Association between Irregular Meal Timing and the Mental Health of Japanese Workers
Abstract
:1. Introduction
2. Materials and Methods
2.1. Ethical Approval
2.2. Target Population and Data Collection
2.3. Variables
2.4. Statistical Analysis
3. Results
3.1. Participants’ Characteristics
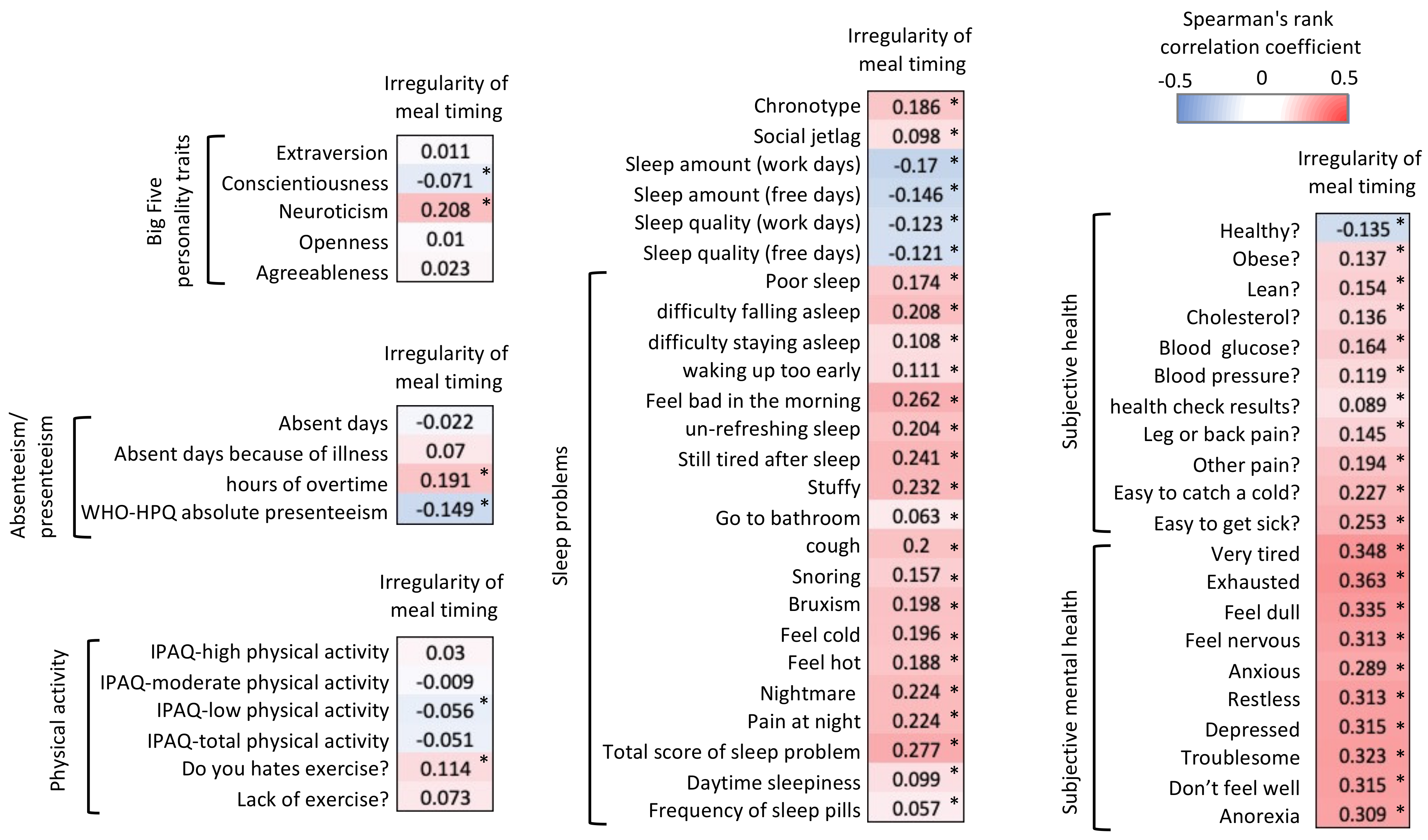
3.2. Correlation Analysis Focusing on Irregular Meal Timing
3.3. Eating Habits with Irregular Meal Timing
3.4. Logistic Regression Analysis for Subjective Health Outcomes
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed consent statement
Acknowledgments
Conflicts of Interest
References
- Imamura, K.; Kawakami, N.; Inoue, A.; Shimazu, A.; Tsutsumi, A.; Takahashi, M.; Totsuzaki, T. Work Engagement as a Predictor of Onset of Major Depressive Episode (MDE) among Workers, Independent of Psychological Distress: A 3-Year Prospective Cohort Study. PLoS ONE 2016, 11, e0148157. [Google Scholar] [CrossRef]
- Facer-Childs, E.R.; Middleton, B.; Skene, D.J.; Bagshaw, A.P. Resetting the late timing of “night owls” has a positive impact on mental health and performance. Sleep Med. 2019, 60, 236–247. [Google Scholar] [CrossRef]
- Janssens, H.; Clays, E.; de Clercq, B.; de Bacquer, D.; Casini, A.; Kittel, F.; Braeckman, L. Association between psychosocial characteristics of work and presenteeism: A cross-sectional study. Int. J. Occup. Med. Environ. Health 2016, 29, 331–344. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Howarth, A.; Quesada, J.; Silva, J.; Judycki, S.; Mills, P.R. The impact of digital health interventions on health-related outcomes in the workplace: A systematic review. Digit. Health 2018, 4, 2055207618770861. [Google Scholar] [CrossRef] [Green Version]
- Ishibashi, Y.; Shimura, A. Association between work productivity and sleep health: A cross-sectional study in Japan. Sleep Health 2020, 6, 270–276. [Google Scholar] [CrossRef] [PubMed]
- Shimura, A.; Sugiura, K.; Inoue, M.; Misaki, S.; Tanimoto, Y.; Oshima, A.; Tanaka, T.; Yokoi, K.; Inoue, T. Which sleep hygiene factors are important? comprehensive assessment of lifestyle habits and job environment on sleep among office workers. Sleep Health 2020, 6, 288–298. [Google Scholar] [CrossRef] [PubMed]
- Godos, J.; Grosso, G.; Castellano, S.; Galvano, F.; Caraci, F.; Ferri, R. Association between diet and sleep quality: A systematic review. Sleep Med. Rev. 2021, 57, 101430. [Google Scholar] [CrossRef] [PubMed]
- Muscaritoli, M. The Impact of Nutrients on Mental Health and Well-Being: Insights From the Literature. Front. Nutr. 2021, 8, 656290. [Google Scholar] [CrossRef] [PubMed]
