New Insights into Non-Dietary Treatment in Celiac Disease: Emerging Therapeutic Options
Abstract
:1. Introduction
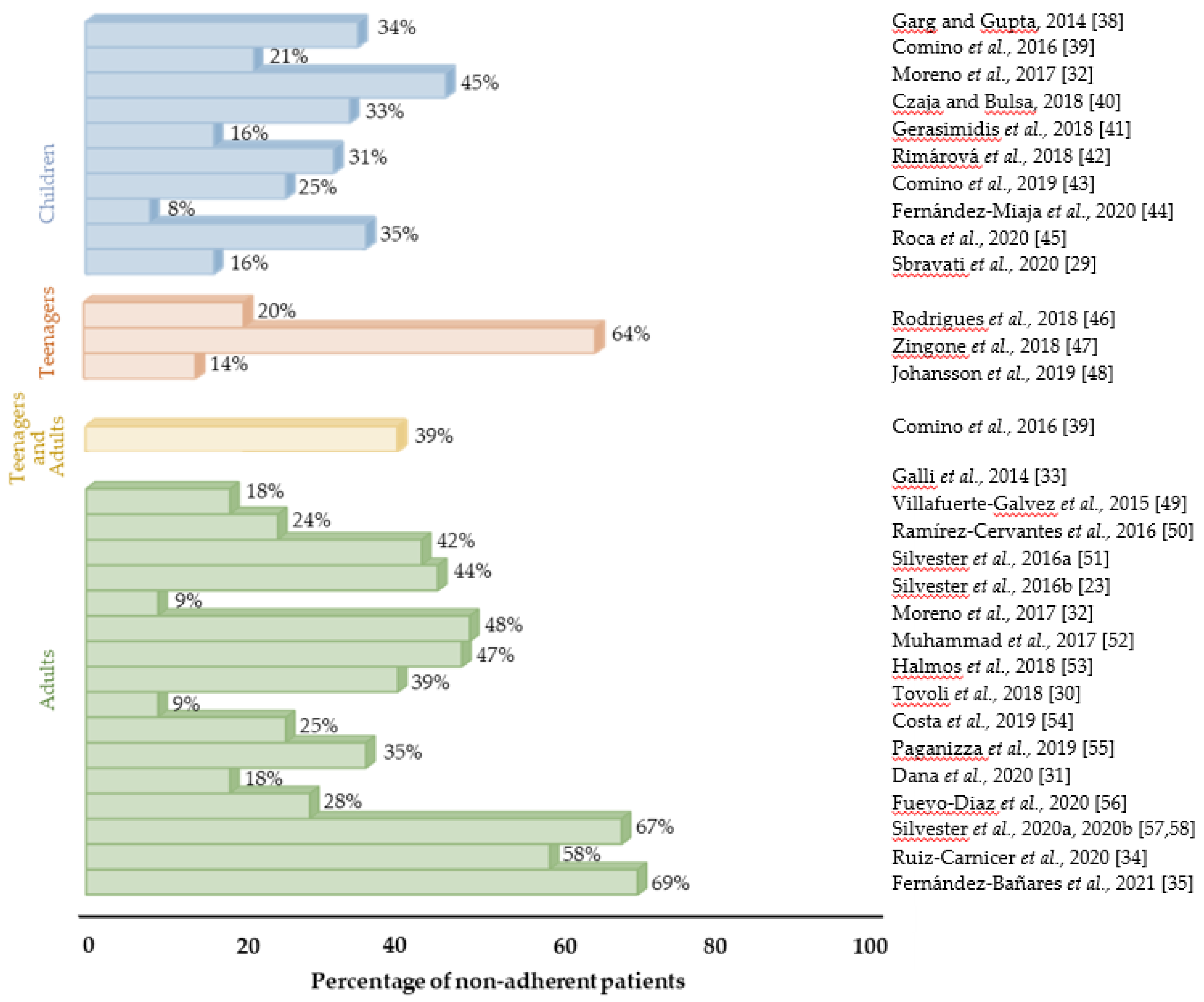
2. Gluten-Free Diet: Challenge and Gluten Exposure
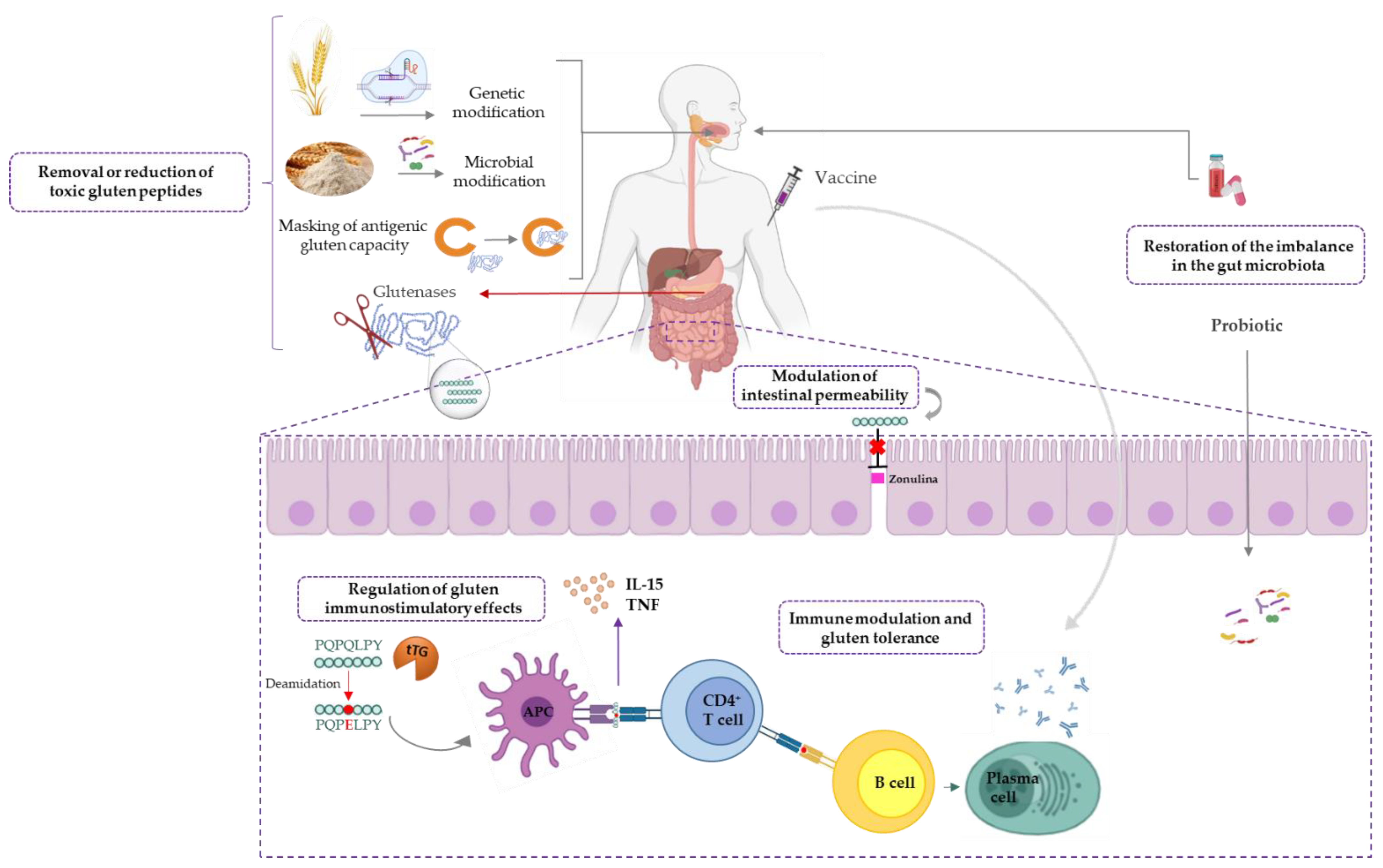
3. Potential Alternative or Adjuvant Non-Dietary Treatments for CD
3.1. Removal or Reduction of Toxic Gluten Peptides
3.1.1. Genetic Modification of Gluten-Containing Cereals
3.1.2. Microbial Gluten Modification
3.1.3. Masking of Antigenic Gluten Capacity
3.1.4. Luminal Gluten Detoxification
3.2. Immune Response Regulation
3.3. Barrier Enhancing Therapies
3.4. Immunomodulation and Gluten Tolerance
3.5. Restoration of the Imbalance in the Gut Microbiota
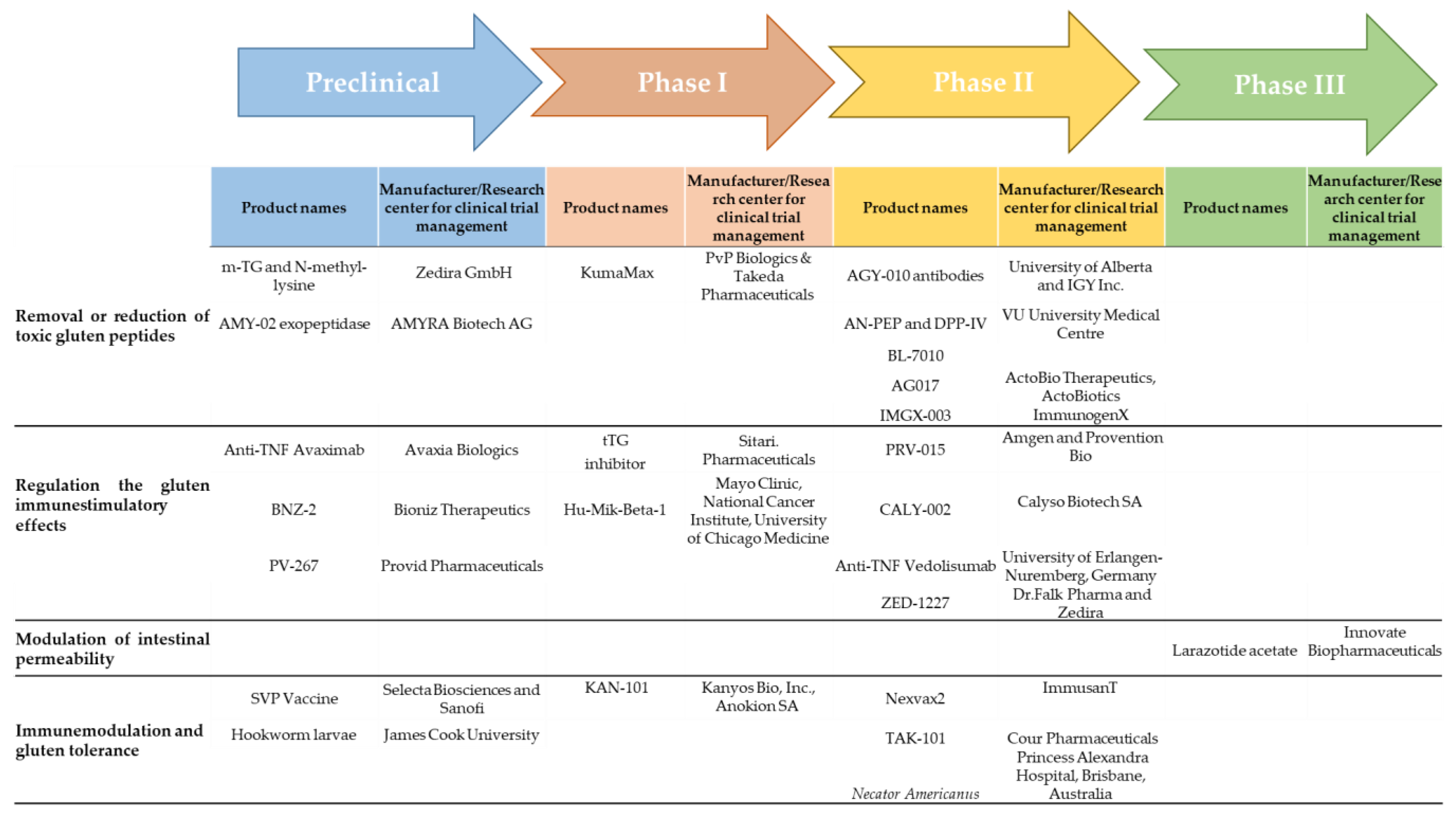
4. Clinical Trials
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Lebwohl, B.; Cao, Y.; Zong, G.; Hu, F.B.; Green, P.H.R.; Neugut, A.I.; Rimm, E.B.; Sampson, L.; Dougherty, L.W.; Giovannucci, E.; et al. Long-term gluten consumption in adults without celiac disease and risk of coronary heart disease: Prospective cohort study. BMJ 2017, 357, j1892. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Al-Toma, A.; Volta, U.; Auricchio, R.; Castillejo, G.; Sanders, D.S.; Cellier, C.; Mulder, C.J.; Lundin, K.E.A. European Society for the Study of Coeliac Disease (ESsCD) guideline for coeliac disease and other gluten-related disorders. United Eur. Gastroenterol. J. 2019, 7, 583–613. [Google Scholar] [CrossRef] [PubMed]
- Lebwohl, B.; Sanders, D.S.; Green, P.H.R. Coeliac disease. Lancet 2018, 391, 70–81. [Google Scholar] [CrossRef]
- Ludvigsson, J.F.; Murray, J.A. Epidemiology of celiac disease. Gastroenterol. Clin. N. Am. 2019, 48, 1–18. [Google Scholar] [CrossRef] [Green Version]
- Singh, P.; Arora, A.; Strand, T.A.; Leffler, D.A.; Catassi, C.; Green, P.H.; Kelly, C.P.; Ahuja, V.; Makharia, G.K. Global prevalence of celiac disease: Systematic review and meta-analysis. Clin. Gastroenterol. Hepatol. 2018, 16, 823–836.e2. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Glissen, J.R.B.; Singh, P. Coeliac disease. Paediatr. Int. Child. Health. 2019, 39, 23–31. [Google Scholar] [CrossRef] [PubMed]
- Mardini, H.E.; Westgate, P.; Grigorian, A.Y. Racial differences in the prevalence of celiac disease in the US population: National Health and Nutrition Examination Survey (NHANES) 2009–2012. Dig. Dis. Sci. 2015, 60, 1738–1742. [Google Scholar] [CrossRef] [PubMed]
- Husby, S.; Koletzko, S.; Korponay-Szabo, I.R.; Mearin, M.L.; Phillips, A.; Shamir, R.; Troncone, R.; Giersiepen, K.; Branski, D.; Catassi, C.; et al. European Society for Pediatric Gastroenterology, Hepatology, and Nutrition guidelines for the diagnosis of coeliac disease. J. Pediatr. Gastroenterol. Nutr. 2012, 54, 136–160. [Google Scholar] [CrossRef]
- Rubio-Tapia, A.; Hill, I.D.; Kelly, C.P.; Calderwood, A.H.; Murray, J.A. American College of Gastroenterology. ACG clinical guidelines: Diagnosis and management of celiac disease. Am. J. Gastroenterol. 2013, 108, 656–676. [Google Scholar] [CrossRef] [Green Version]
- Ludvigsson, J.F.; Bai, J.C.; Biagi, F.; Card, T.R.; Ciacci, C.; Ciclitira, P.J.; Green, P.H.; Hadjivassiliou, M.; Holdoway, A.; van Heel, D.A.; et al. Diagnosis and management of adult coeliac disease: Guidelines from the British Society of Gastroenterology. Gut 2014, 63, 1210–1228. [Google Scholar] [CrossRef]
- Fasano, A.; Sapone, A.; Zevallos, V.; Schuppan, D. Nonceliac gluten sensitivity. Gastroenterology 2015, 148, 1195–1204. [Google Scholar] [CrossRef] [PubMed]
- Mena, M.C.; Sousa, C. Analytical tools for gluten detection. Policies and regulation. In Advances in the Understanding of Gluten Related Pathology and the Evolution of Gluten-Free Foods; Arranz, E., Fernández-Bañares, F., Eds.; OmniaScience: Barcelona, Spain, 2015; pp. 527–564. [Google Scholar]
- Caio, G.; Volta, U.; Sapone, A.; Leffler, D.A.; De Giorgio, R.; Catassi, C.; Fasano, A. Celiac disease: A comprehensive current review. BMC Med. 2019, 17, 142. [Google Scholar] [CrossRef] [Green Version]
- Sharma, N.; Bhatia, S.; Chunduri, V.; Kaur, S.; Sharma, S.; Kapoor, P.; Kumari, A.; Garg, M. Pathogenesis of celiac disease and other gluten related disorders in wheat and strategies for mitigating them. Front. Nutr. 2020, 7, 6. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lindfors, K.; Ciacci, C.; Kurppa, K.; Lundin, K.E.A.; Makharia, G.K.; Mearin, M.L.; Murray, J.A.; Verdu, E.F.; Kaukinen, K. Coeliac disease. Nat. Rev. Dis. Primers 2019, 5, 3. [Google Scholar] [CrossRef]
- Maiuri, L.; Ciacci, C.; Auricchio, S.; Brown, V.; Quaratino, S.; Londei, M. Interleukin 15 mediates epithelialmchanges in celiac disease. Gastroenterology 2000, 119, 996–1006. [Google Scholar] [CrossRef]
- Maiuri, L.; Ciacci, C.; Ricciardelli, I.; Vacca, L.; Raia, V.; Auricchio, S.; Picard, J.; Osman, M.; Quaratino, S.; Londei, M. Association between innate response to gliadin and activation of pathogenic T cells in coeliac disease. Lancet 2003, 362, 30–37. [Google Scholar] [CrossRef]
