Dietary Patterns, Skeletal Muscle Health, and Sarcopenia in Older Adults
Abstract
1. Introduction
2. Evidence about the Role of Dietary Patterns in Muscle Ageing Studies
2.1. Dietary Patterns Derived A Priori: Example of Mediterranean Diet
2.1.1. Main Characteristics of Mediterranean Diet
2.1.2. Systematic Reviews of Mediterranean Diet and Muscle Ageing: Summary of Evidence
2.1.3. Mediterranean Diet and Muscle Ageing: Additional Evidence
2.2. Dietary Patterns Derived A Priori: Example of Diet Quality Indices
2.2.1. Diet Quality Indices and Muscle Ageing: Additional Evidence
2.3. Dietary Patterns Derived A Posteriori
2.3.1. Dietary Patterns Derived A Posteriori and Muscle Ageing: Additional Evidence
2.4. Similarities and Differences between the Findings of Dietary Patterns and Muscle Ageing Studies
3. Potential Mechanisms of Myoprotective Dietary Patterns in Older Adults
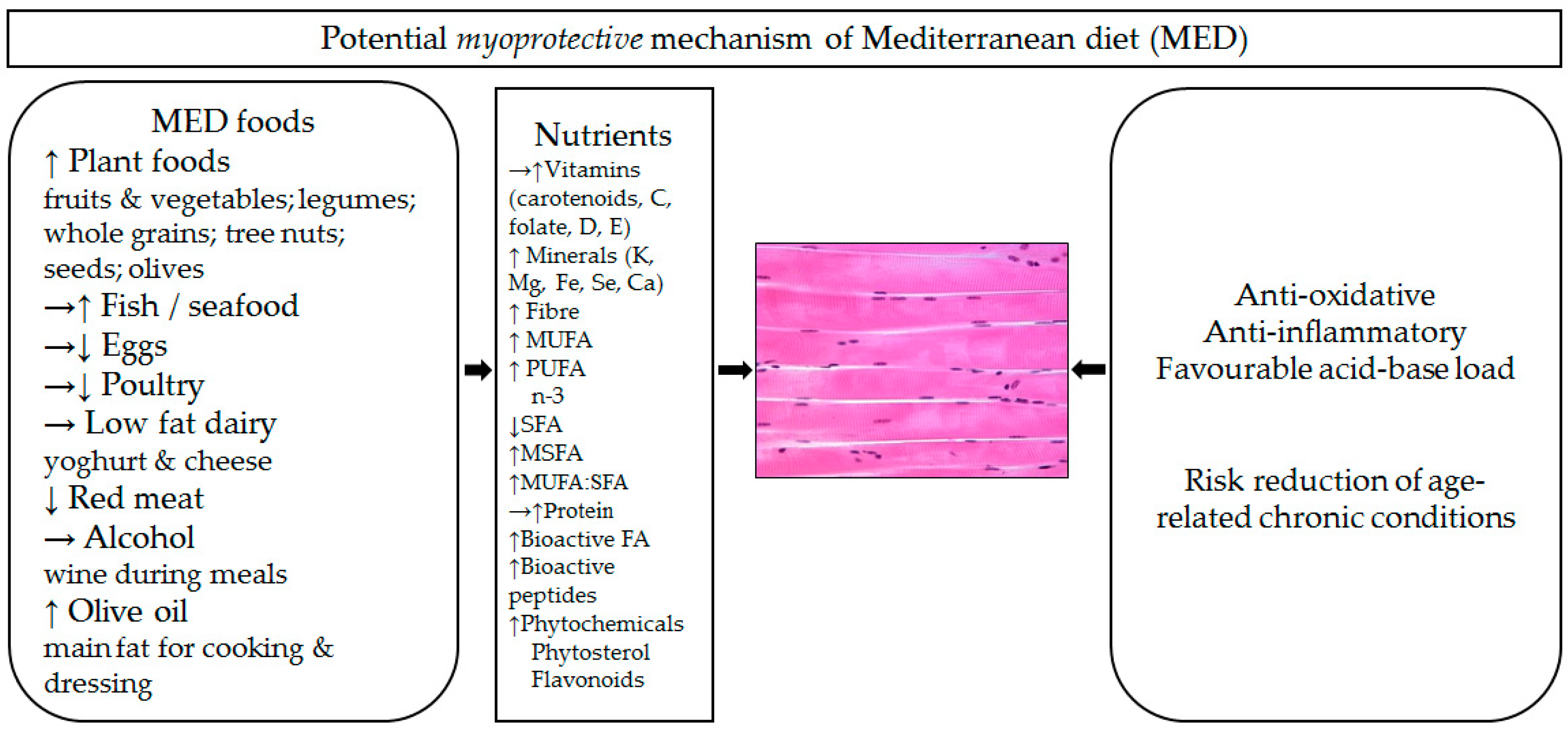
Potential Myoprotective Mechanisms of Healthy Dietary Patterns: Example of Mediterranean Diet
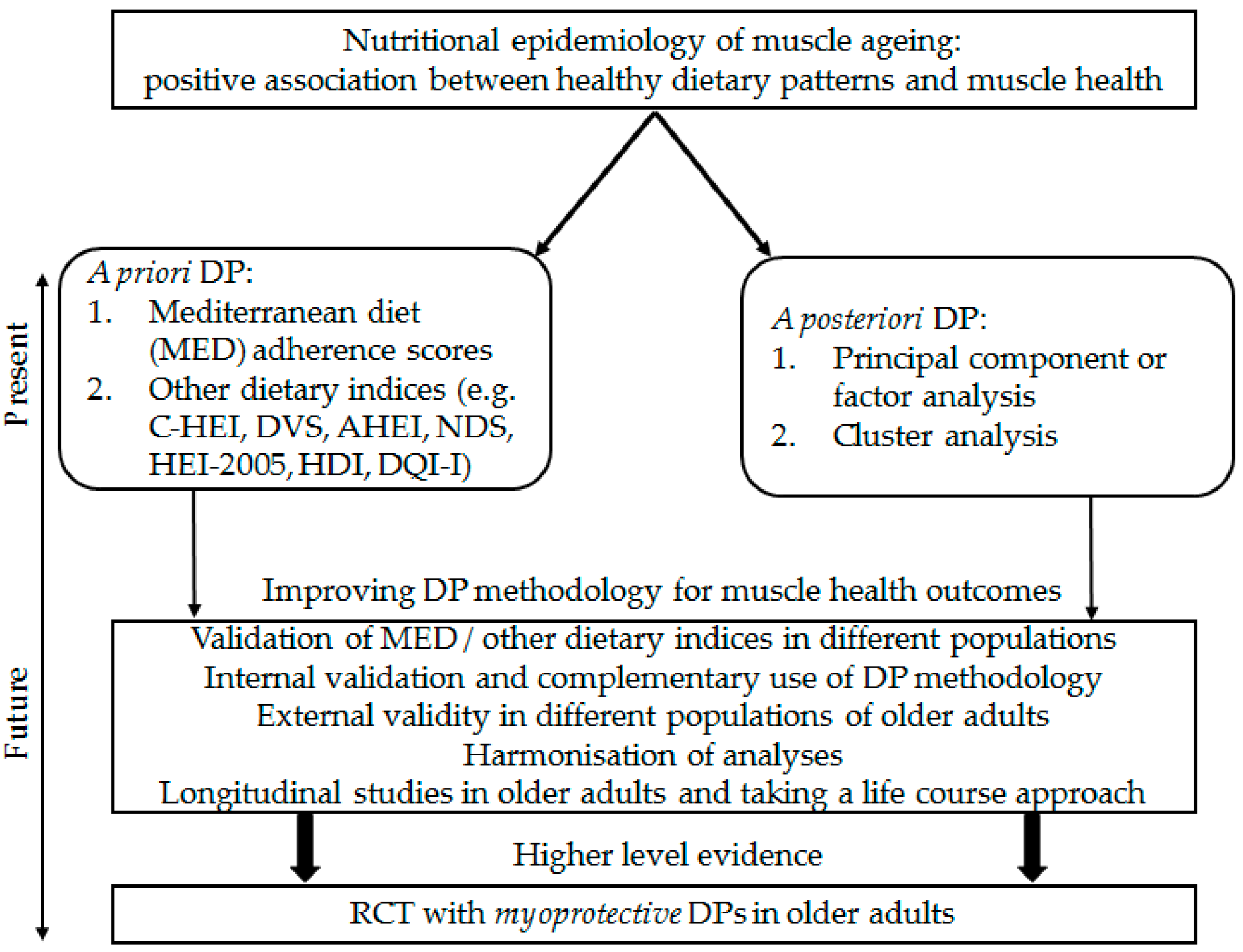
4. Challenges Facing Dietary Patterns Research in Nutritional Epidemiology of Muscle Ageing
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- United Nations, Department of Economic and Social Affairs, Population Division. World Population Ageing 2017—Highlights (ST/ESA/SER.A/397). Available online: http://www.un.org/en/development/desa/population/publications/pdf/ageing/WPA2017_Highlights.pdf (accessed on 12 November 2018).
