Changes in Age at Diagnosis and Nutritional Course of Celiac Disease in the Last Two Decades
Abstract
1. Introduction
2. Materials and Methods
3. Results
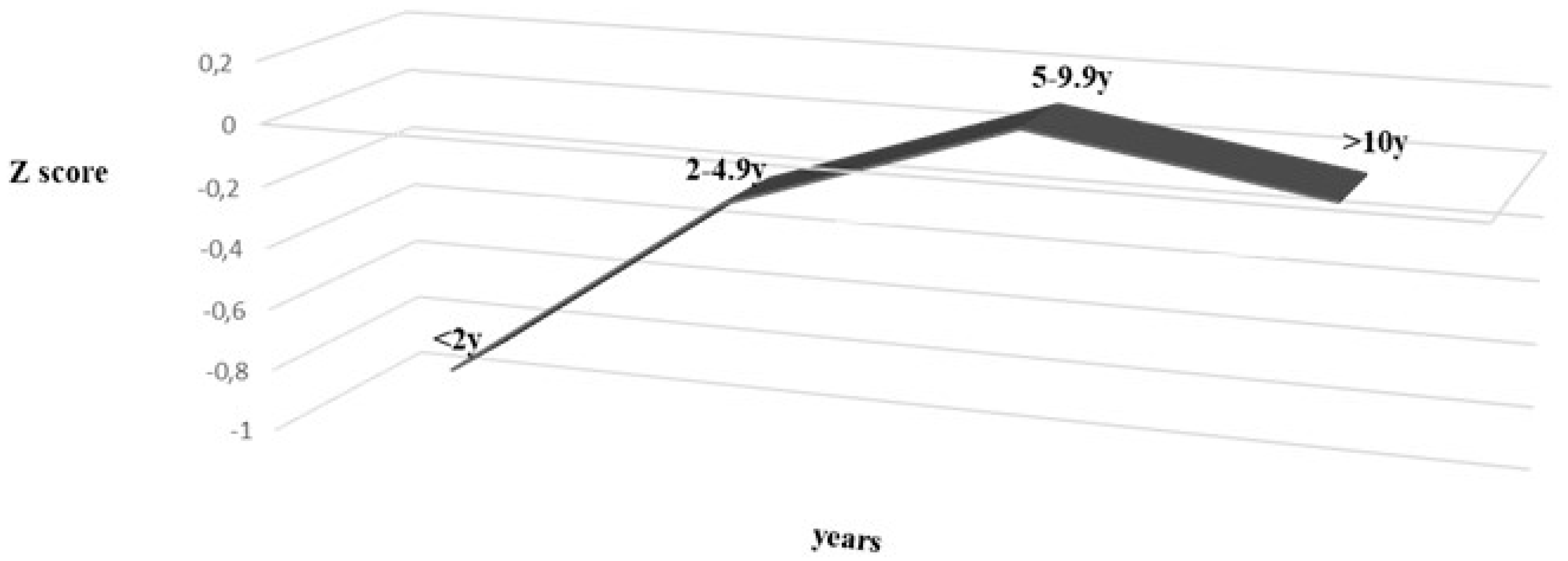
3.1. At Diagnosis
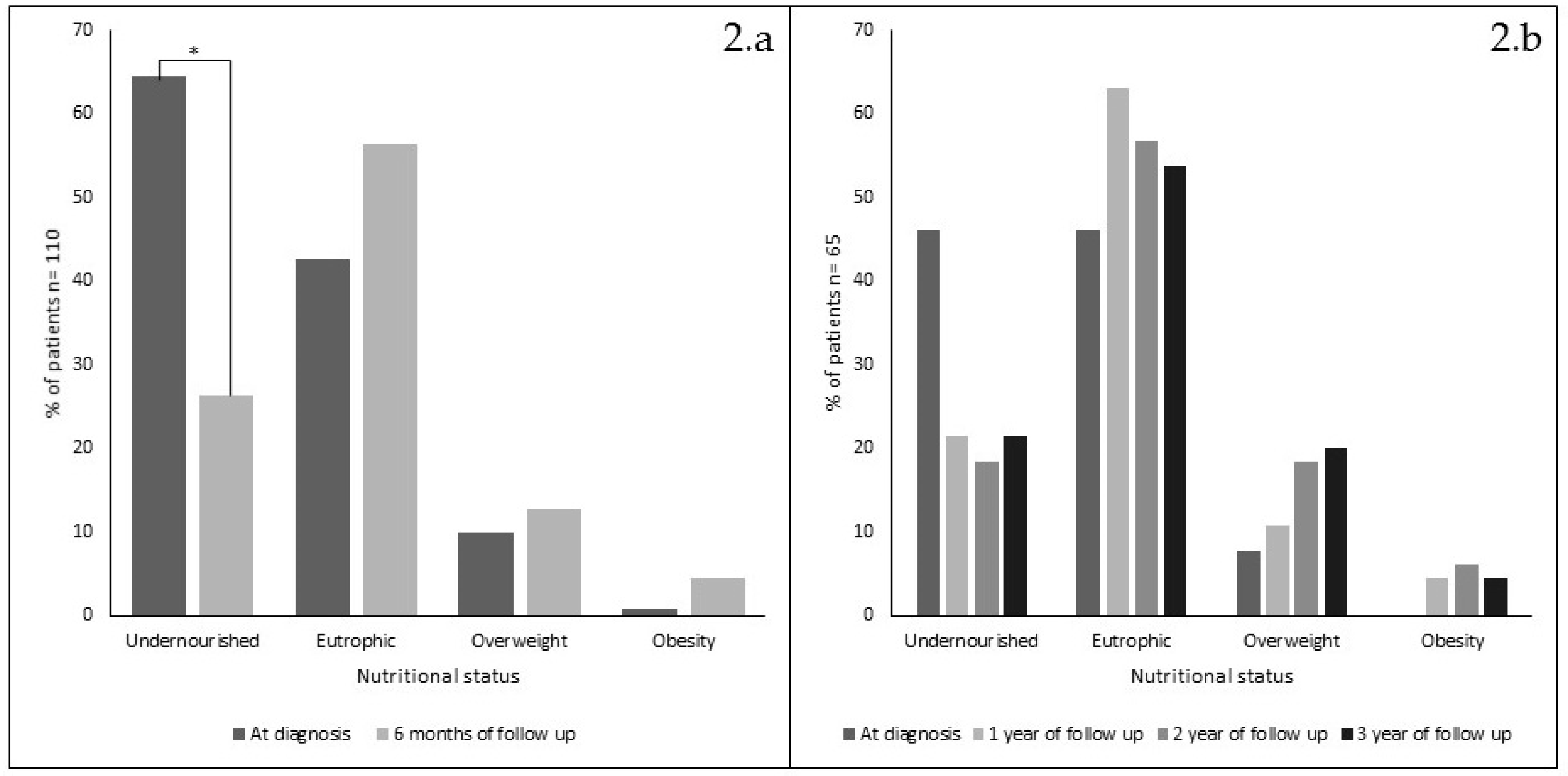
3.2. Nutritional Changes during Follow Up on GFD
4. Discussion
4.1. Frequency of Diagnosis and Clinical Characteristics
4.2. Clinical Characteristics
4.3. Nutritional Status
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Green, P.H.; Jabri, B. Coeliac disease. Lancet 2003, 362, 383–391. [Google Scholar] [CrossRef]
- Lebwohl, B.; Sanders, D.S.; Green, P.H.R. Coeliac disease. Lancet 2018, 391, 70–81. [Google Scholar] [CrossRef]
- Ng, M.; Fleming, T.; Robinson, M.; Thomson, B.; Graetz, N.; Margono, C.; Mullany, E.C.; Biryukov, S.; Abbafati, C.; Abera, S.F.; et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: A systematic analysis for the Global Burden of Disease Study 2013. Lancet 2014, 384, 766–781. [Google Scholar] [CrossRef]
- Dickey, W.; Kearney, N. Overweight in celiac disease: Prevalence, clinical characteristics, and effect of a gluten-free diet. Am. J. Gastroenterol. 2006, 101, 2356–2359. [Google Scholar] [CrossRef]
- Diamanti, A.; Capriati, T.; Basso, M.S.; Panetta, F.; Di Ciommo Laurora, V.M.; Bellucci, F.; Cristofori, F.; Francavilla, R. Celiac disease and overweight in children: An update. Nutrients 2014, 6, 207–220. [Google Scholar] [CrossRef]
- Schilling, K.W.; Yohannessen, K.; Araya, M. Perception of following gluten-free diet and adherence to treatment in pediatric patients with celiac disease. Rev. Chil. Pediatr. 2018, 89, 216–223. [Google Scholar] [CrossRef]
- Statistics MoHNIo. National Health Survey (ENS) 2016–2017; Ministerio de Salud: Santiago, Chile, 2018. [Google Scholar]
- Araya, M.; Mondragon, A.; Perez-Bravo, F.; Roessler, J.L.; Alarcon, T.; Rios, G.; Bergenfreid, C. Celiac disease in a Chilean population carrying Amerindian traits. J. Pediatric Gastroenterol. Nutr. 2000, 31, 381–386. [Google Scholar] [CrossRef] [PubMed]
