Significant Leukocytosis with Hypereosinophilia Secondary to Trichuris trichiura in Adult: A Case Report
Abstract
1. Introduction
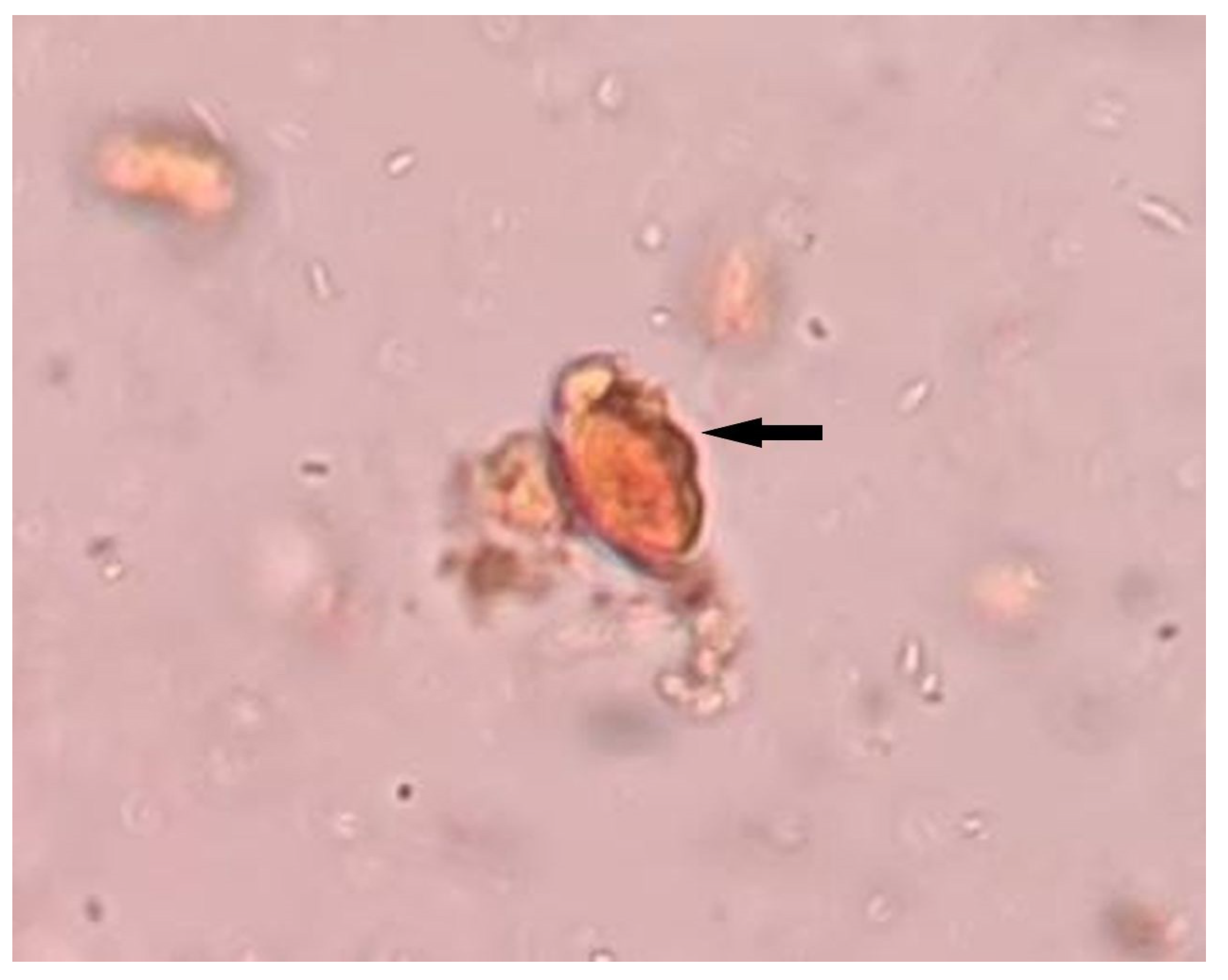
2. Case Presentation
3. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Riley, L.K.; Rupert, J. Evaluation of Patients with Leukocytosis. Am. Fam. Phys. 2015, 92, 1004–1011. [Google Scholar]
- van Balkum, M.; Kluin-Nelemans, H.; van Hellemond, J.; van Genderen, P.; Wismans, P. Hypereosinophilia: A diagnostic challenge. Neth J. Med. 2018, 76, 431–436. [Google Scholar]
- Lee, H.Y. Drug reaction with eosinophilia and systemic symptoms (DRESS). In UpToDate; Corona, R., Ed.; UpToDate: Waltham, MA, USA, 2021; Available online: https://www.uptodate.com/contents/drug-reaction-with-eosinophilia-and-systemic-symptoms(DRESS) (accessed on 12 October 2021).
