Weather-Related Fatalities in Australia between 2006 and 2019: Applying an Equity Lens
Abstract
1. Introduction
2. Materials and Methods
3. Results
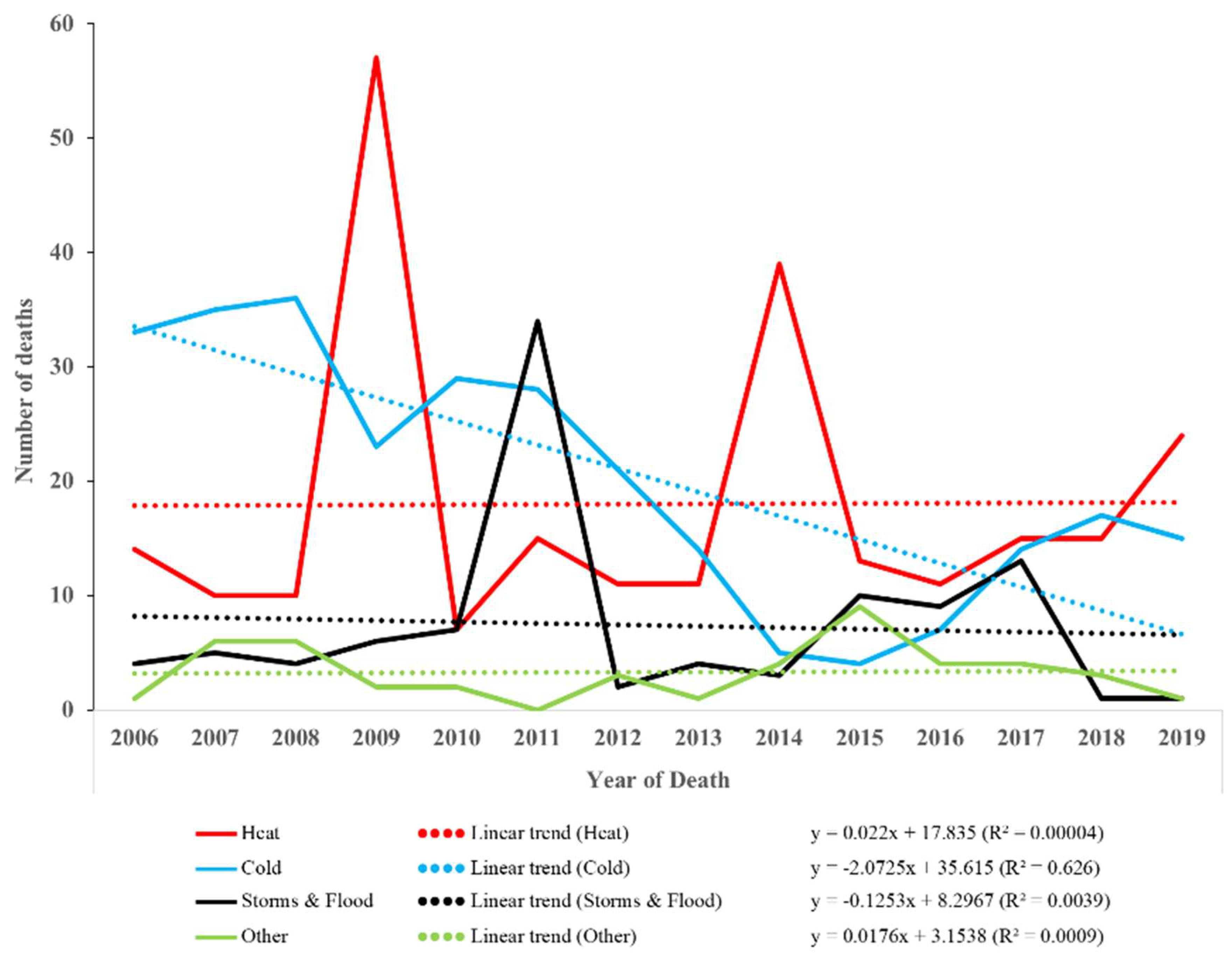
3.1. Fatalities Where Weather-Related Events Were the Underlying Cause of Death
3.2. Fatality Rates of Australian Residents Where Weather-Related Events Were the Underlying Cause of Death
3.3. Fatalities Where Weather-Related Events Were a Contributory Cause of Death
4. Discussion
Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Watts, N.; Amann, M.; Ayeb-Karlsson, S.; Belesova, K.; Bouley, T.; Boykoff, M.; Byass, P.; Cai, W.; Campbell-Lendrum, D.; Chambers, J.; et al. The Lancet Countdown on health and climate change: From 25 years of inaction to a global transformation for public health. Lancet 2018, 391, 581–630. [Google Scholar] [CrossRef] [PubMed]
- Arias, P.; Dereczynski, C.; Alves, L.; Ruiz-Carrascal, D.; Rojas, M.; Sorensson, A.; Ruiz, L.; Vera, C. Climate change in South America: New insights from the most recent IPCC assessment report. AGU Fall Meet. 2021, 2021, GC51B-05. [Google Scholar]
- Matthews, T.K.R.; Wilby, R.L.; Murphy, C. Communicating the deadly consequences of global warming for human heat stress. Proc. Natl. Acad. Sci. USA 2017, 114, 3861–3866. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. COP26 Special Report on Climate Change and Health: The Health Argument for Climate Action. Available online: https://apps.who.int/iris/bitstream/handle/10665/346168/9789240036727-eng.pdf?sequence=1 (accessed on 29 September 2022).
- Akhtar, R. Introduction: Extreme Weather Events and Human Health: A Global Perspective. In Extreme Weather Events and Human Health: International Case Studies; Akhtar, R., Ed.; Springer International Publishing: Cham, Switzerland, 2020; pp. 3–11. [Google Scholar]
- Queensland Floods Commission of Inquiry. Queensland Floods Commission of Inquiry—Final Report; Government of Queensland: Queensland, Australia, 2012. [Google Scholar]
- Ben Smee and agencies. Up to 500,000 drought-stressed cattle killed in Queensland floods. The Guardian, 11 February 2019. [Google Scholar]
- Center for Disaster Philanthropy. 2019–2020 Australian Bushfires. Available online: https://disasterphilanthropy.org/disasters/2019-australian-wildfires/ (accessed on 26 November 2022).
