Abstract
Background: Vitamin C is a water-soluble antioxidant vitamin. Oxidative stress and its markers, along with inflammatory markers, are high during critical illness. Due to conflicting results of the published literature regarding the efficacy of vitamin C in critically ill patients, and especially the concerns for nephrotoxicity raised by some case reports, this meta-analysis was carried out to appraise the evidence and affirmation regarding the role of vitamin C in critically ill patients. Methods: We searched the database thoroughly to collect relevant studies that assessed intravenous vitamin C use in critically ill patients published until 25 February 2021. We included randomized controlled trials and observational studies with 20 or more critically ill patients who have received intravenous ascorbic acid (vitamin C). After screening 18,312 studies from different databases, 53 were included in our narrative synthesis, and 48 were included in the meta-analysis. We used the Covidence software for screening of the retrieved literature. Review Manager (RevMan) 5.4 was used for the pooling of data and Odds Ratios (OR) and Mean difference (MD) as measures of effects with a 95% confidence interval to assess for explanatory variables. Results: Pooling data from 33 studies for overall hospital mortality outcomes using a random-effect model showed a 19% reduction in odds of mortality among the vitamin C group (OR, 0.81; 95% CI, 0.66–0.98). Length of hospital stay (LOS), mortality at 28/30 days, ICU mortality, new-onset AKI and Renal Replacement Therapy (RRT) for AKI did not differ significantly across the two groups. Analysis of data from 30 studies reporting ICU stay disclosed 0.76 fewer ICU days in the vitamin C group than the placebo/standard of care (SOC) group (95% CI, −1.34 to −0.19). This significance for shortening ICU stay persisted even when considering RCTs only in the analysis (MD, −0.70; 95% CI, −1.39 to −0.02). Conclusion: Treatment of critically ill patients with intravenous vitamin C was relatively safe with no significant difference in adverse renal events and decreased in-hospital mortality. The use of vitamin C showed a significant reduction in the length of ICU stays in critically ill patients.
1. Introduction
Vitamin C (ascorbic acid) is a water-soluble essential vitamin synthesized by most plants and animals. Vitamin C and stress have long been associated, and previous research has shown that vitamin C reduces systemic inflammation, helps correct sepsis-induced coagulopathy, and prevents vascular injury [1,2,3]. Vitamin C has drawn substantial interest in critical care medicine, and several studies have been published, especially in the last five years, with intriguing but conflicting results. In a primary study by Fowler et al. [3] in 2014, vitamin C decreased the risk of organ failure in patients with a critical illness. However, the subsequent CITRIS-ALI trial failed to show benefit in organ dysfunction or suppress the inflammatory markers and vascular injury but reported a 28-day mortality benefit: 29.8% in the vitamin C group and 46.3% in the placebo group [4]. Marik et al. [5] showed a reduction in mortality and organ failure with vitamin C use among severe sepsis or septic shock patients. A study by Zabet et al. [6] in 2016 showed a reduction in the dose and duration of vasopressors medication use in surgical septic shock patients. A study by Nakajima et al. [7] in 2019 showed mortality benefit with high dose vitamin C use in patients with severe burn. Thus, vitamin C has been extensively studied in various critical care settings including medical, surgical, trauma and burn ICUs. Prior meta-analyses have shown a reduction in the duration of vasopressor and mechanical ventilation days [8,9], although a mortality benefit has not been seen [9,10,11,12]. Many studies have been published since the publication of the last meta-analyses by Wei et al. and Putzu et al. [10,11].
Thus, in order to fully appraise the available data, we sought to perform this systematic review and meta-analysis, including 53 studies with 352,395 critically ill patients, to evaluate the role of vitamin C, paying particular interest to the renal safety of vitamin C.
2. Methods
The protocol for this systematic review and meta-analysis was prepared and registered in PROSPERO, and the review was conducted according to the protocol’s predefined criteria (CRD42020222906) [13]. We abide by our study as per the standard Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) guidelines [14].
2.1. Search Strategy
We conducted a thorough literature search on PubMed, PubMed Central, Scopus and Embase to collect relevant studies published until 25 February 2021, reporting the use of intravenous vitamin C in critically ill patients. We used appropriate search words such as ascorbic acid, vitamin C, sepsis, septic shock, critical illness, intensive care unit, ICU, burn, ARDS and trauma using appropriate Boolean operators without any filters and language restrictions. Details of the electronic database search are available in Supplementary file S1.
2.2. Selection Criteria
Inclusion criteria:
Type of studies: randomized controlled trials and other observational studies, namely, cohort studies, case–control studies, cross-sectional studies and case series with 20 or more critically ill patients.
Population: Adult patient with a critical illness.
Intervention: Intravenous vitamin C alone or in combination with other antioxidants. The comparator includes standard of care or placebo.
Study outcome: Hospital mortality, 28/30-day mortality, ICU mortality, length of stay in ICU and hospital, the adverse renal outcome in the form of new-onset AKI and AKI requiring renal replacement therapy were our main outcomes of interest. We used Odds Ratios (OR) and mean differences (MD) as a measure of effects to assess the explanatory variables.
Exclusion criteria:
Types of studies: Any form of review including meta-analysis, narrative reviews, case reports, opinions, editorials, letter to the editor with no primary data, study protocols, conference abstracts/presentations, thesis dissertation and animal studies.
Full-text articles that are not retrievable.
Incomplete studies (still ongoing) or preliminary reports with no complete data available.
COVID-19 related studies.
2.3. Data Extraction
We used Covidence software to screen the literature imported from databases for the eligibility assessment [15]. Every citation was reviewed independently by two reviewers (S.K. and S.S.) for eligibility, and conflicts were resolved by a third reviewer (S.M.). After two phases of screening (title and abstract and full-text review), the data from selected studies were extracted in a Microsoft Excel sheet. The number of manuscripts chosen was divided across the reviewers. Each reviewer curated the data from assigned articles, which was later verified for accuracy and any discrepancies by other reviewers. The internal review was carried out thoroughly to ensure the correctness of the data curation among the outcomes of interest with no subjective errors.
2.4. Risk of Bias
We used the Cochrane Risk of Bias (ROB) 2.0 tool for randomized control trials and Joanna Briggs Institute (JBI) critical appraisal checklist for observational studies for quality and risk of bias assessment (Figure 1 and Table 1) [16,17]. We used Review Manager (RevMan) 5.4 for creating a summary of biases for RCTs [18].

Figure 1.
Cochrane ROB 2.0 of the included trials.

Table 1.
JBI Bias Assessment.
2.5. Statistical Analysis
Revman 5.4 was used to pool the data using Odds Ratio (OR) to estimate dichotomous outcome with a 95% Confident Interval (CI). Based on the level of heterogeneities, we used the fixed/random-effects model to pool the result. We used the mean differences (MD) between vitamin C and control groups for continuous variables. Where mean was not available in the study, mean and standard deviation (SD) were estimated using the sample size, median value and inter-quartile ranges [40].
