Novel Nutrition Profiling of New Zealanders’ Varied Eating Patterns
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Data Collection
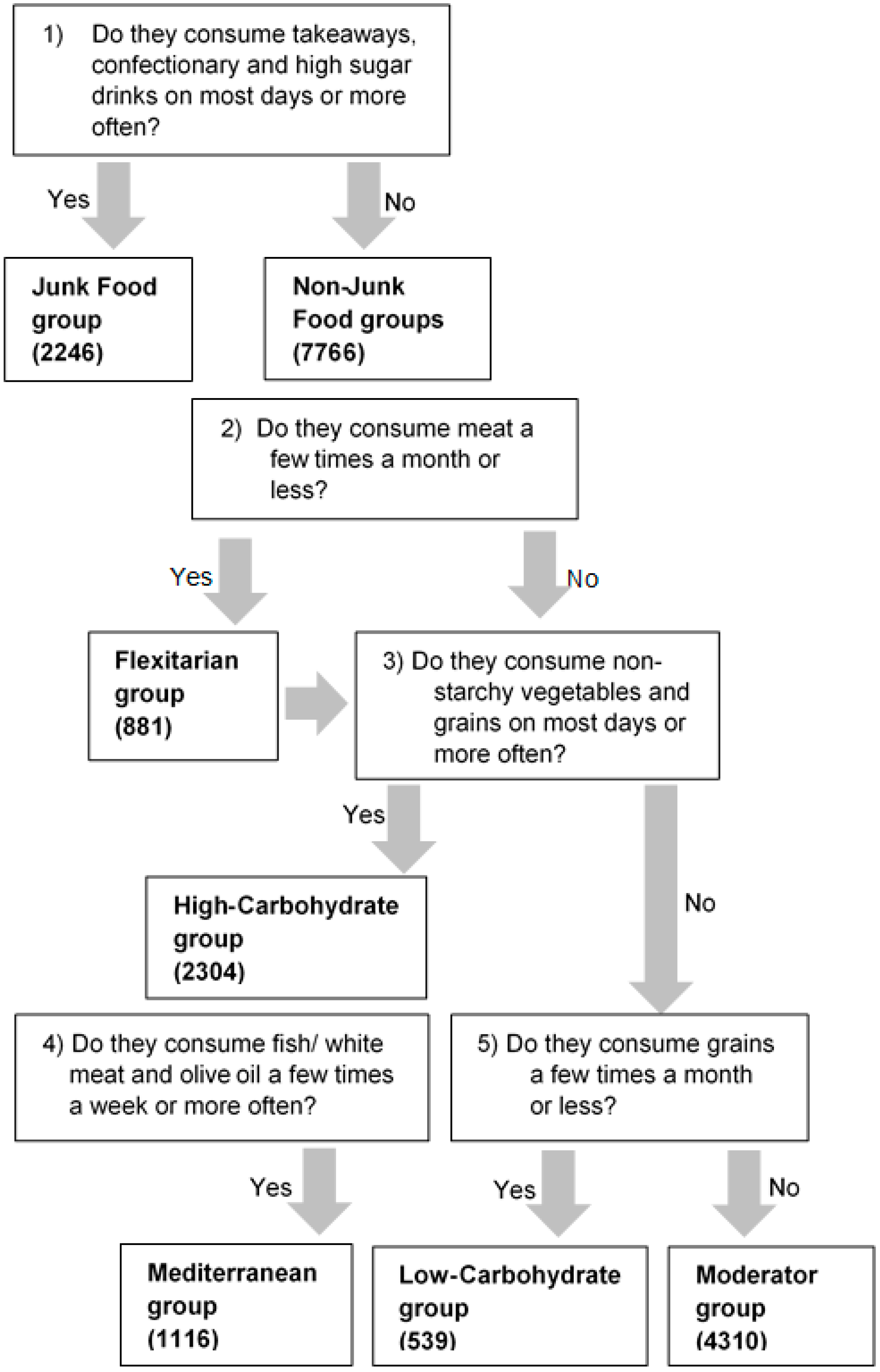
2.3. Profiling Procedures
2.4. Data Analysis
3. Results
3.1. Demographics of Total Sample
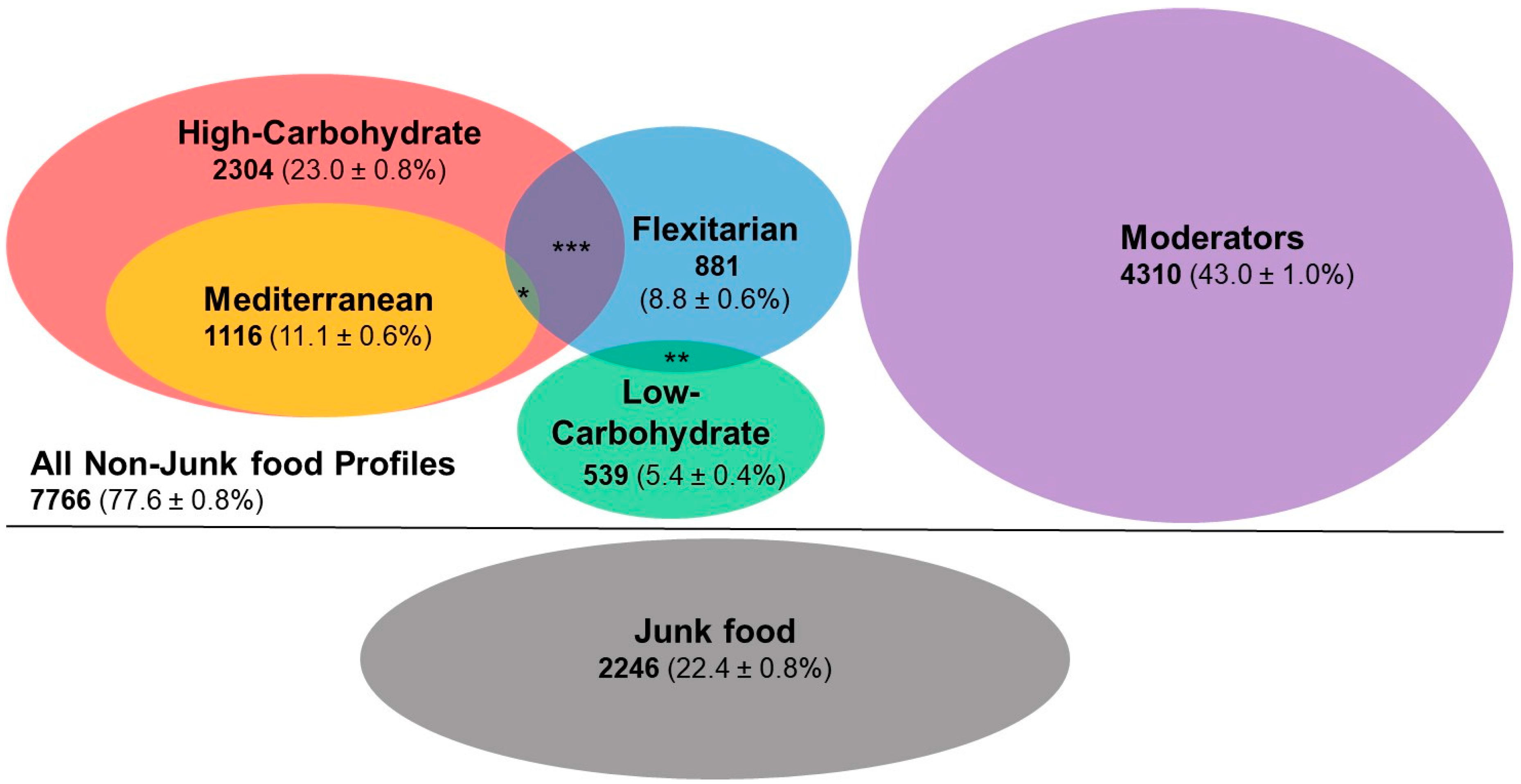
3.2. Prevalence of the Nutrition Profile Groups
3.3. Demographics of the Nutrition Profile Groups
3.4. Prevalence for Individual Nutrition Questions
4. Discussion
4.1. Future Directions
4.2. Study Limitations
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- World Health Organization. Obesity: Prevention and Managing the Global Epidemic: Report of a WHO Consultation; WHO Technical Report Series No. 894; World Health Organization: Geneva, Switzerland, 2000. [Google Scholar]
- Steyn, N.P.; Mann, J.; Bennett, P.H.; Temple, N.; Zimmet, P.; Tuomilehto, J.; Lindström, J.; Louheranta, A. Diet, nutrition and the prevention of type 2 diabetes. Public Health Nutr. 2004, 7, 147–165. [Google Scholar] [CrossRef] [PubMed]
- Reddy, K.S.; Katan, M.B. Diet, nutrition and the prevention of hypertension and cardiovascular diseases. Public Health Nutr. 2004, 7, 167–186. [Google Scholar] [CrossRef]
- Key, T.J.; Schatzkin, A.; Willett, W.C.; Allen, N.E.; Spencer, E.A.; Travis, R.C. Diet, nutrition and the prevention of cancer. Public Health Nutr. 2004, 7, 187–200. [Google Scholar] [CrossRef] [PubMed]
- Mozaffarian, D. Dietary and policy priorities for cardiovascular disease, diabetes, and obesity: A comprehensive review. Circulation 2016, 133, 187–225. [Google Scholar] [CrossRef] [PubMed]
- Hu, F.B. Dietary pattern analysis: A new direction in nutritional epidemiology. Curr. Opin. Lipidol. 2002, 13, 3–9. [Google Scholar] [CrossRef] [PubMed]
- Jacques, P.F.; Tucker, K.L. Are dietary patterns useful for understanding the role of diet in chronic disease? Am. J. Clin. Nutr. 2001, 73, 1–2. [Google Scholar] [PubMed]
- Jacobs, D.R.; Tapsell, L.C. Food, not nutrients, is the fundamental unit in nutrition. Nutr. Rev. 2007, 65, 439–450. [Google Scholar] [CrossRef] [PubMed]
- Pelto, G.H.; Freake, H.C. Social research in an integrated science of nutrition: Future directions. J. Nutr. 2003, 133, 1231–1234. [Google Scholar] [PubMed]
- Hu, F.B.; Rimm, E.; Smith-Warner, S.A.; Feskanich, D.; Stampfer, M.J.; Ascherio, A.; Sampson, L.; Willett, W.C. Reproducibility and validity of dietary patterns assessed with a food-frequency questionnaire. Am. J. Clin. Nutr. 1999, 69, 243–249. [Google Scholar] [PubMed]
