Comparison of Associations between MIND and Mediterranean Diet Scores with Patient-Reported Outcomes in Parkinson’s Disease
Abstract
1. Introduction
2. Materials and Methods
Statistical Analysis
3. Results
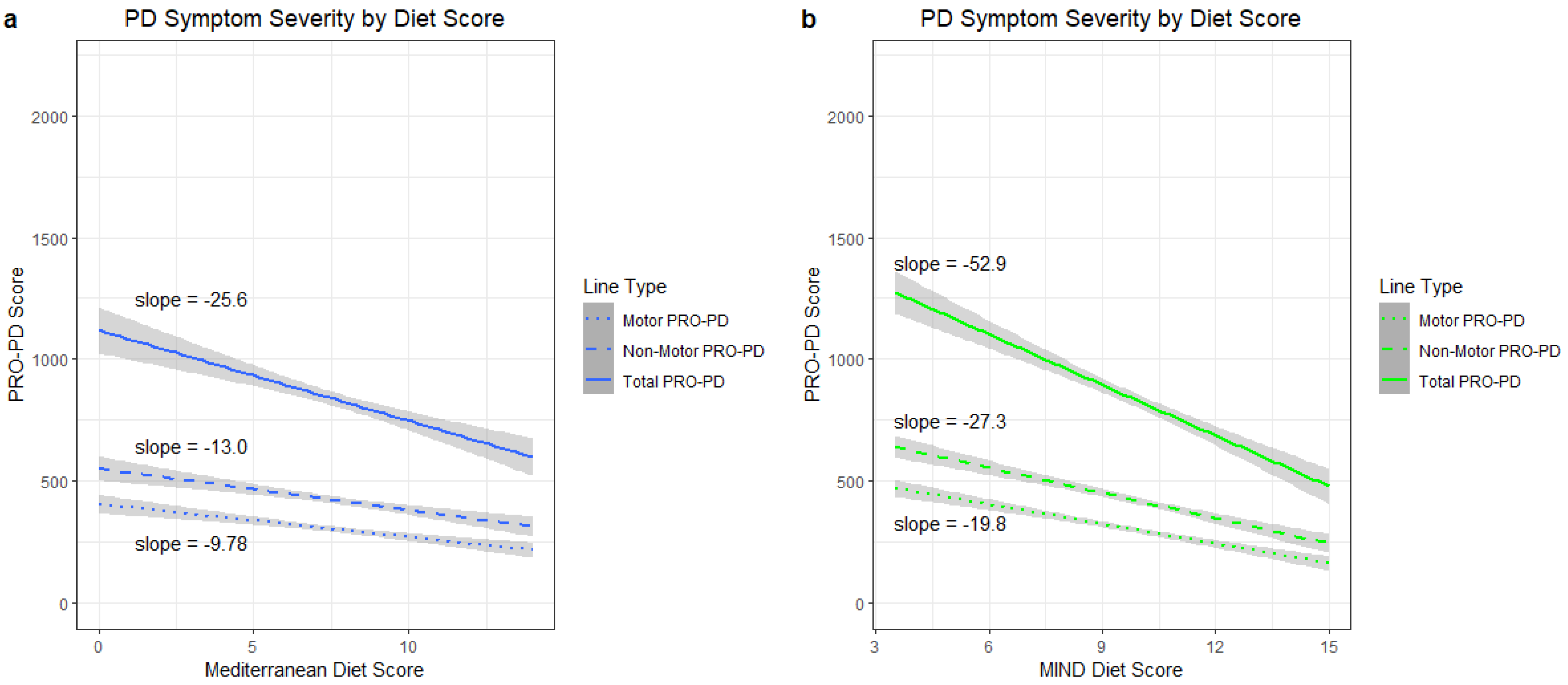
3.1. PRO-PD Score by Diet Score
3.2. PRO-PD Progression and Diet
3.3. PRO-PD Symptoms and Diet
3.4. MIND vs. MEDI Comparison
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Chaudhuri, K.R.; Healy, D.G.; Schapira, A.H.V. Non-Motor Symptoms of Parkinson’s Disease: Diagnosis and Management. Lancet Neurol. 2006, 5, 235–245. [Google Scholar] [CrossRef] [PubMed]
- Schapira, A.H.V.; Chaudhuri, K.R.; Jenner, P. Non-Motor Features of Parkinson Disease. Nat. Rev. Neurosci. 2017, 18, 435–450. [Google Scholar] [CrossRef] [PubMed]
- Chen, Z.; Li, G.; Liu, J. Autonomic Dysfunction in Parkinson’s Disease: Implications for Pathophysiology, Diagnosis, and Treatment. Neurobiol. Dis. 2020, 134. [Google Scholar] [CrossRef] [PubMed]
- Fereshtehnejad, S.M.; Yao, C.; Pelletier, A.; Montplaisir, J.Y.; Gagnon, J.F.; Postuma, R.B. Evolution of Prodromal Parkinson’s Disease and Dementia with Lewy Bodies: A Prospective Study. Brain 2019, 142, 2051–2067. [Google Scholar] [CrossRef]
- Schrag, A.; Horsfall, L.; Walters, K.; Noyce, A.; Petersen, I. Prediagnostic Presentations of Parkinson’s Disease in Primary Care: A Case-Control Study. Lancet Neurol. 2015, 14, 57–64. [Google Scholar] [CrossRef] [PubMed]
- Kaufmann, H.; Norcliffe-Kaufmann, L.; Palma, J.A.; Biaggioni, I.; Low, P.A.; Singer, W.; Goldstein, D.S.; Peltier, A.C.; Shibao, C.A.; Gibbons, C.H.; et al. Natural History of Pure Autonomic Failure: A United States Prospective Cohort. Ann. Neurol. 2017, 81, 287–297. [Google Scholar] [CrossRef]
- Bugalho, P.; Lampreia, T.; Miguel, R.; Mendonça, M.D.; Caetano, A.; Barbosa, R. Non-Motor Symptoms in Portuguese Parkinson’s Disease Patients: Correlation and Impact on Quality of Life and Activities of Daily Living. Sci. Rep. 2016, 6, 32267. [Google Scholar] [CrossRef]
- Tibar, H.; El Bayad, K.; Bouhouche, A.; Ben Haddou, E.H.A.; Benomar, A.; Yahyaoui, M.; Benazzouz, A.; Regragui, W. Non-Motor Symptoms of Parkinson’s Disease and Their Impact on Quality of Life in a Cohort of Moroccan Patients. Front. Neurol. 2018, 9, 170. [Google Scholar] [CrossRef]
