Is Secretory Activation Delayed in Women with Type Two Diabetes? A Pilot Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Data and Sample Collection
2.2. Post-Delivery Data (Collected from Hospital Medical Records)
2.3. Postpartum Data (Collected by Telephone 4 Months Postpartum)
2.4. Breastmilk Collection and Breastmilk Analysis
2.5. Assay Validation and Quality Control
2.6. Statistical Methods
3. Results
3.1. Cohort
3.2. Clinical Parameters
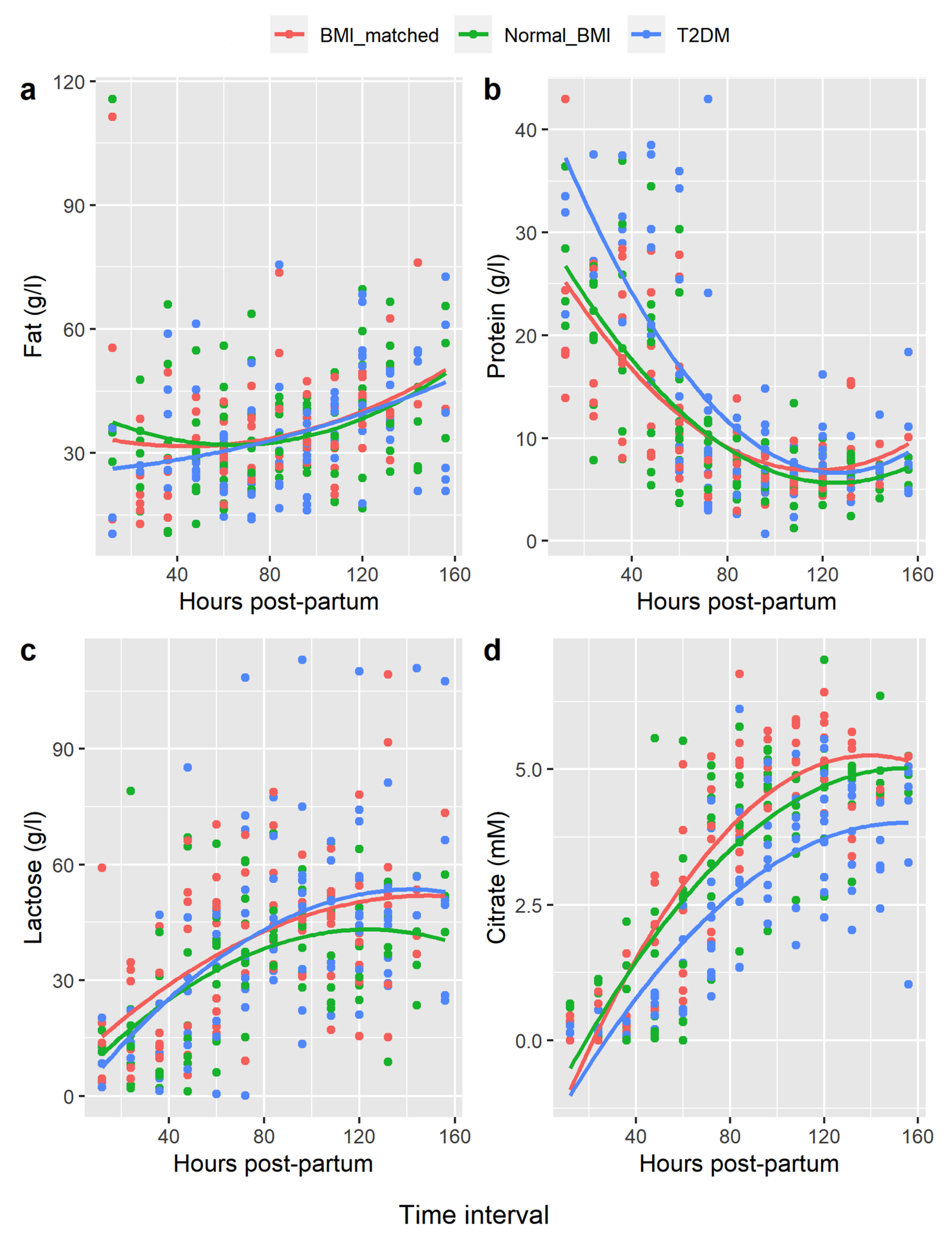
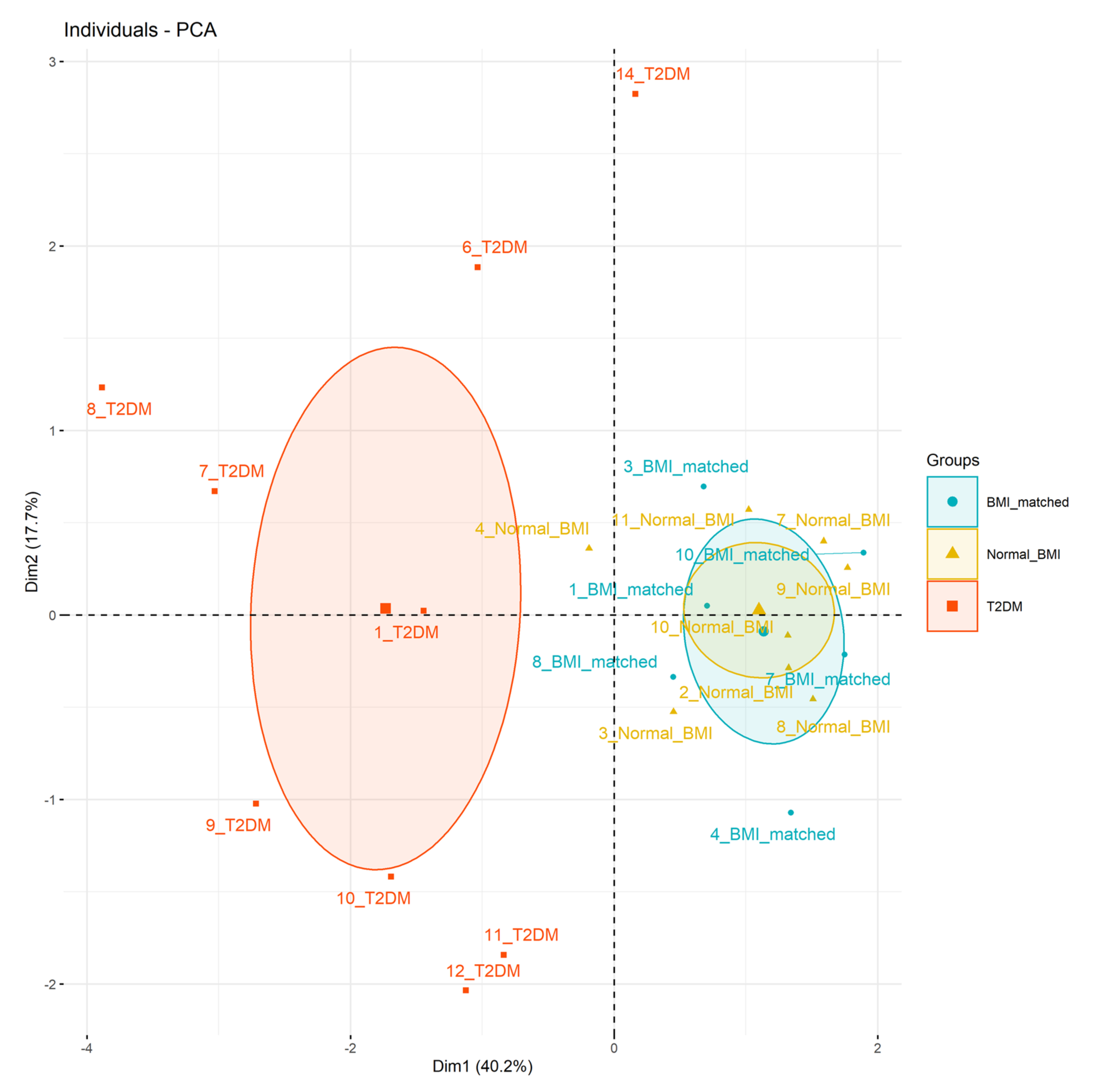
3.3. Breastmilk Analysis
4. Discussion
4.1. Role of Citrate in Lactation and as a Marker of SA
4.2. Breastmilk Constituents in Obesity and Type 2 Diabetes
4.3. Insulin Resistance and SA in Women with Type 2 Diabetes
4.4. Obesity and SA
4.5. Formula Supplementation, Infant Hypoglycaemia, and SA
4.6. Demographic and Iatrogenic Factors Previously Demonstrated to Affect SA
4.7. Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Gunderson, E.P.; Jacobs, D.R., Jr.; Chiang, V.; Lewis, C.E.; Feng, J.; Quesenberry, C.P., Jr.; Sidney, S. Duration of lactation and incidence of the metabolic syndrome in women of reproductive age according to gestational diabetes mellitus status: A 20-Year prospective study in CARDIA (Coronary Artery Risk Development in Young Adults). Diabetes 2010, 59, 495–504. [Google Scholar] [CrossRef] [PubMed]
- Herskin, C.W.; Stage, E.; Barfred, C.; Emmersen, P.; Ladefoged Nichum, V.; Damm, P.; Mathiesen, E.R. Low prevalence of long-term breastfeeding among women with type 2 diabetes. J. Matern.-Fetal Neonatal Med. 2016, 29, 2513–2518. [Google Scholar] [CrossRef] [PubMed]
- Soltani, H.; Arden, M. Factors associated with breastfeeding up to 6 months postpartum in mothers with diabetes. J. Obstet. Gynecol. Neonatal Nurs. JOGNN/NAACOG 2009, 38, 586–594. [Google Scholar] [CrossRef] [PubMed]
- Longmore, D.K.; Barr, E.L.M.; Wilson, A.N.; Barzi, F.; Kirkwood, M.; Simmonds, A.; Lee, I.L.; Hawthorne, E.; Van Dokkum, P.; Connors, C.; et al. Associations of gestational diabetes and type 2 diabetes during pregnancy with breastfeeding at hospital discharge and up to 6 months: The PANDORA study. Diabetologia 2020, 63, 2571–2581. [Google Scholar] [CrossRef] [PubMed]
