Anesthesia Medication’s Impacts on Inflammatory and Neuroendocrine Immune Response in Patients Undergoing Digestive Endoscopy
Abstract
1. Introduction
2. Materials and Methods
- Collection of the patients’ data
- Inclusion and exclusion criteria
- Anesthesia methods
2.1. Blood Collection
2.2. Immunological Determinations of Serum Markers
2.3. Statistic Methods
3. Results
3.1. Concentrations of Serum Catecholamines and Cytokines
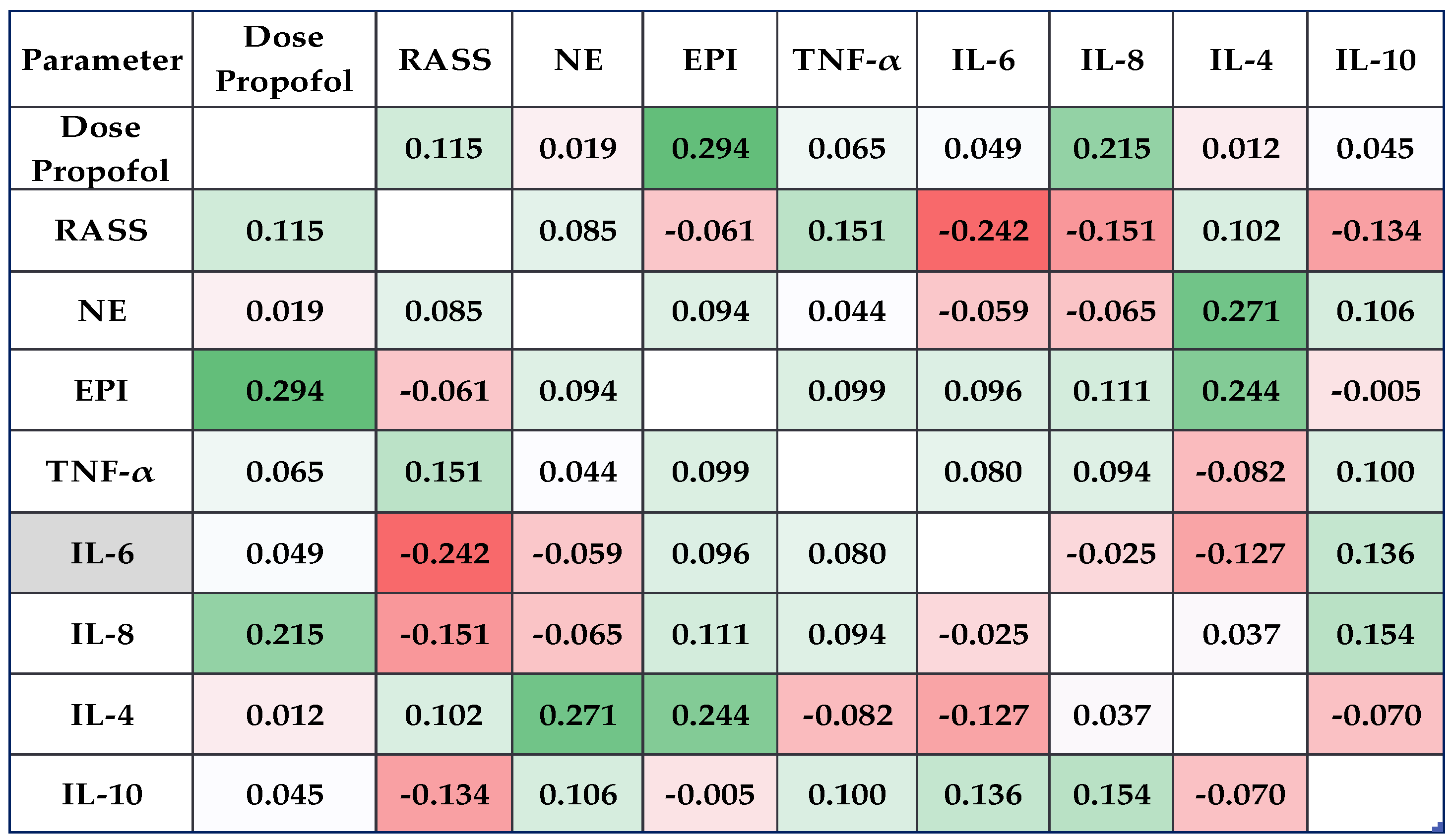
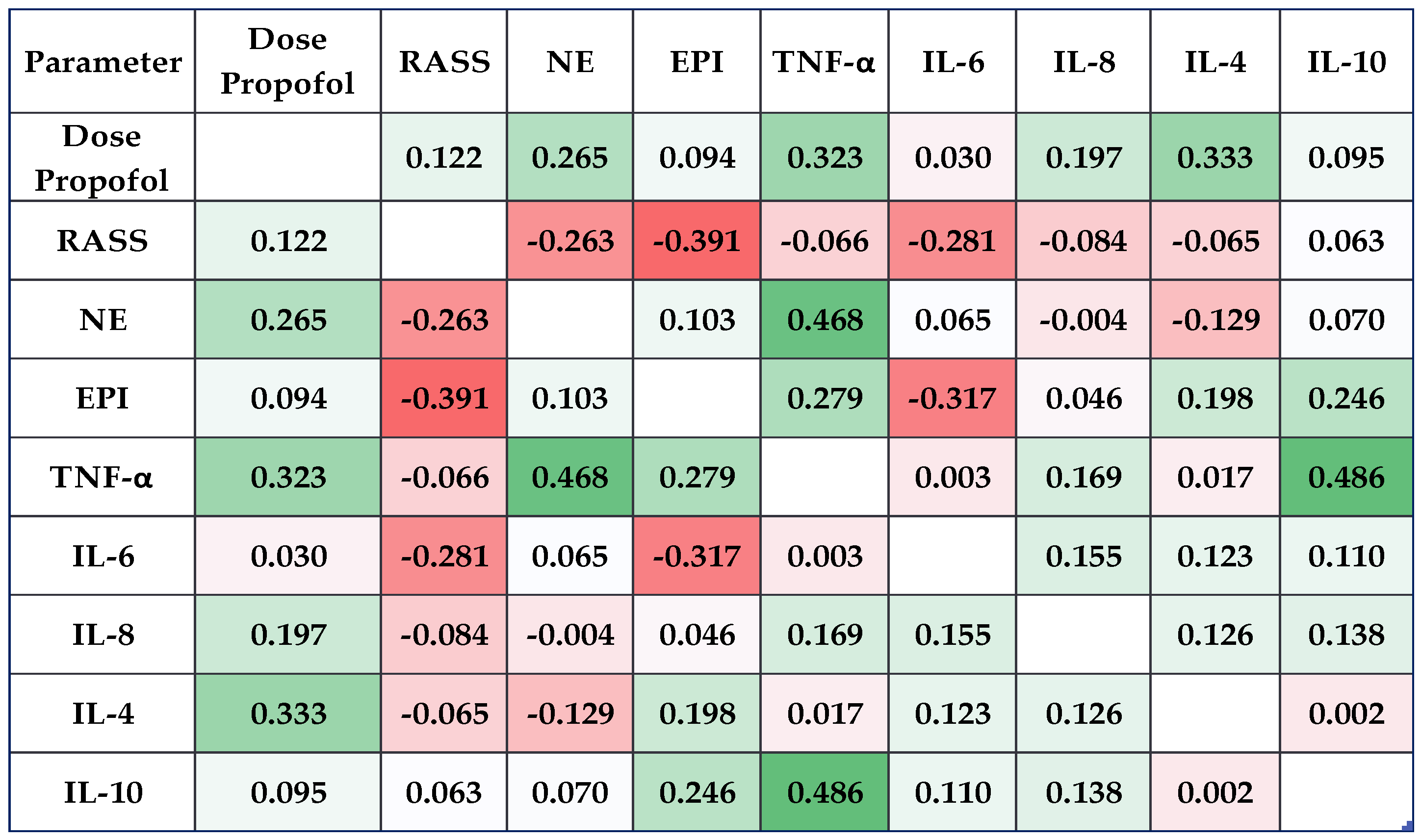
3.2. Catecholamine and Cytokine Levels Correlated Much Better with the Dose of Propofol in L2
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Banihashem, N.; Alijanpour, E.; Basirat, M.; Shokri Shirvany, J.; Kashifard, M.; Taheri HSavadkohi, S.; Hosseini, V.; Solimanian, S.S. Sedation with etomidate-fentanyl versus propofol-fentanyl in colonoscopies: A prospective randomized study. Casp. J. Intern. Med. 2015, 6, 15–19. [Google Scholar]
- Dong, L.X. Effect of etomidate combined with propofol on stress and inflammatory response in painless gastrointestinal endoscopy. J. Hainan Med. Univ. 2017, 23, 144–147. [Google Scholar]
- Kavousi, E.; Shariefnia, H.R.; Pourfakhr, P.; Khajavi, M.; Behseresht, A. Dexmedetomidine versus Propofol in Combination with Fentanyl for Sedation-Analgesia in Colonoscopy Procedures: A Randomized Prospective Study. Middle East. J. Dig. Dis. 2021, 13, 328–332. [Google Scholar] [CrossRef]