- Christensen, K.; Doblhammer, G.; Rau, R.; Vaupel, J.W. Ageing populations: The challenges ahead. Lancet 2009, 374, 1196–1208. [Google Scholar] [CrossRef]
- Sowa, A.; Tobiasz-Adamczyk, B.; Topór-Mądry, R.; Poscia, A.; la Milia, D.I. Predictors of healthy ageing: Public health policy targets. BMC Health Serv. Res. 2016, 16, 289. [Google Scholar] [CrossRef]
- Lowsky, D.J.; Olshansky, S.J.; Bhattacharya, J.; Goldman, D.P. Heterogeneity in healthy aging. J. Gerontol. A Bio.l Sci. Med. Sci. 2014, 69, 640–649. [Google Scholar] [CrossRef]
- Mitnitski, A.; Howlett, S.E.; Rockwood, K. Heterogeneity of human aging and its assessment. J. Gerontol. A Biol. Sci. Med. Sci. 2017, 72, 877–884. [Google Scholar] [CrossRef] [PubMed]
- Steves, C.J.; Spector, T.D.; Jackson, S.H. Ageing, genes, environment and epigenetics: What twin studies tell us now, and in the future. Age Ageing 2012, 41, 581–586. [Google Scholar] [CrossRef] [PubMed]
- Daskalopoulou, C.; Stubbs, B.; Kralj, C.; Koukounari, A.; Prince, M.; Prina, A.M. Physical activity and healthy ageing: A systematic review and meta-analysis of longitudinal cohort studies. Ageing Res. Rev. 2017, 38, 6–17. [Google Scholar] [CrossRef] [PubMed]
- McPhee, J.S.; French, D.P.; Jackson, D.; Nazroo, J.; Pendleton, N.; Degens, H. Physical activity in older age: Perspectives for healthy ageing and frailty. Biogerontology 2016, 17, 567–580. [Google Scholar] [CrossRef]
- Fontana, L.; Partridge, L. Promoting health and longevity through diet: From model organisms to humans. Cell 2015, 161, 106–118. [Google Scholar] [CrossRef]
- Seals, D.R.; Justice, J.N.; LaRocca, T.J. Physiological geroscience: Targeting function to increase healthspan and achieve optimal longevity. J. Physiol. 2016, 594, 2001–2024. [Google Scholar] [CrossRef] [PubMed]
- Kiefte-de Jong, J.C.; Mathers, J.C.; Franco, O.H. Nutrition and healthy ageing: The key ingredients. Proc. Nutr. Soc. 2014, 73, 249–259. [Google Scholar] [CrossRef]
- Vauzour, D.; Camprubi-Robles, M.; Miquel-Kergoat, S.; Andres-Lacueva, C.; Bánáti, D.; Barberger-Gateau, P.; Bowman, G.L.; Caberlotto, L.; Clarke, R.; Hogervorst, E.; et al. Nutrition for the ageing brain: Towards evidence for an optimal diet. Ageing Res Rev. 2017, 35, 222–240. [Google Scholar] [CrossRef]
- Witard, O.C.; McGlory, C.; Hamilton, D.L.; Phillips, S.M. Growing older with health and vitality: A nexus of physical activity, exercise and nutrition. Biogerontology 2016, 17, 529–546. [Google Scholar] [CrossRef]
- Assmann, K.E.; Andreeva, V.A.; Camilleri, G.M.; Verger, E.O.; Jeandel, C.; Hercberg, S.; Galan, P.; Kesse-Guyot, E. Dietary scores at midlife and healthy ageing in a French prospective cohort. Br. J. Nutr. 2016, 116, 666–676. [Google Scholar] [CrossRef] [PubMed]
- Sofi, F.; Macchi, C.; Abbate, R.; Gensini, G.F.; Casini, A. Mediterranean diet and health status: An updated meta-analysis and a proposal for a literature-based adherence score. Pub. Health Nutr. 2014, 17, 2769–2782. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Gonzalez, M.A.; Martin-Calvo, N. Mediterranean diet and life expectancy; beyond olive oil, fruits, and vegetables. Curr. Opin. Clin. Nutr. Metab. Care 2016, 19, 401–407. [Google Scholar] [CrossRef] [PubMed]
- McGregor, R.A.; Cameron-Smith, D.; Poppitt, S.D. It is not just muscle mass: A review of muscle quality, composition and metabolism during ageing as determinants of muscle function and mobility in later life. Longev. Healthspan 2014, 3, 9. [Google Scholar] [CrossRef] [PubMed]
- Koster, A.; Ding, J.; Stenholm, S.; Caserotti, P.; Houston, D.K.; Nicklas, B.J.; You, T.; Lee, J.S.; Visser, M.; Newman, A.B.; et al. Does the amount of fat mass predict age-related loss of lean mass, muscle strength, and muscle quality in older adults? J. Gerontol. A Biol. Sci. Med. Sci. 2011, 66, 888–895. [Google Scholar] [CrossRef]
- Mitchell, W.K.; Williams, J.; Atherton, P.; Larvin, M.; Lund, J.; Narici, M. Sarcopenia, dynapenia, and the impact of advancing age on human skeletal muscle size and strength; a quantitative review. Front. Physiol. 2012, 3, 260. [Google Scholar] [CrossRef]
- Delmonico, M.J.; Harris, T.B.; Visser, M.; Park, S.W.; Conroy, M.B.; Velasquez-Mieyer, P.; Boudreau, R.; Manini, T.M.; Nevitt, M.; Newman, A.B.; et al. Longitudinal study of muscle strength, quality, and adipose tissue infiltration. Am. J. Clin. Nutr. 2009, 90, 1579–1585. [Google Scholar]
- Goodpaster, B.H.; Park, S.W.; Harris, T.B.; Kritchevsky, S.B.; Nevitt, M.; Schwartz, A.V.; Simonsick, E.M.; Tylavsky, F.A.; Visser, M.; Newman, A.B. The loss of skeletal muscle strength, mass, and quality in older adults: The health, aging and body composition study. J. Gerontol. A Biol. Sci. Med. Sci. 2006, 1, 1059–1064. [Google Scholar] [CrossRef]
- McLeod, M.; Breen, L.; Hamilton, D.L.; Philp, A. Live strong and prosper: The importance of skeletal muscle strength for healthy ageing. Biogerontology 2016, 17, 497–510. [Google Scholar] [CrossRef]
- Millward, D.J. Nutrition and sarcopenia: Evidence for an interaction. Proc. Nutr. Soc. 2012, 71, 566–575. [Google Scholar] [CrossRef]
- Mithal, A.; Bonjour, J.P.; Boonen, S.; Burckhardt, P.; Degens, H.; El Hajj Fuleihan, G.; Josse, R.; Lips, P.; Morales Torres, J.; Rizzoli, R.; et al. Impact of nutrition on muscle mass, strength, and performance in older adults. Osteoporos. Int. 2013, 24, 1555–1566. [Google Scholar] [CrossRef]
- Calvani, R.; Miccheli, A.; Lando, F.; Bossola, M.; Cesari, M.; Leeuwenburgh, C.; Sieber, C.C.; Bernabei, R.; Marzetti, E. Current nutritional recommendations and novel dietary strategies to manage sarcopenia. J. Frailty Aging 2013, 2, 38–53. [Google Scholar]
- Cruz-Jentoft, A.J.; Bahat, G.; Bauer, J.; Boirie, Y.; Bruyère, O.; Cederholm, T.; Cooper, C.; Landi, F.; Rolland, Y.; Sayer, A.A.; et al. Sarcopenia: Revised European consensus on definition and diagnosis. Age Ageing. 2018, 48, 16–31. [Google Scholar] [CrossRef] [PubMed]
- Vellas, B.; Fielding, R.A.; Bens, C.; Bernabei, R.; Cawthon, P.M.; Cederholm, T.; Cruz-Jentoft, A.J.; Del Signore, S.; Donahue, S.; Morley, J.; et al. Implications of ICD-10 for sarcopenia clinical practice and clinical trials: Report by the International Conference on Frailty and Sarcopenia Research Task Force. J. Frailty Aging. 2018, 7, 2–9. [Google Scholar] [PubMed]
- Visser, M.; Schaap, L.A. Consequences of sarcopenia. Clin Geriatr Med. 2011, 27, 387–399. [Google Scholar] [CrossRef]
- Amigues, I.; Schott, A.M.; Amine, M.; Gelas-Dore, B.; Veerabudun, K.; Paillaud, E.; Beauchet, O.; Rolland, Y.; Canouï Poitrine, F.; Bonnefoy, M. Low skeletal muscle mass and risk of functional decline in elderly community-dwelling women: The prospective EPIDOS study. J. Am. Med. Dir. Assoc. 2013, 14, 352–357. [Google Scholar] [CrossRef] [PubMed]
- Manrique-Espinoza, B.; Salinas-Rodríguez, A.; Rosas-Carrasco, O.; Gutiérrez-Robledo, L.M.; Avila-Funes, J.A. Sarcopenia is associated with physical and mental components of health-related quality of life in older adults. J. Am. Med. Dir. Assoc. 2017, 18, 636.e1–636.e5. [Google Scholar] [CrossRef]
- Cawthon, P.M.; Lui, L.Y.; Taylor, B.C.; McCulloch, C.E.; Cauley, J.A.; Lapidus, J.; Orwoll, E.; Ensrud, K.E. Clinical definitions of sarcopenia and risk of hospitalization in community-dwelling older men: The Osteoporotic Fractures in Men Study. J. Gerontol. A Biol. Sci. Med. Sci. 2017, 72, 1383–1389. [Google Scholar] [CrossRef]
- Batsis, J.A.; Mackenzie, T.A.; Barre, L.K.; Lopez-Jimenez, F.; Bartels, S.J. Sarcopenia, sarcopenic obesity and mortality in older adults: Results from the National Health and Nutrition Examination Survey III. Eur J Clin Nutr. 2014, 68, 1001–1007. [Google Scholar] [CrossRef]
- Batsis, J.A.; Mackenzie, T.A.; Jones, J.D.; Lopez-Jimenez, F.; Bartels, S.J. Sarcopenia, sarcopenic obesity and inflammation: Results from the 1999–2004 National Health and Nutrition Examination Survey. Clin. Nutr. 2016, 35, 1472–1483. [Google Scholar] [CrossRef] [PubMed]
- Beyer, I.; Mets, T.; Bautmans, I. Chronic low-grade inflammation and age-related sarcopenia. Curr Opin Clin Nutr Metab Care. 2012, 15, 12–22. [Google Scholar] [CrossRef]