- Nolan, C.J.; Damm, P.; Prentki, M. Type 2 diabetes across generations: From pathophysiology to prevention and management. Lancet 2011, 378, 169–181. [Google Scholar] [CrossRef]
- Chapman, D.J.; Perez-Escamilla, R. Identification of risk factors for delayed onset of lactation. J. Am. Diet. Assoc. 1999, 99, 450–454. [Google Scholar] [CrossRef]
- Kulski, J.K.; Hartmann, P.E. Changes in human milk composition during the initiation of lactation. Aust. J. Exp. Biol. Med. Sci. 1981, 59, 101–114. [Google Scholar] [CrossRef]
- Neville, M.C.; Morton, J. Physiology and endocrine changes underlying human lactogenesis II. J. Nutr. 2001, 131, 3005S–3008S. [Google Scholar] [CrossRef]
- Chapman, D.J.; Perez-Escamilla, R. Does delayed perception of the onset of lactation shorten breastfeeding duration? J. Hum. Lact. Off. J Int. Lact. Consult. Assoc. 1999, 15, 107–111. [Google Scholar] [CrossRef]
- De Bortoli, J.; Amir, L.H. Is onset of lactation delayed in women with diabetes in pregnancy? A systematic review. Diabet. Med. J. Br. Diabet. Assoc. 2016, 33, 17–24. [Google Scholar] [CrossRef]
- Nommsen-Rivers, L.A. Does Insulin Explain the Relation between Maternal Obesity and Poor Lactation Outcomes? An Overview of the Literature. Adv. Nutr. 2016, 7, 407–414. [Google Scholar] [CrossRef] [PubMed]
- Chapman, D.J.; Perez-Escamilla, R. Maternal perception of the onset of lactation is a valid, public health indicator of lactogenesis stage II. J. Nutr. 2000, 130, 2972–2980. [Google Scholar] [CrossRef] [PubMed]
- Neville, M.C.; Morton, J.; Umemura, S. Lactogenesis. The transition from pregnancy to lactation. Pediatr. Clin. N. Am. 2001, 48, 35–52. [Google Scholar] [CrossRef]
- Neville, M.C.; Allen, J.C.; Archer, P.C.; Casey, C.E.; Seacat, J.; Keller, R.P.; Lutes, V.; Rasbach, J.; Neifert, M. Studies in human lactation: Milk volume and nutrient composition during weaning and lactogenesis. Am. J. Clin. Nutr. 1991, 54, 81–92. [Google Scholar] [CrossRef]
