Comparison of Bioelectrical Impedance Analysis, Slaughter Skinfold-Thickness Equations, and Dual-Energy X-ray Absorptiometry for Estimating Body Fat Percentage in Colombian Children and Adolescents with Excess of Adiposity
Abstract
1. Introduction
2. Methods
2.1. Study Design, Setting, and Participants
2.2. Anthropometric and Body Composition Measures Parameters
2.3. Body Fat Calculation
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Ng, M.; Fleming, T.; Robinson, M.; Thomson, B.; Graetz, N.; Margono, C.; Mullany, E.C.; Biryukov, S.; Abbafati, C.; Abera, S.F.; et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: A systematic analysis for the Global Burden of Disease Study 2013. Lancet 2014, 384, 766–781. [Google Scholar] [CrossRef]
- Dietz, W.H.; Robinson, T.N. Clinical practice. Overweight children and adolescents. N. Engl. J. Med. 2005, 352, 2100–2109. [Google Scholar] [CrossRef] [PubMed]
- Rivera, J.A.; de Cossio, T.G.; Pedraza, L.S.; Aburto, T.C.; Sanchez, T.G.; Martorell, R. Childhood and adolescent overweight and obesity in Latin America: A systematic review. Lancet Diabetes Endocrinol. 2014, 2, 321–332. [Google Scholar] [CrossRef]
- Nathan, B.M.; Moran, A. Metabolic complications of obesity in childhood and adolescence: More than just diabetes. Curr. Opin. Endocrinol. Diabetes Obes. 2008, 15, 21–29. [Google Scholar] [CrossRef] [PubMed]
- Kumar, S.; Kelly, A.S. Review of Childhood Obesity: From Epidemiology, Etiology, and Comorbidities to Clinical Assessment and Treatment. Mayo Clin. Proc. 2017, 92, 251–265. [Google Scholar] [CrossRef] [PubMed]
- Zeng, Q.; Dong, S.-Y.; Sun, X.-N.; Xie, J.; Cui, Y. Percent body fat is a better predictor of cardiovascular risk factors than body mass index. Braz. J. Med. Biol Res. = Rev. Bras. Pesqui Med. Biol. 2012, 45, 591–600. [Google Scholar] [CrossRef]
- Wells, J.C.K.; Fewtrell, M.S. Measuring body composition. Arch. Dis Child. 2006, 91, 612–617. [Google Scholar] [CrossRef] [PubMed]
- Taylor, R.W.; Jones, I.E.; Williams, S.M.; Goulding, A. Body fat percentages measured by dual-energy X-ray absorptiometry corresponding to recently recommended body mass index cutoffs for overweight and obesity in children and adolescents aged 3–18 y. Am. J. Clin. Nutr. 2002, 76, 1416–1421. [Google Scholar] [CrossRef] [PubMed]
- Pritchard, J.E.; Nowson, C.A.; Strauss, B.J.; Carlson, J.S.; Kaymakci, B.; Wark, J.D. Evaluation of dual energy X-ray absorptiometry as a method of measurement of body fat. Eur. J. Clin. Nutr. 1993, 47, 216–228. [Google Scholar] [PubMed]
- Talma, H.; Chinapaw, M.J.M.; Bakker, B.; HiraSing, R.A.; Terwee, C.B.; Altenburg, T.M. Bioelectrical impedance analysis to estimate body composition in children and adolescents: A systematic review and evidence appraisal of validity, responsiveness, reliability and measurement error. Obes. Rev. 2013, 14, 895–905. [Google Scholar] [CrossRef] [PubMed]
- Kyle, U.G.; Earthman, C.P.; Pichard, C.; Coss-Bu, J.A. Body composition during growth in children: Limitations perspectives of bioelectrical impedance, analysis. Eur. J. Clin. Nutr. 2015, 69, 1298–1305. [Google Scholar] [CrossRef] [PubMed]
- Kabiri, L.S.; Hernandez, D.C.; Mitchell, K. Reliability, Validity, and Diagnostic Value of a Pediatric Bioelectrical Impedance Analysis Scale. Child. Obes. 2015, 11, 650–655. [Google Scholar] [CrossRef] [PubMed]
- Dehghan, M.; Merchant, A.T. Is bioelectrical impedance accurate for use in large epidemiological studies? Nutr. J. 2008, 7, 26. [Google Scholar] [CrossRef] [PubMed]
