Weight Status, Adherence to the Mediterranean Diet, Physical Activity Level, and Sleep Behavior of Italian Junior High School Adolescents
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants and Study Design
2.1.1. Personal Data
2.1.2. Adherence to the Mediterranean Diet (MD)
2.1.3. Physical Activity
2.1.4. Sleep Behavior
2.1.5. School Performance
2.2. Statistical Analysis
3. Results
3.1. Adolescents’Anthropometrics and Lifestyle Factors
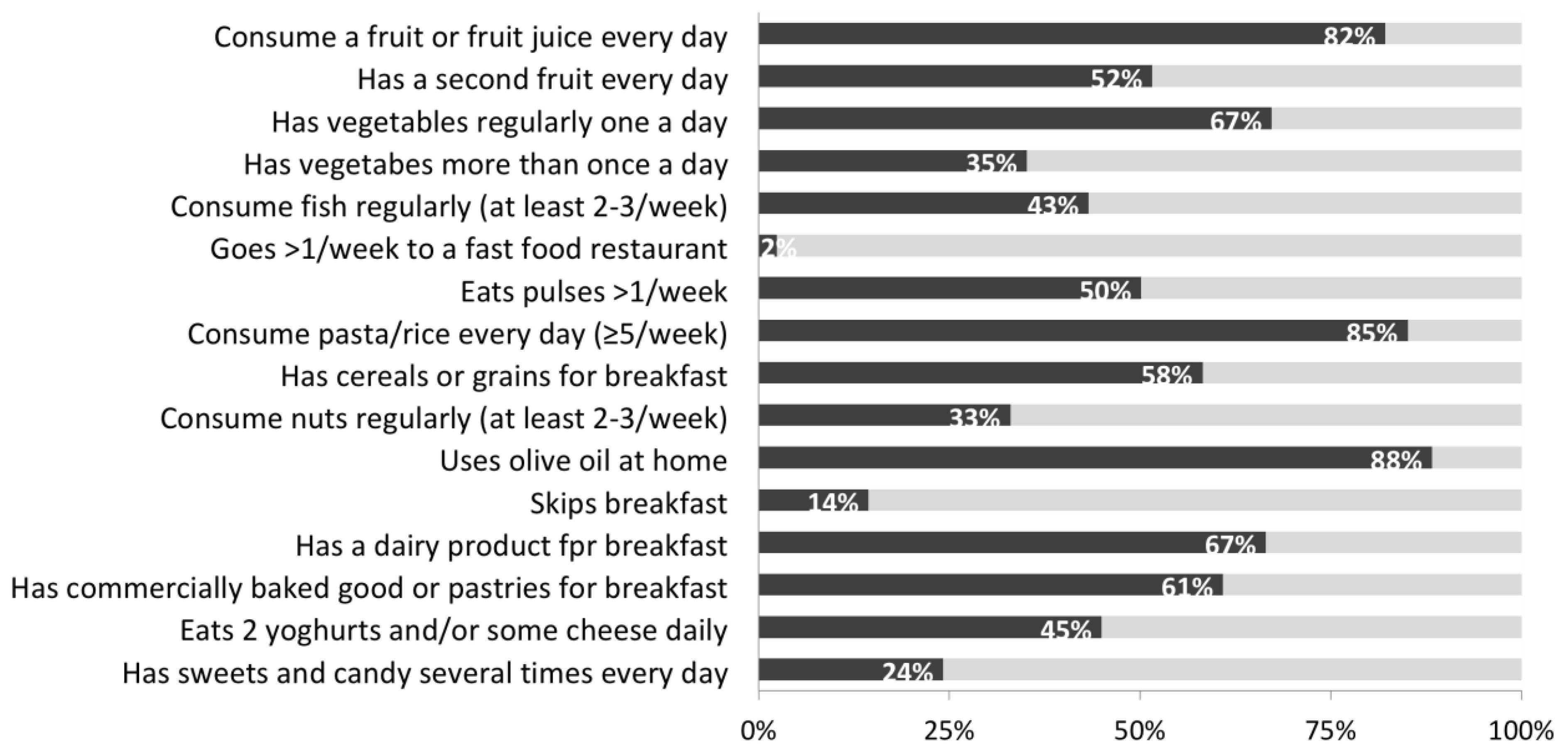
3.2. Dietary Habits
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Medina-Remón, A.; Kirwan, R.; Lamuela-Raventós, R.M.; Estruch, R. Dietary patterns and the risk of obesity, type 2 diabetes mellitus, cardiovascular diseases, asthma, and neurodegenerative diseases. Crit. Rev. Food Sci. Nutr. 2018, 58, 262–296. [Google Scholar] [CrossRef]
- Organization for Economic Cooperation and Development (OECD). Obesity Update 2017. OECD: 2017. Available online: https://www.oecd.org/health/obesity-update.htm (accessed on 24 January 2020).
