Dietary Choices and Habits during COVID-19 Lockdown: Experience from Poland
Abstract
1. Introduction
2. Material and Methods
- Whether quarantine resulted in increased food consumption, snacking, and cooking;
- Daily number of consumed meals and snacks during quarantine;
- Frequency of consumption of selected food products (fresh vegetables and fruits, legumes, grain products, meat products, dairy, fast-foods, sweets, and salty snacks) during the quarantine;
- Frequency of breakfast consumption during quarantine;
- Observed weight change during quarantine;
- Alcohol consumption in the general population and in individuals addicted to alcohol during quarantine;
- Smoking frequency in smokers during quarantine;
- Level of fears of contracting SARS-CoV-2 during grocery shopping and through contact with food products.
3. Results and Discussion
3.1. Demographic Characteristics
3.2. Dietary Patterns
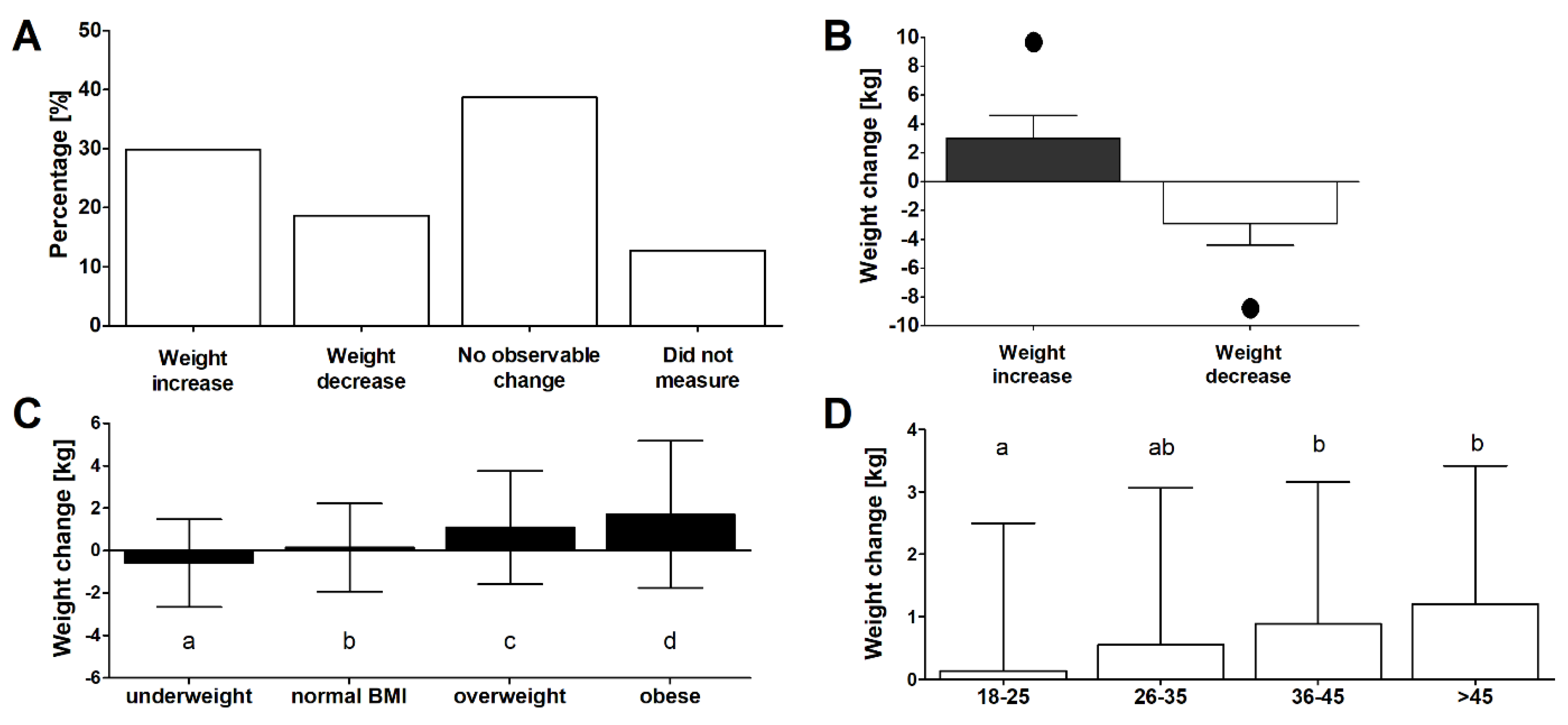
3.3. Reported Change of Weight
3.4. Alcohol Consumption and Smoking
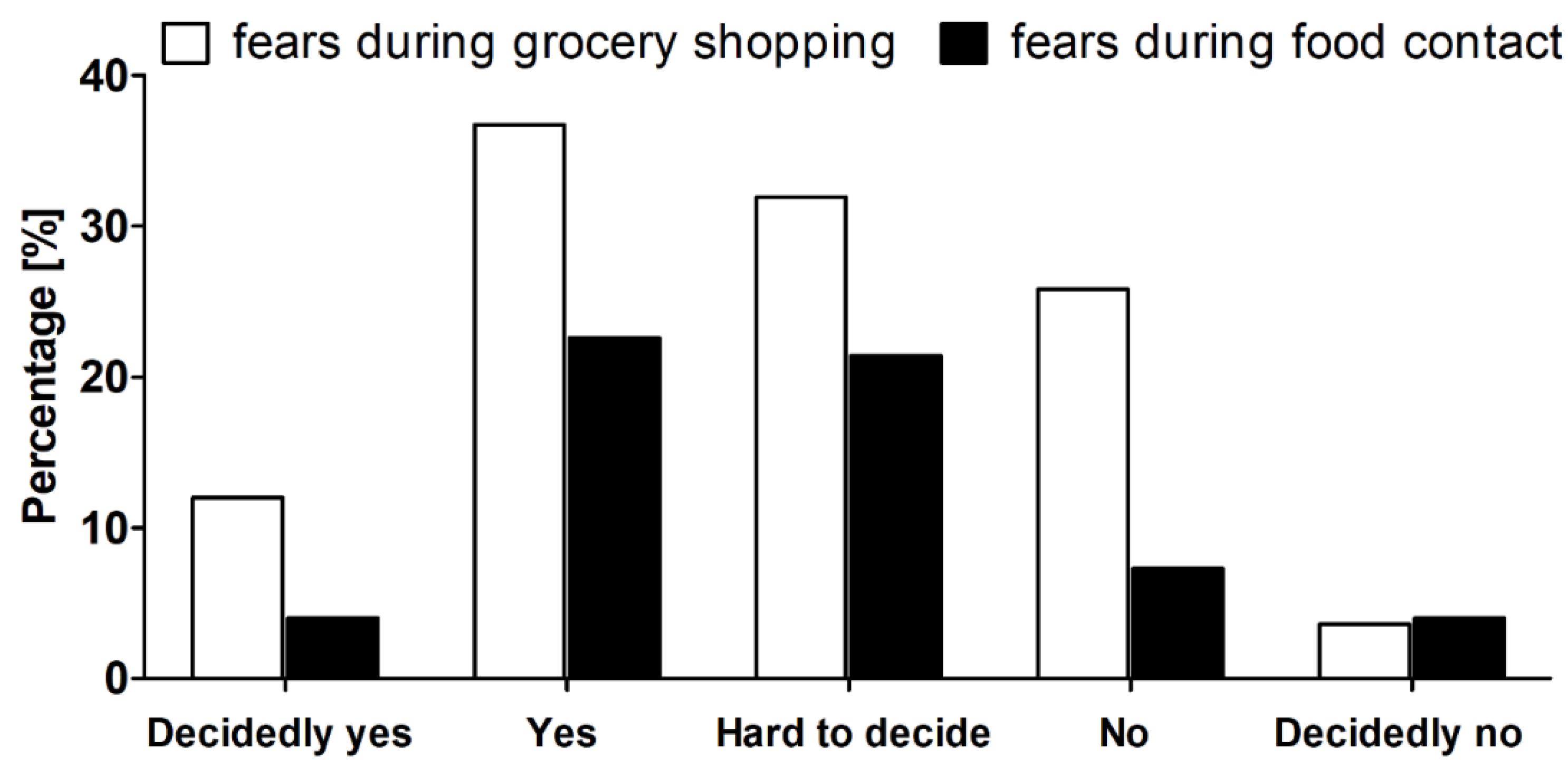
3.5. Fears During Grocery Shopping and Food Contact
3.6. Limitations
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Jiang, S.; Xia, S.; Ying, T.; Lu, L. A novel coronavirus (2019-nCoV) causing pneumonia-associated respiratory syndrome. Cell. Mol. Immunol. 2020. [Google Scholar] [CrossRef]
- Burki, T. Outbreak of coronavirus disease. Lancet Infect. Dis. 2019. [Google Scholar] [CrossRef]
- Cucinotta, D.; Vanelli, M. WHO Declares COVID-19 a Pandemic. Acta Bio-Med. Atenei Parm. 2020, 91, 157–160. [Google Scholar] [CrossRef]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef]
- Yoon, M.-K.; Kim, S.-Y.; Ko, H.-S.; Lee, M.-S. System effectiveness of detection, brief intervention and refer to treatment for the people with post-traumatic emotional distress by MERS: A case report of community-based proactive intervention in South Korea. Int. J. Ment. Health Syst. 2016, 10, 51. [Google Scholar] [CrossRef]
- Hawryluck, L.; Gold, W.L.; Robinson, S.; Pogorski, S.; Galea, S.; Styra, R. SARS control and psychological effects of quarantine, Toronto, Canada. Emerg. Infect. Dis. 2004, 10, 1206–1212. [Google Scholar] [CrossRef]
- Mihashi, M.; Otsubo, Y.; Yinjuan, X.; Nagatomi, K.; Hoshiko, M.; Ishitake, T. Predictive factors of psychological disorder development during recovery following SARS outbreak. Health Psychol. Off. J. Div. Health Psychol. Am. Psychol. Assoc. 2009, 28, 91–100. [Google Scholar] [CrossRef]