2.6. Assessment of Heterogeneity
Based on the established recommendation for the statistical heterogeneity, we stratified heterogeneity as low, moderate and high to I2 values of 25, 50 and 75%, respectively [41]. Based on the calculated heterogeneity I2 test value, we used the random/fixed effect model for the analysis. We conducted sensitivity analysis by re-running the analysis to assess the hidden differences where appropriate.
3. Results
After electronic database searches, we retrieved 18,312 studies imported in Covidence, and 1248 duplicates were removed. After the duplicate check, we screened the 17,064 studies in a title and abstracts review, and we excluded 16,720 studies for not meeting the inclusion criteria. A total of 344 studies were filtered for full-text review, of which 291 studies were excluded for definite reasons. After a full-text review, we included 53 studies in the narrative review and 48 studies (27 randomized controlled trials and 21 observational studies) in the meta-analysis (Figure 2).
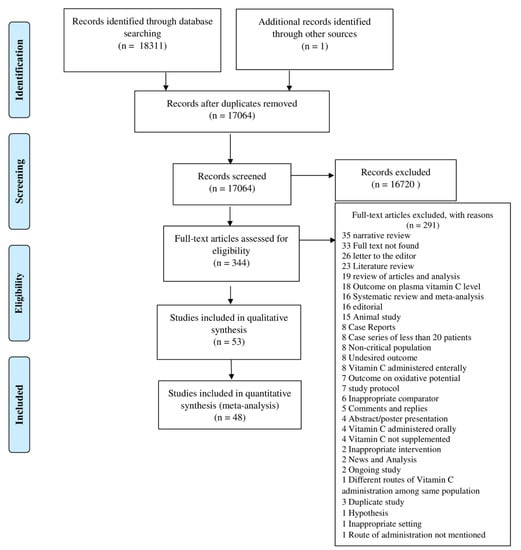
Figure 2.
PRISMA Flow Diagram.
3.1. Narrative Summary
A total of 53 studies were included in the narrative review; of them, 23 were observational studies, while 30 were RCTs (Table 2). Basic study details are presented in Supplementary file S2.

Table 2.
Narrative summary of included studies.
3.2. Quantitative Synthesis
3.2.1. Hospital Mortality
Pooling the data on hospital mortality from the 33 studies using a random effect model showed a 19% reduction in odds for hospital mortality (OR, 0.81; 95% CI, 0.66–0.98; n = 4740; I2 = 31%; p = 0.03). Considering the type of study running subgroup analysis showed that a 33% reduction in mortality was reported among the observational studies (OR 0.67, 95% CI 0.50–0.91; n = 2603; I2 = 50%; p = 0.009). However, pooling the hospital mortality outcome among only 15 RCTs could not establish such a relation (OR 0.97, 95% CI 0.77–1.23; n = 2137; I2 = 0%; p = 0.82) (Figure 3).
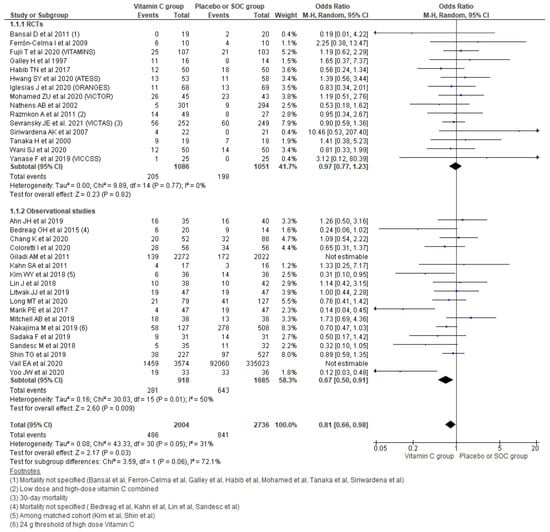
Figure 3.
Forest plot showing overall hospital mortality using random-effect model.
Sensitivity Analysis among RCTs
To further analyze the hospital mortality outcome among RCTs, we re-run the analysis based on the subgroups of critically ill patients as surgical and sepsis/septic shock. Neither among patients with sepsis/septic shock (OR, 0.98; 95% CI, 0.76–1.26; n = 1297; I2 = 0%; p = 0.86) nor among surgical patients (OR, 1.08; 95% CI, 0.63–1.86; n = 860; I2 = 4%) was a significant difference for hospital mortality observed while comparing vitamin C and placebo or SOC groups (Supplementary file S3, Figure S1).
Based on the blinding of RCTs, the odds for mortality was shown to be slightly higher in double blinded trials among the vitamin C group (OR, 1.04; 95% CI, 0.76–1.43; n = 938; I2 = 0%; p = 0.80), while for single blinded/open, odds were slightly reduced (OR 0.92, 95% CI 0.65 to 1.29; n = 1199; I2 = 0%; p = 0.61) compared with the placebo or SOC group, but it could not reach statistical significance (Supplementary file S3, Figure S2).
Re-running analysis was conducted based on concomitant use of antioxidants to see any differences. Analysis comparing placebo/SOC with vitamin C only (OR, 0.93; 95% CI, 0.49–1.76; n = 207; I2 = 5%; p = 0.82) and placebo/SOC with other concomitant antioxidants use with vitamin C (OR, 0.99; 95% CI, 0.77–1.27; n = 1930; I2 = 0%; p = 0.94) also could not show significant differences in hospital mortality (Supplementary file S3, Figure S3).
Sensitivity Analysis among Observational Studies
In the sepsis/septic shock group, mortality could not reach significant differences (OR, 0.73; 95% CI, 0.46–1.15; n = 340,351; I2 = 86%; p = 0.17), while among surgical patients (OR, 0.69; 95% CI, 0.56–0.85; n = 5143; I2 = 4%; p = 0.0005), a significant reduction in hospital mortality was observed comparing the vitamin C with placebo/SOC groups (Supplementary file S3, Figure S4).
The analysis comparing placebo/SOC with vitamin C only could not reach significant differences in mortality (OR, 0.86; 95% CI, 0.64–1.16; n = 963; I2 = 0%; p = 0.32), while comparing placebo/SOC with other concomitant antioxidants use with vitamin C showed a significant reduction in hospital mortality (OR, 0.60; 95% CI, 0.38–0.95; n = 344,531; I2 = 91%; p < 0.0001) (Supplementary file S3, Figure S5).
3.2.2. 28/30-Day Mortality
Using a fixed effect model effect, the pooling of data from 17 studies showed a 0.88 odds of 28/30-day mortality among the vitamin C group compared with placebo/SOC (95% CI, 0.74–1.04; n = 3405; I2 = 28%; p = 0.13), which could not reach statistical significance. Further, the subgroup analysis based on the type of studies showed a 0.80 odds of 28/30-day mortality among the vitamin C group among RCTs (OR, 0.80; 95% CI, 0.64–1.00; n = 2131; I2 = 37%; p = 0.05), which also did not differ significantly with placebo/SOC. Similarly, taking observational studies only also showed no significant differences across the two groups (OR, 1.00; 95% CI, 0.76–1.31; n = 1274; I2 = 4%; p = 0.99) (Figure 4).
