Sustainable Health and Wellness: Effectiveness of a Drama Therapy Program to Improve the Wellbeing of People Affected by Mental Health Decline
Abstract
1. Introduction
1.1. Drama Therapy
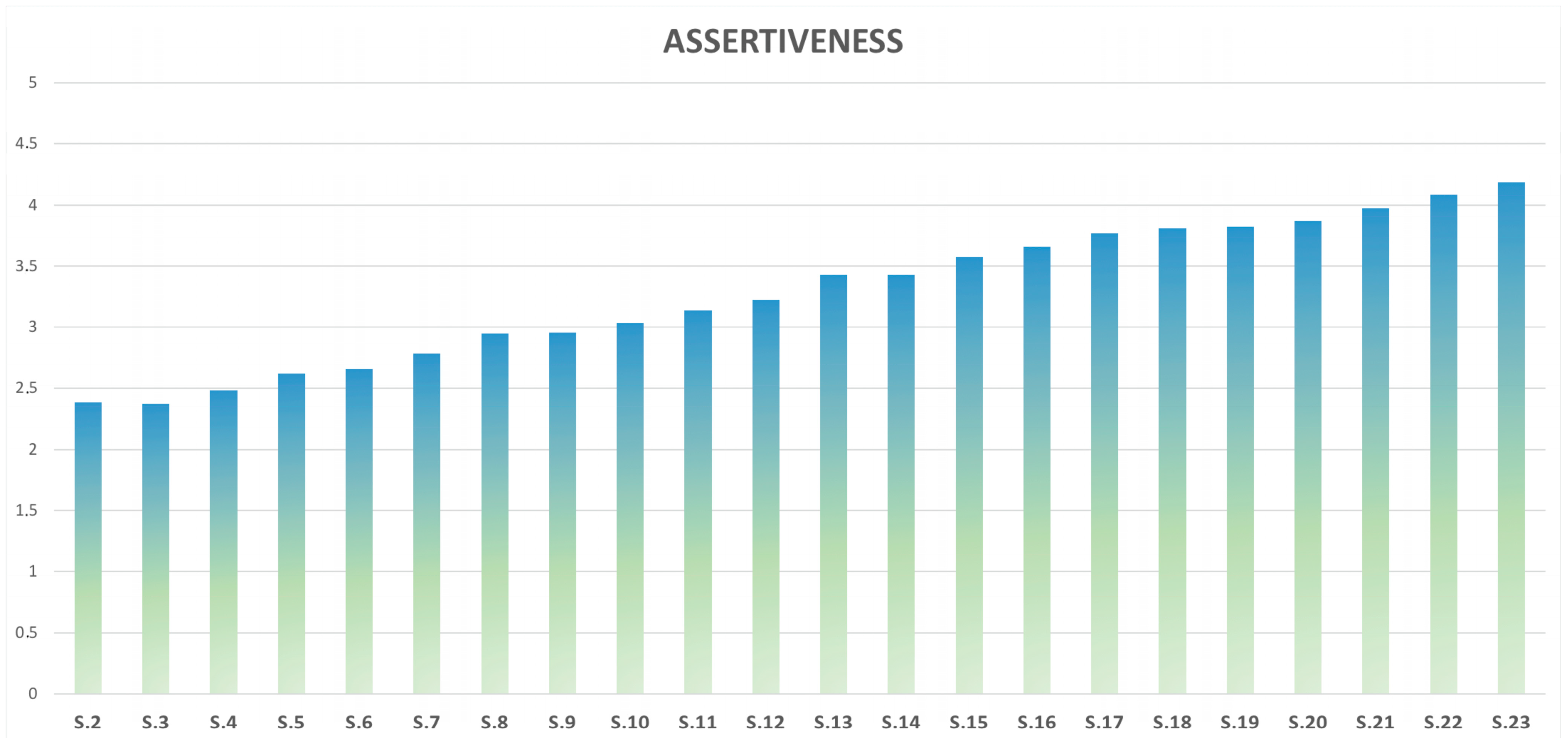
1.2. Assertiveness
1.3. Quality of Life
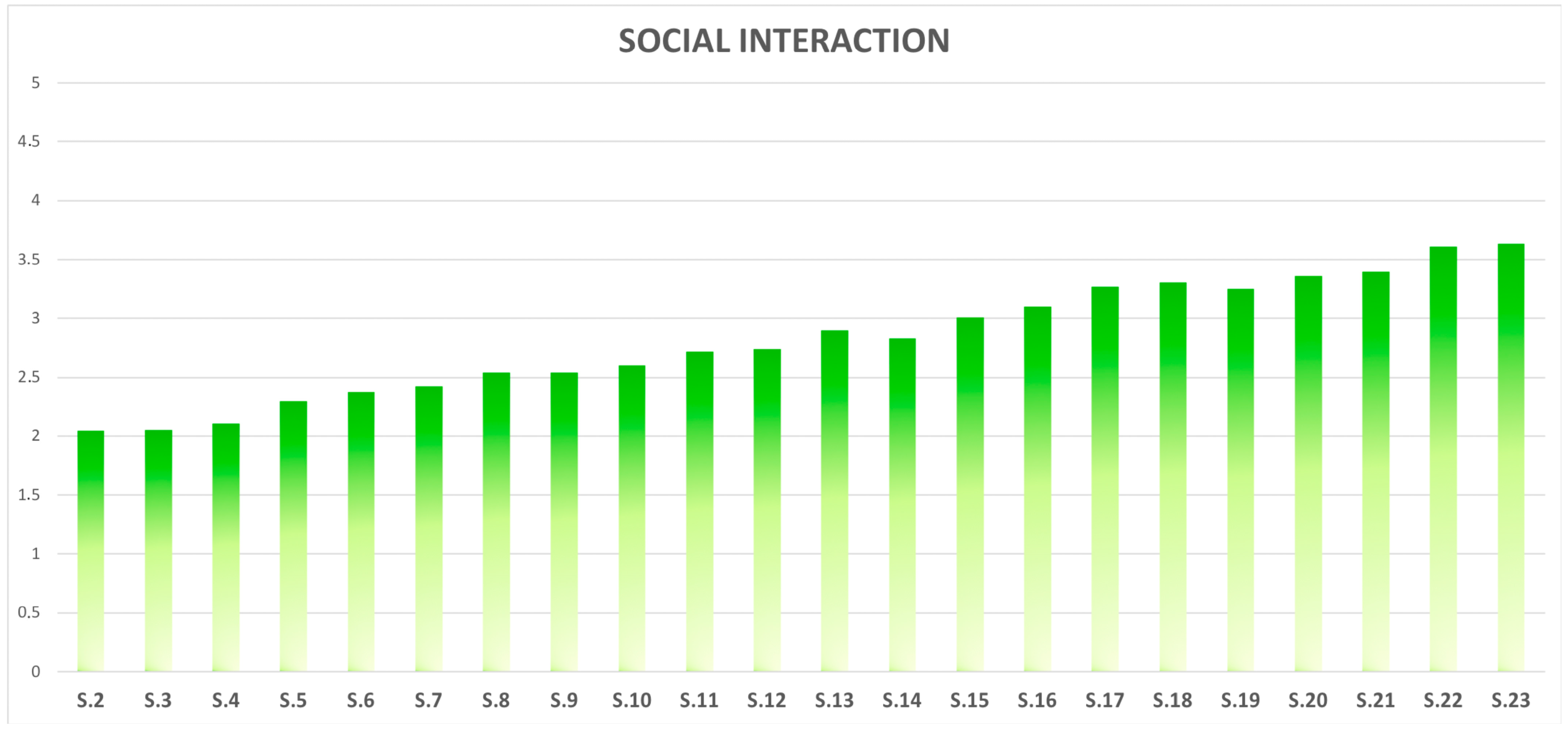
1.4. Social Interaction
2. Materials and Methods
2.1. Population
2.2. Instruments
2.3. Procedure
2.3.1. Ethics Committee
2.3.2. Program
2.3.3. Phases of the Therapeutic Process
