Association between the Dietary Inflammatory Index and Risk of Frailty in Older Individuals with Poor Nutritional Status
Abstract
:1. Introduction
2. Materials and Methods
2.1. Patient Population
2.2. Frailty Assessment
2.3. Mini Nutritional Assessment (MNA)
2.4. Dietary Inflammatory Index (DII)
2.5. Statistical Analyses
3. Results
3.1. Characteristics of Participants
3.2. Association between DII and Frailty Status
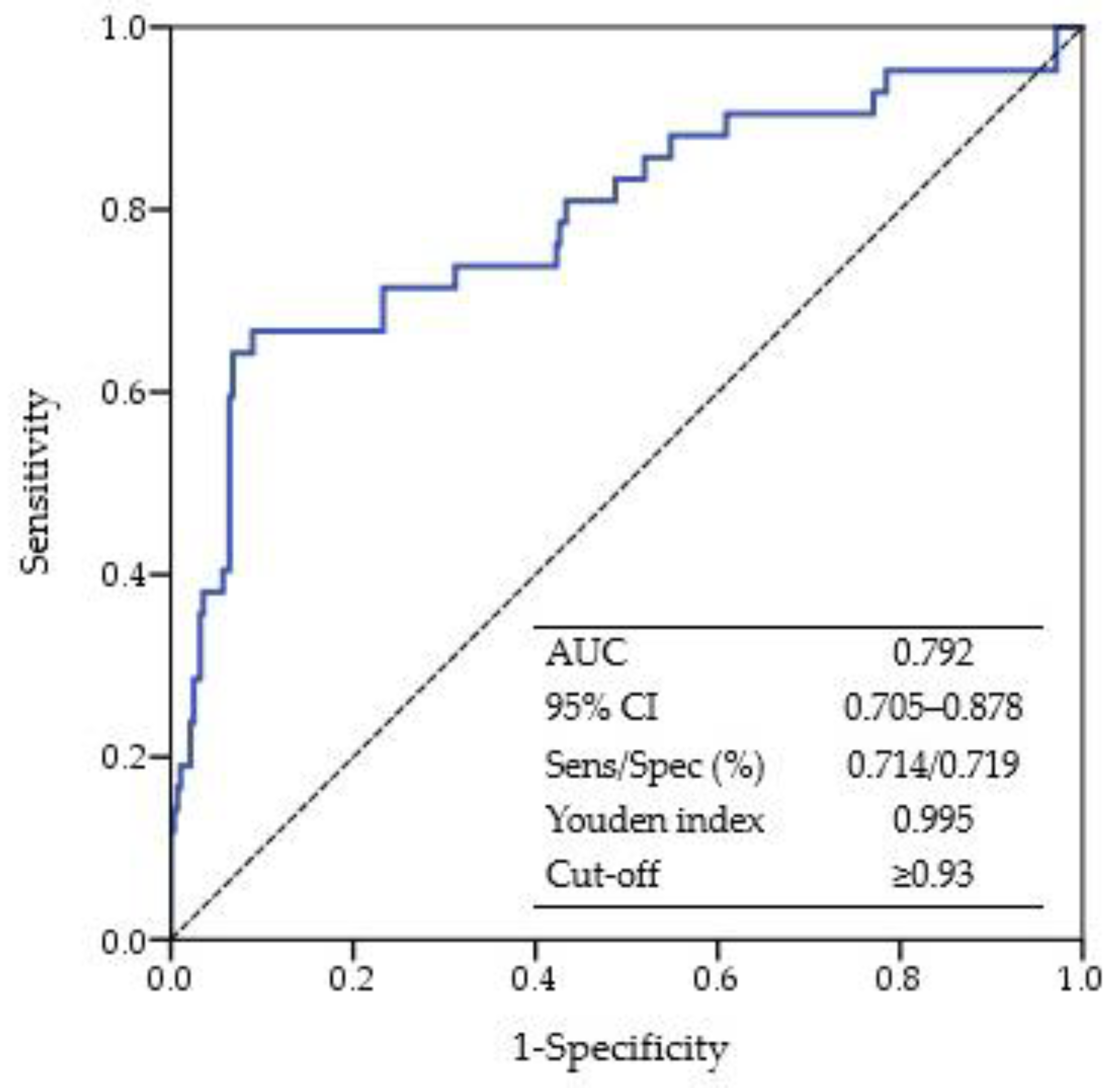
3.3. Predictability of Frailty Using the DII
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Fried, L.P.; Tangen, C.M.; Walston, J.; Newman, A.B.; Hirsch, C.; Gottdiener, J.; Seeman, T.; Tracy, R.; Kop, W.J.; Burke, G.; et al. Frailty in older adults: Evidence for a phenotype. J. Gerontol. A Biol. Sci. Med. Sci. 2001, 56, M146–M156. [Google Scholar] [CrossRef] [PubMed]
- He, B.W.; Goodkind, D.; Kowal, P. International Population Reports: An Aging World: 2015; US Census Bureau: Suitland, MD, USA, 2016.