- Qiao, S.W.; Bergseng, E.; Molberg, O.; Xia, J.; Fleckenstein, B.; Khosla, C.; Sollid, L.M. Antigen presentation to celiac lesion-derived t cells of a 33-mer gliadin peptide naturally formed by gastrointestinal digestion. J. Immunol. 2004, 173, 1757–1762. [Google Scholar] [CrossRef] [Green Version]
- Ráki, M.; Tollefsen, S.; Molberg, Ø.; Lundin, K.E.A.; Sollid, L.M.; Jahnsen, F.L. A Unique dendritic cell subset accumulates in the celiac lesion and efficiently activates gluten-reactive T cells. Gastroenterology 2006, 131, 428–438. [Google Scholar] [CrossRef]
- Tollefsen, S.; Arentz-Hansen, H.; Fleckenstein, B.; Molberg, Ø.; Ráki, M.; Kwok, W.W.; Jung, G.; Lundin, K.E.A.; Sollid, L.M. HLA-DQ2 and -DQ8 signatures of gluten T cell epitopes in celiac disease. J. Clin. Investig. 2006, 116, 2226–2236. [Google Scholar] [CrossRef] [Green Version]
- Martinez, M.; Gómez-Cabellos, S.; Giménez, M.J.; Barro, F.; Diaz, I.; Diaz-Mendozam, M. Plant Proteases: From key enzymes in germination to allies for fighting human gluten-related disorders. Front. Plant Sci. 2019, 10, 721. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gutiérrez, S.; Pérez-Andrés, J.; Martínez-Blanco, H.; Ferrero, M.A.; Vaquero, L.; Vivas, S.; Casqueiro, J.; Rodríguez-Aparicio, L.B. The human digestive tract has proteases capable of gluten hydrolysis. Mol. Metab. 2017, 6, 693–702. [Google Scholar] [CrossRef]
- Silvester, J.A.; Graff, L.A.; Rigaux, L.; Walker, J.R.; Duerksen, D.R. Symptomatic suspected gluten exposure is common among patients with coeliac disease on a gluten-free diet. Aliment. Pharmacol. Ther. 2016, 44, 612–619. [Google Scholar] [CrossRef] [Green Version]
- Stefanolo, J.P.; Tálamo, M.; Dodds, S.; Temprano, M.P.; Costa, A.F.; Moreno, M.L.; Pinto-Sánchez, M.I.; Smecuol, E.; Vázquez, H.; Gonzalez, A.; et al. Real-world gluten exposure in patients with celiac disease on gluten-free diets, determined from gliadin immunogenic peptides in urine and fecal samples. Clin. Gastroenterol. Hepatol. 2021, 19, 484–491.e1. [Google Scholar] [CrossRef]
- Wolf, R.L.; Lebwohl, B.; Lee, A.R.; Zybert, P.; Reilly, N.R.; Cadenhead, J.; Amengual, C.; Green, P.H.R. Hypervigilance to a gluten-free diet and decreased quality of life in teenagers and adults with celiac disease. Dig. Dis. Sci. 2018, 63, 1438–1448. [Google Scholar] [CrossRef]
- Khoury, D.E.; Balfour-Ducharme, S.; Joye, I.J. A review on the gluten-free diet: Technological and nutritional challenges. Nutrients 2018, 10, 1410. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Codex Standard 118-1979. Available online: http://www.fao.org/fao-who-codexalimentarius/sh-proxy/en/?lnk=1&url=https%253A%252F%252Fworkspace.fao.org%252Fsites%252Fcodex%252FStandards%252FCXS%2B118-1979%252FCXS_118e_2015.pdf (accessed on 7 January 2021).
- Cohen, I.S.; Day, A.S.; Shaoul, R. Gluten in celiac disease-more or less? Rambam Maimonides Med. J. 2019, 10, e0007. [Google Scholar] [CrossRef] [PubMed]
- Sbravati, F.; Pagano, S.; Retetangos, C.; Spisni, E.; Bolasco, G.; Labriola, F.; Filardi, M.C.; Grondona, A.G.; Alvisi, P. Adherence to gluten-free diet in a celiac pediatric population referred to the general pediatrician after remission. J. Pediatr. Gastroenterol. Nutr. 2020, 71, 78–82. [Google Scholar] [CrossRef] [PubMed]
- Tovoli, F.; Negrini, G.; Sansone, V.; Faggiano, C.; Catenaro, T.; Bolondi, L.; Granito, A. Celiac disease diagnosed through screening programs in at-risk adults is not associated with worse adherence to the gluten-free diet and might protect from osteopenia/osteoporosis. Nutrients 2018, 10, 1940. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dana, Z.Y.; Lena, B.; Vered, R.; Haim, S.; Efrat, B. Factors associated with non adherence to a gluten free diet in adult with celiac disease: A survey assessed by BIAGI score. Clin. Res. Hepatol. Gastroenterol. 2020, 44, 762–767. [Google Scholar] [CrossRef] [PubMed]
- Moreno, M.L.; Cebolla, Á.; Muñoz-Suano, A.; Carrillo-Carrion, C.; Comino, I.; Pizarro, Á.; León, F.; Rodríguez-Herrera, A.; Sousa, C. Detection of gluten immunogenic peptides in the urine of patients with coeliac disease reveals transgressions in the gluten-free diet and incomplete mucosal healing. Gut 2017, 66, 250–257. [Google Scholar] [PubMed] [Green Version]
- Galli, G.; Esposito, G.; Lahner, E.; Pilozzi, E.; Corleto, V.D.; Di-Giulio, E.; Spiriti, M.A.; Annibale, B. Histological recovery and gluten-free diet adherence: A prospective 1-year follow-up study of adult patients with coeliac disease. Aliment. Pharmacol. Ther. 2014, 40, 639–647. [Google Scholar] [CrossRef] [Green Version]
- Ruiz-Carnicer, A.; Garzón-Benavides, M.; Fombuena, B.; Segura, V.; García-Fernández, F.; Sobrino-Rodríguez, S.; Gómez-Izquierdo, L.; Montes-Cano, M.A.; Rodríguez-Herrera, A.; Millán, R.; et al. Negative predictive value of the repeated absence of gluten immunogenic peptides in the urine of treated celiac patients in predicting mucosal healing: New proposals for follow-up in celiac disease. Am. J. Clin. Nutr. 2020, 112, 1240–1251. [Google Scholar] [CrossRef]
