New Aspects of Sarcomas of Uterine Corpus—A Brief Narrative Review
Abstract
:1. Introduction
2. Uterine Sarcomas
2.1. Uterine Leiomyosarcoma (ULMS)
2.1.1. Epidemiology
2.1.2. Clinical Presentations
2.1.3. Pathogenesis
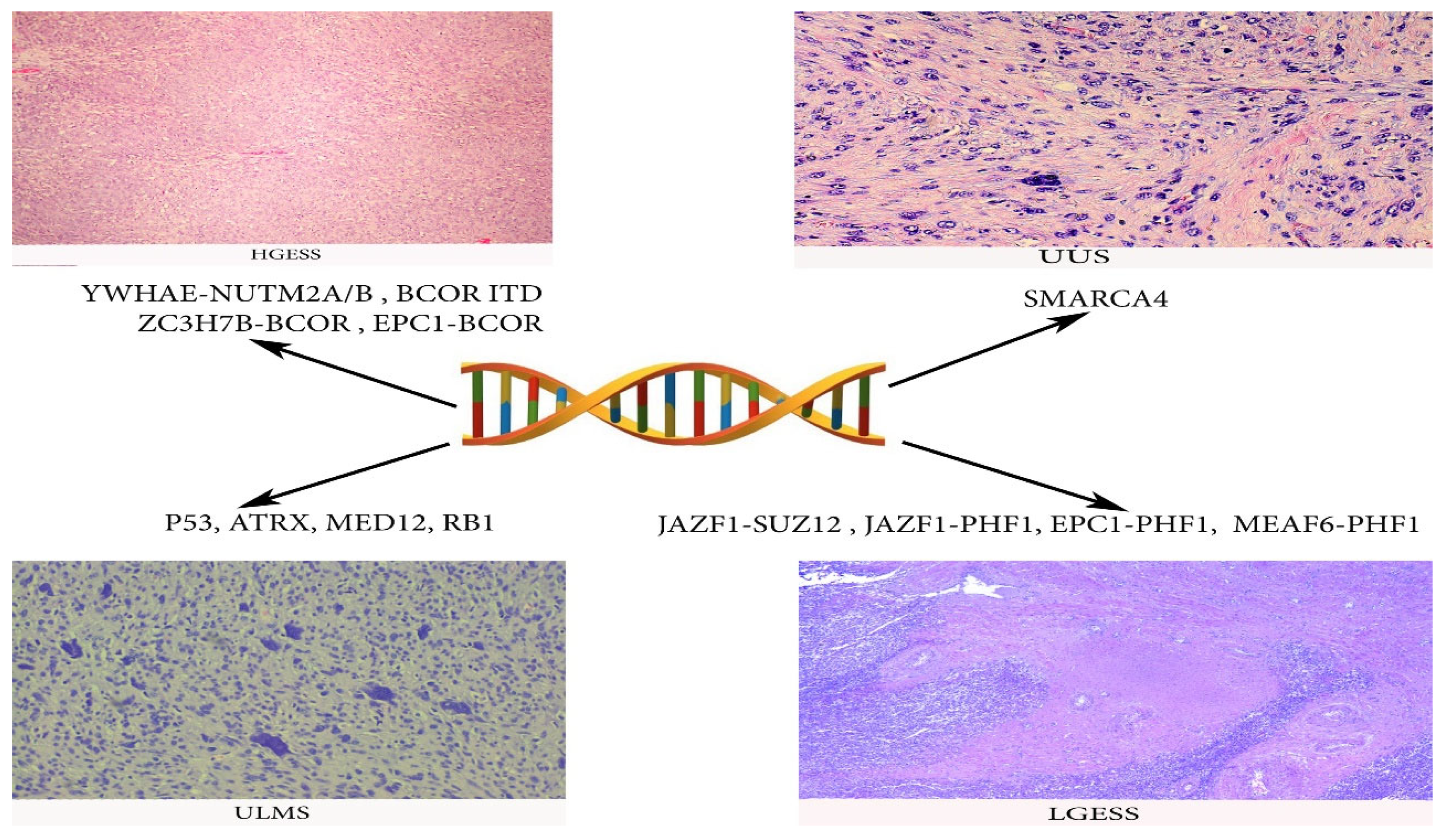
2.1.4. Pathology
2.1.5. Diagnosis
Imaging Modalities
Laboratory Tests
Endometrial Samplings
2.1.6. Prognostic Factors
2.1.7. Treatment
Surgical Treatment
Adjuvant Radiation Therapy (ART)
Adjuvant Chemotherapy (ACT)
Metastatic and Recurrent ULMS
2.2. Endometrial Stromal Sarcomas (ESSs)
2.2.1. LGESS
Pathogenesis and Pathology
Prognostic Factors
Treatment
2.2.2. HGESS
Pathology
Prognostic Factors
Treatment
2.2.3. Undifferentiated Uterine Sarcoma (UUS)
3. Mixed Epithelial–Mesenchymal Uterine Tumors
3.1. Uterine Adenosarcoma (UAS)
3.1.1. Definition, Epidemiology and Pathogenesis
3.1.2. Clinical Characteristics
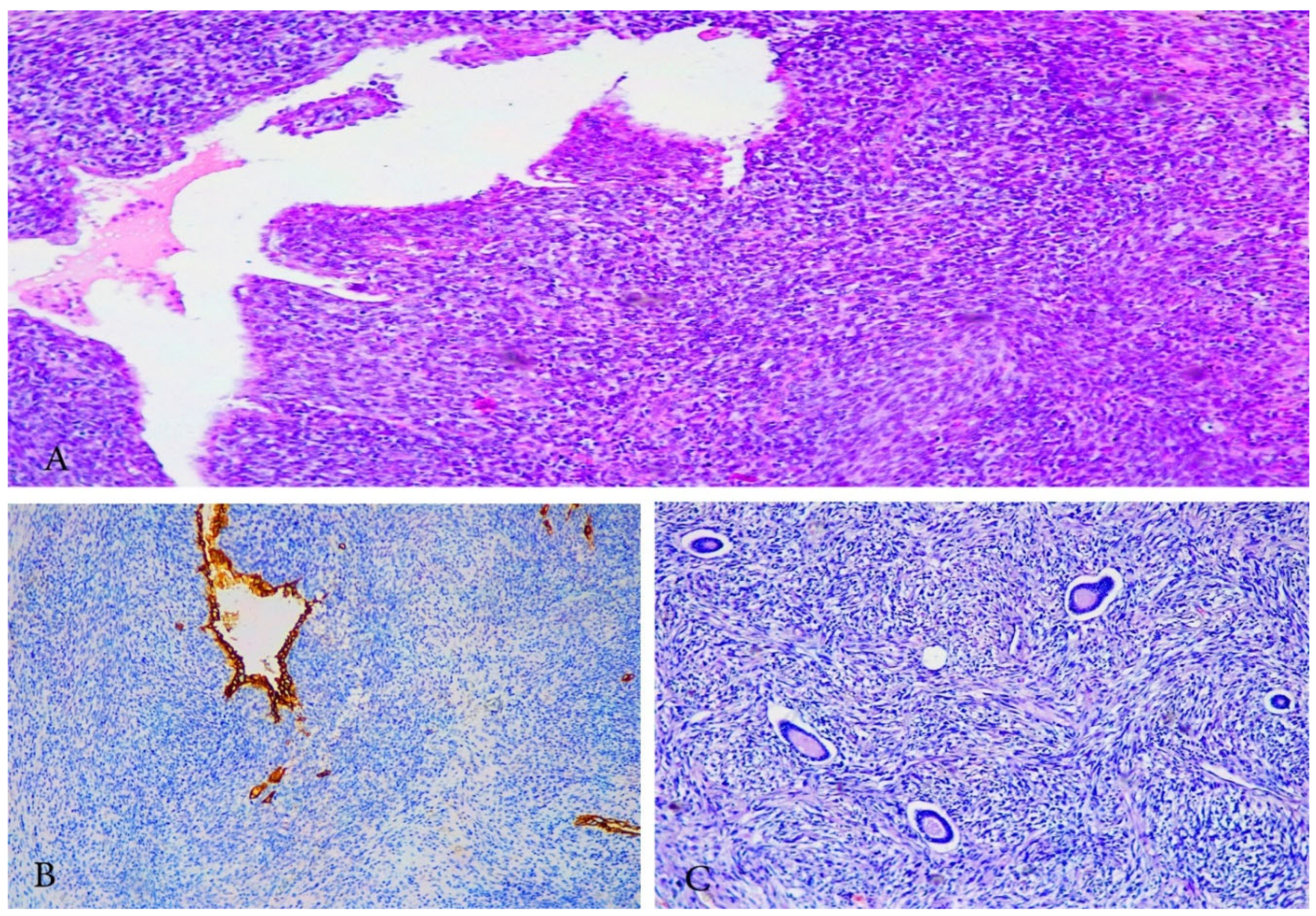
3.1.3. Pathology
- -
- Broad leaf-like appearance, formed by the malignant stroma compressing the benign epithelium.
- -
- The stroma is typically cellular, atypical, with periglandular stromal cuffing, a feature that distinguishes these tumors from endometrial or adenomatous polyps.
- -
- Spindled/round cells are located around the glandular components and form peri-glandular cuffs.
- -
- Mitotic activity ≥2 mitoses/10 HPFs (most noticeable in areas of peri-glandular cuffing).
3.1.4. Diagnosis
3.1.5. Prognostic Factors
3.1.6. Treatment
3.1.7. Recurrent or Metastatic Disease Treatment
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Mocellin, S. Soft Tissue Tumors. In A Practical and Comprehensive Guide to Sarcomas and Benign Neoplasms, 1st ed.; Springer International Publishing: Berlin/Heidelberg, Germany, 2021. [Google Scholar]