- Botero-Lopez, J.E.; Araya, M.; Parada, A.; Mendez, M.A.; Pizarro, F.; Espinosa, N.; Canales, P.; Alarcon, T. Micronutrient deficiencies in patients with typical and atypical celiac disease. J. Pediatric Gastroenterol. Nutr. 2011, 53, 265–270. [Google Scholar] [CrossRef] [PubMed]
- Parada, A.; Araya, M.; Perez-Bravo, F.; Mendez, M.; Mimbacas, A.; Motta, P.; Martin, G.; Botero, J.; Espinosa, N.; Alarcon, T.; et al. Amerindian mtDNA haplogroups and celiac disease risk HLA haplotypes in mixed-blood Latin American patients. J. Pediatric Gastroenterol. Nutr. 2011, 53, 429–434. [Google Scholar] [CrossRef] [PubMed]
- Roessler, J.L.; Rios, G.; Alarcon, T.; Bergenfreid, C.; Mondragon, A.; Araya, M. Celiac disease in adolescents and young adults. A challenge for gastroenterologists of children and adults. Rev. Med. Chil. 2001, 129, 743–748. [Google Scholar] [PubMed]
- Araya, M.; Diaz, J.; Oyarzun, A.; Lucero, Y.; Alarcon, T.; Gonzalez, M.; Canales, P.; Fierro, L.; Perez-Bravo, F. Avoiding Small Intestinal Biopsies for Diagnosis of Celiac Disease in Children: A Reliable Strategy for All Patients? J. Pediatric Gastroenterol. Nutr. 2018, 66, 785–788. [Google Scholar] [CrossRef] [PubMed]
- Marsh, M.N. The immunopathology of the small intestinal reaction in gluten-sensitivity. Immunol. Investig. 1989, 18, 509–531. [Google Scholar] [CrossRef] [PubMed]
- Chile MdSd. Patrones de crecimiento para evaluación nutriconal de niños, niñas y adolescentes desde el nacimineto hasta los 18 años de edad. 2018. [Google Scholar]
- WHO. Anthro Para Computadoras Personales, versión 3.2.2; Software Para Evaluar el Crecimiento y Desarrollo de Los Niños Del Mundo; WHO: Brasilia, Brasil, 2011. [Google Scholar]
- Ginebra, W. Anthro Plus, versión 1.0.4; WHO: Brasilia, Brasil, 2018. [Google Scholar]
