Pregnant Dutch Women Have Inadequate Iodine Status and Selenium Intake
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population and Medical Ethical Aspects
2.2. Data Collection, Storage and Analysis
2.3. Power Analysis
2.4. Parameters of Iodine Status and Selenium Intake
2.5. Data Analysis
3. Results
3.1. Study Population
3.2. Iodine Status
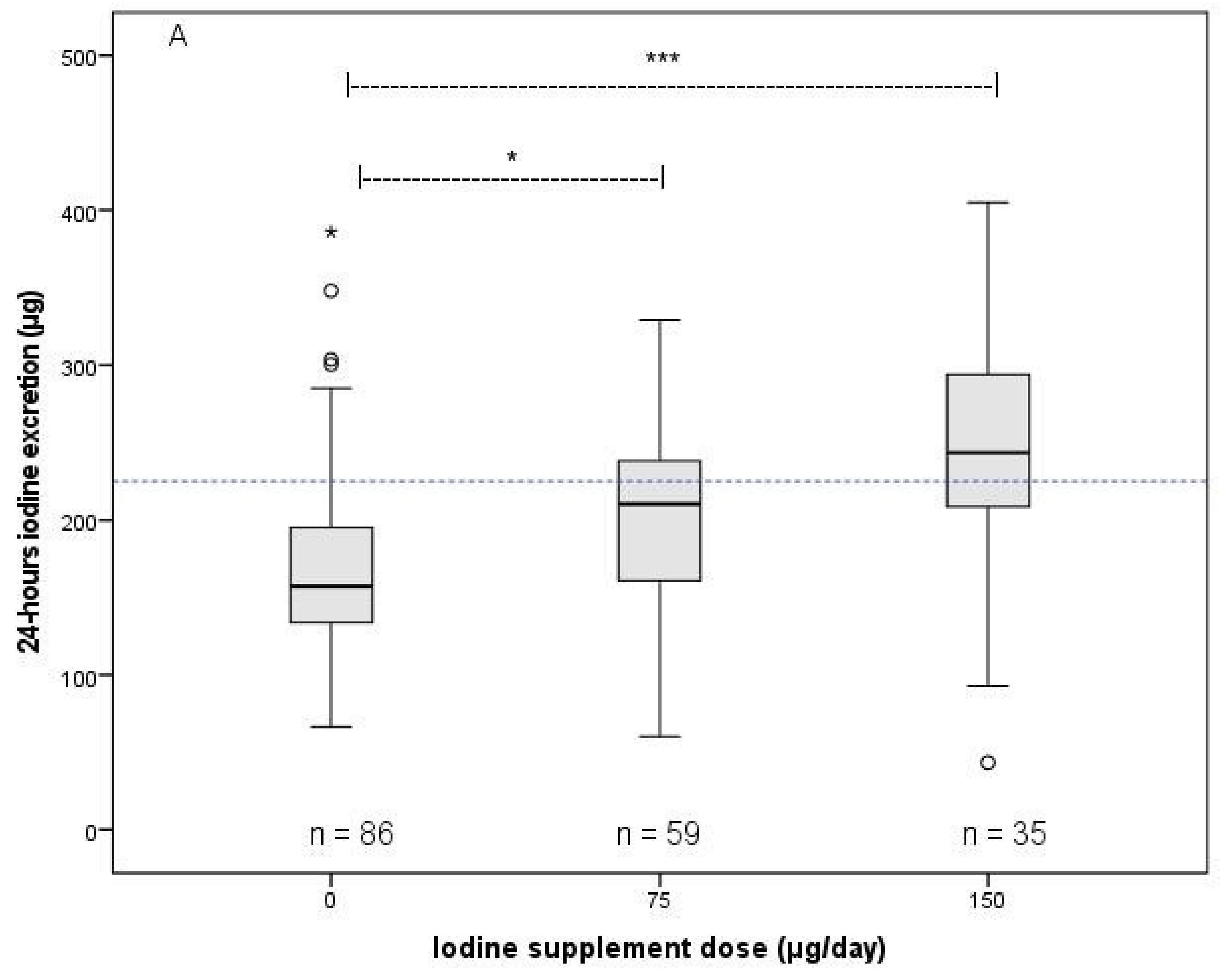
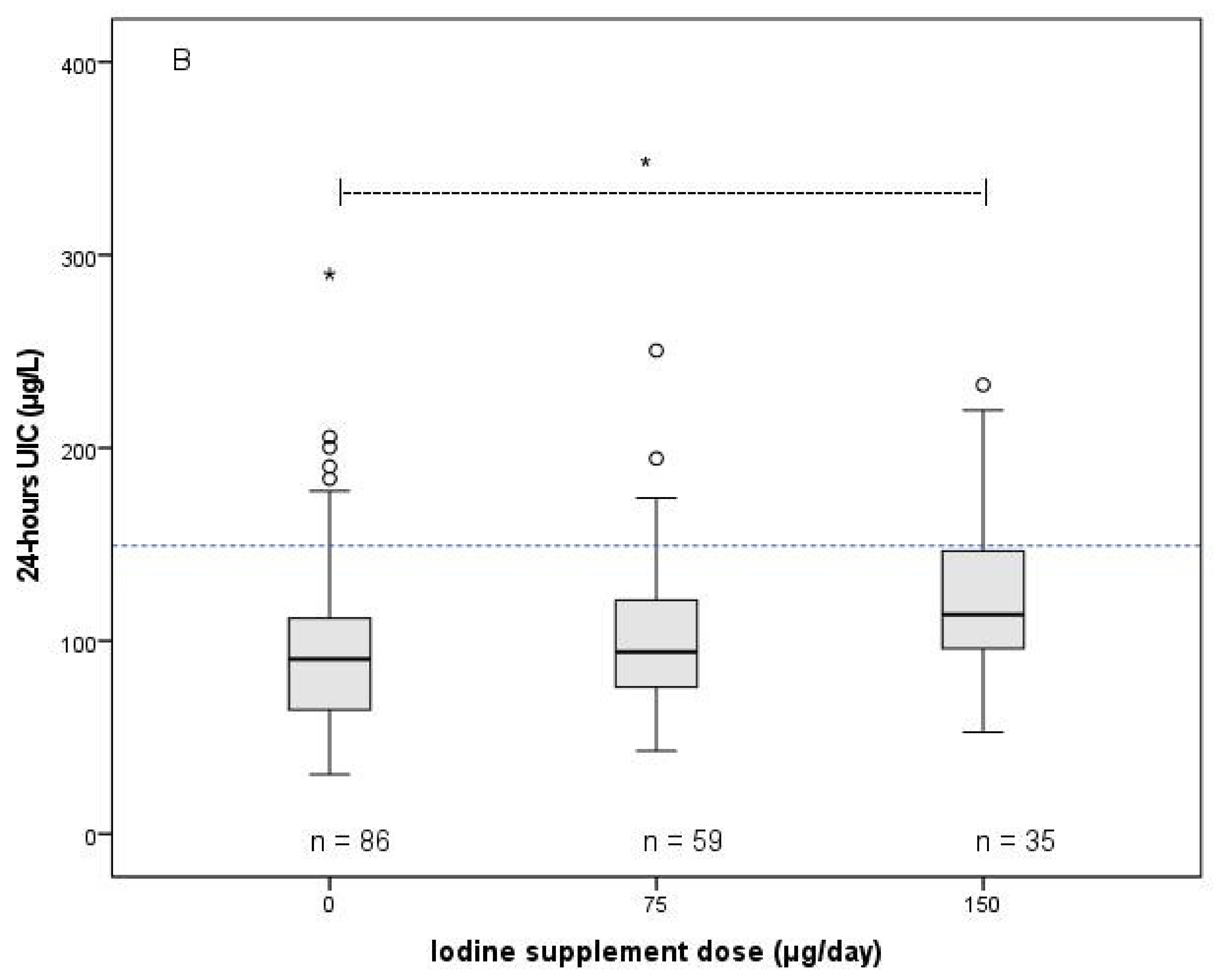
3.3. Association between Iodine Supplement Dose and Iodine Status Parameters
3.4. Iodine Supplement Dose That was Associated with Sufficient Iodine Status
3.5. Selenium Intake in Relation to Nutritional Recommendations
3.6. Combined Insufficient Iodine Status and Inadequate Selenium Intake
4. Discussion
5. Conclusions and Recommendations
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Velasco, I.; Bath, S.C.; Rayman, M.P. Iodine as Essential Nutrient during the First 1000 Days of Life. Nutrients 2018, 10, 290. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez-Diaz, E.; Pearce, E.N. Iodine status and supplementation before, during, and after pregnancy. Best Pract. Res. Clin. Endocrinol. Metab. 2020, 34, 101430. [Google Scholar] [CrossRef]
- Bath, S.C.; Steer, C.D.; Golding, J.; Emmett, P.; Rayman, M.P. Effect of inadequate iodine status in UK pregnant women on cognitive outcomes in their children: Results from the Avon Longitudinal Study of Parents and Children (ALSPAC). Lancet 2013, 382, 331–337. [Google Scholar] [CrossRef]
- Hynes, K.L.; Otahal, P.; Burgess, J.R.; Oddy, W.H.; Hay, I. Reduced Educational Outcomes Persist into Adolescence Following Mild Iodine Deficiency in Utero, Despite Adequacy in Childhood: 15-Year Follow-Up of the Gestational Iodine Cohort Investigating Auditory Processing Speed and Working Memory. Nutrients 2017, 9, 1354. [Google Scholar] [CrossRef] [PubMed]
