Gastrointestinal Digestion Model Assessment of Peptide Diversity and Microbial Fermentation Products of Collagen Hydrolysates
Abstract
1. Introduction
2. Materials and Methods
2.1. Upper Intestinal in Vitro Digestion of Collagen Hydrolysates
2.2. Peptide Profile
2.2.1. Matrix Assisted Laser Desorption/Ionization (MALDI)
2.2.2. Proteomic Analysis
2.3. Dynamic In Vitro Gastrointestinal Digestion of Collagen Hydrolysates
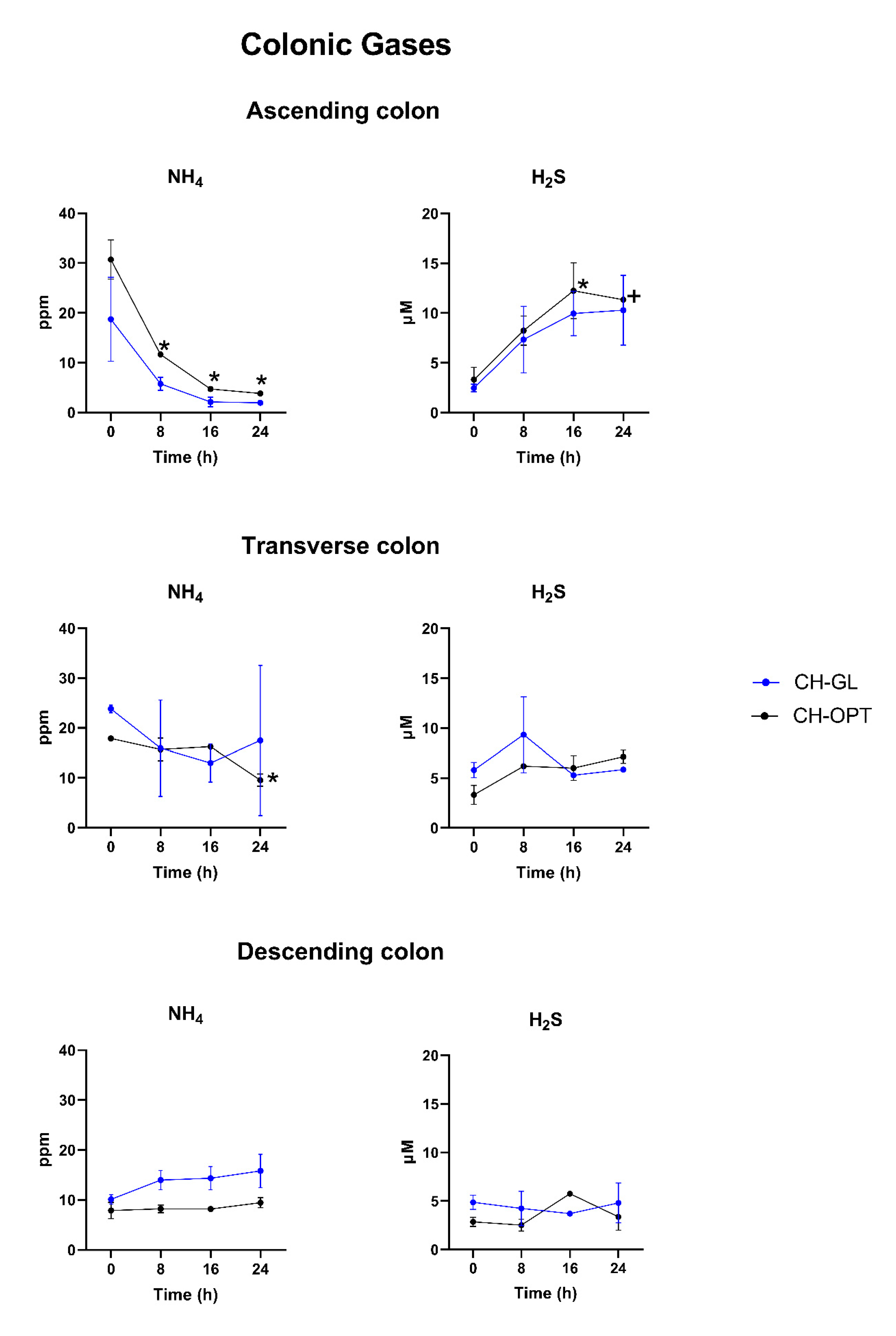
2.4. Colonic Gases
2.4.1. Ammonium (NH4) Content
2.4.2. Hydrogen Sulfide (H2S) Content
2.5. Short- and Branched-Chain Fatty Acids
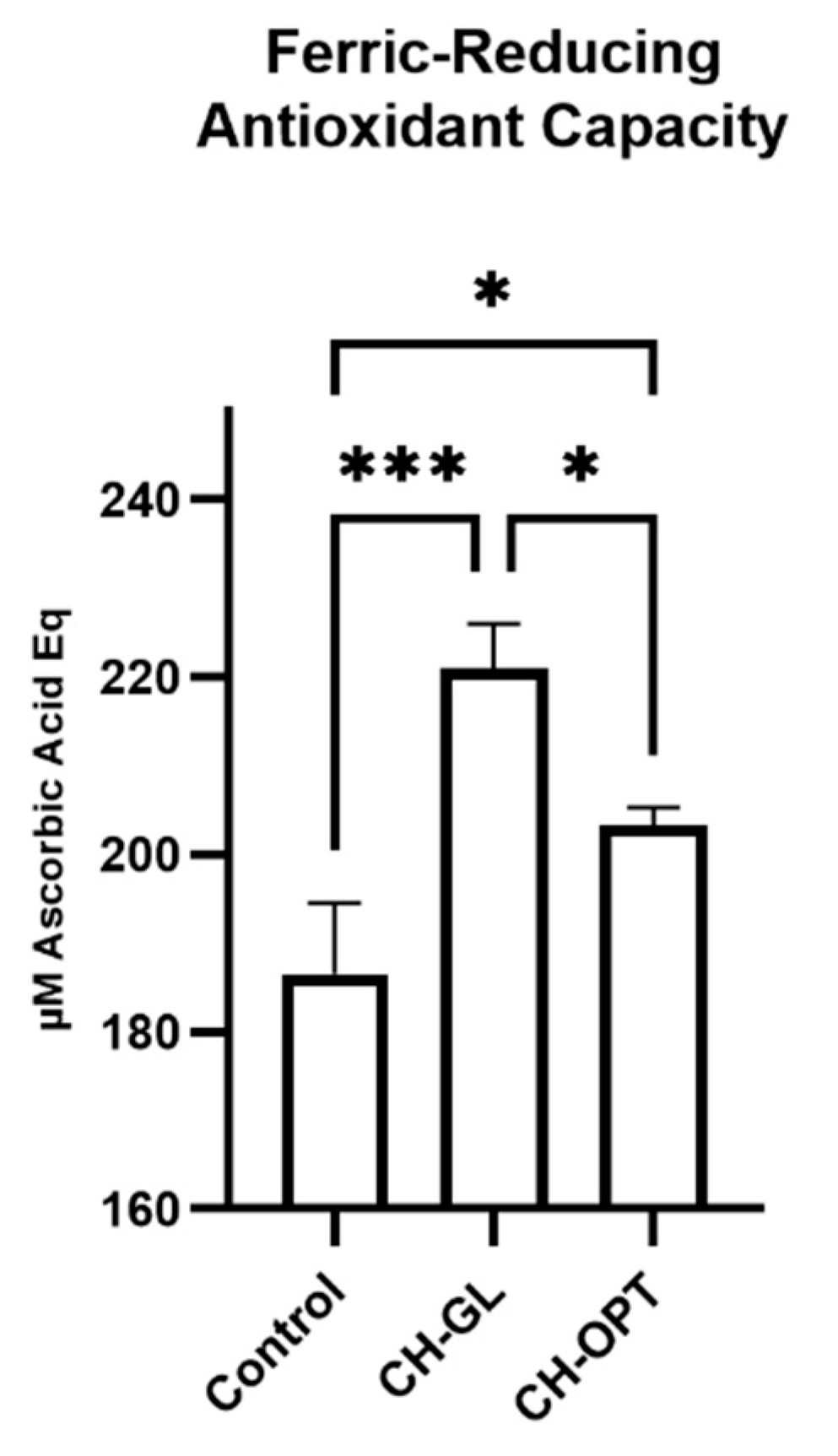
2.6. Antioxidant Capacity
2.6.1. Ferric Reducing Ability of Plasma (FRAP) Assay
2.6.2. DPPH (2,2-Diphenyl-1-picrylhydrazyl) Assay
2.7. Statistical Analysis
3. Results
3.1. Peptide Profile
3.2. Colonic Gases
3.3. SCFAs and BCFAs
3.4. Antioxidant Capacity
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Lane, N.; Shidara, K.; Wise, B. Osteoarthritis year in review 2016: Clinical. Osteoarthr. Cartil. 2017, 25, 209–215. [Google Scholar] [CrossRef]
- Li, M.; Xiao, R.; Li, J.; Zhu, Q. Regenerative approaches for cartilage repair in the treatment of osteoarthritis. Osteoarthr. Cartil. 2017, 25, 1577–1587. [Google Scholar] [CrossRef]
- Bello, A.E.; Oesser, S. Collagen hydrolysate for the treatment of osteoarthritis and other joint disorders:a review of the literature. Curr. Med Res. Opin. 2006, 22, 2221–2232. [Google Scholar] [CrossRef] [PubMed]
- Schott, E.M.; Farnsworth, C.W.; Grier, A.; Lillis, J.A.; Soniwala, S.; Dadourian, G.H.; Bell, R.D.; Doolittle, M.L.; Villani, D.A.; Awad, H.; et al. Targeting the gut microbiome to treat the osteoarthritis of obesity. JCI Insight 2018, 3, 95997. [Google Scholar] [CrossRef] [PubMed]
- Veronese, N.; Cooper, C.; Reginster, J.-Y.; Hochberg, M.; Branco, J.; Bruyère, O.; Chapurlat, R.; Al-Daghri, N.; Dennison, E.; Herrero-Beaumont, G.; et al. Type 2 diabetes mellitus and osteoarthritis. Semin. Arthritis Rheum. 2019, 49, 9–19. [Google Scholar] [CrossRef]
- Eymard, F.; Parsons, C.; Edwards, M.; Petit-Dop, F.; Reginster, J.-Y.; Bruyere, O.; Richette, P.; Cooper, C.; Chevalier, X. Diabetes is a risk factor for knee osteoarthritis progression. Osteoarthr. Cartil. 2015, 23, 851–859. [Google Scholar] [CrossRef] [PubMed]
- Singh, G.; Miller, J.D.; Lee, F.H.; Pettitt, D.; Russell, M.W. Prevalence of cardiovascular disease risk factors among US adults with self-reported osteoarthritis: Data from the Third National Health and Nutrition Examination Survey. Am. J. Manag. Care 2002, 8, 383–391. [Google Scholar]
- Baudart, P.; Louati, K.; Marcelli, C.; Berenbaum, F.; Sellam, J. Association between osteoarthritis and dyslipidaemia: A systematic literature review and meta-analysis. RMD Open 2017, 3, e000442. [Google Scholar] [CrossRef]
- Chun, J.-S.; Collins, K.; Rockel, J.; Iijima, H.; Werdyani, S.; Wang, F.-S.; Batushansky, A. Concurrent session 1: Metabolic osteoarthritis. In Proceedings of the OARSI Connect ’21 Virtual World Congress on Osteoarthritis, Virtual, NJ, USA, 29 April–1 May 2021. [Google Scholar]
- Sellam, J.; Berenbaum, F. Is osteoarthritis a metabolic disease? Jt. Bone Spine 2013, 80, 568–573. [Google Scholar] [CrossRef]
- Kluzek, S.; Newton, J.L.; Arden, N.K. Is osteoarthritis a metabolic disorder? Br. Med. Bull. 2015, 115, 111–121. [Google Scholar] [CrossRef]
