Post-Exercise Whole Body Cryotherapy (−140 °C) Increases Energy Intake in Athletes
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Experimental Overview
2.3. Experimental Protocol in WBC Trial and CON Trial
2.4. Measurements
2.4.1. Blood Parameters
2.4.2. Subjective Feelings of Appetite, Fatigue, and Muscle Soreness
2.4.3. Respiratory Parameters
2.4.4. Skin Temperature
2.4.5. Ad Libitum Buffet Meal
2.5. Statistical Analysis
3. Results
3.1. Exercise Performance
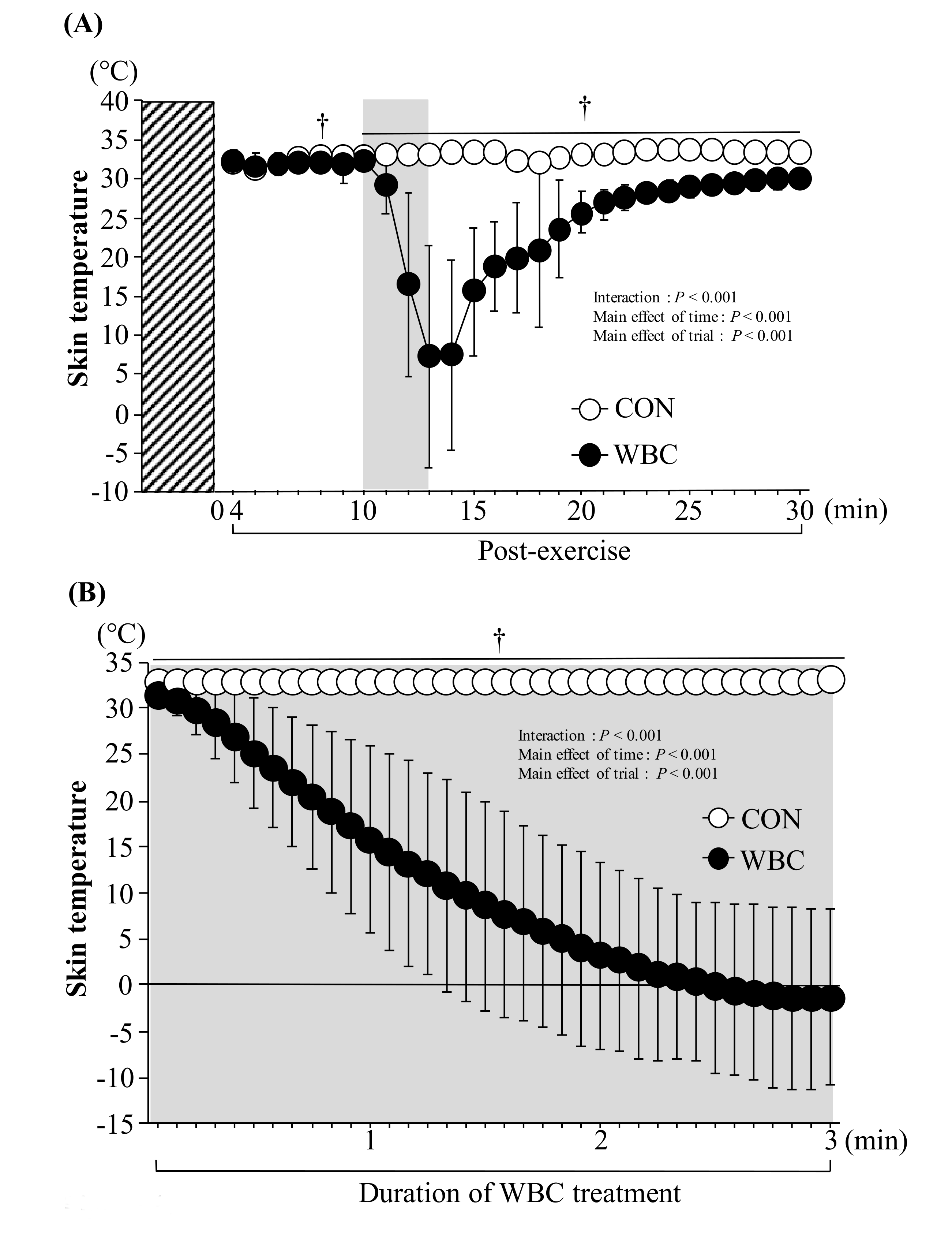
3.2. Skin Temperature
3.3. Ratings of Appetite, Fatigue and Muscle Soreness
3.4. Respiratory Parameters and Heart Rate
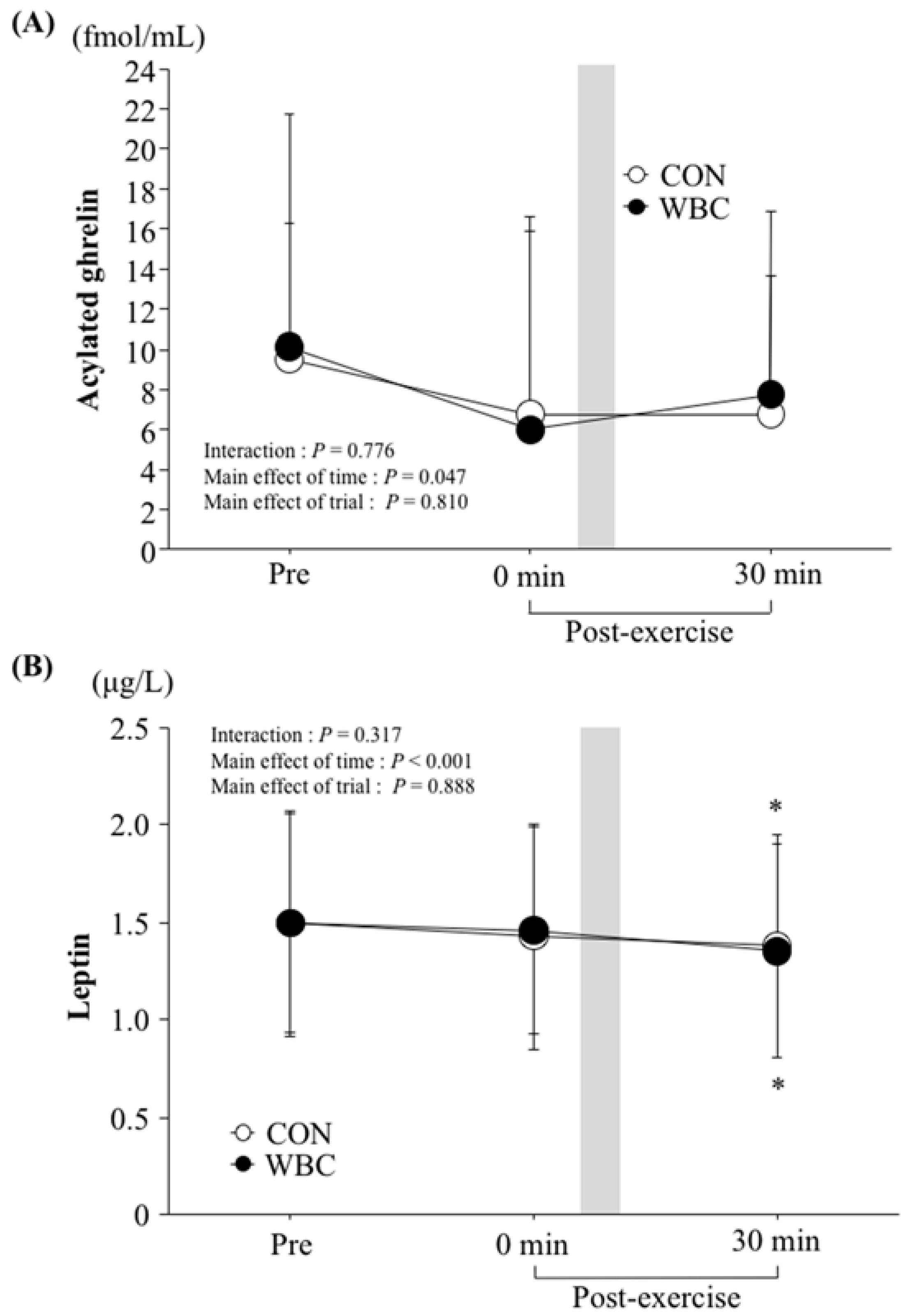
3.5. Blood Parameters
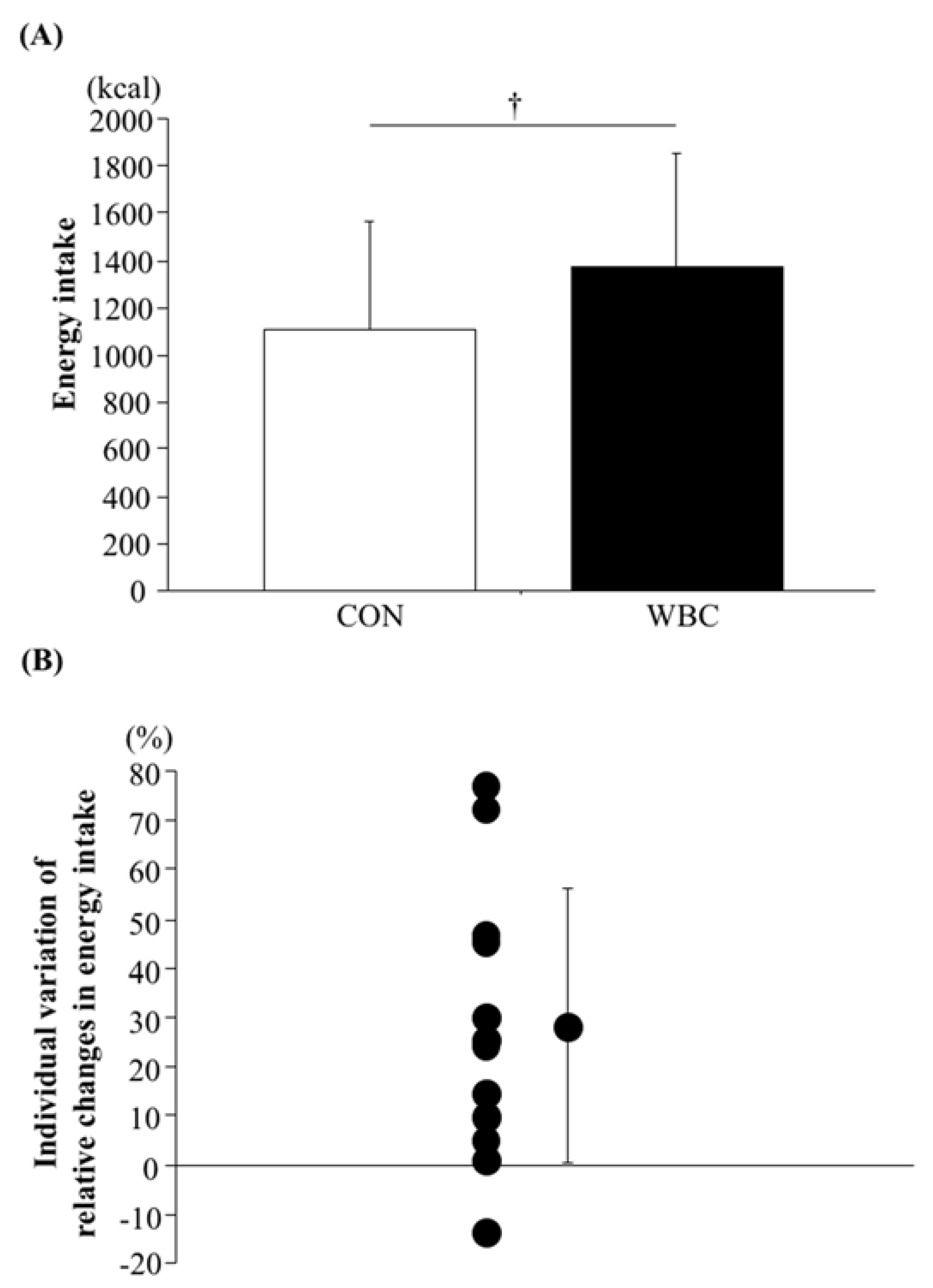
3.6. Energy and Macronutrient Intakes
4. Discussion
4.1. Appetite-Regulating Hormones Following WBC
4.2. Other Potential Mechanisms to Promote Energy Intake Following WBC
4.3. Limitations
4.4. Perspectives
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- King, J.A.; Miyashita, M.; Wasse, L.K.; Stensel, D.J. Influence of prolonged treadmill running on appetite, energy intake and circulating concentrations of acylated ghrelin. Appetite 2010, 54, 492–498. [Google Scholar] [CrossRef] [PubMed]
- Ueda, S.Y.; Yoshikawa, T.; Katsura, Y.; Usui, T.; Fujimoto, S. Comparable effects of moderate intensity exercise on changes in anorectic gut hormone levels and energy intake to high intensity exercise. J. Endocrinol. 2009, 203, 357–364. [Google Scholar] [CrossRef] [PubMed]
- Sim, A.Y.; Wallman, K.E.; Fairchild, T.J.; Guelfi, K.J. High-intensity intermittent exercise attenuates ad-libitum energy intake. Int. J. Obes. 2014, 38, 417–422. [Google Scholar] [CrossRef] [PubMed]
- Schubert, M.M.; Desbrow, B.; Sabapathy, S.; Leveritt, M. Acute exercise and subsequent energy intake. A meta-analysis. Appetite 2013, 63, 92–104. [Google Scholar] [CrossRef] [PubMed]
