Circulating SIRT1 and Sclerostin Correlates with Bone Status in Young Women with Different Degrees of Adiposity
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Population
2.2. Biochemistry and Kidney Function
2.3. Plasma SIRT1 and Sclerostin Assay
2.4. Dual-Energy X-ray Absorptiometry and Trabecular Bone Score (TBS) Analysis
2.5. Statistical Methods
3. Results
3.1. Clinical Features and Differences between Groups Stratified by BMI
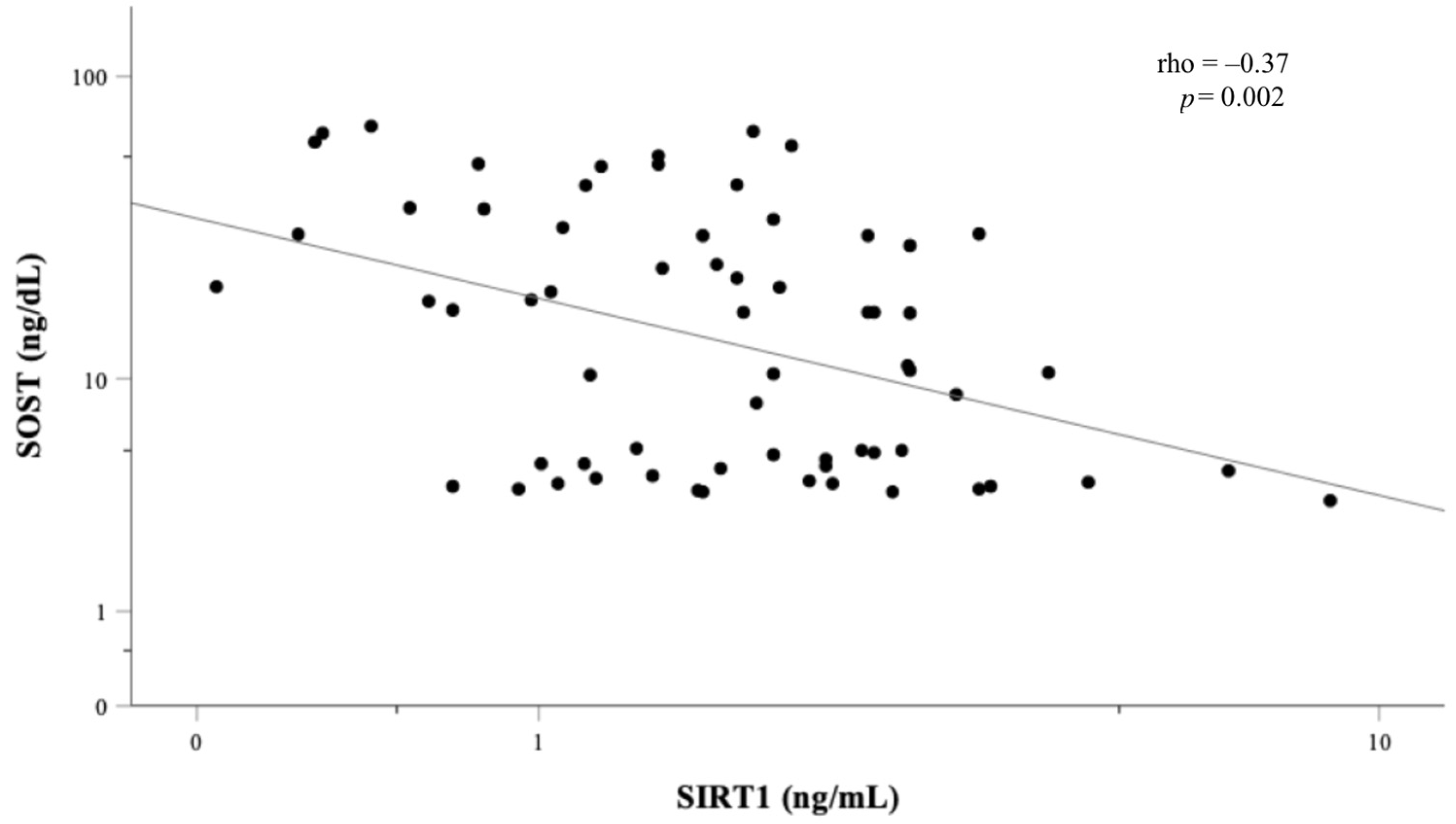
3.2. Association between Body Composition and Circulating SIRT1 and Sclerostin
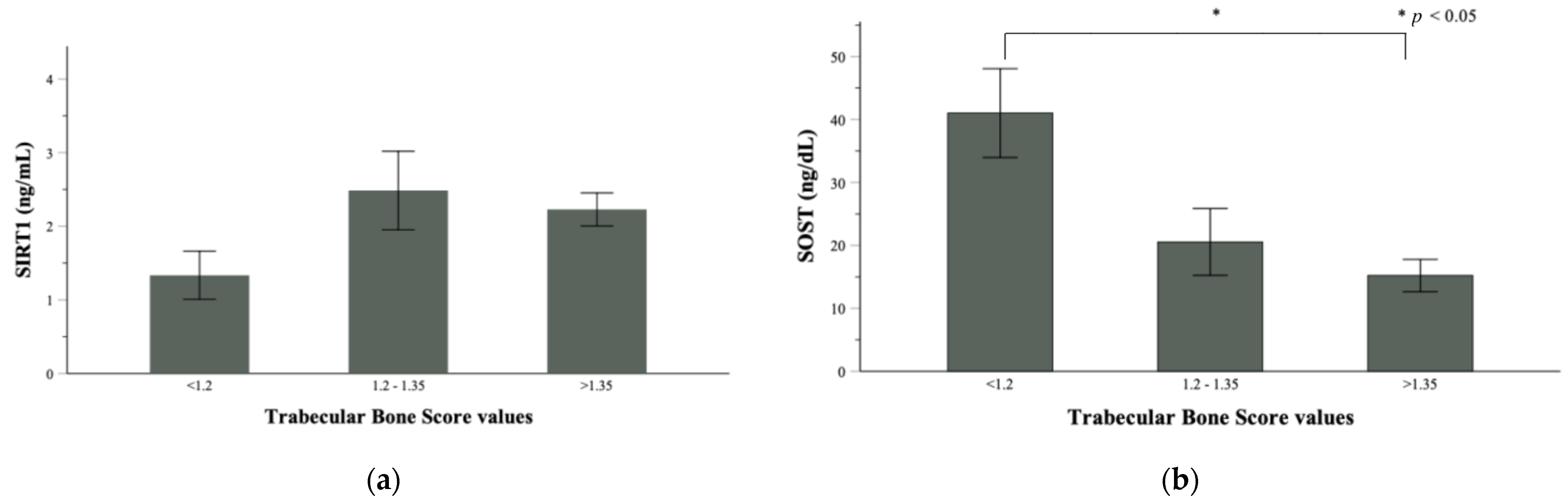
3.3. Correlation Analyses between Bone Parameters, Body Composition and Circulating SIRT1 and Sclerostin, and Multiple Regression Analyses for BMD and TBS Predictors
3.4. Linear Correlation and Multiple Regression Analyses between BMI-Adjusted BMD and TBS and Circulating SIRT1 and Sclerostin
3.5. Linear Correlation and Regression Analyses between SIRT1, Sclerostin and Bone Parameters among Normal-Weight and Obese Patients
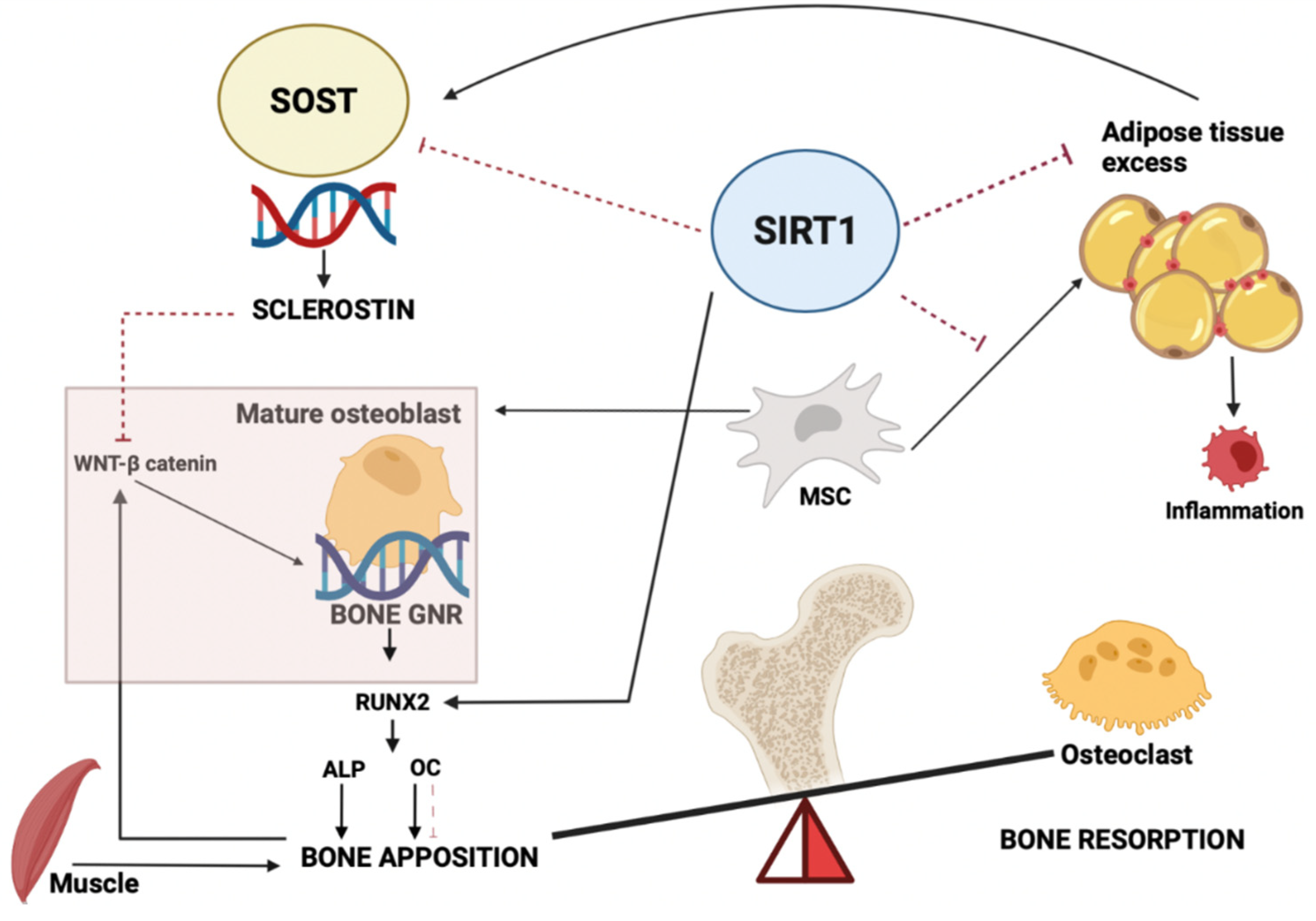
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Liu, J.; Curtis, E.M.; Cooper, C.; Harvey, N.C. State of the Art in Osteoporosis Risk Assessment and Treatment. J. Endocrinol. Invest. 2019, 42, 1149–1164. [Google Scholar] [CrossRef]
- Reid, I.R. A Broader Strategy for Osteoporosis Interventions. Nat. Rev. Endocrinol. 2020, 16, 333–339. [Google Scholar] [CrossRef]
- Turcotte, A.-F.; O’Connor, S.; Morin, S.N.; Gibbs, J.C.; Willie, B.M.; Jean, S.; Gagnon, C. Association between Obesity and Risk of Fracture, Bone Mineral Density and Bone Quality in Adults: A Systematic Review and Meta-Analysis. PLoS ONE 2021, 16, e0252487. [Google Scholar] [CrossRef] [PubMed]
- Fassio, A.; Idolazzi, L.; Rossini, M.; Gatti, D.; Adami, G.; Giollo, A.; Viapiana, O. The Obesity Paradox and Osteoporosis. Eat. Weight Disord. 2018, 23, 293–302. [Google Scholar] [CrossRef] [PubMed]
- Maïmoun, L.; Renard, E.; Humbert, L.; Aouinti, S.; Mura, T.; Boudousq, V.; Lefebvre, P.; Mahadea, K.; Philibert, P.; de Santa-Barbara, P.; et al. Modification of Bone Mineral Density, Bone Geometry and Volumetric BMD in Young Women with Obesity. Bone 2021, 150, 116005. [Google Scholar] [CrossRef] [PubMed]
- Palermo, A.; Tuccinardi, D.; Defeudis, G.; Watanabe, M.; D’Onofrio, L.; Lauria Pantano, A.; Napoli, N.; Pozzilli, P.; Manfrini, S. BMI and BMD: The Potential Interplay between Obesity and Bone Fragility. Int. J. Environ. Res. Public Health 2016, 13, 544. [Google Scholar] [CrossRef]
- Jackuliak, P.; Kužma, M.; Killinger, Z.; Payer, J. Good Long-Term Glycemic Compensation Is Associated with Better Trabecular Bone Score in Postmenopausal Women with Type 2 Diabetes. Physiol. Res. 2019, 68, S149–S156. [Google Scholar] [CrossRef]
- Nakagawa, T.; Guarente, L. Sirtuins at a Glance. J. Cell Sci. 2011, 124, 833–838. [Google Scholar] [CrossRef]
- Mariani, S.; Fiore, D.; Persichetti, A.; Basciani, S.; Lubrano, C.; Poggiogalle, E.; Genco, A.; Donini, L.M.; Gnessi, L. Circulating SIRT1 Increases After Intragastric Balloon Fat Loss in Obese Patients. Obes. Surg. 2016, 26, 1215–1220. [Google Scholar] [CrossRef]
