Platelet Microvesicles, Inflammation, and Coagulation Markers: A Pilot Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Sample Collection and Storage
2.3. Measurements
2.4. Microvesicles Determination
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Wolf, P. The nature and significance of platelet products in human plasma. Br. J. Haematol. 1967, 13, 269–288. [Google Scholar] [CrossRef] [PubMed]
- Sims, P.J.; Faioni, E.; Wiedmer, T.; Shattil, S. Complement proteins C5b-9 cause release of membrane vesicles from the platelet surface that are enriched in the membrane receptor for coagulation factor Va and express prothrombinase activity. J. Biol. Chem. 1988, 263, 18205–18212. [Google Scholar] [CrossRef] [PubMed]
- Ratajczak, M.Z.; Ratajczak, D.; Pedziwiatr, D. Extracellular Microvesicles (ExMVs) in Cell to Cell Communication: A Role of Telocytes. Adv. Exp. Med. Biol. 2016, 913, 41–49. [Google Scholar] [CrossRef]
- Ratajczak, M.Z.; Ratajczak, J. Extracellular Microvesicles as Game Changers in Better Understanding the Complexity of Cellular Interactions-From Bench to Clinical Applications. Am. J. Med. Sci. 2017, 354, 449–452. [Google Scholar] [CrossRef] [PubMed]
- Giesen, P.L.A.; Rauch, U.; Bohrmann, B.; Kling, D.; Roqué, M.; Fallon, J.T.; Badimon, J.J.; Himber, J.; Riederer, M.A.; Nemerson, Y. Blood-borne tissue factor: Another view of thrombosis. Proc. Natl. Acad. Sci. USA 1999, 96, 2311–2315. [Google Scholar] [CrossRef]
- Haze, T.; Sugiyama, M.; Higuchi, M.; Asayama, H.; Karitani, Y.; Nishikawa, T.; Yamashita, K.; Nagami, S.; Nakayama, T.; Kanatani, K.; et al. Level, distribution and correlates of platelet-derived microparticles in healthy individuals with special reference to the metabolic syndrome. Thromb. Haemost. 2008, 100, 280–285. [Google Scholar] [CrossRef]
- Ueba, T.; Nomura, S.; Inami, N.; Nishikawa, T.; Kajiwara, M.; Iwata, R.; Yamashita, K. Plasma level of platelet-derived microparticles is associated with coronary heart disease risk score in healthy men. J. Atheroscler. Thromb. 2010, 17, 342–349. [Google Scholar] [CrossRef][Green Version]
- Wang, L.; Bi, Y.; Yu, M.; Li, T.; Tong, D.; Yang, X.; Zhang, C.; Guo, L.; Wang, C.; Kou, Y.; et al. Phosphatidylserine-exposing blood cells and microparticles induce procoagulant activity in non-valvular atrial fibrillation. Int. J. Cardiol. 2018, 258, 138–143. [Google Scholar] [CrossRef]