- King, N.A.; Burley, V.J.; Blundell, J.E. Exercise-induced suppression of appetite: effects on food intake and implications for energy balance. Eur. J. Clin. Nutr. 1994, 48, 715–724. [Google Scholar] [PubMed]
- Kojima, M.; Kangawa, K. Ghrelin: structure and function. Physiol. Rev. 2005, 85, 495–522. [Google Scholar] [CrossRef] [PubMed]
- Batterham, R.L.; Cowley, M.A.; Small, C.J.; Herzog, H.; Cohen, M.A.; Dakin, C.L.; Wren, A.M.; Brynes, A.E.; Low, M.J.; Ghatei, M.A.; et al. Gut hormone PYY3-36 physiologically inhibits food intake. Nature 2002, 418, 650–654. [Google Scholar] [CrossRef] [PubMed]
- Kreymann, B.; Ghatei, M.A.; Williams, G.; Bloom, S.R. Glucagon-like peptide-1 7-36: a physiological incretin in man. Lancet 1987, 330, 1300–1304. [Google Scholar] [CrossRef]
- Kojima, C.; Ishibashi, A.; Ebi, K.; Goto, K. The Effect of a 20 km Run on Appetite Regulation in Long Distance Runners. Nutrients 2016, 8, 672. [Google Scholar] [CrossRef] [PubMed]
- Kojima, C.; Kasai, N.; Ishibashi, A.; Murakami, Y.; Ebi, K.; Goto, K. Appetite regulations after sprint exercise under hypoxic condition in female athletes. J. Strength Cond. Res. 2017. [Google Scholar] [CrossRef] [PubMed]
- Howe, S.; Hand, T.; Larson-Meyer, D.; Austin, K.; Alexander, B.; Manore, M. No Effect of Exercise Intensity on Appetite in Highly-Trained Endurance Women. Nutrients 2016, 8, 223. [Google Scholar] [CrossRef] [PubMed]
- White, L.J.; Dressendorfer, R.H.; Holland, E.; McCoy, S.C.; Ferguson, M.A. Increased Caloric Intake Soon after Exercise in Cold Water. Int. Sport Nutr. Exerc. Metab. 2005, 15, 38–47. [Google Scholar] [CrossRef]
- King, J.A.; Wasse, L.K.; Stensel, D.J. The Acute Effects of Swimming on Appetite, Food Intake, and Plasma Acylated Ghrelin. J. Obes. 2011, 2011, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Crabtree, D.R.; Blannin, A.K. Effects of exercise in the cold on Ghrelin, PYY, and food intake in overweight adults. Med. Sci. Sports Exerc. 2015, 47, 49–57. [Google Scholar] [CrossRef] [PubMed]
