Nuts and Metabolic Syndrome: Reducing the Burden of Metabolic Syndrome in Menopause
Abstract
:1. Introduction

2. Menopause and Metabolic Disruption
2.1. The Metabolic Impact of Estrogens and Androgens
2.1.1. Estrogens
2.1.2. Androgens
3. Nut Components of Health Interest
3.1. Unsaturated Fat
3.2. Polyphenols
3.3. Other Components
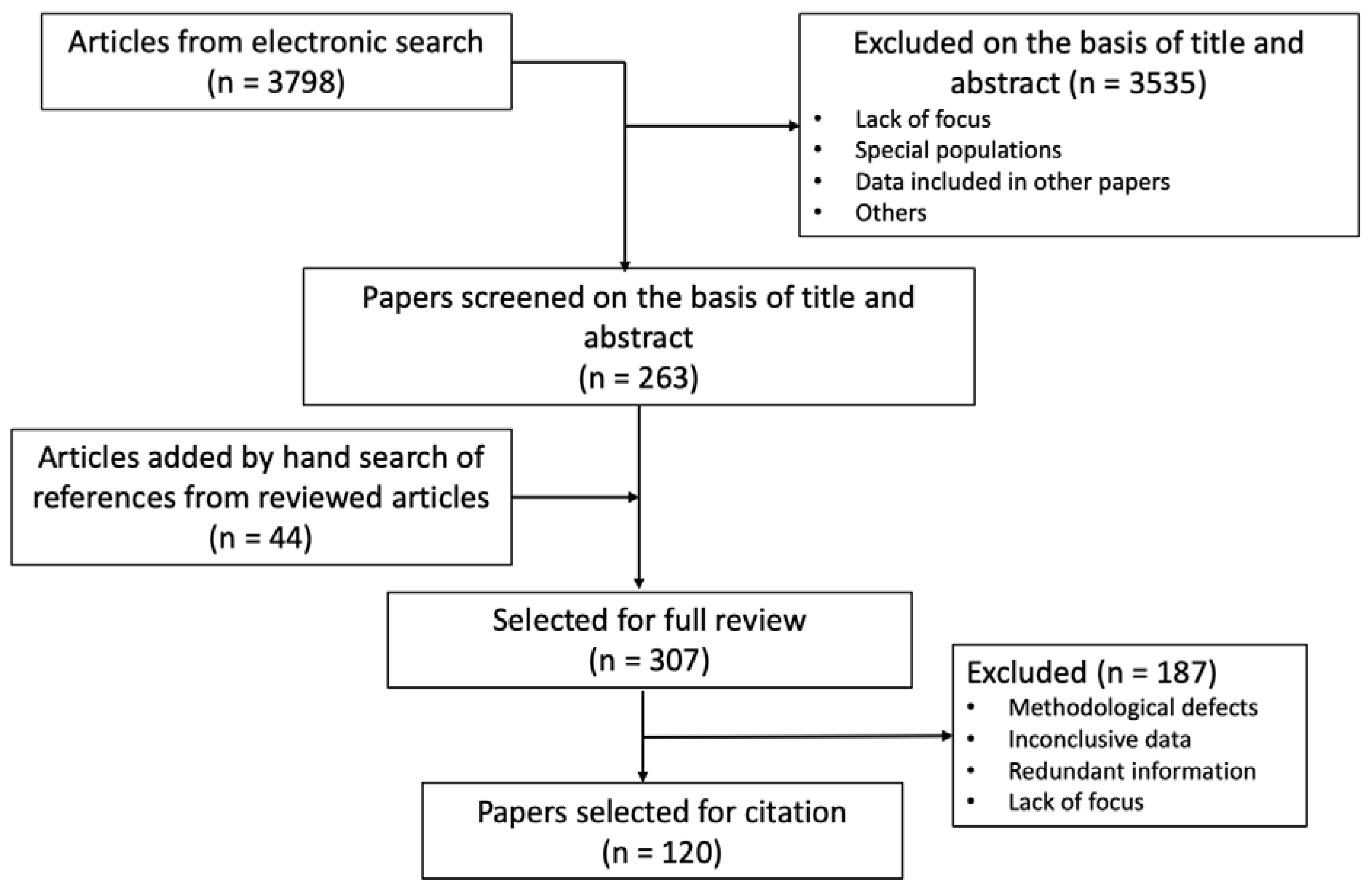
4. Literature Search
5. Effect of Nuts and Their Components on Metabolic Syndrome
5.1. Mechanisms Affecting Components of MetS
5.1.1. Body Weight and Waist Circumference
5.1.2. Carbohydrate Metabolism
5.1.3. Blood Pressure
5.1.4. Lipids
5.2. Clinical Studies
5.2.1. Metabolic Syndrome
5.2.2. Body Weight and Waist Circumference
Nuts in General
Specific Nut Types
Later Clinical Evidence
5.2.3. Carbohydrate Metabolism and Diabetes
Nuts in General
Specific Nut Types
Later Clinical Evidence
5.2.4. Blood Pressure
Nuts in General
Specific Nut Types
Later Clinical Evidence
5.2.5. Lipids
Nuts in General
Specific Nut Types
Later Clinical Evidence
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| aGnRH | Analogues of the gonadotrophin releasing hormone |
| AHA | American Heart Association |
| ATTIS | Almonds Trial Targeting Dietary Intervention with Snacks |
| BF | Body fat |
| BMI | Body mass index |
| BW | Body weight |
| CI | Confidence interval |
| CRP | C-reactive protein |
| CT | Computed tomography |
| CVD | Cardiovascular disease |
| DASH | Dietary Approaches to Stop Hypertension |
| DBP | Diastolic blood pressure |
| DXA | Dual-energy X-ray absorptiometry |
| EPIC-PANACEA | European Prospective Investigation into Cancer and nutrition-Physical Activity, Nutrition, Alcohol, Cessation of smoking, Eating out of home in relation to Anthropometry |
| E2 | Estradiol |
| ER | Estrogen receptors |
| ERKO | ER knock out |
| FBG | Fasting blood glucose |
| FI | Fasting insulin |
| HbA1c | Glycosylated hemoglobin |
| HDL | High-density lipoprotein |
| HOMA-IR | Homeostatic model assessment-estimated insulin resistance |
| HOPE | Women’s Health, Osteoporosis, Progestin, Estrogen |
| IL-6 | Interleukin 6 |
| LDL | Low-density lipoprotein |
| MedDiet | Mediterranean diet |
| MESA | Multi-Ethnic Study of Atherosclerosis |
| MetS | Metabolic syndrome |
| MHT | Menopausal hormone therapy |
| miRNA | Micro-ribonucleic acid |
| MUFA | Monounsaturated fatty acids |
| NHANES | National Health and Nutrition Examination Survey |
| OR | Odds ratio |
| PCOS | Polycystic ovary syndrome |
| PEPI | Postmenopausal Estrogen/Progestin Intervention |
| PREDIMED | Prevención con Dieta Mediiterránea |
| PUFA | Polyunsaturated fatty acids |
| RCT | Randomized controlled trial |
| RR | Relative risk |
| SBP | Systolic blood pressure |
| SR | Systematic review |
| SWAN | The Study of Women Across the Nation |
| T2D | Type 2 diabetes. |
| TC | Total cholesterol |
| TG | Triglycerides |
| WAHA | Walnuts and Healthy Aging |
| WC | Waist circumference |
| WHI | Women’s Health Initiative |
| WMD | Weighted mean difference |
References
- Alberti, K.G.M.M.; Eckel, R.H.; Grundy, S.M.; Zimmet, P.Z.; Cleeman, J.I.; Donato, K.A.; Fruchart, J.C.; James, W.P.T.; Loria, C.M.; Smith, S.C., Jr. Harmonizing the metabolic syndrome: A joint interim statement of the international diabetes federation task force on epidemiology and prevention; National heart, lung, and blood institute; American heart association; World heart federation; International Atherosclerosis Society; International Association for the Study of Obesity. Circulation 2009, 120, 1640–1645. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gluvic, Z.; Zaric, B.; Resanovic, I.; Obradovic, M.; Mitrovic, A.; Radak, D.; Isenovic, E. Link between Metabolic Syndrome and Insulin Resistance. Curr. Vasc. Pharmacol. 2017, 15, 30–39. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Rexrode, K.; van Dam, R.; Li, T.Y.; Hu, F.B. Abdominal Obesity and the Risk of All-Cause, Cardiovascular, and Cancer Mortality. Circulation 2008, 117, 1658–1667. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, M. Improving obesity and blood pressure. Hypertens. Res. 2020, 43, 79–89. [Google Scholar] [CrossRef] [PubMed]
- Matthews, K.A.; Crawford, S.L.; Chae, C.U.; Everson-Rose, S.A.; Sowers, M.F.; Sternfeld, B.; Sutton-Tyrrell, K. Are Changes in Cardiovascular Disease Risk Factors in Midlife Women Due to Chronological Aging or to the Menopausal Transition? J. Am. Coll. Cardiol. 2009, 54, 2366–2373. [Google Scholar] [CrossRef] [Green Version]
- Matthews, K.A.; Chen, X.; Barinas-Mitchell, E.; Brooks, M.M.; Derby, C.A.; Harlow, S.; Jackson, E.A.; Thurston, R.C.; El Khoudary, S.R. Age at Menopause in Relationship to Lipid Changes and Subclinical Carotid Disease Across 20 Years: Study of Women’s Health Across the Nation. J. Am. Heart Assoc. 2021, 10, e021362. [Google Scholar] [CrossRef]
