Abstract
Optimal therapy of biochemically relapsed prostate cancer (BRPC) after local treatment is elusive. An established modified citrus pectin (PectaSol®, P-MCP), a dietary polysaccharide, is an established antagonist of galectin-3, a carbohydrate-binding protein involved in cancer pathogenesis. Based on PSA dynamics, we report on the safety and the primary outcome analysis of a prospective phase II study of P-MCP in non-metastatic BRPC based. Sixty patients were enrolled, and one patient withdrew after a month. Patients (n = 59) were given P-MCP, 4.8 grams X 3/day, for six months. The primary endpoint was the rate without PSA progression and improved PSA doubling time (PSADT). Secondary endpoints were the rate without radiologic progression and toxicity. Patients that did not progress by PSA and radiologically at six months continued for an additional twelve months. After six months, 78% (n = 46) responded to therapy, with a decreased/stable PSA in 58% (n = 34), or improvement of PSADT in 75% (n = 44), and with negative scans, and entered the second twelve months treatment phase. Median PSADT improved significantly (p = 0.003). Disease progression during the first 6 months was noted in only 22% (n = 13), with PSA progression in 17% (n = 10), and PSA and radiologic progression in 5% (n = 3). No patients developed grade 3 or 4 toxicity.
1. Introduction
With over 207,000 newly diagnosed cases in the U.S. annually, prostate cancer is the second most widespread cancer in men in the U.S. [1]. While localized treatment modalities often cure patients with localized disease, approximately 30% demonstrate biochemical relapse at ten years. The ideal management of these patients remains elusive at present. Radiation treatment given for suspected recurrent malignant disease after a period of observation after prostatectomy, also known as salvage radiation therapy (SRT), provides long-term benefits in some patients, and the use of androgen deprivation treatment (ADT) continues to be debatable [2]. While ADT effectively reduces serum PSA levels in the majority of patients, its long-term benefits on survival and quality of life remain unclear. Data emphasize the incidence of accumulative toxicities with ADT, which may offset any potential survival benefit from early intervention and impact the life quality [3].
The natural history of men with biochemically relapsed, non-castrate prostate cancer is quite mixed. They may remain asymptomatic and free of clinical evidence of disease for many years [4]. Extensive data on patients’ natural history of relapsing after surgery and after curative radiotherapy indicate that the PSA doubling time (PSADT) predicts the probability of metastasis-free and prostate cancer-specific survival [5,6,7,8,9,10,11]. PSADT of <3 months, 3.00-8.99 months, and ≥nine months may be associated with poor, intermediate, and good prognosis in disease progression and development of overt metastatic disease. Furthermore, the Prostate-Specific Antigen Working Group’s guidelines on PSADT determined that clinical evidence supports PSADT as a predictive marker of cancer progression among post-local therapy prostate cancer patients experiencing biochemical recurrence [12]. Thus, PSADT has been used in our study design to define endpoints.
Evaluating new compounds in this patient population remains a challenge because of the lack of validated methodology. The time required until conventional clinical and radiological endpoints occur is often lengthy. Knowing PSADT and other dynamics of PSA levels in predicting the outcome of this population, changes in doubling time observed during treatment have been a popular approach applied in clinical studies designed for screening potentially active compounds [4,13,14].
PectaSol® Modified Citrus Pectin (P-MCP; ecoNugenics Inc, Santa Rosa, CA, USA) is derived from the pith of citrus fruit peels and treated with enzymes, pH, and temperature. It is an orally administered competitive inhibitor of galectin-3 (Gal-3), a carbohydrate-binding protein involved in cancer pathogenesis. P-MCP is a dietary supplement form of pectin comprised of low-molecular-weight and low degree of esterification to allow absorption from the small intestinal epithelium into the circulation. Untreated pectin fibers are too long and large in structure. Thus, they are indigestible dietary fibers that pass through the gastrointestinal tract. Pectin is classified by the US-FDA as generally regarded as safe (GRAS). P-MCP produces pleiotropic effects, including but not limited to its antagonism of Gal-3, which have shown benefit in preclinical and clinical studies. Preclinical and clinical data suggest that P-MCP is active in prostate cancer patients [15,16,17]. Specifically, in cancer, P-MCP modulates several rate-limiting steps of the metastatic cascade [18]. P-MCP can also affect cancer cell resistance to chemotherapy and sensitivity to radiation. In addition, studied in fibrotic diseases, P-MCP modulates many of the steps involved in the pathogenesis of organ fibrosis and reduces fibrosis to the kidney, heart, liver, and adipose tissue. Other benefits of MCP include detoxification, anti-inflammatory, antioxidant, and improved immune function [18].
