Infusion-Related Reactions Subsequent to Avelumab, Durvalumab, and Atezolizumab Administration: A Retrospective Observational Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Patients
2.2. Assessments
2.3. Anti-PD-L1 Antibody Administration
2.4. IRRs
2.5. Prophylaxis
2.6. Statical Methods
3. Results
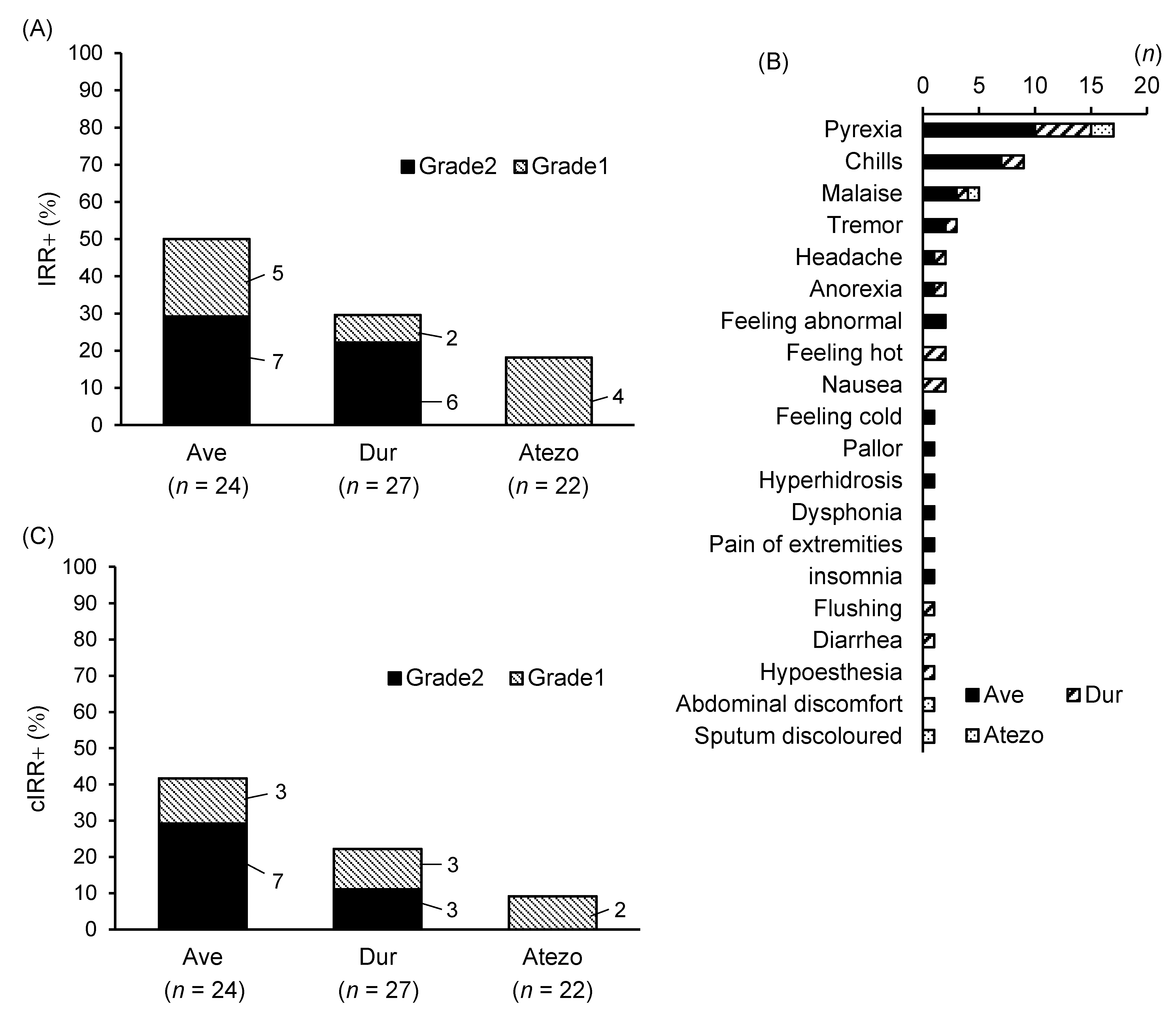
3.1. Comparison of IRRs at the First Infusion
3.2. Exploring Risk Factors for IRR Development
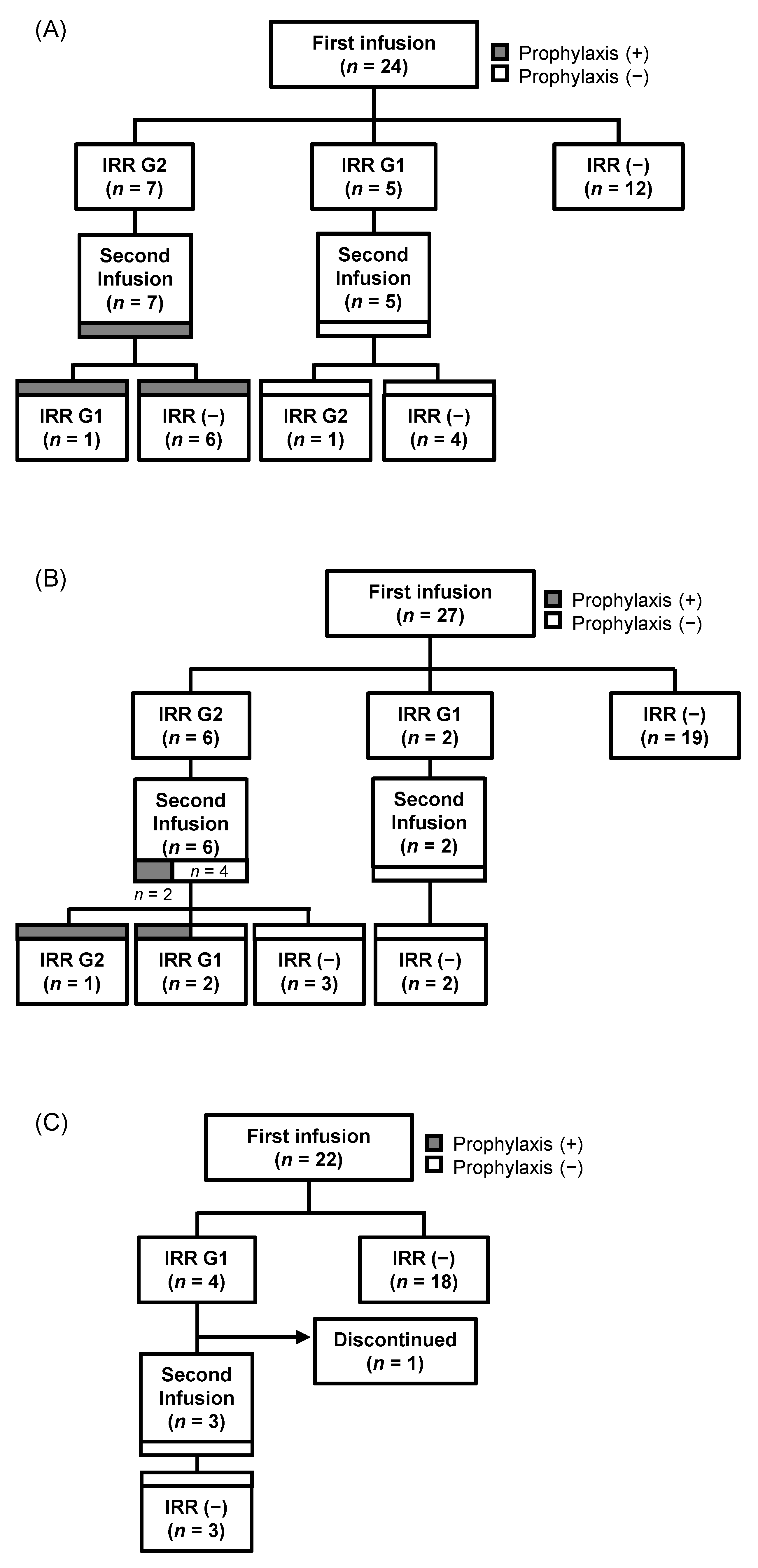
3.3. Comparison of IRRs and Prophylactic Measures at the Second Infusion
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Chen, D.S.; Mellman, I. Oncology meets immunology: The cancer-immunity cycle. Immunity 2013, 39, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Peavy, R.D.; Metcalfe, D.D. Understanding the mechanisms of anaphylaxis. Curr. Opin. Allergy Clin. Immunol. 2008, 8, 310–315. [Google Scholar] [CrossRef] [PubMed]
- Gleich, G.J.; Leiferman, K.M. Anaphylaxis: Implications of monoclonal antibody use in oncology. Oncology 2009, 23, 7–13. [Google Scholar] [PubMed]
- Vultaggio, A.; Castells, M.C. Hypersensitivity reactions to biologic agents. Immunol. Allergy Clin. N. Am. 2014, 34, 615–632, ix. [Google Scholar] [CrossRef] [PubMed]
- Lenz, H.J. Management and preparedness for infusion and hypersensitivity reactions. Oncologist 2007, 12, 601–609. [Google Scholar] [CrossRef] [PubMed]
- Winkler, U.; Jensen, M.; Manzke, O.; Schulz, H.; Diehl, V.; Engert, A. Cytokine-release syndrome in patients with B-cell chronic lymphocytic leukemia and high lymphocyte counts after treatment with an anti-CD20 monoclonal antibody (rituximab, IDEC-C2B8). Blood 1999, 94, 2217–2224. [Google Scholar] [CrossRef] [PubMed]
