Ibero–American Consensus on Low- and No-Calorie Sweeteners: Safety, Nutritional Aspects and Benefits in Food and Beverages
Abstract
1. Introduction: Justification and Need of the Ibero–American Consensus
2. Safety of LNCS and Monitoring Systems
2.1. Background
2.2. International Regulatory Bodies
2.3. Acceptable Daily Intake
2.4. Regulation at National Level
2.4.1. Mercosur
2.4.2. Chile
2.4.3. México
2.4.4. Ecuador
2.4.5. Peru
2.4.6. Canada
2.5 Key Points: Safety of LNCS and Monitoring Systems
- LNCS are some of the most extensively evaluated dietary substances.
- The safety of approved compounds is proven and is continuously re-evaluated to consider new and relevant scientific data.
- The safety of LNCS such as aspartame, cyclamate and saccharin has been reviewed and re-affirmed several times by the US FDA and by EFSA, who recently completed a full risk assessment of aspartame [51].
- Since taste and food application profiles among LNCS can vary, the use of LNCS blends can be important for developing lower-sugar finished food products.
3. Food Composition and Nutrition Labelling for LNCS
3.1. Background
3.2. FCT and LNCS
3.3. Key Points: Food Composition and Nutrition Labelling for LNCS
- It seems necessary to prepare a comparison table for the Ibero–American countries to include the different labelling regulations at present, highlighting strengths and weaknesses.
- It seems critical and urgent to unify the terminology used for LNCS, with special focus on the consumer information.
- The labelling must be clear and precise.
- The use of new technologies to expand the information in the printed label is also encouraged for LNCS.
- Consumer education about additive products must be strengthened in a rigorous, objective way, based on the best scientific evidence and regulatory processes.
- Responsible Administrations and Scientific societies should disseminate clear, objective information about LNCS on their websites and social networks and publish educational materials that contribute to the dismissal of doubts and any misinformation that may exist. This may reinforce the information in the labelling and expansion, as well as trust by the consumers.
- Training provided to primary care and specialized healthcare and educational professionals should be made a priority, in order to be able to explain benefits/risks for the LNCS to the consumer, and labelling content.
4. LNCS Role in Body Weight Management and in Chronic Diseases
4.1. Background
4.2. Observational Studies
4.3. Intervention Studies
- (a)
- Short-term RCTs. Tordoff and Alleva (1990) [99] provided soft drinks sweetened with LNCS or sugar or without any kind of LNCS (controls) to young male and female adults (BMI ≥ 25 kg/m2; n = 30) during three periods of 21 sequential days. All subjects received any subsequent order of the three modalities. Drinks were to be added to their normal daily diet, and the subjects were instructed to consume four bottles of 300 mL daily. The daily caloric load represented by the soft drinks sweetened with sugar was 530 kcal, with 3 kcal/day provided by soft drink sweetened with LNCS. The participants were instructed to make a daily record of their intake keeping a weekly report of their body weight. Analysis of the information indicated that the group with sugary drinks experienced a small but significant weight gain while the LNCS group showed no weight gain. The LNCS group showed no compensatory increase in intake.In a 10-week trial conducted by Raben et al., (2002) [100], healthy males and females aged from 20 to 50 years and with a BMI of 25 to 30 kg/m2 were recruited. They were assigned to one of two groups: the first received foods and drinks containing LNCS (n = 20) and the other received equivalent products but sweetened with sucrose (n = 21). About 80% of the supplements were liquids. At the end of the trial, those consuming supplements with LNCS did not show changes in energy intake or macronutrient composition and did not gain weight. In contrast, the group with sucrose supplements, as it is to be expected, increased caloric intake by 10%, increasing weight and fat percentage significantly.
- (b)
- Mid- and long-term RCTs. Theoretically, long-term studies represent the ideal scenario for studying complex phenomena such as weight change or the incidence of metabolic variables. Longer duration studies have been performed on “outpatient” subjects, without being confined to a controlled research facility. The disadvantage is that the researcher does not have complete control of the subject’s diet.Studies of more than 6 months duration for weight loss comparing foods or beverages sweetened with sugars contrasting them with their equivalents sweetened with LNCS replacing sugars generally show discreet but consistent and significant benefits in the reduction of weight for the LNCS equivalents [100]. In other trials, of the same or longer duration, using water as a comparator vs. drinks with LNCS, has yielded inconsistent results. That is, adding drinks “on top of” a plan for weight reduction, using either water or LNCS beverages (but without replacing sugars) some studies show a slight advantage in weight loss with water [101,102], and in others the advantage in weight reduction is reported in the group using beverages with LNCS [91]. It is possible that the effect of reduction in weight by adding liquids (either water or sweetened beverages with LNCS) depends more on the caloric restriction (of food in general) than on the effect of the non-caloric liquid accompanying or added to the diet. One of the longest studies identified was a 3-years old trial conducted by Blackburn et al. [103], which evaluated the use of LNCS in association with a program of weight loss and its maintenance. The sample consisted of 163 women with obesity (83 women completed the final phase of the study). At the end of the period of active maintenance (week 71), women belonging to the group with LNCS (aspartame) inclusion in the diet plan, showed a weight regain of 2.6 kg while the group that was allowed sugars had regained 5.4 kg. At the end of the second year of follow-up (week 175) subjects in the LNCS group regained 5.1 kg (keeping a 5% reduction with respect to their baseline weight loss) while the control group recovered all the weight lost initially, and ended up with their baseline weight.
- (c)
- Systematic reviews with meta-analyses. Two recent meta-analyses, Miller and Pérez, 2014 [83] and Rogers et al., 2016 [84], analysed published clinical trials, reporting a minimal but favourable effect of LNCS reducing weight when used within a nutrition program replacing sugars. These systematic reviews and meta-analyses examined RCTs from very short term (1 day) to longer trials like those mentioned above, as well as observational studies. In Rogers et al., [84] all different types of studies were examined including animal and human intervention and observational studies, making this publication a very thorough review of the current literature. However, in 2017 Azad et al., published a new systematic review with meta-analysis of both RCTs and also prospective cohort studies [77]. This review only included studies of more than 6 months duration. This meta-analysis according to the authors “cannot support benefits of LNCS for the management of weight loss”. Inconsistent conclusions from available systematic reviews and their meta-analyses may result from including RCT’s developed to answer different research questions and/or experimental design.
4.4. Diabetes and Other Chronic Conditions
4.5. Key Points: LNCS Role in Body Weight Management and in Chronic Diseases
- The ad libitum consumption of LNCS, without being used to replace sugar/ reduce calorie intake from sugar, shows inconsistent results, i.e., seems to have no beneficial or detrimental effect on body weight.
- The use of LNCS in programs of weight reduction, replacing sucrose or simple sugars by LNCS may favour weight loss and weight maintenance. These “programs” should consider structured diet plans, (possibly monitored by healthcare professionals) as we well as an active, healthy lifestyle that includes a sensible, balanced diet and regular physical activity.
- LNCS-use in diabetic patient control programmes may contribute to better glycaemic control.
- Observational studies investigating the impact of LNCS on health outcomes should implement more robust intake assessments that facilitate the determination of overall LNCS intake, as well as intakes of individual LNCS. A potential approach may be to implement a biomarker approach [97].
- All results of observational studies must be considered in the light of evidence from intervention and safety research studies where biological outcomes can be measured directly.