- Marjanovic, Z.; Greenglass, E.R.; Coffey, S. The relevance of psychosocial variables and working conditions in predicting nurses’ coping strategies during the SARS crisis: An online questionnaire survey. Int. J. Nurs. Stud. 2007, 44, 991–998. [Google Scholar] [CrossRef]
- Reynolds, D.L.; Garay, J.R.; Deamond, S.L.; Moran, M.K.; Gold, W.; Styra, R. Understanding, compliance and psychological impact of the SARS quarantine experience. Epidemiol. Infect. 2007, 136, 997–1007. [Google Scholar] [CrossRef]
- Wong, S.L. China Warns that Spread of Deadly Virus will Accelerate. Available online: https://www.ft.com/content/7bb597c8-3ff7-11ea-a047-eae9bd51ceba (accessed on 2 May 2020).
- Matthews, S.; Blanchard, S.; Boyd, C. Russia Closes its Eastern Border as Killer Coronavirus Spreads to EVERY Region of China: Death Toll Jumps to 170 and almost 8300 People Have Caught the Deadly SARS-like Infection Worldwide. Available online: https://www.dailymail.co.uk/health/article-7946387/Killer-coronavirus-spreads-region-China-death-toll-jumps-170.html (accessed on 2 May 2020).
- Hindu. Available online: https://www.thehindu.com/opinion/editorial/alarming-spread/article30677660.ece (accessed on 2 May 2020).
- Shimizu, K. 2019-nCoV, fake news, and racism. Lancet 2020, 395, 685–686. [Google Scholar] [CrossRef]
- Caulfield, T. Pseudoscience and COVID-19—We’ve had enough already. Nature 2020. [Google Scholar] [CrossRef] [PubMed]
- Yau, Y.H.C.; Potenza, M.N. Stress and eating behaviors. Minerva Endocrinol. 2013, 38, 255–267. [Google Scholar] [PubMed]
- Maniscalco, J.W.; Kreisler, A.D.; Rinaman, L. Satiation and stress-induced hypophagia: Examining the role of hindbrain neurons expressing prolactin-releasing Peptide or glucagon-like Peptide 1. Front. Neurosci. 2013, 6, 199. [Google Scholar] [CrossRef]
- Razzoli, M.; Bartolomucci, A. The Dichotomous Effect of Chronic Stress on Obesity. Trends Endocrinol. Metab. 2016, 27, 504–515. [Google Scholar] [CrossRef] [PubMed]
- Maniscalco, J.W.; Rinaman, L. Interoceptive modulation of neuroendocrine, emotional, and hypophagic responses to stress. Physiol. Behav. 2017, 176, 195–206. [Google Scholar] [CrossRef]
- Wu, P.; Liu, X.; Fang, Y.; Fan, B.; Fuller, C.J.; Guan, Z.; Yao, Z.; Kong, J.; Lu, J.; Litvak, I.J. Alcohol abuse/dependence symptoms among hospital employees exposed to a SARS outbreak. Alcohol. Alcohol. 2008, 43, 706–712. [Google Scholar] [CrossRef]
- Gasmi, A.; Noor, S.; Tippairote, T.; Dadar, M.; Menzel, A.; Bjørklund, G. Individual risk management strategy and potential therapeutic options for the COVID-19 pandemic. Clin. Immunol. 2020, 215, 108409. [Google Scholar] [CrossRef]