- Martins, L.B.; Braga Tibães, J.R.; Sanches, M.; Jacka, F.; Berk, M.; Teixeira, A.L. Nutrition-based interventions for mood disorders. Expert. Rev. Neurother. 2021, 21, 303–315. [Google Scholar] [CrossRef]
- Godos, J.; Currenti, W.; Angelino, D.; Mena, P.; Castellano, S.; Caraci, F.; Galvano, F.; Del Rio, D.; Ferri, R.; Grosso, G. Diet and Mental Health: Review of the Recent Updates on Molecular Mechanisms. Antioxidants 2020, 9, 346. [Google Scholar] [CrossRef] [Green Version]
- Chang, Z.S.; Boolani, A.; Conroy, D.A.; Dunietz, T.; Jansen, E.C. Skipping breakfast and mood: The role of sleep. Nutr. Health 2021, 1-7, 260106020984861. [Google Scholar] [CrossRef]
- Charlot, A.; Hutt, F.; Sabatier, E.; Zoll, J. Beneficial Effects of Early Time-Restricted Feeding on Metabolic Diseases: Importance of Aligning Food Habits with the Circadian Clock. Nutrients 2021, 13, 1405. [Google Scholar] [CrossRef]
- Nolan, L.J.; Geliebter, A. Night eating is associated with emotional and external eating in college students. Eat Behav. 2012, 13, 202–206. [Google Scholar] [CrossRef] [Green Version]
- Haraguchi, A.; Fukuzawa, M.; Iwami, S.; Nishimura, Y.; Motohashi, H.; Tahara, Y.; Shibata, S. Night eating model shows time-specific depression-like behavior in the forced swimming test. Sci. Rep. 2018, 8, 1081. [Google Scholar] [CrossRef] [Green Version]
- Phillips, A.J.K.; Clerx, W.M.; O’Brien, C.S.; Sano, A.; Barger, L.K.; Picard, R.W.; Lockley, S.W.; Klerman, E.B.; Czeisler, C.A. Irregular sleep/wake patterns are associated with poorer academic performance and delayed circadian and sleep/wake timing. Sci. Rep. 2017, 7, 3216. [Google Scholar] [CrossRef] [PubMed]
- Tahara, Y.; Shibata, S. Circadian rhythms of liver physiology and disease: Experimental and clinical evidence. Nat. Rev. Gastroenterol. Hepatol. 2016, 13, 217–226. [Google Scholar] [CrossRef]
- Walker, W.H., 2nd; Walton, J.C.; DeVries, A.C.; Nelson, R.J. Circadian rhythm disruption and mental health. Transl. Psychiatry 2020, 10, 28. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tahara, Y.; Aoyama, S.; Shibata, S. The mammalian circadian clock and its entrainment by stress and exercise. J. Physiol. Sci. 2017, 67, 1–10. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tahara, Y.; Shibata, S. Chronobiology and nutrition. Neuroscience 2013, 253, 78–88. [Google Scholar] [CrossRef] [PubMed]
