Dietary Protein Requirement Threshold and Micronutrients Profile in Healthy Older Women Based on Relative Skeletal Muscle Mass
Abstract
:1. Introduction
2. Materials and Methods
2.1. Participant Characteristics
2.2. Skeletal Muscle Mass Measurement and Low Muscle Mass Definition
2.3. Vastus Lateralis and Biceps Brachii Size
2.4. Muscle Strength and Muscle Quality
2.5. Physical Activity Scale for the Elderly Questionnaire
2.6. Dietary Assessment
2.7. Statistics
3. Results
3.1. Dietary Food Items and Nutrient Intake Pattern of Participants with Age-Group Categories and Pre-Sarcopenia
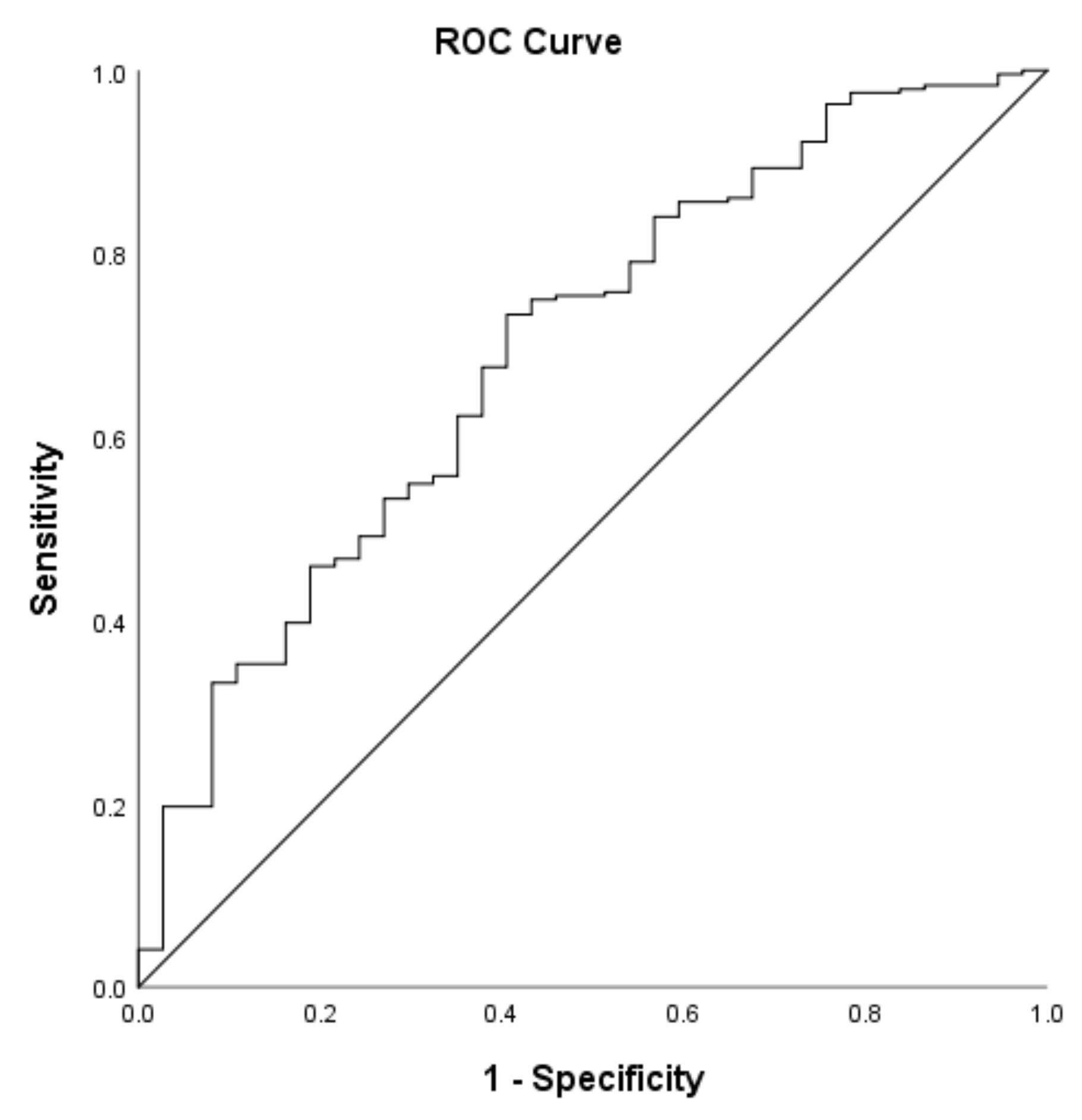
3.2. Minimally Required Dietary Protein Intake for a High Relative Muscle Mass
4. Discussion
4.1. Dietary Nutrients Intake Difference with Age-Groups and Pre-Sarcopenia Status
4.2. Dietary Protein Threshold for Low Relative Skeletal Muscle Mass, Skeletal Muscle Phenotypes and Body Composition
4.3. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Granic, A.; Sayer, A.A.; Robinson, S.M. Dietary patterns, skeletal muscle health, and sarcopenia in older adults. Nutrients 2019, 11, 745. [Google Scholar] [CrossRef] [Green Version]
- Landi, F.; Russo, A.; Liperoti, R.; Tosato, M.; Barillaro, C.; Pahor, M.; Bernabei, R.; Onder, G. Anorexia, Physical Function, and Incident Disability Among the Frail Elderly Population: Results From the ilSIRENTE Study. J. Am. Med. Dir. Assoc. 2010, 11, 268–274. [Google Scholar] [CrossRef] [PubMed]
- Landi, F.; Calvani, R.; Tosato, M.; Martone, A.M.; Ortolani, E.; Savera, G.; Sisto, A.; Marzetti, E. Anorexia of Aging: Risk Factors, Consequences, and Potential Treatments. Nutrients 2016, 8, 69. [Google Scholar] [CrossRef]
- Farsijani, S.; Payette, H.; Morais, J.A.; Shatenstein, B.; Gaudreau, P.; Chevalier, S. Even mealtime distribution of protein intake is associated with greater muscle strength, but not with 3-y physical function decline, in free-living older adults: The Quebec longitudinal study on Nutrition as a Determinant of Successful Aging (NuAge study). Am. J. Clin. Nutr. 2017, 106, 113–124. [Google Scholar] [CrossRef]
- Atherton, C.; McNaughton, L.R.; Close, G.L.; Sparks, A. Post-exercise provision of 40 g of protein during whole body resistance training further augments strength adaptations in elderly males. Res. Sports Med. 2020, 28, 469–483. [Google Scholar] [CrossRef]
- Gorissen, S.H.M.; Horstman, A.M.H.; Franssen, R.; Crombag, J.J.R.; Langer, H.; Bierau, J.; Respondek, F.; Van Loon, L.J. Ingestion of Wheat Protein Increases In Vivo Muscle Protein Synthesis Rates in Healthy Older Men in a Randomized Trial. J. Nutr. 2016, 146, 1651–1659. [Google Scholar] [CrossRef]
- Wolfe, R.R.; Miller, S.L. The recommended dietary allowance of protein: A misunderstood concept. J. Am. Med. Asso. 2008, 299, 2891–2893. [Google Scholar] [CrossRef]
- Volpi, E.; Campbell, W.W.; Dwyer, J.T.; Johnson, M.A.; Jensen, G.L.; Morley, J.E.; Wolfe, R.R. Is the optimal level of protein intake for older adults greater than the recommended dietary allowance? J. Gerontol. 2013, 68, 677–681. [Google Scholar]
- Martone, A.M.; Marzetti, E.; Calvani, R.; Picca, A.; Tosato, M.; Santoro, L.; Di Giorgio, A.; Nesci, A.; Sisto, A.; Santoliquido, A.; et al. Exercise and Protein Intake: A Synergistic Approach against Sarcopenia. BioMed Res. Int. 2017, 2017, 1–7. [Google Scholar] [CrossRef]
- Bauer, J.; Biolo, G.; Cederholm, T.; Cesari, M.; Cruz-Jentoft, A.J.; Morley, J.E.; Phillips, S.; Sieber, C.C.; Stehle, P.; Teta, D.; et al. Evidence-Based Recommendations for Optimal Dietary Protein Intake in Older People: A Position Paper from the PROT-AGE Study Group. J. Am. Med. Dir. Assoc. 2013, 14, 542–559. [Google Scholar] [CrossRef] [PubMed]
- Paddon-Jones, D.; Short, K.; Campbell, W.W.; Volpi, E.; Wolfe, R.R. Role of dietary protein in the sarcopenia of aging. Am. J. Clin. Nutr. 2008, 87, 1562S–1566S. [Google Scholar] [CrossRef] [Green Version]