- Moreno, L.A.; Rodriguez, G.; Fleta, J.; Bueno-Lozano, M.; Lazaro, A.; Bueno, G. Trends of dietary habits in adolescents. Crit. Rev. Food Sci. Nutr. 2010, 50, 106–112. [Google Scholar] [CrossRef]
- Slawson, D.L.; Fitzgerald, N.; Morgan, K.T. Position of the academy of nutrition and dietetics: The role of nutrition in health promotion and chronic disease prevention. J. Acad. Nutr. Diet. 2013, 113, 972–979. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Diet, Nutrition, and the Prevention of Chronic Diseases: Report of a Joint Who/FAO Expert Consultation; World Health Organization: Geneva, Switzerland, 2003; Volume 916. [Google Scholar]
- Adair, L.S.; Popkin, B.M. Are child eating patterns being transformed globally? Obes. Res. 2005, 13, 1281–1299. [Google Scholar] [CrossRef] [PubMed]
- Cavadini, C.; Siega-Riz, A.M.; Popkin, B.M. Us adolescent food intake trends from 1965 to 1996. Arch. Dis. Child. 2000, 83, 18–24. [Google Scholar] [CrossRef] [PubMed]
- Bonaccio, M.; Di Castelnuovo, A.; Bonanni, A.; Costanzo, S.; De Lucia, F.; Persichillo, M.; Zito, F.; Donati, M.B.; de Gaetano, G.; Iacoviello, L. Decline of the mediterranean diet at a time of economic crisis. Results from the moli-sani study. Nutr. Metab. Cardiovasc. Dis. 2014, 24, 853–860. [Google Scholar] [CrossRef]
- León-Muñoz, L.M.; Guallar-Castillón, P.; Graciani, A.; López-García, E.; Mesas, A.E.; Aguilera, M.T.; Banegas, J.R.; Rodríguez-Artalejo, F. Adherence to the mediterranean diet pattern has declined in spanish adults. J. Nutr. 2012, 142, 1843–1850. [Google Scholar] [CrossRef]
- González, K.; Fuentes, J.; Márquez, J.L. Physical inactivity, sedentary behavior and chronic diseases. Korean J. Fam. Med. 2017, 38, 111–115. [Google Scholar] [CrossRef]
- Robinson, T.N.; Banda, J.A.; Hale, L.; Lu, A.S.; Fleming-Milici, F.; Calvert, S.L.; Wartella, E. Screen media exposure and obesity in children and adolescents. Pediatrics 2017, 140, S97–S101. [Google Scholar] [CrossRef]
- Fatima, Y.; Doi, S.A.; Mamun, A.A. Longitudinal impact of sleep on overweight and obesity in children and adolescents: A systematic review and bias-adjusted meta-analysis. Obes. Rev. 2015, 16, 137–149. [Google Scholar] [CrossRef]
- Li, L.; Zhang, S.; Huang, Y.; Chen, K. Sleep duration and obesity in children: A systematic review and meta-analysis of prospective cohort studies. J. Paediatr. Child Health 2017, 53, 378–385. [Google Scholar] [CrossRef] [PubMed]
- Chaput, J.P.; Katzmarzyk, P.T.; LeBlanc, A.G.; Tremblay, M.S.; Barreira, T.V.; Broyles, S.T.; Fogelholm, M.; Hu, G.; Kuriyan, R.; Kurpad, A.; et al. Associations between sleep patterns and lifestyle behaviors in children: An international comparison. Int. J. Obes. Suppl. 2015, 5, S59–S65. [Google Scholar] [CrossRef] [PubMed]
