Obesity Stigma: Is the ‘Food Addiction’ Label Feeding the Problem?
Abstract
1. Introduction
2. Study 1 Method
2.1. Participants
2.2. Procedure
2.3. Measures
2.3.1. Target Specific Stigma: Modified Fat-Phobia Scale (M-FPS)
2.3.2. General Stigma: Anti-fat Attitudes (AFA)
2.3.3. Dutch Eating Behavior Scale (DEBQ)
2.3.4. Self-Perceived Food Addiction (SPFA)
2.3.5. Employability Questions
2.4. Data Analysis
3. Results
3.1. Participant Characteristics
3.2. Effect of Condition on Target-Specific and General Stigma
3.3. Moderating Effect of BMI
4. Interim Discussion
5. Study 2 Method
5.1. Participants
5.2. Materials and Procedure
5.2.1. Addiction Belief Scale (ABS)
5.2.2. Addiction-Like Eating Behaviour Scale (AEBS)
5.2.3. Data Analysis
6. Results
6.1. Participant Characteristics
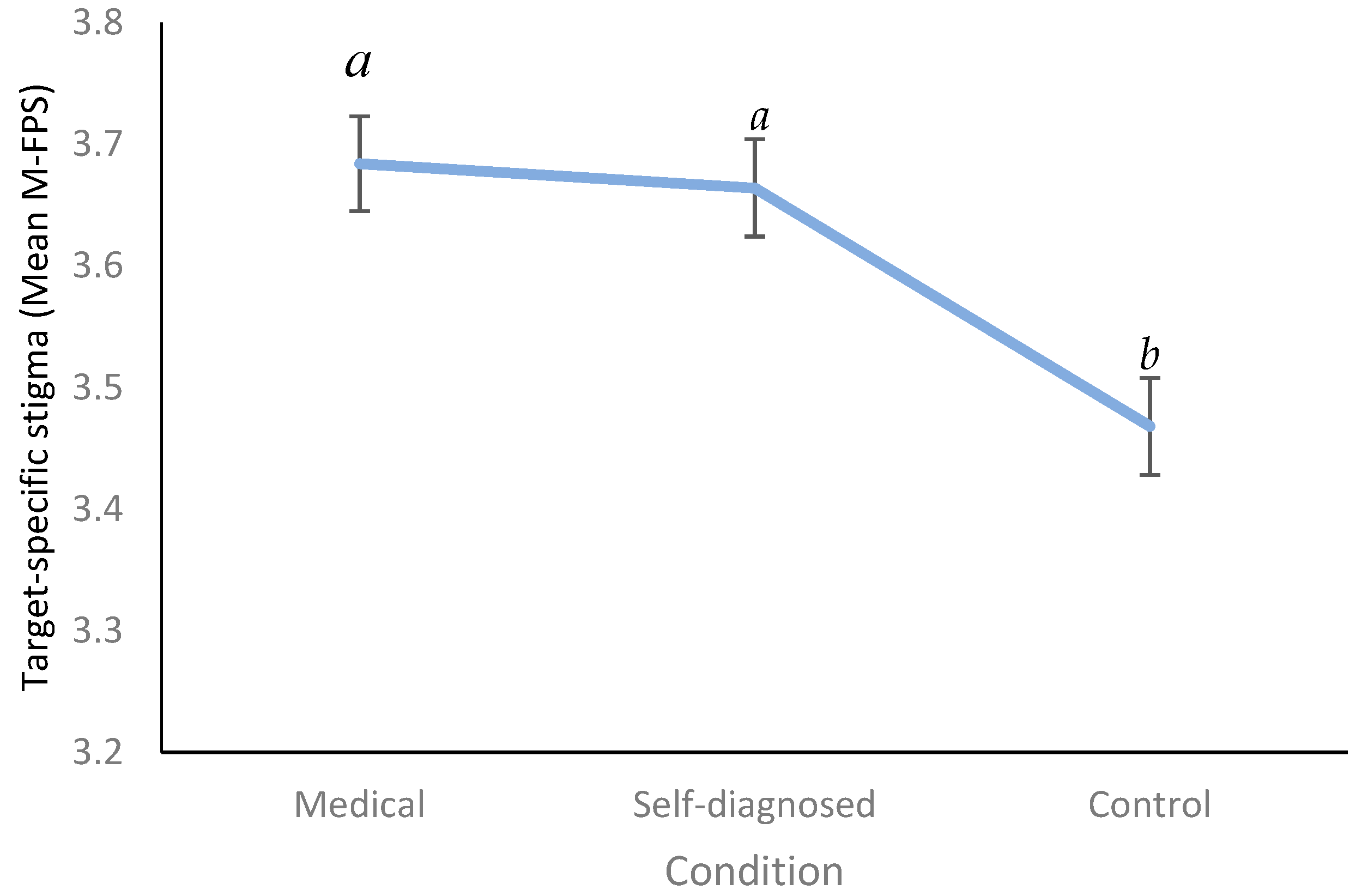
6.2. Effect of Condition and Gender on Target Specific Stigma
6.3. Effect of Condition and Gender on General Stigma
6.4. Effect of Disease Beliefs on Stigma
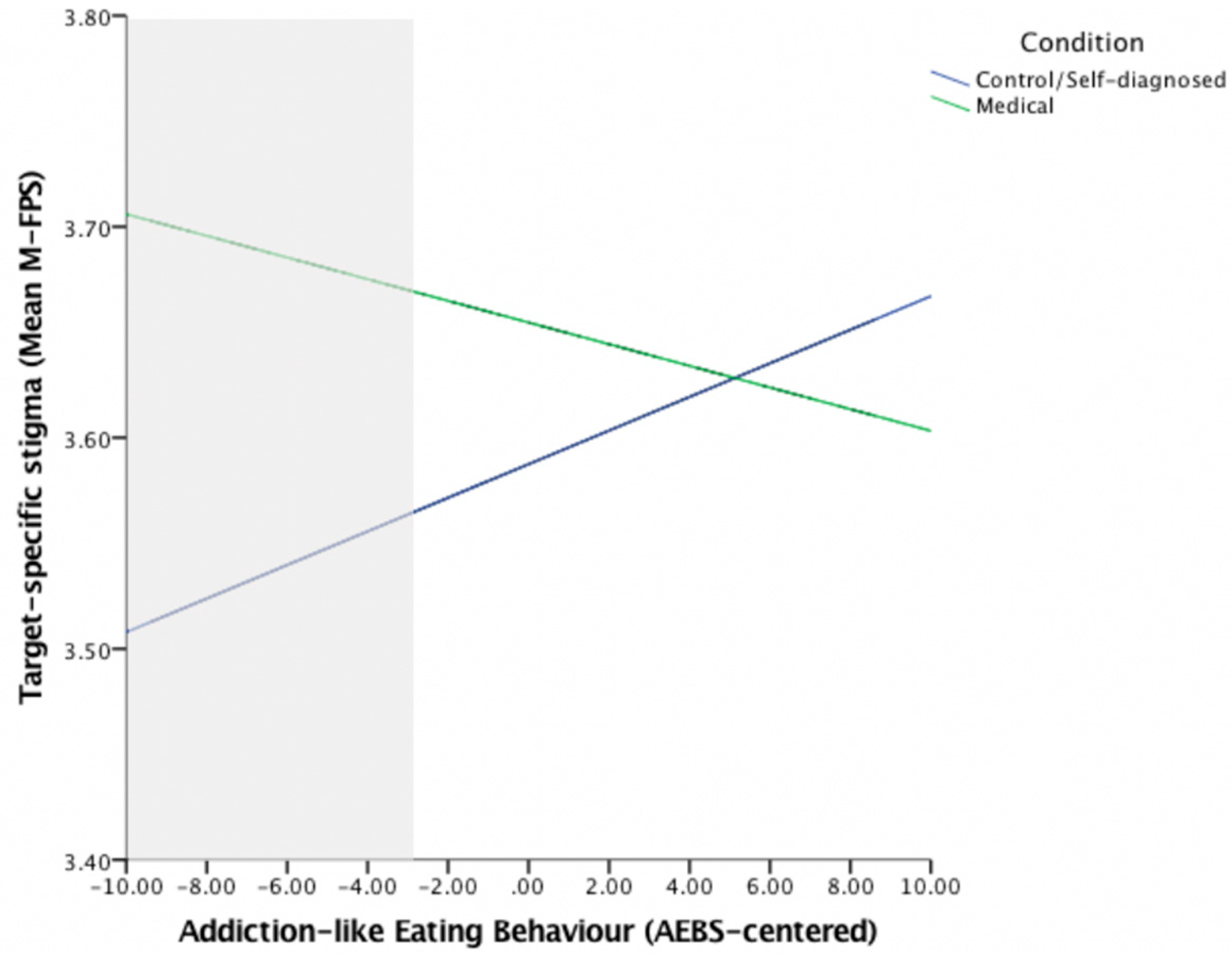
6.5. Addiction-Like Eating Behavior
7. Discussion
8. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- NHS Digital. Available online: Digital.nhs.uk/data-and-information/publications/statistical/sand-diet/statistics-on-obesity-physical-activity-and-diet-england-2019 (accessed on 27 June 2019).
