Trends in Vitamin C Consumption in the United States: 1999–2018
Abstract
1. Introduction
2. Materials and Methods
2.1. Data Sources
2.2. Dietary Recall Data
2.3. Analysis Approach
2.4. Biochemical Indicators of Vitamin C Intake
2.5. Statistical Analyses
3. Results
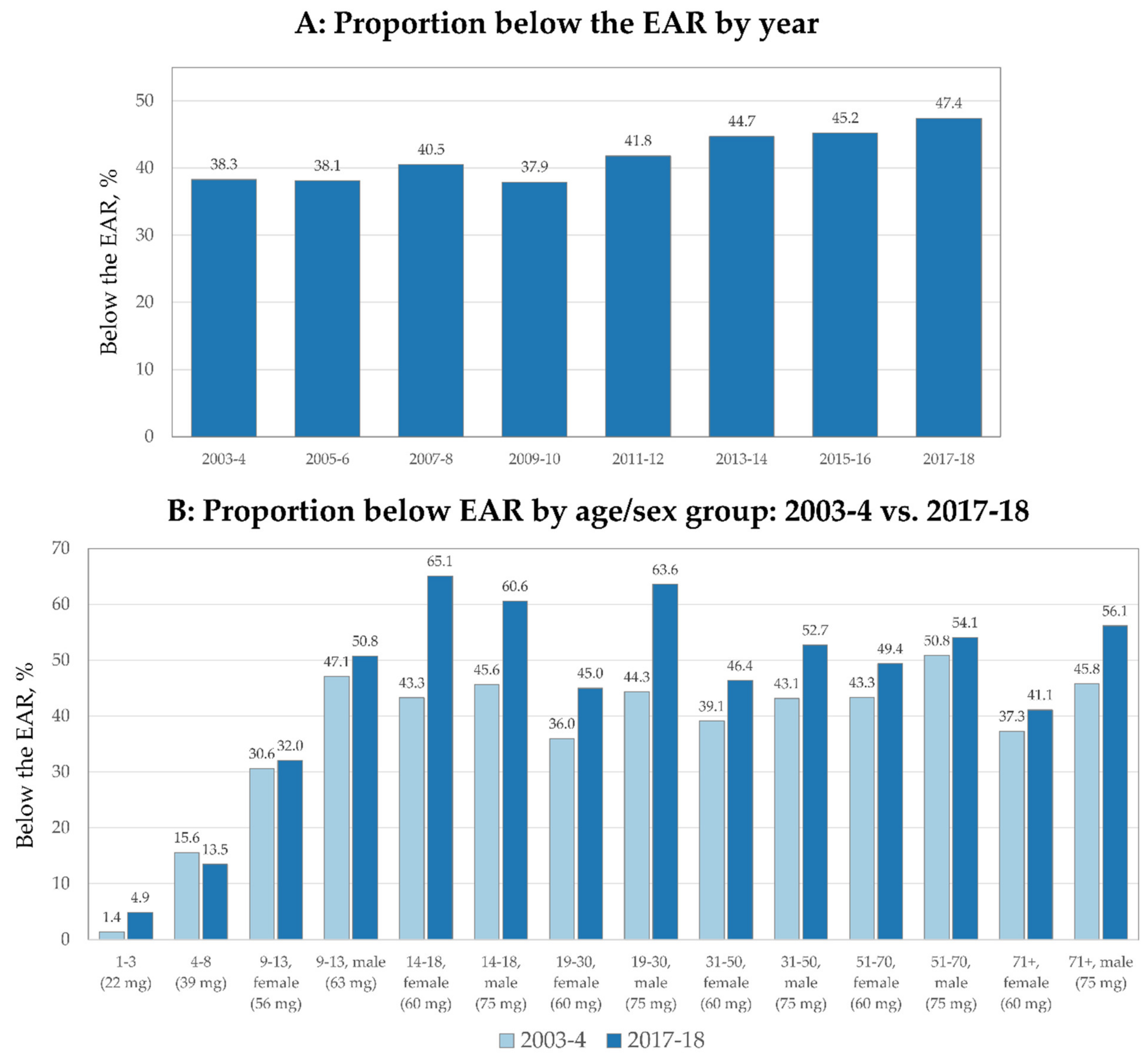
3.1. EAR Results
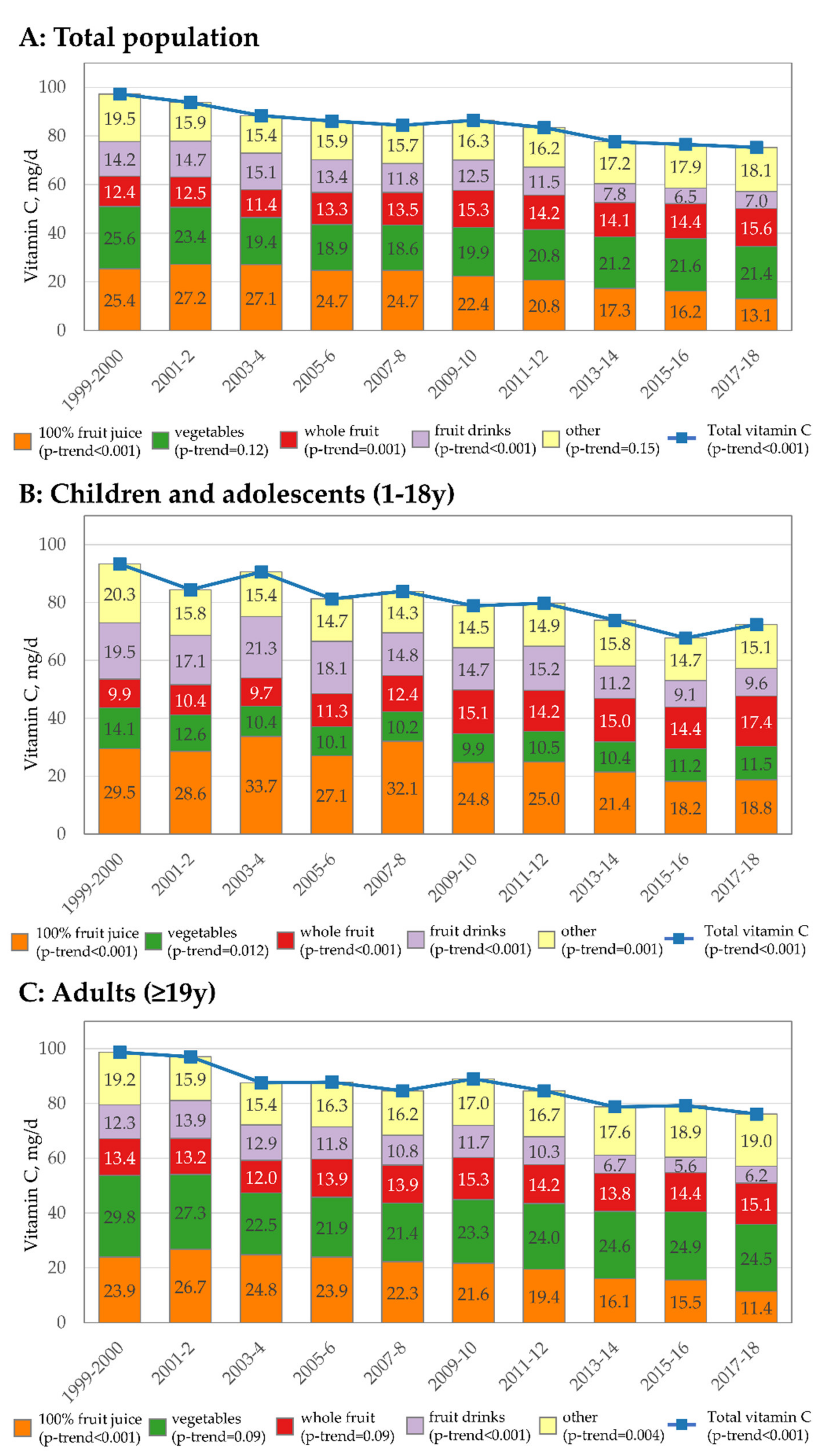
3.2. Trends Based on Biomarkers of Vitamin C
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- U.S. Department of Health and Human Services; U.S. Department of Agriculture. 2015–2020 Dietary Guidelines for Americans; U.S. Department of Health and Human Services; U.S. Department of Agriculture: Washington, DC, USA, 2015.
- Hoy, M.K.; Clemens, J.C.; Martin, C.L.; Moshfegh, A.J. Fruit and Vegetable Consumption of US Adults by Level of Variety, What We Eat in America, NHANES 2013–2016. Curr. Dev. Nutr. 2020, 4, nzaa014. [Google Scholar] [CrossRef] [PubMed]
- U.S. Department of Agriculture. Choose My Plate. Available online: https://www.choosemyplate.gov/ (accessed on 30 September 2020).