- Hayama, T.; Miura, K.; Uchiike, A.; Nakagawa, M.; Tsutsumi, D.; Sakagami, M.; Yoshida, Y.; Takei, M. A clinical prediction model for infusion-related reactions to rituximab in patients with B cell lymphomas. Int. J. Clin. Pharm. 2017, 39, 380–385. [Google Scholar] [CrossRef] [PubMed]
- Ohata, S.; Takenaka, K.; Sugiyama, D.; Sugimoto, T. Bone Marrow Infiltration Is a Distinctive Risk Factor for Rituximab Infusion-Related Reactions in CD20-Positive B-Cell Non-Hodgkin Lymphoma. Adv. Hematol. 2022, 2022, 3688727. [Google Scholar] [CrossRef] [PubMed]
- Cho, K.M.; Keam, B.; Ha, H.; Kim, M.; Jung, J.W.; Song, W.J.; Kim, T.M.; Jeon, Y.K.; Kang, H.R.; Kim, D.W.; et al. Clinical significance of rituximab infusion-related reaction in diffuse large B-cell lymphoma patients receiving R-CHOP. Korean J. Intern. Med. 2019, 34, 885–893. [Google Scholar] [CrossRef] [PubMed]
- Palumbo, A.; Chanan-Khan, A.; Weisel, K.; Nooka, A.K.; Masszi, T.; Beksac, M.; Spicka, I.; Hungria, V.; Munder, M.; Mateos, M.V.; et al. Daratumumab, Bortezomib, and Dexamethasone for Multiple Myeloma. N. Engl. J. Med. 2016, 375, 754–766. [Google Scholar] [CrossRef] [PubMed]
- Kaufman, H.L.; Russell, J.; Hamid, O.; Bhatia, S.; Terheyden, P.; D’Angelo, S.P.; Shih, K.C.; Lebbe, C.; Linette, G.P.; Milella, M.; et al. Avelumab in patients with chemotherapy-refractory metastatic Merkel cell carcinoma: A multicentre, single-group, open-label, phase 2 trial. Lancet Oncol. 2016, 17, 1374–1385. [Google Scholar] [CrossRef]
