Inhalation of Patchouli (Pogostemon Cablin Benth.) Essential Oil Improved Metabolic Parameters in Obesity-Induced Sprague Dawley Rats
Abstract
1. Introduction
2. Materials and Methods
2.1. Essential Oil
2.2. Volatile Compounds and Odor Description
2.3. Animal Care and Experimental Design
2.4. Serum Biomarker Analyses
2.5. Blood Pressure Assessment
2.6. Statistical Analyses
3. Results and Discussion
3.1. Volatile Compounds
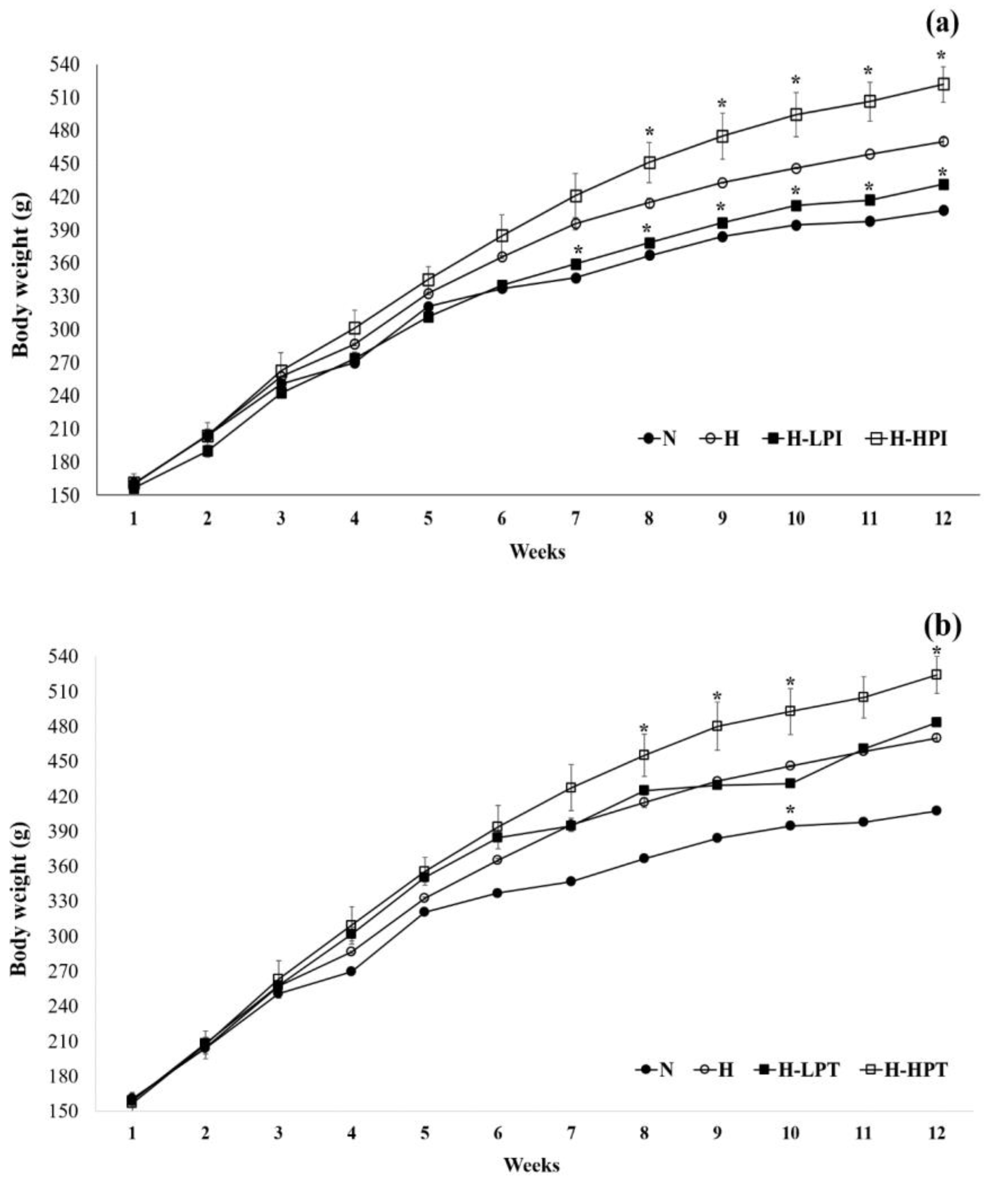
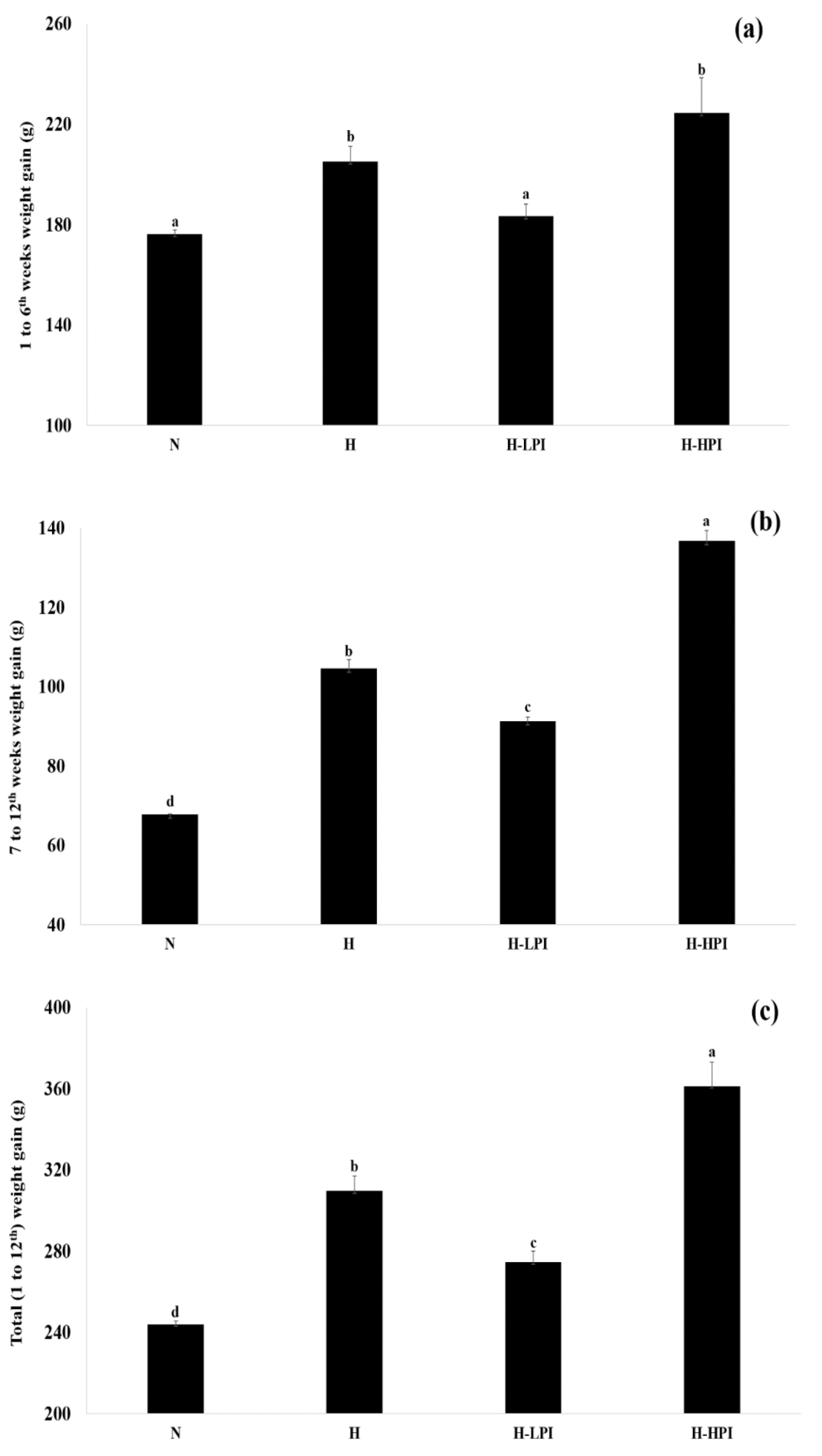
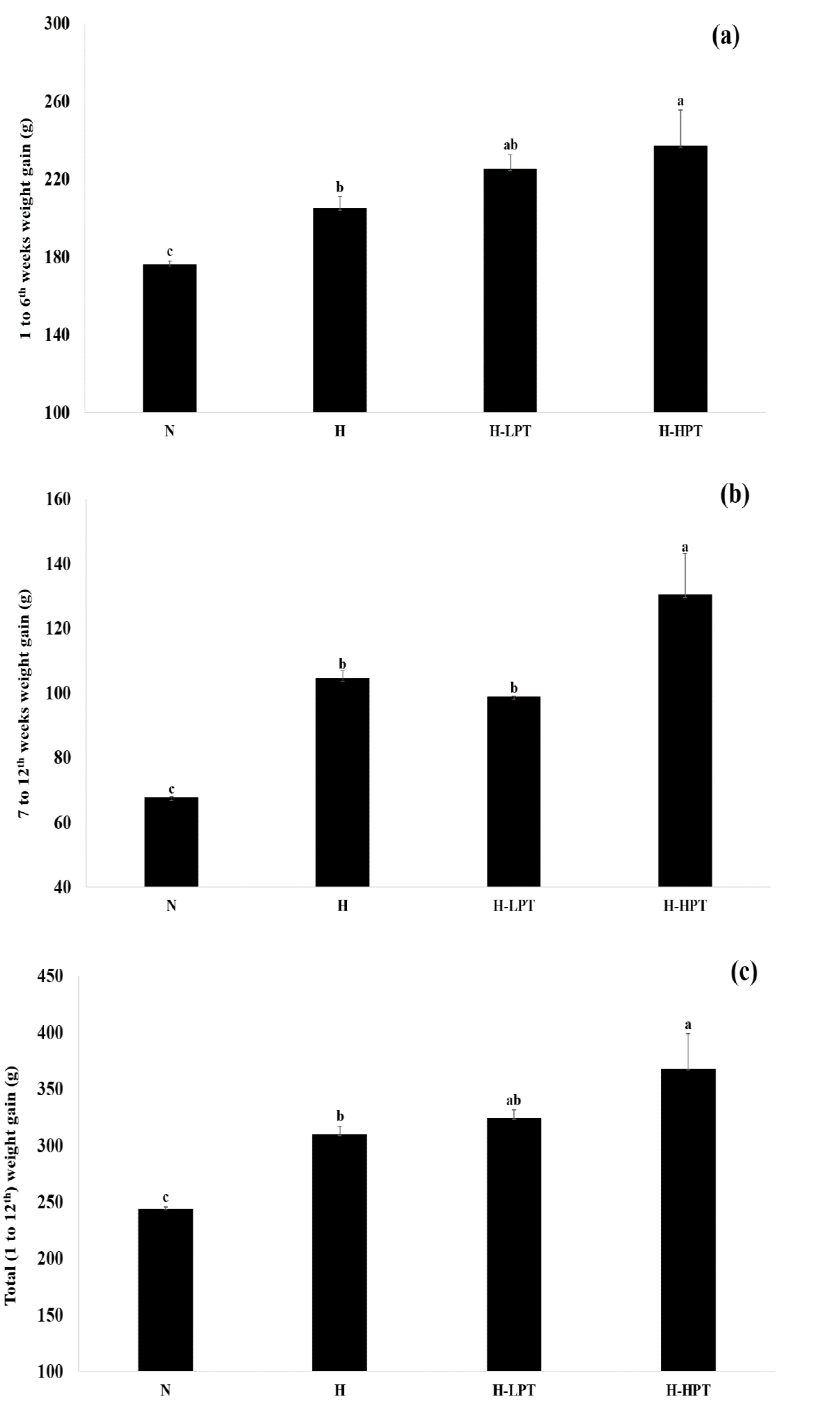
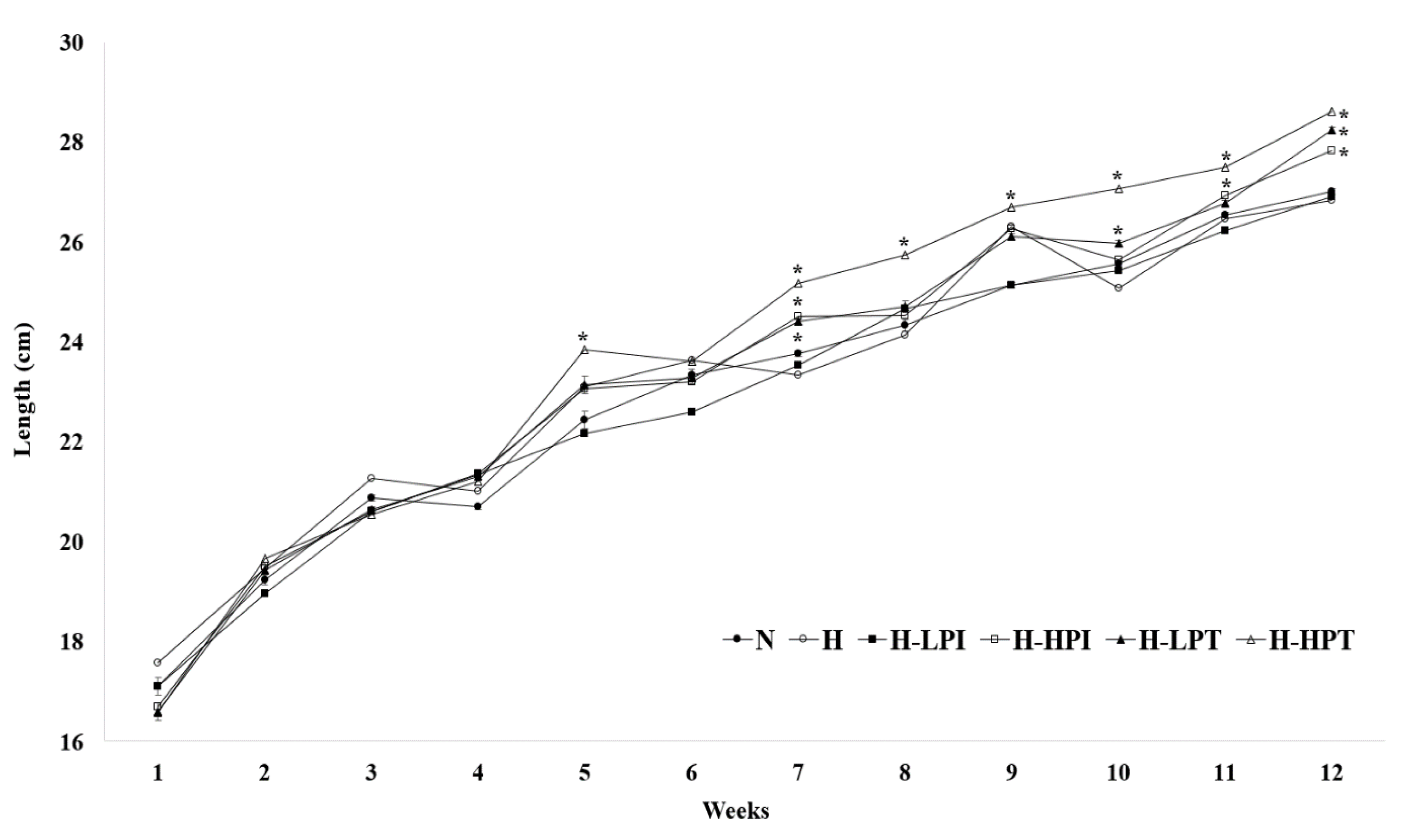
3.2. Food Intake, Body Weight, and Length
3.3. Organ Weight
3.4. Serum Analysis
3.5. Blood Pressure
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Lee, J.Y.; Jeong, Y.; Kim, C.Y. Obesity and dietary supplements for weight loss. Food Ind. Nutr. 2019, 24, 30–40. [Google Scholar]
- Kaplan, N.M. The deadly quartet. Upper-body obesity, glucose intolerance, hypertriglyceridemia, and hypertension. Arch. Intern. Med. 1989, 149, 1514–1520. [Google Scholar] [CrossRef] [PubMed]
- Firestein, S. How the olfactory system makes sense of scents. Nature 2001, 413, 211–218. [Google Scholar] [CrossRef] [PubMed]
- Buck, L.; Axel, R. A novel multigene family may encode odorant receptors: A molecular basis for recognition. Cell 1991, 65, 175–187. [Google Scholar] [CrossRef]
- Gaillard, I.; Rouquier, S.; Pin, J.P.; Mollard, P.; Richard, S.; Barnabe, C.; Demaille, J.; Giorgi, D. A single olfactory receptor specifically binds a set of odorant molecules. Eur. J. Neurosci. 2002, 15, 409–418. [Google Scholar] [CrossRef] [PubMed]
- Bushdidl, C.; Magnasco, M.O.; Vosshall, L.B.; Kellerl, A. Humans can discriminate more than 1 trillion olfactory stimuli. Science 2014, 343, 1370–1373. [Google Scholar] [CrossRef]
- Riera, C.E.; Tsaousidou, E.; Halloran, J.; Follett, P.; Hahn, O.; Pereira, M.M.A.; Ruud, L.E.; Alber, J.; Tharp, K.; Anderson, C.M.; et al. The sense of smell impacts metabolic health and obesity. Cell Metab. 2017, 26, 198–211. [Google Scholar] [CrossRef]