- Chaput, J.-P.; Gray, C.E.; Poitras, V.J.; Carson, V.; Gruber, R.; Olds, T.; Weiss, S.K.; Connor Gorber, S.; Kho, M.E.; Sampson, M.; et al. Systematic review of the relationships between sleep duration and health indicators in school-aged children and youth. Appl. Physiol. Nutr. Metab. 2016, 41, S266–S282. [Google Scholar] [CrossRef] [PubMed]
- Faught, E.L.; Ekwaru, J.P.; Gleddie, D.; Storey, K.E.; Asbridge, M.; Veugelers, P.J. The combined impact of diet, physical activity, sleep and screen time on academic achievement: A prospective study of elementary school students in Nova Scotia, Canada. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 29. [Google Scholar] [CrossRef]
- Cole, T.J.; Lobstein, T. Extended international (IOTF) body mass index cut-offs for thinness, overweight and obesity. Pediatr. Obes. 2012, 7, 284–294. [Google Scholar] [CrossRef]
- Serra-Majem, L.; Ribas, L.; Ngo, J.; Ortega, R.M.; García, A.; Pérez-Rodrigo, C.; Aranceta, J. Food, youth and the mediterranean diet in spain. Development of kidmed, mediterranean diet quality index in children and adolescents. Public Health Nutr. 2004, 7, 931–935. [Google Scholar] [CrossRef]
- Kowalski, K.C.; Crocker, P.R.E.; Donen, R.M. The Physical Activity Questionnaire for Older Children (PAQ-C) and Adolescents (PAQ-A) Manual; College of Kinesiology University of Saskatchewan: Saskatchewan, Saskatoon, 2004. [Google Scholar]
- Hirshkowitz, M.; Whiton, K.; Albert, S.M.; Alessi, C.; Bruni, O.; DonCarlos, L.; Hazen, N.; Herman, J.; Adams Hillard, P.J.; Katz, E.S.; et al. National sleep foundation’s updated sleep duration recommendations: Final report. Sleep Health 2015, 1, 233–243. [Google Scholar] [CrossRef]
- Drake, C.; Nickel, C.; Burduvali, E.; Roth, T.; Jefferson, C.; Badia, P. The pediatric daytime sleepiness scale (PDSS): Sleep habits and school outcomes in middle-school children. Sleep 2003, 26, 455–458. [Google Scholar]
- Cavallo, F.; Lemma, P.; Dalmasso, P.; Vieno, A.; Lazzeri, G.; Galeone, D. Rapporto sui dati HBSC italia 2014; Dipartimento di Scienze della Sanità Pubblica e Pediatriche: Torino, Italy, 2016. [Google Scholar]
- Lazzeri, G.; Giacchi, M.V.; Spinelli, A.; Pammolli, A.; Dalmasso, P.; Nardone, P.; Lamberti, A.; Cavallo, F. Overweight among students aged 11–15 years and its relationship with breakfast, area of residence and parents’ education: Results from the italian hbsc 2010 cross-sectional study. Nutr. J. 2014, 13, 69. [Google Scholar] [CrossRef]
- Ferranti, R.; Marventano, S.; Castellano, S.; Giogianni, G.; Nolfo, F.; Rametta, S.; Matalone, M.; Mistretta, A. Sleep quality and duration is related with diet and obesity in young adolescent living in sicily, southern Italy. Sleep Sci. 2016, 9, 117–122. [Google Scholar] [CrossRef]