The exceptionally low incidence of toxicities and possible clinical effect of P-MCP supports further testing of this compound. In addition, P-MCP’s mechanisms of action would suggest that this compound may be particularly interesting for delaying progression in a group of patients with relatively low disease burden states, such as in the non-metastatic biochemically relapsed paradigm. To evaluate P-MCP’s clinical activity in this early disease state, we employed previously reported methodology [4,13,14] for appraising the safety and preliminary efficacy of non-hormonal compounds on the progression of relapsed, non-metastatic prostate cancer patients. The results (primary outcome analysis) of our prospective phase II study are reported.
2. Materials and Methods
2.1. Inclusion Criteria
Eligible patients were ≥21 years old and had histologically proven prostatic adenocarcinoma. All participants had undergone radical prostatectomy and/or external beam radiation therapy, or brachytherapy, with, subsequently, a confirmed rising serum PSA level (in at least three consecutive tests, at least two weeks apart) of ≥0.2 ng/mL after radical prostatectomy or ≥2 ng/mL above nadir after radiation therapy. Patients’ participation required no evidence of locoregional or distant metastasis determined by a positron emission tomography (PET) prostate-specific membrane antigen (PSMA) scan. All previous local treatment modalities, including radiation and surgery, were completed at least three months before treatment in this study. Patients with prior systemic treatment with androgen deprivation therapy (ADT), experimental drugs, high-dose steroids, or other cancer treatments were discontinued at least six months before study admission. All patients had a normal level of serum testosterone > 150 ng/mL, and adequate bone marrow (absolute neutrophil count ≥ 1.5 × 103/L, platelet count ≥ 100 × 103/L), renal (creatinine ≤ 2.5 times the normal upper serum limit), and liver (total bilirubin ≤ 1.5 mg/dL, aspartate aminotransferase (AST) and alanine transaminase (ALT) ≤ 2 × upper limit of normal range) functions. In addition, all patients had an Eastern Cooperative Oncology Group (ECOG) performance status ≤ 2, a life expectancy > 6 months at study entry. Men were excluded if they had an uncontrolled intercurrent illness that limited study compliance. All participating patients signed an institutional review board (IRB)-approved consent form. Clinical Registry; NCT01681823; https://clinicaltrials.gov/ct2/show/NCT01681823, accessed on 22 November 2021.
Study participants were recruited from five medical centers in Israel (Meir, Rabin, Rambam, Soroka, and Tel-Aviv Sourasky). The sponsor provided P-MCP (PectaSol-C®, EcoNugenics, Inc., Santa Rosa, CA, USA) to be orally taken at 4.8 grams × 3/day given to patients in packs of 270 capsules. An illustration of the study design is in Figure 1.
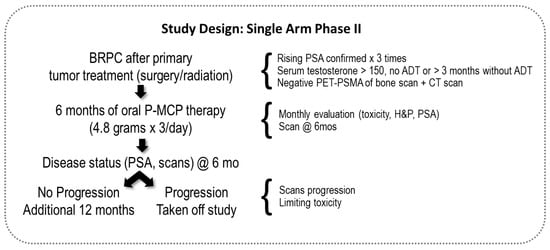
Figure 1.