- Vermiglio, F.; Lo Presti, V.P.; Moleti, M.; Sidoti, M.; Tortorella, G.; Scaffidi, G.; Castagna, M.G.; Mattina, F.; Violi, M.A.; Crisà, A.; et al. Attention Deficit and Hyperactivity Disorders in the Offspring of Mothers Exposed to Mild-Moderate Iodine Deficiency: A Possible Novel Iodine Deficiency Disorder in Developed Countries. J. Clin. Endocrinol. Metab. 2004, 89, 6054–6060. [Google Scholar] [CrossRef] [PubMed]
- Mulder, T.A.; Korevaar, T.I.M.; Peeters, R.P.; van Herwaarden, A.E.; de Rijke, Y.B.; White, T.; Tiemeier, H. Urinary Iodine Concentrations in Pregnant Women and Offspring Brain Morphology. Thyroid 2021, 31, 964–972. [Google Scholar] [CrossRef] [PubMed]
- Berbel, P.; Mestre, J.L.; Santamaría, A.; Palazón, I.; Franco, A.; Graells, M.; González-Torga, A.; de Escobar, G.M. Delayed Neurobehavioral Development in Children Born to Pregnant Women with Mild Hypothyroxinemia During the First Month of Gestation: The Importance of Early Iodine Supplementation. Thyroid Off. J. Am. Thyroid Assoc. 2009, 19, 511–519. [Google Scholar] [CrossRef]
- Dohán, O.; De la Vieja, A.; Paroder, V.; Riedel, C.; Artani, M.; Reed, M.; Ginter, C.S.; Carrasco, N. The Sodium/Iodide Symporter (NIS): Characterization, Regulation, and Medical Significance. Endocr. Rev. 2003, 24, 48–77. [Google Scholar] [CrossRef]
- Vayre, L.; Sabourin, J.C.; Caillou, B.; Ducreux, M.; Schlumberger, M.; Bidart, J.M. Immunohistochemical analysis of Na+/I− symporter distribution in human extra-thyroidal tissues. Eur. J. Endocrinol. 1999, 141, 382–386. [Google Scholar] [CrossRef]
- Ullberg, S.; Ewaldsson, B. Distribution of radio-iodine studied by whole-body autoradiography. Acta Radiol. Ther. Phys. Biol. 1964, 2, 24–32. [Google Scholar] [CrossRef]
- Aceves, C.; Anguiano, B.; Delgado, G. The Extrathyronine Actions of Iodine as Antioxidant, Apoptotic, and Differentiation Factor in Various Tissues. Thyroid 2013, 23, 938–946. [Google Scholar] [CrossRef]