- Morley, J.E.; Argiles, J.M.; Evans, W.J.; Bhasin, S.; Cella, D.; Deutz, N.E.; Doehner, W.; Fearon, K.C.; Ferrucci, L.; Hellerstein, M.K.; et al. Nutritional Recommendations for the Management of Sarcopenia. J. Am. Med. Dir. Assoc. 2010, 11, 391–396. [Google Scholar] [CrossRef] [Green Version]
- Nutrient Requirements; British Nutrition Foundation: London, UK, 2019.
- Janssen, I.; Heymsfield, S.B.; Ross, R. Low relative skeletal muscle mass (sarcopenia) in older persons is asso-ciated with functional impairment and physical disability. J. Am. Geriatr. Soc. 2002, 50, 889–896. [Google Scholar] [CrossRef] [Green Version]
- Lauretani, F.; Russo, C.R.; Bandinelli, S.; Bartali, B.; Cavazzini, C.; Di Iorio, A.; Corsi, A.M.; Rantanen, T.; Guralnik, G.M.; Ferrucci, L. Age-associated changes in skeletal muscles and their effect on mobility: An operational diag-nosis of sarcopenia. J. Appl. Physiol. 2003, 95, 1851–1860. [Google Scholar] [CrossRef]
- Singh, R.B.; Beegom, R.; Rastogi, S.S.; Gaoli, Z.; Shoumin, Z. Association of low plasma concentrations of antioxidant vitamins, magnesium and zinc with high body fat per cent measured by bioelectrical impedance analysis in Indian men. Magnes. Res. 1998, 11, 3–10. [Google Scholar]
- Nakai, K.; Fujii, H.; Kono, K.; Goto, S.; Kitazawa, R.; Kitazawa, S.; Hirata, M.; Shinohara, M.; Fukagawa, M.; Nishi, S. Vitamin D Activates the Nrf2-Keap1 Antioxidant Pathway and Ameliorates Nephropathy in Diabetic Rats. Am. J. Hypertens. 2013, 27, 586–595. [Google Scholar] [CrossRef] [Green Version]
- Nguyen, M.-H.T.; Jafri, M.S. Mitochondrial Calcium Signaling and Energy Metabolism. Ann. N. Y. Acad. Sci. 2005, 1047, 127–137. [Google Scholar] [CrossRef]
- Scott, D.; Blizzard, L.; Fell, J.; Giles, G.; Jones, G. Associations Between Dietary Nutrient Intake and Muscle Mass and Strength in Community-Dwelling Older Adults: The Tasmanian Older Adult Cohort Study. J. Am. Geriatr. Soc. 2010, 58, 2129–2134. [Google Scholar] [CrossRef] [PubMed]
- Hänsch, R.; Mendel, R.R. Physiological functions of mineral micronutrients (Cu, Zn, Mn, Fe, Ni, Mo, B, Cl). Curr. Opin. Plant Biol. 2009, 12, 259–266. [Google Scholar] [CrossRef] [PubMed]
- Powell, S.R. The Antioxidant Properties of Zinc. J. Nutr. 2000, 130, 1447S–1454S. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mastaglia, S.R.; Seijo, M.; Muzio, D.; Somoza, J.; Nuñez, M.; Oliveri, B. Effect of vitamin D nutritional status on muscle function and strength in healthy women aged over sixty-five years. J. Nutr. Health Aging 2010, 15, 349–354. [Google Scholar] [CrossRef]
- Santos, D.A.; Matias, C.N.; Monteiro, C.; Silva, A.; Rocha, P.; Minderico, C.; Sardinha, L.; Laires, M.J. Magnesium intake is associated with strength performance in elite basketball, handball and volleyball players. Magnes. Res. 2011, 24, 215–219. [Google Scholar] [CrossRef] [Green Version]
- Calvani, R.; Emartone, A.M.; Marzetti, E.; Eonder, G.; Esavera, G.; Elorenzi, M.; Eserafini, E.; Bernabei, R.; Elandi, F. Pre-Hospital Dietary Intake Correlates with Muscle Mass at the Time of Fracture in Older Hip-Fractured Patients. Front. Aging Neurosci. 2014, 6, 269. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Landi, F.; Liperoti, R.; Russo, A.; Giovannini, S.; Tosato, M.; Barillaro, C.; Capoluongo, E.D.; Bernabei, R.; Onder, G. Association of anorexia with sarcopenia in a community-dwelling elderly population: Results from the ilSIRENTE study. Eur. J. Nutr. 2012, 52, 1261–1268. [Google Scholar] [CrossRef]
- Ring, S.M.; Dannecker, E.A.; Peterson, C.A. Vitamin D status is not associated with outcomes of experimen-tally-induced muscle weakness and pain in young, healthy volunteers. J. Nutr. Metab. 2010, 2010. [Google Scholar] [CrossRef] [Green Version]
- Chan, R.; Chan, D.; Woo, J.; Ohlsson, C.; Mellström, D.; Kwok, T.; Leung, P.C. Not All Elderly People Benefit From Vitamin D Supplementation with Respect to Physical Function: Results From the Osteoporotic Fractures in Men Study, Hong Kong. J. Am. Geriatr. Soc. 2011, 60, 290–295. [Google Scholar] [CrossRef] [PubMed]
