Zinc Nutritional Status in Patients with Cystic Fibrosis
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Turck, D.; Braegger, C.P.; Colombo, C.; Declercq, D.; Morton, A.; Pancheva, R.; Robberecht, E.; Stern, M.; Strandvik, B.; Wolfe, S.; et al. ESPEN-ESPGHAN-ECFS guidelines on nutrition care for infants, children, and adults with cystic fibrosis. Clin. Nutr. 2016, 35, 557–577. [Google Scholar] [CrossRef]
- Lee, C.M.; Flynn, R.; Hollywood, J.A.; Scallan, M.F.; Ptrick THarrison, P.T. Correction of the DF508 Mutation in the Cystic Fibrosis Transmembrane Conductance Regulator Gene by Zinc-Finger Nuclease Homology-Directed Repair. BioRes. Open Access 2012, 1, 99–108. [Google Scholar] [CrossRef]
- Zsembery, Á.; Fortenberry, J.A.; Liang, L.; Bebok, Z.; Tucker, T.A.; Boyce, A.T.; Braunstein, G.M.; Welty, E.; Bell, P.D.; Sorscher, E.J.; et al. Extracellular Zinc and ATP Restore Chloride Secretion across Cystic Fibrosis Airway Epithelia by Triggering Calcium Entry. J. Biol. Chem. 2004, 279, 10720–10729. [Google Scholar] [CrossRef]
- Krebs, N.F.; Sontag, M.; Accurso, F.J.; Hambidge, K.M. Low plasma zinc concentrations in young infants with cystic fibrosis. J. Pediatr. 1998, 133, 761–764. [Google Scholar] [CrossRef]
- Krężel, A.; Maret, W. The biological inorganic chemistry of zinc ions. Arch. Biochem. Biophys. 2016, 611, 3–19. [Google Scholar] [CrossRef]
- Cousins, R.J. Zinc, 7th ed.; ILSI Press: Washington, DC, USA, 1996. [Google Scholar]
- Young, G.P.; Mortimer, E.K.; Gopalsamy, G.L.; Alpers, D.H.; Binder, H.J.; Manary, M.J.; Ramakrishna, B.S.; Brown, I.L.; Brewer, T.G. Zinc deficiency in children with environmental enteropathy—Development of new strategies: Report from an expert workshop. Am. J. Clin. Nutr. 2014, 100, 1198–1207. [Google Scholar] [CrossRef]
- Zinc: Human Health Fact Sheet; Argonne National Laboratory: Chicago, IL, USA, 2005. Available online: http://www.ead.anl.gov/pub/ doc/zinc.pdf (accessed on 6 December 2011).
- Contaminants: Zinc; E.B.I.: Environmental Bureau of Investigation: Toronto, ON, Canada, 2002. Available online: http://www.e-b-inet/ebi/ contaminants/zinc.html (accessed on 25 March 2002).
- King, J.C.; Brown, K.H.; Gibson, R.S.; Krebs, N.F.; Lowe, N.M.; Siekmann, J.H.; Raiten, D.J. Supplement: Biomarkers of Nutrition for Development (BOND)—Zinc Review. J. Nutr. 2016, 9, 1S–28S. [Google Scholar] [CrossRef]
- Roohani, N.; Hurrell, R.; Kelishadi, R.; Schulin, R. Zinc and its importance for human health: An integrative review. J. Res. Med. Sci. 2013, 18, 144–157. [Google Scholar]
- Freeland-Graves, J.H.; Sanjeevi, N.; Lee, J.J. Global perspectives on trace element requirements. J. Trace Elem. Med. Biol. 2015, 31, 135–141. [Google Scholar] [CrossRef]
- Lin, P.; Sermersheim, M.; Li, H.; Lee, P.H.U.; Steinberg, S.M.; Ma, J. Zinc in Wound Healing Modulation. Nutrients 2018, 10, 16. [Google Scholar] [CrossRef]
- Liuzzi, J.P.; Cousins, R.J. Mammalian zinc transporters. Annu. Rev. Nutr. 2004, 24, 151–172. [Google Scholar] [CrossRef]
- Lukacik, M.; Thomas, R.L.; Aranda, J.V. A meta-analysis of the effects of oral zinc in the treatment of acute and persistent diarrhea. Pediatrics 2008, 121, 326–336. [Google Scholar] [CrossRef]
- Nussbaum, S.R.; Carter, M.J.; Fife, C.E.; da Vanzo, J.; Haught, R.; Nusgart, M.; Cartwright, D. An economic evaluation of the impact, cost, and medicare policy implications for chronic nonhealing wounds. Value Health 2017. [Google Scholar] [CrossRef]
- Morales-Suaréz-Varela, M.; Rubio-López, N.; Ruso, C.; Llopis-Gonzalez, A.; Ruiz-Rojo, E.; Redondo, M.; Pico, Y. Anthropometric Status and Nutritional Intake in Children (6–9 Years) in Valencia (Spain): The ANIVA Study. Int. J. Environ. Res. Public Health 2015, 12, 16082–16095. [Google Scholar] [CrossRef]
- Ackland, M.L.; Michalczyk, A.A. Zinc and Nutrition. Arch. Biochem. Biophys. 2016, 611, 51–57. [Google Scholar] [CrossRef]
- Aggett, P.J. Zinc in Human Biology; Mills, C.F., Ed.; Springer-Verlag: London, UK, 1989; pp. 259–279. [Google Scholar]
- Ibs, K.H.; Rink, L. Zinc-altered immune function. J. Nutr. 2003, 133, 1452S–1456S. [Google Scholar] [CrossRef]
- Salgueiro, M.J.; Zubillaga, M.B.; Lysionek, A.E.; Caro, R.A.; Weill, R.; Boccio, J.R. The role of zinc in the growth and development of children. Nutrition 2002, 18, 510–519. [Google Scholar] [CrossRef]