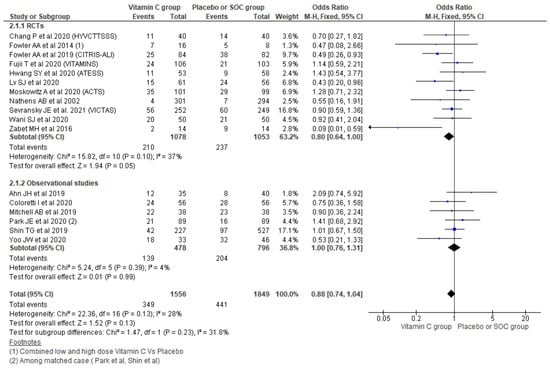
Figure 4.
Forest plot showing 28-days mortality using fixed-effect model.
Considering mild–moderate heterogeneity and pooling the results using random-effect model also showed no significant differences (Supplementary file S3, Figure S6).
3.2.3. ICU Mortality
Pooling data from 14 studies reporting ICU mortality showed an OR of 0.83 for overall ICU mortality (95% CI, 0.61–1.13; n = 2448; I2 = 38%; p = 0.24), though it could not reach statistical significance. Similarly, further subgroup analysis taking the type of study under consideration showed a similar result with RCTs (OR, 1.02; 95% CI, 0.75–1.38; n = 1716; I2 = 0%; p = 0.91) and observational studies (OR, 0.69; 95% CI, 0.41–1.17; n = 732; I2 = 55%; p = 0.17) (Supplementary file S3, Figure S7).
3.2.4. Length of Hospital Stay
Pooling data from 24 studies reporting the length of hospital stay (LoHS) outcome using a random effect model showed a mean difference of -0.84 days comparing the vitamin C group with placebo/SOC (95% CI, −2.11 to 0.44; n = 252,961; I2 = 94%; p = 0.20). Similarly, further subgrouping of the LoHS outcome based on the type of study also could not reach the level of significance for reduction in LoHS among the vitamin C group compared with placebo/SOC among RCTs (MD, −0.69; 95% CI, 1.79 to 0.41; n = 1804; I2 = 62%; p = 0.22) and observational studies (MD, −1.45; 95% CI, −3.78 to 0.87; n = 251,157; I2 = 97%; p = 0.22) (Figure 5).
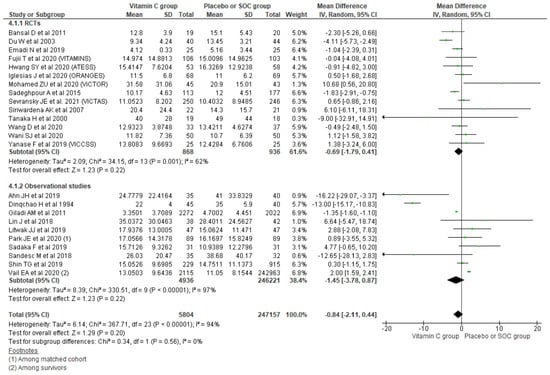
Figure 5.
Forest plot showing mean difference of LoHS using random-effect model.
Sensitivity Analysis among RCTs
Among the patients in sepsis/septic shock, there were no significant differences in the length of hospital stay between the two groups (MD, 0.63; 95% CI, −0.41 to 1.68; n = 1141; I2 = 0%; p = 0.23); however, among critically ill surgical patients, an average 1.7 days reduction in LoHS was observed among the vitamin C group compared with placebo/SOC (MD, −1.70; 95% CI, −2.89 to −0.51; n = 663; I2 = 52%; p = 0.005) (Supplementary file S3, Figure S8).
Running analysis for LoHS taking RCTs based on the blinding of trials showed a significant reduction in the length of hospital stay of the vitamin C group among both double blinded trials (MD, −0.54; 95% CI, −1.43 to 0.36; n = 1247; I2 = 34%; p = 0.24), and the single blinded/open RCTs’ reduction in LoHS among the vitamin C group could not reach statistical significance (MD, −0.78; 95% CI, −3.77 to 2.20; n = 557; I2 = 73%; p = 0.61) compared with the placebo or SOC group (Supplementary file S3, Figure S9).
Analysis comparing vitamin C only with placebo/SOC showed on average a 1.7 day reduction in LoHS among the vitamin C group (MD, −1.70; 95% CI, −3.02 to −0.37; n = 581; I2 = 61%; p = 0.01), while such reduction is not seen in other concomitant antioxidants use with vitamin C (MD, 0.31; 95% CI, −0.91 to 1.53; n = 1223; I2 = 21%; p = 0.62) and also could not show significant differences in hospital mortality (Supplementary file S3, Figure S10).
Sensitivity Analysis among Observational Studies
In both the sepsis/septic shock group (MD, 1.34; 95% CI, −0.43 to 3.10; n = 246,631; I2 = 64%; p = 0.14) and the surgical group (MD, −5.25; 95% CI, −14.19 to 3.69; n = 4526; I2 = 97%; p = 0.25), the reduction in LoHS could not reach statistical significance comparing the vitamin C with the placebo/SOC groups (Supplementary file S3, Figure S11).
Running analysis considering the concomitant use of other antioxidants with vitamin C among observational studies also could not show significant differences in the length of hospital stay comparing placebo/SOC with vitamin C only (MD, −8.12; 95% CI, −19.97 to 3.74; n = 240; I2 = 80%; p = 0.18) or the concomitant use of other antioxidants with vitamin C (MD, 0.83; 95% CI, −1.31 to 2.97; n = 250,917; I2 = 97%; p = 0.45) (Supplementary file S3, Figure S12).
3.2.5. Length of ICU Stay
Polling data from 30 studies reporting the length of ICU stay outcome using a random effect model showed an overall mean difference of −0.76 days, indicating a 0.76-day shorter ICU stay among the vitamin C group compared with placebo/SOC (95% CI, 95% CI, −1.34 to −0.19; n = 252,897; I2 = 96%; p = 0.009). Similarly, further subgrouping of the length of ICU stay based on the type of study also showed a small but significant reduction in the length of ICU stay among the vitamin C group comparing with placebo/SOC among RCTs (MD, −0.70; 95% CI, −1.39 to −0.02; n = 1712; I2 = 86%; p = 0.04), while the observational studies could not reach the level of significance (MD, −0.82; 95% CI, −1.75 to 0.10; n = 251,185; I2 = 98%; p = 0.08) (Figure 6).
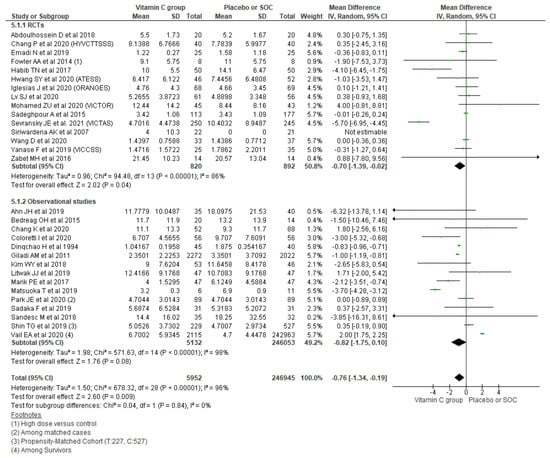
Figure 6.