- Chandra, R.K. Nutrition, immunity and infection: From basic knowledge of dietary manipulation of immune responses to practical application of ameliorating suffering and improving survival. Proc. Natl. Acad. Sci. USA 1996, 93, 14304–14307. [Google Scholar] [CrossRef]
- Bhaskaram, P. Micronutrient malnutrition, infection, and immunity: An overview. Nutr. Rev. 2002, 60, S40–S45. [Google Scholar] [CrossRef]
- Rzymski, P.; Nowicki, M. COVID-19-related prejudice towards Asian medical students: A consequence of SARS-CoV-2 fears in Poland. J. Infect. Public Health 2020. [Google Scholar] [CrossRef]
- Geldsetzer, P. Use of Rapid Online Surveys to Assess People’s Perceptions during Infectious Disease Outbreaks: A Cross-sectional Survey on COVID-19. J. Med. Internet Res. 2020, 22, e18790. [Google Scholar] [CrossRef] [PubMed]
- COVID-19 Dashboard by the Center for Systems Science and Engineering (CSSE) at Johns Hopkins University (JHU). Available online: https://gisanddata.maps.arcgis.com/apps/opsdashboard/index.html (accessed on 8 May 2020).
- Lanham-New, S.; Hill, T.R.; Gallagher, A.M.; Hester, V.H. Introduction to Human Nutrition, 3rd ed.; Wiley-Blackwell: Hoboken, NJ, USA, 2019. [Google Scholar]
- Sahlqvist, S.; Song, Y.; Bull, F.; Adams, E.; Preston, J.; Ogilvie, D.; iConnect, C. Effect of questionnaire length, personalisation and reminder type on response rate to a complex postal survey: Randomised controlled trial. BMC Med. Res. Methodol. 2011, 11, 62. [Google Scholar] [CrossRef]
- Rolstad, S.; Adler, J.; Rydén, A. Response Burden and Questionnaire Length: Is Shorter Better? A Review and Meta-analysis. Value Health 2011, 14, 1101–1108. [Google Scholar] [CrossRef] [PubMed]
- Opichka, K.; Smith, C.; Levine, A.S. Problematic Eating Behaviors Are More Prevalent in African American Women Who Are Overweight or Obese Than African American Women Who Are Lean or Normal Weight. Fam. Community Health 2019, 42, 81–89. [Google Scholar] [CrossRef] [PubMed]
- Larsen, S.C.; Heitmann, B.L. More Frequent Intake of Regular Meals and Less Frequent Snacking Are Weakly Associated with Lower Long-Term Gains in Body Mass Index and Fat Mass in Middle-Aged Men and Women. J. Nutr. 2019, 149, 824–830. [Google Scholar] [CrossRef] [PubMed]
- Barrington, W.E.; Beresford, S.A.A. Eating Occasions, Obesity and Related Behaviors in Working Adults: Does it Matter When You Snack? Nutrients 2019, 11, 2320. [Google Scholar] [CrossRef]