- Li, H.; Zhang, M.; Chen, L.; Zhang, J.; Pei, Z.; Hu, A.; Wang, Q. Nonmotor Symptoms Are Independently Associated with Impaired Health-Related Quality of Life in Chinese Patients with Parkinson’s Disease. Mov. Disord. 2010, 25, 2740–2746. [Google Scholar] [CrossRef]
- Hughes, K.C.; Gao, X.; Kim, I.Y.; Wang, M.; Weisskopf, M.G.; Schwarzschild, M.A.; Ascherio, A. Intake of Dairy Foods and Risk of Parkinson Disease. Neurology 2017, 89, 46–52. [Google Scholar] [CrossRef]
- Mischley, L.K.; Lau, R.C.; Bennett, R.D. Role of Diet and Nutritional Supplements in Parkinson’s Disease Progression. Oxid. Med. Cell. Longev. 2017, 2017, 6405278. [Google Scholar] [CrossRef] [PubMed]
- Yin, W.; Löf, M.; Chen, R.; Hultman, C.M.; Fang, F.; Sandin, S. Mediterranean Diet and Depression: A Population-Based Cohort Study. Int. J. Behav. Nutr. Phys. Act. 2021, 18, 153. [Google Scholar] [CrossRef] [PubMed]
- Strikwerda, A.J.; Dommershuijsen, L.J.; Kamran Ikram, M.; Voortman, T. Diet Quality and Risk of Parkinson’s Disease: The Rotterdam Study. Nutrients 2021, 13, 3970. [Google Scholar] [CrossRef] [PubMed]
- Alcalay, R.N.; Gu, Y.; Mejia-Santana, H.; Cote, L.; Marder, K.S.; Scarmeas, N. The Association between Mediterranean Diet Adherence and Parkinson’s Disease. Lancet. Neurol. 2012, 27, 771–774. [Google Scholar] [CrossRef]
- Gao, X.; Chen, H.; Fung, T.T.; Logroscino, G.; Schwarzschild, M.A.; Hu, F.B.; Ascherio, A. Prospective Study of Dietary Pattern and Risk of Parkinson Disease. Am. J. Clin. Nutr. 2007, 86, 1486–1494. [Google Scholar] [CrossRef]
- García-Conesa, M.T.; Philippou, E.; Pafilas, C.; Massaro, M.; Quarta, S.; Andrade, V.; Jorge, R.; Chervenkov, M.; Ivanova, T.; Dimitrova, D.; et al. Exploring the Validity of the 14-Item Mediterranean Diet Adherence Screener (MEDAS): A Cross-National Study in Seven European Countries around the Mediterranean Region. Nutrients 2020, 12, 2960. [Google Scholar] [CrossRef]
- Morris, M.C.; Tangney, C.C.; Wang, Y.; Sacks, F.M.; Barnes, L.L.; Bennett, D.A.; Aggarwal, N.T. MIND Diet Slows Cognitive Decline with Aging. Alzheimer’s Dement. 2015, 11, 1015–1022. [Google Scholar] [CrossRef]
- Yin, W.; Löf, M.; Pedersen, N.L.; Sandin, S.; Fang, F. Mediterranean Dietary Pattern at Middle Age and Risk of Parkinson’s Disease: A Swedish Cohort Study. Mov. Disord. 2021, 36, 255–260. [Google Scholar] [CrossRef]