- Jung, H.W.; Kim, S.W.; Ahn, S.; Lim, J.Y.; Han, J.W.; Kim, T.H.; Kim, K.W.; Kim, K.I.; Kim, C.H. Prevalence and outcomes of frailty in Korean elderly population: Comparisons of a multidimensional frailty index with two phenotype models. PLoS ONE 2014, 9, E87958. [Google Scholar] [CrossRef] [PubMed]
- Bales, C.W.; Ritchie, C.S. Sarcopenia, weight loss, and nutritional frailty in the elderly. Annu. Rev. Nutr. 2002, 22, 309–323. [Google Scholar] [CrossRef] [PubMed]
- Abellan Van Kan, G.; Vellas, B. Is the mini nutritional assessment an appropriate tool to assess frailty in older adults? J. Nutr. Health Aging 2011, 15, 159–161. [Google Scholar] [CrossRef] [PubMed]
- Bollwein, J.; Volkert, D.; Diekmann, R.; Kaiser, M.J.; Uter, W.; Vidal, K.; Sieber, C.C.; Bauer, J.M. Nutritional status according to the mini nutritional assessment (MNA®) and frailty in community dwelling older persons: A close relationship. J. Nutr. Health Aging 2013, 17, 351–356. [Google Scholar] [CrossRef] [PubMed]
- Katona, P.; Katona-Apte, J. The interaction between nutrition and infection. Clin. Infect. Dis. 2008, 46, 1582–1588. [Google Scholar] [CrossRef] [PubMed]
- Chen, X.; Mao, G.; Leng, S.X. Frailty syndrome: An overview. Clin. Interv. Aging 2014, 9, 433–441. [Google Scholar] [PubMed]
- Soysal, P.; Stubbs, B.; Lucato, P.; Luchini, C.; Solmi, M.; Peluso, R.; Sergi, G.; Isik, A.T.; Manzato, E.; Maggi, S.; et al. Inflammation and frailty in the elderly: A systematic review and meta-analysis. Ageing Res. Rev. 2016, 31, 1–8. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Finkel, T.; Holbrook, N.J. Oxidant, oxidative stress and the biology of ageing. Nature 2000, 408, 239–247. [Google Scholar] [CrossRef] [PubMed]
- Shivappa, N.; Steck, S.E.; Hurley, T.G.; Hussey, J.R.; Hebert, J.R. Designing and developing a literature-derived, population-based dietary inflammatory index. Public Health Nutr. 2014, 17, 1689–1696. [Google Scholar] [CrossRef] [PubMed]
- Shivappa, N.; Steck, S.E.; Hurley, T.G.; Hussey, J.R.; Ma, Y.; Ockene, I.S.; Tabung, F.; Hebert, J.R. A population-based dietary inflammatory index predicts levels of C-reactive protein in the Seasonal Variation of Blood Cholesterol Study (SEASONS). Public Health Nutr. 2014, 17, 1825–1833. [Google Scholar] [CrossRef] [PubMed]
- Tabung, F.K.; Steck, S.E.; Zhang, J.; Ma, Y.; Liese, A.D.; Agalliu, I.; Hingle, M.; Hou, L.; Hurley, T.G.; Jiao, L.; et al. Construct validation of the dietary inflammatory index among postmenopausal women. Ann. Epidemiol. 2015, 25, 398–405. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Shivappa, N.; Hebert, J.R.; Marcos, A.; Diaz, L.E.; Gomez, S.; Nova, E.; Michels, N.; Arouca, A.; Gonzalez-Gil, E.; Frederic, G.; et al. Association between dietary inflammatory index and inflammatory markers in the HELENA study. Mol. Nutr. Food Res. 2017, 61, 1600707. [Google Scholar] [CrossRef] [PubMed]
