Neuroimaging Techniques in Differentiating Parkinson’s Disease from Drug-Induced Parkinsonism: A Comprehensive Review
Abstract
1. Introduction
2. Dopamine Radiotracers
2.1. History
2.2. Mechanism and General Description of Dopamine Transporter (DAT) Radiotracers
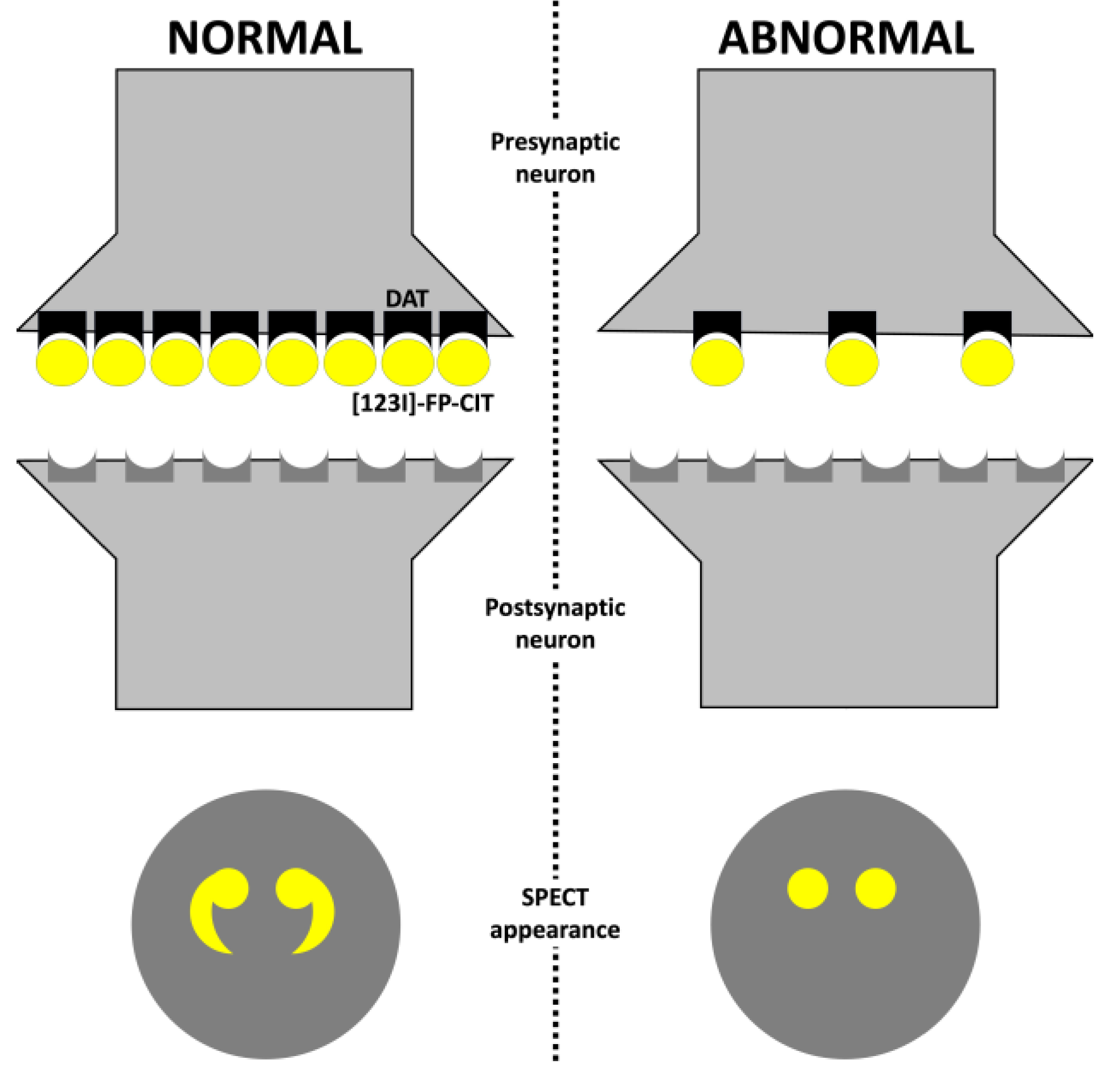
2.3. [123I]-FP-CIT
2.4. [123I]-β-CIT
2.5. [99mTc]-TRODAT-1
2.6. [18F]-DOPA
2.7. [18F]-AV-133
2.8. [18F]-FP-CIT
2.9. Neuroimaging and Receptors Occupancy
3. [18F]-Fluorodeoxyglucose ([18F]-FDG) PET
4. [123I]-MIBG Cardiac Imaging
5. Magnetic Resonance Imaging (MRI)—The Swallowtail Appearance
6. Transcranial Ultrasound
7. Optical Coherence Tomography
8. Expert Recommendations
9. Future Studies
10. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Baizabal-Carvallo, J.F.; Morgan, J.C. Drug-Induced Tremor, Clinical Features, Diagnostic Approach and Management. J. Neurol. Sci. 2022, 435, 120192. [Google Scholar] [CrossRef] [PubMed]
- Rissardo, J.P.; Vora, N.; Mathew, B.; Kashyap, V.; Muhammad, S.; Fornari Caprara, A.L. Overview of Movement Disorders Secondary to Drugs. Clin. Pract. 2023, 13, 959–976. [Google Scholar] [CrossRef] [PubMed]
- Esper, C.D.; Factor, S.A. Failure of Recognition of Drug-Induced Parkinsonism in the Elderly. Mov. Disord. 2008, 23, 401–404. [Google Scholar] [CrossRef]
- de Germay, S.; Montastruc, F.; Carvajal, A.; Lapeyre-Mestre, M.; Montastruc, J.-L. Drug-Induced Parkinsonism: Revisiting the Epidemiology Using the WHO Pharmacovigilance Database. Park. Relat. Disord. 2020, 70, 55–59. [Google Scholar] [CrossRef] [PubMed]
- Feldman, M.; Marmol, S.; Margolesky, J. Updated Perspectives on the Management of Drug-Induced Parkinsonism (DIP): Insights from the Clinic. Ther. Clin. Risk Manag. 2022, 18, 1129–1142. [Google Scholar] [CrossRef]
- Rissardo, J.P.; Caprara, A.L.F. Predictors of Drug-Induced Parkinsonism. APIK J. Intern. Med. 2023. [Google Scholar] [CrossRef]
- Rissardo, J.P.; Fornari Caprara, A.L. Lamotrigine-Associated Movement Disorder: A Literature Review. Neurol. India 2021, 69, 1524–1538. [Google Scholar] [CrossRef]
- Rissardo, J.P.; Caprara, A.L.F. Fluoroquinolone-Associated Movement Disorder: A Literature Review. Medicines 2023, 10, 33. [Google Scholar] [CrossRef]
- Hardie, R.J.; Lees, A.J. Neuroleptic-Induced Parkinson’s Syndrome: Clinical Features and Results of Treatment with Levodopa. J. Neurol. Neurosurg. Psychiatry 1988, 51, 850–854. [Google Scholar] [CrossRef]
- Hitri, A.; Hurd, Y.L.; Wyatt, R.J.; Deutsch, S.I. Molecular, Functional and Biochemical Characteristics of the Dopamine Transporter: Regional Differences and Clinical Relevance. Clin. Neuropharmacol. 1994, 17, 1–22. [Google Scholar] [CrossRef]
- Shaya, E.K.; Scheffel, U.; Dannals, R.F.; Ricaurte, G.A.; Carroll, F.I.; Wagner, H.N.J.; Kuhar, M.J.; Wong, D.F. In Vivo Imaging of Dopamine Reuptake Sites in the Primate Brain Using Single Photon Emission Computed Tomography (SPECT) and Iodine-123 Labeled RTI-55. Synapse 1992, 10, 169–172. [Google Scholar] [CrossRef] [PubMed]
- Flace, P.; Livrea, P.; Basile, G.A.; Galletta, D.; Bizzoca, A.; Gennarini, G.; Bertino, S.; Branca, J.J.V.; Gulisano, M.; Bianconi, S.; et al. The Cerebellar Dopaminergic System. Front. Syst. Neurosci. 2021, 15, 650614. [Google Scholar] [CrossRef] [PubMed]
- Brooks, D.J. Molecular Imaging of Dopamine Transporters. Ageing Res. Rev. 2016, 30, 114–121. [Google Scholar] [CrossRef] [PubMed]
- Benamer, H.T.S.; Patterson, J.; Grosset, D.G.; Booij, J.; de Bruin, K.; van Royen, E.; Speelman, J.D.; Horstink, M.H.I.M.; Sips, H.J.W.A.; Dierckx, R.A.; et al. Accurate Differentiation of Parkinsonism and Essential Tremor Using Visual Assessment of [(123) I]-FP-CIT SPECT Imaging: The [(123) I]-FP-CIT Study Group. Mov. Disord. 2000, 15, 503–510. [Google Scholar] [CrossRef] [PubMed]
- Catafau, A.M.; Tolosa, E. Impact of Dopamine Transporter SPECT Using 123I-Ioflupane on Diagnosis and Management of Patients with Clinically Uncertain Parkinsonian Syndromes. Mov. Disord. 2004, 19, 1175–1182. [Google Scholar] [CrossRef] [PubMed]
- Jennings, D.L.; Seibyl, J.P.; Oakes, D.; Eberly, S.; Murphy, J.; Marek, K. (123I) Beta-CIT and Single-Photon Emission Computed Tomographic Imaging vs Clinical Evaluation in Parkinsonian Syndrome: Unmasking an Early Diagnosis. Arch. Neurol. 2004, 61, 1224–1229. [Google Scholar] [CrossRef]
- Marshall, V.L.; Reininger, C.B.; Marquardt, M.; Patterson, J.; Hadley, D.M.; Oertel, W.H.; Benamer, H.T.S.; Kemp, P.; Burn, D.; Tolosa, E.; et al. Parkinson’s Disease Is Overdiagnosed Clinically at Baseline in Diagnostically Uncertain Cases: A 3-Year European Multicenter Study with Repeat [123I]FP-CIT SPECT. Mov. Disord. 2009, 24, 500–508. [Google Scholar] [CrossRef]
- Carroll, F.I.; Lewin, A.H.; Boja, J.W.; Kuhar, M.J. Cocaine Receptor: Biochemical Characterization and Structure-Activity Relationships of Cocaine Analogues at the Dopamine Transporter. J. Med. Chem. 1992, 35, 969–981. [Google Scholar] [CrossRef]
- Abbasi Gharibkandi, N.; Hosseinimehr, S.J. Radiotracers for Imaging of Parkinson’s Disease. Eur. J. Med. Chem. 2019, 166, 75–89. [Google Scholar] [CrossRef] [PubMed]
- Vaquero, J.J.; Kinahan, P. Positron Emission Tomography: Current Challenges and Opportunities for Technological Advances in Clinical and Preclinical Imaging Systems. Annu. Rev. Biomed. Eng. 2015, 17, 385–414. [Google Scholar] [CrossRef]
- Ba, F.; Martin, W.R.W. Dopamine Transporter Imaging as a Diagnostic Tool for Parkinsonism and Related Disorders in Clinical Practice. Park. Relat. Disord. 2015, 21, 87–94. [Google Scholar] [CrossRef] [PubMed]