- Puhl, R.M.; Heuer, C.A. The stigma of obesity: A review and update. Obesity 2009, 17, 941–964. [Google Scholar] [CrossRef] [PubMed]
- Brinsden, H.; Coltman-Patel, T.; Sievert, K. Weight Stigma in the Media. Available online: https://www.britishlivertrust.org.uk/wp-content/up (accessed on 27 June 2019).
- Pearl, R.L.; Wadden, T.A.; Hopkins, C.M.; Shaw, J.A.; Hayes, M.R.; Bakizada, Z.M.; Alfaris, N.; Chao, A.M.; Pinkasavage, E.; Berkowitz, R.I.; et al. Association between weight bias internalization and metabolic syndrome among treatment-seeking individuals with obesity. Obesity 2017, 25, 317–322. [Google Scholar] [CrossRef] [PubMed]
- Nolan, L.J.; Eshleman, A. Paved with good intentions: Paradoxical eating responses to weight stigma. Appetite 2016, 102, 15–24. [Google Scholar] [CrossRef] [PubMed]
- Rush, L.L. Affective reactions to multiple social stigmas. J. Soc. Psychol. 1998, 138, 421–430. [Google Scholar] [CrossRef]
- Weiner, B. An attributional theory of achievement motivation and emotion. Psychol. Rev. 1985, 92, 548–573. [Google Scholar] [CrossRef] [PubMed]
- Crandall, C.S. Prejudice against fat people: Ideology and self-interest. J. Personal. Soc. Psychol. 1994, 66, 882–894. [Google Scholar] [CrossRef]
- Pearl, R.L.; Lebowitz, M.S. Beyond personal responsibility: Effects of causal attributions for overweight and obesity on weight-related beliefs, stigma, and policy support. Psychol. Health 2014, 29, 1176–1191. [Google Scholar] [CrossRef]
- Hilbert, A.; Rief, W.; Braehler, E. Stigmatizing attitudes toward obesity in a representative population-based sample. Obesity 2008, 16, 1529–1534. [Google Scholar] [CrossRef]
- Teachman, B.A.; Gapinski, K.D.; Brownell, K.D.; Rawlins, M.; Jeyaram, S. Demonstrations of implicit anti-fat bias: The impact of providing causal information and evoking empathy. Health Psychol. 2003, 22, 68–78. [Google Scholar] [CrossRef]
- Lewis, R.J.; Cash, T.F.; Jacobi, L.; Bubb-Lewis, C. Prejudice toward fat people: The development and validation of the antifat attitudes test. Obes. Res. 1997, 5, 297–307. [Google Scholar] [CrossRef]
- Dejong, W. The stigma of obesity: The consequences of naive assumptions concerning the causes of physical deviance. J. Health Soc. Behav. 1980, 21, 75–87. [Google Scholar] [CrossRef] [PubMed]
- Lerma-Cabrera, J.M.; Carvajal, F.; Lopez-Legarrea, P. Food addiction as a new piece of the obesity framework. Nutr. J. 2016, 15, 5. [Google Scholar] [CrossRef]
- Schulte, E.M.; Avena, N.M.; Gearhardt, A.N. Which foods may be addictive? The roles of processing, fat content, and glycemic load. PLoS ONE 2015, 10, e0117959. [Google Scholar] [CrossRef]
- Schulte, E.M.; Grilo, C.M.; Gearhardt, A.N. Shared and unique mechanisms underlying binge eating disorder and addictive disorders. Clin. Psychol. Rev. 2016, 44, 125–139. [Google Scholar] [CrossRef] [PubMed]
- Rogers, P.J. Food and drug addictions: Similarities and differences. Pharmacol. Biochem. Behav. 2017, 153, 182–190. [Google Scholar] [CrossRef]