- Bernado, M.L.R.; Azarcon, A.C., Jr. A randomized control trial on the effects of oral collagen treatment on the medial knee joint space and functional outcome among veterans medical center patients diagnosed with osteoarthritis of the knee. Philipp. Acad. Rehabil. Med. Process. 2012, 4, 1–8. [Google Scholar]
- Bruyère, O.; Zegels, B.; Leonori, L.; Rabenda, V.; Janssen, A.; Bourges, C.; Reginster, J.-Y. Effect of collagen hydrolysate in articular pain: A 6-month randomized, double-blind, placebo controlled study. Complement. Ther. Med. 2012, 20, 124–130. [Google Scholar] [CrossRef]
- Kumar, S.; Sugihara, F.; Suzuki, K.; Inoue, N.; Venkateswarathirukumara, S. A double-blind, placebo-controlled, randomised, clinical study on the effectiveness of collagen peptide on osteoarthritis. J. Sci. Food Agric. 2014, 95, 702–707. [Google Scholar] [CrossRef] [PubMed]
- Zdzieblik, D.; Oesser, S.; Baumstark, M.W.; Gollhofer, A.; König, D. Collagen peptide supplementation in combination with resistance training improves body composition and increases muscle strength in elderly sarcopenic men: A randomised controlled trial. Br. J. Nutr. 2015, 114, 1237–1245. [Google Scholar] [CrossRef]
- Zdzieblik, D.; Oesser, S.; Gollhofer, A.; König, D. Improvement of activity-related knee joint discomfort following supplementation of specific collagen peptides. Appl. Physiol. Nutr. Metab. 2017, 42, 588–595. [Google Scholar] [CrossRef]
- Benito-Ruiz, P.; Camacho-Zambrano, M.; Carrillo-Arcentales, J.; Mestanza-Peralta, M.; Vallejo-Flores, C.; Vargas-López, S.; Villacís-Tamayo, R.; Zurita-Gavilanes, L. A randomized controlled trial on the efficacy and safety of a food ingredient, collagen hydrolysate, for improving joint comfort. Int. J. Food Sci. Nutr. 2009, 60, 99–113. [Google Scholar] [CrossRef]
- Feliciano, D.D.S.; Gonzalex-Suarez, C.B.; Bernardo-Bueno, M.M.; Malvar, A.K.G.; Cua, R.C.A.; Tan-Sales, B.G.K.; Aycardo, S.M.O.; Tan-Ong, M.; Chan, R.; Reyes, F.D.L. Effect of collagen hydrolysate as adjuvant treatment to exercise for knee osteoarthiritis. Philipp. Acad. Rehabil. Med. 2017, 9, 4–15. [Google Scholar]
- Skov, K.; Oxfeldt, M.; Thøgersen, R.; Hansen, M.; Bertram, H.C. Enzymatic Hydrolysis of a Collagen Hydrolysate Enhances Postprandial Absorption Rate-A Randomized Controlled Trial. Nutrients 2019, 11, 1064. [Google Scholar] [CrossRef] [PubMed]
- Aleman, A.; Gómez-Guillén, M.C.; Montero, P. Identification of ace-inhibitory peptides from squid skin collagen after in vitro gastrointestinal digestion. Food Res. Int. 2013, 54, 790–795. [Google Scholar] [CrossRef]
- Guo, L.; Harnedy, P.A.; Zhang, L.; Li, B.; Zhang, Z.; Hou, H.; Zhao, X.; Fitzgerald, R.J. In vitroassessment of the multifunctional bioactive potential of Alaska pollock skin collagen following simulated gastrointestinal digestion. J. Sci. Food Agric. 2015, 95, 1514–1520. [Google Scholar] [CrossRef] [PubMed]
- Fu, Y.; Therkildsen, M.; Aluko, R.E.; Lametsch, R. Exploration of collagen recovered from animal by-products as a precursor of bioactive peptides: Successes and challenges. Crit. Rev. Food Sci. Nutr. 2018, 59, 2011–2027. [Google Scholar] [CrossRef]
- Di Bernardini, R.; Harnedy, P.; Bolton, D.; Kerry, J.; O’Neill, E.; Mullen, A.M.; Hayes, M. Antioxidant and antimicrobial peptidic hydrolysates from muscle protein sources and by-products. Food Chem. 2011, 124, 1296–1307. [Google Scholar] [CrossRef]