- Medina Poeliniz, C.; Engstrom, J.L.; Hoban, R.; Patel, A.L.; Meier, P. Measures of Secretory Activation for Research and Practice: An Integrative Review. Breastfeed. Med. Off. J. Acad. Breastfeed. Med. 2020, 15, 191–212. [Google Scholar] [CrossRef]
- Neville, M.C.; Keller, R.; Seacat, J.; Lutes, V.; Neifert, M.; Casey, C.; Allen, J.; Archer, P. Studies in human lactation: Milk volumes in lactating women during the onset of lactation and full lactation. Am. J. Clin. Nutr. 1988, 48, 1375–1386. [Google Scholar] [CrossRef]
- Arthur, P.G.; Smith, M.; Hartmann, P.E. Milk lactose, citrate and glucose as markers of lactogenesis in normal and diabetic women. J. Pediatr. Gastroenterol. Nutr. 1989, 9, 488–496. [Google Scholar] [CrossRef]
- Azulay Chertok, I.R.; Haile, Z.T.; Shuisong, N.; Kennedy, M. Differences in Human Milk Lactose and Citrate Concentrations Based on Gestational Diabetes Status. Breastfeed. Med. Off. J. Acad. Breastfeed. Med. 2020, 15, 798–802. [Google Scholar] [CrossRef]
- Lucas, A.; Gibbs, J.A.; Lyster, R.L.; Baum, J.D. Creamatocrit: Simple clinical technique for estimating fat concentration and energy value of human milk. Br. Med. J 1978, 1, 1018–1020. [Google Scholar] [CrossRef]
- Mitoulas, L.R.; Kent, J.C.; Cox, D.B.; Owens, R.A.; Sherriff, J.L.; Hartmann, P.E. Variation in fat, lactose and protein in human milk over 24 h and throughout the first year of lactation. Br. J. Nutr. 2002, 88, 29–37. [Google Scholar] [CrossRef]
- Atwood, C.S.; Hartmann, P.E. Collection of fore and hind milk from the sow and the changes in milk composition during suckling. J. Dairy Res. 1992, 59, 287–298. [Google Scholar] [CrossRef] [PubMed]
- Du, J.; Gay, M.C.L.; Lai, C.T.; Trengove, R.D.; Hartmann, P.E.; Geddes, D.T. Comparison of gravimetric, creamatocrit and esterified fatty acid methods for determination of total fat content in human milk. Food Chem. 2017, 217, 505–510. [Google Scholar] [CrossRef] [PubMed]
- Caglar, M.U.; Teufel, A.I.; Wilke, C.O. Sicegar: R package for sigmoidal and double-sigmoidal curve fitting. PeerJ 2018, 6, e4251. [Google Scholar] [CrossRef] [PubMed]