- Dicke, W.K.; Weijers, H.A.; van de Kamer, J.H. Celiac disease-11. The presence in wheat of a factor having a deleterious effect in cases of celiac disease. Acta Pediatrica 1953, 42, 34–42. [Google Scholar] [CrossRef] [PubMed]
- Dicke, W.K. Coeliac Disease. Investigation of the Harmful Effects of Certain Types of Cereal on Patients with Coeliac Disease. Thesis (M.D.), University of Utrecht, Utrecht, The Netherlands, 1950. [Google Scholar]
- Husby, S.; Koletzko, S.; Korponay-Szabo, I.R.; Mearin, M.L.; Phillips, A.; Shamir, R.; Troncone, R.; Giersiepen, K.; Branski, D.; Catassi, C.; et al. European Society for Pediatric Gastroenterology, Hepatology, and Nutrition guidelines for the diagnosis of coeliac disease. J. Pediatric Gastroenterol. Nutr. 2012, 54, 136–160. [Google Scholar] [CrossRef] [PubMed]
- Silvester, J.A.; Kurada, S.; Szwajcer, A.; Kelly, C.P.; Leffler, D.A.; Duerksen, D.R. Tests for Serum Transglutaminase and Endomysial Antibodies Do Not Detect Most Patients with Celiac Disease and Persistent Villous Atrophy on Gluten-free Diets: A Meta-analysis. Gastroenterology 2017, 153, 689–701. [Google Scholar] [CrossRef] [PubMed]
- Canales, P.R.; Magdalena, A.Q.; Alliende, F.; Hunter, B.; Alarcón, T.; Chávez, E. Estado actual del diagnóstico y presentaciones clínicas de enfermedad celíaca. Estudio multicéntrico. Rev. Méd. Chile 2008, 136, 8. [Google Scholar] [CrossRef]
- Oliveira, G.N.; Mohan, R.; Fagbemi, A. Review of Celiac Disease Presentation in a Pediatric Tertiary Centre. Arq. Gastroenterol. 2018, 55, 86–93. [Google Scholar] [CrossRef]
- Kang, J.Y.; Kang, A.H.; Green, A.; Gwee, K.A.; Ho, K.Y. Systematic review: Worldwide variation in the frequency of coeliac disease and changes over time. Aliment. Pharmacol. Ther. 2013, 38, 226–245. [Google Scholar] [CrossRef]