2.3.4. Sessions
2.3.5. Evaluation
2.3.6. Data Collection and Statistical Analysis
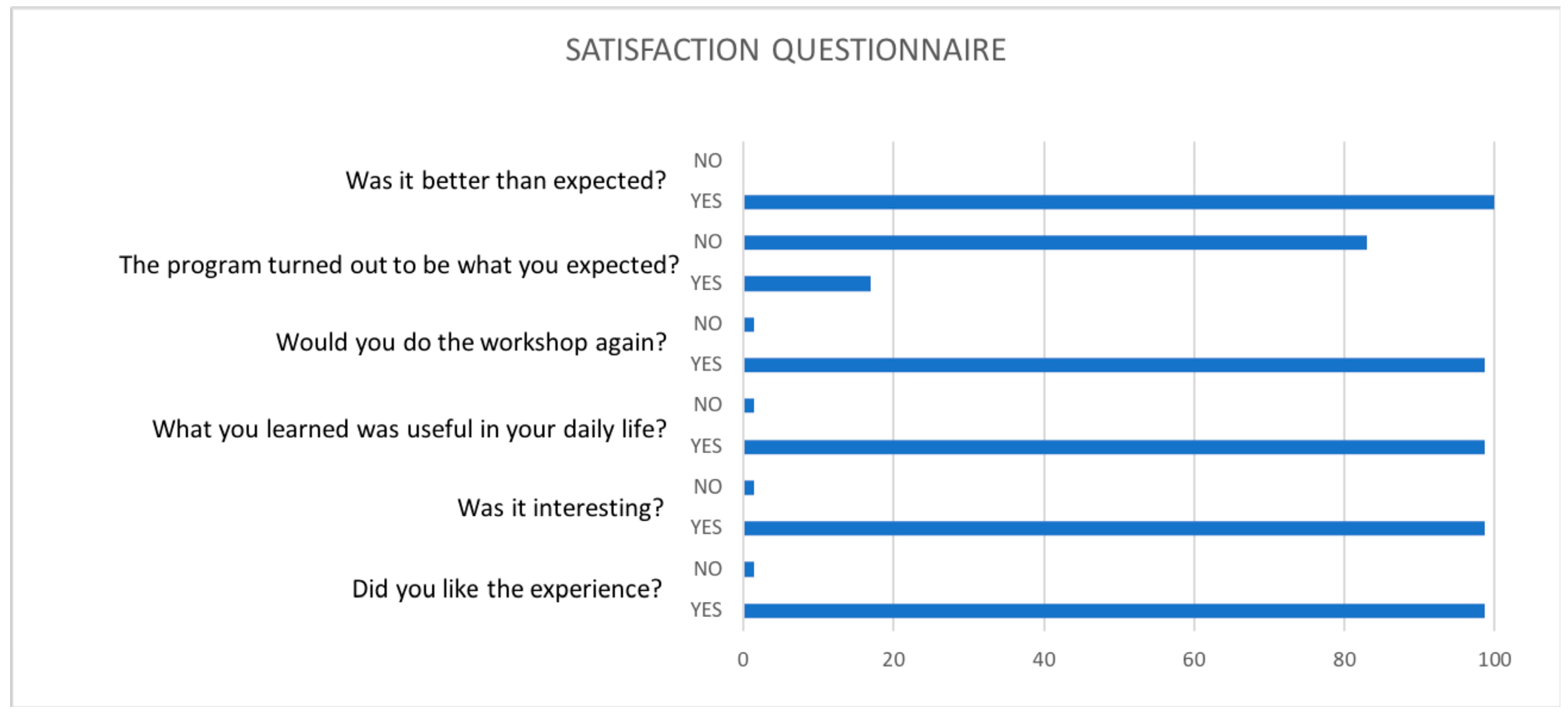
3. Results
“In the beginning, the coordination was hard, we stepped on each other and didn’t think about making a plan beforehand. When the educator stopped the exercise and told us it was very important to agree on something, we realized it was true, and slowly we stopped stepping on each other”(Field Diary session 10)
“At the beginning, we were very uncoordinated, but as soon as we stopped thinking about ourselves and started to see what was in front of us, we managed to walk together without getting hurt”(Field Diary session 10)
4. Discussions
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization. World Mental Health Report. Transforming Mental Health for All. Technical Report. 2022. Available online: https://www.who.int/publications/i/item/9789240049338 (accessed on 21 June 2023).