- Sandstead, H.H.; Freeland-Graves, J.H. Dietary phytate, zinc and hidden zinc deficiency. J. Trace Elem. Med. Biol. 2014, 28, 414–417. [Google Scholar] [CrossRef]
- Brown, K.; Hess, S. Systematic Reviews of Zinc Intervention Strategies. International Zinc Nutrition Consultative Group Technical Document #2. Food Nutr. Bull. 2009, 30, S5–S11. [Google Scholar]
- Wessels, I.; Maywald, M.; Rink, L. Zinc as a Gatekeeper of Immune Function. Nutrients 2017, 9, 1286. [Google Scholar] [CrossRef]
- King, J.C. Zinc: An essential but elusive nutrient. Am. J. Clin. Nutr. 2011, 94, 679S–684S. [Google Scholar] [CrossRef]
- Han, Y.M.; Yoon, H.; Lim, S.; Sung, M.K.; Shin, C.M.; Park, Y.S.; Kim, N.; Lee, D.H.; Kim, J.S. Risk Factors for Vitamin D, Zinc, and Selenium Deficiencies in Korean Patients with Inflammatory Bowel Disease. Gut Liver 2017, 11, 363–369. [Google Scholar] [CrossRef]
- Hess, S.Y. National Risk of Zinc Deficiency as Estimated by National Surveys. Food Nutr. Bull. 2017, 38, 3–17. [Google Scholar] [CrossRef]
- Lowe, N.; Fekete, K.; Decsi, T. Methods of assessment of zinc status in humans: A systematic review. Am. J. Clin. Nutr. 2009, 89, S1–S12. [Google Scholar] [CrossRef]
- Prasad, A.S. Clinical manifestations of zinc deficiency. Ann. Rev. Nutr. 1985, 5, 341–363. [Google Scholar] [CrossRef]
- Prasad, A. Discovery of Zinc for Human Health and Biomarkers of Zinc Deficiency. In Molecular, Genetic, and Nutritional Aspects of Major and Trace Minerals; Academic Press: Cambridge, MA, USA, 2017; Chapter 20; pp. 241–260. [Google Scholar] [CrossRef]
- Gibson, R.; Hess, S.; Hotz, C.; Brown, K. The indicators of zinc status in the population: A review of the evidence. Br. J. Nutr. 2008, 99 (Suppl. 3), S14–S23. [Google Scholar] [CrossRef]
- de Benoist, B.; Darnton-Hill, I.; Davidsson, L.; Fontaine, O.; Hotz, C. Conclusions of the Joint WHO/UNICEF/IAEA/IZiNCG Interagency Meeting on Zinc Status Indicators. Food Nutr. Bull. 2007, 28 (Suppl. 3), S480–S484. [Google Scholar] [CrossRef]
- Ataee, P.; Najafi, M.; Gharagozlou, M.; Aflatounian, M.; Mahmoudi, M.; Khodadad, A.; Farahmand, F.; Motamed, F.; Fallahi, G.H.; Kalantari, N.; et al. Effect of supplementary zinc on body mass index, pulmonary function and hospitalization in children with cystic fibrosis. Turk. J. Pediatr. 2014, 56, 127–132. [Google Scholar]
- Kambe, T.; Nishito, Y.; Fukue, K. Zinc Transporters in Health and Disease. In Molecular, Genetic, and Nutritional Aspects of Major and Trace Minerals; Collins, J., Ed.; Elsevier: Amsterdam, The Netherlands, 2016; Volume 23, pp. 283–291. [Google Scholar]
- Van Biervliet, S.; Van Biervliet, J.P.; Velde, S.V.; Robberecht, E. Serum Zinc Concentration in Cystic Fibrosis Patients Aged Above 4 Years: A Cross-sectional Evaluation. Biol. Trace Elem. Res. 2007, 119, 19–26. [Google Scholar] [CrossRef]
- Krebs, N.; Westcott, J.R.; Arnold, T.D.; Kluger, B.M.; Accurso, F.J.; Miller, L.V.; Hambidge, K.M. Abnormalities in Zinc Homeostasis in Young Infants with Cystic Fibrosis. Pediatr. Res. 2000, 48, 256–261. [Google Scholar] [CrossRef]
- Van Biervliet, S.; Van Biervliet, J.P.; Robberech, E.; Taylor, C. Importance of Zinc in Cystic Fibrosis Patients. Curr. Pediatr. Rev. 2009, 5, 184e8. [Google Scholar] [CrossRef]
- Damphousee, V.; Mailhot, M.; Berthiaume, Y.; Rabasa-Lhoret, R.; Mailhot, G. Plasma zinc in adults with cystic fibrosis: Correlations with clinical outcomes. J. Trace Elem. Med. Biol. 2014, 28, 60–64. [Google Scholar] [CrossRef]
- Gammoh, N.Z.; Rink, L. Zinc in Infection and Inflammation. Nutrients 2017, 9, 624. [Google Scholar] [CrossRef]
- Wieringa, F.T.; Dijkhuizen, M.A.; Fiorentino, M.; Laillou, A.; Berger, J. Determination of Zinc Status in Humans: Which Indicator Should We Use? Nutrients 2015, 7, 3252–3263. [Google Scholar] [CrossRef]
- Hernández, M.; Sobradillo, B.; Aguirre, A.; Aresti, U.; Bilbao, A.; Fernández-Ramos, C.; Lizárraga, A.; Lorenzo, H.; Madariaga, L.; Rica, I.; et al. Curvas y Tablas de Crecimiento (Estudios Longitudinal y Transversal); Fundación Faustino Orbegozo Eizaguirre: Bilbao, Spain, 1985. [Google Scholar]
- Escobedo, M.F.; Barrado, E.; Alonso, C.; Marugán de Miguelsanz, J.M. Comparison study between colorimetric method and flame atomic absorption spectrophotometry in serum zinc status. Nutr. Clin. Diet. Hosp. 2018, 38, 128–133. [Google Scholar] [CrossRef]