Study design. BRPC (Biochemically Relapsed Prostate Cancer); P-MCP (PectaSol® Modified Citrus Pectin); @ 6mo (at six months); ADT (Androgen Deprivation Treatment); PET-PSMA (Positron Emission Tomography-Prostate-Specific Membrane Antigen Scan; CT (Computed Tomography Scan); H&P (History and Physical).
2.2. Toxicity and Disease Status at Follow-Up Monthly Assessments
Patients were evaluated for toxicities, physical exams, serum PSA, testosterone, CRP, and galectin-3 levels. Complete assessments of disease status included positron emission tomography PET–PSMA scan after six months in patients without clinical or PSA progression or earlier upon clinical or PSA progression.
2.3. Treatment Duration
The treatment continued until biochemical or clinical disease progression or dose-limiting toxicity. Biochemical progression was characterized as a ≥25% increase of PSA level at six months over the baseline, without a PSADT prolongation. Clinical disease progression is defined as any new monthly evidence of progression upon a digital rectal examination or scans at six months, suggestive of local or distant disease recurrence. The duration time was defined as the time from treatment initiation to the first observation of a termination event, death by any cause, or discontinuation of treatment for any reason. Patients without evidence of disease progression (PSA and/or radiologically) or dose-limiting toxicity after six months were given an additional twelve months of treatment.
2.4. Safety Evaluation of Toxicity
Toxicity was defined according to the NCI Common Toxicity Criteria. Treatment would be stopped for a patient with grade 3–4 toxicity. At that point, patients would be followed weekly until ≤grade 1 and then reinitiate treatment. Therapy would be stopped upon the recurrence of grade 3/4 events and for any toxicity requiring more than four weeks to recover to ≤grade 1.
2.5. Statistical Analysis
The analysis was performed using the first six months of administration with the investigational supplement. This study’s primary efficacy endpoint was the rate of patients without PSA progression (defined as an increase of ≥25% from baseline) and/or patients with improvement (lengthening) of PSADT versus baseline. PSADT calculation used the natural log of two divided by the slope found from measuring a linear regression with the natural log of PSA against time (months). All the available PSA measurements in the year before patient enrollment were used to calculate baseline pre-treatment PSADT. The post-baseline PSADT was calculated using PSA levels obtained at baseline and monthly during treatment. Secondary endpoints were the rate of patients without radiologic progression, toxicity, and treatment benefits according to the PSADT risk grouping (e.g., poor < 3 months, intermediate 3–8.99 months, and good ≥ nine months).
A cohort size of sixty patients provided 85% statistical power was used to evaluate the decrease in PSA progression rate at six months, from 80% (reported data about the natural history of PSA dynamics without active therapy) [4] to 40% (with P-MCP therapy), and PSADT improvement (lengthening) rate from 25% (reported natural history without active treatment) [19] to 50% (with P-MCP therapy).
Comparisons between pre-and post-treatment parameters and within groups were analyzed by Wilcoxon Signed Rank for abnormally distributed data or a two-tailed Student t-test for normally distributed data, with results reported as a number, percentage, mean or median, and standard deviation (SD).
3. Results
3.1. Patients
Seventy-five (n = 75) patients were assessed for inclusion. Fifteen patients were considered to be out of the inclusion criteria. The reasons for exclusion were metastatic disease (n = 13) and lack of a confirmed rise in PSA (n = 2). Thus, sixty eligible patients (median age 74 years, range 53–89 years) were included. The primary tumor treatment consisted of surgery in 13% (n = 8), radiation in 57% (n = 34), and both in 30% (n = 18). Patients with PSA progression by the present study criteria (i.e., an increase of ≥25% from baseline) within the six months before treatment initiation was noted in 88% (n = 53). The characteristics of the patients is in Table 1.

Table 1.
Summary of the pre-treatment patient characteristics.