- World Health Organization. Basic Documents 49th Edition. Technical Report. 2020. Available online: https://apps.who.int/gb/bd/ (accessed on 21 June 2023).
- Chan, K.K.S.; Tsui, J.K.C. Longitudinal impact of experienced discrimination on mental health among people with mental disorders. Psychiatry Res. 2023, 322, 115099. [Google Scholar] [CrossRef] [PubMed]
- Whiteford, H.A.; Ferrari, A.J.; Degenhardt, L.; Feigin, V.; Vos, T. The Global Burden of Mental, Neurological and Substance Use Disorders: An Analysis from the Global Burden of Disease Study 2010. PLoS ONE 2015, 10, e0116820. [Google Scholar] [CrossRef] [PubMed]
- Yip, C.C.H.; Fung, W.T.W.; Leung, D.C.K.; Chan, K.K.S. The impact of stigma on engaged living and life satisfaction among people with mental illness in Hong Kong. Qual. Life Res. 2023, 32, 161–170. [Google Scholar] [CrossRef]
- Lee, R.S.C.; Hermens, D.F.; Scott, J.; O’Dea, B.; Glozier, N.; Scott, E.M.; Hickie, I.B. A transdiagnostic study of education, employment, and training outcomes in young people with mental illness. Psychol. Med. 2017, 47, 2061–2070. [Google Scholar] [CrossRef] [PubMed]
- Glozah, F.N.; Pevalin, D.J. Association between psychosomatic health symptoms and common mental illness in Ghanaian adolescents: Age and gender as potential moderators. J. Health Psychol. 2017, 22, 1376–1386. [Google Scholar] [CrossRef] [PubMed]
- Chio, F.H.N.; Mark, W.W.S.; Chan, R.C.H.; Tong, A.C.Y. Unraveling the insight paradox: One-year longitudinal study on the relationships between insight, self-stigma, and life satisfaction among people with schizophrenia spectrum disorders. Schizophr. Res. 2018, 197, 124–130. [Google Scholar] [CrossRef]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders–DSM 5-TR; American Psychiatric Association: Washington, DC, USA, 2022. [Google Scholar]
- Freeman, D.; Reeve, S.; Robinson, A.; Ehlers, A.; Clark, D.; Spanlang, B.; Slater, M. Virtual reality in the assessment, understanding, and treatment of mental health disorders. Psychol. Med. 2017, 47, 2393–2400. [Google Scholar] [CrossRef]
- Or, S.E.-B.; Hasson-Ohayon, I.; Feingold, D.; Vahab, K.; Amiaz, R.; Weiser, M.; Lysaker, P.H. Meaning in life, insight and self-stigma among people with severe mental illness. Compr. Psychiatry 2013, 54, 195–200. [Google Scholar]
- Perry, B.L.; Pullen, E.; Pescosolido, B.A. Interactions between patients’ experiences in mental health treatment and lay social network attitudes toward doctors in recovery from mental illness. Netw. Sci. 2017, 5, 355–380. [Google Scholar] [CrossRef]
- Kazdin, A.E. Nonprecsion (Standar) Psychosocial Interventions for the Treatment of Mental Disorders. Int. J. Ment. Health Promot. 2022, 24, 457–473. [Google Scholar] [CrossRef]
- Connell, J.; Brazier, J.; O’Cathain, A.; Lloyd-Jones, M.; Paisley, S. Quality of life of people with mental health problems: A synthesis of qualitative research. Health Qual. Life Outcomes 2012, 10, 138. [Google Scholar] [CrossRef] [PubMed]
- Mengistu, M.E.; Berassa, S.H.; Kassaw, A.T.; Dagnew, E.M.; Mekonen, G.A.; Birarra, M.K. Assessments of functional outcomes and its determinants among bipolar disorder patients un Northwest Ethiopia comprehensive specialized hospitals: A multicenter hospital-based study. Ann. Gen. Psychiatry 2023, 22, 14. [Google Scholar] [CrossRef] [PubMed]