- Mariani, S.; di Giorgio, M.R.; Martini, P.; Persichetti, A.; Barbaro, G.; Basciani, S.; Contini, S.; Poggiogalle, E.; Sarnicola, A.; Genco, A.; et al. Inverse Association of Circulating SIRT1 and Adiposity: A Study on Underweight, Normal Weight, and Obese Patients. Front. Endocrinol. 2018, 9, 449. [Google Scholar] [CrossRef]
- Mansur, A.P.; Roggerio, A.; Goes, M.F.S.; Avakian, S.D.; Leal, D.P.; Maranhão, R.C.; Strunz, C.M.C. Serum Concentrations and Gene Expression of Sirtuin 1 in Healthy and Slightly Overweight Subjects after Caloric Restriction or Resveratrol Supplementation: A Randomized Trial. Int. J. Cardiol. 2017, 227, 788–794. [Google Scholar] [CrossRef]
- Chen, Y.; Zhou, F.; Liu, H.; Li, J.; Che, H.; Shen, J.; Luo, E. SIRT1, a Promising Regulator of Bone Homeostasis. Life Sci. 2021, 269, 119041. [Google Scholar] [CrossRef]
- Zainabadi, K. Drugs Targeting SIRT1, a New Generation of Therapeutics for Osteoporosis and Other Bone Related Disorders? Pharmacol. Res. 2019, 143, 97–105. [Google Scholar] [CrossRef]
- Song, J.; Li, J.; Yang, F.; Ning, G.; Zhen, L.; Wu, L.; Zheng, Y.; Zhang, Q.; Lin, D.; Xie, C.; et al. Nicotinamide Mononucleotide Promotes Osteogenesis and Reduces Adipogenesis by Regulating Mesenchymal Stromal Cells via the SIRT1 Pathway in Aged Bone Marrow. Cell Death Dis. 2019, 10, 336. [Google Scholar] [CrossRef]
- Bäckesjö, C.-M.; Li, Y.; Lindgren, U.; Haldosén, L.-A. Activation of Sirt1 Decreases Adipocyte Formation during Osteoblast Differentiation of Mesenchymal Stem Cells. J. Bone Miner. Res. 2006, 21, 993–1002. [Google Scholar] [CrossRef]
- Zainabadi, K.; Liu, C.J.; Caldwell, A.L.M.; Guarente, L. SIRT1 Is a Positive Regulator of in Vivo Bone Mass and a Therapeutic Target for Osteoporosis. PLoS ONE 2017, 12, e0185236. [Google Scholar] [CrossRef]
- Artsi, H.; Cohen-Kfir, E.; Gurt, I.; Shahar, R.; Bajayo, A.; Kalish, N.; Bellido, T.M.; Gabet, Y.; Dresner-Pollak, R. The Sirtuin1 Activator SRT3025 Down-Regulates Sclerostin and Rescues Ovariectomy-Induced Bone Loss and Biomechanical Deterioration in Female Mice. Endocrinology 2014, 155, 3508–3515. [Google Scholar] [CrossRef]
- Ornstrup, M.J.; Harsløf, T.; Kjær, T.N.; Langdahl, B.L.; Pedersen, S.B. Resveratrol Increases Bone Mineral Density and Bone Alkaline Phosphatase in Obese Men: A Randomized Placebo-Controlled Trial. J. Clin. Endocrinol. Metab. 2014, 99, 4720–4729. [Google Scholar] [CrossRef]
- Morvan, F.; Boulukos, K.; Clément-Lacroix, P.; Roman Roman, S.; Suc-Royer, I.; Vayssière, B.; Ammann, P.; Martin, P.; Pinho, S.; Pognonec, P.; et al. Deletion of a Single Allele of the Dkk1 Gene Leads to an Increase in Bone Formation and Bone Mass. J. Bone Miner. Res. 2006, 21, 934–945. [Google Scholar] [CrossRef]
- Cohen-Kfir, E.; Artsi, H.; Levin, A.; Abramowitz, E.; Bajayo, A.; Gurt, I.; Zhong, L.; D’Urso, A.; Toiber, D.; Mostoslavsky, R.; et al. Sirt1 Is a Regulator of Bone Mass and a Repressor of Sost Encoding for Sclerostin, a Bone Formation Inhibitor. Endocrinology 2011, 152, 4514–4524. [Google Scholar] [CrossRef]
- Mariani, S.; Di Giorgio, M.R.; Rossi, E.; Tozzi, R.; Contini, S.; Bauleo, L.; Cipriani, F.; Toscano, R.; Basciani, S.; Barbaro, G.; et al. Blood SIRT1 Shows a Coherent Association with Leptin and Adiponectin in Relation to the Degree and Distribution of Adiposity: A Study in Obesity, Normal Weight and Anorexia Nervosa. Nutrients 2020, 12, 33506. [Google Scholar] [CrossRef]