- Pardo, J.; Carranza, C.; Muro, A.; Angel-Moreno, A.; Martín, A.-M.; Martín, T.; Hernández-Cabrera, M.; Pérez-Arellano, J.-L. Helminth-related eosinophilia in African immigrants, Gran Canaria. Emerg. Infect. Dis. 2006, 12, 1587. [Google Scholar] [CrossRef]
- Heukelbach, J.; Poggensee, G.; Winter, B.; Wilcke, T.; Kerr-Pontes, L.; Feldmeier, H. Leukocytosis and blood eosinophilia in a polyparasitised population in north-eastern Brazil. Trans. R. Soc. Trop. Med. Hyg. 2006, 100, 32–40. [Google Scholar] [CrossRef]
- Horton, J. Helminth-Nematode: Trichuris trichiura. In Encyclopedia of Food Safety; Motarjemi, Y., Ed.; Academic Press: Waltham, MA, USA, 2014; pp. 111–115. [Google Scholar]
- Teffari, A. Clinical manifestations and diagnosis of polycythemia vera. In UpToDate; Rosmarin, A.G., Ed.; UpToDate: Waltham, MA, USA, 2021; Available online: https://www.uptodate.com/contents/clinical-manifestations-and-diagnosis-of-polycythemia-vera (accessed on 8 September 2021).
- Wang, S.A. The diagnostic work-up of hypereosinophilia. Pathobiology 2019, 86, 39–52. [Google Scholar] [CrossRef] [PubMed]
- Choudhary, S.; McLeod, M.; Torchia, D.; Romanelli, P. Drug reaction with eosinophilia and systemic symptoms (DRESS) syndrome. J. Clin. Aesthetic Dermatol. 2013, 6, 31. [Google Scholar]
- James, J.; Sammour, Y.M.; Virata, A.R.; Nordin, T.A.; Dumic, I. Drug reaction with eosinophilia and systemic symptoms (DRESS) syndrome secondary to furosemide: Case report and review of literature. Am. J. Case Rep. 2018, 19, 163. [Google Scholar] [CrossRef] [PubMed]
- Roufosse, F.; Weller, P.F. Practical approach to the patient with hypereosinophilia. J. Allergy Clin. Immunol. 2010, 126, 39–44. [Google Scholar] [CrossRef] [PubMed]
- Else, K.J.; Keiser, J.; Holland, C.V.; Grencis, R.K.; Sattelle, D.B.; Fujiwara, R.T.; Bueno, L.L.; Asaolu, S.O.; Sowemimo, O.A.; Cooper, P.J. Whipworm and roundworm infections. Nat. Rev. Dis. Primers 2020, 6, 44. [Google Scholar] [CrossRef]
- Khuroo, M.S.; Khuroo, M.S.; Khuroo, N.S. Trichuris dysentery syndrome: A common cause of chronic iron deficiency anemia in adults in an endemic area (with videos). Gastrointest. Endosc. 2010, 71, 200–204. [Google Scholar] [CrossRef]
- Stephenson, L.S.; Holland, C.; Cooper, E. The public health importance of Trichuris trichiura. Parasitology 2000, 121, S73–S95. [Google Scholar] [CrossRef] [PubMed]
- Gottstein, B.; Pozio, E.; Nockler, K. Epidemiology, diagnosis, treatment, and control of trichinellosis. Clin. Microbiol. Rev. 2009, 22, 127–145. [Google Scholar] [CrossRef] [PubMed]
- Pullan, R.L.; Brooker, S.J. The global limits and population at risk of soil-transmitted helminth infections in 2010. Parasites Vectors 2012, 5, 1–14. [Google Scholar] [CrossRef]
- Kattula, D.; Sarkar, R.; Ajjampur, S.S.R.; Minz, S.; Levecke, B.; Muliyil, J.; Kang, G. Prevalence & risk factors for soil transmitted helminth infection among school children in south India. Indian J. Med. Res. 2014, 139, 76. [Google Scholar]
