Components of the Fiber Diet in the Prevention and Treatment of IBD—An Update
Abstract
1. Introduction
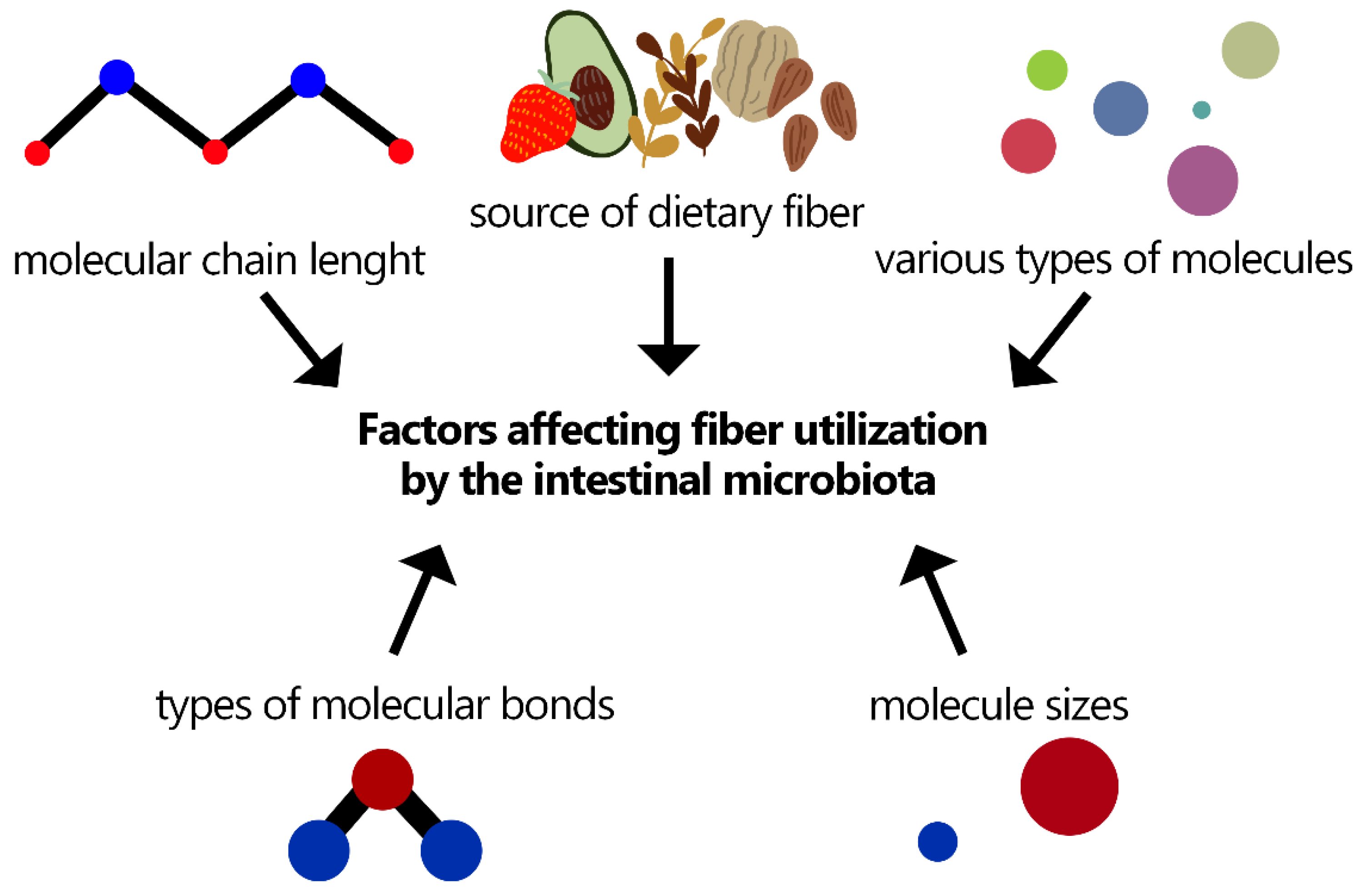
2. Influence of Fiber on the Intestinal Microbiota
3. Link between Dietary Fiber and IBD
3.1. β-Glucan
3.2. Pectin
3.3. Starch
3.4. Inulin
3.5. Fructooligosaccharides
3.6. Hemicellulose
4. Limitations
5. Summary
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Sturm, A.; Maaser, C.; Mendall, M.; Karagiannis, D.; Karatzas, P.; Ipenburg, N.; Sebastian, S.; Rizzello, F.; Limdi, J.; Katsanos, K.; et al. European Crohn’s and Colitis Organisation Topical Review on IBD in the Elderly. J. Crohn’s Colitis 2017, 11, 263–273. [Google Scholar] [CrossRef] [PubMed]
- de Souza, H.; Fiocchi, C.; Iliopoulos, D. The IBD interactome: An integrated view of aetiology, pathogenesis, and therapy. Nat. Rev. Gastroenterol. Hepatol. 2017, 14, 739–749. [Google Scholar] [CrossRef] [PubMed]
- Gomollón, F.; Dignass, A.; Annese, V.; Tilg, H.; Van Assche, G.; Lindsay, J.O.; Peyrin-Biroulet, L.; Cullen, G.J.; Daperno, M.; Kucharzik, T.; et al. 3rd European Evidence-based Consensus on the Diagnosis and Management of Crohn’s Disease 2016: Part 1: Diagnosis and Medical Management. J. Crohn’s Colitis 2017, 1, 3–25. [Google Scholar] [CrossRef] [PubMed]
- Windsor, J.; Kaplan, G. Evolving Epidemiology of IBD. Curr. Gastroenterol. Rep. 2019, 21, 40. [Google Scholar] [CrossRef]
- Holscher, H. Dietary fiber and prebiotics and the gastrointestinal microbiota. Gut Microbes 2017, 8, 172–184. [Google Scholar] [CrossRef]
- O’Grady, J.; O’Connor, E. Review article: Dietary fibre in the era of mi-crobiome science. Aliment. Pharmacol. Ther. 2019, 49, 506–515. [Google Scholar] [CrossRef]
- Dai, F.; Chau, C. Classification and regulatory perspectives of dietary fiber. J. Food Drug Anal. 2017, 25, 37–42. [Google Scholar] [CrossRef]
- Nirmala, P.; Joye, I. Dietary fibre from whole grains and their benefits on metabo-lic health. Nutrients 2020, 12, 3045. [Google Scholar] [CrossRef]
- Grajek, M.; Grabowska; Grot, M.; Białek-Dratwa, A.; Olszewski, Ł. The role of dietary fiber in the nutrition of the elderly. J. Life MEdical Sci. 2020, 4, 61–69. [Google Scholar]
- Cione, E.; Fazio, A.; Curcio, R.; Tucci, P.; LAuria, G.; Cappello, A.R.; Dolce, V. Resistant starches and non-communicable disease: A Focus on mediterranean diet. Foods 2021, 10, 2062. [Google Scholar] [CrossRef]
- Nie, Y.; Luo, F. Dietary fiber: An opportunity for a global control of hyperlipidemia. Oxid. Med. Cell. Longev. 2021, 2021, 5542342. [Google Scholar] [CrossRef] [PubMed]
- Soliman, G. Dietary fiber, atherosclerosis and cardiovascular disease. Nutrients 2019, 11, 1155. [Google Scholar] [CrossRef]
- Currò, D.; Ianiro, G.; Pecere, S.; Bibbò, S.; Cammarota, G. Probiotics, fibre and herbal medicinal products for functional and inflammatory bowel disorders. Br. J. Pharmacol. 2017, 174, 1426–1449. [Google Scholar] [CrossRef]
- Du, B.; Meenu, M.; Liu, H.; Xu, B. A concise review on the molecular structure and func-tion relationship of β-glucan. Int. J. Mol. Sci. 2019, 20, 4032. [Google Scholar] [CrossRef] [PubMed]
- Majtan, J.; Jesenak, M. β-glucans: Multi-functional modulator of wound healing. Molecules 2018, 23, 806. [Google Scholar] [CrossRef] [PubMed]
- Zurbau, A.; Noronha, J.; Khan, T.; Sievenpiper, J.; Wolever, T. The effect of oat β-glucan on postprandial blood glucose and insulin responses: A systematic review and meta-analysis. Eur. J. Clin. Nutr. 2021, 75, 1540–1554. [Google Scholar] [CrossRef]
- Ho, H.; Sievenpiper, J.; Zurbau, A.; Mejia, A.B.; Jovanovski, E.; Au-Yeug, F.; Jenkins, A.L.; Vuksan, V. The effect of oat β-glucan on LDL-cholesterol, non-HDL-cholesterol and apoB for CVD risk reduction: A systematic revie and meta-analysis of randomised-controlled trials. Br. J. Nutr. 2016, 116, 1369–1382. [Google Scholar] [CrossRef]
- Murphy, E.J.; Rezoagli, E.; Major, I.; Rowan, N.; Laffey, J. β-glucan metabolic and immunomodulatory properties and potential for clnical application. J. Fungi 2020, 6, 356. [Google Scholar] [CrossRef]
- D’Argenio, V.; Salvatore, F. The role of the gut microbiome in the healthy adult status. Clin. Chim. Acta 2015, 451, 97–102. [Google Scholar] [CrossRef]
- Walsh, C.; Guinane, C.; O’Toole, P.; Cotter, P. Beneficial modulation of the gut microbiota. FEBS Lett. 2014, 588, 4120–4130. [Google Scholar] [CrossRef]