- Fernández-Bañares, F.; Beltrán, B.; Salas, A.; Comino, I.; Ballester-Clau, R.; Ferrer, C.; Molina-Infante, J.; Rosinach, M.; Modolell, I.; Rodríguez-Moranta, F.; et al. Persistent villous atrophy in de novo adult patients with celiac disease and strict control of gluten-free diet adherence: A multicenter prospective study (CADER Study). Am. J. Gastoenterol. 2021, 116, 1036–1043. [Google Scholar] [CrossRef]
- Abu-Janb, N.; Jaana, M. Facilitators and barriers to adherence to gluten-free diet among adults with celiac disease: A systematic review. J. Hum. Nutr. Diet 2020, 33, 786–810. [Google Scholar] [CrossRef] [PubMed]
- Caio, G.; Ciccocioppo, R.; Zoli, G.; Giorgio, R.D.; Volta, U. Therapeutic options for coeliac disease: What else beyond gluten-free diet? Digest. Liver Dis. 2020, 52, 130–137. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Garg, A.; Gupta, R. Predictors of compliance to gluten-free diet in children with celiac disease. Int. Sch. Res. Not. 2014, 2014, 248402. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Comino, I.; Fernández-Bañares, F.; Esteve, M.; Ortigosa, L.; Castillejo, G.; Fombuena, B.; Ribes-Koninckx, C.; Sierra, C.; Rodríguez-Herrera, A.; Salazar, J.C.; et al. Fecal gluten peptides reveal limitations of serological tests and food questionnaires for monitoring gluten-free diet in celiac disease patients. Am. J. Gastroenterol. 2016, 111, 1456–1465. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Czaja-Bulsa, G.; Bulsa, M. Adherence to gluten-free diet in children with celiac disease. Nutrients 2018, 10, 1424. [Google Scholar] [CrossRef] [Green Version]
- Gerasimidis, K.; Zafeiropoulou, K.; Mackinder, M.; Ijaz, U.Z.; Duncan, H.; Buchanan, E.; Cardigan, T.; Edwards, C.A.; McGrogan, P.; Russell, R.K. Comparison of clinical methods with the faecal gluten immunogenic peptide to assess gluten intake in coeliac disease. J. Pediatr. Gastroenterol. Nutr. 2018, 67, 356–360. [Google Scholar] [CrossRef] [Green Version]
- Rimárová, K.; Dorko, E.; Diabelková, J.; Sulinová, Z.; Makovický, P.; Baková, J.; Uhrin, T.; Jenča, A.; Jenčová, J.; Petrášová, A.; et al. Compliance with gluten-free diet in a selected group of celiac children in the Slovak Republic. Cent. Eur. J. Public Health 2018, 26, S19–S24. [Google Scholar] [CrossRef] [Green Version]
- Comino, I.; Segura, V.; Ortigosa, L.; Espín, B.; Castillejo, G.; Garrote, J.A.; Sierra, C.; Millán, A.; Ribes-Koninckx, C.; Román, E.; et al. Prospective longitudinal study: Use of faecal gluten immunogenic peptides to monitor children diagnosed with coeliac disease during transition to a gluten-free diet. Aliment. Pharmacol. Ther. 2019, 49, 1484–1492. [Google Scholar] [CrossRef] [Green Version]
- Fernández-Miaja, M.; Díaz-Martín, J.J.; Jiménez-Treviño, S.; Suárez-González, M.; Bousoño-García, C. Estudio de la adherencia a la dieta sin gluten en pacientes celiacos [Study of adherence to the gluten-free diet in coeliac patients]. An. Pediatr. 2020, 94, 377–384. [Google Scholar] [CrossRef]
- Roca, M.; Donat, E.; Masip, E.; Crespo-Escobar, P.; Cañada-Martínez, A.J.; Polo, B.; Ribes-Koninckx, C. Analysis of gluten immunogenic peptides in feces to assess adherence to the gluten-free diet in pediatric celiac patients. Eur. J. Nutr. 2020, 60, 2131–2140. [Google Scholar] [CrossRef]
- Rodrigues, M.; Yonamine, G.H.; Fernandes-Satiro, C.A. Rate and determinants of nonadherence to a gluten-free diet and nutritional status assessment in children and adolescents with celiac disease in a tertiary Brazilian referral center: A cross-sectional and retrospective study. BMC Gastroenterol. 2018, 18, 15. [Google Scholar]
- Zingone, F.; Massa, S.; Malamisura, B.; Pisano, P.; Ciacci, C. Coeliac disease: Factors affecting the transition and a practical tool for the transition to adult healthcare. United Eur. Gastroenterol. J. 2018, 6, 1356–1362. [Google Scholar] [CrossRef] [PubMed]
- Johansson, K.; Norström, F.; Nordyke, K.; Myleus, A. Celiac dietary adherence test simplifies determining adherence to a gluten-free diet in swedish adolescents. J. Pediatr. Gastroenterol. Nutr. 2019, 69, 575–580. [Google Scholar] [CrossRef] [PubMed]
- Villafuerte-Galvez, J.; Vanga, R.R.; Dennis, M.; Hansen, J.; Leffler, D.A.; Kelly, C.P.; Mukherjee, R. Factors governing long-term adherence to a gluten-free diet in adult patients with coeliac disease. Aliment. Pharmacol. Ther. 2015, 42, 753–760. [Google Scholar] [CrossRef] [PubMed]
- Ramírez-Cervantes, K.L.; Romero-López, A.V.; Núñez-Álvarez, C.A.; Uscanga-Domínguez, L.F. Adherence to a gluten-free diet in mexican subjects with gluten-related ¡disorders: A high prevalence of inadvertent gluten intake. Rev. Investig. Clin. 2016, 68, 229–234. [Google Scholar]
- Silvester, J.A.; Weiten, D.; Graff, L.A.; Walker, J.R.; Duerksen, D.R. Is it gluten-free? Relationship between self-reported gluten-free diet adherence and knowledge of gluten content of foods. Nutrition 2016, 32, 777–783. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Muhammad, H.; Reeves, S.; Ishaq, S.; Mayberry, J.; Jeanes, Y.M. Adherence to a gluten free diet is associated with receiving gluten free foods on prescription and understanding food labelling. Nutrients 2017, 9, 705. [Google Scholar] [CrossRef] [PubMed]
