Current Response and Management Decisions of the European Union to the COVID-19 Outbreak: A Review
Abstract
1. Introduction
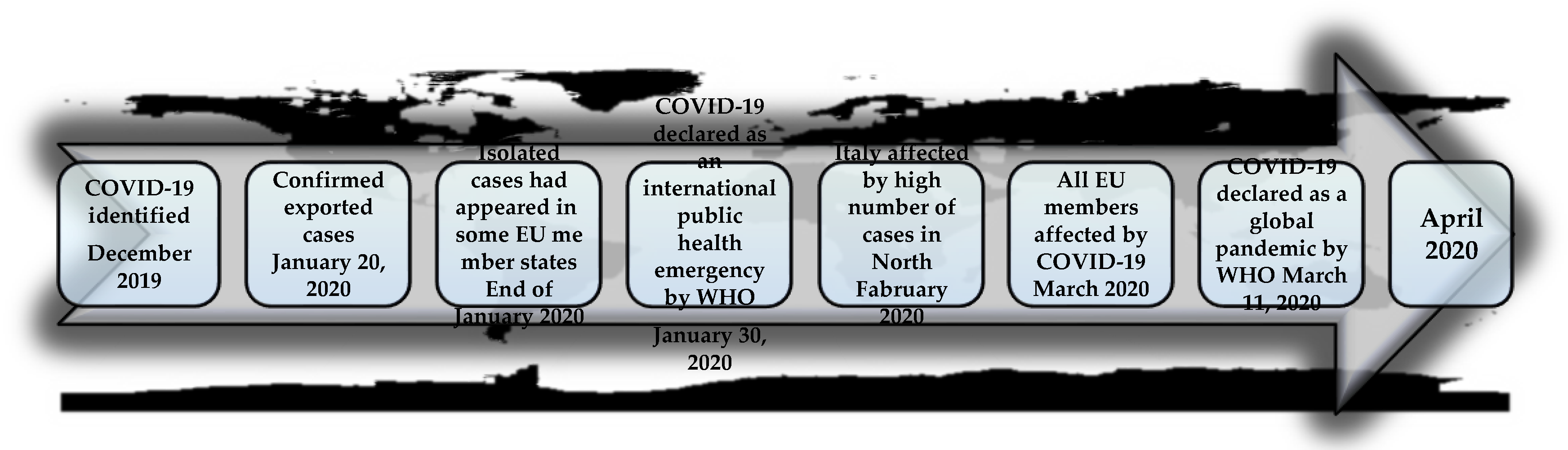
2. Global Emergence of COVID-19
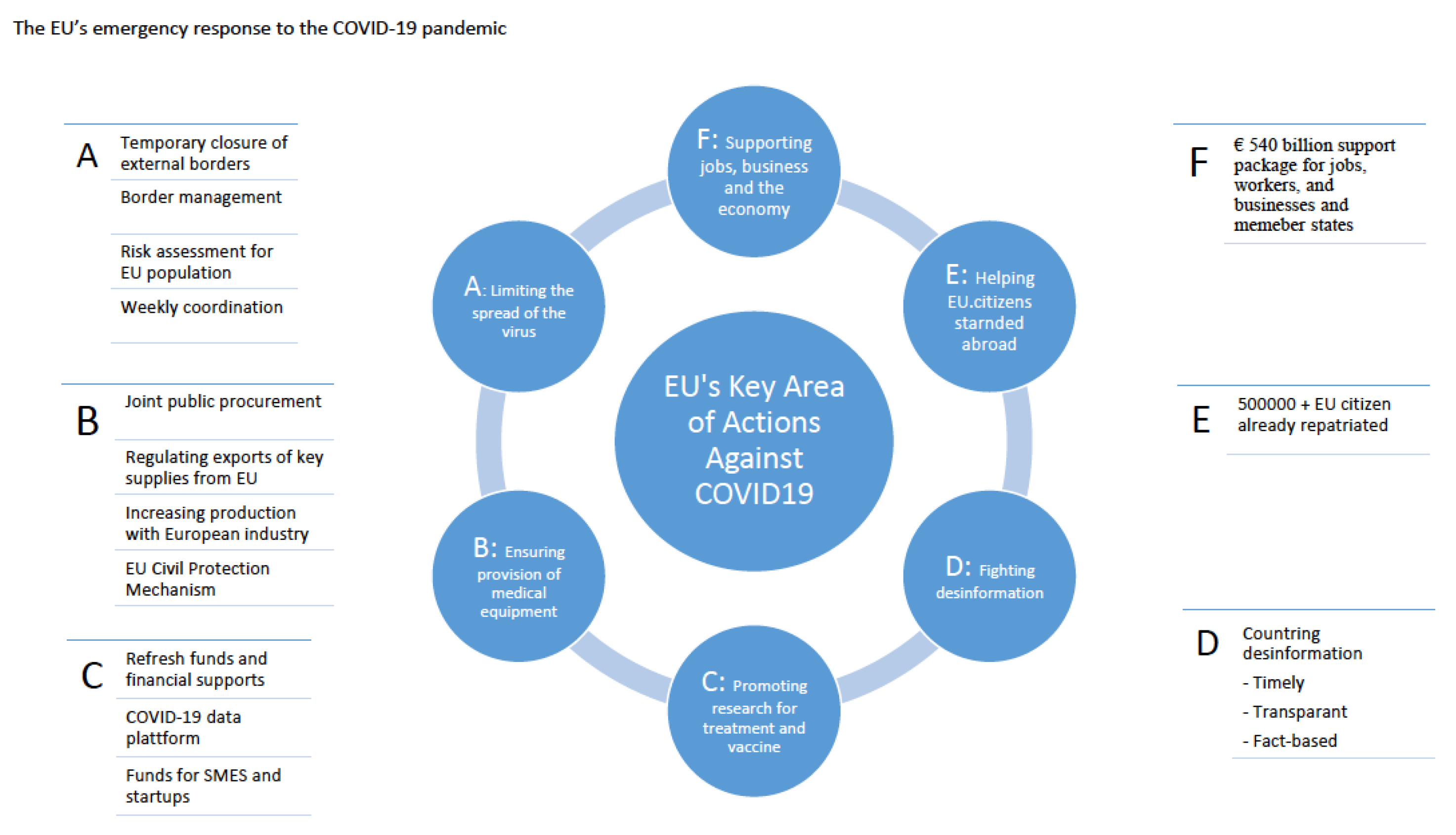
3. The EU’s Response
4. Challenges to Limiting the Spread: Borders and Mobility
5. Ensuring the Provision of Medical Equipment
- Joint public procurement for facemasks and other PPE. On 19 March, rescEU stockpiling was created, a common European reserve of medical equipment such as ventilators, PPE, reusable masks, vaccines and therapeutics, and laboratory supplies, financed at 90% by the EU Commission [24].
- Close contacts with the European industry to increase the production of all necessary supplies. The Commission announced four official calls to gather medical equipment and supplies for health systems in member countries (28 February, 17 and 19 March 2020), with 25 Member States responding to the request. The first call resulted in offers matching the requested amounts. The contracts concerning those calls were underway in the coming weeks, with distribution to member states of equipment and supplies expected shortly afterward. The European Commission coordinated revised harmonized standards enabling manufacturers to introduce into the market more PPE devices for patients, health care workers, and citizens in general [24].
- Regulated exports of personal protective equipment from the EU to ensure supply in all Member States. Member States are responsible for the issuance of authorizations. However, the process is managed by the Emergency Response Coordination Centre (ERCC), and for any questions concerning the supply of PPE within the EU, the Member States may refer to the ERCC. The