- Bi, H.; Gan, Y.; Yang, C.; Chen, Y.; Tong, X.; Lu, Z. Breakfast skipping and the risk of type 2 diabetes: A meta-analysis of observational studies. Public Health Nutr. 2015, 18, 3013–3019. [Google Scholar] [CrossRef]
- Takagi, H.; Hari, Y.; Nakashima, K.; Kuno, T.; Ando, T. Meta-Analysis of Relation of Skipping Breakfast With Heart Disease. Am. J. Cardiol. 2019, 124, 978–986. [Google Scholar] [CrossRef]
- Rong, S.; Snetselaar, L.G.; Xu, G.; Sun, Y.; Liu, B.; Wallace, R.B.; Bao, W. Association of Skipping Breakfast With Cardiovascular and All-Cause Mortality. J. Am. Coll. Cardiol. 2019, 73, 2025–2032. [Google Scholar] [CrossRef]
- Rubin, R. Does Skipping Breakfast Lead to Weight Loss or Weight Gain? JAMA 2019, 321, 1857–1858. [Google Scholar] [CrossRef]
- Nonogaki, K.; Nozue, K.; Oka, Y. Social Isolation Affects the Development of Obesity and Type 2 Diabetes in Mice. Endocrinology 2007, 148, 4658–4666. [Google Scholar] [CrossRef] [PubMed]
- Zarrinpar, A.; Chaix, A.; Panda, S. Daily Eating Patterns and Their Impact on Health and Disease. Trends Endocrinol. Metab. 2016, 27, 69–83. [Google Scholar] [CrossRef] [PubMed]
- Simonnet, A.; Chetboun, M.; Poissy, J.; Raverdy, V. High prevalence of obesity in severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) requiring invasive mechanical ventilation. Obesity 2020. [Google Scholar] [CrossRef] [PubMed]
- Kalligeros, M.; Shehadeh, F.; Mylona, E.K.; Benitez, G.; Beckwith, C.G.; Chan, P.A.; Mylonakis, E. Association of Obesity with Disease Severity among Patients with COVID-19. Obesity 2020. [Google Scholar] [CrossRef] [PubMed]
- Williamson, E.; Walker, A.J.; Bhaskaran, K.J.; Bacon, S.; Bates, C.; Morton, C.E.; Curtis, H.J.; Mehrkar, A.; Evans, D.; Inglesby, P.; et al. OpenSAFELY: Factors associated with COVID-19-related hospital death in the linked electronic health records of 17 million adult NHS patients. medRxiv 2020. [Google Scholar] [CrossRef]
- Duthie, S.J.; Duthie, G.G.; Russell, W.R.; Kyle, J.A.M.; Macdiarmid, J.I.; Rungapamestry, V.; Stephen, S.; Megias-Baeza, C.; Kaniewska, J.J.; Shaw, L.; et al. Effect of increasing fruit and vegetable intake by dietary intervention on nutritional biomarkers and attitudes to dietary change: A randomised trial. Eur. J. Nutr. 2018, 57, 1855–1872. [Google Scholar] [CrossRef]
- Bacchetti, T.; Turco, I.; Urbano, A.; Morresi, C.; Ferretti, G. Relationship of fruit and vegetable intake to dietary antioxidant capacity and markers of oxidative stress: A sex-related study. Nutrition 2019, 61, 164–172. [Google Scholar] [CrossRef]
