Special Low Protein Foods in the UK: An Examination of Their Macronutrient Composition in Comparison to Regular Foods
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. Energy
3.2. Protein and Phenylalanine
3.3. Carbohydrate (Including Sugars)
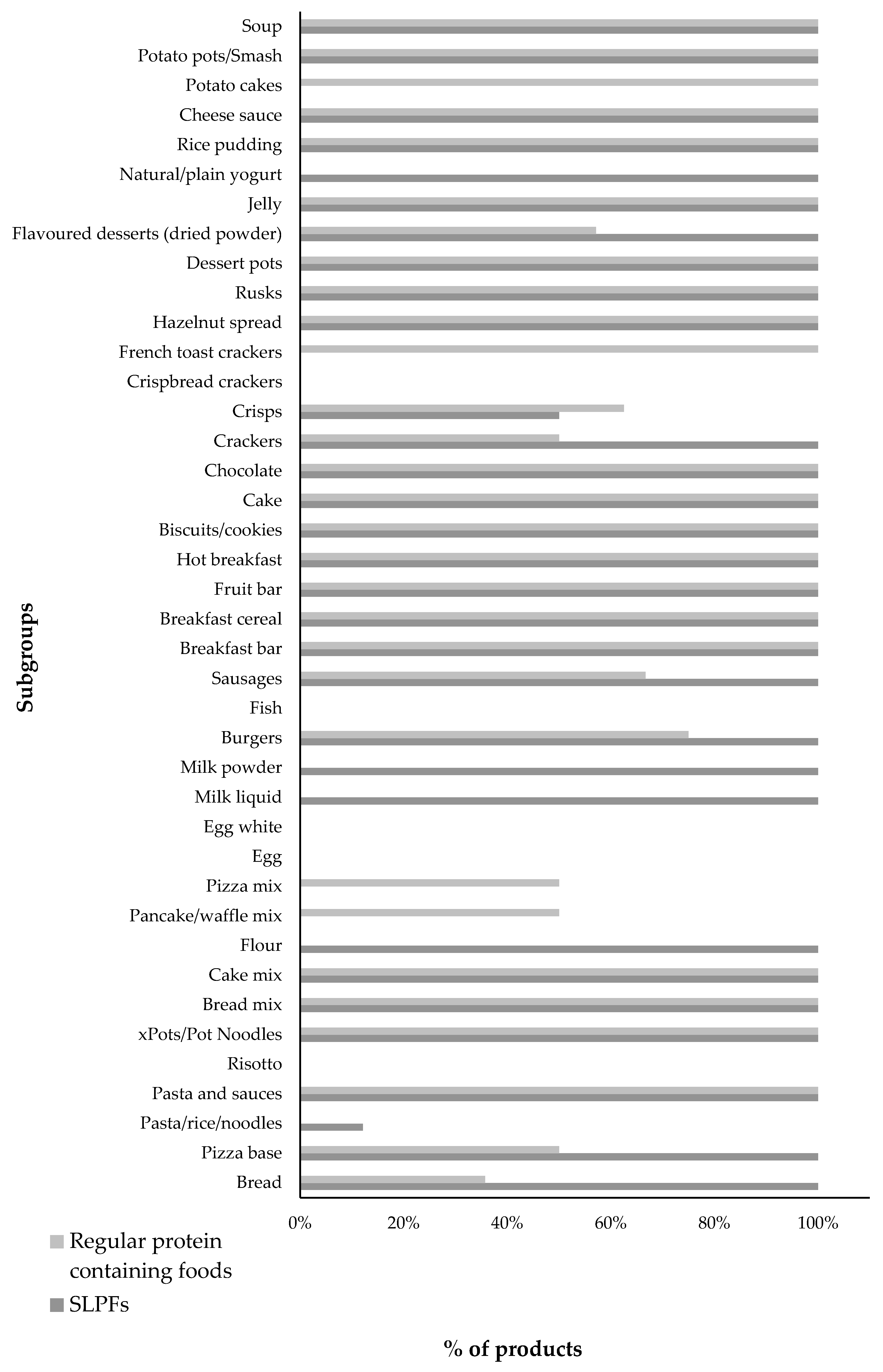
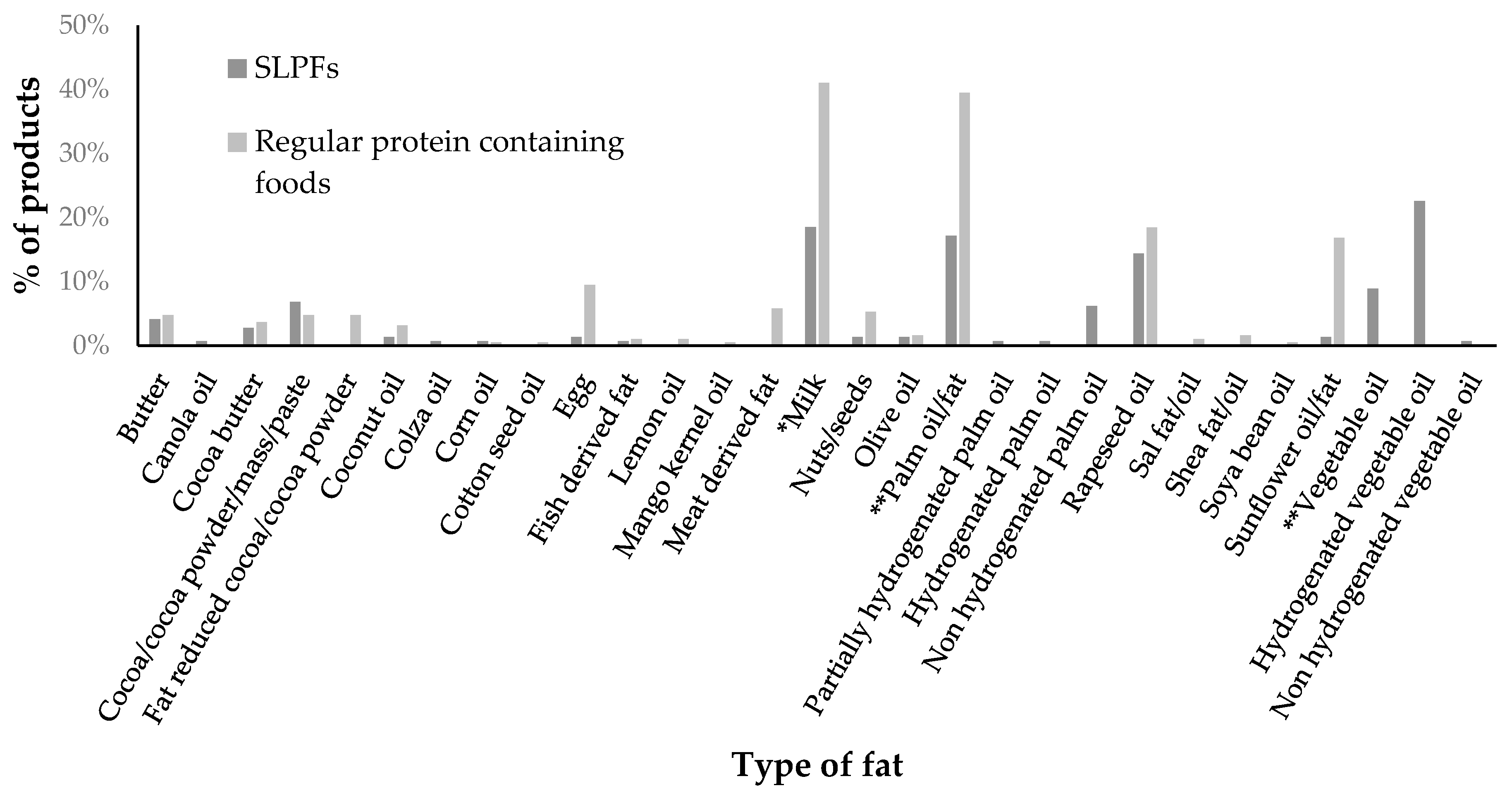
3.4. Total and Saturated Fat
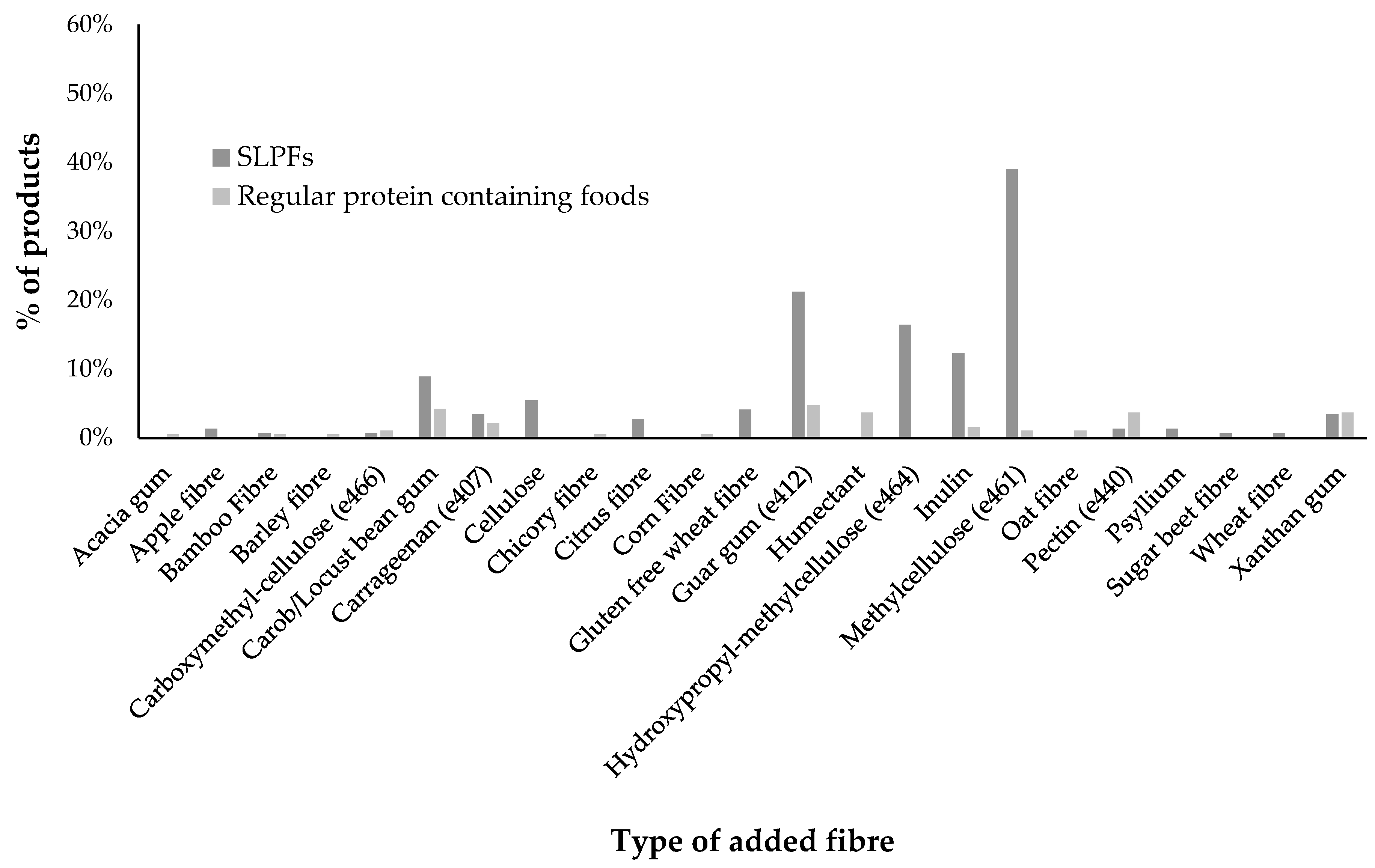
3.5. Fibre
3.6. Salt
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
| Product | Energy (kcal) per 100 g | Protein (g) per 100 g | Phenylalanine (mg) per 100 g | Total Carbohydrate (g) per 100 g | Carbohydrate of Which Is Sugars (g) per 100 g per 100 g | Fibre (g) per 100 g | Total Fat (g) per 100 g | Saturated Fat (g) per 100 g | Salt (g) per 100 g | |
|---|---|---|---|---|---|---|---|---|---|---|
| Breads/Pizza bases | ||||||||||
| Bread | SLPF (n = 13) | 244 | 0.6 | 15 | 47.1 | 3 | 9.2 | 4.3 | 1.2 | 0.5 |
| (214–266) | (0.2–1.0) | (8–30) | (37.0–53.8) | (1.4–4.3) | (3.8–16.0) | (2.7–5.3) | (0.3–2.3) | (0.3–1.3) | ||
| Regular (n = 14) | 255 | 9.7 | 485 | 46.6 | 3.1 | 4 | 2.5 | 0.5 | 0.9 | |
| (221–285) | (8.4–11.9) | (420–595) | (31.4–58.8) | (2.2–4.1) | (1.6–12.4) | (0.6–7.5) | (0.2–1.4) | (0.7–1.1) | ||
| % Difference | −4% | −94% | −97% | 1% | −3% | 130% | 72% | 140% | −44% | |
| Pizza base | SLPF (n = 2) | 290 | 0.9 | 13 | 55.7 | 4.9 | 7.8 | 5.4 | 1.7 | 0.5 |
| (263–316) | (0.8–0.9) | (2–24) | (49.0–62.3) | (4.7–5.0) | (2.6–13) | (4.2–6.5) | (1.4–2.0) | (0.3–0.8) | ||
| Regular (n = 2) | 296 | 8.9 | 445 | 54.3 | 2.4 | 2.7 | 4.2 | 0.6 | 1.4 | |
| (288–304) | (8.8–9.0) | (440–450) | (51.6–57.0) | (2.4–2.4) | (2.6–2.8) | (2.1–6.3) | (0.3–0.9) | (1.4–1.4) | ||
| % Difference | −2% | −90% | −97% | 3% | 104% | 189% | 29% | 183% | −64% | |
| Pasta/rice/noodles | ||||||||||
| Pasta/rice/noodles | SLPF (n = 33) | 356 | 0.3 | 13 | 85.8 | 0.6 | 3.1 | 0.9 | 0.5 | 0.1 |
| (343–366) | (0.1–0.5) | (8–25) | (79.0–88.1) | (0.0–3.2) | (0.2–7.3) | (0.6–1.6) | (0.2–0.9) | (0.1–0.5) | ||
| Regular (n = 23) | 356 | 11.9 | 595 | 72.5 | 2.4 | 2.9 | 1.8 | 0.4 | 0.1 | |
| (336–380) | (7.2–14.0) | (360–700) | (68.6–78.1) | (0.0–4.8) | (1.0–4.3) | (0.7–3.3) | (0.2–0.9) | (0.0–0.8) | ||
| % Difference | 0% | −97% | −98% | 18% | −75% | 7% | −50% | 25% | 0% | |
| Pasta and sauce | SLPF (n = 5) | 123 | 0.5 | 8 | 25.9 | 1.9 | No values | 2 | 0.6 | 0.8 |
| (98–140) | (0.3–0.6) | (3–14) | (23.9–31.3) | (0.4–4.9) | (0.1–1.1) | (0.0–1.1) | (0.6–1.0) | |||
| Regular (n = 10) | 104 | 3.5 | 175 | 18.1 | 2.5 | 1.2 | 1.6 | 0.8 | 0.6 | |
| (81–137) | (2.7–4.8) | (135–240) | (14.0–25.1) | (0.8–4.6) | (<0.5–2.1) | (0.6–4.1) | (0.1–2.4) | (0.3–0.8) | ||
| % Difference | 18% | −86% | −95% | 43% | −24% | − | 25% | −25% | 33% | |
| Risotto | SLPF (n = 1) | 103 | 0.3 | 6 | 14 | <0.2 | 0.5 | 5 | 1.3 | 0.7 |
| Regular (n = 2) | 95 | 2.9 | 145 | 13.8 | 1.4 | 1.4 | 3 | 1.1 | 0.5 | |
| (93–97) | (2.3–3.4) | (115–170) | (13.6–14.0) | (1.0–1.7) | (1 value) | (2.3–3.6) | (1.1–1.1) | (0.4–0.5) | ||
| % Difference | 8% | −90% | −96% | 1% | −86% | −64% | 67% | 18% | 40% | |
| xPots/pot noodles | SLPF (n = 4) | 138 | 0.4 | 9 | 23 | 1.8 | No values | 4.8 | 0.9 | 1.9 |
| (136–140) | (0.3–0.6) | (6–15) | (22.6–23.5) | (1.6–2.1) | (4.5–5.1) | (0.7–1.1) | (1.6–2.3) | |||
| Regular (n = 8) | 131 | 2.9 | 145 | 19.1 | 1.5 | 1.1 | 4.5 | 1.9 | 0.5 | |
| (83–145) | (2.3–3.5) | (115–175) | (17.4–21.6) | (0.9–2.3) | (0.8–1.3) | (0.3–5.7) | (<0.1–2.9) | (0.4–0.7) | ||
| % Difference | 5% | −86% | −94% | 20% | 20% | − | 7% | −54% | 280% | |
| Flour/mixes | ||||||||||
| Bread mix | SLPF (n = 3) | 347 | 0.4 | 15 | 83 | 2.8 | 2.5 | 0.6 | 0.3 | 0.4 |
| (339–354) | (0.1–0.7) | (4–20) | (80.1–86.0) | (1.7–4.6) | (2.0–3.0) | (0.5–0.7) | (0.1–0.5) | (0.1–0.6) | ||
| Regular (n = 2) | 338 | 13.1 | 655 | 70.4 | 3.1 | 3.1 | 1.6 | 0.3 | 1.6 | |
| (334–341) | (13.0–13.1) | (650–655) | (67.6–73.1) | (1.8–4.4) | (2.8–3.4) | (1.2–2.0) | (0.3–0.3) | (1.3–1.9) | ||
| % Difference | 3% | −97% | −98% | 18% | −10% | −19% | −63% | 0% | −75% | |
| Cake mix | SLPF (n = 4) | 366 | 0.5 | 14 | 89 | 39.6 | 3.4 | 0.7 | 0.4 | 0.8 |
| (365–367) | (0.2–0.9) | (4–30) | (84.6–92.1) | (35.7–47.9) | (1.8–7.1) | (0.1–1.3) | (0.0–0.9) | (0.6–0.8) | ||
| Regular (n = 4) | 381 | 5.8 | 290 | 77.4 | 43.5 | 2.1 | 5 | 2.7 | 1.5 | |
| (370–395) | (4.6–6.9) | (230–345) | (74.7–81.9) | (32.8–47.6) | (1.1–3.4) | (4.7–5.3) | (2.5–2.9) | (1.2–2.1) | ||