- Bhasin, S.; Apovian, C.M.; Travison, T.G.; Pencina, K.; Moore, L.L.; Huang, G.; Campbell, W.W.; Li, Z.; Howland, A.S.; Chen, R.; et al. Effect of Protein Intake on Lean Body Mass in Functionally Limited Older Men: A Randomized Clinical Trial. JAMA Intern. Med. 2018, 178, 530–541. [Google Scholar] [CrossRef]
- Bauer, J.M.; Verlaan, S.; Bautmans, I.; Brandt, K.; Donini, L.; Maggio, M.; McMurdo, M.E.; Mets, T.; Seal, C.; Wijers, S.; et al. Effects of a Vitamin D and Leucine-Enriched Whey Protein Nutritional Supplement on Measures of Sarcopenia in Older Adults, the PROVIDE Study: A Randomized, Double-Blind, Placebo-Controlled Trial. J. Am. Med. Dir. Assoc. 2015, 16, 740–747. [Google Scholar] [CrossRef]
- Schröder, H.; Vila, J.; Marrugat, J.; Covas, M.-I. Low Energy Density Diets Are Associated with Favorable Nutrient Intake Profile and Adequacy in Free-Living Elderly Men and Women. J. Nutr. 2008, 138, 1476–1481. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kojima, N.; Kim, M.; Saito, K.; Yoshida, H.; Yoshida, Y.; Hirano, H.; Obuchi, S.; Shimada, H.; Suzuki, T.; Kim, H. Lifestyle-Related Factors Contributing to Decline in Knee Extension Strength among Elderly Women: A Cross-Sectional and Longitudinal Cohort Study. PLoS ONE 2015, 10, e0132523. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Khanal, P.; He, L.; Stebbings, G.K.; Onambele-Pearson, G.L.; Degens, H.; Williams, A.G.; Thomis, M.; Morse, C.I. Static one-leg standing balance test as a screening tool for low muscle mass in healthy elderly women. Aging Clin. Exp. Res. 2021, 33, 1831–1839. [Google Scholar] [CrossRef] [PubMed]
- Shin, H.I.; Kim, D.-K.; Seo, K.M.; Kang, S.H.; Lee, S.Y.; Son, S. Relation Between Respiratory Muscle Strength and Skeletal Muscle Mass and Hand Grip Strength in the Healthy Elderly. Ann. Rehabil. Med. 2017, 41, 686–692. [Google Scholar] [CrossRef]
- Park, B.S.; Yoon, J.S. Relative Skeletal Muscle Mass Is Associated with Development of Metabolic Syndrome. Diabetes Metab. J. 2013, 37, 458–464. [Google Scholar] [CrossRef] [Green Version]
- Han, J.M.; Lee, M.Y.; Lee, K.B.; Kim, H.; Hyun, Y.Y. Low relative skeletal muscle mass predicts incident hypertension in Korean men: A prospective cohort study. J. Hypertens. 2020, 38, 2223–2229. [Google Scholar] [CrossRef] [PubMed]
- Huang, T.-T.; Chung, M.-L.; Chen, F.-R.; Chin, Y.-F.; Wang, B.-H. Evaluation of a combined cognitive-behavioural and exercise intervention to manage fear of falling among elderly residents in nursing homes. Aging Ment. Health 2015, 20, 2–12. [Google Scholar] [CrossRef]
- Hassan, B.H.; Hewitt, J.; Keogh, J.W.; Bermeo, S.; Duque, G.; Henwood, T.R. Impact of resistance training on sarcopenia in nursing care facilities: A pilot study. Geriatr. Nurs. 2015, 37, 116–121. [Google Scholar] [CrossRef] [PubMed]
- Khanal, P.; He, L.; Stebbings, G.; Onambele-Pearson, G.L.; Degens, H.; Williams, A.; Thomis, M.; Morse, C.I. Prevalence and association of single nucleotide polymorphisms with sarcopenia in older wom-en depends on definition. Sci. Rep. 2020, 10, 2913. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Janssen, I.; Heymsfield, S.B.; Baumgartner, R.N.; Ross, R. Estimation of skeletal muscle mass by bioelectrical impedance analysis. J. Appl. Physiol. 2000, 89, 465–471. [Google Scholar] [CrossRef] [Green Version]
- Faria, S.L.; Faria, O.P.; Cardeal, M.D.; Ito, M.K. Validation study of multi-frequency bioelectrical impedance with dual-energy X-ray absorp-tiometry among obese patients. Obesity Surg. 2014, 24, 1476–1480. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.M.; Jang, H.C.; Lim, S. Differences among skeletal muscle mass indices derived from height-, weight-, and body mass index-adjusted models in assessing sarcopenia. Korean J. Intern. Med. 2016, 31, 643–650. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cruz-Jentoft, A.J.; Bahat, G.; Bauer, J.; Boirie, Y.; Bruyère, O.; Cederholm, T.; Cooper, C.; Landi, F.; Rolland, Y.; Sayer, A.A.; et al. Sarcopenia: Revised European consensus on definition and diagnosis. Age Ageing 2018, 48, 16–31. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Miyatani, M.; Kanehisa, H.; Ito, M.; Kawakami, Y.; Fukunaga, T. The accuracy of volume estimates using ultrasound muscle thickness measurements in dif-ferent muscle groups. Eur. J. Appl. Physiol. 2004, 91, 264–272. [Google Scholar]