- Sim, P.Y.; Su, T.T.; Abd Majid, H.; Nahar, A.M.; Jalaludin, M.Y. A comparison study of portable foot-to-foot bioelectrical impedance scale to measure body fat percentage in Asian adults and children. Biomed. Res. Int. 2014, 2014, 475659. [Google Scholar] [CrossRef] [PubMed]
- Wells, J.C.; Fuller, N.J.; Dewit, O.; Fewtrell, M.S.; Elia, M.; Cole, T.J. Four-component model of body composition in children: Density and hydration of fat-free mass and comparison with simpler models. Am. J. Clin. Nutr. 1999, 69, 904–912. [Google Scholar] [CrossRef] [PubMed]
- Goldfield, G.S.; Cloutier, P.; Mallory, R.; Prud’homme, D.; Parker, T.; Doucet, E. Validity of foot-to-foot bioelectrical impedance analysis in overweight and obese children and parents. J. Sports Med. Phys. Fit. 2006, 46, 447–453. [Google Scholar] [PubMed]
- Verney, J.; Metz, L.; Chaplais, E.; Cardenoux, C.; Pereira, B.; Thivel, D. Bioelectrical impedance is an accurate method to assess body composition in obese but not severely obese adolescents. Nutr. Res. 2016, 36, 663–670. [Google Scholar] [CrossRef] [PubMed]
- Ramirez-Velez, R.; Correa-Bautista, J.E.; Martinez-Torres, J.; Gonzalez-Ruiz, K.; Gonzalez-Jimenez, E.; Schmidt-RioValle, J.; Garcia-Hermoso, A. Performance of Two Bioelectrical Impedance Analyses in the Diagnosis of Overweight and Obesity in Children and Adolescents: The FUPRECOL Study. Nutrients 2016, 8, 575. [Google Scholar] [CrossRef] [PubMed]
- Slaughter, M.H.; Lohman, T.G.; Boileau, R.A.; Horswill, C.A.; Stillman, R.J.; Van Loan, M.D.; Bemben, D.A. Skinfold equations for estimation of body fatness in children and youth. Hum. Biol. 1988, 60, 709–723. [Google Scholar] [PubMed]
- Rodriguez, G.; Moreno, L.A.; Blay, M.G.; Blay, V.A.; Fleta, J.; Sarria, A.; Bueno, M. Body fat measurement in adolescents: Comparison of skinfold thickness equations with dual-energy X-ray absorptiometry. Eur. J. Clin. Nutr. 2005, 59, 1158–1166. [Google Scholar] [CrossRef] [PubMed]
- Yeung, D.C.; Hui, S.S. Validity and reliability of skinfold measurement in assessing body fatness of Chinese children. Asia Pac. J. Clin. Nutr. 2010, 19, 350–357. [Google Scholar] [PubMed]
- Radley, D.; Gately, P.J.; Cooke, C.B.; Carroll, S.; Oldroyd, B.; Truscott, J.G. Percentage fat in overweight and obese children: Comparison of DXA and air displacement plethysmography. Obes. Res. 2005, 13, 75–85. [Google Scholar] [CrossRef] [PubMed]
- Lazzer, S.; Bedogni, G.; Agosti, F.; De Col, A.; Mornati, D.; Sartorio, A. Comparison of dual-energy X-ray absorptiometry, air displacement plethysmography and bioelectrical impedance analysis for the assessment of body composition in severely obese Caucasian children and adolescents. Br. J. Nutr. 2008, 100, 918–924. [Google Scholar] [CrossRef] [PubMed]
- Eisenkölbl, J.; Kartasurya, M.; Widhalm, K. Underestimation of percentage fat mass measured by bioelectrical impedance analysis compared to dual energy X-ray absorptiometry method in obese children. Eur. J. Clin. Nutr. 2001, 55, 423–429. [Google Scholar] [CrossRef] [PubMed]
- Lazzer, S.; Boirie, Y.; Meyer, M.; Vermorel, M. Which alternative method to dual-energy X-ray absorptiometry for assessing body composition in overweight and obese adolescents? Arch. Pediatr. 2005, 12, 1094–1101. [Google Scholar] [CrossRef] [PubMed]
- Sluyter, J.D.; Schaaf, D.; Scragg, R.K.R.; Plank, L.D. Prediction of fatness by standing 8-electrode bioimpedance: A multiethnic adolescent population. Obesity (Silver Spring) 2010, 18, 183–189. [Google Scholar] [CrossRef] [PubMed]