| % Difference | −4% | −91% | −95% | 15% | −9% | 62% | −86% | −85% | −47% | |
| Flour | SLPF (n = 4) | 349 | 0.2 | 5 | 85.3 | 5.6 | 2.6 | 0.3 | 0.1 | 0.6 |
| (339–361) | (0.1–0.3) | (4–<10) | (80.1–88.3) | (4.6–7.2) | (2.1–3.1) | (0.0–0.5) | (0.1–0.2) | (0.4–0.7) | ||
| Regular (n = 2) | 335 | 9.8 | 490 | 70 | 1.5 | No values | 1.1 | 0.2 | 0.9 | |
| (330–340) | (9.6–9.9) | (480–495) | (67.9–72.0) | (1.3–1.7) | (0.7–1.4) | (0.1–0.2) | (0.8–1.1) | |||
| % Difference | 4% | −98% | −99% | 22% | 273% | − | −73% | −50% | −33% | |
| Pancake/waffle mix | SLPF (n = 1) | 353 | 0.5 | 22 | 86.5 | 14 | 0.6 | 0.4 | <0.1 | 0.2 |
| Regular (n = 2) | 434 | 9.3 | 465 | 72.1 | 9.6 | 2.6 | 1.3 | 0.2 | 3.1 | |
| (335–532) | (8.5–10.0) | (425–500) | (70.2–74.0) | (4.2–14.9) | (2.6–2.6) | (1.1–1.4) | (0.0–0.3) | (2.3–3.8) | ||
| % Difference | −19% | −95% | −95% | 20% | 46% | −77% | −69% | −51% | −94% | |
| Pizza mix (dried powder) | SLPF (n = 1) | 353 | 0.2 | <31 | 86.9 | <0.1 | No value | <0.5 | <0.1 | 1.4 |
| Regular (n = 2) | 379 | 12.1 | 605 | 70 | 3.9 | 4.3 | 4.7 | 1.7 | 0.4 | |
| (372–386) | (11.3–13.0) | (565–650) | (69.4–70.6) | (3.9–3.9) | (4.0–4.6) | (4.4–4.9) | (1.5–1.9) | (0.4–0.4) | ||
| % Difference | −7% | −98% | −95% | 24% | −97% | − | −89% | −94% | 250% | |
| Eggs/replacers | ||||||||||
| Egg | SLPF (n = 3) (prepared) | 44 | 0 | 1 | 10.7 | 0 | 0.5 | 0 | 0 | 0.1 |
| (32–68) | (0.0–0.0) | (1–1) | (7.5–16.8) | (0.0–0.0) | (0.3–0.7) | (0.0–0.0) | (0.0–0.0) | (0.0–0.1) | ||
| Regular (n = 2) | 131 | 12.6 | 630 | 0.2 | 0.2 | 0 | 9 | 2.5 | 0.4 | |
| (131–131) | (12.6–12.6) | (630–630) | (0.0–< 0.5) | (0.0–< 0.5) | Only 1 value | (9.0–9.0) | (2.5–2.5) | (0.4–0.4) | ||
| % Difference | −66% | −100% | −100% | 5250% | −100% | − | −100% | −100% | −75% | |
| Egg white | SLPF (n = 1) | 185 | Nil added | Nil added | Nil added | Nil added | 92.5 | Nil added | Nil added | 1 |
| Regular (n = 2) | 354 | 83.3 | 4165 | 3.4 | 0.3 | 5.3 | 0.4 | 0.1 | 2.6 | |
| (345–363) | (82.6–84.0) | (4130–4200) | (<0.5–6.3) | (0.0–< 0.5) | Only 1 value | (0.2–< 0.5) | (<0.1–0.1) | (1.8–3.4) | ||
| % Difference | −48% | − | − | − | − | 1645% | − | − | −62% | |
| Milk/replacers | ||||||||||
| Milk (liquid) | SLPF (n = 4) | 62 | 0.2 | 6 | 7.6 | 4.5 | 0.5 | 3.3 | 1.7 | 0.1 |
| (40–89) | (0.0–0.4) | (0–10) | (5.0–10.8) | (3.5–5.8) | (0.2–0.8) | (2.0–4.7) | (1.3–2.3) | (0.0–0.2) | ||
| Regular (n = 2) | 58 | 3.5 | 175 | 4.8 | 4.8 | 0 | 2.7 | 1.7 | 0.1 | |
| (50–65) | (3.4–3.6) | (170–180) | (4.7–4.8) | (4.7–4.8) | (0.0–0.0) | (1.8–3.6) | (1.1–2.3) | (0.1–0.1) | ||
| % Difference | 7% | −94% | −97% | 58% | −6% | − | 22% | 0% | 0% | |
| Milk (powder) | SLPF (n = 1) | 428 | 1.7 | 20 | 77.5 | 45.1 | No value | 12.3 | 6.2 | 0.7 |
| Regular (n = 2) | 428 | 30.8 | 1540 | 43.5 | 43.2 | 0.5 | 14.4 | 9 | 1 | |
| (353–503) | (25.7–35.9) | (1285–1795) | (36.5–50.5) | (36.5–49.8) | (0.0–1.0) | (0.6–28.2) | (0.4–17.6) | (0.9–1.1) | ||
| % Difference | 0% | −94% | −99% | 78% | 4% | − | −15% | −31% | −30% | |
| Meat/replacers | ||||||||||
| Burgers | SLPF (n = 3) | 155 | 0.7 | 25 | 27.9 | 2.2 | 7.4 | 4.1 | 2.7 | 0.7 |
| (155–157) | (0.4–0.8) | (16–31) | (27.4–28.9) | (2.0–2.7) | Only 1 value | (2.7–4.9) | (1.5–3.2) | (0.5–0.8) | ||
| Regular (n = 4) | 249 | 22 | 1100 | 5 | 1.2 | 0.4 | 15.7 | 7.4 | 0.9 | |
| (226–280) | (17.0–25.6) | (850–1280) | (1.2–10.0) | (<0.5–3.3) | (0.0–0.7) | (13.0–17.4) | (6.2–7.9) | (0.7–1.1) | ||
| % Difference | −38% | −97% | −98% | 458% | 83% | 1750% | −74% | −64% | −22% | |
| Fish | SLPF (n = 1) | 138 | 1.1 | 38 | 27.8 | 1.1 | 10.3 | 0.2 | 0 | 2.3 |
| Regular (n = 2) | 98 | 22.5 | 1125 | 0.3 | 0.1 | 0.2 | 0.8 | 0.3 | 0.2 | |
| (98–98) | (21.8–23.1) | (1090–1155) | (0.0–0.5) | (0.0–0.1) | (0.0–0.3) | (0.3–1.2) | (0.1–0.4) | (0.1–0.3) | ||
| % Difference | 41% | −95% | −97% | 9167% | 1000% | 5050% | −75% | −100% | 1050% | |
| Sausages | SLPF (n = 3) | 146 | 0.8 | 33 | 27.8 | 4.1 | No values | 4 | 2.6 | 0.8 |
| (140–150) | (0.6–0.9) | (29–38) | (27.1–28.4) | (1.8–6.3) | (3.1–4.6) | (2.1–2.8) | (0.7–0.9) | |||
| Regular (n = 6) | 260 | 16.2 | 810 | 7.3 | 3 | 1.9 | 18 | 7.9 | 1.4 | |
| (200–309) | (14.0–21.2) | (700–1060) | (0.7–16.0) | (0.7–6.5) | (1.0–3.8) | (13.0–24.5) | (5.0–13.2) | (1.0–1.9) | ||
| % Difference | −44% | −95% | −96% | 281% | 37% | − | −78% | −67% | −43% | |
