Hybrid Nanobeads for Oral Indomethacin Delivery
Abstract
:1. Introduction
2. Materials and Methods
2.1. Materials
2.2. Preparation of NLC Formulations Loading Indomethacin
2.3. Structural Characterization
2.4. Long-Term Physicochemical Stability
2.5. Transmission Electron Microscopy
2.6. Determination of Indomethacin Encapsulation Efficiency
2.7. In Vitro Cell Viability Test
2.8. Preparation of Biopolymers and Nanobeads Loading Indomethacin
2.9. FE-SEM Analyses of Beads and Nanobeads
2.10. Differential Scanning Calorimetry
2.11. In Vitro Water Uptake of Beads and Nanobeads
2.12. In Vitro Indomethacin Release Test
2.13. In Vivo Toxicity Assays through Chicken Embryo Model
2.14. Preparation of Eggs
2.15. CE Viability Test
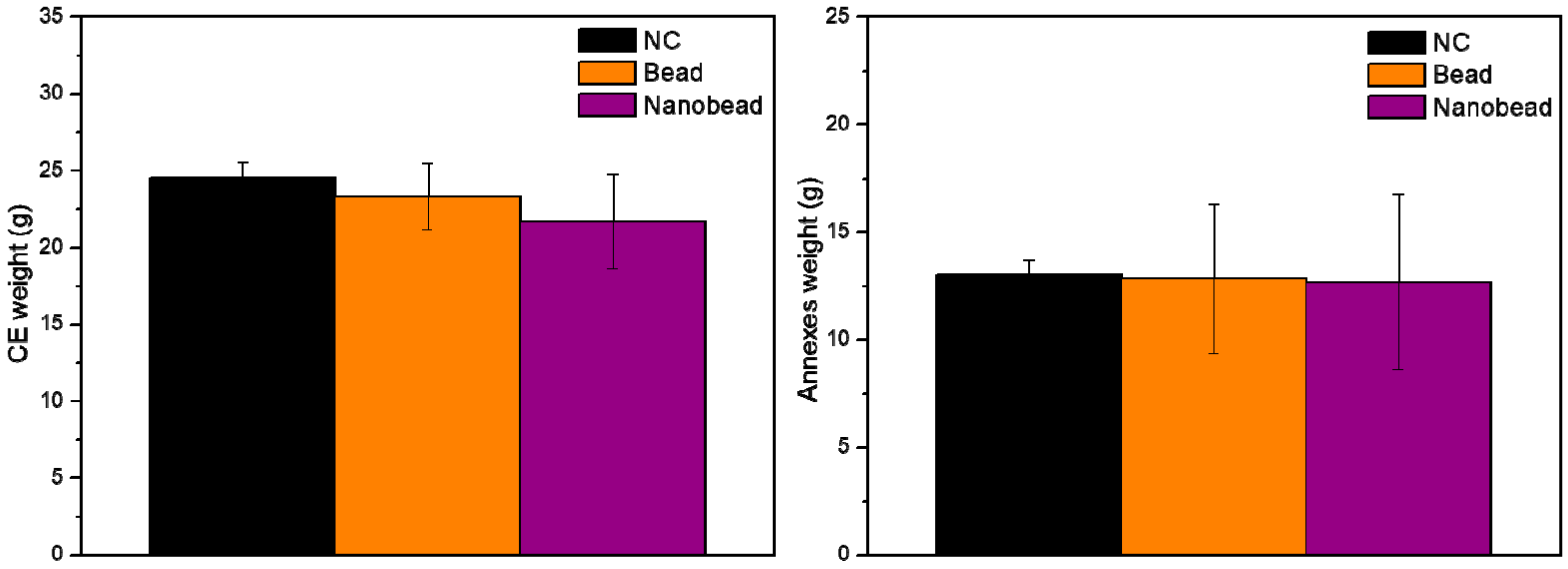
2.16. Changes in the Weights of CE and Annexes
2.17. Biochemical Markers
3. Results
3.1. Preparation of Nanostructured Lipid Carriers Loading Indomethacin
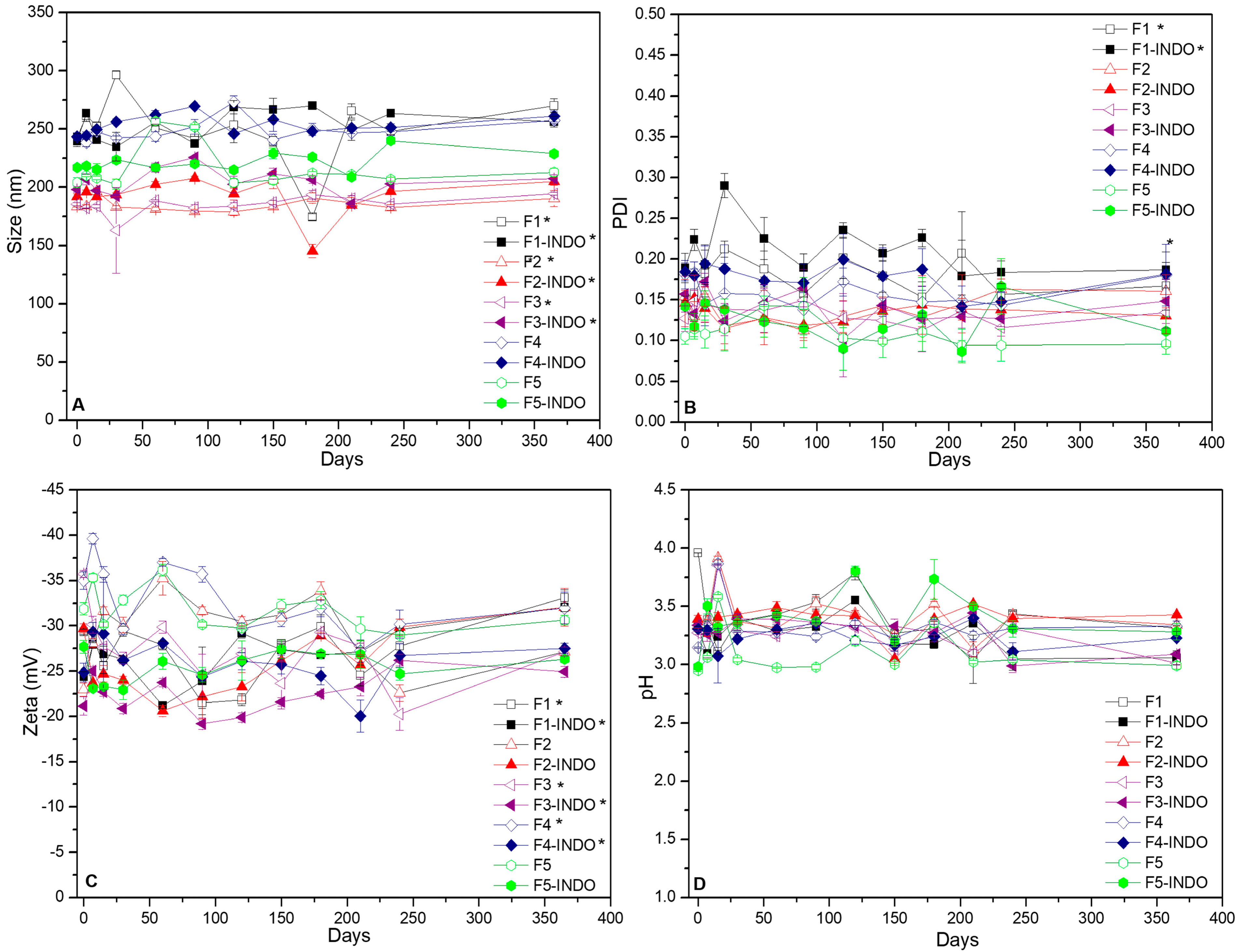
3.2. Long-Term Stability of NLC
3.3. Indomethacin Encapsulation Efficiency by NLC
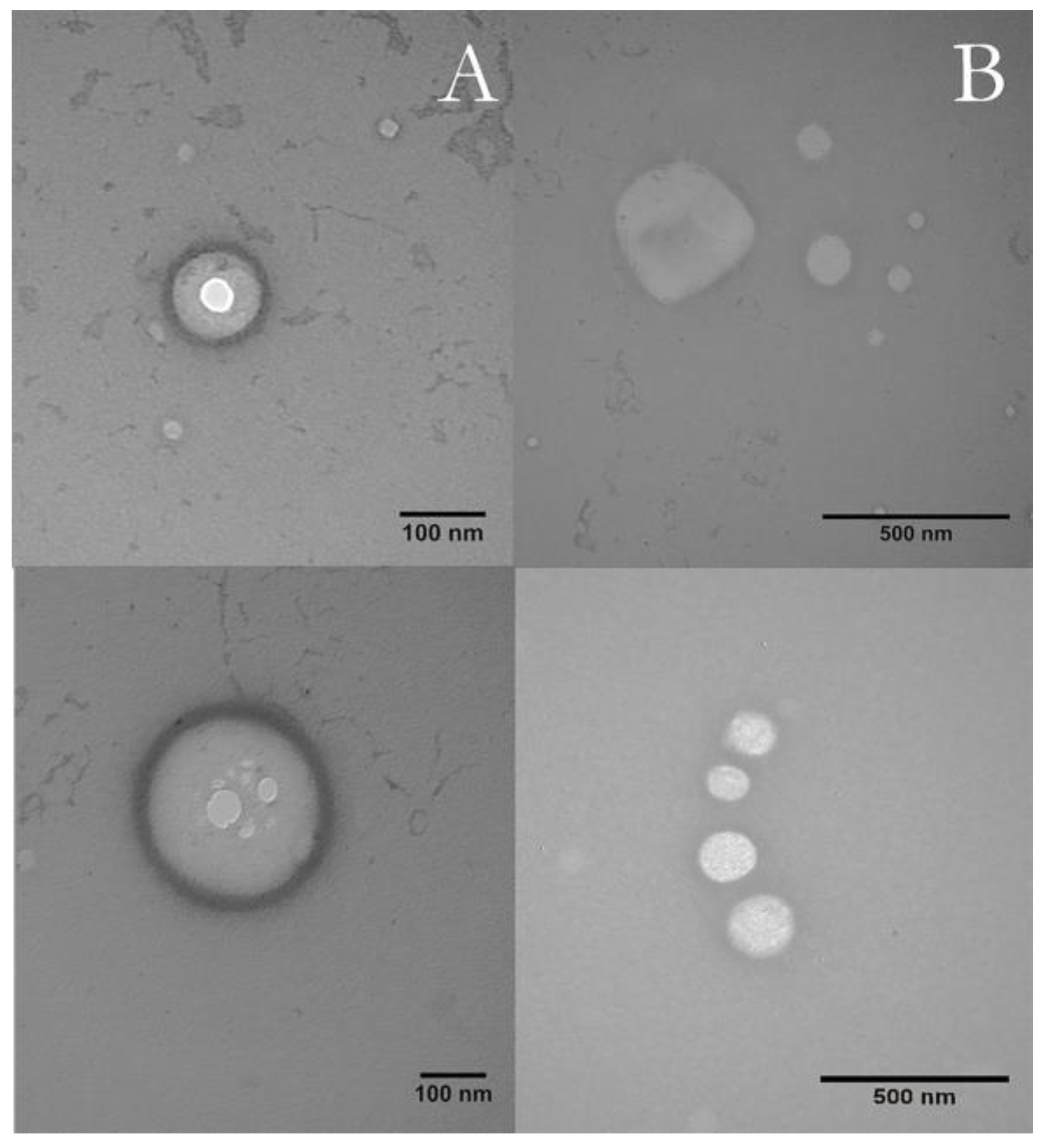
3.4. Transmission Electron Microscopy (TEM)
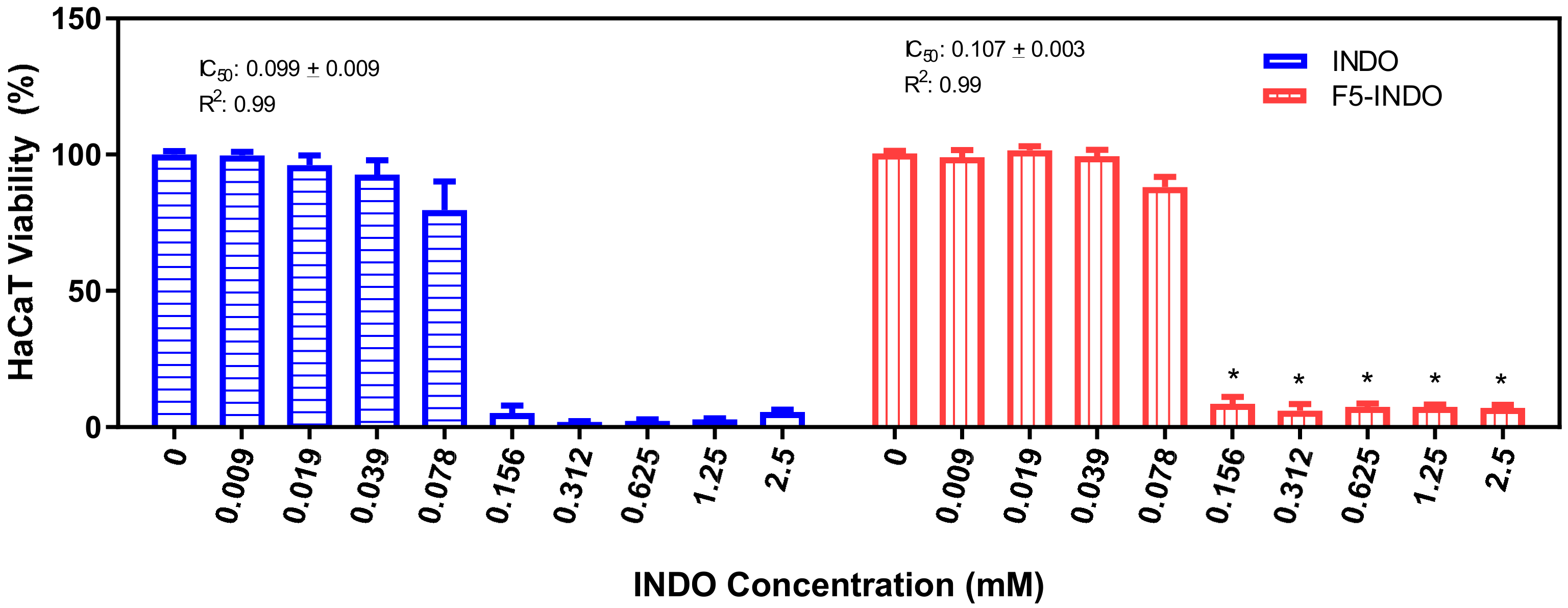
3.5. Cell Viability Tests
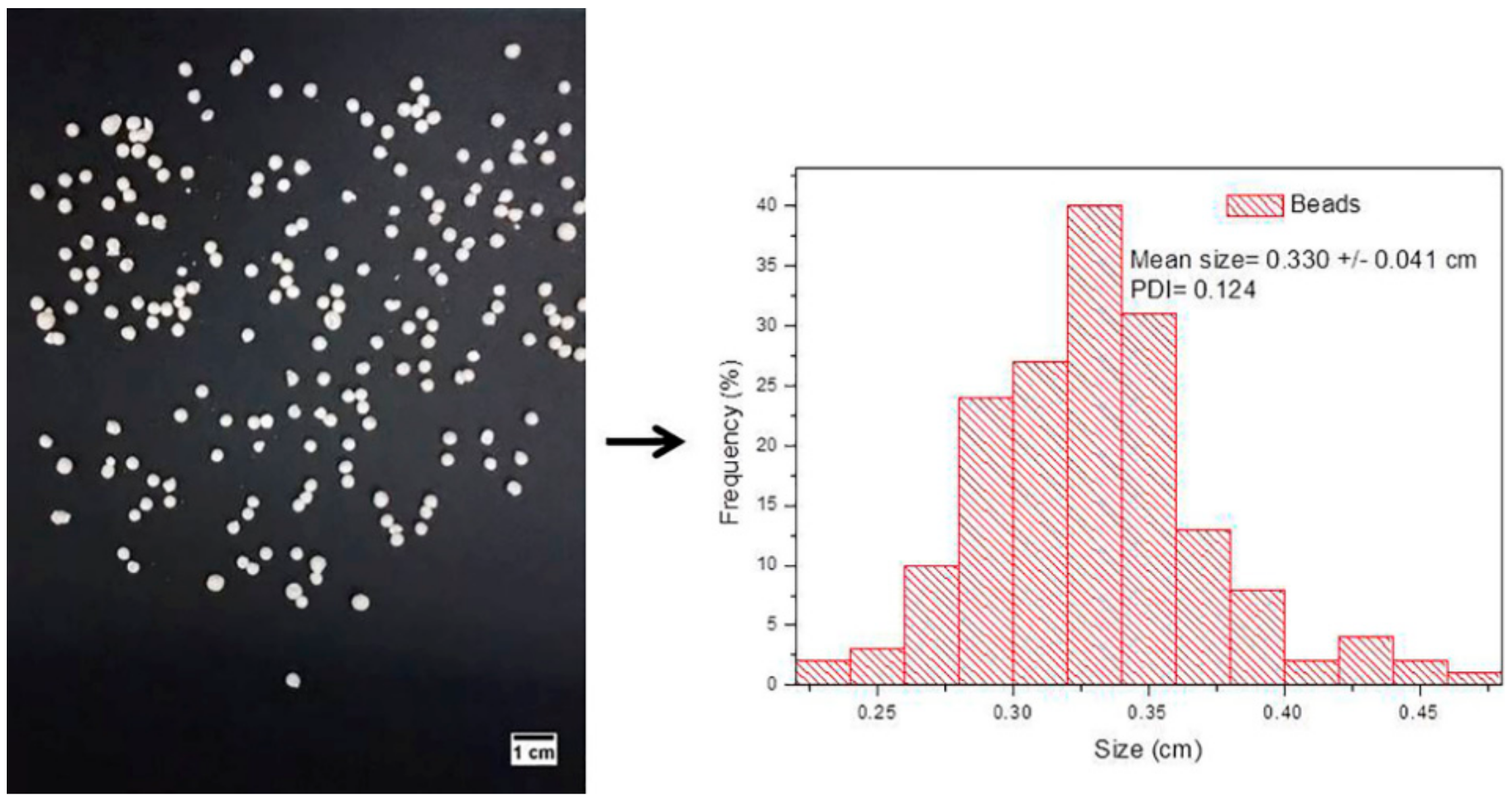
3.6. Preparation of Biopolymers and Hybrid Nanobeads Loading Indomethacin
3.7. FE-SEM Analyses
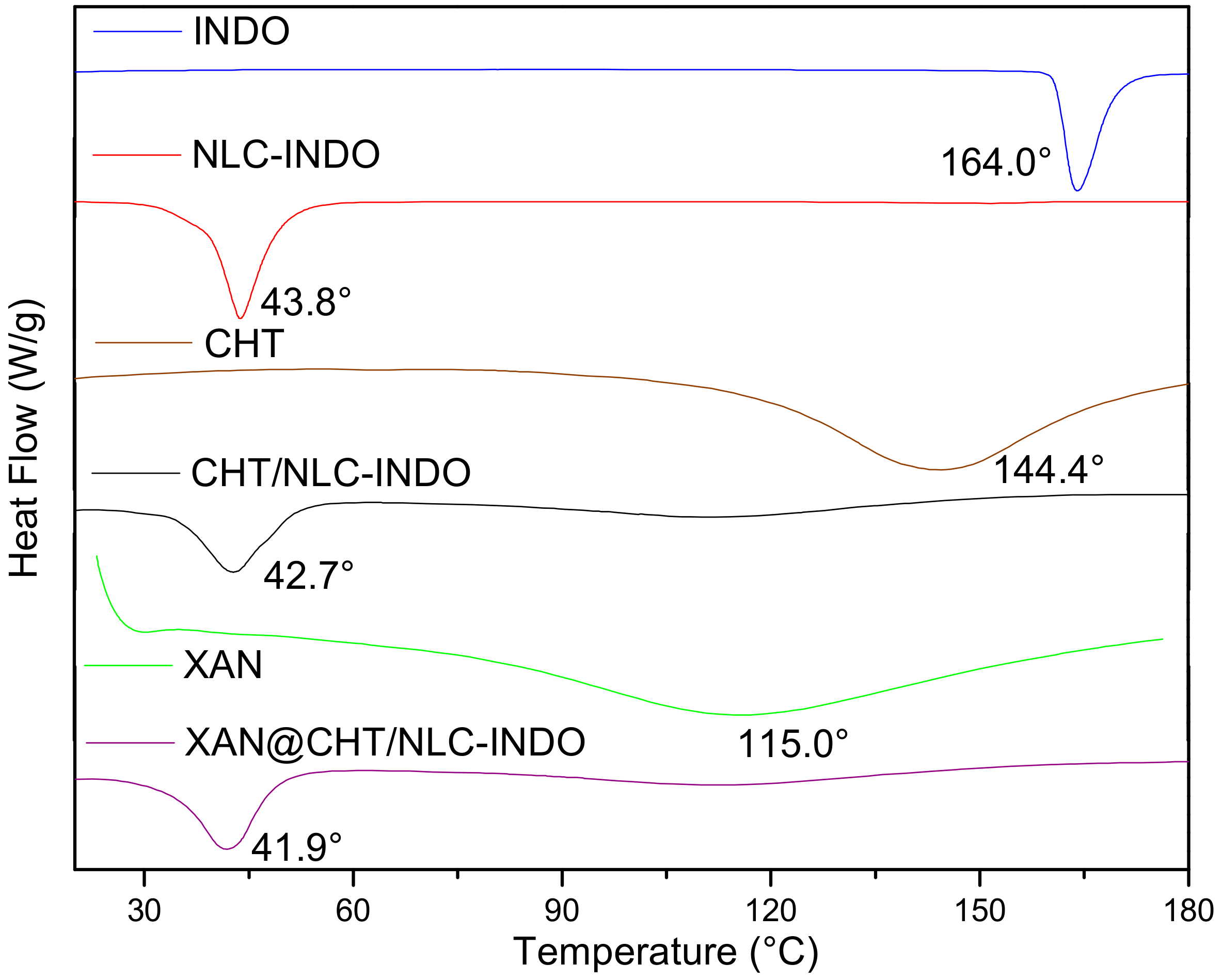
3.8. DSC Analyses
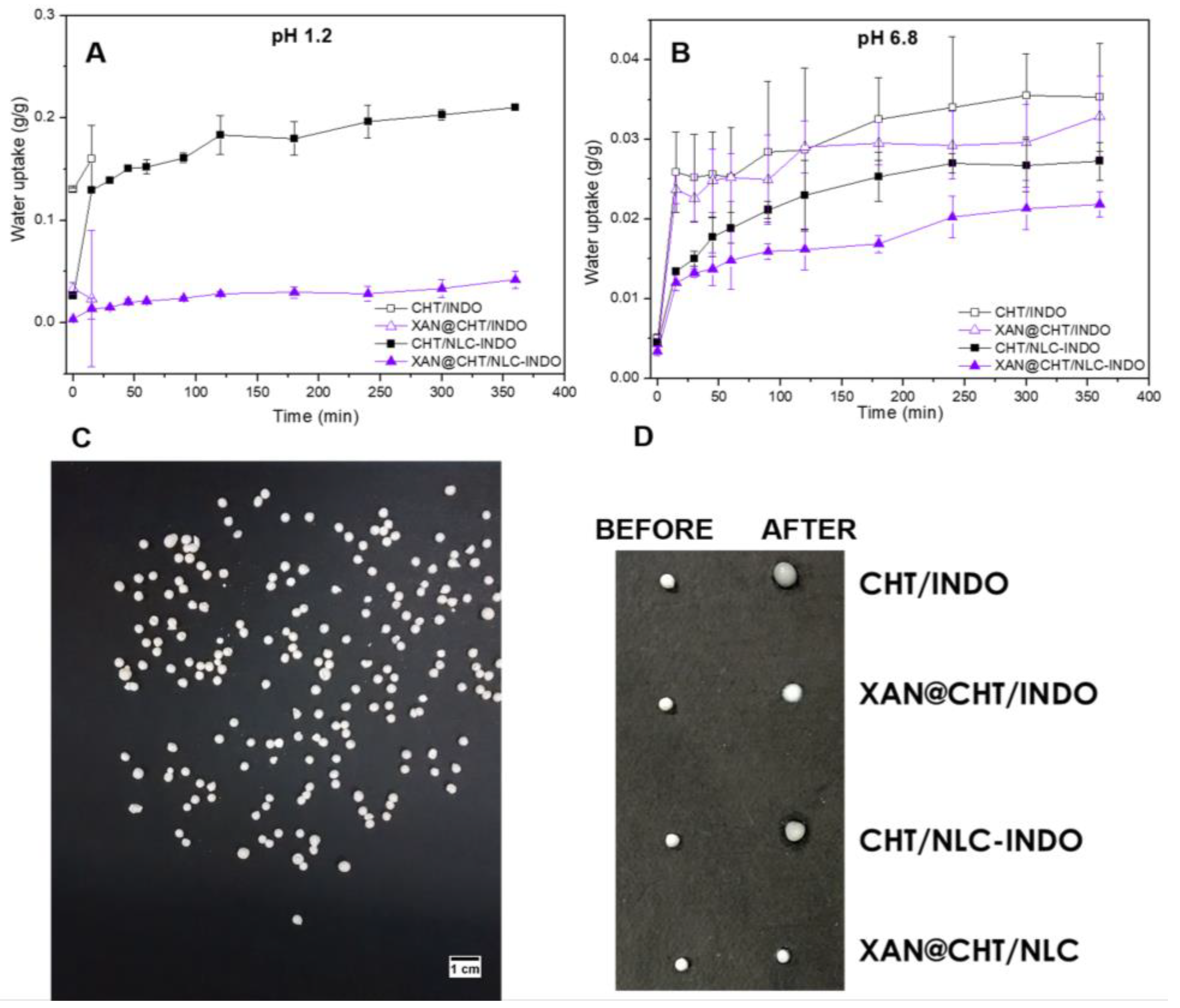
3.9. In Vitro Water Uptake
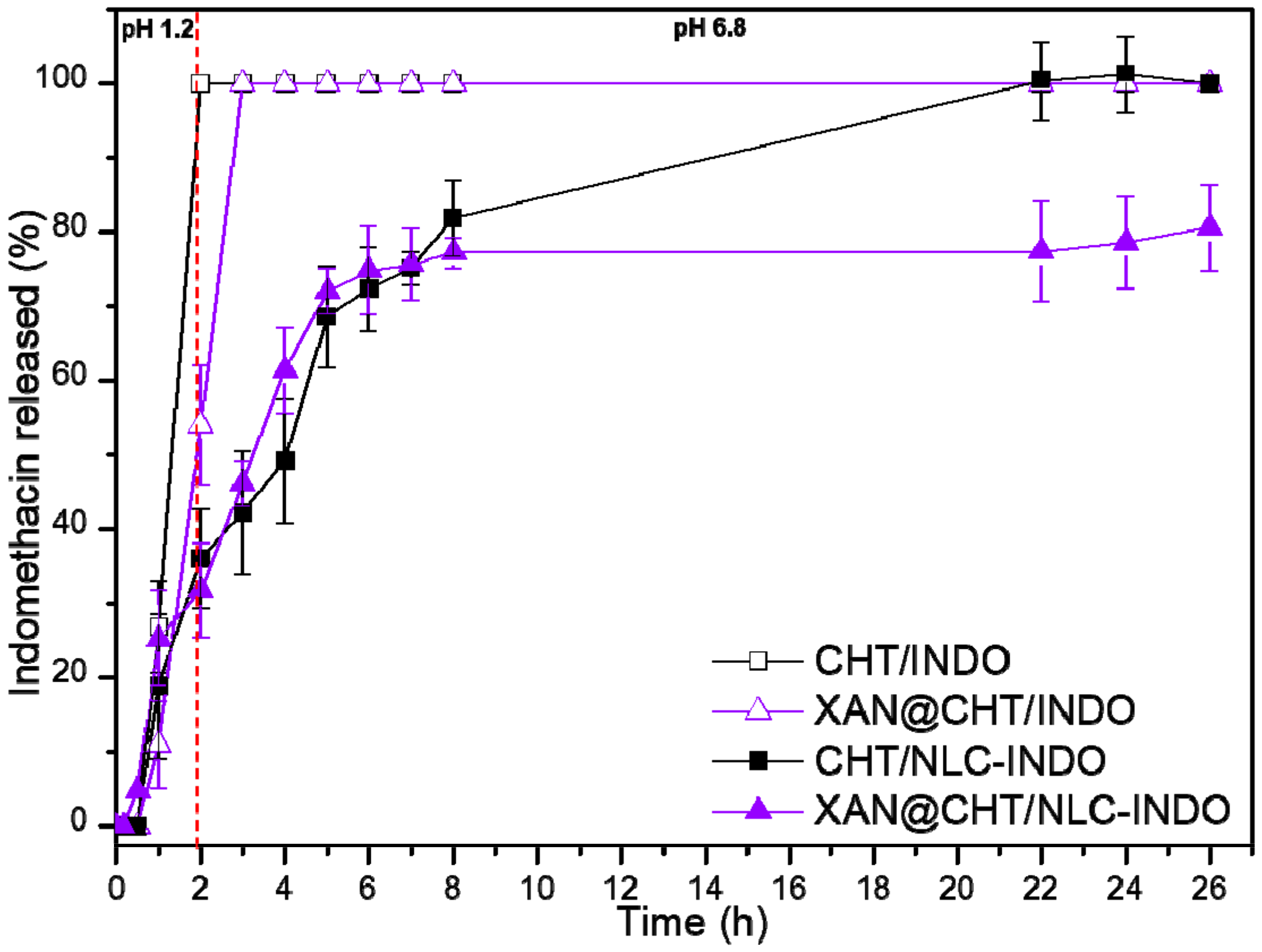
3.10. In Vitro Indomethacin Release Test
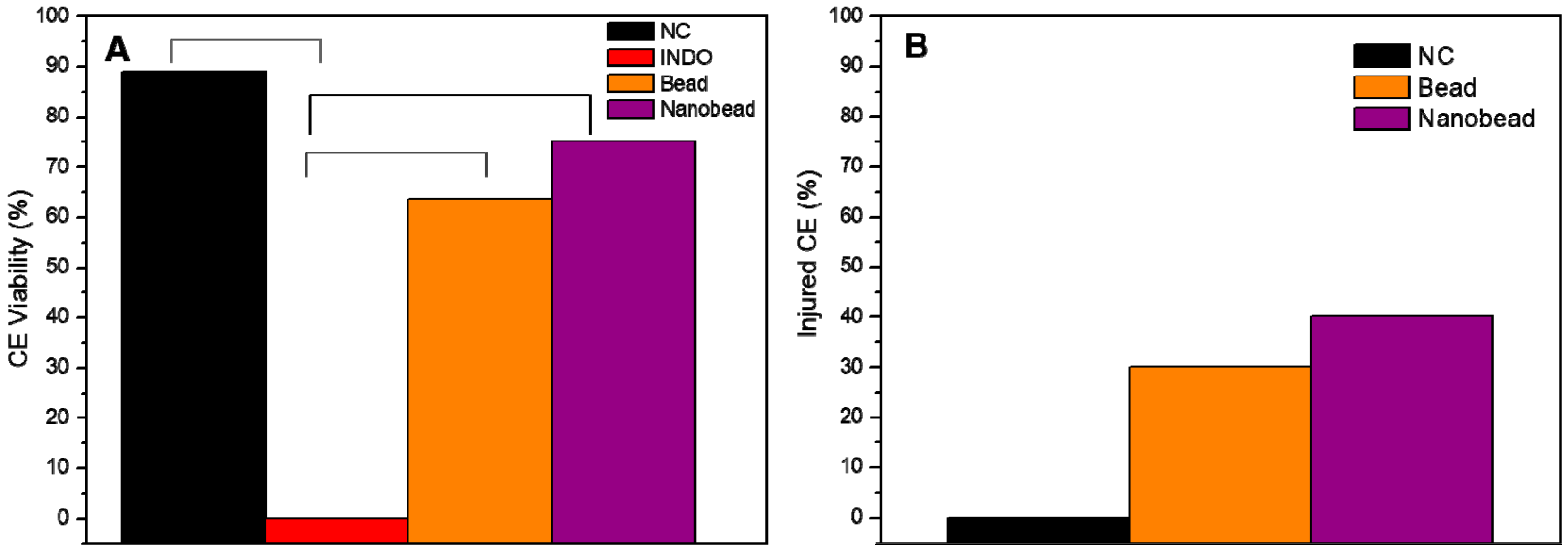
3.11. In Vivo Toxicity Assay through Chicken Embryo Model
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Lucas, S. The pharmacology of indomethacin. Headache Curr. 2016, 56, 436–446. [Google Scholar] [CrossRef] [PubMed]
- Sánchez-Trigueros, M.I.; Méndez-Cruz, F.; Rivera-Espinoza, E.P.-P.Y.A.; Castañeda-Hernández, G.; Chávez-Piña, E.A. Synergistic protective effects between docosahexaenoic acid and omeprazole on the gastrointestinal tract in the indomethacin-induced injury model. Drug Dev. Res. 2021, 82, 543–552. [Google Scholar] [CrossRef] [PubMed]
