Resistivity Technique for the Evaluation of the Integrity of Buccal and Esophageal Epithelium Mucosa for In Vitro Permeation Studies: Swine Buccal and Esophageal Mucosa Barrier Models
Abstract
1. Introduction
2. Material and Methods
2.1. Material
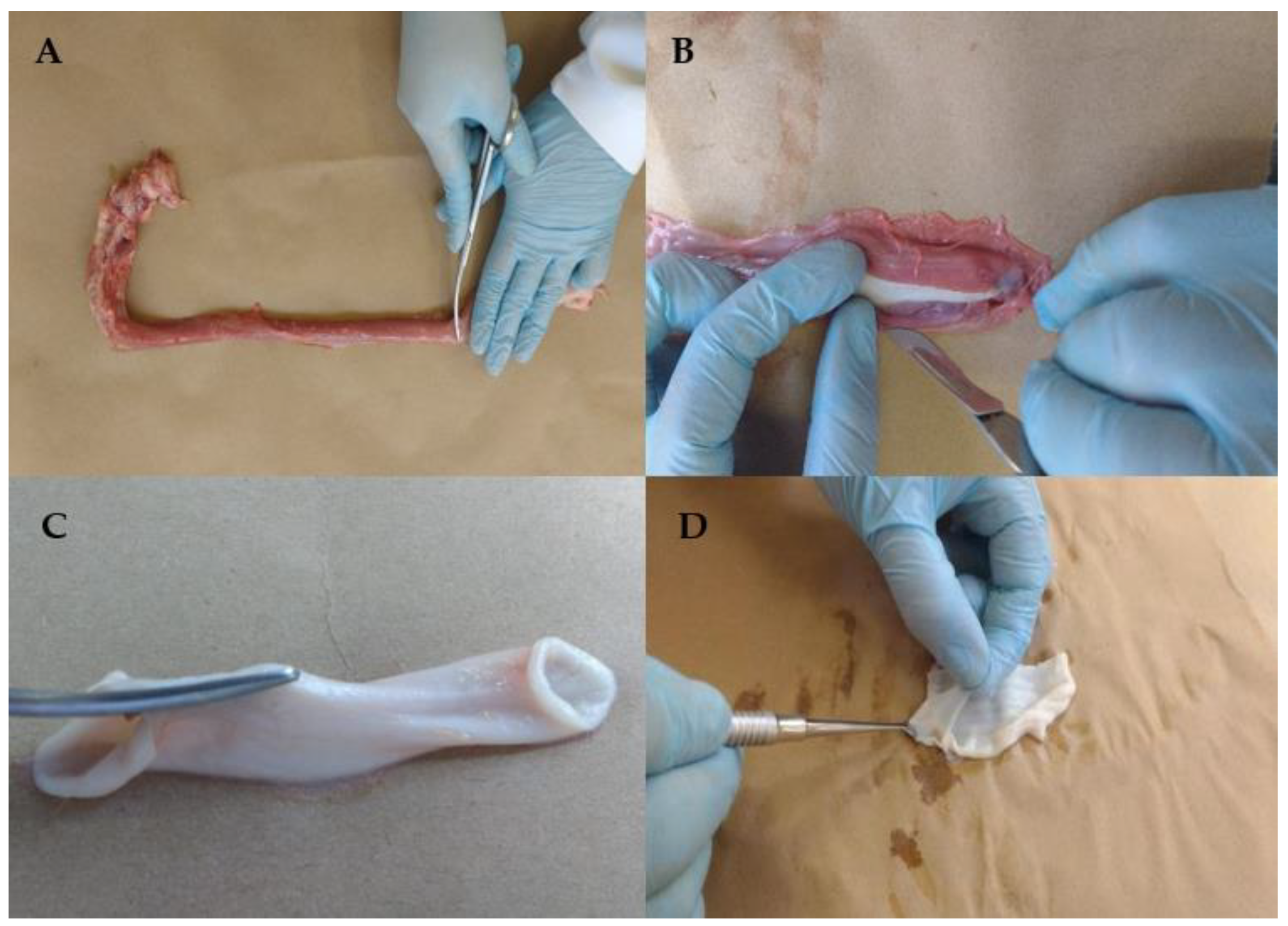