- Kojima, C.; Sasaki, H.; Tsuchiya, Y.; Goto, K. The influence of environmental temperature on appetite-related hormonal responses. J. Physiol. Anthropol. 2015, 34, 22. [Google Scholar] [CrossRef] [PubMed]
- Wasse, L.K.; King, J.A.; Stensel, D.J.; Sunderland, C. Effect of ambient temperature during acute aerobic exercise on short-term appetite, energy intake, and plasma acylated ghrelin in recreationally active males. Appl. Physiol. Nutr. Metab. 2013, 38, 905–909. [Google Scholar] [CrossRef] [PubMed]
- Halse, R.E.; Wallman, K.E.; Guelfi, K.J. Postexercise Water Immersion Increases Short-Term Food Intake in Trained Men. Med. Sci. Sports Exerc. 2011, 43, 632–638. [Google Scholar] [CrossRef] [PubMed]
- Tomasik, P.J.; Sztefko, K.; Pizon, M. The Effect of Short-term Cold and Hot Exposure on Total Plasma Ghrelin Concentrations in Humans. Horm. Metab. Res. 2005, 37, 189–190. [Google Scholar] [CrossRef] [PubMed]
- Zeyl, A.; Stocks, J.M.; Taylor, N.A.S.; Jenkins, A.B. Interactions between temperature and human leptin physiology in vivo and in vitro. Eur. J. Appl. Physiol. 2004, 92, 571–578. [Google Scholar] [CrossRef] [PubMed]
- Pournot, H.; Bieuzen, F.; Louis, J.; Mounier, R.; Fillard, J.R.; Barbiche, E.; Hausswirth, C. Time-course of changes in inflammatory response after whole-body cryotherapy multi exposures following severe exercise. PLoS ONE 2011, 6, e22748. [Google Scholar] [CrossRef]
- Ferreira-Junior, J.B.; Bottaro, M.; Loenneke, J.P.; Vieira, A.; Vieira, C.A.; Bemben, M.G. Could whole-body cryotherapy (below −100°C) improve muscle recovery from muscle damage? Front. Physiol. 2014, 5, 509. [Google Scholar] [CrossRef] [PubMed]
- Hausswirth, C.; Louis, J.; Bieuzen, F.; Pournot, H.; Fournier, J.; Filliard, J.R.; Brisswalter, J. Effects of whole-body cryotherapy vs. far-infrared vs. passive modalities on recovery from exercise-induced muscle damage in highly-trained runners. PLoS ONE 2011, 6, e27749. [Google Scholar] [CrossRef] [PubMed]