- Seifert, K.D.; Wiener, J.I. The Impact of DaTscan on the Diagnosis and Management of Movement Disorders: A Retrospective Study. Am. J. Neurodegener. Dis. 2013, 2, 29–34. [Google Scholar]
- Latif, S.; Jahangeer, M.; Maknoon Razia, D.; Ashiq, M.; Ghaffar, A.; Akram, M.; El Allam, A.; Bouyahya, A.; Garipova, L.; Ali Shariati, M.; et al. Dopamine in Parkinson’s Disease. Clin. Chim. Acta 2021, 522, 114–126. [Google Scholar] [CrossRef] [PubMed]
- Kägi, G.; Bhatia, K.P.; Tolosa, E. The Role of DAT-SPECT in Movement Disorders. J. Neurol. Neurosurg. Psychiatry 2010, 81, 5–12. [Google Scholar] [CrossRef] [PubMed]
- Filippi, L.; Manni, C.; Pierantozzi, M.; Brusa, L.; Danieli, R.; Stanzione, P.; Schillaci, O. 123I-FP-CIT Semi-Quantitative SPECT Detects Preclinical Bilateral Dopaminergic Deficit in Early Parkinson’s Disease with Unilateral Symptoms. Nucl. Med. Commun. 2005, 26, 421–426. [Google Scholar] [CrossRef]
- Bhattacharjee, S.; Shankar, P.V.; Elkider, M. Dopamine Transporter Single-Photon Emission Computed Tomography Brain Scan: A Reliable Way to Distinguish between Degenerative and Drug-Induced Parkinsonism. Indian J. Nucl. Med. 2016, 31, 249–250. [Google Scholar] [CrossRef]
- Manoharan, P.; Jamieson, S.; Bury, R.F. Initial Clinical Experience with [123I]Ioflupane Scintigraphy in Movement Disorders. Clin. Radiol. 2007, 62, 463–471. [Google Scholar] [CrossRef]
- Kleppe, R.; Waheed, Q.; Ruoff, P. DOPA Homeostasis by Dopamine: A Control-Theoretic View. Int. J. Mol. Sci. 2021, 22, 12862. [Google Scholar] [CrossRef]
- Booij, J.; Kemp, P. Dopamine Transporter Imaging with [(123)I]FP-CIT SPECT: Potential Effects of Drugs. Eur. J. Nucl. Med. Mol. Imaging 2008, 35, 424–438. [Google Scholar] [CrossRef]
- Volkow, N.D.; Chang, L.; Wang, G.J.; Fowler, J.S.; Leonido-Yee, M.; Franceschi, D.; Sedler, M.J.; Gatley, S.J.; Hitzemann, R.; Ding, Y.S.; et al. Association of Dopamine Transporter Reduction with Psychomotor Impairment in Methamphetamine Abusers. Am. J. Psychiatry 2001, 158, 377–382. [Google Scholar] [CrossRef]
- Schiffer, W.K.; Logan, J.; Dewey, S.L. Positron Emission Tomography Studies of Potential Mechanisms Underlying Phencyclidine-Induced Alterations in Striatal Dopamine. Neuropsychopharmacology 2003, 28, 2192–2198. [Google Scholar] [CrossRef] [PubMed]
- Ukairo, O.T.; Bondi, C.D.; Newman, A.H.; Kulkarni, S.S.; Kozikowski, A.P.; Pan, S.; Surratt, C.K. Recognition of Benztropine by the Dopamine Transporter (DAT) Differs from That of the Classical Dopamine Uptake Inhibitors Cocaine, Methylphenidate, and Mazindol as a Function of a DAT Transmembrane 1 Aspartic Acid Residue. J. Pharmacol. Exp. Ther. 2005, 314, 575–583. [Google Scholar] [CrossRef] [PubMed]
- Kilbourn, M.R.; Kemmerer, E.S.; Desmond, T.J.; Sherman, P.S.; Frey, K.A. Differential Effects of Scopolamine on in Vivo Binding of Dopamine Transporter and Vesicular Monoamine Transporter Radioligands in Rat Brain. Exp. Neurol. 2004, 188, 387–390. [Google Scholar] [CrossRef] [PubMed]
- Argyelán, M.; Szabó, Z.; Kanyó, B.; Tanács, A.; Kovács, Z.; Janka, Z.; Pávics, L. Dopamine Transporter Availability in Medication Free and in Bupropion Treated Depression: A 99mTc-TRODAT-1 SPECT Study. J. Affect. Disord. 2005, 89, 115–123. [Google Scholar] [CrossRef] [PubMed]
- Volkow, N.D.; Wang, G.-J.; Fowler, J.S.; Learned-Coughlin, S.; Yang, J.; Logan, J.; Schlyer, D.; Gatley, J.S.; Wong, C.; Zhu, W.; et al. The Slow and Long-Lasting Blockade of Dopamine Transporters in Human Brain Induced by the New Antidepressant Drug Radafaxine Predict Poor Reinforcing Effects. Biol. Psychiatry 2005, 57, 640–646. [Google Scholar] [CrossRef]
- Kugaya, A.; Seneca, N.M.; Snyder, P.J.; Williams, S.A.; Malison, R.T.; Baldwin, R.M.; Seibyl, J.P.; Innis, R.B. Changes in Human in Vivo Serotonin and Dopamine Transporter Availabilities during Chronic Antidepressant Administration. Neuropsychopharmacology 2003, 28, 413–420. [Google Scholar] [CrossRef]
- Shang, Y.; Gibbs, M.A.; Marek, G.J.; Stiger, T.; Burstein, A.H.; Marek, K.; Seibyl, J.P.; Rogers, J.F. Displacement of Serotonin and Dopamine Transporters by Venlafaxine Extended Release Capsule at Steady State: A [123I]2beta-Carbomethoxy-3beta-(4-Iodophenyl)-Tropane Single Photon Emission Computed Tomography Imaging Study. J. Clin. Psychopharmacol. 2007, 27, 71–75. [Google Scholar] [CrossRef]
- Schillaci, O.; Pierantozzi, M.; Filippi, L.; Manni, C.; Brusa, L.; Danieli, R.; Bernardi, G.; Simonetti, G.; Stanzione, P. The Effect of Levodopa Therapy on Dopamine Transporter SPECT Imaging with( 123)I-FP-CIT in Patients with Parkinson’s Disease. Eur. J. Nucl. Med. Mol. Imaging 2005, 32, 1452–1456. [Google Scholar] [CrossRef]
- Ahlskog, J.E.; Uitti, R.J.; O’Connor, M.K.; Maraganore, D.M.; Matsumoto, J.Y.; Stark, K.F.; Turk, M.F.; Burnett, O.L. The Effect of Dopamine Agonist Therapy on Dopamine Transporter Imaging in Parkinson’s Disease. Mov. Disord. 1999, 14, 940–946. [Google Scholar] [CrossRef]
- Innis, R.B.; Marek, K.L.; Sheff, K.; Zoghbi, S.; Castronuovo, J.; Feigin, A.; Seibyl, J.P. Effect of Treatment with L-Dopa/Carbidopa or L-Selegiline on Striatal Dopamine Transporter SPECT Imaging with [123I]Beta-CIT. Mov. Disord. 1999, 14, 436–442. [Google Scholar] [CrossRef]
