Development of a Danish Adapted Healthy Plant-Based Diet Based on the EAT-Lancet Reference Diet
Abstract
1. Introduction
2. Materials and Methods
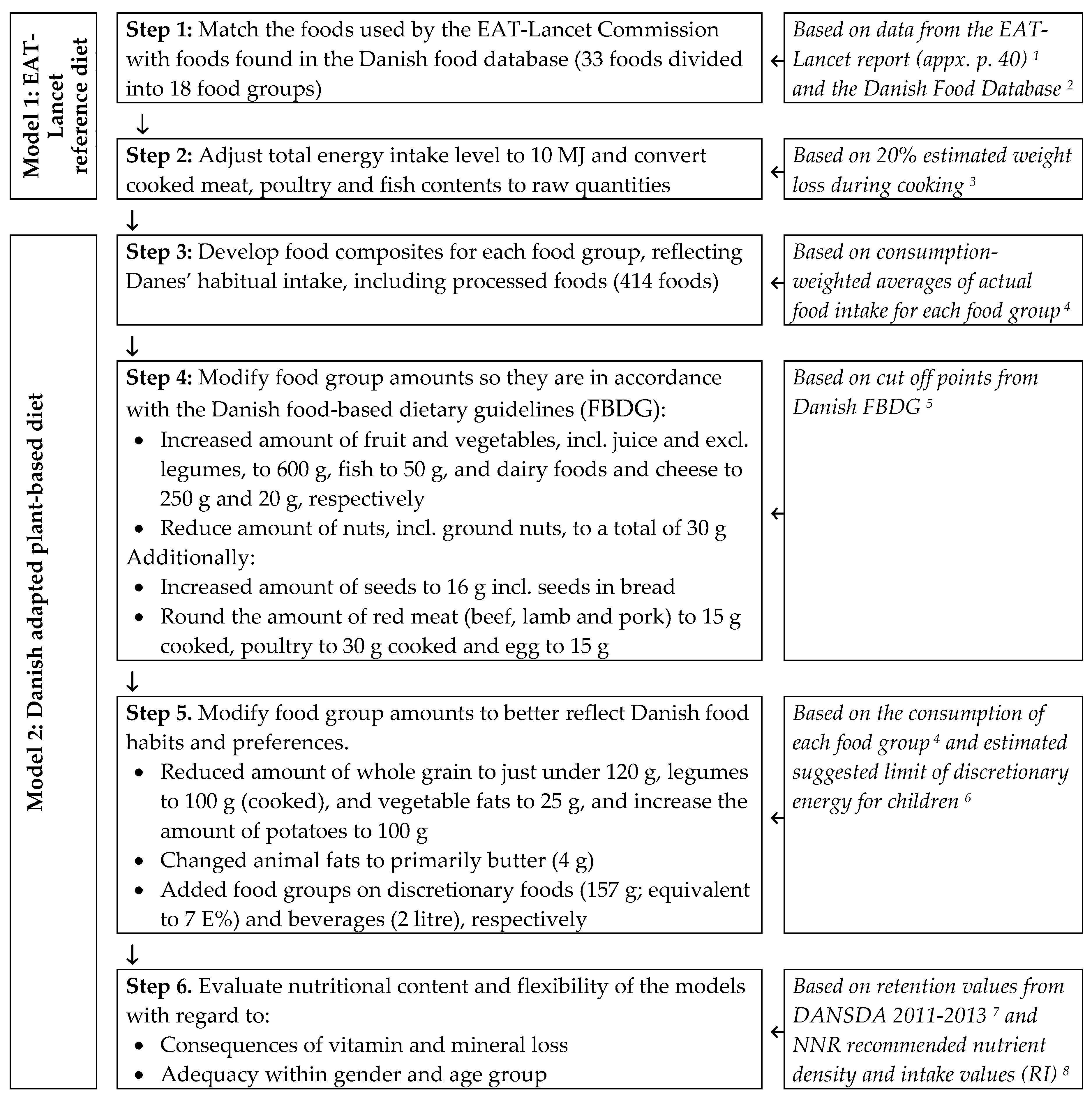
2.1. Development of the EAT-Lancet Reference Diet with Danish Foods (Model 1)
2.2. Development of a Danish Adapted Plant-Based Diet (Model 2)
3. Results
3.1. Food Group Contents
3.2. Macronutrient Contents
3.3. Vitamin Contents
3.4. Mineral contents
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Birt, C.; Buzeti, T.; Grosso, G.; Justesen, L.; Lachat, C.; Lafranconi, A.; Mertanen, E.; Rangelov, N.; Sarlie-Lähteenkorva, S. Healthy and Sustainable Diets for European Countries; European Public Health Association: Utrecht, The Netherlands, 2017. [Google Scholar]
- Halloran, A.; Fischer-Møller, M.F.; Persson, M.; Skylare, E. Solutions Menu—A Nordic Guide to Sustainable Food Policy; Nordic Council of Ministers: Copenhagen, Denmark, 2018. [Google Scholar]
- WHO. Sustainable Healthy Diets—Guiding Principles; WHO: Geneva, Switzerland, 2019. [Google Scholar]
- Fanzo, J. Healthy and Sustainable Diets and Food Systems: the Key to Achieving Sustainable Development Goal 2? Food Ethics 2019, 4, 159–174. [Google Scholar] [CrossRef]
- FAO. Healthy Diets for a #Zerohunger World; FAO: Rome, Italy, 2019. [Google Scholar]
- Rose, D.; Heller, M.C.; Roberto, C.A. Position of the Society for Nutrition Education and Behavior: The Importance of Including Environmental Sustainability in Dietary Guidance. J. Nutr. Educ. Behav. 2019, 51, 3–15. [Google Scholar] [CrossRef] [PubMed]
- Willett, W.; Rockström, J.; Loken, B.; Springmann, M.; Lang, T.; Vermeulen, S.; Garnett, T.; Tilman, D.; DeClerck, F.; Wood, A.; et al. Food in the Anthropocene: The EAT-Lancet Commission on healthy diets from sustainable food systems. Lancet 2019, 393, 447–492. [Google Scholar] [CrossRef]
- Kim, B.F.; Santo, R.E.; Scatterday, A.P.; Fry, J.P.; Synk, C.M.; Cebron, S.R.; Mekonnen, M.M.; Hoekstra, A.Y.; de Pee, S.; Bloem, M.W.; et al. Country-specific dietary shifts to mitigate climate and water crises. Glob. Environ. Chang. 2019, 1–13, In Press. Available online: https://www.sciencedirect.com/science/article/pii/S0959378018306101 (accessed on 7 August 2019). [CrossRef]
- Wilson, N.; Cleghorn, C.L.; Cobiac, L.J.; Mizdrak, A.; Nghiem, N. Achieving Healthy and Sustainable Diets: A Review of the Results of Recent Mathematical Optimization Studies. Adv. Nutr. 2019, 10, S389–S403. [Google Scholar] [CrossRef] [PubMed]
- Springmann, M.; Wiebe, K.; Mason-D’Croz, D.; Sulser, T.B.; Rayner, M.; Scarborough, P. Health and nutritional aspects of sustainable diet strategies and their association with environmental impacts: A global modelling analysis with country-level detail. Lancet Planet Health 2018, 2, e451–e461. [Google Scholar] [CrossRef]