- Shen, J.; Niijima, A.; Tanida, M.; Horii, Y.; Meada, K.; Nagai, K. Olfactory simulation with scent of grapefruit oil affects autonomic nerves, lipolysis and appetite in rats. Neurosci. Lett. 2005, 380, 289–294. [Google Scholar] [CrossRef]
- Schwartz, M.W.; Woods, S.C.; Porte, D.J.; Seeley, R.J.; Baskin, D.G. Central nervous system control of food intake. Nature 2000, 404, 661–671. [Google Scholar] [CrossRef]
- Yamamoto, T.; Inui, T.; Tsuji, T. The odor of Osmanthus fragrans attenuates food intake. Sci. Rep. 2013, 3, 1518. [Google Scholar] [CrossRef]
- Bengt, F.B.; Jens, C.B. CNS leptin and insulin action in the control of energy homostasis. Ann. N. Y. Acad. Sci. 2010, 1212, 97–113. [Google Scholar]
- Myers, M.G.; Cowley, M.A.; Münzberg, H. Mechanisms of leptin action and leptin resistance. Annu. Rev. Physiol. 2008, 70, 537–556. [Google Scholar] [CrossRef]
- Akhila, A.; Tewari, R. Chemistry of patchouli oil: A review. Curr. Res. Med. Aromat. Plants 1984, 6, 38–54. [Google Scholar]
- Amborse, D.C.P.; Annamalai, S.J.K.; Naik, R. Effect of drying on the volatile oil yield of patchouli. Indian J. Sci. Technol. 2013, 6, 5559–5562. [Google Scholar] [CrossRef]
- Huang, Q.H.; Wu, X.; Chen, X.H.; Wu, J.Z.; Su, Z.R.; Liang, J.L.; Li, Y.C.; Lai, X.P.; Chen, J.N.; Liu, Y.H. Patchouli oil isolated from the leaves of Pogostemon cablin ameliorates ethanol-induced acute liver injury in rats via inhibition of oxidative stress and lipid accumulation. RSC Adv. 2018, 8, 24399. [Google Scholar] [CrossRef]
- Beek, V.T.A.; Joulain, D. The essential oil of patchouli, Pogostemon cablin: A review. Flavour Fragr. J. 2017, 33, 6–51. [Google Scholar] [CrossRef]
- Yang, X.; Zhang, X.; Yang, S.P.; Liu, W.Q. Evaluation of the antibacterial activity of patchouli oil. Iran. J. Pharm. Res. 2013, 12, 307–316. [Google Scholar] [PubMed]
- Heo, M.H.; Kim, C.; Kim, C.H.; Ahn, C.H.; Ahn, H.C.; Ahn, H.Y. The effects of inhalation of essential oils on the body weight, food efficiency rate and serum leptin of growing SD rats. J. Korean Acad. Nurs. 2006, 36, 236–243. [Google Scholar]