- Ziauddeen, H.; Farooqi, I.S.; Fletcher, P.C. Obesity and the brain: How convincing is the addiction model? Nat. Rev. Neurosci. 2012, 13, 279–286. [Google Scholar] [CrossRef] [PubMed]
- Hebebrand, J.; Albayrak, Ö.; Adan, R.; Antel, J.; Dieguez, C.; de Jong, J.; Leng, G.; Menzies, J.; Mercer, J.G.; Murphy, M.; et al. “Eating addiction”, rather than “food addiction”, better captures addictive-like eating behavior. Neurosci. Biobehav. Rev. 2014, 47, 295–306. [Google Scholar] [CrossRef] [PubMed]
- Ruddock, H.K.; Hardman, C.A. Food addiction beliefs amongst the lay public: What are the consequences for eating behaviour? Curr. Addict. Rep. 2017, 4, 110–115. [Google Scholar] [CrossRef]
- Lee, N.M.; Lucke, J.; Hall, W.D.; Meurk, C.; Boyle, F.M.; Carter, A. Public views on food addiction and obesity: Implications for policy and treatment. PLoS ONE 2013, 8, e74836. [Google Scholar] [CrossRef]
- Meadows, A.; Nolan, L.J.; Higgs, S. Self-perceived food addiction: Prevalence, predictors, and prognosis. Appetite 2017, 114, 282–298. [Google Scholar] [CrossRef]
- Ruddock, H.K.; Dickson, J.M.; Field, M.; Hardman, C.A. Eating to live or living to eat? Exploring the causal attributions of self-perceived food addiction. Appetite 2015, 95, 262–268. [Google Scholar] [CrossRef] [PubMed]
- Hardman, C.A.; Rogers, P.J.; Dallas, R.; Scott, J.; Ruddock, H.; Robinson, E. “Food addiction is real”: The effects of exposure to this message on self-diagnosed food addiction and eating behaviour. Appetite 2015, 91, 179–184. [Google Scholar] [CrossRef] [PubMed]
- Reid, J.; Brien, K.S.O.; Puhl, R.; Hardman, C.A.; Carter, A. Food addiction and its potential links with weight stigma. Curr. Addict. Rep. 2018, 5, 192–201. [Google Scholar] [CrossRef]
- Cassin, S.E.; Buchman, D.Z.; Leung, S.E.; Kantarovich, K.; Hawa, A.; Carter, A.; Sockalingam, S. Ethical, stigma, and policy implications of food addiction: A scoping review. Nutrients 2019, 11, 710. [Google Scholar] [CrossRef] [PubMed]
- DePierre, J.A.; Puhl, R.M.; Luedicke, J. A new stigmatized identity? Comparisons of a “food addict” label with other stigmatized health conditions. Basic Appl. Soc. Psychol. 2013, 35, 10–21. [Google Scholar] [CrossRef]
- Latner, J.D.; Puhl, R.M.; Murakami, J.M.; O’Brien, K.S. Food addiction as a causal model of obesity. Effects on stigma, blame, and perceived psychopathology. Appetite 2014, 77, 77–82. [Google Scholar] [CrossRef] [PubMed]
- Cullen, A.J.; Barnett, A.; Komesaroff, P.A.; Brown, W.; O’Brien, K.S.; Hall, W.; Carter, A. A qualitative study of overweight and obese Australians’ views of food addiction. Appetite 2017, 115, 62–70. [Google Scholar] [CrossRef]
- Epstein, L.; Ogden, J. A qualitative study of GPs’ views of treating obesity. Br. J. Gen. Pract. 2005, 55, 750–754. [Google Scholar] [PubMed]
- Kvaale, E.P.; Haslam, N.; Gottdiener, W.H. The “side effects” of medicalization: A meta-analytic review of how biogenetic explanations affect stigma. Clin. Psychol. Rev. 2013, 33, 782–794. [Google Scholar] [CrossRef] [PubMed]