| Breakfast and cereal bars | ||||||||||
| Breakfast bar | SLPF (n = 4) | 472 | 0.3 | 17 | 67.2 | 30.5 | No values | 22.3 | 14.1 | 0.5 |
| (464–487) | (0.2–0.5) | (12–25) | (65.5–68.7) | (26.2–33.5) | (20.8–24.4) | (13.0–15.4) | (0.5–0.6) | |||
| Regular (n = 8) | 413 | 7.5 | 375 | 62.7 | 24.6 | 5.9 | 13.9 | 4.1 | 0.4 | |
| (372–485) | (4.7–15.0) | (235–750) | (42.0–74.0) | (19.0–36.1) | (4.3–10.0) | (6.6–26.0) | (0.8–10.4) | (0.0–0.9) | ||
| % Difference | 14% | −96% | −95% | 7% | 24% | − | 60% | 244% | 25% | |
| Breakfast cereal (dried) | SLPF (n = 3) | 380 | 0.4 | 12 | 92.5 | 35.6 | 1.6 | 0.9 | 0.8 | 0.2 |
| (374–385) | (0.2–0.6) | (6–22) | (91.0–93.6) | (34.0–38.9) | (1.1–2.3) | (0.7–1.1) | (0.6–0.9) | (0.2–0.2) | ||
| Regular (n = 6) | 385 | 7.7 | 385 | 78.8 | 19.7 | 5 | 3.3 | 0.7 | 0.7 | |
| (378–398) | (6.0–9.4) | (300–470) | (72.0–84.0) | (8.0–35.0) | (2.5–8.9) | (0.9–4.6) | (0.2–0.9) | (0.2–1.1) | ||
| % Difference | −1% | −95% | −97% | 17% | 81% | −68% | −73% | 14% | −71% | |
| Fruit bar | SLPF (n = 1) | 424 | 0.6 | 16 | 72 | 38 | 3.6 | 14 | 7 | 0.3 |
| Regular (n = 2) | 358 | 4.1 | 205 | 69.7 | 34 | 3.1 | 7.2 | 2.8 | 0.5 | |
| (351–364) | (3.9–4.2) | (195–210) | (67.0–72.3) | (33.0–34.9) | (2.4–3.8) | (6.0–8.3) | (2.5–3.0) | (0.4–0.6) | ||
| % Difference | 18% | −85% | −92% | 3% | 12% | 16% | 94% | 150% | −40% | |
| Hot breakfast cereal (with water) | SLPF (n = 4) | 137 | 0.1 | 4 | 31.5 | 8.3 | No values | 1.1 | 0.7 | 0.2 |
| (130–147) | (0.0–0.1) | (2–6) | (30.0–33.5) | (6.5–10.0) | (1.0–1.4) | (0.6–1.0) | (0.1–0.2) | |||
| Regular (n = 4) | 97 | 3.8 | 190 | 16.6 | 5.6 | 1.6 | 1.3 | 0.3 | 0.1 | |
| (91–104) | (3.4–4.3) | (170–215) | (16.0–17.4) | (4.1–6.3) | (1.1–2.1) | (1.2–1.4) | (0.2–0.3) | (0.1–0.1) | ||
| % Difference | 41% | −97% | −98% | 90% | 48% | − | −15% | 133% | 100% | |
| Snacks | ||||||||||
| Biscuits/cookies | SLPF (n = 9) | 488 | 0.5 | 10 | 75.1 | 17.5 | 0.7 | 20.5 | 8.8 | 0.3 |
| (476–506) | (0.2–0.7) | (1–27) | (68.2–84.0) | (14.9–25.6) | (0.5–1.0) | (15.0–25.0) | (7.3–10.4) | (0.0–0.7) | ||
| Regular (n = 14) | 499 | 5.6 | 280 | 62.6 | 26.3 | 2.6 | 24.8 | 12.6 | 0.7 | |
| (475–531) | (4.1–7.1) | (205–355) | (48.0–72.6) | (16.2–38.1) | (1.3–5.5) | (19.0–32.1) | (2.8–19.0) | (0.5–1.1) | ||
| % Difference | −2% | −91% | −96% | 20% | −33% | −73% | −17% | −30% | −57% | |
| Cake | SLPF (n = 3) | 372 | 0.2 | 6 | 58 | 33.5 | 1.3 | 15.2 | 7.6 | 0.7 |
| (372–372) | (0.2–0.2) | (6–6) | (58.0–58.0) | (33.5–33.5) | (1.3–1.3) | (15.2–15.2) | (7.6–7.6) | (0.7–0.7) | ||
| Regular (n = 2) | 422 | 4.3 | 215 | 55.2 | 27.4 | No values | 21.2 | 2.1 | 0.3 | |
| (393–450) | (4.1–4.4) | (205–220) | (52.4–58.0) | (22.7–32.0) | (19.4–23.0) | (1.8–2.4) | (0.1–0.4) | |||
| % Difference | −12% | −95% | −97% | 5% | 22% | − | −28% | 262% | 133% | |
| Chocolate | SLPF (n = 2) | 566 | 0.3 | 12 | 54.2 | 51.1 | 5.4 | 37.7 | 27.7 | 0 |
| (549–583) | (0.2–0.4) | (<10–14) | (47.0–61.4) | (43.0–59.1) | (0.9–9.8) | (33.4–42) | (25–30.4) | (0.0–0.0) | ||
| Regular (n = 2) | 540 | 7 | 350 | 56.5 | 55.7 | 2.1 | 31.2 | 18.8 | 0.2 | |
| (534–546) | (6.7–7.3) | (335–365) | (56.0–57.0) | (55.4–56) | Only 1 value | (30.0–32.4) | (18.0–19.6) | (0.2–0.3) | ||
| % Difference | 5% | −96% | −97% | −4% | −8% | 157% | 21% | 47% | −100% | |
| Crackers | SLPF (n = 3) | 446 | 0.5 | 12 | 77.3 | 2.5 | 1 | 14.7 | 6.9 | 1.5 |
| (444–450) | (0.4–0.5) | (10–17) | (77.0–78.0) | (1.5–3.0) | (0.9–1.1) | (14.6–15.0) | (6.9–7.0) | (1.3–1.6) | ||
| Regular (n = 6) | 426 | 8.7 | 435 | 72.6 | 5.1 | 3.5 | 11 | 3.6 | 1.8 | |
| (360–470) | (5.7–10.1) | (285–505) | (66.4–82.6) | (1.6–15.0) | (2.5–4.2) | (1.0–19.6) | (0.2–8.7) | (1.2–2.4) | ||
| % Difference | 5% | −94% | −97% | 6% | −51% | −71% | 34% | 92% | −17% | |
| Crisps | SLPF (n = 4) | 437 | 0.3 | 16 | 77.8 | <0.1 | No values | 16.2 | 2.3 | 3.2 |
| (369–465) | (0.1–0.5) | (8–22) | (77.5–78.4) | (<0.1–<0.1) | (16.0–16.6) | (2.3–2.3) | (2.6–4.2) | |||
| Regular (n = 8) | 519 | 5.8 | 290 | 52.8 | 1.8 | 4 | 30.8 | 3.4 | 1.5 | |
| (499–536) | (3.6–6.7) | (180–335) | (51.0–57.1) | (0.2–3.6) | (3.1–4.3) | (28.7–33.0) | (2.5–8.9) | (1.0–2.5) | ||
| % Difference | −16% | −95% | −94% | 47% | −95% | − | −47% | −32% | 113% | |
| Crispbread crackers * | SLPF (n = 1) | 388 | 0.3 | 6 | 88 | 0.1 | 2.6 | 3.3 | 1.8 | 0.6 |
| Regular (n = 2) | 441 | 9.9 | 495 | 67.5 | 1.5 | 3.5 | 13.9 | 6.4 | 1.3 | |