- Das Neves, J.F.; das Neves Araújo, M.M.; de Paiva Araújo, F.; Ferreira, C.M.; Duarte, F.B.; Pace, F.H.; Ornellas, L.C.; Baron, T.H.; Ferreira, L.E. Colonoscopy sedation: Clinical trial comparing propofol and fentanyl with or without midazolam. Braz. J. Anesthesiol. 2016, 66, 231–236. [Google Scholar] [CrossRef]
- Saylan, S.; Akbulut, U.E. A comparison of ketamine-midazolam combination and propofol-fentanyl combination on procedure comfort and recovery process in pediatric colonoscopy procedures. Pak. J. Med. Sci. 2021, 37, 483–488. [Google Scholar] [CrossRef]
- Mihaljevic, S. Vasoactive stress hormone (adrenaline, noradrenaline and cortisol) concentration in plasma after administration of low doses of S-(+)-ketamine epidurally. Period. Biol. 2009, 111, 257–261. [Google Scholar]
- Mohammed, O.K.; Alabbassi, M.G.; Aldujaili, A.A.; Shakoor, D.A.; Almoossaw, M.M. Effect of General and Spinal Anesthesia on Some Anti-inflammatory cytokines and cell adhesion molecules of Iraqi Women Undergo Cesarian Section: Comparative Study. J. Pharm. Sci. Res. 2018, 10, 2846–2849. [Google Scholar]
- Liu, G.; Xiong, Y. Analysis of Stress Response and Analgesic Effect of Remazolam Combined with Etomidate in Painless Gastroenteroscopy. Contrast Media Mol. Imaging 2022, 4863682. [Google Scholar] [CrossRef]
- Dossa, F.; Megetto, O.; Yakubu, M.; Zhang, D.D.Q.; Baxter, N.N. Sedation practices for routine gastrointestinal endoscopy: A systematic review of recommendations. BMC Gastroenterol. 2021, 21, 22. [Google Scholar] [CrossRef]