- Taylor, J.-P.; Colloby, S.J.; McKeith, I.G.; Burn, D.J.; Williams, D.; Patterson, J.; O’Brien, J.T. Cholinesterase Inhibitor Use Does Not Significantly Influence the Ability of 123I-FP-CIT Imaging to Distinguish Alzheimer’s Disease from Dementia with Lewy Bodies. J. Neurol. Neurosurg. Psychiatry 2007, 78, 1069–1071. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Volkow, N.D.; Wang, G.J.; Fischman, M.W.; Foltin, R.W.; Fowler, J.S.; Abumrad, N.N.; Vitkun, S.; Logan, J.; Gatley, S.J.; Pappas, N.; et al. Relationship between Subjective Effects of Cocaine and Dopamine Transporter Occupancy. Nature 1997, 386, 827–830. [Google Scholar] [CrossRef] [PubMed]
- Best, S.E.; Sarrel, P.M.; Malison, R.T.; Laruelle, M.; Zoghbi, S.S.; Baldwin, R.M.; Seibyl, J.P.; Innis, R.B.; van Dyck, C.H. Striatal Dopamine Transporter Availability with [123I]Beta-CIT SPECT Is Unrelated to Gender or Menstrual Cycle. Psychopharmacology 2005, 183, 181–189. [Google Scholar] [CrossRef] [PubMed]
- Madras, B.K.; Xie, Z.; Lin, Z.; Jassen, A.; Panas, H.; Lynch, L.; Johnson, R.; Livni, E.; Spencer, T.J.; Bonab, A.A.; et al. Modafinil Occupies Dopamine and Norepinephrine Transporters in Vivo and Modulates the Transporters and Trace Amine Activity in Vitro. J. Pharmacol. Exp. Ther. 2006, 319, 561–569. [Google Scholar] [CrossRef]
- Mateos, J.J.; Lomeña, F.; Parellada, E.; Mireia, F.; Fernandez-Egea, E.; Pavia, J.; Prats, A.; Pons, F.; Bernardo, M. Lower Striatal Dopamine Transporter Binding in Neuroleptic-Naive Schizophrenic Patients Is Not Related to Antipsychotic Treatment but It Suggests an Illness Trait. Psychopharmacology 2007, 191, 805–811. [Google Scholar] [CrossRef]
- Bergström, K.A.; Jolkkonen, J.; Kuikka, J.T.; Akerman, K.K.; Viinamäki, H.; Airaksinen, O.; Länsimies, E.; Tiihonen, J. Fentanyl Decreases Beta-CIT Binding to the Dopamine Transporter. Synapse 1998, 29, 413–415. [Google Scholar] [CrossRef]
- Zaaijer, E.R.; van Dijk, L.; de Bruin, K.; Goudriaan, A.E.; Lammers, L.A.; Koeter, M.W.J.; van den Brink, W.; Booij, J. Effect of Extended-Release Naltrexone on Striatal Dopamine Transporter Availability, Depression and Anhedonia in Heroin-Dependent Patients. Psychopharmacology 2015, 232, 2597–2607. [Google Scholar] [CrossRef]
- Costa, K.M. The Effects of Aging on Substantia Nigra Dopamine Neurons. J. Neurosci. 2014, 34, 15133–15134. [Google Scholar] [CrossRef]
- Mozley, P.D.; Acton, P.D.; Barraclough, E.D.; Plössl, K.; Gur, R.C.; Alavi, A.; Mathur, A.; Saffer, J.; Kung, H.F. Effects of Age on Dopamine Transporters in Healthy Humans. J. Nucl. Med. 1999, 40, 1812–1817. [Google Scholar]
- Lavalaye, J.; Booij, J.; Reneman, L.; Habraken, J.B.A.; van Royen, E.A. Effect of Age and Gender on Dopamine Transporter Imaging with [123I]FP-CIT SPET in Healthy Volunteers. Eur. J. Nucl. Med. 2000, 27, 867–869. [Google Scholar] [CrossRef]
- Kaasinen, V.; Joutsa, J.; Noponen, T.; Johansson, J.; Seppänen, M. Effects of Aging and Gender on Striatal and Extrastriatal [123I]FP-CIT Binding in Parkinson’s Disease. Neurobiol. Aging 2015, 36, 1757–1763. [Google Scholar] [CrossRef] [PubMed]
- Brigo, F.; Matinella, A.; Erro, R.; Tinazzi, M. [123I]FP-CIT SPECT (DaTSCAN) May Be a Useful Tool to Differentiate between Parkinson’s Disease and Vascular or Drug-Induced Parkinsonisms: A Meta-Analysis. Eur. J. Neurol. 2014, 21, 1369-e90. [Google Scholar] [CrossRef]
- Booij, J.; Speelman, J.D.; Horstink, M.W.; Wolters, E.C. The Clinical Benefit of Imaging Striatal Dopamine Transporters with [123I]FP-CIT SPET in Differentiating Patients with Presynaptic Parkinsonism from Those with Other Forms of Parkinsonism. Eur. J. Nucl. Med. 2001, 28, 266–272. [Google Scholar] [CrossRef] [PubMed]
- Lorberboym, M.; Treves, T.A.; Melamed, E.; Lampl, Y.; Hellmann, M.; Djaldetti, R. [123I]-FP/CIT SPECT Imaging for Distinguishing Drug-Induced Parkinsonism from Parkinson’s Disease. Mov. Disord. 2006, 21, 510–514. [Google Scholar] [CrossRef]
- Vlaar, A.M.M.; de Nijs, T.; Kessels, A.G.H.; Vreeling, F.W.; Winogrodzka, A.; Mess, W.H.; Tromp, S.C.; van Kroonenburgh, M.J.P.G.; Weber, W.E.J. Diagnostic Value of 123I-Ioflupane and 123I-Iodobenzamide SPECT Scans in 248 Patients with Parkinsonian Syndromes. Eur. Neurol. 2008, 59, 258–266. [Google Scholar] [CrossRef] [PubMed]
- Tinazzi, M.; Ottaviani, S.; Isaias, I.U.; Pasquin, I.; Steinmayr, M.; Vampini, C.; Pilleri, M.; Moretto, G.; Fiaschi, A.; Smania, N.; et al. [123I]FP-CIT SPET Imaging in Drug-Induced Parkinsonism. Mov. Disord. 2008, 23, 1825–1829. [Google Scholar] [CrossRef]
- Tinazzi, M.; Antonini, A.; Bovi, T.; Pasquin, I.; Steinmayr, M.; Moretto, G.; Fiaschi, A.; Ottaviani, S. Clinical and [123I]FP-CIT SPET Imaging Follow-up in Patients with Drug-Induced Parkinsonism. J. Neurol. 2009, 256, 910–915. [Google Scholar] [CrossRef]
- Diaz-Corrales, F.J.; Sanz-Viedma, S.; Garcia-Solis, D.; Escobar-Delgado, T.; Mir, P. Clinical Features and 123I-FP-CIT SPECT Imaging in Drug-Induced Parkinsonism and Parkinson’s Disease. Eur. J. Nucl. Med. Mol. Imaging 2010, 37, 556–564. [Google Scholar] [CrossRef]
- Hambÿe, A.-S.; Vervaet, A.; Dethy, S. FP-CIT SPECT in Clinically Inconclusive Parkinsonian Syndrome during Amiodarone Treatment: A Study with Follow-Up. Nucl. Med. Commun. 2010, 31, 583–589. [Google Scholar] [CrossRef]
- Cuberas-Borrós, G.; Lorenzo-Bosquet, C.; Aguadé-Bruix, S.; Hernández-Vara, J.; Pifarré-Montaner, P.; Miquel, F.; Álvarez-Sabin, J.; Castell-Conesa, J. Quantitative Evaluation of Striatal I-123-FP-CIT Uptake in Essential Tremor and Parkinsonism. Clin. Nucl. Med. 2011, 36, 991–996. [Google Scholar] [CrossRef]
- Tinazzi, M.; Cipriani, A.; Matinella, A.; Cannas, A.; Solla, P.; Nicoletti, A.; Zappia, M.; Morgante, L.; Morgante, F.; Pacchetti, C.; et al. [123I]FP-CIT Single Photon Emission Computed Tomography Findings in Drug-Induced Parkinsonism. Schizophr. Res. 2012, 139, 40–45. [Google Scholar] [CrossRef] [PubMed]