- Venturi, S.; Venturi, M. Iodine in Evolution of Salivary Glands and in Oral Health. Nutr. Health (Berkhamsted) 2009, 20, 119–134. [Google Scholar] [CrossRef]
- Köhrle, J. The trace element selenium and the thyroid gland. Biochimie 1999, 81, 527–533. [Google Scholar] [CrossRef]
- Schomburg, L. Selenium, selenoproteins and the thyroid gland: Interactions in health and disease. Nat. Rev. Endocrinol. 2011, 8, 160–171. [Google Scholar] [CrossRef]
- De La Vieja, A.; Santisteban, P. Role of iodide metabolism in physiology and cancer. Endocr.-Relat. Cancer 2018, 25, R225. [Google Scholar] [CrossRef]
- Wang, B.; He, W.; Li, Q.; Jia, X.; Yao, Q.; Song, R.; Qin, Q.; Zhang, J. U-shaped relationship between iodine status and thyroid autoimmunity risk in adults. Eur. J. Endocrinol. 2019, 181, 255–266. [Google Scholar] [CrossRef]
- Rayman, M.P. Multiple nutritional factors and thyroid disease, with particular reference to autoimmune thyroid disease. Proc. Nutr. Soc. 2019, 78, 34–44. [Google Scholar] [CrossRef]
- Avery, J.C.; Hoffmann, P.R. Selenium, Selenoproteins, and Immunity. Nutrients 2018, 10, 1203. [Google Scholar] [CrossRef]
- Varsi, K.; Bolann, B.; Torsvik, I.; Rosvold Eik, T.C.; Høl, P.J.; Bjørke-Monsen, A. Impact of Maternal Selenium Status on Infant Outcome during the First 6 Months of Life. Nutrients 2017, 9, 486. [Google Scholar] [CrossRef]
- Hubalewska-Dydejczyk, A.; Duntas, L.; Gilis-Januszewska, A. Pregnancy, thyroid, and the potential use of selenium. Hormons 2020, 19, 47–53. [Google Scholar] [CrossRef]
- Zachara, B.A. Selenium in Complicated Pregnancy. A Review. Adv. Clin. Chem. 2018, 86, 157–178. [Google Scholar]
- Hwang, E.S.; Ki, K.N.; Chung, H.Y. Proximate Composition, Amino Acid, Mineral, and Heavy Metal Content of Dried Laver. Prev. Nutr. Food Sci. 2013, 18, 139–144. [Google Scholar] [CrossRef] [PubMed]