- Zhao, L.; Wu, X.; Si, Y.; Yao, Z.; Dong, Z.; Novakovic, V.A.; Guo, L.; Tong, D.; Chen, H.; Bi, Y.; et al. Increased blood cell phosphatidylserine exposure and circulating microparticles contribute to procoagulant activity after carotid artery stenting. J. Neurosurg. 2017, 127, 1041–1054. [Google Scholar] [CrossRef]
- Jamaly, S.; Basavaraj, M.G.; Starikova, I.; Olsen, R.; Brækkan, S.K.; Hansen, J. Elevated plasma levels of P-selectin glycoprotein ligand-1-positive microvesicles in patients with unprovoked venous thromboembolism. J. Thromb. Haemost. 2018, 16, 1546–1554. [Google Scholar] [CrossRef]
- Bal, L.; Ederhy, S.; Di Angelantonio, E.; Toti, F.; Zobairi, F.; Dufaitre, G.; Meuleman, C.; Mallat, Z.; Boccara, F.; Tedgui, A.; et al. Circulating procoagulant microparticles in acute pulmonary embolism: A case-control study. Int. J. Cardiol. 2010, 145, 321–322. [Google Scholar] [CrossRef] [PubMed]
- Gidaro, A.; Manetti, R.; Delitala, A.P.; Soloski, M.J.; Deliliers, G.L.; Castro, D.; Soldini, D.; Castelli, R. Incidence of Venous Thromboembolism in Multiple Myeloma Patients across Different Regimens: Role of Procoagulant Microparticles and Cytokine Release. J. Clin. Med. 2022, 11, 2720. [Google Scholar] [CrossRef] [PubMed]
- Aatonen, M.; Grönholm, M.; Siljander, P.R. Platelet-derived microvesicles: Multitalented participants in intercellular communication. Semin. Thromb. Hemost. 2012, 38, 102–113. [Google Scholar] [CrossRef] [PubMed]
- Nomura, S.; Tandon, N.N.; Nakamura, T.; Cone, J.; Fukuhara, S.; Kambayashi, J. High-shear-stress-induced activation of platelets and microparticles enhances expression of cell adhesion molecules in THP-1 and endothelial cells. Atherosclerosis 2001, 158, 277–287. [Google Scholar] [CrossRef] [PubMed]
- Boilard, E.; Nigrovic, P.A.; Larabee, K.; Watts, G.F.M.; Coblyn, J.S.; Weinblatt, M.E.; Massarotti, E.M.; Remold-O’Donnell, E.; Farndale, R.W.; Ware, J.; et al. Platelets Amplify Inflammation in Arthritis via Collagen-Dependent Microparticle Production. Science 2010, 327, 580–583. [Google Scholar] [CrossRef] [PubMed]