- Poniedziałek, B.; Rzymski, P.; Pięt, M.; Gąsecka, M.; Stroińska, A.; Niedzielski, P.; Mleczek, M.; Rzymski, P.; Wilczak, M. Relation between polyphenols, malondialdehyde, antioxidant capacity, lactate dehydrogenase and toxic elements in human colostrum milk. Chemosphere 2018, 191, 548–554. [Google Scholar] [CrossRef]
- Maleki, S.J.; Crespo, J.F.; Cabanillas, B. Anti-inflammatory effects of flavonoids. Food Chem. 2019, 299, 125124. [Google Scholar] [CrossRef]
- Zhu, F.; Du, B.; Xu, B. Anti-inflammatory effects of phytochemicals from fruits, vegetables, and food legumes: A review. Crit. Rev. Food Sci. Nutr. 2018, 58, 1260–1270. [Google Scholar] [CrossRef]
- Paalani, M.; Lee, J.W.; Haddad, E.; Tonstad, S. Determinants of inflammatory markers in a bi-ethnic population. Ethn. Dis. 2011, 21, 142–149. [Google Scholar] [PubMed]
- Craddock, J.C.; Neale, E.P.; Peoples, G.E.; Probst, Y.C. Vegetarian-Based Dietary Patterns and their Relation with Inflammatory and Immune Biomarkers: A Systematic Review and Meta-Analysis. Adv. Nutr. 2019, 10, 433–451. [Google Scholar] [CrossRef] [PubMed]
- Jaceldo-Siegl, K.; Haddad, E.; Knutsen, S.; Fan, J.; Lloren, J.; Bellinger, D.; Fraser, G.E. Lower C-reactive protein and IL-6 associated with vegetarian diets are mediated by BMI. Nutr. Metab. Cardiovasc. Dis. 2018, 28, 787–794. [Google Scholar] [CrossRef] [PubMed]
- Turner-McGrievy, G.M.; Wirth, M.D.; Shivappa, N.; Wingard, E.E.; Fayad, R.; Wilcox, S.; Frongillo, E.A.; Hebert, J.R. Randomization to plant-based dietary approaches leads to larger short-term improvements in Dietary Inflammatory Index scores and macronutrient intake compared with diets that contain meat. Nutr. Res. 2015, 35, 97–106. [Google Scholar] [CrossRef]
- Eichelmann, F.; Schwingshackl, L.; Fedirko, V.; Aleksandrova, K. Effect of plant-based diets on obesity-related inflammatory profiles: A systematic review and meta-analysis of intervention trials. Obes. Rev. Off. J. Int. Assoc. Study Obes. 2016, 17, 1067–1079. [Google Scholar] [CrossRef]
- Shah, B.; Newman, J.D.; Woolf, K.; Ganguzza, L.; Guo, Y.; Allen, N.; Zhong, J.; Fisher, E.A.; Slater, J. Anti-Inflammatory Effects of a Vegan Diet Versus the American Heart Association-Recommended Diet in Coronary Artery Disease Trial. J. Am. Heart Assoc. 2018, 7, e011367. [Google Scholar] [CrossRef]
- Najjar, R.S.; Moore, C.E.; Montgomery, B.D. Consumption of a defined, plant-based diet reduces lipoprotein(a), inflammation, and other atherogenic lipoproteins and particles within 4 weeks. Clin. Cardiol. 2018, 41, 1062–1068. [Google Scholar] [CrossRef]