- Dong, W.X. Effect of remifentanil combined with etomidate on systemic stress reaction during painless fiberoptic bronhoscopy. J. Hainan Med. Univ. 2017, 23, 142–145. [Google Scholar]
- Skiljic, S.; Budrovac, D.; Cicvaric, A.; Neskovic, N.; Kvolik, S. Advances in Analgosedation and Periprocedural Care for Gastrointestinal Endoscopy. Life 2023, 13, 473. [Google Scholar] [CrossRef]
- Mazoti, M.A.; Braz, M.G.; de Assis Golim, M.; Braz, L.G.; Dias, N.H.; Salvadori, D.M.; Braz, J.R.; Fecchio, D. Comparison of inflammatory cytokine profiles in plasma of patients undergoing otorhinological surgery with propofol or isoflurane anesthesia. Inflamm. Res. 2013, 62, 879–885. [Google Scholar] [CrossRef]
- Ramani, T.; Auletta, C.S.; Weinstock, D.; Mounho-Zamora, B.; Ryan, P.C.; Salcedo, T.W.; Bannish, G. Cytokines: The Good, the Bad, and the Deadly. Int. J. Toxicol. 2015, 34, 355–365. [Google Scholar] [CrossRef]
- Lin, J.X.; Leonard, W.J. Fine-Tuning Cytokine Signals. Annu. Rev. Immunol. 2019, 37, 295–324. [Google Scholar] [CrossRef]
- Kany, S.; Vollrath, J.T.; Relja, B. Cytokines in Inflammatory Disease. Int. J. Mol. Sci. 2019, 20, 6008. [Google Scholar] [CrossRef]
- Paravati, S.; Rosani, A.; Warrington, S.J. Physiology, Catecholamines; StatPearls Publishing: Treasure Island, FL, USA, 2022; Available online: https://www.ncbi.nlm.nih.gov/books/NBK507716/ (accessed on 11 December 2023).