- Khanal, P.; He, L.; Herbert, A.J.; Stebbings, G.K.; Onambele-Pearson, G.L.; Degens, H.; Morse, C.I.; Thomis, M.; Williams, A.G. The Association of Multiple Gene Variants with Ageing Skeletal Muscle Phenotypes in Elderly Women. Genes 2020, 11, 1459. [Google Scholar] [CrossRef]
- Washburn, R.A.; Ficker, J.L. Physical Activity Scale for the Elderly (PASE): The relationship with activity measured by a portable accelerometer. J. Sports Med. Phys. Fit. 1999, 39, 336. [Google Scholar]
- Bingham, S.A.; Gill, C.; Welch, A.; Day, K.; Cassidy, A.; Khaw, K.T.; Sneyd, M.J.; Key, T.J.A.; Roe, L.; Day, N.E. Comparison of dietary assessment methods in nutritional epidemiology: Weighed records v. 24 h recalls, food-frequency questionnaires and estimated-diet records. Br. J. Nutr. 1994, 72, 619–643. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Day, N.E.; McKeown, N.; Wong, M.Y.; Welch, A.; Bingham, S. Epidemiological assessment of diet: A comparison of a 7-day diary with a food frequency ques-tionnaire using urinary markers of nitrogen, potassium and sodium. Int. J. Epi. 2001, 30, 309–317. [Google Scholar] [CrossRef] [Green Version]
- Welch, A.A.; Luben, R.; Khaw, K.T.; Bingham, S.A. The CAFE computer program for nutritional analysis of the EPIC-Norfolk food frequency questionnaire and identification of extreme nutrient values. J. Hum. Nutr. Diet. 2005, 18, 99–116. [Google Scholar] [CrossRef] [PubMed]
- Wurtman, J.J.; Lieberman, H.; Tsay, R.; Nader, T.; Chew, B. Calorie and nutrient intakes of elderly and young subjects measured under identical condi-tions. J. Gerontol. 1988, 43, B174–B180. [Google Scholar] [CrossRef]
- Giezenaar, C.; Chapman, I.M.; Luscombemarsh, N.D.; Feinle-Bisset, C.; Horowitz, M.; Soenen, S. Ageing Is Associated with Decreases in Appetite and Energy Intake—A Meta-Analysis in Healthy Adults. Nutrients 2016, 8, 28. [Google Scholar] [CrossRef] [Green Version]
- Van Walleghen, E.L.; Orr, J.S.; Gentile, C.L.; Davy, K.P.; Davy, B.M. Habitual physical activity differentially affects acute and short-term energy intake regulation in young and older adults. Int. J. Obes. 2007, 31, 1277–1285. [Google Scholar] [CrossRef] [Green Version]
- Bartali, B.; Salvini, S.; Turrini, A.; Lauretani, F.; Russo, C.R.; Corsi, A.M.; Bandinelli, S.; D’Amicis, A.; Palli, D.; Guralnik, J.M.; et al. Age and Disability Affect Dietary Intake. J. Nutr. 2003, 133, 2868–2873. [Google Scholar] [CrossRef]
- Granic, A.; Mendonça, N.; Sayer, A.A.; Hill, T.R.; Davies, K.; Adamson, A.; Siervo, M.; Mathers, J.C.; Jagger, C. Low protein intake, muscle strength and physical performance in the very old: The Newcastle 85+ Study. Clin. Nutr. 2017, 37, 2260–2270. [Google Scholar] [CrossRef] [Green Version]
- Robinson, S.M.; Jameson, K.A.; Batelaan, S.F.; Martin, H.J.; Syddall, H.E.; Dennison, E.M.; Cooper, C.; Sayer, A.A. Diet and its relationship with grip strength in community-dwelling older men and wom-en: The Hertfordshire cohort study. J. Am. Geriatr. Soc. 2008, 56, 84–90. [Google Scholar] [CrossRef]
- Nakayama, K.; Saito, Y.; Sanbongi, C.; Murata, K.; Urashima, T. Effects of low-dose milk protein supplementation following low-to-moderate intensity exercise training on muscle mass in healthy older adults: A randomized placebo-controlled trial. Eur. J. Nutr. 2021, 60, 917–928. [Google Scholar] [CrossRef] [PubMed]
- León-Muñoz, L.M.; Guallar-Castillón, P.; López-García, E.; Rodríguez-Artalejo, F. Mediterranean Diet and Risk of Frailty in Community-Dwelling Older Adults. J. Am. Med. Dir. Assoc. 2014, 15, 899–903. [Google Scholar] [CrossRef]
- Shikany, J.M.; Barrett-Connor, E.; Ensrud, K.; Cawthon, P.M.; Lewis, C.E.; Dam, T.-T.L.; Shannon, J.; Redden, D.T.; for the Osteoporotic Fractures in Men (MrOS) Research Group. Macronutrients, Diet Quality, and Frailty in Older Men. J. Gerontol. Ser. A Boil. Sci. Med. Sci. 2013, 69, 695–701. [Google Scholar] [CrossRef]