- Halmos, E.P.; Deng, M.; Knowles, S.R.; Sainsbury, K.; Mullan, B.; Tye-Din, J.A. Food knowledge and psychological state predict adherence to a gluten-free diet in a survey of 5310 Australians and New Zealanders with coeliac disease. Aliment. Pharmacol. Ther. 2018, 48, 78–86. [Google Scholar] [CrossRef] [Green Version]
- Costa, A.F.; Sugai, E.; Temprano, M.P.; Niveloni, S.I.; Vázquez, H.; Moreno, M.L.; Domínguez-Flores, M.R.; Muñoz-Suano, A.; Smecuol, E.; Stefanolo, J.P.; et al. Gluten immunogenic peptide excretion detects dietary transgressions in treated celiac disease patients. World J. Gastroenterol. 2019, 25, 1409–1420. [Google Scholar] [CrossRef]
- Paganizza, S.; Zanotti, R.; D’Odorico, A.; Scapolo, P.; Canova, C. Is adherence to a gluten-free diet by adult patients with celiac disease influenced by their knowledge of the gluten content of foods? Gastroenterol. Nurs. 2019, 42, 55–64. [Google Scholar] [CrossRef] [PubMed]
- Fueyo-Díaz, R.; Magallón-Botaya, R.; Gascón-Santos, S.; Asensio-Martínez, Á.; Navarro, G.P.; Sebastián-Domingo, J.J. The effect of self-efficacy expectations in the adherence to a gluten free diet in celiac disease. Psychol. Health 2020, 35, 734–749. [Google Scholar] [CrossRef] [PubMed]
- Silvester, J.A.; Comino, I.; Kelly, C.P.; Sousa, C.; Duerksen, D.R. The DOGGIE BAG study group. Most patients with celiac disease on gluten-free diets consume measurable amounts of gluten. Gastroenterology 2020, 158, 1497–1499.e1. [Google Scholar] [CrossRef] [PubMed]
- Silvester, J.A.; Comino, I.; Rigaux, L.N.; Segura, V.; Green, K.H.; Cebolla, Á.; Weiten, D.; Dominguez, R.; Leffler, A.; Leon, F.; et al. Exposure sources, amounts and time course of gluten ingestion and excretion in patients with coeliac disease on a gluten-free diet. Aliment. Pharmacol. Ther. 2020, 52, 1469–1479. [Google Scholar] [CrossRef]
- Tanner, G.J.; Blundell, M.J.; Colgrave, M.L.; Howitt, C.A. Creation of the first ultra-low gluten barley (Hordeum vulgare L.) for coeliac and gluten-intolerant populations. Plant Biotechnol. J. 2016, 14, 1139–1150. [Google Scholar] [CrossRef]
- Sánchez-León, S.; Gil-Humanes, J.; Ozuna, C.V.; Giménez, M.J.; Sousa, C.; Voytas, D.F.; Barro, F. Low-gluten, nontransgenic wheat engineered with CRISPR/Cas9. Plant Biotechnol. J. 2018, 16, 902–910. [Google Scholar] [CrossRef]
- Syage, J.A.; Green, P.H.R.; Khosla, C.; Adelman, D.C.; Sealey-Voyksner, J.A.; Murray, J.A. Latiglutenase treatment for celiac disease: Symptom and quality of life improvement for seropositive patients on a gluten-free diet. GastroHep 2019, 1, 293–301. [Google Scholar] [CrossRef]
- Håkansson, Å.; Andrén-Aronsson, C.; Brundin, C.; Oscarsson, E.; Molin, G.; Agardh, D. Effects of Lactobacillus plantarum and Lactobacillus paracasei on the peripheral immune response in children with celiac disease autoimmunity: A randomized, double-blind, placebo-controlled clinical trial. Nutrients 2019, 11, 1925. [Google Scholar] [CrossRef] [Green Version]
- Ruh, T.; Ohsam, J.; Pasternack, R.; Yokoyama, K.; Kumazawa, Y.; Hils, M. Microbial transglutaminase treatment in pasta-production does not affect the immunoreactivity of gliadin with celiac disease patients’ sera. J. Agric. Food Chem. 2014, 62, 7604–7611. [Google Scholar] [CrossRef] [PubMed]
- Liang, L.; Pinier, M.; Leroux, J.C.; Subirade, M. Interaction of alpha-gliadin with poly (HEMA-co-SS): Structural characterization and biological implication. Biopolymers 2009, 91, 169–178. [Google Scholar] [CrossRef]
- Pinier, M.; Fuhrmann, G.; Galipeau, H.J.; Rivard, N.; Murray, J.A.; David, S.H.; Drasarova, H.; Tuckova, L.; Leroux, J.C.; Verdu, E. The copolymer P(HEMA-co-SS) binds gluten and reduces immune response in gluten-sensitized mice and human tissues. Gastroenterology 2012, 142, 316–325.e12. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sánchez-Valverde, F.V.; Denis, S.Z.; Etayo, V.E. Nuevas estrategias terapéuticas en la enfermedad celíaca. In Enfermedad Celíaca: Presente y Future; Allué, P., Ed.; Ergon: Madrid, Spain, 2013; pp. 127–134. [Google Scholar]
- Chevallier, S.; Goeltz, P.; Thibault, P.; Banville, D.; Gagnon, J. Characterization of a prolyl endopeptidase from flavobacterium meningosepticum. complete sequence and localization of the active-site serine. J. Biol. Chem. 1992, 267, 8192–8199. [Google Scholar] [CrossRef]
- Diefenthal, T.; Dargatz, H.; Witte, V.; Reipen, G.; Svendsen, I. Cloning of proline-specific endopeptidase gene from Flavobacterium meningosepticum: Expression in Escherichia coli and purification of the heterologous protein. Appl. Microbiol. Biotechnol. 1993, 40, 90–97. [Google Scholar] [CrossRef] [PubMed]
- Shan, L.; Marti, T.; Sollid, L.M.; Gray, G.M.; Khosla, C. Comparative biochemical analysis of three bacterial prolyl endopeptidases: Implications for coeliac sprue. Biochem. J. 2004, 383 Pt 2, 311–318. [Google Scholar] [CrossRef] [Green Version]
- Kabashima, T.; Fujii, M.; Meng, Y.; Ito, K.; Yoshimoto, T. Prolyl endopeptidase from Sphingomonas capsulata: Isolation and characterization of the enzyme and nucleotide sequence of the gene. Arch. Biochem. Biophys. 1998, 358, 141–148. [Google Scholar] [CrossRef]