- Wirth, M.; Burch, J.; Shivappa, N.; Violanti, J.M.; Burchfiel, C.M.; Fekedulegn, D.; Andrew, M.E.; Hartley, T.A.; Miller, D.B.; Mnatsakanova, A.; et al. Association of a dietary inflammatory index with inflammatory indices and metabolic syndrome among police officers. J. Occup. Environ. Med. 2014, 56, 986–989. [Google Scholar] [CrossRef] [PubMed]
- Wood, L.G.; Shivappa, N.; Berthon, B.S.; Gibson, P.G.; Hebert, J.R. Dietary inflammatory index is related to asthma risk, lung function and systemic inflammation in asthma. Clin. Exp. Allergy 2015, 45, 177–183. [Google Scholar] [CrossRef] [PubMed]
- Orchard, T.; Yildiz, V.; Steck, S.E.; Hebert, J.R.; Ma, Y.; Cauley, J.A.; Li, W.; Mossavar-Rahmani, Y.; Johnson, K.C.; Sattari, M.; et al. Dietary inflammatory index, bone mineral density, and risk of fracture in postmenopausal women: Results from the Women’s Health Initiative. J. Bone Miner. Res. 2017, 32, 1136–1146. [Google Scholar] [CrossRef] [PubMed]
- Jang, H.; Chung, M.S.; Kang, S.S.; Park, Y. Association between the dietary inflammatory index and risk for cancer recurrence and mortality among patients with breast cancer. Nutrients 2018, 10, 1095. [Google Scholar] [CrossRef] [PubMed]
- Tabung, F.K.; Steck, S.E.; Ma, Y.; Liese, A.D.; Zhang, J.; Caan, B.; Hou, L.; Johnson, K.C.; Mossavar-Rahmani, Y.; Shivappa, N.; et al. The association between dietary inflammatory index and risk of colorectal cancer among postmenopausal women: Results from the Women’s Health Initiative. Cancer Causes Control 2015, 26, 399–408. [Google Scholar] [CrossRef] [PubMed]
- Shivappa, N.; Stubbs, B.; Hebert, J.R.; Cesari, M.; Schofield, P.; Soysal, P.; Maggi, S.; Veronese, N. The relationship between the dietary inflammatory index and incident frailty: A longitudinal cohort study. J. Am. Med. Dir. Assoc. 2018, 19, 77–82. [Google Scholar] [CrossRef] [PubMed]
- Vellas, B.; Guigoz, Y.; Garry, P.J.; Nourhashemi, F.; Bennahum, D.; Lauque, S.; Albarede, J.L. The mini nutritional assessment (MNA) and its use in grading the nutritional state of elderly patients. Nutrition 1999, 15, 116–122. [Google Scholar] [CrossRef]
- Swets, J.A. Measuring the accuracy of diagnostic systems. Science 1988, 240, 1285–1293. [Google Scholar] [CrossRef] [PubMed]
- Gale, C.R.; Cooper, C.; Sayer, A.A. Prevalence of frailty and disability: Findings from the English Longitudinal Study of Ageing. Age Ageing 2014, 44, 162–165. [Google Scholar] [CrossRef] [PubMed]
- Cavicchia, P.P.; Steck, S.E.; Hurley, T.G.; Hussey, J.R.; Ma, Y.; Ockene, I.S.; Hebert, J.R. A new dietary inflammatory index predicts interval changes in serum high-sensitivity C-reactive protein. J. Nutr. 2009, 139, 2365–2372. [Google Scholar] [CrossRef] [PubMed]