- Mataix Verdú, J.; García Diaz, J. NUTRIBER. V. 1.0; Fundación Universitaria Iberoamericana: Barcelona, Spain, 2005. [Google Scholar]
- Krebs, N.F. Update on zinc deficiency and excess in clinical paediatric practice. Ann. Nutr. Metab. 2013, 62 (Suppl. 1), 19–29. [Google Scholar] [CrossRef]
- Wenk, K.S.; Higgins, K.B.; Greer, K.E. Cystic fibrosis presenting with dermatitis. Arch Dermatol. 2010, 146, 171–174. [Google Scholar] [CrossRef]
- Halsted, J.A.; Smith, J.C., Jr. Plasma-zinc in health and disease. Lancet 1970, 1, 322–324. [Google Scholar] [CrossRef]
- Kaur, K.; Gupta, R.; Saraf, S.A.; Saraf, S.K. Zinc: The Metal of Life. Compr. Rev. Food Sci. Food Saf. 2014, 13, 358–376. [Google Scholar] [CrossRef]
- Raiten, D.J.; Namaste, S.; Brabin, B.; Combs, G.; L’Abbe, M.R.; Wasantwisut, E.; Darnton-Hill, I. Executive summary—Biomarkers of Nutrition for Development: Building a consensus. Am. J. Clin. 2011, 94, 633S–650S. [Google Scholar] [CrossRef]
- Prasad, A.S. Discovery of Human Zinc Deficiency: Its Impact on Human Health and Disease. Adv. Nutr. 2013, 4, 176–190. [Google Scholar] [CrossRef] [PubMed]
- Goldfrank, L.R.; Flomenbaum, N. Goldfrank’s Toxicologic Emergencies, 8th ed.; McGraw-Hill Professional: New York, NY, USA, 2006; p. 1981. [Google Scholar]
- Noonan, C.W.; Kathman, S.J.; Sarasua, S.M.; White, M.C. Influence of environmental zinc on the association between environmental and biological measures of lead in children. J. Expo. Sci. Environ. Epidemiol. 2003, 13, 318–323. [Google Scholar] [CrossRef] [PubMed]
- Wessells, K.R.; King, J.C.; Brown, K.H. Relationships between plasma zinc concentrations and clinical signs of zinc deficiency. FASEB J. 2014, 28, 1043.9S. [Google Scholar] [CrossRef]
- Sandström, B. Diagnosis of zinc deficiency and excess in individuals and populations. Food. Nutr. Bull. 2001, 22, 133–137. [Google Scholar] [CrossRef]
- Maqbool, A.; Schall, J.; Zemel, B.S.; Garcia-Espana, F.; Stallings, V. Plasma Zinc and Growth Status in Preadolescent Children with Cystic Fibrosis. J. Pediatr. Gastroenterol. Nutr. 2006, 43, 95–101. [Google Scholar] [CrossRef] [PubMed]
- Borowitz, D.; Baker, R.; Stallings, V. Consensus Report on Nutrition for Pediatric Patients with Cystic Fibrosis. J. Pediatr. Gastroenterol. Nutr. 2002, 35, 246–259. [Google Scholar] [CrossRef] [PubMed]
- Van Biervliet, S.; Van Biervliet, J.; Bernard, D.; Vercaemst, R.; Blanton, V. Serum zinc in healthy Belgian children. Biol. Trace Elem. 2002, 94, 33–40. [Google Scholar] [CrossRef]
- Van Biervliet, S.; Vande Velde, S.; Van Biervliet, J.P.; Robberecht, E. The effect of zinc supplements in cystic fibrosis patients. Ann. Nutr. Metab. 2008, 52, 152–156. [Google Scholar] [CrossRef]
- Ozbek, N.; Akman, S. A slurry sampling method for the determination of iron and zinc in baby food by flame atomic absorption spectrometry. Food Addit. Contam. Part A 2012, 29, 208–216. [Google Scholar] [CrossRef]
- Millán, E.G.; Papale, J.; Berné, Y.; Castro, M.; Moreno, J.M.; Alarcón, O.M.; Torres, M. Valores de referencia de cinc (Zn) y de cobre (Cu) séricos en escolares sanos procedentes de la ciudad de Barquisimeto, Venezuela. Revista del Instituto Nacional de Higiene Rafael Rangel 2012, 43. [Google Scholar]
- Junior, J.; Dean, S.; Mayo-Wilson, E.; Imdad, A. Bhutta Zinc supplementation for preventing mortality and morbidity, and promoting growth, in children aged 6 months to 12 years of age (protocol). Cochrane Database Syst. Rev. 2011. [Google Scholar] [CrossRef]
- Giugliano, R.; Millward, D.J. Growth and zinc homeostasis in severely Zn-deficient rat. Br. J. Nutr. 1984, 52, 545–560. [Google Scholar] [CrossRef]
- Ruz, M.; Castillo-Duran, C.; Lara, X.; Codoceo, J.; Rebolledo, A.; Atalah, E. A 14-mo zinc-supplementation trial in apparently healthy Chilean preschool children. Am. J. Clin. Nutr. 1997, 66, 1406–1413. [Google Scholar] [CrossRef] [PubMed]
- Maret, E.; Sandstead, H. Zinc requirements and the risks and benefits of zinc supplementation. J. Trace Elem. Med. Biol. 2006, 20, 3–18. [Google Scholar] [CrossRef] [PubMed]
- Jansen, E.; Ruskovska, T. Serum biomarkers of (anti) oxidant status for epidemiological studies. Int. J. Mol. Sci. 2015, 16, 27378–27390. [Google Scholar] [CrossRef]
- Micronutrient Information Center. Immunity in Depth. 2018. Available online: http://lpi.oregonstate.edu/mic/ health-disease/immunity (accessed on 17 April 2018).