- Stevenson, J.C.; Tsiligiannis, S.; Panay, N. Cardiovascular Risk in Perimenopausal Women. Curr. Vasc. Pharmacol. 2019, 17, 591–594. [Google Scholar] [CrossRef]
- Lovejoy, J.C.; Champagne, C.M.; de Jonge, L.; Xie, H.; Smith, S.R. Increased visceral fat and decreased energy expenditure during the menopausal transition. Int. J. Obes. 2008, 32, 949–958. [Google Scholar] [CrossRef] [Green Version]
- Greendale, G.A.; Sternfeld, B.; Huang, M.; Han, W.; Karvonen-Gutierrez, C.; Ruppert, K.; Cauley, J.A.; Finkelstein, J.S.; Jiang, S.-F.; Karlamangla, A.S. Changes in body composition and weight during the menopause transition. JCI Insight 2019, 4, e124865. [Google Scholar] [CrossRef]
- Ambikairajah, A.; Walsh, E.; Tabatabaei-Jafari, H.; Cherbuin, N. Fat mass changes during menopause: A metaanalysis. Am. J. Obstet. Gynecol. 2019, 221, 393–409.e50. [Google Scholar] [CrossRef]
- Janssen, I. Menopause and the Metabolic SyndromeThe Study of Women’s Health Across the Nation. Arch. Intern. Med. 2008, 168, 1568–1575. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Stuenkel, C.A. Menopause, hormone therapy and diabetes. Climacteric 2017, 20, 11–21. [Google Scholar] [CrossRef]
- Casu, L.; Gillespie, S.; Nisbett, N. Integrating nutrition and physical activity promotion: A scoping review. PLoS ONE 2020, 15, e0233908. [Google Scholar] [CrossRef] [PubMed]
- Wang, D.; Karvonen-Gutierrez, C.A.; Jackson, E.A.; Elliott, M.R.; Appelhans, B.M.; Barinas-Mitchell, E.; Bielak, L.F.; Huang, M.-H.; Baylin, A. Western Dietary Pattern Derived by Multiple Statistical Methods Is Prospectively Associated with Subclinical Carotid Atherosclerosis in Midlife Women. J. Nutr. 2020, 150, 579–591. [Google Scholar] [CrossRef]
- Ko, S.-H.; Kim, H.-S. Menopause-Associated Lipid Metabolic Disorders and Foods Beneficial for Postmenopausal Women. Nutrients 2020, 12, 202. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Silva, T.; Oppermann, K.; Reis, F.; Spritzer, P. Nutrition in Menopausal Women: A Narrative Review. Nutrients 2021, 13, 2149. [Google Scholar] [CrossRef] [PubMed]
- Willett, W.; Rockström, J.; Loken, B.; Springmann, M.; Lang, T.; Vermeulen, S.; Garnett, T.; Tilman, D.; DeClerck, F.; Wood, A.; et al. Food in the Anthropocene: The EAT–Lancet Commission on healthy diets from sustainable food systems. Lancet 2019, 393, 447–492. [Google Scholar] [CrossRef]
- Sánchez-Sánchez, M.L.; García-Vigara, A.; Hidalgo-Mora, J.J.; García-Pérez, M.-Á.; Tarín, J.; Cano, A. Mediterranean diet and health: A systematic review of epidemiological studies and intervention trials. Maturitas 2020, 136, 25–37. [Google Scholar] [CrossRef] [PubMed]
- Cano, A.; Marshall, S.; Zolfaroli, I.; Bitzer, J.; Ceausu, I.; Chedraui, P.; Durmusoglu, F.; Erkkola, R.; Goulis, D.G.; Hirschberg, A.L.; et al. The Mediterranean diet and menopausal health: An EMAS position statement. Maturitas 2020, 139, 90–97. [Google Scholar] [CrossRef]
- Hidalgo-Mora, J.J.; García-Vigara, A.; Sánchez-Sánchez, M.L.; García-Pérez, M.Á.; Tarín, J.; Cano, A. The Mediterranean diet: A historical perspective on food for health. Maturitas 2020, 132, 65–69. [Google Scholar] [CrossRef]
- Becerra-Tomás, N.; Paz-Graniel, I.; WC Kendall, C.; Kahleova, H.; Rahelić, D.; Sievenpiper, J.L.; Salas-Salvadó, J. Nut consumption and incidence of cardiovascular diseases and cardiovascular disease mortality: A meta-analysis of prospective cohort studies. Nutr. Rev. 2019, 77, 691–709. [Google Scholar] [CrossRef] [PubMed]
- Bach-Faig, A.; Berry, E.M.; Lairon, D.; Reguant, J.; Trichopoulou, A.; Dernini, S.; Medina, F.X.; Battino, M.; Belahsen, R.; Miranda, G.; et al. Mediterranean Diet Foundation Expert Group. Mediterranean diet pyramid today. Science and cultural updates. Public Health Nutr. 2011, 14, 2274–2284. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Monget, P.; McNatty, K.; Monniaux, D. The Crazy Ovary. Genes 2021, 12, 928. [Google Scholar] [CrossRef] [PubMed]
- Gershon, E.; Dekel, N. Newly Identified Regulators of Ovarian Folliculogenesis and Ovulation. Int. J. Mol. Sci. 2020, 21, 4565. [Google Scholar] [CrossRef] [PubMed]
- Randolph, J.F.; Zheng, H.; Sowers, M.R.; Crandall, C.; Crawford, S.; Gold, E.B.; Vuga, M. Change in Follicle-Stimulating Hormone and Estradiol Across the Menopausal Transition: Effect of Age at the Final Menstrual Period. J. Clin. Endocrinol. Metab. 2011, 96, 746–754. [Google Scholar] [CrossRef] [PubMed]
