Empowering Patients to Co-Create a Sustainable Healthcare Value
Abstract
1. Introduction
2. Literature Review
2.1. Patient Empowerment and Healthcare Sustainability
- -
- -
- -
- -
- Communication with healthcare professionals: patients’ ability to effectively and efficiently communicate with healthcare professionals [15,26,29]. This is a reciprocal process where patients must be able to make detailed explanations of their symptoms, express considerations and preferences, and ask for more information; clinicians must encourage dialogue, mutual listening and comprehension.
2.2. Value Co-Creation and Patient Empowerment
3. Materials and Method
Sample
4. Results
5. Discussion
6. Conclusions, Practical and Theoretical Implications
7. Research Limitations and Future Research
Author Contributions
Funding
Conflicts of Interest
References
- Aquino, R.P.; Barile, S.; Grasso, A.; Saviano, M. Envisioning smart and sustainable healthcare: 3D Printing technologies for personalized medication. Futures 2018, 103, 35–50. [Google Scholar] [CrossRef]
- ISTAT. Rapporto Annuale 2018—La Situazione del Paese. 2018. Available online: https://www.istat.it/it/archivio/214230 (accessed on 25 September 2018).
- World Health Organization, Regional Office for Europe. Health 2020 Policy Framework and Strategy Document; WHO: Geneva, Switzerland, 2012. [Google Scholar]
- AGI. Tumori: Oncologi, in Italia Costano 19 mld l’Anno. 2018. Available online: http://www.regioni.it/sanita/2018/06/01/tumori-oncologi-in-italia-costano-19-mld-lanno-564182/ (accessed on 1 October 2018).
- Barile, S. Introduzione. In Condizioni di Efficacia Relazionale e di Performance Nell’Azienda Sanitaria; Saviano, M., Ed.; Giappichelli: Torino, Italy, 2012. [Google Scholar]
- Saviano, M.; Bassano, C.; Piciocchi, P.; Di Nauta, P.; Lettieri, M. Monitoring Viability and Sustainability in Healthcare Organizations. Sustainability 2018, 10, 3548. [Google Scholar] [CrossRef]
- Zuckerman, S.; Hadley, J.; Iezzoni, L. Measuring Hospital Efficiency with Frontier Cost Functions. J. Health Econ. 1994, 13, 255–280. [Google Scholar] [CrossRef]
- Conrad, D.; Wickizer, T.; Maynard, C.; Klastorin, T.; Lessler, D.; Ross, A.; Soderstrom, N.; Sullivan, S.; Alexander, J.; Travis, K. Managing Care, Incentives, and Information: An Exploratory Look Inside the ‘Black Box’ of Hospital Efficiency. Health Serv. Res. 1996, 31, 235–259. [Google Scholar] [PubMed]
- Carman, J.M.; Shortell, S.M.; Foster, R.W.; Hughes, E.F.; Boerstler, H.; O’Brien, J.L.; O’Conner, E.J. Keys for successful implementation of total quality management in hospitals. Health Care Manag. Rev. 1996, 21, 48–60. [Google Scholar] [CrossRef]
- Bretthauer, K.M.; Côté, M.J. A model for planning resource requirements in health care organizations. Decis. Sci. 1998, 29, 243–270. [Google Scholar] [CrossRef]
- Arah, O.A.; Klazinga, N.S.; Delnoij, D.M.J.; Ten Asbroek, A.H.A.; Custers, T. Conceptual frameworks for health systems performance: A quest for effectiveness, quality, and improvement. Int. J. Qual. Health Care 2003, 15, 377–398. [Google Scholar] [CrossRef] [PubMed]
- Coulter, A.; Jenkinson, J. European patients’ views on the responsiveness of health systems and healthcare providers. Eur. J. Public Health 2005, 15, 355–360. [Google Scholar] [CrossRef] [PubMed]
- Berry, L.L.; Bendapudi, N. Health care: A fertile field for service research. J. Serv. Res. 2007, 10, 111–122. [Google Scholar] [CrossRef]
- Akaka, M.A.; Vargo, S.L.; Lusch, R.F. The complexity of context: A service ecosystems approach for international marketing. J. Mark. Res. 2013, 21, 1–20. [Google Scholar] [CrossRef]
- Fotoukian, Z.; Shahboulaghi, F.M.; Khoshknab, M.F.; Mohammadi, E. Concept analysis of empowerment in old people with chronic diseases using a hybrid model. Asian Nurs. Res. 2014, 8, 118–127. [Google Scholar] [CrossRef] [PubMed]
- Anderson, R.M.; Funnell, M.M. Patient empowerment: Myths and misconceptions. Patient Educ. Couns. 2010, 79, 277–282. [Google Scholar] [CrossRef] [PubMed]
- Rodwell, C.M. An analysis of the concept of empowerment. J. Adv. Nurs. 1996, 23, 305–313. [Google Scholar] [CrossRef] [PubMed]
- Ouschan, R.; Sweeney, J.C.; Johnson, L.W. Dimensions of patient empowerment: Implications for professional services marketing. Heal. Mark. Q. 2000, 18, 99–114. [Google Scholar] [CrossRef] [PubMed]
- Bann, C.M.; Sirois, F.M.; Walsh, E.G. Provider support in complementary and alternative medicine: Exploring the role of patient empowerment. J. Altern. Complement. Med. 2010, 16, 745–752. [Google Scholar] [CrossRef] [PubMed]