- Nightingale, C.M.; Rudnicka, A.R.; Owen, C.G.; Donin, A.S.; Newton, S.L.; Furness, C.A.; Howard, E.L.; Gillings, R.D.; Wells, J.C.K.; Cook, D.G.; et al. Are ethnic and gender specific equations needed to derive fat free mass from bioelectrical impedance in children of South asian, black african-Caribbean and white European origin? Results of the assessment of body composition in children study. PLoS ONE 2013, 8, e76426. [Google Scholar] [CrossRef] [PubMed]
- Deurenberg, P.; Deurenberg-Yap, M. Validity of body composition methods across ethnic population groups. Forum. Nutr. 2003, 56, 299–301. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez-Ruiz, K.; Correa-Bautista, J.E.; Izquierdo, M.; Garcia-Hermoso, A.; Dominguez-Sanchez, M.A.; Bustos-Cruz, R.H.; Garcia-Prieto, J.C.; Martinez-Vizcaino, V.; Lobelo, F.; Gonzalez-Jimenez, E.; et al. Effects of an exercise program on hepatic metabolism, hepatic fat, and cardiovascular health in overweight/obese adolescents from Bogota, Colombia (the HEPAFIT study): Study protocol for a randomized controlled trial. Trials 2018, 19, 330. [Google Scholar] [CrossRef] [PubMed]
- Cole, T.J.; Lobstein, T. Extended international (IOTF) body mass index cut-offs for thinness, overweight and obesity. Pediatr. Obes. 2012, 7, 284–294. [Google Scholar] [CrossRef] [PubMed]
- Cameron, N. The Methods of Auxological Anthropology; Springer: New York, NY, USA, 1978; Volume 3, pp. 35–90. [Google Scholar]
- Marfell-Jones, M.; Olds, T.; Stewart, A. International Standards for Anthropometric Assessment; International Society for the Advancement of Kinanthropometry: Potchefstroom, South Africa, 2011; ISBN 0620362073. [Google Scholar]
- Bousbiat, S.; Jaffrin, M.Y.; Dongmo, E. Comparison of body fat-free masses calculated from hand-to-foot and foot-to-foot resistances with DXA measurements. Med. Biol. Eng. Comput. 2011, 49, 1329–1336. [Google Scholar] [CrossRef] [PubMed]
- Thurlow, S.; Taylor-Covill, G.; Sahota, P.; Oldroyd, B.; Hind, K. Effects of procedure, upright equilibrium time, sex and BMI on the precision of body fluid measurements using bioelectrical impedance analysis. Eur. J. Clin. Nutr. 2018, 72, 148–153. [Google Scholar] [CrossRef] [PubMed]
- Bosy-Westphal, A.; Schautz, B.; Later, W.; Kehayias, J.J.; Gallagher, D.; Muller, M.J. What makes a BIA equation unique? Validity of eight-electrode multifrequency BIA to estimate body composition in a healthy adult population. Eur. J. Clin. Nutr. 2013, 67 (Suppl. 1), S14–S21. [Google Scholar] [CrossRef] [PubMed]
- Barreira, T.V.; Staiano, A.E.; Katzmarzyk, P.T. Validity assessment of a portable bioimpedance scale to estimate body fat percentage in white and African-American children and adolescents. Pediatr. Obes. 2013, 8, e29–e32. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Hui, S.S.-C. Validity of Four Commercial Bioelectrical Impedance Scales in Measuring Body Fat among Chinese Children and Adolescents. Biomed. Res. Int. 2015, 2015, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Helba, M.; Binkovitz, L.A. Pediatric body composition analysis with dual-energy X-ray absorptiometry. Pediatr. Radiol. 2009, 39, 647–656. [Google Scholar] [CrossRef] [PubMed]
- Lohman, T.G.; Zhao, C. Human Body Composition, 2nd ed.; Heymsfield, S.B., Lohman, T.G., Wang, Z., Going, S.B.E., Eds.; Human Kinetics: Champaign, IL, USA, 2005. [Google Scholar]
- Janz, K.F.; Nielsen, D.H.; Cassady, S.L.; Cook, J.S.; Wu, Y.T.; Hansen, J.R. Cross-validation of the Slaughter skinfold equations for children and adolescents. Med. Sci. Sports. Exerc. 1993, 25, 1070–1076. [Google Scholar] [CrossRef] [PubMed]
- Truesdale, K.P.; Roberts, A.; Cai, J.; Berge, J.M.; Stevens, J. Comparison of Eight Equations That Predict Percent Body Fat Using Skinfolds in American Youth. Child. Obes. 2016, 12, 314–323. [Google Scholar] [CrossRef] [PubMed]