- Mondul, A.; Rodriguez, C.; Jacobs, E.J.; Calle, E.E. Age at Natural Menopause and Cause-specific Mortality. Am. J. Epidemiology 2005, 162, 1089–1097. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Labrie, F.; Bélanger, A.; Cusan, L.; Gomez, J.-L.; Candas, B. Marked Decline in Serum Concentrations of Adrenal C19 Sex Steroid Precursors and Conjugated Androgen Metabolites During Aging. J. Clin. Endocrinol. Metab. 1997, 82, 2396–2402. [Google Scholar] [CrossRef]
- Van Pelt, R.E.; Gavin, K.M.; Kohrt, W.M. Regulation of Body Composition and Bioenergetics by Estrogens. Endocrinol. Metab. Clin. N. Am. 2015, 44, 663–676. [Google Scholar] [CrossRef] [Green Version]
- Melanson, E.L.; Gavin, K.M.; Shea, K.L.; Wolfe, P.; Wierman, M.E.; Schwartz, R.S.; Kohrt, W.M. Regulation of energy expenditure by estradiol in premenopausal women. J. Appl. Physiol. 2015, 119, 975–981. [Google Scholar] [CrossRef] [Green Version]
- Shea, K.L.; Gavin, K.M.; Melanson, E.L.; Gibbons, E.; Stavros, A.; Wolfe, P.; Kittelson, J.M.; Vondracek, S.F.; Schwartz, R.S.; Wierman, M.E.; et al. Body composition and bone mineral density after ovarian hormone suppression with or without estradiol treatment. Menopause 2015, 22, 1045–1052. [Google Scholar] [CrossRef] [Green Version]
- Espeland, M.A.; Stefanick, M.L.; Kritz-Silverstein, D.; Fineberg, S.E.; Waclawiw, M.A.; James, M.K.; Greendale, G.A. Effect of Postmenopausal Hormone Therapy on Body Weight and Waist and Hip Girths. J. Clin. Endocrinol. Metab. 1997, 82, 1549–1556. [Google Scholar] [PubMed] [Green Version]
- Utian, W.H.; Gass, M.L.S.; Pickar, J.H. Body mass index does not influence response to treatment, nor does body weight change with lower doses of conjugated estrogens and medroxyprogesterone acetate in early postmenopausal women. Menopause 2004, 11, 306–314. [Google Scholar] [CrossRef] [PubMed]
- Jensen, L.; Vestergaard, P.; Hermann, A.; Gram, J.; Eiken, P.; Abrahamsen, B.; Brot, C.; Kolthoff, N.; Sørensen, O.; Beck-Nielsen, H.; et al. Hormone Replacement Therapy Dissociates Fat Mass and Bone Mass, and Tends to Reduce Weight Gain in Early Postmenopausal Women: A Randomized Controlled 5-Year Clinical Trial of the Danish Osteoporosis Prevention Study. J. Bone Miner. Res. 2003, 18, 333–342. [Google Scholar] [CrossRef] [PubMed]
- Chen, Z.; Bassford, T.; Green, S.B.; Cauley, J.A.; Jackson, R.D.; Lacroix, A.Z.; LeBoff, M.; Stefanick, M.L.; Margolis, K. Postmenopausal hormone therapy and body composition—a substudy of the estrogen plus progestin trial of the Women’s Health Initiative. Am. J. Clin. Nutr. 2005, 82, 651–656. [Google Scholar] [CrossRef] [PubMed]
- Ruth, K.S.; The Endometrial Cancer Association Consortium; Day, F.R.; Tyrrell, J.; Thompson, D.J.; Wood, A.R.; Mahajan, A.; Beaumont, R.N.; Wittemans, L.; Martin, S.; et al. Using human genetics to understand the disease impacts of testosterone in men and women. Nat. Med. 2020, 26, 252–258. [Google Scholar] [CrossRef] [PubMed]
- Simons, P.I.H.G.; Valkenburg, O.; Bons, J.A.P.; Stehouwer, C.D.A.; Brouwers, M.C.G.J. The relationships of sex hormone-binding globulin, total testosterone, androstenedione and free testosterone with metabolic and reproductive features of polycystic ovary syndrome. Endocrinol. Diabetes Metab. 2021, 4, e00267. [Google Scholar] [CrossRef] [PubMed]
- Hernández-Alonso, P.; Camacho-Barcia, L.; Bulló, M.; Salas-Salvadó, J. Nuts and Dried Fruits: An Update of Their Beneficial Effects on Type 2 Diabetes. Nutrients 2017, 9, 673. [Google Scholar] [CrossRef] [Green Version]
- Garcia-Aloy, M.; Hulshof, P.J.M.; Estruel-Amades, S.; Osté, M.C.J.; Lankinen, M.; Geleijnse, J.M.; De Goede, J.; Ulaszewska, M.; Mattivi, F.; Bakker, S.J.L.; et al. Biomarkers of food intake for nuts and vegetable oils: An extensive literature search. Genes Nutr. 2019, 14, 7. [Google Scholar] [CrossRef]
- López-Uriarte, P.; Bulló, M.; Casas-Agustench, P.; Babio, N.; Salas-Salvadó, J. Nuts and oxidation: A systematic review. Nutr. Rev. 2009, 67, 497–508. [Google Scholar] [CrossRef]
- Jiang, R.; Jacobs, D.R., Jr.; Mayer-Davis, E.; Szklo, M.; Herrington, D.; Jenny, N.S.; Kronmal, R.; Barr, R.G. Nut and Seed Consumption and Inflammatory Markers in the Multi-Ethnic Study of Atherosclerosis. Am. J. Epidemiol. 2006, 163, 222–231. [Google Scholar] [CrossRef] [Green Version]
- Salas-Salvadó, J.; Garcia-Arellano, A.; Estruch, R.; Marquez-Sandoval, F.; Corella, D.; Fiol, M.; Gómez-Gracia, E.; Viñoles, E.; Arós, F.; Herrera, C.; et al. Components of the mediterranean-type food pattern and serum inflammatory markers among patients at high risk for cardiovascular disease. Eur. J. Clin. Nutr. 2008, 62, 651–659. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Abdelhamid, A.; Martin, N.; Bridges, C.; Brainard, J.S.; Wang, X.; Brown, T.J.; Hanson, S.; Jimoh, O.F.; Ajabnoor, S.M.; Deane, K.H.; et al. Polyunsaturated fatty acids for the primary and secondary prevention of cardiovascular disease. Cochrane Database Syst. Rev. 2018, 11, CD012345. [Google Scholar] [CrossRef] [PubMed]