- Hu, F.B.; Rimm, E.B.; Stampfer, M.J.; Ascherio, A.; Spiegelman, D.; Willett, W.C. Prospective study of major dietary patterns and risk of coronary heart disease in men. Am. J. Clin. Nutr. 2000, 72, 912–921. [Google Scholar] [PubMed]
- Reidlinger, D.P.; Darzi, J.; Hall, W.L.; Seed, P.T.; Chowienczyk, P.J.; Sanders, T.A.B. How effective are current dietary guidelines for cardiovascular disease prevention in healthy middle-aged and older men and women? A randomized controlled trial. Am. J. Clin. Nutr. 2015, 101, 922–930. [Google Scholar] [CrossRef] [PubMed]
- Grosso, G.; Marventano, S.; Yang, J.; Micek, A.; Pajak, A.; Scalfi, L.; Galvano, F.; Kales, S.N. A comprehensive meta-analysis on evidence of mediterranean diet and cardiovascular disease: Are individual components equal? Crit. Rev. Food Sci. Nutr. 2017, 57, 3218–3232. [Google Scholar] [CrossRef] [PubMed]
- Ndanuko, R.N.; Tapsell, L.C.; Charlton, K.E.; Neale, E.P.; Batterham, M.J. Dietary patterns and blood pressure in adults: A systematic review and meta-analysis of randomized controlled trials. Adv. Nutr. Int. Rev. J. 2016, 7, 76–89. [Google Scholar] [CrossRef] [PubMed]
- Estruch, R.; Ros, E.; Salas-Salvadó, J.; Covas, M.-I.; Corella, D.; Arós, F.; Gómez-Gracia, E.; Ruiz-Gutiérrez, V.; Fiol, M.; Lapetra, J.; et al. Primary prevention of cardiovascular disease with a mediterranean diet. N. Engl. J. Med. 2013, 368, 1279–1290. [Google Scholar] [CrossRef] [PubMed]
- Schwingshackl, L.; Missbach, B.; König, J.; Hoffmann, G. Adherence to a mediterranean diet and risk of diabetes: A systematic review and meta-analysis. Public Health Nutr. 2014, 18, 1292–1299. [Google Scholar] [CrossRef] [PubMed]
- Jannasch, F.; Kröger, J.; Schulze, M.B. Dietary patterns and type 2 diabetes: A systematic literature review and meta-analysis of prospective studies. J. Nutr. 2017, 147, 1174–1182. [Google Scholar] [CrossRef] [PubMed]
- Siervo, M.; Lara, J.; Chowdhury, S.; Ashor, A.; Oggioni, C.; Mathers, J.C. Effects of the dietary approach to stop hypertension (DASH) diet on cardiovascular risk factors: A systematic review and meta-analysis. Br. J. Nutr. 2014, 113, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Liyanage, T.; Ninomiya, T.; Wang, A.; Neal, B.; Jun, M.; Wong, M.G.; Jardine, M.; Hillis, G.S.; Perkovic, V. Effects of the mediterranean diet on cardiovascular outcomes—A systematic review and meta-analysis. PLoS ONE 2016, 11, e0159252. [Google Scholar] [CrossRef] [PubMed]