5. Dietary Guidelines for LNCS
5.1. Background
5.2. Key Points: Dietary Guidelines for LNCS
- Dialogue with food and beverage manufacturers is required to discuss product reformulation to reduce the consumption of added sugars and/or replace total or partial content of sugar by LNCS.
- Given that sugars have many functional roles other than simply sweetening the product, reformulating with LNCS alone is unlikely to be appropriate for all types of products; therefore, other strategies to reduce free sugars intake such as reducing portion sizes should be considered in conjunction with reformulation.
- Many dietary guidelines and recommendations have been designed for adults only. It is recommended to prepare guidelines, with recommendations stratified for different age groups, with particular consideration for children and adolescents.
- Although there are no toxicological/safety concern or legal cut-off for children younger than 6 years, the consumption of foods and beverages with LNCS is unadvised within the context of education and sweet taste perception. LNCS however can be recommended in younger children with specific health conditions (diabetes, overweight, severe tooth decay history or any other condition where sugar intake restrictions is need).
- Foods and beverages containing LNCS can be recommended to replace foods and beverages with added sugars for patients with diabetes, dyslipidaemia, obesity or cardiovascular diseases.
- The use of LNCS is safe by pregnant women provided intakes do not exceed recommended intakes.
- Advice for lactating women is similar to that for pregnant women. Relevant local cultural aspects regarding recommendations for lactation and complementary feeding should be carefully considered.
6. Food and Nutrition Education and Consumer Behaviour
6.1. Background
6.2. Key Points: Food and Nutrition Education and Consumer Behaviour
- Consumers often find multiple sources of information on food and health issues, which do not always provide quality, transparent, sufficiently contrasted, and reliable information. In addition, the increasing use of new technologies and social networks favour the rapid diffusion and exchange of information, not all of which is reliable.
- It is necessary to facilitate access to information that is of proven quality, evidence-based, transparent, and easy-to-understand by the general public, to support warranted recommendations for their use.
- Sensory education, identification and recognition of flavours, taste, aroma and texture of foods and beverages plays a very important role in food education, which should be enhanced both in the family and in educational settings from early ages. In this context, recognizing the high preference for sweet taste, it would be desirable to educate the preference for lower sweetness intensity. This measure would be desirable both as an educational strategy during childhood, as in-patient’s education and dietary counselling.
- Continuing education of health professionals is required, since they are a source of reference information on issues related to food and health, for both the general population and patients. In this sense, the publication of positioning statements and consensus documents in academic reference publications may be adequate and convenient.
- It may also be appropriate to disseminate information through periodical bulletins, professional forums, scientific meetings, congresses and other regular communication channels established by scientific and professional societies in different health-related fields.
- Accredited reference websites can be interesting media, both to reach consumers and practitioners.
7. Conclusions and Key Messages
- Safety of LNCS and monitoring systems: LNCS are some of the most extensively evaluated substances in the human food chain. The safety of currently used LNCS has been reviewed and confirmed by health regulatory agencies globally, such as the FDA and EFSA.
- Food composition and nutrition labelling for LNCS: Consumer education about these products must be strengthened in a rigorous, objective way, based on the best scientific evidence and regulatory processes.
- LNCS role in body weight management and chronic diseases: The use of LNCS in programs of weight reduction replacing sucrose or simple sugars by LNCS may favour the reduction of excess weight and maintenance of weight loss in the context of structured diet plans. Furthermore, their use in diabetes control programme, replacing sucrose or simple sugars, may contribute to a better glycaemic control. These substances also provide dental health benefits.
- Dietary guidelines for LNCS: It is suggested that foods and beverages with LNCS are included as alternative options to sugar use in dietary guidelines.
- Food and nutrition education and consumer behaviour: Since health professionals are an important source of information for both the general population and patients on issues related to food and health, continuing education on the safety of and the regulatory processes around LNCS this group is necessary. In this sense, the publication of positioning statements and consensus documents in academic reference publications is highly desirable.
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Floros, J.D.; Newsome, R.; Fisher, W.; Barbosa-Cánovas, G.V.; Chen, H.; Dunne, C.P.; German, J.B.; Hall, R.L.; Heldman, D.R.; Karwe, M.V.; et al. Feeding the World Today and Tomorrow: The Importance of Food Science and Technology. Compr. Rev. Food Sci. Food Saf. 2010, 9, 572–599. [Google Scholar] [CrossRef]
- European Union (EU). European Parliament and Council Directive 94/35/EC of 30 June 1994 on Sweeteners for Use in Foodstuffs. Available online: http://eur-lex.europa.eu/legal-content/EN/TXT/HTML/?uri=CELEX:31994L0035&from=EN (accessed on 18 March 2018).
- European Union (EU). Regulation (EC) No 1333/2008 of the European Parliament and of the Council of 16 December 2008 on Food Additives. Available online: http://data.europa.eu/eli/reg/2008/1333/oj (accessed on 18 March 2018).
- European Union. Regulation (EU) No. 497/2014 Amending Annex II to Regulation (EC) No. 1333/2008 of the European Parliament and of the Council and the Annex to Commission Regulation No. 231/2012 as Regards the Use of Advantame as a Sweetener. Available online: http://eur-lex.europa.eu/legal-content/EN/TXT/?uri=CELEX%3A32014R0497 (accessed on 18 March 2018).
- European Union (EU). Commission Regulation (EU) No 257/2010 of 25 March 2010 Setting Up a Programme for the Re-Evaluation of Approved Food Additives in Accordance with Regulation (EC) No 1333/2008 of the European Parliament and of the Council on Food Additives. Available online: http://data.europa.eu/eli/reg/2010/257/oj (accessed on 18 March 2018).
- Reuber, M.D. Carcinogenicity of Saccharin. Environ. Health Perspect. 1978, 25, 173–200. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Cohen, S.M.; Cano, M.; Earl, R.A.; Carson, S.D.; Garland, E.M. A proposed role for silicates and protein in the proliferative effects of saccharin on the male rat urothelium. Carcinogenesis 1991, 12, 1551–1555. [Google Scholar] [PubMed]
- Chappel, C.I. A review and biological risk assessment of sodium saccharin. Regul. Toxicol. Pharmacol. 1992, 15, 253–270. [Google Scholar] [CrossRef]
- Whysner, J.; Williams, G.M. Saccharin mechanistic data and risk assessment: Urine composition, enhanced cell proliferation, and tumor promotion. Pharmacol. Ther. 1996, 71, 225–252. [Google Scholar] [CrossRef]
- U.S. Department of Health and Human Services. 14th Report on Carcinogens, National Toxicology Program’s Report on Carcinogens. 2016. Available online: https://ntp.niehs.nih.gov/pubhealth/roc/index-1.html#A (accessed on 18 March 2018).
- Lohner, S.; Toews, I.; Meerpohl, J.J. Health outcomes of non-nutritive sweeteners: Analysis of the research landscape. Nutr. J. 2017, 16, 55. [Google Scholar] [CrossRef] [PubMed]
- Fitch, C.; Keim, K.S. Academy of Nutrition and Dietetics. Position of the Academy of Nutrition and Dietetics: Use of nutritive and nonnutritive sweeteners. J. Acad. Nutr. Diet. 2012, 112, 739–758. [Google Scholar] [CrossRef] [PubMed]
- Gardner, C.; Wylie-Rosett, J.; Gidding, S.S.; Steffen, L.M.; Johnson, R.K.; Reader, D.; Lichtenstein, A.H.; American Heart Association Nutrition Committee of the Council on Nutrition; Physical Activity and Metabolism; Council on Arteriosclerosis; et al. Nonnutritive sweeteners: Current use and health perspectives: A scientific statement from the American Heart Association and the American Diabetes Association. Circulation 2012, 126, 509–519. [Google Scholar] [CrossRef] [PubMed]
- US Department of Health and Human Services. Scientific Report of the 2015 Dietary Guidelines Advisory Committee. Added Sugars and Low-Calorie Sweeteners. Available online: https://health.gov/dietaryguidelines/2015-scientific-report/11-chapter-6/d6-3.asp (accessed on 19 November 2017).