- Hemler, E.C.; Hu, F.B. Plant-Based Diets for Cardiovascular Disease Prevention: All Plant Foods Are Not Created Equal. Curr. Atheroscler. Rep. 2019, 21, 18. [Google Scholar] [CrossRef]
- Aleksandrowicz, L.; Green, R.; Joy, J.M.; Smith, P.; Haines, A. The Impacts of Dietary Change on Greenhouse Gas Emissions, Land Use, Water Use, and Health: A Systematic Review. PLoS ONE 2016, 11, 1–16. [Google Scholar] [CrossRef]
- Fresán, U.; Sabaté, J. Vegetarian Diets: Planetary Health and Its Alignment with Human Health. Adv. Nutr. 2019, 10, S380–S388. [Google Scholar] [CrossRef]
- Harris, F.; Moss, C.; Joy, E.J.M.; Quinn, R.; Scheelbeek, P.F.D.; Dangour, A.D.; Green, R. The Water Footprint of Diets: A Global Systematic Review and Meta-analysis. Adv. Nutr. 2019, 00, 1–12. [Google Scholar] [CrossRef]
- Madigan, M.; Karhu, E. The role of plant-based nutrition in cancer prevention. J. Unexplored Med. Data 2018, 3, 9. [Google Scholar] [CrossRef]
- Qian, F.; Liu, G.; Hu, F.B.; Bhupathiraju, S.N.; Sun, Q. Association between Plant-Based Dietary Patterns and Risk of Type 2 Diabetes: A Systematic Review and Meta-analysis. JAMA Intern. Med. 2019, 179, 1335–1344. [Google Scholar] [CrossRef] [PubMed]
- Satija, A.; Hu, F.B. Plant-based diets and cardiovascular health. Trends Cardiovasc. Med. 2018, 28, 437–441. [Google Scholar] [CrossRef]
- Satija, A.; Bhupathiraju, S.N.; Spiegelman, D.; Chiuve, S.E.; Manson, J.E.; Willett, W.; Rexrode, K.M.; Rimm, E.B.; Hu, F.B. Healthful and Unhealthful Plant-Based Diets and the Risk of Coronary Heart Disease in US Adults. J. Am. Coll. Cardiol. 2017, 70, 411–422. [Google Scholar] [CrossRef] [PubMed]
- Satija, A.; Bhupathiraju, N.; Rimm, B.; Spiegelman, D.; Chiuve, E.; Borgi, L.; Willett, C.; Manson, E.; Sun, Q.; Hu, B. Plant-Based Dietary Patterns and Incidence of Type 2 Diabetes in US Men and Women: Results from Three Prospective Cohort Studies. PLoS Med. 2016, 13, 1–18. [Google Scholar] [CrossRef] [PubMed]
- Baden, M.Y.; Liu, G.; Satija, A.; Li, Y.; Sun, Q.; Fung, T.T.; Rimm, E.B.; Willett, W.C.; Hu, F.B.; Bhupathiraju, S.N. Changes in Plant-Based Diet Quality and Total and Cause-Specific Mortality. Circulation 2019, 140, 979–991. [Google Scholar] [CrossRef] [PubMed]
- Tuomisto, H.L. The complexity of sustainable diets. Nat. Ecol. Evol. 2019, 3, 720–721. [Google Scholar] [CrossRef]
- Mithril, C.; Dragsted, L.O.; Meyer, C.; Tetens, I.; Biltoft-Jensen, A.; Astrup, A. Dietary composition and nutrient content of the New Nordic Diet. Public Health Nutr. 2013, 16, 777–785. [Google Scholar] [CrossRef]