- Alemán-Mateo, H.; López Teros, M.T.; Ramírez, F.A.; Astiazarán-García, H. Association between insulin resistance and low relative appendicular skeletal muscle mass: Evidence from a cohort study in community-dwelling older men and women participants. J. Gerontol. A Biol. Sci. Med. Sci. 2014, 69, 871–877. [Google Scholar] [CrossRef]
- Dela, F.; Helge, J.W. Insulin resistance and mitochondrial function in skeletal muscle. Int. J. Biochem. Cell Biol. 2013, 45, 11–15. [Google Scholar] [CrossRef]
- Cuthbertson, D.; Smith, K.; Babraj, J.; Leese, G.; Waddell, T.; Atherton, P.; Wackerhage, H.; Taylor, P.M.; Rennie, M.J. Anabolic signaling deficits underlie amino acid resistance of wasting, aging muscle. FASEB J. 2005, 19, 422–424. [Google Scholar] [CrossRef] [PubMed]
- Breen, L.; Phillips, S.M. Skeletal muscle protein metabolism in the elderly: Interventions to counteract the “anabolic resistance” of ageing. Nutr. Metab. 2011, 8, 68. [Google Scholar] [CrossRef] [PubMed]
- Burd, N.A.; Gorissen, S.H.; van Loon, L.J. Anabolic resistance of muscle protein synthesis with aging. Exerc. Sport Sci. Rev. 2013, 41, 169–173. [Google Scholar] [CrossRef] [PubMed]
- Anderson, L.J.; Liu, H.; Garcia, J.M. Sex differences in muscle wasting. Adv. Exp. Med. Biol. 2017, 1043, 153–197. [Google Scholar]
- Messier, V.; Rabasa-Lhoret, R.; Barbat-Artigas, S.; Elisha, B.; Karelis, A.D.; Aubertin-Leheudre, M. Menopause and sarcopenia: A potential role for sex hormones. Maturitas 2011, 68, 331–336. [Google Scholar] [CrossRef]
- Joseph, A.M.; Adhihetty, P.J.; Leeuwenburgh, C. Beneficial effects of exercise on age-related mitochondrial dysfunction and oxidative stress in skeletal muscle. J. Physiol. 2016, 594, 5105–5123. [Google Scholar] [CrossRef]
- Gomes, M.J.; Martinez, P.F.; Pagan, L.U.; Damatto, R.L.; Cezar, M.D.M.; Lima, A.R.R.; Okoshi, K.; Okoshi, M.P. Skeletal muscle aging: Influence of oxidative stress and physical exercise. Oncotarget. 2017, 8, 20428–20440. [Google Scholar] [CrossRef]
- Deutz, N.E.; Bauer, J.M.; Barazzoni, R.; Biolo, G.; Boirie, Y.; Bosy-Westphal, A.; Cederholm, T.; Cruz-Jentoft, A.; Krznariç, Z.; Nair, K.S.; et al. Protein intake and exercise for optimal muscle function with aging: Recommendations from the ESPEN Expert Group. Clin. Nutr. 2014, 33, 929–936. [Google Scholar] [CrossRef]
- Cruz-Jentoft, A.J.; Kiesswetter, E.; Drey, M.; Sieber, C.C. Nutrition, frailty, and sarcopenia. Aging. Clin. Exp. Res. 2017, 29, 43–48. [Google Scholar] [CrossRef] [PubMed]
- Verlaan, S.; Aspray, T.J.; Bauer, J.M.; Cederholm, T.; Hemsworth, J.; Hill, T.R.; McPhee, J.S.; Piasecki, M.; Seal, C.; Sieber, C.C.; et al. Nutritional status, body composition, and quality of life in community-dwelling sarcopenic and non-sarcopenic older adults: A case-control study. Clin. Nutr. 2017, 36, 267–274. [Google Scholar] [CrossRef]
- Montero-Fernández, N.; Serra-Rexach, J.A. Role of exercise on sarcopenia in the elderly. Eur. J. Phys. Rehabil. Med. 2013, 49, 131–143. [Google Scholar] [PubMed]
- Marzetti, E.; Calvani, R.; Tosato, M.; Cesari, M.; Di Bari, M.; Cherubini, A.; Broccatelli, M.; Savera, G.; D’Elia, M.; Pahor, M.; et al. Physical activity and exercise as countermeasures to physical frailty and sarcopenia. Aging. Clin. Exp. Res. 2017, 29, 35–42. [Google Scholar] [CrossRef] [PubMed]
- Volaklis, K.A.; Halle, M.; Thorand, B.; Peters, A.; Ladwig, K.H.; Schulz, H.; Koenig, W.; Meisinger, C. Handgrip strength is inversely and independently associated with multimorbidity among older women: Results from the KORA-Age study. Eur. J. Intern. Med. 2016, 31, 35–40. [Google Scholar] [CrossRef]
- Bianchi, L.; Volpato, S. Muscle dysfunction in type 2 diabetes: A major threat to patient’s mobility and independence. Acta Diabetol. 2016, 53, 879–889. [Google Scholar] [CrossRef]
- Springer, J.; Springer, J.I.; Anker, S.D. Muscle wasting and sarcopenia in heart failure and beyond: Update 2017. ESC Heart Fail. 2017, 4, 492–498. [Google Scholar] [CrossRef]
- Deer, R.R.; Volpi, E. Protein intake and muscle function in older adults. Curr. Opin. Clin. Nutr. Metab. Care. 2015, 18, 248–253. [Google Scholar] [CrossRef] [PubMed]
- Beasley, J.M.; Shikany, J.M.; Thomson, C.A. The role of dietary protein intake in the prevention of sarcopenia of aging. Nutr. Clin. Pract. 2013, 28, 684–690. [Google Scholar] [CrossRef]
- Muir, S.W.; Montero-Odasso, M. Effect of vitamin D supplementation on muscle strength, gait and balance in older adults: A systematic review and meta-analysis. J. Am. Geriatr. Soc. 2011, 59, 2291–2300. [Google Scholar] [CrossRef] [PubMed]
- Inzitari, M.; Doets, E.; Bartali, B.; Benetou, V.; Di Bari, M.; Visser, M.; Volpato, S.; Gambassi, G.; Topinkova, E.; De Groot, L.; et al. Nutrition in the age-related disablement process. J. Nutr. Health Aging 2011, 15, 599–604. [Google Scholar] [CrossRef]
- Bloom, I.; Shand, C.; Cooper, C.; Robinson, S.; Baird, J. Diet quality and sarcopenia in older adults: A systematic review. Nutrients 2018, 10, 308. [Google Scholar] [CrossRef] [PubMed]
- Craig, J.V.; Bunn, D.K.; Hayhoe, R.P.; Appleyard, W.O.; Lenaghan, E.A.; Welch, A.A. Relationship between the Mediterranean dietary pattern and musculoskeletal health in children, adolescents, and adults: Systematic review and evidence map. Nutr. Rev. 2017, 75, 830–857. [Google Scholar] [CrossRef] [PubMed]
- Silva, R.; Pizato, N.; da Mata, F.; Figueiredo, A.; Ito, M.; Pereira, M.G. Mediterranean diet and musculoskeletal-functional outcomes in community-dwelling older people: A systematic review and meta-analysis. J. Nutr. Health Aging 2018, 22, 655–663. [Google Scholar] [CrossRef]
- McClure, R.; Villani, A. Mediterranean Diet attenuates risk of frailty and sarcopenia: New insights and future directions. J. Cachexia Sarcopenia Muscle Clin. Rep. 2017, 2. [Google Scholar] [CrossRef]
- Reedy, J.; Krebs-Smith, S.M.; Hammond, R.A.; Hennessy, E. Advancing the science of dietary patterns research to leverage a complex systems approach. J. Acad. Nutr. Diet. 2017, 117, 1019–1022. [Google Scholar] [CrossRef]
- Moeller, S.M.; Reedy, J.; Millen, A.E.; Dixon, L.B.; Newby, P.K.; Tucker, K.L.; Krebs-Smith, S.M.; Guenther, P.M. Dietary patterns: Challenges and opportunities in dietary patterns research an Experimental Biology workshop, April 1, 2006. J. Am. Diet. Assoc. 2007, 107, 1233–1239. [Google Scholar] [CrossRef]
- Hu, F.B. Dietary pattern analysis: A new direction in nutritional epidemiology. Curr. Opin. Lipidol. 2002, 13, 3–9. [Google Scholar] [CrossRef]
- Tucker, K.L. Dietary patterns, approaches, and multicultural perspective. Appl. Physiol. Nutr. Metab. 2010, 35, 211–218. [Google Scholar] [CrossRef]
- Guasch-Ferré, M.; Salas-Salvadó, J.; Ros, E.; Estruch, R.; Corella, D.; Fitó, M.; Martínez-González, M.A.; PREDIMED Investigators. The PREDIMED trial, Mediterranean diet and health outcomes: How strong is the evidence? Nutr. Metab. Cardiovasc. Dis. 2017, 27, 624–632. [Google Scholar]
- Reedy, J.; Krebs-Smith, S.M.; Miller, P.E.; Liese, A.D.; Kahle, L.L.; Park, Y.; Subar, A.F. Higher diet quality is associated with decreased risk of all-cause, cardiovascular disease, and cancer mortality among older adults. J. Nutr. 2014, 144, 881–889. [Google Scholar] [CrossRef] [PubMed]
- Willcox, D.C.; Scapagnini, G.; Willcox, B.J. Healthy aging diets other than the Mediterranean: A focus on the Okinawan diet. Mech. Ageing Dev. 2014, 136–137, 148–162. [Google Scholar] [CrossRef] [PubMed]
- Schwingshackl, L.; Hoffmann, G. Diet quality as assessed by the Healthy Eating Index, the Alternate Healthy Eating Index, the Dietary Approaches to Stop Hypertension score, and health outcomes: A systematic review and meta-analysis of cohort studies. J. Acad. Nutr. Diet. 2015, 115, 780–800. [Google Scholar] [CrossRef]
- Gorman, B.S.; Primavera, L.H. The complimentary use of cluster and factor analysis methods. J. Exp. Educ. 1983, 51, 165–168. [Google Scholar] [CrossRef]