- McAllister, M.; Dunn, G.; Payne, K.; Davies, L.; Todd, C. Patient empowerment: The need to consider it as a measurable patient-reported outcome for chronic conditions. BMC Health Serv. Res. 2012, 12, 157. [Google Scholar] [CrossRef] [PubMed]
- Aujoulat, I.; Deccache, A.; Marcolongo, R.; Bonadiman, L. Reconsidering patient empowerment in chronic illness: A critique of models of self-efficacy and bodily control. Soc. Sci. Med. 2008, 66, 1228–1239. [Google Scholar] [CrossRef] [PubMed]
- Moretta Tartaglione, A.; Cavacece, Y.; Cassia, F.; Russo, G. The excellence of patient-centered healthcare: Investigating the links between empowerment, cocreation and satisfaction. TQM J. 2018, 30, 153–167. [Google Scholar] [CrossRef]
- Polese, F.; Moretta Tartaglione, A.; Cavacece, Y. Patient empowerment for healthcare service quality improvements: A value co-creation view. In Proceedings of the 19th Toulon-Verona International Conference Excellence in Services, Huelva, Spain, 5–6 September 2016; pp. 385–397. [Google Scholar]
- Seiders, K.; Flynn, A.G.; Berry, L.L.; Haws, K.L. Motivating customers to adhere to expert advice in professional services a medical service context. J. Serv. Res. 2015, 18, 39–58. [Google Scholar] [CrossRef]
- Hibbard, J.H.; Stockard, J.; Mahoney, E.R.; Tusler, M. Development of the Patient Activation Measure (PAM): Conceptualizing and measuring activation in patients and consumers. Health Serv. Res. 2004, 39, 1005–1026. [Google Scholar] [CrossRef] [PubMed]
- Small, N.; Bower, P.; Chew-Graham, C.; Whalley, D.; Protheroe, J. Patient empowerment in long-term conditions: Development and preliminary testing of a new measure. BMC Heal. Serv. Res. 2013, 13, 263. [Google Scholar] [CrossRef] [PubMed]
- Salmon, P.; Hall, G.M. Patient empowerment or the emperor’s new clothes. J. R. Soc. Med. 2004, 97, 53–56. [Google Scholar] [CrossRef] [PubMed]
- Oh, H.J.; Lee, B. The Effect of computer-mediated social support in online communities on patient empowerment and doctor-patient communication. Health Commun. 2012, 27, 30–41. [Google Scholar] [CrossRef] [PubMed]
- Aujoulat, I.; D’Hoore, W.; Deccache, A. Patient empowerment in theory and practice: Polysemy or cacophony? Patient Educ. Couns. 2007, 66, 13–20. [Google Scholar] [CrossRef] [PubMed]
- Vargo, S.L.; Lusch, R.F. Evolving to a New Dominant Logic for Marketing. J. Mark. 2004, 68, 1–17. [Google Scholar] [CrossRef]
- Vargo, S.L.; Lusch, R.F. Service-dominant logic: Continuing the evolution. J. Acad. Mark. Sci. 2008, 36, 1–10. [Google Scholar] [CrossRef]
- Grönroos, C. Service logic revisited: Who creates value? And who co-creates? Eur. Bus. Rev. 2008, 20, 298–314. [Google Scholar] [CrossRef]
- Grönroos, C. Service Management and Marketing. A Customer Relationship Management Approach; John Wiley: Chichester, UK, 2000. [Google Scholar]
- Maglio, P.; Spohrer, J. Fundamentals of service science. J. Acad. Mark. Sci. 2008, 36, 18–20. [Google Scholar] [CrossRef]
- Vargo, S.L.; Maglio, P.P.; Akaka, M.A. On value and value co-creation: A service systems and service logic perspective. Eur. Manag. J. 2008, 26, 145–152. [Google Scholar] [CrossRef]
- Spohrer, J.; Maglio, P.P.; Bailey, J.; Gruhl, D. Steps toward a science of service systems. Computer 2007, 40, 71–77. [Google Scholar] [CrossRef]
- Vargo, S.L. Customer Integration and Value Creation: Paradigmatic Traps and Perspectives. J. Serv. Res. 2008, 11, 211–215. [Google Scholar] [CrossRef]
- Saviano, M.; Barile, S.; Spohrer, J.C.; Caputo, F. A service research contribution to the global challenge of sustainability. J. Serv. Theory Pract. 2017, 27, 951–976. [Google Scholar] [CrossRef]
- Aquilani, B.; Silvestri, C.; Ruggieri, A. Sustainability, TQM and Value Co-Creation Processes: The Role of Critical Success Factors. Sustainability 2016, 8, 995. [Google Scholar] [CrossRef]
- Yi, Y.; Gong, T. Customer value co-creation behavior: Scale development and validation. J. Bus. Res. 2013, 66, 1279–1284. [Google Scholar] [CrossRef]
- McWilliam, C.L. Patients, persons or partners? Involving those with chronic disease in their care. Chronic Illn. 2009, 5, 277–292. [Google Scholar] [CrossRef] [PubMed]
- Carrubbo, L.; Bruni, R.; Cavacece, Y.; Moretta Tartaglione, A. Service System Platforms to Improve Value Co-Creation: Insights for Translational Medicine. In Service Dominant Logic, Network and Systems Theory and Service Science: Integrating Three Perspectives for a New Service Agenda; Gummesson, E., Mele, C., Polese, F., Eds.; Giannini Editore: Napoli, Italy, 2015. [Google Scholar]
- Nordgren, L. The performativity of the service management discourse: “Value creating customers” in health care”. J. Health Organ. Manag. 2008, 22, 510–528. [Google Scholar] [CrossRef] [PubMed]