- Health Council of The Netherlands. Towards Maintaining Optimal Iodine Intake (Naar behoud van een Optimale Jodiuminname); Minister of Health, Welfare and Sport: Amsterdam, The Netherlands, 2008. (In Dutch)
- Statute Holding Changing the Addition of Micronutrients to Food: Regarding Iodine. (Besluit van 13 juni 2008, Houdende Wijziging van het Warenwetbesluit Toevoeging micro–Voedingsstoffen aan Levensmiddelen, Inzake het toevoegen van jodium. Staatsblad 2008). Available online: http://extwprlegs1.fao.org/docs/pdf/net84947.pdf (accessed on 11 July 2022). (In Dutch).
- Verkaik-Kloosterman, J.; Buurma-Rethans, E.J.M.; Dekkers, A.L.M.; van Rossum, C.T.M. Decreased, but still sufficient, iodine intake of children and adults in the Netherlands. Br. J. Nutr. 2017, 117, 1020–1031. [Google Scholar] [CrossRef] [PubMed]
- Hendriksen, M.; Etemad, Z.; van den Bogaard, C.; van der A, D.L. Salt, iodine and potassium intake 2015. Nutritional survey in adults in Doetichem. (Zout-, jodium- en kaliuminname 2015). Voedingsstatusonderzoek bij volwassenen uit Doetinchem); Report; Rijksinstituut Voor Volksgezond En Milieu: Bilthoven, The Netherlands, 2016; pp. 1–36. [Google Scholar]
- Stoutjesdijk, E.; Schaafsma, A.; Dijck-Brouwer, D.A.J.; Muskiet, F.A.J. Iodine status during pregnancy and lactation: A pilot study in the Netherlands. Neth. J. Med. 2018, 76, 210–217. [Google Scholar]
- Fordyce, F. Essentials of Medical Geology; Springer: Berlin/Heidelberg, Germany, 2013; pp. 375–416. [Google Scholar]
- Stoffaneller, R.; Morse, N.L. A Review of Dietary Selenium Intake and Selenium Status in Europe and the Middle East. Nutrients 2015, 7, 1494–1537. [Google Scholar] [CrossRef] [PubMed]
- Selenium Intake in Dutch Women; What is Consumed by the Dutch. (Inname Selenium Nederlandse Vrouwen; wat eet nederland). Available online: https://wateetnederland.nl/resultaten/vitamines-en-mineralen/inname/selenium (accessed on 11 July 2022). (In Dutch).