- Motulsky, H.J.; Brown, R.E. Detecting outliers when fitting data with nonlinear regression–a new method based on robust nonlinear regression and the false discovery rate. BMC Bioinform. 2006, 7, 123. [Google Scholar] [CrossRef] [PubMed]
- Meurant, G. Handbook of Milk Composition; Jensen, R.G., Ed.; Academic Press: Cambridge, MA, USA, 1995. [Google Scholar]
- Peaker, M.; Linzell, J.L. Citrate in milk: A harbinger of lactogenesis. Nature 1975, 253, 464. [Google Scholar] [CrossRef]
- Matias, S.L.; Dewey, K.G.; Quesenberry, C.P., Jr.; Gunderson, E.P. Maternal prepregnancy obesity and insulin treatment during pregnancy are independently associated with delayed lactogenesis in women with recent gestational diabetes mellitus. Am. J. Clin. Nutr. 2014, 99, 115–121. [Google Scholar] [CrossRef] [PubMed]
- Chamorro, R.; Bascunan, K.A.; Barrera, C.; Sandoval, J.; Puigrredon, C.; Valenzuela, R. Reduced n-3 and n-6 PUFA (DHA and AA) Concentrations in Breast Milk and Erythrocytes Phospholipids during Pregnancy and Lactation in Women with Obesity. Int. J. Environ. Res. Public Health 2022, 19, 1930. [Google Scholar] [CrossRef]
- Rudland, V.L.; Price, S.A.L.; Hughes, R.; Barrett, H.L.; Lagstrom, J.; Porter, C.; Britten, F.L.; Glastras, S.; Fulcher, I.; Wein, P.; et al. ADIPS 2020 guideline for pre-existing diabetes and pregnancy. Aust. N. Z. J. Obstet. Gynaecol. 2020, 60, E18–E52. [Google Scholar] [CrossRef]
- Berlato, C.; Doppler, W. Selective response to insulin versus insulin-like growth factor-I and -II and up-regulation of insulin receptor splice variant B in the differentiated mouse mammary epithelium. Endocrinology 2009, 150, 2924–2933. [Google Scholar] [CrossRef]
- Neville, M.C.; Picciano, M.F. Regulation of milk lipid secretion and composition. Annu. Rev. Nutr. 1997, 17, 159–183. [Google Scholar] [CrossRef]
- Vanky, E.; Nordskar, J.J.; Leithe, H.; Hjorth-Hansen, A.K.; Martinussen, M.; Carlsen, S.M. Breast size increment during pregnancy and breastfeeding in mothers with polycystic ovary syndrome: A follow-up study of a randomised controlled trial on metformin versus placebo. BJOG 2012, 119, 1403–1409. [Google Scholar] [CrossRef] [PubMed]