- Institutes of Medicine (IoM). Nutrition Standards for Foods in Schools: Leading the Way toward Healthier Youth; National Academies Press: Washington, DC, USA, 2007. [Google Scholar]
- Joint FAO/WHO Expert Committee of Food Additives (JECFA). Toxicological Evaluation of Certain Food Additives with a Review of General Principles and Specifications; WHO: Geneva, Switzerland, 1974. [Google Scholar]
- Martyn, D.; Darch, M.; Roberts, A.; Lee, H.Y.; Yaqiong Tian, T.; Kaburagi, N.; Belmar, P. Low-/No-Calorie Sweeteners: A Review of Global Intakes. Nutrients 2018, 10, 357. [Google Scholar] [CrossRef] [PubMed]
- Sylvetsky, A.C.; Rother, K.I. Trends in the consumption of low-calorie sweeteners. Physiol. Behav. 2016, 164 Pt B, 446–450. [Google Scholar] [CrossRef] [PubMed]
- Serra-Majem, L.; Riobó Serván, P.; Belmonte Cortés, S.; Anadón Navarro, A.; Aranceta Bartrina, J.; Franco Vargas, E.; García-Closas, R.; Gómez-Candela, C.; Herrero Sancho, E.; La Vecchia, C.; et al. Chinchón declaration; decalogue on low- and no-calorie sweeteners (LNCS). Nutr. Hosp. 2014, 29, 719–734. [Google Scholar] [CrossRef] [PubMed]
- WHO. Incentives and Disincentives for Reducing Sugar in Manufactured Foods. An Exploratory Supply Chain Analysis; A Set of Insights for Member States in the Context of the WHO European Food and Nutrition Action Plan 2015–2020; World Health Organisation Regional Office for Europe: København, Denmark, 2017. [Google Scholar]
- Magnuson, B.A.; Carakostas, M.C.; Moore, N.H.; Poulos, S.P.; Renwick, A.G. Biological Fate of low-calorie sweeteners. Nutr. Rev. 2016, 74, 670–689. [Google Scholar] [CrossRef] [PubMed]
- O’Brien-Nabors, L. Alternative Sweeteners, 4th ed.; CRC Press: Boca Raton, FL, USA, 2012; ISBN 978-1439846148. [Google Scholar]
- Emerton, V.; Choi, E. Essential Guide to Food Additives, 3rd ed.; Leatherhead Publishing: Surrey, UK, 2008; ISBN 9781905224500. [Google Scholar]
- Codex Alimentarius Commission (CAC). Procedural Manual: Joint FAO/WHO Food Standards Programme, 18th ed.; Food and Agricultural Organisation of the United Nations: Rome, Italy, 2008. [Google Scholar]
- General Standard for Food Additives (GSFA). 2010. Available online: http://www.fao.org/gsfaonline/index.html (accessed on 18 September 2017).
- European Food Safety Authority (EFSA). Guidance for Submission for Food Additive Evaluations. EFSA Panel on Food Additives and Nutrient Sources Added to Food (ANS), 2012. Available online: https://www.efsa.europa.eu/en/efsajournal/pub/2760 (accessed on 16 November 2017).
- European Food Safety Authority (EFSA). Commission Regulation (EU) 2017/228 Amending Regulation (EC) No 178/2002 of the European Parliament and of the Council as Regards the Names and the Areas of Competence of the Scientific Panels of the European Food Safety Authority. 2017. Available online: http://www.efsa.europa.eu/en/aboutefsa.htm (accessed on 16 November 2017).
- European Food Safety Authority (EFSA). Sweeteners. Health Claims Related to Intense Sweeteners. 2011. Available online: https://www.efsa.europa.eu/en/topics/topic/sweeteners (accessed on 18 September 2017).
- Carocho, M.; Morales, P.; Ferreira, I.C.F.R. Sweeteners as food additives in the XXI century: A review of what is known, and what is to come. Food Chem. Toxicol. 2017, 107, 302–317. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, H. Sweeteners and Sugar Alternatives in Food Technology; Blackwell Publishing: Oxford, UK, 2006; ISBN 9781405134347. [Google Scholar]
- Otabe, A.; Fujieda, T.; Masuyama, T. Evaluation of the teratogenic potential of N-[N-[3-(3-hydroxy-4-methoxyphenyl) propyl]-α-aspartyl]-l-phenylalanine 1-methyl ester, monohydrate (advantame) in the rat and rabbit. Food Chem. Toxicol. 2011, 49, S60–S69. [Google Scholar] [CrossRef] [PubMed]
- Varzakas, T.; Labropoulos, A.; Anestis, S. Sweeteners, Nutritional Aspects, Applications, and Production Technology; CRC Press: Boca Raton, FL, USA, 2012. [Google Scholar]
- European Union. Regulation (EU) No 231/2012 of 9 March 2012 Laying Down Specifications for Food Additives Listed in Annexes II and III to Regulation (EC) No 1333/2008 of the European Parliament and of the Council. Available online: https://publications.europa.eu/en/publication-detail/-/publication/a42dd9b2-b63f-438b-a790-1fa5995b7d41 (accessed on 18 March 2018).
- European Commission (EC). Opinion of the Scientific Committee on Food on Sucralose. September 2000. Available online: https://ec.europa.eu/food/sites/food/files/safety/docs/sci-com_scf_out68_en.pdf (accessed on 18 March 2018).
- European Food Safety Authority (EFSA). Scientific Opinion of the Panel on Food Additives, Flavourings, Processing Aids and Materials in Contact with Food on a request from European Commission on Neotame as a sweetener and flavour enhancer. EFSA J. 2007, 581, 1–43. [Google Scholar]
- European Food Safety Authority (EFSA). Panel on Food Additives and Nutrient Sources Added to Food, 2015. Scientific Opinion on the safety of the extension of use of thaumatin (E 957). EFSA J. 2015, 13, 4290. [Google Scholar] [CrossRef]
- Rulis, A.M.; Levitt, J.A. FDA’s food ingredient approval process. Safety assurance based on scientific assessment. Regul. Toxicol. Pharmacol. 2009, 53, 20–31. [Google Scholar] [CrossRef] [PubMed]
- Food and Drug Administration (FDA). Substances Generally Recognised as Safe; [Docket No. 97N-0103]; Federal Register 74; FDA: Silver Spring, MD, USA, 1997; pp. 18937–18964.
- Roberts, A. The safety and regulatory process for low calorie sweeteners in the United States. Physiol. Behav. 2016, 164 Pt B, 439–444. [Google Scholar] [CrossRef] [PubMed]
- U.S. Department of Health and Human Services; Food and Drug Administration; Center for Food Safety and Applied Nutrition. Redbook 2000. Toxicological Principles for the Safety Assessment of Direct Food Additives and Color Additives Used in Food. Available online: https://www.fda.gov/Food/GuidanceRegulation/GuidanceDocumentsRegulatoryInformation/IngredientsAdditivesGRASPackaging/ucm078044.htm (accessed on 19 September 2017).