- Hoffmann, K.; Schulze, M.B.; Schienkiewitz, A.; Nöthlings, U.; Boeing, H. Application of a new statistical method to derive dietary patterns in nutritional epidemiology. Am J Epidemiol. 2004, 159, 935–944. [Google Scholar] [CrossRef]
- Trichopoulou, A.; Costacou, T.; Bamia, C.; Trichopoulos, D. Adherence to a Mediterranean diet and survival in a Greek population. N. Engl. J. Med. 2003, 348, 2599–2608. [Google Scholar] [CrossRef] [PubMed]
- Singh, B.; Parsaik, A.K.; Mielke, M.M.; Erwin, P.J.; Knopman, D.S.; Petersen, R.C.; Roberts, R.O. Association of Mediterranean diet with mild cognitive impairment and Alzheimer’s disease: A systematic review and meta-analysis. J. Alzheimers. Dis. 2014, 39, 271–282. [Google Scholar] [CrossRef]
- Petersson, S.D.; Philippou, E. Mediterranean diet, cognitive function, and dementia: A systematic review of the evidence. Adv. Nutr. 2016, 7, 889–904. [Google Scholar] [CrossRef] [PubMed]
- Talegawkar, S.A.; Bandinelli, S.; Bandeen-Roche, K.; Milaneschi, Y.; Tanaka, T.; Semba, R.D.; Guralnik, J.M.; Ferrucci, L. A higher adherence to a Mediterranean-style diet is inversely associated with the development of frailty in community-dwelling elderly men and women. J. Nutr. 2012, 142, 2161–2166. [Google Scholar] [CrossRef] [PubMed]
- Kojima, G.; Avgerinou, C.; Iliffe, S.; Walters, K. Adherence to Mediterranean diet reduces incident frailty risk: Systematic review and meta-analysis. J. Am. Geriatr. Soc. 2018, 66, 783–788. [Google Scholar] [CrossRef]
- Schwingshackl, L.; Schwedhelm, C.; Galbete, C.; Hoffmann, G. Adherence to Mediterranean diet and risk of cancer: An updated systematic review and meta-analysis. Nutrients 2017, 9, 1063. [Google Scholar] [CrossRef] [PubMed]
- Willett, W.C.; Sacks, F.; Trichopoulou, A.; Drescher, G.; Ferro-Luzzi, A.; Helsing, E.; Trichopoulos, D. Mediterranean diet pyramid: A cultural model for healthy eating. Am. J. Clin. Nutr. 1995, 61, 1402S–1406S. [Google Scholar] [CrossRef] [PubMed]
- Saulle, R.; La Torre, G. The Mediterranean Diet, recognized by UNESCO as a cultural heritage of humanity. Ital. J. Pub. Health 2010, 7, 414–415. [Google Scholar]
- United Nations Educational, Scientific and Cultural Organization, Invariable Cultural Heritage. Mediterranean Diet. Available online: https://ich.unesco.org/en/RL/mediterranean-diet-00884 (accessed on 2 January 2019).
- Zaragoza-Martí, A.; Cabañero-Martínez, M.J.; Hurtado-Sánchez, J.A.; Laguna-Pérez, A.; Ferrer-Cascales, R. Evaluation of Mediterranean diet adherence scores: A systematic review. BMJ Open 2018, 8, e019033. [Google Scholar] [CrossRef]
- Bach, A.; Serra-Majem, L.; Carrasco, J.L.; Roman, B.; Ngo, J.; Bertomeu, I.; Obrador, B. The use of indexes evaluating the adherence to the Mediterranean diet in epidemiological studies: A review. Pub. Health Nutr. 2006, 9, 132–146. [Google Scholar] [CrossRef]
- Bach-Faig, A.; Berry, E.M.; Lairon, D.; Reguant, J.; Trichopoulou, A.; Dernini, S.; Medina, F.X.; Battino, M.; Belahsen, R.; Miranda, G.; et al. Mediterranean diet pyramid today. Science and cultural updates. Pub. Health Nutr. 2011, 14, 2274–2284. [Google Scholar] [CrossRef]
- U.S. Department of Health and Human Services; U.S. Department of Agriculture. 2015–2020 Dietary Guidelines for Americans. Available online: https://health.gov/dietaryguidelines/2015/guidelines/ (accessed on 18 December 2018).
- Chan, R.; Leung, J.; Woo, J. A prospective cohort study to examine the association between dietary patterns and sarcopenia in Chinese community-dwelling older people in Hong Kong. J. Am. Med. Dir. Assoc. 2016, 17, 336–342. [Google Scholar] [CrossRef] [PubMed]
- Kelaiditi, E.; Jennings, A.; Steves, C.J.; Skinner, J.; Cassidy, A.; MacGregor, A.J.; Welch, A.A. Measurements of skeletal muscle mass and power are positively related to a Mediterranean dietary pattern in women. Osteoporos. Int. 2016, 27, 3251–3260. [Google Scholar] [CrossRef] [PubMed]
- Isanejad, M.; Sirola, J.; Mursu, J.; Rikkonen, T.; Kröger, H.; Tuppurainen, M.; Erkkilä, A.T. Association of the Baltic Sea and Mediterranean diets with indices of sarcopenia in elderly women, OSPTRE-FPS study. Eur. J. Nutr. 2018, 57, 1435–1448. [Google Scholar] [CrossRef] [PubMed]
- Milaneschi, Y.; Bandinelli, S.; Corsi, A.M.; Lauretani, F.; Paolisso, G.; Dominguez, L.J.; Semba, R.D.; Tanaka, T.; Abbatecola, A.M.; Talegawkar, S.A.; et al. Mediterranean diet and mobility decline in older persons. Exp. Gerontol. 2011, 46, 303–308. [Google Scholar] [CrossRef] [PubMed]
- Shahar, D.R.; Houston, D.K.; Hue, T.F.; Lee, J.S.; Sahyoun, N.R.; Tylavsky, F.A.; Geva, D.; Vardi, H.; Harris, T.B. Adherence to Mediterranean diet and decline in walking speed over 8 years in community-dwelling older adults. J. Am. Geriatr. Soc. 2012, 60, 1881–1888. [Google Scholar] [CrossRef]
- Zbeida, M.; Goldsmith, R.; Shimony, T.; Vardi, H.; Naggan, L.; Shahar, D.R. Mediterranean diet and functional indicators among older adults in non-Mediterranean and Mediterranean countries. J. Nutr. Health Aging 2014, 18, 411–418. [Google Scholar] [CrossRef]
- Bollwein, J.; Diekmann, R.; Kaiser, M.J.; Bauer, J.M.; Uter, W.; Sieber, C.C.; Volkert, D. Dietary quality is related to frailty in community-dwelling older adults. J. Gerontol. A Biol. Sci. Med. Sci. 2012, gls204. [Google Scholar] [CrossRef] [PubMed]
- Tyrovolas, S.; Haro, J.-M.; Mariolis, A.; Piscopo, S.; Valacchi, G.; Bountziouka, V.; Anastasiou, F.; Zeimbekis, A.; Tyrovola, D.; Foscolou, A.; et al. Skeletal muscle mass and body fat in relation to successful ageing of older adults: The multi-national MEDIS study. Arch. Gerontol. Geriatr. 2016, 66, 95–101. [Google Scholar] [CrossRef]
- Fougère, B.; Mazzuco, S.; Spagnolo, P.; Guyonnet, S.; Vellas, B.; Cesari, M.; Gallucci, M. Association between the Mediterranean-style dietary pattern score and physical performance: Results from TRELONG study. J. Nutr. Health Aging 2016, 20, 415–419. [Google Scholar] [CrossRef]
- Nikolov, J.; Spira, D.; Aleksandrova, K.; Otten, L.; Meyer, A.; Demuth, I.; Steinhagen-Thiessen, E.; Eckardt, R.; Norman, K. Adherence to a Mediterranean-style diet and appendicular lean mass in community-dwelling older people: Results from the Berlin Aging Study II. J. Gerontol A Biol. Sci. Med. Sci. 2015, glv218. [Google Scholar] [CrossRef]
- Struijk, E.A.; Guallar-Castillón, P.; Rodríguez-Artalejo, F.; López-García, E. Mediterranean dietary patterns and impaired physical function in older adults. J. Gerontol. A Biol. Sci. Med. Sci. 2018, 73, 333–339. [Google Scholar] [CrossRef] [PubMed]
- Rahi, B.; Ajana, S.; Tabue-Teguo, M.; Dartigues, J.F.; Peres, K.; Feart, C. High adherence to a Mediterranean diet and lower risk of frailty among French older adults community-dwellers: Results from the Three-City-Bordeaux Study. Clin. Nutr. 2018, 37, 1293–1298. [Google Scholar] [CrossRef]
- Leon-Munoz, L.; Guallar-Castillon, P.; Lopez-Garcia, E.; Rodriguez-Artalejo, F. Mediterranean diet and risk of frailty in community-dwelling older adults. J. Am. Med. Dir. Assoc. 2014, 15, 899–903. [Google Scholar] [CrossRef]
- Xu, B.; Houston, D.K.; Locher, J.L.; Ellison, K.J.; Gropper, S.; Buys, D.R.; Zizza, C.A. Higher Healthy Eating Index-2005 scores are associated with better physical performance. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2012, 67, 93–99. [Google Scholar] [CrossRef] [PubMed]
- Smee, D.; Pumpa, K.; Falchi, M.; Lithander, F.E. The relationship between diet quality and falls risk, physical function and body composition in older adults. J. Nutr. Health Aging 2015, 19, 1037–1042. [Google Scholar] [CrossRef] [PubMed]
- Rahi, B.; Morais, J.A.; Dionne, I.J.; Gaudreau, P.; Payette, H.; Shatenstein, B. The combined effects of diet quality and physical activity on maintenance of muscle strength among diabetic older adults from the NuAge cohort. Exp. Gerontol. 2014, 49, 40–46. [Google Scholar] [CrossRef] [PubMed]
- Bibiloni, M.D.M.; Julibert, A.; Argelich, E.; Aparicio-Ugarriza, R.; Palacios, G.; Pons, A.; Gonzalez-Gross, M.; Tur, J.A. Western and Mediterranean dietary patterns and physical activity and fitness among Spanish older adults. Nutrients 2017, 9, 704. [Google Scholar] [CrossRef] [PubMed]