- Hanna, E.G.; McIver, L.J. Climate change: A brief overview of the science and health impacts for Australia. Med. J. Aust. 2018, 208, 311–315. [Google Scholar] [CrossRef]
- Borchers Arriagada, N.; Bowman, D.M.J.S.; Palmer, A.J.; Johnston, F.H. Climate Change, Wildfires, Heatwaves and Health Impacts in Australia. In Extreme Weather Events and Human Health: International Case Studies; Akhtar, R., Ed.; Springer International Publishing: Cham, Switzerland, 2020; pp. 99–116. [Google Scholar]
- Ashcroft, L.; Karoly, D.J.; Dowdy, A.J. Historical extreme rainfall events in southeastern Australia. Weather Clim. Extrem. 2019, 25, 100210. [Google Scholar] [CrossRef]
- Mason, H.; King, J.C.; Peden, A.E.; Franklin, R.C. Systematic review of the impact of heatwaves on health service demand in Australia. BMC Health Serv. Res. 2022, 22, 960. [Google Scholar] [CrossRef]
- Reifels, L.; Mills, K.; Dückers, M.L.A.; O’Donnell, M.L. Psychiatric epidemiology and disaster exposure in Australia. Epidemiol. Psychiatr. Sci. 2019, 28, 310–320. [Google Scholar] [CrossRef]
- Yu, W.; Vaneckova, P.; Mengersen, K.; Pan, X.; Tong, S. Is the association between temperature and mortality modified by age, gender and socio-economic status? Sci. Total Environ. 2010, 408, 3513–3518. [Google Scholar] [CrossRef]
- Schaffer, A.; Muscatello, D.; Broome, R.; Corbett, S.; Smith, W. Emergency department visits, ambulance calls, and mortality associated with an exceptional heat wave in Sydney, Australia, 2011: A time-series analysis. Environ. Health 2012, 11, 3. [Google Scholar] [CrossRef]
- Cheng, J.; Xu, Z.; Bambrick, H.; Su, H.; Tong, S.; Hu, W. Impacts of heat, cold, and temperature variability on mortality in Australia, 2000–2009. Sci. Total Environ. 2019, 651, 2558–2565. [Google Scholar] [CrossRef]
- Vardoulakis, S.; Dear, K.; Hajat, S.; Heaviside, C.; Eggen, B.; McMichael, A.J. Comparative assessment of the effects of climate change on heat-and cold-related mortality in the United Kingdom and Australia. Environ. Health Perspect. 2014, 122, 1285–1292. [Google Scholar] [CrossRef] [PubMed]
- AAP. ‘Climate Change is Already Killing Australians’: Calls for Urgent Rollout of Climate-Health Action Plan. Available online: https://www.sbs.com.au/news/article/climate-change-is-already-killing-australians-calls-for-urgent-rollout-of-climate-health-action-plan/90ydswgl7 (accessed on 13 December 2022).