- Gibson, M.; Crofts, T.; Dantas, G. Antibiotics and the developing infant gut microbiota and resistome. Curr. Opin. Microbiol. 2015, 27, 51–56. [Google Scholar] [CrossRef] [PubMed]
- Ianiro, G.; Tilg, H.; Gasbarrini, A. Antibiotics as deep modulators of gut microbiota: Between good and evil. Gut 2016, 65, 1906–1915. [Google Scholar] [CrossRef] [PubMed]
- Lange, K.; Buerger, M.; Stallmach, A.; Bruns, T. Effects of Antibiotics on Gut Microbiota. Dig. Dis. 2016, 34, 260–268. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.; Covington, A.; Pamer, E. The intestinal microbiota: Antibiotics, colonization resistance, and enteric pathogens. Immunol. Rev. 2017, 279, 90–105. [Google Scholar] [CrossRef] [PubMed]
- Kurilshikov, A.; Wijmenga, C.; Fu, J.; Zhernakova, A. Host Genetics and Gut Microbiome: Challenges and Perspectives. Trends Immunol. 2017, 38, 633–647. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.; Huang, X.; Fang, S.; Yang, H.; He, M.; Zhao, Y.; Huang, L. Contribution of Host Genetics to the Variation of Microbial Composition of Cecum Lumen and Feces in Pigs. Front. Microbiol. 2018, 9, 2626. [Google Scholar] [CrossRef]
- Rothschild, D.; Weissbrod, O.; Barkan, E.; Kurilshikov, A.; Korem, T.; Zeevi, D.; Costea, P.I.; Godneva, A.; Kalka, I.N.; Bar, N.; et al. Environment dominates over host genetics in shaping human gut microbiota. Nature 2018, 555, 210–215. [Google Scholar] [CrossRef]
- Matsumoto, N.; Park, J.; Tomizawa, R.; Kawashima, H.; Hosomi, K.; Mizuguchi, K.; Honda, C.; Ozaki, R.; Iwatani, Y.; Watanabe, M.; et al. Relationship between Nutrient Intake and Human Gut Microbiota in Monozygotic Twins. Medicina 2021, 57, 275. [Google Scholar] [CrossRef]
- De Angelis, M.; Garruti, G.; Minervini, F.; Bonfrate, L.; Portincasa, P.; Gobbetti, M. The Food-gut Human Axis: The Effects of Diet on Gut Microbiota and Metabolome. Curr. Med. Chem. 2019, 26, 3567–3583. [Google Scholar] [CrossRef]
- Sakkas, H.; Bozidis, P.; Touzios, C.; Kolios, D.; Athanasiou, G.; Athanasopoulou, E.; Gerou, I.; Gartzonika, C. Nutritional Status and the Influence of the Vegan Diet on the Gut Microbiota and Human Health. Medicina 2020, 56, 88. [Google Scholar] [CrossRef]
- Hills, R.J.; Pontefract, B.; Mishcon, H.; Black, C.; Sutton, S.; Theberge, C. Gut Microbiome: Profound Implications for Diet and Disease. Nutrients 2019, 11, 1613. [Google Scholar] [CrossRef] [PubMed]
- Beam, A.; Clinger, E.; Hao, L. Effect of Diet and Dietary Components on the Composition of the Gut Microbiota. Nutrients 2021, 13, 2795. [Google Scholar] [CrossRef] [PubMed]
- Dahl, W.; Rivero Mendoza, D.; Lambert, J. Diet, nutrients and the microbiome. Prog. Mol. Biol. Transl. Sci. 2020, 171, 237–263. [Google Scholar] [CrossRef] [PubMed]
- Reddel, S.; Putignani, L.; Del Chierico, F. The Impact of Low-FODMAPs, Gluten-Free, and Ketogenic Diets on Gut Microbiota Modulation in Pathological Conditions. Nutrients 2019, 11, 373. [Google Scholar] [CrossRef]
- Odamaki, T.; Kato, K.; Sugahara, H.; Hashikura, N.; Takahashi, S.; Xiao, J.; Abe, F.; Osawa, R. Age-related changes in gut microbiota composition from newborn to centenarian: A cross-sectional study. BMC Microbiol. 2016, 16, 90. [Google Scholar] [CrossRef]
- Bosco, N.; Noti, M. The aging gut microbiome and its impact on host immunity. Genes Immun. 2021, 22, 289–303. [Google Scholar] [CrossRef]
- Abreu, A.A.Y.; Milke-García, M.; Argüello-Arévalo, G.; la Barca, A.C.-D.; Carmona-Sánchez, R.; Consuelo-Sánchez, A.; Coss-Adame, E.; García-Cedillo, M.; Hernández-Rosiles, V.; Icaza-Chávez, M.; et al. Dietary fiber and the microbiota: A narrative review by a group of experts from the Asociación Mexicana de Gastroenterología. Rev. Gastroenterol. Mex. 2021, 86, 287–304. [Google Scholar] [CrossRef]
- Sonnenburg, E.; Smits, S.; Tikhonov, M.; Higginbottom, S.; Wingreen, N.; Sonnenburg, J. Diet-induced extinctions in the gut microbiota compound over generations. Nature 2016, 529, 212–215. [Google Scholar] [CrossRef] [PubMed]
- Usuda, H.; Okamoto, T.; Wada, K. Leaky Gut: Effect of Dietary Fiber and Fats on Microbiome and Intestinal Barrier. Int. J. Mol. Sci. 2021, 22, 7613. [Google Scholar] [CrossRef]
- Hytting-Andreasen, R.; Balk-Møller, E.; Hartmann, B.; Pedersen, J.; Windeløv, J.; Holst, J.; Kissow, H. Endogenous glucagon-like peptide- 1 and 2 are essential for regeneration after acute intestinal injury in mice. PLoS ONE 2018, 13, e0198046. [Google Scholar] [CrossRef]