- Nakatani, S.; Mano, H.; Sampei, C.; Shimizu, J.; Wada, M. Chondroprotective effect of the bioactive peptide prolyl-hydroxyproline in mouse articular cartilage in vitro and in vivo. Osteoarthr. Cartil. 2009, 17, 1620–1627. [Google Scholar] [CrossRef]
- Kouguchi, T.; Ito, A.; Iwai, K.; Shimizu, M.; Takahata, Y.; Suzuki, T.; Morimatsu, F.; Tanabe, S. Chicken Collagen Hydrolysate-derived Peptides Inhibit Tumor Necrosis Factor-α-induced Inflammatory Response in Endothelial Cells. Food Sci. Technol. Res. 2012, 18, 667–671. [Google Scholar] [CrossRef]
- Ohara, H.; Ichikawa, S.; Matsumoto, H.; Akiyama, M.; Fujimoto, N.; Kobayashi, T.; Tajima, S. Collagen-derived dipeptide, proline-hydroxyproline, stimulates cell proliferation and hyaluronic acid synthesis in cultured human dermal fibroblasts. J. Dermatol. 2010, 37, 330–338. [Google Scholar] [CrossRef] [PubMed]
- Hatanaka, T.; Kawakami, K.; Uraji, M. Inhibitory effect of collagen-derived tripeptides on dipeptidylpeptidase-IV activity. J. Enzym. Inhib. Med. Chem. 2014, 29, 823–828. [Google Scholar] [CrossRef]
- Knight, C.; Morton, L.F.; Onley, D.J.; Peachey, A.R.; Ichinohe, T.; Okuma, M.; Farndale, R.W.; Barnes, M.J. Collagen-platelet interaction: Gly-Pro-Hyp is uniquely specific for platelet Gp VI and mediates platelet activation by collagen. Cardiovasc. Res. 1999, 41, 450–457. [Google Scholar] [CrossRef]
- Valko, M.; Leibfritz, D.; Moncol, J.; Cronin, M.T.D.; Mazur, M.; Telser, J. Free radicals and antioxidants in normal physiological functions and human disease. Int. J. Biochem. Cell Biol. 2007, 39, 44–84. [Google Scholar] [CrossRef] [PubMed]
- Finkel, T.; Holbrook, N.J. Oxidants, oxidative stress and the biology of ageing. Nature 2000, 408, 239–247. [Google Scholar] [CrossRef]
- Ao, J.; Li, B. Amino acid composition and antioxidant activities of hydrolysates and peptide fractions from porcine collagen. Food Sci. Technol. Int. 2012, 18, 425–434. [Google Scholar] [CrossRef]
- Sun, L.; Chang, W.; Ma, Q.; Zhuang, Y. Purification of Antioxidant Peptides by High Resolution Mass Spectrometry from Simulated Gastrointestinal Digestion Hydrolysates of Alaska Pollock (Theragra chalcogramma) Skin Collagen. Mar. Drugs 2016, 14, 186. [Google Scholar] [CrossRef]
- Arulselvan, P.; Fard, M.T.; Tan, W.S.; Gothai, S.; Fakurazi, S.; Norhaizan, M.E.; Kumar, S.S. Role of Antioxidants and Natural Products in Inflammation. Oxidative Med. Cell. Longev. 2016, 2016, 5276130. [Google Scholar] [CrossRef]
- Bianchi, M.A.; Scazzina, F.; Del Rio, D.; Valtueña, S.; Pellegrini, N.; Franzini, L.; Callegari, M.L.; Pellacani, C.; Buschini, A.; Zavaroni, I.; et al. Ability of a high-total antioxidant capacity diet to increase stool weight and bowel antioxidant status in human subjects. Br. J. Nutr. 2010, 104, 1500–1507. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Amigo, L.; Hernández-Ledesma, B. Current evidence on the bioavailability of food bioactive peptides. Molecules 2020, 25, 4479. [Google Scholar] [CrossRef] [PubMed]
- Mora, L.; Bolumar, T.; Heres, A.; Toldrá, F. Effect of cooking and simulated gastrointestinal digestion on the activity of generated bioactive peptides in aged beef meat. Food Funct. 2017, 8, 4347–4355. [Google Scholar] [CrossRef]