- Andreis, D.T.; Singer, M. Catecholamines for inflammatory shock: A Jekyll-and-Hyde conundrum. Intensive Care Med. 2016, 42, 1387–1397. [Google Scholar] [CrossRef]
- Boyanova, L. Stress hormone epinephrine (adrenaline) and norepinephrine (noradrenaline) effects on the anaerobic bacteria. Anaerobe 2017, 44, 13–19. [Google Scholar] [CrossRef]
- Lymperopoulos, A.; Rengo, G.; Zincarelli, C.; Soltys, S.; Koch, W.J. Modulation of adrenal catecholamine secretion by in vivo gene transfer and manipulation of G protein-coupled receptor kinase-2 activity. Mol. Ther. 2008, 16, 302–307. [Google Scholar] [CrossRef]
- Geginat, J.; Larghi, P.; Paroni, M.; Nizzoli, G.; Penatti, A.; Pagani, M.; Gagliani, N.; Meroni, P.; Abrignani, S.; Flavell, R.A. The light and the dark sides of Interleukin-10 in immune-mediated diseases and cancer. Cytokine Growth Factor Rev. 2016, 30, 87–93. [Google Scholar] [CrossRef]
- Hsing, C.H.; Wang, J.J. Clinical implication of perioperative inflammatory cytokine alteration. Acta Anaesthesiol. Taiwan 2015, 53, 23–28. [Google Scholar] [CrossRef] [PubMed]
- Jang, D.I.; Lee, A.H.; Shin, H.Y.; Song, H.R.; Park, J.H.; Kang, T.B.; Lee, S.R.; Yang, S.H. The Role of Tumor Necrosis Factor Alpha (TNF-α) in Autoimmune Disease and Current TNF-α Inhibitors in Therapeutics. Int. J. Mol. Sci. 2021, 22, 2719. [Google Scholar] [CrossRef] [PubMed]
- Markovic-Bozic, J.; Karpe, B.; Potocnik, I.; Jerin, A.; Vranic, A.; Novak-Jankovic, V. Effect of propofol and sevoflurane on the inflammatory response of patients undergoing craniotomy. BMC Anesthesiol. 2016, 16, 18. [Google Scholar] [CrossRef] [PubMed]
- Portmann, K.; Linder, A.; Oelgarth, N.; Eyer, K. Single-cell deep phenotyping of cytokine release unmasks stimulation-specific biological signatures and distinct secretion dynamics. Cell Rep. Methods 2023, 3, 100502. [Google Scholar] [CrossRef]
- Orosz, J.E.; Braz, M.G.; Golim, M.A.; Barreira, M.A.; Fecchio, D.; Braz, L.G.; Braz, J.R. Cytokine profile in patients undergoing minimally invasive surgery with balanced anesthesia. Inflammation 2012, 35, 1807–1813. [Google Scholar] [CrossRef] [PubMed]
- Available online: https://www.asahq.org/standards-and-practice-parameters/statement-on-asa-physical-status-classification-system (accessed on 20 October 2023).
- Sessler, C.N.; Gosnell, M.S.; Grap, M.J.; Brophy, G.M.; O’Neal, P.V.; Keane, K.A.; Tesoro, E.P.; Elswick, R.K. The Richmond Agitation-Sedation Scale: Validity and reliability in adult intensive care unit patients. Am. J. Respir. Crit. Care Med. 2002, 166, 1338–1344. [Google Scholar] [CrossRef] [PubMed]
- Available online: https://www.mdcalc.com/richmond-agitation-sedation-scale-rass (accessed on 10 January 2024).
- Kim, T.K.; Niklewski, P.J.; Martin, J.F.; Obara, S.; Egan, T.D. Enhancing a sedation score to include truly noxious stimulation: The Extended Observer’s Assessment of Alertness and Sedation (EOAA/S). Br. J. Anaesth. 2015, 115, 569–577. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Available online: https://bmcpharmacoltoxicol.biomedcentral.com/articles/10.1186/s40360-023-00642-5/tables/1 (accessed on 3 November 2023).
- Nasef, N.A.; Mehta, S. Role of Inflammation in Pathophysiology of Colonic Disease: An Update. Int. J. Mol. Sci. 2020, 21, 4748. [Google Scholar] [CrossRef] [PubMed]
- Wang, K.; Wu, M.; Xu, J.; Wu, C.; Zhang, B.; Wang, G.; Ma, D. Effects of dexmedetomidine on perioperative stress, inflammation, and immune function: Systematic review and meta-analysis. Br. J Anaesth. 2019, 123, 777–794. [Google Scholar] [CrossRef]
- O’Bryan, L.J.; Atkins, K.J.; Lipszyc, A.; Scott, D.A.; Silbert, B.S.; Evered, L.A. Inflammatory Biomarker Levels After Propofol or Sevoflurane Anesthesia: A Meta-analysis. Anesth. Analg. 2022, 134, 69–81. [Google Scholar] [CrossRef]
- Cusack, B.; Buggy, D.J. Anaesthesia, analgesia, and the surgical stress response. BJA Educ. 2020, 20, 321–328. [Google Scholar] [CrossRef]
- Sandrini, S.; Aldriwesh, M.; Alruways, M.; Freestone, P. Microbial endocrinology: Host-bacteria communication within the gut microbiome. J. Endocrinol. 2015, 225, R21–R34. [Google Scholar] [CrossRef] [PubMed]
- Schwarz, L.A.; Luo, L. Organization of the locus coeruleus-norepinephrine system. Curr. Biol. 2015, 25, R1051–R1056. [Google Scholar] [CrossRef]
- Hussain, L.S.; Reddy, V.; Maani, C.V. Physiology, Noradrenergic Synapse; StatPearls Publishing: Treasure Island, FL, USA, 2023; Available online: https://www.ncbi.nlm.nih.gov/books/NBK540977/ (accessed on 15 November 2023).