- Fernández-Aguayo, S. Programa de dramaterapia para personas con deterioro de su salud mental. In Diseño y Evaluación de Programas Educativos en el Ámbito Social: Actividad Física y Dramaterapia; Pino-Juste, M., Ed.; Alianza: Madrid, Spain, 2017; pp. 153–195. [Google Scholar]
- Cornejo, S.; Brik Levy, L. La Representación de las Emociones en la Dramaterapia; Editorial médica Panamericana: Buenos Aires, Argentina, 2003. [Google Scholar]
- Fernández-Aguayo, S. Drama como Técnica Terapéutica en Salud Mental: Diseño y Evaluación de un Programa. Ph.D. Thesis, University de Vigo, Vigo, Spain, 2018. [Google Scholar]
- Orkibi, H.; Keisari, S.; Sajnani, N.; Witte, M. Effectiveness of Drama-Based Therapies on Mental Health Outcomes: A Systematic Review and Meta-Analysis of Controlled Studies. Psychol. Aesthet. Creat. Arts 2023. [Google Scholar] [CrossRef]
- Ghavami, M.; Emami, M.; Bonakdar, S.A. Effectiveness of Narrative Therapy on the Increase of Self-Assertiveness in Female High School Students (Case Study: Iran (Isfahan), 2013–2014). Int. J Acad. Res. Psychol. 2014, 2, 105–111. [Google Scholar]
- Khalil, M.; Ghayas, S.; Adil, A.; Niazi, S. Self-efficacy and Mental health among university students: Mediating role of assertiveness. Rawal Med. J. 2021, 46, 416–419. [Google Scholar]
- Korem, A.; Horenczyk, G.; Tatar, M. Inter-group and intra-group assertiveness: Adolescents’ social skills following cultural transition. J. Adolesc. 2012, 35, 855–862. [Google Scholar] [CrossRef]
- Berrocal-Izquierdo, N.; Bernardo, M. Esquizofrenia y enfermedad cerebrovascular. Descripción de una serie y revisión bibliográfica. Actas Españolas Psiquiatr. 2014, 42, 74–82. [Google Scholar]
- Ho, A.H.Y.; Potash, J.S.; Fong, T.C.T.; Ho, V.F.L.; Chen, E.Y.H.; Lau, R.H.W.; Ho, R.T.H. Psychometric properties of a Chinese version of the Stigma Scale: Examining the complex experience of stigma and its relationship with self-esteem and depression among people living with mental illness in Hong Kong. Compr. Psychiatry 2015, 56, 198–205. [Google Scholar] [CrossRef] [PubMed]
- Casados, A.T. Reducing the Stigma of Mental Illness: Current Approaches and Future Directions. Clin. Psychol. Sci. Pract. 2017, 24, 306–323. [Google Scholar] [CrossRef]
- Defar, S.; Abraham, Y.; Reta, Y.; Deribe, B.; Jisso, M.; Yeheyis, T.; Ayalew, M. Health related quality of life among people with mental illness: The role of socio-clinical characteristics and level of functional disability. Front. Public Health 2023, 11, 1134032. [Google Scholar] [CrossRef] [PubMed]
- Saavedra, J.; Brzeska, J.; Matías-García, J.A.; Arias-Sánchez, S. Quality of life and psychiatric distress in people with serious mental illness, the role of personal recovery. Psychol. Psychoter. Theory Res. Pract. 2023, 96, 525–541. [Google Scholar] [CrossRef]
- Buonocore, M.; Bosia, M.; Baraldi, M.; Bechi, M.; Spangaro, M.; Cocchi, F.; Cavallaro, R. Achieving recovery in patients with schizophrenia through psychosocial interventions: A retrospective study. Psychiatry Clin. Neurosci. 2018, 72, 28–34. [Google Scholar] [CrossRef] [PubMed]
- Cernea, M.; Neagu, A.; Georgescu, M.; Modan, A.; Zaulet, D.; Hirit Alina, C.; Stan, V. Promoting the resilient process for deaf children by play and drama therapy. In Proceedings of the Second World Congress on Resilience: From Person to Society, Timisoara, Romania, 8–10 May 2014. [Google Scholar]