3.2. Toxicity and Compliance
No patients with severe grade 3/4 toxicity were reported. Twenty percent (n = 12) had grade 1 toxicity (bloating) that was transient and reversible and did not require treatment discontinuation. One patient (with a baseline intermediate-risk PSADT) withdrew consent after one month. Of the remaining 59 patients, after six months, 78% (n = 46) responded to therapy with a decrease or stabilization of PSA, and/or improvement (lengthening) of PSADT, and with negative scans, and entered the second 12 months treatment phase. Specifically, versus baseline pre-treatment, 75% (n = 44) had improvement (lengthening) of PSADT, and 58% (n = 34) had a stabilization/decrease of PSA. Median PSADT improved significantly (p = 0.003), with a median (range) pretreatment PSADT of 9.12 (1.4–55) months versus a median (range) post-treatment PSADT of 15.2 (1.4–677.0) months. Table 2 and Figure 2 summarize treatment characteristics and response for prostate-specific antigen level, doubling time changes, and disease progression.

Table 2.
Treatment characteristics and response at 6 months.
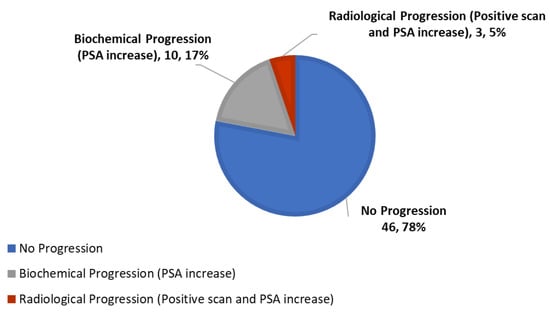
Figure 2.
Response to therapy, no progression defined as a decreased/stable PSA and/or improvement of PSADT (n, %).
3.3. Analysis of the PSADT
The benefits of therapy in terms of PSA stabilization (no change in level)/decrease and/or PSADT lengthening (% of patients and median) were seen in all PSADT risk groups (Table 2). In addition, there was a favorable change of the PSADT risk grouping during therapy (Table 2, Figure 3), with a decrease in the number of patients with a poor (<3 months) and intermediate PSADT (3.00–8.99 months) risk from 48% (n = 29) before therapy to 29% (n = 17) after therapy and an increase of the number of patients with a good risk PSADT (≥9.00) from 52% (n = 31) before therapy to 71% (n = 42) after therapy.
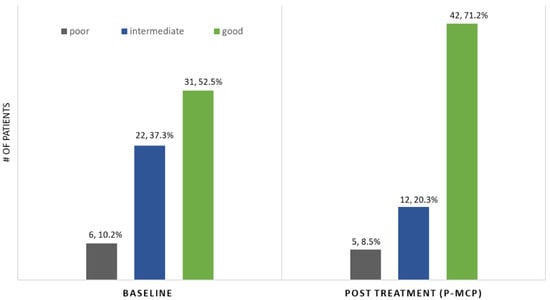
Figure 3.
PSADT risk grouping: pre- versus post-P-MCP (n, %).
Overall, 27% of patients (n = 16) favorably changed their PSADT risk grouping. Specifically, 55% (n = 12/22) of patients with baseline intermediate PSADT risk grouping (3–8.99 months) improved it to a good risk (≥nine months), and 66% (n = 4/6) of patients with baseline poor PSADT risk grouping (<3 months) improved it to intermediate risk (Figure 4).
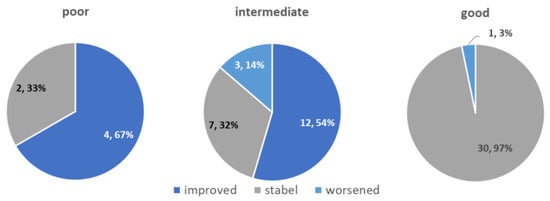
Figure 4.
Post-P-MCP treatment change of PSADT in different pre-treatment PSADT risk groups (n, %).
A subgroup analysis of the PSADT risk grouping (Table 1 and Table 2) revealed a significant change of median PSADT after P-MCP therapy (versus baseline) in patients with good (median PSADT 20.4 versus 14.7 months, p = 0.0006) and intermediate (6.5 versus 5.21 months, p = 0.0025) risk.