- García-Esquinas, E.; Ortolá, R.; Banegas, J.R.; Lopez-García, E.; Rodríguez-Artalejo, F. Dietary n-3 polyunsaturated fatty acids, fish intake and healthy ageing. Int. J. Epi. 2019, 48, 1914–1924. [Google Scholar] [CrossRef]
- Gil, A.; de Victoria, E.M.; Olza, J. Indicators for the evaluation of diet quality. Nutr. Hosp. 2015, 31, 128–144. [Google Scholar]
- Bao, W.; Tobias, D.K.; Olsen, S.F.; Zhang, C. Pre-pregnancy fried food consumption and the risk of gestational diabetes mellitus: A prospective cohort study. Diabetologia 2014, 57, 2485–2491. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Carlsen, M.H.; Andersen, L.F.; Dahl, L.; Norberg, N.; Hjartåker, A. New Iodine Food Composition Database and Updated Calculations of Iodine Intake among Norwegians. Nutrients 2018, 10, 930. [Google Scholar] [CrossRef] [Green Version]
- Cardoso, B.R.; Duarte, G.B.S.; Reis, B.Z.; Cozzolino, S. Brazil nuts: Nutritional composition, health benefits and safety aspects. Food Res. Int. 2017, 100, 9–18. [Google Scholar] [CrossRef]
- Surai, P.F.; Kochish, I.I.; Romanov, M.N.; Griffin, D.K. Nutritional modulation of the antioxidant capacities in poultry: The case of vitamin E. Poult. Sci. 2019, 98, 4030–4041. [Google Scholar] [CrossRef]
- Salvatore, D.; Simonides, W.S.; Dentice, M.; Zavacki, A.M.; Larsen, P.R. Thyroid hormones and skeletal muscle—New insights and potential implications. Nat. Rev. Endocrinol. 2013, 10, 206–214. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chen, P.; Bornhorst, J.; Aschner, M. Manganese metabolism in humans. Front. Biosci. 2018, 23, 1655–1679. [Google Scholar] [CrossRef] [Green Version]
- Campbell, W.W.; Leidy, H.J. Dietary Protein and Resistance Training Effects on Muscle and Body Composition in Older Persons. J. Am. Coll. Nutr. 2007, 26, 696S–703S. [Google Scholar] [CrossRef] [PubMed]
- Gregorio, L.; Brindisi, J.; Kleppinger, A.; Sullivan, R.; Mangano, K.; Bihuniak, J.D.; Kenny, A.M.; Kerstetter, J.E.; Insogna, K. Adequate dietary protein is associated with better physical performance among post-menopausal women 60–90 years. J. Nutr. Heal. Aging 2013, 18, 155–160. [Google Scholar] [CrossRef] [Green Version]
- Tomlinson, D.J.; Erskine, R.M.; Morse, C.I.; Onambélé, G.L. Impact of Above-Average Proanabolic Nutrients Is Overridden by High Protein and En-ergy Intake in the Muscle-Tendon Unit Characteristics of Middle-to Older-Aged Adults. J. Nutr. 2018, 148, 1776–1785. [Google Scholar] [CrossRef] [PubMed]
- Vinknes, K.J.; De Vogel, S.; Elshorbagy, A.K.; Nurk, E.; Drevon, C.A.; Gjesdal, C.G.; Tell, G.S.; Vollset, S.E.; Refsum, H. Dietary Intake of Protein Is Positively Associated with Percent Body Fat in Middle-Aged and Older Adults. J. Nutr. 2011, 141, 440–446. [Google Scholar] [CrossRef] [PubMed]
- Vivodtzev, I.; Moncharmont, L.; Tamisier, R.; Borel, J.C.; Arbib, F.; Wuyam, B.; Lévy, P.; Maltais, F.; Ferretti, G.; Pépin, J.L. Quadriceps muscle fat infiltration is associated with cardiometabolic risk in COPD. Clin. Physiol. Funct. Imaging 2017, 38, 788–797. [Google Scholar] [CrossRef] [PubMed]
- Komici, K.; Iacono, A.D.; De Luca, A.; Perrotta, F.; Bencivenga, L.; Rengo, G.; Rocca, A.; Guerra, G. Adiponectin and Sarcopenia: A Systematic Review with Meta-Analysis. Front. Endocrinol. 2021, 12, 329. [Google Scholar] [CrossRef]
- Freedman, L.S.; Schatzkin, A.; Midthune, D.; Kipnis, V. Dealing With Dietary Measurement Error in Nutritional Cohort Studies. J. Natl. Cancer Inst. 2011, 103, 1086–1092. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Macdonald, H.M.; Mavroeidi, A.; Barr, R.; Black, A.J.; Fraser, W.D.; Reid, D.M. Vitamin D status in postmenopausal women living at higher latitudes in the UK in relation to bone health, overweight, sunlight exposure and dietary vitamin D. Bone 2008, 42, 996–1003. [Google Scholar] [CrossRef]