- Kim, D.S.; Goo, Y.M.; Cho, J.J.; Lee, J.K.; Lee, D.Y.; Sin, S.M.; Kil, Y.S.; Jeong, W.M.; Ko, K.H.; Yang, K.J.; et al. Effect of volatile organic chemicals in chrysanthemum indicum linné on blood pressure and electroencephalogram. Molecules 2018, 23, 2063. [Google Scholar] [CrossRef]
- Sundaresan, V.; Singh, S.P.; Mishra, A.N.; Shasany, A.K.; Darokar, M.P.; Kalra, A.; Naqvi, A.A. Composition and comparison of essential oils of pogostemon cablin (blanco) benth. (patchouli) and pogostemon travancoricus bed. Var. travancoricus. J. Essent. Oil Res. 2009, 21, 220–222. [Google Scholar] [CrossRef]
- Li, Y.C.; Xian, Y.F.; Ip, S.P.; Su, Z.R.; Su, J.Y.; He, J.J.; Xie, Q.F.; Lai, X.P.; Lin, Z.X. Anti-inflammatory activity of patchouli alcohol isolated from Pogostemonis Herba in animal models. Fitoterapia 2011, 82, 1295–1301. [Google Scholar] [CrossRef] [PubMed]
- Wu, J.Z.; Liu, Y.H.; Liang, J.L.; Huang, Q.H.; Dou, Y.X.; Nie, J.; Zhuo, J.Y.; Wu, X.; Chen, J.N.; Su, Z.R.; et al. Protective role of β-patchoulene from Pogostemon cablin against indomethacin-induced gastric ulcer in rats: Involvement of anti-inflammation and angiogenesis. Phytomedicine 2017, 39, 111–118. [Google Scholar] [CrossRef] [PubMed]
- Linck, V.D.M.; Silva, A.L.D.; Figueiro, M.; Piato, A.L.; Herrmann, A.P.; Brick, F.D.; Caramao, E.B.; Nunes, D.S.; Moreno, P.R.H.; Elisabetsky, E. Inhaled linalool-induced sedation in mice. Phytomedicine 2009, 16, 303–307. [Google Scholar] [CrossRef] [PubMed]
- Fonseca, D.V.D.; Filho, C.D.S.M.B.; Lima, T.C.; Almeida, R.N.D.; Sousa, D.P.D. Anticonvulsant essential oils and their relationship with oxidative stress in epilepsy. Biomolecules 2019, 9, 835. [Google Scholar] [CrossRef] [PubMed]
- Batubara, I.; Suparto, I.; Sa’diah, S.; Matsuoka, R.; Mitsunaga, T. Effects of inhaled citronella oil and related compounds on rat body weight and brown adipose tissue sympathetic nerve. Nutrients 2015, 7, 1859–1870. [Google Scholar] [CrossRef]