- Savino, W.; Dardenne, M. Nutritional imbalances and infections affect the thymus: Consequences on T-cell-mediated immune responses. Proc. Nutr. Soc. 2010, 69, 636–643. [Google Scholar] [CrossRef]
- Maggini, S.; Pierre, A.; Calder, P.C. Immune Function and Micronutrient Requirements Change over the Life Course. Nutrients 2018, 10, 1531. [Google Scholar] [CrossRef]
- NHANES 1999–2000 Data Files, National Health and Nutrition Survey Data; Public Health Survey, Center for Disease Control and Prevention: Hyattsville, MD, USA, 2004.
- Olza, J.; Aranceta-Bartrina, J.; González-Gross, M.; Ortega, R.M.; Serra-Majem, L.; Varela-Moreiras, G.; Gil, Á. Reported Dietary Intake and Food Sources of Zinc, Selenium, and Vitamins A, E and C in the Spanish Population: Findings from the ANIBES Study. Nutrients 2017, 9, 697. [Google Scholar] [CrossRef] [PubMed]
- Livingstone, C. Zinc: Physiology, deficiency, and parenteral nutrition. Nutr. Clin. Pract. 2015, 30, 371–382. [Google Scholar] [CrossRef] [PubMed]
- Prasad, A.S. Zinc is an Antioxidant and Anti-Inflammatory Agent: Its Role in Human Health. Front. Nutr. 2014, 1, 14. [Google Scholar] [CrossRef] [PubMed]
- Wessells, K.R.; Brown, K.H. Estimating the global prevalence of zinc deficiency: Results based on zinc availability in national food supplies and the prevalence of stunting. PLoS ONE 2012, 7, e50568. [Google Scholar] [CrossRef] [PubMed]
- Abdulhamid, I.; Beck, F.; Millard, S.; Chen, X.; Prasad, A. Effect of Zinc Supplementation on Respiratory Tract Infections in Children with Cystic Fibrosis. Pediatr. Pulmonol. 2008, 43, 281–287. [Google Scholar] [CrossRef]
- Chausmer, A. Zinc, insulin and diabetes. J. Am. Coll. Nutr. 1998, 17, 109–115. [Google Scholar] [CrossRef] [PubMed]
- Alpers, D.H. Intraluminal bioavailability of divalent cations. Curr. Opin. Gastroenterol. 2013, 29, 164–169. [Google Scholar] [CrossRef] [PubMed]
- Hambidge, K.M.; Miller, L.V.; Westcott, J.; Sheng, X.; Krebs, N.F. Zinc bioavailability and homeostasis. Am. J. Clin. Nutr. 2010, 91, 1478S–1483S. [Google Scholar] [CrossRef]