- Tanes, C.; Bittinger, K.; Gao, Y.; Friedman, E.S.; Nessel, L.; Paladhi, U.R.; Chau, L.; Panfen, E.; Fischbach, M.A.; Braun, J.; et al. Role of dietary fiber in the recovery of the human gut microbiome and its metabolome. Cell Host Microbe 2021, 29, 394–407. [Google Scholar] [CrossRef] [PubMed]
- Myhrstad, M.; Tunsjø, H.; Charnock, C.; Telle-Hansen, V. Dietary Fiber, Gut Microbiota, and Metabolic Regulation-Current Status in Human Randomized Trials. Nutrients 2020, 12, 859. [Google Scholar] [CrossRef]
- Makki, K.; Deehan, E.; Walter, J.; Bäckhed, F. The Impact of Dietary Fiber on Gut Microbiota in Host Health and Disease. Cell Host Microbe 2018, 23, 705–715. [Google Scholar] [CrossRef] [PubMed]
- Blaak, E.E.; Canfora, E.E.; Theis, S.; Frost, G.; Groen, A.K.; Mithieux, G.; Nauta, A.; Scott, K.; Stahl, B.; Van Harsselaar, J.; et al. Short chain fatty acids in human gut and metabolic health. Benef. Microbes 2020, 11, 411–445. [Google Scholar] [CrossRef] [PubMed]
- Louis, P.; Duncan, S.; McCrae, S.; Millar, J.; Jackson, M.S.; Flint, H.J. Restricted distribution of the butyrate kinase pathway among butyrate-producing bacteria from the human colon. J. Bacteriol. 2004, 186, 2099–2106. [Google Scholar] [CrossRef] [PubMed]
- Martin-Gallausiaux, C.; Marinelli, L.; Blottière, H.; Larraufie, P.; Lapaque, N. SCFA: Mechanisms and functional importance in the gut. Proc. Nutr. Soc. 2021, 80, 37–49. [Google Scholar] [CrossRef]
- So, D.; Whelan, K.; Rossi, M.; Morrison, M.; Holtmann, G.; Kelly, J.T.; Shanahan, E.R.; Staudacher, H.M.; Campbell, K.L. Dietary fiber intervention on gut microbiota composition in healthy adults: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2018, 107, 965–983. [Google Scholar] [CrossRef]
- Fischer, F.; Romero, R.; Hellhund, A.; Linne, U.; Bertrams, W.; Pinkenburg, O. Dietary cellulose induces anti-inflammatory immunity and transcriptional programs via maturation of the intestinal microbiota. Gut Microbes 2020, 12, 1829962. [Google Scholar] [CrossRef]
- Dürholz, K.; Hofmann, J.; Iljazovic, A.; Häger, J.; Lucas, S.; Sarter, K.; Strowig, T.; Bang, H.; Rech, J.; Schett, G.; et al. Dietary Short-Term Fiber Interventions in Arthritis Patients Increase Systemic SCFA Levels and Regulate Inflammation. Nutrients 2020, 12, 3207. [Google Scholar] [CrossRef]
- Guan, Z.; Yu, E.; Feng, Q. Soluble Dietary Fiber, One of the Most Important Nutrients for the Gut Microbiota. Molecules 2021, 26, 6802. [Google Scholar] [CrossRef]
- Ciecierska, A.; Drywień, M.; Hamulka, J.; Sadkowski, T. Nutraceutical functions of beta-glucans in human nutrition. Rocz. Panstw. Zakl. Hig. 2019, 70, 315–324. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Ames, N.; Tun, H.; Tosh, S.; Jones, P.; Khafipour, E. High Molecular Weight Barley β-Glucan Alters Gut Microbiota Toward Reduced Cardiovascular Disease Risk. Front. Microbiol. 2016, 7, 129. [Google Scholar] [CrossRef] [PubMed]
- Carlson, J.; Erickson, J.; Hess, J.; Gould, T.; Slavin, J. Prebiotic Dietary Fiber and Gut Health: Comparing the in Vitro Fermentations of Beta-Glucan, Inulin and Xylooligosaccharide. Nutrients 2017, 9, 1361. [Google Scholar] [CrossRef] [PubMed]
- De Angelis, M.; Montemurno, E.; Vannini, L.; Cosola, C.; Cavallo, N.; Gozzi, G.; Maranzano, V.; Di Cagno, R.; Gobbeti, M.; Gesualdo, L. Effect of Whole-Grain Barley on the Human Fecal Microbiota and Metabolome. Appl. Environ. Microbiol. 2015, 81, 7945–7956. [Google Scholar] [CrossRef] [PubMed]
- Wark, G.; Samocha-Bonet, D.; Ghaly, S.; Danta, M. The role of diet in the pathogenesis and management of inflammatory bowe disease: A review. Nutrients 2021, 13, 135. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.; Chang, E. Inflammatory bowel diseases and the microbiome: Searching the crime scene for clues. Gastroenterology 2021, 160, 524–537. [Google Scholar] [CrossRef]
- Alipour, M.; Zaidi, D.; Valcheva, R.; Jovel, J.; Martínez, I.; Sergi, C.; Walter, J.; Mason, A.; Wong, G.K.-S.; Dieleman, L.A.; et al. Mucosal barier depletion and loss of bacterial diversity are primary abnormalities in paediatric ulcerative colitis. J. Crohn’s Colitis 2016, 10, 462–471. [Google Scholar] [CrossRef]
- Sokol, H.; Pigneur, B.; Watterlot, L.; Lakhdari, O.; Bermúdez-Humaran, L.G.; Gratadoux, J.-J.; Blugeon, S.; Bridonneau, C.; Furet, J.-P.; Corthier, G.; et al. Faecalibacterium prausnitzii is an anti-inflammatory commensal bacterium identified by gut microbiota analysis of crohn disease patients. Proc. Natl. Acad. Sci. USA 2008, 105, 16731–16736. [Google Scholar] [CrossRef]