- Ali Sajid, M.; Muthukumaran, J.; Jain, M.; Al-Sanea, A.S.S.; Al-Lohedan, H.A. Experimental and in silico investigation on the interaction of indomethacin with bovine serum albumin: Effect of sodium dodecyl sulfate surfactant monomers on the binding. J. Mol. Liq. 2021, 336, 116858. [Google Scholar] [CrossRef]
- Guilherme, V.A.; Ribeiro, L.N.M.; Tofoli, G.R.; Franz-Montan, M.; de Paula, E.; de Jesus, M.B. Current challenges and future of lipid nanoparticles formulations for topical drug application to oral mucosa, skin, and eye. Curr. Pharm. Des. 2018, 23, 6659–6675. [Google Scholar] [CrossRef]
- Ribeiro, L.N.M.; de Paula, E.; Rossi, D.A.; Melo, R.T.; Monteiro, G.P.; Goulart, L.R.; Fonseca, B.B. Nanocarriers from Natural Lipids with in vitro activity against campylobacter jejuni. Front. Cell. Infect. Microbiol. 2021, 10, 571040. [Google Scholar] [CrossRef]
- Guilherme, V.A.; Ribeiro, L.N.M.; Alcântara, A.C.S.; Castro, S.R.; Rodrigues da Silva, G.H.; da Silva, C.G.; Breitkreitz, M.C.; Clemente-Napimoga, J.; Macedo, C.G.; Abdalla, H.B.; et al. Improved efficacy of naproxen-loaded NLC for temporomandibular joint administration. Sci. Rep. 2019, 9, 11160. [Google Scholar] [CrossRef] [Green Version]
- Kumari, S.; Dandamudi, M.; Rani, S.; Behaeghel, E.; Behl, G.; Kent, D.; Reilly, N.J.O.; Donovan, O.O.; Mcloughlin, P.; Fitzhenry, L. Dexamethasone-loaded nanostructured lipid carriers for the treatment of dry eye disease. Pharmaceutics 2021, 13, 905. [Google Scholar] [CrossRef]
- Sharma, M.; Chaudhary, D. Exploration of bromelain laden nanostructured lipid carriers: An oral platform for bromelain delivery in rheumatoid arthritis management. Int. J. Pharm. 2021, 594, 120176. [Google Scholar] [CrossRef]
- Ribeiro, L.N.M.; Franz-Montan, M.; Breitkreitz, M.C.; Alcântara, A.C.S.; Castro, S.R.; Guilherme, V.A.; Barbosa, R.M.; de Paula, E. Nanostructured lipid carriers as robust systems for topical lidocaine-prilocaine release in dentistry. Eur. J. Pharm. Sci. 2016, 93, 192–202. [Google Scholar] [CrossRef]