- Xie, B.; Goldberg, A.; Shi, L. A comprehensive evaluation of the potential binding poses of fentanyl and its analogs at the µ-opioid receptor. Comput. Struct. Biotechnol. J. 2022, 20, 2309–2321. [Google Scholar] [CrossRef] [PubMed]
- Bosch, D.J.; Meurs, M.V.; Jongman, R.M.; Heeringa, P.; Abdulahad, W.H.; Struys, M.M.R.F. Effects of propofol and dexmedetomidine with and without remifentanil on serum cytokine concentrations in healthy volunteers: A post hoc analysis. Br. J. Anaesth. 2020, 125, 267–274. [Google Scholar] [CrossRef] [PubMed]
- Hsiao, H.T.; Wu, H.; Huang, P.C.; Tsai, Y.C.; Liu, Y.C. The effect of propofol and sevoflurane on antioxidants and proinflammatory cytokines in a porcine ischemia-reperfusion model. Acta Anaesthesiol. Taiwan 2016, 54, 6–10. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Yang, L. Effects of propofol and sevoflurane on blood glucose, hemodynamics, and inflammatory factors of patients with type 2 diabetes mellitus and gastric cancer. Oncol. Lett. 2020, 19, 1187–1194. [Google Scholar] [CrossRef] [PubMed]
- Qiu, Q.; Choi, S.W.; Wong, S.S.; Irwin, M.G.; Cheung, C.W. Effects of intra-operative maintenance of general anaesthesia with propofol on postoperative pain outcomes—A systematic review and meta-analysis. Anaesthesia 2016, 71, 1222–1233. [Google Scholar] [CrossRef] [PubMed]
- Chidambaran, V.; Costandi, A.; D’Mello, A. Propofol: A review of its role in pediatric anesthesia and sedation. CNS Drugs 2015, 29, 543–563. [Google Scholar] [CrossRef]
- Fan, W.; Zhu, X.; Wu, L.; Wu, Z.; Li, D.; Huang, F.; He, H. Propofol: An anesthetic possessing neuroprotective effects. Eur. Rev. Med. Pharmacol. Sci. 2015, 19, 1520–1529. [Google Scholar] [PubMed]
- Cruz, F.F.; Rocco, P.R.; Pelosi, P. Anti-inflammatory properties of anesthetic agents. Crit. Care 2017, 21, 67. [Google Scholar] [CrossRef]
- Chalkias, A.; Spyropoulos, V.; Georgiou, G.; Laou, E.; Koutsovasilis, A.; Pantazopoulos, I.; Kolonia, K.; Vrakas, S.; Papalois, A.; Demeridou, S.; et al. Baseline Values and Kinetics of IL-6, Procalcitonin, and TNF-α in Landrace-Large White Swine Anesthetized with Propofol-Based Total Intravenous Anesthesia. Biomed. Res. Int. 2021, 6672573. [Google Scholar] [CrossRef] [PubMed]
- Kallioinen, M.; Scheinin, A.; Maksimow, M.; Långsjö, J.; Kaisti, K.; Takala, R.; Vahlberg, T.; Valli, K.; Salmi, M.; Scheinin, H.; et al. The influence of dexmedetomidine and propofol on circulating cytokine levels in healthy subjects. BMC Anesthesiol. 2019, 19, 222. [Google Scholar] [CrossRef] [PubMed]
- Hino, H.; Matsuura, T.; Kihara, Y.; Tsujikawa, S.; Mori, T.; Nishikawa, K. Comparison between hemodynamic effects of propofol and thiopental during general anesthesia induction with remifentanil infusion: A double-blind, age-stratified, randomized study. J. Anesth. 2019, 33, 509–515. [Google Scholar] [CrossRef] [PubMed]
- Yao, Y.; Guan, J.; Liu, L.; Fu, B.; Chen, L.; Zheng, X. Discharge readiness after remimazolam versus propofol for colonoscopy: A randomised, double-blind trial. Eur. J. Anaesthesiol. 2022, 39, 911–917. [Google Scholar] [CrossRef] [PubMed]
- Ramsay, M.A.; Newman, K.B.; Jacobson, R.M.; Richardson, C.T.; Rogers, L.; Brown, B.J.; Hein, H.A.; De Vol, E.B.; Daoud, Y.A. Sedation levels during propofol administration for outpatient colonoscopies. Proc. (Bayl. Univ. Med. Cent.) 2014, 27, 12–15. [Google Scholar] [CrossRef] [PubMed]