- Shackley, P.; Ryan, M. What is the Role of the Consumer in Health Care? J. Soc. Policy 1994, 23, 517–541. [Google Scholar] [CrossRef]
- Elg, M.; Engström, J.; Witell, L.; Poksinska, B. Co-creation and learning in health-care service development. J. Serv. Manag. 2012, 23, 328–343. [Google Scholar] [CrossRef]
- Rantala, K.; Karjaluoto, H. Co-creation in health care: Insights into the transformation from value creation to value co-creation through digitization. In Proceedings of the 20th International Academic Mindtrek Conference, Tampere, Finland, 17–18 October 2016; pp. 34–41. [Google Scholar]
- Nambisan, P.; Nambisan, S. Models of consumer value cocreation in health care. Health Care Manag. Rev. 2009, 47, 23–30. [Google Scholar] [CrossRef] [PubMed]
- Gill, L.; White, L.; Cameron, I.D. Service co-creation in community-based aged healthcare. Manag. Serv. Qual. Int. J. 2011, 21, 152–177. [Google Scholar] [CrossRef]
- Van Oerle, S.; Mahr, D.; Lievens, A. Coordinating online health communities for cognitive and affective value creation. J. Serv. Manag. 2016, 27, 481–506. [Google Scholar] [CrossRef]
- McColl-Kennedy, J.R.; Vargo, S.L.; Dagger, T.S.; Sweeney, J.C.; van Kasteren, Y. Health Care Customer Value Cocreation Practice Styles. J. Serv. Res. 2012, 12, 370–389. [Google Scholar] [CrossRef]
- Casali, G.L.; Perano, M.; Moretta Tartaglione, A.; Zolin, R. How Business Idea Fit Affects Sustainability and Creates Opportunities for Value Co-Creation in Nascent Firms. Sustainability 2018, 10, 189. [Google Scholar] [CrossRef]
- Aslani, P. Patient empowerment and informed decision-making. Int. J. Pharm. Pract. 2013, 21, 347–348. [Google Scholar] [CrossRef] [PubMed]
- Bulsara, C.; Styles, I.; Ward, A.M.; Bulsara, M. The psychometrics of developing the patient empowerment scale. J. Psychosoc. Oncol. 2006, 24, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Shearer, N.; Cisar, N.; Greenberg, E.A. A telephone-delivered empowerment intervention with patients diagnosed with heart failure. Hearung 2007, 36, 159–169. [Google Scholar] [CrossRef] [PubMed]
- Boudioni, M.; McLaren, S.M.; Lister, G. Cross-national diagnostic analysis of patient empowerment in England and Greece. Int. J. Caring Sci. 2012, 5, 246–264. [Google Scholar]
- Wentzer, H.S.; Bygholm, A. Narratives of empowerment and compliance: Studies of communication in online patient support groups. Int. J. Med. Inform. 2013, 82, 386–394. [Google Scholar] [CrossRef] [PubMed]
- Jerofke, T.A. Concept analysis of empowerment from survivor and nurse perspectives within the context of cancer survivorship. Res. Theory Nurs. Pract. 2013, 27, 157–172. [Google Scholar] [CrossRef] [PubMed]
- Ünver, Ö.; Atzori, W. Document D3.2—Questionnaire for Patient Empowerment Measurement Version 1.0; ICT PSP—Empowering Patients: Bruxelles, Belgium, 2013. [Google Scholar]
- Sheridan, S.L. Shared decision making about screening and chemoprevention: A suggested approach from the U.S. preventive service task force. Am. J. Prev. Med. 2004, 26, 56–66. [Google Scholar] [CrossRef] [PubMed]
- Aghili, R.; Khamseh, M.E.; Malek, M.; Banikarimi, A.S.; Baradaran, H.R.; Ebrahim Valojerdi, A. Development and validation of diabetes empowerment questionnaire in Iranian people with type 2 diabetes. Int. Nurs. Rev. 2013, 60, 267–273. [Google Scholar] [CrossRef] [PubMed]
- Schulz, P.J.; Nakamoto, K. Patient behavior and the benefits of artificial intelligence: The perils of “dangerous” literacy and illusory patient empowerment. Patient Educ. Couns. 2013, 92, 223–228. [Google Scholar] [CrossRef] [PubMed]
- Camerini, A.L.; Schulz, P.J. Health literacy and patient empowerment: Separating con-joined twins in the context of chronic low back pain. PLoS ONE 2015, 10, e0118032. [Google Scholar] [CrossRef] [PubMed]
- Eyüboğlu, E.; Schulz, P.J. Do health literacy and patient empowerment affect self-care behaviour? A survey study among Turkish patients with diabetes. BMJ Open 2016, 6, e010186. [Google Scholar] [CrossRef] [PubMed]
- Porr, C.; Drummond, J.; Richter, S. Health literacy as an empowerment tool for low-income mothers. Fam. Community Health 2006, 29, 328–335. [Google Scholar] [CrossRef] [PubMed]
- McGuckin, M.; Govednik, J. Patient empowerment begins with knowledge: Consumer perceptions and knowledge sources for hand hygiene compliance rates. Am. J. Infect. Control 2014, 42, 1106–1108. [Google Scholar] [CrossRef] [PubMed]
- Edwards, M.; Wood, F.; Davies, M.; Edwards, A. The development of health literacy in patients with a long-term health condition: The health literacy pathway model. BMC Public Health 2012, 12, 130. [Google Scholar] [CrossRef] [PubMed]
