Impact on Dietary Intake of Two Levels of Technology-Assisted Personalized Nutrition: A Randomized Trial
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Participants and Recruitment
2.3. Intervention Groups
2.3.1. Low Personalization Group
2.3.2. High Personalization Group
2.4. Outcome Measures
2.4.1. Dietary Intake Assessment
2.4.2. Feedback on Intervention Components
2.4.3. Other Measures
2.5. Statistical Analysis
3. Results
3.1. Participant Baseline Characteristics and Dietary Intakes
3.2. Dietary Intake Outcomes
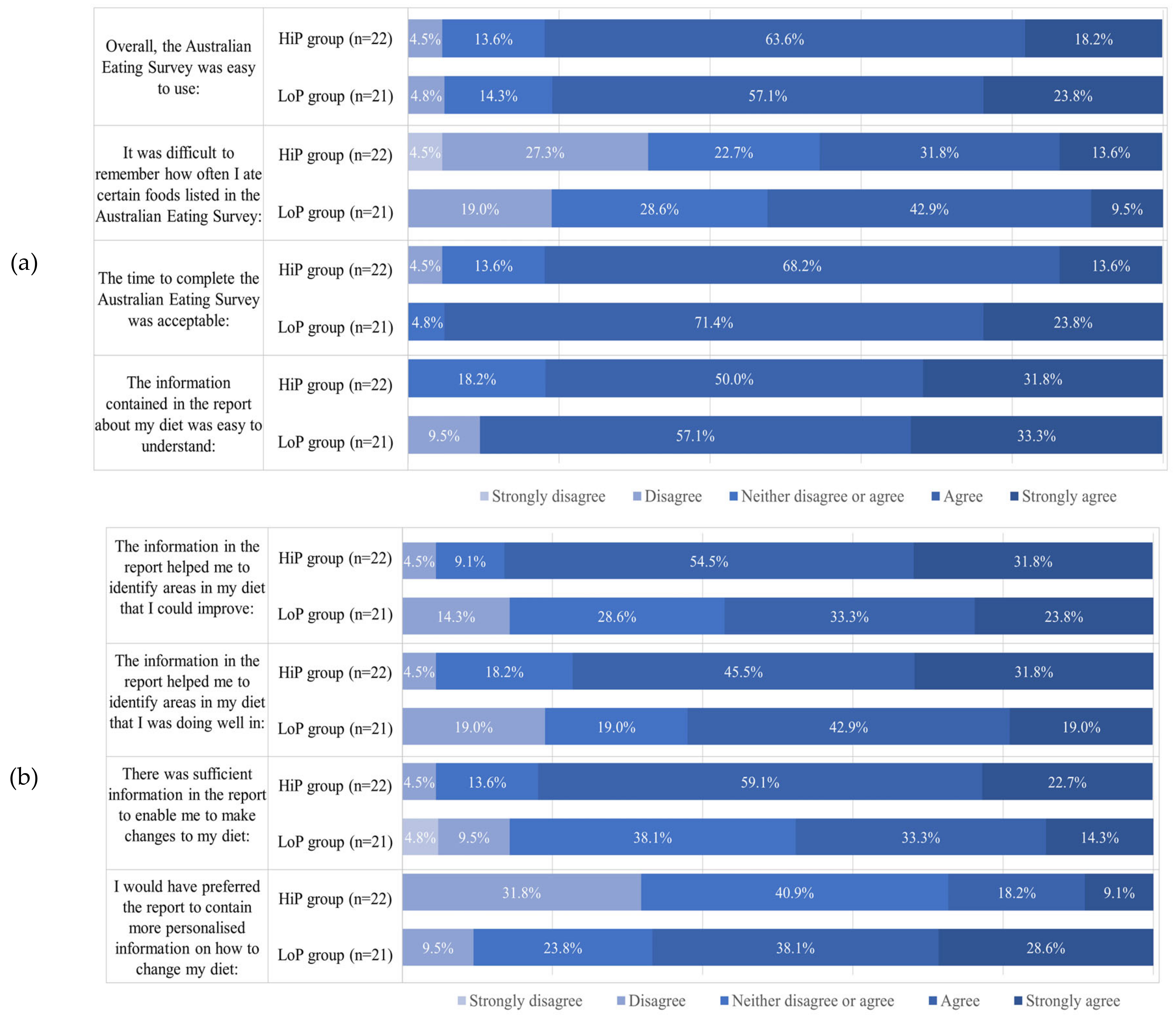
3.3. Perceptions of the AES and Feedback Report
3.4. Participant Perceptions of Dietitian Video Coaching Sessions
3.5. Perceptions of Dietary Intake Self-Monitoring and Text Message Feedback
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Onvani, S.; Haghighatdoost, F.; Surkan, P.J.; Larijani, B.; Azadbakht, L. Adherence to the Healthy Eating Index and Alternative Healthy Eating Index dietary patterns and mortality from all causes, cardiovascular disease and cancer: A meta-analysis of observational studies. J. Hum. Nutr. Diet. 2016, 30, 216–226. [Google Scholar] [CrossRef]
- Potter, J.; Brown, L.J.; Haslam, R.L.; Byles, J.E.; Collins, C.E. Diet Quality and Cancer Outcomes in Adults: A Systematic Review of Epidemiological Studies. Int. J. Mol. Sci. 2016, 17, 1052. [Google Scholar] [CrossRef]
- Schwingshackl, L.; Hoffmann, G. Diet Quality as Assessed by the Healthy Eating Index, the Alternate Healthy Eating Index, the Dietary Approaches to Stop Hypertension Score, and Health Outcomes: A Systematic Review and Meta-Analysis of Cohort Studies. J. Acad. Nutr. Diet. 2015, 115, 780–800.e5. [Google Scholar] [CrossRef] [PubMed]
- Stanaway, J.D.; Afshin, A.; Gakidou, E.; Lim, S.S.; Abate, D.; Abate, K.H.; Abbafati, C.; Abbasi, N.; Abbastabar, H.; Abd-Allah, F.; et al. Global, regional, and national comparative risk assessment of 84 behavioural, environmental and occupational, and metabolic risks or clusters of risks for 195 countries and territories, 1990–2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018, 392, 1923–1994. [Google Scholar] [CrossRef]
- Afshin, A.; Sur, P.J.; Fay, K.A.; Cornaby, L.; Ferrara, G.; Salama, J.S.; Mullany, E.C.; Abate, K.H.; Abbafati, C.; Abebe, Z.; et al. Health effects of dietary risks in 195 countries, 1990–2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2019, 393, 1958–1972. [Google Scholar] [CrossRef]