- Royal Australasian College of Physicians. Climate Change and Health. Available online: https://www.racp.edu.au/advocacy/policy-and-advocacy-priorities/climate-change-and-health (accessed on 13 December 2022).
- Marmot, M. Social determinants and the health of Indigenous Australians. Med. J. Aust. 2011, 194, 512–513. [Google Scholar] [CrossRef] [PubMed]
- Peden, A.E.; Franklin, R.C. Child Injury Prevention: It Is Time to Address the Determinants of Health. Children 2021, 8, 46. [Google Scholar] [CrossRef]
- Australian Bureau of Statistics. Statistical Area Level 2 (SA2). Available online: https://www.abs.gov.au/ausstats/abs@.nsf/lookup/by%20subject/1270.0.55.001~july%202016~main%20features~statistical%20area%20level%202%20(sa2)~10014 (accessed on 15 September 2022).
- Australian Bureau of Statistics. The Australian Statistical Geography Standard (ASGS) Remoteness Structure. Available online: https://www.abs.gov.au/websitedbs/d3310114.nsf/home/remoteness+structure (accessed on 15 February 2022).
- Australian Bureau of Statistics. 2033.0.55.001—Census of Population and Housing: Socio-Economic Indexes for Areas (SEIFA), Australia. 2016. Available online: https://www.abs.gov.au/ausstats/abs@.nsf/Lookup/by%20Subject/2033.0.55.001~2016~Main%20Features~IRSAD~20 (accessed on 15 September 2022).
- Thacker, M.T.F.; Lee, R.; Sabogal, R.I.; Henderson, A. Overview of deaths associated with natural events, United States, 1979–2004. Disasters 2008, 32, 303–315. [Google Scholar] [CrossRef] [PubMed]
- IBM Corp. IBM SPSS Statistics for Windows Version 25; IBM Corp.: Armonk, NY, USA, 2020. [Google Scholar]
- Keppel, G. Design and Analysis: A Researcher’s Handbook, 3rd ed.; Prentice Hall: Englewood Cliffs, NJ, USA, 1991. [Google Scholar]
- Australian Bureau of Statistics. Population—Australia by Sex and Single Year of Age. Available online: https://www.abs.gov.au/statistics/people/population/national-state-and-territory-population/mar-2022/3101059.xlsx (accessed on 14 October 2022).
- Australian Bureau of Statistics. Population Estimates by Significant Urban Area and Remoteness Area (ASGC2016), 2001 to 2021. Available online: https://www.abs.gov.au/statistics/people/population/regional-population/2021/32180DS0004_2001-21.xlsx (accessed on 14 October 2022).
- Australian Bureau of Statistics. Table 1: Estimated Resident Population, Aboriginal and Torres Strait Islander Australians, Australia, States and Territories by Sex—2006 to 2016. Available online: https://www.abs.gov.au/statistics/people/aboriginal-and-torres-strait-islander-peoples/estimates-and-projections-aboriginal-and-torres-strait-islander-australians/2006-2031#data-download (accessed on 14 October 2022).
- Australian Bureau of Statistics. Stat Data Explorer—Projected Population, Aboriginal and Torres Strait Islander Australians, Australia, State and Territories, 2016 to 2031. Available online: https://explore.data.abs.gov.au/vis?fs[0]=People%2C0%7CAboriginal%20and%20Torres%20Strait%20Islander%20Peoples%23ATSIP%23&pg=0&fc=People&df[ds]=PEOPLE_TOPICS&df[id]=ABORIGINAL_POP_PROJ&df[ag]=ABS&df[vs]=1.0.0 (accessed on 14 October 2022).