- Na, W.; Kim, M.; Sohn, C. Dietary inflammatory index and its relationship with high-sensitivity C-reactive protein in Korean: Data from the health examinee cohort. J. Clin. Biochem. Nutr. 2018, 62, 83–88. [Google Scholar] [CrossRef] [PubMed]
- Shivappa, N.; Hebert, J.R.; Rietzschel, E.R.; De Buyzere, M.L.; Langlois, M.; Debruyne, E.; Marcos, A.; Huybrechts, I. Associations between dietary inflammatory index and inflammatory markers in the Asklepios Study. Brit. J. Nutr. 2015, 113, 665–671. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sergi, G.; Veronese, N.; Fontana, L.; De Rui, M.; Bolzetta, F.; Zambon, S.; Corti, M.C.; Baggio, G.; Toffanello, E.D.; Crepaldi, G.; et al. Pre-frailty and risk of cardiovascular disease in elderly men and women. J. Am. Coll. Cardiol. 2015, 65, 976–983. [Google Scholar] [PubMed]
- Piggott, D.A.; Varadhan, R.; Mehta, S.H.; Brown, T.T.; Li, H.; Walston, J.D.; Leng, S.X.; Kirk, G.D. Frailty, inflammation, and mortality among persons aging with HIV infection and injection drug use. J. Gerontol. A Biol. Sci. Med. Sci. 2015, 70, 1542–1547. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.P.; Schwartz, R.J.; Waddell, I.D.; Holloway, B.R.; Reid, M.B. Skeletal muscle myocytes undergo protein loss and reactive oxygen-mediated NF-κB activation in response to tumor necrosis factor α. FASEB J. 1998, 12, 871–880. [Google Scholar] [CrossRef] [PubMed]
- Roubenoff, R. Sarcopenia: A major modifiable cause of frailty in the elderly. J. Nutr. Health Aging 2000, 4, 140–142. [Google Scholar] [PubMed]
- Bano, G.; Trevisan, C.; Carraro, S.; Solmi, M.; Luchini, C.; Stubbs, B.; Manzato, E.; Sergi, G.; Veronese, N. Inflammation and sarcopenia: A systematic review and meta-analysis. Maturitas 2017, 96, 10–15. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Schaap, L.A.; Pluijm, S.M.F.; Deeg, D.J.H.; Visser, M. Inflammatory markers and loss of muscle mass (sarcopenia) and strength. Am. J. Med. 2006, 119, 526-e9–526-e17. [Google Scholar] [CrossRef] [PubMed]
- Taaffe, D.R.; Harris, T.B.; Ferrucci, L.; Rowe, J.; Seeman, T.E. Cross-sectional and prospective relationships of interleukin-6 and C-reactive protein with physical performance in elderly persons: MacArthur Studies of Successful Aging. J. Gerontol. A Biol. Sci. Med. Sci. 2000, 55, M709–M715. [Google Scholar] [CrossRef] [PubMed]
- Ferrucci, L.; Penninx, B.W.J.H.; Volpato, S.; Harris, T.B.; Bandeen-Roche, K.; Balfour, J.; Leveille, S.G.; Fried, L.P.; Guralnik, J.M. Change in muscle strength explains accelerated decline of physical function in older women with high interleukin-6 serum levels. J. Am. Geriatr. Soc. 2002, 50, 1947–1954. [Google Scholar] [CrossRef] [PubMed]
- Wallace, J.I.; Schwartz, R.S. Involuntary weight loss in elderly outpatients: Recognition, etiologies, and treatment. Clin. Geriatr. Med. 1997, 13, 717–735. [Google Scholar] [CrossRef]