- Barrea, L.; Muscogiuri, G.; Di Somma, C.; Tramontano, G.; De Luca, V.; Illario, M.; Colao, A.; Savastano, S. Association between Mediterranean diet and hand grip strength in older adult women. Clin. Nutr. 2018, 38, 721–729. [Google Scholar] [CrossRef]
- Perälä, M.M.; von Bonsdorff, M.B.; Männistö, S.; Salonen, M.K.; Simonen, M.; Pohjolainen, P.; Kajantie, E.; Rantanen, T.; Eriksson, J.G. The Healthy Nordic Diet and Mediterranean Diet and incidence of disability 10 years later in home-dwelling old adults. J. Am. Med. Dir. Assoc. 2018. [Google Scholar] [CrossRef]
- Tepper, S.; Alter Sivashensky, A.; Rivkah Shahar, D.; Geva, D.; Cukierman-Yaffe, T. The association between Mediterranean Diet and the risk of falls and physical function indices in older type 2 diabetic people varies by age. Nutrients 2018, 10, 767. [Google Scholar] [CrossRef]
- Perälä, M.M.; von Bonsdorff, M.B.; Männistö, S.; Salonen, M.K.; Simonen, M.; Kanerva, N.; Rantanen, T.; Pohjolainen, P.; Eriksson, J.G. The healthy Nordic diet predicts muscle strength 10 years later in old women, but not old men. Age Ageing 2017, 46, 588–594. [Google Scholar] [CrossRef]
- Parsons, T.J.; Papachristou, E.; Atkins, J.L.; Papacosta, O.; Ash, S.; Lennon, L.T.; Whincup, P.H.; Ramsay, S.E.; Wannamethee, S.G. Healthier diet quality and dietary patterns are associated with lower risk of mobility limitation in older men. Eur. J. Nutr. 2018. [Google Scholar] [CrossRef] [PubMed]
- Jeong, G.W.; Kim, Y.J.; Park, S.; Kim, H.; Kwon, O. Associations of recommended food score and physical performance in Korean elderly. BMC Pub. Health 2019, 19, 128. [Google Scholar] [CrossRef] [PubMed]
- Chen, L.K.; Liu, L.K.; Woo, J.; Assantachai, P.; Auyeung, T.W.; Bahyah, K.S.; Chou, M.Y.; Chen, L.Y.; Hsu, P.S.; Krairit, O.; et al. Sarcopenia in Asia: Consensus report of the Asian Working Group for Sarcopenia. J. Am. Med. Dir. Assoc. 2014, 15, 95–101. [Google Scholar] [CrossRef] [PubMed]
- Hoffman, R.; Gerber, M. Evaluating and adapting the Mediterranean diet for non-Mediterranean populations: A critical appraisal. Nutr. Rev. 2013, 71, 573–584. [Google Scholar] [CrossRef] [PubMed]
- D’Alessandro, A.; De Pergola, G. The Mediterranean Diet: Its definition and evaluation of a priori dietary indexes in primary cardiovascular prevention. Int. J. Food. Sci. Nutr. 2018, 69, 647–659. [Google Scholar] [CrossRef]
- Schap, T.; Kuczynski, K.; Hiza, H. Healthy Eating Index-beyond the score. J. Acad. Nutr. Diet. 2017, 117, 519–521. [Google Scholar] [CrossRef] [PubMed]
- Guerrerro, M.L.P.; Pérez-Rodríguez, F. Diet quality indices for nutrition assessment: Types and applications. In Functional Food-Improve Health through Adequate Food, 1st ed.; Hueda, M.C., Ed.; IntechOpen Limited: London, UK, 2017; Volume 1, pp. 283–308. [Google Scholar]
- Hashemi, R.; Motlagh, A.D.; Heshmat, R.; Esmaillzadeh, A.; Payab, M.; Yousefinia, M.; Siassi, F.; Pasalar, P.; Baygi, F. Diet and its relationship to sarcopenia in community dwelling Iranian elderly: A cross sectional study. Nutrition 2015, 31, 97–104. [Google Scholar] [CrossRef] [PubMed]
- Oh, C.; No, J.K.; Kim, H.S. Dietary pattern classifications with nutrient intake and body composition changes in Korean elderly. Nutr. Res. Pract. 2014, 8, 192–197. [Google Scholar] [CrossRef]
- Robinson, S.M.; Jameson, K.A.; Batelaan, S.F.; Martin, H.J.; Syddall, H.E.; Dennison, E.M.; Cooper, C.; Sayer, A.A.; Hertfordshire Cohort Study Group. Diet and its relationship with grip strength in community-dwelling older men and women: The Hertfordshire cohort study. J. Am. Geriatr. Soc. 2008, 56, 84–90. [Google Scholar] [CrossRef]
- Akbaraly, T.; Sabia, S.; Hagger-Johnson, G.; Tabak, A.G.; Shipley, M.J.; Jokela, M.; Brunner, E.J.; Hamer, M.; Batty, G.D.; Singh-Manoux, A.; et al. Does overall diet in midlife predict future aging phenotypes? A cohort study. Am. J. Med. 2013, 126, 411–419. [Google Scholar] [CrossRef]
- Martin, H.; Aihie Sayer, A.; Jameson, K.; Syddall, H.; Dennison, E.M.; Cooper, C.; Robinson, S. Does diet influence physical performance in community-dwelling older people? Findings from the Hertfordshire Cohort Study. Age Ageing 2011, 40, 181–186. [Google Scholar] [CrossRef] [PubMed]
- Granic, A.; Jagger, C.; Davies, K.; Adamson, A.; Kirkwood, T.; Hill, T.R.; Siervo, M.; Mathers, J.C.; Sayer, A.A. Effect of dietary patterns on muscle strength and physical performance in the very old: Findings from the Newcastle 85+ Study. PLoS ONE 2016, 11, e0149699. [Google Scholar] [CrossRef]
- Leon-Munoz, L.M.; Garcia-Esquinas, E.; Lopez-Garcia, E.; Banegas, J.R.; Rodriguez-Artalejo, F. Major dietary patterns and risk of frailty in older adults: A prospective cohort study. BMC Med. 2015, 13, 11. [Google Scholar] [CrossRef] [PubMed]
- Granic, A.; Mendonça, N.; Sayer, A.A.; Hill, T.R.; Davies, K.; Siervo, M.; Mathers, J.C.; Jagger, C. Effect of dietary patterns and low protein intake on sarcopenia risk in the very old: The Newcastle 85+ Study. Clin. Nutr. 2019. [Google Scholar] [CrossRef] [PubMed]
- Pilleron, S.; Pérès, K.; Jutand, M.A.; Helmer, C.; Dartigues, J.F.; Samieri, C.; Féart, C. Dietary patterns and risk of self-reported activity limitation in older adults from the Three-City Bordeaux Study. Br. J. Nutr. 2018, 120, 549–556. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.Y.; Lee, S. Dietary patterns related to appendicular skeletal muscle mass: The Korea National Health and Nutrition Examination Survey 2008–2011. J. Am. Coll. Nutr. 2018. [Google Scholar] [CrossRef] [PubMed]
- Machón, M.; Mateo-Abad, M.; Vrotsou, K.; Zupiria, X.; Güell, C.; Rico, L.; Vergara, I. Dietary patterns and their relationship with frailty in functionally independent older adults. Nutrients 2018, 10, 406. [Google Scholar] [CrossRef] [PubMed]
- Robinson, S.M.; Westbury, L.D.; Cooper, R.; Kuh, D.; Ward, K.; Syddall, H.E.; Sayer, A.A.; Cooper, C. Adult lifetime diet quality and physical performance in older age: Findings from a British Birth Cohort. J. Gerontol. A Biol. Sci. Med. Sci. 2018, 73, 1532–1537. [Google Scholar] [CrossRef]
- Reinders, I.; Murphy, R.A.; Koster, A.; Brouwer, I.A.; Visser, M.; Garcia, M.E.; Launer, L.J.; Siggeirsdottir, K.; Eiriksdottir, G.; Jonsson, P.V.; et al. Muscle quality and muscle fat infiltration in relation to incident mobility disability and gait speed decline: The Age, Gene/Environment Susceptibility-Reykjavik Study. J. Gerontol. A Biol. Sci. Med. Sci. 2015, 70, 1030–1036. [Google Scholar] [CrossRef] [PubMed]
- Visser, M.; Goodpaster, B.H.; Kritchevsky, S.B.; Newman, A.B.; Nevitt, M.; Rubin, S.M.; Simonsick, E.M.; Harris, T.B. Muscle mass, muscle strength, and muscle fat infiltration as predictors of incident mobility limitations in well-functioning older persons. J. Gerontol. A Biol. Sci. Med. Sci. 2005, 60, 324–333. [Google Scholar] [CrossRef] [PubMed]
- Cesari, M.; Penninx, B.W.; Pahor, M.; Lauretani, F.; Corsi, A.M.; Rhys Williams, G.; Guralnik, J.M.; Ferrucci, L. Inflammatory markers and physical performance in older persons: The InCHIANTI study. J. Gerontol. A Biol. Sci. Med. Sci. 2004, 59, 242–248. [Google Scholar] [CrossRef]
- Windham, B.G.; Wilkening, S.R.; Lirette, S.T.; Kullo, I.J.; Turner, S.T.; Griswold, M.E.; Mosley, T.H., Jr. Associations between inflammation and physical function in African Americans and European Americans with prevalent cardiovascular risk factors. J. Am. Geriatr. Soc. 2016, 64, 1448–1455. [Google Scholar] [CrossRef] [PubMed]
- Meng, S.J.; Yu, L.J. Oxidative stress, molecular inflammation and sarcopenia. Int. J. Mol. Sci. 2010, 11, 1509–1526. [Google Scholar] [CrossRef] [PubMed]
- Baumann, C.W.; Kwak, D.; Liu, H.M.; Thompson, L.V. Age-induced oxidative stress: How does it influence skeletal muscle quantity and quality? J. Appl. Physiol. 2016, 121, 1047–1052. [Google Scholar] [CrossRef] [PubMed]
- Cleasby, M.E.; Jamieson, P.M.; Atherton, P.J. Insulin resistance and sarcopenia: Mechanistic links between common co-morbidities. J. Endocrinol. 2016, 229, R67–R81. [Google Scholar] [CrossRef] [PubMed]