- Rosi, A.; Calestani, M.V.; Parrino, L.; Milioli, G.; Palla, L.; Volta, E.; Brighenti, F.; Scazzina, F. Weight status is related with gender and sleep duration but not with dietary habits and physical activity in primary school italian children. Nutrients 2017, 9, 579. [Google Scholar] [CrossRef] [PubMed]
- Binkin, N.; Fontana, G.; Lamberti, A.; Cattaneo, C.; Baglio, G.; Perra, A.; Spinelli, A. A national survey of the prevalence of childhood overweight and obesity in Italy. Obes. Rev. 2010, 11, 2–10. [Google Scholar] [CrossRef] [PubMed]
- Archero, F.; Ricotti, R.; Solito, A.; Carrera, D.; Civello, F.; Di Bella, R.; Bellone, S.; Prodam, F. Adherence to the mediterranean diet among school children and adolescents living in northern italy and unhealthy food behaviors associated to overweight. Nutrients 2018, 10, 1322. [Google Scholar] [CrossRef] [PubMed]
- Inchley, J.; Currie, D. Growing up Unequal: Gender and Socioeconomic Differences in Young People’s Health and Well-Being; International Report from the HBSC Study; Health Behaviour in School-aged Children (HBSC): Copenhagen, Denmark, 2013; Volume 2014, pp. 2–3. [Google Scholar]
- Currie, C.; Zanotti, C.; Morgan, A.; Currie, D.; De Looze, M.; Roberts, C.; Samdal, O.; Smith, O.; Barnekow, V. Social determinants of health and well-being among young people: HBSC international report from the 2009/2010 survey. Health Policy Child Adolesc. 2012, 6, 130–131. [Google Scholar]
- Arcila-Agudelo, A.M.; Ferrer-Svoboda, C.; Torres-Fernàndez, T.; Farran-Codina, A. Determinants of adherence to healthy eating patterns in a population of children and adolescents: Evidence on the mediterranean diet in the city of Mataró (Catalonia, Spain). Nutrients 2019, 11, 854. [Google Scholar] [CrossRef]
- Rosi, A.; Paolella, G.; Biasini, B.; Scazzina, F.; Alicante, P.; De Blasio, F.; dello Russo, M.; Paolella, G.; Rendina, D.; Rosi, A.; et al. Dietary habits of adolescents living in north america, europe or oceania: A review on fruit, vegetable and legume consumption, sodium intake, and adherence to the Mmediterranean Diet. Nutr. Metab. Cardiovasc. Dis. 2019. [Google Scholar] [CrossRef]
- Roccaldo, R.; Censi, L.; D’Addezio, L.; Toti, E.; Martone, D.; D’Addesa, D.; Cernigliaro, A. Adherence to the mediterranean diet in italian school children (the Zoom8 study). Int. J. Food Sci. Nutr. 2014, 65, 621–628. [Google Scholar] [CrossRef]
- Deshmukh-Taskar, P.R.; Nicklas, T.A.; O’Neil, C.E.; Keast, D.R.; Radcliffe, J.D.; Cho, S. The relationship of breakfast skipping and type of breakfast consumption with nutrient intake and weight status in children and adolescents: The national health and nutrition examination survey 1999–2006. J. Am. Diet. Assoc. 2010, 110, 869–878. [Google Scholar] [CrossRef]