- Ardawi, M.-S.M.; Al-Kadi, H.A.; Rouzi, A.A.; Qari, M.H. Determinants of Serum Sclerostin in Healthy Pre- and Postmenopausal Women. J. Bone Miner. Res. 2011, 26, 2812–2822. [Google Scholar] [CrossRef] [PubMed]
- Sheng, Z.; Tong, D.; Ou, Y.; Zhang, H.; Zhang, Z.; Li, S.; Zhou, J.; Zhang, J.; Liao, E. Serum Sclerostin Levels Were Positively Correlated with Fat Mass and Bone Mineral Density in Central South Chinese Postmenopausal Women. Clin. Endocrinol. 2012, 76, 797–801. [Google Scholar] [CrossRef] [PubMed]
- Kuipers, A.L.; Zhang, Y.; Yu, S.; Kammerer, C.M.; Nestlerode, C.S.; Chu, Y.; Bunker, C.H.; Patrick, A.L.; Wheeler, V.W.; Miljkovic, I.; et al. Relative Influence of Heritability, Environment and Genetics on Serum Sclerostin. Osteoporos. Int. 2014, 25, 905–912. [Google Scholar] [CrossRef] [PubMed]
- Levey, A.S.; Stevens, L.A.; Schmid, C.H.; Zhang, Y.L.; Castro, A.F.; Feldman, H.I.; Kusek, J.W.; Eggers, P.; Van Lente, F.; Greene, T.; et al. A New Equation to Estimate Glomerular Filtration Rate. Ann. Intern. Med. 2009, 150, 604–612. [Google Scholar] [CrossRef]
- Mariani, S.; Fiore, D.; Varone, L.; Basciani, S.; Persichetti, A.; Watanabe, M.; Saponara, M.; Spera, G.; Moretti, C.; Gnessi, L. Obstructive Sleep Apnea and Bone Mineral Density in Obese Patients. Diabetes Metab. Syndr. Obes. 2012, 5, 395–401. [Google Scholar] [CrossRef] [PubMed]
- Adult Positions. ISCD. Available online: https://iscd.org/learn/official-positions/adult-positions/ (accessed on 15 December 2021).
- Silva, B.C.; Leslie, W.D.; Resch, H.; Lamy, O.; Lesnyak, O.; Binkley, N.; McCloskey, E.V.; Kanis, J.A.; Bilezikian, J.P. Trabecular Bone Score: A Noninvasive Analytical Method Based upon the DXA Image. J. Bone Miner. Res. 2014, 29, 518–530. [Google Scholar] [CrossRef] [PubMed]
- Obesity and Overweight. Available online: https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight (accessed on 15 December 2021).
- Devlin, M.J.; Rosen, C.J. The Bone-Fat Interface: Basic and Clinical Implications of Marrow Adiposity. Lancet Diabetes Endocrinol. 2015, 3, 141–147. [Google Scholar] [CrossRef]
- Cohen, A.; Dempster, D.W.; Stein, E.M.; Nickolas, T.L.; Zhou, H.; McMahon, D.J.; Müller, R.; Kohler, T.; Zwahlen, A.; Lappe, J.M.; et al. Increased Marrow Adiposity in Premenopausal Women with Idiopathic Osteoporosis. J. Clin. Endocrinol. Metab. 2012, 97, 2782–2791. [Google Scholar] [CrossRef]
- Reid, I.R.; Baldock, P.A.; Cornish, J. Effects of Leptin on the Skeleton. Endocr. Rev. 2018, 39, 938–959. [Google Scholar] [CrossRef]
- Chait, A.; den Hartigh, L.J. Adipose Tissue Distribution, Inflammation and Its Metabolic Consequences, Including Diabetes and Cardiovascular Disease. Front. Cardiovasc. Med. 2020, 7, 22. [Google Scholar] [CrossRef]
- Iyer, S.; Han, L.; Bartell, S.M.; Kim, H.-N.; Gubrij, I.; de Cabo, R.; O’Brien, C.A.; Manolagas, S.C.; Almeida, M. Sirtuin1 (Sirt1) Promotes Cortical Bone Formation by Preventing β-Catenin Sequestration by FoxO Transcription Factors in Osteoblast Progenitors. J. Biol. Chem. 2014, 289, 24069–24078. [Google Scholar] [CrossRef]
- Lemieux, M.E.; Yang, X.; Jardine, K.; He, X.; Jacobsen, K.X.; Staines, W.A.; Harper, M.E.; McBurney, M.W. The Sirt1 Deacetylase Modulates the Insulin-like Growth Factor Signaling Pathway in Mammals. Mech. Ageing Dev. 2005, 126, 1097–1105. [Google Scholar] [CrossRef]