- International, H. Older People in Emergencies: Identifying and Reducing Risks. Available online: https://www.humanitarianlibrary.org/resource/older-people-emergencies-%E2%80%93-identifying-and-reducing-risks (accessed on 14 October 2022).
- Vaneckova, P.; Beggs, P.J.; Jacobson, C.R. Spatial analysis of heat-related mortality among the elderly between 1993 and 2004 in Sydney, Australia. Soc. Sci. Med. 2010, 70, 293–304. [Google Scholar] [CrossRef]
- Clemens, T.; Peden, A.E.; Franklin, R.C. Exploring a Hidden Epidemic: Drowning Among Adults Aged 65 Years and Older. J. Aging Health 2021, 33, 8982643211014770. [Google Scholar] [CrossRef]
- James, S.L.; Castle, C.D.; Dingels, Z.V.; Fox, J.T.; Hamilton, E.B.; Liu, Z.; Roberts, N.L.S.; Sylte, D.O.; Henry, N.J.; LeGrand, K.E.; et al. Global injury morbidity and mortality from 1990 to 2017: Results from the Global Burden of Disease Study 2017. Inj. Prev. 2020, 26, i96–i114. [Google Scholar] [CrossRef]
- Evans, J. Mapping the vulnerability of older persons to disasters. Int. J. Older People Nurs. 2010, 5, 63–70. [Google Scholar] [CrossRef]
- Kwan, C.; Walsh, C.A. Seniors’ disaster resilience: A scoping review of the literature. Int. J. Disaster Risk Reduct. 2017, 25, 259–273. [Google Scholar] [CrossRef]
- Chan, E.Y.Y. Disaster Public Health and Older People; Routledge: Abingdon, Oxfordshire, UK, 2019. [Google Scholar]
- Sakurai, M.; Murayama, Y. Information technologies and disaster management—Benefits and issues. Prog. Disaster Sci. 2019, 2, 100012. [Google Scholar] [CrossRef]
- Khan, A.; Gupta, S.; Gupta, S.K. Emerging UAV technology for disaster detection, mitigation, response, and preparedness. J. Field Robot. 2022, 39, 905–955. [Google Scholar] [CrossRef]
- Lai, C.-H.; Chib, A.; Ling, R. Digital disparities and vulnerability: Mobile phone use, information behaviour, and disaster preparedness in Southeast Asia. Disasters 2018, 42, 734–760. [Google Scholar] [CrossRef] [PubMed]
- Brockie, L.; Miller, E. Older adults’ disaster lifecycle experience of the 2011 and 2013 Queensland floods. Int. J. Disaster Risk Reduct. 2017, 22, 211–218. [Google Scholar] [CrossRef]
- Timalsina, R.; Songwathana, P. Factors enhancing resilience among older adults experiencing disaster: A systematic review. Australas. Emerg. Care 2020, 23, 11–22. [Google Scholar] [CrossRef]
- Brockie, L.; Miller, E. Understanding older adults’ resilience during the Brisbane floods: Social capital, life experience, and optimism. Disaster Med. Public Health Prep. 2017, 11, 72–79. [Google Scholar] [CrossRef]
- Lin, P.-S.S.; Chen, S.-S. Social networks for older people’s resilient aging-in-place: Lessons from the post-landslide Ksunu tribe in Taiwan. Int. J. Disaster Risk Reduct. 2022, 82, 103336. [Google Scholar] [CrossRef]
- Howard, A.; Blakemore, T.; Bevis, M. Older people as assets in disaster preparedness, response and recovery: Lessons from regional Australia. Ageing Soc. 2017, 37, 517–536. [Google Scholar] [CrossRef]
- Benevolenza, M.A.; DeRigne, L. The impact of climate change and natural disasters on vulnerable populations: A systematic review of literature. J. Hum. Behav. Soc. Environ. 2019, 29, 266–281. [Google Scholar] [CrossRef]
- Australian Bureau of Statistics. Underlying Causes of Death (Australia). Available online: https://www.abs.gov.au/statistics/health/causes-death/causes-death-australia/latest-release#data-download (accessed on 13 November 2020).