- Motzer, R.J.; Penkov, K.; Haanen, J.; Rini, B.; Albiges, L.; Campbell, M.T.; Venugopal, B.; Kollmannsberger, C.; Negrier, S.; Uemura, M.; et al. Avelumab plus Axitinib versus Sunitinib for Advanced Renal-Cell Carcinoma. N. Engl. J. Med. 2019, 380, 1103–1115. [Google Scholar] [CrossRef] [PubMed]
- Powles, T.; Park, S.H.; Voog, E.; Caserta, C.; Valderrama, B.P.; Gurney, H.; Kalofonos, H.; Radulovic, S.; Demey, W.; Ullen, A.; et al. Avelumab Maintenance Therapy for Advanced or Metastatic Urothelial Carcinoma. N. Engl. J. Med. 2020, 383, 1218–1230. [Google Scholar] [CrossRef]
- Antonia, S.J.; Villegas, A.; Daniel, D.; Vicente, D.; Murakami, S.; Hui, R.; Yokoi, T.; Chiappori, A.; Lee, K.H.; de Wit, M.; et al. Durvalumab after Chemoradiotherapy in Stage III Non-Small-Cell Lung Cancer. N. Engl. J. Med. 2017, 377, 1919–1929. [Google Scholar] [CrossRef]
- Herbst, R.S.; Giaccone, G.; de Marinis, F.; Reinmuth, N.; Vergnenegre, A.; Barrios, C.H.; Morise, M.; Felip, E.; Andric, Z.; Geater, S.; et al. Atezolizumab for First-Line Treatment of PD-L1-Selected Patients with NSCLC. N. Engl. J. Med. 2020, 383, 1328–1339. [Google Scholar] [CrossRef] [PubMed]
- Boyerinas, B.; Jochems, C.; Fantini, M.; Heery, C.R.; Gulley, J.L.; Tsang, K.Y.; Schlom, J. Antibody-Dependent Cellular Cytotoxicity Activity of a Novel Anti-PD-L1 Antibody Avelumab (MSB0010718C) on Human Tumor Cells. Cancer Immunol. Res. 2015, 3, 1148–1157. [Google Scholar] [CrossRef] [PubMed]
- Common Terminology Criteria for Adverse Events (CTCAE). Available online: https://ctep.cancer.gov/protocoldevelopment/electronic_applications/ctc.htm#ctc_50 (accessed on 6 December 2023).