- Mercken, E.M.; Mitchell, S.J.; Martin-Montalvo, A.; Minor, R.K.; Almeida, M.; Gomes, A.P.; Scheibye-Knudsen, M.; Palacios, H.H.; Licata, J.J.; Zhang, Y.; et al. SRT2104 Extends Survival of Male Mice on a Standard Diet and Preserves Bone and Muscle Mass. Aging Cell 2014, 13, 787–796. [Google Scholar] [CrossRef]
- Chekroun, A.; Pujo-Menjouet, L.; Falcoz, S.; Tsuen, K.; Yueh-Hsun Yang, K.; Berteau, J.-P. Theoretical Evidence of Osteoblast Self-Inhibition after Activation of the Genetic Regulatory Network Controlling Mineralization. J. Theor. Biol. 2022, 537, 111005. [Google Scholar] [CrossRef]
- Zainabadi, K.; Liu, C.J.; Guarente, L. SIRT1 Is a Positive Regulator of the Master Osteoblast Transcription Factor, RUNX2. PLoS ONE 2017, 12, e0178520. [Google Scholar] [CrossRef]
- Edwards, J.R.; Perrien, D.S.; Fleming, N.; Nyman, J.S.; Ono, K.; Connelly, L.; Moore, M.M.; Lwin, S.T.; Yull, F.E.; Mundy, G.R.; et al. Silent Information Regulator (Sir)T1 Inhibits NF-ΚB Signaling to Maintain Normal Skeletal Remodeling. J. Bone Miner. Res. 2013, 28, 960–969. [Google Scholar] [CrossRef]
- Zuo, H.-L.; Xin, H.; Yan, X.-N.; Huang, J.; Zhang, Y.-P.; Du, H. 17β-Estradiol Improves Osteoblastic Cell Function through the Sirt1/NF-ΚB/MMP-8 Pathway. Climacteric 2020, 23, 404–409. [Google Scholar] [CrossRef]
- Tamolienė, V.; Remmel, L.; Gruodyte-Raciene, R.; Jürimäe, J. Relationships of Bone Mineral Variables with Body Composition, Blood Hormones and Training Volume in Adolescent Female Athletes with Different Loading Patterns. Int. J. Environ. Res. Public Health 2021, 18, 6571. [Google Scholar] [CrossRef]
- Fowler, T.W.; Mitchell, T.L.; Janda, C.Y.; Xie, L.; Tu, S.; Chen, H.; Zhang, H.; Ye, J.; Ouyang, B.; Yuan, T.Z.; et al. Development of Selective Bispecific Wnt Mimetics for Bone Loss and Repair. Nat. Commun. 2021, 12, 3247. [Google Scholar] [CrossRef]
- Niziolek, P.J.; Farmer, T.L.; Cui, Y.; Turner, C.H.; Warman, M.L.; Robling, A.G. High-Bone-Mass-Producing Mutations in the Wnt Signaling Pathway Result in Distinct Skeletal Phenotypes. Bone 2011, 49, 1010–1019. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Kocijan, R.; Haschka, J.; Feurstein, J.; Zwerina, J. New Therapeutic Options for Bone Diseases. Wien. Med. Wochenschr. 2021, 171, 120–125. [Google Scholar] [CrossRef] [PubMed]
- Ma, S.; Wang, D.-D.; Ma, C.-Y.; Zhang, Y.-D. MicroRNA-96 Promotes Osteoblast Differentiation and Bone Formation in Ankylosing Spondylitis Mice through Activating the Wnt Signaling Pathway by Binding to SOST. J. Cell Biochem. 2019, 120, 15429–15442. [Google Scholar] [CrossRef] [PubMed]
- Aznou, A.; Meijer, R.; van Raalte, D.; den Heijer, M.; Heijboer, A.; de Jongh, R. Serum Sclerostin Is Negatively Associated with Insulin Sensitivity in Obese but Not Lean Women. Endocr. Connect. 2021, 10, 131–138. [Google Scholar] [CrossRef]
- Kim, S.P.; Frey, J.L.; Li, Z.; Kushwaha, P.; Zoch, M.L.; Tomlinson, R.E.; Da, H.; Aja, S.; Noh, H.L.; Kim, J.K.; et al. Sclerostin Influences Body Composition by Regulating Catabolic and Anabolic Metabolism in Adipocytes. Proc. Natl. Acad. Sci. USA 2017, 114, E11238–E11247. [Google Scholar] [CrossRef]