- King, J.C.; Shames, D.M.; Woodhouse, L.R. Zinc homeostasis in humans. J Nutr. 2000, 130, 1360S–1366S. [Google Scholar] [CrossRef] [PubMed]
- Brown, K.H.; Rivera, J.A.; Bhutta, Z.; Gibson, R.S.; King, J.C.; Lönnerdal, B.; Ruel, M.T.; Sandström, B.; Wasantwisut, E.; Hotz, C. International Zinc Nutrition Consultative Group (IZiNCG) technical document #1. Assessment of the risk of zinc deficiency in populations and options for its control. Food Nutr. Bull. 2004, 25 (Suppl. 2), S94–S203. [Google Scholar]
- King, J.C. Determinants of maternal zinc status during pregnancy. Am. J. Clin. Nutr. 2000, 71, 1334S–1343S. [Google Scholar] [CrossRef]
- Maret, W. Zinc biochemistry, physiology, and homeostasis: Recent insights and current trends. BioMetals 2001, 14, 187–190. [Google Scholar] [CrossRef]
- Ozutemiz, A.O.; Aydin, H.H.; Isler, M.; Celik, H.A.; Batur, Y. Effect of omeprazole on plasma zinc levels after oral zinc administration. Indian J. Gastroenterol. 2002, 21, 216–218. [Google Scholar]
- Proesmans, M.; De Boeck, K. Omeprazole, a proton pump inhibitor, improves residual steatorrhoea in cystic fibrosis patients treated with high dose pancreatic enzymes. Eur. J. Pediatr. 2003, 162, 760–763. [Google Scholar] [CrossRef] [PubMed]
- Farrell, C.P.; Morgan, M.; Rudolph, D.S.; Hwang, A.; Albert, N.E.; Valenzano, M.C.; Wang, X.; Mercogliano, G.; Mullin, J.M. Proton Pump Inhibitors Interfere with Zinc Absorption and Zinc Body Stores. Gastroenterol. Res. 2011, 4, 243–251. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. C-Reactive Protein Concentrations as a Marker of Inflammation or Infection for Interpreting Biomarkers of Micronutrient Status; Vitamin and Mineral Nutrition Information System Inside; WHO/NMH/NHD/EPG/14.7; World Health Organization: Geneva, Switzerland, 2014; pp. 1–4. [Google Scholar]
- Prasad, A.S. Laboratory diagnosis of zinc deficiency. J. Am. Coll. Nutr. 1985, 4, 591–598. [Google Scholar] [CrossRef] [PubMed]
- Singh, A.; Smoak, B.L.; Patterson, K.Y.; LeMay, L.G.; Veillon, C.; Deuster, P.A. Biochemical indices of selected trace minerals in men: Effect of stress. Am. J. Clin. Nutr. 1991, 53, 126–131. [Google Scholar] [CrossRef] [PubMed]