- Ishikawa, H.; Kiuchi, T. Health literacy and health communication. Biopsychosoc. Med. 2010, 4, 18. [Google Scholar] [CrossRef] [PubMed]
- Stiles, E. Promoting health literacy in patients with diabetes. Nurs. Stand. 2011, 26, 35–40. [Google Scholar] [CrossRef] [PubMed]
- Johnson, M.O.; Rose, C.D.; Dilworth, S.E.; Neilands, T.B. Advances in the conceptualization and measurement of health care development and validation of the health care empowerment inventory. PLoS ONE 2012, 7, e45692. [Google Scholar] [CrossRef] [PubMed]
- Topac, V.; Stoicu-Tivadar, V. Patient empowerment by increasing the understanding of medical language for lay users. Methods Inf. Med. 2013, 52, 454–462. [Google Scholar] [PubMed]
- Smith, S.G.; Curtis, L.M.; Wardle, J.; von Wagner, C.; Wolf, M.S. Skill set or mind set? Associations between health literacy. Patient Activation and Health. PLoS ONE 2013, 8, e74373. [Google Scholar] [CrossRef] [PubMed]
- Heijmans, M.; Waverijn, G.; Rademakers, J.; van der Vaart, R.; Rijkena, M. Functional, communicative and critical health literacy of chronic disease patients and their importance for self-management. Patient Educ. Couns. 2015, 98, 41–48. [Google Scholar] [CrossRef] [PubMed]
- Erlen, J.A. Functional health illiteracy. Ethical concerns. Orthop. Nurs. 2004, 23, 150–153. [Google Scholar] [CrossRef] [PubMed]
- Palumbo, R. The Bright Side and the Dark Side of Patient Empowerment. Co-Creation and Co-Destruction of Value in the Healthcare Environment; Springer: New York, NY, USA, 2017. [Google Scholar]
- Wang, R.H.; Hsu, H.C.; Lee, Y.J.; Shin, S.J.; Lin, K.D.; An, L.W. Patient empowerment interacts with health literacy to associate with subsequent self-management behaviors in patients with type 2 diabetes: A prospective study in Taiwan. Patient Educ. Couns. 2016, 99, 1626–1631. [Google Scholar] [CrossRef] [PubMed]
- Shin, K.S.; Lee, E.H. Relationships of health literacy to self-care behaviors in people with diabetes aged 60 and above: Empowerment as a mediator. J. Adv. Nurs. 2018, 74, 2363–2372. [Google Scholar] [CrossRef] [PubMed]
- Halbach, S.M.; Ernstmann, N.; Kowalski, C.; Pfaff, H.; Pförtner, T.K.; Wesselmannc, S. Unmet information needs and limited health literacy in newly diagnosed breast cancer patients over the course of cancer treatment. Patient Educ. Couns. 2016, 99, 1511–1518. [Google Scholar] [CrossRef] [PubMed]
- Gazmararian, J.A.; Williams, M.V.; Peel, J.; Baker, D.W. Health literacy and knowledge of chronic disease. Patient Educ. Couns. 2003, 51, 267–275. [Google Scholar] [CrossRef]
- Federman, A.D.; Wisnivesky, J.P.; Wolf, M.S.; Leventhal, H.; Halm, E.A. Inadequate health literacy is associated with suboptimal health beliefs in older asthmatics. J. Asthma 2010, 47, 620–626. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.C.; Boren, D.; Solem, S.L. The Kim Alliance Scale: Development and preliminary testing. Clin. Nurs. Res. 2001, 10, 314–331. [Google Scholar] [CrossRef] [PubMed]
- Palumbo, R.; Annarumma, C.; Adinolfi, P.; Musella, M. The missing link to patient engagement in Italy. The role of health literacy in enabling patients. J. Health Organ. Manag. 2016, 30, 1183–1203. [Google Scholar] [CrossRef] [PubMed]
- Mancuso, C.A.; Rincon, M. Asthma patients’ assessments of health care and medical decision making: The role of health care. J. Asthma 2006, 43, 41–44. [Google Scholar] [CrossRef] [PubMed]
- McCaffery, K.J.; Holmes-Rovner, M.; Smith, S.K.; Rovner, D.; Nutbeam, D.; Clayman, M.L. Addressing health literacy in patient decision aids. BMC Med. Inform. Decis. 2013, 13, 10–23. [Google Scholar] [CrossRef] [PubMed]
- Saviano, M.; Bassano, C.; Calabrese, M. A VSA-SS Approach to Healthcare Service System. The Triple Target of Effectiveness, Efficiency and Sustainability. Serv. Sci. 2010, 2, 41–61. [Google Scholar] [CrossRef]
- Ippolito, A.; Zoccoli, P. Theoretical Contribution to Develop the Classical BSC to Health Care Needs. Int. J. Healthc. Manag. 2013, 6, 37–44. [Google Scholar] [CrossRef]
- Adinolfi, P.; Starace, F.; Palumbo, R. Health Outcomes and Patient Empowerment: The Case of Health Budgets in Italy. J. Health Manag. 2016, 18, 117–133. [Google Scholar] [CrossRef]
- Powers, T.L.; Bendall, D. Improving Health Outcomes Through Patient Empowerment. J. Hosp. Mark. Public Relat. 2004, 15, 45–59. [Google Scholar] [CrossRef]
- Zainuddin, N.; Russell-Bennett, R.; Previte, J. The value of health and wellbeing: An empirical model of value creation in social marketing. Eur. J. Mark. 2013, 47, 1504–1524. [Google Scholar] [CrossRef]