- Butler, J.D. Playing with madness: Developmental Transformations and the treatment of schizophrenia. Arts Psychother. 2012, 39, 87–94. [Google Scholar] [CrossRef]
- Hasson-Ohayon, I.; Mashiach-Eizenberg, M.; Lavi-Rotenberg, A.; Roe, D. Randomized Controlled Trial of Adjunctive Social Cognition and Interaction Training, Adjunctive Therapeutic Alliance Focused Therapy, and Treatment as Usual Among Persons With Serious Mental Illness. Front. Psychiatry 2019, 10, 362. [Google Scholar] [CrossRef] [PubMed]
- Schön, U.K.; Denhov, A.; Topor, A. Social Relationships as a Decisive Factor in Recovering from Severe Mental Illness. Int. J. Soc. Psychiatry 2009, 55, 336–347. [Google Scholar] [CrossRef] [PubMed]
- Ma, X.; Sayama, H. Mental disorder recovery correlated with centralities and interactions on an online social network. PeerJ 2015, 3, e1163. [Google Scholar] [CrossRef] [PubMed]
- Drapalski, A.L.; Tonge, N.; Muralidharan, A.; Brown, C.H.; Lucksted, A. Even mild internalized stigma merits attention among adults with serious mental illness. Psychol. Serv. 2023. [Google Scholar] [CrossRef] [PubMed]
- Bielańska, A.; Cechnicki, A. Drama therapy in a community treatment programme. In Therapeutic Communities for Psychosis: Philosophy, History and Clinical Practice; Gale, J., Realpe, A., Eds.; Routledge/Taylor & Francis Group: New York, NY, USA, 2008; pp. 224–229. [Google Scholar]
- Greg, P. The operational components of drama therapy. J. Group Psychother. Psychodrama Sociom. 1992, 45, 40–44. [Google Scholar]
- Feniger-Schaal, R. A dramatherapy case study with a young man who has dual diagnosis of intellectual disability and mental health problems. Arts Psychother. 2016, 50, 40–45. [Google Scholar] [CrossRef]
- Fabian, R.; Tarasova, D.; Bergmann, T.; Sappok, T. An improvisational theatre intervention in people with intellectual disabilities and mental health problems. Int. J. Dev. Disabil. 2022. [Google Scholar] [CrossRef]
- Bourne, J.; Brown, C.; Corrigan, D.; Goldblatt, P.; Hackett, S. Advances for future working following an online dramatherapy group for adults with intellectual disabilities and mental ill health during the COVID-19 pandemic: A service evaluation for Cumbria, Northumberland Tyne and Wear NHS Foundation Trust. Br. J. Learn. Disabil. 2022, 50, 376–384. [Google Scholar] [CrossRef] [PubMed]
- Landy, R. Role theory and role method of drama therapy. In Current Approaches in Drama Therapy; Johnson, D., Emunah, R., Eds.; Charles Thomas: Chicago, IL, USA, 2009; pp. 65–88. [Google Scholar]
- Bademci, H.O.; Karaday, E.F.; Zulueta, F. Attachment intervention through peer-based interaction: Working with Istanbul’s street boys in a university setting. Child Youth Serv. Rev. 2015, 49, 20–31. [Google Scholar] [CrossRef]
- Bourne, J.; Andersen-Warren, M.; Hackett, S. A systematic review to investigate dramatherapy group work with working age adults who have a mental health problem. Arts Psychother. 2018, 61, 1–9. [Google Scholar] [CrossRef]
- Melero Aguilar, N. El paradigma crítico y los aportes de la investigación acción participativa en la transformación de la realidad social: Un análisis desde las ciencias sociales. Cuest. Pedagógicas 2012, 21, 339–355. [Google Scholar]
- Jiménez Chaves, V.E. El Estudio de Caso y su Implementación en la Investigación. Rev. Int. Investig. Cienc. Soc. 2012, 8, 141–150. Available online: http://dialnet.unirioja.es/servlet/articulo?codigo=3999526 (accessed on 21 June 2023).