- Manach, C.; Williamson, G.; Morand, C.; Scalbert, A.; Rémésy, C. Bioavailability and bioefficacy of polyphenols in humans. I. Review of 97 bioavailability studies. Am. J. Clin. Nutr. 2005, 81, 230S–242S. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fraga, C.G.; Croft, K.D.; Kennedy, D.O.; Tomás-Barberán, F.A. The effects of polyphenols and other bioactives on human health. Food Funct. 2019, 10, 514–528. [Google Scholar] [CrossRef] [Green Version]
- Guasch-Ferré, M.; Merino, J.; Sun, Q.; Fitó, M.; Salas-Salvadó, J. Dietary Polyphenols, Mediterranean Diet, Prediabetes, and Type 2 Diabetes: A Narrative Review of the Evidence. Oxid. Med. Cell. Longev. 2017, 2017, 6723931. [Google Scholar] [CrossRef]
- Luca, S.V.; Macovei, I.; Bujor, A.; Miron, A.; Skalicka-Woźniak, K.; Aprotosoaie, A.C.; Trifan, A. Bioactivity of dietary polyphenols: The role of metabolites. Crit. Rev. Food Sci. Nutr. 2020, 60, 626–659. [Google Scholar] [CrossRef]
- Cano-Marquina, A.; Tarín, J.J.; Cano, A. The impact of coffee on health. Maturitas 2013, 75, 7–21. [Google Scholar] [CrossRef]
- Casas-Agustench, P.; Bulló, M.; Salas-Salvadó, J. Nuts, inflammation and insulin resistance. Asia Pac. J. Clin. Nutr. 2010, 19, 124–130. [Google Scholar]
- Lorenzon Dos Santos, J.; Quadros, A.S.; Weschenfelder, C.; Garofallo, S.B.; Marcadenti, A. Oxidative Stress Biomarkers, Nut-Related Antioxidants, and Cardiovascular Disease. Nutrients 2020, 12, 682. [Google Scholar] [CrossRef] [Green Version]
- Kim, Y.; Keogh, J.B.; Clifton, P.M. Benefits of Nut Consumption on Insulin Resistance and Cardiovascular Risk Factors: Multiple Potential Mechanisms of Actions. Nutr. 2017, 9, 1271. [Google Scholar] [CrossRef] [Green Version]
- Coelho, S.B.; de Sales, R.L.; Iyer, S.S.; Bressan, J.; Costa, N.M.B.; Lokko, P.; Mattes, R. Effects of peanut oil load on energy expenditure, body composition, lipid profile, and appetite in lean and overweight adults. Nutrition 2006, 22, 585–592. [Google Scholar] [CrossRef] [PubMed]
- Agebratt, C.; Ström, E.; Romu, T.; Dahlqvist-Leinhard, O.; Borga, M.; Leanderson, P.; Nystrom, F.H. A Randomized Study of the Effects of Additional Fruit and Nuts Consumption on Hepatic Fat Content, Cardiovascular Risk Factors and Basal Metabolic Rate. PLoS ONE 2016, 11, e0147149. [Google Scholar] [CrossRef] [PubMed]
- Sugizaki, C.S.A.; Naves, M.M.V. Potential Prebiotic Properties of Nuts and Edible Seeds and Their Relationship to Obesity. Nutrients 2018, 10, 1645. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Castro-Barquero, S.; Lamuela-Raventós, R.M.; Doménech, M.; Estruch, R. Relationship between Mediterranean Dietary Polyphenol Intake and Obesity. Nutrients 2018, 10, 1523. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kang, I.; Buckner, T.; Shay, N.F.; Gu, L.; Chung, S. Improvements in Metabolic Health with Consumption of Ellagic Acid and Subsequent Conversion into Urolithins: Evidence and Mechanisms. Adv. Nutr. Int. Rev. J. 2016, 7, 961–972. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Xiong, Y.; Swaminath, G.; Cao, Q.; Yang, L.; Guo, Q.; Salomonis, H.; Lu, J.; Houze, J.B.; Dransfield, P.J.; Wang, Y.; et al. Activation of FFA1 mediates GLP-1 secretion in mice. Evidence for allosterism at FFA1. Mol. Cell. Endocrinol. 2013, 369, 119–129. [Google Scholar] [CrossRef] [PubMed]
- Corella, L.; Ordovas, J.M. How does the Mediterranean diet promote cardiovascular health? Current progress toward molecular mechanisms. BioEssays 2014, 36, 526–537. [Google Scholar] [CrossRef]
- Ortega, F.J.; Cardona-Alvarado, M.I.; Mercader, J.M.; Moreno-Navarrete, J.M.; Moreno, M.; Sabater-Masdeu, M.; Fuentes-Batllevell, N.; Ramirez-Chavez, E.; Ricart, W.; Torres, J.M.; et al. Circulating profiling reveals the effect of a polyunsaturated fatty acid-enriched diet on common microRNAs. J. Nutr. Biochem. 2015, 26, 1095–1101. [Google Scholar] [CrossRef]
- Hernández-Alonso, P.; Giardina, S.; Salas-Salvadó, J.; Arcelin, P.; Bulló, M. Chronic pistachio intake modulates circulating microRNAs related to glucose metabolism and insulin resistance in prediabetic subjects. Eur. J. Nutr. 2017, 56, 2181–2191. [Google Scholar] [CrossRef]
- Chrysant, S.G.; Chrysant, G.S. Association of hypomagnesemia with cardiovascular diseases and hypertension. Int. J. Cardiol. Hypertens. 2019, 1, 100005. [Google Scholar] [CrossRef]
- Dominguez, L.J.; Veronese, N.; Barbagallo, M. Magnesium and Hypertension in Old Age. Nutrients 2020, 13, 139. [Google Scholar] [CrossRef] [PubMed]