- Shushkevich, A.; Thaker, P.H.; Littell, R.D.; Shah, N.A.; Chiang, S.; Thornton, K.; Hensley, M.L.; Slomovitz, B.M.; Holcomb, K.M.; Leitao, M.M.; et al. State of the science: Uterine sarcomas: From pathology to practice. Gynecol. Oncol. 2020, 159, 3–7. [Google Scholar] [CrossRef] [PubMed]
- Cree, I.A.; White, V.A.; Indave, B.I.; Lokuhetty, D. Revising the WHO Classification: Female Genital Tract Tumours. Histopathology 2020, 76, 151–156. [Google Scholar] [CrossRef] [PubMed]
- Juhasz-Böss, I.; Gabriel, L.; Bohle, R.M.; Horn, L.C.; Solomayer, E.F.; Breitbach, G.P. Uterine Leiomyosarcoma. Oncol. Res. Treat. 2018, 41, 680–686. [Google Scholar] [CrossRef] [PubMed]
- Cui, R.R.; Wright, J.D.; Hou, J.Y. Uterine leiomyosarcoma: A review of recent advances in molecular biology, clinical management and outcome. BJOG 2017, 124, 1028–1037. [Google Scholar] [CrossRef] [Green Version]
- Roberts, M.E.; Aynardi, J.T.; Chu, C.S. Uterine leiomyosarcoma: A review of the literature and update on management options. Gynecol. Oncol. 2018, 151, 562–572. [Google Scholar] [CrossRef]
- Ricci, S.; Stone, R.L.; Fader, A.N. Uterine leiomyosarcoma: Epidemiology, contemporary treatment strategies and the impact of uterine morcellation. Gynecol. Oncol. 2017, 145, 208–216. [Google Scholar] [CrossRef]
- Gockley, A.A.; Rauh-Hain, J.A.; del Carmen, M.G. Uterine leiomyosarcoma: A review article. Int. J. Gynecol. Cancer 2014, 24, 1538–1542. [Google Scholar] [CrossRef]
- Mhawech-Fauceglia, P. Leiomyosarcoma. Pathology Outlines.com Website. Available online: https://www.pathologyoutlines.com/topic/uteruslms.html (accessed on 4 January 2021).