- Suijun, W.; Zhen, Y.; Ying, G.; Yanfang, W. A role for trans-caryophyllene in the moderation of insulin secretion. Biochem. Biophys. Res. Commun. 2014, 444, 451–454. [Google Scholar] [CrossRef]
- Fernandes, E.S.; Passos, G.F.; Medeiros, R.; Cunha, F.M.D.; Ferreira, J.; Campos, M.M.; Pianowski, L.F.; Calixto, J.B. Anti-inflammatory effects of compounds alpha-humulene and(-)-trans-caryophyllene isolated from the essential oil of Cordia verbenacea. Eur. J. Pharmacol. 2007, 569, 228–236. [Google Scholar] [CrossRef]
- Paula-Freire, L.I.G.; Andersen, M.L.; Gama, V.S.; Molska, G.R.; Carlini, E.L.A. The oral administration of trans-caryophyllene attenuates acute and chronic pain in mice. Phytomedicine 2014, 21, 356–362. [Google Scholar] [CrossRef]
- Chandra, M.; Prakash, O.; Kumar, R.; Bachheti, R.; Bhushan, B.; Kumar, M.; Pant, A. β-selinene-rich essential oils from the parts of callicarpa macrophylla and their antioxidant and pharmacological activities. Medicines 2017, 4, 52. [Google Scholar] [CrossRef]
- Tsuji, T.; Tanaka, S.; Bakhshishayan, S.; Kogo, M.; Yamamoto, T. Olfactory stimulation modulates the blood glucose level in rats. Int. J. Med. Sci. 2018, 15, 269–273. [Google Scholar] [CrossRef]
- Despres, J.P. Is visceral obesity the cause of the metabolic syndrome? Ann. Med. 2006, 38, 52–63. [Google Scholar] [CrossRef]
- Oppenheim, R.W. The concept of uptake and retrograde transport of neurotrophic molecules during development: History and present status. Neurochem. Res. 1996, 21, 769–777. [Google Scholar] [CrossRef]
- Yanai, R.; Yamada, N.; Inui, M.; Nishida, T. Correlation of proliferative and anti-apoptotic effects of HGF, insulin, IGF-1, IGF-2, and EGF in SV40-transformed human corneal epithelial cells. Exp. Eye Res. 2006, 83, 76–83. [Google Scholar] [CrossRef] [PubMed]
- Arner, P. Differences in lipolysis between human subcutaneous and omental adipose tissues. Ann. Med. 1995, 27, 435–438. [Google Scholar] [CrossRef] [PubMed]