Disease progression during the first six months of therapy was noted in only 22% (n = 13), with PSA progression (an increase of ≥25% from baseline) only (without radiographic progression) in 17% (n = 10), and both PSA and radiological progression in 5% (n = 3). Of note, in all, three patients with a radiographic progression, on-treatment PSA progression (an increase of ≥25% from baseline), and no lengthening of PSADT were observed.
4. Discussion
This clinical trial evaluated the feasibility, safety, and benefit of P-MCP in prostate cancer patients with increasing PSA levels following radiation or radical prostatectomy. The study met its primary objective, with 58% of patients without PSA progression and 75% with lengthening of PSADT versus baseline. Furthermore, the rates of patients without PSA progression and with PSADT lengthening were observed, regardless of the baseline PSADT risk grouping. Again, under P-MCP therapy, most patients with a baseline poor or intermediate risk PSADT improved their PSADT risk grouping (i.e., changed from poor to intermediate and intermediate to good). In addition, only 5% of patients had a meaningful disease progression (radiological) under therapy. Finally, a subgroup analysis of the PSADT risk groups revealed a significant change of PSADT (post-P-MCP therapy versus baseline) in patients with intermediate and good risk. At present, such an effect in the small (n = 6) poor-risk group could be observed, and further studies with a more substantial number of men with poor-risk PSADT are needed to confirm such an effect.
Since the eligible patients have no other evidence of active disease at the time of enrollment, according to previously reported clinical trials in such patients [4,14], we relied on PSA dynamics changes as a potential signal for antitumor activity. Based on prior data, any expression of PSA dynamics (e.g., PSADT, PSA slopes) represents the strongest prognosticator in this population [4,11]. Although the number is small, and no definitive conclusions can be drawn, in all three patients with on-treatment radiological disease progression in the present study, on treatment PSA progression and no lengthening of PSADT were observed (in accordance with data suggesting that the endpoints of PSA dynamics and PSADT are in correlation with disease control).
The sample size was computed to identify a 50% decrease in the rate of disease progression observed at six months, from 80% to 40%. This endpoint was selected based on preceding data in this patient cohort, indicating that 80% of the eligible patients for this study would continue to demonstrate evidence of progression at 6-months without treatment [4]. While the 50% decrease in progression rate at 6-months has not been validated in relation to clinically relevant events (for example, bone metastasis or survival), it was used as an endpoint in previous studies in this patient population [4]. Therefore, we feel that this represents a realistic choice of potential clinical significance to employ in initial screening for a signal of activity. Additional validation of this approach will require specially designed phase III trials.
The incidence and severity of adverse drug-related reactions were modest and reversible, and most patients stayed on treatment per protocol. These findings are consistent with the FDA classification of P-MCP as GRAS and support that this compound is appropriate for long-term treatment.
The observations of PSA stabilization/response and lengthening of PSADT in patients treated with P-MCP are consistent with prior preclinical and clinical data. The extracellular galectin-3 protein participates in the tumorigenesis process by various mechanisms, including inflammation, cellular proliferation, angiogenesis, and progression to an overt metastatic state via cancer cell–endothelial adhesion in distant organs. Elevated galectin-3 serum level was reported in prostate cancer patients [16,17,18,19,20,21,22,23,24,25,26]. P-MCP is an oral competitive inhibitor of galectin-3, and preliminary preclinical and clinical data suggest that it is active in patients with prostate cancer [17,18].
The major limitation of our study is the lack of a placebo arm. A placebo arm was considered; however, given the perceived positivity of P-MCP, a placebo control was felt to pose difficulties for patient accrual. Furthermore, although retrospective studies have shown that PSADT is a strong predictor of metastasis-free survival [11] and overall survival [7,9], or both [19,27], another limitation is whether changes in PSA and PSADT are acceptable endpoints for clinical trials in this patient population.