- Turner, G.M.; Larsen, K.; Candy, S.; Ogilvy, S.; Ananthapavan, J.; Moodie, M.; James, S.; Friel, S.; Ryan, C.J.; Lawrence, M.G.; et al. Squandering Australia’s food security—The environmental and economic costs of our unhealthy diet and the policy Path We’re On. J. Clean. Prod. 2018, 195, 1581–1599. [Google Scholar] [CrossRef]
- Broekhuizen, K.; Kroeze, W.; Van Poppel, M.N.M.; Oenema, A.; Brug, J. A Systematic Review of Randomized Controlled Trials on the Effectiveness of Computer-Tailored Physical Activity and Dietary Behavior Promotion Programs: An Update. Ann. Behav. Med. 2012, 44, 259–286. [Google Scholar] [CrossRef]
- Gibney, M.; Walsh, M.C. The future direction of personalised nutrition: My diet, my phenotype, my genes. Proc. Nutr. Soc. 2013, 72, 219–225. [Google Scholar] [CrossRef]
- Celis-Morales, C.; Livingstone, K.M.; Marsaux, C.F.M.; Forster, H.; O’Donovan, C.B.; Woolhead, C.; Macready, A.L.; Fallaize, R.; Navas-Carretero, S.; San-Cristobal, R.; et al. Design and baseline characteristics of the Food4Me study: A web-based randomised controlled trial of personalised nutrition in seven European countries. Genes Nutr. 2014, 10, 450. [Google Scholar] [CrossRef] [PubMed]
- Celis-Morales, C.A.; Livingstone, K.M.; Marsaux, C.F.; Macready, A.L.; Fallaize, R.; O’Donovan, C.B.; Woolhead, C.; Forster, H.; Walsh, M.C.; Navas-Carretero, S.; et al. Effect of personalized nutrition on health-related behaviour change: Evidence from the Food4me European randomized controlled trial. Int. J. Epidemiology 2016, 46, 578–588. [Google Scholar] [CrossRef]
- Li, S.X.; Ye, Z.; Whelan, K.; Truby, H. The effect of communicating the genetic risk of cardiometabolic disorders on motivation and actual engagement in preventative lifestyle modification and clinical outcome: A systematic review and meta-analysis of randomised controlled trials. Br. J. Nutr. 2016, 116, 924–934. [Google Scholar] [CrossRef] [PubMed]
- Collins, C.E.; Boggess, M.M.; Watson, J.F.; Guest, M.; Duncanson, K.; Pezdirc, K.; Rollo, M.E.; Hutchesson, M.J.; Burrows, T.L. Reproducibility and comparative validity of a food frequency questionnaire for Australian adults. Clin. Nutr. 2014, 33, 906–914. [Google Scholar] [CrossRef] [PubMed]
- Collins, C.E.; Burrows, T.L.; Rollo, M.E.; Boggess, M.M.; Watson, J.F.; Guest, M.; Duncanson, K.; Pezdirc, K.; Hutchesson, M.J. The Comparative Validity and Reproducibility of a Diet Quality Index for Adults: The Australian Recommended Food Score. Nutrients 2015, 7, 785–798. [Google Scholar] [CrossRef]
- National Health and Medical Research Council; Australian Government Department of Health and Ageing; New Zealand Ministry of Health. Nutrient Reference Values for Australia and New Zealand Including Recommended Dietary Intakes; National Health and Medical Research Council: Canberra, Australia, 2006.