- Nissensohn, M.; Román-Viñas, B.; Sánchez-Villegas, A.; Piscopo, S.; Serra-Majem, L. The effect of the mediterranean diet on hypertension: A systematic review and meta-analysis. J. Nutr. Educ. Behav. 2016, 48, 42–53. [Google Scholar] [CrossRef] [PubMed]
- Bazzano, L.A.; Hu, T.; Reynolds, K.; Yao, L.; Bunol, C.; Liu, Y.; Chen, C.; Klag, M.J.; Whelton, P.K.; He, J. Effects of low-carbohydrate and low-fat diets. Ann. Int. Med. 2014, 161, 309–318. [Google Scholar] [CrossRef] [PubMed]
- Nakamura, Y.; Okuda, N.; Okamura, T.; Kadota, A.; Miyagawa, N.; Hayakawa, T.; Kita, Y.; Fujiyoshi, A.; Nagai, M.; Takashima, N.; et al. Low carbohydrate diets and cardiovascualr and total mortality in Japanes: A 29-year follow-up of NIPPON DATA80. Br. J. Nutr. 2014, 112, 916–924. [Google Scholar] [CrossRef] [PubMed]
- Schofield, G.; Henderson, G.; Thornley, S.; Crofts, C. Very low-carbohydrate diets in the management of diabetes revisited. N. Z. Med. J. 2016, 129, 67–74. [Google Scholar] [PubMed]
- Te Morenga, L.; Mallard, S.; Mann, J. Dietary sugars and body weight: Systematic review and meta-analyses of randomised controlled trials and cohort studies. Br. Med. J. 2013, 346, e7492. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Guideline: Sugars Intake for Adults and Children; World Health Organization: Geneva, Switzerland, 2015. [Google Scholar]
- Key, T.J.; Appleby, P.N.; Rosell, M.S. Health effects of vegetarian and vegan diets. Proc. Nutr. Soc. 2006, 65, 35–41. [Google Scholar] [CrossRef] [PubMed]
- Appleby, P.N.; Thorogood, M.; Mann, J.I.; Key, T.J. The oxford vegetarian study: An overview. Am. J. Clin. Nutr. 1999, 70, 525s–531s. [Google Scholar] [PubMed]
- Ministry of Health. Eating and Activity Guidelines for New Zealand Adults. Available online: http://www.health.govt.nz/publication/eating-and-activity-guidelines-new-zealand-adults (accessed on 1 November 2015).
- Health Promotion Agency. 2016 Health and Lifestyles Survey Questionnaire; Health Promotion Agency Research and Evaluation Unit: Wellington, New Zealand, 2017. [Google Scholar]
- Health Promotion Agency. 2012 Health and Lifestyles Survey; Health Promotion Agency Research and Evaluation Unit: Wellington, New Zealand, 2013. [Google Scholar]
- Ministry of Health. A Focus on Nutrition: Key Findings of the 2008/09 New Zealand Adult Nutrition Survey; Ministry of Health: Wellington, New Zealand, 2011.
- Ministry of Health. Annual Update of Key Results 2015/2016: New Zealand Health Survey; Ministry of Health: Wellington, New Zealand, 2016.