- Banfi, G.; Melegati, G.; Barassi, A.; Dogliotti, G.; Melzi d’Eril, G.; Dugué, B.; Corsi, M.M. Effects of whole-body cryotherapy on serum mediators of inflammation and serum muscle enzymes in athletes. J. Therm. Biol. 2009, 34, 55–59. [Google Scholar] [CrossRef]
- Fonda, B.; Sarabon, N. Effects of whole-body cryotherapy on recovery after hamstring damaging exercise: A crossover study. Scand. J. Med. Sci. Sports 2013, 23, e270–e278. [Google Scholar] [CrossRef] [PubMed]
- Mila-Kierzenkowska, C.; Jurecka, A.; Woźniak, A.; Szpinda, M.; Augustyńska, B.; Woźniak, B. The Effect of Submaximal Exercise Preceded by Single Whole-Body Cryotherapy on the Markers of Oxidative Stress and Inflammation in Blood of Volleyball Players. Oxid. Med. Cell Longev. 2013, 2013, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Kasai, N.; Kojima, C.; Sumi, D.; Takahashi, H.; Goto, K.; Suzuki, Y. Impact of 5 Days of Sprint Training in Hypoxia on Performance and Muscle Energy Substances. Int. J. Sports Med. 2017, 38, 983–991. [Google Scholar] [CrossRef] [PubMed]
- Klimek, A.; Lubkowska, A.; Szyguła, Z.; Chudecka, M.; Frączek, B. Influence of the ten sessionsof the whole body cryostimulationon aerobic and anaerobic capacity. Int. J. Occup. Med. Environ. Health 2010, 23, 181–189. [Google Scholar] [CrossRef] [PubMed]
- Vieira, A.; Bottaro, M.; Ferreira-Junior, J.B.; Vieira, C.; Cleto, V.A.; Cadore, E.L.; Simões, H.G.; Do Carmo, J.; Brown, L.E. Does whole-body cryotherapy improve vertical jump recovery following a high-intensity exercise bout? Open Access J. Sports Med. 2015, 6, 49–54. [Google Scholar] [CrossRef] [PubMed]