- Seo, S.M.; Jo, S.M.; Kim, M.; Lee, M.; Lee, Y.; Kang, I.H. Peanut sprout extracts attenuate triglyceride accumulation by promoting mitochondrial fatty acid oxidation in adipocytes. Int. J. Mol. Sci. 2019, 20, 1216. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.U.; Shin, G.; Park, S.H.; Cho, H.K. Insulin resistance and visceral fat obesity in hyperlipidemia. Korean Circ. J. 1999, 29, 673–679. [Google Scholar] [CrossRef]
- You, M.; Fan, R.; Kim, J.; Shin, S.H.; Chung, S. Alpha-linolenic acid-enriched butter promotes fatty acid remodeling and thermogenic activation in the brown adipose tissue. Nutrients 2020, 12, 136. [Google Scholar] [CrossRef]
- Zhao, H.L.; Cho, K.H.; Ha, Y.W.; Jeong, T.S.; Lee, W.S.; Kim, Y.S. Cholesterol-lowering effect of platycodin D in hypercholesterolemic ICR mice. Eur. J. Phamcol. 2006, 537, 166–173. [Google Scholar] [CrossRef]
- Lucka, A.; Wysokinski, A. Association between adiposity and fasting serum levels of appetite-regulating peptides: Leptin, neuropeptide Y, desacyl ghrelin, peptide YY (1–36), and agouti-related pertein in nonobese participants. Chin. J. Physiol. 2019, 62, 217–225. [Google Scholar]
- Nam, S.Y.; Kratzsch, J.; Kim, K.W.; Kim, K.R.; Lim, S.K.; Marcus, C. Cerebrospinal fluid and plasma concentrations of leptin, NPY, and α -MSH in obese women and their relationship to negative energy balance. J. Clin. Endocrinol. Metab. 2001, 86, 4849–4853. [Google Scholar]
- Simonds, S.E.; Cowley, M.A. Hypertension in obesity: Is leptin the culprit? Trends Neurosci. 2013, 13, 121–132. [Google Scholar] [CrossRef] [PubMed]
| Major Compound | RT 1 | RI 2 | Mean ± SD | Odor Intensity | Odor Description | I.D. 3 |
|---|---|---|---|---|---|---|
| (min) | (µg/100 g) | |||||
| Alcohols (6) | ||||||
| Eucalyptol | 16.14 | 1057 | 44.68 ± 30.14 | 2 | Cool | MS |
| Linalool | 18.08 | 1118 | 12.75 ± 5.84 | 3 | Forest, patchouli | MS/RI |
| Isopulegol | 18.76 | 1142 | 0.49 ± 0.70 | 2 | Bug | MS |
| α-Terpineol | 20.79 | 1210 | 4.03 ± 0.64 | 3 | Sweet | MS/RI |
| Citronellol | 21.84 | 1250 | 4.28 ± 3.44 | 3 | Patchouli | MS |
| Patchouli alcohol | 32.97 | >1700 | 2439.91 ± 2175.56 | - | N.D. | MS |