- Montonen, J.; Boeing, H.; Fritsche, A.; Schleicher, E.; Joost, H.G.; Schulze, M.B.; Steffen, A.; Pischon, T. Consumption of red meat and whole-grain bread in relation to biomarkers of obesity, inflammation, glucose metabolism and oxidative stress. Eur. J. Nutr. 2013, 52, 337–345. [Google Scholar] [CrossRef] [PubMed]
- Christ, A.; Günther, P.; Lauterbach, M.A.R.; Duewell, P.; Biswas, D.; Pelka, K.; Scholz, C.J.; Oosting, M.; Haendler, K.; Baßler, K.; et al. Western Diet Triggers NLRP3-Dependent Innate Immune Reprogramming. Cell 2018, 172, 162–175. [Google Scholar] [CrossRef]
- Verity, R.; Okell, L.C.; Dorigatti, I.; Winskill, P.; Whittaker, C.; Imai, N.; Cuomo-Dannenburg, G.; Thompson, H.; Walker, P.G.T.; Fu, H.; et al. Estimates of the severity of coronavirus disease 2019: A model-based analysis. Lancet Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Szabo, G.; Saha, B. Alcohol’s Effect on Host Defense. Alcohol Res. 2015, 37, 159–170. [Google Scholar] [PubMed]
- Weiss, I.C.; Pryce, C.R.; Jongen-Relo, A.L.; Nanz-Bahr, N.I.; Feldon, J. Effect of social isolation on stress-related behavioural and neuroendocrine state in the rat. Behav. Brain Res. 2004, 152, 279–295. [Google Scholar] [CrossRef] [PubMed]
- Clay, J.M.; Parker, M.O. Alcohol use and misuse during the COVID-19 pandemic: A potential public health crisis? Lancet Public Health 2020, 5, e259. [Google Scholar] [CrossRef]
- Zhang, S.X.; Wang, Y.; Rauch, A.; Wei, F. Unprecedented disruption of lives and work: Health, distress and life satisfaction of working adults in China one month into the COVID-19 outbreak. Psychiatry Res. 2020, 288, 112958. [Google Scholar] [CrossRef] [PubMed]
- Fidler, J.A.; West, R. Self-perceived smoking motives and their correlates in a general population sample. Nicotine Tob. Res. Off. J. Soc. Res. Nicotine Tob. 2009, 11, 1182–1188. [Google Scholar] [CrossRef]
- Choi, D.; Ota, S.; Watanuki, S. Does cigarette smoking relieve stress? Evidence from the event-related potential (ERP). Int. J. Psychophysiol. Off. J. Int. Organ. Psychophysiol. 2015, 98, 470–476. [Google Scholar] [CrossRef]
- Lawless, M.H.; Harrison, K.A.; Grandits, G.A.; Eberly, L.E.; Allen, S.S. Perceived stress and smoking-related behaviors and symptomatology in male and female smokers. Addict. Behav. 2015, 51, 80–83. [Google Scholar] [CrossRef]
- Hajek, P.; Taylor, T.; McRobbie, H. The effect of stopping smoking on perceived stress levels. Addiction 2010, 105, 1466–1471. [Google Scholar] [CrossRef]
- Stein, R.J.; Pyle, S.A.; Haddock, C.K.; Poston, W.S.; Bray, R.; Williams, J. Reported stress and its relationship to tobacco use among U.S. military personnel. Mil. Med. 2008, 173, 271–277. [Google Scholar] [CrossRef]