- Viñuela-Berni, V.; Doníz-Padilla, L.; Figueroa-Vega, N.; Portillo-Salazar, H.; Abud-Mendoza, C.; Baranda, L.; González-Amaro, R. Proportions of several types of plasma and urine microparticles are increased in patients with rheumatoid arthritis with active disease. Clin. Exp. Immunol. 2015, 180, 442–451. [Google Scholar] [CrossRef]
- Hooten, N.N.; McFarland, M.H.; Freeman, D.W.; Mode, N.A.; Ezike, N.; Zonderman, A.B.; Evans, M.K. Association of Extracellular Vesicle Protein Cargo with Race and Clinical Markers of Mortality. Sci. Rep. 2019, 9, 17582. [Google Scholar] [CrossRef]
- Wu, Y.; Liu, W.; Zhou, Y.; Hilton, T.; Zhao, Z.; Wang, M.; Yeon, J.; Houck, K.; Thiagarajan, P.; Zhang, F.; et al. von Willebrand factor enhances microvesicle-induced vascular leakage and coagulopathy in mice with traumatic brain injury. Blood 2018, 132, 1075–1084. [Google Scholar] [CrossRef]
- Tian, Y.; Salsbery, B.; Wang, M.; Yuan, H.; Yang, J.; Zhao, Z.; Wu, X.; Zhang, Y.; Konkle, B.A.; Thiagarajan, P.; et al. Brain derived microparticles induce systemic coagulation in a murine model of traumatic brain injury. Blood 2015, 125, 2151–2159. [Google Scholar] [CrossRef]
- Dong, J.-F.; Moake, J.L.; Nolasco, L.; Bernardo, A.; Arceneaux, W.; Shrimpton, C.N.; Schade, A.J.; McIntire, L.V.; Fujikawa, K.; López, J.A. ADAMTS-13 rapidly cleaves newly secreted ultralarge von Willebrand factor multimers on the endothelial surface under flowing conditions. Blood 2002, 100, 4033–4039. [Google Scholar] [CrossRef]
- Zarà, M.; Guidetti, G.F.; Camera, M.; Canobbio, I.; Amadio, P.; Torti, M.; Tremoli, E.; Barbieri, S.S. Biology and Role of Extracellular Vesicles (EVs) in the Pathogenesis of Thrombosis. Int. J. Mol. Sci. 2019, 20, 2840. [Google Scholar] [CrossRef]
- Morel, O.; Pereira, B.; Averous, G.; Faure, A.; Jesel, L.; Germain, P.; Grunebaum, L.; Ohlmann, P.; Freyssinet, J.M.; Bareiss, P.; et al. Increased levels of procoagulant tissue factor-bearing microparticles within the occluded coronary artery of patients with ST-segment elevation myocardial infarction: Role of endothelial damage and leukocyte activation. Atherosclerosis 2009, 204, 636–641. [Google Scholar] [CrossRef]