- Olivares Romero, J.; Arjona Padillo, A. Diagnostic accuracy of 123 I-FP-CIT SPECT in diagnosing drug-induced parkinsonism: A prospective study. Neurologia 2013, 28, 276–282. [Google Scholar] [CrossRef] [PubMed]
- Tinazzi, M.; Morgante, F.; Matinella, A.; Bovi, T.; Cannas, A.; Solla, P.; Marrosu, F.; Nicoletti, A.; Zappia, M.; Luca, A.; et al. Imaging of the Dopamine Transporter Predicts Pattern of Disease Progression and Response to Levodopa in Patients with Schizophrenia and Parkinsonism: A 2-Year Follow-up Multicenter Study. Schizophr. Res. 2014, 152, 344–349. [Google Scholar] [CrossRef] [PubMed]
- Morley, J.F.; Cheng, G.; Dubroff, J.G.; Wood, S.; Wilkinson, J.R.; Duda, J.E. Olfactory Impairment Predicts Underlying Dopaminergic Deficit in Presumed Drug-Induced Parkinsonism. Mov. Disord. Clin. Pract. 2017, 4, 603–606. [Google Scholar] [CrossRef]
- Tachibana, K.; HIrata, Y.; Katoh, N.; Ishikawa, H.; Shimada, T.; Shindo, A.; Matsuura, K.; Asahi, M.; Satoh, M.; Ii, Y.; et al. Differentiation of Drug-Induced Parkinsonism and PD.; Utility of 123I-FP-CIT SPECT(DaTscan). J. Neurol. Sci. 2017, 381, 954. [Google Scholar] [CrossRef]
- Gajos, A.; Dąbrowski, J.; Bieńkiewicz, M.; Płachcińska, A.; Kuśmierek, J.; Bogucki, A. The Symptoms Asymmetry of Drug-Induced Parkinsonism Is Not Related to Nigrostriatal Cell Degeneration: A SPECT-DaTSCAN Study. Neurol. Neurochir. Pol. 2019, 53, 311–314. [Google Scholar] [CrossRef]
- Aamodt, W.W.; Dubroff, J.G.; Cheng, G.; Taylor, B.; Wood, S.; Duda, J.E.; Morley, J.F. Gait Abnormalities and Non-Motor Symptoms Predict Abnormal Dopaminergic Imaging in Presumed Drug-Induced Parkinsonism. NPJ Park. Dis. 2022, 8, 53. [Google Scholar] [CrossRef]
- Neumeyer, J.L.; Wang, S.; Gao, Y.; Milius, R.A.; Kula, N.S.; Campbell, A.; Baldessarini, R.J.; Zea-Ponce, Y.; Baldwin, R.M.; Innis, R.B. N-Omega-Fluoroalkyl Analogs of (1R)-2 Beta-Carbomethoxy-3 Beta-(4-Iodophenyl)-Tropane (Beta-CIT): Radiotracers for Positron Emission Tomography and Single Photon Emission Computed Tomography Imaging of Dopamine Transporters. J. Med. Chem. 1994, 37, 1558–1561. [Google Scholar] [CrossRef]
- Abi-Dargham, A.; Gandelman, M.S.; DeErausquin, G.A.; Zea-Ponce, Y.; Zoghbi, S.S.; Baldwin, R.M.; Laruelle, M.; Charney, D.S.; Hoffer, P.B.; Neumeyer, J.L.; et al. SPECT Imaging of Dopamine Transporters in Human Brain with Iodine-123-Fluoroalkyl Analogs of Beta-CIT. J. Nucl. Med. 1996, 37, 1129–1133. [Google Scholar]
- Seibyl, J.P.; Marek, K.; Sheff, K.; Zoghbi, S.; Baldwin, R.M.; Charney, D.S.; van Dyck, C.H.; Innis, R.B. Iodine-123-Beta-CIT and Iodine-123-FPCIT SPECT Measurement of Dopamine Transporters in Healthy Subjects and Parkinson’s Patients. J. Nucl. Med. 1998, 39, 1500–1508. [Google Scholar]
- Eerola, J.; Tienari, P.J.; Kaakkola, S.; Nikkinen, P.; Launes, J. How Useful Is [123I]Beta-CIT SPECT in Clinical Practice? J. Neurol. Neurosurg. Psychiatry 2005, 76, 1211–1216. [Google Scholar] [CrossRef] [PubMed]
- Easterford, K.; Clough, P.; Kellett, M.; Fallon, K.; Duncan, S. Reversible Parkinsonism with Normal Beta-CIT-SPECT in Patients Exposed to Sodium Valproate. Neurology 2004, 62, 1435–1437. [Google Scholar] [CrossRef] [PubMed]
- Laruelle, M.; Abi-Dargham, A.; van Dyck, C.H.; Gil, R.; D’Souza, C.D.; Erdos, J.; McCance, E.; Rosenblatt, W.; Fingado, C.; Zoghbi, S.S.; et al. Single Photon Emission Computerized Tomography Imaging of Amphetamine-Induced Dopamine Release in Drug-Free Schizophrenic Subjects. Proc. Natl. Acad. Sci. USA 1996, 93, 9235–9240. [Google Scholar] [CrossRef] [PubMed]
- Bolzati, C.; Dolmella, A. Nitrido Technetium-99 m Core in Radiopharmaceutical Applications: Four Decades of Research. Inorganics 2020, 8, 3. [Google Scholar] [CrossRef]
- Sasannezhad, P.; Juibary, A.G.; Sadri, K.; Sadeghi, R.; Sabour, M.; Kakhki, V.R.D.; Alizadeh, H. (99m)Tc-TRODAT-1 SPECT Imaging in Early and Late Onset Parkinson’s Disease. Asia Ocean. J. Nucl. Med. Biol. 2017, 5, 114–119. [Google Scholar] [CrossRef]
- Fallahi, B.; Esmaeili, A.; Beiki, D.; Oveisgharan, S.; Noorollahi-Moghaddam, H.; Erfani, M.; Tafakhori, A.; Rohani, M.; Fard-Esfahani, A.; Emami-Ardekani, A.; et al. Evaluation of (99m)Tc-TRODAT-1 SPECT in the Diagnosis of Parkinson’s Disease versus Other Progressive Movement Disorders. Ann. Nucl. Med. 2016, 30, 153–162. [Google Scholar] [CrossRef]
- Fabiani, G.; Camargo, C.H.F.; Filho, R.M.; Froehner, G.S.; Teive, H.A.G. Evaluation of Brain SPECT with (99m)Tc-TRODAT-1 in the Differential Diagnosis of Parkinsonism. Parkinsons Dis. 2022, 2022, 1746540. [Google Scholar] [CrossRef]
- Burn, D.J.; Brooks, D.J. Nigral Dysfunction in Drug-Induced Parkinsonism: An 18F-Dopa PET Study. Neurology 1993, 43, 552–556. [Google Scholar] [CrossRef]
- Dackis, C.A.; Gold, M.S. New Concepts in Cocaine Addiction: The Dopamine Depletion Hypothesis. Neurosci. Biobehav. Rev. 1985, 9, 469–477. [Google Scholar] [CrossRef]
- Mulvihill, K.G. Presynaptic Regulation of Dopamine Release: Role of the DAT and VMAT2 Transporters. Neurochem. Int. 2019, 122, 94–105. [Google Scholar] [CrossRef]
- Alexander, P.K.; Lie, Y.; Jones, G.; Sivaratnam, C.; Bozinvski, S.; Mulligan, R.S.; Young, K.; Villemagne, V.L.; Rowe, C.C. Management Impact of Imaging Brain Vesicular Monoamine Transporter Type 2 in Clinically Uncertain Parkinsonian Syndrome with (18)F-AV133 and PET. J. Nucl. Med. 2017, 58, 1815–1820. [Google Scholar] [CrossRef] [PubMed]