- Addo, O.Y.; Himes, J.H. Reference curves for triceps and subscapular skinfold thicknesses in US children and adolescents. Am. J. Clin. Nutr. 2010, 91, 635–642. [Google Scholar] [CrossRef] [PubMed]
- Ramírez-Vélez, R.; Rodrigues-Bezerra, D.; Correa-Bautista, J.E.; Izquierdo, M.; Lobelo, F. Reliability of health-related physical fitness tests among Colombian children and adolescents: The Fuprecol study. PLoS ONE 2015, 10, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Mirwald, R.L.; Baxter-Jones, A.D.G.; Bailey, D.A.; Beunen, G.P. An assessment of maturity from anthropometric measurements. Med. Sci. Sports. Exerc. 2002, 34, 689–694. [Google Scholar] [PubMed]
- Tanner, J.M.; Whitehouse, R.H. Clinical longitudinal standards for height, weight, height velocity, weight velocity, and stages of puberty. Arch. Dis. Child. 1976, 51, 170–179. [Google Scholar] [CrossRef] [PubMed]
- Bland, J.M.; Altman, D.G. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1986, 1, 307–310. [Google Scholar] [CrossRef]
- Lin, L.I. A concordance correlation coefficient to evaluate reproducibility. Biometrics 1989, 45, 255–268. [Google Scholar] [CrossRef] [PubMed]
- Leahy, S.; O’Neill, C.; Sohun, R.; Jakeman, P. A comparison of dual energy X-ray absorptiometry and bioelectrical impedance analysis to measure total and segmental body composition in healthy young adults. Eur J. Appl. Physiol. 2012, 112, 589–595. [Google Scholar] [CrossRef] [PubMed]
- Wan, C.S.; Ward, L.C.; Halim, J.; Gow, M.L.; Ho, M.; Briody, J.N.; Leung, K.; Cowell, C.T.; Garnett, S.P. Bioelectrical impedance analysis to estimate body composition, and change in adiposity, in overweight and obese adolescents: Comparison with dual-energy x-ray absorptiometry. BMC Pediatr. 2014, 14, 249. [Google Scholar] [CrossRef] [PubMed]
- Lazzer, S.; Boirie, Y.; Meyer, M.; Vermorel, M. Evaluation of two foot-to-foot bioelectrical impedance analysers to assess body composition in overweight and obese adolescents. Br. J. Nutr. 2003, 90, 987. [Google Scholar] [CrossRef] [PubMed]
- Deurenberg, P. Limitations of the bioelectrical impedance method for the assessment of body fat in severe obesity. Am. J. Clin. Nutr. 1996, 64, 449S–452S. [Google Scholar] [CrossRef] [PubMed]
- Forbes, G.B. Human Body Composition; Springer: New York, NY, USA, 1987; ISBN 978-1-4612-4654-1. [Google Scholar]
- Schoeller, D.A. Changes in total body water with age. Am. J. Clin. Nutr. 1989, 50, 1175–1176. [Google Scholar] [CrossRef] [PubMed]
- Waki, M.; Kral, J.G.; Mazariegos, M.; Wang, J.; Pierson, R.N.J.; Heymsfield, S.B. Relative expansion of extracellular fluid in obese vs. nonobese women. Am. J. Physiol. 1991, 261, E199–E203. [Google Scholar] [CrossRef] [PubMed]
- Battistini, N.; Virgili, F.; Severi, S.; Brambilla, P.; Manzoni, P.; Beccaria, L.; Chiumello, G. Relative expansion of extracellular water in obese vs. normal children. J. Appl. Physiol. 1995, 79, 94–96. [Google Scholar] [CrossRef] [PubMed]
- Lukaski, H.C. Evolution of bioimpedance: A circuitous journey from estimation of physiological function to assessment of body composition and a return to clinical research. Eur. J. Clin. Nutr. 2013, 67, S2–S9. [Google Scholar] [CrossRef] [PubMed]
- Lukaski, H.C.; Kyle, U.G.; Kondrup, J. Assessment of adult malnutrition and prognosis with bioelectrical impedance analysis. Curr. Opin. Clin. Nutr. Metab. Care 2017, 20, 330–339. [Google Scholar] [CrossRef] [PubMed]
- Purnell, J. Definitions, Classification, and Epidemiology of Obesity; MDText.com, Inc.: South Dartmouth, MA, USA, 2000. Available online: https://www.ncbi.nlm.nih.gov/books/NBK279167/ (accessed on 13 August 2018).