- An, Y.; Wang, S.; Li, S.; Zhang, L.; Wang, D.; Wang, H.; Zhu, S.; Zhu, W.; Li, Y.; Chen, W.; et al. Distinct molecular subtypes of uterine leiomyosarcoma respond differently to chemotherapy treatment. BMC Cancer 2017, 17, 639. [Google Scholar] [CrossRef]
- Yang, C.Y.; Liau, J.Y.; Huang, W.J.; Chang, Y.T.; Chang, M.C.; Lee, J.C.; Tsai, J.H.; Su, Y.N.; Hung, C.C.; Jeng, Y.M. Targeted next-generation sequencing of cancer genes identified frequent TP53 and ATRX mutations in leiomyosarcoma. Am. J. Transl. Res. 2015, 7, 2072–2081. [Google Scholar]
- Moinfar, F.; Azodi, M.; Tavassoli, F.A. Uterine sarcomas. Pathology 2007, 39, 55–71. [Google Scholar] [CrossRef]
- Leitao, M.M.; Soslow, R.A.; Nonaka, D.; Olshen, A.B.; Aghajanian, C.; Sabbatini, P.; Dupont, J.; Hensley, M.; Sonoda, Y.; Barakat, R.R.; et al. Tissue microarray immunohistochemical expression of estrogen, progesterone, and androgen receptors in uterine leiomyomata and leiomyosarcoma. Cancer 2004, 101, 1455–1462. [Google Scholar] [CrossRef]
- Atkins, K.A.; Arronte, N.; Darus, C.J.; Rice, L.W. The Use of p16 in enhancing the histologic classification of uterine smooth muscle tumors. Am. J. Surg. Pathol. 2008, 32, 98–102. [Google Scholar] [CrossRef]
- Lee, C.H.; Turbin, D.A.; Sung, Y.C.; Espinosa, I.; Montgomery, K.; van de Rijn, M.; Gilks, C.B. A panel of antibodies to determine site of origin and malignancy in smooth muscle tumors. Mod. Pathol. 2009, 22, 1519–1531. [Google Scholar] [CrossRef] [Green Version]
- Cho, H.Y.; Kim, K.; Kim, Y.B.; No, J.H. Differential diagnosis between uterine sarcoma and leiomyoma using preoperative clinical characteristics. J. Obstet. Gynaecol. Res. 2016, 42, 313–318. [Google Scholar] [CrossRef]
- DeMulder, D.; Ascher, S.M. Uterine Leiomyosarcoma: Can MRI Differentiate Leiomyosarcoma from Benign Leiomyoma Before Treatment? AJR Am. J. Roentgenol. 2018, 211, 1405–1415. [Google Scholar] [CrossRef]
- Hata, K.; Hata, T.; Maruyama, R.; Hirai, M. Uterine sarcoma: Can it be differentiated from uterine leiomyoma with Doppler ultrasonography? A preliminary report. Ultrasound Obstet. Gynecol. 1997, 9, 101–104. [Google Scholar] [CrossRef] [PubMed]
- Nagai, T.; Takai, Y.; Akahori, T.; Ishida, H.; Hanaoka, T.; Uotani, T.; Sato, S.; Matsunaga, S.; Baba, K.; Seki, H. Novel uterine sarcoma preoperative diagnosis score predicts the need for surgery in patients presenting with a uterine mass. Springerplus 2014, 3, 678. [Google Scholar] [CrossRef] [Green Version]
- Song, K.J.; Yu, X.N.; Lv, T.; Chen, Y.L.; Diao, Y.C.; Liu, S.L.; Wang, Y.K.; Yao, Q. Expression and prognostic value of lactate dehydrogenase-A and -D subunits in human uterine myoma and uterine sarcoma. Medicine 2018, 97, e0268. [Google Scholar] [CrossRef]
- Nishigaya, Y.; Kobayashi, Y.; Matsuzawa, Y.; Hasegawa, K.; Fukasawa, I.; Watanabe, Y.; Tokunaga, H.; Yaegashi, N.; Iwashita, M. Diagnostic value of combination serum assay of lactate dehydrogenase, D-dimer, and C-reactive protein for uterine leiomyosarcoma. J. Obstet. Gynaecol. Res. 2019, 45, 189–194. [Google Scholar] [CrossRef] [Green Version]
- Hosh, M.; Antar, S.; Nazzal, A.; Warda, M.; Gibreel, A.; Refky, B. Uterine Sarcoma: Analysis of 13,089 Cases Based on Surveillance, Epidemiology, and End Results Database. Int. J. Gynecol. Cancer 2016, 26, 1098–1104. [Google Scholar] [CrossRef]
- Pedra Nobre, S.; Hensley, M.L.; So, M.; Zhou, Q.C.; Iasonos, A.; Leitao, M.M., Jr.; Ducie, J.; Chiang, S.; Mueller, J.J.; Abu-Rustum, N.R.; et al. The impact of tumor fragmentation in patients with stage I uterine leiomyosarcoma on patterns of recurrence and oncologic outcome. Gynecol. Oncol. 2020, 160, 99–105. [Google Scholar] [CrossRef]
- U.S. Food and Drug Administration. UPDATE: The FDA Recommends Performing Contained Morcellation in Women When Laparoscopic Power Morcellation Is Appropriate; FDA: Silver Spring, MD, USA, 2020. Available online: https://www.fda.gov/medical-devices/safety-communications/update-fda-recommends-performing-contained-morcellation-women-when-laparoscopic-power-morcellation (accessed on 4 May 2021).