- Saxe, H. The New Nordic Diet is an effective tool in environmental protection: It reduces the associated socioeconomic cost of diets. Am. J. Clin. Nutr. 2014, 99, 1117–1125. [Google Scholar] [CrossRef]
- Pedersen, A.N.; Christensen, T.; Matthiessen, J.; Knudsen, V.K.; Sørensen, M.R.; Biltoft-Jensen, A.P.; Hinsch, H.J.; Ygil, K.H.; Kørup, K.; Saxholt, E.; et al. Dietary habits in Denmark 2011-2013. Main results; DTU Food: Copenhagen, Denmark, 2015. [Google Scholar]
- Wang, D.D.; Li, Y.; Afshin, A.; Springmann, M.; Mozaffarian, D.; Stampfer, M.J.; Hu, F.B.; Murray, C.J.L.; Willett, W.C. Global Improvement in Dietary Quality Could Lead to Substantial Reduction in Premature Death. J. Nutr. 2019, 149, 1065–1074. [Google Scholar] [CrossRef]
- Hirvonen, K.; Bai, Y.; Headey, D.; Masters, W.A. Affordability of the EAT-Lancet reference diet: A global analysis. Lancet Glob. Health 2020, 8, e59–e66. [Google Scholar] [CrossRef]
- Wood, A.; Gordon, L.J.; Röös, E.; Karlsson, J.; Häyhä, T.; Bignet, V.; Rydenstam, T.; af Segerstad, L.H.; Brukner, M. Nordic food systems for improved health and sustainability: Baseline assessment to inform transformation. Swedish Stockholm Resilience Center: Stockholm University, Sweden, 2019. [Google Scholar]
- Blackstone, N.T.; Conrad, Z. Comparing the Recommended Eating Patterns of the EAT-Lancet Commission and Dietary Guidelines for Americans: Implications for Sustainable Nutrition. Curr. Dev. Nutr. 2020. Published on 4 February. [Google Scholar] [CrossRef]
- Nordic Council of Ministers. Nordic Nutrition Recommendations 2012: Integrating Nutrition and Physical Activity, 5th ed.; Nordic Council of Ministers: Copenhagen, Denmark, 2014. [Google Scholar]
- Danish Veterinary and Food Administration: The Official Dietary Guidelines. Available online: https://altomkost.dk/english/#c41067 (accessed on 1 April 2019).
- Tetens, I.; Andersen, L.B.; Astrup, A.; Gondolf, U.H.; Hermansen, K.; Uhre Jakobsen, M.; Knudsen, V.K.; Mejborn, H.; Schwarz, P.; Tjønneland, A.; et al. The Evidence-Base for the Danish Guidelines for Diet and Physical Activity; DTU Food: Copenhagen, Denmark, 2013. [Google Scholar]
- Meltzer, H.M.; Brantsæter, A.L.; Trolle, E.; Eneroth, H.; Fogelholm, M.; Ydersbond, T.A.; Birgisdottir, B.E. Environmental Sustainability Perspectives of the Nordic Diet. Nutrients 2019, 11, 2248. [Google Scholar] [CrossRef] [PubMed]
- NFA. Find Your Way to Eat Greener, not too Much and Be Active; National Food Agency: Uppsala, Swedish, 2015. [Google Scholar]
- The German Nutrition Society: 10 Guidelines of the German Nutrition Society (DGE) for a Wholesome Diet. Available online: https://www.dge.de/ernaehrungspraxis/vollwertige-ernaehrung/10-regeln-der-dge/10-guidelines-of-the-german-nutrition-society/ (accessed on 15 January 2019).