- Mullan, K.R.; McMullan, P.; Hunter, A.; McCance, D.R.; Smyth, P.; Bath, S.C.; Rayman, M.; Woodside, J.V. Selenium status in a Northern Irish pregnant cohort with iodine deficiency. Eur. J. Clin. Nutr. 2021, 75, 403–405. [Google Scholar] [CrossRef]
- Jin, Y.; Coad, J.; Weber, J.L.; Thomson, J.S.; Brough, L. Selenium Intake in Iodine-Deficient Pregnant and Breastfeeding Women in New Zealand. Nutrients 2019, 11, 69. [Google Scholar] [CrossRef]
- Stråvik, M.; Gustin, K.; Barman, M.; Skröder, H.; Sandin, A.; Wold, A.E.; Sandberg, A.; Kippler, M.; Vahter, M. Infant Iodine and Selenium Status in Relation to Maternal Status and Diet During Pregnancy and Lactation. Front. Nutr. 2021, 8. [Google Scholar] [CrossRef]
- Bu, Y.; Yuan, L.; Tian, C.; Zhao, C.; Ji, C.; Gao, X.; Cai, Y.; Sun, D.; Liu, Y. 24 h urinary creatinine excretion during pregnancy and its application in appropriate estimation of 24 h urinary iodine excretion. J. Trace Elem. Med. Biol. 2021, 66, 126751. [Google Scholar] [CrossRef]
- World Health Organization. Assessment of Iodine Deficiency Disorders and Monitoring their Elimination: A Guide for Programme Managers; World Health Organization: Geneva, Switzerland, 2007.
- Censi, S.; Watutantrige-Fernando, S.; Groccia, G.; Manso, J.; Plebani, M.; Faggian, D.; Mion, M.M.; Venturini, R.; Andrisani, A.; Casaro, A.; et al. The Effects of Iodine Supplementation in Pregnancy on Iodine Status, Thyroglobulin Levels and Thyroid Function Parameters: Results from a Randomized Controlled Clinical Trial in a Mild-to-Moderate Iodine Deficiency Area. Nutrients 2019, 11, 2639. [Google Scholar] [CrossRef]
- Kim, H.K.; Lee, S.Y.; Lee, J.I.; Jang, H.W.; Kim, S.K.; Chung, H.S.; Tan, A.; Hyun, K.; Hur, K.Y.; Kim, J.H.; et al. Usefulness of iodine/creatinine ratio from spot-urine samples to evaluate the effectiveness of low-iodine diet preparation for radioiodine therapy. Clin. Endocrinol. 2010, 73, 114–118. [Google Scholar] [CrossRef]
- Ghassabian, A.; Steenweg-de Graaff, J.; Peeters, R.P.; Ross, H.A.; Jaddoe, V.W.; Hofman, A.; Verhulst, F.C.; White, T.; Tiemeier, H. Maternal urinary iodine concentration in pregnancy and children’s cognition: Results from a population-based birth cohort in an iodine-sufficient area. BMJ Open 2014, 4, e005520. [Google Scholar] [CrossRef]
- Thomson, C.D.; Smith, T.E.; Butler, K.A.; Packer, M.A. An Evaluation of Urinary Measures of Iodine and Selenium Status. J. Trace Elem. Med. Biol. 1996, 10, 214–222. [Google Scholar] [CrossRef]
- Compounds Institute of Medicine (U.S.). Panel on Dietary Antioxidants and Related Selenium; National Academies Press (US): Washington, DC, USA, 2000. [Google Scholar]
- EFSA Scientific Opinion on Dietary Reference Values for selenium. EFSA J. 2014, 12, 3846. [CrossRef]
- Health Council of the Netherlands. An Evaluation of Dietary Reference Values for Vitamins and Minerals for Pregnant Women; Health Council of the Netherland: Hague, The Netherlands, 2021; pp. 1–209. [Google Scholar]