- Ribeiro, L.N.M.; de Paula, E.; Rossi, D.A.; Monteiro, G.P.; Valadares, E.C.; Silva, R.R.; Franco, R.R.; Espindola, S.F.; Goulart, L.R.; Fonseca, B.B. Hybrid pectin-liposome formulation against multi-resistant bacterial strains. Pharmaceutics 2020, 12, 769. [Google Scholar] [CrossRef]
- Hadinoto, K.; Sundaresan, A.; Cheow, W.S. Lipid-polymer hybrid nanoparticles as a new generation therapeutic delivery platform: A review. Eur. J. Pharm. Biopharm. 2013, 85, 427–443. [Google Scholar] [CrossRef]
- Ribeiro, L.N.M.; Alcântara, A.C.S.; Franz-Montan, M.; Couto, V.M.; Nista, S.V.G.; de Paula, E. Nanostructured organic-organic bio-hybrid delivery systems. In Biomedical Applications of Nanoparticles; Grumezescu, A.M., Ed.; Elsevier: Amsterdam, The Netherlands, 2019; pp. 341–374. ISBN 9780128165065. [Google Scholar]
- Sanchez Armengol, E.; Laffleur, F. Generations of chitosan: The progress in drug delivery. In Advances in Polymer Sciences; Springer: Berlin/Heidelberg, Germany, 2021; pp. 1–22. [Google Scholar]
- Liu, Y.; Chen, D.; Zhang, A.; Xiao, M.; Li, Z.; Luo, W.; Pan, Y.; Qu, W.; Xie, S. Composite inclusion complexes containing hyaluronic acid/chitosan nanosystems for dual responsive enrofloxacin release. Carbohydr. Polym. 2021, 252, 117162. [Google Scholar] [CrossRef]
- Ribeiro, L.N.M.; Franz-Montan, M.; Breitkreitz, M.C.; Rodrigues da Silva, G.; Castro, S.; Guilherme, V.; de Araújo, D.; de Paula, E. Nanohybrid hydrogels designed for transbuccal anesthesia. Int. J. Nanomed. 2018, 13, 6453–6463. [Google Scholar] [CrossRef] [Green Version]
- Petitjean, M.; Isasi, J.R. Chitosan, xanthan and locust bean gum matrices crosslinked with β-cyclodextrin as green sorbents of aromatic compounds. Int. J. Biol. Macromol. 2021, 180, 570–577. [Google Scholar] [CrossRef]
- Ribeiro, L.N.M.; Breitkreitz, M.C.; Guilherme, V.A.; Rodrigues da Silva, G.H.; Couto, V.M.; Castro, S.R.; De Paula, B.O.; Machado, D.; de Paula, E. Natural lipids-based NLC containing lidocaine: From pre-formulation to in vivo studies. Eur. J. Pharm. Sci. 2017, 106, 102–112. [Google Scholar] [CrossRef]