- Hong, J.Y.; Sunwoo, M.K.; Oh, J.S.; Kim, J.S.; Sohn, Y.H.; Lee, P.H. Persistent Drug-Induced Parkinsonism in Patients with Normal Dopamine Transporter Imaging. PLoS ONE 2016, 11, e0157410. [Google Scholar] [CrossRef] [PubMed]
- Oh, Y.-S.; Yoo, S.-W.; Lyoo, C.H.; Kim, J.-S. Decreased Thalamic Monoamine Availability in Drug-Induced Parkinsonism. Sci. Rep. 2022, 12, 3749. [Google Scholar] [CrossRef]
- Shin, H.-W.; Kim, J.S.; Oh, M.; You, S.; Kim, Y.J.; Kim, J.; Kim, M.-J.; Chung, S.J. Clinical Features of Drug-Induced Parkinsonism Based on [18F] FP-CIT Positron Emission Tomography. Neurol. Sci. 2015, 36, 269–274. [Google Scholar] [CrossRef] [PubMed]
- Nordström, A.L.; Nyberg, S.; Olsson, H.; Farde, L. Positron Emission Tomography Finding of a High Striatal D2 Receptor Occupancy in Olanzapine-Treated Patients. Arch. Gen. Psychiatry 1998, 55, 283–284. [Google Scholar] [CrossRef] [PubMed]
- Raedler, T.J.; Knable, M.B.; Lafargue, T.; Urbina, R.A.; Egan, M.F.; Pickar, D.; Weinberger, D.R. In Vivo Determination of Striatal Dopamine D2 Receptor Occupancy in Patients Treated with Olanzapine. Psychiatry Res. 1999, 90, 81–90. [Google Scholar] [CrossRef]
- Nyberg, S.; Eriksson, B.; Oxenstierna, G.; Halldin, C.; Farde, L. Suggested Minimal Effective Dose of Risperidone Based on PET-Measured D2 and 5-HT2A Receptor Occupancy in Schizophrenic Patients. Am. J. Psychiatry 1999, 156, 869–875. [Google Scholar] [CrossRef]
- Heinz, A.; Knable, M.B.; Weinberger, D.R. Dopamine D2 Receptor Imaging and Neuroleptic Drug Response. J. Clin. Psychiatry 1996, 57 (Suppl. 11), 84–88, discussion 89–93. [Google Scholar]
- Meyer, P.T.; Frings, L.; Rücker, G.; Hellwig, S. (18)F-FDG PET in Parkinsonism: Differential Diagnosis and Evaluation of Cognitive Impairment. J. Nucl. Med. 2017, 58, 1888–1898. [Google Scholar] [CrossRef]
- Kotomin, I.; Korotkov, A.; Solnyshkina, I.; Didur, M.; Cherednichenko, D.; Kireev, M. Parkinson’s Disease-Related Brain Metabolic Pattern Is Expressed in Schizophrenia Patients during Neuroleptic Drug-Induced Parkinsonism. Diagnostics 2022, 13, 74. [Google Scholar] [CrossRef]
- Pagano, G.; Niccolini, F.; Politis, M. Imaging in Parkinson’s Disease. Clin. Med. 2016, 16, 371–375. [Google Scholar] [CrossRef]
- Lee, P.H.; Kim, J.S.; Shin, D.H.; Yoon, S.-N.; Huh, K. Cardiac 123I-MIBG Scintigraphy in Patients with Drug Induced Parkinsonism. J. Neurol. Neurosurg. Psychiatry 2006, 77, 372–374. [Google Scholar] [CrossRef] [PubMed]
- Lee, P.H.; Yeo, S.H.; Yong, S.W.; Kim, Y.J. Odour Identification Test and Its Relation to Cardiac 123I-Metaiodobenzylguanidine in Patients with Drug Induced Parkinsonism. J. Neurol. Neurosurg. Psychiatry 2007, 78, 1250–1252. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.-S.; Oh, Y.-S.; Kim, Y.-I.; Yang, D.-W.; Chung, Y.-A.; You, I.-R.; Lee, K.-S. Combined Use of 123I-Metaiodobenzylguanidine (MIBG) Scintigraphy and Dopamine Transporter (DAT) Positron Emission Tomography (PET) Predicts Prognosis in Drug-Induced Parkinsonism (DIP): A 2-Year Follow-up Study. Arch. Gerontol. Geriatr. 2013, 56, 124–128. [Google Scholar] [CrossRef] [PubMed]
- Shafie, M.; Mayeli, M.; Saeidi, S.; Mirsepassi, Z.; Abbasi, M.; Shafeghat, M.; Aghamollaii, V. The Potential Role of the Cardiac MIBG Scan in Differentiating the Drug-Induced Parkinsonism from Parkinson’s Disease. Clin. Park. Relat. Disord. 2022, 6, 100130. [Google Scholar] [CrossRef] [PubMed]
- Prasuhn, J.; Neumann, A.; Strautz, R.; Dreischmeier, S.; Lemmer, F.; Hanssen, H.; Heldmann, M.; Schramm, P.; Brüggemann, N. Clinical MR Imaging in Parkinson’s Disease: How Useful Is the Swallow Tail Sign? Brain Behav. 2021, 11, e02202. [Google Scholar] [CrossRef] [PubMed]
- Sung, Y.H.; Noh, Y.; Lee, J.; Kim, E.Y. Drug-Induced Parkinsonism versus Idiopathic Parkinson Disease: Utility of Nigrosome 1 with 3-T Imaging. Radiology 2016, 279, 849–858. [Google Scholar] [CrossRef]
- Cosottini, M.; Frosini, D.; Pesaresi, I.; Costagli, M.; Biagi, L.; Ceravolo, R.; Bonuccelli, U.; Tosetti, M. MR Imaging of the Substantia Nigra at 7 T Enables Diagnosis of Parkinson Disease. Radiology 2014, 271, 831–838. [Google Scholar] [CrossRef]
- Berg, D.; Roggendorf, W.; Schröder, U.; Klein, R.; Tatschner, T.; Benz, P.; Tucha, O.; Preier, M.; Lange, K.W.; Reiners, K.; et al. Echogenicity of the Substantia Nigra: Association with Increased Iron Content and Marker for Susceptibility to Nigrostriatal Injury. Arch. Neurol. 2002, 59, 999–1005. [Google Scholar] [CrossRef]
- Mehnert, S.; Reuter, I.; Schepp, K.; Maaser, P.; Stolz, E.; Kaps, M. Transcranial Sonography for Diagnosis of Parkinson’s Disease. BMC Neurol. 2010, 10, 9. [Google Scholar] [CrossRef]
- Bouwmans, A.E.P.; Vlaar, A.M.M.; Mess, W.H.; Kessels, A.; Weber, W.E.J. Specificity and Sensitivity of Transcranial Sonography of the Substantia Nigra in the Diagnosis of Parkinson’s Disease: Prospective Cohort Study in 196 Patients. BMJ Open 2013, 3, e002613. [Google Scholar] [CrossRef] [PubMed]
- Olivares Romero, J.; Arjona Padillo, A.; Barrero Hernández, F.J.; Martín González, M.; Gil Extremera, B. Utility of Transcranial Sonography in the Diagnosis of Drug-Induced Parkinsonism: A Prospective Study. Eur. J. Neurol. 2013, 20, 1451–1458. [Google Scholar] [CrossRef] [PubMed]
- Oh, Y.-S.; Kwon, D.-Y.; Kim, J.-S.; Park, M.-H.; Berg, D. Transcranial Sonographic Findings May Predict Prognosis of Gastroprokinetic Drug-Induced Parkinsonism. Park. Relat. Disord. 2018, 46, 36–40. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.-Y.; Ahn, J.; Kim, T.W.; Jeon, B.S. Optical Coherence Tomography in Parkinson’s Disease: Is the Retina a Biomarker? J. Park. Dis. 2014, 4, 197–204. [Google Scholar] [CrossRef] [PubMed]