- Hummel, S.; Hummel, M.; Knopff, A.; Bonifacio, E.; Ziegler, A.G. Breastfeeding in women with gestational diabetes. Dtsch. Med. Wochenschr. 2008, 133, 180–184. [Google Scholar] [CrossRef]
- Gaudio, M.; Dozio, N.; Feher, M.; Scavini, M.; Caretto, A.; Joy, M.; Van Vlymer, J.; Hinton, W.; de Lusignan, S. Trends in Factors Affecting Pregnancy Outcomes Among Women With Type 1 or Type 2 Diabetes of Childbearing Age (2004-2017). Fr. Endocrinol. 2020, 11, 596633. [Google Scholar] [CrossRef]
- Nommsen-Rivers, L.A.; Chantry, C.J.; Peerson, J.M.; Cohen, R.J.; Dewey, K.G. Delayed onset of lactogenesis among first-time mothers is related to maternal obesity and factors associated with ineffective breastfeeding. Am. J. Clin. Nutr. 2010, 92, 574–584. [Google Scholar] [CrossRef] [PubMed]
- Amir, L.H.; Donath, S. A systematic review of maternal obesity and breastfeeding intention, initiation and duration. BMC Pregnancy Childbirth 2007, 7, 9. [Google Scholar] [CrossRef]
- Morrow, D.A. Fat cow syndrome. J. Dairy Sci. 1976, 59, 1625–1629. [Google Scholar] [CrossRef]
- Shaw, M.A.; Rasmussen, K.M.; Myers, T.R. Consumption of a High Fat Diet Impairs Reproductive Performance in Sprague-Dawley Rats. J. Nutr. 1997, 127, 64–69. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Chantry, C.J.; Dewey, K.G.; Peerson, J.M.; Wagner, E.A.; Nommsen-Rivers, L.A. In-hospital formula use increases early breastfeeding cessation among first-time mothers intending to exclusively breastfeed. J. Pediatr. 2014, 164, 1339-45.e5. [Google Scholar] [CrossRef]
- Parry, J.E.; Ip, D.K.; Chau, P.Y.; Wu, K.M.; Tarrant, M. Predictors and consequences of in-hospital formula supplementation for healthy breastfeeding newborns. J. Hum. Lact. Off. J. Int. Lact. Consult. Assoc. 2013, 29, 527–536. [Google Scholar] [CrossRef]
- Whipps, M.D.M.; Yoshikawa, H.; Demirci, J.R.; Hill, J. Estimating the Impact of In-Hospital Infant Formula Supplementation on Breastfeeding Success. Breastfeed. Med. Off J. Acad. Breastfeed. Med. 2021, 16, 530–538. [Google Scholar] [CrossRef]