- Mathew, G.M.; Hale, L.; Chang, A.M. Social jetlag, eating behaviours and BMI among adolescents in the USA. Br. J. Nutr. 2020, 124, 979–987. [Google Scholar] [CrossRef] [PubMed]
- Chaix, A.; Manoogian, E.N.C.; Melkani, G.C.; Panda, S. Time-Restricted Eating to Prevent and Manage Chronic Metabolic Diseases. Annu. Rev. Nutr. 2019, 39, 291–315. [Google Scholar] [CrossRef]
- Currenti, W.; Godos, J.; Castellano, S.; Caruso, G.; Ferri, R.; Caraci, F.; Grosso, G.; Galvano, F. Association between Time Restricted Feeding and Cognitive Status in Older Italian Adults. Nutrients 2021, 13, 191. [Google Scholar] [CrossRef] [PubMed]
- Diener, E.; Emmons, R.A.; Larsen, R.J.; Griffin, S. The Satisfaction With Life Scale. J. Personal. Assess. 1985, 49, 71–75. [Google Scholar] [CrossRef]
- Rothmann, S.; Coetzer, E.P. The big five personality dimensions and job performance. SA J. Ind. Psychol. 2003, 29, 68–74. [Google Scholar] [CrossRef] [Green Version]
- Craig, C.L.; Marshall, A.L.; Sjöström, M.; Bauman, A.E.; Booth, M.L.; Ainsworth, B.E.; Pratt, M.; Ekelund, U.; Yngve, A.; Sallis, J.F.; et al. International physical activity questionnaire: 12-country reliability and validity. Med. Sci. Sports Exerc. 2003, 35, 1381–1395. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kessler, R.C.; Barber, C.; Beck, A.; Berglund, P.; Cleary, P.D.; McKenas, D.; Pronk, N.; Simon, G.; Stang, P.; Ustun, T.B.; et al. The World Health Organization Health and Work Performance Questionnaire (HPQ). J. Occup. Environ. Med. 2003, 45, 156–174. [Google Scholar] [CrossRef]
- Chimed-Ochir, O.; Nagata, T.; Nagata, M.; Kajiki, S.; Mori, K.; Fujino, Y. Potential Work Time Lost Due to Sickness Absence and Presence Among Japanese Workers. J. Occup. Environ. Med. 2019, 61, 682–688. [Google Scholar] [CrossRef] [PubMed]
- Kitamura, S.; Hida, A.; Aritake, S.; Higuchi, S.; Enomoto, M.; Kato, M.; Vetter, C.; Roenneberg, T.; Mishima, K. Validity of the Japanese version of the Munich ChronoType Questionnaire. Chronobiol. Int. 2014, 31, 845–850. [Google Scholar] [CrossRef] [PubMed]
- Doi, Y.; Minowa, M.; Uchiyama, M.; Okawa, M.; Kim, K.; Shibui, K.; Kamei, Y. Psychometric assessment of subjective sleep quality using the Japanese version of the Pittsburgh Sleep Quality Index (PSQI-J) in psychiatric disordered and control subjects. Psychiatry Res. 2000, 97, 165–172. [Google Scholar] [CrossRef]
- Kawakami, N.; Tsutsumi, A. The Stress Check Program: A new national policy for monitoring and screening psychosocial stress in the workplace in Japan. J. Occup. Health 2016, 58, 1–6. [Google Scholar] [CrossRef] [Green Version]