- Washburn, R.A.; McAuley, E.; Katula, J.; Mihalko, S.L.; Boileau, R.A. The Physical Activity Scale for the Elderly (PASE): Evidence for Validity. J. Clin. Epidemiol. 1999, 52, 643–651. [Google Scholar] [CrossRef]
- Schuit, A.J.; Schouten, E.G.; Westerterp, K.R.; Saris, W.H. Validity of the physical activity scale for the elderly (PASE): According to energy expenditure assessed by the doubly labeled water method. J. Clin. Epidemiol. 1997, 50, 541–546. [Google Scholar] [CrossRef] [Green Version]
- Ryan, D.J.; Wullems, J.A.; Stebbings, G.K.; Morse, C.I.; Stewart, C.E.; Onambele-Pearson, G.L. Reliability and validity of the international physical activity questionnaire compared to cali-brated accelerometer cut-off points in the quantification of sedentary behaviour and physical activity in older adults. PLoS ONE 2018, 13, e0195712. [Google Scholar]
| General Characteristics | All Participants n = 281 | 60–64 Years n = 39 | 65–69 Years n = 98 | 70–74 Years n = 94 | 75–79 Years n = 34 | 80–91 Years n = 16 | p-Value (Age Groups) | Low Relative Skeletal Muscle Mass n = 37 | High Relative Skeletal Muscle Mass n = 244 | p-Value (Relative Skeletal Muscle Mass Groups) |
|---|---|---|---|---|---|---|---|---|---|---|
| Age (years) | 70 (7) | 62 (2)2,3,4,5 | 68 (2) 1,3,4,5 | 73 (3) 1,2,4,5 | 77 (3) 1,2,3 | 82 (8) 1,2,3 | <0.001 | 70 (6) | 70 (7) | 0.682 |
| Body mass (kg) | 65 (14) | 64.8 (16.0) | 66.3 (12.1) | 65.6 (12.2) | 61.8 (17.3) | 69.2 (13.1) | 0.108 | 76.1 (20.9) | 64.8 (11.8) | <0.001 |
| Height (m) | 1.60 (0.08) | 1.60 (0.06) | 1.60 (0.07) | 1.60 (0.08) | 1.58 (0.09) | 1.56 (0.13) | 0.032 | 1.60 (0.08) | 1.60 (0.08) | 0.788 |
| BMI (kg/m2) | 25.4 (4.5) | 24.7 (4.8) 4 | 25.5 (4.4) 4 | 25.4 (5.1) | 24.8 (3.9) 1,2 | 27.1 (5.9) | 0.029 | 30.3 (7.8) | 24.9 (4.1) | <0.001 |
| SMMr | 25.8 ± 4.0 | 27.6 (5.8) 3,5 | 25.9 (4.6) | 25.2 (5.1) 1 | 26.0 (3.9) | 23.9 (5.2) 1 | 0.007 | 20.1 (2.2) | 26.2 (4.3) | <0.001 |
| SMM (kg) | 16.9(3.1) | 17.1(2.5) 3,4,5 | 17.6 (3.3) 3,4 | 16.6 (3.0) 1,2 | 16.5 (2.8) 1,2, | 15.8 (3.3) 1 | 0.013 | 15.0 (4.2) | 17.1(2.8) | <0.001 |
| Fat mass (kg) | 27.1 (8.6) | 25.1 (11.4) 5 | 27.3 (8.3) | 27.4 (8.3) | 25.8 (8.0) | 31.4 (8.5) 1 | 0.012 | 37.6 (12.3) | 26.5 (7.7) | <0.001 |
| RMR (kcal) | 1268 ± 110 | 1288 ± 111 4 | 1291 ± 112 4 | 1262 ± 98 | 1213 ± 121 1,2 | 1235 ± 89 | 0.003 | 1288 ± 110 | 1265 ± 110 | 0.246 |
| Biceps brachii thickness (cm) | 1.71 (0.41) | 1.80 (0.48) | 1.73 (0.43) | 1.69 (0.43) | 1.87 (0.50) | 1.64 (0.33) | 0.482 | 1.74 (0.43) | 1.69 (0.41) | 0.521 |
| VLACSA (cm2) | 16.4 ± 3.3 | 18.6 ± 3.1 2,3,4,5 | 16.6 ± 3.4 1 | 16.2 ± 3.2 1 | 15.3 ± 2.9 1 | 14.7 ± 2.5 1 | <0.001 | 17.0 ± 3.7 | 16.4 ± 3.3 | 0.306 |
| HGS (kg) | 30.0 ± 4.9 | 32.5 (6.1) 4,5 | 30.8 (6.3) 4,5 | 29.9 (5.1) 5 | 27.4 (3.9) 1,2 | 23.7 (7.8) 1,2,3 | <0.001 | 28.7 ± 4.6 | 30.2 ± 5.0 | 0.081 |
| MVCEF (N·m) | 28.3 (9.1) | 31.1 (11.6) 5 | 28.9 (8.7) 5 | 28.4 (8.5) | 27.6 (8.4) | 24.7 (7.8) 1,2 | 0.020 | 26.7 (9.0) | 28.5 (9.1) | 0.140 |
| MVCKE (N·m) | 64.7 ± 21.3 | 72.3 (27.8) 4,5 | 66.4 (31.5) 5 | 65.6 (27.6) | 54.4 (33.2) 1 | 47.0 (32.1) 1,2 | <0.001 | 53.1 (26.2) | 65.9 (28.3) | 0.022 |
| HGS/Body mass (kg/kg) | 0.46 ± 0.09 | 0.51 ± 0.10 3,5 | 0.47 ± 0.10 5 | 0.46 ± 0.09 1,5 | 0.46 ± 0.08 5 | 0.36 ± 0.08 1,2,3,4 | <0.001 | 0.38 ± 0.07 | 0.47 ± 0.09 | <0.001 |
| PASE | 158 ± 50 | 156 (67) | 153 (69) | 161 (56) | 158 (52) | 122 (59) | 0.209 | 145 ± 51 | 160 ± 50 | 0.089 |
| Dietary Nutrients Intake (Per Day) | All Participants n = 281 | 60–64 Years n = 39 | 65–69 Years n = 98 | 70–74 Years n = 94 | 75–79 Years n = 34 | 80–91 Years n = 16 | p-Value (Age Groups) | Low Relative Skeletal Muscle Mass n = 37 | High Relative Skeletal Muscle Mass n = 244 | p-Value (Relative Skeletal Muscle Mass Groups) |
|---|---|---|---|---|---|---|---|---|---|---|
| Energy(kcal) | 1735 (552) | 1821 (498) | 1696 (527) | 1728 (623) | 1850 (565) | 1746 (684) | 0.476 | 1685 (545) | 1739 (568) | 0.217 |
| Carbohydrate (g) | 199 (71) | 206 (86) | 192 (65) | 200 (80) | 218 (57) | 202 (70) | 0.336 | 183 (68) | 201 (68) | 0.206 |