- Prendergast, K. Towards a Framework for Postive Health; Auckland University of Technology: Auckland, New Zealand, 2016. [Google Scholar]
- Mackay, L.M.; Schofield, G.M.; Jarden, A.; Prendergast, K. Sovereign Wellbeing Index; Auckland University of Technology: Auckland, New Zealand, 2015. [Google Scholar]
- Maclaren, O.; Mackay, L.; Schofield, G.; Zinn, C. The development and validation of a new survey tool: The first step to profiling New Zealanders’ eating styles and moving patterns. Aust. N. Z. J. Public Health 2016, 40, 396–397. [Google Scholar] [CrossRef] [PubMed]
- Bach-Faig, A.; Berry, E.M.; Lairon, D.; Reguant, J.; Trichopoulou, A.; Dernini, S.; Medina, F.X.; Battino, M.; Belahsen, R.; Miranda, G.; et al. Mediterranean diet pyramid today. Science and cultural updates. Public Health Nutr. 2011, 14, 2274–2284. [Google Scholar] [CrossRef] [PubMed]
- Human Potential Centre. Sovereign Wellbeing Index (1-2012): Technical Report (Edition 1.0); Auckland University of Technology: Auckland, New Zealand, 2012. [Google Scholar]
- Statistics New Zealand. 2013 Census Data and Reports; Statistics New Zealand: Wellington, New Zealand, 2013.
- Fenech, M.; El-Sohemy, A.; Cahill, L.; Ferguson, L.R.; French, T.A.C.; Tai, E.S.; Milner, J.; Koh, W.P.; Xie, L.; Zucker, M.; et al. Nutrigenetics and nutrigenomics: Viewpoints on the current status and applications in nutrition research and practice. J. Nutr. Nutr. 2011, 4, 69–89. [Google Scholar] [CrossRef] [PubMed]
- Gemming, L.; Jiang, Y.; Swinburn, B.; Utter, J.; Ni Mhurchu, C. Under-reporting remains a key limitation of self-reported dietary intake: An analysis of the 2008/09 New Zealand Adult Nutrition survey. Eur. J. Clin. Nutr. 2013, 259–264. [Google Scholar] [CrossRef] [PubMed]
- Ministry of Health. A Potrait of Health. Key Results of the 2006/07 New Zealand Health Survey; Ministry of Health: Wellington, New Zealand, 2008.
| Questions | Response Options |
|---|---|
On average over the past 4 weeks, how often have you consumed the following food?
|
|
| N | % | |
|---|---|---|
| Total Population | 10,012 | 100.0 |
| Gender | 9904 | 98.9 |
| Male | 4797 | 47.9 |
| Female | 5107 | 51.0 |
| Age | 8614 | 86.0 |
| under 20 years | 270 | 2.7 |
| 20–29 years | 1692 | 16.9 |
| 30–39 years | 1602 | 16.0 |
| 40–49 years | 1655 | 16.5 |
| 50–59 years | 1694 | 16.9 |
| 60 years and over | 1701 | 17.0 |
| Ethnicity 1 | 10,444 | 97.4 |
| Maori | 956 | 8.9 |
| European | 7605 | 70.9 |
| Pacific people | 310 | 2.9 |
| Asian | 1269 | 11.8 |
| Other | 304 | 2.8 |
| Labour Force Status | 9613 | 96.0 |
| Employed | 5503 | 55.0 |
| Unemployed | 714 | 7.1 |
| Not in the labour force 2 | 2822 | 28.2 |
| Other | 574 | 5.7 |
| Quintiles of Household Income | 7654 | 76.4 |
| ≤$30,000 | 1821 | 18.2 |
| $30,001–$50,000 | 1456 | 14.5 |
| $50,001–$70,000 | 1305 | 13.0 |
| $70,001–$100,000 | 1535 | 15.3 |
| ≥$100,001 | 1537 | 15.4 |
| Food Group | Consumpt-Ion Level 3 | Total Sample | Junk | Flexitarian | Mediterranean | Low-Carbohydrate | High-Carbohydrate | Moderator | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n | % | 95% CI 2 | n | % | 95% CI | n | % | 95% CI | n | % | 95% CI | n | % | 95% CI | n | % | 95% CI | n | % | 95% CI | ||
| Total N | 10,012 | 2246 | 881 | 1116 | 539 | 2304 | 4310 | |||||||||||||||
| All grain products | Avoiders | 413 | 4.3 | (3.9–4.7) | 102 | 4.6 | (3.8–5.5) | 57 | 6.5 | (5.0–8.3) | 0 | 0.0 | (0.0–0.0) | 116 | 21.5 | (18.2–25.1) | 0 | 0.0 | (0.0–0.0) | 145 | 3.7 | (3.1–4.3) |