- Sahinovic, M.M.; Struys, M.M.R.F.; Absalom, A.R. Clinical Pharmacokinetics and Pharmacodynamics of Propofol. Clin. Pharmacokinet. 2018, 57, 1539–1558. [Google Scholar] [CrossRef]
- Yang, X.; Wu, X.; Qin, B.; Wang, Z.; Zhu, X.; Huang, S. Effects of Propofol anesthesia combined with remifentanil on inflammation, stress response and immune function in children undergoing tonsil and adenoid surgery. Cell. Mol. Biol. 2022, 68, 87–93. [Google Scholar] [CrossRef] [PubMed]
- Salmasi, V.; Maheshwari, K.; Yang, D.; Mascha, E.J.; Singh, A.; Sessler, D.I.; Kurz, A. Relationship between Intraoperative Hypotension, Defined by Either Reduction from Baseline or Absolute Thresholds, and Acute Kidney and Myocardial Injury after Noncardiac Surgery: A Retrospective Cohort Analysis. Anesthesiology 2017, 126, 47–65. [Google Scholar] [CrossRef]
- Bick, M.J.; Greisen, P.J.; Morey, K.J.; Antunes, M.S.; La, D.; Sankaran, B.; Reymond, L.; Johnsson, K.; Medford, J.I.; Baker, D. Computational design of environmental sensors for the potent opioid fentanyl. eLife 2017, 6, e28909. [Google Scholar] [CrossRef]
- Benzoni, T.; Cascella, M. Procedural Sedation; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar] [PubMed]
- Turan, A.; Dalton, J.E.; Kasuya, Y.; Akça, O.; Sessler, D.I.; Rauch, S. Correlation between bispectral index, observational sedation scale, and lower esophageal sphincter pressure in volunteers using dexmedetomidine or propofol. Med. Sci. Monit. 2012, 18, CR593–CR596. [Google Scholar] [CrossRef]
- Sachdeva, A.; Jaswal, S.; Walia, H.S.; Batra, Y.K. Correlating the Depth of Sedation Between the Ramsay Sedation Scale and Bispectral Index Using Either Intravenous Midazolam or Intravenous Propofol in Elderly Patients Under Spinal Anaesthesia. Cureus 2023, 15, e50763. [Google Scholar] [CrossRef] [PubMed]
- Rasheed, A.M.; Amirah, M.F.; Abdallah, M.; PJ, P.; Issa, M.; Alharthy, A. Ramsay Sedation Scale and Richmond Agitation Sedation Scale: A Cross-sectional Study. Dimens. Crit. Care Nurs. 2019, 38, 90–95. [Google Scholar] [CrossRef] [PubMed]
- Tapia, R.; López-Herce, J.; Arias, Á.; Del Castillo, J.; Mencía, S. Validity and Reliability of the Richmond Agitation-Sedation Scale in Pediatric Intensive Care Patients: A Multicenter Study. Front. Pediatr. 2022, 9, 795487. [Google Scholar] [CrossRef] [PubMed]
- Medlej, K. Calculated decisions: Richmond Agitation-Sedation Scale (RASS). Emerg. Med. Pract. 2021, 23, CD3–CD4. [Google Scholar] [PubMed]
- Plaschke, K.; Weiskircher, A.; Benner, L.; Klein, B.; Loukanov, T.; Gorenflo, M.; Weigand, M.A.; Rauch, H. Depth of anesthesia by Narcotrend® and postoperative characteristics in children undergoing cardiac surgery under extracorporeal circulation: A retrospective comparison of two anesthetic regimens. Perfusion 2020, 35, 427–435. [Google Scholar] [CrossRef]

| Parameters | L1 (n = 40) | L2 (n = 40) | L3 (n = 40) | |
|---|---|---|---|---|
| Gender, male/female, (n) | 21/19 | 21/19 | 18/22 | |
| Average age (standard deviation) | 56.3 ± 16.7 | 59.2 ± 14.4 | 54.4 ± 15.1 | |
| Area of residence, urban/rural, (n) | 14/26 | 11/29 | 9/31 | |
| ASA I, (n) | 16 | 15 | 20 | |