- Chiba, M.; Tsuji, T.; Nakane, K.; Komatsu, M. High amount of dietary fiber not harmful but favorable for crohn disease. Perm. J. 2015, 19, 58–61. [Google Scholar] [CrossRef]
- Akbar, A.; Shreenath, A. High Fiber Diet; StatPearls [Internet] StatPearls Publishing: Treasure Island, FL, USA, 2022. [Google Scholar]
- Pascal, V.; Pozuelo, M.; Borruel, N.; Casellas, F.; Campos, D.; Santiago, A.; Martinez, X.; Varela, E.; Sarrabayrouse, G.; Machiels, K.; et al. A microbial signature for Crohn’s disease. Gut 2017, 66, 813–822. [Google Scholar] [CrossRef]
- Kumari, R.; Ahuja, V.; Paul, J. Fluctuations in butyrate-producing bacteria in ulcerative colitis patients of North India. World J. Gastroenterol. 2013, 19, 3404–3414. [Google Scholar] [CrossRef] [PubMed]
- Joossens, M.; Huys, G.; Cnockaert, M.; De Preter, V.; Verbeke, K.; Rutgeerts, P.; Vandamme, P.; Vermeire, S. Dysbiosis of the faecal microbiota in patients with Crohn’s disease and their unaffected relatives. Gut 2011, 60, 631–637. [Google Scholar] [CrossRef] [PubMed]
- Tan, P.; Li, X.; Shen, J.; Feng, Q. Fecal microbiota transplantation for the treatment of inflammatory bowel disease: An update Front. Pharmacol. 2020, 11, 574533. [Google Scholar] [CrossRef] [PubMed]
- Owczarek, D.; Rodacki, T.; Domagała-Rodacka, R.; Cibor, D.; Mach, T. Diet and nutritional factors in inflammatory bowel diseases. World J. Gastroenterol. 2016, 22, 895–905. [Google Scholar] [CrossRef] [PubMed]
- Sasson, A.; Ananthakrishnan, A.; Raman, M. Diet in treatment of inflammatory bowel diseases. Clin. Gastroenterol. Hepatol. 2021, 19, 425–435. [Google Scholar] [CrossRef]
- Fritsch, J.; Garces, L.; Quintero, M.A.; Pignac-Kobinger, J.; Santander, A.M.; Fernández, I.; Ban, Y.J.; Kwon, D.; Phillips, M.C.; Knight, K.; et al. Low-fat, high-fiber diet reduces markers of inflammation and dysbiosis and improves quality of life in patients with ulcerative colitis. Clin. Gastroenterol. Hepatol. 2021, 16, 1189–1199. [Google Scholar] [CrossRef]
- Yusuf, K.; Saha, S.; Umar, S. Health benefits of dietary fiber for the management of inflammatory bowel disease. Biomedicines 2022, 10, 1242. [Google Scholar] [CrossRef]
- Swan, O.; Kilpatrick, M.; Breslin, M.; Oddy, W. Dietary fiber and its associations with depression and inflammation. Nutr. Rev. 2020, 78, 394–411. [Google Scholar] [CrossRef]
- Stidham, R.; Higgins, P. Colorectal cancer in inflammatory bowel disease. Clin. Colon Rectal Surg. 2018, 31, 168–178. [Google Scholar] [CrossRef]
- Yang, J.; Yu, J. The association of diet, gut microbiota and colorectal canceer: What we eat may imply what we get. Protein Cell 2018, 9, 474–487. [Google Scholar] [CrossRef]
- Bishehsari, F.; Engen, P.A.; Preite, N.Z.; Tuncil, Y.E.; Naqib, A.; Shaikh, M.; Rossi, M.; Wilber, S.; Green, S.J.; Hamaker, B.R.; et al. Dietary fiber treatment corrects the composition of gut microbiota, promotes SCFA production and suppresses colon carcinogenesis. Genes 2018, 9, 102. [Google Scholar] [CrossRef] [PubMed]
- Hullings, A.; Sinha, R.; Liao, L. Whole grain and dietary fiber intake and risk colorectal cancer in the NIH-AARP diet and healthy study cohort. Am. J. Clin. Nutr. 2020, 112, 603–612. [Google Scholar] [CrossRef] [PubMed]
- Kunzmann, A.; Coleman, H.G.; Huang, W. Dietary fiber intake and risk of colorectal cancer and incydent and recurrent adenoma in the prostatę, lung, colorectal and ovarian cancer screening trial. Am. J. Clin. Nutr. 2015, 102, 881–890. [Google Scholar] [CrossRef]
- Song, M.; Wu, K.; Meyerhardt, J. Fiber intake and survival after colorectal cancer diagnosis. JAMA Oncol. 2018, 4, 71–79. [Google Scholar] [CrossRef] [PubMed]
- Liu, B.; Lin, Q.; Yang, T.; Zeng, L.; Shi, L.; Chen, Y.; Luo, F. Oat β-glucan ameliorates dextran sulfate sodium (DSS)-induced ulcerative colitis in mice. Food Funct. 2015, 6, 3454–3463. [Google Scholar] [CrossRef]
- Bai, J.; Zhao, J.; Al-Ansi, W.; Wang, J.; Xue, L.; Liu, J.; Wang, Y.; Fan, M.; Qian, H.; Li, Y.; et al. Oat β-glucan alleviates DSS-induced colitis via regulating gut microbiota metabolism in mice. Food Funct. 2021, 12, 8976–8993. [Google Scholar] [CrossRef]
- Chen, M.; Tian, S.; Li, S.; Pang, X.; Sun, J.; Zhu, X.; Lv, F.; Lu, Z.; Li, X. β-glucan extracted from highland barley alleviates destran sulfate dosium-induced ulcerative colitis in C57BL/6J. Mice. Molecules 2021, 26, 5812. [Google Scholar] [CrossRef]