| Limiters | 1371 | 14.3 | (13.6–15.0) | 290 | 13.0 | (11.7–14.5) | 208 | 23.7 | (21.0–26.6) | 0 | 0.0 | (0.0–0.0) | 423 | 78.5 | (74.9–81.8) | 0 | 0.0 | (0.0–0.0) | 495 | 12.6 | (11.6–13.7) | |
| Includers | 7824 | 81.4 | (80.6–82.2) | 1837 | 82.4 | (80.8–84.0) | 612 | 69.8 | (66.7–72.8) | 1116 | 100.0 | (100.0–100.0) | 0 | 0.0 | (0.0–0.0) | 2304 | 100.0 | (100.0–100.0) | 3287 | 83.7 | (82.5–84.8) | |
| Full-fat dairy products | Avoiders | 951 | 9.9 | (9.3–10.5) | 137 | 6.1 | (5.2–7.2) | 154 | 17.5 | (15.1–20.1) | 112 | 10.0 | (8.4–11.9) | 89 | 16.5 | (13.6–19.8) | 281 | 12.2 | (10.9–13.6) | 354 | 9.0 | (8.2–9.9) |
| Limiters | 1531 | 15.9 | (15.2–16.6) | 281 | 12.6 | (11.3–14.0) | 246 | 28.0 | (25.1–31.0) | 137 | 12.3 | (10.5–14.3) | 112 | 20.8 | (17.5–24.4) | 294 | 12.8 | (11.5–14.2) | 649 | 16.5 | (15.4–17.7) | |
| Includers | 7125 | 74.2 | (73.3–75.1) | 1814 | 81.3 | (79.6–82.8) | 479 | 54.5 | (51.2–57.8) | 866 | 77.7 | (75.2–80.0) | 338 | 62.7 | (58.6–66.7) | 1726 | 75.0 | (73.2–76.7) | 2921 | 74.4 | (73.1–75.8) | |
| Butter | Avoiders | 2612 | 27.2 | (26.3–28.1) | 523 | 23.5 | (21.7–25.3) | 322 | 36.6 | (33.5–39.8) | 226 | 20.3 | (18.0–22.7) | 169 | 31.4 | (27.5–35.4) | 611 | 26.5 | (24.8–28.4) | 1078 | 27.5 | (26.1–28.9) |
| Limiters | 2461 | 25.6 | (24.7–26.5) | 470 | 21.1 | (19.4–22.8) | 284 | 32.3 | (29.2–35.4) | 304 | 27.2 | (24.7–29.9) | 128 | 23.7 | (20.3–27.5) | 640 | 27.8 | (26.0–29.7) | 1024 | 26.1 | (24.8–27.5) | |
| Includers | 4530 | 47.2 | (46.2–48.2) | 1235 | 55.4 | (53.4–57.5) | 274 | 31.1 | (28.1–34.3) | 586 | 52.5 | (49.6–55.4) | 242 | 44.9 | (40.7–49.1) | 1051 | 45.7 | (43.6–47.7) | 1820 | 46.4 | (44.8–48.0) | |
| Low-fat dairy products | Avoiders | 2216 | 23.1 | (22.3–23.9) | 471 | 21.2 | (19.6–23.0) | 269 | 30.5 | (27.6–33.6) | 213 | 19.1 | (16.9–21.5) | 181 | 33.6 | (29.7–37.6) | 502 | 21.8 | (20.2–23.5) | 872 | 22.2 | (21.0–23.6) |
| Limiters | 1723 | 18.0 | (17.2–18.8) | 383 | 17.3 | (15.7–18.9) | 229 | 26.0 | (23.2–29.0) | 135 | 12.1 | (10.3–14.1) | 99 | 18.4 | (15.3–21.8) | 298 | 13.0 | (11.6–14.4) | 757 | 19.3 | (18.1–20.6) | |
| Includers | 5654 | 58.9 | (57.9–59.9) | 1366 | 61.5 | (59.5–63.5) | 383 | 43.5 | (40.2–46.8) | 767 | 68.8 | (66.0–71.5) | 259 | 48.1 | (43.9–52.3) | 1501 | 65.2 | (63.3–67.2) | 2291 | 58.4 | (56.9–60.0) | |
| Eggs | Avoiders | 623 | 6.5 | (6.0–7.0) | 171 | 7.7 | (6.6–8.8) | 151 | 17.2 | (14.8–19.8) | 25 | 2.2 | (1.5–3.2) | 42 | 7.8 | (5.8–10.3) | 120 | 5.2 | (4.4–6.2) | 193 | 4.9 | (4.3–5.6) |
| Limiters | 2502 | 26.0 | (25.1–26.9) | 534 | 24.0 | (22.2–25.8) | 358 | 40.7 | (37.5–44.0) | 203 | 18.2 | (16.0–20.5) | 131 | 24.3 | (20.9–28.1) | 528 | 22.9 | (21.3–24.7) | 1035 | 26.4 | (25.0–27.8) | |
| Includers | 6481 | 67.5 | (66.6–68.4) | 1523 | 68.4 | (66.4–70.3) | 370 | 42.1 | (38.9–45.4) | 888 | 79.6 | (77.1–81.9) | 365 | 67.8 | (63.8–71.7) | 1654 | 71.9 | (70.0–73.7) | 2698 | 68.7 | (67.3–70.2) | |
| Margarine or other non-butter spreads | Avoiders | 2470 | 25.7 | (24.8–26.6) | 478 | 21.5 | (19.9–23.3) | 303 | 34.5 | (31.4–37.7) | 307 | 27.5 | (24.9–30.2) | 223 | 41.4 | (37.3–45.6) | 644 | 28.0 | (26.2–29.8) | 930 | 23.7 | (22.4–25.0) |
| Limiters | 1357 | 14.1 | (13.4–14.8) | 272 | 12.2 | (10.9–13.7) | 215 | 24.5 | (21.7–27.4) | 115 | 10.3 | (8.6–12.2) | 76 | 14.1 | (11.4–17.2) | 267 | 11.6 | (10.3–13.0) | 577 | 14.7 | (13.6–15.8) | |