- Vanelli, M.; Iovane, B.; Bernardini, A.; Chiari, G.; Errico, M.K.; Gelmetti, C.; Corchia, M.; Ruggerini, A.; Volta, E.; Rossetti, S. Breakfast habits of 1202 northern italian children admitted to a summer sport school. Breakfast skipping is associated with overweight and obesity. Acta Biomed. 2005, 76, 79–85. [Google Scholar]
- Iaccarino Idelson, P.; Scalfi, L.; Valerio, G. Adherence to the mediterranean diet in children and adolescents: A systematic review. Nutr. Metab. Cardiovasc. Dis. 2017, 27, 283–299. [Google Scholar] [CrossRef]
- Grosso, G.; Galvano, F. Mediterranean diet adherence in children and adolescents in southern european countries. NFS J. 2016, 3, 13–19. [Google Scholar] [CrossRef]
- Grosso, G.; Marventano, S.; Buscemi, S.; Scuderi, A.; Matalone, M.; Platania, A.; Giorgianni, G.; Rametta, S.; Nolfo, F.; Galvano, F.; et al. Factors associated with adherence to the Mediterranean diet among adolescents living in Sicily, Southern Italy. Nutrients 2013, 5, 4908–4923. [Google Scholar] [CrossRef] [PubMed]
- Bartel, K.A.; Gradisar, M.; Williamson, P. Protective and risk factors for adolescent sleep: A meta-analytic review. Sleep Med. Rev. 2015, 21, 72–85. [Google Scholar] [CrossRef] [PubMed]
- Al-Hazzaa, H.M.; Al-Sobayel, H.I.; Abahussain, N.A.; Qahwaji, D.M.; Alahmadi, M.A.; Musaiger, A.O. Association of dietary habits with levels of physical activity and screen time among adolescents living in saudi arabia. J. Hum. Nutr. Diet. 2014, 27, 204–213. [Google Scholar] [CrossRef] [PubMed]
- Garaulet, M.; Ortega, F.B.; Ruiz, J.R.; Rey-López, J.P.; Béghin, L.; Manios, Y.; Cuenca-García, M.; Plada, M.; Diethelm, K.; Kafatos, A.; et al. Short sleep duration is associated with increased obesity markers in european adolescents: Effect of physical activity and dietary habits. The HELENA study. Int. J. Obes. 2011, 35, 1308. [Google Scholar] [CrossRef] [PubMed]
- Westerlund, L.; Ray, C.; Roos, E. Associations between sleeping habits and food consumption patterns among 10–11-year-old children in Finland. Br. J. Nutr. 2009, 102, 1531–1537. [Google Scholar] [CrossRef]
- Esteban-Cornejo, I.; Izquierdo-Gomez, R.; Gómez-Martínez, S.; Padilla-Moledo, C.; Castro-Piñero, J.; Marcos, A.; Veiga, O.L. Adherence to the mediterranean diet and academic performance in youth: The up&down study. Eur. J. Nutr. 2016, 55, 1133–1140. [Google Scholar] [CrossRef]
- Dumith, S.C.; Muniz, L.C.; Tassitano, R.M.; Hallal, P.C.; Menezes, A.M.B. Clustering of risk factors for chronic diseases among adolescents from southern brazil. Prev. Med. 2012, 54, 393–396. [Google Scholar] [CrossRef]
- Coe, D.P.; Pivarnik, J.M.; Womack, C.J.; Reeves, M.J.; Malina, R.M. Effect of physical education and activity levels on academic achievement in children. Med. Sci. Sport Exerc. 2006, 38, 1515–1519. [Google Scholar] [CrossRef]