- Chen, W.; Wu, Y.; Lin, L.; Tan, L.; Shen, J.; Pearce, E.N.; Guo, X.; Wang, W.; Bian, J.; Jiang, W.; et al. 24-Hour Urine Samples Are More Reproducible Than Spot Urine Samples for Evaluation of Iodine Status in School-Age Children. J. Nutr. 2016, 146, 142–146. [Google Scholar] [CrossRef]
- Eastman, C.J.; Ma, G.; Li, M. Optimal Assessment and Quantification of Iodine Nutrition in Pregnancy and Lactation: Laboratory and Clinical Methods, Controversies and Future Directions. Nutrients 2019, 11, 2378. [Google Scholar] [CrossRef]
- Li, C.; Peng, S.; Zhang, X.; Xie, X.; Wang, D.; Mao, J.; Teng, X.; Shan, Z.; Teng, W. The Urine Iodine to Creatinine as an Optimal Index of Iodine During Pregnancy in an Iodine Adequate Area in China. J. Clin. Endocrinol. Metab. 2016, 101, 1290–1298. [Google Scholar] [CrossRef]
- Perrine, C.G.; Cogswell, M.E.; Swanson, C.A.; Sullivan, K.M.; Chen, T.; Carriquiry, A.L.; Dodd, K.W.; Caldwell, K.L.; Wang, C. Comparison of population iodine estimates from 24-hour urine and timed-spot urine samples. Thyroid 2014, 24, 748–757. [Google Scholar] [CrossRef]
- Vandevijvere, S.; Amsalkhir, S.; Mourri, A.B.; Van Oyen, H.; Moreno-Reyes, R. Iodine deficiency among Belgian pregnant women not fully corrected by iodine-containing multivitamins: A national cross-sectional survey. Br. J. Nutr. 2013, 109, 2276–2284. [Google Scholar] [CrossRef]
- Knight, B.A.; Shields, B.M.; He, X.; Pearce, E.N.; Braverman, L.E.; Sturley, R.; Vaidya, B. Iodine deficiency amongst pregnant women in South-West England. Clin. Endocrinol. 2017, 86, 451–455. [Google Scholar] [CrossRef]
- Granfors, M.; Andersson, M.; Stinca, S.; Åkerud, H.; Skalkidou, A.; Poromaa, I.S.; Wikström, A.; Nyström, H.F. Iodine deficiency in a study population of pregnant women in Sweden. Acta Obstet. Gynecol. Scand. 2015, 94, 1168–1174. [Google Scholar] [CrossRef] [PubMed]
- Manousou, S.; Andersson, M.; Eggertsen, R.; Hunziker, S.; Hulthén, L.; Nyström, H.F. Iodine deficiency in pregnant women in Sweden: A national cross-sectional study. Eur. J. Nutr. 2019, 59, 2535–2545. [Google Scholar] [CrossRef]
- Kirkegaard-Klitbo, D.M.; Perslev, K.; Andersen, S.L.; Perrild, H.; Knudsen, N.; Weber, T.; Rasmussen, L.B.; Laurberg, P. Iodine deficiency in pregnancy is prevalent in vulnerable groups in Denmark. Dan. Med. J. 2016, 63, 1–5. [Google Scholar]
- Lindorfer, H.; Krebs, M.; Kautzky-Willer, A.; Bancher-Todesca, D.; Sager, M.; Gessl, A. Iodine deficiency in pregnant women in Austria. Eur. J. Clin. Nutr. 2015, 69, 349–354. [Google Scholar] [CrossRef] [PubMed]
- Schuurman, R.W.C.; Beukers, M.H.; van Rossum, C.T.M. Do the Dutch eat and Drink According To The Guideline? Results From The Food Consumption Survey, (Eet En Drinkt Nl Volgens De Schijf Van Vijf); National Institute for Public Health: Hague, The Netherlands, 2020. [Google Scholar]
- Thomson, C.D.; Packer, M.A.; Butler, J.A.; Duffield, A.J.; O’Donaghue, K.L.; Whanger, P.D. Urinary selenium and iodine during pregnancy and lactation. J. Trace Elem. Med. Biol. 2001, 14, 210–217. [Google Scholar] [CrossRef]