Centre runs 24/7 and aims to help any country inside or outside the EU affected by a major disaster upon request from the national authorities or a United Nations (UN) body. The agency also is responsible for emergency communication and monitoring of instruments through the Common Emergency Communication and Information System (CECIS), a web-based alert and notification application enabling real-time exchange of information.
- Priority lanes to facilitate the free circulation of goods and people who need to cross borders. The implementation of the Union’s policies is governed by the principle of solidarity among the Member States. To avoid shortages and avoid worsening the existing social and economic difficulties, Member States should not undertake measures that jeopardize the integrity of the Single Market for goods, of supply chains, or engage in any unfair practices. They must always admit their citizens and residents, and facilitate the transit of other EU citizens and residents who are returning home. New guidelines set out principles for an integrated approach to effective border management to protect health while preserving the integrity of the Single Market [25].
6. Promoting Research for Treatments and Vaccines
7. Supporting Employment, Businesses, and the Economy
8. Crisis Coordination
9. Limitations
10. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Graffunder, C.; Sakurada, B. Preparing Health Care and Public Health Professionals for Team Performance: The Community as a Classroom. NAM Perspectives. 2016. Available online: http://nam.edu/wp-content/uploads/2016/04/Preparing-Health-Care-and-Public-Health-Professionals-for-Team-Performance-The-Community-as-Classroom.pdf (accessed on 10 April 2020).