| (440–442) | (9.7–10.0) | (485–500) | (67.2–67.7) | (1.4–1.6) | (3.1–3.8) | (13.5–14.3) | (6.2–6.5) | (1.3–1.3) | ||
| % Difference | −12% | −97% | −99% | 30% | −93% | −26% | −76% | −72% | −54% | |
| French toast crackers | SLPF (n = 1) | 413 | <1.0 | 30 | 76.3 | 5.2 | 7 | 10 | 5.6 | 0.1 |
| Regular (n = 2) | 440 | 8 | 400 | 75 | 18.3 | 2.9 | 11.4 | 5.1 | 0.4 | |
| (440–440) | (7.8–8.2) | (390–410) | (74.5–75.5) | (18.0–18.6) | (2.8–2.9) | (11.0–11.7) | (5.0–5.1) | (0.4–0.4) | ||
| % Difference | −6% | −99% | −93% | 2% | −72% | 141% | −13% | 10% | −75% | |
| Hazelnut spread | SLPF (n = 1) | 347 | 0.5 | 19 | 42 | 7 | 0.5 | 19.6 | 10.6 | 0.2 |
| Regular (n = 2) | 549 | 6.3 | 315 | 54.8 | 53.2 | 3.2 | 33.5 | 8.9 | 0.1 | |
| (539–558) | (6.3–6.3) | (315–315) | (52.0–57.5) | (50.0–56.3) | (3.2–3.2) | (30.9–36.0) | (7.2–10.6) | (0.1–0.1) | ||
| % Difference | −37% | −92% | −94% | −23% | −87% | −84% | −41% | 19% | 100% | |
| Rusks | SLPF (n = 1) | 388 | 0.3 | 4 | 68.8 | 24.5 | 0.3 | 12.1 | 7.6 | 0.3 |
| Regular (n = 2) | 410 | 7.8 | 390 | 75.2 | 26.5 | 4.6 | 7.6 | 3.6 | 0.2 | |
| (405–414) | (7.0–8.5) | (350–425) | (71.2–79.2) | (24.0–29.0) | (2.1–7.0) | (7.2–8) | (3.1–4.0) | (0.0–0.4) | ||
| % Difference | −5% | −96% | −99% | −9% | −8% | −93% | 59% | 111% | 50% | |
| Desserts | ||||||||||
| Dessert pot | SLPF (n = 2) | 181 | 0 | <4 | 27 | 12.1 | No values | 8.2 | 0.7 | 0.1 |
| (181–181) | (0.0–0.0) | (<4–<4) | (26.9–27.1) | (11.7–12.5) | (8.1–8.2) | (0.6–0.8) | (0.1–0.1) | |||
| Regular (n = 4) | 133 | 3.7 | 185 | 17.6 | 14.8 | 0.2 | 5.3 | 3.4 | 0.1 | |
| (114–181) | (3.3–4.3) | (165–215) | (15.4–20.0) | (13.0–20.0) | (3.4–9.3) | (2.6–5.1) | (0.1–0.2) | |||
| % Difference | 36% | −100% | −98% | 53% | −18% | − | 55% | −79% | 0% | |
| Flavoured desserts (dried powder) | SLPF (n = 4) | 406 | 0.4 | 20 | 91.5 | 48.3 | No values | 4.5 | 3.6 | 0.9 |
| (400–409) | (0.1–0.9) | (4–50) | (89.3–95.3) | (46.1–51.5) | (2.2–5.4) | (2.1–4.3) | (0.1–3.1) | |||
| Regular (n = 7) | 424 | 2.2 | 110 | 77.9 | 35.8 | 0.1 | 11.4 | 9.4 | 1.2 | |
| (352–485) | (0.4–4.6) | (20–230) | (71.4–87.5) | (0.1–58.3) | (0.0–0.2) | (0.2–20.9) | (0.1–17.5) | (0.0–2.4) | ||
| % Difference | −4% | −82% | −82% | 17% | 35% | − | −61% | −62% | −25% | |
| Jelly (dried) | SLPF (n = 2) | 356 | 0 | <2 | 88 | 87 | No values | 0 | 0 | 0 |
| (356–356) | (0.0–0.0) | (<2–<2) | (88.0–88.0) | (87.0–87.0) | (0.0–0.0) | (0.0–0.0) | (0.0–0.0) | |||
| Regular (n = 4) | 332 | 2.8 | 140 | 81 | 74.6 | No values | 0 | 0 | 0.3 | |
| (296–375) | (0.0–5.5) | (0–275) | (68.5–94.5) | (57.4–94.5) | (0.0–0.0) | (0.0–0.0) | (0.02–0.5) | |||
| % Difference | 7% | −100% | −99% | 9% | 17% | − | 0% | 0% | −100% | |
| Rice pudding | SLPF (n = 4) | 121 | 0.1 | 6 | 26.4 | 2.3 | No values | 1.6 | 1.5 | 0 |
| (119–122) | (0.1–0.2) | (5–8) | (26.3–26.6) | (1.3–2.8) | (1.4–1.8) | (1.3–1.7) | (0.0–0.0) | |||
| Regular (n = 6) | 102 | 3 | 150 | 17.6 | 11.1 | 0.3 | 2.2 | 1.2 | 0.2 | |
| (96–107) | (2.7–3.4) | (135–170) | (15.8–18.8) | (8.9–13.3) | (0.0–0.5) | (1.9–2.6) | (1.0–1.5) | (0.1–0.2) | ||
| % Difference | 19% | −97% | −96% | 50% | −79% | − | −27% | 25% | −100% | |
| Yogurt ** | SLPF (n = 1) | 61 | 0.1 | 2 | 8 | 1 | 1 | 2.6 | 1 | 0.1 |
| Regular (n = 2) | 75 | 4.4 | 220 | 4.5 | 4.5 | No values | 4.1 | 2.7 | 0.1 | |
| (68–82) | (3.7–5.1) | (185–255) | (3.4–5.6) | (3.4–5.6) | (3.7–4.5) | (2.4–2.9) | (0.1–0.2) | |||
| % Difference | −19% | −98% | −99% | 78% | −78% | − | −37% | −63% | 0% | |
| Other snacks/meals | ||||||||||
| Cheese sauce (prepared) | SLPF (n = 1) | 86 | 0.8 | 13 | 18.4 | 0.9 | No value | 1 | 0.7 | 0.9 |
| Regular (n = 2) | 76 | 1.4 | 70 | 9.5 | 1.5 | 0.5 | 3.4 | 2.4 | 0.9 | |
| (65–86) | (1.2–1.6) | (60–80) | (9.2–9.8) | (1.4–1.5) | (<0.5–0.5) | (2.0–4.8) | (1.1–3.6) | (0.7–1.0) | ||
| % Difference | 13% | −43% | −81% | 94% | −40% | − | −71% | −71% | 0% | |
| Potato cakes | SLPF (n = 1) | 165 | 0.8 | 46 | 30.9 | 0.6 | No value | 3.7 | 0.5 | 0.6 |
| Regular (n = 2) | 190 | 2.3 | 115 | 22.5 | 0.8 | 2 | 9.6 | 1.2 | 0.6 | |
| (175–205) | (1.9–2.6) | (95–130) | (21.0–23.9) | (<0.5–1.2) | (1.8–2.1) | (8.6–10.5) | (1.1–1.2) | (0.5–0.7) | ||
| % Difference | −13% | −65% | −60% | 37% | −25% | − | −61% | −58% | 0% | |
| Potato pots/Smash | SLPF (n = 3) | 112 | 0.5 | 25 | 22.8 | 0.6 | No values | 1.8 | 1 | 0.9 |