- de Escobar, G.M.; Obregón, M.J.; del Rey, F.E. Iodine deficiency and brain development in the first half of pregnancy. Public Health Nutr. 2007, 10, 1554–1570. [Google Scholar] [CrossRef]
- Lazarus, J.; Brown, R.S.; Daumerie, C.; Hubalewska-Dydejczyk, A.; Negro, R.; Vaidya, B. 2014 European thyroid association guidelines for the management of subclinical hypothyroidism in pregnancy and in children. Eur. Thyroid J. 2014, 3, 76–94. [Google Scholar] [CrossRef]
- Moleti, M.; Di Bella, B.; Giorgianni, G.; Mancuso, A.; De Vivo, A.; Alibrandi, A.; Trimarchi, F.; Vermiglio, F. Maternal thyroid function in different conditions of iodine nutrition in pregnant women exposed to mild-moderate iodine deficiency: An observational study. Clin. Endocrinol. 2011, 74, 762–768. [Google Scholar] [CrossRef]
- Gowachirapant, S.; Jaiswal, N.; Melse-Boonstra, A.; Galetti, V.; Stinca, S.; Mackenzie, I.; Thomas, S.; Thomas, T.; Winichagoon, P.; Srinivasan, K.; et al. Effect of iodine supplementation in pregnant women on child neurodevelopment: A randomised, double-blind, placebo-controlled trial. Lancet Diabetes Endocrinol. 2017, 5, 853–863. [Google Scholar] [CrossRef]
- Negro, R.; Greco, G.; Mangieri, T.; Pezzarossa, A.; Dazzi, D.; Hassan, H. The Influence of Selenium Supplementation on Postpartum Thyroid Status in Pregnant Women with Thyroid Peroxidase Autoantibodies. J. Clin. Endocrinol. Metab. 2007, 92, 1263–1268. [Google Scholar] [CrossRef]
- Amorós, R.; Murcia, M.; González, L.; Rebagliato, M.; Iñiguez, C.; Lopez-Espinosa, M.; Vioque, J.; Broberg, K.; Ballester, F.; Llop, S. Maternal selenium status and neuropsychological development in Spanish preschool children. Environ. Res. 2018, 166, 215–222. [Google Scholar] [CrossRef]
- Arthur, J.R.; Beckett, G.J.; Mitchell, J.H. The interactions between selenium and iodine deficiencies in man and animals. Nutr. Res. Rev. 2008, 12, 55–73. [Google Scholar] [CrossRef]
- Verkaik-Kloosterman, J.; Buurma-Rethans, E.; Dekkers, A. Knowledge of the Iodine Intake by Children and Adults in The Netherlands. Results of the Food consumption survey 2007–2010. (Inzicht in de jodiuminname van kinderen en volwassenen in Nederland. Resultaten uit de Voedselconsumptiepeiling 2007–2010); Report; Rijksinstituut Voor Volksgezond En Milieu: Bilthoven, The Netherlands, 2012. (In Dutch) [Google Scholar]
- Samson, L.; Hircsu, I.; Katko, M.; Bodor, M.; Gazdag, A.; Gazso, A.A.; Kovacs, B.; Posta, J.; Balogh, E.; Mocsary, P.; et al. Lower educational status interferes with maternal iodine intake during both pregnancy and lactation. Endocr. Connect. 2021, 10, 742–749. [Google Scholar] [CrossRef]
- Dijck-Brouwer, D.A.J.; Muskiet, F.A.J.; Verheesen, R.H.; Schaafsma, G.; Schaafsma, A.; Geurts, J.M.W. Thyroidal and extra-thyroidal requirements for iodine and selenium: A combined evolutionary and (patho)physiological approach. Nutrients 2022. This review will be part of this special Issue, it is accepted. [Google Scholar]
- What is consumed by the Dutch (wat eet nederland). Available online: https://www.wateetnederland.nl (accessed on 11 July 2022). (in Dutch).