- Zeng, J.; Xiao, Q.; Li, X.; Chen, J. Advanced Oxidation Protein Products Aggravate Age-related Bone Loss by Increasing Sclerostin Expression in Osteocytes via ROS-dependent Downregulation of Sirt1. Int. J. Mol. Med. 2021, 47, 108. [Google Scholar] [CrossRef]
- Ross, D.S.; Yeh, T.-H.; King, S.; Mathers, J.; Rybchyn, M.S.; Neist, E.; Cameron, M.; Tacey, A.; Girgis, C.M.; Levinger, I.; et al. Distinct Effects of a High Fat Diet on Bone in Skeletally Mature and Developing Male C57BL/6J Mice. Nutrients 2021, 13, 1666. [Google Scholar] [CrossRef]
- Szulc, P.; Foesser, D.; Chapurlat, R. High Cardiovascular Risk in Older Men with Poor Bone Microarchitecture-The Prospective STRAMBO Study. J. Bone Miner. Res. 2021, 36, 879–891. [Google Scholar] [CrossRef]
- Morales-Santana, S.; García-Fontana, B.; García-Martín, A.; Rozas-Moreno, P.; García-Salcedo, J.A.; Reyes-García, R.; Muñoz-Torres, M. Atherosclerotic Disease in Type 2 Diabetes Is Associated with an Increase in Sclerostin Levels. Diabetes Care 2013, 36, 1667–1674. [Google Scholar] [CrossRef]
- Piccoli, A.; Cannata, F.; Strollo, R.; Pedone, C.; Leanza, G.; Russo, F.; Greto, V.; Isgrò, C.; Quattrocchi, C.C.; Massaroni, C.; et al. Sclerostin Regulation, Microarchitecture, and Advanced Glycation End-Products in the Bone of Elderly Women with Type 2 Diabetes. J. Bone Miner. Res. 2020, 35, 2415–2422. [Google Scholar] [CrossRef]
- Costa, A.G.; Walker, M.D.; Zhang, C.A.; Cremers, S.; Dworakowski, E.; McMahon, D.J.; Liu, G.; Bilezikian, J.P. Circulating Sclerostin Levels and Markers of Bone Turnover in Chinese-American and White Women. J. Clin. Endocrinol. Metab. 2013, 98, 4736–4743. [Google Scholar] [CrossRef][Green Version]
- Gaudio, A.; Pennisi, P.; Bratengeier, C.; Torrisi, V.; Lindner, B.; Mangiafico, R.A.; Pulvirenti, I.; Hawa, G.; Tringali, G.; Fiore, C.E. Increased Sclerostin Serum Levels Associated with Bone Formation and Resorption Markers in Patients with Immobilization-Induced Bone Loss. J. Clin. Endocrinol. Metab. 2010, 95, 2248–2253. [Google Scholar] [CrossRef]
- Suarjana, I.N.; Isbagio, H.; Soewondo, P.; Rachman, I.A.; Sadikin, M.; Prihartono, J.; Malik, S.G.; Soeroso, J. The Role of Serum Expression Levels of Microrna-21 on Bone Mineral Density in Hypostrogenic Postmenopausal Women with Osteoporosis: Study on Level of RANKL, OPG, TGFβ-1, Sclerostin, RANKL/OPG Ratio, and Physical Activity. Acta Med. Indones. 2019, 51, 245–252. [Google Scholar]
- Hannan, M.T.; Felson, D.T.; Dawson-Hughes, B.; Tucker, K.L.; Cupples, L.A.; Wilson, P.W.; Kiel, D.P. Risk Factors for Longitudinal Bone Loss in Elderly Men and Women: The Framingham Osteoporosis Study. J. Bone Miner. Res. 2000, 15, 710–720. [Google Scholar] [CrossRef]
- Ishimura, E.; Okuno, S.; Ichii, M.; Norimine, K.; Yamakawa, T.; Shoji, S.; Nishizawa, Y.; Inaba, M. Relationship between Serum Sclerostin, Bone Metabolism Markers, and Bone Mineral Density in Maintenance Hemodialysis Patients. J. Clin. Endocrinol. Metab. 2014, 99, 4315–4320. [Google Scholar] [CrossRef]
- Cejka, D.; Jäger-Lansky, A.; Kieweg, H.; Weber, M.; Bieglmayer, C.; Haider, D.G.; Diarra, D.; Patsch, J.M.; Kainberger, F.; Bohle, B.; et al. Sclerostin Serum Levels Correlate Positively with Bone Mineral Density and Microarchitecture in Haemodialysis Patients. Nephrol. Dial. Transplant. 2012, 27, 226–230. [Google Scholar] [CrossRef]