| (111–115) | (0.4–0.5) | (23–27) | (22.7–22.9) | (0.4–0.8) | (1.6–2.1) | (0.9–1.1) | (0.9–0.9) | |||
| Regular (n = 4) | 82 | 1.8 | 90 | 13.9 | 1 | 1.3 | 2 | 1.1 | 0.3 | |
| (75–87) | (1.6–2.1) | (80–105) | (12.0–15.4) | (0.7–1.4) | (1.1–1.3) | (1.5–2.2) | (0.8–1.4) | (0.1–0.5) | ||
| % Difference | 37% | −72% | −72% | 64% | −40% | − | −10% | −9% | 200% | |
| Soup | SLPF (n = 4) | 37 | 0.2 | 2 | 7.5 | 1.5 | No value | 0.6 | 0.3 | 0.6 |
| (35–40) | (0.2–0.4) | (1–2) | (6.6–8.5) | (1.4–1.8) | (0.3–0.8) | (0.1–0.4) | (0.4–0.8) | |||
| Regular (n = 8) | 37 | 0.7 | 35 | 6.2 | 2 | 0.4 | 1 | 0.6 | 0.5 | |
| (26–48) | (<0.5–1.1) | (<25–55) | (4.9–8.3) | (<0.5–4.5) | (0.1–0.5) | (0.4–1.9) | (0.1–1.4) | (0.5–0.6) | ||
| % Difference | 0% | −71% | −94% | 21% | −25% | − | −40% | −50% | 20% | |
References
- Van Wegberg, A.M.J.; MacDonald, A.; Ahring, K.; Bélanger-Quintana, A.; Blau, N.; Bosch, A.M.; Burlina, A.; Campistol, J.; Feillet, F.; Giżewska, M.; et al. The complete European guidelines on phenylketonuria: Diagnosis and treatment. Orphanet J. Rare Dis. 2017, 12, 162. Available online: https://ojrd.biomedcentral.com/articles/10.1186/s13023-017-0685-2 (accessed on 20 May 2020). [CrossRef] [PubMed]
- Ford, S.; O’Driscoll, M.; MacDonald, A. Living with phenylketonuria: Lessons from the PKU community. Mol. Genet. Metab. Rep. 2018, 17, 57–63. [Google Scholar] [CrossRef] [PubMed]
- Rocha, J.C.; MacDonald, A.; Trefz, F. Is overweight an issue in phenylketonuria? Mol. Genet. Metab. 2013, 110 (Suppl.), S18–S24. [Google Scholar] [CrossRef] [PubMed]
- Rocha, J.C.; MacDonald, A. Dietary intervention in the management of phenylketonuria: Current perspectives. Pediatr. Health Med. Ther. 2016, 7, 155–163. [Google Scholar] [CrossRef]
- Cochrane, B.; Schwahn, B.; Galloway, P.; Robinson, P.; Gerasimidis, K. A questionnaire survey on the usage of low protein staple foods by people with phenylketonuria in Scotland. J. Hum. Nutr. Diet. 2014, 27, 533–541. [Google Scholar] [CrossRef] [PubMed]
- European Commission. Commission Directive 1999/21/EC on dietary foods for special medical purposes. Off. J. Eur. Union 1999, 42, 29–36. [Google Scholar]
- Advisory Committee on Borderline Substances. Nutritional Legislation and Other Guidance with Which Products Must Comply. Available online: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/792996/Appendix3.pdf (accessed on 16 February 2020).
- Food Standards Agency. Food Information Regulations 2014: Summary Guidance for Food Business Operators and Enforcement Officers in Scotland, Wales and Northern Ireland. Available online: https://www.food.gov.uk/sites/default/files/media/document/fir−guidance2014.pdf (accessed on 16 February 2020).
- Department of Health. The Medical Food (England) Regulations. Statutory Instrument No. 845. 2000. Available online: http://www.legislation.gov.uk/uksi/2000/845/made (accessed on 16 February 2020).
- Pena, M.J.; Almeida, M.F.; Van Dam, E.; Ahring, K.; Bélanger-Quintana, A.; Dokoupil, K.; Gokmen-Ozel, H.; Lammardo, A.M.; MacDonald, A.; Robert, M.; et al. Special low protein foods for phenylketonuria: Availability in Europe and an examination of their nutritional profile. Orphanet J. Rare Dis. 2015, 10, 162. Available online: https://ojrd.biomedcentral.com/articles/10.1186/s13023-015-0378-7 (accessed on 20 May 2020). [CrossRef]
- Moretti, F.; Pellegrini, N.; Salvatici, E.; Rovelli, V.; Banderali, G.; Radaelli, G.; Scazzina, F.; Giovannini, M.; Verduci, E. Dietary glycemic index, glycemic load and metabolic profile in children with phenylketonuria. Nutr. Metab. Cardiovasc. Dis. 2017, 27, 176–182. [Google Scholar] [CrossRef]
- Dixon, M.; MacDonald, A.; White, F.; Stafford, J. Disorders of amino acid metabolism, organic acidaemias, and urea cycle disorders. In Clinical Paediatric Dietetics, 4th ed.; Shaw, V., Ed.; Wiley Blackwell: Chichester, UK, 2015; pp. 381–525. [Google Scholar]
- Karam, P.E.; Majdalani, M.N.; Daher, R.T.; Barhoumi, A.; Yazbeck, N. Cardiovascular disease biomarkers in patients with inborn errors of protein metabolism: A pilot study. J. Hum. Nutr. Diet. 2015, 28, 344–349. [Google Scholar] [CrossRef]
- Rocha, J.C.; van Spronsen, F.J.; Almeida, M.F.; Soares, G.; Quelhas, D.; Ramos, E.; Guimarães, J.T.; Borges, N. Dietary treatment in phenylketonuria does not lead to increased risk of obesity or metabolic syndrome. Mol. Genet. Metab. 2012, 107, 659–663. [Google Scholar] [CrossRef]