- Xiao, B.; Zhang, C.; Song, X.; Wu, M.; Mao, J.; Yu, R.; Zheng, Y. Rationally engineered prolyl endopeptidases from Sphingomonas capsulata with improved hydrolytic activity towards pathogenic peptides of celiac diseases. Eur. J. Med. Chem. 2020, 15, 112499. [Google Scholar] [CrossRef] [PubMed]
- Knorr, V.; Wieser, H.; Koehler, P. Production of gluten-free beer by peptidase treatment. Eur. Food Res. Technol. 2016, 242, 1129–1140. [Google Scholar] [CrossRef]
- Lähdeaho, M.L.; Kaukinen, K.; Laurila, K.; Vuotikka, P.; Koivurova, O.P.; Kärjä-Lahdensuu, T.; Marcantonio, A.; Adelman, D.C.; Mäki, M. Glutenase ALV003 attenuates gluten-induced mucosal injury in patients with celiac disease. Gastroenterology 2014, 146, 1649–1658. [Google Scholar] [CrossRef] [Green Version]
- Osorio, C.E.; Wen, N.; Mejías, J.H.; Mitchell, S.; von Wettstein, D.; Rustgi, S. Directed-Mutagenesis of Flavobacterium meningosepticum prolyl-oligopeptidase and a glutamine-specific endopeptidase from barley. Front. Nutr. 2020, 7, 11. [Google Scholar] [CrossRef] [Green Version]
- Darwish, G.; Helmerhorst, E.J.; Schuppan, D.; Oppenheim, F.G.; Wei, G. Pharmaceutically modified subtilisins withstand acidic conditions and effectively degrade gluten in vivo. Sci. Rep. 2019, 9, 7505. [Google Scholar] [CrossRef] [Green Version]
- Lähdeaho, M.L.; Scheinin, M.; Vuotikka, P.; Taavela, J.; Popp, A.; Laukkarinen, J.; Koffert, J.; Koivurova, O.P.; Pesu, M.; Kivelä, L.; et al. Safety and efficacy of AMG 714 in adults with coeliac disease exposed to gluten challenge: A phase 2a, randomised, double-blind, placebo-controlled study. Lancet Gastroenterol. Hepatol. 2019, 4, 948–959. [Google Scholar] [CrossRef]
- Kapoerchan, V.V.; Wiesner, M.; Hillaert, U.; Drijfhout, J.W.; Overhand, M.; Alard, P.; van der Marel, G.A.; Overkleeft, H.S.; Koning, F. Design, synthesis and evaluation of high-affinity binders for the celiac disease associated HLA-DQ2 molecule. Mol. Immunol. 2010, 47, 1091–1097. [Google Scholar] [CrossRef] [PubMed]
- Tang, F.; Sally, B.; Lesko, K.; Discepolo, V.; Abadie, V.; Ciszewski, C.; Semrad, C.; Guandalini, S.; Kupfer, S.S.; Jabri, B. Cysteinyl leukotrienes mediate lymphokine killer activity induced by NKG2D and IL-15 in cytotoxic T cells during celiac disease. J. Exp. Med. 2015, 212, 1487–1495. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Haghbin, M.; Rostami-Nejad, M.; Forouzesh, F.; Sadeghi, A.; Rostami, K.; Aghamohammadi, E.; Asadzadeh-Aghdaei, H.; Masotti, A.; Zali, M.R. The role of CXCR3 and its ligands CXCL10 and CXCL11 in the pathogenesis of celiac disease. Medicine 2019, 98, e15949. [Google Scholar] [CrossRef] [PubMed]
- Cellier, C.; Bouma, G.; van Gils, T.; Khater, S.; Malamut, G.; Crespo, L.; Collin, P.; Green, P.H.R.; Crowe, S.E.; Tsuji, W.; et al. Safety and efficacy of AMG 714 in patients with type 2 refractory coeliac disease: A phase 2a, randomised, double-blind, placebo-controlled, parallel-group study. Lancet Gastroenterol. Hepatol. 2019, 4, 960–970. [Google Scholar] [CrossRef]
- Benedetti, E.; Viscido, A.; Castelli, V.; Maggiani, C.; d’Angelo, M.; Di Giacomo, E.; Antonosante, A.; Picarelli, A.; Frieri, G. Mesalazine treatment in organotypic culture of celiac patients: Comparative study with gluten free diet. J. Cell Physiol. 2018, 233, 4383–4390. [Google Scholar] [CrossRef] [PubMed]
- Leffler, D.A.; Kelly, C.P.; Green, P.H.; Fedorak, R.N.; DiMarin, A.; Perrow, W.; Rasmussen, H.; Wang, C.; Bercik, P.; Bachir, N.M.; et al. Larazotide acetate for persistent symptoms of celiac disease despite a gluten-free diet: A randomized controlled trial. Gastroenterology 2015, 148, 1311–1319.e6. [Google Scholar] [CrossRef] [Green Version]
- Khaleghi, S.; Ju, J.M.; Lamba, A.; Murray, J.A. The potential utility of tight junction regulation in celiac disease: Focus on larazotide acetate. Therap. Adv. Gastroenterol. 2016, 9, 37–49. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Daveson, A.J.M.; Ee, H.C.; Andrews, J.M.; King, T.; Goldstein, K.E.; Dzuris, J.L.; MacDougall, J.A.; Williams, L.J.; Treohan, A.; Cooreman, M.P.; et al. Epitope-specific immunotherapy targeting CD4-positive T cells in celiac disease: Safety, pharmacokinetics, and effects on intestinal histology and plasma cytokines with escalating dose regimens of NEXVAX2 in a randomized, double-blind, placebo-controlled phase 1 study. EBioMedicine 2017, 26, 78–90. [Google Scholar] [PubMed] [Green Version]
- Goel, G.; King, T.; Daveson, A.J.; Andrews, J.M.; Krishnarajah, J.; Krause, R.; Brown, G.J.E.; Fogel, R.; Barish, C.F.; Epstein, R.; et al. Epitope-specific immunotherapy targeting CD4-positive T cells in coeliac disease: Two randomised, double-blind, placebo-controlled phase 1 studies. Lancet Gastroenterol. Hepatol. 2017, 2, 479–493. [Google Scholar] [CrossRef]
- Database ClinicalTrials.gov. Available online: https://clinicaltrials.gov/ct2/show/NCT04530123 (accessed on 5 January 2021).
- Database ClinicalTrials.gov. Available online: https://clinicaltrials.gov/ct2/show/NCT04248855 (accessed on 6 January 2021).