- Corbo, M.D.; Lam, J. Zinc deficiency and its management in the pediatric population: A literature review and proposed etiologic classification. J. Am. Acad. Dermatol. 2013, 69, 616–624. [Google Scholar] [CrossRef] [PubMed]
- Prentice, S. They are what you eat: Can nutritional factors during gestation and early infancy modulate the neonatal immune response? Front Immunol. 2017, 8, 1641. [Google Scholar] [CrossRef]
- Calder, P.; Prescott, S.; Caplan, M. Scientific Review: The Role of Nutrients in Immune Function of Infants and Young Children; Emerging Evidence for Long-Chain Polyunsaturated Fatty Acids; Mead Johnson & Company: Glenview, IL, USA, 2007. [Google Scholar]
- Wintergerst, E.; Maggini, S.; Hornig, D. Immune-enhancing role of vitamin C and zinc and effect on clinical conditions. Ann. Nutr. Metab. 2006, 50, 85–94. [Google Scholar] [CrossRef]
- Brooks, W. Zinc for severe pneumonia in very young children: Double-blind placebo-controlled trial. Lancet 2004, 363, 1683–1688. [Google Scholar] [CrossRef]
- Sharma, G.; Lodha, R.; Shastri, S.; Saini, S.; Kapil, A.; Singla, M.; Mukherjee, A.; Jat, K.R.; Kabra, M.; Kabra, S.K. Zinc Supplementation for One Year Among Children with Cystic Fibrosis Does Not Decrease Pulmonary Infection. Respir. Care 2016, 61, 78–84. [Google Scholar] [CrossRef]
- Safai-Kutti, S.; Selin, E.; Larsson, S.; Jagenburg, R.; Denfors, I.; Sten, G.; Kjellmer, I. Zinc therapy in children with cystic fibrosis. Beiträge zur Infusionstherapie 1991, 27, 104–114. [Google Scholar]
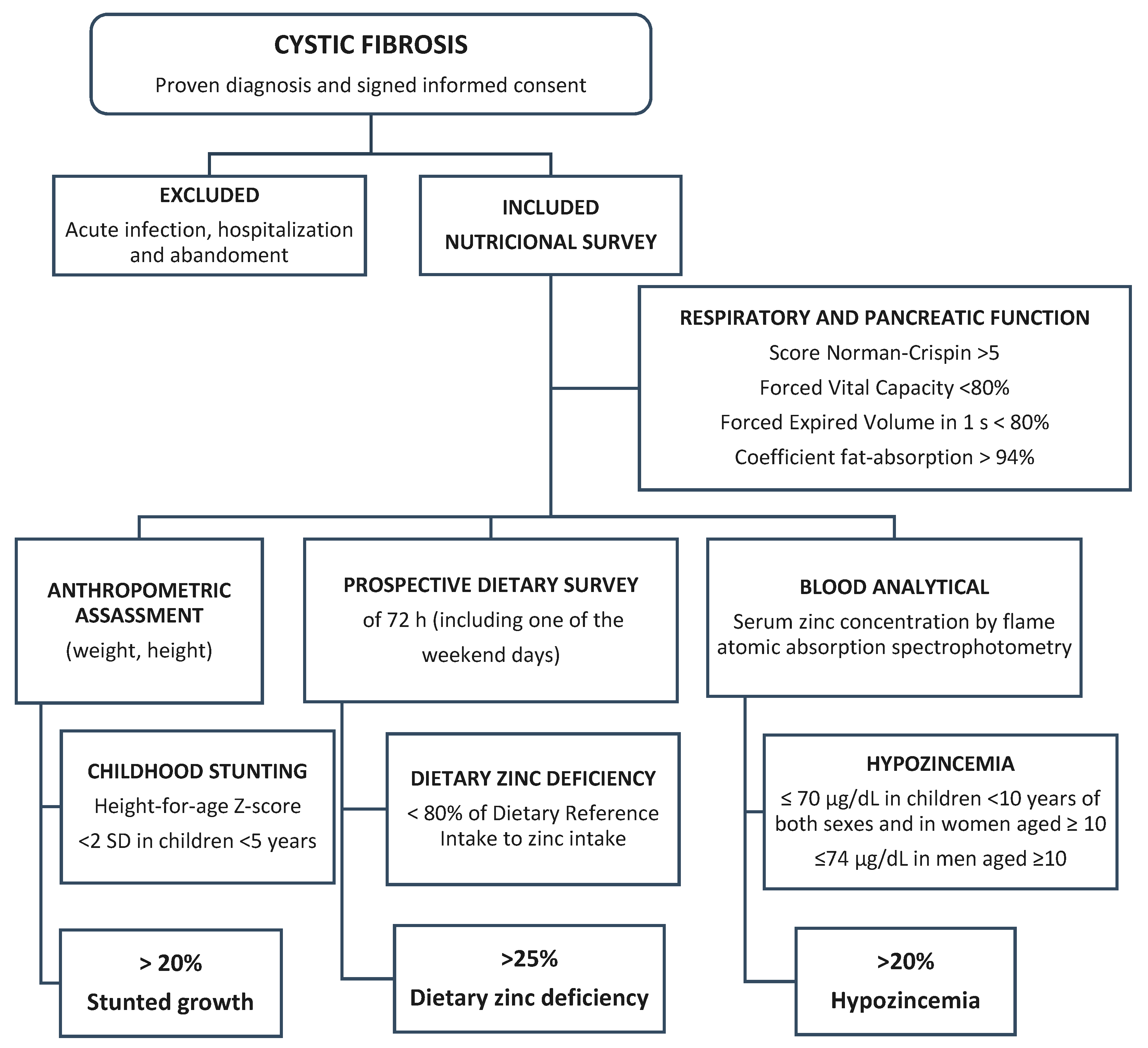
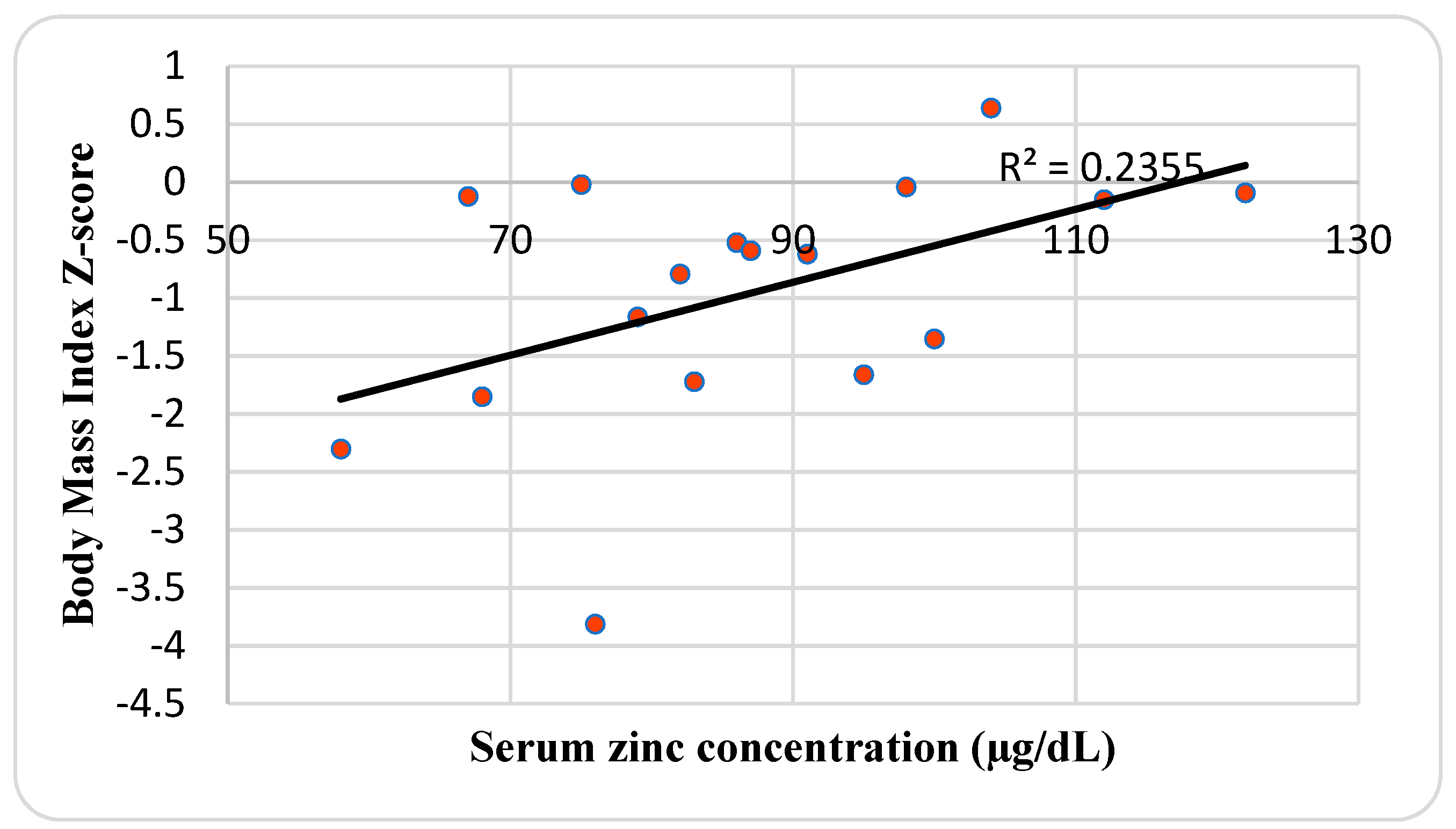
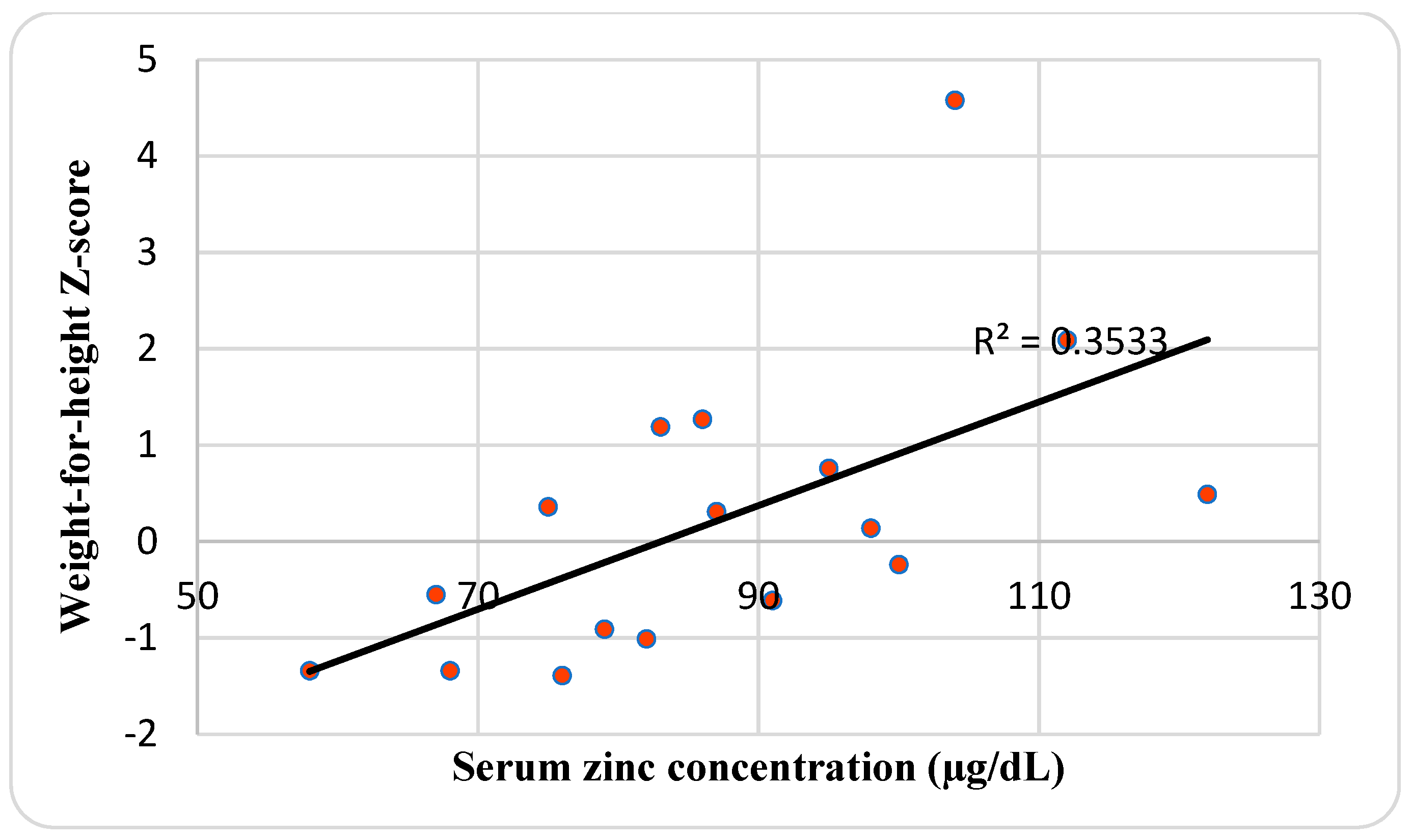
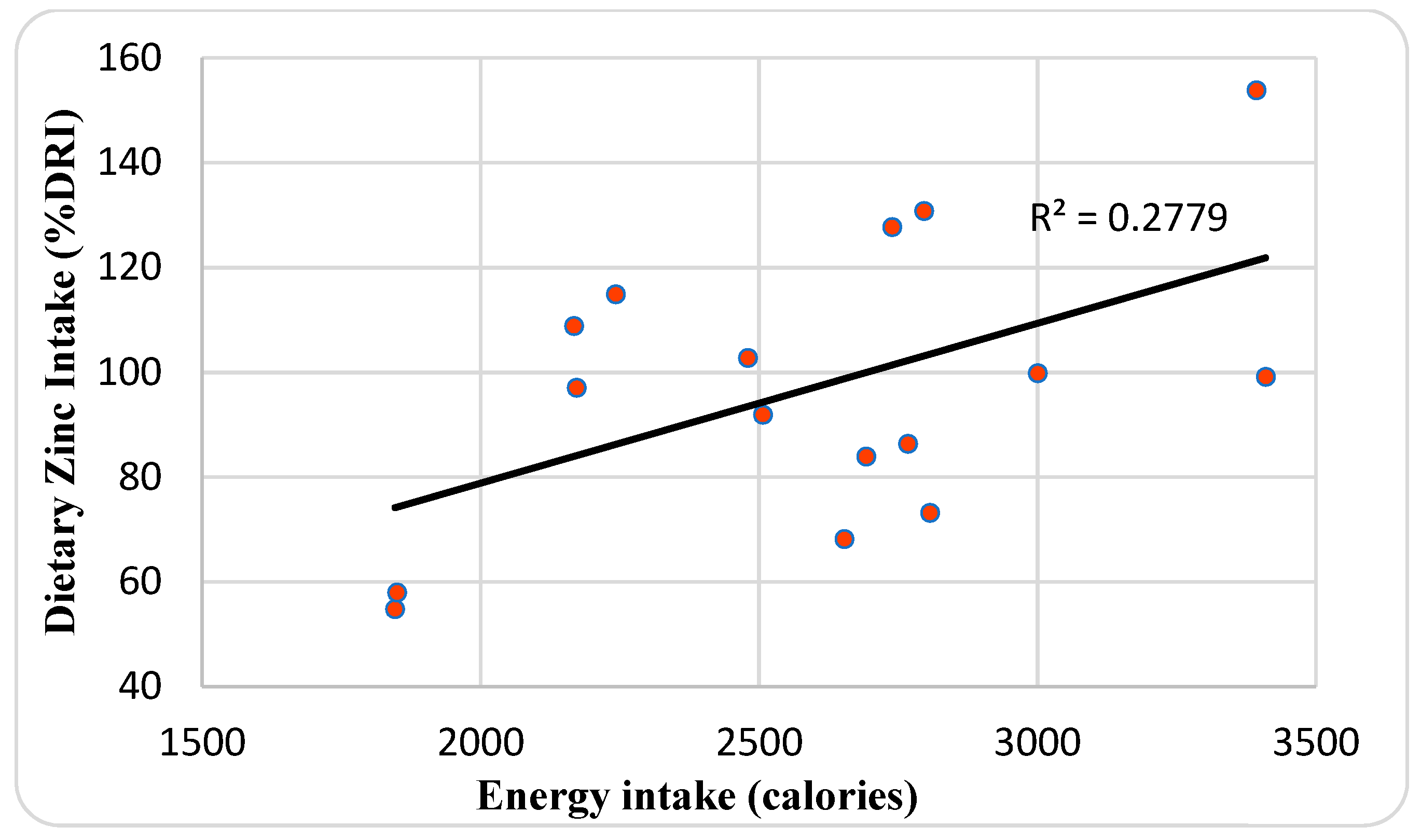
| Characteristics | Mean ± SD or No. (%) | Median | Range |
|---|---|---|---|
| Female (%) | 10 (58.8%) | ||
| Male (%) | 7 (41.2%) | ||
| Age (years) | 14.8 ± 8 | 15 | 2–31 |
| Sick time (months) | 159.7 ± 85 | 148 | 29–298 |
| Genotype (%) (n − 17) | |||
| Homozygous ∆F580 | 6 (35.3%) | ||
| Heterozygous ∆F508 | 7 (41.2%) | ||