- Osei-Frimpong, K. Examining the effects of patient characteristics and prior value needs on the patient-doctor encounter process in healthcare service delivery. Int. J. Pharm. Healthc. Mark. 2006, 10, 192–213. [Google Scholar] [CrossRef]
- Loane, S.S.; Webster, C.M. Consumer-to-consumer value within social networks. Mark. Rev. 2014, 14, 447–462. [Google Scholar] [CrossRef]
- Buranarach, M.; Thatphithakkul, N.; Kawtrakul, A.; Wongrochananan, S.; Kulnawan, N.; Jiamjarasrangsi, W. Development of service systems to support diabetes patient self-management using a personalized service framework. In Proceedings of the 2011 Annual SRII Global Conference, San Jose, CA, USA, 29 March–2 April 2011; pp. 363–370. [Google Scholar]
- McColl-Kennedy, J.R.; Vargo, S.L.; Dagger, T.S.; Sweeney, J.C. Customers as Resource Integrators: Styles of Customer Co-creation. In Service Science, S-D Logic and Network Theory; Gummesson, E., Mele, C., Polese, F., Eds.; Giannini Editore: Napoli, Italy, 2009. [Google Scholar]
- Lusch, R.F.; Vargo, S.L. Service-dominant logic: Reactions, reflections and refinements. Mark. Theory 2006, 6, 281–288. [Google Scholar] [CrossRef]
- Bove, L.L.; Pervan, S.J.; Beatty, S.E.; Shiu, E. Service worker role in encouraging customer organizational citizenship behaviors. J. Bus. Res. 2008, 62, 698–705. [Google Scholar] [CrossRef]
- Groth, M. Customers as good soldiers: Examining citizenship behaviors in internet service deliveries. J. Manag. 2005, 31, 7–27. [Google Scholar] [CrossRef]
- Yi, Y.; Gong, T. If employees “go the extra mile”, do customers reciprocate with similar behavior? Psychol. Mark. 2008, 25, 961–986. [Google Scholar] [CrossRef]
- Yi, Y.; Nataraajanb, R.; Gong, T. Customer participation and citizenship behavioural influences on employee performance, satisfaction, commitment, and turnover intention. J. Bus. Res. 2011, 64, 87–95. [Google Scholar] [CrossRef]
- Fumagalli, L.; Radaelli, G.; Emanuele, L.; Bertele’, P.; Masella, C. Patient Empowerment and its neighbours: Clarifying the boundaries and their mutual relationships. Health Policy 2015, 119, 384–394. [Google Scholar] [CrossRef] [PubMed]
- Barr, P.J.; Scholl, I.; Bravo, P.; Faber, M.J.; Elwyn, G.; McAllister, M. Assessment of patient empowerment: A systematic review of measures. PLoS ONE 2015, 10, e0126553. [Google Scholar] [CrossRef] [PubMed]
- Cerezo, P.G.; Juvé-Udina, M.E.; Delgado-Hito, P. Concepts and measures of patient empowerment: A comprehensive review. Revista da Escola de Enfermagem da USP 2016, 50, 664–671. [Google Scholar] [CrossRef] [PubMed]
- Defrère, D.; Hinz, P.M.; Mennesson, B.; Hoffmann, W.F.; Millan-Gabet, R.; Skemer, A.J.; Grenz, P. Nulling data reduction and on-sky performance of the Large Binocular Telescope Interferometer. Astrophys. J. 2016, 824, 66. [Google Scholar] [CrossRef]
- Randall, W.S.; Gravier, M.J.; Prybutok, V.R. Connection, trust, and commitment: Dimensions of co-creation? J. Strateg. Mark. 2011, 19, 3–24. [Google Scholar] [CrossRef]
- Xie, C.; Bagozzi, R.P.; Troye, S.V. Trying to prosume: Toward a theory of consumers as co-creators of value. J. Acad. Mark. Sci. 2008, 36, 109–122. [Google Scholar] [CrossRef]
- Payne, A.F.; Storbacka, K.; Frow, P. Managing the co-creation of valu. J. Acad. Mark. Sci. 2008, 36, 83–96. [Google Scholar] [CrossRef]
- Neghina, C.; Caniëls, M.C.J.; Bloemer, J.M.M.; Van Birgelen, M.J.H. Value co-creation in service interactions: Dimensions and antecedents. Mark. Theory 2014, 10, 1–22. [Google Scholar]
- European Patients Forum. Empowered Patients Are an Asset to Society; Conference Report; European Patients Forum: Brussels, Belgium, 2015. [Google Scholar]
- Elfil, M.; Negida, A. Sampling methods in Clinical Research; an Educational Review. Emergency 2017, 5, e52. [Google Scholar] [PubMed]
- Lloyd, R. Quality Health Care: A Guide to Developing and Using Indicators; Jones & Bartlett Publishers: Burlington, MA, USA, 2004. [Google Scholar]
- Gravetter, F.; Forzano, L. Research Methods for the Behavioral Sciences, 4th ed.; Wadsworth: Belmont, CA, USA, 2012. [Google Scholar]
- Smith, J.; Noble, H. Bias in research. Evid.-Based Nurs. 2014, 17, 100–101. [Google Scholar] [CrossRef] [PubMed]
- Kline, R.B. Principles and Practice of Structural Equation Modelling, 3rd ed.; Guilford Press: New York, NY, USA, 2011. [Google Scholar]
- Hair, J.F.; Ringle, C.M.; Sarstedt, M. PLS-SEM: Indeed a silver bullet. J. Mark. Theory Pract. 2011, 19, 139–151. [Google Scholar] [CrossRef]
- Chin, W.W.; Peterson, R.A.; Brown, S.P. Structural equation modeling in marketing: Some practical reminders. J. Mark. Theory Pract. 2008, 16, 287–298. [Google Scholar] [CrossRef]