- Vu, V.; Muthuramalingan, K.; Singh, V.; Hyun, C.; Kim, Y.M.; Unno, T.; Cho, M. Effects of β-glucan probiotics and symbiotics on obesity-associated colitis and hepatic manifestations in C57BL/6J. mice. Eur. J. Nutr. 2022, 61, 793–807. [Google Scholar] [CrossRef]
- Muthuramalingam, K.; Singh, V.; Choi, C.; Choi, S.; Kim, Y.M.; Unno, T.; Cho, M. Dietary intervention using (1,3)/(1,6)-β-glucan, a fungus-derived soluble prebiotic ameliorates high-fat-diet-induced metabolic distress and alters beneficially the ut microbiota in mice model. Eur. J. Nutr. 2020, 59, 2617–2629. [Google Scholar] [CrossRef]
- Mio, K.; Otake, N.; Nakashima, S.; Matsuoka, T.; Aoe, S. Ingestion of High β-glucan barley flour enhances the intestinal immune system of diet-induced obese mice by prebiotic effects. Nutrients 2021, 13, 907. [Google Scholar] [CrossRef]
- Faghfoori, Z.; Shakerhosseini, R.; Navai, L.; Somi, M.; Nikniaz, Z.; Abadi, A. Effects of an oral supplementation of germinated barley foodstuff on serum CRP level and clinical signs in patients with ulcerative colitis. Health Promot. Perspect 2014, 4, 116–121. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Zhou, Z.; Cao, J.; Liu, X.; Li, M. Evidence for the butyrate metabolism as key pathway improving ulcerative colitis in both pediatric and adult patients. Bioengineered 2021, 12, 8309–8324. [Google Scholar] [CrossRef]
- Williams, B.; Mikkelsen, D.; Flanagan, B.; Gidley, M. Dietary fibre: Moving beyond the “soluble/insoluble” classification for monogastric nutrition, with an emphasis on humans and pigs. J. Anim. Sci. Biotechnol. 2019, 10, 45. [Google Scholar] [CrossRef] [PubMed]
- McRorie, J.; McKeown, N. Understanding the Physics of Functional Fibers in the Gastrointestinal Tract: An Evidence-Based Approach to Resolving Enduring Misconceptions about Insoluble and Soluble Fiber. J. Acad. Nutr. Diet. 2017, 117, 251–264. [Google Scholar] [CrossRef] [PubMed]
- Spagnuolo, R.; Cosco, C.; Mancina, R.; Ruggiero, R.; Garieri, P.; Cosco, V.; Doldo, P. Beta-glucan, inositol and digestive enzymes improve quality of life of patients with inflammatory bowel disease and irritable bowel syndrome. Eur. Rev. Med. Pharmacol. Sci. 2017, 21, 102–107. [Google Scholar]
- Gudej, D.; Filip, R.; Harasym, J.; Wilczak, J.; Dziendzikowska, K.; Oczkowski, M.; Jałosińska, M.; Juszczak, M.; Lange, E.; Gromadzka-Ostrowska, J. Clinical Outcomes after Oat Beta-Glucans Dietary Treatment in Gastritis Patients. Nutrients 2021, 13, 2791. [Google Scholar] [CrossRef]
- Ishisono, K.; Mano, T.; Yabe, T.; Kitaguchi, K. Dietary fiber pectins ameliorates experimental colitis in a neutral sugar side chain-dependent manner. Front. Immunol. 2019, 10, 2979. [Google Scholar] [CrossRef]
- Llewellyn, S.R.; Britton, G.J.; Contijoch, E.J.; Vennaro, O.H.; Mortha, A.; Colombel, J.-F.; Grinspan, A.; Clemente, J.C.; Merad, M.; Faith, J.J. Interactions between diet and the intestinal microbiota alter intestinal premeability and colitis severity in mice. Gastroenterology 2018, 154, 1037–1046. [Google Scholar] [CrossRef]
- Ananthakrishnan, A.N.; Khalili, H.; Konijeti, G.G.; Higuchi, L.M.; de Silva, P.; Korzenik, J.R.; Fuchs, C.S.; Willett, W.C.; Richter, J.M.; Chan, A.T. A prospective study of long-term intake of dietary fiber and risk of Crohn’s disease and ulcerative colitis. Gastroenterology 2013, 145, 970–977. [Google Scholar] [CrossRef]
- Ananthakrishnan, A.; Khalili, H.; Song, M. High School Diet and Risk of Crohn’s Disease and Ulcerative Colitis. Inflamm. Bowel Dis. 2015, 21, 2311–2319. [Google Scholar] [CrossRef] [PubMed]
- Wu, D.; Chen, S.; Ye, X.; Ahmadi, S.; Hu, W.; Yu, C.; Zhu, K.; Cheng, H.; Linhardt, R.J.; He, Q. Protective effects of six different pectic polysaccharides on DSS-induced IBD in mice. Food Hydrocoll. 2021, 127, 107209. [Google Scholar] [CrossRef]
- Wójcik-Pastuszka, D.; Potempa, A.; Musiał, W. Bipolymeric pectin milibeads doped with functionall polymers as matrices for the controlled and targeted release of mesalazine. Molecules 2020, 25, 5711. [Google Scholar] [CrossRef] [PubMed]