- Souza, F.; Souza, D.; Costa, A. Investigação Qualitativa: Inovação, Dilemas e Desafíos; Ed. Ludomedia: Aveiro, Portugal, 2015. [Google Scholar]
- Royse, D.; Thyer, B.; Padgett, D. Program Evaluation. An Introduction to an Evidence-Based Approach, 6th ed.; Cengage Learning: Boston, MA, USA, 2016. [Google Scholar]
- Fernández-Aguayo, S.; Pino-Juste, M. Drama therapy and theater as an intervention tool: Bibliometric analysis of programs based on drama therapy and theater. Arts Psychother. 2018, 59, 83–93. [Google Scholar] [CrossRef]
- Sajnani, N. Reflection-in-action: An argument for arts-based practice as research in drama therapy. In Through the Looking Glass: Dimensions of Reflection in the Arts Therapies; Hougham, R., Pitruzzella, S., Scoble, S., Eds.; University of Plymouth Press: Devon, UK, 2015; pp. 101–118. [Google Scholar]
- Jones, P. Three challenges for drama therapy research: Keynote NADTA conference, Montreal 2013. Drama Ther. Rev. 2015, 1, 87–99. [Google Scholar] [CrossRef]
- Armstrong, C.; Rozenberg, M.; Powell, M.; Honce, J.; Bronstein, L.; Gingras, G.; Han, E. A step toward empirical evidence: Operationalizing and uncovering drama therapy change processes. Arts Psychother. 2016, 46, 27–33. [Google Scholar] [CrossRef]
- Alonso, J. Cuestionario de Salud SF-36 y Cuestionario de Salud SF-12. BiblioPRO; Instituto Municipal de Investigaciones Médicas: Barcelona, Spain, 1996; Available online: https://bibliopro.org/buscador/663/cuestionario-de-salud-sf-12 (accessed on 21 June 2023).
- Carrasco, I.; Clemente, M.; Llavona, L. Análisis del inventario de aserción de Gambrill y Richey. Estud. Psicol. 1989, 37, 63–74. [Google Scholar] [CrossRef]
- Casas-Anguera, E.; Prat, G.; Vilamala, S.; Escandell, M.; García-Franco, M.; Martin, J.; Ochoa, S. Validación de la versión española del inventario de asertividad Gambrill y Richey en población con diagnóstico de esquizofrenia. An. Psicol. 2014, 30, 431–437. [Google Scholar] [CrossRef][Green Version]
- Pino-Juste, M. La evaluación de los aprendizajes. In Diseño y Desarrollo del Currículum; Cantón, I., Pino-Juste, M., Eds.; Alianza: Madrid, Spain, 2011; pp. 247–265. [Google Scholar]
- Crook, R.A. A Drama Therapy Program for Sexually Traumatized School-Age Children with Dissociative Characteristics. Ph.D. Thesis, Faculty of the Chicago School of Professional Psychology, Chicago, IL, USA, 2009. [Google Scholar]
- Tevelev, V. Fairy tale group therapy: A cognitive-behavioral group therapy program by means of drama-therapy for children with disruptive behavior disorders. Isr. J. Psychiatry Relat. Sci. 2012, 49, 61. [Google Scholar]
- Mosley, J. An evaluative account of the working of a dramatherapy peer support group within a comprehensive school. Support Learn. 1991, 6, 156–164. [Google Scholar] [CrossRef]
- Eliaz, E.; Flashman, A. Road signs: Elements of transference in drama therapy: Case study. Arts Psychother. 1994, 21, 59–73. [Google Scholar] [CrossRef]
- Haste, E.; McKenna, P. Clinical effectiveness of dramatherapy in the recovery from severe neuro-trauma. In Drama as Therapy Volume 2: Clinical Work and Research into Practice; Jones, P., Ed.; Routledge/Taylor & Francis Group: New York, NY, USA, 2010; pp. 84–104. [Google Scholar]
- Pearlyn, P. Drama therapy for persons with intellectual disability in Singapore: Review of a 3-month program. J. Policy Pract. Intellect. Disabil. 2009, 6, 127. [Google Scholar]