- Griel, A.E.; Kris-Etherton, P.M. Tree nuts and the lipid profile: A review of clinical studies. Br. J. Nutr. 2006, 96, S68–S78. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- García-Conesa, M.T.; Chambers, K.; Combet, E.; Pinto, P.; Garcia-Aloy, M.; Andres-Lacueva, C.; De Pascual-Teresa, S.; Mena, P.; Ristic, A.K.; Hollands, W.J.; et al. Meta-Analysis of the Effects of Foods and Derived Products Containing Ellagitannins and Anthocyanins on Cardiometabolic Biomarkers: Analysis of Factors Influencing Variability of the Individual Responses. Int. J. Mol. Sci. 2018, 19, 694. [Google Scholar] [CrossRef] [Green Version]
- European Food Safety Authority (EFSA). Available online: https://www.efsa.europa.eu/en/efsajournal/pub/2074 (accessed on 15 December 2021).
- Feng, S.; Belwal, T.; Li, L.; Limwachiranon, J.; Liu, X.; Luo, Z. Phytosterols and their derivatives: Potential health-promoting uses against lipid metabolism and associated diseases, mechanism, and safety issues. Compr. Rev. Food Sci. Food Saf. 2020, 19, 1243–1267. [Google Scholar] [CrossRef] [PubMed]
- Julibert, A.; del Mar Bibiloni, M.; Gallardo-Alfaro, L.; Abbate, M.; Martínez-González, M.; Salas-Salvadó, J.; Corella, D.; Fitó, M.; Martínez, J.A.; Alonso-Gómez, M.; et al. Metabolic Syndrome Features and Excess Weight Were Inversely Associated with Nut Consumption after 1-Year Follow-Up in the PREDIMED-Plus Study. J. Nutr. 2020, 150, 3161–3170. [Google Scholar] [CrossRef]
- Ahola, A.J.; Forsblom, C.M.; Harjutsalo, V.; Groop, P.-H. Nut Consumption Is Associated with Lower Risk of Metabolic Syndrome and Its Components in Type 1 Diabetes. Nutrients 2021, 13, 3909. [Google Scholar] [CrossRef]
- Mozaffarian, D.; Hao, T.; Rimm, E.B.; Willett, W.C.; Hu, F.B. Changes in Diet and Lifestyle and Long-Term Weight Gain in Women and Men. N. Engl. J. Med. 2011, 364, 2392–2404. [Google Scholar] [CrossRef] [Green Version]
- Schlesinger, S.; Neuenschwander, M.; Schwedhelm, C.; Hoffmann, G.; Bechthold, A.; Boeing, H.; Schwingshackl, L. Food Groups and Risk of Overweight, Obesity, and Weight Gain: A Systematic Review and Dose-Response Meta-Analysis of Prospective Studies. Adv. Nutr. Int. Rev. J. 2019, 10, 205–218. [Google Scholar] [CrossRef] [Green Version]
- Akhlaghi, M.; Ghobadi, S.; Zare, M.; Foshati, S. Effect of nuts on energy intake, hunger, and fullness, a systematic review and meta-analysis of randomized clinical trials. Crit. Rev. Food Sci. Nutr. 2020, 60, 84–93. [Google Scholar] [CrossRef]
- Fernández-Rodríguez, R.; Mesas, A.; Garrido-Miguel, M.; Martínez-Ortega, I.; Jiménez-López, E.; Martínez-Vizcaíno, V. The Relationship of Tree Nuts and Peanuts with Adiposity Parameters: A Systematic Review and Network Meta-Analysis. Nutrients 2021, 13, 2251. [Google Scholar] [CrossRef]
- Fernández-Rodríguez, R.; Martínez-Vizcaíno, V.; Garrido-Miguel, M.; Martínez-Ortega, I.A.; Álvarez-Bueno, C.; Mesas, A.E. Nut consumption, body weight, and adiposity in patients with type 2 diabetes: A systematic review and meta-analysis of randomized controlled trials. Nutr. Rev. 2021, 80, 645–655. [Google Scholar] [CrossRef] [PubMed]
- Guarneiri, L.L.; Cooper, J.A. Intake of Nuts or Nut Products Does Not Lead to Weight Gain, Independent of Dietary Substitution Instructions: A Systematic Review and Meta-Analysis of Randomized Trials. Adv. Nutr. Int. Rev. J. 2021, 12, 384–401. [Google Scholar] [CrossRef] [PubMed]
- Nishi, S.K.; Viguiliouk, E.; Mejia, S.B.; Kendall, C.W.C.; Bazinet, R.P.; Hanley, A.J.; Comelli, E.M.; Salvadó, J.S.; Jenkins, D.J.A.; Sievenpiper, J.L. Are fatty nuts a weighty concern? A systematic review and meta-analysis and dose–response meta-regression of prospective cohorts and randomized controlled trials. Obes. Rev. 2021, 22, e13330. [Google Scholar] [CrossRef] [PubMed]
- Fang, Z.; Dang, M.; Zhang, W.; Wang, Y.; Kord-Varkaneh, H.; Nazary-Vannani, A.; Santos, H.O.; Tan, S.C.; Clark, C.C.; Zanghelini, F.; et al. Effects of walnut intake on anthropometric characteristics: A systematic review and dose-response meta-analysis of randomized controlled trials. Complement. Ther. Med. 2020, 50, 102395. [Google Scholar] [CrossRef] [PubMed]
- Asbaghi, O.; Hadi, A.; Campbell, M.S.; Venkatakrishnan, K.; Ghaedi, E. Effects of pistachios on anthropometric indices, inflammatory markers, endothelial function and blood pressure in adults: A systematic review and meta-analysis of randomised controlled trials. Br. J. Nutr. 2020, 126, 718–729. [Google Scholar] [CrossRef] [PubMed]
- Xia, K.; Yang, T.; An, L.-Y.; Lin, Y.-Y.; Qi, Y.-X.; Chen, X.-Z.; Sun, D.-L. The relationship between pistachio (Pistacia vera L) intake and adiposity. Medicine 2020, 99, e21136. [Google Scholar] [CrossRef] [PubMed]
- Jamshidi, S.; Moradi, Y.; Nameni, G.; Mohsenpour, M.A.; Vafa, M. Effects of cashew nut consumption on body composition and glycemic indices: A meta-analysis and systematic review of randomized controlled trials. Diabetes Metab. Syndr. Clin. Res. Rev. 2021, 15, 605–613. [Google Scholar] [CrossRef]
