Pathways from Food Insecurity to Health Outcomes among California University Students
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Context
Participants and Data Collection
2.2. Measures
2.2.1. Independent Variable
2.2.2. Mediators
2.2.3. Dependent Variables
2.3. Analysis
3. Results
3.1. Participant Characteristics
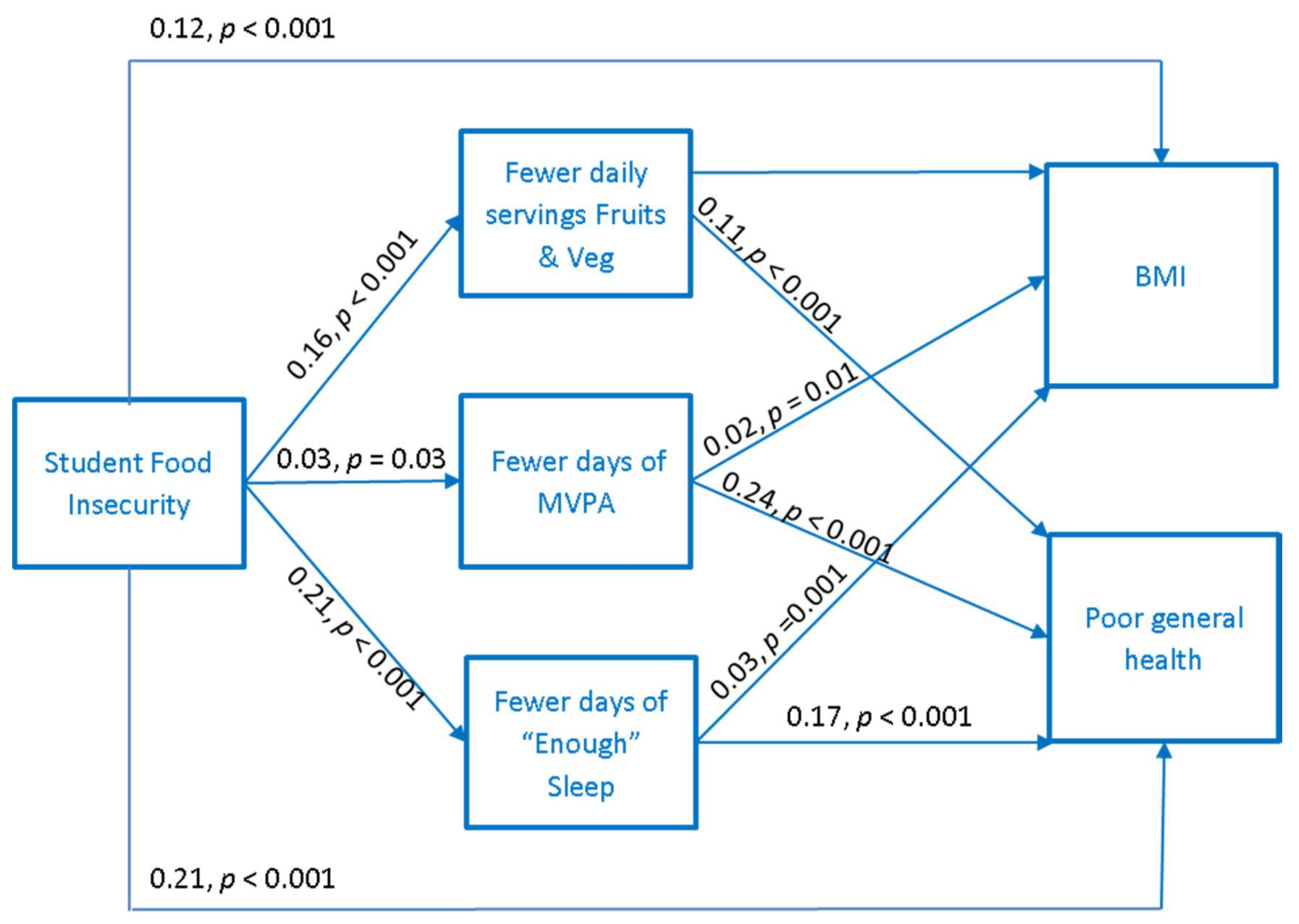
3.2. Path Analysis
4. Discussion
4.1. University Student Context of Food Insecurity
4.2. Higher Education Institutional Strategies for Addressing Food Insecurity
4.3. Federal Level Policies Influencing Basic Needs in Higher Education
4.4. Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Financial Disclosure
Abbreviations
| Food insecurity | (FI) |
| Body mass index | (BMI) |
| Fruits and vegetables | (FV) |
| Moderate to vigorous intensity physical activity | (MVPA) |
| National College Health Assessment | (NCHA) |
| University of California | (UC) |
References
- U.S. Department of Agriculture Economic Research Service. Food Security in the U.S.: Measurement. Available online: www.ers.usda.gov/topics/food-nutrition-assistance/food-security-in-the us/measurement.aspx#measurement (accessed on 10 April 2014).