- Freedman, D.S.; Horlick, M.; Berenson, G.S. A comparison of the Slaughter skinfold-thickness equations and BMI in predicting body fatness and cardiovascular disease risk factor levels in children1-4. Am. J. Clin. Nutr. 2013, 98, 1417–1424. [Google Scholar] [CrossRef] [PubMed]
- Shaikh, M.G.; Crabtree, N.J.; Shaw, N.J.; Kirk, J.M.W. Body fat estimation using bioelectrical impedance. Horm. Res. 2007, 68, 8–10. [Google Scholar] [CrossRef] [PubMed]
- Watts, K.; Naylor, L.H.; Davis, E.A.; Jones, T.W.; Beeson, B.; Bettenay, F.; Siafarikas, A.; Bell, L.; Ackland, T.; Green, D.J. Do skinfolds accurately assess changes in body fat in obese children and adolescents? Med. Sci. Sports Exerc. 2006, 38, 439–444. [Google Scholar] [CrossRef] [PubMed]
- Cumberledge, E.A.; Myers, C.; Venditti, J.J.; Dixon, C.B.; Andreacci, J.L. The Effect of the Menstrual Cycle on Body Composition Determined by Contact-Electrode Bioelectrical Impedance Analyzers. Int. J. Exerc. Sci. 2018, 11, 625–632. [Google Scholar] [PubMed]
- McKee, J.E.; Cameron, N. Bioelectrical impedance changes during the menstrual cycle. Am. J. Hum. Biol. 1997, 9, 155–161. [Google Scholar] [CrossRef]
| Characteristics | Boys | Girls | p-Value |
|---|---|---|---|
| (n= 42) | (n = 85) a | ||
| Chronological age (years) | 12.9 (1.2) | 13.7 (1.7) | 0.003 |
| Age of PHV (years) | 12.3 (0.6) | 14.4 (0.6) | 0.001 |
| Weight (kg) | 57.3 (9.4) | 57.7 (10.4) | 0.829 |
| Height (cm) | 154.8 (8.4) | 155.9 (7.5) | 0.486 |
| Sitting height (cm) | 77.2 (4.5) | 81.1 (4.2) | <0.001 |
| Body mass index (kg/m2) | 24.2 (2.5) | 23.5 (4.1) | 0.359 |
| Overweight+obese prevalence (%) * | 41.1 | 55.9 | 0.066 |
| BF > 30% by DXA prevalence (%) * | 97.6 | 100 | 0.997 |
| z-BMI | 1.73 (0.64) | 1.39 (0.85) | 0.013 |