- Buttriss, J.L. The Eatwell Guide refreshed. Nutr. Bull. 2016, 41, 135–141. [Google Scholar] [CrossRef]
- Brink, E.; van Rossum, C.; Postma-Smeets, A.; Stafleu, A.; Wolvers, D.; Van Dooren, C.; Toxopeus, I.; Buurma-Rethans, E.; Geurts, M.; Ocké, M. Development of healthy and sustainable food-based dietary guidelines for the Netherlands. Public Health Nutr. 2019, 22, 2419–2435. [Google Scholar] [CrossRef]
- Fisher, C.G.; Garnett, T. Plates, pyramids and planets: Developments in national healthy and sustainable dietary guidelines: A state of play assessment. FAO and the University of Oxford, 2016. [Google Scholar]
- EAT-Lancet Commission. Supplementary appendix to: Willett W, Rockström J, Loken B, et al. Food in the Anthropocene: the EAT-Lancet Commission on healthy diets from sustainable food systems. Lancet 2019.
- DTU Food. Food Data, version 3. 2018. Available online: https://frida.fooddata.dk/ (accessed on 1 May 2018).
- Jakobsen, J.; Bysted, A.; Nielsen, C.W.; Saxholt, E.; Ygil, K.H.; Trolle, E. Nutrient Content in Flour, Grains, Grains and Seeds [In Danish: Næringsstofindhold I Mel, Gryn, Kerner Og Frø]; DTU Food: Copenhagen, Denmark, 2019. [Google Scholar]
- Jakobsen, J.; Bysted, A.; Lanza, E.; Langwagen, M.; Nielsen, C.W.; Ygil, K.H.; Trolle, E. Nutrient Content in Fish and Fish Products—With Extra Focus on Farmed Salmon [in Danish: Næringsstofindhold i fisk og fiskeprodukter - med ekstra fokus på opdrætslaks]; DTU Food: Copenhagen, Denmark, 2019. [Google Scholar]
- USDA: Vegetable Group Food Gallery. Available online: https://www.choosemyplate.gov/eathealthy/vegetables/vegetable-group-food-gallery (accessed on 7 November 2019).
- Ygil, K.H. Dimensions, Weight and Portion Sizes of Foods [in Danish: Mål, vægt og portionsstørrelser på fødevarer]; DTU Food: Copenhagen, Denmark, 2013. [Google Scholar]
- Biltoft-Jensen, A.; Trolle, E.; Christensen, T.; Ygil, K.H.; Fagt, S.; Matthiessen, J.; Groth, M.V.; Tetens, I. Development of a recommended food intake pattern for healthy Danish adolescents consistent with the Danish dietary guidelines, nutrient recommendations and national food preferences. J. Hum. Nutr. Diet. 2008, 21, 451–463. [Google Scholar] [CrossRef]
- The Whole Grain Partnership: Danish Whole Grain Logo—User Manual. Available online: https://fuldkorn.dk/wp-content/uploads/2019/08/2015-Logo-manual_english.pdf (accessed on 7 November 2019).
- Biltoft-Jensen, A.; Ygil, K.H.; Christensen, L.M.; Christensen, S.M.; Christensen, T. Proposed guidelines for healthy eating in schools and institutions [in Danish: Forslag til retningslinjer for sund kost i skoler og institutioner]; DTU Food: Copenhagen, Denmark, 2005. [Google Scholar]
- Pedersen, A.N.; Fagt, S.; Groth, M.; Christensen, T.; Biltoft-Jensen, A.; Matthiessen, J.; Andersen, N.L.; Kørup, K.; Hartkopp, H.B.; Ygil, K.H.; et al. Dietary Habits in Denmark 2003–2008. Main Results [in Danish: Danskernes Kostvaner 2003–2008:Hovedresultater]; DTU Food: Copenhagen, Denmark, 2010. [Google Scholar]
- USDA ChooseMyPlate: What Are Included in the Dairy group? Available online: https://www.choosemyplate.gov/eathealthy/dairy (accessed on 1 April 2019).
- World Health Organization. Protein and Amino Acid Requirements in Human Nutrition. Report of a Joint WHO/FAO/UNU Expert Consultation; World Health Organization Technical Report Series; World Health Organization: Geneva, Switzerland, 2007. [Google Scholar]
- Outzen, M.; Tjønneland, A.; Larsen, E.H.; Andersen, K.K.; Christensen, J.; Overvad, K.; Olsen, A. The Effect on Selenium Concentrations of a Randomized Intervention with Fish and Mussels in a Population with Relatively Low Habitual Dietary Selenium Intake. Nutrients 2015, 7, 608–624. [Google Scholar] [CrossRef]
- Stoffaneller, R.; Morse, N.L. A review of dietary selenium intake and selenium status in Europe and the Middle East. Nutrients 2015, 7, 1494–1537. [Google Scholar] [CrossRef]
- Tørris, C.; Småstuen, M.C.; Molin, M. Nutrients in Fish and Possible Associations with Cardiovascular Disease Risk Factors in Metabolic Syndrome. Nutrients 2018, 10, 952. [Google Scholar] [CrossRef]
- Hallström, E.; Bergman, K.; Mifflin, K.; Parker, R.; Tyedmers, P.; Troell, M.; Ziegler, F. Combined climate and nutritional performance of seafoods. J. Clean. Prod. 2019, 230, 402–411. [Google Scholar] [CrossRef]
- WWF: Denmark Seafood Guide. Available online: https://fiskeguiden.wwf.dk/wwf-recommendations (accessed on 15 January 2019).