- Young, F.E. Report in Response to Questions on the Sweetener, Aspartame; Report from US Commissioner of Food and Drug to Senator John Heinz; US Senate: Washington, DC, USA, 1985.
- Frank, P.; Ottoboni, M.A. The Dose Makes the Poison: A Plain Language Guide to Toxicology, 3rd ed.; John Wiley & Sons: Hoboken, NJ, USA, 2011; ISBN 978-0470381120. [Google Scholar]
- International Programme on Chemical Safety (IPCS). Principles for the Safety Assessment of Food Additives and Contaminants in Food. 1987. Available online: http://www.inchem.org/documents/ehc/ehc/ehc70.htm#PartNumber:2 (accessed on 18 September 2017).
- MERCOSUR Technical Regulation. MERCOSUR/GMC/RES. N° 11/06. Harmonized General List of Food Additives and Their Functional Classes. 2006. Available online: http://servicios.infoleg.gob.ar/infolegInternet/anexos/115000-119999/118978/norma.htm (accessed on 10 January 2018).
- Ministerio de Salud de Chile (MINSAL). Reglamento Sanitario de los Alimentos de Chile. 2015. Available online: http://web.minsal.cl/sites/default/files/files/DECRETO_977_96%20actualizado%20a%20Enero%202015.pdf (accessed on 30 January 2018).
- Comisión Federal para la Protección contra Riesgos Sanitarios (COFEPRIS). List of Sweeteners with an Established ADI. Health Secretary, United States of Mexico, 2012. Available online: http://www.cofepris.gob.mx/MJ/Documents/AcuerdosSecretario/acaditivo160712.pdf (accessed on 10 January 2018).
- Comisión Federal para la Protección contra Riesgos Sanitarios (COFEPRIS). List of Sweeteners with an Established ADI. Health Secretary, United States of Mexico, 2017. Available online: https://www.gob.mx/cofepris/documentos/anexo-vii (accessed on 10 January 2018).
- Norma Técnica Ecuatoriana. NTE INEN 2074 (2012) (Spanish): Aditivos Alimentarios Permitidos Para Consumo Humano. Listas Positivas, Requisitos. Available online: https://ia801900.us.archive.org/35/items/ec.nte.2074.2012/ec.nte.2074.2012.pdf (accessed on 10 January 2018).
- Instituto Nacional de Calidad-INACAL. Normas Técnicas: Aditivos Alimentarios. Edulcorantes, Clasificación; Código NTP 209.703:2012; Instituto Nacional de Calidad-INACAL: Lima, Perú, 2012. [Google Scholar]
- Health Canada. List of Permitted Sweeteners. Government of Canada, 2016. Available online: https://www.canada.ca/en/health-canada/services/food-nutrition/food-safety/food-additives/lists-permitted/9-sweeteners.html (accessed on 10 January 2018).
- European Food Safety Authority (EFSA). EFSA Explains the Safety of Aspartame. Scientific Opinion on Aspartame. 2013. Available online: http://www.efsa.europa.eu/en/topics/topic/aspartame (accessed on 16 November 2017).
- European Union (EU). Regulation (EU) No. 1169/2011 of the European Parliament and of the Council of 25 October 2011 on the Provision of Food Information to Consumers. Available online: http://eur-lex.europa.eu/legal-content/en/ALL/?uri=CELEX:32011R1169 (accessed on 10 January 2018).
- Tennant, D.R.; Bruyninckx, C. The potential application of European market research data in dietary exposure modelling of food additives. Food Addit. Contam. Part A Chem. Anal. Control Expo. Risk Assess. 2018, 35, 412–424. [Google Scholar] [CrossRef] [PubMed]
- Le Donne, C.; Catasta, G.; Ferrari, M.; Hearty, A.; Connolly, A.; Leclercq, C. Use of market share data to select food products for an occurrence survey on flavourings in eight EU countries within the FACET project. Int. J. Food Sci. Nutr. 2013, 64, 768–779. [Google Scholar] [CrossRef] [PubMed]
- FACET Consortium. Final Report Summary-FACET (Flavours, Additives and Food Contact Material Exposure Task). Available online: https://cordis.europa.eu/result/rcn/45323_en.html (accessed on 12 January 2018).
- Huvaere, K.; Vandevijvere, S.; Hasni, M.; Vinkx, C.; Van Loco, J. Dietary intake of artificial sweeteners by the Belgian population. Food Addit. Contam. Part A Chem. Anal. Control Expo. Risk Assess. 2012, 29, 54–65. [Google Scholar] [CrossRef] [PubMed]
- Martyn, D.M.; Nugent, A.P.; McNulty, B.A.; O’Reilly, E.; Tlustos, C.; Walton, J.; Flynn, A.; Gibney, M.J. Dietary intake of four artificial sweeteners by Irish pre-school children. Food Addit. Contam. Part A Chem. Anal. Control Expo. Risk Assess. 2016, 33, 592–602. [Google Scholar] [CrossRef] [PubMed]
- Buffini, M.; Goscinny, S.; Van Loco, J.; Nugent, A.P.; Walton, J.; Flynn, A.; Gibney, M.J.; McNulty, B.A. Dietary intakes of six intense sweeteners by Irish adults. Food Addit. Contam. Part A Chem. Anal. Control Expo. Risk Assess. 2017, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Le Donne, C.; Mistura, L.; Goscinny, S.; Janvier, S.; Cuypers, K.; D’Addezio, L.; Sette, S.; Catasta, G.; Ferrari, M.; Piccinelli, R.; et al. Assessment of dietary intake of 10 intense sweeteners by the Italian population. Food Chem. Toxicol. 2017, 102, 186–197. [Google Scholar] [CrossRef] [PubMed]
- Sylvetsky, A.C.; Dietz, W.H. Nutrient-content claims—Guidance or cause for confusion? N. Engl. J. Med. 2014, 371, 195–198. [Google Scholar] [CrossRef] [PubMed]
- Canadian Food Inspection Agency. Guide to Food Labelling and Advertising; Supplementary Information on Specific Products; Canadian Food Inspection Agency: Ottawa, ON, Canada, 2011. [Google Scholar]
- Gortmaker, S.L.; Story, M.; Powell, L.M.; Krebs-Smith, S.M. Building infrastructure to document the U.S. food stream. Am. J. Prev. Med. 2013, 44, 192–193. [Google Scholar] [CrossRef] [PubMed]
- WHO. Diet, Nutrition and the Prevention of Chronic Diseases: Report of a WHO Study Group; WHO Technical Report Series 797; World Health Organisation: Geneva, Switzerland, 1990; Available online: http://www.who.int/nutrition/publications/obesity/WHO_TRS_797/en/ (accessed on 17 September 2017).
- WHO/FAO. Diet, Nutrition and the Prevention of Chronic Diseases: Report of a Joint WHO/FAO Expert Consultation; WHO Technical Report Series, No. 916; World Health Organisation: Geneva, Switzerland, 2003; Available online: http://whqlibdoc.who.int/trs/WHO_TRS_916.pdf (accessed on 17 September 2017).