- Michie, S.; Van Stralen, M.M.; West, R. The behaviour change wheel: A new method for characterising and designing behaviour change interventions. Implement. Sci. 2011, 6, 42. [Google Scholar] [CrossRef]
- Michie, S.; Atkins, L.; West, R. The Behaviour Change Wheel: A Guide to Designing Interventions; Silverback Publishing: London, UK, 2014. [Google Scholar]
- Michie, S.; Ashford, S.; Sniehotta, F.F.; Dombrowski, S.U.; Bishop, A.; French, D.P. A refined taxonomy of behaviour change techniques to help people change their physical activity and healthy eating behaviours: The CALO-RE taxonomy. Psychol. Heal. 2011, 26, 1479–1498. [Google Scholar] [CrossRef] [PubMed]
- National Health and Medical Research Council. Australian Dietary Guidelines; National Health and Medical Research Council: Canberra, Australia, 2013. [Google Scholar]
- Ashman, A.M.; Collins, C.E.; Brown, L.J.; Rae, K.M.; Rollo, M.E.; Wennberg, A.L.; Siapco, G. A Brief Tool to Assess Image-Based Dietary Records and Guide Nutrition Counselling Among Pregnant Women: An Evaluation. JMIR mHealth uHealth 2016, 4, e123. [Google Scholar] [CrossRef] [PubMed]
- Ashman, A.M.; Collins, C.E.; Brown, L.J.; Rae, K.M.; Rollo, M.E. Validation of a Smartphone Image-Based Dietary Assessment Method for Pregnant Women. Nutrients 2017, 9, 73. [Google Scholar] [CrossRef]
- Rollo, M.E.; Ash, S.; Lyons, P.M.; Russell, A. Trial of a mobile phone method for recording dietary intake in adults with type 2 diabetes: Evaluation and implications for future applications. J. Telemed. Telecare 2011, 17, 318–323. [Google Scholar] [CrossRef]
- Rollo, M.E.; Ash, S.; Lyons-Wall, P.; Russell, A.W. Evaluation of a Mobile Phone Image-Based Dietary Assessment Method in Adults with Type 2 Diabetes. Nutrients 2015, 7, 4897–4910. [Google Scholar] [CrossRef]
- Kerr, D.A.; Harray, A.J.; Pollard, C.M.; Dhaliwal, S.S.; Delp, E.J.; Howat, P.A.; Pickering, M.R.; Ahmad, Z.; Meng, X.; Pratt, I.S.; et al. The connecting health and technology study: A 6-month randomized controlled trial to improve nutrition behaviours using a mobile food record and text messaging support in young adults. Int. J. Behav. Nutr. Phys. Act. 2016, 13, 1–14. [Google Scholar] [CrossRef]
- Food Standards Australia New Zealand (FSANZ). AUSNUT 1999—Australian Food and Nutrient Database 1999 for Estimation of Dietary Intake; FSANZ: Canberra, Australia, 1999. [Google Scholar]
- Australian Bureau of Statistics (ABS). National Nutrition Survey: Nutrient Intakes and Physical Measurements; ABS: Canberra, Australia, 1998. [Google Scholar]