- French, S.A.; Folsom, A.R.; Jeffery, R.W.; Williamson, D.F. Prospective study of intentionality of weight loss and mortality in older women: The Iowa Women’s Health Study. Am. J. Epidemiol. 1999, 149, 504–514. [Google Scholar] [CrossRef] [PubMed]
- Wannamethee, S.G.; Shaper, A.G.; Lennon, L. Reasons for intentional weight loss, unintentional weight loss, and mortality in older men. Arch. Intern. Med. 2005, 165, 1035–1040. [Google Scholar] [CrossRef] [PubMed]
- Ruscin, J.M.; Page, R.L.; Yeager, B.F.; Wallace, J.I. Tumor necrosis factor-alpha and involuntary weight loss in elderly, community-dwelling adults. Pharmacotherapy 2005, 25, 313–319. [Google Scholar] [CrossRef] [PubMed]
- Fearon, K.C.; Glass, D.J.; Guttridge, D.C. Cancer cachexia: Mediators, signaling, and metabolic pathways. Cell. MeTable 2012, 16, 153–166. [Google Scholar] [CrossRef] [PubMed]
- Artaza-Artabe, I.; Saez-Lopez, P.; Sanchez-Hernandez, N.; Fernandez-Gutierrez, N.; Malafarina, V. The relationship between nutrition and frailty: Effects of protein intake, nutritional supplementation, vitamin D and exercise on muscle metabolism in the elderly. A systematic review. Maturitas 2016, 93, 89–99. [Google Scholar] [CrossRef] [PubMed]
- Bartali, B.; Frongillo, E.A.; Bandinelli, S.; Lauretani, F.; Semba, R.D.; Fried, L.P.; Ferrucci, L. Low nutrient intake is an essential component of frailty in older persons. J. Gerontol. A. Biol. Sci. Med. Sci. 2006, 61, 589–593. [Google Scholar] [CrossRef] [PubMed]
- Gordon, S.R.; Kelly, S.L.; Sybyl, J.R.; Mill, M.; Kramer, A.; Jahnigen, D.W. Relationship in very elderly veterans of nutritional status, self-perceived chewing ability, dental status, and social isolation. J. Am. Geriatr. Soc. 1985, 33, 334–339. [Google Scholar] [CrossRef] [PubMed]
- Iwasaki, M.; Kimura, Y.; Sasiwongsaroj, K.; Kettratad-Pruksapong, M.; Suksudaj, S.; Ishimoto, Y.; Chang, N.Y.; Sakamoto, R.; Matsubayashi, K.; Songpaisan, Y.; et al. Association between objectively measured chewing ability and frailty: A cross-sectional study in central Thailand. Geriatr. Gerontol. Int. 2018, 18, 860–866. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.Y.; Kim, C.O.; Lim, H. Quality of diet and level of physical performance related to inflammatory markers in community-dwelling frail, elderly people. Nutrition 2017, 38, 48–53. [Google Scholar] [CrossRef] [PubMed]
- Hubbard, R.E.; O’Mahony, M.S.; Calver, B.L.; Woodhouse, K.W. Nutrition, inflammation, and leptin levels in aging and frailty. J. Am. Geriatr. Soc. 2008, 56, 279–284. [Google Scholar] [CrossRef] [PubMed]
- Carriere, I.; Dupuy, A.M.; Lacroux, A.; Cristol, J.P.; Delcourt, C. Biomarkers of inflammation and malnutrition associated with early death in healthy elderly people. J. Am. Geriatr. Soc. 2008, 56, 840–846. [Google Scholar] [CrossRef] [PubMed]
- National Cancer Center. Estimation of Dietary Trans Fat of Koreans; Korea Food and Drug Administration: Cheongsong gun, Korea, 2006; p. 15.