- Taylor, C.A.; Hampl, J.S.; Johnston, C.S. Low Intakes of Vegetables and Fruits, Especially Citrus Fruits, Lead to Inadequate Vitamin C Intakes among Adults. Eur. J. Clin. Nutr. 2000, 54, 573–578. [Google Scholar] [CrossRef] [PubMed]
- National Institutes of Health. Vitamin C Fact Sheet for Consumers. Available online: https://ods.od.nih.gov/pdf/factsheets/VitaminC-Consumer.pdf (accessed on 4 October 2020).
- Granger, M.; Eck, P. Dietary Vitamin C in Human Health. Adv. Food Nutr. Res. 2018, 83, 281–310. [Google Scholar] [PubMed]
- Gombart, A.F.; Pierre, A.; Maggini, S. A Review of Micronutrients and the Immune System-Working in Harmony to Reduce the Risk of Infection. Nutrients 2020, 12, 236. [Google Scholar] [CrossRef] [PubMed]
- Mousavi, S.; Bereswill, S.; Heimesaat, M.M. Immunomodulatory and Antimicrobial Effects of Vitamin C. Eur. J. Microbiol. Immunol. (Bp) 2019, 9, 73–79. [Google Scholar] [CrossRef]
- Pullar, J.M.; Carr, A.C.; Vissers, M.C.M. The Roles of Vitamin C in Skin Health. Nutrients. 2017, 9, 866. [Google Scholar] [CrossRef]
- Figueroa-Méndez, R.; Rivas-Arancibia, S. Vitamin C in Health and Disease: Its Role in the Metabolism of Cells and Redox State in the Brain. Front. Physiol. 2015, 6, 397. [Google Scholar] [CrossRef]
- Aune, D.; Keum, N.; Giovannucci, E.; Fadnes, L.T.; Boffetta, P.; Greenwood, D.C.; Tonstad, S.; Vatten, L.J.; Riboli, E.; Norat, T. Dietary Intake and Blood Concentrations of Antioxidants and the Risk of Cardiovascular Disease, Total Cancer, and All-Cause Mortality: A Systematic Review and Dose-Response Meta-Analysis of Prospective Studies. Am. J. Clin. Nutr. 2018, 108, 1069–1091. [Google Scholar] [CrossRef]
- Woodside, J.V.; Draper, J.; Lloyd, A.; McKinley, M.C. Use of Biomarkers to Assess Fruit and Vegetable Intake. Proc. Nutr. Soc. 2017, 76, 308–315. [Google Scholar] [CrossRef]
- Institute of Medicine. Dietary Reference Intakes for Vitamin C, Vitamin E, Selenium, and Caroteinoids; Food and Nutrition Board; National Academy Press: Washington, DC, USA, 2000.
- Maxfield, L.; Crane, J.S. Vitamin C Deficiency; StatPearls Publishing: Treasure Island, FL, USA, 2020. [Google Scholar]
- U.S. Department of Agriculture; U.S. Department of Health and Human Services. Dietary Guidelines for Americans; Government Printing Office: Washington, DC, USA, 2005.
- United States Department of Agriculture; United States Department of Health and Human Services. Dietary Guidelines for Americans. Available online: https://health.gov/sites/default/files/2020-01/DietaryGuidelines2010.pdf (accessed on 15 October 2020).
- Centers for Disease Control and Prevention. NHANES Response Rates and Population Totals. Available online: https://wwwn.cdc.gov/nchs/nhanes/responserates.aspx#response-rates (accessed on 13 December 2020).
- Centers for Disease Control and Prevention. National Health and Nutrition Examination Survey. Available online: https://www.cdc.gov/nchs/nhanes/index.htm (accessed on 22 October 2020).
- Freedman, L.S.; Commins, J.M.; Willett, W.; Tinker, L.F.; Spiegelman, D.; Rhodes, D.; Potischman, N.; Neuhouser, M.L.; Moshfegh, A.J.; Kipnis, V.; et al. Evaluation of the 24-Hour Recall as a Reference Instrument for Calibrating Other Self-Report Instruments in Nutritional Cohort Studies: Evidence from the Validation Studies Pooling Project. Am. J. Epidemiol. 2017, 186, 73–82. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. National Health and Nutrition Examination Survey (NHANES), MEC in-Person Dietary Interviewers Procedures Manual. Available online: https://wwwn.cdc.gov/nchs/data/nhanes/2017-2018/manuals/2017_MEC_In-Person_Dietary_Interviewers_Manual.pdf (accessed on 5 October 2020).