- Alisha, C.J.; Rabbitt, M.P.; Gregory, C.A.; Singh, A. Household Food Security in the United States in 2016, Err-237. U.S. Department of Agriculture, Economic Research Service. Available online: https://www.ers.usda.gov/publications/pub-details/?pubid=79430 (accessed on 28 September 2016).
- Nazmi, A.; Martinez, S.; Byrd, A.; Robinson, D.; Bianco, S.; Maguire, J.; Crutchfield, R.M.; Condron, K.; Ritchie, L. A Systematic Review of Food Insecurity among U.S. Students in Higher Education. J. Hunger Environ. Nutr. 2018, 1–16. [Google Scholar]
- Martinez, S.M.; Webb, K.; Frongillo, E.A.; Ritchie, L.D. Food Insecurity in California’s Public University System: What Are the Risk Factors? J. Hunger Environ. Health 2018, 13, 1–18. [Google Scholar] [CrossRef]
- Martinez, S.M.; Frongillo, E.A.; Leung, C.; Ritchie, L. No Food for Thought: Food Insecurity Is Related to Poor Mental Health and Lower Academic Performance among Students in California’s Public University System. J. Health Psychol. 2018. [Google Scholar] [CrossRef]
- Watson, T.D.; Malan, H.; Glik, D.; Martinez, S.M. College Students Identify Food Literacy as a Key Strategy to Address Food Insecurity on Campus. Calif. Agric. 2017, 71, 130–138. [Google Scholar] [CrossRef]
- Meza, A.; Altman, E.; Martinez, S.; Leung, C.W. It’s a Feeling That One Is Not Worth Food: A Qualitative Study Exploring the Psychosocial Experience and Academic Consequences of Food Insecurity among College Students. J. Acad. Nutr. Diet. 2018. [Google Scholar] [CrossRef]
- Olson, C.M.; Strawderman, M.S. The Relationship between Food Insecurity and Obesity in Rural Childbearing Women. J. Rural Health 2008, 24, 60–66. [Google Scholar] [CrossRef]
- Townsend, M.S.; Peerson, J.; Love, B.; Achterberg, C.; Murphy, S.P. Food Insecurity Is Positively Related to Overweight in Women. J. Nutr. 2001, 131, 1738–1745. [Google Scholar] [CrossRef]
- Jones, A.D. Food Insecurity and Mental Health Status: A Global Analysis of 149 Countries. Am. J. Prev. Med. 2017, 53, 264–273. [Google Scholar] [CrossRef]
- Hamre, R.; Kuester, S.; Renaud, J.; Williams-Piehota, P.; Franco, E.; Roussel, A.; Hersey, J. Improving Nutrition, Physical Activity and Obesity Prevention: Performance Report of the Nutrition and Physical Activity Program to Prevent Obesity and Other Chronic Diseases: 1 July–31 December 2005. Available online: http://www.cdc.gov/obesity/downloads/NPAO_Performance_Report_2005.pdf (accessed on 26 August 2013).