- Brodsky, S.V.; Malinowski, K.; Golightly, M.; Jesty, J.; Goligorsky, M.S. Plasminogen activator inhibitor-1 promotes formation of endothelial microparticles with procoagulant potential. Circulation 2002, 106, 2372–2378. [Google Scholar] [CrossRef]
- Peterson, D.B.; Sander, T.; Kaul, S.; Wakim, B.T.; Halligan, B.; Twigger, S.; Pritchard, K.A.; Oldham, K.T.; Ou, J.-S. Comparative proteomic analysis of PAI-1 and TNF-alpha-derived endothelial microparticles. Proteomics 2008, 8, 2430–2446. [Google Scholar] [CrossRef]
- Sebbagh, M.; Renvoizé, C.; Hamelin, J.; Riché, N.; Bertoglio, J.; Bréard, J. Caspase-3-mediated cleavage of ROCK I induces MLC phosphorylation and apoptotic membrane blebbing. Nat. Cell Biol. 2001, 3, 346–352. [Google Scholar] [CrossRef]
- Totsukawa, G.; Yamakita, Y.; Yamashiro, S.; Hartshorne, D.J.; Sasaki, Y.; Matsumura, F. Distinct roles of ROCK (Rho-kinase) and MLCK in spatial regulation of MLC phosphorylation for assembly of stress fibers and focal adhesions in 3T3 fibroblasts. J. Cell Biol. 2000, 150, 797–806. [Google Scholar] [CrossRef]
- Cartier-Michaud, A.; Malo, M.; Charrière-Bertrand, C.; Gadea, G.; Anguille, C.; Supiramaniam, A.; Lesne, A.; Delaplace, F.; Hutzler, G.; Roux, P.; et al. Matrix-bound PAI-1 supports cell blebbing via RhoA/ROCK1 signaling. PLOS ONE 2012, 7, e32204. [Google Scholar] [CrossRef]
- Zhu, J.; Xie, R.; Piao, X.; Hou, Y.; Zhao, C.; Qiao, G.; Yang, B.; Shi, J.; Lu, Y. Homocysteine enhances clot-promoting activity of endothelial cells via phosphatidylserine externalization and microparticles formation. Amino Acids 2012, 43, 1243–1250. [Google Scholar] [CrossRef]
- Xie, R.; Jia, D.; Gao, C.; Zhou, J.; Sui, H.; Wei, X.; Zhang, T.; Han, Y.; Shi, J.; Bai, Y. Homocysteine induces procoagulant activity of red blood cells via phosphatidylserine exposure and microparticles generation. Amino Acids 2014, 46, 1997–2004. [Google Scholar] [CrossRef] [PubMed]
- Kuriyama, N.; Nagakane, Y.; Hosomi, A.; Ohara, T.; Kasai, T.; Harada, S.; Takeda, K.; Yamada, K.; Ozasa, K.; Tokuda, T.; et al. Evaluation of factors associated with elevated levels of platelet-derived microparticles in the acute phase of cerebral infarction. Clin. Appl. Thromb. 2010, 16, 26–32. [Google Scholar] [CrossRef] [PubMed]