- Standen, J.C.; Spencer, J.; Lee, G.W.; Van Buskirk, J.; Matthews, V.; Hanigan, I.; Boylan, S.; Jegasothy, E.; Breth-Petersen, M.; Morgan, G.G. Aboriginal Population and Climate Change in Australia: Implications for Health and Adaptation Planning. Int. J. Environ. Res. Public Health 2022, 19, 7502. [Google Scholar] [CrossRef]
- Taylor, D.H.; Peden, A.E.; Franklin, R.C. Disadvantaged by More Than Distance: A Systematic Literature Review of Injury in Rural Australia. Safety 2022, 8, 66. [Google Scholar] [CrossRef]
- Peden, A.E.; Franklin, R.C. Exploring Flood-Related Unintentional Fatal Drowning of Children and Adolescents Aged 0–19 Years in Australia. Safety 2019, 5, 46. [Google Scholar] [CrossRef]
- Nygaard, C.A.; Parkinson, S. Analysing the impact of COVID-19 on urban transitions and urban-regional dynamics in Australia*. Aust. J. Agric. Resour. Econ. 2021, 65, 878–899. [Google Scholar] [CrossRef] [PubMed]
- Santamouris, M.; Paolini, R.; Haddad, S.; Synnefa, A.; Garshasbi, S.; Hatvani-Kovacs, G.; Gobakis, K.; Yenneti, K.; Vasilakopoulou, K.; Feng, J.; et al. Heat mitigation technologies can improve sustainability in cities. An holistic experimental and numerical impact assessment of urban overheating and related heat mitigation strategies on energy consumption, indoor comfort, vulnerability and heat-related mortality and morbidity in cities. Energy Build. 2020, 217, 110002. [Google Scholar] [CrossRef]
- Chen, D.; Wang, X.; Thatcher, M.; Barnett, G.; Kachenko, A.; Prince, R. Urban vegetation for reducing heat related mortality. Environ. Pollut. 2014, 192, 275–284. [Google Scholar] [CrossRef] [PubMed]
- Yenneti, K.; Ding, L.; Prasad, D.; Ulpiani, G.; Paolini, R.; Haddad, S.; Santamouris, M. Urban Overheating and Cooling Potential in Australia: An Evidence-Based Review. Climate 2020, 8, 126. [Google Scholar] [CrossRef]
- Imran, H.M.; Kala, J.; Ng, A.; Muthukumaran, S. Effectiveness of green and cool roofs in mitigating urban heat island effects during a heatwave event in the city of Melbourne in southeast Australia. J. Clean. Prod. 2018, 197, 393–405. [Google Scholar] [CrossRef]
- Yang, J.; Santamouris, M. Urban Heat Island and mitigation technologies in Asian and Australian Cities—Impact and mitigation. Urban Sci. 2018, 2, 74. [Google Scholar] [CrossRef]
- Loughnan, M.; Carroll, M.; Tapper, N.J. The relationship between housing and heat wave resilience in older people. Int. J. Biometeorol. 2015, 59, 1291–1298. [Google Scholar] [CrossRef]
- Adnan, M.S.G.; Dewan, A.; Botje, D.; Shahid, S.; Hassan, Q.K. Vulnerability of Australia to heatwaves: A systematic review on influencing factors, impacts, and mitigation options. Environ. Res. 2022, 213, 113703. [Google Scholar] [CrossRef]
- Peden, A.; Franklin, R.C. Exploring the Impact of Remoteness and Socio-Economic Status on Child and Adolescent Injury-Related Mortality in Australia. Children 2021, 8, 5. [Google Scholar] [CrossRef]
- Boon, H. Preparedness and vulnerability: An issue of equity in Australian disaster situations. Aust. J. Emerg. Manag. 2013, 28, 12–16. [Google Scholar]
- Howard, A.; Agllias, K.; Bevis, M.; Blakemore, T. How Social Isolation Affects Disaster Preparedness and Response in Australia: Implications for Social Work. Aust. Soc. Work 2018, 71, 392–404. [Google Scholar] [CrossRef]