- Moriguchi, J.; Sakuragi, S.; Kitagawa, Y.; Matsui, M.; Mori, Y.; Ohashi, F.; Ikeda, M. Comparative study on the activities of part-time occupational physicians in Japan between 2008 and 2016: Effects of the stress-check program. Ind. Health 2020, 58, 287–301. [Google Scholar] [CrossRef] [Green Version]
- Hayashida, T.; Shimura, A.; Higashiyama, M.; Fujimura, Y.; Ono, K.; Inoue, T. Psychosomatic Stress Responses and Sleep Disturbance Mediate the Effects of Irregular Mealtimes on Presenteeism. Neuropsychiatr. Dis. Treat. 2021, 17, 315–321. [Google Scholar] [CrossRef]
- Currenti, W.; Godos, J.; Castellano, S.; Mogavero, M.P.; Ferri, R.; Caraci, F.; Grosso, G.; Galvano, F. Time restricted feeding and mental health: A review of possible mechanisms on affective and cognitive disorders. Int. J. Food Sci. Nutr. 2020, 1–11. [Google Scholar] [CrossRef]
- Shimizu, H.; Hanzawa, F.; Kim, D.; Sun, S.; Laurent, T.; Umeki, M.; Ikeda, S.; Mochizuki, S.; Oda, H. Delayed first active-phase meal, a breakfast-skipping model, led to increased body weight and shifted the circadian oscillation of the hepatic clock and lipid metabolism-related genes in rats fed a high-fat diet. PLoS ONE 2018, 13, e0206669. [Google Scholar] [CrossRef]
- Ogata, H.; Hatamoto, Y.; Goto, Y.; Tajiri, E.; Yoshimura, E.; Kiyono, K.; Uehara, Y.; Kawanaka, K.; Omi, N.; Tanaka, H. Association between breakfast skipping and postprandial hyperglycaemia after lunch in healthy young individuals. Br. J. Nutr. 2019, 122, 431–440. [Google Scholar] [CrossRef]
- Koch, C.E.; Begemann, K.; Kiehn, J.T.; Griewahn, L.; Mauer, J.; Hess, M.E.; Moser, A.; Schmid, S.M.; Brüning, J.C.; Oster, H. Circadian regulation of hedonic appetite in mice by clocks in dopaminergic neurons of the VTA. Nat. Commun. 2020, 11, 3071. [Google Scholar] [CrossRef] [PubMed]
- Zerón-Rugerio, M.F.; Hernáez, Á.; Porras-Loaiza, A.P.; Cambras, T.; Izquierdo-Pulido, M. Eating Jet Lag: A Marker of the Variability in Meal Timing and Its Association with Body Mass Index. Nutrients 2019, 11, 2980. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Garaulet, M.; Gómez-Abellán, P.; Alburquerque-Béjar, J.J.; Lee, Y.C.; Ordovás, J.M.; Scheer, F.A. Timing of food intake predicts weight loss effectiveness. Int. J. Obes. 2013, 37, 604–611. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Almoosawi, S.; Vingeliene, S.; Gachon, F.; Voortman, T.; Palla, L.; Johnston, J.D.; Van Dam, R.M.; Darimont, C.; Karagounis, L.G. Chronotype: Implications for Epidemiologic Studies on Chrono-Nutrition and Cardiometabolic Health. Adv. Nutr. 2019, 10, 30–42. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Muscogiuri, G.; Barrea, L.; Aprano, S.; Framondi, L.; Di Matteo, R.; Laudisio, D.; Pugliese, G.; Savastano, S.; Colao, A. Chronotype and adherence to the mediterranean diet in obesity: Results from the opera prevention project. Nutrients 2020, 12, 1354. [Google Scholar] [CrossRef] [PubMed]
- Barrea, L.; Frias-Toral, E.; Aprano, S.; Castellucci, B.; Pugliese, G.; Rodriguez-Veintimilla, D.; Vitale, G.; Gentilini, D.; Colao, A.; Savastano, S.; et al. The clock diet: A practical nutritional guide to manage obesity through chrononutrition. Minerva Med. 2021. [Google Scholar]
- St-Onge, M.P.; St-Pizinger, T.; Kovtun, K.; RoyChoudhury, A. Sleep and meal timing influence food intake and its hormonal regulation in healthy adults with overweight/obesity. Eur. J. Clin. Nutr. 2019, 72 (Suppl. 1), 76–82. [Google Scholar] [CrossRef]
- Muscogiuri, G.; Barrea, L.; Aprano, S.; Framondi, L.; Di Matteo, R.; Laudisio, D.; Pugliese, G.; Savastano, S.; Colao, A. Sleep quality in obesity: Does adherence to the mediterranean diet matter? Nutrients 2020, 12, 1364. [Google Scholar] [CrossRef] [PubMed]
- Wee, L.H.; Yeap, L.L.L.; Chan, C.M.H.; Wong, J.E.; Jamil, N.A.; Swarna Nantha, Y.; Siau, C.S. Anteceding factors predicting absenteeism and presenteeism in urban area in Malaysia. BMC Public Health 2019, 19, 540. [Google Scholar] [CrossRef] [Green Version]
- St-Onge, M.P.; Ard, J.; Baskin, M.L.; Chiuve, S.E.; Johnson, H.M.; Kris-Etherton, P.; Varady, K. Meal Timing and Frequency: Implications for Cardiovascular Disease Prevention: A Scientific Statement From the American Heart Association. Circulation 2017, 135, e96–e121. [Google Scholar] [CrossRef] [PubMed]
- Yoshizaki, T.; Kawano, Y.; Noguchi, O.; Onishi, J.; Teramoto, R.; Sunami, A.; Yokoyama, Y.; Tada, Y.; Hida, A.; Togo, F. Association of eating behaviours with diurnal preference and rotating shift work in Japanese female nurses: A cross-sectional study. BMJ Open 2016, 6, e011987. [Google Scholar] [CrossRef] [PubMed]
- Yoshizaki, T.; Komatsu, T.; Tada, Y.; Hida, A.; Kawano, Y.; Togo, F. Association of habitual dietary intake with morningness-eveningness and rotating shift work in Japanese female nurses. Chronobiol. Int. 2018, 35, 392–404. [Google Scholar] [CrossRef]
- Mota, M.C.; Silva, C.M.; Balieiro, L.C.T.; Gonçalves, B.F.; Fahmy, W.M.; Crispim, C.A. Association between social jetlag food consumption and meal times in patients with obesity-related chronic diseases. PLoS ONE 2019, 14, e0212126. [Google Scholar] [CrossRef] [Green Version]