| ASA II, (n) | 24 | 25 | 20 | |
| Dose of propofol, (mean ± SD) (mg) | - | 272.00 ± 59.25 | 164.50 ± 25.43 | |
| RASS score, (mean ± SD) | - | −3.10 ± 1.20 | −4.90 ± 0.30 | |
| Duration of the endoscopic procedure, (min) (mean ± SD) | 23.10 ± 3.69 | 17.75 ± 2.61 | 15.10 ± 1.94 | |
| Wake-up time, (min) (mean ± SD) | - | 3.30 ± 0.90 | 5.20 ± 1.00 | |
| BMI, (n) | Normal weight | 10 | 16 | 14 |
| Overweight | 13 | 5 | 16 | |
| Obesity | 17 | 19 | 10 | |
| Comorbidities, (n) | Hypertension | 11 | 9 | 12 |
| Diabetes | 7 | 4 | 7 | |
| Digestive cancer | 8 | 3 | 2 | |
| p-Value | |||||||
|---|---|---|---|---|---|---|---|
| EPI (pg/mL) | Student’s t-Test | One-Way ANOVA | |||||
| Lot (n = 40) | T0 | T1 | T2 | T0 vs. T1 | T0 vs. T2 | T1 vs. T2 | |
| L1 | 606.0 ± 189.2 | 898.3 ± 274.0 | 1046.6 ± 261.5 | <0.0001 *** | <0.0001 *** | 0.015 * | <0.0001 *** |
| L2 | 534.3 ± 95.7 | 671.9 ± 119.2 | 465.1 ± 87.6 | <0.0001 *** | 0.001 ** | <0.0001 *** | <0.0001 *** |
| L3 | 446.7 ± 147.9 | 522.2 ± 153.4 | 297.0 ± 115.0 | 0.028 * | <0.0001 *** | <0.0001 *** | <0.0001 *** |
| One-way ANOVA | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L1 vs. L2 (p) | 0.037 * | <0.0001 *** | <0.0001 *** | ||||
| L1 vs. L3 (p) | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L2 vs. L3 (p) | 0.002 ** | <0.0001 *** | <0.0001 *** | ||||
| NE (ng/mL) | |||||||
| L1 | 10.7 ± 1.9 | 12.4 ± 2.4 | 14.2 ± 2.4 | 0.001 ** | <0.0001 *** | 0.001 ** | <0.0001 *** |
| L2 | 9.3 ± 2.1 | 10.8 ± 2.9 | 7.2 ± 1.8 | 0.010 * | <0.0001 *** | <0.0001 *** | 0.004 ** |
| L3 | 9.2 ± 1.4 | 8.7 ± 2.2 | 3.4 ± 1.2 | 0.040 * | <0.0001 *** | <0.0001 *** | <0.0001 *** |
| T0 | T1 | T2 | |||||
| One-way ANOVA | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L1 vs. L2 (p) | 0.004 ** | 0.009 ** | <0.0001 *** | ||||
| L1 vs. L3 (p) | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L2 vs. L3 (p) | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| p-Value | |||||||
|---|---|---|---|---|---|---|---|
| IL-6 (pg/mL) | Student’s t-Test | One-Way ANOVA | |||||
| Lot (n = 40) | T0 | T1 | T2 | T0 vs. T1 | T0 vs. T2 | T1 vs. T2 | |
| L1 | 8.3 ± 3.1 | 13.6 ± 2.9 | 16.4 ± 3.4 | <0.0001 *** | <0.0001 *** | <0.0001 *** | <0.0001 *** |
| L2 | 6.4 ± 1.1 | 8.2 ± 1.5 | 5.1 ± 1.2 | <0.0001 *** | <0.0001 *** | <0.0001 *** | <0.0001 *** |
| L3 | 5.4 ± 1.7 | 6.9 ± 2.6 | 3.1 ± 1.1 | <0.0001 *** | 0.003 ** | <0.0001 *** | <0.0001 *** |
| One-way ANOVA | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L1 vs. L2 (p) | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L1 vs. L3 (p) | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L2 vs. L3 (p) | 0.002 ** | 0.007 ** | <0.0001 *** | ||||
| IL-8 (pg/mL) | |||||||
| L1 | 160.3 ± 40.5 | 243.3 ± 59.5 | 295.4 ± 56.8 | <0.0001 *** | <0.0001 *** | <0.0001 *** | <0.0001 *** |
| L2 | 111.7 ± 23.0 | 138.7 ± 27.3 | 89.7 ± 14.4 | <0.0001 *** | <0.0001 *** | <0.0001 *** | <0.0001 *** |
| L3 | 85.5 ± 36.2 | 119.0 ± 37.6 | 41.2 ± 16.1 | <0.0001 *** | <0.0001 *** | <0.0001 *** | <0.0001 *** |
| T0 | T1 | T2 | |||||
| One-way ANOVA | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L1 vs. L2 (p) | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L1 vs. L3 (p) | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L2 vs. L3 (p) | <0.0001 *** | 0.009 ** | <0.0001 *** | ||||