- Oganesyan, V.; Gao, C.; Shirinian, L.; Wu, H.; Dall’Acqua, W.F. Structural characterization of a human Fc fragment engineered for lack of effector functions. Acta Crystallogr. D Biol. Crystallogr. 2008, 64, 700–704. [Google Scholar] [CrossRef] [PubMed]
- Stewart, R.; Morrow, M.; Hammond, S.A.; Mulgrew, K.; Marcus, D.; Poon, E.; Watkins, A.; Mullins, S.; Chodorge, M.; Andrews, J.; et al. Identification and Characterization of MEDI4736, an Antagonistic Anti-PD-L1 Monoclonal Antibody. Cancer Immunol. Res. 2015, 3, 1052–1062. [Google Scholar] [CrossRef] [PubMed]
- Wilkinson, I.; Anderson, S.; Fry, J.; Julien, L.A.; Neville, D.; Qureshi, O.; Watts, G.; Hale, G. Fc-engineered antibodies with immune effector functions completely abolished. PLoS ONE 2021, 16, e0260954. [Google Scholar] [CrossRef] [PubMed]
- Herbst, R.S.; Soria, J.C.; Kowanetz, M.; Fine, G.D.; Hamid, O.; Gordon, M.S.; Sosman, J.A.; McDermott, D.F.; Powderly, J.D.; Gettinger, S.N.; et al. Predictive correlates of response to the anti-PD-L1 antibody MPDL3280A in cancer patients. Nature 2014, 515, 563–567. [Google Scholar] [CrossRef] [PubMed]
| Ave | All | Non–IRR | IRR | p-Value | |
|---|---|---|---|---|---|
| n = 24 | n = 12 | n = 12 | |||
| Renal cell carcinoma (Ave + axitinib) | 21 | 10 | 11 | ||
| Bladder cancer (Ave) | 2 | 1 | 1 | ||
| Merkel cell carcinoma (Ave) | 1 | 1 | 0 | ||
| Age (years) | 67.6 (33.8–86.1) | 67.7 (37.8–86.1) | 67.5 (33.8–86.0) | 0.977 a | |
| ≥65 years (n [%]) | 16 (66.7) | 7 (58.3) | 9 (75.0) | 0.667 b | |
| <65 years (n [%]) | 8 (33.3) | 5 (41.7) | 3 (25.0) | ||
| Body height (cm) | 164.0 (143.4–184.1) | 165.1 (143.4–184.1) | 162.8 (145.0–178.3) | 0.863 a | |
| Body weight (kg) | 59.7 (39.8–113.9) | 62.6 (41.2–113.9) | 56.7 (39.8–74.0) | 0.840 a | |
| Body mass index (kg/m2) | 22.0 (15.8–36.3) | 22.7 (15.8–36.3) | 21.2 (16.8–24.5) | 0.885 a | |
| Sex (n [%]) | Male | 15 (62.5) | 8 (66.7) | 7 (58.3) | 1.000 b |
| Female | 9 (37.5) | 4 (33.3) | 5 (41.7) | ||
| Cardiovascular disease (n [%]) | Yes | 11 (45.8) | 4 (33.3) | 7 (58.3) | 0.414 b |
| No | 13 (54.2) | 8 (66.7) | 5 (41.7) | ||
| Pulmonary disease (n [%]) | Yes | 8 (33.3) | 5 (41.7) | 3 (25.0) | 0.667 b |
| No | 16 (66.7) | 7 (58.3) | 9 (75.0) | ||
| Drug allergy (n [%]) | Yes | 9 (37.5) | 5 (41.7) | 4 (33.3) | 1.000 b |
| No | 15 (62.5) | 7 (58.3) | 8 (66.7) | ||
| Food allergy (n [%]) | Yes | 2 (8.3) | 0 | 2 (16.7) | 0.478 b |