- Roberfroid, M.; Gibson, G.R.; Hoyles, L.; McCartney, A.L.; Rastall, R.; Rowland, I.; Wolvers, D.; Watzl, B.; Szajewska, H.; Stahl, B.; et al. Prebiotic effects: Metabolic and health benefits. Br. J. Nutr. 2010, 104, S1–S63. [Google Scholar] [CrossRef] [PubMed]
- Dorożyńska, I.; Majewska-Szczepanik, M.; Marcińska, K.; Szczepanik, M. Partial depletion of natural gut flora by antibiotic aggravates collagen induced arthritis (CIA) in mice. Pharmacol. Rep. 2014, 66, 250–255. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.; Zeng, B.; Zhang, J.; Li, W.; Mou, F.; Wang, H.; Zou, Q.; Zhong, B.; Wu, L.; Wei, H.; et al. Role of the Gut Microbiome in Modulating Arthritis Progression in Mice. Sci. Rep. 2016, 6, 30594. [Google Scholar] [CrossRef]
- Rowland, I.; Gibson, G.; Heinken, A.; Scott, K.; Swann, J.; Thiele, I.; Tuohy, K. Gut microbiota functions: Metabolism of nutrients and other food components. Eur. J. Nutr. 2018, 57, 1–24. [Google Scholar] [CrossRef]
- Peng, M.; Biswas, D. Short chain and polyunsaturated fatty acids in host gut health and foodborne bacterial pathogen inhibition. Crit. Rev. Food Sci. Nutr. 2016, 57, 3987–4002. [Google Scholar] [CrossRef]
- Ashaolu, T.J.; Ashaolu, J.O. Prebiotic peptides, their formation, fermentation in the gut, and health implications. Biotechnol. Prog. 2021, e3142. [Google Scholar] [CrossRef]
- Diether, N.E.; Willing, B.P. Microbial Fermentation of Dietary Protein: An Important Factor in Diet–Microbe–Host Interaction. Microorganisms. 2019, 7, 19. [Google Scholar] [CrossRef]
- Sirico, F.; Miressi, S.; Castaldo, C.; Spera, R.; Montagnani, S.; Di Meglio, F.; Nurzynska, D. Habits and beliefs related to food supplements: Results of a survey among Italian students of different education fields and levels. PLoS ONE 2018, 13, e0191424. [Google Scholar] [CrossRef]
- Dickinson, A.; Mackay, D.; Wong, A. Consumer attitudes about the role of multivitamins and other dietary supplements: Report of a survey. Nutr. J. 2015, 14, 66. [Google Scholar] [CrossRef] [PubMed]
- Nyangale, E.P.; Mottram, D.S.; Gibson, G.R. Gut Microbial Activity, Implications for Health and Disease: The Potential Role of Metabolite Analysis. J. Proteome Res. 2012, 11, 5573–5585. [Google Scholar] [CrossRef]
- Rahim, M.B.H.A.; Chilloux, J.; Gili, L.M.; Neves, A.L.; Myridakis, A.; Gooderham, N.; Dumas, M.-E. Diet-induced metabolic changes of the human gut microbiome: Importance of short-chain fatty acids, methylamines and indoles. Acta Diabetol. 2019, 56, 493–500. [Google Scholar] [CrossRef] [PubMed]
- Rios-Covian, D.; Ruas-Madiedo, P.; Margolles, A.; Gueimonde, M.; De los Reyes-Gavilán, C.G.; Salazar, N. Intestinal Short Chain Fatty Acids and their Link with Diet and Human Health. Front. Microbiol. 2016, 7, 185. [Google Scholar] [CrossRef]
- Matt, S.; Allen, J.; Lawson, M.A.; Mailing, L.J.; Woods, J.A.; Johnson, R.W. Butyrate and Dietary Soluble Fiber Improve Neuroinflammation Associated with Aging in Mice. Front. Immunol. 2018, 9, 1832. [Google Scholar] [CrossRef] [PubMed]
- Li, Z.; Yi, C.-X.; Katiraei, S.; Kooijman, S.; Zhou, E.; Chung, C.K.; Gao, Y.; van den Heuvel, J.K.; Meijer, O.C.; Berbée, J.F.P.; et al. Butyrate reduces appetite and activates brown adipose tissue via the gut-brain neural circuit. Gut 2018, 67, 1269–1279. [Google Scholar] [CrossRef] [PubMed]