- Itkonen, S.T.; Andersen, R.; Björk, A.K.; Brugård Konde, Å.; Eneroth, H.; Erkkola, M.; Holvik, K.; Madar, A.A.; Meyer, H.E.; Tetens, I.; et al. Vitamin D status and current policies to achieve adequate vitamin D intake in the Nordic countries. Scand. J. Public Health 2020, 1–14. First Published 9 January. [Google Scholar] [CrossRef] [PubMed]
- Hansen, L.; Tjønneland, A.; Køster, B.; Brot, C.; Andersen, R.; Cohen, S.; Frederiksen, K.; Olsen, A. Vitamin D Status and Seasonal Variation among Danish Children and Adults: A Descriptive Study. Nutrients 2018, 10, 1801. [Google Scholar] [CrossRef] [PubMed]
- Ministry of the Environment and Food. Statutory Order on the Addition of Iodine to Household Salt and Salt in Bread and Ordinary Baked Goods; Ministry of the Environment and Food: Copenhagen, Denmark, 2019. [Google Scholar]
- Blanco-Rojo, R.; Vaquero, M.P. Iron bioavailability from food fortification to precision nutrition: A review. Innov. Food Sci. Emerg. Technol. 2019, 51, 126–138. [Google Scholar] [CrossRef]
- Platel, K.; Srinivasan, K. Bioavailability of micronutrients from plant foods: An update. Crit. Rev. Food Sci. Nutr. 2016, 56, 1608–1619. [Google Scholar] [CrossRef] [PubMed]
- Röös, E.; Carlsson, G.; Ferawati, F.; Hefni, M.; Stephan, A.; Tidåker, P.; Witthöft, C. Less meat, more legumes: prospects and challenges in the transition toward sustainable diets in Sweden. Renew. Agric. Food Syst. 2018, 1–14. [Google Scholar] [CrossRef]
- Bjørnsbo, K.S.; Riis, N.L.; Andreasen, A.H.; Petersen, J.; Lassen, A.D.; Trolle, E.; Frederiksen, A.K.S.; Munk, J.K.; Toft, U. Salt Reduction Intervention in Families Investigating Metabolic, Behavioral and Health Effects of Targeted Intake Reductions: Study Protocol for a Four Months Three-Armed, Randomized, Controlled Real-Life Trial. Int. J. Environ. Res. Public Health 2019, 16, 3532. [Google Scholar] [CrossRef]
- Lassen, A.; Trolle, E.; Bysted, A.; Knuthsen, P.; Andersen, E. The Salt Content of Lunch Meals Eaten at Danish Worksites. Nutrients 2018, 10, 1367. [Google Scholar] [CrossRef]
- Dougkas, A.; Vannereux, M.; Giboreau, A.S. The Impact of Herbs and Spices on Increasing the Appreciation and Intake of Low-Salt Legume-Based Meals. Nutrients 2019, 11, 2901. [Google Scholar] [CrossRef]
- MacDiarmid, J.I.; Whybrow, S. Nutrition from a climate change perspective. Proc. Nutr. Soc. 2019, 78, 380–387. [Google Scholar] [CrossRef]
- Poore, J.; Nemecek, T. Reducing food environmental impacts through producers and consumers. Science 2018, 360, 987–992. [Google Scholar] [CrossRef] [PubMed]
- Thompson, R.; Mitrou, G.; Brown, S.; Almond, E.; Bandurek, I.; Brockton, N.; Kälfors, M.; Ginley-Gieser, D.; Sinclair, B.; Meincke, L.; et al. Major new review of global evidence on diet, nutrition and physical activity: A blueprint to reduce cancer risk. Nutr. Bull. 2018, 43, 269–283. [Google Scholar] [CrossRef]
- Astrup, A.; Bertram, H.C.S.; Bonjour, J.P.; De Groot, L.C.P.; De Oliveira Otto, M.C.; Feeney, E.L.; Garg, M.L.; Givens, I.; Kok, F.J.; Krauss, R.M.; et al. WHO draft guidelines on dietary saturated and trans fatty acids: Time for a new approach? BMJ 2019, 366, 14137. [Google Scholar] [CrossRef] [PubMed]
- Leroy, F.; Cofnas, N. Should dietary guidelines recommend low red meat intake? Crit. Rev. Food Sci. Nutr. 2019, 1–10, Published online 5 September. [Google Scholar] [CrossRef] [PubMed]
- O’Connor, L.E.; Kim, J.E.; Campbell, W.W. Total red meat intake of >=0.5 servings/d does not negatively influence cardiovascular disease risk factors: A systemically searched meta-analysis of randomized controlled trials. Am. J. Clin. Nutr. 2017, 105, 57–69. [Google Scholar] [CrossRef] [PubMed]