- Bianchi, V.E.; Herrera, P.F.; Laura, R. Effect of Nutrition on Neurodegenerative Diseases. A Systematic Review. Nutr. Neurosci. 2021, 24, 810–834. [Google Scholar] [CrossRef]
- Bonaccio, M.; Pounis, G.; Cerletti, C.; Donati, M.B.; Iacoviello, L.; de Gaetano, G. Mediterranean Diet, Dietary Polyphenols and Low Grade Inflammation: Results from the MOLI-SANI Study. Br. J. Clin. Pharmacol. 2017, 83, 107–113. [Google Scholar] [CrossRef]
- Trichopoulou, A.; Costacou, T.; Bamia, C.; Trichopoulos, D. Adherence to a Mediterranean Diet and Survival in a Greek Population. N. Engl. J. Med. 2003, 348, 2599–2608. [Google Scholar] [CrossRef] [PubMed]
- Morris, M.C.; Tangney, C.C.; Wang, Y.; Sacks, F.M.; Bennett, D.A.; Aggarwal, N.T. MIND Diet Associated with Reduced Incidence of Alzheimer’s Disease. Alzheimer’s Dement. 2015, 11, 1007–1014. [Google Scholar] [CrossRef] [PubMed]
- Dhana, K.; James, B.D.; Agarwal, P.; Aggarwal, N.T.; Cherian, L.J.; Leurgans, S.E.; Barnes, L.L.; Bennett, D.A.; Schneider, J.A.; Gardener, H. MIND Diet, Common Brain Pathologies, and Cognition in Community-Dwelling Older Adults. J. Alzheimers. Dis. 2021, 83, 683–692. [Google Scholar] [CrossRef] [PubMed]
- Van Den Brink, A.C.; Brouwer-Brolsma, E.M.; Berendsen, A.A.M.; Van De Rest, O. The Mediterranean, Dietary Approaches to Stop Hypertension (DASH), and Mediterranean-DASH Intervention for Neurodegenerative Delay (MIND) Diets Are Associated with Less Cognitive Decline and a Lower Risk of Alzheimer’s Disease—A Review. Adv. Nutr. 2019, 10, 1040–1065. [Google Scholar] [CrossRef] [PubMed]
- Metcalfe-Roach, A.; Yu, A.C.; Golz, E.; Cirstea, M.; Sundvick, K.; Kliger, D.; Foulger, L.H.; Mackenzie, M.; Finlay, B.B.; Appel-Cresswell, S. MIND and Mediterranean Diets Associated with Later Onset of Parkinson’s Disease. Mov. Disord. 2021, 36, 977–984. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, P.; Wang, Y.; Buchman, A.S.; Holland, T.M.; Bennett, D.A.; Morris, M.C. MIND Diet Associated with Reduced Incidence and Delayed Progression of ParkinsonismA in Old Age. J. Nutr. Health Aging 2018, 22, 1211–1215. [Google Scholar] [CrossRef] [PubMed]