Forest plot showing mean difference of length of ICU stays using a random-effect model.
3.2.6. New-Onset Acute Kidney Injury (AKI)
Pooling new onset AKI outcomes using a fixed effect model from 12 studies showed no significant increment in new AKI (OR, 1.23; 95% CI, 0.95 to 1.59; n = 5330; I2 = 0%; p = 0.12). Similarly, considering the type of study also could not show a significant increment in new AKI among observational studies (OR, 1.36; 95% CI, 0.87 to 2.12; n = 4482; I2 = 37%; p = 0.18) and RCTs (OR, 1.16; 95% CI, 0.85 to 1.60; n = 848; I2 = 0%; p = 0.35) (Figure 7).
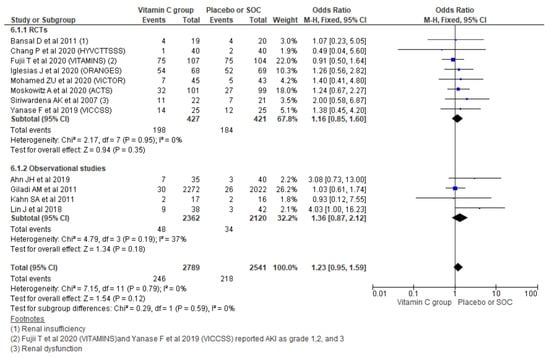
Figure 7.
Forest plot showing the new occurrence of AKI using a fixed-effect model.
Pooling the new onset AKI outcomes using a random-effect model also showed no significant difference in new AKI outcomes (OR, 1.22; 95% CI, 0.94 to 1.58; n = 5330; I2 = 0%; p = 0.14). Similarly, the type of study could not show significant changes among observational studies and RCTs (Supplementary file S3, Figure S13).
3.2.7. Renal Replacement Therapy (RRT) for AKI
The pooling requirement of RRT for AKI using a random-effect model from 13 studies showed no significant differences in the overall requirement of RRT for AKI (OR, 0.80; 95% CI, 0.63 to 1.01; n = 1989; I2 = 0%; p = 0.06). Similarly, considering the type of study also could not show a significant difference among the two treatment groups in observational studies (OR, 0.80; 95% CI, 0.61 to 1.04; n = 1518; I2 = 0%; p = 0.09) and RCTs (OR, 0.81; 95% CI, 0.47 to 1.39; n = 471; I2 = 9%; p = 0.44) (Figure 8).
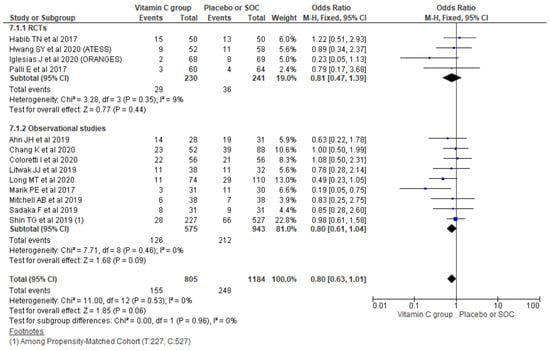
Figure 8.
Forest plot showing requirement of RRT for AKI using a random-effect model.
4. Discussion
Herein, we report a comprehensive systematic review and meta-analysis including 48 previously published studies. We have included 27 randomized controlled trials and 21 observational studies that have studied the role of intravenous vitamin C in critically ill patients. We found a reduction in overall hospital mortality among critically ill patients who received vitamin C, in contrast to the findings of an earlier meta-analyses by Langlois et al. and Wei et al. [11,12]. However, this finding could have been impacted by the inclusion of observational studies in the cumulative analysis. These findings could not be replicated when a subgroup analysis was performed for the randomized controlled trials alone. Mortality benefit was observed when a cumulative analysis was performed for the observational studies alone.
Oxidative stress is thought to play a central role in the pathophysiology of the inflammatory syndrome post-operative state after surgery and sepsis. Vitamin C deficiency is commonly seen in surgical patients and patients in intensive care units [43,71]. The intense inflammatory process leads to an increased turnover of vitamin C, further resulting in severe deficiency [43,71]. Parenteral vitamin C has been investigated for its potential anti-inflammatory, antioxidant effects [3]. Vitamin C has also been studied for its properties to improve immune function, regulate microcirculation and prevent thrombosis [3]. Although the therapeutic efficacy of vitamin C is seen in individual studies, we found no difference in mortality among patients receiving intravenous vitamin C while performing a subgroup analysis of RCTs including surgical patients or patients with sepsis/septic shock. A reduction in mortality was observed among surgical patients in observational studies. We found no difference in the length of hospital stay in the analysis of the cohort and subgroup analyses. A reduction in the length of ICU stay was observed while analyzing studies reporting ICU stay and also among RCTs only separately, although a level of statistical significance could not be achieved while analyzing observational studies separately. Prior meta-analyses conducted by Langlois et al., Putzu et al. and Wei et al. found no difference in the duration of hospital stay and the length of ICU stay [10,11,12]. However, in a subgroup analysis, Putzu et al. found decreased lengths of hospital and ICU stays among patients undergoing cardiac surgery [10]. Vitamin C has shown to decrease the risk of postoperative atrial fibrillation in patients undergoing cardiac surgery, a further benefit observed in terms of the deceased length of ICU stay suggests that vitamin C may have beneficial effects from mechanisms yet to be recognized [72,73].
Vitamin C is metabolized into oxalate compounds that can accumulate in the kidneys and trigger acute kidney injury [44]. In our meta-analysis, we found no increase in the new-onset acute kidney injury or requirement for renal replacement therapy among the patients receiving vitamin C. This finding is consistent with the results of a prior meta-analyses conducted by Putzu et al. and Wei et al. [10,11]. Collectively, this suggests that vitamin C is potentially more renally safe than perceived.
We have sought to perform the most comprehensive meta-analysis, including 48 studies in quantitative analysis evaluating the vitamin C use in critically ill patients and their clinical outcomes. We have only included studies in which vitamin C was administered parenterally. High dose oral vitamin C saturates the intestinal absorption mechanism; thus, a higher plasma concentration cannot be achieved by a higher oral dose administration. We assumed that the intravenous administration makes it possible to achieve the higher plasma concentration required to scavenge oxidizing radicals and protect from their deleterious effects. Prior meta-analyses conducted in the role of vitamin C among critically ill patients have included fewer studies than our analysis [10,11,12]. They have included studies using both oral and parenteral formulations of vitamin C, which adds to the strength of our study [10,11,12]. Our analysis is further strengthened by the subgroup analyses conducted based on the clinical settings, medical and surgical etiology of hospitalization, sepsis and septic shock, and the type of studies.