- United States Department of Agriculture. Food and Nutrient Database for Dietary Studies. Available online: https://www.ars.usda.gov/northeast-area/beltsville-md-bhnrc/beltsville-human-nutrition-research-center/food-surveys-research-group/docs/fndds-download-databases/ (accessed on 13 December 2020).
- Centers for Disease Control and Prevention. National Health and Nutrition Examination Survey 2005–2006 Data Documentation, Codebook and Frequencies Vitamin C. Available online: https://wwwn.cdc.gov/nchs/nhanes/2005-2006/VIC_D.htm (accessed on 13 December 2020).
- Centers for Disease Control and Prevention. National Health and Nutrition Examination Survey 2017–2018 Data Documentation, Codebook, and Frequencies. Available online: https://wwwn.cdc.gov/Nchs/Nhanes/2017-2018/VIC_J.htm (accessed on 13 December 2020).
- Schleicher, R.L.; Carroll, M.D.; Ford, E.S.; Lacher, D.A. Serum Vitamin C and the Prevalence of Vitamin C Deficiency in the United States: 2003–2004 National Health and Nutrition Examination Survey (NHANES). Am. J. Clin. Nutr. 2009, 90, 1252–1263. [Google Scholar] [CrossRef] [PubMed]
- Kim, S. Overview of Cotinine Cutoff Values for Smoking Status Classification. Int. J. Environ. Res. Public Health 2016, 13, 1236. [Google Scholar] [CrossRef] [PubMed]
- Drope, J.; Liber, A.C.; Cahn, Z.; Stoklosa, M.; Kennedy, R.; Douglas, C.E.; Henson, R.; Drope, J. Who’s Still Smoking? Disparities in Adult Cigarette Smoking Prevalence in the United States. CA Cancer J. Clin. 2018, 68, 106–115. [Google Scholar] [CrossRef] [PubMed]
- Hales, C.M.; Fryar, C.D.; Carroll, M.D.; Freedman, D.S.; Aoki, Y.; Ogden, C.L. Prevalence of Obesity and Severe Obesity among Adults: United States, 2017–2018. NCHS Data Brief 2020, 360, 1–8. [Google Scholar]
- Institute of Medicine (US) Committee to Review Dietary Reference Intakes for Vitamin D and Calcium. Dietary Reference Intakes for Calcium and Vitamin D; Taylor, C.L., Ross, A.C., Yaktine, A.L., Eds.; National Academies Press: Washington, DC, USA, 2011.
- Tooze, J.A.; Midthune, D.; Dodd, K.W.; Freedman, L.S.; Krebs-Smith, S.M.; Subar, A.F.; Guenther, P.M.; Carroll, R.J.; Kipnis, V. A New Statistical Method for Estimating the Usual Intake of Episodically Consumed Foods with Application to Their Distribution. J. Am. Diet. Assoc. 2006, 106, 1575–1587. [Google Scholar] [CrossRef] [PubMed]
- National Cancer Institute, Division of Cancer Control & Population. Usual Dietary Intakes: SAS Macros for the NCI Method. Available online: https://epi.grants.cancer.gov/diet/usualintakes/macros.html (accessed on 13 December 2020).
- Rehm, C.D.; Peñalvo, J.L.; Afshin, A.; Mozaffarian, D. Dietary Intake among Us Adults, 1999–2012. Jama 2016, 315, 2542–2553. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Rehm, C.D.; Onopa, J.; Mozaffarian, D. Trends in Diet Quality among Youth in the United States, 1999–2016. Jama 2020, 323, 1161–1174. [Google Scholar] [CrossRef]
- Miller, G.; Merlo, C.; Demissie, Z.; Sliwa, S.; Park, S. Trends in Beverage Consumption among High School Students—United States, 2007–2015. MMWR Morb. Mortal. Wkly. Rep. 2017, 66, 112–116. [Google Scholar] [CrossRef]
- Miles, G.; Siega-Riz, A.M. Trends in Food and Beverage Consumption among Infants and Toddlers: 2005–2012. Pediatrics 2017, 139, e20163290. [Google Scholar] [CrossRef]
- Nicklas, T.A.; O’Neil, C.E.; Saab, R.; Fulgoni, V.L., III. Trends in Orange Juice Consumption and Nutrient Adequacy in Children 2003–2016. Lifesci. Global 2020, 9, 100–114. [Google Scholar] [CrossRef]
- Mintel. Juice and Juice Drinks: Including Impact of Covid-19—Us—June. 2020. Available online: https://store.mintel.com/report/juice-and-juice-drinks-incl-impact-of-covid-19-us-june-2020 (accessed on 8 December 2020).