- Barbosa, R.M.; Ribeiro, L.N.M.; Casadei, B.; da Silva, C.; Queiróz, V.; Duran, N.; de Araújo, D.; Severino, P.; de Paula, E. Solid lipid nanoparticles for dibucaine sustained release. Pharmaceutics 2018, 10, 231. [Google Scholar] [CrossRef] [Green Version]
- Tres, F.; Treacher, K.; Booth, J.; Hughes, L.P.; Wren, S.A.C.; Aylott, J.W.; Burley, J.C. Indomethacin-Kollidon VA64 Extrudates: A mechanistic study of pH- dependent controlled release. Mol. Pharm. 2016, 13, 166–1175. [Google Scholar] [CrossRef]
- Ferrari, M.; Fornasiero, M.C.; Isetta, A.M. MTT colorimetric assay for testing macrophage cytotoxic activity in vitro. J. Immunol. Methods 1990, 131, 165–172. [Google Scholar] [CrossRef]
- Ribeiro, L.N.M.; Alcântara, A.C.S.; Darder, M.; Aranda, P.; Araújo-Moreira, F.M.; Ruiz-Hitzky, E. Pectin-coated chitosan-LDH bionanocomposite beads as potential systems for colon-targeted drug delivery. Int. J. Pharm. 2014, 463, 1–9. [Google Scholar] [CrossRef]
- Mendyk, A.; Jachowicz, R. Unified methodology of neural analysis in decision support systems built for pharmaceutical technology. Expert Syst. Appl. 2007, 32, 1124–1131. [Google Scholar] [CrossRef]
- Ribeiro, L.N.M.; Alcântara, A.C.S.; Darder, M.; Aranda, P.; Herrmann, P.S.P.; Araújo-Moreira, F.M.; García-Hernández, M.; Ruiz-Hitzky, E. Bionanocomposites containing magnetic graphite as potential systems for drug delivery. Int. J. Pharm. 2014, 477, 553–563. [Google Scholar] [CrossRef]
- Poletto, F.S.; Jäger, E.; Ré, M.I.; Guterres, S.S.; Pohlmann, A.R. Rate-modulating PHBHV/PCL microparticles containing weak acid model drugs. Int. J. Pharm. 2007, 345, 70–80. [Google Scholar] [CrossRef]
- Papadopoulou, V.; Kosmidis, K.; Vlachou, M.; Macheras, P. On the use of the Weibull function for the discernment of drug release mechanisms. Int. J. Pharm. 2006, 309, 44–50. [Google Scholar] [CrossRef]
- Muniz, B.V.; Baratelli, D.; Di Carla, S.; Serpe, L.; da Silva, C.B.; Guilherme, V.A.; Ribeiro, L.N.M.; Cereda, C.M.S.; de Paula, E.; Volpato, M.C.; et al. Hybrid hydrogel composed of polymeric nanocapsules co-loading lidocaine and prilocaine for topical intraoral anesthesia. Sci. Rep. 2018, 8, 17972. [Google Scholar] [CrossRef]