| No | 22 (91.7) | 12 (100) | 10 (83.3) | ||
| Pollinosis (n [%]) | Yes | 5 (20.8) | 1 (4.2) | 4 (33.3) | 0.317 b |
| No | 19 (79.2) | 11 (91.7) | 8 (66.7) | ||
| Asthma (n [%]) | Yes | 3 (12.5) | 2 (16.7) | 1 (8.3) | 1.000 b |
| No | 21 (87.5) | 10 (83.3) | 11 (91.7) | ||
| Dur | All | Non–IRR | IRR | p-Value | |
| n = 27 | n = 19 | n = 8 | |||
| Age (years) | 68.5 (44.7–82.0) | 67.3 (44.7–80.0) | 71.2 (56.8–82.0) | 0.300 a | |
| ≥65 years (n [%]) | 19 (70.4) | 13 (68.4) | 6 (75.0) | 1.000 b | |
| <65 years (n [%]) | 8 (29.6) | 6 (31.6) | 2 (25.0) | ||
| Body height (cm) | 166.1 (146.7–180.3) | 166.1 (156.5–179.4) | 166.1 (146.7–180.3) | 0.730 a | |
| Body weight (kg) | 62.9 (39.9–100.1) | 62.6 (42.7–95.5) | 63.6 (39.9–100.1) | 1.000 a | |
| Body mass index (kg/m2) | 22.5 (15.7–30.8) | 22.5 (15.7–29.7) | 22.6 (18.1–30.8) | 0.853 a | |
| Sex (n [%]) | Male | 21 (77.8) | 15 (78.9) | 6 (75.0) | 1.000 b |
| Female | 6 (22.2) | 4 (21.1) | 2 (25.0) | ||
| Cardiovascular disease (n [%]) | Yes | 16 (59.3) | 13 (68.4) | 3 (37.5) | 0.206 b |
| No | 11 (40.7) | 6 (31.6) | 5 (62.5) | ||
| Drug allergy (n [%]) | Yes | 8 (29.6) | 5 (26.3) | 3 (37.5) | 0.658 b |
| No | 19 (70.4) | 14 (73.7) | 5 (62.5) | ||
| Food allergy (n [%]) | Yes | 2 (7.4) | 2 (10.5) | 0 | 1.000 b |
| No | 25 (92.6) | 17 (89.5) | 8 (100) | ||
| Pollinosis (n [%]) | Yes | 4 (14.8) | 3 (15.8) | 1 (12.5) | 1.000 b |
| No | 23 (85.2) | 16 (84.2) | 7 (87.5) | ||
| Asthma (n [%]) | Yes | 1 (3.7) | 1 (5.3) | 0 | 1.000 b |
| No | 26 (96.3) | 18 (94.7) | 8 (100) | ||
| Atezo | All | Non–IRR | IRR | p-Value | |
| n = 22 | n = 18 | n = 4 | |||
| Age (years) | 70.4 (42.6–82.9) | 71.5 (59.2–82.9) | 65.3 (42.6–75.0) | 0.766 a | |
| ≥65 years (n [%]) | 18 (81.8) | 15 (83.3) | 3 (75.0) | 1.000 b | |
| <65 years (n [%]) | 4 (18.2) | 3 (16.7) | 1 (25.0) | ||
| Body height (cm) | 164.1 (148.6–181.5) | 163.3 (148.6–174.6) | 167.7 (155.6–181.5) | 0.523 a | |
| Body weight (kg) | 57.1 (36.7–70.6) | 57.3 (36.7–70.6) | 56.3 (47.4–61.6) | 0.640 a | |
| Body mass index (kg/m2) | 21.2 (15.4–27.9) | 21.5 (15.4–27.9) | 20.2 (16.9–24.7) | 0.469 a | |
| Sex (n, %) | Male | 15 (68.2) | 12 (66.7) | 3 (75.0) | 1.000 b |
| Female | 7 (31.8) | 6 (33.3) | 1 (25.0) | ||
| Cardiovascular disease (n [%]) | Yes | 12 (54.5) | 8 (44.4) | 4 (100) | 0.096 b |
| No | 10 (45.5) | 10 (55.6) | 0 | ||
| Drug allergy (n [%]) | Yes | 7 (31.8) | 5 (27.8) | 2 (50.0) | 0.565 b |
| No | 15 (68.2) | 13 (72.2) | 2 (50.0) | ||