- Lee-Bravatti, M.A.; Wang, J.; Avendano, E.E.; King, L.; Johnson, E.J.; Raman, G. Almond Consumption and Risk Factors for Cardiovascular Disease: A Systematic Review and Meta-analysis of Randomized Controlled Trials. Adv. Nutr. 2019, 10, 1076–1088. [Google Scholar] [CrossRef]
- Fantino, M.; Bichard, C.; Mistretta, F.; Bellisle, F. Daily consumption of pistachios over 12 weeks improves dietary profile without increasing body weight in healthy women: A randomized controlled intervention. Appetite 2020, 144, 104483. [Google Scholar] [CrossRef]
- Rock, C.L.; Zunshine, E.; Nguyen, H.T.; Perez, A.O.; Zoumas, C.; Pakiz, B.; White, M.M. Effects of Pistachio Consumption in a Behavioral Weight Loss Intervention on Weight Change, Cardiometabolic Factors, and Dietary Intake. Nutrients 2020, 12, 2155. [Google Scholar] [CrossRef]
- Wang, J.; Wang, S.; Henning, S.; Qin, T.; Pan, Y.; Yang, J.; Huang, J.; Tseng, C.-H.; Heber, D.; Li, Z. Mixed Tree Nut Snacks Compared to Refined Carbohydrate Snacks Resulted in Weight Loss and Increased Satiety during Both Weight Loss and Weight Maintenance: A 24-Week Randomized Controlled Trial. Nutrients 2021, 13, 1512. [Google Scholar] [CrossRef] [PubMed]
- Freisling, H.; Noh, H.; Slimani, N.; Chajès, V.; May, A.M.; Peeters, P.H.; Weiderpass, E.; Cross, A.J.; Skeie, G.; Jenab, M.; et al. Nut intake and 5-year changes in body weight and obesity risk in adults: Results from the EPIC-PANACEA study. Eur. J. Nutr. 2018, 57, 2399–2408. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Estruch, R.; Martínez-González, M.A.; Corella, D.; Salas-Salvadó, J.; Fitó, M.; Chiva-Blanch, G.; Fiol, M.; Gómez-Gracia, E.; Arós, F.; Lapetra, J.; et al. Effect of a high-fat Mediterranean diet on bodyweight and waist circumference: A prespecified secondary outcomes analysis of the PREDIMED randomised controlled trial. Lancet Diabetes Endocrinol. 2019, 7, e6–e17. [Google Scholar] [CrossRef]
- Salas-Salvadó, J.; Guasch-Ferré, M.; Bulló, M.; Sabaté, J. Nuts in the prevention and treatment of metabolic syndrome. Am. J. Clin. Nutr. 2014, 100, 399S–407S. [Google Scholar] [CrossRef] [Green Version]
- Afshin, A.; Micha, R.; Khatibzadeh, S.; Mozaffarian, D. Consumption of nuts and legumes and risk of incident ischemic heart disease, stroke, and diabetes: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2014, 100, 278–288. [Google Scholar] [CrossRef]
- Kim, Y.; Keogh, J.; Clifton, P.M. Nuts and Cardio-Metabolic Disease: A Review of Meta-Analyses. Nutrients 2018, 10, 1935. [Google Scholar] [CrossRef] [Green Version]
- Becerra-Tomás, N.; Paz-Graniel, I.; Hernández-Alonso, P.; Jenkins, D.J.A.; Kendall, C.W.C.; Sievenpiper, J.L.; Salas-Salvadó, J. Nut consumption and type 2 diabetes risk: A systematic review and meta-analysis of observational studies. Am. J. Clin. Nutr. 2021, 113, 960–971. [Google Scholar] [CrossRef]
- Tindall, A.M.; Johnston, E.A.; Kris-Etherton, P.M.; Petersen, K.S. The effect of nuts on markers of glycemic control: A systematic review and meta-analysis of randomized controlled trials. Am. J. Clin. Nutr. 2019, 109, 297–314. [Google Scholar] [CrossRef]
- Ntzouvani, A.; Antonopoulou, S.; Nomikos, T. Effects of nut and seed consumption on markers of glucose metabolism in adults with prediabetes: A systematic review of randomised controlled trials. Br. J. Nutr. 2019, 122, 361–375. [Google Scholar] [CrossRef]
- Muley, A.; Fernandez, R.; Ellwood, L.; Muley, P.; Shah, M. Effect of tree nuts on glycemic outcomes in adults with type 2 diabetes mellitus: A systematic review. JBI Évid. Synth. 2021, 19, 966–1002. [Google Scholar] [CrossRef]
- Ojo, O.; Wang, X.-H.; Ojo, O.O.; Adegboye, A.R.A. The Effects of Almonds on Gut Microbiota, Glycometabolism, and Inflammatory Markers in Patients with Type 2 Diabetes: A Systematic Review and Meta-Analysis of Randomised Controlled Trials. Nutrients 2021, 13, 3377. [Google Scholar] [CrossRef] [PubMed]
- Brown, R.; Ware, L.; Gray, A.R.; Chisholm, A.; Tey, S.L. Snacking on Almonds Lowers Glycaemia and Energy Intake Compared to a Popular High-Carbohydrate Snack Food: An Acute Randomised Crossover Study. Int. J. Environ. Res. Public Health 2021, 18, 10989. [Google Scholar] [CrossRef] [PubMed]
- Arab, L.; Dhaliwal, S.K.; Martin, C.J.; Larios, A.D.; Jackson, N.J.; Elashoff, D. Association between walnut consumption and diabetes risk in NHANES. Diabetes/Metab. Res. Rev. 2018, 34, e3031. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Neale, E.P.; Guan, V.; Tapsell, L.C.; Probst, Y.C. Effect of walnut consumption on markers of blood glucose control: A systematic review and meta-analysis. Br. J. Nutr. 2020, 124, 641–653. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Guo, Z.; Qi, S.; Fang, T.; Zhu, H.; Santos, H.O.; Khani, V.; Wong, C.H.; Qiu, Z. Walnut intake may increase circulating adiponectin and leptin levels but does not improve glycemic biomarkers: A systematic review and meta-analysis of randomized clinical trials. Complement. Ther. Med. 2020, 52, 102505. [Google Scholar] [CrossRef] [PubMed]