- Guasch-Ferre, M.; Satija, A.; Blondin, S.A.; Janiszewski, M.; Emlen, E.; O’Connor, L.E.; Campbell, W.W.; Hu, F.B.; Willett, W.C.; Stampfer, M.J. Meta-Analysis of Randomized Controlled Trials of Red Meat Consumption in Comparison With Various Comparison Diets on Cardiovascular Risk Factors. Circulation 2019, 139, 1828–1845. [Google Scholar] [CrossRef] [PubMed]
- Chen, G.C.; Lv, D.B.; Pang, Z.; Liu, Q.F. Red and processed meat consumption and risk of stroke: A meta-analysis of prospective cohort studies. Eur. J. Clin. Nutr. 2013, 67, 91–95. [Google Scholar] [CrossRef]
- Feskens, E.J.M.; Sluik, D.; Van Woudenbergh, G.J. Meat consumption, diabetes, and its complications. Curr. Nutr. Rep. 2013, 13, 298–306. [Google Scholar] [CrossRef]
- Kim, K.; Hyeon, J.; Lee, S.A.; Kwon, S.O.; Lee, H.; Keum, N.N.; Lee, J.K.; Park, S.M. Role of total, red, processed, and white meat consumption in stroke incidence and mortality: A systematic review and meta-analysis of prospective cohort studies. J. Am. Heart Assoc. 2017, 6, e005983. [Google Scholar] [CrossRef]
- Schwingshackl, L.; Schwedhelm, C.; Hoffmann, G.; Lampousi, A.M.; Knüppel, S.; Iqbal, K.; Bechthold, A.; Schlesinger, S.; Boeing, H. Food groups and risk of all-cause mortality: A systematic review and meta-analysis of prospective studies. Am. J. Clin. Nutr. 2017, 105, 1462–1473. [Google Scholar] [CrossRef]
- Abete, I.; Romaguera, D.; Vieira, A.R.; Lopez De Munain, A.; Norat, T. Association between total, processed, red and white meat consumption and all-cause, CVD and IHD mortality: A meta-analysis of cohort studies. Br. J. Nutr. 2014, 112, 762–775. [Google Scholar] [CrossRef] [PubMed]
- Zeraatkar, D.; Han, M.A.; Guyatt, G.H.; Vernooij, R.W.M.; El Dib, R.; Cheung, K.; Milio, K.; Zworth, M.; Bartoszko, J.J.; Valli, C.; et al. Red and processed meat consumption and risk for all-cause mortality and cardiometabolic outcomes a systematic review and meta-analysis of cohort studies. Ann. Intern. Med. 2019, 171, 703–710. [Google Scholar] [CrossRef] [PubMed]
- Vernooij, R.W.M.; Zeraatkar, D.; Han, M.A.; El Dib, R.; Zworth, M.; Milio, K.; Sit, D.; Lee, Y.; Gomaa, H.; Valli, C.; et al. Patterns of red and processed meat consumption and risk for cardiometabolic and cancer outcomes a systematic review and meta-analysis of cohort studies. Ann. Intern. Med. 2019, 171, 732–741. [Google Scholar] [CrossRef] [PubMed]
- Pan, A.; Sun, Q.; Bernstein, A.M.; Schulze, M.B.; Manson, J.A.; Stampfer, M.J.; Willett, W.C.; Hu, F.B. Red meat consumption and mortality: Results from 2 prospective cohort studies. Arch. Intern. Med. 2012, 172, 555–563. [Google Scholar] [PubMed]
- Pan, A.; Sun, Q.; Bernstein, A.M.; Schulze, M.B.; Manson, J.A.; Willett, W.C.; Hu, F.B. Red meat consumption and risk of type 2 diabetes: 3 Cohorts of US adults and an updated meta-analysis. Am. J. Clin. Nutr. 2011, 94, 1088–1096. [Google Scholar] [CrossRef] [PubMed]
- de Gavelle, E.; Davidenko, O.; Fouillet, H.; Delarue, J.; Darcel, N.; Huneau, J.F.; Mariotti, F. The Willingness to Modify Portion Sizes or Eat New Protein Foods Largely Depends on the Dietary Pattern of Protein Intake. Nutrients 2019, 11, 156. [Google Scholar] [CrossRef] [PubMed]
- Figueira, N.; Curtain, F.; Beck, E.; Grafenauer, S. Consumer Understanding and Culinary Use of Legumes in Australia. Nutrients 2019, 11, 1575. [Google Scholar] [CrossRef]
- Kamboj, R.; Nanda, V. Proximate composition, nutritional profile and health benefits of legumes: A review. Legume Res. 2018, 41, 325–332. [Google Scholar]
- Becerra-Tomás, N.; Paz-Graniel, I.; Kendall, C.; Kahleova, H.; Rahelic, D.; Sievenpiper, J.L.; Salas-Salvadó, J. Nut consumption and incidence of cardiovascular diseases and cardiovascular disease mortality: A meta-analysis of prospective cohort studies. Nutr. Rev. 2019, 77, 691–709. [Google Scholar] [CrossRef]