| Food allergy (n [%]) | Yes | 6 (27.3) | 5 (27.8) | 1 (25.0) | 1.000 b |
| No | 16 (72.7) | 13 (72.2) | 3 (75.0) | ||
| Asthma (n [%]) | Yes | 6 (27.3) | 4 (22.2) | 2 (50.0) | 0.292 b |
| No | 16 (72.7) | 14 (77.8) | 2 (50.0) |
| Ave | All | Non–IRR | IRR | p-Value | |
|---|---|---|---|---|---|
| n =24 | n =12 | n =12 | |||
| WBC (103/μL) | 5.87 (3.46–8.35) | 6.13 (3.67–8.35) | 5.62 (3.46–8.16) | 0.371 a | |
| RBC (106/μL) | 4.04 (2.68–5.84) | 3.98 (3.39–5.01) | 4.10 (2.68–5.84) | 0.954 a | |
| MCV (fL) | 92.5 (79.3–105.2) | 92.9 (86.0–101.7) | 92.1 (79.3–105.2) | 0.665 a | |
| MCH (pg) | 30.4 (24.5–33.6) | 31.0 (27.3–32.8) | 29.7 (24.5–33.6) | 0.126 a | |
| MCHC (%) | 32.8 (30.9–36.5) | 33.4 (31.3–36.5) | 32.3 (30.9–34.4) | 0.078 a | |
| Hemoglobin (g/dL) | 12.2 (8.2–15.9) | 12.3 (10.3–14.7) | 12.1 (8.2–15.9) | 1.000 a | |
| Hematocrit (%) | 37.1 (26.3–48.0) | 36.8 (30.7–43.1) | 37.4 (26.3–48.0) | 0.665 a | |
| Platelets (103/μL) | 246 (160–430) | 252 (189–373) | 240 (160–430) | 0.436 a | |
| Neutrophil | number (103/μL) | 3.84 (1.93–5.93) | 4.12 (2.38–5.93) | 3.56 (1.93–5.74) | 0.248 a |
| ratio (%) | 64.4 (45.5–72.4) | 66.8 (51.5–71.8) | 62.0 (45.5–72.4) | 0.126 a | |
| Lymphocyte | number (103/μL) | 1.44 (0.81–2.55) | 1.36 (0.81–2.16) | 1.52 (1.08–2.55) | 0.312 a |
| ratio (%) | 25.4 (14.3–47.6) | 22.5 (14.3–36.4) | 28.3 (18.3–47.6) | 0.112 a | |
| Monocyte | number (103/μL) | 0.38 (0.22–0.70) | 0.40 (0.27–0.65) | 0.36 (0.22–0.70) | 0.194 a |
| ratio (%) | 6.6 (3.3–11.2) | 6.8 (3.3–9.7) | 6.4 (4.6–11.2) | 0.686 a | |
| Eosinophil | number (103/μL) | 0.17 (0.03–0.45) | 0.21 (0.03–0.45) | 0.14 (0.04–0.21) | 0.751 a |
| ratio (%) | 2.9 (0.7–6.0) | 3.2 (0.7–6.0) | 2.55 (0.9–4.5) | 0.665 a | |
| Basophil | number (103/μL) | 0.04 (0.01–0.09) | 0.05 (0.01–0.09) | 0.04 (0.01–0.07) | 0.371 a |
| ratio (%) | 0.7 (0.2–1.6) | 0.8 (0.2–1.5) | 0.7 (0.2–1.6) | 0.600 a | |
| NLR | 2.9 (1.0–4.9) | 3.3 (1.4–4.9) | 2.4 (1.0–3.7) | 0.100 a | |
| MLR | 0.3 (0.1–0.7) | 0.3 (0.1–0.7) | 0.3 (0.1–0.6) | 0.100 a | |
| PLR | 181 (79–266) | 197 (117–266) | 164 (79–245) | 0.157 a | |
| CRP (mg/dL) | 1.26 (0.02–9.83) | 1.21 (0.02–6.01) | 1.31 (0.02–9.83) | 0.397 a | |
| Dur | All | Non–IRR | IRR | p-Value | |
| n = 27 | n = 19 | n = 8 | |||
| WBC (103/μL) | 5.49 (1.25–19.32) | 5.37 (1.25–19.32) | 5.77 (3.78–9.24) | 0.441 a | |
| RBC (106/μL) | 3.49 (2.27–4.36) | 3.45 (2.27–4.27) | 3.58 (2.81–4.36) | 0.614 a | |