- Pawelczyk, M.; Kaczorowska, B.; Baj, Z. Fibrinogen concentrations in ischaemic stroke patients with metabolic disorders. Neurol. Neurochir. Polska 2020, 54, 259–264. [Google Scholar] [CrossRef]
- Campello, E.; Spiezia, L.; Radu, C.M.; Bulato, C.; Gavasso, S.; Tormene, D.; Woodhams, B.; Valle, F.D.; Simioni, P. Circulating microparticles and the risk of thrombosis in inherited deficiencies of antithrombin, protein C and protein S. Thromb. Haemost. 2016, 115, 81–88. [Google Scholar] [CrossRef]
- Stavenuiter, F.; Davis, N.F.; Duan, E.; Gale, A.J.; Heeb, M.J. Platelet protein S directly inhibits procoagulant activity on platelets and microparticles. Thromb. Haemost. 2013, 109, 229–237. [Google Scholar] [CrossRef]
- Somajo, S.; Koshiar, R.L.; Norström, E.; Dahlbäck, B. Protein S and factor V in regulation of coagulation on platelet microparticles by activated protein C. Thromb. Res. 2014, 134, 144–152. [Google Scholar] [CrossRef]
- Faizullin, D.; Valiullina, Y.; Salnikov, V.; Zuev, Y. Direct interaction of fibrinogen with lipid microparticles modulates clotting kinetics and clot structure. Nanomedicine 2020, 23, 102098. [Google Scholar] [CrossRef]
- Orbe, J.; Alexandru, N.; Roncal, C.; Belzunce, M.; Bibiot, P.; Rodriguez, J.A.; Meijers, J.C.; Georgescu, A.; Paramo, J.A. Lack of TAFI increases brain damage and microparticle generation after thrombolytic therapy in ischemic stroke. Thromb. Res. 2015, 136, 445–450. [Google Scholar] [CrossRef]
- Gidaro, A.; Manetti, R.; Delitala, A.P.; Salvi, E.; Bergamaschini, L.; Vidili, G.; Castelli, R. Prothrombotic and Inflammatory Markers in Elderly Patients with Non-Alcoholic Hepatic Liver Disease before and after Weight Loss: A Pilot Study. J. Clin. Med. 2021, 10, 4906. [Google Scholar] [CrossRef]
- Théry, C.; Witwer, K.W.; Aikawa, E. Minimal information for studies of extracellular vesicles 2018 (MISEV2018): A position statement of the International Society for Extracellular Vesicles and update of the MISEV2014 guidelines. J. Extracell. Vesicles 2018, 7, 1535750. [Google Scholar] [CrossRef] [PubMed]
- Snir, O.; Wilsgård, L.; Latysheva, N.; Wahlund, C.J.E.; Brækkan, S.K.; Hindberg, K.; Hansen, J. Plasma levels of platelet-derived microvesicles are associated with risk of future venous thromboembolism. J. Thromb. Haemost. 2022, 20, 899–908. [Google Scholar] [CrossRef] [PubMed]