Our study has several limitations. The included RCTs and observational studies have their own inherent limitations. The baseline characteristics of the population studied and the assessment of organ dysfunction were not individually reported across the studies. The formulations, dosing and duration of vitamin C use are comparable and offer granularity of data in assessing individual influence. Further, the patients could have been enrolled in different stages, and the severity of sepsis and ARDS, and clinical outcomes could have been influenced by the stage of the pathology.
ICU pathophysiology is complex and clinical outcomes are determined several factors relating to patients’ general health and acute physiological state. This includes factors that cannot be reversed by vitamin C therapy alone and results can be confounded. Various studies in our analysis included treatment with other antioxidants such as thiamine and steroids, which can act as potential confounders. Nevertheless, our observation of no significant difference across the two groups in acute kidney injury and need for renal replacement therapy is reassuring in terms of the renal safety of intravenous vitamin C therapy and can guide future investigators.
5. Conclusions
The treatment of critically ill patients with vitamin C did not offer mortality benefits in terms of a reduction in in-hospital mortality, 28/30-day mortality and ICU mortality based on the cumulative analysis of the randomized controlled trials. However, vitamin C did reduce the length of hospitalization, although it did not reduce the number of ICU days. In addition, vitamin C therapy was relatively safe, especially from a renal standpoint, given the no significant group difference in the incidence of acute kidney injury and the need for renal replacement therapy.
Supplementary Materials
The following are available online at https://www.mdpi.com/article/10.3390/nu13103564/s1, Supplementary file S1: Electronic search details, Supplementary file S2. Basic study details, Supplementary file S3: Additional analysis.
Author Contributions
D.B.S., P.B. and Y.R.S. contributed to the concept and design, analysis and interpretation of data. D.B.S., P.B., Y.R.S., S.K.M., S.S., S.K., R.K.B., M.G.K., X.Q. and A.A.F. contributed to the review and initial manuscript drafting. All authors were involved in drafting and revising the manuscript and approved the final version. All authors have read and agreed to the published version of the manuscript.
Funding
This article did not receive any specific grant from funding agencies in the public, commercial, or other sectors.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
The datasets analyzed during the current study are available from the corresponding author on reasonable request.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Fisher, B.J.; Kraskauskas, D.; Martin, E.J.; Farkas, D.; Wegelin, J.A.; Brophy, D.; Ward, K.R.; Voelkel, N.F.; Fowler, A.A.; Natarajan, R. Mechanisms of attenuation of abdominal sepsis induced acute lung injury by ascorbic acid. Am. J. Physiol. Lung Cell. Mol. Physiol. 2012, 303, L20–L32. [Google Scholar] [CrossRef]
- Fisher, B.J.; Seropian, I.M.; Kraskauskas, D.; Thakkar, J.N.; Voelkel, N.F.; Fowler, A.A.; Natarajan, R. Ascorbic acid attenuates lipopolysaccharide-induced acute lung injury. Crit. Care Med. 2011, 39, 1454–1460. [Google Scholar] [CrossRef]
- Fowler, A.A.; Syed, A.A.; Knowlson, S.; Sculthorpe, R.; Farthing, D.; DeWilde, C.; Farthing, C.A.; Larus, T.L.; Martin, E.; Brophy, D.F.; et al. Phase I safety trial of intravenous ascorbic acid in patients with severe sepsis. J. Transl. Med. 2014, 12, 1–10. [Google Scholar] [CrossRef] [Green Version]
- Truwit, J.; Hite, R.; Morris, P.; DeWilde, C.; Jama, A.P. Effect of Vitamin C Infusion on Organ Failure and Biomarkers of Inflammation and Vascular Injury in Patients with Sepsis and Severe Acute Respiratory Failure: The CITRIS. Available online: http://jamanetwork.com (accessed on 26 January 2021).
- Marik, P.E.; Khangoora, V.; Rivera, R.; Hooper, M.H.; Catravas, J. Hydrocortisone, Vitamin C, and Thiamine for the Treatment of Severe Sepsis and Septic Shock: A Retrospective Before-After Study. Chest 2017, 151, 1229–1238. [Google Scholar] [CrossRef]
- Zabet, M.; Mohammadi, M.; Ramezani, M.; Khalili, H. Effect of high-dose Ascorbic acid on vasopressor′s requirement in septic shock. J. Res. Pharm. Pract. 2016, 5, 94. [Google Scholar] [CrossRef]
- Nakajima, M.; Kojiro, M.; Aso, S.; Matsui, H.; Fushimi, K.; Kaita, Y.; Goto, H.; Yamaguchi, Y.; Yasunaga, H. Effect of high-dose vitamin C therapy on severe burn patients: A nationwide cohort study. Crit. Care 2019, 23, 407. [Google Scholar] [CrossRef] [Green Version]
- Wang, Y.; Lin, H.; Lin, B.W.; Lin, J.-D. Effects of different ascorbic acid doses on the mortality of critically ill patients: A meta-analysis. Ann. Intensive Care 2019, 9, 58. [Google Scholar] [CrossRef] [Green Version]
- Zhang, M.; Jativa, D.F. Vitamin C supplementation in the critically ill: A systematic review and meta-analysis. SAGE Open Med. 2018, 6, 205031211880761. [Google Scholar] [CrossRef] [Green Version]
- Putzu, A.; Daems, A.-M.; Lopez-Delgado, J.C.; Giordano, V.F.; Landoni, G. The Effect of Vitamin C on Clinical Outcome in Critically Ill Patients. Crit. Care Med. 2019, 47, 774–783. [Google Scholar] [CrossRef]
- Wei, X.; Wang, Z.; Liao, X.; Guo, W.; Wen, J.Y.; Qin, T.; Wang, S. Efficacy of vitamin C in patients with sepsis: An updated meta-analysis. Eur. J. Pharmacol. 2020, 868, 172889. [Google Scholar] [CrossRef]
- Langlois, P.L.; Manzanares, W.; Adhikari, N.K.J.; Lamontagne, F.; Stoppe, C.; Hill, A.; Heyland, D.K. Vitamin C Administration to the Critically Ill: A Systematic Review and Meta-Analysis. J. Parenter. Enter. Nutr. 2019, 43, 335–346. [Google Scholar] [CrossRef]
- Shrestha, D.; Budhathoki, P.; Sedhai, Y.R.; Baniya, R.K.; Mandal, S.K.; Karki, S.; Shikhrakar, S. Role of Vitamin C in Critically Ill Patients: A Systematic Review and Meta-Analysis. Available online: https://www.crd.york.ac.uk/prospero/display_record.php?RecordID=222906 (accessed on 11 September 2021).
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.A.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: Explanation and elaboration. BMJ 2009, 339, b2700. [Google Scholar] [CrossRef] [Green Version]
- How Can I Cite Covidence? Available online: https://support.covidence.org/help/how-can-i-cite-covidence (accessed on 26 January 2021).