- Norman, C.D.; Skinner, H.A. eHEALS: The eHealth Literacy Scale. J. Med Internet Res. 2006, 8, e27. [Google Scholar] [CrossRef]
- Kelly, J.T.; Reidlinger, D.P.; Hoffmann, T.; Campbell, K.L. Telehealth methods to deliver dietary interventions in adults with chronic disease: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2016, 104, 1693–1702. [Google Scholar] [CrossRef]
- Ball, L.; Larsson, R.; Gerathy, R.; Hood, P.; Lowe, C. Working profile of Australian private practice Accredited Practising Dietitians. Nutr. Diet. 2013, 70, 196–205. [Google Scholar] [CrossRef]
- Jansen, S.; Ball, L.; Lowe, C. Impact of the Medicare Chronic Disease Management program on the conduct of Australian dietitians’ private practices. Aust. Heal. Rev. 2015, 39, 183–189. [Google Scholar] [CrossRef]
- Rollo, M.E.; Hutchesson, M.J.; Burrows, T.L.; Krukowski, R.A.; Harvey, J.R.; Hoggle, L.B.; Collins, C.E. Video Consultations and Virtual Nutrition Care for Weight Management. J. Acad. Nutr. Diet. 2015, 115, 1213–1225. [Google Scholar] [CrossRef]
- Jones, A.; Mitchell, L.J.; O’Connor, R.; Rollo, M.E.; Slater, K.; Williams, L.T.; Ball, L.; Chen, J.; Pankomera, R. Investigating the Perceptions of Primary Care Dietitians on the Potential for Information Technology in the Workplace: Qualitative Study. J. Med Internet Res. 2018, 20, e265. [Google Scholar] [CrossRef]
- O’Connor, R.; Slater, K.; Ball, L.; Jones, A.; Mitchell, L.J.; Rollo, M.E.; Williams, L.T. The tension between efficiency and effectiveness: A study of dietetic practice in primary care. J. Hum. Nutr. Diet. 2019, 32, 259–266. [Google Scholar] [CrossRef]
- Kicklighter, J.R.; Dorner, B.; Hunter, A.M.; Kyle, M.; Prescott, M.P.; Roberts, S.; Spear, B.; Hand, R.K.; Byrne, C. Visioning Report 2017: A Preferred Path Forward for the Nutrition and Dietetics Profession. J. Acad. Nutr. Diet. 2017, 117, 110–127. [Google Scholar] [CrossRef]
- Hales, S.; Dunn, C.; Wilcox, S.; Turner-McGrievy, G.M. Is a Picture Worth a Thousand Words? Few Evidence-Based Features of Dietary Interventions Included in Photo Diet Tracking Mobile Apps for Weight Loss. J. Diabetes Sci. Technol. 2016, 10, 1399–1405. [Google Scholar] [CrossRef]
- Zhou, L.; Zhang, C.; Liu, F.; Qiu, Z.; He, Y. Application of Deep Learning in Food: A Review. Compr. Rev. Food Sci. Food Saf. 2019, 18, 1793–1811. [Google Scholar] [CrossRef]
- Lee, K.; Hoti, K.; Hughes, J.D.; Emmerton, L.M. Consumer Use of “Dr Google”: A Survey on Health Information-Seeking Behaviors and Navigational Needs. J. Med Internet Res. 2015, 17, e288. [Google Scholar] [CrossRef]