- Croese, J.; Giacomin, P.; Navarro, S.; Clouston, A.; McCann, L.; Dougall, A.; Ferreira, I.; Susianto, A.; O’Rourke, P.; Howlett, M.; et al. Experimental hookworm infection and gluten microchallenge promote tolerance in celiac disease. J. Allergy Clin. Immunol. 2015, 135, 508–516. [Google Scholar] [CrossRef] [PubMed]
- Freire, R.; Ingano, L.; Serena, G.; Cetinbas, M.; Anselmo, A.; Sapone, A.; Sadreyev, R.I.; Fasano, A.; Senger, S. Human gut derived-organoids provide model to study gluten response and effects of microbiota-derived molecules in celiac disease. Sci. Rep. 2019, 9, 7029. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cristofori, F.; Indrio, F.; Miniello, V.L.; De Angelis, M.; Francavilla, R. Probiotics in celiac disease. Nutrients 2018, 10, 1824. [Google Scholar] [CrossRef] [Green Version]
- Ramedani, N.; Sharifan, A.; Gholam-Mostafaei, F.S.; Rostami-Nejad, M.; Yadegar, A.; Ehsani-Ardakani, M.J. The potentials of probiotics on gluten hydrolysis; a review study. Gastroenterol. Hepatol. Bed Bench 2020, 13 (Suppl. 1), S1–S7. [Google Scholar]
- Zanini, B.; Petroboni, B.; Not, T.; di Toro, N.; Villanacci, V.; Lanzarotto, F.; Pogna, N.; Ricci, C.; Lanzini, A. Search for atoxic cereals: A single blind, cross-over study on the safety of a single dose of Triticum monococcum, in patients with celiac disease. BMC Gastroenterol. 2013, 13, 92. [Google Scholar] [CrossRef] [Green Version]
- Vaquero, L.; Comino, I.; Vivas, S.; Rodríguez-Martín, L.; Giménez, M.J.; Pastor, J.; Sousa, C.; Barro, F. Tritordeum: A novel cereal for food processing with good acceptability and significant reduction in gluten immunogenic peptides in comparison with wheat. J. Sci. Food Agric. 2018, 98, 2201–2209. [Google Scholar] [CrossRef]
- Jouanin, A.; Gilissen, L.J.W.J.; Schaart, J.G.; Leigh, F.J.; Cockram, J.; Wallington, E.J.; Boyd, L.A.; van den Broeck, H.C.; van der Meer, I.M.; America, A.H.P.; et al. CRISPR/Cas9 gene editing of gluten in wheat to reduce gluten content and exposure-reviewing methods to screen for coeliac safety. Front. Nutr. 2020, 7, 51. [Google Scholar] [CrossRef]
- Troncone, R.; Auricchio, R.; Granata, V. Issues related to gluten-free diet in coeliac disease. Curr. Opin. Clin. Nutr. Metab. Care 2008, 11, 329–333. [Google Scholar] [CrossRef]
- Barro, F.; Lehisa, J.C.; Giménez, M.J.; García-Molina, M.D.; Ozun, C.V.; Comino, I.; Sousa, C.; Gil-Humanes, J. Targeting of prolamins by RNAi in bread wheat: Effectiveness of seven silencing-fragment combinations for obtaining lines devoid of coeliac disease epitopes from highly immunogenic gliadins. Plant Biotechnol. J. 2016, 14, 986–996. [Google Scholar] [CrossRef] [Green Version]
- Haro, C.; Villatoro, M.; Vaquero, L.; Pastor, J.; Giménez, M.J.; Ozuna, C.V.; Sánchez-León, S.; García-Molina, M.D.; Segura, V.; Comino, I.; et al. The dietary intervention of transgenic low-gliadin wheat bread in patients with non-celiac gluten sensitivity (NCGS) showed no differences with gluten free diet (GFD) but provides better gut microbiota profile. Nutrients 2018, 10, 1964. [Google Scholar] [CrossRef] [Green Version]
- Picozzi, C.; Mariotti, M.; Cappa, C.; Tedesco, B.; Vigentini, I.; Foschino, R.; Lucisano, M. Development of a Type I gluten-free sourdough. Lett. Appl. Microbiol. 2016, 62, 119–125. [Google Scholar] [CrossRef]
- Kõiv, V.; Tenson, T. Gluten-degrading bacteria: Availability and applications. Appl. Microbiol. Biotechnol. 2021, 105, 3045–3059. [Google Scholar] [CrossRef]
- Francavilla, R.; Piccolo, M.; Francavilla, A.; Polimeno, L.; Semeraro, F.; Cristofori, F.; Castellaneta, S.; Barone, M.; Indrio, F.; Gobbetti, M.; et al. Clinical and microbiological effect of a multispecies probiotic supplementation in celiac patients with persistent ibs-type symptoms: A randomized, double-blind, placebo-controlled, multicenter trial. J. Clin. Gastroenterol. 2019, 53, e117–e125. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- De Angelis, M.; Rizzello, C.G.; Fasano, A.; Clemente, M.G.; De Simone, C.; Silano, M.; De Vincenzi, M.; Losito, I.; Gobbetti, M. VSL#3 probiotic preparation has the capacity to hydrolyze gliadin polypeptides responsible for Celiac Sprue. Biochim. Biophys. Acta 2006, 1762, 80–93. [Google Scholar]
- Harnett, J.; Myers, S.P.; Rolfe, M. Probiotics and the microbiome in celiac disease: A Randomised Controlled Trial. Evid. Based Complement. Alternat. Med. 2016, 2016, 9048574. [Google Scholar] [CrossRef] [Green Version]
- Vaquero, L.; Rodríguez-Martín, L.; León, F.; Jorquera, F.; Vivas, S. Nuevas terapias en la enfermedad celiaca y sus complicaciones. Gastroenterol. Hepatol. 2018, 41, 191–204. [Google Scholar] [CrossRef]
- Aaron, L.; Torsten, M. Microbial transglutaminase: A new potential player in celiac disease. Clin. Immunol. 2019, 199, 37–43. [Google Scholar] [CrossRef]
- Zhou, G.; Sprengers, D.; Boor, P.P.C.; Doukas, M.; Schutz, H.; Mancham, S.; Pedroza-Gonzalez, A.; Polak, W.G.; de Jonge, J.; Gaspersz, M.; et al. Antibodies Against Immune Checkpoint Molecules Restore Functions of Tumor-Infiltrating T Cells in Hepatocellular Carcinomas. Gastroenterology 2017, 153, 1107–1119.e10. [Google Scholar] [CrossRef]
- McCarville, J.L.; Nisemblat, Y.; Galipeau, H.J.; Jury, J.; Tabakman, R.; Cohen, A.; Naftali, E.; Neiman, B.; Halbfinger, E.; Murray, J.A.; et al. BL-7010 demonstrates specific binding to gliadin and reduces gluten-associated pathology in a chronic mouse model of gliadin sensitivity. PLoS ONE 2014, 9, e109972. [Google Scholar] [CrossRef] [Green Version]
- Database ClinicalTrials.gov. Available online: https://clinicaltrials.gov/ct2/show/NCT03707730 (accessed on 10 March 2021).