- Schulte, E.M.; Tuttle, H.M.; Gearhardt, A.N. Belief in food addiction and obesity-related policy support. PLoS ONE 2016, 11, e0147557. [Google Scholar] [CrossRef]
- Bacon, J.; Scheltema, K.; Robinson, B. Fat phobia scale revisited: The short form. Int. J. Obes. 2001, 25, 252. [Google Scholar] [CrossRef] [PubMed]
- Van Strien, T.; Frijters, J.E.R.; van Staveren, W.A.; Defares, P.B.; Deurenberg, P. The predictive validity of the Dutch restrained eating scale. Int. J. Eat. Disord. 1986, 5, 747–755. [Google Scholar] [CrossRef]
- Van Strien, T.; Bergers, G.P.A.; Defares, P.B. The Dutch eating behavior questionnaire (DEBQ) for assessment of restrained, emotional, and external eating behavior. Int. J. Eat. Disord. 1986, 5, 295–315. [Google Scholar] [CrossRef]
- Van Strien, T.; Peter Herman, C.; Anschutz, D. The predictive validity of the DEBQ-external eating scale for eating in response to food commercials while watching television. Int. J. Eat. Disord. 2012, 45, 257–262. [Google Scholar] [CrossRef] [PubMed]
- Oliver Georgina, L.; Wardle Jane, L.; Gibson, E.L. Stress and food choice: A laboratory study. Psychosom. Med. 2000, 62, 853–865. [Google Scholar] [CrossRef] [PubMed]
- Ruddock, H.K.; Field, M.; Hardman, C.A. Exploring food reward and calorie intake in self-perceived food addicts. Appetite 2017, 115, 36–44. [Google Scholar] [CrossRef] [PubMed]
- Schaler, J.A. The addiction belief scale. Int. J. Addict. 1995, 30, 117–134. [Google Scholar] [CrossRef]
- DePierre, J.A.; Puhl, R.M.; Luedicke, J. Public perceptions of food addiction: A comparison with alcohol and tobacco. J. Subst. Use 2014, 19, 1–6. [Google Scholar] [CrossRef]
- Cunningham, J.A.; Sobell, L.C.; Freedman, J.L.; Sobell, M.B. Beliefs about the causes of substance abuse: A comparison of three drugs. J. Subst. Abus. 1994, 6, 219–226. [Google Scholar] [CrossRef]
- O’Brien, K.S.; Puhl, R.M.; Latner, J.D.; Mir, A.S.; Hunter, J.A. Reducing anti-fat prejudice in preservice health students: A randomized trial. Obesity 2010, 18, 2138–2144. [Google Scholar] [CrossRef]
- Meurk, C.; Carter, A.; Partridge, B.; Lucke, J.; Hall, W. How is acceptance of the brain disease model of addiction related to Australians’ attitudes towards addicted individuals and treatments for addiction? BMC Psychiatry 2014, 14, 373. [Google Scholar] [CrossRef] [PubMed]
- Tajfel, H.; Turner, J. The Social Identity Theory of Intergroup Behaviour. U: Worchel S. i Austin WG (ur.) Psychology of Intergroup Relations; Nelson Hall: Chicago, IL, USA, 1986. [Google Scholar]
- Ruddock, H.K.; Christiansen, P.; Halford, J.C.G.; Hardman, C.A. The development and validation of the addiction-like eating behaviour scale. Int. J. Obes. 2017, 41, 1710. [Google Scholar] [CrossRef] [PubMed]
- Gormally, J.; Black, S.; Daston, S.; Rardin, D. The assessment of binge eating severity among obese persons. Addict. Behav. 1982, 7, 47–55. [Google Scholar] [CrossRef]
- Gearhardt, A.N.; Corbin, W.R.; Brownell, K.D. Preliminary validation of the Yale food addiction scale. Appetite 2009, 52, 430–436. [Google Scholar] [CrossRef] [PubMed]