| TNF-α (pg/mL) | |||||||
| L1 | 20.3 ± 6.7 | 24.2 ± 7.6 | 29.5 ± 8.3 | <0.0001 *** | 0.017 * | <0.0001 *** | 0.004 ** |
| L2 | 15.4 ± 1.9 | 16.5 ± 2.0 | 8.0 ± 1.4 | <0.0001 *** | 0.013 * | <0.0001 *** | <0.0001 *** |
| L3 | 13.9 ± 2.4 | 15.2 ± 2.7 | 3.2 ± 0.6 | <0.0001 *** | 0.021 * | <0.0001 *** | <0.0001 *** |
| T0 | T1 | T2 | |||||
| One-way ANOVA | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L1 vs. L2 (p) | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L1 vs. L3 (p) | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L2 vs. L3 (p) | 0.002 ** | 0.013 * | <0.0001 *** | ||||
| p-Value | |||||||
|---|---|---|---|---|---|---|---|
| IL-4 (pg/mL) | Student’s t-Test | One-Way ANOVA | |||||
| Lot (n = 40) | T0 | T1 | T2 | T0 vs. T1 | T0 vs. T2 | T1 vs. T2 | |
| L1 | 102.8 ± 24.2 | 136.2 ± 26.9 | 154.8 ± 26.7 | <0.0001 *** | 0.019 * | <0.0001 *** | 0.003 ** |
| L2 | 97.1 ± 9.3 | 116.1 ± 22.7 | 77.5 ± 9.8 | <0.0001 *** | <0.0001 *** | <0.0001 *** | <0.0001 *** |
| L3 | 88.8 ± 22.5 | 100.7 ± 26.2 | 42.2 ± 11.4 | <0.0001 *** | 0.032 * | <0.0001 *** | <0.0001 *** |
| One-way ANOVA | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L1 vs. L2 (p) | <0.0001 *** | 0.001 ** | <0.0001 *** | ||||
| L1 vs. L3 (p) | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L2 vs. L3 (p) | 0.037 * | 0.006 ** | <0.0001 *** | ||||
| IL-10 (pg/mL) | |||||||
| L1 | 10.9 ± 2.1 | 12.1 ± 2.2 | 14.1 ± 3.1 | <0.0001 *** | 0.010 * | <0.0001 *** | 0.002 ** |
| L2 | 9.4 ± 1.5 | 10.5 ± 1.8 | 7.2 ± 1.4 | <0.0001 *** | 0.006 ** | <0.0001 *** | <0.0001 *** |
| L3 | 8.7 ± 1.8 | 9.6 ± 1.8 | 5.1 ± 1.5 | <0.0001 *** | 0.021 * | <0.0001 *** | <0.0001 *** |
| One-way ANOVA | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L1 vs. L2 (p) | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L1 vs. L3 (p) | <0.0001 *** | <0.0001 *** | <0.0001 *** | ||||
| L2 vs. L3 (p) | 0.047 * | 0.045 * | <0.0001 *** | ||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Popa-Ion, D.-A.; Boldeanu, L.; Gheonea, D.-I.; Denicu, M.M.; Boldeanu, M.V.; Chiuțu, L.C. Anesthesia Medication’s Impacts on Inflammatory and Neuroendocrine Immune Response in Patients Undergoing Digestive Endoscopy. Clin. Pract. 2024, 14, 1171-1184. https://doi.org/10.3390/clinpract14030093
Popa-Ion D-A, Boldeanu L, Gheonea D-I, Denicu MM, Boldeanu MV, Chiuțu LC. Anesthesia Medication’s Impacts on Inflammatory and Neuroendocrine Immune Response in Patients Undergoing Digestive Endoscopy. Clinics and Practice. 2024; 14(3):1171-1184. https://doi.org/10.3390/clinpract14030093
Chicago/Turabian StylePopa-Ion, Denisa-Ancuța, Lidia Boldeanu, Dan-Ionuț Gheonea, Madalina Maria Denicu, Mihail Virgil Boldeanu, and Luminița Cristina Chiuțu. 2024. "Anesthesia Medication’s Impacts on Inflammatory and Neuroendocrine Immune Response in Patients Undergoing Digestive Endoscopy" Clinics and Practice 14, no. 3: 1171-1184. https://doi.org/10.3390/clinpract14030093
APA StylePopa-Ion, D.-A., Boldeanu, L., Gheonea, D.-I., Denicu, M. M., Boldeanu, M. V., & Chiuțu, L. C. (2024). Anesthesia Medication’s Impacts on Inflammatory and Neuroendocrine Immune Response in Patients Undergoing Digestive Endoscopy. Clinics and Practice, 14(3), 1171-1184. https://doi.org/10.3390/clinpract14030093