- Stadlmann, V.; Harant, H.; Korschineck, I.; Hermann, M.; Forster, F.; Missbichler, A. Novel avian single-chain fragment variable (scFv) targets dietary gluten and related natural grain prolamins, toxic entities of celiac disease. BMC Biotechnol. 2015, 15, 109. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Moreno, M.L.; Arévalo-Rodríguez, M.; Mellado, E.; Martínez-Reyes, J.C.; Sousa, C. A new microbial gluten-degrading prolyl endopeptidase: Potential application in celiac disease to reduce gluten immunogenic peptides. PLoS ONE 2019, 14, e0218346. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Krishnareddy, S.; Stier, K.; Recanati, M.; Lebwohl, B.; Green, P.H. Commercially available glutenases: A potential hazard in coeliac disease. Therap. Adv. Gastroenterol. 2017, 10, 473–481. [Google Scholar] [CrossRef]
- Moreno, M.L.; Sánchez-Muñoz, D.; Sanders, D.; Rodríguez-Herrera, A.; Sousa, C. Verifying diagnosis of refractory celiac disease with urine gluten immunogenic peptides as biomarker. Front. Med. 2021, 7, 601854. [Google Scholar] [CrossRef]
- Tian, N.; Wei, G.; Schuppan, D.; Helmerhorst, E.J. Effect of Rothia mucilaginosa enzymes on gliadin (gluten) structure, deamidation, and immunogenic epitopes relevant to celiac disease. Am. J. Physiol. Gastrointest. Liver Physiol. 2014, 307, G769–G776. [Google Scholar] [CrossRef] [Green Version]
- Socha, P.; Mickowska, B.; Urminská, D.; Kacmárová, K. The use of different proteases to hydrolyze gliadins. J. Microbiol. Biotechnol. Food Sci. 2015, 4, 101–104. [Google Scholar] [CrossRef] [Green Version]
- Wei, G.; Tian, N.; Valery, A.C.; Zhong, Y.; Schuppan, D.; Helmerhorst, E.J. Identification of pseudolysin (lasB) as an aciduric gluten-degrading enzymewith high therapeutic potential for celiac disease. Am. J. Gastroenterol. 2015, 110, 899–908. [Google Scholar] [CrossRef] [Green Version]
- Wagh, S.K.; Gadge, P.P.; Padul, M.V. Significant hydrolysis of wheat gliadin by bacillus tequilensis (10bT/HQ223107): A Pilot Study. Probiotics Antimicrob. Proteins. 2018, 10, 662–667. [Google Scholar] [CrossRef]
- Rashmi, B.S.; Gayathri, D.; Vasudha, M.; Prashantkumar, C.S.; Swamy, C.T.; Sunil, K.S.; Somaraja, P.K.; Prakash, P. Gluten hydrolyzing activity of Bacillus spp isolated from sourdough. Microb. Cell Factories 2020, 19, 130. [Google Scholar] [CrossRef]
- Cavaletti, L.; Taravella, A.; Carrano, L.; Carenzi, G.; Sigurta, A.; Solinas, N.; De Caro, S.; Di Stasio, L.; Piscascia, S.; Laezza, M.; et al. E40, a novel microbial protease efficiently detoxifying gluten proteins, for the dietary management of gluten intolerance. Sci. Rep. 2019, 9, 13147. [Google Scholar] [CrossRef] [Green Version]
- Ehren, J.; Morón, B.; Martin, E.; Bethune, M.T.; Gray, G.M.; Khosla, C. A foodgrade enzyme preparation with modest gluten detoxification properties. PLoS ONE 2009, 4, e6313. [Google Scholar] [CrossRef] [Green Version]
- Janssen, G.; Christis, C.; Kooy-Winkelaar, Y.; Edens, L.; Smith, D.; van Veelen, P.; Koning, F. Ineffective degradation of immunogenic gluten epitopes by currently available enzyme supplements. PLoS ONE 2015, 10, e0128065. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bethune, M.T.; Ribka, E.; Khosla, C.; Sestak, K. Transepithelial transport and enzymatic detoxification of gluten in gluten-sensitive rhesus macaques. PLoS ONE 2008, 3, e1857. [Google Scholar] [CrossRef] [PubMed]
- Cornell, H.J.; Doherty, W.; Stelmasiak, T. Papaya latex enzymes capable of detoxification of gliadin. Amino Acids 2009, 38, 155–165. [Google Scholar] [CrossRef]
- Savvateeva, L.V.; Gorokhovets, N.V.; Makarov, V.A.; Serebryakova, M.V.; Solovyev, A.G.; Morozov, S.Y.; Reddy, V.P.; Zernii, E.Y.; Zamyatnin, A.A., Jr.; Aliev, G. Glutenase and collagenase activities of wheat cysteine protease Triticain-α: Feasibility for enzymatic therapy assays. Int. J. Biochem. Cell Biol. 2015, 62, 115–124. [Google Scholar] [CrossRef]
- Mika, N.; Zorn, H.; Rühl, M. Prolyl-specific peptidases for applications in food protein hydrolysis. Appl. Microbiol. Biotechnol. 2015, 99, 7837–7846. [Google Scholar] [CrossRef]
- Tereshchenkova, V.F.; Goptar, I.A.; Zhuzhikov, D.P.; Belozersky, M.A.; Dunaevsky, Y.E.; Oppert, B.; Filippova, I.Y.; Elpidina, E.N. Prolidase is a critical enzyme for complete gliadin digestion in Tenebrio molitor larvae. Arch. Insect Biochem. Physiol. 2017, 95, e21395. [Google Scholar] [CrossRef]
- Murray, J.A.; Kelly, C.P.; Green, P.H.R.; Marcantonio, A.; Wu, T.T.; Mäki, M.; Adelman, D.C.; CeliAction Study Group of Investigators. No difference between latiglutenase and placebo in reducing villous atrophy or improving symptoms in patients with symptomatic celiac disease. Gastroenterology 2017, 152, 787–798.e2. [Google Scholar] [CrossRef] [Green Version]
- Syage, J.A.; Murray, J.A.; Green, P.H.R.; Khosla, C. Latiglutenase improves symptoms in seropositive celiac disease patients while on a gluten-free diet. Dig. Dis. Sci. 2017, 62, 2428–2432. [Google Scholar] [CrossRef]
- Database ClinicalTrials.gov. Available online: https://clinicaltrials.gov/ct2/show/NCT03585478 (accessed on 13 March 2021).
- Mitea, C.; Havenaar, R.; Drijfhout, J.W.; Edens, L.; Dekking, L.; Koning, F. Efficient degradation of gluten by a prolyl endoprotease in a gastrointestinal model: Implications for coeliac disease. Gut 2008, 57, 25–32. [Google Scholar] [CrossRef]
- Xia, J.; Bergseng, E.; Fleckenstein, B.; Siegel, M.; Kim, C.Y.; Khosla, C.; Sollid, L.M. Cyclic and dimeric gluten peptide analogues inhibiting DQ2-mediated antigen presentation in celiac disease. Bioorg. Med. Chem. 2007, 15, 6565–6573. [Google Scholar] [CrossRef] [Green Version]
- Esposito, C.; Caputo, I.; Troncone, R. New therapeutic strategies for coeliac disease: Tissue transglutaminase as a target. Curr. Med. Chem. 2007, 14, 2572–2580. [Google Scholar] [CrossRef]
- Alhassan, E.; Yadav, A.; Kelly, C.P.; Mukherjee, R. Novel nondietary therapies for celiac disease. Cell Mol. Gastroenterol. Hepatol. 2019, 8, 335–345. [Google Scholar] [CrossRef] [Green Version]
- Palanski, B.A.; Khosla, C. Cystamine and disulfiram inhibit human transglutaminase 2 via an oxidative mechanism. Biochemistry 2018, 57, 3359–3363. [Google Scholar] [CrossRef]
- Database ClinicalTrials.gov. Available online: https://grantome.com/grant/NIH/R01-DK100619-01A1 (accessed on 1 April 2021).
- Sollid, L.M.; Khosla, C. Novel therapies for coeliac disease. J. Intern. Med. 2011, 269, 604–613. [Google Scholar] [CrossRef] [Green Version]
- Database ClinicalTrials.gov. Available online: https://clinicaltrials.gov/ct2/show/NCT04593251 (accessed on 1 April 2021).
- Reinisch, W. How to manage loss of response to anti-TNF in Crohn’s disease? Curr. Drug Targets 2010, 11, 152–155. [Google Scholar] [CrossRef] [PubMed]
- Phan-Ba, R.; Lambinet, N.; Louis, E.; Delvenne, P.; Tshibanda, L.; Boverie, J.; Moonen, G.; Belachew, S. Natalizumab to kill two birds with one stone: A case of celiac disease and multiple sclerosis. Inflamm. Bowel Dis. 2011, 17, E62–E63. [Google Scholar] [CrossRef] [PubMed]
- Rath, T.; Billmeier, U.; Ferrazzi, F.; Vieth, M.; Ekici, A.; Neurath, F.M.; Atreya, R. Effects of anti-integrin treatment with vedolizumab on immune pathways and cytokines in inflammatory bowel diseases. Front. Immunol. 2018, 9, 1700. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Saruta, M.; Yu, Q.T.; Avanesyan, A.; Fleshner, P.R.; Targan, S.R.; Papadakis, K.A. Phenotype and effector function of CC chemokine receptor 9-expressing lymphocytes in small intestinal Crohn’s disease. J. Immunol. 2007, 178, 3293–3300. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Walters, M.J.; Wang, Y.; Lai, N.; Baumgart, T.; Zhao, B.N.; Dairaghi, D.J.; Bekker, P.; Ertl, L.S.; Penfold, M.E.; Jaen, J.C.; et al. Characterization of CCX282-B, an orally bioavailable antagonist of the CCR9 chemokine receptor, for treatment of inflammatory bowel disease. J. Pharmacol. Exp. Ther. 2010, 335, 61–69. [Google Scholar] [CrossRef]
- Kivelä, L.; Caminero, A.; Leffler, D.A.; Pinto-Sanchez, M.I.; Tye-Din, J.A.; Lindfors, K. Current and emerging therapies for coeliac disease. Nat. Rev. Gastroenterol. Hepatol. 2021, 18, 181–195. [Google Scholar] [CrossRef] [PubMed]
- Gopalakrishnan, S.; Tripathi, A.; Tamiz, A.P.; Alkan, S.S.; Pandey, N.B. Larazotide acetate promotes tight junction assembly in epithelial cells. Peptides 2012, 35, 95–101. [Google Scholar] [CrossRef] [PubMed]
- Gopalakrishnan, S.; Durai, M.; Kitchens, K.; Tamiz, A.P.; Somerville, R.; Ginski, M.; Paterson, B.M.; Murray, J.A.; Verdu, E.F.; Alkan, S.S.; et al. Larazotide acetate regulates epithelial tight junctions in vitro and in vivo. Peptides 2012, 35, 86–94. [Google Scholar] [CrossRef] [PubMed]
- Serena, G.; Kelly, C.P.; Fasano, A. Nondietary therapies for celiac disease. Gastroenterol. Clin. N. Am. 2019, 48, 145–163. [Google Scholar] [CrossRef] [PubMed]
- Tye-Din, J.A.; Stewart, J.A.; Dromey, J.A.; Beissbarth, T.; van Heel, D.A.; Tatham, A.; Henderson, K.; Mannering, S.I.; Gianfrani, C.; Jewell, D.P.; et al. Comprehensive, quantitative mapping of T cell epitopes in gluten in celiac disease. Sci. Transl. Med. 2010, 2, 41ra51. [Google Scholar] [CrossRef] [PubMed]
- Database ClinicalTrials.gov. Available online: https://clinicaltrials.gov/ct2/show/NCT03738475 (accessed on 10 April 2021).