- Rasberry, C.N.; Lee, S.M.; Robin, L.; Laris, B.A.; Russell, L.A.; Coyle, K.K.; Nihiser, A.J. The association between school-based physical activity, including physical education, and academic performance: A systematic review of the literature. Prev. Med. 2011, 52, S10–S20. [Google Scholar] [CrossRef]
- Vilhjalmsson, R.; Kristjansdottir, G. Gender differences in physical activity in older children and adolescents: The central role of organized sport. Soc. Sci. Med. 2003, 56, 363–374. [Google Scholar] [CrossRef]
- Paruthi, S.; Brooks, L.J.; D’Ambrosio, C.; Hall, W.A.; Kotagal, S.; Lloyd, R.M.; Malow, B.A.; Maski, K.; Nichols, C.; Quan, S.F. Recommended amount of sleep for pediatric populations: A consensus statement of the american academy of sleep medicine. J. Clin. Sleep Med. 2016, 12, 785–786. [Google Scholar] [CrossRef] [PubMed]
- Shochat, T.; Cohen-Zion, M.; Tzischinsky, O. Functional consequences of inadequate sleep in adolescents: A systematic review. Sleep Med. Rev. 2014, 18, 75–87. [Google Scholar] [CrossRef] [PubMed]
- Bel, S.; Michels, N.; De Vriendt, T.; Patterson, E.; Cuenca-García, M.; Diethelm, K.; Gutin, B.; Grammatikaki, E.; Manios, Y.; Leclercq, C.; et al. Association between self-reported sleep duration and dietary quality in european adolescents. Br. J. Nutr. 2013, 110, 949–959. [Google Scholar] [CrossRef]
- Patel, S.R.; Hu, F.B. Short sleep duration and weight gain: A systematic review. Obesity (Silver Spring) 2008, 16. [Google Scholar] [CrossRef]
- Lytle, L.A.; Murray, D.M.; Laska, M.N.; Pasch, K.E.; Anderson, S.E.; Farbakhsh, K. Examining the longitudinal relationship between change in sleep and obesity risk in adolescents. Health Educ. Behav. 2012, 40, 362–370. [Google Scholar] [CrossRef]
| Variables | Total Sample (n = 409) | Male (n = 222) | Female (n = 187) | p Value |
|---|---|---|---|---|
| Age (years) | 12.5 ± 0.6 | 12.5 ± 0.6 | 12.5 ± 0.7 | 0.759 |
| Weight (kg) | 44.9 ± 9.1 | 45.7 ± 9.2 | 43.9 ± 8.9 | 0.055 |
| Height (m) | 1.6 ± 0.1 | 1.6 ± 0.1 | 1.6 ± 0.1 | 0.888 |
| BMI (kg/m2) | 18.4 ± 2.7 | 18.7 ± 2.6 | 18.1 ± 2.8 | 0.014 |
| BMI category | 0.004 | |||
| Underweight | 67 (16%) | 25 (11%) | 42 (22%) | |
| Normal weight | 284 (70%) | 159 (72%) | 125 (67%) | |
| Overweight | 58 (14%) | 38 (17%) | 20 (11%) | |
| KIDMED score (points) | 6.0 ± 2.3 | 6.0 ± 2.3 | 6.1 ± 2.3 | 0.857 |
| Adherence to the MD | 0.979 | |||
| Low | 51 (12%) | 27 (12%) | 24 (13%) | |
| Medium | 244 (60%) | 133 (60%) | 111 (59%) | |
| High | 114 (28%) | 62 (28%) | 52 (28%) | |
| Physical Activity Level | 0.938 | |||
| Sedentary | 2 (0%) | 1 (1%) | 1 (1%) | |
| Light | 76 (23%) | 38 (22%) | 38 (25%) | |
| Moderate | 206 (63%) | 110 (63%) | 96 (62%) | |