- Breman, J.G. Population-Based Medicine. JAMA 1984, 252, 1188. [Google Scholar] [CrossRef]
- Population Health Management: Steps to Risk Sharing and Data Analytics. Brentwood (T.N.): Health Leaders Media. 2013. Available online: http://www.healthleadersmedia.com/intelligence/detail/cfm?content_id=296742&year=2013 (accessed on 20 April 2020).
- Coombs, W.T.; Holladay, S.J. (Eds.) The Handbook of Crisis Communication; John Wiley & Sons: Hoboken, NJ, USA, 2011. [Google Scholar]
- Burkle, F.M. Challenges of Global Public Health Emergencies: Development of a Health-Crisis Management Framework. Tohoku J. Exp. Med. 2019, 249, 33–41. [Google Scholar] [CrossRef]
- Foddai, A.; Lindberg, A.; Lubroth, J.; Ellis-Iversen, J. Surveillance to improve evidence for community control decisions during the COVID-19 pandemic–opening the animal epidemic toolbox for public health. One Health 2020. [Google Scholar] [CrossRef] [PubMed]
- The Flether School. A Multidisciplinary Approach to the Crisis: Fletcher Experts Weigh in. 19 March 2020. Available online: https://fletcher.tufts.edu/news-events/news/multidisciplinary-approach-crisis-fletcher-experts-weigh (accessed on 10 April 2020).
- Sohrabi, C.; Alsafi, Z.; O’Neill, N.; Khan, M.; Kerwan, A.; Al-Jabir, A.; Iosifidis, C.; Agha, R. World Health Organization declares global emergency: A review of the 2019 novel coronavirus (COVID-19). Int. J. Surg. 2020. [Google Scholar] [CrossRef]
- Johnson, H.C.; Gossner, C.M.; Colzani, E.; Kinsman, J.; Alexakis, L.; Beauté, J.; Würz, A.; Tsolova, S.; Bundle, N.; Ekdahl, K. Potential scenarios for the progression of a COVID-19 epidemic in the European Union and the European Economic Area, March 2020. Eurosurveillance 2020, 25. [Google Scholar] [CrossRef] [PubMed]
- Pullano, G.; Pinotti, F.; Valdano, E.; Boëlle, P.Y.; Poletto, C.; Colizza, V. Novel coronavirus (2019-nCoV) early-stage importation risk to Europe, January 2020. Eurosurveillance 2020, 25. [Google Scholar] [CrossRef]
- Stoecklin, S.B.; Rolland, P.; Silue, Y.; Mailles, A.; Campese, C.; Simondon, A.; Mechain, M.; Meurice, L.; Nguyen, M.; Bassi, C.; et al. First cases of coronavirus disease 2019 (COVID-19) in France: Surveillance, investigations and control measures, January 2020. Eurosurveillance 2020, 25. [Google Scholar] [CrossRef]
- Rothe, C.; Schunk, M.; Sothmann, P.; Bretzel, G.; Froeschl, G.; Wallrauch, C.; Zimmer, T.; Thiel, V.; Janke, C.; Guggemos, W.; et al. Transmission of 2019-nCoV infection from an asymptomatic contact in Germany. N. Engl. J. Med. 2020, 382, 970–971. [Google Scholar] [CrossRef]
- Dong, E.; Du, H.; Gardner, L. An interactive web-based dashboard to track COVID-19 in real time. Lancet Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Lescurem, F.X.; Bouadma, L.; Nguyen, D.; Parisey, M.; Wicky, P.H.; Behillil, S.; Gaymard, A.; Bouscambert-Duchamp, M.; Donati, F.; Le Hingrat, Q.; et al. Clinical and virological data of the first cases of COVID-19 in Europe: A case series. Lancet Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Council Implementing Decision (EU) 2018/1993 of 11 December 2018 on the EU Integrated Political Crisis Response Arrangements ST/13422/2018/INIT. OJ L 320, 17.12.2018; pp. 28–34. Available online: https://eur-lex.europa.eu/eli/dec_impl/2018/1993/oj (accessed on 7 April 2020).
- European Council. Conclusions by the President of the European Council Following the Video Conference with Members of the European Council on COVID-19. Available online: https://www.consilium.europa.eu/en/press/press-releases/2020/03/17/conclusions-by-the-president-of-the-european-council-following-the-video-conference-with-members-of-the-european-council-on-covid-19/ (accessed on 5 April 2020).