- Azad, B.J.; Daneshzad, E.; Azadbakht, L. Peanut and cardiovascular disease risk factors: A systematic review and meta-analysis. Crit. Rev. Food Sci. Nutr. 2020, 60, 1123–1140. [Google Scholar] [CrossRef] [PubMed]
- Ghanavati, M.; Rahmani, J.; Clark, C.C.; Hosseinabadi, S.M.; Rahimlou, M. Pistachios and cardiometabolic risk factors: A systematic review and meta-analysis of randomized controlled clinical trials. Complement. Ther. Med. 2020, 52, 102513. [Google Scholar] [CrossRef]
- Guasch-Ferré, M.; Hernández-Alonso, P.; Drouin-Chartier, J.-P.; Ruiz-Canela, M.; Razquin, C.; Toledo, E.; Li, J.; Dennis, C.; Wittenbecher, C.; Corella, D.; et al. Walnut Consumption, Plasma Metabolomics, and Risk of Type 2 Diabetes and Cardiovascular Disease. J. Nutr. 2021, 151, 303–311. [Google Scholar] [CrossRef]
- Djoussé, L.; Rudich, T.; Gaziano, J.M. Nut consumption and risk of hypertension in US male physicians. Clin. Nutr. 2009, 28, 10–14. [Google Scholar] [CrossRef] [Green Version]
- Martínez-Lapiscina, E.; Pimenta, A.; Beunza, J.; Bes-Rastrollo, M.; Martínez, J.; Martínez-González, M. Nut consumption and incidence of hypertension: The SUN prospective cohort. Nutr. Metab. Cardiovasc. Dis. 2010, 20, 359–365. [Google Scholar] [CrossRef]
- Ndanuko, R.N.; Tapsell, L.C.; Charlton, K.E.; Neale, E.P.; Batterham, M.J. Dietary Patterns and Blood Pressure in Adults: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Adv. Nutr. Int. Rev. J. 2016, 7, 76–89. [Google Scholar] [CrossRef] [PubMed]
- Del Gobbo, L.C.; Falk, M.C.; Feldman, R.; Lewis, K.; Mozaffarian, D. Effects of tree nuts on blood lipids, apolipoproteins, and blood pressure: Systematic review, meta-analysis, and dose-response of 61 controlled intervention trials. Am. J. Clin. Nutr. 2015, 102, 1347–1356. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Schwingshackl, L.; Hoffmann, G.; Iqbal, K.; Schwedhelm, C.; Boeing, H. Food groups and intermediate disease markers: A systematic review and network meta-analysis of randomized trials. Am. J. Clin. Nutr. 2018, 108, 576–586. [Google Scholar] [CrossRef] [PubMed]
- Jalali, M.; Karamizadeh, M.; Ferns, G.A.; Zare, M.; Moosavian, S.P.; Akbarzadeh, M. The effects of cashew nut intake on lipid profile and blood pressure: A systematic review and meta-analysis of randomized controlled trials. Complement. Ther. Med. 2020, 50, 102387. [Google Scholar] [CrossRef] [PubMed]
- Eslampour, E.; Asbaghi, O.; Hadi, A.; Abedi, S.; Ghaedi, E.; Lazaridi, A.-V.; Miraghajani, M. The effect of almond intake on blood pressure: A systematic review and meta-analysis of randomized controlled trials. Complement. Ther. Med. 2020, 50, 102399. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Jiang, B.; Santos, H.O.; Santos, D.; Singh, A.; Wang, L. Effects of walnut intake on blood pressure: A systematic review and meta-analysis of randomized controlled trials. Phytother. Res. 2020, 34, 2921–2931. [Google Scholar] [CrossRef]
- Sabaté, J.; Oda, K.; Ros, E. Nut Consumption and Blood Lipid Levels. Arch. Intern. Med. 2010, 170, 821–827. [Google Scholar] [CrossRef] [Green Version]
- Guasch-Ferré, M.; Li, J.; Hu, F.B.; Salas-Salvadó, J.; Tobias, D.K. Effects of walnut consumption on blood lipids and other car-diovascular risk factors: An updated meta-analysis and systematic review of controlled trials. Am. J. Clin. Nutr. 2018, 108, 174–187. [Google Scholar] [CrossRef] [Green Version]
- Liu, K.; Hui, S.; Wang, B.; Kaliannan, K.; Guo, X.; Liang, L. Comparative effects of different types of tree nut consumption on blood lipids: A network meta-analysis of clinical trials. Am. J. Clin. Nutr. 2020, 111, 219–227. [Google Scholar] [CrossRef]
- Hadi, A.; Asbaghi, O.; Kazemi, M.; Haghighian, H.K.; Pantovic, A.; Ghaedi, E.; Zadeh, F.A. Consumption of pistachio nuts positively affects lipid profiles: A systematic review and meta-analysis of randomized controlled trials. Crit. Rev. Food Sci. Nutr. 2021, 1–14. [Google Scholar] [CrossRef]
- Musa-Veloso, K.; Paulionis, L.; Poon, T.; Lee, H.Y. The effects of almond consumption on fasting blood lipid levels: A systematic review and meta-analysis of randomised controlled trials. J. Nutr. Sci. 2016, 5, e34. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Asbaghi, O.; Moodi, V.; Hadi, A.; Eslampour, E.; Shirinbakhshmasoleh, M.; Ghaedi, E.; Miraghajani, M. The effect of almond intake on lipid profile: A systematic review and meta-analysis of randomized controlled trials. Food Funct. 2021, 12, 1882–1896. [Google Scholar] [CrossRef] [PubMed]