- Kraemer, W.J.; Bush, J.A.; Wickham, R.B.; Denegar, C.R.; Gómez, A.L.; Gotshalk, L.A.; Duncan, N.D.; Volek, J.S.; Putukian, M.; Sebastianelli, W.J. Influence of Compression Therapy on Symptoms Following Soft Tissue Injury from Maximal Eccentric Exercise. J. Orthop. Sports Phys. Ther. 2001, 31, 282–290. [Google Scholar] [CrossRef] [PubMed]
- Flint, A.; Raben, A.; Blundell, J.E.; Astrup, A. Reproducibility, power and validity of visual analogue scales in assessment of appetite sensations in single test meal studies. Int. J. Obes. 2000, 24, 38–48. [Google Scholar] [CrossRef]
- Charlot, K.; Faure, C.; Antoine-Jonville, S. Influence of Hot and Cold Environments on the Regulation of Energy Balance Following a Single Exercise Session: A Mini-Review. Nutrients 2017, 9, 592. [Google Scholar] [CrossRef] [PubMed]
- Schaal, K.; Le Meur, Y.; Bieuzen, F.; Petit, O.; Hellard, P.; Toussaint, J.F.; Hausswirth, C. Effect of recovery mode on postexercise vagal reactivation in elite synchronized swimmers. Appl. Physiol. Nutr. Metab. 2013, 38, 126–133. [Google Scholar] [CrossRef] [PubMed]
- Hausswirth, C.; Schaal, K.; Le Meur, Y.; Bieuzen, F.; Filliard, J.R.; Volondat, M.; Louis, J. Parasympathetic Activity and Blood Catecholamine Responses Following a Single Partial-Body Cryostimulation and a Whole-Body Cryostimulation. PLoS ONE 2013, 8, e72658. [Google Scholar] [CrossRef] [PubMed]
- Shibahara, N.; Matsuda, H.; Umeno, K.; Shimada, Y.; Itoh, T.; Terasawa, K. The responses of skin blood flow, mean arterial pressure and R-R interval induced by cold stimulation with cold wind and ice water. J. Auton. Nerv. Syst. 1996, 61, 109–115. [Google Scholar] [CrossRef]
- Pump, B.; Shiraishi, M.; Gabrielsen, A.; Bie, P.; Christensen, N.J.; Norsk, P. Cardiovascular effects of static carotid baroreceptor stimulation during water immersion in humans. Am. J. Physiol. Heart Circ. Physiol. 2001, 280, H2607–H2615. [Google Scholar] [CrossRef] [PubMed]
- Horner, K.M.; Schubert, M.M.; Desbrow, B.; Byrne, N.M.; King, N.A. Acute Exercise and Gastric Emptying: A Meta-Analysis and Implications for Appetite Control. Sports Med. 2015, 45, 659–678. [Google Scholar] [CrossRef] [PubMed]