- Flaherman, V.J.; Cabana, M.D.; McCulloch, C.E.; Paul, I.M. Effect of Early Limited Formula on Breastfeeding Duration in the First Year of Life: A Randomized Clinical Trial. JAMA Pediatr. 2019, 173, 729–735. [Google Scholar] [CrossRef] [PubMed]
- Fok, D.; Aris, I.M.; Ho, J.H.; Chan, Y.H.; Rauff, M.; Lui, J.K.; Cregan, M.D.; Hartmann, P.; Chong, Y.S.; Mattar, C.N. Early initiation and regular breast milk expression reduces risk of lactogenesis II delay in at-risk Singaporean mothers in a randomised trial. Singap. Med. J. 2019, 60, 80–88. [Google Scholar] [CrossRef] [PubMed]
- Edwards, T.; Harding, J.E. Clinical Aspects of Neonatal Hypoglycemia: A Mini Review. Front. Pediatr 2020, 8, 562251. [Google Scholar] [CrossRef] [PubMed]
- Merjaneh, N.; Williams, P.; Inman, S.; Schumacher, M.; Ciurte, A.; Smotherman, C.; Alissa, R.; Hudak, M. The impact on the exclusive breastfeeding rate at 6 months of life of introducing supplementary donor milk into the level 1 newborn nursery. J. Perinatol. Off. J. Calif. Perinat. Assoc. 2020, 40, 1109–1114. [Google Scholar] [CrossRef] [PubMed]
- Australian Institute of Health and Welfare. Australia’s Children; Report No.: Cat. no. CWS 69; AIHW: Canberra, Australia, 2020. [Google Scholar]
| T2DM (a) | BMI-Matched (b) | Normal BMI (c) | Comparison, p-Value | |
|---|---|---|---|---|
| n | 14 | 10 | 12 | |
| Pre-pregnancy BMI | 30.6 ± 6.1 | 27.9 ± 4.7 | 21.1 ± 1.6 | <0.001 *** a vs. b, 0.37 a vs. c, <0.001 *** b vs. c, 0.005 ** |
| Pre-delivery BMI | 33.7 ± 6.8 | 33.1 ± 5.5 | 25.8 ± 2.6 | 0.001 ** a vs. b, 0.96 a vs. c, 0.002 ** b vs. c, 0.009 ** |
| Age at due date (years) | 35.1 ± 5.2 | 33.1 ± 5.6 | 34.0 ± 4.1 | a vs. b, vs. c, 0.63 |
| Education (degree or higher) | (11/14) 79% | (5/10) 50% | (8/12) 67% | a vs. b, 0.20 a vs. c, 0.67 |
| Parity (1 or greater) | (10/14) 72% | 50% (5/10) | 75% (9/12) | a vs. b, 0.40 a vs. c, >0.99 |
| Breastfeeding intentions score (/16) | 14 ± 2 | 15 ± 2 | 15 ± 1 | a vs. b vs. c, 0.31 |
| Ethnicity (Caucasian vs. SE Asian) | 7/14 (50%) | 10/10 (100%) | 10/12 (83%) | a vs. b, 0.02 * a vs. c, 0.11 |
| Income >$AUD 50,000 AUD (>poverty threshold) | (11/14) (79%) | (10/10) 100% | 10/10 (100%) | a vs. b, 0.24 a vs. c, 0.24 |