- Mameli, A.; Barcellona, D.; Marongiu, F. Rheumatoid arthritis and thrombosis. Clin. Exp. Rheumatol. 2009, 27, 846–855. [Google Scholar] [PubMed]
- Garcia-Romero, N.; Esteban-Rubio, S.; Rackov, G.; Carrión-Navarro, J.; Belda-Iniesta, C.; Ayuso-Sacido, A. Extracellular vesicles compartment in liquid biopsies: Clinical application. Mol. Asp. Med. 2018, 60, 27–37. [Google Scholar] [CrossRef] [PubMed]
- Gustafson, C.M.; Shepherd, A.J.; Miller, V.M.; Jayachandran, M. Age- and sex-specific differences in blood-borne microvesicles from apparently healthy humans. Biol. Sex Differ. 2015, 6, 10. [Google Scholar] [CrossRef] [PubMed]
- Wolberg, A.S.; Rosendaal, F.R.; Weitz, J.I.; Jaffer, I.H.; Agnelli, G.; Baglin, T.; Mackman, N. Venous thrombosis. Nat. Rev. Dis. Prim. 2015, 1, 15006. [Google Scholar] [CrossRef] [PubMed]
- Castelli, R.; Gidaro, A.; Casu, G.; Merella, P.; Profili, N.I.; Donadoni, M.; Maioli, M.; Delitala, A.P. Aging of the Arterial System. Int. J. Mol. Sci. 2023, 24, 6910. [Google Scholar] [CrossRef]
- Cesari, M.; Pahor, M.; Incalzi, R.A. Plasminogen activator inhibitor-1 (PAI-1): A key factor linking fibrinolysis and age-related subclinical and clinical conditions. Cardiovasc. Ther. 2010, 28, e72–e91. [Google Scholar] [CrossRef]
- Cugno, M.; Castelli, R.; Mari, D.; Mozzi, E.; Zappa, M.A.; Boscolo-Anzoletti, M.; Roviaro, G.; Mannucci, P.M. Inflammatory and prothrombotic parameters in normotensive non-diabetic obese women: Effect of weight loss obtained by gastric banding. Intern. Emerg. Med. 2011, 7, 237–242. [Google Scholar] [CrossRef]
- Yamaguchi, R.; Sakamoto, A.; Yamaguchi, R.; Haraguchi, M.; Narahara, S.; Sugiuchi, H.; Yamaguchi, Y. Di-(2-Ethylhexyl) Phthalate Promotes Release of Tissue Factor-Bearing Microparticles from Macrophages via the TGFβ1/Smad/PAI-1 Signaling Pathway. Am. J. Med. Sci. 2019, 357, 492–506. [Google Scholar] [CrossRef]

| A. Whole Population | B. Individuals with MVs ≤ 700 kMP | C. Individuals with MVs > 700 kMP | p-Value B vs. C | |
|---|---|---|---|---|
| Number of patients | 246 | 169 | 77 | |
| Age (years) | 65 (54–72) | 61 (48–68) | 72 (70–73) | <0.001 |
| Gender male/female | 161/85 | 136/73 | 25/12 | 0.85 |