- Neves, M.F.; Trombin, V.G.; Marques, V.N.; Martinez, L.F. Global Orange Juice Market: A 16-Year Summary and Opportunities for Creating Value. Trop. Plant Pathol. 2020, 45, 166–174. [Google Scholar] [CrossRef]
- Smedman, A.; Lindmark-Månsson, H.; Drewnowski, A.; Edman, A.K.M. Nutrient Density of Beverages in Relation to Climate Impact. Food Nutr. Res. 2010, 54, 5170. [Google Scholar] [CrossRef] [PubMed]
- Guasch-Ferré, M.; Hu, F.B. Are Fruit Juices Just as Unhealthy as Sugar-Sweetened Beverages? Jama Netw. Open 2019, 3, e193109. [Google Scholar] [CrossRef] [PubMed]
- Heyman, M.B.; Abrams, S.A. Fruit Juice in Infants, Children, and Adolescents: Current Recommendations. Pediatrics 2017, 139, e20170967. [Google Scholar] [CrossRef] [PubMed]
- Brauchla, M.; Rehm, C.D.; Fulgoni, V.L., III. Cost-Effective Options for Increasing Consumption of Underconsumed Food Groups and Nutrients in the US. Public Health Nutr. 2021, in press. [Google Scholar]
- Miller, V.; Yusuf, S.; Chow, C.K.; Dehghan, M.; Corsi, D.J.; Lock, K.; Popkin, B.; Rangarajan, S.; Khatib, R.; Lear, S.A.; et al. Availability, Affordability, and Consumption of Fruits and Vegetables in 18 Countries across Income Levels: Findings from the Prospective Urban Rural Epidemiology (Pure) Study. Lancet Glob. Health 2016, 4, e695–e703. [Google Scholar] [CrossRef]
- Mook, K.; Laraia, B.A.; Oddo, V.M.; Jones-Smith, J.C. Food Security Status and Barriers to Fruit and Vegetable Consumption in Two Economically Deprived Communities of Oakland, California, 2013–2014. Prev. Chronic Dis. 2016, 13, E21. [Google Scholar] [CrossRef]
- Rehm, C.D.; Monsivais, P.; Drewnowski, A. Relation between Diet Cost and Healthy Eating Index 2010 Scores among Adults in the United States 2007–2010. Prev. Med. 2015, 73, 70–75. [Google Scholar] [CrossRef]
- Jack, D.; Neckerman, K.; Schwartz-Soicher, O.; Lovasi, G.S.; Quinn, J.; Richards, C.; Bader, M.; Weiss, C.; Konty, K.; Arno, P.; et al. Socio-Economic Status, Neighbourhood Food Environments and Consumption of Fruits and Vegetables in New York City. Public Health Nutr. 2013, 16, 1197–1205. [Google Scholar] [CrossRef]
- Blitstein, J.L.; Snider, J.; Evans, W.D. Perceptions of the Food Shopping Environment Are Associated with Greater Consumption of Fruits and Vegetables. Public Health Nutr. 2012, 15, 1124–1129. [Google Scholar] [CrossRef]
- Haynes-Maslow, L.; Parsons, S.E.; Wheeler, S.B.; Leone, L.A. A Qualitative Study of Perceived Barriers to Fruit and Vegetable Consumption among Low-Income Populations, North Carolina, 2011. Prev. Chronic. Dis. 2013, 10, E34. [Google Scholar] [CrossRef] [PubMed]
- Lucan, S.C.; Barg, F.K.; Long, J.A. Promoters and Barriers to Fruit, Vegetable, and Fast-Food Consumption among Urban, Low-Income African Americans—A Qualitative Approach. Am. J. Public Health 2010, 100, 631–635. [Google Scholar] [CrossRef] [PubMed]
- Lee-Kwan, S.H.; Moore, L.V.; Blanck, H.M.; Harris, D.M.; Galuska, D. Disparities in State-Specific Adult Fruit and Vegetable Consumption—United States, 2015. MMWR Morb. Mortal. Wkly Rep. 2017, 66, 1241–1247. [Google Scholar] [CrossRef] [PubMed]
- U.S. Department of Agriculture. Interactive Chart: Most and Least Expensive Fruits and Vegetables. Available online: https://www.ers.usda.gov/data-products/fruit-and-vegetable-prices/interactive-chart-most-and-least-expensive-fruits-and-vegetables/ (accessed on 13 December 2020).