- Abbatecola, A.M.; Paolisso, G.; Fattoretti, P.; Evans, W.J.; Fiore, V.; Dicioccio, L.; Lattanzio, F. Discovering pathways of sarcopenia in older adults: A role for insulin resistance on mitochondria dysfunction. J. Nutr. Health Aging 2011, 15, 890–895. [Google Scholar] [CrossRef] [PubMed]
- Boccardi, V.; Paolisso, G. The link between insulin resistance and mobility limitation in older persons. Curr. Pharm. Des. 2014, 20, 3095–3098. [Google Scholar] [CrossRef] [PubMed]
- Romagnolo, D.F.; Selmin, O.I. Mediterranean diet and prevention of chronic diseases. Nutr. Today 2017, 52, 208–222. [Google Scholar] [CrossRef]
- Davies, C.; Bryan, J.; Hodgson, J.; Murphy, K. Definition of the Mediterranean diet: A literature review. Nutrients 2015, 7, 9139–9153. [Google Scholar] [CrossRef]
- Berner, L.A.; Becker, G.; Wise, M.; Doi, J. Characterization of dietary protein among older adults in the United States: Amount, animal sources, and meal patterns. J. Acad. Nutr. Diet. 2013, 113, 809–815. [Google Scholar] [CrossRef]
- Robinson, S.M.; Reginster, J.Y.; Rizzoli, R.; Shaw, S.C.; Kanis, J.A.; Bautmans, I.; Bischoff-Ferrari, H.; Bruyère, O.; Cesari, M.; Dawson-Hughes, B.; et al. Does nutrition play a role in the prevention and management of sarcopenia? Clin. Nutr. 2018, 37, 1121–1132. [Google Scholar] [CrossRef] [PubMed]
- Milaneschi, Y.; Tanaka, T.; Ferrucci, L. Nutritional determinants of mobility. Curr. Opin. Clin. Nutr. Metab. Care 2010, 13, 625–629. [Google Scholar] [CrossRef]
- Rondanelli, M.; Faliva, M.; Monteferrario, F.; Peroni, G.; Repaci, E.; Allieri, F.; Perna, S. Novel insights on nutrient management of sarcopenia in elderly. Biomed. Res. Int. 2015, 2015, 524948. [Google Scholar] [CrossRef]
- Welch, A. Nutritional influences on age-related skeletal muscle loss. Proc. Nutr. Soc. 2014, 73, 16–33. [Google Scholar] [CrossRef] [PubMed]
- Landi, F.; Calvani, M.; Tosato, M.; Martone, A.A.; Ortolani, E.; Savera, G.; D’Angelo, A.; Sisto, A.; Marzetti, E. Protein intake and muscle health in old age: From biological plausibility to clinical evidence. Nutrients 2016, 8, 295. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.-S.; Wilson, J.M.; Lee, S.-R. Dietary implications on mechanisms of sarcopenia: Roles of protein, amino acids and anitoxidants. J. Nutr. Biochem. 2010, 21, 1–13. [Google Scholar] [CrossRef]
- Witard, O.C.; Wardle, S.L.; Macnaughton, L.S.; Hodgson, A.B.; Tipton, K.D. Protein consideration for optimising skeletal muscle mass in healthy young and older adults. Nutrients 2016, 8, 181. [Google Scholar] [CrossRef]
- Naseeb, M.A.; Volpe, S.L. Protein and exercise in the prevention of sarcopenia and aging. Nutr. Res. 2017, 40, 1–20. [Google Scholar] [CrossRef]
- Beaudart, C.; Dawson, A.; Shaw, S.C.; Harvey, N.C.; Kanis, J.A.; Binkley, N.; Reginster, J.Y.; Chapurlat, R.; Chan, D.C.; Bruyère, O.; et al. Nutrition and physical activity in the prevention and treatment of sarcopenia: Systematic review. Osteoporos. Int. 2017, 28, 1817–1833. [Google Scholar] [CrossRef]
- Wolfe, R.R. Update on protein intake: Importance of milk proteins for health status of the elderly. Nutr. Rev. 2015, 73, 41–47. [Google Scholar] [CrossRef] [PubMed]
- Hanach, N.I.; McCullough, F.; Avery, A. The impact of dairy protein intake on muscle mass, muscle strength, and physical performance in middle-aged to older adults with or without existing sarcopenia: A systematic review and meta-analysis. Adv. Nutr. 2019, 10, 59–69. [Google Scholar] [CrossRef] [PubMed]
- Tachtsis, B.; Camera, D.; Lachman-Kaplan, O. Potential roles of n-3 PUFAs during skeletal muscle growth and regeneration. Nutrients 2018, 10, 309. [Google Scholar] [CrossRef] [PubMed]
- Gray, S.R.; Mittendorfer, B. Fish oil-derived n-3 polyunsaturated fatty acids for the prevention and treatment of sarcopenia. Curr. Opin. Clin. Nutr. Metab. Care. 2018, 21, 104–109. [Google Scholar] [CrossRef]
- Van Dronkelaar, C.; van Velzen, A.; Abdelrazek, M.; van der Steen, A.; Weijs, P.J.M.; Tieland, M. Minerals and sarcopenia; the role of calcium, iron, magnesium, phosphorus, potassium, selenium, sodium, and zinc on muscle mass, muscle strength, and physical performance in older adults: A systematic review. J. Am. Med. Dir. Assoc. 2018, 19, 6–11. [Google Scholar] [CrossRef]
- Semba, R.D.; Lauretani, F.; Ferrucci, L. Carotenoids as protection against sarcopenia in older adults. Arch. Biochem. Biophys. 2007, 458, 141–145. [Google Scholar] [CrossRef]
- Bonjour, J.P.; Kraenzlin, M.; Levasseur, R.; Warren, M.; Whiting, S. Dairy in adulthood: From foods to nutrient interactions on bone and skeletal muscle health. J. Am. Coll. Nutr. 2013, 32, 251–263. [Google Scholar] [CrossRef]
- Phillips, S.M.; Martinson, W. Nutrient-rich, high-quality, protein-containing dairy foods in combination with exercise in aging persons to mitigate sarcopenia. Nutr. Rev. 2018, 77, 216–229. [Google Scholar] [CrossRef] [PubMed]
- Lynch, G.S.; Koopman, R. Dietary meat and protection against sarcopenia. Meat. Sci. 2018, 144, 180–185. [Google Scholar] [CrossRef]
- Rondanelli, M.; Perna, S.; Faliva, M.A.; Peroni, G.; Infantino, V.; Pozzi, R. Novel insights on intake of meat and prevention of sarcopenia: All reasons for adequate consumption. Nutr. Hosp. 2015, 32, 2136–2143. [Google Scholar] [PubMed]
- Ter Borg, S.; de Groot, L.C.; Mijnarends, D.M.; de Vries, J.H.; Verlaan, S.; Meijboom, S.; Luiking, Y.C.; Schols, J.M. Differences in nutrient intake and biochemical nutrient status between sarcopenic and nonsarcopenic older adults-results from the Maastricht Sarcopenia Study. J. Am. Med. Dir. Assoc. 2016, 17, 393–401. [Google Scholar] [CrossRef]
- Kim, T.N.; Choi, K.M. The implications of sarcopenia and sarcopenic obesity on cardiometabolic disease. J. Cell. Biochem. 2015, 116, 1171–1178. [Google Scholar] [CrossRef] [PubMed]
- Scott, D.; de Courten, B.; Ebeling, P.R. Sarcopenia: A potential cause and consequence of type 2 diabetes in Australia’s ageing population? Med. J. Aust. 2016, 205, 329–333. [Google Scholar] [CrossRef]
- König, M.; Spira, D.; Demuth, I.; Steinhagen-Thiessen, E.; Norman, K. Polypharmacy as a risk factor for clinically relevant sarcopenia: Results from the Berlin Aging Study II. J. Gerontol. A Biol. Sci. Med. Sci. 2017, 73, 117–122. [Google Scholar] [CrossRef] [PubMed]
- Welch, A.A.; MacGregor, A.J.; Skinner, J.; Spector, T.D.; Moayyeri, A.; Cassidy, A. A higher alkaline dietary load is associated with greater indexes of skeletal muscle mass in women. Osteoporos. Int. 2013, 24, 1899–1908. [Google Scholar] [CrossRef] [PubMed]
- Jehle, S.; Krapf, R. Effects of acidogenic diet forms on musculoskeletal function. J. Nephrol. 2010, 23, S77–S84. [Google Scholar]
- Ortega, R. Importance of functional foods in the Mediterranean diet. Pub. Health Nutr. 2006, 9, 1136–1140. [Google Scholar] [CrossRef] [PubMed]
- He, L.; He, T.; Farrar, S.; Ji, L.; Liu, T.; Ma, X. Antioxidants maintain cellular redox homeostasis by elimination of reactive oxygen species. Cell. Physiol. Biochem. 2017, 44, 532–553. [Google Scholar] [CrossRef]
- Sakellariou, G.K.; Lightfoot, A.P.; Earl, K.E.; Stofanko, M.; McDonagh, B. Redox homeostasis and age-related deficits in neuromuscular integrity and function. J. Cachexia Sarcopenia Muscle 2017, 8, 881–906. [Google Scholar] [CrossRef] [PubMed]
- Traustadóttir, T.; Davies, S.S.; Su, Y.; Choi, L.; Brown-Borg, H.M.; Roberts, L.J., 2nd; Harman, S.M. Oxidative stress in older adults: Effects of physical fitness. Age 2012, 34, 969–982. [Google Scholar]
- Nyberg, M.; Mortensen, S.P.; Cabo, H.; Gomez-Cabrera, M.C.; Viña, J.; Hellsten, Y. Roles of sedentary aging and lifelong physical activity in exchange of glutathione across exercising human skeletal muscle. Free Radic. Biol. Med. 2014, 73, 166–173. [Google Scholar] [CrossRef] [PubMed]
- Matsusaka, T.; Fujikawa, K.; Nishio, Y.; Mukaida, N.; Matsushima, K.; Kishimoto, T.; Akira, S. Transcription factors NF-IL6 and NF-kappa B synergistically activate transcription of the inflammatory cytokines, interleukin 6 and interleukin 8. Proc. Natl. Acad. Sci. USA 1993, 90, 10193–10197. [Google Scholar] [CrossRef]