- Grandner, M.A.; Chakravorty, S.; Michael, L.P.; Linden, O.; Gurubhagavatula, I. Habitual Sleep Duration Associated with Self-Reported and Objectively Determined Cardiometabolic Risk Factors. Sleep Med. 2014, 15, 42–50. [Google Scholar] [CrossRef]
- Whinnery, J.; Jackson, N.; Rattanaumpawan, P.; Grandner, M.A. Short and Long Sleep Duration Associated with Race/Ethnicity, Sociodemographics, and Socioeconomic Position. Sleep 2014, 37, 601–611. [Google Scholar] [CrossRef]
- Liu, Y.; Wheaton, A.G.; Chapman, D.P.; Croft, J.B. Sleep Duration and Chronic Diseases among U.S. Adults Age 45 Years and Older: Evidence from the 2010 Behavioral Risk Factor Surveillance System. Sleep 2013, 36, 421–427. [Google Scholar]
- Patton-Lopez, M.M.; Lopez-Cevallos, D.F.; Cancel-Tirado, D.I.; Vazquez, L. Prevalence and Correlates of Food Insecurity among Students Attending a Midsize Rural University in Oregon. J. Nutr. Educ. Behav. 2014, 46, 209–214. [Google Scholar] [CrossRef]
- Ekelund, U.; Besson, H.; Luan, J.; May, A.M.; Sharp, S.J.; Brage, S.; Travier, N.; Agudo, A.; Slimani, N.; Rinaldi, S.; et al. Physical Activity and Gain in Abdominal Adiposity and Body Weight: Prospective Cohort Study in 288,498 Men and Women. Am. J. Clin. Nutr. 2011, 93, 826–835. [Google Scholar] [CrossRef]
- American College Health Association. National College Health Assessment II. Available online: http://www.acha-ncha.org/docs/ACHA-NCHAII_sample.pdf (accessed on 15 January 2015).
- Laguilles, J.S.; Williams, E.A.; Saunders, D.B. Can Lottery Incentives Boost Web Survey Response Rates? Findings from Four Experiments. Res. High. Educ. 2011, 52, 537–553. [Google Scholar] [CrossRef]
- Muthen, B.O. Applications of Causally Defined Direct and Indirect Effects in Mediation Analysis Using SEM in Mplus. Available online: http://www.statmodel.com/download/causalmediation.pdf (accessed on 30 August 2017).
- Vaccaro, J.A.; Huffman, F.G. Sex and Race/Ethnic Disparities in Food Security and Chronic Diseases in U.S. Older Adults. Gerontol. Geriatr. Med. 2017, 3. [Google Scholar] [CrossRef]
- Kendall, A.; Christine, M.O.; Edward, A.F. Relationship of Hunger and Food Insecurity to Food Availability and Consumption. J. Am. Diet. Assoc. 1996, 96, 1019–1024. [Google Scholar] [CrossRef]
- Dietz, W.H. Does Hunger Cause Obesity? Pediatrics 1995, 95, 766–767. [Google Scholar]
- Knol, L.L.; Robb, C.A.; McKinley, E.A.; Wood, M. Food Insecurity, Self-Rated Health, and Obesity among College Students. Am. J. Health Educ. 2017, 48, 248–255. [Google Scholar] [CrossRef]
- Ding, M.; Keiley, M.K.; Garza, K.B.; Duffy, P.A.; Zizza, C.A. Food Insecurity Is Associated with Poor Sleep Outcomes among Us Adults. J. Nutr. 2015, 145, 615–621. [Google Scholar] [CrossRef]
- Bruening, M.; van Woerden, I.; Todd, M.; Laska, M.N. Hungry to Learn: The Prevalence and Effects of Food Insecurity on Health Behaviors and Outcomes over Time among a Diverse Sample of University Freshmen. Int. J. Behav. Nutr. Phys. Act 2018, 15, 9. [Google Scholar] [CrossRef]
- Walker, R.E.; Kawachi, I. Use of Concept Mapping to Explore the Influence of Food Security on Food Buying Practices. J. Acad. Nutr. Diet. 2012, 112, 711–717. [Google Scholar] [CrossRef]
- Chaput, J.P.; McNeil, J.; Després, J.P.; Bouchard, C.; Tremblay, A. Seven to Eight Hours of Sleep a Night Is Associated with a Lower Prevalence of the Metabolic Syndrome and Reduced Overall Cardiometabolic Risk in Adults. PLoS ONE 2013, 8, e72832. [Google Scholar] [CrossRef]
- Shan, Z.; Ma, H.; Xie, X.; Yan, P.; Guo, Y.; Bao, W.; Rong, Y.; Chandra, L.J.; Hu, F.B.; Liu, L. Sleep Duration and Risk of Type 2 Diabetes: A Meta-Analysis of Prospective Studies. Diabetes Care 2015, 38, 529–537. [Google Scholar] [CrossRef]
- Williams, C.J.; Hu, F.B.; Patel, S.R.; Mantzoros, C.S. Sleep Duration and Snoring in Relation to Biomarkers of Cardiovascular Disease Risk among Women with Type 2 Diabetes. Diabetes Care 2007, 30, 1233–1240. [Google Scholar] [CrossRef]
- University of California Office of the President and Institutional Research and Academic Planning. First-Generation Student Success at the University of California. Available online: https://www.universityofcalifornia.edu/sites/default/files/First-Generation%20Student%20Success%20at%20UC%208-2017.pdf (accessed on 30 August 2017).