- Viguiliouk, E.; Glenn, A.J.; Nishi, S.K.; Chiavaroli, L.; Seider, M.; Khan, T.; Bonaccio, M.; Iacoviello, L.; Mejia, S.B.; Jenkins, D.J.A.; et al. Associations between Dietary Pulses Alone or with Other Legumes and Cardiometabolic Disease Outcomes: An Umbrella Review and Updated Systematic Review and Meta-analysis of Prospective Cohort Studies. Adv. Nutr. 2019, 10, S308–S319. [Google Scholar] [CrossRef]
- Vanham, D.; Mekonnen, M.M.; Hoekstra, A.Y. Treenuts and groundnuts in the EAT-Lancet reference diet: Concerns regarding sustainable water use. Glob. Food Secur. 2020, 24, 100357. [Google Scholar] [CrossRef] [PubMed]
- Feeney, M.J.; Dwyer, J.; Hasler-Lewis, C.M.; Milner, J.A.; Noakes, M.; Rowe, S.; Wach, M.; Beelman, R.B.; Caldwell, J.; Cantorna, M.T.; et al. Mushrooms and health summit proceedings. J. Nutr. 2014, 144, 1128S–1136S. [Google Scholar] [CrossRef] [PubMed]
- Rotola-Pukkila, M.; Yang, B.; Hopia, A. The effect of cooking on umami compounds in wild and cultivated mushrooms. Food Chem. 2019, 278, 56–66. [Google Scholar] [CrossRef] [PubMed]
- Schwingshackl, L.; Schwedhelm, C.; Hoffmann, G.; Boeing, H. Potatoes and risk of chronic disease: A systematic review and dose response meta-analysis. Eur. J. Nutr. 2019, 58, 2243–2251. [Google Scholar] [CrossRef]
- Frankowska, A.; Jeswani, H.K.; Azapagic, A. Environmental impacts of vegetables consumption in the UK. Sci. Total Environ. 2019, 682, 80–105. [Google Scholar] [CrossRef]
- Röös, E.; Karlsson, H. Effect of eating seasonal on the carbon footprint of Swedish vegetable consumption. J. Clean. Prod. 2013, 59, 63–72. [Google Scholar] [CrossRef]
- Hadjikakou, M. Trimming the excess: Environmental impacts of discretionary food consumption in Australia. Ecol. Econ. 2017, 131, 119–128. [Google Scholar] [CrossRef]
- Hallström, E.; Carlsson-Kanyama, A.; Borjesson, P. Environmental impact of dietary change: A systematic review. J. Clean. Prod. 2015, 91, 1–11. [Google Scholar] [CrossRef]
- Hu, F.B.; Otis, B.O.; McCarthy, G. Can Plant-Based Meat Alternatives Be Part of a Healthy and Sustainable Diet? JAMA 2019, 322, 1547–1548. [Google Scholar] [CrossRef]
- Schanes, K.; Dobernig, K.; Goezet, B. Food waste Matters—A systematic review of household food waste practices and their policy implications. J. Clean. Prod. 2018, 182, 978–991. [Google Scholar] [CrossRef]
- Canales Holzeis, C.; Fears, R.; Moughan, P.J.; Benton, T.G.; Hendriks, S.L.; Clegg, M.; ter Meulen, V.; von Braun, J. Food systems for delivering nutritious and sustainable diets: Perspectives from the global network of science academies. Glob. Food Secur. 2019, 21, 72–76. [Google Scholar] [CrossRef]
- Darmon, N.; Drewnowski, A. Contribution of food prices and diet cost to socioeconomic disparities in diet quality and health: A systematic review and analysis. Nutr. Rev. 2015, 73, 643–660. [Google Scholar] [CrossRef] [PubMed]
- Taufik, D.; Verain, M.C.D.; Bouwman, E.P.; Reinders, M.J. Determinants of real-life behavioural interventions to stimulate more plant-based and less animal-based diets: A systematic review. Trends Food Sci. Technol. 2019, 93, 281–303. [Google Scholar] [CrossRef]
| Food Groups | Model 1: EAT-Lancet Reference Diet with Danish Foods (g per 10 MJ) 4 | Model 2: Danish Adapted Plant-Based Diet (g per 10 MJ) |
|---|---|---|
| Bread and cereals | 220 (dry, raw) | 390 (cooked) |
| Whole grain content | 220 | 116 |
| Potatoes | 47 | 100 |
| All vegetables (excl. legumes) | 285 | 300 |
| Dark green vegetables | 95 | 100 |
| Red and orange vegetables | 95 | 100 |
| Other vegetables | 95 | 100 |
| All fruits and berries, incl. juice | 189 | 300 |