- Mollica, M.P.; Raso, G.M.; Cavaliere, G.; Trinchese, G.; De Filippo, C.; Aceto, S.; Prisco, M.; Pirozzi, C.; Di Guida, F.; Lama, A.; et al. Butyrate Regulates Liver Mitochondrial Function, Efficiency, and Dynamics in Insulin-Resistant Obese Mice. Diabetes 2017, 66, 1405–1418. [Google Scholar] [CrossRef] [PubMed]
- Chang, Y.; Chen, Y.; Zhou, Q.; Wang, C.; Chen, L.; Di, W.; Zhang, Y. Short-chain fatty acids accompanying changes in the gut microbiome contribute to the development of hypertension in patients with preeclampsia. Clin. Sci. 2020, 134, 289–302. [Google Scholar] [CrossRef] [PubMed]
- Saresella, M.; Marventano, I.; Barone, M.; La Rosa, F.; Piancone, F.; Mendozzi, L.; D’Arma, A.; Rossi, V.; Pugnetti, L.; Roda, G.; et al. Alterations in Circulating Fatty Acid Are Associated With Gut Microbiota Dysbiosis and Inflammation in Multiple Sclerosis. Front. Immunol. 2020, 11, 1390. [Google Scholar] [CrossRef] [PubMed]
- Sheflin, A.; Borresen, E.C.; Wdowik, M.J.; Rao, S.; Brown, R.J.; Heuberger, A.L.; Broeckling, C.D.; Weir, T.L.; Ryan, E.P. Pilot Dietary Intervention with Heat-Stabilized Rice Bran Modulates Stool Microbiota and Metabolites in Healthy Adults. Nutrients 2015, 7, 1282–1300. [Google Scholar] [CrossRef] [PubMed]
- Utzschneider, K.M.; Kratz, M.; Damman, C.J.; Hullarg, M. Mechanisms Linking the Gut Microbiome and Glucose Metabolism. J. Clin. Endocrinol. Metab. 2016, 101, 1445–1454. [Google Scholar] [CrossRef] [PubMed]
- Pietro, C.; Viviane, V.; Estefania, P.r.C.; Jerome, S.; Anna-Maria, K. Biomarkers of gastrointestinal functionality in animal nutrition and health. Anim. Feed Sci. Technol. 2019, 250, 9–31. [Google Scholar]
- Ma, N.; Ma, X. Dietary Amino Acids and the Gut-Microbiome-Immune Axis: Physiological Metabolism and Therapeutic Prospects. Compr. Rev. Food Sci. Food Saf. 2019, 18, 221–242. [Google Scholar] [CrossRef]
- Wallace, J.L.; Motta, J.-P.; Buret, A.G. Hydrogen sulfide: An agent of stability at the microbiome-mucosa interface. Am. J. Physiol. Liver Physiol. 2018, 314, G143–G149. [Google Scholar] [CrossRef]
- Dupont, D.; Alric, M.; Blanquet-Diot, S.; Bornhorst, G.; Cueva, C.; Deglaire, A.; Denis, S.; Ferrua, M.; Havenaar, R.; Lelieveld, J.; et al. Can dynamic in vitro digestion systems mimic the physiological reality? Crit. Rev. Food Sci. Nutr. 2018, 59, 1–17. [Google Scholar] [CrossRef]
- Van de Wiele, T.; Van den Abbeele, P.; Ossieur, W.; Possemiers, S.; Marzorati, M. The simulator of the human intestinal microbial ecosystem (Shime®). In The Impact of Food Bioactives on Health: In Vitro And ex Vivo Models; Verhoeckx, K., Cotter, P., López-Expósito, I., Kleiveland, C., Lea, T., Mackie, A., Requena, T., Swiatecka, D., Wichers, H., Eds.; Springer International Publishing: Cham, Switzerland, 2015; pp. 305–317. [Google Scholar]
- Cao, X.; Gibbs, S.T.; Fang, L.; Miller, H.A.; Landowski, C.; Shin, H.-C.; Lennernas, H.; Zhong, Y.; Amidon, G.L.; Yu, L.X.; et al. Why is it Challenging to Predict Intestinal Drug Absorption and Oral Bioavailability in Human Using Rat Model. Pharm. Res. 2006, 23, 1675–1686. [Google Scholar] [CrossRef]
- Musther, H.; Olivares-Morales, A.; Hatley, O.J.; Liu, B.; Hodjegan, A.R. Animal versus human oral drug bioavailability: Do they correlate? Eur. J. Pharm. Sci. 2014, 57, 280–291. [Google Scholar] [CrossRef]
- Nagpal, R.; Wang, S.; Woods, L.C.S.; Seshie, O.; Chung, S.T.; Shively, C.A.; Register, T.C.; Craft, S.; McClain, D.A.; Yadav, H. Comparative microbiome signatures and short-chain fatty acids in mouse, rat, non-human primate, and human feces. Front. Microbiol. 2018, 9, 2897. [Google Scholar] [CrossRef]