- Evans, M.; Truby, H.; Boneh, A. The relationship between dietary intake, growth and body composition in phenylketonuria. Mol. Genet. Metab. 2017, 122, 36–42. [Google Scholar] [CrossRef] [PubMed]
- Robertson, L.V.; Mcstravick, N.; Ripley, S.; Weetch, E.; Donald, S.; Adam, S.; Micciche, A.; Boocock, S.; MacDonald, A. Body mass index in adult patients with diet–treated phenylketonuria. J. Hum. Nutr. Diet. 2013, 26 (Suppl. 1), 1–6. [Google Scholar] [CrossRef] [PubMed]
- Verduci, E.; Banderali, G.; Moretti, F.; Lassandro, C.; Cefalo, G.; Radaelli, G.; Salvatici, E.; Giovannini, M. Diet in children with phenylketonuria and risk of cardiovascular disease: A narrative overview. Nutr. Metab. Cardiovasc. Dis. 2016, 26, 171–177. [Google Scholar] [CrossRef] [PubMed]
- Dhaka, V.; Gulia, N.; Ahlawat, K.S.; Khatkar, B.S. Trans fats–sources, health risks and alternative approach—A review. J. Food Sci. Technol. 2011, 48, 534–541. [Google Scholar] [CrossRef] [PubMed]
- Klonoff, D.C. Replacements for trans fats—Will there be an oil shortage? J. Diabetes Sci. Technol. 2007, 1, 415–422. [Google Scholar] [CrossRef] [PubMed]
- Hosseinpour−Niazi, S.; Mirmiran, P.; Hosseini−Esfahani, F.; Azizi, F. Is the metabolic syndrome inversely associates with butter, non–hydrogenated– and hydrogenated–vegetable oils consumption: Tehran lipid and glucose study. Diabetes Res. Clin. Pract. 2016, 112, 20–29. [Google Scholar] [CrossRef]
- Mach, F.; Baigent, C.; Catapano, A.L.; Koskinas, K.C.; Casula, M.; Badimon, L.; Chapman, M.J.; De Backer, G.G.; Delgado, V. 2019 ESC/EAS Guidelines for the management of dyslipidaemias: Lipid modification to reduce cardiovascular risk: The Task Force for the management of dyslipidaemias of the European Society of Cardiology (ESC) and European Atherosclerosis Society (EAS). Eur. Heart J. 2020, 41, 111–188. [Google Scholar] [CrossRef]
- Boateng, L.; Ansong, R.; Owusu, W.B.; Steiner-Asiedu, M. Coconut oil and palm oil’s role in nutrition, health and national development: A review. Ghana Med. J. 2016, 50, 189–196. [Google Scholar]
- Montoya, C.; Cochard, B.; Flori, A.; Cros, D.; Lopes, R.; Cuellar, T.; Espeout, S.; Syaputra, I.; Villeneuve, P.; Pina, M.; et al. Genetic architecture of palm oil fatty acid composition in cultivated oil palm (Elaeis guineensis Jacq.) compared to its wild relative E. oleifera (H.B.K) Cortés. PLoS ONE 2014, 9, e95412. Available online: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0095412 (accessed on 21 May 2020). [CrossRef]
- Mozaffarian, D. Dairy foods, obesity and metabolic health: The role of the food matrix compared with single nutrients. Adv. Nutr. 2019, 10, 917S–923S. [Google Scholar] [CrossRef]
- Soltanizadeh, N.; Mirmoghtadaie, L. Strategies used in production of phenylalanine–free foods for PKU management. Compr. Rev. Food Sci. Food Saf. 2014, 13, 287–299. [Google Scholar] [CrossRef]
- Schober, T.J. Manufacture of Gluten–Free Specialty Breads and Confectionery Products. In Gluten—Free Food Science and Technology; Gallagher, E., Ed.; Blackwell Publishing Ltd.: Oxford, UK, 2009; pp. 130–180. [Google Scholar]
- Henry, C.; Lightowler, H.; Kendall, F.; Storey, M. The impact of the addition of toppings/fillings on the glycaemic response to commonly consumed carbohydrate foods. Eur. J. Clin. Nutr. 2006, 60, 763–769. [Google Scholar] [CrossRef] [PubMed]
- Couce, M.L.; Sánchez-Pintos, P.; Vitoria, I.; De Castro, M.J.; Aldámiz-Echevarría, L.; Correcher, P.; Fernández-Marmiesse, A.; Roca, I.; Hermida, A.; Martínez-Olmos, M.; et al. Carbohydrate status in patients with phenylketonuria. Orphanet J. Rare Dis. 2018, 13, 103. Available online: https://ojrd.biomedcentral.com/articles/10.1186/s13023-018-0847-x (accessed on 21 May 2020). [CrossRef] [PubMed]
- Ormazabal, V.; Nair, S.; Elfeky, O.; Aguayo, C.; Salomon, C.; Zuñiga, F. Association between insulin resistance and the development of cardiovascular disease. Cardiovasc. Diabetol. 2018, 17, 122. Available online: https://cardiab.biomedcentral.com/articles/10.1186/s12933-018-0762-4#citeas (accessed on 27 May 2020). [CrossRef] [PubMed]
- El Khoury, D.; Balfour-Ducharme, S.; Joye, I.J. A review on the gluten–free diet: Technological and nutritional challenges. Nutrients 2018, 10, 1410. Available online: https://www.mdpi.com/2072-6643/10/10/1410 (accessed on 21 May 2020). [CrossRef]