- Chinazzi, M.; Davis, J.T.; Ajelli, M.; Gioannini, C.; Litvinova, M.; Merler, S.; Pastore YPiontti, A.; Mu, K.; Rossi, L.; Sun, K.; et al. The effect of travel restrictions on the spread of the 2019 novel coronavirus (COVID-19) outbreak. Science 2020. [Google Scholar] [CrossRef] [PubMed]
- Website of the Republic of Poland. Coronavirus: Information and Recommendations. Available online: https://www.gov.pl/web/coronavirus (accessed on 9 April 2020).
- Djalante, R.; Shaw, R.; Dewit, A. Building resilience against biological hazards and pandemics: COVID-19 and its implications for the Sendai Framework. Prog. Disaster Sci. 2020. [Google Scholar] [CrossRef]
- De Miguel Beriain, I.; Atienza-Macías, E.; Armaza, E. The European Union integrated political crisis response arrangements: Improving the European Union’s major crisis response coordination capacities. Disaster Med. Public Health Prep. 2015, 9, 234–238. [Google Scholar] [CrossRef] [PubMed]
- European Council. Statement on COVID-19 Economic Policy Response. Available online: https://www.consilium.europa.eu/en/press/press-releases/2020/03/16/statement-on-covid-19-economic-policy-response (accessed on 5 April 2020).
- European Commission. Coronavirus Response. Available online: https://ec.europa.eu/info/live-work-travel-eu/health/coronavirus-response_en (accessed on 27 March 2020).
- Outbreak of Novel Coronavirus Disease 2019 (COVID-19): Increased Transmission Globally—Fifth Update. Available online: https://www.ecdc.europa.eu/sites/default/files/documents/RRA-outbreak-novel-coronavirus-disease-2019-increase-transmission-globally-COVID-19.pdf (accessed on 20 April 2020).
- European Commission. Ensuring the Availability of Supplies and Equipment. Available online: https://ec.europa.eu/info/live-work-travel-eu/health/coronavirus-response/public-health_en#health-crisis-management (accessed on 5 April 2020).
- European Commission. Guidelines for Border Management Measures to Protect Health and Ensure the Availability of Goods and Essential Services. Available online: https://ec.europa.eu/home-affairs/sites/homeaffairs/files/what-we-do/policies/european-agenda-migration/20200316_covid-19-guidelines-for-border-management.pdf (accessed on 8 April 2020).
- Bozorgmehr, K.; Saint, V.; Kaasch, A.; Stuckler, D.; Kentikelenis, A. COVID and the convergence of three crises in Europe. Lancet Public Health 2020. [Google Scholar] [CrossRef]
- Clifford Chance. Coronavirus: Government Financial Aid to Business an International Guide. 23 March 2020. Available online: https://www.cliffordchance.com/content/dam/cliffordchance/briefings/2020/03/coronavirus-government-financial-aid-to-business-an-international-guide.pdf (accessed on 5 April 2020).
- Government Office of Sweden. Economic Measures in Response to COVID-19. Available online: https://www.government.se/articles/2020/03/economic-measures-in-response-to-covid-19/ (accessed on 16 March 2020).
- European Commision. A European Instrument for Temporary Support to Mitigate Unemployment Risks in an Emergency (SURE). Available online: https://ec.europa.eu/info/business-economy-euro/economic-and-fiscal-policy-coordination/eu-financial-assistance/loan-programmes/sure_en (accessed on 20 April 2020).
- European Commision. Migration and Home Affairs. Available online: https://ec.europa.eu/home-affairs/what-we-do/networks/european_migration_network/glossary_search/third-country-national_en) (accessed on 20 April 2020).
- European Union. External Action. Available online: https://eeas.europa.eu/headquarters/headquarters-homepage/76203/good-stories-consular-support-eu-citizens-stranded-abroad_en (accessed on 9 April 2020).
- European Commision. About European Civil Protection and Humanitarian Aid Operations. Available online: https://ec.europa.eu/echo/who/about-echo_en (accessed on 20 April 2020).
- Khorram-Manesh, A.; Berlin, J.; Carlström, E. Two validated ways of improving the ability of decision-making in emergencies; Results from a literature review. Bull. Emerg. Trauma 2016, 4, 186. [Google Scholar] [PubMed]
- La, V.P.; Pham, T.; Ho, M.; Nguyen, M.; Nguyen, K.P.; Vuong, T.; Nguyen, H.T.; Tran, T.; Khuc, Q.; Ho, M.-T.; et al. Policy response, social media and science journalism for the sustainability of the public health system amid COVID-19 outbreak: The Vietnam lessons. Sustainability 2020, 12, 2931. [Google Scholar] [CrossRef]
- Lewnard, J.A.; Lo, N.C. Scientific and ethical basis for social-distancing interventions against COVID-19. Lancet Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Khorram-Manesh, A. Flexible Surge Capacity—Public Health, Public Education, and Disaster Management. Health Promot. Perspect. 2020. Available online: https://hpp.tbzmed.ac.ir/ (accessed on 7 May 2020).