| Vigorous | 45 (14%) | 25 (14%) | 20 (13%) | |
| Week sleep time (hh:mm) | 8:33 ± 00:49 | 8:29 ± 00:50 | 8:38 ± 00:46 | 0.640 |
| Weekend sleep time (hh:mm) | 9:55 ± 01:31 | 9:51 ± 01:27 | 10:00 ± 01:35 | 0.892 |
| Average sleep time (hh:mm) | 8:56 ± 00:50 | 8:52 ± 00:51 | 9:01 ± 00:49 | 0.801 |
| Average sleep time adequacy | 0.464 | |||
| Low | 55 (13%) | 32 (14%) | 23 (12%) | |
| Adequate | 352 (86%) | 190 (86%) | 162 (87%) | |
| High | 1 (0%) | 0 (0%) | 1 (1%) | |
| PDSS score (points) | 15.8 ± 5.7 | 15.3 ± 5.9 | 16.4 ± 5.4 | 0.072 |
| Sleep quality | 0.526 | |||
| Low | 88 (22%) | 43 (20%) | 45 (24%) | |
| Medium | 244 (60%) | 136 (62%) | 108 (58%) | |
| High | 74 (18%) | 41 (19%) | 33 (18%) | |
| School average (grade) | 7.8 ± 1.0 | 7.8 ± 1.0 | 7.8 ± 1.1 | 0.744 |
| School performance | 0.373 | |||
| Excellent | 103 (25%) | 52 (23%) | 51 (27%) | |
| Good | 268 (65%) | 152 (68%) | 116 (62%) | |
| Poor | 38 (9%) | 18 (8%) | 20 (11%) |
| Variables | Total Sample (n = 409) | Underweight (n = 67) | Normal Weight (n = 284) | Overweight (n = 58) | p Value |
|---|---|---|---|---|---|
| KIDMED score (points) | 6.0 ± 2.3 | 6.2 ± 2.4 | 6.0 ± 2.1 | 5.8 ± 2.7 | 0.569 |
| Adherence to the MD | 0.459 | ||||
| Low | 51 (12%) | 7 (10%) | 33 (12%) | 11 (19%) | |
| Medium | 244 (60%) | 39 (58%) | 175 (62%) | 30 (52%) | |
| High | 114 (28%) | 21 (31%) | 76 (27%) | 17 (29%) | |
| Physical Activity Level | 0.313 | ||||
| Sedentary | 2 (0%) | 1 (1%) | 1 (0%) | 0 (0%) | |
| Light | 76 (23%) | 11 (22%) | 50 (22%) | 15 (31%) | |
| Moderate | 206 (63%) | 32 (63%) | 150 (66%) | 24 (49%) | |
| Vigorous | 45 (14%) | 7 (14%) | 28 (12%) | 10 (20%) | |
| Week sleep time (hh:mm) | 08:33 ± 00:49 | 08:36 ± 00:49 | 08:34 ± 00:47 | 08:22 ± 00:55 | 0.194 |
| Weekend sleep time (hh:mm) | 09:55 ± 01:31 | 09:58 ± 01:48 | 09:56 ± 01:24 | 09:44 ± 01:41 | 0.648 |
| Average sleep time (hh:mm) | 08:56 ± 00:50 | 08:59 ± 00:56 | 08:57 ± 00:48 | 08:45 ± 00:55 | 0.224 |
| Average sleep time adequacy | 0.696 | ||||
| Low | 55 (14%) | 9 (13%) | 35 (12%) | 11 (19%) | |
| Adequate | 352 (86%) | 58 (87%) | 247 (87%) | 47 (81%) | |
| High | 1 (0%) | 0 (0%) | 1 (0%) | 0 (0%) | |
| PDSS score (points) | 15.8 ± 5.7 | 16.0 ± 5.8 | 15.8 ± 5.5 | 15.7 ± 6.3 | 0.959 |
| Sleep quality | 0.880 | ||||
| Low | 88 (22%) | 16 (24%) | 58 (21%) | 14 (25%) | |
| Medium | 244 (60%) | 41 (61%) | 171 (61%) | 32 (56%) | |
| High | 74 (18%) | 10 (15%) | 53 (19%) | 11 (19%) | |
| School average (grade) | 7.8 ± 1.0 | 7.9 ± 0.9 | 7.8 ± 1.0 | 7.6 ± 1.0 | 0.302 |
| School performance | 0.498 | ||||
| Excellent | 103 (25%) | 15 (22%) | 75 (26%) | 13 (22%) | |
| Good | 268 (66%) | 49 (73%) | 180 (63%) | 39 (67%) | |
| Poor | 38 (9%) | 3 (5%) | 29 (10%) | 6 (10%) |
| Adherence to the Mediterranean Diet | |||||