- Parija, S.C.; Chidambaram, M.; Mandal, J. Epidemiology and clinical features of soil-transmitted helminths. Trop. Parasitol. 2017, 7, 81. [Google Scholar] [PubMed]
- Ok, K.S.; Kim, Y.S.; Song, J.H.; Lee, J.H.; Ryu, S.H.; Lee, J.H.; Moon, J.S.; Whang, D.H.; Lee, H.K. Trichuris trichiura infection diagnosed by colonoscopy: Case reports and review of literature. Korean J. Parasitol. 2009, 47, 275–280. [Google Scholar] [CrossRef][Green Version]
- Kim, J.; Seo, K.I. Trichuris trichiura Infection in North Korean Defector Resulted in Chronic Abdominal Pain and Growth Retardation. Korean J. Gastroenterol. 2017, 69, 243. [Google Scholar] [CrossRef]
- Gachinmath, S.B.; Pratibha, S.; Dias, M.; Mallikarjun, P. Extensive persistent Trichuriasis: A case report. Int. J. Med. Public Health 2014, 4, 523–525. [Google Scholar] [CrossRef]
- Azira, N.M.; Zeehaida, M. Severe chronic iron deficiency anaemia secondary to Trichuris dysentery syndrome—A case report. Trop. Biomed. 2012, 29, 626–631. [Google Scholar]
- Krishnamurthy, S.; Samanta, D.; Yadav, S. Trichuris dysentery syndrome with eosinophilic leukemoid reaction mimicking inflammatory bowel disease. J. Postgrad. Med. 2009, 55, 76–77. [Google Scholar] [CrossRef]
- Mohamed, Z.; Zueter, A.; Zairi, N.Z. Trichuris dysentery syndrome: Do we learn enough from case studies? Trop. Biomed. 2015, 32, 1–6. [Google Scholar]
| Parameters | Pre-Treatment with Oral Albendazole | Post-Treatment with Oral Albendazole | Reference Range |
|---|---|---|---|
| Hb (g/dL) | 17.1 | 18.3 | 13.0–17.0 |
| HCT (%) | 49.1 | 52.8 | 40.0–50.0 |
| Platelet (×109/L) | 365 | 328 | 150–410 |
| WBC (×109/L) | 20.69 | 9.58 | 4.00–10.00 |
| WBC differentials (%) | |||
| Neutrophils (%) | 12.6 | 48.2 | 40.0–80.0 |
| Lymphocytes (%) | 22.0 | 39.1 | 20.0–40.0 |
| Monocytes (%) | 5.0 | 7.5 | 2.0–10.0 |
| Eosinophils (%) | 60.1 (AEC: 12.44 × 109/L) | 4.6 | 1.0–6.0 |
| Basophils (%) | 0.3 | 2.6 | 0.0–2.0 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Abdullah, N.; Baharudin, N.; Mohd Rustam, F.R.; Khalid, Z. Significant Leukocytosis with Hypereosinophilia Secondary to Trichuris trichiura in Adult: A Case Report. Clin. Pract. 2021, 11, 785-790. https://doi.org/10.3390/clinpract11040094
Abdullah N, Baharudin N, Mohd Rustam FR, Khalid Z. Significant Leukocytosis with Hypereosinophilia Secondary to Trichuris trichiura in Adult: A Case Report. Clinics and Practice. 2021; 11(4):785-790. https://doi.org/10.3390/clinpract11040094
Chicago/Turabian StyleAbdullah, Nasturah, Noorhida Baharudin, Farah Roslinda Mohd Rustam, and Zalizah Khalid. 2021. "Significant Leukocytosis with Hypereosinophilia Secondary to Trichuris trichiura in Adult: A Case Report" Clinics and Practice 11, no. 4: 785-790. https://doi.org/10.3390/clinpract11040094
APA StyleAbdullah, N., Baharudin, N., Mohd Rustam, F. R., & Khalid, Z. (2021). Significant Leukocytosis with Hypereosinophilia Secondary to Trichuris trichiura in Adult: A Case Report. Clinics and Practice, 11(4), 785-790. https://doi.org/10.3390/clinpract11040094