| Includers | 5774 | 60.1 | (59.1–61.1) | 1471 | 66.2 | (64.2–68.2) | 361 | 41.1 | (37.9–44.3) | 694 | 62.2 | (59.3–65.0) | 240 | 44.5 | (40.4–48.7) | 1391 | 60.4 | (58.4–62.4) | 2421 | 61.6 | (60.1–63.1) | |
| Oils: olive, avocado, macadamia, coconut | Avoiders | 2796 | 29.2 | (28.3–30.1) | 697 | 31.4 | (29.5–33.4) | 310 | 35.2 | (32.1–38.4) | 0 | 0.0 | (0.0–0.0) | 147 | 27.4 | (23.7–31.3) | 524 | 22.8 | (21.1–24.6) | 1191 | 30.4 | (29.0–31.8) |
| Limiters | 2283 | 23.8 | (22.9–24.7) | 462 | 20.8 | (19.2–22.5) | 267 | 30.3 | (27.3–33.4) | 0 | 0.0 | (0.0–0.0) | 108 | 20.1 | (16.9–23.7) | 522 | 22.7 | (21.1–24.5) | 981 | 25.0 | (23.7–26.4) | |
| Includers | 4508 | 47.0 | (46.0–48.0) | 1061 | 47.8 | (45.7–49.9) | 304 | 34.5 | (31.4–37.7) | 1116 | 100.0 | (100.0–100.0) | 282 | 52.5 | (48.3–56.7) | 1250 | 54.4 | (52.4–56.5) | 1749 | 44.6 | (43.1–46.2) | |
| Oils: any other vegetable oil | Avoiders | 1902 | 19.8 | (19.0–20.6) | 388 | 17.4 | (15.9–19.1) | 229 | 26.1 | (23.2–29.0) | 198 | 17.8 | (15.6–20.1) | 167 | 31.0 | (27.2–35.0) | 389 | 16.9 | (15.4–18.5) | 783 | 20.0 | (18.8–21.3) |
| Limiters | 2316 | 24.2 | (23.3–25.1) | 476 | 21.4 | (19.7–23.1) | 312 | 35.5 | (32.4–38.7) | 171 | 15.3 | (13.3–17.5) | 117 | 21.7 | (18.4–25.4) | 472 | 20.5 | (18.9–22.2) | 994 | 25.4 | (24.0–26.7) | |
| Includers | 5372 | 56.0 | (55.0–57.0) | 1360 | 61.2 | (59.1–63.2) | 338 | 38.5 | (35.3–41.7) | 746 | 66.9 | (64.1–69.6) | 254 | 47.2 | (43.0–51.4) | 1437 | 62.5 | (60.5–64.5) | 2142 | 54.7 | (53.1–56.2) | |
| Red meat | Avoiders | 674 | 7.0 | (6.5–7.5) | 140 | 6.3 | (5.3–7.4) | 356 | 40.4 | (37.2–43.7) | 38 | 3.4 | (2.5–4.6) | 35 | 6.5 | (4.6–8.8) | 193 | 8.4 | (7.3–9.6) | 109 | 2.8 | (2.3–3.3) |
| Limiters | 1479 | 15.4 | (14.7–16.1) | 270 | 12.1 | (10.8–13.5) | 525 | 59.6 | (56.3–62.8) | 92 | 8.2 | (6.7–10.0) | 83 | 15.4 | (12.5–18.6) | 264 | 11.5 | (10.2–12.8) | 446 | 11.4 | (10.4–12.4) | |
| Includers | 7454 | 77.6 | (76.8–78.4) | 1816 | 81.6 | (79.9–83.2) | 0 | 0.0 | (0.0–0.0) | 986 | 88.4 | (86.4–90.1) | 421 | 78.1 | (74.5–81.4) | 1845 | 80.1 | (78.5–81.7) | 3372 | 85.9 | (84.8–86.9) | |
| White meat | Avoiders | 478 | 5.0 | (4.6–5.4) | 92 | 4.1 | (3.4–5.0) | 303 | 34.4 | (31.3–37.6) | 13 | 1.2 | (0.7–1.9) | 31 | 5.8 | (4.0–8.0) | 132 | 5.7 | (4.8–6.7) | 52 | 1.3 | (1.0–1.7) |
| Limiters | 1252 | 13.0 | (12.3–13.7) | 235 | 10.5 | (9.3–11.9) | 578 | 65.6 | (62.4–68.7) | 26 | 2.3 | (1.6–3.3) | 55 | 10.2 | (7.9–13.0) | 210 | 9.1 | (8.0–10.3) | 310 | 7.9 | (7.1–8.8) | |
| Includers | 7883 | 82.0 | (81.2–82.8) | 1902 | 85.3 | (83.8–86.8) | 0 | 0.0 | (0.0–0.0) | 1077 | 96.5 | (95.3–97.5) | 453 | 84.0 | (80.8–87.0) | 1961 | 85.1 | (83.7–86.6) | 3567 | 90.8 | (89.9–91.7) | |
| Protein powders and or bars | Avoiders | 7049 | 73.5 | (72.6–74.4) | 1475 | 66.5 | (64.5–68.5) | 712 | 81.0 | (78.3–83.5) | 826 | 74.1 | (71.5–76.7) | 416 | 77.6 | (73.9–81.0) | 1815 | 78.9 | (77.2–80.6) | 2856 | 72.9 | (71.4–74.2) |
| Limiters | 1138 | 11.9 | (11.3–12.5) | 295 | 13.3 | (11.9–14.8) | 102 | 11.6 | (9.6–13.8) | 116 | 10.4 | (8.7–12.3) | 47 | 8.8 | (6.6–11.4) | 222 | 9.7 | (8.5–10.9) | 493 | 12.6 | (11.6–13.6) | |
| Includers | 1397 | 14.6 | (13.9–15.3) | 447 | 20.2 | (18.5–21.9) | 65 | 7.4 | (5.8–9.3) | 172 | 15.4 | (13.4–17.7) | 73 | 13.6 | (10.9–16.7) | 262 | 11.4 | (10.1–12.7) | 571 | 14.6 | (13.5–15.7) | |
| Processed meat | Avoiders | 2152 | 22.4 | (21.6–23.2) | 357 | 16.0 | (14.6–17.6) | 498 | 56.5 | (53.2–59.8) | 235 | 21.1 | (18.7–23.5) | 163 | 30.4 | (26.6–34.3) | 576 | 25.0 | (23.3–26.8) | 750 | 19.1 | (17.9–20.4) |