- United States Department of Agriculture. The Estimated Amount, Value, and Calories of Postharvest Food Losses at the Retail and Consumer Levels in the United States; Wells, H.F., Buzby, J.C., Hyman, F., Eds.; United States Department of Agriculture: Washington, DC, USA, 2014. Available online: https://www.ers.usda.gov/webdocs/publications/43833/43680_eib121.pdf?v=9667.8 (accessed on 10 December 2020).
- American Heart Association. Vitamin Supplements: Hype or Help for Healthy Eating. Available online: https://www.heart.org/en/healthy-living/healthy-eating/eat-smart/nutrition-basics/vitamin-supplements-hype-or-help-for-healthy-eating (accessed on 8 December 2020).
- American Institute for Cancer Research. Supplements and Nutrients, Accept No Substitutes. Available online: https://www.aicr.org/cancer-prevention/healthy-eating/supplements-nutrients/ (accessed on 13 December 2020).
- Marra, M.V.; Boyar, A.P. Position of the American Dietetic Association: Nutrient Supplementation. J. Am. Diet. Assoc. 2009, 85, 257S–264S. [Google Scholar]
- US Preventive Services Task Force. Vitamin Supplementation to Prevent Cancer and CVD: Preventive Medication. Available online: https://www.uspreventiveservicestaskforce.org/uspstf/document/RecommendationStatementFinal/vitamin-supplementation-to-prevent-cancer-and-cvd-counseling (accessed on 23 November 2020).
- Bailey, R.L.; Gahche, J.J.; Miller, P.E.; Thomas, P.R.; Dwyer, J.T. Why US Adults Use Dietary Supplements. JAMA Intern. Med. 2013, 173, 355–361. [Google Scholar] [CrossRef]
- Kantor, E.D.; Rehm, C.D.; Du, M.; White, E.; Giovannucci, E.L. Trends in Dietary Supplement Use among US Adults from 1999–2012. Jama 2016, 316, 1464–1474. [Google Scholar] [CrossRef]
- Stierman, B.; Mishra, S.; Gahche, J.J.; Potischman, N.; Hales, C.M. Dietary Supplement Use in Children and Adolescents Aged ≤ 19 Years—United States, 2017–2018. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 1557–1562. [Google Scholar] [CrossRef]
- Lobo, V.; Patil, A.; Phatak, A.; Chandra, N. Free Radicals, Antioxidants and Functional Foods: Impact on Human Health. Pharmacogn. Rev. 2010, 4, 118–126. [Google Scholar] [CrossRef]
- Cowan, A.E.; Jun, S.; Tooze, J.A.; Eicher-Miller, H.A.; Dodd, K.W.; Gahche, J.J.; Guenther, P.M.; Dwyer, J.T.; Potischman, N.; Bhadra, A.; et al. Total Usual Micronutrient Intakes Compared to the Dietary Reference Intakes among U.S. Adults by Food Security Status. Nutrients 2019, 12, 38. [Google Scholar] [CrossRef]
- Teucher, B.; Olivares, M.; Cori, H. Enhancers of Iron Absorption: Ascorbic Acid and Other Organic Acids. Int. J. Vitam. Nutr. Res. 2004, 74, 403–419. [Google Scholar] [CrossRef]
- Aschemann-Witzel, J.; Gantriis, R.F.; Fraga, P.; Perez-Cueto, F.J. Plant-Based Food and Protein Trend from a Business Perspective: Markets, Consumers, and the Challenges and Opportunities in the Future. Crit. Rev. Food Sci. Nutr. 2020, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Shan, Z.; Rehm, C.D.; Rogers, G.; Ruan, M.; Wang, D.D.; Hu, F.B.; Mozaffarian, D.; Zhang, F.F.; Bhupathiraju, S.N. Trends in Dietary Carbohydrate, Protein, and Fat Intake and Diet Quality among Us Adults, 1999–2016. JAMA 2019, 322, 1178–1187. [Google Scholar] [CrossRef] [PubMed]