- Maraki, M.I.; Yannakoulia, M.; Stamelou, M.; Stefanis, L.; Xiromerisiou, G.; Kosmidis, M.H.; Dardiotis, E.; Hadjigeorgiou, G.M.; Sakka, P.; Anastasiou, C.A.; et al. Mediterranean Diet Adherence Is Related to Reduced Probability of Prodromal Parkinson’s Disease. Mov. Disord. 2019, 34, 48–57. [Google Scholar] [CrossRef]
- Postuma, R.B.; Berg, D. Prodromal Parkinson’s Disease: The Decade Past, the Decade to Come. Mov. Disord. 2019, 34, 665–675. [Google Scholar] [CrossRef]
- Molsberry, S.; Bjornevik, K.; Hughes, K.C.; Healy, B.; Schwarzschild, M.; Ascherio, A. Diet Pattern and Prodromal Features of Parkinson Disease. Neurology 2020, 95, e2095–e2108. [Google Scholar] [CrossRef]
- Lawrie, S.; Coe, S.; Mansoubi, M.; Welch, J.; Razzaque, J.; Hu, M.T.; Dawes, H. Dietary Patterns and Nonmotor Symptoms in Parkinson’s Disease: A Cross-Sectional Analysis. J. Am. Nutr. Assoc. 2022, 1–10. [Google Scholar] [CrossRef]
- Mischley, L.K.; Lau, R.C.; Weiss, N.S. Use of a Self-Rating Scale of the Nature and Severity of Symptoms in Parkinson’s Disease (PRO-PD): Correlation with Quality of Life and Existing Scales of Disease Severity. NPJ Park. Dis. 2017, 3, 20. [Google Scholar] [CrossRef] [PubMed]
- Weldring, T.; Smith, S.M.S. Patient-Reported Outcomes (PROs) and Patient-Reported Outcome Measures (PROMs). Health Serv. Insights 2013, 6. [Google Scholar] [CrossRef]
- Harris, P.A.; Taylor, R.; Thielke, R.; Payne, J.; Gonzalez, N.; Conde, J.G. Research Electronic Data Capture (REDCap)—A Metadata-Driven Methodology and Workflow Process for Providing Translational Research Informatics Support. J. Biomed. Inform. 2009, 42, 377–381. [Google Scholar] [CrossRef] [PubMed]
- Schade, S.; Mollenhauer, B.; Trenkwalder, C. Levodopa Equivalent Dose Conversion Factors: An Updated Proposal Including Opicapone and Safinamide. Mov. Disord. Clin. Pract. 2020, 7, 343–345. [Google Scholar] [CrossRef] [PubMed]
- Chaudhuri, K.R.; Sauerbier, A.; Rojo, J.M.; Sethi, K.; Schapira, A.H.V.; Brown, R.G.; Antonini, A.; Stocchi, F.; Odin, P.; Bhattacharya, K.; et al. The Burden of Non-Motor Symptoms in Parkinson’s Disease Using a Self-Completed Non-Motor Questionnaire: A Simple Grading System. Park. Relat. Disord. 2015, 21, 287–291. [Google Scholar] [CrossRef] [PubMed]
- RStudio|Open Source & Professional Software for Data Science Teams—RStudio. Available online: https://www.rstudio.com/ (accessed on 23 September 2022).