- U.S. Food and Drug Administration. Update: Perform only Contained Morcellation When Laparoscopic Power Morcellation is Appropriate. FDA Safety Communication; FDA: Silver Spring, MD, USA, 2020. Available online: https://www.fda.gov/medical-devices/safety-communications/update-perform-only-contained-morcellation-when-laparoscopic-power-morcellation-appropriate-fda (accessed on 4 May 2021).
- TNM Classification of Malignant Tumourshttps. Available online: https://www.legeforeningen.no/contentassets/201604933ce448e888a101ab969a4205/tnm-classification-of-malignant-tumours-8th-edition.pdf (accessed on 5 June 2021).
- Nasioudis, D.; Chapman-Davis, E.; Frey, M.; Holcomb, K. Safety of ovarian preservation in premenopausal women with stage I uterine sarcoma. J. Gynecol. Oncol. 2017, 28, e46. [Google Scholar] [CrossRef] [Green Version]
- Reed, N.S.; Mangioni, C.; Malmström, H.; Scarfone, G.; Poveda, A.; Pecorelli, S.; Tateo, S.; Franchi, M.; Jobsen, J.J.; Coens, C.; et al. Phase III randomised study to evaluate the role of adjuvant pelvic radiotherapy in the treatment of uterine sarcomas stages I and II: An European Organisation for Research and Treatment of Cancer Gynaecological Cancer Group Study (protocol 55874). Eur. J. Cancer 2008, 44, 808–818. [Google Scholar] [CrossRef]
- Casali, P.G.; Abecassis, N.; Aro, H.T.; Bauer, S.; Biagini, R.; Bielack, S.; Bonvalot, S.; Boukovinas, I.; Bovee, J.; Brodowicz, T.; et al. Soft tissue and visceral sarcomas: ESMO-EURACAN Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann. Oncol. 2018, 29 (Suppl. S4), iv51–iv67. [Google Scholar] [CrossRef]
- Kyriazoglou, A.; Liontos, M.; Ntanasis-Stathopoulos, I.; Gavriatopoulou, M. The systemic treatment of uterine leiomyosarcomas: A systematic review. No news is good news? Medicine 2021, 100, e25309. [Google Scholar] [CrossRef]
- Hensley, M.L.; Enserro, D.; Hatcher, H.; Ottevanger, P.B.; Krarup-Hansen, A.; Blay, J.Y.; Fisher, C.; Moxley, K.M.; Lele, S.B.; Lea, J.S.; et al. Adjuvant Gemcitabine Plus Docetaxel Followed by Doxorubicin Versus Observation for High-Grade Uterine Leiomyosarcoma: A Phase III NRG Oncology/Gynecologic Oncology Group Study. J. Clin. Oncol. 2018, 36, JCO1800454. [Google Scholar] [CrossRef] [Green Version]
- Pautier, P.; Floquet, A.; Gladieff, L.; Bompas, E.; Ray-Coquard, I.; Piperno-Neumann, S.; Selle, F.; Guillemet, C.; Weber, B.; Largillier, R.; et al. A randomized clinical trial of adjuvant chemotherapy with doxorubicin, ifosfamide, and cisplatin followed by radiotherapy versus radiotherapy alone in patients with localized uterine sarcomas (SARCGYN study). A study of the French Sarcoma Group. Ann. Oncol. 2013, 24, 1099–1104. [Google Scholar] [CrossRef]
- Burt, B.M.; Ocejo, S.; Mery, C.M.; Dasilva, M.; Bueno, R.; Sugarbaker, D.J.; Jaklitsch, M.T. Repeated and Aggressive Pulmonary Resections for Leiomyosarcoma Metastases Extends Survival. Ann. Thorac. Surg. 2011, 92, 1202–1207. [Google Scholar] [CrossRef]
- Levenback, C.; Rubin, S.C.; McCormack, P.M.; Hoskins, W.J.; Atkinson, E.N.; Lewis, J.L., Jr. Resection of pulmonary metastases from uterine sarcomas. Gynecol. Oncol. 1992, 45, 202–205. [Google Scholar] [CrossRef]
- Arend, R.C.; Toboni, M.D.; Montgomery, A.M.; Burger, R.A.; Olawaiye, A.B.; Monk, B.J.; Herzog, T.J. Systemic Treatment of Metastatic/Recurrent Uterine Leiomyosarcoma: A Changing Paradigm. Oncologist 2018, 23, 1533–1545. [Google Scholar] [CrossRef] [Green Version]
- Hensley, M.L.; Maki, R.; Venkatraman, E.; Geller, G.; Lovegren, M.; Aghajanian, C.; Sabbatini, P.; Tong, W.; Barakat, R.; Spriggs, D.R. Gemcitabine and docetaxel in patients with unresectable leiomyosarcoma: Results of a phase II trial. J. Clin. Oncol. 2002, 20, 2824–2831. [Google Scholar] [CrossRef] [PubMed]
- Hensley, M.L.; Blessing, J.A.; Mannel, R.; Rose, P.G. Fixed-dose rate gemcitabine plus docetaxel as first-line therapy for metastatic uterine leiomyosarcoma: A Gynecologic Oncology Group phase II trial. Gynecol. Oncol. 2008, 109, 329–334. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hensley, M.L.; Miller, A.; O’Malley, D.M.; Mannel, R.S.; Behbakht, K.; Bakkum-Gamez, J.N.; Michael, H. Randomized phase III trial of gemcitabine plus docetaxel plus bevacizumab or placebo as first-line treatment for metastatic uterine leiomyosarcoma: An NRG Oncology/Gynecologic Oncology Group study. J. Clin. Oncol. 2015, 33, 1180–1185. [Google Scholar] [CrossRef] [PubMed]