5. Conclusions
The present study suggests that P-MCP in BRPC has a potential benefit and is safe, as evident by changes in PSADT, lower than expected rates of disease progression compared to historical data, and no significant toxicity. The exceptionally low incidence of toxicities and possible clinical activity of P-MCP observed in the present study supports further testing of this compound in this patient population. Furthermore, P-MCP’s mechanisms of action suggest that this compound may be particularly interesting for delaying disease progression in a group of patients with relatively low disease burden states, such as in the non-metastatic biochemically relapsed prostate cancer. For more definitive conclusions regarding the efficacy of P-MCP in this patient population, further testing in prospective randomized studies evaluating more conventional disease endpoints is warranted.
Author Contributions
D.K., M.F., A.P.: Investigation, I.K., E.R., D.S., I.L., R.M., O.Y., D.M., I.W., R.G., H.D., K.R., N.R., I.E., D.K.: Conceptualization, Methodology, Investigation, Formal analysis, Writing—Original Draft, Review & Editing, Project administration, Supervision. M.F.: Conceptualization, Investigation, A.P.: Investigation. I.K.: Investigation. E.R.: Investigation. D.S.: Investigation. I.L.: Investigation. R.M.: Investigation. O.Y.: Investigation. D.M.: Investigation. I.W.: Investigation. R.G.: Investigation. K.R.: Investigation. N.R.: Investigation. I.E.: Conceptualization, Methodology, Investigation, Formal analysis, Writing Original Draft, Review & Editing, Project administration, Supervision. All authors have read and agreed to the published version of the manuscript.
Funding
This research was provided by EcoNugenics, Inc., Santa Rosa, CA, USA.
Institutional Review Board Statement
The study was conducted according to the guidelines of the Declaration of Helsinki and approved by the Institutional Review Board (IRB) committee of our institutions. The study was registered at clinicaltrials.gov (NCT01681823).
Informed Consent Statement
Written informed consent was obtained from all subjects involved in the study.
Data Availability Statement
Provided upon request.
Acknowledgments
The authors acknowledge ecoNugenics, Inc. (Santa Rosa, CA, USA) for providing P-MCP and funding support. Anat Stern and Barry Wilk for their assistance in the study and manuscript editing.
Conflicts of Interest
IE discloses being the developer of the sponsoring dietary supplement company. The other authors declare no potential conflict of interest.
References
- Siegel, R.L.; Miller, K.D.; Jemal, A. Cancer Statistics. Cancer J. Clin. 2019, 69, 7–34. [Google Scholar] [CrossRef] [Green Version]
- Artibani, W.; Porcaro, A.B.; De Marco, V.; Cerruto, M.A.; Siracusano, S. Management of Biochemical Recurrence after Primary Curative Treatment for Prostate Cancer: A Review. Urol. Int. 2017, 100, 251–262. [Google Scholar] [CrossRef]
- Keating, N.L.; O’Malley, A.J.; Smith, M.R. Diabetes and Cardiovascular Disease During Androgen Deprivation Therapy for Prostate Cancer. J. Clin. Oncol. 2006, 24, 4448–4456. [Google Scholar] [CrossRef]