- Hooper, D.; Coughlan, J.; Mullen, M.R. Structural equation modelling: Guidelines for determining model fit. Electron. J. Bus. Res. Methods 2008, 6, 53–60. [Google Scholar]
- Bagozzi, R.P.; Yi, Y. Specification, evaluation, and interpretation of structural equation models. J. Acad. Mark. Sci. 2012, 40, 8–34. [Google Scholar] [CrossRef]
- Wheaton, B.; Muthen, B.; Alwin, D.F.; Summers, G. Assessing Reliability and Stability in Panel Models. Sociol. Methodol. 1977, 8, 84–136. [Google Scholar] [CrossRef]
- Tabachnick, B.G.; Fidell, L.S. Using Multivariate Statistics, 5th ed.; Allyn and Bacon: New York, NY, USA, 2007. [Google Scholar]
- Awang, Z. Structural Equation Modeling Using Amos Graphic; UiTM Press: Shah Alam, Malaysia, 2012. [Google Scholar]
- Hu, L.T.; Bentler, P.M. Cutoff Criteria for Fit Indexes in Covariance Structure Analysis: Conventional Criteria Versus New Alternatives. Struct. Equ. Model. 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Steiger, J.H. Understanding the limitations of global fit assessment in structural equation modeling. Personal. Individ. Differ. 2007, 42, 893–898. [Google Scholar] [CrossRef]
- MacCallum, R.C.; Browne, M.W.; Sugawara, H.M. Power analysis and determination of sample size for covariance structure modeling. Psychol. Methods 1996, 1, 130. [Google Scholar] [CrossRef]
- Byrne, B.M. Structural Equation Modeling with LISREL, PRELIS and SIMPLIS: Basic Concepts, Applications and Programming; Lawrence Erlbaum Associates: Mahwah, NJ, USA, 1998. [Google Scholar]
- Diamantopoulos, A.; Siguaw, J.A. Introducing LISREL; Sage Publications: London, UK, 2000. [Google Scholar]
- Chin, W.W. The partial least squares approach to structural equation modeling. Mod. Methods Bus. Res. 1998, 2, 295–336. [Google Scholar]
- Fornell, C.; Larcker, D.F. Evaluating structural equation models with unobservable variables and measurement error. J. Mark. Res. 1981, 18, 39–50. [Google Scholar] [CrossRef]
- Kim, S.C.; Kim, S.; Boren, D. The quality of therapeutic alliance between patient and provider predicts general satisfaction. Mil. Med. 2008, 173, 85–90. [Google Scholar] [CrossRef] [PubMed]
- Wensing, M. Evidence-based patient empowerment. BMJ Qual. Saf. 2000, 9, 200–201. [Google Scholar] [CrossRef]
- Bridges, J.F.P.; Loukanova, S.; Carrera, P. Patient empowerment in health care. In International Encyclopedia of Public Health; Elsevier: San Diego, CA, USA, 2008; pp. 17–28. [Google Scholar]
- Friedman, B.; Wamsley, B.R.; Liebel, D.V.; Saad, Z.B.; Eggert, G.M. Patient satisfaction, empowerment, and health and disability status effects of a disease management-health promotion nurse intervention among Medicare beneficiaries with disabilities. Gerontologist 2009, 49, 778–792. [Google Scholar] [CrossRef] [PubMed]
- Rakhonde, A.K.; Seth, A.; Rakhonde, N.; Chanchlani, R. A prospective study of level of satisfaction among surgical patients in a tertiary care hospital of central India. Int. Surg. J. 2015, 2, 499–504. [Google Scholar] [CrossRef]
- Yeh, M.Y.; Wu, S.C.; Tung, T.H. The relation between patient education, patient empowerment and patient satisfaction: A cross-sectional-comparison study. Appl. Nurs. Res. 2018, 39, 11–17. [Google Scholar] [CrossRef] [PubMed]
- Prakash, B. Patient satisfaction. J. Cutan. Aesthetic Surg. 2010, 3, 151–155. [Google Scholar] [CrossRef] [PubMed]
- Reichheld, F.F. The one number you need to grow. Harv. Bus. Rev. 2003, 81, 46–54. [Google Scholar] [PubMed]
- Prahalad, C.K.; Ramaswamy, V. Co-opting Customer Competence. Harv. Bus. Rev. 2000, 78, 79–87. [Google Scholar]
- Lusch, R.F.; Vargo, S.L.; O’Brien, M. Competing through service: Insights from service-dominant logic. J. Retail. 2007, 83, 5–18. [Google Scholar] [CrossRef]
- Kohler, T.; Fueller, J.; Matzler, K.; Stieger, D. Cocreation in virtual worlds: The design of the user experience. MIS Q. 2011, 35, 773–788. [Google Scholar] [CrossRef]
- Sweeney, J.C.; Danaher, T.S.; McColl-Kennedy, J.R. Customer effort in value cocreation activities improving quality of life and behavioral intentions of health care customers. J. Serv. Res. 2015, 18, 318–335. [Google Scholar] [CrossRef]
- Shaw, G.; Bailey, A.; Williams, A. Aspects of service-dominant logic and its implications for tourism management: Examples from the hotel industry. Tour. Manag. 2011, 32, 207–214. [Google Scholar] [CrossRef]
- Hardyman, W.; Daunt, K.L.; Kitchener, M. Value co-creation through patient engagement in health care: A micro-level approach and research agenda. Public Manag. Rev. 2015, 17, 90–107. [Google Scholar] [CrossRef]