- Harapan, H.; Rajamoorthy, Y.; Anwar, S.; Bustamam, A.; Radiansyah, A.; Angraini, P.; Fasli, R.; Salwiyadi, S.; Bastian, R.A.; Oktiviyari, A.; et al. Knowledge, attitude, and practice regarding dengue virus infection among inhabitants of Aceh, Indonesia: A cross-sectional study. BMC Infect. Dis. 2018, 18, 96. [Google Scholar] [CrossRef]
- Stover, C.T.; Smith, D.K.; Schmid, D.S.; Pellett, P.E.; Stewart, J.A.; Klein, R.S.; Mayer, K.; Vlahov, D.; Schuman, P.; Group, H.E.R.S. Prevalence of and Risk Factors for Viral Infections among Human Immunodeficiency Virus (HIV)-Infected and High-Risk HIV-Uninfected Women. J. Infect. Dis. 2003, 187, 1388–1396. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Hahn, R.A.; Truman, B.I. Education Improves Public Health and Promotes Health Equity. Int. J. Health Serv. 2015, 45, 657–678. [Google Scholar] [CrossRef] [PubMed]
- McLean, C.P.; Anderson, E.R. Brave men and timid women? A review of the gender differences in fear and anxiety. Clin. Psychol. Rev. 2009, 29, 496–505. [Google Scholar] [CrossRef]
- Collignon, S. Women More Worried than Men about the Spread of Coronavirus. Available online: https://www.pandemicpolitics.net/post/women-more-worried-than-men-about-the-spread-of-coronavirus (accessed on 12 May 2020).
- Dryhurst, S.; Schneider, C.R.; Kerr, J.; Freeman, A.L.J.; Recchia, G.; van der Bles, A.M.; Spiegelhalter, D.; van der Linden, S. Risk perceptions of COVID-19 around the world. J. Risk Res. 2020, 1–13. [Google Scholar] [CrossRef]
- Jin, J.-M.; Bai, P.; He, W.; Wu, F.; Liu, X.-F.; Han, D.-M.; Liu, S.; Yang, J.-K. Gender Differences in Patients With COVID-19: Focus on Severity and Mortality. Front. Public Health 2020, 8. [Google Scholar] [CrossRef] [PubMed]
- Chen, X.; Ran, L.; Liu, Q.; Hu, Q.; Du, X.; Tan, X. Hand Hygiene, Mask-Wearing Behaviors and Its Associated Factors during the COVID-19 Epidemic: A Cross-Sectional Study among Primary School Students in Wuhan, China. Int. J. Environ. Res. Public Health 2020, 17, 2893. [Google Scholar] [CrossRef]
- So, W.K.; Chan, S.S.; Lee, A.C.; Tiwari, A.F. The knowledge level and precautionary measures taken by older adults during the SARS outbreak in Hong Kong. Int. J. Nurs. Stud. 2004, 41, 901–909. [Google Scholar] [CrossRef]
- EFSA. Coronavirus: No Evidence that Food is a Source or Transmission Route. Available online: https://www.efsa.europa.eu/en/news/coronavirus-no-evidence-food-source-or-transmission-route (accessed on 12 May 2020).