- Viebke, C.; Al-Assaf, S.; Phillips, G.O. Food hydrocolloids and health claims. Bioact. Carbohydr. Diet. Fibre 2014, 4, 101–114. [Google Scholar] [CrossRef]
- Trefz, K.F.; Muntau, A.C.; Kohlscheen, K.M.; Altevers, J.; Jacob, C.; Braun, S.; Greiner, W.; Jha, A.; Jain, M.; Alvarez, I.; et al. Clinical burden of illness in patients with phenylketonuria (PKU) and associated comorbidities—A retrospective study of German health insurance claims data. Orphanet J. Rare Dis. 2019, 14, 181. Available online: https://ojrd.biomedcentral.com/articles/10.1186/s13023−019−1153−y (accessed on 21 May 2020). [CrossRef]
- Burton, B.K.; Bradford Jones, K.; Cederbaum, S.; Rohr, F.; Waisbren, S.; Irwin, D.E.; Kim, G.; Lilienstein, J.; Alvarez, I.; Jurecki, E.; et al. Prevalence of comorbid conditions among adult patients diagnosed with phenylketonuria. Mol. Genet. Metab. 2018, 125, 228–234. [Google Scholar] [CrossRef]
- Azabdaftari, A.; van der Giet, M.; Schuchardt, M.; Hennermann, J.B.; Plöckinger, U.; Querfeld, U. The cardiovascular phenotype of adult patients with phenylketonuria. Orphanet J. Rare Dis. 2019, 14, 213. Available online: https://ojrd.biomedcentral.com/articles/10.1186/s13023-019-1188-0 (accessed on 21 May 2020). [CrossRef]
- Hermida-Ameijeiras, A.; Crujeiras, V.; Roca, I.; Calvo, C.; Leis, R.; Couce, M.L. Arterial stiffness assessment in patients with phenylketonuria. Medicine 2017, 96, e9322. Available online: https://journals.lww.com/md-journal/Fulltext/2017/12220/Arterial_stiffness_assessment_in_patients_with.94.aspx (accessed on 21 May 2020).
- Rocha, J.C.; van Rijn, M.; van Dam, E.; Ahring, K.; Bélanger-Quintana, A.; Dokoupil, K.; Gokmen-Ozel, H.; Lammardo, A.M.; Robert, M.; Heidenborg, C.; et al. Weight Management in Phenylketonuria: What Should Be Monitored? Ann. Nutr. Metab. 2016, 68, 60–65. [Google Scholar] [CrossRef] [PubMed]
- Albersen, M.; Bonthuis, M.; de Roos, N.M.; van den Hurk, D.A.M.; Carbasius Weber, E.; Hendriks, M.M.W.B.; de Sain-van der Velden, M.G.M.; de Koning, T.J.; Visser, G. Whole body composition analysis by the BodPod air−displacement plethysmography method in children with phenylketonuria shows a higher body fat percentage. J. Inherit. Metab. Dis. 2010, 33 (Suppl. 3), S283–S288. [Google Scholar] [CrossRef] [PubMed]
- Belanger-Quintana, A.; Martínez-Pardo, M. Physical development in patients with phenylketonuria on dietary treatment: A retrospective study. Mol. Genet. Metab. 2011, 104, 480–484. [Google Scholar] [CrossRef] [PubMed]
- Burrage, L.C.; McConnell, J.; Haesler, R.; O’Riordan, M.A.; Sutton, V.R.; Kerr, D.S.; McCandless, S.E. High prevalence of overweight and obesity in females with phenylketonuria. Mol. Genet. Metab. 2012, 107, 43–48. [Google Scholar] [CrossRef] [PubMed]
- Doulgeraki, A.; Skarpalezou, A.; Theodosiadou, A.; Monopolis, I.; Schulpis, K. Body composition profile of young patients with phenylketonuria and mild hyperphenylalaninemia. Int. J. Endocrinol. Metab. 2014, 12, e16061. Available online: https://sites.kowsarpub.com/ijem/articles/17675.html (accessed on 21 May 2020). [CrossRef]
- Evans, S.; Ford, S.; Adam, S.; Adams, S.; Ash, J.; Ashmore, C.; Caine, G.; Carruthers, R.; Cawtherley, S.; Chahal, S.; et al. Development of national consensus statements on food labelling interpretation and protein allocation in a low phenylalanine diet for PKU. Orphanet J. Rare Dis. 2019, 14, 2. Available online: https://ojrd.biomedcentral.com/articles/10.1186/s13023−018−0950−z (accessed on 21 May 2020). [CrossRef]
- MacDonald, A.; Lilburn, M.; Davies, P.; Evans, S.; Daly, A.; Hall, S.K.; Hendriksz, C.; Chakrapani, A.; Lee, P. ‘Ready to drink’ protein substitute is easier is for people with phenylketonuria. J. Inherit. Metab. Dis. 2006, 29, 526–531. [Google Scholar] [CrossRef]
- MacDonald, A.; Lilburn, M.; Cochrane, B.; Davies, P.; Daly, A.; Asplin, D.; Hall, S.K.; Cousins, A.; Chakrapani, A.; Robinson, P.; et al. A new, low–volume protein substitute for teenagers and adults with phenylketonuria. J. Inherit. Metab. Dis. 2004, 27, 127–135. [Google Scholar] [CrossRef]
- Evans, S.; Adam, S.; Adams, S.; Allen, H.; Ashmore, A.; Bailey, S.; Banks, J.; Churchill, H.; Cochrane, B.; Cook, J.; et al. Uniformity of food protein interpretation amongst dietitians for patients with phenylketonuria (PKU): 2020 UK National Consensus Statements. Nutrients. under Review.