- Sterne, J.A.C.; Savović, J.; Page, M.J.; Elbers, R.G.; Blencowe, N.S.; Boutron, I.; Cates, C.J.; Cheng, H.Y.; Corbett, M.S.; Eldridge, S.M.; et al. RoB 2: A revised tool for assessing risk of bias in randomised trials. BMJ 2019, 366, l4898. [Google Scholar] [CrossRef] [Green Version]
- Critical-Appraisal-Tools—Critical Appraisal Tools|Joanna Briggs Institute. Available online: https://joannabriggs.org/critical-appraisal-tools (accessed on 18 December 2020).
- RevMan for Non-Cochrane Reviews|Cochrane Training. Available online: https://training.cochrane.org/online-learning/core-software-cochrane-reviews/revman/revman-non-cochrane-reviews (accessed on 26 January 2021).
- Ahn, J.H.; Oh, D.K.; Huh, J.W.; Lim, C.M.; Koh, Y.; Hong, S.B. Vitamin C alone does not improve treatment outcomes in mechanically ventilated patients with severe sepsis or septic shock: A retrospective cohort study. J. Thorac. Dis. 2019, 11, 1562–1570. [Google Scholar] [CrossRef]
- Bedreag, O.H.; Rogobete, A.F.; Sărăndan, M.; Cradigati, A.C.; Păpurică, M.; Roşu, O.M.; Luca, L.; Vernic, C.; Nartiţă, R.; Săndesc, D. Influence of antioxidant therapy on the clinical status of multiple trauma patients. A retrospective single center study. Rom. J. Anaesth. Intensive Care 2015, 22, 89–96. [Google Scholar]
- Chang, K.; Harbin, M.; Shuster, C.; Griesdale, D.E.G.; Foster, D.; Sweet, D.; Wood, M.D.; Dhingra, V.K. Adding vitamin C to hydrocortisone lacks benefit in septic shock: A historical cohort study. Can. J. Anesth. 2020, 67, 1798–1805. [Google Scholar] [CrossRef]
- Coloretti, I.; Biagioni, E.; Venturelli, S.; Munari, E.; Tosi, M.; Roat, E.; Brugioni, L.; Gelmini, R.; Venturelli, C.; Girardis, M. Adjunctive therapy with vitamin c and thiamine in patients treated with steroids for refractory septic shock: A propensity matched before-after, case-control study. J. Crit. Care 2020, 59, 37–41. [Google Scholar] [CrossRef]
- Dingchao, H.; Zhiduan, Q.; Liye, H.; Xiaodong, F. The protective effects of high-dose ascorbic acid on myocardium against reperfusion injury during and after cardiopulmonary bypass. Thorac. Cardiovasc. Surg. 1994, 42, 276–278. [Google Scholar] [CrossRef]
- Giladi, A.M.; Dossett, L.A.; Fleming, S.B.; Abumrad, N.N.; Cotton, B.A. High-dose antioxidant administration is associated with a reduction in post-injury complications in critically ill trauma patients. Injury 2011, 42, 78–82. [Google Scholar] [CrossRef]
- Kahn, S.A.; Beers, R.J.; Lentz, C.W. Resuscitation after severe burn injury using high-dose ascorbic acid: A retrospective review. J. Burn Care Res. 2011, 32, 110–117. [Google Scholar] [CrossRef]
- Kim, W.Y.; Jo, E.J.; Eom, J.S.; Mok, J.; Kim, M.H.; Kim, K.U.; Park, H.K.; Lee, M.K.; Lee, K. Combined vitamin C, hydrocortisone, and thiamine therapy for patients with severe pneumonia who were admitted to the intensive care unit: Propensity score-based analysis of a before-after cohort study. J. Crit. Care 2018, 47, 211–218. [Google Scholar] [CrossRef]
- Lin, J.; Falwell, S.; Greenhalgh, D.; Palmieri, T.; Sen, S. High-dose ascorbic acid for burn shock resuscitation may not improve outcomes. J. Burn Care Res. 2018, 39, 708–712. [Google Scholar] [CrossRef]
- Litwak, J.; Cho, N.; Nguyen, H.; Moussavi, K.; Bushell, T. Vitamin C, Hydrocortisone, and Thiamine for the Treatment of Severe Sepsis and Septic Shock: A Retrospective Analysis of Real-World Application. J. Clin. Med. 2019, 8, 478. [Google Scholar] [CrossRef] [Green Version]
- Long, M.T.; Frommelt, M.A.; Ries, M.P.; Murray, M.; Osman, F.; Krause, B.M.; Kory, P.; Ries, M.-C.P. Early hydrocortisone, ascorbate and thiamine therapy for severe sep-tic shock. Crit. Care Shock 2020, 23, 23–24. [Google Scholar]
- Masood, H.; Burki, A.M.; Sultan, A.; Sharif, H.; Ghauri, A.; Khan, S.; Qureshi, M.S.S.; Qadeer, A.; Rasheed, G. Effect of Intravenous Vitamin C, Thiamine, and Hydrocortisone (The Metabolic Resuscitation Protocol) on Early Weaning from Vasopressors in Patients with Septic Shock. A Descriptive Case Series Study. Cureus 2019, 11, e5016. [Google Scholar] [CrossRef]
- Matsuoka, T.; Shinozaki, H.; Ozawa, S.; Izawa, Y.; Koyanagi, K.; Lefor, A.K.; Kobayashi, K. Administration of corticosteroids, ascorbic acid, and thiamine improves oxygenation after thoracoscopic esophagectomy. Ann. Thorac. Cardiovasc. Surg. 2020, 26, 133–139. [Google Scholar] [CrossRef]
- Mitchell, A.B.; Ryan, T.E.; Gillion, A.R.; Wells, L.D.; Muthiah, M.P. Vitamin C and Thiamine for Sepsis and Septic Shock. Am. J. Med. 2020, 133, 635–638. [Google Scholar] [CrossRef]
- Nagel, S.S.; Radu, C.A.; Kremer, T.; Meess, D.; Horter, J.; Ziegler, B.; Hirche, C.; Schmidt, V.J.; Kneser, U.; Hundeshagen, G. Safety, pharmacodynamics, and efficacy of high- versus low-dose ascorbic acid in severely burned adults. J. Burn Care Res. 2020, 41, 871–877. [Google Scholar] [CrossRef]
- Park, J.E.; Shin, T.G.; Jo, I.J.; Jeon, K.; Suh, G.Y.; Park, M.; Won, H.; Chung, C.R.; Hwang, S.Y. Impact of Vitamin C and Thiamine Administration on Delirium-Free Days in Patients with Septic Shock. J. Clin. Med. 2020, 9, 193. [Google Scholar] [CrossRef] [Green Version]
- Sadaka, F.; Grady, J.; Organti, N.; Donepudi, B.; Korobey, M.; Tannehill, D.; O’Brien, J. Ascorbic Acid, Thiamine, and Steroids in Septic Shock: Propensity Matched Analysis. J. Intensive Care Med. 2020, 35, 1302–1306. [Google Scholar] [CrossRef]
- Sandesc, M.; Rogobete, A.F.; Bedreag, O.H.; Dinu, A.; Papurica, M.; Cradigati, C.A.; Sarandan, M.; Popovici, S.E.; Bratu, L.M.; Bratu, T.; et al. Analysis of oxidative stress-related markers in critically ill polytrauma patients: An observational prospective single-center study. Bosn. J. Basic Med. Sci. 2018, 18, 191–197. [Google Scholar] [CrossRef] [Green Version]
- Shin, T.G.; Kim, Y.-J.; Ryoo, S.M.; Hwang, S.Y.; Jo, I.J.; Chung, S.P.; Choi, S.-H.; Suh, G.J.; Kim, W.Y. Early Vitamin C and Thiamine Administration to Patients with Septic Shock in Emergency Departments: Propensity Score-Based Analysis of a Before-and-After Cohort Study. J. Clin. Med. 2019, 8, 102. [Google Scholar] [CrossRef] [Green Version]
- Vail, E.A.; Wunsch, H.; Pinto, R.; Bosch, N.A.; Walkey, A.J.; Lindenauer, P.K.; Gershengorn, H.B. Use of hydrocortisone, ascorbic acid, and thiamine in adults with septic shock. Am. J. Respir. Crit. Care Med. 2020, 202, 1531–1539. [Google Scholar] [CrossRef]
- Yoo, J.W.; Kim, R.B.; Ju, S.; Lee, S.J.; Cho, Y.J.; Jeong, Y.Y.; Lee, J.D.; Kim, H.C. Clinical impact of supplementation of vitamins B1 and C on patients with sepsis-related acute respiratory distress syndrome. Tuberc. Respir. Dis. 2020, 83, 248–254. [Google Scholar] [CrossRef]
- Mean Variance Estimation. Available online: https://web.archive.org/web/20181224162602/http:/www.comp.hkbu.edu.hk/~xwan/median2mean.html (accessed on 16 February 2021).