- Krabbe, K.S.; Pedersen, M.; Bruunsgaard, H. Inflammatory mediators in the elderly. Exp. Gerontol. 2004, 39, 687–699. [Google Scholar] [CrossRef]
- Fougère, B.; Boulanger, E.; Nourhashémi, F.; Guyonnet, S.; Cesari, M. Chronic inflammation: Accelerator of biological aging. J. Gerontol. A Biol. Sci. Med. Sci. 2017, 72, 1218–1225. [Google Scholar] [CrossRef]
- Hommelberg, P.P.; Langen, R.C.; Schols, A.M.; Mensink, R.P.; Plat, J. Inflammatory signaling in skeletal muscle insulin resistance: Green signal for nutritional intervention? Curr. Opin. Clin. Nutr. Metab. Care. 2010, 13, 647–655. [Google Scholar] [CrossRef]
- Abdul-Ghani, M.A.; DeFronzo, R.A. Pathogenesis of insulin resistance in skeletal muscle. J. Biomed. Biotechnol. 2010, 2010, 476279. [Google Scholar] [CrossRef] [PubMed]
- Panickar, K.S.; Jewell, D.E. The beneficial role of anti-inflammatory dietary ingredients in attenuating markers of chronic low-grade inflammation in aging. Horm. Mol. Biol. Clin. Investig. 2015, 23, 59–70. [Google Scholar] [CrossRef] [PubMed]
- Strandberg, E.; Ponsot, E.; Piehl-Aulin, K.; Falk, G.; Kadi, F. Resistance training alone or combined with n-3 PUFA-rich diet in older women: Effects on muscle fiber hypertrophy. J. Gerontol. A Biol. Sci. Med. Sci. 2019, 74, 489–494. [Google Scholar] [CrossRef] [PubMed]
- Chauveau, P.; Aparicio, M.; Bellizzi, V.; Campbell, K.; Hong, X.; Johansson, L.; Kolko, A.; Molina, P.; Sezer, S.; Wanner, C.; et al. Mediterranean diet as the diet of choice for patients with chronic kidney disease. Nephrol. Dial. Transplant. 2018, 33, 725–735. [Google Scholar] [CrossRef] [PubMed]
- Dawson-Hughes, B.; Harris, S.S.; Ceglia, L. Alkaline diets favor lean tissue mass in older adults. Am. J. Clin. Nutr. 2008, 87, 662–665. [Google Scholar] [CrossRef] [PubMed]
- Allès, B.; Samieri, C.; Féart, C.; Jutand, M.A.; Laurin, D.; Barberger-Gateau, P. Dietary patterns: A novel approach to examine the link between nutrition and cognitive function in older individuals. Nutr. Res. Rev. 2012, 25, 207–222. [Google Scholar] [CrossRef]
- Fielding, R.A.; Vellas, B.; Evans, W.J.; Bhasin, S.; Morley, J.E.; Newman, A.B.; Abellan van Kan, G.; Andrieu, S.; Bauer, J.; Breuille, D.; et al. Sarcopenia: An undiagnosed condition in older adults. Current consensus definition: Prevalence, etiology, and consequences. International working group on sarcopenia. J. Am. Med. Dir. Assoc. 2011, 12, 249–256. [Google Scholar] [CrossRef] [PubMed]
- Sayer, A.A. Sarcopenia the new geriatric giant: Time to translate research findings into clinical practice. Age Ageing 2014, 43, 736–737. [Google Scholar] [CrossRef] [PubMed]
- Sayer, A.A.; Robinson, S.M.; Patel, H.P.; Shavlakadze, T.; Cooper, C.; Grounds, M.D. New horizons in the pathogenesis, diagnosis and management of sarcopenia. Age Ageing 2013, 42, 145–150. [Google Scholar] [CrossRef] [PubMed]
- Jacobs, D.R., Jr.; Tapsell, L.C. Food, not nutrients, is the fundamental unit in nutrition. Nutr. Rev. 2007, 65, 439–450. [Google Scholar] [CrossRef] [PubMed]
| Ref. | Study Design/Duration | Participants/Setting | Measure of Muscle Health/Function | Dietary Assessment | Findings |
|---|---|---|---|---|---|
| Summary of systematic reviews a | |||||
| [57] b | 1 longitudinal/4 years [83]; 1 cross-sectional [84]; | older adults (aged ≥65), Hong Kong [83]; women (aged ≥50), the TwinUK registry [84]; | prevalent and incident sarcopenia [83]; muscle mass and leg explosive power [84] | FFQ/MDS score [83,84]; | →association between MDS and sarcopenia [83]; ↑association between %FFM and higher MDS, ↑leg extension power with ↑MDS [84]; Systematic review conclusion: Inconclusive evidence for the role of the MED in musculoskeletal health across the life course; |
| [59] b | 1 mixed (longitudinal and cross-sectional)/3 years [85]; 2 longitudinal [86,87]/9 and 8 years, respectively; 5 cross-sectional [88,89,90,91,92]c; | women (aged 65–72), Kupio, Finland [85]; older adults (aged ≥65), the InCHIANTI Study, Italy [86]; older adults (aged 70-79), the Health ABC Study, US [87]; | 10-m walking speed, chair rises, one leg stance, knee extension, grip strength, squat, LBMQ [85]; SPPB [86]; 20-m walking speed (usual and rapid) [87]; | 3-day food record/MDS [85]; FFQ/MDS score [86,87]; | ↑association between MDS walking speed, LBMQ and squat test, lowest MDS quartile associated with greater loss of relative skeletal muscle and lean mass, no other associations [85]; ↑association between MDS and SPPB at baseline, higher MDS associated with less decline in SPPB at 3-, 6-, 9-year follow-ups, higher MDS associated with lower risk of mobility disability, and slower decline in mobility [86]; higher MDS associated with higher usual and rapid walking speed and less decline in rapid walking speed [87]; Systematic review conclusion: Lower risk of sarcopenic symptomatology with higher adherence to the MED; |
| [58] b | 2 longitudinal [93,94]/3 and 2 years, respectively; | older adults (aged ≥60), the Senior-ENRICA, Madrid, Spain [93]; older adults (aged ≥65), the Three-City-Bordeaux Study, France [94]; | physical function limitations (Rosow and Breslau scale, SF-12) [93]; modified frailty phenotype (Rosow and Breslau scale, chair stands) [94]; | diet history/MDS, MEDAS [93]; FFQ/MDS [94]; | →association between MDS, mobility impairment, and agility (Rosow and Breslau scale), →association between MDS and physical function decline (SF-12), the highest tertile of MEDAS associated with the decreased risk of developing agility, mobility, and physical functioning impairments [93]; the highest MDS associated with the reduced risk of developing mobility and lower extremity impairments [94]; Systematic review conclusion: Higher adherence to the MED associated with the lower risk of frailty and functional impairment, →association between the MED and sarcopenia in cohort studies, ↑association between the MED and sarcopenia in cross-sectional studies; |
| [56] b,d | 2 longitudinal [73,95] b/6 and 3.5 years, respectively b; 2 cross-sectional [96,97] d; 2 longitudinal [83,98] d/4 and 3 years, respectively; | older adults (aged ≥65), the InCHIANTI, Italy [73]; older adults (aged ≥60), the Senior-ENRICA, Madrid, Spain [95]; older adults (aged ≥60), NHANES 1999–2002, US [96]; older adults (aged ≥60), the Falls Risk and Osteoporosis Longitudinal Study, Australia [97]; older adults (aged ≥65), Hong Kong [83]; older adults (mean age 74.6 years), NuAge cohort, Quibeck, Canada [98]; | grip strength, walking speed (over 15 feet) [73]; grip strength, 3-m walking speed [95]; knee extensor power, 20-feet gait speed [96]; lean mass, SPPB [97]; prevalent and incident sarcopenia [83]; grip strength, knee extensor, and elbow flexor strength [98]; | FFQ/MDS score [73]; diet history/MDS, MEDAS score [95]; 24-hr multi-pass dietary recall/HEI-2005 [96]; FFQ/HEI, HDI [97]; FFQ/DQ-I [83]; three 24-hr dietary recalls/C-HEI [98]; | higher MDS associated with the reduced risk of developing low walking speed, →association between MDS and grip strength [73]; →association between MDS, walking speed and grip strength, but the highest MEDAS tertile associated with reduced risk of low walking speed [95]; ↑association between HEI-2005, knee extension power and gait speed, but attenuated by physical activity [96]; →association between lean mass, SPPB, and HEI, ↑weak association between lean mass and HDI (women), and SPPB and HDI (men) [97]; the highest quintile of DQ-I associated with the reduced risk of prevalent sarcopenia (men), →association between DQ-I and 4-year incident sarcopenia (men and women) [83]; →association between C-HEI and muscle strength (grip strength, knee extensor, elbow flexor) maintenance over 3 years [98]; Systematic review conclusion: Strong observational evidence for the association between ‘heathier’ diets and lower risk of decline in physical performance, but not for decline in muscle strength; |
| Additional evidence e | |||||