- Egger, L.; Ménard, O.; Baumann, C.; Duerr, D.; Schlegel, P.; Stoll, P.; Vergères, G.; Dupont, D.; Portmann, R. Digestion of milk proteins: Comparing static and dynamic in vitro digestion systems with in vivo data. Food Res. Int. 2019, 118, 32–39. [Google Scholar] [CrossRef] [PubMed]
- Miranda, L.; Deußer, H.; Evers, D. The impact of in vitro digestion on bioaccessibility of polyphenols from potatoes and sweet potatoes and their influence on iron absorption by human intestinal cells. Food Funct. 2013, 4, 1595–1601. [Google Scholar] [CrossRef] [PubMed]
- Minkiewicz, P.; Dziuba, J.; Iwaniak, A.; Dziuba, M.; Darewicz, M. BIOPEP Database and Other Programs for Processing Bioactive Peptide Sequences. J. AOAC Int. 2008, 91, 965–980. [Google Scholar] [CrossRef] [PubMed]
- Kubow, S.; Iskandar, M.M.; Melgar-Bermudez, E.; Sleno, L.; Sabally, K.; Azadi, B.; How, E.; Prakash, S.; Burgos, G.; Felde, T.Z. Effects of Simulated Human Gastrointestinal Digestion of Two Purple-Fleshed Potato Cultivars on Anthocyanin Composition and Cytotoxicity in Colonic Cancer and Non-Tumorigenic Cells. Nutrients 2017, 9, 953. [Google Scholar] [CrossRef]
- Ekbatan, S.S.; Sleno, L.; Sabally, K.; Khairallah, J.; Azadi, B.; Rodes, L.; Prakash, S.; Donnelly, D.J.; Kubow, S. Biotransformation of polyphenols in a dynamic multistage gastrointestinal model. Food Chem. 2016, 204, 453–462. [Google Scholar] [CrossRef]
- Gaisawat, M.B.; Iskandar, M.M.; MacPherson, C.W.; Tompkins, T.A.; Kubow, S. Probiotic Supplementation is Associated with Increased Antioxidant Capacity and Copper Chelation in C. difficile-Infected Fecal Water. Nutrients 2019, 11, 2007. [Google Scholar] [CrossRef]
- Gumienna, M.; Lasik, M.; Czarnecki, Z. Bioconversion of grape and chokeberry wine polyphenols during simulated gastrointestinal in vitro digestion. Int. J. Food Sci. Nutr. 2011, 62, 226–233. [Google Scholar] [CrossRef]
- Harris, S.; Powers, S.; Monteagudo-Mera, A.; Kosik, O.; Lovegrove, A.; Shewry, P.; Charalampopoulos, D. Determination of the prebiotic activity of wheat arabinogalactan peptide (AGP) using batch culture fermentation. Eur. J. Nutr. 2019, 59, 297–307. [Google Scholar] [CrossRef]
- Gaisawat, M.B.; MacPherson, C.W.; Tremblay, J.; Piano, A.; Iskandar, M.M.; Tompkins, T.A.; Kubow, S. Probiotic Supplementation in a Clostridium difficile-Infected Gastrointestinal Model Is Associated with Restoring Metabolic Function of Microbiota. Microorganisms 2019, 8, 60. [Google Scholar] [CrossRef] [PubMed]
- Benzie, I.F.; Strain, J.J. The Ferric Reducing Ability of Plasma (FRAP) as a Measure of “Antioxidant Power”: The FRAP Assay. Anal. Biochem. 1996, 239, 70–76. [Google Scholar] [CrossRef]
- Nurilmala, M.; Hizbullah, H.H.; Karnia, E.; Kusumaningtyas, E.; Ochiai, Y. Characterization and Antioxidant Activity of Collagen, Gelatin, and the Derived Peptides from Yellowfin Tuna (Thunnus albacares) Skin. Mar. Drugs 2020, 18, 98. [Google Scholar] [CrossRef]
- Mischak, H.; Julian, B.A.; Novak, J. High-resolution proteome/peptidome analysis of peptides and low-molecular-weight proteins in urine. Proteom. Clin. Appl. 2007, 1, 792–804. [Google Scholar] [CrossRef] [PubMed]