- Svagan, A.J.; Kusic, A.; De Gobba, C.; Larsen, F.H.; Sassene, P.; Zhou, Q.; van de Weert, M.; Mullertz, A.; Jørgensen, B.; Ulvskov, P. Rhamnogalacturonan-I based microcapsules for targeted drug release. PLoS ONE 2016, 11, E0168050. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Chen, L.; Hu, M.; Kim, J.J.; Lin, R.; Xu, J.; Fan, L.; Qi, Y.; Wang, L.; Liu, W.; et al. Dietary type 2 resistant starch improves systemic inflammation and intestinal permeability by modulating microbiota and metabolites in aged mice on high-fat diet. Aging 2020, 12, 9173–9187. [Google Scholar] [CrossRef]
- Ren, M.; Li, M.; Lu, L.; Liu, Y.; Ann, F.; Huang, K.; Fu, Z. Arenga pinnata resistant starch modulate gut microbiota and ameliorate intestinal inflammation in aged mice. Nutrients 2022, 14, 3931. [Google Scholar] [CrossRef]
- Keenan, M.; Zhou, J.; Hegsted, M.; Pelkman, C.; Durham, H.A.; Coulon, D.B.; Martin, R.J. Role of resistant starch in improving gut health, adiposity and inssulin resistance. Adv. Nutr. 2015, 6, 198–205. [Google Scholar] [CrossRef]
- Trachsel, J.; Briggs, C.; Gabler, N.; Allen, H.K.; Loving, C.L. Dietary resistant potato starch alters intestinal microbial communities and their metabolites and markers of immune regulation and barrier function in swine. Front. Immunol. 2019, 19, 1381. [Google Scholar] [CrossRef]
- Wan, J.; Zhang, J.; Chen, D.; Yu, B.; Mao, X.; Zheng, P.; Yu, J.; Luo, J.; He, J. Influences of dietary starch structure on intestinal morphology, barrier functions and epithelium apoptosis in weaned pigs. Food Funct. 2020, 11, 4446–4455. [Google Scholar] [CrossRef]
- Metzler-Zebeli, B.; Canibe, N.; Motagne, L. Resistant starch reduces large intestinal pH and promotes fecal lactobacilli and bifidobacteria in pigs. Animal 2019, 13, 64–73. [Google Scholar] [CrossRef]
- Shen, D.; Bai, H.; Li, Z.; Yu, Y.; Zhang, H.; Chen, L. Positive effects of resistant starch supplementation on bowel function in healthy adults: A systematic review and meta-analysis of randomized controlled trials. Int. J. Food Sci. Nutr. 2017, 68, 149–157. [Google Scholar] [CrossRef]
- Montroy, J.; Berjawi, R.; Lalu, M.; Podolsky, E.; Peixoto, C.; Sahin, L.; Stintzi, A.; Mack, D.; Fergusson, D.A. The effects of resistant starches on inflammatory bowel disease in preclinical and clinical settings: A systematic review and meta-analysis. BMC Gastroenterol. 2020, 20, 372. [Google Scholar] [CrossRef] [PubMed]
- Rose, D.; Venema, K.; Keshavarzian, A.; Hamaker, B. Starch-entrapped microspheres show a beneficial fermentation profile and decrease in potentially harmful bacteria during in vitro fermentation in faecal microbiota obtained from patients with inflammatory bowel disease. Br. J. Nutr. 2010, 103, 1514–1524. [Google Scholar] [CrossRef] [PubMed]
- Brotherton, C.; Taylor, A. Dietary fiber information for individuals with Crohn disease: Reports of gastrointestinal effects. Gastroenterol. Nurs. 2013, 36, 320–327. [Google Scholar] [CrossRef]
- Shoaib, M.; Shehzad, A.; Omar, M.; Rakha, A.; Raza, H.; Sharif, H.; Shakeel, A.; Ansari, A.; Niazi, S. Inulin: Properties, health benefits and food applications. Carbohydr. Polym. 2016, 147, 444–454. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Liu, F.; Wang, W.; Sun, C.; Gao, D.; Ma, J.; Hussain, M.A.; Xu, C.; Jiang, Z.; Hou, J. Study of the alleviation effects of a combination of Lactobacillus rhamnosus and inulin on mice with colitis. Food Funct. 2020, 11, 3823–3837. [Google Scholar] [CrossRef]
- Qiao, H.; Zhao, T.; Yin, J.; Zhang, Y.; Ran, H.; Chen, S.; Wu, Z.; Zhang, R.; Wang, X.; Gan, L.; et al. Structural characteristics of inulin and microcrystalline cellulose and their effect on ameliorating colitis and altering colonic microbiota in destran sodium sulfate-induced colitis mice. ACS Omega 2022, 7, 10921–10932. [Google Scholar] [CrossRef]
- Song, J.; Li, Q.; Everaert, N.; Liu, R.; Zheng, M.; Zhao, G.; Wen, J. Effects of inulin supplementation on intestinal barrier function and immunity in specific pathogen-free chickens with Salmonella infection. J. Anim. Sci. 2020, 98, 396. [Google Scholar] [CrossRef]
- Beisner, J.; Filipe Rosa, L.; Kaden-Volynets, V.; Stolzer, I.; Günther, C.; Bischoff, S. Prebiotic Inulin and Sodium Butyrate Attenuate Obesity-Induced Intestinal Barrier Dysfunction by Induction of Antimicrobial Peptides. Front. Immunol. 2021, 12, 678360. [Google Scholar] [CrossRef]
- Akram, W.; Garud, N.; Joshi, R. Role of inulin as prebiotics on inflammatory bowel disease. Drug Discov. Ther. 2019, 13, 1–8. [Google Scholar] [CrossRef]
- Ali, M.S.; Hussein, R.M.; Gaber, Y.; Hamman, O.A.; Kandeil, M.A. Modulation of JNK-1/β-catein signaling by Lactobacillus casei, inulin and their combination in 1,2-dimethylhydrazine-induced colon cancer in mice. RSC Adv. 2019, 9, 29368–29383. [Google Scholar] [CrossRef]