| Body mass index (BMI) | 23.7 (21.5–24.8) | 23.5 (21.4–24.6) | 23.8 (21.6–24.9) | 0.85 |
| Median follow-up (months) | 40.1 (27–51) | 40.2 (28–51) | 39.9 (27–49) | 0.64 |
| Venous thromboembolism | 3/246 | 0/169 | 3/77 | 0.03 |
| CRP (mg/L) 0.5–10 mg/L | 6 (3–12) | 4 (2.3–8) | 7 (5–9) | <0.001 |
| Fibrinogen (mg/dL) 200–400 mg/dL | 262 (117–321) | 134 (109–256) | 340 (300–435) | <0.001 |
| Fibrinogen > 400 mg/dL | 28 | 1 (3.6%) | 27 (96.4%) | <0.001 |
| PAI-1 (UI/mL) 5–40 UI/mL | 20.0 (12.0–26.25) | 15 (4–20) | 36 (25–46) | <0.001 |
| PAI-1 > 40 UI/mL | 27 | 1 (3.7%) | 26 (96.3%) | <0.001 |
| vWF (%) 60–160% | 68 (62–120) | 64 (58–68) | 140 (111–164) | <0.001 |
| vWF > 160% | 23 | 1 (4.4%) | 22 (95.6%) | <0.001 |
| FVII (%) 65–140% | 67 (52–110) | 54 (40–67) | 150 (120–160) | <0.001 |
| F VII > 140% | 50 | 1 (2%) | 49 (98%) | <0.001 |
| Homocysteine (µmol/L) 4–14 µmol/L | 8 (4–14) | 5 (3–6) | 18 (14–22) | <0.001 |
| Homocysteine > 14 µmol/L | 58 | 7 (12.1%) | 51 (87.9%) | <0.001 |
| TAFI (%) 75–275% | 117 (80–132) | 127 (115–138) | 78 (66–84) | <0.001 |
| TAFI < 75% | 35 | 1 (2.9%) | 34 (97.1%) | <0.001 |
| Protein S (%) 60–130% | 56 (44–67) | 65 (46–68) | 46 (43–48) | <0.001 |
| Protein S <60% | 115 | 47 (40.9%) | 68 (59.1%) | <0.001 |
| IL6 (pg/mL) 0.64–10 pg/mL | 2 (4–12) | 4 (2–5) | 20 (12–30) | <0.001 |
| IL6 (pg/mL) > 10 pg/mL | 64 | 4 (6.3%) | 60 (93.7%) | <0.001 |
| IL10 (pg/mL) 2.6–20 pg/mL | 12 (12–18) | 12 (12–12) | 22 (18–26) | <0.001 |
| IL10 (pg/mL) > 20 pg/mL | 42 | 0 | 42 (100%) | <0.001 |
| IL17 (pg/mL) 1.3–20 pg/mL | 20 (18–22) | 20 (18–20) | 22 (20–24) | <0.001 |
| IL17 (pg/mL) > 20 pg/mL | 71 | 26 (36.7%) | 45 (63.3%) | <0.001 |
| TGF-β (pg/mL) 10–2500 pg/mL | 367 (311–2348) | 321 (307–498) | 2424 (2280–2512) | <0.001 |
| TGFβ (pg/mL) > 2500 pg/mL | 21 | 2 (9.6%) | 19 (90.4%) | <0.001 |
| A: Univariate Analysis p-Value | B: Univariate Analysis Pearson Correlation | C: Linear Regression Model p-Value | D: B (95% CI) | |
|---|---|---|---|---|
| Age (year) | <0.001 | 0.574 | 0.008 | 3.23 (0.84–5.62) |
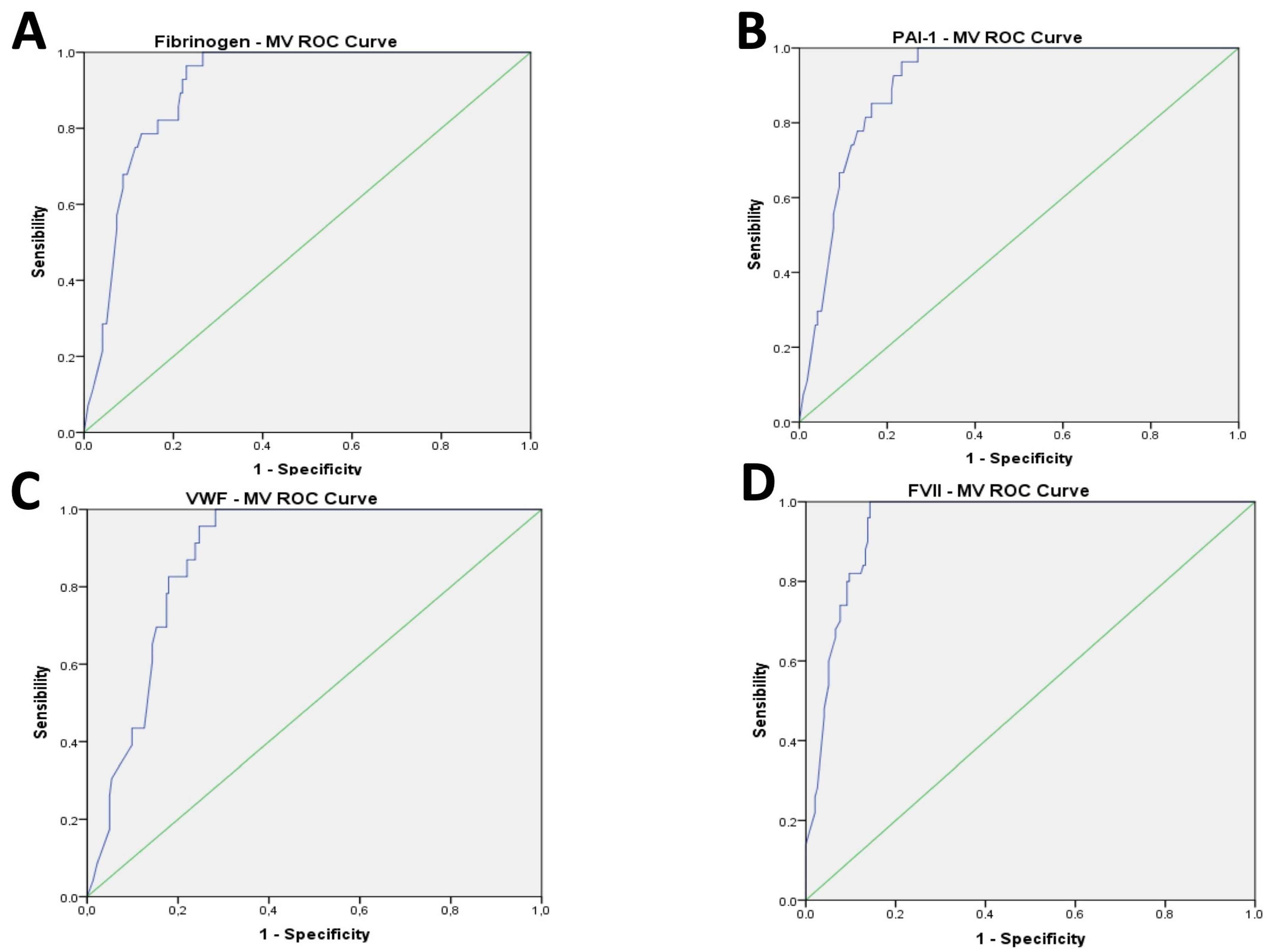
| Fibrinogen (mg/dL) | <0.001 | 0.647 | 0.019 | 0.4 (0.07–0.74) |
| PAI-1 (UI/mL) | <0.001 | 0.683 | 0.002 | 4.16 (1.5–6.82) |
| vWF (%) | <0.001 | 0.834 | 0.018 | 1.91 (0.34–3.48) |