- Forster, H.; Walsh, M.C.; O’Donovan, C.B.; Woolhead, C.; McGirr, C.; Daly, E.J.; O’Riordan, R.; Celis-Morales, C.; Fallaize, R.; Macready, A.L.; et al. A Dietary Feedback System for the Delivery of Consistent Personalized Dietary Advice in the Web-Based Multicenter Food4Me Study. J. Med Internet Res. 2016, 18, e150. [Google Scholar] [CrossRef] [PubMed]
- Fallaize, R.; Franco, R.Z.; Hwang, F.; Lovegrove, J.A. Evaluation of the eNutri automated personalised nutrition advice by users and nutrition professionals in the UK. PLoS ONE 2019, 14, e0214931. [Google Scholar] [CrossRef] [PubMed]
- Brain, K.; Burrows, T.L.; Rollo, M.E.; Hayes, C.; Hodson, F.J.; Collins, C.E. The Effect of a Pilot Dietary Intervention on Pain Outcomes in Patients Attending a Tertiary Pain Service. Nutrients 2019, 11, 181. [Google Scholar] [CrossRef] [PubMed]
- Haslam, R.L.; Pezdirc, K.; Truby, H.; Attia, J.; Hutchesson, M.J.; Burrows, T.; Callister, R.; Hides, L.; Bonevski, B.; Kerr, D.A.; et al. Investigating the Efficacy and Cost-Effectiveness of Technology-Delivered Personalized Feedback on Dietary Patterns in Young Australian Adults in the Advice, Ideas, and Motivation for My Eating (Aim4Me) Study: Protocol for a Randomized Controlled Trial. JMIR Res. Protoc. 2020, 9, e15999. [Google Scholar] [CrossRef] [PubMed]
- Subar, A.F.; Freedman, L.S.; Tooze, J.A.; Kirkpatrick, S.I.; Boushey, C.J.; Neuhouser, M.L.; Thompson, F.E.; Potischman, N.; Guenther, P.M.; Tarasuk, V.; et al. Addressing Current Criticism Regarding the Value of Self-Report Dietary Data. J. Nutr. 2015, 145, 2639–2645. [Google Scholar] [CrossRef] [PubMed]
- Kirkpatrick, S.I.; Collins, C.E.; Keogh, R.; Krebs-Smith, S.M.; Neuhouser, M.L.; Wallace, A. Assessing Dietary Outcomes in Intervention Studies: Pitfalls, Strategies, and Research Needs. Nutrients 2018, 10, 1001. [Google Scholar] [CrossRef]
| Variables | Mean (SD) or Count (%) | |
|---|---|---|
| HiP Group (n = 26) | LoP Group (n = 24) | |
| Sex | ||
| Female | 23 (88.5%) | 20 (83.3%) |
| Male | 3 (11.5%) | 4 (16.7%) |
| Age (years) | 37.3 (11.6) | 41.3 (13.2) |
| Height (m) | 1.7 (0.1) | 1.7 (0.1) |
| Weight (kg) | 71.8 (15.9) | 75.2 (18.5) |
| BMI (kg/m2) | 25.6 (5.0) | 27.3 (6.9) |
| Born in Australia | 20 (76.9%) | 18 (75.0%) |
| Highest Level of Education Obtained | ||
| High School Certificate (Year 10/ Year 12) | 3 (11.5%) | 2 (8.3%) |
| Diploma or Certificate | 4 (15.4%) | 3 (12.5%) |
| Bachelors degree | 7 (26.9%) | 6 (25.0%) |
| Postgraduate degree | 12 (46.2%) | 13 (54.2%) |
| Employment status | ||
| Full-time | 8 (30.8%) | 13 (54.2%) |