- Van Staveren, W.A.; de Groot, L.C.; Blauw, Y.H.; van der Wielen, R.P. Assessing diets of elderly people: Problems and approaches. Am. J. Clin. Nutr. 1994, 59, 221S–223S. [Google Scholar] [CrossRef] [PubMed]
- Sun, Y.; Roth, D.L.; Ritchie, C.S.; Burgio, K.L.; Locher, J.L. Reliability and predictive validity of energy intake measures from the 24-h dietary recalls of homebound older adults. J. Am. Diet. Assoc. 2010, 110, 773–778. [Google Scholar] [CrossRef] [PubMed]
| Dietary Parameters | Inflammatory Effect Score 1 |
|---|---|
| Carbohydrate (g) | 0.097 |
| Total fat (g) | 0.298 |
| Protein (g) | 0.021 |
| Fiber (g) | −0.663 |
| Vitamin A (μg RE) | −0.401 |
| Vitamin D (μg) | −0.446 |
| Vitamin E (mg) | −0.419 |
| Vitamin C (mg) | −0.424 |
| Beta carotene (μg) | −0.584 |
| Thiamin (mg) | −0.098 |
| Riboflavin (mg) | −0.068 |
| Niacin (mg) | −0.246 |
| Vitamin B6 (mg) | −0.365 |
| Folate (μg) | −0.190 |
| Vitamin B12 (mg) | 0.106 |
| Magnesium (mg) | −0.484 |
| Iron (mg) | 0.032 |
| Zinc (mg) | −0.313 |
| Selenium (μg) | −0.191 |
| n-3 fatty acids (g) | −0.436 |
| n-6 fatty acids (g) | −0.159 |
| Cholesterol (mg) | 0.110 |
| Saturated fat (g) | 0.373 |
| Polyunsaturated fatty acids (g) | −0.337 |
| Monounsaturated fatty acids (g) | −0.009 |
| Garlic (g) | −0.412 |
| Ginger (g) | −0.453 |
| Onion (g) | −0.301 |
| Turmeric (mg) | −0.785 |
| Green/black tea (g) | −0.536 |
| Pepper (g) | −0.131 |
| Alcohol (g) | −0.278 |
| Caffeine (g) | −0.110 |
| Variables | Non-Frail (n = 92) | Pre-Frail (n = 187) | Frail (n = 42) | p-Value |
|---|---|---|---|---|
| Age (years) | 75.98 ± 3.77 a | 76.78 ± 3.73 ab | 77.88 ± 3.79 b | 0.023 |
| Female, n (%) | 60 (65.2) | 129 (69.0) | 29 (69.0) | 0.087 |
| BMI (kg/m2) | 24.66 ± 3.34 | 24.68 ± 3.26 | 24.45 ± 3.36 | 0.918 |
| Medical history, n (%) | ||||
| Diabetes | 18 (19.6) | 51 (27.3) | 15 (35.7) | 0.124 |
| Cardio-cerebrovascular disease | 58 (63.0) | 140 (74.9) | 31 (73.8) | 0.113 |
| Gastrointestinal disease | 4 (4.3) | 16 (8.6) | 0 (0.0) | 0.079 |
| Musculoskeletal disease | 25 (27.2) | 45 (24.1) | 14 (33.3) | 0.451 |
| Depression | 1 (1.1) | 7 (3.7) | 1 (2.4) | 0.443 |
| Chewing ability, n (%) | ||||
| Poor | 20 (21.7) | 71 (38.0) | 3 (64.3) | <0.001 |
| Moderate | 9 (9.8) | 17 (9.1) | 2 (4.8) | |
| Good | 63 (68.5) | 99 (52.9) | 13 (31.0) | |
| Energy intake (kcal) | 1438.6 ± 414.3 a | 1305.2 ± 362.1 b | 1055.5 ± 340.9 c | <0.001 |
| MNA score | 24.09 ± 2.84 a | 22.03 ± 3.01 b | 19.76 ± 2.79 c | <0.001 |
| MNA category, n (%) | ||||
| Well-nourished | 53 (57.6) | 47 (25.1) | 3 (7.1) | <0.001 |
| At risk of malnutrition | 38 (41.3) | 134 (71.7) | 33 (78.6) | |
| Malnutrition | 1 (1.1) | 6 (3.2) | 6 (14.3) | |
| DII score | −0.81 ± 2.06 a | −0.15 ± 2.18 a | 2.27 ± 2.53 b | <0.001 |
| Variables | Correlation Index | Total (n = 321) | Good Nutritional Status (n = 103) | Poor Nutritional Status (n = 218) |