- Willett, W. Nutritional Epidemiology, 3rd ed.; New York Oxford University Press: New York, NY, USA, 2012. [Google Scholar]

| N | Weighted % | Mean Vitamin C, mg/d (95% CI) | |
|---|---|---|---|
| Total | 84,902 | 100.0 | 85 (83, 86) |
| Age group | |||
| 1–3 | 6605 | 4.0 | 88 (85, 91) |
| 4–8 | 8534 | 6.8 | 81 (78, 84) |
| 9–13 | 9219 | 6.9 | 75 (73, 78) |
| 14–18 | 9976 | 7.1 | 81 (77, 84) |
| 19–30 | 11,211 | 17.0 | 87 (84, 90) |
| 31–50 | 16,322 | 27.6 | 86 (83, 89) |
| 51–70 | 15,214 | 22.4 | 85 (83, 88) |
| ≥71 | 7821 | 8.1 | 85 (82, 88) |
| Sex | |||
| Female | 43,138 | 51.2 | 79 (77, 80) |
| Male | 41,764 | 48.8 | 91 (89, 93) |
| Race/ethnicity | |||
| Non-Hispanic White | 32,117 | 65.3 | 80 (78, 82) |
| Non-Hispanic Black | 20,007 | 12.0 | 94 (92, 97) |
| Mexican-American | 18,577 | 9.8 | 95 (91, 98) |
| Other Hispanic | 6801 | 5.7 | 92 (89, 96) |
| Other race/mixed race | 7400 | 7.1 | 87 (83, 90) |
| Family income-to-poverty ratio a | |||
| <1.00 [lower income] | 20,621 | 16.2 | 85 (82, 88) |
| 1.00–1.99 | 20,957 | 20.1 | 80 (77, 83) |
| 2.00–3.99 | 19,880 | 26.5 | 81 (79, 83) |
| ≥4.00 [higher income] | 16,625 | 30.2 | 90 (87, 93) |
| Missing | 6819 | 6.9 | 87 (94, 91) |
| Vitamin C mg/d (95% CI) | p-Value for Trend | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| EAR (mg) | 1999–2000 | 2001–2002 | 2003–2004 | 2005–2006 | 2007–2008 | 2009–2010 | 2011–2012 | 2013–2014 | 2015–2016 | 2017–2018 | ||
| Total population (age ≥ 1 y) | - | 97 (90, 105) | 94 (87, 100) | 88 (83, 94) | 86 (83, 89) | 84 (77, 91) | 86 (84, 89) | 83 (77, 90) | 78 (75, 80) | 77 (72, 81) | 75 (71, 80) | <0.001 |
| Age/sex groups | ||||||||||||
| 1–3 | 22 | 109 (95, 123) | 92 (86, 98) | 105 (93, 116) | 84 (75, 94) | 102 (91, 112) | 81 (74, 88) | 85 (71, 99) | 81 (75, 88) | 68 (61, 76) | 74 (63, 84) | <0.001 |
| 4–8 | 39 | 93 (85, 101) | 80 (71, 90) | 91 (83, 99) | 80 (70, 91) | 86 (77, 94) | 79 (71, 86) | 84 (76, 92) | 72 (66, 79) | 67 (55, 78) | 79 (68, 90) | <0.001 |
| 9–13, female | 56 | 77 (68, 87) | 82 (71, 92) | 84 (74, 94) | 76 (66, 86) | 67 (53, 81) | 73 (62, 85) | 69 (58, 80) | 64 (57, 72) | 64 (59, 68) | 80 (62, 98) | 0.08 |
| 9–13, male | 63 | 81 (68, 94) | 81 (69, 92) | 77 (67, 87) | 73 (63, 83) | 87 (73, 101) | 68 (55, 81) | 80 (70, 90) | 80 (69, 92) | 73 (61, 84) | 70 (56, 83) | 0.21 |
| 14–18, female | 60 | 91 (84, 99) | 78 (63, 92) | 77 (68, 86) | 74 (64, 84) | 77 (65, 89) | 73 (62, 85) | 59 (54, 64) | 65 (54, 76) | 66 (54, 79) | 55 (46, 63) | <0.001 |
| 14–18, male | 75 | 107 (89, 125) | 97 (84, 110) | 106 (80, 132) | 98 (87, 108) | 79 (69, 90) | 98 (83, 114) | 96 (58, 135) | 79 (66, 92) | 70 (60, 80) | 71 (54, 88) | <0.001 |
| 19–30, female | 60 | 87 (76, 97) | 88 (77, 98) | 82 (70, 94) | 78 (71, 85) | 80 (66, 95) | 80 (72, 89) | 80 (69, 92) | 71 (66, 75) | 75 (65, 85) | 71 (62, 80) | 0.002 |
| 19–30, male | 75 | 100 (84, 116) | 123 (93, 154) | 94 (81, 108) | 106 (90, 121) | 96 (82, 111) | 101 (86, 116) | 96 (78, 114) | 87 (75, 100) | 87 (75, 99) | 71 (61, 81) | <0.001 |