- Alkharusi, H. Categorical variables in regression analysis: A comparison of dummy and effect coding. Int. J. Educ. 2012, 4, 202–210. [Google Scholar] [CrossRef]
- Johnson, P.O.; Neyman, J. Tests of certain linear hypotheses and their application to some educational problems. Stat. Res. Mem. 1936, 1, 57–93. [Google Scholar]
- Hayes, A.F.; Montoya, A.K. A tutorial on testing, visualizing, and probing an interaction involving a multicategorical variable in linear regression analysis. Commun. Methods Meas. 2017, 11, 1–30. [Google Scholar] [CrossRef]
- Hayes, A.F. Introduction to Mediation, Moderation, and Conditional Process Analysis; The Guildford Press: New York, NY, USA, 2017. [Google Scholar]
- Bannon, K.L.; Hunter-Reel, D.; Wilson, G.T.; Karlin, R.A. The effects of causal beliefs and binge eating on the stigmatization of obesity. Int. J. Eat. Disord. 2009, 42, 118–124. [Google Scholar] [CrossRef]
- Phelan, J.C. Genetic bases of mental illness—A cure for stigma? Trends Neurosci. 2002, 25, 430–431. [Google Scholar] [CrossRef]
- Phelan, J.C. Geneticization of deviant behavior and consequences for stigma: The case of mental illness. J. Health Soc. Behav. 2005, 46, 307–322. [Google Scholar] [CrossRef]
- Puhl, R.M.; Andreyeva, T.; Brownell, K.D. Perceptions of weight discrimination: Prevalence and comparison to race and gender discrimination in America. Int. J. Obes. 2008, 32, 992–1000. [Google Scholar] [CrossRef] [PubMed]
| Variable | Medical (N = 148) | Self-Diagnosed (N = 144) | Control (N = 146) | Between-Group Differences |
|---|---|---|---|---|
| Age (y) | 21.09 (±6.44) | 21.07 (±7.45) | 21.38 (±7.32) | F(2,435) =0.09, p = 0.916 |
| BMI (kg/m2) | 22.60 (±3.22) * | 21.60 (±2.95) * | 22.04 (±2.93) | F(2,432) =3.64, p = 0.027 |
| DEBQ-Restraint | 2.94 (±0.96) | 2.72 (±0.90) | 2.89 (±0.86) | F(2,436) =2.38, p = 0.094 |
| DEBQ-Emotion | 2.97 (±0.90) | 2.80 (±0.90) | 2.84 (±0.86) | F(2,436) =1.43, p = 0.240 |
| DEBQ-External | 3.34 (±0.69) | 3.21 (±0.59) | 3.35 (±0.71) | F(2,436) =1.95, p = 0.143 |
| Ethnicity (% Caucasian) | 93.3 | 91.0 | 86.4 | X2(2) = 4.12, p = 0.127 |
| Occupation (% students) | 83.2 | 83.3 | 81.6 | X2(2) = 0.186, p = 0.911 |
| Model | B | SE | t | p |
|---|---|---|---|---|
| Step 1 | ||||
| BMI | −0.015 * | 0.007 | −2.119 | 0.035 |
| Medical | 0.230 ** | 0.056 | 4.109 | <0.001 |
| Self-diagnosed | 0.189 ** | 0.056 | 3.360 | 0.001 |
| Step 2 | ||||
| BMI | −0.034 * | 0.013 | −2.547 | 0.011 |
| Medical | 0.223 ** | 0.056 | 3.992 | <0.001 |
| Self-diagnosed | 0.190 ** | 0.056 | 3.360 | 0.001 |
| BMI × Medical | 0.031 | 0.017 | 1.816 | 0.070 |
| BMI × Self-diagnosed | 0.019 | 0.019 | 0.980 | 0.327 |
| Variable | Medical (N = 178) | Self-Diagnosed (N = 175) | Control (N = 170) | Between-Group Differences |
|---|---|---|---|---|
| Age (y) | 26.6 (11.1) | 26.9 (10.9) | 27.8 (12.0) | F(2,511) = 0.34, p = 0.711 |
| BMI (kg/m2) | 23.6 (4.5) | 23.6 (4.2) | 23.5 (3.7) | F(2,511) = 0.03, p = 0.974 |
| DEBQ-Restraint | 2.66 (0.91) | 2.67 (.86) | 2.76 (0.90) | F(2,511) = 0.47, p = 0.626 |