- De Moura, L.D.; Ribeiro, L.N.M.; De Carvalho, V.; Rodrigues, G.H.; Fernandes, P.C.L.; Brunetto, S.Q.; Ramos, C.D.; Velloso, L.A.; De Ara, D.R.; De Paula, E. Docetaxel and lidocaine co-loaded (NLC-in-hydrogel) hybrid system designed for the treatment of melanoma. Pharmaceutics 2021, 13, 1552. [Google Scholar] [CrossRef]
- Ramos, J.J.M.; Taveira-Marques, R.; Diogo, H.P. Estimation of the fragility index of indomethacin by DSC using the heating and cooling rate dependency of the glass transition. J. Pharm. Sci. 2004, 93, 1503–1507. [Google Scholar] [CrossRef] [PubMed]
- Islan, G.A.; Cortez, P.; Abraham, G.A.; Duran, N.; Castro, G.R. Smart lipid nanoparticles containing levofloxacin and DNase for lung delivery. Design and characterization. Coll. Surf. B Biointerfaces 2016, 143, 168–176. [Google Scholar] [CrossRef] [Green Version]
- Consumi, M.; Leone, G.; Pepi, S.; Tamasi, G.; Lamponi, S.; Donati, A.; Bonechi, C.; Rossi, C.; Magnani, A. Xanthan Gum-Chitosan: Delayed, prolonged, and burst-release tablets using same components in different ratio. Adv. Polym. Technol. 2018, 1–10. [Google Scholar] [CrossRef]
- Fonseca, B.B.; Silva, M.V.; Ribeiro, L.N.M. The chicken embryo as in vivo experimental model for drug testing: Advantages and limitations. Lab. Anim. 2021, 50, 138–139. [Google Scholar] [CrossRef]
- Vinarov, Z.; Abrahamsson, B.; Artursson, P.; Batchelor, H.; Berben, P.; Bernkop-schnürch, A.; Butler, J.; Ceulemans, J.; Davies, N.; Dupont, D.; et al. Current challenges and future perspectives in oral absorption research: An opinion of the UNGAP network. Adv. Drug Deliv. Rev. 2021, 171, 289–331. [Google Scholar] [CrossRef]
- Porter, J.H.; Charman, W.N. Uptake of drugs into the intestinal lymphatics. Adv. Drug Deliv. Rev. 1997, 25, 71–89. [Google Scholar] [CrossRef]
- Balguri, S.P.; Adelli, G.R.; Majumdar, S. Topical ophthalmic lipid nanoparticle formulations (SLN, NLC) of indomethacin for delivery to the posterior segment ocular tissues. Eur. J. Pharm. Biopharm. 2016, 109, 224–235. [Google Scholar] [CrossRef] [Green Version]
