Sedentary lifestyle | 1.65 ± 0.86 | 1.53 ± 0.80 | 4.85 × 10−16 |
| Physical activity (min) | 148.32 ± 167.94 | 128.51 ± 150.12 | 1.72 × 10−9 |
| Alcohol consumption | 1.68 ± 0.77 | 1.67 ± 0.84 | 0.0037 |
| Water consumption | 3.41 ± 0.64 | 3.41 ± 0.63 | 0.8178 |
| Coffee consumption | 1.59 ± 0.65 | 1.75 ± 0.70 | 1.53 × 10−42 |
| Fast-food consumption | 2.53 ± 0.74 | 2.35 ± 0.76 | 3.81 × 10−38 |
| Consumption of fried foods | 2.35 ± 0.83 | 2.13 ± 0.78 | 7.76 × 10−55 |
| Consumption of ultra-processed food | 2.48 ± 0.93 | 2.35 ± 0.95 | 1.41 × 10−15 |
| Fish consumption | 1.75 ± 0.51 | 1.82 ± 0.47 | 1.47 × 10−15 |
| EDUCATIONAL LEVEL | Basic studies | Superior studies | p-value * |
| Body mass index (BMI) | 24 ± 4.77 | 23.15 ± 4.08 | 6.59 × 10−16 |
| Healthy eating index (IASE) | 51.95 ± 10.29 | 54.56 ± 9.47 | 8.38 × 10−43 |
| Self-perceived health | 3.65 ± 0.87 | 3.85 ± 0.79 | 3.02 × 10−34 |
| Sedentary lifestyle | 1.52 ± 0.80 | 1.62 ± 0.84 | 7.95 × 10−13 |
| Physical activity (min) | 134.32 ± 170.60 | 140.51 ± 155.11 | 3.01 × 10−9 |
| Alcohol consumption | 1.58 ± 0.77 | 1.71 ± 0. | 2.95 × 10−20 |
| Water consumption | 3.41 ± 0.67 | 3.42 ± 0.62 | 0.5632 |
| Coffee consumption | 1.63 ± 0.70 | 1.69 ± 0.67 | 4.63 × 10−9 |
| Fast-food consumption | 2.50 ± 0.76 | 2.42 ± 0.75 | 1.75 × 10−7 |
| Consumption of fried foods | 2.36 ± 0.86 | 2.19 ± 0.79 | 5.41 × 10−24 |
| Consumption of ultra-processed food | 2.52 ± 0.95 | 2.37 ± 0.93 | 1.59 × 10−14 |
| Fish consumption | 1.72 ± 0.51 | 1.81 ± 0.48 | 1.78 × 10−21 |
| INCOMES LEVEL | Low Incomes | High Incomes | p-value * |
| Body mass index (BMI) | 23.65 ± 4.48 | 23.13 ± 4.10 | 1.72 × 10−9 |
| Healthy eating index (IASE) | 52.85 ± 10.03 | 54.81 ± 9.41 | 2.39 × 10−30 |
| Self-perceived health | 3.69 ± 0.84 | 3.90 ± 0.77 | 2.26 × 10−17 |
| Sedentary lifestyle | 1.54 ± 0.82 | 1.64 ± 0.84 | 0.000 |
| Physical activity (min) | 142.90 ± 166.37 | 134.17 ± 152.35 | 0.30 |
| Alcohol consumption | 1.64 ± 0.78 | 1.72 ± 0.82 | 2.34 × 10−9 |
| Water consumption | 3.41 ± 0.64 | 3.42 ± 0.62 | 0.68 |
| Coffee consumption | 1.64 ± 0.69 | 1.69 ± 0.68 | 3.41 × 10−7 |
| Fast-food consumption | 2.47 ± 0.76 | 2.42 ± 0.74 | 0.0005 |
| Consumption of fried foods | 2.25 ± 0.84 | 2.23 ± 0.78 | 0.33 |
| Consumption of ultra-processed food | 2.45 ± 0.95 | 2.38 ± 0.93 | 9.99 × 10−6 |
| Fish consumption | 1.75 ± 0.51 | 1.82 ± 0.48 | 6.05 × 10−19 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sandri, E.; Cantín Larumbe, E.; Cerdá Olmedo, G. The Influence of Socio-Economic Factors on Diet and Active Lifestyle in the Spanish Female Population. Nutrients 2023, 15, 3319. https://doi.org/10.3390/nu15153319
Sandri E, Cantín Larumbe E, Cerdá Olmedo G. The Influence of Socio-Economic Factors on Diet and Active Lifestyle in the Spanish Female Population. Nutrients. 2023; 15(15):3319. https://doi.org/10.3390/nu15153319
Chicago/Turabian StyleSandri, Elena, Eva Cantín Larumbe, and Germán Cerdá Olmedo. 2023. "The Influence of Socio-Economic Factors on Diet and Active Lifestyle in the Spanish Female Population" Nutrients 15, no. 15: 3319. https://doi.org/10.3390/nu15153319
APA StyleSandri, E., Cantín Larumbe, E., & Cerdá Olmedo, G. (2023). The Influence of Socio-Economic Factors on Diet and Active Lifestyle in the Spanish Female Population. Nutrients, 15(15), 3319. https://doi.org/10.3390/nu15153319