- Reilly, N.R.; Aguilar, K.; Hassid, B.G.; Cheng, J.; Defelice, A.R.; Kazlow, P.; Bhagat, G.; Green, P.H. Celiac disease in normal-weight and overweight children: Clinical features and growth outcomes following a gluten-free diet. J. Pediatric Gastroenterol. Nutr. 2011, 53, 528–531. [Google Scholar] [CrossRef]
- Venkatasubramani, N.; Telega, G.; Werlin, S.L. Obesity in pediatric celiac disease. J. Pediatric Gastroenterol. Nutr. 2010, 51, 295–297. [Google Scholar] [CrossRef]
- Araya, M.; Oyarzun, A.; Lucero, Y.; Espinosa, N.; Perez-Bravo, F. DQ2, DQ7 and DQ8 Distribution and Clinical Manifestations in Celiac Cases and Their First-Degree Relatives. Nutrients 2015, 7, 4955–4965. [Google Scholar] [CrossRef] [PubMed]
- Mansueto, P.; Soresi, M.; La Blasca, F.; Fayer, F.; D’Alcamo, A.; Carroccio, A. Body Mass Index and Associated Clinical Variables in Patients with Non-Celiac Wheat Sensitivity. Nutrients 2019, 11. [Google Scholar] [CrossRef] [PubMed]
- Bhattacharya, M.; Kapoor, S.; Dubey, A.P. Celiac disease presentation in a tertiary referral centre in India: Current scenario. Indian J. Gastroenterol. 2013, 32, 98–102. [Google Scholar] [CrossRef] [PubMed]
- Brambilla, P.; Picca, M.; Dilillo, D.; Meneghin, F.; Cravidi, C.; Tischer, M.C.; Vivaldo, T.; Bedogni, G.; Zuccotti, G.V. Changes of body mass index in celiac children on a gluten-free diet. Nutr. Metab. Cardiovasc. Dis. 2013, 23, 177–182. [Google Scholar] [CrossRef] [PubMed]
- Valletta, E.; Fornaro, M.; Cipolli, M.; Conte, S.; Bissolo, F.; Danchielli, C. Celiac disease and obesity: Need for nutritional follow-up after diagnosis. Eur. J. Clin. Nutr. 2010, 64, 1371–1372. [Google Scholar] [CrossRef]
- Chile MdSd. Segunda Encuesta Nacioanl de Salud. Available online: https://www.minsal.cl/portal/url/item/bcb03d7bc28b64dfe040010165012d23.pdf (accessed on 3 December 2019).
- (JUNAEB), JdAEyB. Mapa Nutricional Infantil. Available online: https://www.junaeb.cl/wp-content/uploads/2013/03/MapaNutricional_2018.pdf (accessed on 3 December 2019).