- Shah, S.; Famta, P.; Raghuvanshi, R.S.; Singh, S.B.; Srivastava, S. Lipid polymer hybrid nanocarriers: Insights into synthesis aspects, characterization, release mechanisms, surface functionalization and potential implications. Colloid Interface Sci. Commun. 2022, 46, 100570. [Google Scholar] [CrossRef]
- Rose, F.; Wern, J.E.; Ingvarsson, P.T.; van de Weert, M.; Andersen, P.; Follmann, F.; Foged, C. Engineering of a novel adjuvant based on lipid-polymer hybrid nanoparticles: A quality-by-design approach. J. Control. Release 2015, 210, 48–57. [Google Scholar] [CrossRef]
- Siepmann, J.; Faham, A.; Clas, S.D.; Boyd, B.J.; Jannin, V.; Bernkop-Schnürch, A.; Zhao, H.; Lecommandoux, S.; Evans, J.C.; Allen, C.; et al. Lipids and polymers in pharmaceutical technology: Lifelong companions. Int. J. Pharm. 2019, 558, 128–142. [Google Scholar] [CrossRef]
- Czarnocka, J.K.; Alhnan, M.A. Gastro-resistant characteristics of GRAS-grade enteric coatings for pharmaceutical and nutraceutical products. Int. J. Pharm. 2015, 486, 167–174. [Google Scholar] [CrossRef]
- Sun, W.; Griffiths, M.W. Survival of bifidobacteria in yogurt and simulated gastric juice following immobilization in gellan–xanthan beads. Int. J. Food Microbiol. 2000, 61, 17–25. [Google Scholar] [CrossRef]
- Ribeiro, L.N.M.; Rodrigues da Silva, G.; Couto, V.M.; Castro, S.R.; Breitkreitz, M.C.; Martinez, C.S.; Igartúa, D.E.; Prieto, M.J.; de Paula, E. Functional hybrid nanoemulsions for sumatriptan intranasal delivery. Front. Chem. 2020, 8, 589503. [Google Scholar] [CrossRef]
- Ribeiro, L.N.M.; Franz-Montan, M.; Alcântara, A.C.S.; Breitkreitz, M.C.; Castro, S.R.; Guilherme, V.A.; Muniz, B.V.; Rodrigues, G.H.; de Paula, E. Hybrid nanofilms as topical anesthetics for pain-free procedures in dentistry. Sci. Rep. 2020, 10, 11341. [Google Scholar] [CrossRef]
- de Araújo, D.R.; Ribeiro, L.N.M.; de Paula, E. Lipid-based carriers for the delivery of local anesthetics. Expert Opin. Drug Deliv. 2019, 16, 1–14. [Google Scholar] [CrossRef]