- Hazell, T.J.; Islam, H.; Townsend, L.K.; Schmale, M.S.; Copeland, J.L. Effects of exercise intensity on plasma concentrations of appetite-regulating hormones: Potential mechanisms. Appetite 2016, 98, 80–88. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Kondo, T.; Suzukamo, Y.; Oouchida, Y.; Izumi, S.-I. Vagal Nerve Regulation Is Essential for the Increase in Gastric Motility in Response to Mild Exercise. Tohoku J. Exp. Med. 2010, 222, 155–163. [Google Scholar] [CrossRef] [PubMed]
- Howe, S.; Hand, T.; Manore, M. Exercise-Trained Men and Women: Role of Exercise and Diet on Appetite and Energy Intake. Nutrients 2014, 6, 4935–4960. [Google Scholar] [CrossRef] [PubMed]
- Krüger, M.; de Mareés, M.; Dittmar, K.H.; Sperlich, B.; Mester, J. Whole-body cryotherapy's enhancement of acute recovery of running performance in well-trained athletes. Int. J. Sports Physiol. Perform. 2015, 10, 605–612. [Google Scholar] [CrossRef] [PubMed]
| Pre | Post-Exercise | After Meal | Interaction (Trial × Time) | Main Effect | |||||
|---|---|---|---|---|---|---|---|---|---|
| 0 Min | 15 Min | 30 Min | Trial | Time | |||||
| Fatigue (mm) | WBC | 25 ± 20 | 87 ± 10 * | 49 ± 25 * | 48 ± 16 * | 43 ± 15 * | 0.288 | 0.058 | <0.001 |
| CON | 29 ± 17 | 87 ± 11 * | 65 ± 19 * | 59 ± 19 * | 49 ± 18 * | ||||
| Muscle soreness (mm) | WBC | 28 ± 22 | 56 ± 25 * | 34 ± 17 | 37 ± 13 | 37 ± 15 | 0.210 | 0.032 | <0.001 |
| CON | 33 ± 22 | 66 ± 20 * | 54 ± 18 *,† | 48 ± 19 † | 42 ± 20 | ||||
| Hunger (mm) | WBC | 66 ± 14 | 24 ± 15 * | 47 ± 16 * | 59 ± 20 | 9 ± 9 * | 0.422 | 0.912 | <0.001 |
| CON | 66 ± 17 | 30 ± 18 * | 42 ± 18 * | 55 ± 16 | 13 ± 10 * | ||||
| Fullness (mm) | WBC | 17 ± 16 | 44 ± 29 * | 33 ± 19 | 24 ± 15 | 91 ± 8 * | 0.005 | 0.881 | <0.001 |
| CON | 16 ± 13 | 50 ± 25 * | 40 ± 22 * | 30 ± 18 | 76 ± 23 *,† | ||||