- Keizman, D.; Zahurak, M.; Sinibaldi, V.; Carducci, M.; Denmeade, S.; Drake, C.; Pili, R.; Antonarakis, E.S.; Hudock, S.; Eisenberger, M. Lenalidomide in Nonmetastatic Biochemically Relapsed Prostate Cancer: Results of a Phase I/II Double-Blinded, Randomized Study. Clin. Cancer Res. 2010, 16, 5269–5276. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pound, C.; Partin, A.; Eisenberger, M.; Chan, D.W.; Pearson, J.D.; Walsh, P.C. Natural history of progression after PSA elevation following radical prostatectomy. JAMA 1999, 281, 1591–1597. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zelefsky, M.J.; Ben-Porat, L.; Scher, H.I.; Chan, H.M.; Fearn, P.A.; Fuks, Z.Y.; Leibel, S.A.; Venkatraman, E. Outcome Predictors for the Increasing PSA State After Definitive External-Beam Radiotherapy for Prostate Cancer. J. Clin. Oncol. 2005, 23, 826–831. [Google Scholar] [CrossRef] [PubMed]
- Freedland, S.J.; Humphreys, E.B.; Mangold, L.A.; Eisenberger, M.; Dorey, F.J.; Walsh, P.C.; Partin, A.W. Risk of prostate cancer-specific mortality following biochemical recurrence after radical prostatectomy. JAMA 2005, 294, 433–439. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Antonarakis, E.S.; Feng, Z.; Trock, B.J.; Humphreys, E.B.; Carducci, M.A.; Partin, A.W.; Walsh, P.C.; Eisenberger, M.A. The natural history of metastatic progression in men with prostate-specific antigen recurrence after radical prostatectomy: Long-term follow-up. BJU Int. 2012, 109, 32–39. [Google Scholar] [CrossRef] [PubMed]
- D’Amico, A.V.; Moul, J.W.; Carroll, P.R.; Sun, L.; Lubeck, D.; Chen, M.H. Surrogate end point for prostate cancer-specific mortality after radical prostatectomy or radiation therapy. J. Natl. Cancer Inst. 2003, 95, 1376–1383. [Google Scholar] [CrossRef]
- Zhou, P.; Chen, M.-H.; McLeod, D.; Carroll, P.R.; Moul, J.W.; D’Amico, A.V. Predictors of Prostate Cancer–Specific Mortality After Radical Prostatectomy or Radiation Therapy. J. Clin. Oncol. 2005, 23, 6992–6998. [Google Scholar] [CrossRef]
- Antonarakis, E.S.; Zahurak, M.L.; Lin, J.; Keizman, D.; Carducci, M.A.; Eisenberger, M.A. Changes in PSA kinetics predict metastasis-free survival in men with PSA-recurrent prostate cancer treated with nonhormonal agents. Cancer 2011, 118, 1533–1542. [Google Scholar] [CrossRef] [Green Version]
- Arlen, P.M.; Bianco, F.; Dahut, W.L.; D’Amico, A.; Figg, W.D.; Freedland, S.J.; Gulley, J.L.; Kantoff, P.W.; Kattan, M.W.; Lee, A.; et al. Prostate specific antigen working group guidelines on prostate specific antigen doubling time. J. Urol. 2008, 179, 2181–2185. [Google Scholar] [CrossRef] [Green Version]
- Rosenbaum, E.; Zahurak, M.; Sinibaldi, V.; Carducci, M.A.; Pili, R.; Laufer, M.; Deweese, T.L.; Eisenberger, M.A. Marimastat in the Treatment of Patients with Biochemically Relapsed Prostate Cancer: A Prospective Randomized, Double-Blind, Phase I/II Trial. Clin. Cancer Res. 2005, 11, 4437–4443. [Google Scholar] [CrossRef] [Green Version]
- Paller, C.J.; Ye, X.; Wozniak, P.J.; Gillespie, B.K.; Sieber, P.R.; Greengold, R.H.; Stockton, B.R.; Hertzman, B.L.; Efros, M.D.; Roper, R.P.; et al. A randomized phase II study of pomegranate extract for men with rising PSA following initial therapy for localized prostate cancer. Prostate Cancer Prostatic Dis. 2012, 16, 50–55. [Google Scholar] [CrossRef]
- Conti, S.; Vexler, A.; Hagoel, L.; Kalich-Philosoph, L.; Corn, B.W.; Honig, N.; Shtraus, N.; Meir, Y.; Ron, I.; Eliaz, I.; et al. Modified Citrus Pectin as a Potential Sensitizer for Radiotherapy in Prostate Cancer. Integr. Cancer Ther. 2018, 17, 1225–1234. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pienta, K.J.; Naik, H.; Akhtar, A.; Yamazaki, K.; Replogle, T.S.; Lehr, J.; Donat, T.L.; Tait, L.; Hogan, V.; Raz, A. Inhibition of spontaneous metastasis in a rat prostate cancer model by oral administration of modified citrus pectin. J. Natl. Cancer Inst. 1995, 87, 348–353. [Google Scholar] [CrossRef]