- Caio, G.; Volta, U.; Sapone, A.; Leffler, D.A.; De Giorgio, R.; Catassi, C.; Fasano, A. Celiac disease: A comprehensive current review. BMC Med. 2019, 17, 142. [Google Scholar] [CrossRef]
- Volta, U.; Caio, G.; Stanghellini, V.; De Giorgio, R. The changing clinical profile of celiac disease: A 15-year experience (1998-2012) in an Italian referral center. BMC Gastroenterol. 2014, 14, 194. [Google Scholar] [CrossRef]
| Period A 1994–2001 (n = 15/155) mean ± SD | Period B 2002–2009 (n = 42/155) mean ± SD | Period C 2010–2017 (n = 98/155) mean ± SD | Total (n = 155) mean ± SD | p * | |
|---|---|---|---|---|---|
| Age at diagnosis (y) | 1.9 ±1.2 | 5.1 ± 3,8 | 5.7 ±4,3 | 5.1 ± 3.6 | 0.003 |
| Sex. Girls, n(%) | 10 (66.7%) | 27 (64.3%) | 63 (64.3%) | 100 (64.5%) | 0.983 |
| Gastrointestinal symptoms, n (%) | 0.090 | ||||
| Diarrhea | 12(80) | 17 (40.5) | 57 (58.1) | 86 (55.4%) | |
| Vomiting | 4 (26.7) | 10 (2.4) | 18 (18.4) | 32 (20.65%) | |
| Abdominal pain | 1 (6.7) | 5 (11.9) | 28 (28.6) | 34 (21.94%) | |
| Abdominal distension | 7 (46.7) | 9 (21.4) | 33 (33.7) | 49 (31.61%) | |
| Constipation | 0 (0.0) | 5 (11.9) | 18 (18.4) | 23 (14.84%) | |
| Total | 13 (86.7) | 26 (61.9) | 75 (76.5) | ||
| Extraintestinal symptoms, n (%) | |||||
| Failure to thrive | 9 (60) | 22 (52.3) | 32 (32.7) | 63(40.65%) | 0.020 |
| Short stature | 2 (13.3) | 8 (19.1) | 22 (22.5) | 32(20.65%) | |
| Anemia | 3 (20) | 8 (19.1) | 8 (8.2) | 19(12.26%) | |
| Wasted bottoms | 0 (0.0) | 4 (9.5) | 9 (9.1) | 13(8.39%) | |
| Irritability/Apathy | 2 (13.3) | 0 (0.0) | 4 (4.1) | 6(3.87%) | |
| Dermatitis Herpetiformis | 0 (0.0) | 0 (0.0) | 3 (3.1) | 3(1.94%) | 0.003 |
| Oral aphthae | 0 (0.0) | 0(0.0) | 2 (2.0) | 2(1.29%) | |
| Enamel hypoplasia | 0 (0.0) | 1 (2.4) | 1 (1.0) | 2(1.29%) | |
| Pubertal delay | 0(0.0) | 0 (0.0) | 1 (1.0) | 1(0.65%) | |
| Weakness | 0 (0.0) | 1 (2.4) | 0 (0.0) | 1(0.65%) | |
| Total | 13 (86.7) | 32 (76.2) | 58 (59.2) | ||
| Asymptomatic | 0 (0.0) | 2 (4.8) | 5 (5.1) | 7(4.52%) | |
| Presenting comorbidities | 1 (6.7) | 8 (19.1) | 24 (24.5) | 33(21.2%) | |
| Positive family history | 0 (0.0) | 8 (19.1) | 4 (4.1) | 12(7.74%) | |
| Belongs to risk group | 1 (6.7) | 7 (16.7) | 18 (18.4) | 26(16.7%) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Villanueva, M.; Oyarzún, A.; Leyton, B.; González, M.; Navarro, E.; Canales, P.; Ossa, C.; Muñoz, M.P.; Bascuñán, K.A.; Araya, M. Changes in Age at Diagnosis and Nutritional Course of Celiac Disease in the Last Two Decades. Nutrients 2020, 12, 156. https://doi.org/10.3390/nu12010156
Villanueva M, Oyarzún A, Leyton B, González M, Navarro E, Canales P, Ossa C, Muñoz MP, Bascuñán KA, Araya M. Changes in Age at Diagnosis and Nutritional Course of Celiac Disease in the Last Two Decades. Nutrients. 2020; 12(1):156. https://doi.org/10.3390/nu12010156
Chicago/Turabian StyleVillanueva, Mónica, Amaya Oyarzún, Bárbara Leyton, Mónica González, Elizabeth Navarro, Paulina Canales, Cristobal Ossa, María Paz Muñoz, Karla A. Bascuñán, and Magdalena Araya. 2020. "Changes in Age at Diagnosis and Nutritional Course of Celiac Disease in the Last Two Decades" Nutrients 12, no. 1: 156. https://doi.org/10.3390/nu12010156
APA StyleVillanueva, M., Oyarzún, A., Leyton, B., González, M., Navarro, E., Canales, P., Ossa, C., Muñoz, M. P., Bascuñán, K. A., & Araya, M. (2020). Changes in Age at Diagnosis and Nutritional Course of Celiac Disease in the Last Two Decades. Nutrients, 12(1), 156. https://doi.org/10.3390/nu12010156