| MCV (fL) | 95.1 (85.3–106.6) | 95.0 (88.4–106.6) | 95.3 (85.3–103.1) | 0.577 a | |
| MCH (pg) | 31.4 (27.4–35.4) | 31.4 (27.6–35.4) | 31.3 (27.4–32.8) | 1.000 a | |
| MCHC (%) | 33.0 (30.7–35.6) | 33.1 (30.7–35.6) | 32.8 (31.6–34.8) | 0.472 a | |
| Hemoglobin (g/dL) | 10.9 (6.8–14.3) | 10.8 (6.8–12.7) | 11.2 (8.7–14.3) | 0.791 a | |
| Hematocrit (%) | 33.1 (21.7–41.1) | 32.7 (21.7–38.9) | 34.0 (27.5–41.1) | 0.790 a | |
| Platelets (103/μL) | 236 (97–358) | 235 (118–358) | 240 (97–357) | 0.937 a | |
| Neutrophil | number (103/μL) | 3.45 (0.81–6.76) | 3.31 (0.81–6.64) | 3.81 (2.28–6.76) | 0.690 a |
| ratio (%) | 66.7 (20.5–86.4) | 67.2 (20.5–86.4) | 65.7 (52.4–79.0) | 0.313 a | |
| Lymphocyte | number (103/μL) | 1.41 (0.21–14.57) | 1.48 (0.21–14.57) | 1.25 (0.47–3.47) | 0.212 a |
| ratio (%) | 20.8 (4.6–75.4) | 20.2 (4.6–75.4) | 22.2 (5.4–37.6) | 0.203 a | |
| Monocyte | number (103/μL) | 0.47 (0.13–1.07) | 0.44 (0.13–0.68) | 0.53 (0.28–1.07) | 0.614 a |
| ratio (%) | 9.5 (2.8–14.8) | 9.6 (2.8–14.8) | 9.1 (6.7–12.4) | 0.791 a | |
| Eosinophil | number (103/μL) | 0.13 (0.01–0.36) | 0.12 (0.01–0.36) | 0.14 (0.03–0.25) | 0.381 a |
| ratio (%) | 2.4 (0.1–6.5) | 2.4 (0.1–6.5) | 2.5 (0.7–4.6) | 0.577 a | |
| Basophil | number (103/μL) | 0.03 (0–0.08) | 0.03 (0–0.08) | 0.04 (0.01–0.08) | 0.652 a |
| ratio (%) | 0.6 (0–1.5) | 0.6 (0–1.5) | 0.6 (0.2–1.0) | 0.789 a | |
| NLR | 5.1 (0.3–18.1) | 5.3 (0.3–18.1) | 4.7 (1.4–14.5) | 0.193 a | |
| MLR | 0.6 (0.0–2.3) | 0.6 (0.0–1.8) | 0.7 (0.2–2.3) | 0.301 a | |
| PLR | 327 (25–984) | 351 (25–984) | 268 (66–607) | 0.232 a | |
| CRP (mg/dL) | 1.68 (0.02–13.2) | 1.63 (0.02–13.2) | 1.79 (0.02–7.21) | 0.595 a | |
| Atezo | All | Non–IRR | IRR | p-Value | |
| n = 22 | n = 18 | n = 4 | |||
| WBC (103/μL) | 7.90 (3.75–15.61) | 7.16 (3.75–10.51) | 11.22 (8.66–15.61) | 0.024 *,a | |
| RBC (106/μL) | 3.99 (2.51–5.63) | 4.08 (2.75–5.63) | 3.59 (2.51–4.85) | 0.523 a | |
| MCV (fL) | 92.8 (76.3–103.6) | 94.1 (81.2–103.6) | 87.1 (76.3–100.4) | 0.328 a | |
| MCH (pg) | 29.9 (22.7–33.7) | 30.5 (26.8–33.7) | 26.9 (22.7–31.5) | 0.089 a | |
| MCHC (%) | 32.2 (29.7–33.3) | 32.5 (30.5–33.3) | 30.8 (29.7–31.3) | 0.008 *,a | |
| Hemoglobin (g/dL) | 11.9 (7.9–17.3) | 12.4 (8.7–17.3) | 9.3 (7.9–11.0) | 0.019 *,a | |
| Hematocrit (%) | 36.8 (25.2–52.6) | 38.3 (28.5–52.6) | 30.2 (25.2–37.0) | 0.045 *,a | |
| Platelets (103/μL) | 299 (132–526) | 283 (132–515) | 372 (291–526) | 0.055 a | |