| Pubertal stage, (genital maturity I to V) (%) * | 0.0/43.9/24.4/26.8/4.9 | 0.0/3.5/25.9/48.2/22.4 | 0.001 |
| Pubertal stage (pubic hair I to V) (%) * | 2.4/46.3/29.3/19.5/2.4 | 8.2/20.0/27.1/31.8/12.9 | 0.001 |
| Waist circumference (cm) | 79.4 (6.8) | 74.6 (8.4) | 0.009 |
| Body fat percentage | |||
| BF% by DXA | 38.0 (4.6) | 40.8 (4.1) | 0.001 |
| BF% by Seca® mBCA 514 | 23.4 (6.2) | 32.3 (5.8) | <0.001 |
| BF% by Tanita® BC 420MA | 24.0 (6.4) | 29.5 (6.0) | <0.001 |
| BF% by skinfold-thickness equations | 29.0 (7.3) | 29.8 (5.8) | 0.510 |
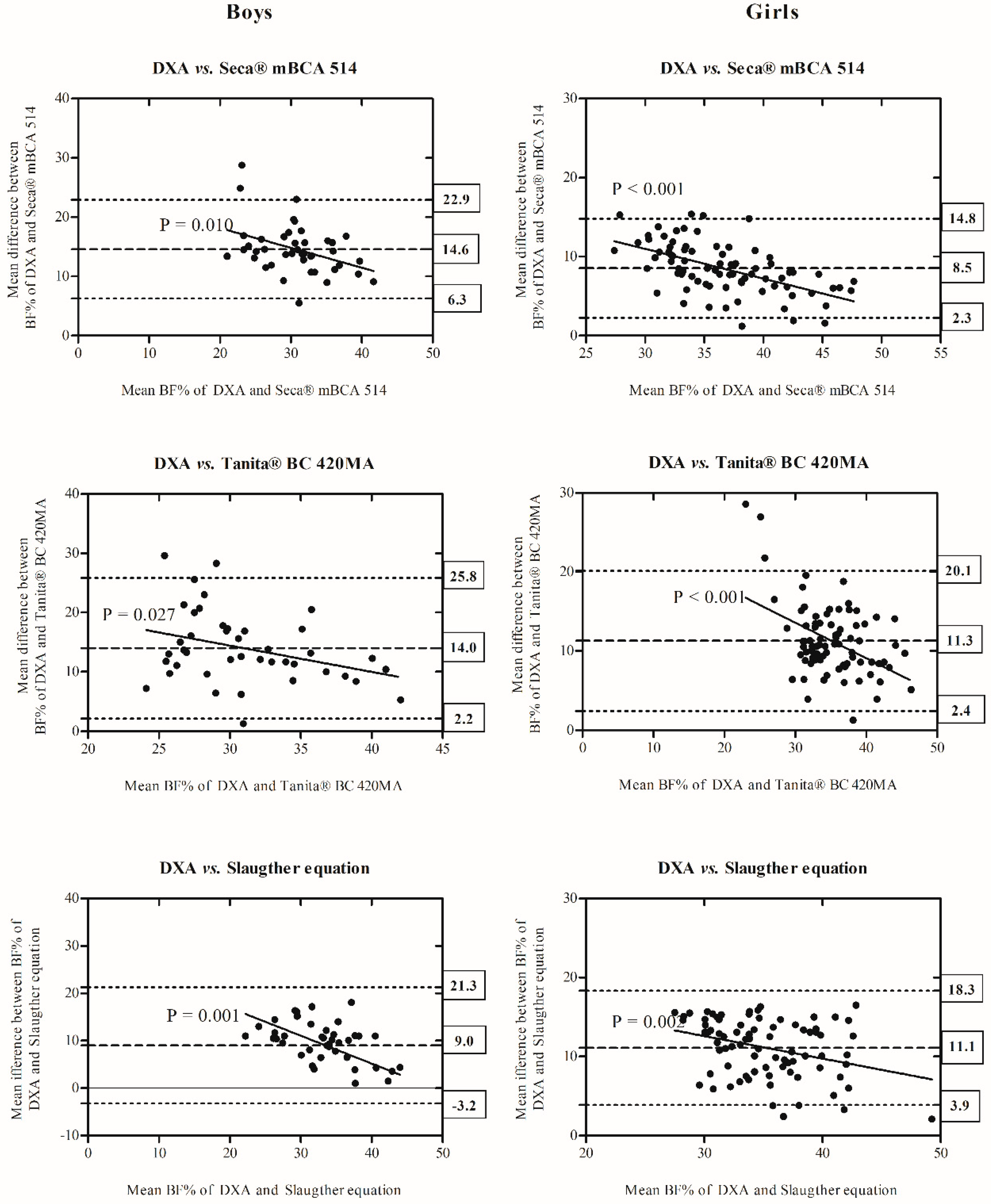
| Boys (n = 42) | |||||
| DXA vs. Seca® mBCA 514 | DXA vs. Tanita® BC 420MA | DXA vs. Slaughter equations | |||
| BF% (95% CI) | ρc (95% CI) | BF% (95% CI) | ρc (95% CI) | BF% (95% CI) | ρc (95% CI) |
| 14.6 * | 0.149 | 14.0 * | 0.096 | 9.0 * | 0.227 |
| (13.3–15.9) | (0.078–0.218) | (12.1–15.9) | (0.023–0.168) | (12.1–11.0) | (0.092–0.353) |
| Girls (n = 85) a | |||||
| DXA vs. Seca® mBCA 514 | DXA vs. Tanita® BC 420MA | DXA vs. Slaughter equations | |||
| BF% (95% CI) | ρc (95% CI) | BF% (95% CI) | ρc (95% CI) | BF% (95% CI) | ρc (95% CI) |
| 8.5 * | 0.323 | 11.3 * | 0.175 | 11.1 * | 0.179 |
| (7.8–9.3) | (0.241–0.400) | (10.3–12.3) | (0.112–0.237) | (10.3–11.9) | (0.119–0.238) |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
González-Ruíz, K.; Medrano, M.; Correa-Bautista, J.E.; García-Hermoso, A.; Prieto-Benavides, D.H.; Tordecilla-Sanders, A.; Agostinis-Sobrinho, C.; Correa-Rodríguez, M.; Schmidt Rio-Valle, J.; González-Jiménez, E.; et al. Comparison of Bioelectrical Impedance Analysis, Slaughter Skinfold-Thickness Equations, and Dual-Energy X-ray Absorptiometry for Estimating Body Fat Percentage in Colombian Children and Adolescents with Excess of Adiposity. Nutrients 2018, 10, 1086. https://doi.org/10.3390/nu10081086