- Rubio, M.J.; Lecumberri, M.J.; Varela, S.; Alarcón, J.; Ortega, M.E.; Gaba, L.; Espinós, J.; Calzas, J.; Barretina, P.; Ruiz, I.; et al. Efficacy and safety of trabectedin in metastatic uterine leiomyosarcoma: A retrospective multicenter study of the Spanish ovarian cancer research group (GEICO). Gynecol. Oncol. Rep. 2020, 33, 100594. [Google Scholar] [CrossRef]
- Hensley, M.L.; Patel, S.R.; von Mehren, M.; Ganjoo, K.; Jones, R.L.; Staddon, A.; Rushing, D.; Milhem, M.; Monk, B.; Wang, G.; et al. Efficacy and safety of trabectedin or dacarbazine in patients with advanced uterine leiomyosarcoma after failure of anthracycline-based chemotherapy: Subgroup analysis of a phase 3, randomized clinical trial. Gynecol. Oncol. 2017, 146, 531–537. [Google Scholar] [CrossRef]
- Ali, R.H.; Rouzbahman, M. Endometrial stromal tumours revisited: An update based on the 2014 WHO classification. J. Clin. Pathol. 2015, 68, 325–332. [Google Scholar] [CrossRef]
- Seagle, B.L.; Shilpi, A.; Buchanan, S.; Goodman, C.; Shahabi, S. Low-grade and high-grade endometrial stromal sarcoma: A National Cancer Database study. Gynecol. Oncol. 2017, 146, 254–262. [Google Scholar] [CrossRef]
- Pernick, N. Low Grade Endometrial Stromal Sarcoma. PathologyOutlines.com Website. Available online: https://www.pathologyoutlines.com/topic/uterusESSlowgrade.html (accessed on 6 January 2021).
- Horng, H.C.; Wen, K.C.; Wang, P.H.; Chen, Y.J.; Yen, M.S.; Ng, H.T. Taiwan Association of Gynecology Systematic Review Group. Uterine sarcoma Part II-Uterine endometrial stromal sarcoma: The TAG systematic review. Taiwan J. Obstet. Gynecol. 2016, 55, 472–479. [Google Scholar] [CrossRef] [Green Version]
- Maeda, O.; Moritani, S.; Ichihara, S.; Inoue, T.; Ishihara, Y.; Yamamoto, S.; Ito, M.; Matsumura, Y.; Sugiyama, K.; Horio, M.; et al. Long-term survival in low-grade endometrial stromal sarcoma with childbirth and multidisciplinary treatment: A case report. J. Med. Case Rep. 2015, 9, 233. [Google Scholar] [CrossRef] [Green Version]
- Thiel, F.C.; Halmen, S. Low-Grade Endometrial Stromal Sarcoma—A Review. Oncol. Res. Treat. 2018, 41, 687–692. [Google Scholar] [CrossRef] [Green Version]
- Hoang, L.; Chiang, S.; Lee, C.H. Endometrial stromal sarcomas and related neoplasms: New developments and diagnostic considerations. Pathology 2018, 50, 162–177. [Google Scholar] [CrossRef]
- Masand, R.P. Unusual Presentations of Gynecologic Tumors: Primary, Extrauterine, Low-Grade Endometrioid Stromal Sarcoma. Arch. Pathol. Lab. Med. 2018, 142, 536–541. [Google Scholar] [CrossRef] [Green Version]
- Oliva, E.; Egger, J.F.; Young, R.H. Primary endometrioid stromal sarcoma of the ovary: A clinicopathologic study of 27 cases with morphologic and behavioral features similar to those of uterine low-grade endometrial stromal sarcoma. Am. J. Surg. Pathol. 2014, 38, 305–315. [Google Scholar] [CrossRef]
- Cui, R.; Yuan, F.; Wang, Y.; Li, X.; Zhang, Z.; Bai, H. Clinicopathological characteristics and treatment strategies for patients with low-grade endometrial stromal sarcoma. Medicine 2017, 96, e6584. [Google Scholar] [CrossRef]
- Chang, K.L.; Crabtree, G.S.; Lim-Tan, S.K.; Kempson, R.L.; Hendrickson, M.R. Primary uterine endometrial stromal neoplasms. A clinicopathologic study of 117 cases. Am. J. Surg. Pathol 1990, 14, 415–438. [Google Scholar] [CrossRef]
- Micci, F.; Gorunova, L.; Gatius, S.; Matias-Guiu, X.; Davidson, B.; Heim, S.; Panagopoulos, I. MEAF6/PHF1 is a recurrent gene fusion in endometrial stromal sarcoma. Cancer Lett. 2014, 347, 75–78. [Google Scholar] [CrossRef]
- Chan, J.K.; Kawar, N.M.; Shin, J.Y.; Osann, K.; Chen, L.-M.; Powell, C.B.; Kapp, D.S. Endometrial stromal sarcoma: A population-based analysis. Br. J. Cancer 2008, 99, 1210–1215. [Google Scholar] [CrossRef]
- Riopel, J.; Plante, M.; Renaud, M.C.; Roy, M.; Tetu, B. Lymph node metastases in low-grade endometrial stromal sarcoma. Gynecol. Oncol. 2005, 96, 402–406. [Google Scholar] [CrossRef]
- Xie, W.; Cao, D.; Yang, J.; Jiang, X.; Shen, K.; Pan, L.; Huang, H.; Lang, J.; You, Y.; Chen, J. Fertility-Sparing Surgery for Patients with Low-Grade Endometrial Stromal Sarcoma. Oncotarget 2017, 8, 10602–10608. [Google Scholar] [CrossRef] [Green Version]
- Available online: https://www.nccn.org/professionals/physician_gls/pdf/uterine.pdf (accessed on 3 February 2021).