| Income >$AUD 100,000 (>median income) | 4/14 (29%) | 5/10 (50%) | 5/10 (50%) | a vs. b, 0.40 a vs. c, 0.40 |
| Hypertension | 2/14 | 0/10 | 0/12 | a vs. b, 0.49 a vs. c, 0.48 |
| Polycystic ovarian syndrome | 2/14 (14%) | 2/10 (20%) | 0/12 (0%) | a vs. b, >0.99 a vs. c, 0.48 |
| Asthma | 4/14 (29%) | 3/10 (30%) | 1/12 (8%) | a vs. b, >0.99 a vs. c, 0.36 |
| Hypothyroidism | 3/14 (21%) | 1/10 (10%) | 1/12 (8%) | a vs. b, 0.61 a vs. c, 0.60 |
| Depression | 2/14 (14%) | 1/10 (10%) | 2/12 (17%) | a vs. b, >0.99 a vs. c, >0.99 |
| Other major systemic medical condition | 1/14 (7%) | 0/10 (0%) | 1/12 (0%) | a vs. b, >0.99 a vs. c, >0.99 |
| T2DM (a) | BMI-Matched (b) | Normal BMI (c) | Comparison, p-Value | |
|---|---|---|---|---|
| 14 | 10 | 12 | ||
| Infant birthweight (g) | 3248 ± 354 | 3367 ± 339 | 3316 ±469 | a vs. b vs. c, 0.76 |
| Gestational age at delivery (weeks) | 38.7 ± 1.1 | 39.4 ± 1.6 | 39.2 ± 0.9 | a vs. b vs. c, 0.39 |
| Vaginal birth (vs. caesarean section) | 7/14 (50%) | 7/10 (70%) | 6/12 (50%) | a vs. b, 0.42 a vs. c, >0.99 |
| Blood loss greater than 500 mls | 3/14 (21%) | 4/10 (40%) | 3/12 (25%) | a vs. b, 0.39 a vs. c, 0.99 |
| Pre-ecclampsia | 2/14 (14.2%) | 0/10 (0%) | 0/10 (0%) | a vs. b, 0.49 a vs. c, 0.48 |
| Regional anaesthesia for delivery | 10/14 (71%) | 8/10 (80%) | 9/12 (75%) | a vs. b, >0.99 a vs. c, >0.99 |
| SCN or ICN admission | 4/14 (29%) | 1/10 (10%) | 2/12 (17%) | a vs. b, 0.36 a vs. c, 0.65 |
| Neonatal hypoglycaemia | 10/14 (71%) | 0/10 (0%) | 1/12 (8%) | a vs. b, >0.001 *** a vs. c, 0.002 ** |
| Breastfed in first hour of life | 13/14 (92.86%) | 7/10 (70.0%) | 11/12 (92%) | a vs. b, 0.27 a vs. c, >0.99 |
| Supplemented formula during admission | 10/14 (71%) | 3/10 (30%) | 3/12 (25%) | a vs. b, 0.09 a vs. c, 0.047 * b vs. c, >0.99 |
| Breastfeeding fully + discharge (vs. breastmilk and formula) | 6/14 (43%) | 9/10 (90%) | 11/12 (92%) | a vs. b, 0.03 * a vs. c, 0.01 * b vs. c, >0.99 |
| Breastfeeding fully + at 4 months postpartum | 3/13 (23%) | 2/9 (22%) | 8/12 (67%) | a vs. b, >0.99 a vs. c, 0.047 * b vs. c, 0.08 |