González-Ruíz K, Medrano M, Correa-Bautista JE, García-Hermoso A, Prieto-Benavides DH, Tordecilla-Sanders A, Agostinis-Sobrinho C, Correa-Rodríguez M, Schmidt Rio-Valle J, González-Jiménez E, et al. Comparison of Bioelectrical Impedance Analysis, Slaughter Skinfold-Thickness Equations, and Dual-Energy X-ray Absorptiometry for Estimating Body Fat Percentage in Colombian Children and Adolescents with Excess of Adiposity. Nutrients. 2018; 10(8):1086. https://doi.org/10.3390/nu10081086
Chicago/Turabian StyleGonzález-Ruíz, Katherine, María Medrano, Jorge Enrique Correa-Bautista, Antonio García-Hermoso, Daniel Humberto Prieto-Benavides, Alejandra Tordecilla-Sanders, César Agostinis-Sobrinho, María Correa-Rodríguez, Jacqueline Schmidt Rio-Valle, Emilio González-Jiménez, and et al. 2018. "Comparison of Bioelectrical Impedance Analysis, Slaughter Skinfold-Thickness Equations, and Dual-Energy X-ray Absorptiometry for Estimating Body Fat Percentage in Colombian Children and Adolescents with Excess of Adiposity" Nutrients 10, no. 8: 1086. https://doi.org/10.3390/nu10081086
APA StyleGonzález-Ruíz, K., Medrano, M., Correa-Bautista, J. E., García-Hermoso, A., Prieto-Benavides, D. H., Tordecilla-Sanders, A., Agostinis-Sobrinho, C., Correa-Rodríguez, M., Schmidt Rio-Valle, J., González-Jiménez, E., & Ramírez-Vélez, R. (2018). Comparison of Bioelectrical Impedance Analysis, Slaughter Skinfold-Thickness Equations, and Dual-Energy X-ray Absorptiometry for Estimating Body Fat Percentage in Colombian Children and Adolescents with Excess of Adiposity. Nutrients, 10(8), 1086. https://doi.org/10.3390/nu10081086