| DEBQ-Emotion | 2.67 (0.90) | 2.64 (.98) | 2.77 (0.99) | F(2,511) = 1.16, p = 0.314 |
| DEBQ-External | 3.29 (0.58) | 3.26 (.57) | 3.38 (0.55) | F(2,511) = 2.44, p = 0.088 |
| AEBS | 36.57 (9.65) | 35.99 (9.87) | 36.05 (8.70) | F(2,511) = 0.33, p = 0.720 |
| ABS-disease | 25.80 (3.75) | 25.19 (3.92) | 25.86 (4.41) | F(2,511) = 1.45, p = 0.236 |
| ABS-Free Will | 30.01 (3.29) | 29.95 (3.72) | 30.15 (4.04) | F(2,511) = 0.14, p = 0.873 |
| Ethnicity (% Caucasian) | 89% | 89% | 88% | X2(2) = 0.119, p=0.942 |
| Occupation (% students) | 57% | 49% | 52% | X2(2) = 2.08, p = 0.354 |
| Gender (% male) | 42% | 31% | 38% | X2(2) = 4.95, p = 0.084 |
| Model | B | SE | t | p |
|---|---|---|---|---|
| Step 1 | ||||
| Medical | 0.072 | 0.050 | 1.427 | 0.154 |
| Self-diagnosed | 0.091 | 0.051 | 1.797 | 0.073 |
| ABS-disease | 0.023 ** | 0.005 | 4.439 | 0.000 |
| Step 2 | ||||
| Medical | 0.071 | 0.050 | 1.415 | 0.158 |
| Self-diagnosed | 0.090 | 0.051 | 1.781 | 0.076 |
| ABS-disease | 0.022 ** | 0.008 | 2.685 | 0.007 |
| ABS-Disease × Medical | 0.002 | 0.012 | 0.195 | 0.846 |
| ABS-Disease × Self-diagnosed | 0.000 | 0.012 | −0.034 | 0.972 |
| Model | B | SE | t | p |
|---|---|---|---|---|
| Step 1 | ||||
| Medical | −0.056 | 0.109 | −0.516 | 0.606 |
| Self-diagnosed | −0.146 | 0.110 | −1.331 | 0.184 |
| ABS-disease | 0.047 ** | 0.011 | 4.281 | 0.000 |
| Step 2 | ||||
| Medical | −0.053 | 0.109 | −0.482 | 0.630 |
| Self-diagnosed | −0.147 | 0.110 | −1.337 | 0.182 |
| ABS-disease | 0.059 ** | 0.018 | 3.295 | 0.001 |
| ABS-Disease × Medical | −0.016 | 0.027 | −0.582 | 0.560 |
| ABS-Disease × Self-diagnosed | −0.021 | 0.026 | −0.791 | 0.429 |
| Model | B | SE | t | p |
|---|---|---|---|---|
| Step 1 | ||||
| Medical | 0.067 | 0.051 | 1.32 | 0.186 |
| Self-diagnosed | 0.071 | 0.051 | 1.38 | 0.168 |
| AEBS | 0.003 | 0.002 | 1.42 | 0.156 |
| Step 2 | ||||
| Medical | 0.067 | 0.051 | 1.32 | 0.187 |
| Self-diagnosed | 0.071 | 0.051 | 1.39 | 0.165 |
| AEBS | 0.008 | 0.004 | 1.90 | 0.058 |
| AEBS × Medical | −0.013 * | 0.006 | −2.35 | 0.019 |
| AEBS × Self-diagnosed | 0.000 | 0.006 | −0.065 | 0.948 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ruddock, H.K.; Orwin, M.; Boyland, E.J.; Evans, E.H.; Hardman, C.A. Obesity Stigma: Is the ‘Food Addiction’ Label Feeding the Problem? Nutrients 2019, 11, 2100. https://doi.org/10.3390/nu11092100
Ruddock HK, Orwin M, Boyland EJ, Evans EH, Hardman CA. Obesity Stigma: Is the ‘Food Addiction’ Label Feeding the Problem? Nutrients. 2019; 11(9):2100. https://doi.org/10.3390/nu11092100
Chicago/Turabian StyleRuddock, Helen K., Michael Orwin, Emma J. Boyland, Elizabeth H. Evans, and Charlotte A. Hardman. 2019. "Obesity Stigma: Is the ‘Food Addiction’ Label Feeding the Problem?" Nutrients 11, no. 9: 2100. https://doi.org/10.3390/nu11092100
APA StyleRuddock, H. K., Orwin, M., Boyland, E. J., Evans, E. H., & Hardman, C. A. (2019). Obesity Stigma: Is the ‘Food Addiction’ Label Feeding the Problem? Nutrients, 11(9), 2100. https://doi.org/10.3390/nu11092100