| F VII (%) | <0.001 | 0.744 | 0.001 | 1.47 (0.64–2.3) |
| Homocysteine (µmol/L) | <0.001 | 0.639 | <0.001 | 6.76 (3.36–10.16) |
| TAFI (%) | <0.001 | −0.69 | <0.001 | −3.06 (−4.22–−1.89) |
| Protein S (%) | <0.001 | −0.451 | ≤0.001 | −4.21 (−6.16–−2.27) |
| A: Univariate Analysis p-Value | B: Univariate Analysis Pearson Correlation | C: Linear Regression Model p-Value | D: B (95% CI) | |
|---|---|---|---|---|
| Age (year) | <0.001 | 0.574 | 0.195 | 1.33 (−0.69–3.34) |
| CRP (mg/dL) | <0.001 | 0.406 | 0.514 | 1.54 (−6.48–3.41) |
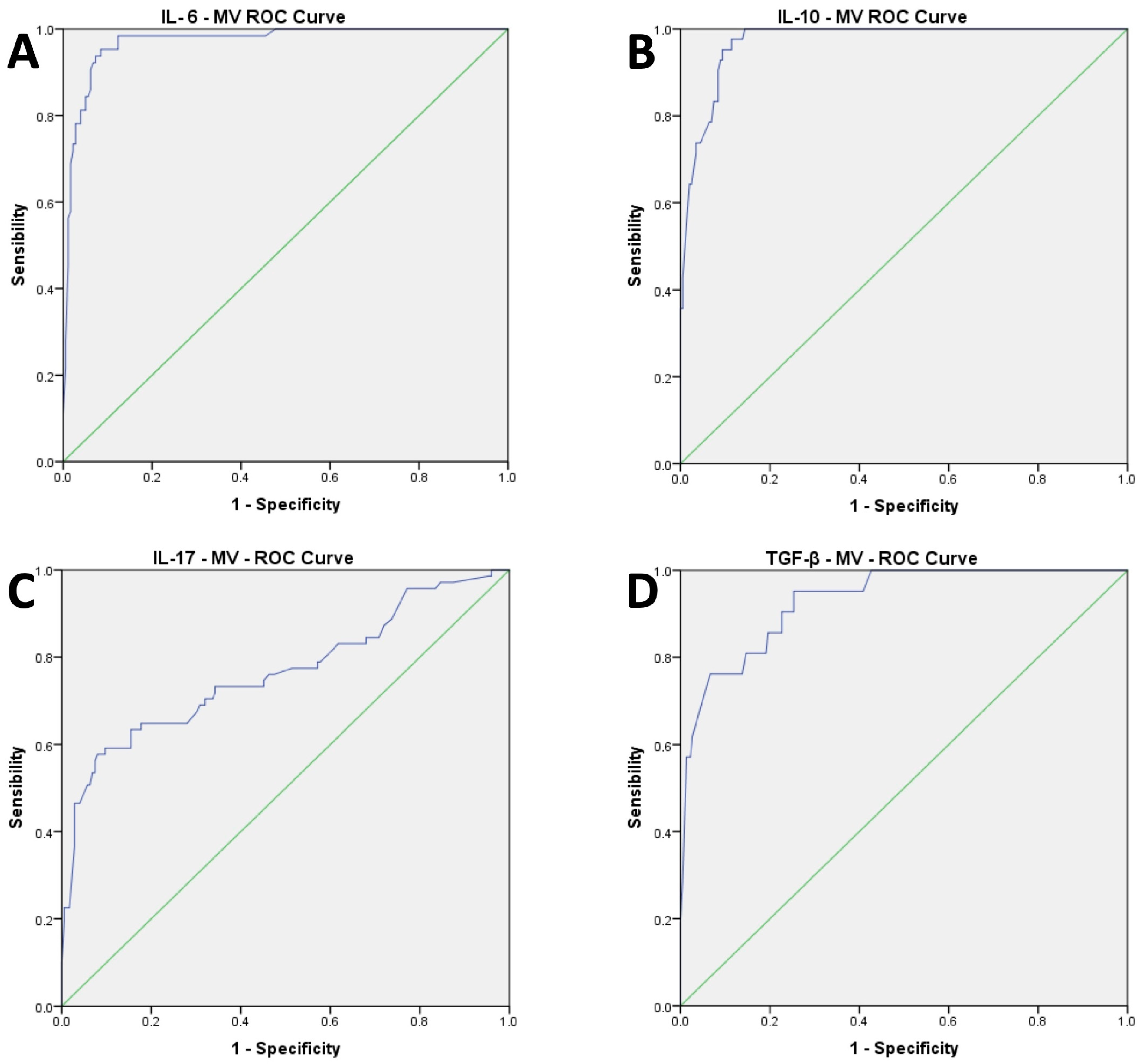
| TGF-β (pg/mL) | <0.001 | 0.843 | >0.001 | 0.141 (0.1–0.18) |
| IL-6 (pg/mL) | <0.001 | 0.850 | >0.001 | 14.3 (9.6–19) |
| IL-10 (pg/mL) | <0.001 | 0.816 | >0.001 | 21.6 (15.5–27.8) |
| IL-17 (pg/mL) | <0.001 | 0.456 | 0.02 | 13.3 (2.1–24.5) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gidaro, A.; Delitala, A.P.; Manetti, R.; Caccia, S.; Soloski, M.J.; Lambertenghi Deliliers, G.; Castro, D.; Donadoni, M.; Bartoli, A.; Sanna, G.; et al. Platelet Microvesicles, Inflammation, and Coagulation Markers: A Pilot Study. Hematol. Rep. 2023, 15, 684-695. https://doi.org/10.3390/hematolrep15040069
Gidaro A, Delitala AP, Manetti R, Caccia S, Soloski MJ, Lambertenghi Deliliers G, Castro D, Donadoni M, Bartoli A, Sanna G, et al. Platelet Microvesicles, Inflammation, and Coagulation Markers: A Pilot Study. Hematology Reports. 2023; 15(4):684-695. https://doi.org/10.3390/hematolrep15040069
Chicago/Turabian StyleGidaro, Antonio, Alessandro Palmerio Delitala, Roberto Manetti, Sonia Caccia, Mark J. Soloski, Giorgio Lambertenghi Deliliers, Dante Castro, Mattia Donadoni, Arianna Bartoli, Giuseppe Sanna, and et al. 2023. "Platelet Microvesicles, Inflammation, and Coagulation Markers: A Pilot Study" Hematology Reports 15, no. 4: 684-695. https://doi.org/10.3390/hematolrep15040069
APA StyleGidaro, A., Delitala, A. P., Manetti, R., Caccia, S., Soloski, M. J., Lambertenghi Deliliers, G., Castro, D., Donadoni, M., Bartoli, A., Sanna, G., Bergamaschini, L., & Castelli, R. (2023). Platelet Microvesicles, Inflammation, and Coagulation Markers: A Pilot Study. Hematology Reports, 15(4), 684-695. https://doi.org/10.3390/hematolrep15040069