- Jiménez, B.; Ascaso, F.J.; Cristóbal, J.A.; López del Val, J. Development of a Prediction Formula of Parkinson Disease Severity by Optical Coherence Tomography. Mov. Disord. 2014, 29, 68–74. [Google Scholar] [CrossRef]
- Suh, W.; Baek, S.U.; Oh, J.S.; Seo, S.Y.; Kim, J.S.; Han, Y.M.; Kim, M.S.; Kang, S.Y. Retinal Thickness and Its Interocular Asymmetry Between Parkinson’s Disease and Drug-Induced Parkinsonism. J. Korean Med. Sci. 2023, 38, e86. [Google Scholar] [CrossRef]
- Rissardo, J.P.; Caprara, A.L.F. Cinnarizine- and Flunarizine-Associated Movement Disorder: A Literature Review. Egyp. J. Neurol. Psych. Neurosurg. 2020, 56, 61. [Google Scholar] [CrossRef]


| Radionuclide | Half-Life | Type of Emission | Energy | Intensity |
|---|---|---|---|---|
| 11C | 20.3 min | Positron | 961 Kev | 99.8% |
| 18F | 109.7 min | Positron | 634 Kev | 97% |
| 123I | 13.3 h | Gamma | 159 Kev | 83% |
| 99mTc | 6 h | Gamma | 140 Kev | 89% |
| Grade | Description | Diagram | |
|---|---|---|---|
| Normal | Caudate nucleus appears like a “full stop” and putamen-like “tail” (whole appearance is like a comma on both sides) |  | |
| SWIDD (scans with ipsilateral dopaminergic deficit) | Type 1 | Normal “full stop” with unilateral disappearing “comma” (asymmetrical loss of putaminal tail) |  OR OR |
| Type 2 | “Two full stops” (bilateral loss of putaminal tails) |  | |
| Type 3 | “Disappearing full stops” (partial to complete loss of caudate and putaminal signals) |  | |
| Agent | Agent Effect in the Striatal Binding | Half-Life | Recommended Time to Hold before Imaging | Reference | |
|---|---|---|---|---|---|
| Adrenergic agonists | Phenylephrine | Increased when infused at high doses | NA | NA | [29] |
| Norepinephrine | NA | NA | |||
| Amphetamines | Decreased | 5–30 h | 3–7 days | [30] | |
| Anesthetics | Ketamine | Decreased | 3 h | 15 h | [31] |
| Phencyclidine | 7–46 h | 10 days | |||
| Isoflurane | 2.1 min | 10.5 min | |||
| Anticholinergics | Benztropine | Decreased | 12–24 h | 5 days | [32] |
| Scopolamine-like | Increased, but no effect on visual assessment | 9.5 h | 2 days | [33] | |
| Antidepressants | Bupropion | Decreased/none | 12–30 h | 8 days | [34] |
| Mazindol | Decreased | 10–13 h | 3 days | [29] | |
| Radafaxine | Decreased | NA | NA | [35] | |
| SNRIs | Increased, but no effect on visual assessment | NA | Not required | [36] | |
| SSRIs | Increased, but no effect on visual assessment | NA | Not required | [37] | |
| Tricyclic antidepressants | None | NA | Not required | [29] | |
| Antiparkinsonian medication | L-DOPA | None, but possible downregulation of dopamine transporters | NA | Not required | [38] |
| Dopamine agonists | NA | Not required | [39] | ||
| NMDA receptors blockers | NA | Not required | [29] | ||
| MAO-B inhibitors | NA | Not required | [40] | ||
| COMT inhibitors | NA | Not required | [29] | ||
| Cholinesterase inhibitors | None | NA | Not required | [41] | |
| CNS stimulants | Phentermine | Decreased | 25 h | 6 days | [29] |
| Ephedrine | 6 h | 30 h | |||
| Cocaine | Decreased | 1 h | 2 days | [42] | |
| Estrogen replacement post menopause | Increased, but no effect on visual assessment | NA | Not required | [29] | |
| Lithium | Decreased | 24 h | 5 days | [21] | |
| Menstrual cycle | None | NA | NA | [43] | |
| Modafinil | Decreased | 15 h | 3 days | [44] | |
| Neuroleptics/antipsychotics | None | NA | Not required | [45] | |
| Opioids | Fentanyl | Decreased | 2–4 h | 20 h | [46] |
| Naltrexone | None | NA | Not required | [47] | |
| Abbreviation | Other Names | Approval | PET/SPECT | Radiopharmaceutical Agent | Mechanism |
|---|---|---|---|---|---|
| [123I]-FP-CIT | DaTscan, Ioflupane | FDA EMA | SPECT | 123I-N-3-fluoropropyl-2bcarboxymethoxy- 3b-(4-iodophenyl) tropane | Pre-synaptic. DAT. |
| [123I]-β-CIT | Dopascan | EMA | SPECT | 123I-(2)-2β-carboxymethoxy-3b-(4-iodophenyl) tropane | Pre-synaptic. DAT. |
| [99mTc]-TRODAT-1 | NA | NA | SPECT | 99mTc-TRODAT-1 ([2-[2-[3-(4-chlorophenyl)-8-methyl-8-azabicyclo [3,2,1]oct-2-yl] methyl](2-mercaptoethyl) -amino] ethyl] amino] ethanethiolato (3-)-N2, N2′, S2, S2′]oxo-[1R-(exo-exo)]) | Pre-synaptic. DAT. |
| [18F]-DOPA | Fluorodopa | FDA EMA | PET | 6-[18F]fluoro-L-3,4-dihydroxyphenylalanine | Pre-synaptic. DOPA decarboxylase. |
| [18F]-AV-133 | NA | NA | PET | 9-[(18)F]fluoropropyl-(+)-dihydrotetrabenazine | Pre-synaptic. VMAT2. |
| [18F]-FP-CIT | NA | NA | PET | 18F-N-(3-fluoropropyl)-2beta-carbon ethoxy-3beta-(4-iodophenyl) nortropane | Pre-synaptic. DAT. |
| Query | MeSH Terms | Results |
|---|---|---|
| ([123I]-FP-CIT) AND (drug-induced parkinsonism) | (“2 carbomethoxy 8 3 fluoropropyl 3 4 iodophenyl tropane”[Supplementary Concept] OR “2 carbomethoxy 8 3 fluoropropyl 3 4 iodophenyl tropane”[All Fields] OR “123i fp cit”[All Fields]) AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 33 |
| ([18F]-FP-CIT) AND (drug-induced parkinsonism) | (“2 carbomethoxy 8 3 fluoropropyl 3 4 iodophenyl tropane”[Supplementary Concept] OR “2 carbomethoxy 8 3 fluoropropyl 3 4 iodophenyl tropane”[All Fields] OR “18f fp cit”[All Fields]) AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 30 |
| ([18F]-DOPA) AND (drug-induced parkinsonism) | (“fluorodopa f 18”[Supplementary Concept] OR “fluorodopa f 18”[All Fields] OR “18f dopa”[All Fields]) AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 9 |
| ([123I]-β-CIT) AND (drug-induced parkinsonism) | “123i beta cit”[All Fields] AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 4 |