| Part-time | 9 (34.6%) | 6 (25.0%) |
| Casual or other type of work | 5 (19.2%) | 2 (8.3%) |
| Not currently in paid employment | 1 (3.8%) | 2 (8.3%) |
| Student | 3 (11.5%) | 1 (4.2%) |
| Income (Individual Level) | ||
| ≤$41,599/year | 11 (42.3%) | 6 (25.0%) |
| $41,600–$77,999/year | 8 (30.8%) | 5 (20.8%) |
| ≥$78,000/year | 6 (23.1%) | 10 (41.7%) |
| Not reported | 1 (3.8%) | 3 (12.5%) |
| Martial Status | ||
| Married or living with a partner | 16 (61.5%) | 15 (62.5%) |
| Divorced | 2 (7.7%) | 2 (8.3%) |
| Never married | 8 (30.8%) | 7 (29.2%) |
| eHEALS [26] (out of 40) | 29.8 (5.1) | 29.8 (4.9) |
| Variables | Mean (SD) | |
|---|---|---|
| HiP Group (n = 26) | LoP Group (n = 24) | |
| ARFS: overall (out of 73) | 36.0 (10.0) | 36.8 (9.1) |
| ARFS: vegetable sub-scale (out of 21) | 14.6 (4.3) | 14.7 (4.7) |
| ARFS: fruit sub-scale (out of 12) | 5.9 (2.9) | 5.9 (3.0) |
| ARFS: Meat, fish, poultry and other flesh foods (out of 7) | 2.7 (1.3) | 2.7 (1.5) |
| ARFS: vegetarian protein sources (out of 6) | 2.4 (1.8) | 2.8 (1.0) |
| ARFS: grains, breads and cereals (out of 13) | 5.2 (2.0) | 5.4 (2.1) |
| ARFS: dairy (out of 11) | 3.8 (2.1) | 3.9 (1.7) |
| ARFS: sauces and spreads (out of 2) | 0.8 (0.7) | 0.6 (0.7) |
| ARFS: water (out of 1) | 0.6 (0.5) | 0.8 (0.4) |
| Proportion of energy intake from Core Foods (%) | 64.7 (11.8) | 69.1 (13.5) |
| Proportion of energy intake from Non-Core Foods (%) | 35.3 (11.8) | 30.9 (13.5) |
| Proportion of energy intake from protein (%) | 19.4 (4.0) | 19.0 (3.0) |
| Proportion of energy intake from carbohydrates (%) | 43.5 (7.3) | 41.7 (6.1) |
| Proportion of energy intake from fats (%) | 34.9 (5.2) | 35.7 (5.1) |
| Proportion of energy intake from saturated fats (%) | 14.3 (3.3) | 14.1 (3.7) |
| Proportion of energy intake from alcohol (%) | 2.3 (3.9) | 3.6 (5.7) |
| Variables | HiP Group within-Group Difference | LoP Group within-Group Difference | Between-Group Difference | Group × Time | |||
|---|---|---|---|---|---|---|---|
| Mean (95%CI) | p-Value | Mean (95%CI) | p-Value | Mean (95% CI) | Sig | p-Value | |
| ARFS: overall (out of 73) | 5.0 (2.1 to 8) | 0.001 | −0.6 (−3.7 to 2.6) | 0.71 | 5.6 (1.3 to 10) | 0.01 | 0.01 |
| ARFS: vegetable sub-scale (out of 21) | 1.5 (0.1 to 3) | 0.04 | −0.2 (−1.7 to 1.4) | 0.82 | 1.7 (−0.4 to 3.9) | 0.11 | 0.11 |
| ARFS: fruit sub-scale (out of 12) | 0.5 (−0.4 to 1.5) | 0.28 | 0.8 (−0.2 to 1.9) | 0.12 | −0.3 (−1.7 to 1.2) | 0.69 | 0.69 |
| ARFS: Meat, fish, poultry and other flesh foods (out of 7) 1 | 0.7 (0.2 to 1.2) | 0.004 | −0.2 (−0.7 to 0.3) | 0.34 | 0.9 (0.2 to 1.6) | 0.01 | 0.01 |