- World Cancer Research Fund (WCRF). Recommendations for Cancer Prevention; WCRF: London, UK, 2007. [Google Scholar]
- Yang, Q. Gain weight by “going diet?” Artificial sweeteners and the neurobiology of sugar cravings: Neuroscience 2010. Yale J. Biol. Med. 2010, 83, 101–108. [Google Scholar] [PubMed]
- Fowler, S.P. Low-calorie sweetener use and energy balance: Results from experimental studies in animals, and large-scale prospective studies in humans. Physiol. Behav. 2016, 164, 517–523. [Google Scholar] [CrossRef] [PubMed]
- Swithers, S.E.; Davidson, T.L. A role for sweet taste: Calorie predictive relations in energy regulation by rats. Behav. Neurosci. 2008, 122, 161–173. [Google Scholar] [CrossRef] [PubMed]
- Rogers, P.J. The role of low-calorie sweeteners in the prevention and management of overweight and obesity: Evidence v. conjecture. Proc. Nutr. Soc. 2017, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Fujimaru, T.; Park, J.H.; Lim, J. Sensory characteristics and relative sweetness of tagatose and other sweeteners. J. Food Sci. 2012, 77, S323–S328. [Google Scholar] [CrossRef] [PubMed]
- Magnuson, B.A.; Burdock, G.A.; Doull, J.; Kroes, R.M.; Marsh, G.M.; Pariza, M.W.; Spencer, P.S.; Waddell, W.J.; Walker, R.; Williams, G.M. Aspartame: A Safety Evaluation Based on Current Use Levels, Regulations, and Toxicological and Epidemiological Studies. Crit. Rev. Toxicol. 2007, 37, 629–727. [Google Scholar] [CrossRef] [PubMed]
- Chattopadhyay, S.; Raychaudhuri, U.; Chakraborty, R. Artificial sweeteners—A review. J. Food. Sci. Technol. 2014, 51, 611–621. [Google Scholar] [CrossRef] [PubMed]
- Beauchamp, G.K.; Mennella, J.A. Flavor Perception in Human Infants: Development and Functional Significance. Digestion 2011, 83 (Suppl. 1), 1–6. [Google Scholar] [CrossRef] [PubMed]
- Drewnowski, A.; Mennella, J.A.; Johnson, S.L.; Bellisle, F. Sweetness and food preference. J. Nutr. 2012, 142, 1142S–1148S. [Google Scholar] [CrossRef] [PubMed]
- Bellisle, F.; Drewnowski, A.; Anderson, G.H.; Westerterp-Plantenga, M.; Martin, C.K. Sweetness, satiation, and satiety. J. Nutr. 2012, 142, 1149S–1154S. [Google Scholar] [CrossRef] [PubMed]
- Choudhary, A.K.; Lee, Y.Y. Neurophysiological symptoms and aspartame: What is the connection? Nutr. Neurosci. 2017, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Azad, M.B.; Abou-Setta, A.M.; Chauhan, B.F.; Rabbani, R.; Lys, J.; Copstein, L.; Mann, A.; Jeyaraman, M.M.; Reid, A.E.; Fiander, M.; et al. Nonnutritive sweeteners and cardiometabolic health: A systematic review and meta-analysis of randomized controlled trials and prospective cohort studies. Can. Med. Assoc. J. 2017, 189, E929–E939. [Google Scholar] [CrossRef] [PubMed]
- Drewnowski, A.; Massien, C.; Louis-Sylvestre, J.; Fricker, J.; Chapelot, D.; Apfelbaum, M. The effects of aspartame versus sucrose on motivational ratings, taste preferences, and energy intakes in obese and lean women. Int. J. Obes. Relat. Metab. Disord. 1994, 18, 570–578. [Google Scholar] [PubMed]
- Drewnowski, A.; Massien, C.; Louis-Sylvestre, J.; Fricker, J.; Chapelot, D.; Apfelbaum, M. Comparing the effects of aspartame and sucrose on motivational ratings, taste preferences, and energy intakes in humans. Am. J. Clin. Nutr. 1994, 59, 338–345. [Google Scholar] [CrossRef] [PubMed]
- Souza Bda, S.; Cunha, D.B.; Pereira, R.A.; Sichieri, R. Soft drink consumption, mainly diet ones, is associated with increased blood pressure in adolescents. Hypertens 2016, 34, 221–225. [Google Scholar] [CrossRef] [PubMed]
- Spencer, M.; Gupta, A.; Dam, L.V.; Shannon, C.; Menees, S.; Chey, W.D. Artificial Sweeteners: A Systematic Review and Primer for Gastroenterologists. J. Neurogastroenterol. Motil. 2016, 22, 168–180. [Google Scholar] [CrossRef] [PubMed]
- Nettleton, J.E.; Reimer, R.A.; Shearer, J. Reshaping the gut microbiota: Impact of low calorie sweeteners and the link to insulin resistance? Physiol. Behav. 2016, 164, 488–493. [Google Scholar] [CrossRef] [PubMed]
- Miller, P.E.; Perez, V. Low-calorie sweeteners and body weight and composition: A meta-analysis of randomized controlled trials and prospective cohort studies. Am. J. Clin. Nutr. 2014, 100, 765–777. [Google Scholar] [CrossRef] [PubMed]
- Rogers, P.J.; Hogenkamp, P.S.; De Graaf, C.; Higgs, S.; Lluch, A.; Ness, A.R.; Penfold, C.; Perry, R.; Putz, P.; Yeomans, M.R.; et al. Does low-energy sweetener consumption affect energy intake and body weight? A systematic review, including meta-analyses, of the evidence from human and animal studies. Int. J. Obes. 2016, 40, 381–394. [Google Scholar] [CrossRef] [PubMed]
- Bryant, C.; Mclaughlin, J. Low calorie sweeteners: Evidence remains lacking for effects on human gut function. Physiol. Behav. 2016, 64 (Pt B), 482–485. [Google Scholar] [CrossRef] [PubMed]
- Taillie, L.S.; Ng, S.W.; Xue, Y.; Busey, E.; Harding, M. No Fat, No Sugar, No Salt, No Problem? Prevalence of “Low-Content” Nutrient Claims and Their Associations with the Nutritional Profile of Food and Beverage Purchases in the United States. J. Acad. Nutr. Diet. 2017, 117, 1366–1374. [Google Scholar] [CrossRef] [PubMed]
- Wise, P.M.; Nattress, L.; Flammer, L.J.; Beauchamp, G.K. Reduced dietary intake of simple sugars alters perceived sweet taste intensity but not perceived pleasantness. Am. J. Clin. Nutr. 2016, 103, 50–60. [Google Scholar] [CrossRef] [PubMed]
- Yeon, J.Y.; Lee, S.K. Perception of sugar reduction, nutrition education, and frequency of snacking in children by the self-perceived sweet dietary habits of mothers in Busan. Nutr. Res. Pract. 2016, 10, 546–554. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Drewnowski, A.; Rehm, C.D. Consumption of low-calorie sweeteners among U.S. adults is associated with higher healthy eating index (HEI 2005) scores and more physical activity. Nutrients 2014, 6, 4389–4403. [Google Scholar] [CrossRef] [PubMed]