| ([99mTc]-TRODAT-1) AND (drug-induced parkinsonism) | (“technetium tc 99m trodat 1”[Supplementary Concept] OR “technetium tc 99m trodat 1”[All Fields] OR “99mtc trodat 1”[All Fields]) AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 4 |
| ([18F]-AV-133) AND (drug-induced parkinsonism) | (“florbenazine f 18”[Supplementary Concept] OR “florbenazine f 18”[All Fields] OR “18f av 133”[All Fields]) AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 1 |
| ([123I]-IPT) AND (drug-induced parkinsonism) | (“n 3 iodopropen 1 yl 2 carbomethoxy 3 4 chlorophenyl tropane”[Supplementary Concept] OR “n 3 iodopropen 1 yl 2 carbomethoxy 3 4 chlorophenyl tropane”[All Fields] OR “123i ipt”[All Fields]) AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 0 |
| ([11C]-DOPA) AND (drug-induced parkinsonism) | “11c dopa”[All Fields] AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 0 |
| ([11C]-DOPA) AND (drug-induced parkinsonism) | “11c dopa”[All Fields] AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 0 |
| [18F]-Dihydrotetrabenazine | “18f dihydrotetrabenazine”[All Fields] AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 0 |
| ([123I]-Altropane) AND (drug-induced parkinsonism) | “123i altropane”[All Fields] AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 0 |
| ([11C]-Altropane) AND (drug-induced parkinsonism) | “11c altropane”[All Fields] AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 0 |
| ([11C]-WIN35428) AND (drug-induced parkinsonism) | “11C”[All Fields] AND “win35428”[All Fields] AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 0 |
| [18F]-CFT | “18F”[All Fields] AND “cft”[All Fields] AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 0 |
| ([11C]-PE2I) AND (drug-induced parkinsonism) | (“n 3 iodoprop 2 enyl 2 beta carbomethoxy 3 4 methylphenyl nortropane”[Supplementary Concept] OR “n 3 iodoprop 2 enyl 2 beta carbomethoxy 3 4 methylphenyl nortropane”[All Fields] OR “11c pe2i”[All Fields]) AND (“drug-induced”[All Fields] AND (“parkinson disease”[MeSH Terms] OR (“parkinson”[All Fields] AND “disease”[All Fields]) OR “parkinson disease”[All Fields] OR “parkinsons”[All Fields] OR “parkinson”[All Fields] OR “parkinson s”[All Fields] OR “parkinsonian disorders”[MeSH Terms] OR (“parkinsonian”[All Fields] AND “disorders”[All Fields]) OR “parkinsonian disorders”[All Fields] OR “parkinsonism”[All Fields] OR “parkinsonisms”[All Fields] OR “parkinsons s”[All Fields])) | 0 |
| Agency | Descriptor |
|---|---|
| European Medicines Agency | This medicinal product is for diagnostic use only. DaTSCAN is indicated for detecting loss of functional dopaminergic neuron terminals in the striatum: |
| (1) In patients with clinically uncertain parkinsonian syndromes, in order to help differentiate essential tremor from parkinsonian syndromes related to idiopathic Parkinson’s disease, multiple system atrophy, and progressive supranuclear palsy. DaTSCAN is unable to discriminate between Parkinson’s disease, multiple system atrophy, and progressive supranuclear palsy. | |
| (2) To help differentiate probable dementia with Lewy bodies from Alzheimer’s disease. DaTSCAN is unable to discriminate between dementia with Lewy bodies and Parkinson’s disease dementia. | |
| US Food and Drug Administration | DaTscan is a radiopharmaceutical indicated for striatal dopamine transporter visualization using single-photon emission computed tomography brain imaging to assist in the evaluation of adult patients with suspected parkinsonian syndromes. In these patients, DaTscan may be used to help differentiate essential tremor from tremor due to parkinsonian syndromes (idiopathic Parkinson’s disease, multiple system atrophy, and progressive supranuclear palsy). DaTscan is an adjunct to other diagnostic evaluations. |
| Reference | Population | Main Findings |
|---|---|---|
| Booij et al. (2001) [53] | 8 PD, 3 DIP, 4 VP | All the individuals with DIP presented normal SPECT imaging. |
| Lorberboym et al. (2006) [54] | 20 patients with parkinsonism | The clinical symptoms between patients with normal and abnormal scans were similar. Nine individuals had normal scans and were diagnosed with DIP. |
| Manoharan et al. (2007) [27] | 13 PD, 1 DIP, 1 VP | Two individuals were using neuroleptics and developed parkinsonism. One had abnormal imaging and was managed as Parkinson’s disease; the other had normal imaging and was treated as DIP. |
| Vlaar et al. (2008) [55] | 248 patients with parkinsonism | The mean odds ratio to differentiate PD from DIP was 36 (95% confidence interval, 2–697) with [123I]-FP-CIT. The specificity was 100%, and the sensitivity was 80%. |
| Tinazzi et al. (2008) [56] | 32 DIP, 26 healthy controls | Uptake was normal in 18 patients and reduced in 14 patients, who were diagnosed with PD unmasked by the anti-dopaminergic medication. The symmetry of motor symptoms and orofacial dyskinesias were more frequent in patients with normal uptake. |
| Tinazzi et al. (2009) [57] | 10 DIP with normal SPECT (group 1), 9 DIP with abnormal SPECT (group 2) | Upon follow-up, it was observed that all patients in group 1 had normal SPECT results and their UPDRS motor score values had not progressed. Meanwhile, patients in group 2 showed progression in both putaminal dopaminergic denervation on the scan and UPDRS motor scores. Levodopa treatment had a positive impact on motor symptoms in 30% of patients in group 1 and in 88.9% of patients in group 2. |