| Limiters | 4229 | 44.0 | (43.0–45.0) | 800 | 36.0 | (34.0–38.0) | 383 | 43.5 | (40.2–46.8) | 514 | 46.1 | (43.1–49.0) | 256 | 47.7 | (43.5–51.9) | 1057 | 45.9 | (43.9–48.0) | 1809 | 46.1 | (44.5–47.6) | |
| Includers | 3222 | 33.6 | (32.7–34.5) | 1068 | 48.0 | (45.9–50.1) | 0 | 0.0 | (0.0–0.0) | 367 | 32.9 | (30.2–35.7) | 118 | 22.0 | (18.6–25.6) | 669 | 29.1 | (27.2–30.9) | 1367 | 34.8 | (33.3–36.3) | |
| Fish and shellfish | Avoiders | 2172 | 22.5 | (21.7–23.3) | 532 | 23.8 | (22.0–25.5) | 368 | 42.0 | (38.7–45.2) | 121 | 10.8 | (9.1–12.8) | 109 | 20.2 | (17.0–23.8) | 435 | 18.9 | (17.3–20.5) | 848 | 21.5 | (20.2–22.8) |
| Limiters | 4560 | 47.3 | (46.3–48.3) | 937 | 41.8 | (39.8–43.9) | 380 | 43.3 | (40.1–46.6) | 525 | 47.0 | (44.1–50.0) | 275 | 51.0 | (46.8–55.2) | 1115 | 48.4 | (46.4–50.4) | 1950 | 49.5 | (47.9–51.0) | |
| Includers | 2903 | 30.1 | (29.2–31.0) | 771 | 34.4 | (32.5–36.4) | 129 | 14.7 | (12.5–17.2) | 470 | 42.1 | (39.2–45.0) | 155 | 28.8 | (25.1–32.7) | 754 | 32.7 | (30.8–34.7) | 1145 | 29.0 | (27.6–30.5) | |
| Fruit | Avoiders | 339 | 3.5 | (3.1–3.9) | 103 | 4.6 | (3.8–5.5) | 46 | 5.2 | (3.9–6.9) | 11 | 1.0 | (0.5–1.7) | 27 | 5.0 | (3.4–7.1) | 30 | 1.3 | (0.9–1.8) | 137 | 3.5 | (2.9–4.1) |
| Limiters | 1260 | 13.1 | (12.4–13.8) | 321 | 14.3 | (12.9–15.8) | 191 | 21.8 | (19.1–24.6) | 40 | 3.6 | (2.6–4.8) | 58 | 10.8 | (8.4–13.6) | 114 | 4.9 | (4.1–5.9) | 589 | 14.9 | (13.8–16.1) | |
| Includers | 8042 | 83.4 | (82.7–84.1) | 1820 | 81.1 | (79.4–82.7) | 640 | 73.0 | (70.0–75.8) | 1065 | 95.4 | (94.1–96.5) | 454 | 84.2 | (81.0–87.1) | 2160 | 93.8 | (92.7–94.7) | 3219 | 81.6 | (80.4–82.8) | |
| Starchy vegetables | Avoiders | 297 | 3.1 | (2.8–3.4) | 64 | 2.9 | (2.2–3.6) | 61 | 7.0 | (5.4–8.8) | 10 | 0.9 | (0.5–1.6) | 37 | 6.9 | (5.0–9.2) | 27 | 1.2 | (0.8–1.7) | 118 | 3.0 | (2.5–3.6) |
| Limiters | 1315 | 13.6 | (12.9–14.3) | 238 | 10.6 | (9.4–11.9) | 272 | 31.1 | (28.1–34.2) | 66 | 5.9 | (4.6–7.4) | 70 | 13.0 | (10.3–16.0) | 184 | 8.0 | (6.9–9.1) | 595 | 15.1 | (14.0–16.2) | |
| Includers | 8022 | 83.3 | (82.6–84.0) | 1940 | 86.5 | (85.1–87.9) | 543 | 62.0 | (58.7–65.2) | 1040 | 93.2 | (91.6–94.6) | 432 | 80.1 | (76.6–83.3) | 2093 | 90.8 | (89.6–92.0) | 3228 | 81.9 | (80.7–83.1) | |
| Non-starchy vegetables | Avoiders | 553 | 5.8 | (5.3–6.3) | 145 | 6.5 | (5.5–7.6) | 88 | 10.1 | (8.2–12.2) | 0 | 0.0 | (0.0–0.0) | 0 | 0.0 | (0.0–0.0) | 0 | 0.0 | (0.0–0.0) | 320 | 8.2 | (7.3–9.1) |
| Limiters | 1113 | 11.6 | (11.0–12.2) | 236 | 10.6 | (9.4–11.9) | 210 | 24.0 | (21.3–26.9) | 0 | 0.0 | (0.0–0.0) | 0 | 0.0 | (0.0–0.0) | 0 | 0.0 | (0.0–0.0) | 667 | 17.0 | (15.9–18.2) | |
| Includers | 7930 | 82.6 | (81.8–83.4) | 1847 | 82.9 | (81.3–84.4) | 576 | 65.9 | (62.7–69.0) | 1116 | 100.0 | (100.0–100.0) | 539 | 100.0 | (100.0–100.0) | 2304 | 100.0 | (100.0–100.0) | 2932 | 74.8 | (73.4–76.2) | |
| Cakes and biscuits 4 | Avoiders | 584 | 6.1 | (5.6–6.6) | 53 | 2.4 | (1.8–3.1) | 108 | 12.3 | (10.3–14.6) | 59 | 5.3 | (4.1–6.7) | 89 | 16.5 | (13.6–19.9) | 112 | 4.9 | (4.0–5.8) | 254 | 6.4 | (5.7–7.2) |
| Limiters | 2676 | 27.8 | (26.9–28.7) | 256 | 11.4 | (10.2–12.8) | 355 | 40.5 | (37.3–43.8) | 242 | 21.7 | (19.3–24.2) | 224 | 41.6 | (37.5–45.8) | 548 | 23.8 | (22.1–25.6) | 1367 | 34.7 | (33.2–36.2) | |
| Includers | 6370 | 66.1 | (65.2–67.0) | 1932 | 86.2 | (84.7–87.6) | 413 | 47.1 | (43.9–50.5) | 815 | 73.0 | (70.4–75.6) | 225 | 41.8 | (37.7–46.0) | 1644 | 71.4 | (69.5–73.2) | 2318 | 58.8 | (57.3–60.4) | |