- Identifying and Measuring Heterogeneity. Available online: https://handbook-5-1.cochrane.org/chapter_9/9_5_2_identifying_and_measuring_heterogeneity.htm (accessed on 18 December 2020).
- Abdoulhossein, D.; Taheri, I.; Saba, M.; Akbari, H.; Shafagh, S.; Zataollah, A. Effect of vitamin C and vitamin E on lung contusion: A randomized clinical trial study. Ann. Med. Surg. 2018, 36, 152–157. [Google Scholar] [CrossRef]
- Doll, S.; Ricou, B. Severe vitamin C deficiency in a critically ill adult: A case report. Eur. J. Clin. Nutr. 2013, 67, 881–882. [Google Scholar] [CrossRef] [Green Version]
- Colliou, E.; Mari, A.; Delas, A.; Delarche, A.; Faguer, S. Oxalate nephropathy following vitamin C intake within intensive care unit. Clin. Nephrol. 2017, 88, 354–358. [Google Scholar] [CrossRef]
- Emadi, N.; Nemati, M.H.; Ghorbani, M.; Allahyari, E. The effect of high-dose vitamin c on biochemical markers of myocardial injury in coronary artery bypass surgery. Braz. J. Cardiovasc. Surg. 2019, 34, 517–524. [Google Scholar] [CrossRef]
- Sevransky, J.E.; Rothman, R.E.; Hager, D.N.; Bernard, G.R.; Brown, S.M.; Buchman, T.G.; Busse, L.W.; Coopersmith, C.M.; DeWilde, C.; Ely, E.W.; et al. Effect of Vitamin C, Thiamine, and Hydrocortisone on Ventilator—and Vasopressor-Free Days in Patients With Sepsis. JAMA 2021, 325, 742. [Google Scholar] [CrossRef]
- Ferrón-Celma, I.; Mansilla, A.; Hassan, L.; Garcia-Navarro, A.; Comino, A.M.; Bueno, P.; Ferrón, J.A. Effect of Vitamin C Administration on Neutrophil Apoptosis in Septic Patients After Abdominal Surgery. J. Surg. Res. 2009, 153, 224–230. [Google Scholar] [CrossRef]
- Wani, S.J.; Mufti, S.A.; Jan, R.A.; Shah, S.U.; Qadri, S.M.; Khan, U.H.; Bagdadi, F.; Mehfooz, N.; Koul, P.A. Combination of vitamin C, thiamine and hydrocortisone added to standard treatment in the management of sepsis: Results from an open label randomised controlled clinical trial and a review of the literature. Infect. Dis. 2020, 52, 271–278. [Google Scholar] [CrossRef]
- Hwang, S.Y.; Ryoo, S.M.; Park, J.E.; Jo, Y.H.; Jang, D.-H.; Suh, G.J.; Kim, T.; Kim, Y.-J.; Kim, S.; Cho, H.; et al. Combination therapy of vitamin C and thiamine for septic shock: A multi-centre, double-blinded randomized, controlled study. Intensive Care Med. 2020, 46, 2015–2025. [Google Scholar] [CrossRef]
- Balakrishnan, M.; Gandhi, H.; Shah, K.; Pandya, H.; Patel, R.; Keshwani, S.; Yadav, N. Hydrocortisone, vitamin C and thiamine for the treatment of sepsis and septic shock following cardiac surgery. Indian J. Anaesth. 2018, 62, 934–939. [Google Scholar] [CrossRef]
- Chang, P.; Liao, Y.; Guan, J.; Guo, Y.; Zhao, M.; Hu, J.; Zhou, J.; Wang, H.; Cen, Z.; Tang, Y.; et al. Combined Treatment with Hydrocortisone, Vitamin C, and Thiamine for Sepsis and Septic Shock: A Randomized Controlled Trial. Chest 2020, 158, 174–182. [Google Scholar] [CrossRef]
- Du, W.D.; Yuan, Z.R.; Sun, J.; Tang, J.X.; Cheng, A.Q.; Shen, D.M.; Huang, C.J.; Song, X.H.; Yu, X.F.; Zheng, S.B. Therapeutic efficacy of high-dose vitamin C on acute pancreatitis and its potential mechanisms. World J. Gastroenterol. 2003, 9, 2565–2569. [Google Scholar] [CrossRef] [Green Version]
- Fujii, T.; Luethi, N.; Young, P.J.; Frei, D.R.; Eastwood, G.M.; French, C.J.; Deane, A.M.; Shehabi, Y.; Hajjar, L.A.; Oliveira, G.; et al. Effect of Vitamin C, Hydrocortisone, and Thiamine vs Hydrocortisone Alone on Time Alive and Free of Vasopressor Support among Patients with Septic Shock: The VITAMINS Randomized Clinical Trial. JAMA J. Am. Med. Assoc. 2020, 323, 423–431. [Google Scholar] [CrossRef]
- Iglesias, J.; Vassallo, A.V.; Patel, V.V.; Sullivan, J.B.; Cavanaugh, J.; Elbaga, Y. Outcomes of Metabolic Resuscitation Using Ascorbic Acid, Thiamine, and Glucocorticoids in the Early Treatment of Sepsis: The ORANGES Trial. Chest 2020, 158, 164–173. [Google Scholar] [CrossRef]
- Lv, S.J.; Zhang, G.H.; Xia, J.M.; Yu, H.; Zhao, F. Early use of high-dose vitamin C is beneficial in treatment of sepsis. Ir. J. Med. Sci. 2020, 190, 1183–1188. [Google Scholar] [CrossRef]
- Mirmohammadsadeghi, M.; Mirmohammadsadeghi, A.; Mahmoudian, M. Preventive Use of Ascorbic Acid for Atrial Fibrillation After Coronary Artery Bypass Graft Surgery. Heart Surg. Forum 2018, 21, E415–E417. [Google Scholar] [CrossRef]
- Mohamed, Z.U.; Prasannan, P.; Moni, M.; Edathadathil, F.; Prasanna, P.; Menon, A.; Nair, S.; Greeshma, C.R.; Sathyapalan, D.T.; Menon, V.; et al. Vitamin C Therapy for Routine Care in Septic Shock (ViCTOR) Trial: Effect of Intravenous Vitamin C, Thiamine, and Hydrocortisone Administration on Inpatient Mortality among Patients with Septic Shock. Indian J. Crit. Care Med. 2020, 24, 653–661. [Google Scholar] [CrossRef]