- Nazlı, A.B.; Açıkel, Y.S. Loading of cancer drug resveratrol to pH-Sensitive, smart, alginate-chitosan hydrogels and investigation of controlled release kinetics. J. Drug Deliv. Sci. Technol. 2019, 53, 101199. [Google Scholar] [CrossRef]
- Albano, J.M.R.; Ribeiro, L.N.M.; Couto, V.M.; Barbosa Messias, M.; Rodrigues da Silva, G.H.; Breitkreitz, M.C.; de Paula, E.; Pickholz, M. Rational design of polymer-lipid nanoparticles for docetaxel delivery. Coll. Surf. B Biointerfaces 2019, 175, 56–64. [Google Scholar] [CrossRef] [PubMed]
- Bernauer, U.; Bodin, L.; Chaudhry, Q.; Jan, P.; Dusinska, M.; Gaffet, E.; Panteri, E.; Rogiers, V.; Rousselle, C.; Stepnik, M.; et al. The SCCS scientific advice on the safety of nanomaterials in cosmetics. Regul. Toxicol. Pharmacol. 2021, 126, 105046. [Google Scholar] [CrossRef]
- Khan, S.; Yusufi, F.N.K.; Yusufi, A.N.K. Comparative effect of indomethacin (IndoM) on the enzymes of carbohydrate metabolism, brush border membrane and oxidative stress in the kidney, small intestine and liver of rats. Toxicol. Rep. 2019, 6, 389–394. [Google Scholar] [CrossRef]

| Formulation | INDO (%) | MM:CO (%) | P68 (%) |
|---|---|---|---|
| F1 | 0 | 80:20 | 2 |
| F1/INDO | 2 | 80:20 | 2 |
| F2 | 0 | 70:30 | 5 |
| F2/INDO | 2 | 70:30 | 5 |
| F3 | 0 | 60:40 | 5 |
| F3/INDO | 2 | 60:40 | 5 |
| F4 | 0 | 70:30 | 2 |
| F4/INDO | 2 | 70:30 | 2 |
| F5 | 0 | 80:20 | 5 |
| F5/INDO | 2 | 80:20 | 5 |
| Sample | Composition | Form |
|---|---|---|
| CHT/INDO | Chitosan, indomethacin | Bead |
| XAN@CHT/INDO | Xanthan, chitosan and indomethacin | Coated Bead |
| CHT/NLC-INDO | Chitosan, nanostructured lipid carrier loading indomethacin | Nanobead |
| XAN@CHT/NLC-INDO | Xanthan and chitosan, nanostructured lipid carrier loading indomethacin | Coated Nanobead |
| Formulations | %EE |
|---|---|
| F1 | - |
| F1-INDO | 98.7 ± 0.2 |
| F2 | - |
| F2-INDO | 99.1 ± 0.1 |
| F3 | - |
| F3-INDO | 98.9 ± 0.8 |
| F4 | - |
| F4-INDO | 99.0 ± 0.7 |
| F5 | - |
| F5-INDO | 99.0 ± 0.2 |
| Bead | Size (cm) | PDI |
|---|---|---|
| CHT/INDO | 0.398 ± 0.009 | 0.112 ± 0.001 |
| CHT/NLC-INDO | 0.370 ± 0.004 | 0.102 ± 0.006 |