- Gibson, S.A.; Horgan, G.W.; Francis, L.E.; Gibson, A.A.; Stephen, A.M. Low calorie beverage consumption is associated with energy and nutrient intakes and diet quality in British adults. Nutrients 2016, 8, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Peters, J.C.; Beck, J.; Cardel, M.; Wyatt, H.R.; Foster, G.D.; Pan, Z.; Wojtanowski, A.C.; Vander Veur, S.S.; Herring, S.J.; Brill, C.; et al. The effects of water and non-nutritive sweetened beverages on weight loss and weight maintenance: A randomized clinical trial. Obesity 2016, 24, 297–304. [Google Scholar] [CrossRef] [PubMed]
- Reid, A.E.; Chauhan, B.F.; Rabbani, R.; Lys, J.; Copstein, L.; Mann, A.; Abou-Setta, A.M.; Fiander, M.; MacKay, D.S.; McGavock, J.; et al. Early exposure to nonnutritive sweeteners and long-term metabolic health: A systematic review. Pediatrics 2016, 137, e20153603. [Google Scholar] [CrossRef] [PubMed]
- Riley, P.; Moore, D.; Ahmed, F.; Sharif, M.O.; Worthington, H.V. Xylitol-containing products for preventing dental caries in children and adults. Cochrane Database Syst. Rev. 2015, 3, CD010743. [Google Scholar] [CrossRef] [PubMed]
- Fowler, S.P.; Williams, K.; Resendez, R.G.; Hunt, K.J.; Hazuda, H.P.; Stern, M.P. Fueling the obesity epidemic? Artificially sweetened beverage use and long-term weight gain. Obesity 2008, 16, 1894–1900. [Google Scholar] [CrossRef] [PubMed]
- Nettleton, J.A.; Lutsey, P.L.; Wang, Y.; Lima, J.A.; Michos, E.D.; Jacobs, D.R. Diet soda intake and risk of incident metabolic syndrome and type 2 diabetes in the Multi-Ethnic Study of Atherosclerosis (MESA). Diabetes Care 2009, 32, 688–694. [Google Scholar] [CrossRef] [PubMed]
- Romo-Romo, A.; Aguilar-Salinas, C.A.; Gomez-Diaz, R.A.; Brito-Córdova, G.X.; Gómez-Velasco, D.V.; López-Rocha, M.J.; Almeda-Valdés, P. Non-Nutritive Sweeteners: Evidence on their Association with Metabolic Diseases and Potential Effects on Glucose Metabolism and Appetite. Rev. Investig. Clin. 2017, 69, 129–138. [Google Scholar] [CrossRef]
- Logue, C.; Dowey, L.C.; Strain, J.J.; Verhagen, H.; Gallagher, A.M. Application of liquid chromatography–tandem mass spectrometry to determine urinary concentrations of five commonly used low-calorie sweeteners: A novel biomarker approach for assessing recent intakes? J. Agric. Food Chem. 2017, 65, 4516–4525. [Google Scholar] [CrossRef] [PubMed]
- Sylvetsky, A.C.; Rother, K.I. Nonnutritive Sweeteners in Weight Management and Chronic Disease: A Review. Obesity 2018, 26, 635–640. [Google Scholar] [CrossRef] [PubMed]
- Tordoff, M.G.; Alleva, A.M. Effect of drinking soda sweetened with aspartame or high-fructose corn syrup on food intake and body weight. Am. J. Clin. Nutr. 1990, 51, 963–969. [Google Scholar] [CrossRef] [PubMed]
- Raben, A.; Vasilaras, T.H.; Møller, A.C.; Astrup, A. Sucrose compared with artificial sweeteners: Different effects on ad libitum food intake and body weight after 10 wk of supplementation in overweight subjects. Am. J. Clin. Nutr. 2002, 76, 721–729. [Google Scholar] [CrossRef] [PubMed]
- Vázquez-Duran, M.; Castillo-Martínez, L.; Orea-Tejeda, A.; López-Rodríguez, Y.; Téllez-Olvera, L.G.; Delgado-Pérez, D.A. Effect of decreasing the consumption of sweetened caloric and non-caloric beverages on weight, body composition and blood pressure in young adults. Eur. J. Prev. Cardiol. 2013, 20 (Suppl. 1), S1–S20. [Google Scholar]
- Madjd, A.; Taylor, M.A.; Delavari, A.; Malekzadeh, R.; Macdonald, I.A.; Farshchi, H.R. Effects on weight loss in adults of replacing diet beverages with water during a hypoenergetic diet: A randomized, 24-wk clinical trial. Am. J. Clin. Nutr. 2015, 102, 1305–1312. [Google Scholar] [CrossRef] [PubMed]
- Blackburn, G.L.; Kanders, B.S.; Lavin, P.T.; Keller, S.D.; Whatley, J. The effect of aspartame as part of a multidisciplinary weight-control program on short- and longterm control of body weight. Am. J. Clin. Nutr. 1997, 65, 409–418. [Google Scholar] [CrossRef] [PubMed]
- Cooper, P.; Wahlqvist, M.; Simpson, R. Sucrose versus Saccharin as an Added Sweetener in Non-insulin-dependent Diabetes: Short-and Medium-term Metabolic Effects. Diabet. Med. 1988, 5, 676–680. [Google Scholar] [CrossRef] [PubMed]
- Colagiuri, S.; Miller, J.J.; Edwards, R.A. Metabolic effects of adding sucrose and aspartame to the diet of subjects with noninsulin-dependent diabetes mellitus. Am. J. Clin. Nutr. 1989, 50, 474–478. [Google Scholar] [CrossRef] [PubMed]
- Barriocanal, L.A.; Palacios, M.; Benitez, G.; Benitez, S.; Jimenez, J.T.; Jimenez, N.; Rojas, V. Apparent lack of pharmacological effect of steviol glycosides used as sweeteners in humans. A pilot study of repeated exposures in some normotensive and hypotensive individuals and in Type 1 and Type 2 diabetics. Regul. Toxicol. Pharmacol. 2008, 51, 37–41. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.W.; Brown, M.M.B.; Onken, K.L.; Beitz, D.C. Short-term consumption of sucralose, a nonnutritive sweetener, is similar to water with regard to select markers of hunger signaling and short-term glucose homeostasis in women. Nutr. Res. 2011, 31, 882–888. [Google Scholar] [CrossRef] [PubMed]
- Pepino, M.Y.; Tiemann, C.D.; Patterson, B.W.; Wice, B.M.; Klein, S. Sucralose affects glycemic and hormonal responses to an oral glucose load. Diabetes Care 2013, 36, 2530–2535. [Google Scholar] [CrossRef] [PubMed]
- Temizkan, S.; Deyneli, O.; Yasar, M.; Arpa, M.; Gunes, M.; Yazici, D.; Sirikci, O.; Haklar, G.; Imeryuz, N.; Yavuz, D.G. Sucralose enhances GLP-1 release and lowers blood glucose in the presence of carbohydrate in healthy subjects but not in patients with type 2 diabetes. Eur. J. Clin. Nutr. 2015, 69, 162–166. [Google Scholar] [CrossRef] [PubMed]