- Lade, S.J.; Steffen, W.; de Vries, W.; Carpenter, S.R.; Donges, J.F.; Gerten, D.; Hoff, H.; Newbold, T.; Richardson, K.; Rockström, J. Human impacts on planetary boundaries amplified by Earth system interactions. Nat. Sustain. 2020, 3, 119–128. [Google Scholar] [CrossRef]
- Cardona, O.D.; Van Aalst, M.K.; Birkmann, J.; Fordham, M.; Mc Gregor, G.; Rosa, P.; Pulwarty, R.S.; Schipper, E.L.F.; Sinh, B.T.; Décamps, H. Determinants of risk: Exposure and vulnerability. In Managing the Risks of Extreme Events and Disasters to Advance Climate Change Adaptation: Special Report of the Intergovernmental Panel on Climate Change; Cambridge University Press: Cambridge, UK, 2012; pp. 65–108. [Google Scholar]
- Lindsay, J.R. The Determinants of Disaster Vulnerability: Achieving Sustainable Mitigation through Population Health. Nat. Hazards 2003, 28, 291–304. [Google Scholar] [CrossRef]
- Franklin, R.C.; Miller, L.; Watt, K.; Leggat, P.A. Tourist injury. In Tourist Health, Safety and Wellbeing in the New Normal; Springer: New York, NY, USA, 2021; pp. 189–218. [Google Scholar]
- Leggat, P.A. Travel medicine and tourist health. In Tourist Health, Safety and Wellbeing in the New Normal; Springer: New York, NY, USA, 2021; pp. 25–46. [Google Scholar]
- Grozinger, P.; Parsons, S.J.B. The COVID-19 Outbreak and Australia’s Education and Tourism Exports; RBA Bulletin; Reserve Bank of Australia: Canberra, Australia, December 2020. [Google Scholar]
- United Nations Office for Disaster Risk Reduction. Terminology—Disaster. Available online: https://www.undrr.org/terminology/disaster (accessed on 31 October 2022).
- Bureau of Meterology. Map of Climate Zones of Australia. Available online: http://www.bom.gov.au/climate/how/newproducts/images/zones.shtml (accessed on 26 November 2022).
| Disaster Event | ICD-10 Codes | Categories Used for Analysis |
|---|---|---|
| Heat | X30 exposure to excessive natural heat | Heat |
| Cold | X31 exposure to excessive natural cold | Cold |
| Weather event not specified | X32 exposure to sunlight X39 exposure to other and unspecified forces of nature | Other |
| Lightning | X33 victim of lightning | Other |
| Storms and floods | X37 victim of cataclysmic storms (includes blizzards, tornadoes, and hurricanes) X38 victim of flood | Storms and Floods |
| Variable | Total (n = 682) | Heat (n = 252) | Cold (n = 281) | Storms & Flood (n = 103) | Other (n = 46) | X2 (p Value) |
|---|---|---|---|---|---|---|
| Sex | ||||||
| Female | 257 | 99 | 115 | 34 | 9 | 8.922 (p = 0.030) |
| Male | 425 | 153 | 166 | 69 | 37 | |
| Age group | ||||||
| 0–17 years | 43 | 24 | 0 | 18 | NP | 116.204 (p < 0.001) |
| 18–39 years | 92 | 43 | 15 | 19 | 15 | |
| 40–64 years | 203 | 79 | 71 | 34 | 19 | |
| 65+ years | 344 | 106 | 195 | 32 | 11 | |
| Aboriginal and Torres Strait Islander Peoples | ||||||
| Aboriginal and/or Torres Strait Islander | 46 | 25 | NP | 13 | 5 | 25.542 (p < 0.001) |
| Non-Indigenous | 622 | 224 | 272 | 86 | 40 | |
| Not Stated | 14 | NP | 6 | NP | NP | - |
| Visitor Status | ||||||
| Death in state of residence | 633 | 217 | 276 | 101 | 39 | 43.419 (p < 0.001) |
| Interstate Death | 22 | 13 | 5 | NP | NP | |
| International visitor | 27 | 22 | 0 | 0 | 5 | |
| Remoteness classification of decedent resident location | ||||||