- Rauh-Hain, J.A.; del Carmen, M.G. Endometrial Stromal Sarcoma. Obstet. Gynecol. 2013, 122, 676–683. [Google Scholar] [CrossRef]
- Capozzi, V.A.; Monfardini, L.; Ceni, V.; Cianciolo, A.; Butera, D.; Gaiano, M.; Berretta, R. Endometrial stromal sarcoma: A review of rare mesenchymal uterine neoplasm. J. Obstet. Gynaecol. Res. 2020, 46, 2221–2236. [Google Scholar] [CrossRef]
- Zhang, Y.Y.; Li, Y.; Qin, M.; Cai, Y.; Jin, Y.; Pan, L.Y. High-grade endometrial stromal sarcoma: A retrospective study of factors influencing prognosis. Cancer Manag. Res. 2019, 11, 831–837. [Google Scholar] [CrossRef] [Green Version]
- Ondič, O. High Grade Endometrial Stromal Sarcoma. PathologyOutlines.com Website. Available online: https://www.pathologyoutlines.com/topic/uterusESShighgrade.html (accessed on 8 January 2021).
- Ondič, O.; Bednářová, B.; Ptáková, N.; Hájková, V.; Šteiner, P.; Šidlová, H.; Presl, J.; Bouda, J.; Alaghehbandan, R.; Michal, M. ZC3H7B-BCOR high-grade endometrial stromal sarcoma may present as myoma nascens with cytoplasmic signet ring cell change. Virchows Arch. 2020, 476, 615–619. [Google Scholar] [CrossRef]
- Zhang, Y.; Chen, C.; Ren, M.; Cong, X.; Li, Z.; Yang, L. Treatment of uterine high-grade endometrial stromal sarcoma with apatinib combined with chemotherapy: A case report. Medicine 2019, 98, e15050. [Google Scholar] [CrossRef]
- Chiang, S.; Lee, C.H.; Stewart, C.J.R.; Oliva, E.; Hoang, L.N.; Ali, R.H.; Hensley, M.L.; Iii, J.A.A.-S.; Frosina, D.; Jungbluth, A.A.; et al. BCOR is a robust diagnostic immunohistochemical marker of genetically diverse high-grade endometrial stromal sarcoma, including tumors exhibiting variant morphology. Mod. Pathol. 2017, 30, 1251–1261. [Google Scholar] [CrossRef]
- Lewis, N.; Soslow, R.A.; Delair, D.F.; Park, K.J.; Murali, R.; Hollmann, T.J.; Davidson, B.; Micci, F.; Panagopoulos, I.; Hoang, L.N.; et al. ZC3H7B-BCOR high-grade endometrial stromal sarcomas: A report of 17 cases of a newly defined entity. Mod. Pathol. 2018, 31, 674–684. [Google Scholar] [CrossRef] [Green Version]
- Mariño-Enriquez, A.; Lauria, A.; Przybyl, J.; Ng, T.L.; Kowalewska, M.; Debiec-Rychter, M.; Ganesan, R.; Sumathi, V.; George, S.; McCluggage, W.G.; et al. BCOR Internal Tandem Duplication in High-grade Uterine Sarcomas. Am. J. Surg. Pathol. 2018, 42, 335–341. [Google Scholar] [CrossRef]
- Wu, J.; Zhang, H.; Li, L.; Hu, M.; Chen, L.; Wu, S.; Xu, B.; Song, Q. Prognostic nomogram for predicting survival in patients with high grade endometrial stromal sarcoma: A Surveillance Epidemiology, and End Results database analysis. Int. J. Gynecol. Cancer 2020, 30, 1520–1527. [Google Scholar] [CrossRef]
- Verschoor, A.J.; Warmerdam, F.A.R.M.; Bosse, T.; Bovée, J.V.M.G.; Gelderblom, H. A remarkable response to pazopanib, despite recurrent liver toxicity, in a patient with a high grade endometrial stromal sarcoma, a case report. BMC Cancer 2018, 18, 92. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cabrera, S.; Bebia, V.; Acosta, U.; Franco-Camps, S.; Mañalich, L.; García-Jiménez, A.; Gil-Moreno, A. Survival outcomes and prognostic factors of endometrial stromal sarcoma and undifferentiated uterine sarcoma. Clin. Transl. Oncol. 2020, 23, 1210–1219. [Google Scholar] [CrossRef] [PubMed]
- Desouki, M. Undifferentiated Uterine Sarcoma. PathologyOutlines.com Website. Available online: https://www.pathologyoutlines.com/topic/uterussarcoma.html (accessed on 8 January 2021).