| Carbohydrate (%TEI) | 43.2 (8.8) | 43.5 (8.8) | 42.5 (8.6) | 43.6 (8.1) | 43.1 (10.0) | 42.8 (10.0) | 0.816 | 43.3 (8.5) | 43.2 (8.8) | 0.707 |
| Fat-total (g) | 66 (28) | 66 (23) | 64 (27) | 62 (26) | 70 (26) | 68 (31) | 0.207 | 64 (24) | 66 (30) | 0.272 |
| Fat-total (%TEI) | 34.2 (7.8) | 34.3 (10.3) | 34.3 (7.2) | 33.7 (7.5) | 35.3 (7.7) | 36.6 (8.1) | 0.482 | 33.7 (8.6) | 34.2 (7.8) | 0.533 |
| Protein (g) | 86 (31) | 81 (39) | 85 (30) | 86 (28) | 89 (32) | 86 (33) | 0.848 | 86 (32) | 86 (31) | 0.778 |
| Protein (g/kg/d) | 1.31 (0.55) | 1.26 (0.51) | 1.29 (0.57) | 1.31 (0.55) | 1.44 (0.63) | 1.38 (0.58) | 0.404 | 1.08 (0.49) | 1.33 (0.55) | <0.001 |
| SFA (g) | 24 (12) | 23 (12) | 24 (13) | 22 (10) | 28 (12) | 26 (11) | 0.276 | 25 (11) | 24 (12) | 0.902 |
| MUFA (g) | 24 (11) | 25 (13) | 24 (11) | 23 (10) | 26 (11) | 24 (14) | 0.323 | 22 (9) | 24 (11) | 0.160 |
| PUFA (g) | 12 (6) | 13 (7) | 11 (6) | 12 (5) | 13 (8) | 13 (8) | 0.100 | 11 (4) | 13 (7) | 0.023 |
| Calcium (mg) | 968(345) | 976 (263) | 985 (339) | 1010 (318) | 1025 (417) | 967 (452) | 0.284 | 887 (254) | 982 (359) | 0.241 |
| Zinc (mg) | 9.44 (3.21) | 9.33 (4.31) | 9.68 (3.58) | 9.23 (2.83) | 9.82 (2.83) | 10.34 (3.73) | 0.790 | 9.57 (3.44) | 9.43 (3.26) | 0.859 |
| Iodine (µg) | 177 (79) | 169 (78) | 168 (71) | 189 (80) | 186 (89) | 166 (99) | 0.421 | 150 (70) | 180 (78) | 0.015 |
| Iron (mg) | 12.1 (3.9) | 12.9 (5.7) | 11.7 (4.3) | 11.9 (3.6) | 12.5 (4.1) | 11.6 (4.7) | 0.877 | 12.5 (3.9) | 12.1 (4.0) | 0.900 |
| Selenium (µg) | 65 (31) | 63 (35) | 65 (28) | 64 (29) | 71 (41) | 61 (39) | 0.999 | 62 (32) | 66 (32) | 0.195 |
| Potassium (mg) | 3955 (1217) | 3882 (1573) | 3897 (1131) | 3932 (1036) | 4318 (1567) | 4064 (1254) | 0.302 | 3843 (1129) | 3977 (1243) | 0.281 |
| Phosphorus (mg) | 1506 (486) | 1502 (508) | 1499 (483) | 1496 (495) | 1656 (512) | 1544 (366) | 0.501 | 1447 (368) | 1508 (488) | 0.151 |
| Niacin (mg) | 24 (9) | 22 (12) | 23 (8) | 24 (7) | 25 (11) | 25 (10) | 0.567 | 25 (8) | 24 (9) | 0.523 |
| Vit B12 (µg) | 8.19 (5.24) | 7.46 (5.84) | 8.23 (5.08) | 8.38 (4.69) | 8.28 (6.26) | 8.21 (5.22) | 0.924 | 7.00 (5.35) | 8.31 (5.27) | 0.449 |
| Vit C (mg) | 140 (74) | 150 (97) | 142 (64) | 132 (77) | 143 (88) | 130 (63) | 0.703 | 134 (88) | 142 (72) | 0.520 |
| Vit E (mg) | 12.2 (5.1) | 12.1 (4.6) | 11.2 (5.3) | 12.2 (4.7) | 12.9 (5.7) | 12.1 (6.7) | 0.059 | 10.6 (4.1) | 12.2 (5.3) | 0.047 |
| Vit B2 (mg) | 2.12 (0.75) | 2.09 (0.80) | 1.99 (0.64) | 2.15 (0.74) | 2.31 (0.86) | 2.34 (0.58) | 0.063 | 2.0 (0.62) | 2.16 (0.77) | 0.163 |
| Vit B6 (mg) | 2.37 (0.89) | 2.44 (1.11) | 2.37 (0.92) | 2.32 (0.80) | 2.46 (0.97) | 2.36 (1.02) | 0.826 | 2.35 (0.97) | 2.39 (0.88) | 0.722 |
| Vit B1 (mg) | 1.52 (0.50) | 1.47 (0.62) | 1.50 (0.51) | 1.51 (0.46) | 1.64 (0.60) | 1.47 (0.54) | 0.480 | 1.44 (0.47) | 1.56 (0.50) | 0.308 |
| Vit D2 (µg) | 3.22 (3.15) | 2.86 (3.21) | 3.27 (3.08) | 3.08 (3.07) | 3.92 (3.20) | 2.92 (2.66) | 0.984 | 2.79 (3.15) | 3.30 (3.15) | 0.187 |
| Vit A-retinol (µg) | 346 (700) | 300 (257) | 359 (779) | 333 (753) | 342 (401) | 636 (814) | 0.338 | 387 (753) | 344 (7688) | 0.589 |
| Vit A- retinol equivalents (µg) | 1264 (899) | 1257 (848) | 1259 (868) | 1266 (769) | 1242 (1053) | 1361 (936) | 0.868 | 1296 (1078) | 1259 (870) | 0.403 |
| Sodium (mg) | 2525 (1000) | 2462 (1088) | 2549 (924) | 2496 (1016) | 2680 (1003) | 2546 (1372) | 0.380 | 2463 (752) | 2545 (1020) | 0.313 |
| Magnesium (mg) | 348 (109) | 372 (134) | 343 (95) | 344 (96) | 379 (127) | 335 (95) | 0.520 | 332 (96) | 353 (110) | 0.066 |
| Chloride (mg) | 3889 (1463) | 3764 (1491) | 3876 (1341) | 3822 (1606) | 4076 (1429) | 3939 (1856) | 0.349 | 3666 (972) | 3935 (1493) | 0.218 |
| Manganese (mg) | 3.83 (1.64) | 4.08 (2.08) | 3.83 (1.67) | 3.84 (1.32) | 4.13 (1.74) | 3.23 (1.05) | 0.190 | 3.30 (1.0) | 3.97 (1.59) | 0.009 |
| Copper (mg) | 1.22 (0.56) | 1.30 (0.60) | 1.18 (0.56) | 1.21 (0.48) | 1.19 (0.57) | 1.20 (0.78) | 0.804 | 1.12 (0.57) | 1.22 (0.54) | 0.305 |