- Larder, C.E.; Iskandar, M.M.; Sabally, K.; Kubow, S. Capillary electrophoresis: A fast, cost effective and efficient method replacement for LC-MS when identifying and quantifying small peptides from simulated gastrointestinal digestion of collagen hydrolysate. In Proceedings of the BenefiQ Conference Quebec City Convention Centre, Québec City, QC, Canada, 2–4 October 2018. [Google Scholar]
- Walker, A.; Duncan, S.; Leitch, C.; Child, M.W.; Flint, H.J. pH and Peptide Supply Can Radically Alter Bacterial Populations and Short-Chain Fatty Acid Ratios within Microbial Communities from the Human Colon. Appl. Environ. Microbiol. 2005, 71, 3692–3700. [Google Scholar] [CrossRef] [PubMed]
- Yamashiro, K.; Tanaka, R.; Urabe, T.; Ueno, Y.; Yamashiro, Y.; Nomoto, K.; Takahashi, T.; Tsuji, H.; Asahara, T.; Hattori, N. Gut dysbiosis is associated with metabolism and systemic inflammation in patients with ischemic stroke. PLoS ONE 2017, 12, e0171521. [Google Scholar] [CrossRef]
- Luu, M.; Pautz, S.; Kohl, V.; Singh, R.; Romero, R.; Lucas, S.; Hofmann, J.; Raifer, H.; Vachharajani, N.; Carrascosa, L.C.; et al. The short-chain fatty acid pentanoate suppresses autoimmunity by modulating the metabolic-epigenetic crosstalk in lymphocytes. Nat. Commun. 2019, 10, 1–12. [Google Scholar] [CrossRef]
- Berenbaum, F. Osteoarthritis as an inflammatory disease (osteoarthritis is not osteoarthrosis!). Osteoarthr. Cartil. 2013, 21, 16–21. [Google Scholar] [CrossRef]
- König, D.; Oesser, S.; Scharla, S.; Zdzieblik, D.; Gollhofer, A. Specific Collagen Peptides Improve Bone Mineral Density and Bone Markers in Postmenopausal Women—A Randomized Controlled Study. Nutrients 2018, 10, 97. [Google Scholar] [CrossRef]
- Trč, T.; Bohmova, J. Efficacy and tolerance of enzymatic hydrolysed collagen (EHC) vs. glucosamine sulphate (GS) in the treatment of knee osteoarthritis (KOA). Int. Orthop. 2010, 35, 341–348. [Google Scholar] [CrossRef] [PubMed]
| SCFA | BCFA | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Time (h) | Acetic Acid | Propionic Acid | Butyric Acid | Valeric Acid | Caproic Acid | Heptanoic Acid | Isobutyric Acid | Isovaleric Acid | Isocaproic Acid |
| Ascending colon | |||||||||
| 0 | 12.43 ± 4.43 | 0.08 ± 0.07 | 0.05 ± 0.02 | 0.00 ± 0.00 | 0.00 ± 0.00 | 0.00 ± 0.00 | 0.40 ± 0.05 | 0.04 ± 0.01 | 0.00 ± 0.00 |
| 8 | 24.83 ± 1.84 | 0.16 ± 0.05 | 0.05 ± 0.02 | 0.00 ± 0.00 | 0.00 ± 0.00 | 0.00 ± 0.00 | 0.23 ± 0.04 + | 0.04 ± 0.00 | 0.00 ± 0.00 |
| 16 | 25.17 ± 1.95 | 0.18 ± 0.04 | 0.05 ± 0.00 | 0.00 ± 0.00 | 0.00 ± 0.00 | 0.00 ± 0.00 | 0.26 ± 0.01 | 0.04 ± 0.00 | 0.01 ± 0.01 |
| 24 | 21.48 ± 0.20 | 0.22 ± 0.06 | 0.05 ± 0.00 | 0.00 ± 0.00 | 0.01 ± 0.01 | 0.00 ± 0.00 | 0.19 ± 0.01 * | 0.03 ± 0.01 | 0.01 ± 0.00 |
| Transverse colon | |||||||||
| 0 | 3.10 ± 0.67 | 1.34 ± 1.27 | 4.67 ± 3.21 | 1.56 ± 1.24 | 0.43 ± 0.43 | 0.00 ± 0.00 | 0.54 ± 0.17 | 0.35 ± 0.18 | 0.01 ± 0.01 |
| 8 | 6.87 ± 2.68 | 1.52 ± 1.49 | 5.26 ± 2.65 | 1.74 ± 1.12 | 0.41 ± 0.38 | 0.00 ± 0.00 | 0.55 ± 0.09 | 0.43 ± 0.22 | 0.01 ± 0.01 |
| 16 | 10.56 ± 6.86 | 1.74 ± 1.72 | 3.85 ± 2.35 | 1.42 ± 1.09 | 0.29 ± 0.03 | 0.00 ± 0.00 | 0.40 ± 0.23 | 0.35 ± 0.27 | 0.02 ± 0.01 |
| 24 | 12.2 ± 10.56 | 1.29 ± 0.51 | 2.16 ± 1.14 | 0.85 ± 0.54 | 0.14 ± 0.12 | 0.00 ± 0.00 | 0.32 ± 0.10 | 0.26 ± 0.16 | 0.02 ± 0.01 |
| Descending colon | |||||||||
| 0 | 4.50 ± 1.73 | 2.08 ± 1.90 | 4.56 ± 3.54 | 1.09 ± 1.60 | 0.46 ± 0.42 | 0.00 ± 0.00 | 0.79 ± 0.33 | 0.50 ± 0.26 | 0.01 ± 0.01 |