- Merritt, J.M. The Effects of A Program of Drama Therapy on the Social Skills Behaviors of Institutionalized Mentally Retarded Adults. Ph.D. Thesis, Pittsburgh University, Pittsburgh, PA, USA, 1985. [Google Scholar]
- James, M.; Johnson, D.R. Drama therapy in the treatment of combat-related post-traumatic stress disorder. Arts Psychother. 1996, 23, 383–395. [Google Scholar] [CrossRef]
- Towers, T. An Examination of the Challenges of Veteran Reintegration and the Application of Drama Therapy Techniques. Ph.D. Thesis, Chicago School of Professional Psychology, Chicago, IL, USA, 2013. [Google Scholar]
- Cyr, D.P. Spirit in Motion: Developing a Spiritual Practice in Drama Therapy; California Institute of Integral Studies: San Francisco, CA, USA, 1998. [Google Scholar]
- Castaños, S.; Reyes, I.; Rivera, S.; Díaz, R. Estandarización del Inventario de Asertividad de Gabmbrill y Richey-II. Rev. Iberoam. Diagnóstico Evaluación Avaliação Psicológica 2011, 29, 27–50. [Google Scholar]
- Jakovljević, M. Creativity, Mental Disorders and their Treatment: Recovery-Oriented Psychopharmacotherapy. Psychiatr. Danub. 2013, 25, 311–315. [Google Scholar] [PubMed]
- Rippon, D.; Shepherd, J.; Wakefield, S.; Lee, A.; Pollet, T.V. The role of self-efficacy and self-esteem in mediating positive associations between functional social support and psychological wellbeing in people with a mental health diagnosis. J. Ment. Health 2022. [Google Scholar] [CrossRef] [PubMed]
- O’Beirne, L. Creating community connections and reconstituting self in the face of psychiatric disability. Int. J. Interdiscip. Soc. Sci. 2010, 5, 107–117. [Google Scholar] [CrossRef]
- Price, J.H.; Murnan, J. Research Limitations and the Necessity of Reporting Them. Am. J. Health Educ. 2004, 35, 66–67. [Google Scholar] [CrossRef]
| Variables | Components | Min. | Max. | Mean | Min. | Max. | Mean | Student’s t |
|---|---|---|---|---|---|---|---|---|
| Pretest | Posttest | Sig. | ||||||
| Assertiveness | Discomfort | 65 | 174 | 116,20 | 47 | 158 | 103.49 | 0.002 |
| Probability | 73 | 153 | 115,78 | 91 | 139 | 109.43 | 0.022 | |
| Quality of life | Physical health | 11.67 | 95.83 | 57.7451 | 11.67 | 100 | 58.56 | 0.115 |
| Mental health | 8.33 | 89.17 | 49.6895 | 3.33 | 100 | 54.06 | 0.773 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fernández-Aguayo, S.; Pino-Juste, M. Sustainable Health and Wellness: Effectiveness of a Drama Therapy Program to Improve the Wellbeing of People Affected by Mental Health Decline. Sustainability 2023, 15, 12485. https://doi.org/10.3390/su151612485
Fernández-Aguayo S, Pino-Juste M. Sustainable Health and Wellness: Effectiveness of a Drama Therapy Program to Improve the Wellbeing of People Affected by Mental Health Decline. Sustainability. 2023; 15(16):12485. https://doi.org/10.3390/su151612485
Chicago/Turabian StyleFernández-Aguayo, Sara, and Margarita Pino-Juste. 2023. "Sustainable Health and Wellness: Effectiveness of a Drama Therapy Program to Improve the Wellbeing of People Affected by Mental Health Decline" Sustainability 15, no. 16: 12485. https://doi.org/10.3390/su151612485
APA StyleFernández-Aguayo, S., & Pino-Juste, M. (2023). Sustainable Health and Wellness: Effectiveness of a Drama Therapy Program to Improve the Wellbeing of People Affected by Mental Health Decline. Sustainability, 15(16), 12485. https://doi.org/10.3390/su151612485