- Meyboom-de Jong, B. Guidelines Adequate Nutrition 2015 (Richtlijnen goede voeding 2015). In Guideline; Health Council of the Netherlands: The Hague, The Netherlends, 2015. [Google Scholar]
- Lofstedt, A.; de Roos, B.; Fernandes, P.G. Less than half of the European dietary recommendations for fish consumption are satisfied by national seafood supplies. Eur. J. Nutr. 2021, 60, 4219–4228. [Google Scholar] [CrossRef]
- Cunnane, S.C. Survival of the Fattest; World Scientific: Hackensack, NJ, USA, 2005. [Google Scholar]
- Barone, G.; Storelli, A.; Meleleo, D.; Dambrosio, A.; Garofalo, R.; Busco, A.; Storelli, M.M. Levels of Mercury, Methylmercury and Selenium in Fish: Insights into Children Food Safety. Toxics 2021, 9, 39. [Google Scholar] [CrossRef]
- Zou, C.; Yin, D.; Wang, R. Mercury and selenium bioaccumulation in wild commercial fish in the coastal East China Sea: Selenium benefits versus mercury risks. Mar. Pollut. Bull. 2022, 180, 113754. [Google Scholar] [CrossRef]
- Zwolak, I. The Role of Selenium in Arsenic and Cadmium Toxicity: An Updated Review of Scientific Literature. Biol. Trace Elem. Res. 2019, 193, 44–63. [Google Scholar] [CrossRef]


| Variable | Unit | Median (Range)/n (%) |
|---|---|---|
| Age | years | 31 (21–43) |
| Pre-pregnancy BMI | kg/m2 | 23 (17–51) |
| Gestational age | weeks | 29 (6–42) |
| Number of pregnancies | n | 2 (1–6) |
| Parity | n | 1 (0–3) |
| Education | ||
| High | n (%) | 158 (78.6) |
| Low | n (%) | 43 (21.4) |
| Nutritional supplements | ||
| Unknown | n (%) | 21 (10.4) |
| No supplement | n (%) | 32 (15.9) |
| Use of supplement | n (%) | 148 (73.6) |
| Supplement without iodine | n (%) | 54 (26.9) |
| Iodine-containing supplement | n (%) | 94 (46.8) |
| 75 µg/day | n (%) | 59 (29.4) |
| 150 µg/day | n (%) | 35 (17.4) |
| Selenium-containing supplement | n (%) | 100 (49.8) |
| Parameter | Unit | Median | Range | % Insufficient | Cut-Off Value | ||
|---|---|---|---|---|---|---|---|
| 24 h UIE | µg | 185 | 43 | - | 2654 | 69.7 | 225 |
| 24 h UIC | µg/L | 95 | 31 | - | 1072 | 88.1 | 150 |
| 24 h ICR | µg/g | 141 | 42 | - | 1938 | 57.7 | 150 |
| Morning UIC | µg/L | 129 | 34 | - | 4401 | 64.3 | 150 |
| Morning ICR | µg/g | 114 | 37 | - | 6282 | 73.4 | 150 |
| 24 h urine volume | mL | 1940 | 400 | - | 5550 | ||
| Creatinine concentration: | |||||||
| 24 h urine | g/L | 0.67 | 0.21 | - | 2.73 | ||
| Morning urine | g/L | 1.07 | 0.21 | - | 4.09 | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mayunga, K.C.; Lim-A-Po, M.; Lubberts, J.; Stoutjesdijk, E.; Touw, D.J.; Muskiet, F.A.J.; Dijck-Brouwer, D.A.J. Pregnant Dutch Women Have Inadequate Iodine Status and Selenium Intake. Nutrients 2022, 14, 3936. https://doi.org/10.3390/nu14193936
Mayunga KC, Lim-A-Po M, Lubberts J, Stoutjesdijk E, Touw DJ, Muskiet FAJ, Dijck-Brouwer DAJ. Pregnant Dutch Women Have Inadequate Iodine Status and Selenium Intake. Nutrients. 2022; 14(19):3936. https://doi.org/10.3390/nu14193936
Chicago/Turabian StyleMayunga, K. Clara, Melany Lim-A-Po, Janniek Lubberts, Eline Stoutjesdijk, Daan J. Touw, Frits A. J. Muskiet, and D. A. Janneke Dijck-Brouwer. 2022. "Pregnant Dutch Women Have Inadequate Iodine Status and Selenium Intake" Nutrients 14, no. 19: 3936. https://doi.org/10.3390/nu14193936
APA StyleMayunga, K. C., Lim-A-Po, M., Lubberts, J., Stoutjesdijk, E., Touw, D. J., Muskiet, F. A. J., & Dijck-Brouwer, D. A. J. (2022). Pregnant Dutch Women Have Inadequate Iodine Status and Selenium Intake. Nutrients, 14(19), 3936. https://doi.org/10.3390/nu14193936