- Britt, T.W.; Castro, C.A.; Adler, A.B. Self-engagement, stressors, and health: A longitudinal study. Personal. Soc. Psychol. Bull. 2005, 31, 1475–1486. [Google Scholar] [CrossRef] [PubMed]
- Bloom, G.; Standing, H.; Lloyd, R. Markets, information asymmetry and health care: Towards new social contracts. Soc. Sci. Med. 2008, 66, 2076–2087. [Google Scholar] [CrossRef] [PubMed]
- Engström, J. Co-Creation in Health Care Service Development—A Diary-Based approach. Linköping Studies in Science and Technology. Ph.D. Thesis, Linköping University, Linköping, Sweden, 2012. [Google Scholar]
- Barile, S.; Saviano, M.; Polese, F. Information asymmetry and co-creation in health care services. Australas. Mark. J. 2014, 22, 205–217. [Google Scholar] [CrossRef]
- Barile, S.; Orecchini, F.; Saviano, M.; Farioli, F. People, technology, and governance for sustainability: The contribution of systems and cyber-systemic thinking. Sustain. Sci. 2018, 13, 1197–1208. [Google Scholar] [CrossRef]
- Caputo, F. Approccio Sistemico e Co-Creazione di Valore in Sanità; Edizioni Nuova Cultura: Rome, Italy, 2018. [Google Scholar]
- Faulkner, M. A measure of patient empowerment in hospital environments catering for older people. J. Adv. Nurs. 2001, 34, 676–686. [Google Scholar] [CrossRef] [PubMed]
- Shiu, A.T.; Wong, R.Y.; Thompson, D.R. Development of a reliable and valid Chinese version of the diabetes empowerment scale. Diabetes Care 2003, 26, 2817–2821. [Google Scholar] [CrossRef] [PubMed]
- Tol, A.; Sharifirad, G.R.; Pourreza, A.G.; Rahimi, A.; Shojaeezadeh, D.; Mohrajeritehrani, M.R.; Alhani, F. Development of a valid and reliable diabetes empowerment scale: An Iranian version. Iran. Red. Crescent Med. J. 2012, 14, 305–308. [Google Scholar] [PubMed]
- Leksell, J.; Funnell, M.; Sandberg, G.; Smide, B.; Wiklund, G.; Wikblad, K. Psychometric properties of the Swedish Diabetes Empowerment Scale. Scand. J. Caring Sci. 2007, 21, 247–252. [Google Scholar] [CrossRef] [PubMed]
- Chen, M.F.; Wang, R.H.; Cheng, C.P.; Chin, C.C.; Stocker, J.; Tang, S.M.; Chen, S.W. Diabetes Empowerment Process Scale: Development and psychometric testing of the Chinese version. J. Adv. Nurs. 2011, 67, 204–214. [Google Scholar] [CrossRef] [PubMed]
- Arvidsson, S.; Bergman, S.; Arvidsson, B.; Fridlund, B.; Tingstrom, P. Psychometric properties of the Swedish Rheumatic Disease Empowerment Scale, SWE-RES-23. Musculoskelet. Care 2012, 10, 101–109. [Google Scholar] [CrossRef] [PubMed]
- Hansson, L.; Bjorkman, T. Empowerment in people with a mental illness: Reliability and validity of the Swedish version of an empowerment scale. Scand. J. Caring Sci. 2005, 19, 32–38. [Google Scholar] [CrossRef] [PubMed]
- Yamada, S.; Suzuki, K. Application of Empowerment Scale to patients with schizophrenia: Japanese experience. Psychiatry Clin. Neurosci. 2007, 61, 594–601. [Google Scholar] [CrossRef] [PubMed]
- Corrigan, P.W.; Faber, D.; Rashid, F.; Leary, M. The construct validity of empowerment among consumers of mental health services. Schizophr. Res. 1999, 38, 77–84. [Google Scholar] [CrossRef]
| PE Dimension. | Value for Organizations | Value for the Community |
|---|---|---|
| Health literacy |
|
|
| Patient participation |
|
|
| Patient control |
|
|
| Communication with healthcare professionals |
|
|
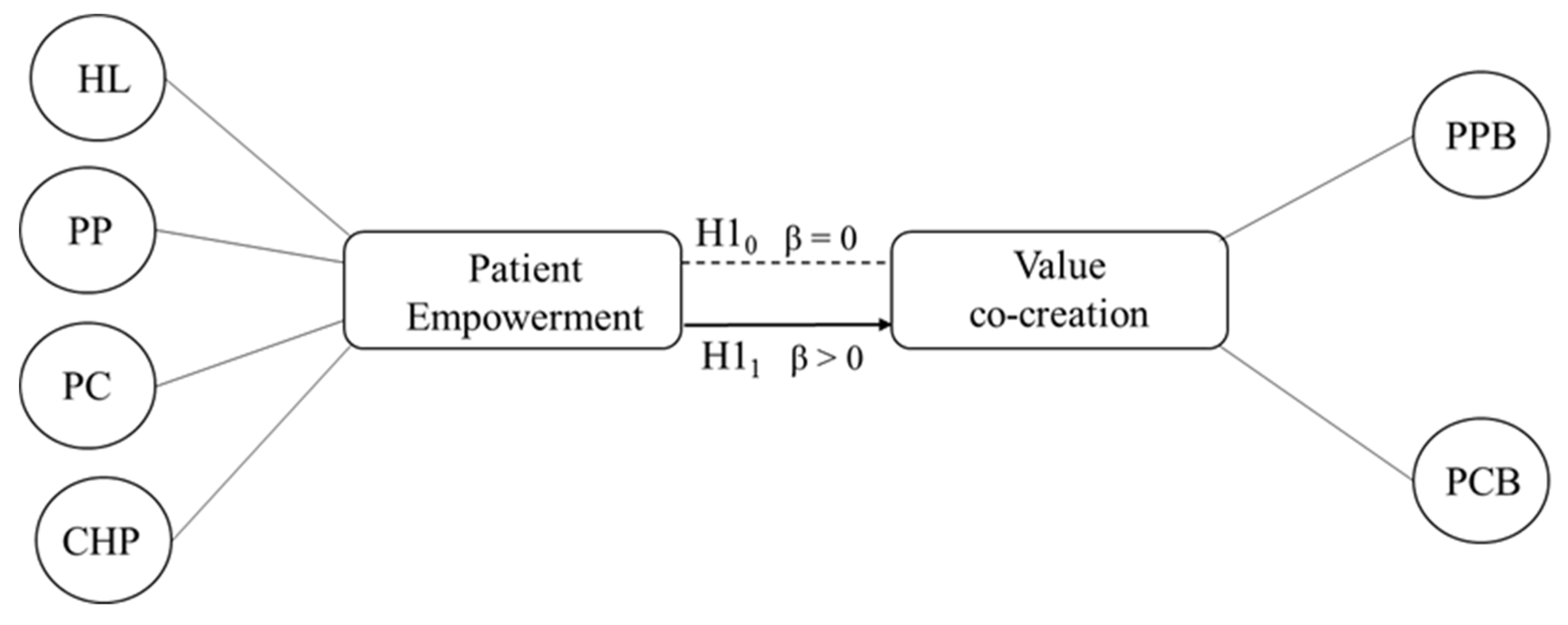
| Main Constructs | Scales | Items | Sources |
|---|---|---|---|
| Patient empowerment | Health Literacy (HL) | 5 | [72] |
| Patient Participation (PP) | 3 | [26,60] | |
| Patient Control (PC) | 4 | [20,21] | |
| Communication with Healthcare Professionals (CHP) | 10 | [25] | |
| Value co-creation | Patient Participation Behavior (PPB) | 10 | [40] |
| Patient Citizenship Behavior (PCB) | 5 |
| Variable | n (%) |
|---|---|
| Age | |
| 18–30 | 33 (13.2%) |
| 31–50 | 86 (34.4%) |
| 51–70 | 101 (40.4%) |
| >70 | 30 (12.0%) |
| Levels of education | |
| Primary education | 29 (11.6%) |
| Lower secondary education | 49 (19.6%) |
| Upper secondary education | 82 (32.8%) |
| First stage of tertiary education | 55 (22.0%) |
| Second stage of tertiary education | 35 (14.0%) |
| Chronic diseases * | |
| Diabetes | 48 (19.2%) |
| Hypertension | 35 (14.0%) |
| Cardiac decompensation/cardiovascular diseases | 50 (20.0%) |
| Arthrosis | 28 (11.2%) |
| Arthritis | 25 (10.0%) |
| Muscle-degenerative diseases | 21 (8.4%) |
| Chronic respiratory diseases/COPD | 20 (8.0%) |
| Others | 23 (9.2%) |
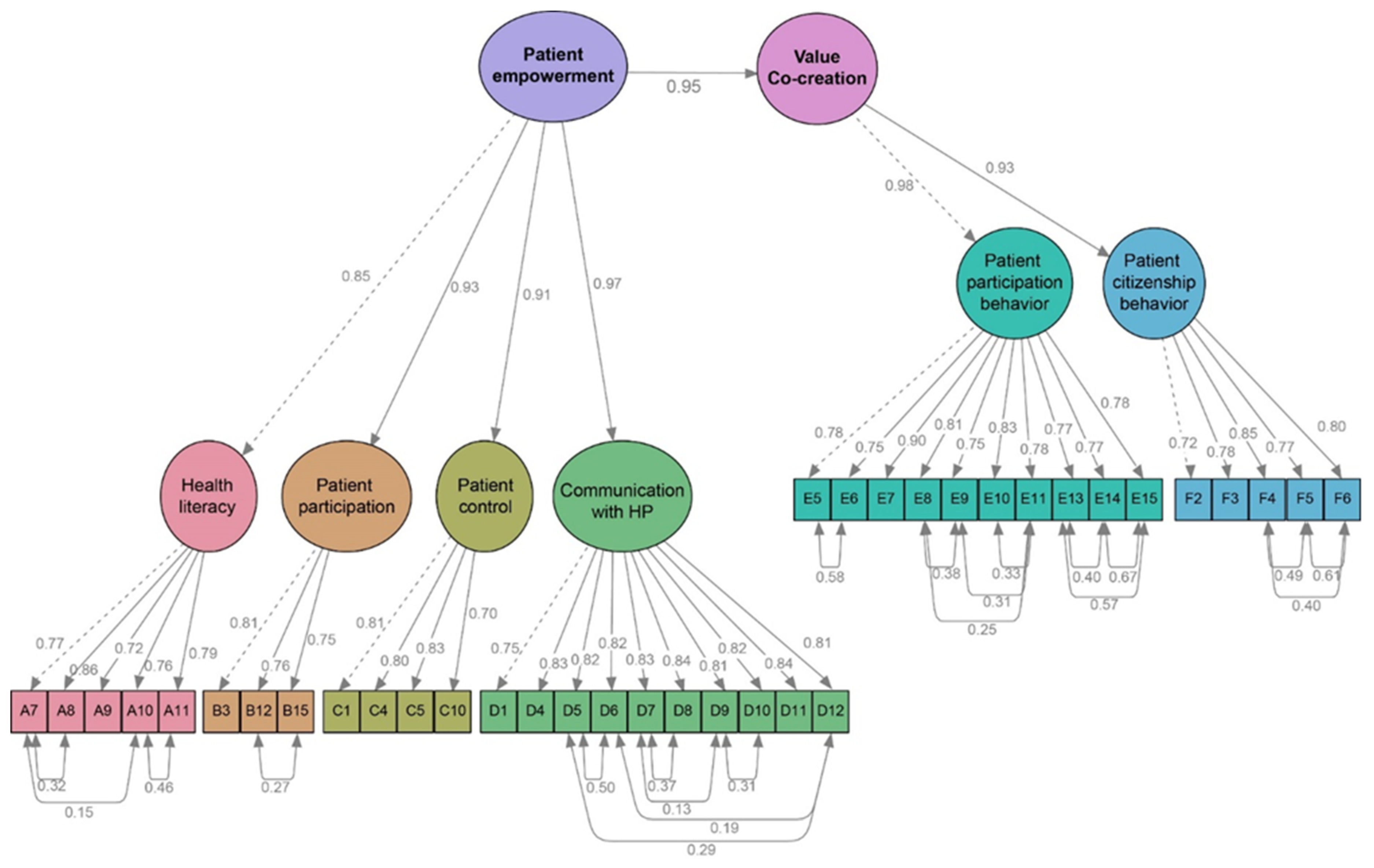
| Construct | Item | Composite Reliability | Factor loading |
|---|---|---|---|
| Second-order construct | |||
| Patient empowerment | HL | - | 0.85 |