- Horne, R.; Foster, J.A. Metabolic and Microbiota Measures as Peripheral Biomarkers in Major Depressive Disorder. Front Psychiatry 2018, 9, 513. [Google Scholar] [CrossRef] [Green Version]
- Van Der Feltz-Cornelis, C.M.; Varley, D.; Allgar, V.L.; de Beurs, E. Workplace Stress, Presenteeism, Absenteeism, and Resilience Amongst University Staff and Students in the COVID-19 Lockdown. Front. Psychiatry 2020, 11, 588803. [Google Scholar] [CrossRef]
- Tahara, Y.; Shinto, T.; Inoue, K.; Roshanmehr, F.; Ito, A.; Michie, M.; Shibata, S. Changes in sleep phase and body weight of mobile health App users during COVID-19 mild lockdown in Japan. Int. J. Obes. 2021, 1–4. [Google Scholar] [CrossRef]

| Regular Meal Timing | Irregular Meal Timing | p Value | |||
|---|---|---|---|---|---|
| Category | All (n = 4490) | (Score: 0–4; n = 3410) | (Score: 5–7; n = 1080) | Regular vs. Irregular | |
| Sex | male % (n) | 73.3 (3291) | 73.5 (2507) | 72.5 (783) | 0.497 |
| female % (n) | 26.7 (1199) | 26.5 (904) | 27.5 (297) | ||
| Age | (years) | 47.41 ± 0.17 | 48.06 ± 0.20 | 45.36 ± 0.34 | < 0.001 |
| BMI | (kg/m2) | 22.69 ± 0.05 | 22.64 ± 0.06 | 22.83 ± 0.12 | 0.138 |
| Night shift worker | % (n) | 15.5 (695) | 11.4 (388) | 28.4 (307) | < 0.001 |
| SWLS | (score) | 17.24 ± 0.09 | 17.52 ± 0.10 | 16.35 ± 0.20 | < 0.001 |
| All Samples (n = 4490) | Randomly Selected Samples (n = 1405) | |||||||
|---|---|---|---|---|---|---|---|---|
| Objective Variable | Irregularity of Meal Timing | Irregularity of Meal Timing | ||||||
| B | p | OR | 95% CI | B | p | OR | 95% CI | |
| Subjective health | ||||||||
| Healthy? | −0.111 | p < 0.001 | 0.895 | 0.856, 0.936 | −0.107 | p < 0.01 | 0.898 | 0.828, 0.974 |
| Worried about being obese? | 0.079 | p < 0.01 | 1.082 | 1.032, 1.134 | 0.094 | p < 0.05 | 1.098 | 1.007, 1.197 |
| Worried about being lean? | 0.163 | p < 0.001 | 1.177 | 1.101, 1.258 | 0.111 | 0.08 | 1.117 | 0.987, 1.264 |
| Worried about your blood cholesterol level? | 0.063 | p < 0.01 | 1.065 | 1.018, 1.113 | 0.021 | 0.618 | 1.021 | 0.941, 1.108 |
| Worried about your blood glucose level? | 0.072 | p < 0.01 | 1.074 | 1.022, 1.129 | 0.07 | 0.136 | 1.072 | 0.978, 1.175 |
| Worried about your blood pressure level? | 0.048 | p < 0.05 | 1.049 | 1.000, 1.101 | 0.048 | 0.284 | 1.049 | 0.961, 1.146 |
| Worried about your health check results? | 0.022 | 0.117 | 1.034 | 0.992, 1.079 | −0.039 | 0.33 | 0.962 | 0.889, 1.04 |