- Descriptive Statistics. IBM SPSS Statistics 25 Step by Step; Routledge: London, UK, 2018; pp. 126–134. [Google Scholar] [CrossRef]
- Rusch, C.; Beke, M.; Tucciarone, L.; Nieves, C.; Ukhanova, M.; Tagliamonte, M.S.; Mai, V.; Suh, J.H.; Wang, Y.; Chiu, S.; et al. Mediterranean Diet Adherence in People With Parkinson’s Disease Reduces Constipation Symptoms and Changes Fecal Microbiota After a 5-Week Single-Arm Pilot Study. Front. Neurol. 2021, 12, 794640. [Google Scholar] [CrossRef] [PubMed]
- Paknahad, Z.; Sheklabadi, E.; Derakhshan, Y.; Bagherniya, M.; Chitsaz, A. The Effect of the Mediterranean Diet on Cognitive Function in Patients with Parkinson’s Disease: A Randomized Clinical Controlled Trial. Complement. Ther. Med. 2020, 50, 102366. [Google Scholar] [CrossRef] [PubMed]
- Sánchez-Villegas, A.; Martínez-González, M.A.; Estruch, R.; Salas-Salvadó, J.; Corella, D.; Covas, M.I.; Arós, F.; Romaguera, D.; Gómez-Gracia, E.; Lapetra, J.; et al. Mediterranean Dietary Pattern and Depression: The PREDIMED Randomized Trial. BMC Med. 2013, 11, 208. [Google Scholar] [CrossRef]
- Sánchez-Villegas, A.; Delgado-Rodríguez, M.; Alonso, A.; Schlatter, J.; Lahortiga, F.; Serra-Majem, L.; Martínez-González, M.A. Association of the Mediterranean Dietary Pattern with the Incidence of Depression: The Seguimiento Universidad de Navarra/University of Navarra Follow-up (SUN) Cohort. Arch. Gen. Psychiatry 2009, 66, 1090–1098. [Google Scholar] [CrossRef]
- Fan, Y.; Zhao, L.; Deng, Z.; Li, M.; Huang, Z.; Zhu, M.; Xu, W. Non-Linear Association between Mediterranean Diet and Depressive Symptom in U.S. Adults: A Cross-Sectional Study. Front. Psychiatry 2022, 13, 1558. [Google Scholar] [CrossRef]
- Berendsen, A.M.; Kang, J.H.; Feskens, E.J.M.; de Groot, C.P.G.M.; Grodstein, F.; van de Rest, O. Association of Long-Term Adherence to the MIND Diet with Cognitive Function and Cognitive Decline in American Women. J. Nutr. Health Aging 2018, 22, 222–229. [Google Scholar] [CrossRef]
- Strathearn, K.E.; Yousef, G.G.; Grace, M.H.; Roy, S.L.; Tambe, M.A.; Ferruzzi, M.G.; Wu, Q.L.; Simon, J.E.; Lila, M.A.; Rochet, J.C. Neuroprotective Effects of Anthocyanin- and Proanthocyanidin-Rich Extracts in Cellular Models of Parkinson’s Disease. Brain Res. 2014, 1555, 60–77. [Google Scholar] [CrossRef] [PubMed]
- Bastianetto, S.; Ménard, C.; Quirion, R. Neuroprotective Action of Resveratrol. Biochim. Biophys. Acta 2015, 1852, 1195–1201. [Google Scholar] [CrossRef] [PubMed]
- Burckhardt, M.; Herke, M.; Wustmann, T.; Watzke, S.; Langer, G.; Fink, A. Omega-3 Fatty Acids for the Treatment of Dementia. Cochrane Database Syst. Rev. 2016, 4. [Google Scholar] [CrossRef] [PubMed]