| ARFS: vegetarian protein sources (out of 6) | 0.4 (0 to 0.8) | 0.06 | −0.4 (−0.8 to 0.1) | 0.13 | 0.8 (0.1 to 1.4) | 0.021 | 0.02 |
| ARFS: grains, breads and cereals (out of 13) 1 | 0.8 (−0.1 to 1.7) | 0.10 | −0.5 (−1.4 to 0.5) | 0.31 | 1.3 (−0.1 to 2.6) | 0.06 | 0.06 |
| ARFS: dairy (out of 11) | 1.2 (0.5 to 1.9) | 0.001 | −0.1 (−0.8 to 0.6) | 0.78 | 1.3 (0.3 to 2.3) | 0.01 | 0.01 |
| ARFS: sauces and spreads (out of 2) | −0.2 (−0.5 to 0.1) | 0.12 | −0.2 (−0.5 to 0.1) | 0.13 | 0.0 (−0.4 to 0.4) | 0.99 | 0.99 |
| ARFS: water (out of 1) 1 | 0.8 (−0.1 to 0.2) | 0.26 | −0.1 (−0.2 to 0.1) | 0.45 | 0.1 (−0.1 to 0.3) | 0.19 | 0.19 |
| Proportion of energy intake from Core Foods (%) 1 | 11.7 (7.2 to 16.2) | 0.001 | 4.5 (−0.3 to 9.3) | 0.07 | 7.2 (0.5 to 13.8) | 0.04 | 0.03 |
| Proportion of energy intake from Non-Core Foods (%) 1 | −11.7 (−16.2 to −7.2) | 0.001 | −4.5 (−9.3 to 0.3) | 0.65 | −7.2 (−13.8 to −0.5) | 0.04 | 0.03 |
| Proportion of energy intake from protein (%) 1 | 1.7 (0.7 to 2.8) | 0.001 | 0.9 (−0.2 to 2) | 0.10 | 0.8 (−0.7 to 2.3) | 0.30 | 0.30 |
| Proportion of energy intake from carbohydrates (%) 1 | −1.6 (−3.8 to 0.6) | 0.16 | 0.1 (−2.3 to 2.4) | 0.94 | −1.7 (−4.9 to 1.6) | 0.31 | 0.31 |
| Proportion of energy intake from fats (%) | −0.5 (−2.3 to 1.2) | 0.56 | −0.8 (−2.7 to 1) | 0.38 | 0.3 (−2.3 to 2.9) | 0.81 | 0.81 |
| Proportion of energy intake from saturated fats (%) | −0.8 (−1.7 to 0.2) | 0.11 | −0.9 (−1.9 to 0.1) | .08 | 0.1 (−1.3 to 1.5) | 0.85 | 0.85 |
| Proportion of energy intake from alcohol (%) 1 | −0.2 (−0.8 to 0.4) | 0.55 | −0.6 (−1.3 to 0) | .06 | 0.4 (−0.5 to 1.3) | 0.32 | 0.32 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rollo, M.E.; Haslam, R.L.; Collins, C.E. Impact on Dietary Intake of Two Levels of Technology-Assisted Personalized Nutrition: A Randomized Trial. Nutrients 2020, 12, 3334. https://doi.org/10.3390/nu12113334
Rollo ME, Haslam RL, Collins CE. Impact on Dietary Intake of Two Levels of Technology-Assisted Personalized Nutrition: A Randomized Trial. Nutrients. 2020; 12(11):3334. https://doi.org/10.3390/nu12113334
Chicago/Turabian StyleRollo, Megan E., Rebecca L. Haslam, and Clare E. Collins. 2020. "Impact on Dietary Intake of Two Levels of Technology-Assisted Personalized Nutrition: A Randomized Trial" Nutrients 12, no. 11: 3334. https://doi.org/10.3390/nu12113334
APA StyleRollo, M. E., Haslam, R. L., & Collins, C. E. (2020). Impact on Dietary Intake of Two Levels of Technology-Assisted Personalized Nutrition: A Randomized Trial. Nutrients, 12(11), 3334. https://doi.org/10.3390/nu12113334