|---|---|---|---|---|---|
| Variables | Total Sample (n = 409) | Low (n = 51) | Medium (n = 244) | High (n = 114) | p Value |
| Physical activity level | 0.135 | ||||
| Sedentary | 2 (0%) | 1 (3%) | 1 (1%) | 0 (0%) | |
| Light | 76 (23%) | 8 (21%) | 51 (26%) | 17 (18%) | |
| Moderate | 206 (63%) | 27 (71%) | 117 (60%) | 62 (64%) | |
| Vigorous | 45 (14%) | 2 (5%) | 25 (13%) | 18 (19%) | |
| Week sleep time (hh:mm) | 08:33 ± 00:49 | 08:43 ± 00:47 | 08:30 ± 00:50 | 08:35 ± 00:47 | 0.138 |
| Weekend sleep time (hh:mm) | 09:55 ± 01:31 | 09:56 ± 01:46 | 09:53 ± 01:28 | 09:57 ± 01:30 | 0.471 |
| Average sleep time (hh:mm) | 08:56 ± 00:50 | 09:04 ± 00:56 | 08:54 ± 00:51 | 08:59 ± 00:47 | 0.134 |
| Average sleep time adequacy | 0.025 | ||||
| Low | 55 (13%) | 10 (20%) | 35 (14%) | 10 (9%) | |
| Adequate | 352 (86%) | 40 (78%) | 208 (86%) | 104 (91%) | |
| High | 1 (0%) | 1 (2%) | 0 (0%) | 0 (0%) | |
| PDSS score (points) | 15.8 ± 5.7 | 17.4 ± 5.4 a | 16.1 ± 5.7 ab | 14.5 ± 5.4 b | 0.005 |
| Sleep quality | 0.010 | ||||
| Low | 88 (22%) | 17 (33%) | 58 (24%) | 13 (12%) | |
| Medium | 244 (60%) | 29 (57%) | 142 (58%) | 73 (65%) | |
| High | 74 (18%) | 5 (10%) | 43 (18%) | 26 (23%) | |
| School average (grade) | 7.8 ± 1.0 | 7.5 ± 1.0 b | 7.8 ± 1.0 ab | 8.0 ± 1.0 a | 0.018 |
| School performance | 0.083 | ||||
| Excellent | 103 (25%) | 9 (18%) | 58 (24%) | 36 (32%) | |
| Good | 268 (66%) | 33 (65%) | 165 (68%) | 70 (61%) | |
| Poor | 38 (9%) | 9 (18%) | 21 (9%) | 8 (7%) | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rosi, A.; Giopp, F.; Milioli, G.; Melegari, G.; Goldoni, M.; Parrino, L.; Scazzina, F. Weight Status, Adherence to the Mediterranean Diet, Physical Activity Level, and Sleep Behavior of Italian Junior High School Adolescents. Nutrients 2020, 12, 478. https://doi.org/10.3390/nu12020478
Rosi A, Giopp F, Milioli G, Melegari G, Goldoni M, Parrino L, Scazzina F. Weight Status, Adherence to the Mediterranean Diet, Physical Activity Level, and Sleep Behavior of Italian Junior High School Adolescents. Nutrients. 2020; 12(2):478. https://doi.org/10.3390/nu12020478
Chicago/Turabian StyleRosi, Alice, Francesca Giopp, Giulia Milioli, Gabriele Melegari, Matteo Goldoni, Liborio Parrino, and Francesca Scazzina. 2020. "Weight Status, Adherence to the Mediterranean Diet, Physical Activity Level, and Sleep Behavior of Italian Junior High School Adolescents" Nutrients 12, no. 2: 478. https://doi.org/10.3390/nu12020478
APA StyleRosi, A., Giopp, F., Milioli, G., Melegari, G., Goldoni, M., Parrino, L., & Scazzina, F. (2020). Weight Status, Adherence to the Mediterranean Diet, Physical Activity Level, and Sleep Behavior of Italian Junior High School Adolescents. Nutrients, 12(2), 478. https://doi.org/10.3390/nu12020478