| 31–50, female | 60 | 87 (72, 102) | 82 (69, 96) | 85 (73, 96) | 76 (63, 89) | 75 (63, 87) | 80 (71, 88) | 76 (68, 84) | 74 (66, 82) | 73 (64, 82) | 74 (67, 82) | 0.028 |
| 31–50, male | 75 | 109 (96, 122) | 107 (89, 125) | 99 (84, 115) | 95 (87, 103) | 95 (83, 108) | 97 (85, 108) | 86 (73, 99) | 76 (70, 82) | 84 (74, 95) | 85 (72, 98) | <0.001 |
| 51–70, female | 60 | 101 (89, 112) | 94 (87, 101) | 78 (68, 87) | 78 (71, 85) | 82 (72, 91) | 91 (78, 105) | 76 (69, 82) | 75 (69, 80) | 74 (66, 82) | 70 (62, 77) | <0.001 |
| 51–70, male | 75 | 109 (96, 122) | 101 (92, 110) | 87 (80, 94) | 98 (89, 108) | 85 (75, 95) | 91 (84, 98) | 99 (83, 114) | 83 (75, 90) | 83 (73, 93) | 81 (72, 90) | <0.001 |
| ≥71, female | 60 | 94 (85, 103) | 85 (75, 94) | 83 (76, 89) | 81 (75, 88) | 74 (68, 80) | 78 (72, 85) | 81 (71, 92) | 85 (78, 92) | 76 (64, 87) | 75 (63, 87) | 0.031 |
| ≥71, male | 75 | 112 (99, 125) | 90 (82, 99) | 87 (79, 96) | 98 (84, 112) | 86 (78, 95) | 89 (75, 103) | 83 (69, 96) | 97 (85, 109) | 88 (74, 101) | 85 (71, 99) | 0.06 |
| Vitamin C mg/d (95% CI) | p-Value for Trend | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| 1999–2000 | 2001–2002 | 2003–2004 | 2005–2006 | 2007–2008 | 2009–2010 | 2011–2012 | 2013–2014 | 2015–2016 | 2017–2018 | ||
| Unadjusted | 97 (90, 105) | 94 (87, 100) | 88 (83, 94) | 86 (83, 89) | 84 (77, 91) | 86 (84, 89) | 83 (77, 90) | 78 (75, 80) | 77 (72, 81) | 75 (71, 80) | <0.001 |
| Age-adjusted | 97 (90, 105) | 94 (88, 100) | 88 (83, 94) | 86 (83, 90) | 84 (77, 91) | 86 (84, 89) | 83 (77, 90) | 78 (75, 80) | 76 (72, 81) | 75 (71, 79) | <0.001 |
| Age/sex-adjusted | 97 (90, 105) | 94 (88, 100) | 88 (83, 94) | 86 (83, 90) | 84 (77, 92) | 86 (84, 89) | 83 (77, 90) | 77 (75, 80) | 76 (72, 81) | 75 (71, 80) | <0.001 |
| Age/sex/race adjusted | 98 (91, 105) | 94 (89, 100) | 89 (84, 94) | 87 (83, 90) | 85 (78, 91) | 86 (84, 89) | 83 (77, 89) | 77 (75, 80) | 76 (71, 80) | 74 (70, 79) | <0.001 |
| Energy- adjusted | 94 (87, 101) | 90 (84, 96) | 84 (78, 89) | 83 (79, 86) | 83 (76, 90) | 85 (82, 87) | 80 (74, 87) | 76 (74, 78) | 76 (71, 80) | 73 (69, 77) | <0.001 |
| Fully-adjusted | 94 (88, 101) | 91 (85, 96) | 84 (80, 89) | 83 (79, 87) | 83 (77, 89) | 85 (82, 87) | 79 (73, 86) | 75 (73, 78) | 74 (70, 79) | 72 (67, 76) | <0.001 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Brauchla, M.; Dekker, M.J.; Rehm, C.D. Trends in Vitamin C Consumption in the United States: 1999–2018. Nutrients 2021, 13, 420. https://doi.org/10.3390/nu13020420
Brauchla M, Dekker MJ, Rehm CD. Trends in Vitamin C Consumption in the United States: 1999–2018. Nutrients. 2021; 13(2):420. https://doi.org/10.3390/nu13020420
Chicago/Turabian StyleBrauchla, Mary, Mark J. Dekker, and Colin D. Rehm. 2021. "Trends in Vitamin C Consumption in the United States: 1999–2018" Nutrients 13, no. 2: 420. https://doi.org/10.3390/nu13020420
APA StyleBrauchla, M., Dekker, M. J., & Rehm, C. D. (2021). Trends in Vitamin C Consumption in the United States: 1999–2018. Nutrients, 13(2), 420. https://doi.org/10.3390/nu13020420