- Guess, B.W.; Scholz, M.C.; Strum, S.B.; Lam, R.Y.; Johnson, H.J.; Jennrich, R.I. Modified citrus pectin (MCP) increases the prostate-specific antigen doubling time in men with prostate cancer: A phase II pilot study. Prostate Cancer Prostatic Dis. 2003, 6, 301–304. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Eliaz, I.; Raz, A. Pleiotropic Effects of Modified Citrus Pectin. Nutrients 2019, 11, 2619. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Antonarakis, E.S.; Chen, Y.; Elsamanoudi, S.I.; Brassell, S.A.; Da Rocha, M.V.; Eisenberger, M.A.; McLeod, D.G. Long-term overall survival and metastasis-free survival for men with prostate-specific antigen-recurrent prostate cancer after prostatectomy: Analysis of the Center for Prostate Disease Research National Database. BJU Int. 2010, 108, 378–385. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Harazono, Y.; Kho, D.H.; Balan, V.; Nakajima, K.; Hogan, V.; Raz, A. Extracellular galectin-3 programs multidrug resistance through Na+/K+-ATPase and P-glycoprotein signaling. Oncotarget 2015, 6, 19592–19604. [Google Scholar] [CrossRef] [Green Version]
- Balan, V.; Nangia-Makker, P.; Kho, D.H.; Wang, Y.; Raz, A. Tyrosine-phosphorylated Galectin-3 Protein Is Resistant to Prostate-specific Antigen (PSA) Cleavage. J. Biol. Chem. 2012, 287, 5192–5198. [Google Scholar] [CrossRef] [Green Version]
- Glinskii, O.V.; Sud, S.; Mossine, V.V.; Mawhinney, T.P.; Anthony, D.C.; Glinsky, G.V.; Pienta, K.J.; Glinsky, V.V. Inhibition of Prostate Cancer Bone Metastasis by Synthetic TF Antigen Mimic/Galectin-3 Inhibitor Lactulose-l-Leucine. Neoplasia 2012, 14, 65–73. [Google Scholar] [CrossRef] [Green Version]
- Nakajima, K.; Kho, D.H.; Yanagawa, T.; Harazono, Y.; Gao, X.; Hogan, V.; Raz, A. Galectin-3 Inhibits Osteoblast Differentiation through Notch Signaling. Neoplasia 2014, 16, 939–949. [Google Scholar] [CrossRef] [Green Version]
- Nakajima, K.; Kho, D.H.; Yanagawa, T.; Harazono, Y.; Hogan, V.; Chen, W.; Ali-Fehmi, R.; Mehra, R.; Raz, A. Galectin-3 Cleavage Alters Bone Remodeling: Different Outcomes in Breast and Prostate Cancer Skeletal Metastasis. Cancer Res. 2016, 76, 1391–1402. [Google Scholar] [CrossRef] [Green Version]
- Nakajima, K.; Kho, D.H.; Yanagawa, T.; Zimel, M.; Heath, E.; Hogan, V.; Raz, A. Galectin-3 in bone tumor microenvironment: A beacon for individual skeletal metastasis management. Cancer Metastasis Rev. 2016, 35, 333–346. [Google Scholar] [CrossRef] [PubMed]
- Nakajima, K.; Heilbrun, L.K.; Hogan, V.; Smith, D.; Heath, E.; Raz, A. Positive associations between galectin-3 and PSA levels in prostate cancer patients: A prospective clinical study-I. Oncotarget 2016, 7, 82266–82272. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Paller, C.J.; Olatoye, D.; Xie, S.; Zhou, X.; Denmeade, S.R.; Eisenberger, M.A.; Antonarakis, E.S.; Carducci, M.A.; Rosner, G.L. The effect of the frequency and duration of PSA measurement on PSA doubling time calculations in men with biochemically recurrent prostate cancer. Prostate Cancer Prostatic Dis. 2013, 17, 28–33. [Google Scholar] [CrossRef] [PubMed] [Green Version]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).