| Hydrocarbons (10) | ||||||
| Myrcene | 14.78 | 1012 | 1.96 ± 0.71 | 1 | Grape | MS/RI |
| α-Terpinene | 15.56 | 1038 | 11.83 ± 6.26 | 2 | Mint | MS |
| 1,3,7-Dimethyl-3,7-octatriene | 16.54 | 1069 | 0.73 ± 1.03 | 1 | Forest | MS |
| Estragole | 23.59 | 1313 | 0.44 ± 0.62 | 1 | Sweet | MS |
| Aromadendrene | 25.59 | 1390 | 1.94 ± 2.74 | 3 | Forest | MS |
| β-Patchoulene | 26.36 | 1421 | 2384.05 ± 1132.99 | 3 | Patchouli | MS |
| β-Caryophyllene | 27.14 | 1453 | 1065.62 ± 390.37 | 3 | Patchouli | MS/RI |
| α-Patchoulene | 28.62 | 1513 | 2570.51 ± 119.99 | 2 | Cool, Flower | MS/RI |
| β-Selinene | 28.89 | 1524 | 414.90 ± 350.10 | 2 | Forest | MS |
| β-Humulene | 30.04 | 1573 | 9.51 ± 13.45 | 2 | Forest | MS |
| Heterocyclics (2) | ||||||
| 2,5-Diethyltetrahydro-5-diethyltetrahydrofuran | 11.41 | 911 | 2.96 ± 3.63 | 2 | Cool | MS |
| Limonene oxide | 18.68 | 1139 | 0.12 ± 0.17 | 3 | Sweet | MS/RI |
| Ketone (1) | ||||||
| Carvone | 22.55 | 1275 | 479.75 ± 493.67 | 4 | Mint | MS |
| Group | Food Intake (g/day) | Initial Length (cm) | Final Length (cm) | Length Gain (cm) |
|---|---|---|---|---|
| N | 18.18 ± 0.02 a | 17.1 ± 0.1 a,b | 27.0 ± 0.1 b,c | 9.9 ± 0.1 c |
| H | 16.90 ± 1.69 a,b | 17.6 ± 0.1 a | 26.8 ± 0.4 c | 9.2 ± 0.3 d |
| H-LPI | 14.88 ± 0.23 b | 17.1 ± 0.3 a,b | 26.9 ± 0.2 c | 9.8 ± 0.1 c |
| H-HPI | 15.97 ± 0.13 a,b | 16.7 ± 0.2 b | 27.8 ± 0.3 a,b | 11.1 ± 0.1 b |
| H-LPT | 15.59 ± 0.07 a,b | 16.6 ± 0.2 b | 28.2 ± 0.5 a | 11.6 ± 0.3 a,b |
| H-HPT | 16.74 ± 0.01 a,b | 16.6 ± 0.1 b | 28.6 ± 0.3 a | 12.0 ± 0.2 a |
| Group | Brain | Liver | Kidney | Heart | WAT | BAT |
|---|---|---|---|---|---|---|
| N | 4.20 ± 0.01 a | 24.82 ± 0.07 a | 5.35 ± 0.01 a | 2.85 ± 0.03 a | 37.57 ± 1.25 d | 0.61 ± 0.05 a,b |
| H | 3.91 ± 0.06 b | 20.72 ± 0.36 b | 5.08 ± 0.11 a,b | 2.55 ± 0.04 b,c | 58.48 ± 1.65 b,c | 0.72 ± 0.06 a |
| H-LPI | 4.20 ± 0.06 a | 23.06 ± 1.30 a | 5.33 ± 0.17 a,b | 2.71 ± 0.02 a,b | 57.23 ± 0.92 b,c | 0.60 ± 0.11 a,b |