| Any breastfeeding at 4 months postpartum | 8/13 (62%) | 5/9 (56%) | 10/12 (83%) | a vs. b, >0.99 a vs. c, 0.38 b vs. c, 0.33 |
| Variable | T2DM (Group a) | BMI-Matched (Group b) | Normal BMI (Group c) | Comparison, p-Value |
|---|---|---|---|---|
| Plateau Citrate Value for all available curves (mM) (n = 30) | n = 10 3.63 ± 0.60 | n = 10 4.59 ± 0.66 | n = 10 4.33 ± 0.60 | 0.005 ** a vs. b, 0.005** a vs. c, 0.04* b vs. c, 0.64 |
| Time to Plateau Citrate Value for all available curves (n = 30) | n = 10 82.25 ± 22.40 | n = 10 76.25 ± 12.29 | n = 10 67.69 ± 19.21 | a vs. b vs. c, 0.23 |
| Mean citrate at midpoint of rapid rise (mM) | n = 10 2.06 ± 0.38 | n = 10 2.60 ± 0.38 | n = 10 2.46 ± 0.34 | 0.005 ** a vs. b, 0.005** a vs. c, 0.04* b vs. c, 0.64 |
| Time to mean citrate at midpoint of rapid rise | n = 10 68.7 ± 12.33 | n = 10 59.86 ± 12.69 | n = 10 55.09 ± 17.72 | a vs. b vs. c, 0.12 |
| Time to Citrate 2.4 (mM) | n = 10 72.92 ± 16.20 | n = 10 58.08 ± 13.33 | n = 10 55.19 ± 16.87 | a vs. b vs. c, 0.04* a vs. b, 0.10 a vs. c, 0.04* b vs. c, 0.91 |
| Time to Citrate 3.6 (mM) | n = 7 77.88 ± 21.38 | n = 10 65.83 ± 11.90 | n = 10 63.14 ± 17.39 | a vs. b vs. c, 0.20 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Britten, F.L.; Lai, C.T.; Geddes, D.T.; Callaway, L.K.; Duncan, E.L. Is Secretory Activation Delayed in Women with Type Two Diabetes? A Pilot Study. Nutrients 2022, 14, 1323. https://doi.org/10.3390/nu14071323
Britten FL, Lai CT, Geddes DT, Callaway LK, Duncan EL. Is Secretory Activation Delayed in Women with Type Two Diabetes? A Pilot Study. Nutrients. 2022; 14(7):1323. https://doi.org/10.3390/nu14071323
Chicago/Turabian StyleBritten, Fiona L., Ching T. Lai, Donna T. Geddes, Leonie K. Callaway, and Emma L. Duncan. 2022. "Is Secretory Activation Delayed in Women with Type Two Diabetes? A Pilot Study" Nutrients 14, no. 7: 1323. https://doi.org/10.3390/nu14071323
APA StyleBritten, F. L., Lai, C. T., Geddes, D. T., Callaway, L. K., & Duncan, E. L. (2022). Is Secretory Activation Delayed in Women with Type Two Diabetes? A Pilot Study. Nutrients, 14(7), 1323. https://doi.org/10.3390/nu14071323