| Prospective food consumption (mm) | WBC | 63 ± 16 | 26 ± 21 * | 44 ± 18 * | 54 ± 19 | 12 ± 11 * | 0.631 | 0.740 | <0.001 |
| CON | 62 ± 17 | 30 ± 17 * | 42 ± 19 * | 53 ± 18 | 19 ± 15 * | ||||
| WBC | CON | p | |
|---|---|---|---|
| O2 (mL/min) | 349 ± 42 | 362 ± 48 | 0.196 |
| CO2 (mL/min) | 201 ± 55 | 240 ± 55 † | 0.007 |
| E (L/min) | 11.3 ± 3.4 | 14.0 ± 4.2 † | 0.016 |
| HR beats per minute (bpm) | 95 ± 11 | 101 ± 8 † | 0.042 |
| Pre | Post-Exercise | Interaction (Trial × Time) | Main Effect | ||||
|---|---|---|---|---|---|---|---|
| 0 Min | 30 Min | Trial | Time | ||||
| Glucose (mmol/L) | WBC | 5.0 ± 0.3 | 5.6 ± 2.4 * | 5.1 ± 1.4 | 0.498 | 0.252 | 0.004 |
| CON | 4.8 ± 0.4 | 6.0 ± 1.3 * | 4.8 ± 1.1 | ||||
| Lactate (mmol/L) | WBC | 1.4 ± 0.3 | 20.5 ± 2.8 * | 10.9 ± 2.5 * | 0.871 | 0.995 | <0.001 |
| CON | 1.4 ± 0.4 | 20.3 ± 2.4 * | 11.0 ± 2.4 * | ||||
| Insulin (pmol/L) | WBC | 44 ± 8 | 125 ± 40 * | 72 ± 66 | 0.518 | 0.748 | <0.001 |
| CON | 40 ± 14 | 129 ± 36 * | 64 ± 40 | ||||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kojima, C.; Kasai, N.; Kondo, C.; Ebi, K.; Goto, K. Post-Exercise Whole Body Cryotherapy (−140 °C) Increases Energy Intake in Athletes. Nutrients 2018, 10, 893. https://doi.org/10.3390/nu10070893
Kojima C, Kasai N, Kondo C, Ebi K, Goto K. Post-Exercise Whole Body Cryotherapy (−140 °C) Increases Energy Intake in Athletes. Nutrients. 2018; 10(7):893. https://doi.org/10.3390/nu10070893
Chicago/Turabian StyleKojima, Chihiro, Nobukazu Kasai, Chika Kondo, Kumiko Ebi, and Kazushige Goto. 2018. "Post-Exercise Whole Body Cryotherapy (−140 °C) Increases Energy Intake in Athletes" Nutrients 10, no. 7: 893. https://doi.org/10.3390/nu10070893
APA StyleKojima, C., Kasai, N., Kondo, C., Ebi, K., & Goto, K. (2018). Post-Exercise Whole Body Cryotherapy (−140 °C) Increases Energy Intake in Athletes. Nutrients, 10(7), 893. https://doi.org/10.3390/nu10070893