- Fijalkowski, I.; Geets, E.; Steenackers, E.; Van Hoof, V.; Ramos, F.J.; Mortier, G.; Fortuna, A.M.; Van Hul, W.; Boudin, E. A Novel Domain-Specific Mutation in a Sclerosteosis Patient Suggests a Role of LRP4 as an Anchor for Sclerostin in Human Bone. J. Bone Miner. Res. 2016, 31, 874–881. [Google Scholar] [CrossRef]
- Malgo, F.; Appelman-Dijkstra, N.M.; Termaat, M.F.; van der Heide, H.J.L.; Schipper, I.B.; Rabelink, T.J.; Hamdy, N.A.T. High Prevalence of Secondary Factors for Bone Fragility in Patients with a Recent Fracture Independently of BMD. Arch. Osteoporos. 2016, 11, 12. [Google Scholar] [CrossRef]
- Somemura, S.; Kumai, T.; Yatabe, K.; Sasaki, C.; Fujiya, H.; Niki, H.; Yudoh, K. Physiologic Mechanical Stress Directly Induces Bone Formation by Activating Glucose Transporter 1 (Glut 1) in Osteoblasts, Inducing Signaling via NAD+-Dependent Deacetylase (Sirtuin 1) and Runt-Related Transcription Factor 2 (Runx2). Int. J. Mol. Sci. 2021, 22, 9070. [Google Scholar] [CrossRef]
- Kong, S.H.; Hong, N.; Kim, J.-W.; Kim, D.Y.; Kim, J.H. Application of the Trabecular Bone Score in Clinical Practice. J. Bone Metab. 2021, 28, 101–113. [Google Scholar] [CrossRef]
- Giner, M.; Miranda, C.; Vázquez-Gámez, M.A.; Altea-Manzano, P.; Miranda, M.-J.; Casado-Díaz, A.; Pérez-Cano, R.; Montoya-García, M.-J. Microstructural and Strength Changes in Trabecular Bone in Elderly Patients with Type 2 Diabetes Mellitus. Diagnostics 2021, 11, 577. [Google Scholar] [CrossRef]
- Martineau, P.; Leslie, W.D. Trabecular Bone Score (TBS): Method and Applications. Bone 2017, 104, 66–72. [Google Scholar] [CrossRef]
- Watters, A.; Fielding, L.; Mehler, P.S. Bone Quality Assessed by Trabecular Bone Score in Severe Anorexia Nervosa: A Brief Report. Int J. Eat. Disord 2021, 54, 903–907. [Google Scholar] [CrossRef]
- Messina, C.; Buonomenna, C.; Menon, G.; Magnani, S.; Albano, D.; Gitto, S.; Ulivieri, F.M.; Sconfienza, L.M. Fat Mass Does Not Increase the Precision Error of Trabecular Bone Score Measurements. J. Clin. Densitom. 2019, 22, 359–366. [Google Scholar] [CrossRef]
- Romagnoli, E.; Lubrano, C.; Carnevale, V.; Costantini, D.; Nieddu, L.; Morano, S.; Migliaccio, S.; Gnessi, L.; Lenzi, A. Assessment of Trabecular Bone Score (TBS) in Overweight/Obese Men: Effect of Metabolic and Anthropometric Factors. Endocrine 2016, 54, 342–347. [Google Scholar] [CrossRef]
- Moon, H.U.; Lee, N.; Chung, Y.-S.; Choi, Y.J. Reduction of Visceral Fat Could Be Related to the Improvement of TBS in Diabetes Mellitus. J. Bone Miner. Metab. 2020, 38, 702–709. [Google Scholar] [CrossRef]
- Olmos, J.M.; Hernández, J.L.; Pariente, E.; Martínez, J.; Valero, C.; González-Macías, J. Trabecular Bone Score and Bone Quantitative Ultrasound in Spanish Postmenopausal Women. The Camargo Cohort Study. Maturitas 2020, 132, 24–29. [Google Scholar] [CrossRef] [PubMed]
- Koide, M.; Yamashita, T.; Murakami, K.; Uehara, S.; Nakamura, K.; Nakamura, M.; Matsushita, M.; Ara, T.; Yasuda, H.; Penninger, J.M.; et al. Sclerostin Expression in Trabecular Bone Is Downregulated by Osteoclasts. Sci. Rep. 2020, 10, 13751. [Google Scholar] [CrossRef] [PubMed]
- Braud, L.; Pini, M.; Stec, D.F.; Manin, S.; Derumeaux, G.; Stec, D.E.; Foresti, R.; Motterlini, R. Increased Sirt1 Secreted from Visceral White Adipose Tissue Is Associated with Improved Glucose Tolerance in Obese Nrf2-Deficient Mice. Redox. Biol. 2021, 38, 101805. [Google Scholar] [CrossRef] [PubMed]