| Major Cities | 386 | 132 | 215 | 20 | 19 | 131.723 (p < 0.001) |
| Inner Regional | 138 | 35 | 44 | 49 | 10 | |
| Outer Regional | 68 | 29 | 16 | 18 | 5 | |
| Remote | 28 | 12 | NP | 9 | NP | |
| Very Remote | 30 | 20 | 0 | 7 | NP | |
| Usual residence overseas | 27 | 22 | 0 | 0 | 5 | |
| Usual residence unknown | 5 | NP | NP | 0 | NP | - |
| Index of Relative Socio-economic Advantage and Disadvantage (IRSAD) of decedent resident location | ||||||
| Low | 196 | 82 | 62 | 38 | 14 | 39.470 (p < 0.001) |
| Mid | 260 | 84 | 101 | 55 | 20 | |
| High | 147 | 50 | 86 | 6 | 5 | |
| Missing | 79 | 36 | 32 | NP | 7 | - |
| Season | ||||||
| Summer (December–February) | 283 | 185 | 14 | 62 | 22 | 349.900 (p < 0.001) |
| Autumn (March–May) | 106 | 17 | 57 | 23 | 9 | |
| Winter (June–August) | 182 | 7 | 157 | 14 | NP | |
| Spring (September–November) | 111 | 43 | 53 | NP | 11 | |
| Variable | Number of Resident Deaths | Rate/ 100,000 Population | RR (95% Confidence Interval [CI]) |
|---|---|---|---|
| Sex | |||
| Female | 248 | 0.15 | 1 |
| Male | 407 | 0.22 | 1.43 (1.22–1.68) |
| Age group | |||
| 0–17 years | 42 | 0.06 | 1 |
| 19–39 years | 83 | 0.08 | 1.44 (0.99–2.09) |
| 40–64 years | 191 | 0.19 | 3.27 (2.34–4.57) |
| 65+ years | 339 | 0.74 | 12.78 (9.28–17.62) |
| Indigenous status | |||
| Aboriginal and/or Torres Strait Islander Peoples | 46 | 0.44 | 2.31 (1.71–3.11) |
| Non-Indigenous | 595 | 0.19 | 1 |
| Remoteness classification of decedent resident location | |||
| Major Cities | 386 | 0.17 | 1 |
| Inner Regional | 138 | 0.24 | 1.39 (1.14–1.69) |
| Outer Regional | 68 | 0.24 | 1.43 (1.11–1.86) |
| Remote | 28 | 0.67 | 3.97 (2.71–5.83) |
| Very Remote | 30 | 1.06 | 6.23 (4.30–9.04) |
| Category of Condition | Total (n = 401) | Heat (n = 170) | Cold (n = 203) | Storms & Flood (n = 0) | Other (n = 28) |
|---|---|---|---|---|---|
| Circulatory system | 202 | 125 | 72 | 0 | 5 |
| Digestive system | 15 | NP | 12 | 0 | 0 |
| Endocrine and metabolic | 20 | 7 | 13 | 0 | 0 |
| External cause | 61 | 10 | 44 | 0 | 7 |
| Genitourinary system | 9 | 0 | 9 | 0 | 0 |
| Infectious and parasitic | 18 | NP | 16 | 0 | 0 |
| Mental and behavioural | 10 | 5 | NP | 0 | NP |
| Musculoskeletal | NP | NP | NP | 0 | NP |
| Neoplasms | 27 | 5 | 11 | 0 | 11 |
| Nervous system | 10 | NP | 6 | 0 | NP |
| Respiratory system | 22 | 9 | 12 | 0 | NP |
| Skin | NP | 0 | NP | 0 | 0 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Peden, A.E.; Heslop, D.; Franklin, R.C. Weather-Related Fatalities in Australia between 2006 and 2019: Applying an Equity Lens. Sustainability 2023, 15, 813. https://doi.org/10.3390/su15010813
Peden AE, Heslop D, Franklin RC. Weather-Related Fatalities in Australia between 2006 and 2019: Applying an Equity Lens. Sustainability. 2023; 15(1):813. https://doi.org/10.3390/su15010813
Chicago/Turabian StylePeden, Amy E, David Heslop, and Richard C Franklin. 2023. "Weather-Related Fatalities in Australia between 2006 and 2019: Applying an Equity Lens" Sustainability 15, no. 1: 813. https://doi.org/10.3390/su15010813
APA StylePeden, A. E., Heslop, D., & Franklin, R. C. (2023). Weather-Related Fatalities in Australia between 2006 and 2019: Applying an Equity Lens. Sustainability, 15(1), 813. https://doi.org/10.3390/su15010813