- Etminan, M.; Gill, S.S.; Samii, A. Intake of Vitamin E, Vitamin C, and Carotenoids and the Risk of Parkinson’s Disease: A Meta-Analysis. Lancet Neurol. 2005, 4, 362–365. [Google Scholar] [CrossRef] [PubMed]
- Wu, L.Y.; Chen, J.X.; Chen, G.S.; Gao, H.; Huo, J.H.; Pang, Y.F.; Gao, Q.H. Dietary β-Carotene and Vitamin A and Risk of Parkinson Disease: A Protocol for Systematic Review and Meta-Analysis. Medicine 2022, 101, E31002. [Google Scholar] [CrossRef]
- Chen, H.; Song, H.; Li, M.; Hu, S.; Xiong, X.; Jiang, H.; Xu, J. The Impact of Awareness and Attitudes towards Long-Action Reversible Contraceptives on the Intention to Use: A Survey among Youth with Unintended Pregnancies. Eur. J. Contracept. Reprod. Health Care 2022, 27, 121–126. [Google Scholar] [CrossRef] [PubMed]
- Myhrstad, M.C.W.; Tunsjø, H.; Charnock, C.; Telle-Hansen, V.H. Dietary Fiber, Gut Microbiota, and Metabolic Regulation-Current Status in Human Randomized Trials. Nutrients 2020, 12, 859. [Google Scholar] [CrossRef]
| Characteristics of Study Participants | |
|---|---|
| N = 1205 | |
| Age, mean (years, SD) | 66.4 (8.76) |
| Years Since Diagnosis (years, SD) | 7.19 (5.44) |
| PRO-PD, mean (year, SD) | 844.5 (497.4) |
| Estimate Hoehn & Yahr | |
| 1-sided symptoms only, minimal disability | 533 (45.8%) |
| Both sides affected, balance is stable | 247 (21.2%) |
| Mild to moderate disability, balance affected | 326 (28.0%) |
| Severe disability, able to walk and stand without help | 42 (3.6%) |
| Confinement to bed or wheelchair unless aided | 4 (0.34% |
| Don’t know | 11 (0.95%) |
| Gender | |
| Male | 474 (39%) |
| Female | 714 (59%) |
| Non-Binary | 3 (0.25%) |
| NA | 14 (1.2%) |
| Race | |
| Caucasian | 1104 (91%) |
| Black | 8 (0.66%) |
| Hispanic | 22 (1.8%) |
| Native American | 3 (0.25%) |
| Asian/Pacific Islander | 22 (1.8%) |
| Other | 33 (2.7%) |
| NA | 13 (1.1%) |
| Income | |
| <$20,000 | 59 (4.9%) |
| $20–40,000 | 107 (8.9%) |
| $40–60,000 | 145 (12%) |
| $60–80,000 | 188 (16%) |
| $80–100,000 | 155 (13%) |
| $100–150,000 | 208(17%) |
| >$150,000 | 252 (21%) |
| NA | 91 (7.6%) |
| Education | |
| Grades 9–11 | 8 (0.67%) |
| Completed High School/GED | 8.6 (104%) |
| Technical school certification | 5.14 (62%) |
| Associate Degree | 7.5 (90%) |
| Bachelor’s degree | 27 (32%) |
| Graduate/Professional degree | 50 (604%) |
| NA | 0.91 (11%) |
| Parkinsonism | |
| Idiopathic PD | 1145 (95%) |
| Parkinsonism | 42 (3.5%) |
| No Dx but increased risk | 2 (0.17%) |
| Other | 15 (1.3%) |
| MEDI | MIND | |||||
|---|---|---|---|---|---|---|
| Non-Motor Symptoms | β | p | β | p | F-Statistic | p |