| PP | 10.901 | 0.928 | |
| PC | 10.797 | 0.905 | |
| CHP | 10.61 | 0.964 | |
| Value co-creation | PPB | - | 0.98 |
| PCB | 10.989 | 0.931 | |
| First-order constructs | |||
| HL | I collect additional information on my disease from various sources | - | 0.771 |
| I select the most relevant information for my specific case | 16.954 | 0.859 | |
| I understand the information obtained | 11.334 | 0.723 | |
| I ensure that the information obtained is appropriate for my disease | 12.784 | 0.759 | |
| I check the validity, reliability and credibility of the information obtained | 12.346 | 0.787 | |
| PP | I look for information about possible treatment alternatives | 0.815 | |
| I talk to my doctor if I change idea about my treatment | 12.736 | 0.756 | |
| When treatment goals are not met, I discuss any remedies with my doctor | 12.552 | 0.748 | |
| PC | I am committed to keeping my health status as best I can | - | 0.815 |
| I recognize when my lifestyle is worsening my health | 14.256 | 0.802 | |
| I take the commitment to my treatment seriously | 14.863 | 0.827 | |
| I maintain lifestyle changes that are necessary for my health | 11.848 | 0.697 | |
| CHP | I always express my opinion to professionals | 0.751 | |
| I provide all the information my doctors need | 13.784 | 0.826 | |
| I ask all the questions necessary to get the answers I need | 13.574 | 0.816 | |
| I ask for further explanation of what I do not understand | 13.696 | 0.822 | |
| I describe my symptoms in detail | 13.794 | 0.827 | |
| I describe in detail my clinical history and allergies | 13.964 | 0.835 | |
| I am honest about my habits and lifestyle even when they are damaging to health | 13.374 | 0.805 | |
| I admit when I do not follow the directions or the treatment as prescribed | 13.633 | 0.818 | |
| I can easily dialogue with professionals | 14.102 | 0.842 | |
| I always ask for additional information | 13.421 | 0.808 | |
| PPB | I gave the professional proper information | - | 0.781 |
| I provided necessary information so that the professional could perform his or her duties | 19.695 | 0.748 | |
| I answered all the professional’s service-related questions | 16.268 | 0.899 | |
| I performed all the tasks that are required | 14.088 | 0.807 | |
| I adequately completed all the expected behaviors | 12.932 | 0.755 | |
| I behaved responsibly towards health professionals | 14.73 | 0.835 | |
| I followed the professional’s directives or orders | 13.526 | 0.783 | |
| I was friendly to the professional | 13.298 | 0.771 | |
| I was kind to the professional | 13.194 | 0.767 | |
| I was polite to the professional | 13.478 | 0.779 | |
| PCB | When I receive good service from the professional, I comment about it | - | 0.716 |
| When I experience a problem, I let the professional know about it | 11.787 | 0.784 | |
| I said positive things about the service and the professionals to others | 12.687 | 0.85 | |
| I recommended the service and the professionals to others | 11.444 | 0.769 | |
| I encouraged friends and relatives to use the same service | 11.855 | 0.796 | |
| Measure | HL | PP | PC | CHP | PPB | PCB | AVE | Composite Reliability |
|---|---|---|---|---|---|---|---|---|
| HL | 1.00 | 0.61 | 0.886 | |||||
| PP | 0.676 | 1.00 | 0.598 | 0.816 | ||||
| PC | 0.677 | 0.744 | 1.00 | 0.619 | 0.866 | |||
| CHP | 0.712 | 0.768 | 0.763 | 1.00 | 0.664 | 0.951 | ||
| PPB | 0.686 | 0.663 | 0.762 | 0.840 | 1.00 | 0.629 | 0.944 | |
| PCB | 0.621 | 0.655 | 0.664 | 0.761 | 0.803 | 1.00 | 0.614 | 0.888 |
| Unst. Coeff. | SE | Std. Coeff. | |
|---|---|---|---|
| Structural effects | |||
| Patient empowerment → Value Co-creation | 0.95 ** | 0.092 | 0.950 |
| Model fit | |||
| χ2 | 1334.56, df = 601, p < 0.01 | ||
| RMSEA | 0.069 | ||
| CFI | 0.921 | ||
| SRMR | 0.04 | ||
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Russo, G.; Moretta Tartaglione, A.; Cavacece, Y. Empowering Patients to Co-Create a Sustainable Healthcare Value. Sustainability 2019, 11, 1315. https://doi.org/10.3390/su11051315
Russo G, Moretta Tartaglione A, Cavacece Y. Empowering Patients to Co-Create a Sustainable Healthcare Value. Sustainability. 2019; 11(5):1315. https://doi.org/10.3390/su11051315
Chicago/Turabian StyleRusso, Giuseppe, Andrea Moretta Tartaglione, and Ylenia Cavacece. 2019. "Empowering Patients to Co-Create a Sustainable Healthcare Value" Sustainability 11, no. 5: 1315. https://doi.org/10.3390/su11051315
APA StyleRusso, G., Moretta Tartaglione, A., & Cavacece, Y. (2019). Empowering Patients to Co-Create a Sustainable Healthcare Value. Sustainability, 11(5), 1315. https://doi.org/10.3390/su11051315