- Martinez, S.M.; Maynard, K.; Lorrene, D.R. Global Food Initiative Student Food Access and Security Study; University of California. Available online: https://regents.universityofcalifornia.edu/regmeet/july16/e1attach.pdf (accessed on 16 July 2016).
- Reutter, L.I.; Miriam, J.S.; Gerry, V.; Rhonda, L.; Dennis, R.; Edward, M. Who Do They Think We Are, Anyway: Perceptions of and Responses to Poverty Stigma. Qual. Health Res. 2009, 19, 297–311. [Google Scholar] [CrossRef]
- Goldrick-Rab, S. Paying the Price: College Costs, Financial Aid, and the Betrayal of the American Dream; University of Chicago Press: Chicago, IL, USA, 2016. [Google Scholar]
| Characteristics | Total Sample | Food Secure | Food Insecure |
|---|---|---|---|
| Total | 100 (8705) | 61 (5627) | 40 (3438) |
| Age (years), mean, SD | 23, 6 | 24, 5 | 23, 5 |
| Gender | |||
| Female | 67 (5818) | 67 (3514) | 67 (2304) |
| Male | 33 (2817) | 33 (1720) | 32 (1097) |
| Race/ethnicity | |||
| Non-Hispanic White | 34 (2974) | 41 (2147) | 24 (827) |
| Non-Hispanic Black | 2 (206) | 2 (100) | 3 (106) |
| Hispanic | 21 (1844) | 15 (797) | 31 (1047) |
| Asian | 31 (2691) | 31 (1637) | 31 (1054) |
| Mixed race or other | 11 (990) | 11 (586) | 12 (404) |
| Academic level | |||
| Undergraduate | 66 (5720) | 57 (3006) | 79 (2714) |
| Graduate | 34 (2994) | 43 (2233) | 22 (711) |
| Hours worked for pay | |||
| 0 h | 48 (4121) | 49 (2557) | 46 (1564) |
| 1–19 h | 31 (3662) | 27 (1479) | 36 (1233) |
| 20+ h | 16 (1403) | 25 (1257) | 19 (631) |
| Received financial aid, need-based scholarship, grant, loan | 65 (5628) | 73 (1386) | 82 (1247) |
| Childhood history of food insecurity | 22 (1926) | 24 (467) | 76 (1459) |
| Total Sample | Food Secure | Food Insecure | |
|---|---|---|---|
| Health factors | |||
| Body mass index (kg/m2) *** | 23.65 (4.82) | 23.22 (4.23) | 24.30 (5.55) |
| Poor self-report health (median, interquartile range) | 3 (2–3) | 2 (2–3) | 3 (2–4) |
| Overweight/obese (%, n) *** | 28, 2349 | 25, 1270 | 33, 1110 |
| Lifestyle behaviors | |||
| Daily servings of F/V *** | 2.30 (1.38) | 2.50 (1.41) | 2.00 (1.28) |
| No. days of enough sleep *** | 3.34 (1.99) | 3.64 (1.98) | 2.87 (1.91) |
| No. days of MVPA ** | 1.77 (1.56) | 1.81 (1.53) | 1.72 (1.60) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Martinez, S.M.; Grandner, M.A.; Nazmi, A.; Canedo, E.R.; Ritchie, L.D. Pathways from Food Insecurity to Health Outcomes among California University Students. Nutrients 2019, 11, 1419. https://doi.org/10.3390/nu11061419
Martinez SM, Grandner MA, Nazmi A, Canedo ER, Ritchie LD. Pathways from Food Insecurity to Health Outcomes among California University Students. Nutrients. 2019; 11(6):1419. https://doi.org/10.3390/nu11061419
Chicago/Turabian StyleMartinez, Suzanna M., Michael A. Grandner, Aydin Nazmi, Elias Ruben Canedo, and Lorrene D. Ritchie. 2019. "Pathways from Food Insecurity to Health Outcomes among California University Students" Nutrients 11, no. 6: 1419. https://doi.org/10.3390/nu11061419
APA StyleMartinez, S. M., Grandner, M. A., Nazmi, A., Canedo, E. R., & Ritchie, L. D. (2019). Pathways from Food Insecurity to Health Outcomes among California University Students. Nutrients, 11(6), 1419. https://doi.org/10.3390/nu11061419