| constipation | −1.08 (−1.68–−0.467) | 0.001 | −2.11 (−2.83–−1.39) | <0.001 | 6.96 | 0.01 |
| motivation | −1.39 (−1.97–−0.809) | <0.001 | −2.46 (−3.13–−1.79) | <0.001 | 3.9 | 0.06 |
| depression | −0.727 (−1.21–−00.244) | 0.01 | −1.41 (−1.98–−0.838) | <0.001 | 2.96 | 0.1 |
| withdrawn | −1.15 (−1.7–−0.578) | 0.001 | −1.94 (−2.60–−1.28) | <0.001 | 2.31 | 0.1 |
| anxiety | −0.739 (−1.34–−0.134) | 0.1 | −1.59 (−2.30–−0.890) | <0.001 | 6.18 | 0.02 |
| fatigue | −0.675 (−1.31–−0.0348) | 0.4 | −1.83 (−2.58–−1.07) | 0.4 | 6.58 | 0.01 |
| daytime sleepiness | −1.04 (−1.66–−0.426) | 0.01 | −1.91 (−2.64–−1.18) | <0.001 | 3.86 | 0.06 |
| visual disturbance | −0.583 (−1.12–−0.0480) | 0.4 | −1.26 (−1.88–−0.645) | <0.001 | 2.21 | 0.2 |
| insomnia | −1.07 (−1.75–−0.399) | 0.02 | −2.14 (−2.93–−1.35) | <0.001 | 5.51 | 0.02 |
| REM sleep behavior disorder | −0.514 (−1.17–0.142) | 0.9 | −1.20 (−1.98–−0.424) | 0.03 | 1.71 | 0.2 |
| muscle pain | −0.975 (−1.61–−0.341) | 0.03 | −1.80 (−2.55–−1.05) | <0.001 | 3.58 | 0.06 |
| drool | −0.182 (−0.785−0.422) | 0.9 | −1.20 (−1.91–−0.498) | 0.009 | 5.91 | 0.03 |
| memory/forgetfulness | −1.17 (−1.72–−0.623) | 0.004 | −2.12 (−2.77–−1.48) | <0.001 | 6.92 | 0.01 |
| comprehension | −0.801 (−1.31–−0.292) | 0.02 | −1.34 (−1.93–−0.748) | <0.001 | 2.46 | 0.13 |
| sexual dysfunction | −0.906 (−1.69–−0.121) | 0.3 | −2.16 (−3.07–−1.24) | <0.001 | 4.58 | 0.04 |
| urinary symptoms | −0.133 (−0.806–0.539) | 0.9 | −1.44 (−2.23–−0.649) | 0.004 | 7.54 | <0.001 |
| hallucinations | −0.316 (−0.694–0.0619) | 0.9 | −0.523 (−0.969–−0.0772) | 0.2 | 1.98 | 0.1 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fox, D.J.; Park, S.J.; Mischley, L.K. Comparison of Associations between MIND and Mediterranean Diet Scores with Patient-Reported Outcomes in Parkinson’s Disease. Nutrients 2022, 14, 5185. https://doi.org/10.3390/nu14235185
Fox DJ, Park SJ, Mischley LK. Comparison of Associations between MIND and Mediterranean Diet Scores with Patient-Reported Outcomes in Parkinson’s Disease. Nutrients. 2022; 14(23):5185. https://doi.org/10.3390/nu14235185
Chicago/Turabian StyleFox, Devon J., Sarah JaeHwa Park, and Laurie K. Mischley. 2022. "Comparison of Associations between MIND and Mediterranean Diet Scores with Patient-Reported Outcomes in Parkinson’s Disease" Nutrients 14, no. 23: 5185. https://doi.org/10.3390/nu14235185
APA StyleFox, D. J., Park, S. J., & Mischley, L. K. (2022). Comparison of Associations between MIND and Mediterranean Diet Scores with Patient-Reported Outcomes in Parkinson’s Disease. Nutrients, 14(23), 5185. https://doi.org/10.3390/nu14235185