- Daveson, A.J.; Jones, D.M.; Gaze, S.; McSorley, H.; Clouston, A.; Pascoe, A.; Cooke, S.; Speare, R.; Macdonald, G.A.; Anderson, R.; et al. Effect of hookworm infection on wheat challenge in celiac disease-a randomised double-blinded placebo-controlled trial. PLoS ONE 2011, 6, e17366. [Google Scholar] [CrossRef] [PubMed]
- Chibbar, R.; Dieleman, L.A. The gut microbiota in celiac disease and probiotics. Nutrients 2019, 11, 2375. [Google Scholar] [CrossRef] [Green Version]
- Caminero, A.; Verdu, E.F. Metabolism of wheat proteins by intestinal microbes: Implications for wheat related disorders. Gastroenterol. Hepatol. 2019, 42, 449–457. [Google Scholar] [CrossRef]
- Palma, M.L.; Garcia-Bates, T.M.; Martins, F.S.; Douradinha, B. Genetically engineered probiotic Saccharomyces cerevisiae strains mature human dendritic cells and stimulate Gag-specific memory CD8+ T cells ex vivo. Appl. Microbiol. Biotechnol. 2019, 103, 5183–5192. [Google Scholar] [CrossRef]
- Francavilla, R.; Cristofori, F.; Vacca, M.; Barone, M.; De Angelis, M. Advances in understanding the potential therapeutic applications of gut microbiota and probiotic mediated therapies in celiac disease. Expert. Rev. Gastroenterol. Hepatol. 2020, 14, 323–333. [Google Scholar] [CrossRef] [PubMed]
- Strimbu, K.; Tavel, J.A. What are biomarkers? Curr. Opin. HIV AIDS 2010, 5, 463–466. [Google Scholar] [CrossRef]
- Gottlieb, K.; Dawson, J.; Hussain, F.; Murray, J.A. Development of drugs for celiac disease: Review of endpoints for Phase 2 and 3 trials. Gastroenterol. Rep. 2015, 3, 91–102. [Google Scholar] [CrossRef] [PubMed] [Green Version]
| Strategy | Goal | Therapy | References | |
|---|---|---|---|---|
| Removal of toxic gluten peptides before reaching the intestine | Genetic modification of gluten-containing cereals | Genetically modified wheat flours | [59,60,61] | |
| Microbial gluten modification | Pretreatment with probiotic bacteria of the genus Lactobacillus (VSL#3) | [62] | ||
| Pretreatment with microbial transglutaminase (m-TG) and N-methyl-lysine | [63] | |||
| Masking of antigenic gluten capacity | Polymeric resins HEMA-co-SS | [64,65] | ||
| AGY-010 | [66] | |||
| Luminal gluten detoxification | Prolyl endopeptidases (PEPs) | Flavobacterium meningosepticum (FM-PEP) | [67,68] | |
| Myxococcus xanthus (MX-PEP) | [69] | |||
| Sphingomonas capsulata (SC-PEP) | [70,71] | |||
| Aspergillus niger (AN-PEP) | [72] | |||
| Gluten hydrolytic enzyme cocktail | SC-PEP and EPB-2 (ALV003) | [73] | ||
| FM-PEP and EPB-2 | [74] | |||
| Subtilisin derived from Rothia mucilaginosa (Sub-A) | [75] | |||
| Cysteine endopeptidase derived from Hordeum vulgare (EP-B2) | [21] | |||
| Elastase derived from Homo sapiens (CEL-3B) | [22] | |||
| Regulation of the immunostimulatory effects of toxic gluten peptides | Immune response regulation | Inhibition of transglutaminase (ZED 1227) | [76] | |
| Blocker of HLA DQ binding to T-cells | [77] | |||
| NK lymphocyte activation blocker: NKG2D receptor antagonists | [78] | |||
| Lymphocyte recruitment blocker | Anti-α4 integrin (natalizumab) | [79] | ||
| Anti-integrin α4β7 (vedolizumab) | ||||
| Binding inhibitors CD40-CD40L | ||||
| Binding inhibitors CXCL10- CXCR3 | ||||
| Binding inhibitors CCL25-CCR9 | ||||
| Anti-cytokines | Anti-IL-15, PRV-015, CALY-002 (AMG714) | [76,80] | ||
| Anti-TNF-α (infliximab and adalimumab) | ||||
| Anti-TNF- γ (fontolizumab) | ||||
| Inhibition of the proinflammatory cascade | Anti-inflammatories (generic corticosteroids, budesonide, mesalazine) | [81] | ||
| Modulation of intestinal permeability | Barrier enhancing therapies | Larazotide acetate (AT-1001 and INN-202) | [82,83] | |
| Immune modulation and induction of tolerance to gluten | Immunomodulation and gluten tolerance | Vaccine Nexvax2 | [84,85] | |
| TAK-101 (CNP-101 and TIMP-GLIA) | [86] | |||
| KAN-101 | [87] | |||
| Hookworm infection (Necator americanus) | [88] | |||
| Mucosal tolerance due to genetic modification | [89] | |||
| Restoration of the imbalance in the gut microbiota | Probiotic supplementation | Microbial therapies | [90,91] | |
| Source of Enzymes | Peptidase Type | Organism | Isolated Enzyme | References |
|---|---|---|---|---|
| Bacterial peptidases | Prolyl endopeptidase | S. capsulata | SC-PEP | [68] |
| M. xanthus | MX-PEP | [65] | ||
| F.meningosepticum | FM-PEP | [66] | ||
| Chryseobacterium taeanense | PEP 2RA3 | [109] | ||
| Subtilisin | Rothia aeria | ND | [112] | |
| R. mucilaginosa | Sub-A | [112] | ||
| Bacillus licheniformis | ND | [113] | ||
| Pseudolysin | Pseudomonas aeruginosa | lasB | [114] | |
| Thermolysin | Bacillus thermoproteolyticus | ND | [113] | |
| Serine peptidase | Bacillus tequilensis | ND | [115] | |
| ND | Bacillus spp GS 188 | ND | [116] | |
| Serine carboxyl peptidase | Actinoallomurus A8 | E40 | [117] | |
| Fungal peptidases | Prolyl endopeptidase | A. niger | AN-PEP | [72] |
| Aspergillopepsin | A. niger | ASP | [118] | |
| Exopeptidase | Aspergillus oryzae | AO-DPP-IV | [119] | |
| Plant peptidases | Cysteine endopeptidase | H. vulgare | EP-B2 | [120] |
| Carica papaya | Caricain | [121] | ||
| Triticum aestivum | Triticain-α | [122] | ||
| H. vulgare | HvPap-6 CysProt | [123] | ||
| Insect peptidases | Prolyl peptidase | Rhizopertha dominica | ND | [123] |
| Prolidase | Tenebrio molitor | ND | [124] | |
| Human peptidases | Elastase | Homo sapiens | CEL3B | [22] |
| Homo sapiens | CEL2A | [22] | ||
| Carboxypeptidase | Homo sapiens | CBPA1 | [22] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Segura, V.; Ruiz-Carnicer, Á.; Sousa, C.; Moreno, M.d.L. New Insights into Non-Dietary Treatment in Celiac Disease: Emerging Therapeutic Options. Nutrients 2021, 13, 2146. https://doi.org/10.3390/nu13072146
Segura V, Ruiz-Carnicer Á, Sousa C, Moreno MdL. New Insights into Non-Dietary Treatment in Celiac Disease: Emerging Therapeutic Options. Nutrients. 2021; 13(7):2146. https://doi.org/10.3390/nu13072146
Chicago/Turabian StyleSegura, Verónica, Ángela Ruiz-Carnicer, Carolina Sousa, and María de Lourdes Moreno. 2021. "New Insights into Non-Dietary Treatment in Celiac Disease: Emerging Therapeutic Options" Nutrients 13, no. 7: 2146. https://doi.org/10.3390/nu13072146
APA StyleSegura, V., Ruiz-Carnicer, Á., Sousa, C., & Moreno, M. d. L. (2021). New Insights into Non-Dietary Treatment in Celiac Disease: Emerging Therapeutic Options. Nutrients, 13(7), 2146. https://doi.org/10.3390/nu13072146