| Other mutations | 4 (23.5%) | ||
| Management | |||
| Lipase (IU/kg/day) | 4881 ± 1469 | 5000 | 14,500–7200 |
| Vitamin A (IU) | 5500 ± 3438 | 5000 | 0–10,000 |
| Vitamin E (IU) | 223 ± 137 | 200 | 0–420 |
| Vitamin D3 (IU) | 578 ± 360 | 666 | 0–1333 |
| Vitamin K (mg/w) | 9.5 ± 4.3 | 10 | 0–20 |
| Respiratory and Pancreatic Function | |||
| Forced Vital Capacity (%) | 83.9 ± 38.1 | 78.8 | 33–198 |
| Forced Expired Volume in 1 s (%) | 79.2 ± 25.8 | 78.9 | 29–129 |
| Score Norman-Crispin | 6.3 ± 5.5 | 6.5 | 0–19 |
| Coefficient fat-absorption (%) | 88.4 ± 8.6 | 91.3 | 72.3, 100 |
| Nitrogen Balance | 3.7 ± 5.3 | 2.8 | −6.4–11.4 |
| Anthropometric Assessment | |||
| Body Mass Index (Kg/m2) | 17.4 ± 2.6 | 16.3 | 14.2–23.4 |
| Body Mass Index Z-score | −0.95 ± 1.1 | −0.6 | −3.8–0.6 |
| Weight (kg) | 37.9 ± 15.4 | 36.7 | 10.7–60.4 |
| Height (cm) | 143.9 ± 24.4 | 154.8 | 85–169.9 |
| Weight-for-age Z-score | −1.2 ± 1.1 | −1.3 | −2.9–0.4 |
| Height-for-age Z-score | −0.6 ± 1.1 | −1.2 | −1.9–0.92 |
| Weight-for-height Z-score | 0.22 ± 1.51 | 0.1 | −1.4–4.58 |
| Growth rate (cm/year) | 5.12 ± 2.3 | 5.5 | 0.19–7.56 |
| Blood Analytic | |||
| Serum Zinc level (µg/dL) | 87.2 ± 16.7 | 86 | 58–122 |
| C-reactive protein (u/L) | 4.6 ± 2.4 | 3.7 | 3.1–12 |
| Erythrocyte sedimentation rate (mm/h) | 13.1 ± 5 | 12 | 6–23 |
| C-reactive protein (>4 u/L) | 3 (17.7%) | ||
| Erythrocyte sedimentation rate * | 2 (11.8%) | ||
| Prospective Dietary Survey | |||
| Dietary zinc intake (%DRI) | 97 ± 26.9 | 98.2 | 54.9–153.9 |
| Zinc intake (mg/day) | 14.5 ± 4 | 14.7 | 8.2–23.1 |
| Energy intake (calories) | 2594.9 ± 464.5 | 2672.4 | 1846–3409.6 |
| Comorbidities (%) | |||
| Undernutrition | 5 (29.4%) | ||
| Hypozincemia (µg/dL) | 3 (17.6%) | ||
| Dietary zinc deficiency (%DRI) | 4 (23.5%) | ||
| Respiratory insufficiency | 9 (52.9%) | ||
| Pancreatic insufficiency | 13 (76.5%) |
| Genotipe of Fibrosis Cystic Patients | Number |
|---|---|
| Delta F-508 homozygous | 8 |
| Delta F508/2183AA → G | 2 |
| Delta F-508 mutation in intrón 12 (1898 +1G → A) | 1 |