- Potthast, A.B.; Nebl, J.; Wasserfurth, P.; Haufe, S.; Eigendorf, J.; Hahn, A.; Das, A. Impact of Nutrition on Short-Term Exercise-Induced Sirtuin Regulation: Vegans Differ from Omnivores and Lacto-Ovo Vegetarians. Nutrients 2020, 12, 1004. [Google Scholar] [CrossRef]
- Wasserfurth, P.; Nebl, J.; Rühling, M.R.; Shammas, H.; Bednarczyk, J.; Koehler, K.; Boßlau, T.K.; Krüger, K.; Hahn, A.; Das, A.M. Impact of Dietary Modifications on Plasma Sirtuins 1, 3 and 5 in Older Overweight Individuals Undergoing 12-Weeks of Circuit Training. Nutrients 2021, 13, 3824. [Google Scholar] [CrossRef]
- Gou, G.-H.; Tseng, F.-J.; Wang, S.-H.; Chen, P.-J.; Shyu, J.-F.; Pan, R.-Y. Nutritional Factors Associated with Femoral Neck Bone Mineral Density in Children and Adolescents. BMC Musculoskelet. Disord. 2019, 20, 520. [Google Scholar] [CrossRef]
- Idolazzi, L.; El Ghoch, M.; Dalle Grave, R.; Bazzani, P.V.; Calugi, S.; Fassio, S.; Caimmi, C.; Viapiana, O.; Bertoldo, F.; Braga, V.; et al. Bone Metabolism in Patients with Anorexia Nervosa and Amenorrhoea. Eat. Weight Disord. 2018, 23, 255–261. [Google Scholar] [CrossRef]
- Boskey, A.L.; Imbert, L. Bone Quality Changes Associated with Aging and Disease: A Review. Ann. N. Y. Acad. Sci. 2017, 1410, 93–106. [Google Scholar] [CrossRef]
- Bemer, P.; Di Lodovico, L.; Haykanush, O.; Théodon, H.; Briot, K.; Carlier, R.; Dicembre, M.; Duquesnoy, M.; Melchior, J.-C.; Hanachi, M. Bone Mineral Density at Extremely Low Weight in Patients with Anorexia Nervosa. Clin. Endocrinol. 2021, 95, 423–429. [Google Scholar] [CrossRef]
| Underweight | Normal Weight | Obesity | p-Value | |
|---|---|---|---|---|
| n | 16 | 25 | 25 | - |
| Age (years) | 22.9 ± 9.4 | 28.5 ± 6.5 | 36.5 ± 11.6 | <0.001 |
| Weight (kg) | 44.3 ± 10.1 | 65.8 ± 8.5 | 104.1 ± 15.6 | <0.001 |
| BMI (kg/m2) | 16.7 ± 2.8 | 22.5 ± 1.7 | 38.7 ± 4.2 | <0.001 |
| Biochemistry | ||||
| SIRT1 (ng/mL) | 3.07 ± 2.3 | 2.5 ± 0.9 | 1.27 ± 0.87 | <0.001 |
| Sclerostin (ng/dL) | 5.05 ± 1.5 | 15.3 ± 11.4 | 35.9 ± 20.6 | <0.001 |
| Glucose (mg/dL) | 73.2 ± 6.6 | 81.8 ± 7.8 | 89.9 ± 7.8 | <0.001 |
| Creatinine (mg/dL) | 0.69 ± 0.11 | 0.79 ± 0.12 | 0.73 ± 0.13 | <0.05 |
| BUN (mg/dL) | 27.2 ± 7.7 | 33.1 ± 9.77 | 29.5 ± 8.0 | ns |
| eGFR (mL/min/1.73 m2) | 123.5 ± 9.7 | 114.2 ± 9.2 | 110.5 ± 15.0 | <0.01 |
| ALP (U/L) | 61.6 ± 17.7 | 53.8 ± 12.6 | 64.3 ± 18.1 | ns |
| Calcium (mg/dL) | 9.8 ± 0.4 | 9.5 ± 0.4 | 9.4 ± 0.4 | <0.01 |
| Phosphorus (mg/dL) | 3.9 ± 0.5 | 4.0 ± 0.6 | 3.5 ± 0.6 | <0.05 |
| Magnesium (mg/dL) | 2.1 ± 0.2 | 2.0 ± 0.1 | 2.0 ± 0.1 | ns |
| 25OHVitD (ng/mL) | 37.3 ± 14.6 | 29.6 ± 11.2 | 24.7 ± 13.7 | <0.05 |
| PTH (pg/mL) | 30.4 ± 8.3 | 35.6 ± 15.7 | 48.5 ± 23.9 | <0.01 |
| Body Composition | ||||
| Total FM (%) | 19.7 ± 7.0 | 26.6 ± 6.5 | 41.0 ± 4.2 | <0.001 |
| Trunk FM (%) | 14.1 ± 6.7 | 22.2 ± 7.0 | 39.1 ± 4.3 | <0.001 |
| Abdominal VAT (cm2) | 15.2 ± 10.1 | 46.7 ± 21.4 | 120.8 ± 48.4 | <0.001 |
| Trunk/legs FM ratio | 0.69 ± 0.2 | 0.9 ± 0.3 | 1.24 ± 0.3 | <0.001 |
| Lean mass (kg) | 33.4 ± 5.3 | 46.0 ± 6.9 | 59.2 ± 10.4 | <0.001 |
| DXA Bone Parameters | ||||
| L1–L4 BMD (g/cm2) | 0.87 ± 0.10 | 1.04 ± 0.14 | 1.14 ± 0.14 | <0.001 |