| Nuts | Avoiders | 1941 | 20.2 | (19.4–21.0) | 434 | 19.5 | (17.9–21.2) | 210 | 23.9 | (21.2–26.9) | 98 | 8.8 | (7.2–10.5) | 123 | 22.9 | (19.5–26.6) | 323 | 14.0 | (12.6–15.5) | 891 | 22.6 | (21.4–24.0) |
| Limiters | 3282 | 34.1 | (33.2–35.0) | 651 | 29.2 | (27.3–31.1) | 294 | 33.5 | (30.5–36.7) | 315 | 28.2 | (25.6–30.9) | 168 | 31.2 | (27.4–35.2) | 739 | 32.1 | (30.2–34.0) | 1495 | 38.0 | (36.5–39.5) | |
| Includers | 4393 | 45.7 | (44.7–46.7) | 1144 | 51.3 | (49.2–53.4) | 373 | 42.5 | (39.3–45.8) | 703 | 63.0 | (60.1–65.8) | 247 | 45.9 | (41.7–50.1) | 1242 | 53.9 | (51.9–55.9) | 1550 | 39.4 | (37.9–40.9) | |
| Confectionary: sweets and chocolate | Avoiders | 1067 | 11.1 | (10.5–11.7) | 48 | 2.1 | (1.6–2.8) | 166 | 19.0 | (16.5–21.7) | 126 | 11.3 | (9.5–13.3) | 123 | 22.9 | (19.5–26.6) | 275 | 11.9 | (10.7–13.3) | 502 | 12.8 | (11.7–13.8) |
| Limiters | 3875 | 40.3 | (39.3–41.3) | 286 | 12.8 | (11.4–14.2) | 444 | 50.7 | (47.4–54.0) | 511 | 45.8 | (42.9–48.8) | 273 | 50.8 | (46.6–55.1) | 1067 | 46.3 | (44.3–48.4) | 1925 | 48.9 | (47.4–50.5) | |
| Includers | 4682 | 48.6 | (47.6–49.6) | 1909 | 85.1 | (83.6–86.5) | 265 | 30.3 | (27.3–33.4) | 478 | 42.9 | (40.0–45.8) | 141 | 26.3 | (22.7–30.1) | 961 | 41.7 | (39.7–43.8) | 1507 | 38.3 | (36.8–39.8) | |
| Full sugar soft drinks 5 | Avoiders | 3284 | 34.1 | (33.2–35.0) | 293 | 13.1 | (11.7–14.5) | 405 | 46.2 | (42.9–49.5) | 480 | 43.0 | (40.1–45.9) | 302 | 56.1 | (51.9–60.3) | 1028 | 44.6 | (42.6–46.7) | 1398 | 35.5 | (34.1–37.1) |
| Limiters | 3038 | 31.6 | (30.7–32.5) | 314 | 14.0 | (12.6–15.5) | 327 | 37.3 | (34.1–40.5) | 436 | 39.1 | (36.2–42.0) | 157 | 29.2 | (25.5–33.1) | 860 | 37.3 | (35.4–39.3) | 1461 | 37.1 | (35.6–38.7) | |
| Includers | 3303 | 34.3 | (33.4–35.2) | 1634 | 72.9 | (71.0–74.7) | 145 | 16.5 | (14.2–19.1) | 200 | 17.9 | (15.8–20.3) | 79 | 14.7 | (11.9–17.9) | 416 | 18.1 | (16.5–19.7) | 1074 | 27.3 | (25.9–28.7) | |
| Takeaways 6 | Avoiders | 1506 | 15.6 | (14.9–16.3) | 164 | 7.3 | (6.3–8.4) | 246 | 28.0 | (25.1–31.1) | 206 | 18.5 | (16.3–20.8) | 137 | 25.5 | (21.9–29.3) | 437 | 19.0 | (17.4–20.6) | 607 | 15.4 | (14.3–16.6) |
| Limiters | 5542 | 57.6 | (56.6–58.6) | 976 | 43.5 | (41.5–45.6) | 541 | 61.6 | (58.4–64.8) | 736 | 65.9 | (63.1–68.7) | 320 | 59.5 | (55.3–63.6) | 1517 | 65.8 | (63.9–67.8) | 2345 | 59.6 | (58.1–61.1) | |
| Includers | 2581 | 26.8 | (25.9–27.7) | 1102 | 49.2 | (47.1–51.2) | 91 | 10.4 | (8.5–12.5) | 174 | 15.6 | (13.6–17.8) | 81 | 15.1 | (12.2–18.3) | 350 | 15.2 | (13.8–16.7) | 983 | 25.0 | (23.6–26.4) | |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Maclaren, O.; Mackay, L.; Schofield, G.; Zinn, C. Novel Nutrition Profiling of New Zealanders’ Varied Eating Patterns. Nutrients 2018, 10, 30. https://doi.org/10.3390/nu10010030
Maclaren O, Mackay L, Schofield G, Zinn C. Novel Nutrition Profiling of New Zealanders’ Varied Eating Patterns. Nutrients. 2018; 10(1):30. https://doi.org/10.3390/nu10010030
Chicago/Turabian StyleMaclaren, Olivia, Lisa Mackay, Grant Schofield, and Caryn Zinn. 2018. "Novel Nutrition Profiling of New Zealanders’ Varied Eating Patterns" Nutrients 10, no. 1: 30. https://doi.org/10.3390/nu10010030
APA StyleMaclaren, O., Mackay, L., Schofield, G., & Zinn, C. (2018). Novel Nutrition Profiling of New Zealanders’ Varied Eating Patterns. Nutrients, 10(1), 30. https://doi.org/10.3390/nu10010030