| H-HPI | 3.43 ± 0.05 d | 21.07 ± 0.58 b | 4.58 ± 0.03 c | 2.45 ± 0.04 c | 72.10 ± 5.98 a | 0.59 ± 0.02 a,b |
| H-LPT | 3.50 ± 0.02 c,d | 20.25 ± 0.80 b | 4.90 ± 0.31 b,c | 2.52 ± 0.01 c | 55.46 ± 1.68 c | 0.66 ± 0.05 a |
| H-HPT | 3.65 ± 0.16 c | 20.77 ± 0.26 b | 4.65 ± 0.10 c | 2.49 ± 0.14 c | 64.18 ± 0.18 b | 0.50 ± 0.01 b |
| HDL (mg/dL) | TC (mg/dL) | LDL (mg/dL) | AI (mg/dL) | CRF (mg/dL) | LHR (mg/dL) | TG (mg/dL) | Leptin (pg/mL) | AST (Karmen/mL) | ALT (Karmen/mL) | |
|---|---|---|---|---|---|---|---|---|---|---|
| N | 28.80 ± 3.48 c | 148.89 ± 5.61 a,b | 109.50 ± 4.34 a | 4.20 ± 0.45 a | 5.20 ± 0.45 a | 3.83 ± 0.30 a | 120.26 ± 4.79 a | 2954.50 ± 380.31 a | 21.78 ± 3.29 a | 54.60 ± 2.47 b,c |
| H | 34.87 ± 3.79 c | 149.53 ± 8.86 a,b | 114.66 ± 9.01 a | 3.32 ± 0.50 a,b | 4.32 ± 0.50 a,b | 3.32 ± 0.50 a | 115.74 ± 5.45 a | 4204.50 ± 434.33 a | 10.16 ± 5.47 a | 85.61 ± 27.54 a,b |
| H-LPI | 42.54 ± 10.00 b,c | 136.68 ± 4.18 b | 73.72 ± 4.28 b | 2.31 ± 0.64 b,c | 3.31 ± 0.64 b,c | 1.79 ± 0.39 b | 137.45 ± 11.39 a | 4021.06 ± 1189.34 a | 24.73 ± 7.57 a | 111.68 ± 5.24 a |
| H-HPI | 59.77 ± 3.24 a | 144.44 ± 8.11 b | 90.52 ± 0.86 b | 1.42 ± 0.23 c | 2.42 ± 0.23 c | 1.51 ± 0.07 b | 118.85 ± 14.80 a | 3079.72 ± 850.18 a | 20.16 ± 5.75 a | 110.75 ± 1.99 a |
| H-LPT | 54.26 ± 3.65 a,b | 166.49 ± 8.81 a | 113.73 ± 6.30 a | 2.08 ± 0.34 c | 3.07 ± 0.34 c | 2.10 ± 0.16 b | 147.14 ± 58.99 a | 2659.33 ± 439.30 a | 19.69 ± 8.61 a | 52.21 ± 0.87 c |
| H-HPT | 57.95 ± 1.07 a | 145.38 ± 9.13 b | 87.43 ± 10.01 b | 1.51 ± 0.20 c | 2.51 ± 0.20 c | 1.51 ± 0.20 b | 144.82 ± 9.23 a | 3239.72 ± 252.16 a | 12.31 ± 1.00 a | 53.98 ± 4.25 b,c |
| Initial Period | Obesity-Induced Period | Final Period | |
|---|---|---|---|
| Systolic (mmHg) | |||
| N | 135.7 ± 1.2 a,b | 218.0 ± 3.5 b | 226.7 ± 4.5 a,b |
| H | 156.0 ± 7.8 a | 248.3 ± 4.0 a | 235.7 ± 4.9 a |
| H-LPI | 148.7 ± 15.6 a,b | 197.0 ± 4.6 b,c | 224.0 ± 6.0 a,b,c |
| H-HPI | 148.7 ± 11.5 a,b | 208.0 ± 8.9 b,c | 211.3 ± 5.9 c |
| H-LPT | 128.7 ± 8.4 b | 203.7 ± 8.4 c | 219.7 ± 3.5 b,c |