- Van Doremalen, N.; Bushmaker, T.; Morris, D.H.; Holbrook, M.G.; Gamble, A.; Williamson, B.N.; Tamin, A.; Harcourt, J.L.; Thornburg, N.J.; Gerber, S.I.; et al. Aerosol and Surface Stability of SARS-CoV-2 as Compared with SARS-CoV-1. N. Engl. J. Med. 2020, 382, 1564–1567. [Google Scholar] [CrossRef]
- Cruz, R.M.S.; Rico, B.P.M.; Vieira, M.C. 9 -Food packaging and migration. In Food Quality and Shelf Life; Galanakis, C.M., Ed.; Academic Press: Cambridge, MA, USA, 2019; pp. 281–301. [Google Scholar] [CrossRef]
| Age (years) mean ± SD (min–max) 18–25, n (%) 26–35, n (%) 36–45, n (%) >45, n (%) | 27.7 ± 9.0 (18–71) 588 (53.6) 310 (28.3) 144 (13.1) 54 (4.9) |
| Gender Female, n (%)/Male, n (%) | 1043 (95.1)/54 (4.9) |
| Weight (kg) mean ± SD (min–max) Body Mass Index (kg/m2) mean ± SD (min–max) Underweight (<18.5), n (%) Normal weight (18.5–24.9), n (%) Overweight (25.0–29.9), n (%) Obesity (≥30.0), n (%) | 66.0 ± 14.5 (40–140) 23.5 ± 4.8 (14.4–57.8) 87 (7.9) 699 (63.7) 217 (19.8) 94 (8.6) |
| Occupation Unemployed, n (%) Student, n (%) Full-time worker, n (%) | 110 (10.0) 518 (47.2) 469 (42.8) |
| Place of living Urban, n (%)/Rural, n (%) | 881 (80.3)/216 (19.7) |
| Education Primary, n (%) Secondary, n (%) Tertiary, n (%) Vocational, n (%) | 35 (3.2) 474 (43.2) 567 (51.7) 21 (1.9) |
| Declared addictions Alcohol, n (%)/Smoking, n (%) | 14 (1.3)/155 (14.1) |
| Underweight | Normal BMI | Overweight | Obese | Pearson’s χ2 | |
|---|---|---|---|---|---|
| Eating more | 40.7 | 30.6 | 48.8 | 55.3 | p < 0.05 |
| Snacking more | 46.5 | 50.1 | 55.3 | 61.7 | p < 0.05 |
| Cooking more | 63.3 | 62.1 | 62.6 | 63.3 | p > 0.05 |
| >1 per Day | Once per Day | Few Times per Week | Once per Week | Once per Month | Occasionally | Never | |
|---|---|---|---|---|---|---|---|
| Percentage of Surveyed [%] | |||||||
| Vegetables and fruits | 25.1 | 42.1 | 25.5 | 5.0 | 0.7 | 1.0 | 0.5 |
| Legumes | 3.6 | 16.8 | 40.2 | 20.7 | 11.4 | 5.5 | 1.9 |
| Grain products | 19.4 | 44.8 | 26.1 | 6.1 | 1.5 | 1.4 | 0.7 |
| Meat products | 3.1 | 18.0 | 28.5 | 7.0 | 1.6 | 4.8 | 36.8 |
| Dairy | 11.0 | 38.1 | 30.3 | 8.8 | 2.6 | 3.6 | 5.7 |
| Fast-foods | 0.3 | 0.7 | 6.7 | 12.8 | 27.8 | 28.3 | 23.4 |
| Instant products | 0.0 | 0.2 | 2.8 | 5.7 | 41.5 | 0.0 | 39.2 |
| Sweets | 6.7 | 26.1 | 36.6 | 17.7 | 5.2 | 4.9 | 2.8 |
| Salty snacks | 1.5 | 6.3 | 22.6 | 25.3 | 19.8 | 13.7 | 10.8 |
| Coffee | 27.7 | 30.1 | 10.4 | 5.7 | 2.9 | 6.1 | 17.1 |
| Tea | 37.1 | 29.6 | 17.4 | 5.3 | 2.6 | 4.6 | 3.4 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sidor, A.; Rzymski, P. Dietary Choices and Habits during COVID-19 Lockdown: Experience from Poland. Nutrients 2020, 12, 1657. https://doi.org/10.3390/nu12061657
Sidor A, Rzymski P. Dietary Choices and Habits during COVID-19 Lockdown: Experience from Poland. Nutrients. 2020; 12(6):1657. https://doi.org/10.3390/nu12061657
Chicago/Turabian StyleSidor, Aleksandra, and Piotr Rzymski. 2020. "Dietary Choices and Habits during COVID-19 Lockdown: Experience from Poland" Nutrients 12, no. 6: 1657. https://doi.org/10.3390/nu12061657
APA StyleSidor, A., & Rzymski, P. (2020). Dietary Choices and Habits during COVID-19 Lockdown: Experience from Poland. Nutrients, 12(6), 1657. https://doi.org/10.3390/nu12061657