- Del Fabbro, S.; Calder, P.; Cholds, C. Microbiota-independent immunological effects of non-digestible oligosaccharides in the context of inflammatory bowel diseases. Proc. Nutr. Soc. 2020, 79, 468–478. [Google Scholar] [CrossRef] [PubMed]
- Casellas, F.; Borruel, N.; Torrejón, A.; Varela, E.; Antolin, M.; Guarner, F.; Malagelada, J.R. Oral oligofructose-enriched inulin supplementation in acute ulcerative colitis is well tolerated and associated with lowered faecal calprotectin. Aliment. Pharmacol. Ther. 2007, 25, 1061–1067. [Google Scholar] [CrossRef] [PubMed]
- Wagas, A.; Summer, R. Functional and therapeutic potential of inulin: A comprehensive review. Crit. Rev. Food Sci. Nutr. 2019, 59, 1–13. [Google Scholar] [CrossRef]
- Sun, Q.; Arif, M.; Chi, Z.; Li, G.; Liu, C. Macrophages-targeting mannosylated nanoparticles basen on inulin for the treatment of inflammatory bowel disease (IBD). Int. J. Biol. Macromol. 2021, 169, 206–215. [Google Scholar] [CrossRef] [PubMed]
- Shahdadi Sardou, H.; Akhgari, A.; Mohammadpour, A.; Kamali, H.; Jafarian, A.; Garekani, H.; Sadeghi, F. Application of inulin/Eudragit RS in 5-ASA pellet coating with tuned, sustained-release feature in an animal model of ulcerative colitis. Int. J. Pharm. 2021, 597, 120347. [Google Scholar] [CrossRef]
- Singh, V.; Yeoh, B.S.; Walker, R.; Xiao, X.; Saha, P.; Golonka, R.M.; Cai, J.; Bretin, A.C.A.; Cheng, X.; Liu, Q.; et al. Microbiota fermentation-NLRP3 axis shapes the impact of dietary fibres on intestinal inflammation. Gut 2019, 68, 1801–1812. [Google Scholar] [CrossRef]
- Cherbut, C.; Michel, C.; i Lecannu, G. The Prebiotic Characteristics of Fructooligosaccharides Are Necessary for Reduction of TNBS-Induced Colitis in Rats. J. Nutr. 2003, 133, 21–27. [Google Scholar] [CrossRef]
- Kim, H.; Jeong, Y.; Kang, S.; You, H.; Ji, G. Co-culture with Bifidobacterium catenulatum improves the growth, gut colonization and butyrate production of Faecalibacterium prausnitzii: In vitro and in vivo studies. Microorganisms 2020, 8, 788. [Google Scholar] [CrossRef]
- Koleva, P.; Ketabi, A.; Valcheva, R.; Ganzle, M.G.; Dieleman, L.A. Chemically definited diet alters the protective properties of fructo-oligosaccharides and isomalto-oligosaccharides in HLA-B27 transgenic rats. PLoS ONE 2014, 9, e111717. [Google Scholar] [CrossRef]
- Anderson, J.L.; Hedin, C.R.; Benjamin, J.L.; Koutsoumpas, A.; Ng, S.C.; Hart, A.L.; Forbes, A.; Stagg, A.J.; Lindsay, J.O.; Whelan, K. Dietary intake of inulin-type fructans in active and inactive Crohn’s disease and healthy controls: A case-control study. J. Crohn’s Colitis 2015, 9, 1024–1031. [Google Scholar] [CrossRef]
- Lindsay, J.; Whelan, K.; Stagg, A.; Gobin, P.; Al-Hassi, H.; Rayment, N.; Kamm, M.; Knight, S.; Forbes, A. Clinical, microbiological, and immunological effects of fructo-oligosaccharide in patients with Crohn’s disease. Gut 2006, 55, 348–355. [Google Scholar] [CrossRef] [PubMed]
- Benjamin, J.L.; Hedin, C.; Koutsoumpas, A.; Ng, S.C.; McCarthy, N.; Hart, A.L.; Kamm, M.A.; Sanderson, J.D.; Knight, S.C.; Forbes, A.; et al. Randomised, double-blind, placebo-controlled trial of fructo-oligosaccharides in active Crohn’s disease. Gut 2011, 60, 923–929. [Google Scholar] [CrossRef] [PubMed]
- Caviglia, G.; De Blasio, F.; Vernero, M.; Armandi, A.; Ross, C.; Saracco, G.M.; Bugianesi, E.; Astegiano, M.; Ribaldone, D.G. Efficacy of a Preparation Based on Calcium Butyrate, Bifidobacterium bifidum, Bifidobacterium lactis, and Fructooligosaccharides in the Prevention of Relapse in Ulcerative Colitis: A Prospective Observational Study. J. Clin. Med. 2021, 10, 4961. [Google Scholar] [CrossRef] [PubMed]
- Szczeklik, A.; Gajewski, P. Interna Szczeklika 2018/2019. Medycyna Prakt. 2018, 1, 1033–1045. [Google Scholar]
- Bamba, T.; Andoh, A.; Fujiyama, Y. A new prebiotic from germinated barley for nutraceutical treatment of ulcerative colitis. J. Gatroenterol. Hepatol. 2002, 17, 818–824. [Google Scholar] [CrossRef]
- Mach, T.; Szczeklik, K.; Garlicka, M.; Owczarek, D. Owrzodzenia w obrębie jamy ustnej u chorego z aktywną chorobą Leśniowskiego-Crohna. Przegląd astroenterol. 2007, 2, 201–213. [Google Scholar]