- Khorram-Manesh, A.; Ashkenazi, M.; Djalali, A.; Ingrassia, P.L.; Friedl, T.; von Armin, G.; Lupesco, O.; Kaptan, K.; Arculeo, C.; Hreckovski, B.; et al. Education in disaster management and emergencies: Defining a new European course. Disaster Med. Public Health Prep. 2015, 9, 245–255. [Google Scholar] [CrossRef]
- Khorram-Manesh, A.; Hedelin, A.; Örtenwall, P. Hospital-related incidents; causes and its impact on disaster preparedness and prehospital organisations. Scand. J. TraumaResusc. Emerg. Med. 2009, 17, 26. [Google Scholar] [CrossRef]
- Burkle, F.M. Population-based triage management in response to surgen And Emergency Medicine.paredness and prehobioevent disaster. Acad. Emerg. Med. 2006, 13, 1118–1129. [Google Scholar] [CrossRef] [PubMed]
- Goniewicz, K.; Magiera, M.; Burkle, F.M.; Goniewicz, M. Prospective study on the potential use of satellite data for disaster prevention, preparedness, and mitigation in Poland. Prehospital Disaster Med. 2020, 1–4. [Google Scholar] [CrossRef] [PubMed]
- Goniewicz, K.; Misztal-Okońska, P.; Pawłowski, W.; Burkle, F.M., Jr.; Czerski, R.; Hertelendy, A.J.; Goniewicz, M. Evacuation from Healthcare Facilities in Poland: Legal Preparedness and Preparation. Int. J. Environ. Res. Public Health 2020, 17, 1779. [Google Scholar] [CrossRef] [PubMed]
- European Commision. Fighting Disinformation. Available online: https://ec.europa.eu/info/live-work-travel-eu/health/coronavirus-response/fighting-disinformation_en (accessed on 20 April 2020).
- Khorram-Manesh, A.; Lupesco, O.; Friedl, T.; Arnim, G.; Kaptan, K.; Djalali, A.R.; Foletti, M.; Ingrasia, P.L.; Ashkenazi, M.; Arculeo, C.; et al. Education in disaster management: What do we offer and what do we need? Proposing a New Global Program. Disaster Med. Public Health Prep. 2016, 10, 854–873. [Google Scholar] [CrossRef]
- Ranney, M.L.; Griffeth, V.; Jha, A.K. Critical Supply Shortages—The Need for Ventilators and Personal Protective Equipment during the Covid-19 Pandemic. N. Engl. J. Med. 2020. [Google Scholar] [CrossRef]
- World Health Organization. Key Planning Recommendations for Mass Gatherings in the Context of COVID-19: Interim Guidance, 19 March 2020 (No. WHO/2019-nCoV/POE Mass Gathering/2020.2). World Health Organization. Available online: https://www.who.int/publications-detail/key-planning-recommendations-for-mass-gatherings-in-the-context-of-the-current-covid-19-outbreak (accessed on 8 April 2020).
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Goniewicz, K.; Khorram-Manesh, A.; Hertelendy, A.J.; Goniewicz, M.; Naylor, K.; Burkle, F.M., Jr. Current Response and Management Decisions of the European Union to the COVID-19 Outbreak: A Review. Sustainability 2020, 12, 3838. https://doi.org/10.3390/su12093838
Goniewicz K, Khorram-Manesh A, Hertelendy AJ, Goniewicz M, Naylor K, Burkle FM Jr. Current Response and Management Decisions of the European Union to the COVID-19 Outbreak: A Review. Sustainability. 2020; 12(9):3838. https://doi.org/10.3390/su12093838
Chicago/Turabian StyleGoniewicz, Krzysztof, Amir Khorram-Manesh, Attila J. Hertelendy, Mariusz Goniewicz, Katarzyna Naylor, and Frederick M. Burkle, Jr. 2020. "Current Response and Management Decisions of the European Union to the COVID-19 Outbreak: A Review" Sustainability 12, no. 9: 3838. https://doi.org/10.3390/su12093838
APA StyleGoniewicz, K., Khorram-Manesh, A., Hertelendy, A. J., Goniewicz, M., Naylor, K., & Burkle, F. M., Jr. (2020). Current Response and Management Decisions of the European Union to the COVID-19 Outbreak: A Review. Sustainability, 12(9), 3838. https://doi.org/10.3390/su12093838