| H-HPT | 130.7 ± 1.5 a,b | 193.0 ± 14.2 c | 215.7 ± 4.9 b,c |
| Diastolic (mmHg) | |||
| N | 76.7 ± 5.1 a | 99.7 ± 6.8 a,b | 91.3 ± 2.1 b |
| H | 82.7 ± 5.8 a | 110.7 ± 19.9 a | 140.0 ± 36.5 a |
| H-LPI | 98.7 ± 28.2 a | 64.7 ± 16.8 b | 115.0 ± 4.4 a,b |
| H-HPI | 94.3 ± 18.1 a | 77.3 ± 7.0 a,b | 104.0 ± 7.9 a,b |
| H-LPT | 79.0 ± 4.4 a | 76.0 ± 15.1 a,b | 96.3 ± 15.9 a,b |
| H-HPT | 65.0 ± 23.3 a | 65.7 ± 4.6 b | 127.0 ± 11.5 a,b |
| Pulse (beats/min) | |||
| N | 477.7 ± 11.4 a | 383.7 ± 1.5 a,b | 366.0 ± 1.7 b |
| H | 421.0 ± 12.5 b | 414.3 ± 3.8 a | 382.7 ± 15.5 a,b |
| H-LPI | 404.3 ± 18.1 b | 383.0 ± 38.1 a,b | 372.0 ± 18.5 a,b |
| H-HPI | 381.0 ± 19.0 b | 354.0 ± 22.3 b | 363.7 ± 24.1 b |
| H-LPT | 411.7 ± 17.1 b | 384.7 ± 2.1 a,b | 420.3 ± 18.5 a |
| H-HPT | 394.3 ± 4.0 b | 372.3 ± 5.1 a,b | 396.0 ± 24.0 a,b |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hong, S.J.; Cho, J.; Boo, C.G.; Youn, M.Y.; Pan, J.H.; Kim, J.K.; Shin, E.-C. Inhalation of Patchouli (Pogostemon Cablin Benth.) Essential Oil Improved Metabolic Parameters in Obesity-Induced Sprague Dawley Rats. Nutrients 2020, 12, 2077. https://doi.org/10.3390/nu12072077
Hong SJ, Cho J, Boo CG, Youn MY, Pan JH, Kim JK, Shin E-C. Inhalation of Patchouli (Pogostemon Cablin Benth.) Essential Oil Improved Metabolic Parameters in Obesity-Induced Sprague Dawley Rats. Nutrients. 2020; 12(7):2077. https://doi.org/10.3390/nu12072077
Chicago/Turabian StyleHong, Seong Jun, Jinju Cho, Chang Guk Boo, Moon Yeon Youn, Jeong Hoon Pan, Jae Kyeom Kim, and Eui-Cheol Shin. 2020. "Inhalation of Patchouli (Pogostemon Cablin Benth.) Essential Oil Improved Metabolic Parameters in Obesity-Induced Sprague Dawley Rats" Nutrients 12, no. 7: 2077. https://doi.org/10.3390/nu12072077
APA StyleHong, S. J., Cho, J., Boo, C. G., Youn, M. Y., Pan, J. H., Kim, J. K., & Shin, E.-C. (2020). Inhalation of Patchouli (Pogostemon Cablin Benth.) Essential Oil Improved Metabolic Parameters in Obesity-Induced Sprague Dawley Rats. Nutrients, 12(7), 2077. https://doi.org/10.3390/nu12072077