| Femoral neck BMD (g/cm2) | 0.72 ± 0.11 | 0.85 ± 0.11 | 0.9 ± 0.15 | <0.001 |
| TBS | 1.38 ± 0.06 | 1.42 ± 0.06 | 1.29 ± 0.14 | <0.001 |
| SIRT1 | Sclerostin | |||
|---|---|---|---|---|
| ρ | p-Value | ρ | p-Value | |
| Age (years) | −0.126 | 0.31 | 0.494 | <0.001 |
| BMI (kg/m2) | −0.407 | 0.001 | 0.596 | <0.001 |
| Glycemia (mg/dL) | −0.302 | 0.014 | 0.481 | <0.001 |
| Total FM (%) | −0.485 | <0.001 | 0.504 | <0.001 |
| Abdominal VAT (cm2) | −0.329 | 0.009 | 0.626 | <0.001 |
| Trunk/legs FM ratio | −0.206 | 0.098 | 0.509 | <0.001 |
| Lean mass (kg) | −0.210 | 0.096 | 0.499 | <0.001 |
| Spine BMD (g/cm2) | −0.381 | 0.002 | 0.480 | <0.001 |
| Femoral neck BMD (g/cm2) | −0.275 | 0.027 | 0.292 | 0.019 |
| TBS | 0.032 | 0.806 | −0.142 | 0.274 |
| Lumbar Spine BMD | Femoral Neck BMD | TBS | ||||
|---|---|---|---|---|---|---|
| β | p-Value | β | p-Value | β | p-Value | |
| Age (years) | 0.107 | 0.42 | −0.136 | 0.34 | −0.197 | 0.18 |
| SIRT1 (ng/mL) | −0.236 | 0.049 | −0.173 | 0.17 | −0.228 | 0.08 |
| Sclerostin (ng/dL) | 0.082 | 0.56 | −0.073 | 0.64 | −0.006 | 0.97 |
| Trunk/legs FM ratio | −0.033 | 0.82 | −0.092 | 0.56 | −0.020 | 0.90 |
| BMI (kg/m2) | 0.379 | 0.019 | 0.578 | 0.001 | −0.462 | 0.014 |
| SIRT1 | Sclerostin | |||
|---|---|---|---|---|
| ρ | p-Value | ρ | p-Value | |
| Spine BMD/BMI ratio | 0.320 | 0.009 | −0.472 | <0.001 |
| Femoral neck BMD/BMI ratio | 0.326 | 0.008 | −0.526 | <0.001 |
| TBS/BMI ratio | 0.394 | 0.002 | −0.598 | <0.001 |
| Spine BMD/BMI | Femoral Neck BMD/BMI | TBS/BMI | ||||
|---|---|---|---|---|---|---|
| Β | p-Value | β | p-Value | β | p-Value | |
| Age (years) | −0.181 | 0.175 | −0.333 | 0.008 | −0.280 | 0.015 |
| SIRT1 (ng/mL) | 0.119 | 0.316 | 0.096 | 0.375 | 0.219 | 0.033 |
| Sclerostin (ng/dL) | −0.353 | 0.014 | −0.347 | 0.008 | −0.402 | 0.001 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tozzi, R.; Masi, D.; Cipriani, F.; Contini, S.; Gangitano, E.; Spoltore, M.E.; Barchetta, I.; Basciani, S.; Watanabe, M.; Baldini, E.; et al. Circulating SIRT1 and Sclerostin Correlates with Bone Status in Young Women with Different Degrees of Adiposity. Nutrients 2022, 14, 983. https://doi.org/10.3390/nu14050983
Tozzi R, Masi D, Cipriani F, Contini S, Gangitano E, Spoltore ME, Barchetta I, Basciani S, Watanabe M, Baldini E, et al. Circulating SIRT1 and Sclerostin Correlates with Bone Status in Young Women with Different Degrees of Adiposity. Nutrients. 2022; 14(5):983. https://doi.org/10.3390/nu14050983
Chicago/Turabian StyleTozzi, Rossella, Davide Masi, Fiammetta Cipriani, Savina Contini, Elena Gangitano, Maria Elena Spoltore, Ilaria Barchetta, Sabrina Basciani, Mikiko Watanabe, Enke Baldini, and et al. 2022. "Circulating SIRT1 and Sclerostin Correlates with Bone Status in Young Women with Different Degrees of Adiposity" Nutrients 14, no. 5: 983. https://doi.org/10.3390/nu14050983
APA StyleTozzi, R., Masi, D., Cipriani, F., Contini, S., Gangitano, E., Spoltore, M. E., Barchetta, I., Basciani, S., Watanabe, M., Baldini, E., Ulisse, S., Lubrano, C., Gnessi, L., & Mariani, S. (2022). Circulating SIRT1 and Sclerostin Correlates with Bone Status in Young Women with Different Degrees of Adiposity. Nutrients, 14(5), 983. https://doi.org/10.3390/nu14050983