- Momeni-Boroujeni, A.; Chiang, S. Uterine mesenchymal tumours: Recent advances. Histopathology 2020, 76, 64–75. [Google Scholar] [CrossRef] [PubMed]
- Binzer-Panchal, A.; Hardell, E.; Viklund, B.; Ghaderi, M.; Bosse, T.; Nucci, M.R.; Lee, C.-H.; Hollfelder, N.; Corcoran, P.; Gonzalez-Molina, J.; et al. Integrated Molecular Analysis of Undifferentiated Uterine Sarcomas Reveals Clinically Relevant Molecular Subtypes. Clin. Cancer Res. 2019, 25, 2155–2165. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hardell, E.; Josefson, S.; Ghaderi, M.; Skeie-Jensen, T.; Westbom-Fremer, S.; Cheek, E.H.; Bell, D.; Selling, J.; Schoolmeester, J.K.; Måsbäck, A.; et al. Validation of a Mitotic Index Cutoff as a Prognostic Marker in Undifferentiated Uterine Sarcomas. Am. J. Surg. Pathol. 2017, 41, 1231–1237. [Google Scholar] [CrossRef] [PubMed]
- Meurer, M.; Floquet, A.; Ray-Coquard, I.; Bertucci, F.; Auriche, M.; Cordoba, A.; Piperno-Neumann, S.; Salas, S.; Delannes, M.; Chevalier, T.; et al. Localized high grade endometrial stromal sarcoma and localized undiferentiated uterine sarcoma: A retrospective series of the French Sarcoma Group. Int. J. Gynecol. Cancer 2019, 29, 691–698. [Google Scholar] [CrossRef]
- Yuan, Z.; Cao, D.; Yu, M.; Shen, K.; He, Y. Uterine and Cervical Adenosarcoma: A Retrospective Study of Overall Oncologic Outcomes and Fertility Preservation in Early-Stage Disease. Oncologist 2019, 24, e870–e879. [Google Scholar] [CrossRef] [Green Version]
- Tate, K.; Watanabe, R.; Yoshida, H.; Shimizu, H.; Uehara, T.; Ishikawa, M.; Ikeda, S.-I.; Hiraoka, N.; Kato, T. Uterine adenosarcoma in Japan: Clinicopathologic features, diagnosis and management. Asia-Pac. J. Clin. Oncol. 2018, 14, 318–325. [Google Scholar] [CrossRef]
- Ulrich, U.A.; Denschlag, D. Uterine Adenosarcoma. Oncol. Res. Treat. 2018, 41, 693–696. [Google Scholar] [CrossRef]
- Nathenson, M.J.; Ravi, V.; Fleming, N.; Wang, W.L.; Conley, A. Uterine Adenosarcoma: A Review. Curr. Oncol. Rep. 2016, 18, 68. [Google Scholar] [CrossRef]
- Lee, S.J.; Park, J.Y. A Rare Case of Intramural Müllerian Adenosarcoma Arising from Adenomyosis of the Uterus. J. Pathol. Transl. Med. 2017, 51, 433–440. [Google Scholar] [CrossRef]
- Vara, A.R.; Ruzics, E.P.; Moussabeck, O.; Martin, D.C. Endometrioidadenosarcoma of the bladder arising from endometriosis. J. Urol. 1990, 143, 813–815. [Google Scholar] [CrossRef]
- Yang, F.; Yang, K.X.; Yao, X.Y.; Gong, J.; Song, B. Adenosarcoma arising in abdominal scar endometriosis: Report of a case. Zhonghua Bing Li Xue Za Zhi 2008, 37, 643–644. [Google Scholar]
- Piscuoglio, S.; Burke, K.A.; Ng, C.K.; Papanastasiou, A.D.; Geyer, F.C.; Macedo, G.S.; Martelotto, L.G.; de Bruijn, I.; De Filippo, M.R.; Schultheis, A.M.; et al. Uterine adenosarcomas are mesenchymal neoplasms. J. Pathol. 2016, 238, 381–388. [Google Scholar] [CrossRef]
- Pinto, A.; Howitt, B. Uterine Adenosarcoma. Arch. Pathol. Lab. Med. 2016, 140, 286–290. [Google Scholar] [CrossRef] [Green Version]
- Özen, Ö. Müllerian Adenosarcoma. PathologyOutlines.com Website. Available online: https://www.pathologyoutlines.com/topic/uterusadenosarcoma.html (accessed on 9 January 2021).