- Araki, Y.; Andoh, A.; Koyana, S.; Fujiyama, Y.; Kanauchi, O.; Bamba, T. Effects of germinated barley foodstuff on microflora and short chain fatty acid production in dextran sulfate sodium-induced coltis in rats. Bioscence Biotechnol. Biochem. 2000, 64, 1794–1800. [Google Scholar] [CrossRef]
- Kanauchi, O.; Suga, T.; Tochihara, M.; Hibi, T.; Naganuma, M.; Homma, T.; Asakura, H.; Nakano, H.; Takahama, K.; Fujiyama, Y.; et al. Treatment of ulcerative coltis by feeding with germinated barley foodstuff: First report of a multcenter open control trial. J. Gastroenterol. 2002, 37, 67–72. [Google Scholar] [CrossRef]
- Payne, A.; Barker, H. Dietetyka I Żywienie Kliniczne. Edra Urban Partn. 2017, 1, 71–76. [Google Scholar]
- Serra, J.; Pohl, D.; Azpiroz, F.; Chiarioni, G.; Ducrotté, P.; Gourcerol, G.; Hungin, A.P.S.; Layer, P.; Mendive, J.; Pfeifer, J.; et al. Functional Constipation Guidelines Working Group. European society of neurogastroenterology and motility guidelines on functional constipation in adults. Neurogastroenterol. Motil. 2020, 32, e13762. [Google Scholar] [CrossRef]
- Van der Schoot, A.; Drysdale, C.; Whelan, K.; Dimidi, E. The effect of fiber supplementation on chronic constipation in adults: An updated systematic review and meta-analysis of randomized controlled trials. Am. J. Clin. Nutr. 2022, 116, 953–969. [Google Scholar] [CrossRef] [PubMed]
- Anderson, J.W.; Baird, P.; Davis, R.H.; Ferreri, S.; Knudtson, M.; Koraym, A.; Waters, V.; Williams, C. Health benefits of dietary fiber. Nutr. Rev. 2009, 67, 188–205. [Google Scholar] [CrossRef] [PubMed]
- Wagenaar, C.A.; van de Put, M.; Bisschops, M.; Walrabenstein, W.; de Jonge, C.S.; Herrema, H.; van Schaardenburg, D. The effect of dietary interventions on chronic inflammatory diseases in relation to the microbiome: A systematic review. Nutrients 2021, 13, 3208. [Google Scholar] [CrossRef]
- McRae, M.P. Effectiveness of fiber supplementation for constipation, weight loss and supporting gastrointestinal function: A narrative review of meta-analyses. J. Chiropr Med. 2020, 19, 58–64. [Google Scholar] [CrossRef] [PubMed]
| Component | Biological Role |
|---|---|
| β-glucan | Reduction of CRP (C reactive protein) in patients with UC (ulcerative colitis). Improvement in gastrointestinal symptoms in patients taking mesalazine. Control of lipid and carbohydrate metabolism. Reduction of pro-inflammatory cytokine production. Modulation of the intestinal microbiota. |
| Pectin | Preventive effect of IBD (inflammatory bowel diseases). |
| Starch | Maintain clinical remission in patients with IBD. Reduction of symptoms associated with active disease. Increase in the production of SCFA (short-chain fatty acids) production. Reduction of inflammation in the colon. Reduction of harmful bacteria. |
| Inulin | Positive effect on the intestinal microbiota by increasing Bifidobacteria. Reduction of inflammation. Decrease in fecal calprotectin concentration. Alleviation of dyspeptic symptoms. Indirect production of SCFAs. Potential immunomodulator in IBD. |
| Fructooligosaccharides | Growth of fecal Bifidobacteria. Reduction of inflammation, indirectly affecting the reduction of anorexia and weight loss Reduction in the Harvey–Bradshaw index. Improving quality of life by reducing pain and improving stool consistency. Promoting the healing of the intestinal epithelium. |
| Hemicellulose | Reduction of inflammation in the intestines. Assist in the reconstruction of the intestinal epithelium. Increase the production of butyric acid and acetic acid. Increasing the number of bifidobacteria and eubacteria. Reduction in the level of clinical activity of patients with UC. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ferenc, K.; Jarmakiewicz-Czaja, S.; Filip, R. Components of the Fiber Diet in the Prevention and Treatment of IBD—An Update. Nutrients 2023, 15, 162. https://doi.org/10.3390/nu15010162
Ferenc K, Jarmakiewicz-Czaja S, Filip R. Components of the Fiber Diet in the Prevention and Treatment of IBD—An Update. Nutrients. 2023; 15(1):162. https://doi.org/10.3390/nu15010162
Chicago/Turabian StyleFerenc, Katarzyna, Sara Jarmakiewicz-Czaja, and Rafał Filip. 2023. "Components of the Fiber Diet in the Prevention and Treatment of IBD—An Update" Nutrients 15, no. 1: 162. https://doi.org/10.3390/nu15010162
APA StyleFerenc, K., Jarmakiewicz-Czaja, S., & Filip, R. (2023). Components of the Fiber Diet in the Prevention and Treatment of IBD—An Update. Nutrients, 15(1), 162. https://doi.org/10.3390/nu15010162