| [99] b,d | cross-sectional; | older adults (aged 55–80 (men), and 60–80 (women)), Balearic Islands and Madrid, Spain; | physical fitness (grip strength, 30-s arm curls, 30-s chair stand, 8-foot TUG, 30-m gait speed, 6-min walk test); | FFQ/MED and Westernized DP/factor analysis; | ↑association between the highest quartile of the MED and 30-s chair stands (men), and 6-min walking speed (women), →association between the MED and muscle strength (grip strength and arm curls) in both sexes, the highest MED quartile associated with less time to complete TUG test and 30-m gait speed (men), higher quartiles of a ‘Westernized’ DP associated with slower gait speed, lower body strength (chair rises), agility (8-foot TUG), and aerobic endurance (6-min walk test) in both sexes; |
| [100] b | cross-sectional; | older women (aged 60–85), the PERSSILAA study, Campania Region, Italy; | grip strength; | 7-day food records/PREDIMED score; | women with higher grip strength had higher PREDIMED scores and were more likely to belong to the ‘high adherence’ PREDIMED group (score ≥10); |
| [101] b,d | longitudinal/10 years; | older adults (mean age 61.6 years), the Helsinki Birth Cohort Study, Finland; | mobility limitations; | FFQ/mMDS /NDS; | →association between mMDS and mobility limitations at 10-year follow-up, the highest tertile of NDS associated with the lower risk of developing mobility limitations; |
| [102] b | cross-sectional; | type-2 diabetes patients (aged >60 years), the Center for Successful Aging, Diabetes at Sheba Medical Center, Israel; | Berg balance test, TUG, 6-min walk test, 10-m walk test, four square step test, 30-s chair stand, grip strength; | FFQ/MDS; | ↑association between MDS and grip strength, but not after adjustment for key covariates, age × MDS interaction: The highest MDS tertile associated with longer distance achieved in 6-min walking test, faster time 10-m walk, and better balance score in those aged ≥75 years; |
| [103] b | longitudinal/10 years; | older adults (aged >60), the Helsinki Birth Cohort Study, Finland; | grip strength, leg strength, lean body mass | FFQ/MDS; | ↑association between grip strength and NDS (women) at 10-year follow-up, →associations between NDS and muscle mass in both sexes; |
| [104] d | longitudinal/15 years; | older men (aged 66 at baseline)/the British Regional Heart Study, UK; | mobility limitations (going up or down stairs or walking 400 yards); | FFQ/HDI/EDI; | the highest HDI and EDI category at baseline associated with the reduced risk of mobility limitations 15 years later; |
| [105] d | cross-sectional; | older adults (aged ≥65), the National Fitness Award project, the Ministry of Culture, Sports, and Tourism, South Korea; | fitness tests (2-min step test, TUG, figure-of-8 walk test, grip strength, arm curls); | FFQ/RFS; | ↑association between RFS and grip strength (women), →association between RFS and other physical performance tests; |
| Evidence summary for studies with a priori DPs: Higher adherence to the MED associated with better lower extremity functioning, mobility, better walking speed, and less decline over time; inconclusive evidence for muscle strength; mixed evidence for Diet Quality Indices and sarcopenia/elements of sarcopenia; emerging evidence for ↑association between ‘healthier’ DP and mobility/mobility limitations. | |||||
| Ref. | Study Design/Duration | Participants/Setting | Measure of Muscle Health/Function | Dietary Assessment | Findings |
|---|---|---|---|---|---|
| Summary of systematic review a | |||||
| [56] | 4 cross-sectional [111,112,113,115]; 3 longitudinal [114,116,117]/3.5 to 16 years; | older adults (aged ≥65), the KNHANES, South Korea [112]; older adults (aged 59–73), the Hertfordshire Cohort Study, UK [113]; older adults (mean age 68 years), the Hertfordshire Cohort Study, UK [115]; older adults (aged ≥55), Tehran, Iran [111]; older adults (aged ≥60 at the final follow-up) [114]; older adults (aged ≥85), the Newcastle 85+ Study, UK [116]; older adults (aged ≥60), the Senior-ENRICA, Madrid, Spain [117]; | appendicular skeletal muscle mass [112]; grip strength [113]; short SPPB (3-m walk test, 5 chair rises, one-legged standing balance [115]; 8-feet walking speed [114]; sarcopenia [111]; grip strength, TUG [116]; grip strength, 3-m walking speed [117]; | 24-hr dietary recall/clustering analysis [112];FFQ/PCA [111,113,114,115]; 24-h dietary recall/cluster analysis [116]; diet history/PCA [117]; | a ‘Westernized Korean’ DP associated with increased abnormalities in lean mass compared with a ‘Traditional Korean’ DP [112]; ↑association between ‘Prudent diet’ and grip strength, but partly explained by fatty fish consumption in men and not in women [113]; →association between diet and SPPB in men, higher ‘Prudent diet’ score associated with better 3-m walk time chair stands and balance in women, but not after adjustment for key covariates [115]; the highest tertile of a ‘MED-like’ DP associated with the reduced risk of sarcopenia, but →association between a ‘Westernized’ DP and sarcopenia [111]; →association between a ‘Healthy-foods’ DP and physical function, the highest tertile of a ‘Western-type’ DP associated with the increased risk of poor physical function [114]; men belonging to ‘High Red Meat’ DP had worse GS at baseline, and greater GS decline over 5 years [116]; →association between a ‘Prudent diet’ and grip strength, a ‘Westernized’ DP associated with slow walking speed [117]; Systematic review conclusion: The evidence for the association between ‘heathier’ diets, physical performance and muscle strength has been mixed; |
| Additional evidence b | |||||
| [118] | longitudinal/3 years; | older adults (aged ≥85), the Newcastle 85+ Study, UK; | sarcopenia; | 24-h dietary recall/cluster analysis; | ‘Traditional British’ DP associated with the increased risk of sarcopenia at baseline and 3-year follow-up in older adults with good protein intake; |
| [119] | longitudinal/10 years; | older adults (aged ≥67), the Three-City Bordeaux Study, France; | mobility limitations (Rosow-Breslau scale); | FFQ/hybrid clustering method; | ‘Biscuits and snacking’ cluster associated with a 3-fold increased risk of mobility restriction compared with a ‘healthy cluster’ in men; →association between clusters and mobility in women; |
| [120] | cross-sectional; | older adults (aged ≥60), the KNHNES 2008–2011, South Korea; | appendicular skeletal muscle mass; | FFQ/factor analysis; | a ‘Healthy’ DP associated with higher muscle mass in men, but not in women; |
| [121] | cross-sectional; | older adults (aged ≥70), Gipuzkoa, Spain; | TUG; | FFQ/multiple correspondence and cluster analysis; | three DPs with progressively worse adherence to dietary recommendations; a gradient effect of DPs in relation to TUG; |
| [122] | longitudinal/60–64 years; | British 1946 birth cohort, the MRC National Survey of Health and Development study, UK; | chair rises, TUG, and standing balance (at age 60–64); | prospective 5-day food diaries (completed in 1982, 1989, 1999, and 2006–2010)/PCA; | ↑association between a ‘healthier’ DP at ages 36, 43, 53, and 60–64 and physical performance at age 60–64; |
| Evidence summary for studies with a posteriori DPs: Mixed evidence for ‘healthier’ DPs and components of sarcopenia; higher adherence to ‘Westernized’ DPs associated with impairments in mobility and physical performance. | |||||
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Granic, A.; Sayer, A.A.; Robinson, S.M. Dietary Patterns, Skeletal Muscle Health, and Sarcopenia in Older Adults. Nutrients 2019, 11, 745. https://doi.org/10.3390/nu11040745
Granic A, Sayer AA, Robinson SM. Dietary Patterns, Skeletal Muscle Health, and Sarcopenia in Older Adults. Nutrients. 2019; 11(4):745. https://doi.org/10.3390/nu11040745
Chicago/Turabian StyleGranic, Antoneta, Avan A. Sayer, and Sian M. Robinson. 2019. "Dietary Patterns, Skeletal Muscle Health, and Sarcopenia in Older Adults" Nutrients 11, no. 4: 745. https://doi.org/10.3390/nu11040745
APA StyleGranic, A., Sayer, A. A., & Robinson, S. M. (2019). Dietary Patterns, Skeletal Muscle Health, and Sarcopenia in Older Adults. Nutrients, 11(4), 745. https://doi.org/10.3390/nu11040745