- Moskowitz, A.; Huang, D.T.; Hou, P.C.; Gong, J.; Doshi, P.B.; Grossestreuer, A.V.; Andersen, L.W.; Ngo, L.; Sherwin, R.L.; Berg, K.M.; et al. Effect of Ascorbic Acid, Corticosteroids, and Thiamine on Organ Injury in Septic Shock: The ACTS Randomized Clinical Trial. JAMA 2020, 324, 642–650. [Google Scholar] [CrossRef]
- Nathens, A.B.; Neff, M.J.; Jurkovich, G.J.; Klotz, P.; Farver, K.; Ruzinski, J.T.; Radella, F.; Garcia, I.; Maier, R.V. Randomized, prospective trial of antioxidant supplementation in critically III surgical patients. Ann. Surg. 2002, 236, 814–822. [Google Scholar] [CrossRef]
- Palli, E.; Makris, D.; Papanikolaou, J.; Garoufalis, G.; Tsilioni, I.; Zygoulis, P.; Zakynthinos, E. The impact of N-acetylcysteine and ascorbic acid in contrast-induced nephropathy in critical care patients: An open-label randomized controlled study. Crit. Care 2017, 21, s13054-017. [Google Scholar] [CrossRef] [Green Version]
- Reddy, P.R.; Aluru, N.; Yelle, S.; Rajyalakshmi, B. Metabolic Resuscitation Using Hydrocortisone, Ascorbic Acid, and Thiamine: Do Individual Components Influence Reversal of Shock Independently? Indian J. Crit. Care Med. 2020, 24, 649–652. [Google Scholar] [CrossRef]
- Sadeghpour, A.; Alizadehasl, A.; Kyavar, M.; Sadeghi, T.; Moludi, J.; Gholizadeh, F.; Totonchi, Z.; Ghadrdoost, B. Impact of vitamin C supplementation on post-cardiac surgery ICU and hospital length of stay. Anesthesiol. Pain Med. 2015, 5, e25337. [Google Scholar] [CrossRef] [Green Version]
- Siriwardena, A.K.; Mason, J.M.; Balachandra, S.; Bagul, A.; Galloway, S.; Formela, L.; Hardman, J.G.; Jamdar, S. Randomised, double blind, placebo controlled trial of intravenous antioxidant (n-acetylcysteine, selenium, vitamin C) therapy in severe acute pancreatitis. Gut 2007, 56, 1439–1444. [Google Scholar] [CrossRef] [Green Version]
- Wang, D.; Wang, M.; Zhang, H.; Zhu, H.; Zhang, N.; Liu, J. Effect of intravenous injection of vitamin c on postoperative pulmonary complications in patients undergoing cardiac surgery: A double-blind, randomized trial. Drug Des. Devel. Ther. 2020, 14, 3263–3270. [Google Scholar] [CrossRef]
- Yanase, F.; Bitker, L.; Hessels, L.; Osawa, E.; Naorungroj, T.; Cutuli, S.L.; Young, P.J.; Ritzema, J.; Hill, G.; Latimer-Bell, C.; et al. A Pilot, Double-Blind, Randomized, Controlled Trial of High-Dose Intravenous Vitamin C for Vasoplegia After Cardiac Surgery. J. Cardiothorac. Vasc. Anesth. 2020, 34, 409–416. [Google Scholar] [CrossRef]
- Nabil Habib, T.; Ahmed, I. Early Adjuvant Intravenous Vitamin C Treatment in Septic Shock may Resolve the Vasopressor Dependence. Int. J. Microbiol. Adv. Immunol. 2017, 5, 77–81. [Google Scholar] [CrossRef]
- Tanaka, H.; Matsuda, T.; Miyagantani, Y.; Yukioka, T.; Matsuda, H.; Shimazaki, S. Reduction of resuscitation fluid volumes in severely burned patients using ascorbic acid administration: A randomized, prospective study. Arch. Surg. 2000, 135, 326–331. [Google Scholar] [CrossRef] [Green Version]
- Galley, H.F.; Howdle, P.D.; Walker, B.E.; Webster, N.R. The effects of intravenous antioxidants in patients with septic shock. Free Radic. Biol. Med. 1997, 23, 768–774. [Google Scholar] [CrossRef]
- Razmkon, A.; Sadidi, A.; Sherafat-Kazemzadeh, E.; Mehrafshan, A.; Jamali, M.; Malekpour, B.; Saghafinia, M. Administration of vitamin C and vitamin E in severe head injury: A randomized double-blind controlled trial. Clin. Neurosurg. 2011, 58, 133–137. [Google Scholar] [CrossRef] [Green Version]
- Bansal, D.; Bhalla, A.; Bhasin, D.K.; Pandhi, P.; Sharma, N.; Rana, S.; Malhotra, S. Safety and efficacy of vitamin-based antioxidant therapy in patients with severe acute pancreatitis: A randomized controlled trial. Saudi J. Gastroenterol. 2011, 17, 174–179. [Google Scholar] [CrossRef]
- Luo, M.; Fernandez-Estivariz, C.; Jones, D.P.; Accardi, C.R.; Alteheld, B.; Bazargan, N.; Hao, L.; Griffith, D.P.; Blumberg, J.B.; Galloway, J.R.; et al. Depletion of plasma antioxidants in surgical intensive care unit patients requiring parenteral feeding: Effects of parenteral nutrition with or without alanyl-glutamine dipeptide supplementation. Nutrition 2008, 24, 37–44. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hemilä, H.; Chalker, E. Vitamin C Can Shorten the Length of Stay in the ICU: A Meta-Analysis. Nutrients 2019, 11, 708. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Shi, R.; Li, Z.H.; Chen, D.; Wu, Q.C.; Zhou, X.L.; Tie, H.T. Sole and combined vitamin C supplementation can prevent postoperative atrial fibrillation after cardiac surgery: A systematic review and meta-analysis of randomized controlled trials. Clin. Cardiol. 2018, 41, 871–878. [Google Scholar] [CrossRef] [PubMed] [Green Version]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).