| 8 | 5.56 ± 1.12 | 1.75 ± 1.51 | 4.70 ± 1.98 | 1.80 ± 0.99 | 0.41 ± 0.32 | 0.00 ± 0.00 | 1.00 ± 0.53 | 0.60 ± 0.11 | 0.01 ± 0.01 |
| 16 | 3.83 ± 0.13 | 1.49 ± 1.44 | 3.83 ± 2.04 | 1.49 ± 0.98 | 0.40 ± 0.28 | 0.00 ± 0.00 | 0.60 ± 0.02 | 0.50 ± 0.17 | 0.02 ± 0.02 |
| 24 | 6.80 ± 2.98 | 1.51 ± 1.43 | 4.63 ± 0.92 | 1.68 ± 0.69 | 0.38 ± 0.26 | 0.00 ± 0.00 | 0.76 ± 0.23 | 0.60 ± 0.07 | 0.02 ± 0.02 |
| SCFA | BCFA | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Time (h) | Acetic Acid | Propionic Acid | Butyric Acid | Valeric Acid | Caproic Acid | Heptanoic Acid | Isobutyric Acid | Isovaleric Acid | Isocaproic Acid |
| Ascending colon | |||||||||
| 0 | 3.96 ± 2.18 | 0.50 ± 0.47 | 2.92 ± 0.21 | 2.12 ± 0.05 | 1.80 ± 0.22 | 1.50 ± 0.08 | 4.27 ± 1.39 | 2.20 ± 0.09 | 1.56 ± 0.05 |
| 8 | 8.55 ± 3.71 | 5.05 ± 0.43 | 4.90 ± 0.26 | 4.42 ± 0.21 * | 3.65 ± 0.10 | 2.87 ± 0.54 | 3.80 ± 0.22 | 3.20 ± 0.13 | 2.66 ± 0.55 |
| 16 | 14.12 ± 2.73 | 7.59 ± 0.59 * | 6.97 ± 0.20 * | 5.91 ± 0.37 * | 4.44 ± 1.13 | 3.10 ± 0.36 | 5.19 ± 0.13 | 3.69 ± 0.34 * | 2.80 ± 0.18 |
| 24 | 14.20 ± 7.02 | 6.53 ± 1.71 * | 5.78 ± 1.21 * | 5.07 ± 0.70 * | 3.83 ± 0.08 | 3.12 ± 0.49 | 4.65 ± 0.61 | 2.81 ± 0.17+ | 2.55 ± 0.47 |
| Transverse colon | |||||||||
| 0 | 3.27 ± 2.13 | 0.16 ± 0.03 | 1.68 ± 0.38 | 1.29 ± 0.21 | 0.89 ± 0.03 | 0.78 ± 0.16 | 2.67 ± 1.26 | 0.86 ± 0.04 | 0.64 ± 0.19 |
| 8 | 2.75 ± 0.41 | 0.82 ± 0.72 | 1.77 ± 0.50 | 1.52 ± 0.26 | 1.11 ± 0.47 | 0.76 ± 0.13 | 2.20 ± 0.10 | 0.98 ± 0.36 | 0.59 ± 0.10 |
| 16 | 2.94 ± 1.46 | 1.06 ± 1.00 | 1.37 ± 0.18 | 1.09 ± 0.03 | 0.82 ± 0.23 | 0.57 ± 0.08 | 2.20 ± 0.07 | 0.82 ± 0.10 | 0.52 ± 0.05 |
| 24 | 6.63 ± 2.54 | 1.52 ± 1.46 | 2.17 ± 0.18 | 1.84 ± 0.12 | 1.20 ± 0.37 | 0.91 ± 0.05 | 5.64 ± 0.87 | 1.09 ± 0.17 | 0.73 ± 0.02 |
| Descending colon | |||||||||
| 0 | 2.43 ± 0.37 | 0.85 ± 0.68 | 2.23 ± 0.39 | 1.35 ± 0.17 | 0.83 ± 0.23 | 0.46 ± 0.10 | 1.97 ± 0.09 | 1.09 ± 0.07 | 0.40 ± 0.13 |
| 8 | 4.34 ± 1.07 | 1.21 ± 0.92 | 3.70 ± 0.60 | 2.26 ± 0.40 | 1.4 ± 0.0.41 | 0.61 ± 0.21 | 2.35 ± 0.11 | 1.76 ± 0.17 | 0.45 ± 0.18 |
| 16 | 3.84 ± 1.16 | 0.37 ± 0.08 | 3.72 ± 1.27 | 2.01 ± 0.05 | 1.34 ± 0.06 | 0.54 ± 0.11 | 3.38 ± 0.73 | 1.73 ± 0.15 | 0.52 ± 0.17 |
| 24 | 3.39 ± 3.39 | 0.43 ± 0.12 | 3.95 ± 1.45 | 2.12 ± 0.12 | 1.32 ± 0.01 | 0.54 ± 0.11 | 4.17 ± 0.95 | 1.76 ± 0.24 | 0.46 ± 0.13 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Larder, C.E.; Iskandar, M.M.; Kubow, S. Gastrointestinal Digestion Model Assessment of Peptide Diversity and Microbial Fermentation Products of Collagen Hydrolysates. Nutrients 2021, 13, 2720. https://doi.org/10.3390/nu13082720
Larder CE, Iskandar MM, Kubow S. Gastrointestinal Digestion Model Assessment of Peptide Diversity and Microbial Fermentation Products of Collagen Hydrolysates. Nutrients. 2021; 13(8):2720. https://doi.org/10.3390/nu13082720
Chicago/Turabian StyleLarder, Christina E., Michèle M. Iskandar, and Stan Kubow. 2021. "Gastrointestinal Digestion Model Assessment of Peptide Diversity and Microbial Fermentation Products of Collagen Hydrolysates" Nutrients 13, no. 8: 2720. https://doi.org/10.3390/nu13082720
APA StyleLarder, C. E., Iskandar, M. M., & Kubow, S. (2021). Gastrointestinal Digestion Model Assessment of Peptide Diversity and Microbial Fermentation Products of Collagen Hydrolysates. Nutrients, 13(8), 2720. https://doi.org/10.3390/nu13082720