| Delta F-508/1717-IG-A | 1 |
| Delta F-508/S549R | 1 |
| Mutation 1717-1G | 1 |
| Mutation 1341-A → G exon 8 | 1 |
| Mutation G → A exon 8, G673X exon 13 | 1 |
| Mutation L97F exon 17 | 1 |
| Total | 17 |
| Characteristics | Male | Female | p-Value |
| Age (years) | 10.4 ± 7.2 | 17.2 ± 7.9 | 0.091 |
| Serum zinc concentration (µg/dL) | 93.3 ± 10.2 | 83 ± 19.5 | 0.223 |
| Dietary zinc intake (mg/day) | 12.8 ± 3.9 | 15.9 ± 3.8 | 0.142 |
| Dietary zinc intake (%DRI) | 85.6 ± 25.9 | 105.9 ± 25.5 | 0.140 |
| Colonisation | Yes | No | t-value |
| FVC | 76.9 ± 24.2 | 94.5 ± 53.7 | 0.478 |
| FEV1 | 74.9 ± 27.3 | 84.9 ± 27.5 | 0.511 |
| Respiratory function | Sufficient | Insufficient | t-value |
| Serum zinc concentration (µg/dL) | 90 ± 16.6 | 84.8 ± 17.4 | 0.537 |
| Dietary zinc intake (%DRI) | 81.5 ± 20.8 | 112.5 ± 23.6 | 0.015 |
| Pancreatic function | Sufficient | Insufficient | t-value |
| Serum zinc concentration (µg/dL) | 82 ± 1204 | 88.8 ± 17.9 | 0.417 |
| Dietary zinc intake (%DRI) | 103.2 ± 11.4 | 95.6 ± 29.5 | 0.484 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Escobedo Monge, M.F.; Barrado, E.; Alonso Vicente, C.; Redondo del Río, M.P.; Manuel Marugán de Miguelsanz, J. Zinc Nutritional Status in Patients with Cystic Fibrosis. Nutrients 2019, 11, 150. https://doi.org/10.3390/nu11010150
Escobedo Monge MF, Barrado E, Alonso Vicente C, Redondo del Río MP, Manuel Marugán de Miguelsanz J. Zinc Nutritional Status in Patients with Cystic Fibrosis. Nutrients. 2019; 11(1):150. https://doi.org/10.3390/nu11010150
Chicago/Turabian StyleEscobedo Monge, Marlene Fabiola, Enrique Barrado, Carmen Alonso Vicente, María Paz Redondo del Río, and José Manuel Marugán de Miguelsanz. 2019. "Zinc Nutritional Status in Patients with Cystic Fibrosis" Nutrients 11, no. 1: 150. https://doi.org/10.3390/nu11010150
APA StyleEscobedo Monge, M. F., Barrado, E., Alonso Vicente, C., Redondo del Río, M. P., & Manuel Marugán de Miguelsanz, J. (2019). Zinc Nutritional Status in Patients with Cystic Fibrosis. Nutrients, 11(1), 150. https://doi.org/10.3390/nu11010150