- Imamura, F.; O’Connor, L.; Ye, Z.; Mursu, J.; Hayashino, Y.; Bhupathiraju, S.N.; Forouhi, N.G. Consumption of sugar sweetened beverages, artificially sweetened beverages, and fruit juice and incidence of type 2 diabetes: Systematic review, meta-analysis, and estimation of population attributable fraction. BMJ 2015, 351, h3576. [Google Scholar] [CrossRef] [PubMed]
- Romo-Romo, A.; Aguilar-Salinas, C.A.; Brito-Córdova, G.X.; Díaz, R.A.G.; Valentín, D.V.; Almeda-Valdes, P. Effects of the non-nutritive sweeteners on glucose metabolism and appetite regulating hormones: Systematic review of observational prospective studies and clinical trials. PLoS ONE 2016, 11, e0161264. [Google Scholar] [CrossRef] [PubMed]
- Tucker, R.M.; Tan, S.-Y. Do non-nutritive sweeteners influence acute homeostasis in humans? A systematic review. Physiol. Behav. 2017, 182, 17–26. [Google Scholar] [CrossRef] [PubMed]
- Okuno, G.; Kawakami, F.; Tako, H.; Kashihara, T.; Shibamoto, S.; Yamazaki, T.; Yamamoto, K.; Saeki, M. Glucose tolerance, blood lipid, insulin and glucagon concentration after single or continuous administration of aspartame in diabetics. Diabetes Res. Clin. Pract. 1986, 2, 23–27. [Google Scholar] [CrossRef]
- Härtel, B.; Graubaum, H.; Schneider, B. The influence of sweetener solutions on the secretion of insulin and the blood glucose level. Ernährungsumschau 1993, 40, 152–155. [Google Scholar]
- Hsieh, M.H.; Chan, P.; Sue, Y.M.; Liu, J.C.; Liang, T.H.; Huang, T.Y.; Tomlinson, B.; Chow, M.S.; Kao, P.F.; Chen, Y.J. Efficacy and tolerability of oral stevioside in patients with mild essential hypertension: A two year, randomized, placebo-controlled study. Clin. Ther. 2003, 25, 2797–2808. [Google Scholar] [CrossRef]
- Ferri, L.A.; Alves-Do-Prado, W.; Yamada, S.S.; Gazola, S.; Batista, M.R.; Bazotte, R.B. Investigation of the antihypertensive effect of oral crude stevioside in patients with mild essential hypertension. Phytother. Res. 2006, 20, 732–736. [Google Scholar] [CrossRef] [PubMed]
- Anton, S.D.; Martin, C.K.; Han, H.; Coulon, S.; Cefalu, W.T.; Geiselman, P.; Williamson, D.A. Effects of stevia, aspartame, and sucrose on food intake, satiety, and postprandial glucose and insulin levels. Appetite 2010, 55, 37–43. [Google Scholar] [CrossRef] [PubMed]
- Wiebe, N.; Padwal, R.; Field, C.; Marks, S.; Jacobs, R.; Tonelli, M. A systematic review on the effect of sweeteners on glycemic response and clinically relevant outcomes. BMC Med. 2011, 9, 123. [Google Scholar] [CrossRef] [PubMed]
- Grotz, V.L.; Pi-Sunyer, X.; Porte, D.J.; Roberts, A.; Trout, J.R. A 12-week randomized clinical trial investigating the potential for sucralose to affect glucose homeostasis. Regul. Toxicol. Pharmacol. 2017, 88, 22–33. [Google Scholar] [CrossRef] [PubMed]
- Lohner, S.; Toews, I.; Kuellenberg de Gaudry, D.; Sommer, H.; Meerpohl, J.J. Non-nutritive sweeteners for diabetes mellitus. Cochrane Database Syst. Rev. 2017. [Google Scholar] [CrossRef]
- Agence Nationale de Sécurité Sanitaire, alimentation, environnement, travail (ANSES). Évaluation des Bénéfices et des Risques Nutritionnels des édulcorants Intenses; Avis de l’Anses Rapport d’expertise Collective; ANSES: Buenos Aires, Argentina, 2015.
- Gupta, P.; Gupta, N.; Pawar, A.P.; Birajdar, S.S.; Natt, A.S.; Singh, H.P. Role of Sugar and Sugar Substitutes in Dental Caries: A Review. ISRN Dent. 2013, 519421. [Google Scholar] [CrossRef] [PubMed]
- Gibson, S.; Drewnowski, A.; Hill, J.; Raben, A.B.; Tuorila, H.; Widström, E. Consensus statement on benefits of low-calorie sweeteners. Nutr. Bull. 2014, 39, 386–389. [Google Scholar] [CrossRef]
- WHO. Guideline: Sugars Intake for Adults and Children; World Health Organisation: Geneva, Switzerland, 2015. [Google Scholar]
- Scientific Advisory Committee on Nutrition. Carbohydrates and Health; TSO: London, UK, 2015. [Google Scholar]
- Clemens, R.A.; Jones, J.M.; Kern, M.; Lee, S.-Y.; Mayhew, E.J.; Slavin, J.L.; Zivanovic, S. Functionality of Sugars in Foods and Health. Compr. Rev. Food Sci. Food Saf. 2016, 15, 433–470. [Google Scholar] [CrossRef]
- SENC; Aranceta Bartrina, J.; Arija Val, V.; Maíz Aldalur, E.; Martínez de la Victoria Muñoz, E.; Ortega Anta, R.M.; Pérez-Rodrigo, C.; Quiles Izquierdo, J.; Rodríguez Martín, A.; Román Viñas, B.; et al. Dietary guidelines for the Spanish population (SENC, December 2016); the new graphic icon of healthy nutrition. Nutr. Hosp. 2016, 33 (Suppl. 8), S1–S48. [Google Scholar] [CrossRef]
- FAO. Food Based Dietary Guidelines. Available online: http://www.fao.org/nutrition/nutrition-education/food-dietary-guidelines/regions/en/ (accessed on 30 January 2018).
- FAO. Grupo de Educación Nutricional y de Sensibilización del Consumidor. División de Nutrición Organización de las Naciones Unidas para la Alimentación y la Agricultura, Roma, 2014. El Estado de las Guías Alimentarias Basadas en Alimentos en América Latina y el Caribe. 21 años Después de la Conferencia Internacional Sobre Nutrición. Available online: http://www.fao.org/3/a-i3677s.pdf (accessed on 10 January 2018).
- Public Health England in Association with the Welsh Government, Food Standards Scotland and the Food Standards Agency in Northern Ireland. 2016; Eat Well Guide. Available online: http://www.gov.uk/government/publications/the-eatwell-guide (accessed on 30 January 2018).
- Vigez De actieve Voedingsdriehoek. Belgium. Available online: http://www.vigez.be/projecten/actieve-voedingsdriehoek (accessed on 30 January 2018).
- Santé Publique France. Manger Bouger. Programe National Nutritión Santé Les 9 Repères Produits Sucrés: A Limiter ! Available online: http://www.mangerbouger.fr/Les-9-reperes/Les-9-reperes-a-la-loupe/Produits-sucres] (accessed on 30 January 2018).
- Commission Regulation (EU) No 1129/2011 of 11 November 2011 Amending Annex II to Regulation (EC) No 1333/2008 of the European Parliament and of the Council by Establishing a Union List of Food Additives. Available online: https://eur-lex.europa.eu/legal-content/EN/ALL/?uri=CELEX%3A32011R1129 (accessed on 30 January 2018).