| Folate (µg) | 330 (113) | 359 (150) | 323 (111) | 328 (115) | 352 (123) | 333 (109) | 0.681 | 331 (119) | 331 (116) | 0.480 |
| Nitrogen (g) | 13.8 (5.0) | 13.1 (6.5) | 13.9 (4.9) | 13.9 (4.7) | 14.4 (5.0) | 13.8 (5.4) | 0.868 | 13.8 (5.1) | 13.8 (5.0) | 0.776 |
| Carotene (µg) | 4449 (2807) | 4785 (3029) | 4724 (2838) | 4034 (3007) | 4951 (3455) | 4692 (1788) | 0.329 | 4886 (2896) | 4410 (2819) | 0.753 |
| Food Items | All Participants n = 281 | 60–64 Years n = 39 | 65–69 Years n = 98 | 70–74 Years n = 94 | 75–79 Years n = 34 | 80–91 Years n = 16 | p-Value (Age Groups) | Low Relative Skeletal Muscle Mass n = 37 | High Relative Skeletal Muscle Mass n = 244 | p-Value (Relative Skeletal Muscle Mass Groups) |
|---|---|---|---|---|---|---|---|---|---|---|
| Cereals and its products (g) | 212 (125) | 249 (122) | 218 (134) | 205 (119) | 217 (104) | 172 (119) | 0.206 | 186 (113) | 216 (133) | 0.140 |
| Milk and milk products (g) | 416 (232) | 388 (301) | 363 (176) | 432 (231) | 465 (288) | 436 (263) | 0.087 | 347 (149) | 426 (264) | 0.035 |
| Eggs and egg dishes (g) | 22 (18)1 | 22 (15) | 22 (15) | 22 (19) | 22 (25) | 22 (20) | 0.545 | 22 (25) | 22 (15) | 0.342 |
| Fats and oils (g) | 13 (13) | 12 (12) | 13 (14) | 13 (9) | 16 (17) | 15 (12) | 0.345 | 13 (15) | 13 (12) | 0.864 |
| Fish and fish products (g) | 57 (60) | 57 (57) | 55 (57) | 68 (61) | 54 (72) | 46 (55) | 0.887 | 35 (46) | 61 (58) | 0.006 |
| Fruit (g) | 276 (199) | 269 (266) | 271 (168) | 278 (213) | 318 (209) | 208 (238) | 0.410 | 224 (199) | 279 (192) | 0.133 |
| Meat and meat products (g) | 87 (77) | 76 (111) | 85 (89) | 90 (65) | 80 (45) | 116 (67) | 0.142 | 110 (87) | 83 (74) | 0.007 |
| Nuts and seeds (g) | 4 (21) | 13 (22) | 4 (24) | 4 (13) | 4 (30) | 2 (19) | 0.283 | 2.1 (12.9) | 4.2 (21.6) | 0.005 |
| Potatoes (g) | 71 (60) | 63 (48) | 71 (48) | 71 (48) | 79 (80) | 73 (85) | 0.235 | 74.5 (49.2) | 71.4 (62.8) | 0.932 |
| Soups and sauces (g) | 55 (70) | 51 (34) | 49 (77) | 56 (77) | 75 (97) | 53 (75) | 0.304 | 62 (90) | 55 (69) | 0.785 |
| Vegetables (g) | 339 (217) | 333 (226) | 353 (219) | 318 (202) | 338 (245) | 341 (185) | 0.451 | 370 (318) | 335 (196) | 0.793 |
| Sugars; preservatives and snacks (g) | 24 (26) | 23 (29) | 22 (27) | 24 (27) | 24 (24) | 28 (46) | 0.765 | 25 (33) | 23 (24) | 0.972 |
| Outcome Variables | Unstandardized Coefficients (B) Protein Threshold | 95% C.I | p-Value | Partial Correlations |
|---|---|---|---|---|
| BMI (kg/m2) | −3.877 | (−4.933; −2.821) | <0.001 | −0.399 |
| Fat mass (kg) | −7.836 | (−9.751; −5.922) | <0.001 | −0.437 |
| Biceps brachii (cm) | −0.155 | (−0.235; −0.074) | <0.001 | −0.223 |
| HGS/Body mass (kg/kg) | 0.063 | (0.039;0.087) | <0.001 | 0.299 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Khanal, P.; He, L.; Degens, H.; Stebbings, G.K.; Onambele-Pearson, G.L.; Williams, A.G.; Thomis, M.; Morse, C.I. Dietary Protein Requirement Threshold and Micronutrients Profile in Healthy Older Women Based on Relative Skeletal Muscle Mass. Nutrients 2021, 13, 3076. https://doi.org/10.3390/nu13093076
Khanal P, He L, Degens H, Stebbings GK, Onambele-Pearson GL, Williams AG, Thomis M, Morse CI. Dietary Protein Requirement Threshold and Micronutrients Profile in Healthy Older Women Based on Relative Skeletal Muscle Mass. Nutrients. 2021; 13(9):3076. https://doi.org/10.3390/nu13093076
Chicago/Turabian StyleKhanal, Praval, Lingxiao He, Hans Degens, Georgina K. Stebbings, Gladys L. Onambele-Pearson, Alun G. Williams, Martine Thomis, and Christopher I. Morse. 2021. "Dietary Protein Requirement Threshold and Micronutrients Profile in Healthy Older Women Based on Relative Skeletal Muscle Mass" Nutrients 13, no. 9: 3076. https://doi.org/10.3390/nu13093076
APA StyleKhanal, P., He, L., Degens, H., Stebbings, G. K., Onambele-Pearson, G. L., Williams, A. G., Thomis, M., & Morse, C. I. (2021). Dietary Protein Requirement Threshold and Micronutrients Profile in Healthy Older Women Based on Relative Skeletal Muscle Mass. Nutrients, 13(9), 3076. https://doi.org/10.3390/nu13093076