| Having pain in your leg or back? | 0.039 | 0.075 | 1.04 | 0.996, 1.086 | 0.014 | 0.73 | 1.014 | 0.937, 1.098 |
| Having pain in your other place? | 0.109 | p < 0.001 | 1.115 | 1.068, 1.164 | 0.072 | 0.078 | 1.074 | 0.992, 1.163 |
| Easy to catch a cold? | 0.14 | p < 0.001 | 1.15 | 1.085, 1.218 | 0.114 | p < 0.05 | 1.121 | 1.001, 1.255 |
| Easy to get sick? | 0.171 | p < 0.001 | 1.187 | 1.111, 1.268 | 0.111 | 0.091 | 1.117 | 0.983, 1.271 |
| Subjective mental health | ||||||||
| Very tired | 0.232 | p < 0.001 | 1.262 | 1.206, 1.320 | 0.215 | p < 0.001 | 1.239 | 1.142, 1.346 |
| Exhausted | 0.269 | p < 0.001 | 1.309 | 1.246, 1.375 | 0.304 | p < 0.001 | 1.355 | 1.236, 1.485 |
| Feel dull | 0.219 | p < 0.001 | 1.245 | 1.187, 1.305 | 0.246 | p < 0.001 | 1.279 | 1.172, 1.395 |
| Feel nervous | 0.214 | p < 0.001 | 1.239 | 1.182, 1.298 | 0.311 | p < 0.01 | 1.365 | 1.110, 1.679 |
| Anxious | 0.152 | p < 0.001 | 1.164 | 1.111, 1.220 | 0.243 | p < 0.05 | 1.275 | 1.044, 1.557 |
| Restless | 0.185 | p < 0.001 | 1.203 | 1.142, 1.268 | 0.208 | 0.054 | 1.231 | 0.996, 1.521 |
| Depressed | 0.187 | p < 0.001 | 1.205 | 1.147, 1.267 | 0.283 | p < 0.01 | 1.327 | 1.076, 1.635 |
| Troublesome | 0.201 | p < 0.001 | 1.223 | 1.165, 1.283 | 0.526 | p < 0.001 | 1.691 | 1.345, 2.128 |
| Don’t feel well | 0.205 | p < 0.001 | 1.227 | 1.169, 1.289 | 0.355 | p < 0.01 | 1.426 | 1.158, 1.757 |
| Anorexia | 0.36 | p < 0.001 | 1.433 | 1.319, 1.557 | 0.33 | p < 0.05 | 1.391 | 1.006, 1.925 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tahara, Y.; Makino, S.; Suiko, T.; Nagamori, Y.; Iwai, T.; Aono, M.; Shibata, S. Association between Irregular Meal Timing and the Mental Health of Japanese Workers. Nutrients 2021, 13, 2775. https://doi.org/10.3390/nu13082775
Tahara Y, Makino S, Suiko T, Nagamori Y, Iwai T, Aono M, Shibata S. Association between Irregular Meal Timing and the Mental Health of Japanese Workers. Nutrients. 2021; 13(8):2775. https://doi.org/10.3390/nu13082775
Chicago/Turabian StyleTahara, Yu, Saneyuki Makino, Takahiko Suiko, Yuki Nagamori, Takao Iwai, Megumi Aono, and Shigenobu Shibata. 2021. "Association between Irregular Meal Timing and the Mental Health of Japanese Workers" Nutrients 13, no. 8: 2775. https://doi.org/10.3390/nu13082775
APA StyleTahara, Y., Makino, S., Suiko, T., Nagamori, Y., Iwai, T., Aono, M., & Shibata, S. (2021). Association between Irregular Meal Timing and the Mental Health of Japanese Workers. Nutrients, 13(8), 2775. https://doi.org/10.3390/nu13082775