- Bernardo, W.M.; Simoes, R.S.; Buzzini, R.F.; Nunes, V.M.; Glina, F. Adverse effects of the consumption of artificial sweeteners-systematic review. Rev. Assoc. Med. Bras. 2016, 62, 120–122. [Google Scholar] [CrossRef] [PubMed]
- Araujo, J.R.; Martel, F.; Keating, E. Exposure to non-nutritive sweeteners during pregnancy and lactation: Impact in programming of metabolic diseases in the progeny later in life. Reprod. Toxicol. 2014, 49, 196–201. [Google Scholar] [CrossRef] [PubMed]
- Rodrigues, J.F.; Andrade, R.D.S.; Bastos, S.C.; Coelho, S.B.; Pinheiro, A.C.M. Miracle fruit: An alternative sugar substitute in sour beverages. Appetite 2016, 107, 645–653. [Google Scholar] [CrossRef] [PubMed]
- Piernas, C.; Ng, S.W.; Popkin, B. Trends in purchases and intake of foods and beverages containing caloric and low-calorie sweeteners over the last decade in the United States. Pediatr. Obes. 2013, 8, 294–306. [Google Scholar] [CrossRef] [PubMed]
- Sylvetsky, A.C.; Welsh, J.A.; Brown, R.J.; Vos, M.B. Low-calorie sweetener consumption is increasing in the United States. Am. J. Clin. Nutr. 2012, 96, 640–646. [Google Scholar] [CrossRef] [PubMed]
- Sylvetsky, A.C.; Jin, Y.; Clark, E.J.; Welsh, J.A.; Rother, K.I.; Talegawkar, S.A. Consumption of low-calorie sweeteners among children and adults in the United States. J. Acad. Nutr. Diet. 2017, 117, 441–448. [Google Scholar] [CrossRef] [PubMed]
- Slining, M.M.; Ng, S.W.; Popkin, B.M. Food companies’ calorie-reduction pledges to improve United States diet. Am. J. Prev. Med. 2013, 44, 174–184. [Google Scholar] [CrossRef] [PubMed]
- Mattes, R.D. Low calorie sweeteners: Science and controversy. Physiol. Behav. 2016, 164 (Pt B), 429–431. [Google Scholar] [CrossRef] [PubMed]
- International Sweeteners Association—ISA. Available online: https://www.sweeteners.org/category/11/sweeteners/54/what-are-low-calorie-sweeteners (accessed on 30 January 2018).
- Hedrick, V.E.; Passaro, E.M.; Davy, B.M.; You, W.; Zoellner, J.M. Characterization of non-nutritive sweetener intake in rural southwest Virginian adults living in a health-disparate region. Nutrients 2017, 9. [Google Scholar] [CrossRef] [PubMed]
- Drewnowski, A.; Rehm, C.D. Socio-demographic correlates and trends in low-calorie sweetener use among adults in the United States from 1999 to 2008. Eur. J. Clin. Nutr. 2015, 69, 1035–1041. [Google Scholar] [CrossRef] [PubMed]
- Sylvetsky, A.C.; Walter, P.J.; Garraffo, H.M.; Robien, K.; Rother, K.I. Widespread sucralose exposure in a randomized clinical trial in healthy young adults. Am. J. Clin. Nutr. 2017, 105, 820–823. [Google Scholar] [CrossRef] [PubMed]
- Comisión del Codex Alimentarius. Programa Conjunto FAO/OMS Sobre Normas Alimentarias. In Proceedings of the 44th Reunión, Hangzhou, China, 12–16 March 2012; CX/FA 12/44/2. Available online: http://www.fao.org/tempref/codex/Meetings/CCFA/CCFA44/fa44_02s.pdf (accessed on 20 September 2017).
| International Numbering System | Sweetener | ADI (FDA) (mg/kg Body Weight) | ADI (EFSA) (mg/kg Body Weight) | Sweetening Power 1 | Discovery Date | Start of Use in EU | Chemical Structure |
|---|---|---|---|---|---|---|---|
| 950 | Acesulfame K | 15 | 9 | 200 | 1967 | 1983 |  |
| 951 | Aspartame | 50 | 40 | 200 | 1969 | 1983 | 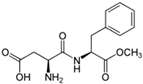 |
| 952 | Cyclamates (Cyclamic acid and its Na and Ca salts) | Not approved | 7 | 30–40 | 1937 | 1954 |  |
| 954 | Saccharin and its Na, K and Ca salts | 15 | 5 | 300–500 | 1879 | 1887 | 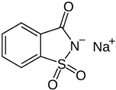 |
| 955 | Sucralose | 5 | 15 | 600–650 2 | 1976 | 2000 | 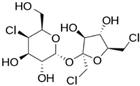 |
| 960 | Steviol Glycosides | 4 3 | 4 3 | 200–300 | 1931 | 2010 (Periodical JECFA evaluations since 2004) | RebaudiosideA 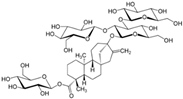 |
| 969 | Advantame | 32.8 | 5 | 37,000 4 | 2013 | 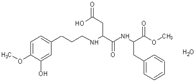 | |
| 961 | Neotame | 0.3 | 2 | 7000–13,000 5 | 1990 | 2010 2002 FDA | 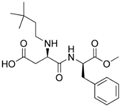 |
| 956 | Alitame | Not approved | 1 | 2000 | 1980 | 1996 | 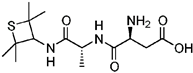 |
| 957 | Thaumatin | Not approved | Not specified 6 | 2000–3000 | 1979 | 1999 | 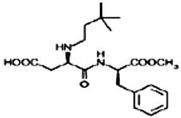 |
| 959 | Neohesperidine Dihydrochalcone | Not approved | 5 | 1.500 | 1960 | 1994 | 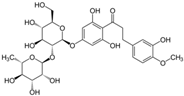 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Serra-Majem, L.; Raposo, A.; Aranceta-Bartrina, J.; Varela-Moreiras, G.; Logue, C.; Laviada, H.; Socolovsky, S.; Pérez-Rodrigo, C.; Aldrete-Velasco, J.A.; Meneses Sierra, E.; et al. Ibero–American Consensus on Low- and No-Calorie Sweeteners: Safety, Nutritional Aspects and Benefits in Food and Beverages. Nutrients 2018, 10, 818. https://doi.org/10.3390/nu10070818
Serra-Majem L, Raposo A, Aranceta-Bartrina J, Varela-Moreiras G, Logue C, Laviada H, Socolovsky S, Pérez-Rodrigo C, Aldrete-Velasco JA, Meneses Sierra E, et al. Ibero–American Consensus on Low- and No-Calorie Sweeteners: Safety, Nutritional Aspects and Benefits in Food and Beverages. Nutrients. 2018; 10(7):818. https://doi.org/10.3390/nu10070818
Chicago/Turabian StyleSerra-Majem, Lluis, António Raposo, Javier Aranceta-Bartrina, Gregorio Varela-Moreiras, Caomhan Logue, Hugo Laviada, Susana Socolovsky, Carmen Pérez-Rodrigo, Jorge Antonio Aldrete-Velasco, Eduardo Meneses Sierra, and et al. 2018. "Ibero–American Consensus on Low- and No-Calorie Sweeteners: Safety, Nutritional Aspects and Benefits in Food and Beverages" Nutrients 10, no. 7: 818. https://doi.org/10.3390/nu10070818
APA StyleSerra-Majem, L., Raposo, A., Aranceta-Bartrina, J., Varela-Moreiras, G., Logue, C., Laviada, H., Socolovsky, S., Pérez-Rodrigo, C., Aldrete-Velasco, J. A., Meneses Sierra, E., López-García, R., Ortiz-Andrellucchi, A., Gómez-Candela, C., Abreu, R., Alexanderson, E., Álvarez-Álvarez, R. J., Álvarez Falcón, A. L., Anadón, A., Bellisle, F., ... Cunha Velho de Sousa, S. (2018). Ibero–American Consensus on Low- and No-Calorie Sweeteners: Safety, Nutritional Aspects and Benefits in Food and Beverages. Nutrients, 10(7), 818. https://doi.org/10.3390/nu10070818
