- Piepoli, M.F.; Abreu, A.; Albus, C.; Ambrosetti, M.; Brotons, C.; Catapano, A.L.; Corra, U.; Cosyns, B.; Deaton, C.; Graham, I.; et al. Update on cardiovascular prevention in clinical practice: A position paper of the European Association of Preventive Cardiology of the European Society of Cardiology. Eur. J. Prev. Cardiol. 2020, 27, 181–205. [Google Scholar] [CrossRef]
- Zmora, N.; Suez, J.; Elinav, E. You are what you eat: Diet, health and the gut microbiota. Nat. Rev. 2019, 16, 35–56. [Google Scholar] [CrossRef]
| SLPF Subgroup | Phenylalanine (mg) per 100 g of Product | Identified Sources of Natural Protein/Phenylalanine in Each SLPF Subgroup |
|---|---|---|
| Bread (n = 13) | 15 (8–30) | Yeast (n = 13), fennel seeds (n = 1), anis seeds (n = 1) |
| Pizza base (n = 2) | 13 (2–24) | Yeast (n = 2) |
| Pasta/rice/noodles (n = 33) | 13 (8–25) | Rice flour (n = 5) |
| Pasta and sauces (prepared) (n = 5) | 8 (3–14) | Milk (n = 4), yeast extract (n = 1), cheese powder (n = 1) |
| Risotto (n = 1) | 6 | Milk (n = 1) |
| xPots/pot noodles (prepared) (n = 4) | 9 (6–15) | Peas (dried) (n = 1), milk (n = 4) |
| Bread mix (n = 3) | 15 (4–20) | Yeast (n = 1) |
| Cake mix (n = 4) | 14 (4–30) | Cocoa powder (n = 1), cocoa (n = 1) |
| Flour (n = 4) | 5 (4–<10) | No sources identified |
| Pancake/waffle mix (n = 1) | 22 | No sources identified |
| Pizza mix (n = 1) | <31 | No sources identified |
| Egg replacer (dried mix) (n = 3) | 7 (<5–10) | No sources identified |
| Egg white replacer (n = 1) | Nil added | No sources identified |
| Milk (liquid) (n = 4) | 6 (0–10) | Milk (n = 4), whey powder (n = 2) |
| Milk (powder) (n = 1) | 20 | Milk (n = 1), whey permeate (n = 1) |
| Burgers (prepared) (n = 3) | 25 (16–31) | Milk (n = 2), yeast (n = 1) |
| Fish substitute (prepared) (n = 1) | 38 | Shrimps (n = 1), cod (n = 1), rice flour (n = 1), milk (n = 1) |
| Sausages (prepared) (n = 3) | 33 (29–38) | Milk (n = 3), potato flake (n = 3) |
| Breakfast bar (n = 4) | 17 (12–25) | Milk (n = 4), cocoa powder (n = 1) |
| Breakfast cereal (dried) (n = 3) | 12 (6–22) | Cocoa powder (n = 1) |
| Fruit bar (n = 1) | 16 | Egg (n = 1) |
| Hot breakfast cereal (prepared with water) (n = 4) | 4 (2–6) | Cocoa powder (n = 1), milk (n = 4) |
| Biscuits/cookies (n = 9) | 10 (1–27) | Cocoa mass (n = 1), egg (n = 1), cocoa (n = 2) |
| Cake (n = 3) | 6 (6–6) | No sources identified |
| Chocolate (n = 2) | 12 (<10–14) | Milk (n = 1), cocoa powder (n = 1), carob flour (n = 1) |
| Crackers (n = 3) | 12 (10–17) | No sources identified |
| Crisps (n = 4) | 16 (8–22) | Wheat flour (n = 2), rice flour (n = 1), whey powder (n = 2), yeast extract powder (n = 1), cheese powder (n = 1), yeast powder (n = 1) |
| Crispbread crackers (n = 1) | 6 | Pea starch (n = 1) |
| French toast crackers (n = 1) | 30 | Baker’s yeast (n = 1) |
| Hazelnut spread (n = 1) | 19 | Milk (n = 1), hazelnuts (n = 1), almonds (n = 1), cocoa paste (n = 1) |
| Rusks (n = 1) | 4 | Milk (n = 1) |
| Dessert pot (n = 2) | <4 | No sources identified |
| Flavoured desserts (prepared) (n = 4) | 5 (1–13) | Milk (n = 4), chocolate powder (n = 1) |
| Jelly (dried) (n = 2) | <2 | No sources identified |
| Rice pudding (n = 4) | 6 (5–8) | Milk (n = 4) |
| Yogurt (prepared) (n = 1) | 2 | No sources identified |
| Cheese sauce (prepared) (n = 1) | 13 | Milk (n = 1) |
| Potato cakes (prepared) (n = 1) | 46 | Potato flake (n = 1) |
| Potato pots/Smash (prepared) (n = 3) | 25 (23–27) | Potato flake (n = 3), milk (n = 3) |
| Soup (prepared) (n = 4) | 2 (1–2) | Milk (n = 4), peas (n = 2) |
| Key Sources of Added Sugar | % of SLPF (n = 146) | % of Regular Protein Containing Foods (n = 190) |
|---|---|---|
| Sugar | 52% (n = 76/146) | 58% (n = 111/190) |
| Glucose | 29% (n = 43/146) | 23% (n = 44/190) |
| Maltodextrin | 23% (n = 33/146) | 13% (n = 25/190) |
| Dextrose | 15% (n = 22/146) | 12% (n = 22/190) |
| Sucrose | 3% (n = 5/146) | 1% (n = 2/190) |
| Fructose | <1% (n = 1/146) | 6% (n = 12/190) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wood, G.; Evans, S.; Pointon-Bell, K.; Rocha, J.C.; MacDonald, A. Special Low Protein Foods in the UK: An Examination of Their Macronutrient Composition in Comparison to Regular Foods. Nutrients 2020, 12, 1893. https://doi.org/10.3390/nu12061893
Wood G, Evans S, Pointon-Bell K, Rocha JC, MacDonald A. Special Low Protein Foods in the UK: An Examination of Their Macronutrient Composition in Comparison to Regular Foods. Nutrients. 2020; 12(6):1893. https://doi.org/10.3390/nu12061893
Chicago/Turabian StyleWood, Georgina, Sharon Evans, Kiri Pointon-Bell, Júlio César Rocha, and Anita MacDonald. 2020. "Special Low Protein Foods in the UK: An Examination of Their Macronutrient Composition in Comparison to Regular Foods" Nutrients 12, no. 6: 1893. https://doi.org/10.3390/nu12061893
APA StyleWood, G., Evans, S., Pointon-Bell, K., Rocha, J. C., & MacDonald, A. (2020). Special Low Protein Foods in the UK: An Examination of Their Macronutrient Composition in Comparison to Regular Foods. Nutrients, 12(6), 1893. https://doi.org/10.3390/nu12061893