- Nathenson, M.J.; Conley, A.P. Prognostic factors for uterine adenosarcoma: A review. Expert Rev. Anticancer Ther. 2018, 18, 1093–1100. [Google Scholar] [CrossRef]
- Lee, Y.J.; Kim, D.Y.; Suh, D.S.; Kim, J.H.; Kim, Y.M.; Kim, Y.T.; Nam, J.H. Feasibility of uterine preservation in the management of early-stage uterine adenosarcomas: A single institute experience. World J. Surg. Oncol. 2017, 15, 87. [Google Scholar] [CrossRef]
- L’Heveder, A.; Jones, B.P.; Saso, S.; Barcroft, J.; Richardson, R.; Kaur, B.; Ghaem-Maghami, S.; Yazbek, J.; Smith, J.R. Conservative management of uterine adenosarcoma: Lessons learned from 20 years of follow-up. Arch. Gynecol. Obstet. 2019, 300, 1383–1389. [Google Scholar] [CrossRef] [Green Version]
- Tanner, E.J.; Toussaint, T.; Leitao, M.M., Jr.; Hensley, M.L.; Soslow, R.A.; Gardner, G.J.; Jewell, E.L. Management of uterine adenosarcomas with and without sarcomatous overgrowth. Gynecol. Oncol. 2013, 129, 140–144. [Google Scholar] [CrossRef]

| Prognostic Factors | Favorable | Unfavorable |
|---|---|---|
| Initial tumor stage | Early | Advanced |
| Patient’s age | <50 years | >50 years |
| Mitotic count | <10 mitoses | >10 mitoses |
| Tumor size | <10 cm | >10 cm |
| Tumor margins | Negative | Positive |
| Race | White | Afro-American |
| Vascular space involvement | No | Yes |
| Oestrogen/Progesterone receptors | Yes | No |
| Ki-67 expression | Low | High |
| P-53 expression | No | Yes |
| P-16 overexpression | No | Yes |
| Morcellation | No | Yes |
| Cervical invasion | No | Yes |
| Locoregional metastasis | No | Yes |
| Distant metastasis | No | Yes |
| Bcl-2 expression | Yes | No |
| Percentage of necrosis | Low | High |
| Stage I | Tumor confined to the uterus |
| IA | Less than 5 cm |
| IB | More than 5 cm |
| Stage II | Tumor extends beyond the uterus, within the pelvis |
| IIA | Adnexal involvement |
| IIB | Involvement of other pelvic tissues |
| Stage III | Tumor infiltrates abdominal tissues (lesions must not just protrude into abdominal cavity) |
| IIIA | Tumor infiltrates abdominal tissues in 1 site |
| IIIB | Tumor infiltrates abdominal tissues in > 1 site |
| IIIC | Pelvic and/or para-aortic lymph nodes involvement |
| Stage IV | |
| IVA | Tumor invades the bladder and/or the rectum |
| IVB | Distant metastasis |
| Prognostic Factors | Favorable | Unfavorable |
|---|---|---|
| Patient’s age | <53 | >53 |
| Initial tumor stage | Early | Advanced |
| Sarcomatous overgrowth | No | Yes |
| Myometrial invasion | No, or <50% | >50% |
| Morcellation | No | Yes |
| Lymph node involvement | No | Yes |
| Lymphovascular invasion | No | Yes |
| Tumor necrosis * | No | Yes |
| Cellular atypia * | Mild | Severe |
| Stage I | Tumor confined to the uterus |
| IA | Tumor confined to endometrium/endocervix with no myometrial invasion |
| IB | <50% myometrial invasion |
| IC | >50% myometrial invasion |
| Stage II | Tumor extends beyond the uterus, within the pelvis |
| IIA | Adnexal involvement |
| IIB | Other pelvic structures involvement |
| Stage III | Tumor infiltrates abdominal tissues (lesions must not just protrude into abdominal cavity) |
| IIIA | Tumor infiltrates abdominal tissues in one site |
| IIIB | Tumor infiltrates abdominal tissues in > one site |
| IIIC | Pelvic and/or para-aortic lymph nodes involvement |
| Stage IV | |
| IVA | Tumor invades bladder and/or rectum |
| IVB | Distant metastasis |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kostov, S.; Kornovski, Y.; Ivanova, V.; Dzhenkov, D.; Metodiev, D.; Watrowski, R.; Ivanova, Y.; Slavchev, S.; Mitev, D.; Yordanov, A. New Aspects of Sarcomas of Uterine Corpus—A Brief Narrative Review. Clin. Pract. 2021, 11, 878-900. https://doi.org/10.3390/clinpract11040103
Kostov S, Kornovski Y, Ivanova V, Dzhenkov D, Metodiev D, Watrowski R, Ivanova Y, Slavchev S, Mitev D, Yordanov A. New Aspects of Sarcomas of Uterine Corpus—A Brief Narrative Review. Clinics and Practice. 2021; 11(4):878-900. https://doi.org/10.3390/clinpract11040103
Chicago/Turabian StyleKostov, Stoyan, Yavor Kornovski, Vesela Ivanova, Deyan Dzhenkov, Dimitar Metodiev, Rafał Watrowski, Yonka Ivanova, Stanislav Slavchev, Dimitar Mitev, and Angel Yordanov. 2021. "New Aspects of Sarcomas of Uterine Corpus—A Brief Narrative Review" Clinics and Practice 11, no. 4: 878-900. https://doi.org/10.3390/clinpract11040103
APA StyleKostov, S., Kornovski, Y., Ivanova, V., Dzhenkov, D., Metodiev, D., Watrowski, R., Ivanova, Y., Slavchev, S., Mitev, D., & Yordanov, A. (2021). New Aspects of Sarcomas of Uterine Corpus—A Brief Narrative Review. Clinics and Practice, 11(4), 878-900. https://doi.org/10.3390/clinpract11040103