- Morvaridzadeh, M.; Sepidarkish, M.; Farsi, F.; Akbari, A.; Mostafai, R.; Omidi, A.; Potter, E.; Heshmati, J. Effect of Cashew Nut on Lipid Profile: A Systematic Review and Meta-Analysis. Complement. Med. Res. 2020, 27, 348–356. [Google Scholar] [CrossRef] [PubMed]
- Campos, V.P.; Portal, V.L.; Markoski, M.M.; Quadros, A.S.; Bersch-Ferreira, C.; Garavaglia, J.; Marcadenti, A. Effects of a healthy diet enriched or not with pecan nuts or extra-virgin olive oil on the lipid profile of patients with stable coronary artery disease: A randomised clinical trial. J. Hum. Nutr. Diet. 2019, 33, 439–450. [Google Scholar] [CrossRef]
- Dikariyanto, V.; Smith, L.; Francis, L.; Robertson, M.; Kusaslan, E.; O’Callaghan-Latham, M.; Palanche, C.; D’Annibale, M.; Christodoulou, D.; Basty, N.; et al. Snacking on whole almonds for 6 weeks improves endothelial function and lowers LDL cholesterol but does not affect liver fat and other cardiometabolic risk factors in healthy adults: The ATTIS study, a randomized controlled trial. Am. J. Clin. Nutr. 2020, 111, 1178–1189. [Google Scholar] [CrossRef]
- Ghanavati, M.; Alipour Parsa, S.; Nasrollahzadeh, J. A calorie-restricted diet with nuts favourably raises plasma high-density lipoprotein-cholesterol in overweight and obese patients with stable coronary heart disease: A randomised controlled trial. Int. J. Clin. Pract. 2021, 75, e14431. [Google Scholar] [CrossRef]
- Rajaram, S.; Cofán, M.; Sala-Vila, A.; Haddad, E.; Serra-Mir, M.; Bitok, E.; Roth, I.; Freitas-Simoes, T.M.; Kaur, A.; Valls-Pedret, C.; et al. Effects of Walnut Consumption for 2 Years on Lipoprotein Subclasses Among Healthy Elders. Circulation 2021, 144, 1083–1085. [Google Scholar] [CrossRef]
- Hernáez, Á.; Castañer, O.; Elosua, R.; Pintó, X.; Estruch, R.; Salas-Salvadó, J.; Corella, D.; Arós, F.; Serra-Majem, L.; Fiol, M. Mediterranean Diet Improves High-Density Lipoprotein Function in High-Cardiovascular-Risk Individuals. Circulation 2017, 135, 633–643. [Google Scholar] [CrossRef] [Green Version]
- Grundy, S.M.; Stone, N.; Bailey, A.L.; Beam, C.; Birtcher, K.K.; Blumenthal, R.S.; Braun, L.T.; De Ferranti, S.; Faiella-Tommasino, J.; Forman, D.E.; et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA Guideline on the Management of Blood Cholesterol: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation 2019, 139, e1082–e1143. [Google Scholar] [CrossRef]
| Nutrient | Almonds | Cashews | Hazelnuts | Peanuts | Pecans | Pistachios | Walnuts |
|---|---|---|---|---|---|---|---|
| Total fat (g) | 49.9 | 43.9 | 60.8 | 49.2 | 72.0 | 45.3 | 65.2 |
| SFA (g) | 3.8 | 7.8 | 4.5 | 6.3 | 6.2 | 5.9 | 6.1 |
| MUFA (g) | 31.6 | 23.8 | 45.7 | 24.4 | 40.8 | 23.3 | 9.0 |
| PUFA (g) | 12.3 | 7.8 | 7.9 | 15.6 | 21.6 | 14.4 | 47.2 |
| CHO (g) | 21.6 | 30.2 | 16.7 | 16.1 | 13.9 | 27.2 | 13.7 |
| Protein (g) | 21.2 | 18.2 | 15.0 | 25.8 | 9.2 | 20.2 | 15.2 |
| Fiber (g) | 12.5 | 3.3 | 9.7 | 8.5 | 9.6 | 10.6 | 6.7 |
| Ca (mg) | 269 | 37 | 114 | 92 | 70 | 105 | 98 |
| K (mg) | 733 | 660 | 680 | 705 | 410 | 1025 | 441 |
| Mg (mg) | 270 | 292 | 163 | 168 | 121 | 121 | 158 |
| P (mg) | 481 | 593 | 290 | 376 | 277 | 490 | 346 |
| Phytosterols (mg) | 197 | 151 | 122 | NA | 158.8 | 214 | 110.2 |
| Total phenols (mg) | 287 | 137 | 687 | 406 | 1284 | 867 | 1576 |
| Vitamin E (mg) | 25.6 | 0.9 | 15.0 | 8.3 | 1.4 | 2.9 | 0.7 |
| Energy (Kcal) | 579 | 553 | 628 | 567 | 691 | 560 | 654 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bauset, C.; Martínez-Aspas, A.; Smith-Ballester, S.; García-Vigara, A.; Monllor-Tormos, A.; Kadi, F.; Nilsson, A.; Cano, A. Nuts and Metabolic Syndrome: Reducing the Burden of Metabolic Syndrome in Menopause. Nutrients 2022, 14, 1677. https://doi.org/10.3390/nu14081677
Bauset C, Martínez-Aspas A, Smith-Ballester S, García-Vigara A, Monllor-Tormos A, Kadi F, Nilsson A, Cano A. Nuts and Metabolic Syndrome: Reducing the Burden of Metabolic Syndrome in Menopause. Nutrients. 2022; 14(8):1677. https://doi.org/10.3390/nu14081677
Chicago/Turabian StyleBauset, Celia, Ana Martínez-Aspas, Sara Smith-Ballester, Alicia García-Vigara, Aitana Monllor-Tormos, Fawzi Kadi, Andreas Nilsson, and Antonio Cano. 2022. "Nuts and Metabolic Syndrome: Reducing the Burden of Metabolic Syndrome in Menopause" Nutrients 14, no. 8: 1677. https://doi.org/10.3390/nu14081677
APA StyleBauset, C., Martínez-Aspas, A., Smith-Ballester, S., García-Vigara, A., Monllor-Tormos, A., Kadi, F., Nilsson, A., & Cano, A. (2022). Nuts and Metabolic Syndrome: Reducing the Burden of Metabolic Syndrome in Menopause. Nutrients, 14(8), 1677. https://doi.org/10.3390/nu14081677