| Diaz-Corrales et al. (2010) [58] | 25 PD unmasked by antidopaminergic drugs, 22 PD without a previous antidopaminergic treatment, 32 DIP | Normal results in 29 (90.6%) patients with DIP. Abnormal uptake was observed in all patients with PD (qualitative assessments of SPECT images). |
| Hambye et al. (2010) [59] | 22 individuals with probable amiodarone-induced parkinsonism | The patients were undifferentiated by clinical symptoms. Imaging was used to design specific management. Individuals who had normal imaging were managed with an adjustment of amiodarone dose. Those individuals with abnormal imaging were treated with antiparkinsonian medications. |
| Cuberas-Borros et al. (2011) [60] | 20 PD, 20 DIP, and 20 essential tremor | Decreased uptake in the putamen nuclei was only noted in patients with PD. |
| Tinazzi et al. (2012) [61] | 448 schizophrenic patients treated with antipsychotics for at least 6 months | DIP was found in 33% of patients and 42% of patients with neuroimaging abnormalities had PD unmasked by the drug. |
| Olivares Romero et al. (2013) [62] | 19 DIP evaluated at least 6 months after discontinuation of antidopaminergic drugs | Sensitivity of 66.7%, specificity and positive predictive value of 100%, negative predictive value of 86.7%, and a negative likelihood ratio of 0.33 for diagnosis of iatrogenic parkinsonism or subclinical drug-exacerbated parkinsonism. |
| Tinazzi et al. (2014) [63] | 60 patients with schizophrenia and parkinsonism with SPECT at baseline evaluation (normal SPECT = 33; abnormal SPECT = 27) | Patients with baseline abnormal SPECT had higher UPDRS motor scores at follow-up and were more likely to respond to levodopa trial. |
| Morley et al. (2017) [64] | 33 patients with DIP | The patients were evaluated with imaging and olfactory testing. Imaging was abnormal in 21% cases. Motor symptoms were similar in individuals with normal and abnormal scans. Olfactory testing was concordant with imaging in 90% cases. |
| Tachibana et al. (2017) [65] | 9 patients with DIP | Neurological signs and imaging may be useful to diagnose early stages of unmasked PD in individuals with a previous diagnosis of DIP. |
| Gajos et al. (2019) [66] | 11 patients with DIP and asymmetric symptoms | The authors calculated the indices for the whole striatum, putamen, caudate, and putamen/caudate ratio. They did not find significant differences in radiotracer uptake in structures contralateral to more severe clinical symptoms when compared to the homolateral hemisphere. |
| Aamodt et al. (2022) [67] | 34 US Veterans with DIP | Imaging was abnormal in 35%. Compared to normal, the individuals with abnormal imaging had gait impairment, hyposmia, and non-motor symptoms. |
| Agency | Descriptor |
|---|---|
| European Medicines Agency | This medicinal product is for diagnostic use only. Fluorodopa (18F) is indicated for use with positron emission tomography (PET) in adults and paediatric population. |
| Neurology PET with fluorodopa (18F) is indicated for detecting the loss of functional dopaminergic neuron terminals in the striatum. It can be used for the diagnosis of Parkinson’s disease and differentiation between essential tremor and parkinsonian syndromes. To help differentiate probable dementia with Lewy bodies from Alzheimer’s disease. DaTSCAN is unable to discriminate between dementia with Lewy bodies and Parkinson’s disease dementia. | |
| US Food and Drug Administration | Fluorodopa F 18 Injection is a radioactive diagnostic agent indicated for use in positron emission tomography (PET) to visualize dopaminergic nerve terminals in the striatum for the evaluation of adult patients with suspected Parkinsonian syndromes (PS). Fluorodopa F 18 PET is an adjunct to other diagnostic evaluations. |
| Neuroimaging | Pros | Cons |
|---|---|---|
| Dopamine radiotracers | Less confounding factors than others scintigraphy studies | Invasive, scintigraphy study |
| [18F]-FDG | Disease-related pattern | Invasive, scintigraphy study. A significant number of false-positive results |
| [123I]-MIBG | Cardiac abnormalities are found before striatal region lesions in PD | Invasive, scintigraphy study |
| MRI (swallowtail appearance) | Non-invasive | 15% of the patients with DIP will have abnormal results |
| Transcranial ultrasound | Non-invasive, high specificity | Sensitivity depends on the exact cut-off value of the area being analyzed |
| Optical coherence tomography | Non-invasive | There is no benefit in early stage of DIP |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pitton Rissardo, J.; Caprara, A.L.F. Neuroimaging Techniques in Differentiating Parkinson’s Disease from Drug-Induced Parkinsonism: A Comprehensive Review. Clin. Pract. 2023, 13, 1427-1448. https://doi.org/10.3390/clinpract13060128
Pitton Rissardo J, Caprara ALF. Neuroimaging Techniques in Differentiating Parkinson’s Disease from Drug-Induced Parkinsonism: A Comprehensive Review. Clinics and Practice. 2023; 13(6):1427-1448. https://doi.org/10.3390/clinpract13060128
Chicago/Turabian StylePitton Rissardo, Jamir, and Ana Letícia Fornari Caprara. 2023. "Neuroimaging Techniques in Differentiating Parkinson’s Disease from Drug-Induced Parkinsonism: A Comprehensive Review" Clinics and Practice 13, no. 6: 1427-1448. https://doi.org/10.3390/clinpract13060128
APA StylePitton Rissardo, J., & Caprara, A. L. F. (2023). Neuroimaging Techniques in Differentiating Parkinson’s Disease from Drug-Induced Parkinsonism: A Comprehensive Review. Clinics and Practice, 13(6), 1427-1448. https://doi.org/10.3390/clinpract13060128