| Dairy foods | 236 | 250 |
| Cheese | Included in dairy foods | 20 |
| Beef, lamb, pork, cooked 1 | 12 | 15 |
| Poultry, cooked 1 | 27 | 30 |
| Eggs | 12 | 15 |
| Fish, cooked 1 | 27 | 50 |
| Legumes, cooked 2 | 178 | 100 |
| Nuts, ground nuts and seeds | 48 | 46 |
| Vegetable fats | 44 | 25 |
| Animal fats | 4 | 4 |
| Coffee, tea and water | Not specified | 2000 |
| Discretionary foods 3 | Not specified | 157 |
| Macronutrients | Model 1: EAT-Lancet Reference Diet with Danish Foods (per 10 MJ) | Model 2: Danish Adapted Plant-Based Diet (per 10 MJ) | Nordic Nutrition Recommendations 2012 3 |
|---|---|---|---|
| Protein, g | 82 | 92 | |
| Carbohydrates, g | 264 | 275 | |
| Added, refined sugars, g | 29 | 23 | |
| Fat, g | 102 | 89 | |
| Saturated fatty acids, g | 23 | 24 | |
| n-3 fatty acids, g | 3 | 4 | |
| Alcohol, g | 0 | 5 | |
| Protein, E% 1 | 14 | 16 | 10-20 (15) |
| Carbohydrates, E% 1 | 48 | 51 | 45-60 (52-53) |
| Added, refined sugars, E% 1 | 5.0 | 4.0 | ≤10 |
| Dietary fibre, g/10 MJ | 43 | 43 | ≥30 |
| Fat, E% 1 | 38 | 33 | 25-40 (32-33) |
| Saturated fatty acids, E% 1 | 8.6 | 8.8 | ≤10 |
| n-3 fatty acids, E% 1 | 1.0 | 1.3 | ≥1 |
| Alcohol, E% | 0 | 1.4 2 | <5 |
| Vitamins | Model 1: EAT-Lancet Reference Diet with Danish Foods (per 10 MJ) 1 | Model 2: Danish Adapted Plant-Based Diet (per 10 MJ) 1 | Nordic Nutrition Recommendations 2012 2 |
|---|---|---|---|
| Vitamin A, RE | 751 | 941 | 800 |
| Vitamin D, µg | 2.5 | 4.7 | 14 |
| Vitamin E, α-TE | 21 | 15 | 9 |
| Vitamin B1, mg | 1.9 | 1.7 | 1.2 |
| Vitamin B2, mg | 1.5 | 1.8 | 1.4 |
| Niacin, NE | 30 | 37 | 16 |
| Vitamin B6, mg | 2.5 | 2.2 | 1.3 |
| Folate, µg | 672 | 694 | 450 |
| Vitamin B12, µg | 2.4 | 5.4 | 2 |
| Vitamin C, mg | 153 | 221 | 80 |
| Minerals | Model 1: EAT-Lancet Reference Diet with Danish Foods (per 10 MJ) 1 | Model 2: Danish Adapted Plant-Based Diet (per 10 MJ) 1 | Nordic Nutrition Recommendations 2012 2 |
|---|---|---|---|
| Sodium, mg | 383 | 2355 | ≤2400 3 |
| Potassium, g | 3.9 | 4.6 | 3.5 |
| Calcium, mg | 684 | 1037 | 1000 |
| Magnesium, mg | 584 | 555 | 320 |
| Phosphorus, mg | 1787 | 1769 | 800 |
| Iron, mg | 18 | 16 | 16 |
| Zinc, mg | 11 | 12 | 12 |
| Iodine, µg | 85 | 154 | 170 |
| Selenium, µg | 35 | 57 | 57 |
| Eat More of | Eat Adequate/ Moderate Amounts of | Limit Intake of |
|---|---|---|
| Vegetables, including dark green and red/orange vegetables | Fish and seafood (choose the most sustainable) | Red meat (particularly beef) and processed meat |
| Legumes | Milk (low-fat) and dairy products | Discretionary foods |
| Nuts and seeds | Vegetable oils | Salt |
| Fruits and berries | Poultry and eggs | Alcohol |
| Whole-grain products and potatoes | (Mushrooms) | Ultra-processed foods |
| Avoid over-consumption and minimize food waste | ||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lassen, A.D.; Christensen, L.M.; Trolle, E. Development of a Danish Adapted Healthy Plant-Based Diet Based on the EAT-Lancet Reference Diet. Nutrients 2020, 12, 738. https://doi.org/10.3390/nu12030738
Lassen AD, Christensen LM, Trolle E. Development of a Danish Adapted Healthy Plant-Based Diet Based on the EAT-Lancet Reference Diet. Nutrients. 2020; 12(3):738. https://doi.org/10.3390/nu12030738
Chicago/Turabian StyleLassen, Anne D., Lene M. Christensen, and Ellen Trolle. 2020. "Development of a Danish Adapted Healthy Plant-Based Diet Based on the EAT-Lancet Reference Diet" Nutrients 12, no. 3: 738. https://doi.org/10.3390/nu12030738
APA StyleLassen, A. D., Christensen, L. M., & Trolle, E. (2020). Development of a Danish Adapted Healthy Plant-Based Diet Based on the EAT-Lancet Reference Diet. Nutrients, 12(3), 738. https://doi.org/10.3390/nu12030738