|---|---|---|---|---|
| DII score | Spearman’s ρ | 0.369 ** | 0.162 | 0.352 ** |
| p-value | <0.001 | 0.103 | <0.001 | |
| Age | Spearman’s ρ | 0.170 ** | 0.142 | 0.143 * |
| p-value | 0.002 | 0.151 | 0.035 | |
| Energy intake | Spearman’s ρ | −0.289 ** | −0.144 | −0.251 ** |
| p-value | <0.001 | 0.146 | <0.001 |
| Total (n = 321) | Good Nutritional Status (n = 103) | Poor Nutritional Status (n = 218) | |
|---|---|---|---|
| Non-frail/pre-frail, n | 92/187 | 53/47 | 39/140 |
| Crude OR (95% CI) | 1.15 (1.02–1.29) * | 1.01 (0.83–1.23) | 1.11 (0.94–1.30) |
| Adjusted OR (95% CI) 1 | 1.01 (0.85–1.19) | 0.86 (0.65–1.14) | 1.10 (0.87–1.39) |
| Non-frail/frail, n | 92/42 | 53/3 | 39/39 |
| Crude OR (95% CI) | 1.89 (1.55–2.31) ** | 2.15 (1.16–3.97) * | 1.73 (1.38–2.19) ** |
| Adjusted OR (95% CI) 1 | 1.64 (1.25–2.17) ** | 3.13 (0.96–10.20) | 1.68 (1.21–2.34) ** |
| Total (n = 321) | Good Nutritional Status (n = 103) | Poor Nutritional Status (n = 218) | |
|---|---|---|---|
| Weight loss/non-weight loss, n | 38/283 | 4/99 | 34/184 |
| Crude OR (95% CI) | 1.15 (1.02–1.29) * | 1.26 (0.82–1.94) | 1.09 (0.93–1.28) |
| Adjusted OR (95% CI) 1 | 1.29 (1.03–1.60) * | 1.50 (0.82–2.74) | 1.26 (0.99–1.60) |
| Exhaustion/non-exhaustion, n | 184/137 | 31/72 | 153/65 |
| Crude OR (95% CI) | 1.16 (1.05–1.27) ** | 0.96 (0.78–1.17) | 1.11 (0.98–1.26) |
| Adjusted OR (95% CI) 1 | 1.04 (0.90–1.20) | 0.89 (0.67–1.19) | 1.08 (0.89–1.30) |
| Low physical activity/non-low physical activity, n | 43/278 | 6/97 | 37/181 |
| Crude OR (95% CI) | 1.41 (1.21–1.63) ** | 1.50 (1.04–2.18) * | 1.33 (1.13–1.58) ** |
| Adjusted OR (95% CI) 1 | 1.16 (0.94–1.45) | 1.52 (0.90–2.57) | 1.08 (0.85–1.37) |
| Low walking speed/non-low walking speed, n | 65/256 | 11/92 | 54/164 |
| Crude OR (95% CI) | 1.43 (1.25–1.62) ** | 1.45 (1.08–1.95) * | 1.37 (1.18–1.59) ** |
| Adjusted OR (95% CI) 1 | 1.33 (1.10–1.61) ** | 1.35 (0.90–2.02) | 1.33 (1.07–1.65) * |
| Low grip strength/non-low grip strength, n | 74/247 | 22/81 | 52/166 |
| Crude OR (95% CI) | 1.28 (1.14–1.44) ** | 1.25 (1.00–1.55) | 1.33 (1.15–1.54) ** |
| Adjusted OR (95% CI) 1 | 1.34 (1.13–1.60) ** | 1.28 (0.94–1.74) | 1.37 (1.11–1.70) ** |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kim, D.; Park, Y. Association between the Dietary Inflammatory Index and Risk of Frailty in Older Individuals with Poor Nutritional Status. Nutrients 2018, 10, 1363. https://doi.org/10.3390/nu10101363
Kim D, Park Y. Association between the Dietary Inflammatory Index and Risk of Frailty in Older Individuals with Poor Nutritional Status. Nutrients. 2018; 10(10):1363. https://doi.org/10.3390/nu10101363
Chicago/Turabian StyleKim, Doyeon, and Yongsoon Park. 2018. "Association between the Dietary Inflammatory Index and Risk of Frailty in Older Individuals with Poor Nutritional Status" Nutrients 10, no. 10: 1363. https://doi.org/10.3390/nu10101363