| Neutrophil | number (103/μL) | 5.83 (2.36–14.03) | 5.12 (2.36–8.15) | 9.00 (7.07–14.03) | 0.009 a |
| ratio (%) | 71.8 (46.2–89.9) | 70.1 (46.2–84.2) | 79.5 (65.7–89.9) | 0.136 a | |
| Lymphocyte | number (103/μL) | 1.39 (0.55–2.77) | 1.40 (0.55–2.30) | 1.37 (0.70–2.77) | 0.580 a |
| ratio (%) | 19.5 (4.5–45.1) | 21.0 (9.2–45.1) | 12.8 (4.5–24.2) | 0.136 a | |
| Monocyte | number (103/μL) | 0.48 (0.11–0.93) | 0.44 (0.11–0.93) | 0.65 (0.43–0.75) | 0.046 *,a |
| ratio (%) | 6.0 (2.8–9.9) | 6.0 (2.8–9.9) | 5.9 (4.7–7.6) | 1.000 a | |
| Eosinophil | number (103/μL) | 0.16 (0–0.54) | 0.17 (0–0.54) | 0.15 (0.07–0.33) | 0.832 a |
| ratio (%) | 2.2 (0–7.8) | 2.4 (0–7.8) | 1.3 (0.6–2.9) | 0.250 a | |
| Basophil | number (103/μL) | 0.04 (0.01–0.08) | 0.03 (0.01–0.08) | 0.05 (0.03–0.08) | 0.136 a |
| ratio (%) | 0.5 (0.1–1.5) | 0.5 (0.1–1.5) | 0.5 (0.2–0.7) | 1.000 a | |
| NLR | 5.3 (1.0–20.0) | 4.4 (1.0–8.8) | 9.4 (2.7–20.0) | 0.136 a | |
| MLR | 0.4 (0.1–1.1) | 0.3 (0.1–0.8) | 0.6 (0.3–1.1) | 0.067 a | |
| PLR | 259 (62–646) | 235 (62–484) | 368 (111–646) | 0.251 a | |
| CRP (mg/dL) | 1.43 (0.02–6.86) | 1.08 (0.02–6.86) | 3.01 (0.02–6.18) | 0.268 a | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hata, K.; Nakamura, K.; Maeda, S.; Maeda, M.; Fujio, Y.; Hirobe, S. Infusion-Related Reactions Subsequent to Avelumab, Durvalumab, and Atezolizumab Administration: A Retrospective Observational Study. Clin. Pract. 2024, 14, 377-387. https://doi.org/10.3390/clinpract14020029
Hata K, Nakamura K, Maeda S, Maeda M, Fujio Y, Hirobe S. Infusion-Related Reactions Subsequent to Avelumab, Durvalumab, and Atezolizumab Administration: A Retrospective Observational Study. Clinics and Practice. 2024; 14(2):377-387. https://doi.org/10.3390/clinpract14020029
Chicago/Turabian StyleHata, Keiko, Keina Nakamura, Shinichiro Maeda, Makiko Maeda, Yasushi Fujio, and Sachiko Hirobe. 2024. "Infusion-Related Reactions Subsequent to Avelumab, Durvalumab, and Atezolizumab Administration: A Retrospective Observational Study" Clinics and Practice 14, no. 2: 377-387. https://doi.org/10.3390/clinpract14020029
APA StyleHata, K., Nakamura, K., Maeda, S., Maeda, M., Fujio, Y., & Hirobe, S. (2024). Infusion-Related Reactions Subsequent to Avelumab, Durvalumab, and Atezolizumab Administration: A Retrospective Observational Study. Clinics and Practice, 14(2), 377-387. https://doi.org/10.3390/clinpract14020029