| XAN@CHT/INDO | 0.352 ± 0.011 | 0.110 ± 0.040 |
| XAN@CHT/NLC-INDO | 0.330 ± 0.021 | 0.124 ± 0.009 |
| Formulation | 0 Order | Weibull | Baker–Lonsdale |
|---|---|---|---|
| CHT/INDO | 0.95 | 0.78 | 0.83 |
| XAN@CHT/INDO | 0.97 | 0.82 | 0.75 |
| CHT/NLC-INDO | 0.66 | 0.74 | 0.99 |
| XAN@CHT/NLC-INDO | 0.46 | 0.91 | 0.59 |
| Markers | NC | Bead | Nanobead |
|---|---|---|---|
| UA (mg/dL) CK (U/L) | 31.70 (±15.2) 1356.0 (±1494.0) | 18.97 (±12.6) | 50.69 (±43.4) |
| 513.1 (±501.1) | 582.4 (±420.9) | ||
| ALP (U/L) | 429.6 (±230.4) a | 1168.0 (±454.8) b | 946.7 (±449.2) ab |
| GGT (U/L) | 6.98 (±4.9) | 6.52 (±3.7) | 5.28 (±4.3) |
| AST (U/L) | 144.6 (±146.4) | 118.6 (±31.4) | 153.8 (±94.0) |
| ALT (U/L) | 11.40 (±8.0) | 5.80 (±3.3) | 4.60 (±5.7) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bonetti, F.M.R.; de Paula, E.; Fonseca, B.B.; da Silva, G.R.; da Silva, L.S.S.; de Moura, L.D.; Breitkreitz, M.C.; Rodrigues da Silva, G.H.; de Morais Ribeiro, L.N. Hybrid Nanobeads for Oral Indomethacin Delivery. Pharmaceutics 2022, 14, 583. https://doi.org/10.3390/pharmaceutics14030583
Bonetti FMR, de Paula E, Fonseca BB, da Silva GR, da Silva LSS, de Moura LD, Breitkreitz MC, Rodrigues da Silva GH, de Morais Ribeiro LN. Hybrid Nanobeads for Oral Indomethacin Delivery. Pharmaceutics. 2022; 14(3):583. https://doi.org/10.3390/pharmaceutics14030583
Chicago/Turabian StyleBonetti, Flávia Monique Rocha, Eneida de Paula, Belchiolina Beatriz Fonseca, Gabriela Ribeiro da Silva, Leandro Santana Soares da Silva, Ludmilla David de Moura, Márcia Cristina Breitkreitz, Gustavo Henrique Rodrigues da Silva, and Lígia Nunes de Morais Ribeiro. 2022. "Hybrid Nanobeads for Oral Indomethacin Delivery" Pharmaceutics 14, no. 3: 583. https://doi.org/10.3390/pharmaceutics14030583
APA StyleBonetti, F. M. R., de Paula, E., Fonseca, B. B., da Silva, G. R., da Silva, L. S. S., de Moura, L. D., Breitkreitz, M. C., Rodrigues da Silva, G. H., & de Morais Ribeiro, L. N. (2022). Hybrid Nanobeads for Oral Indomethacin Delivery. Pharmaceutics, 14(3), 583. https://doi.org/10.3390/pharmaceutics14030583