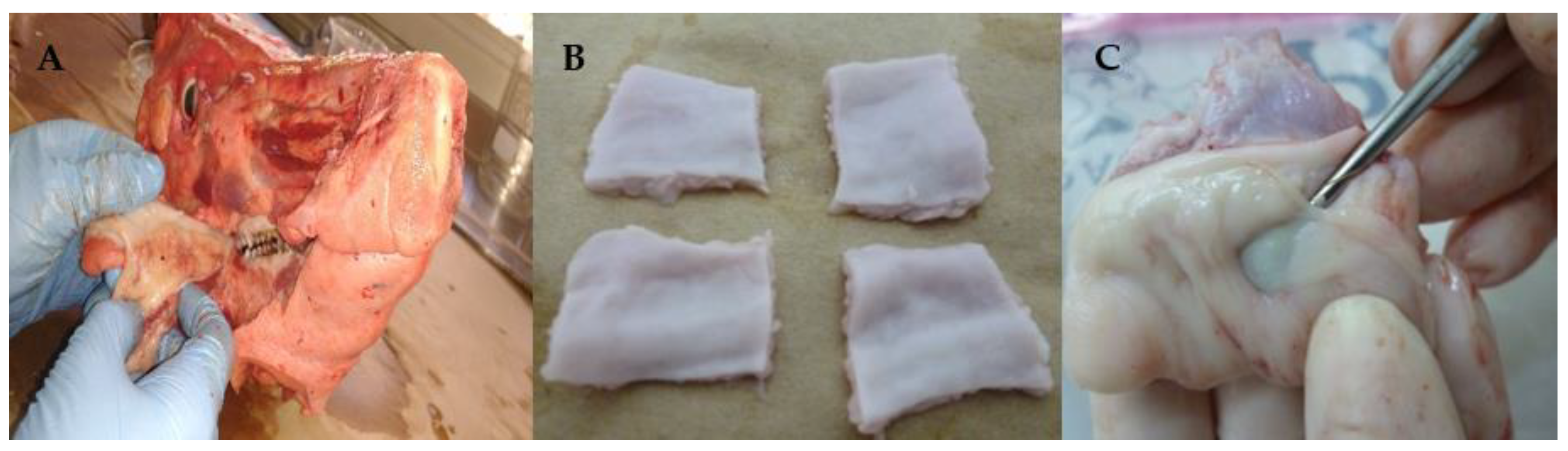
2.2. Mucosa Preparation
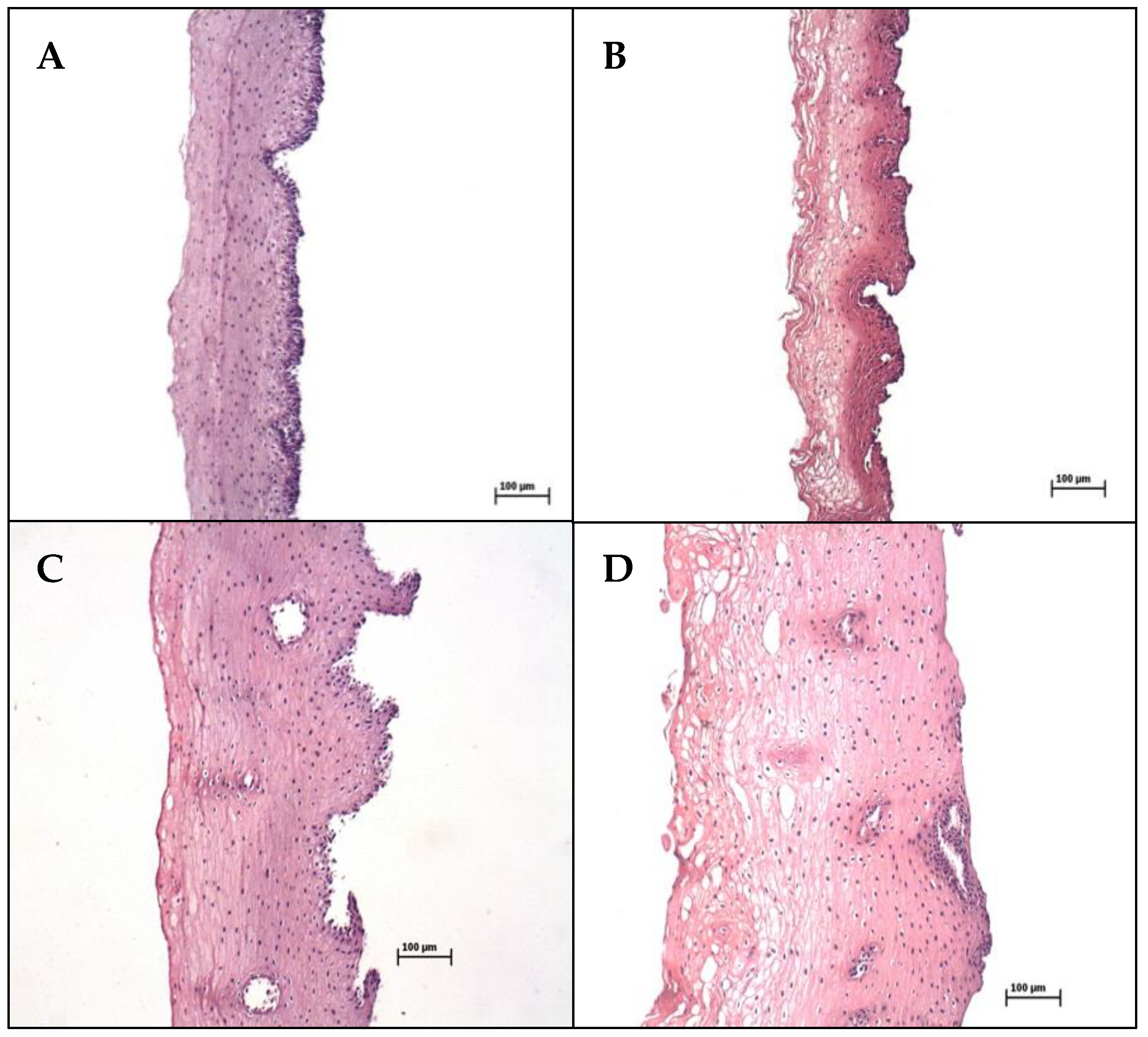
2.3. Histological Assessment
2.4. Electrical Resistivity (ER) Measurement
2.5. Tissue Storage
2.6. Permeation Assays
2.7. Lidocaine Analysis
2.8. Statistical Analysis
3. Results
3.1. Histological Controls
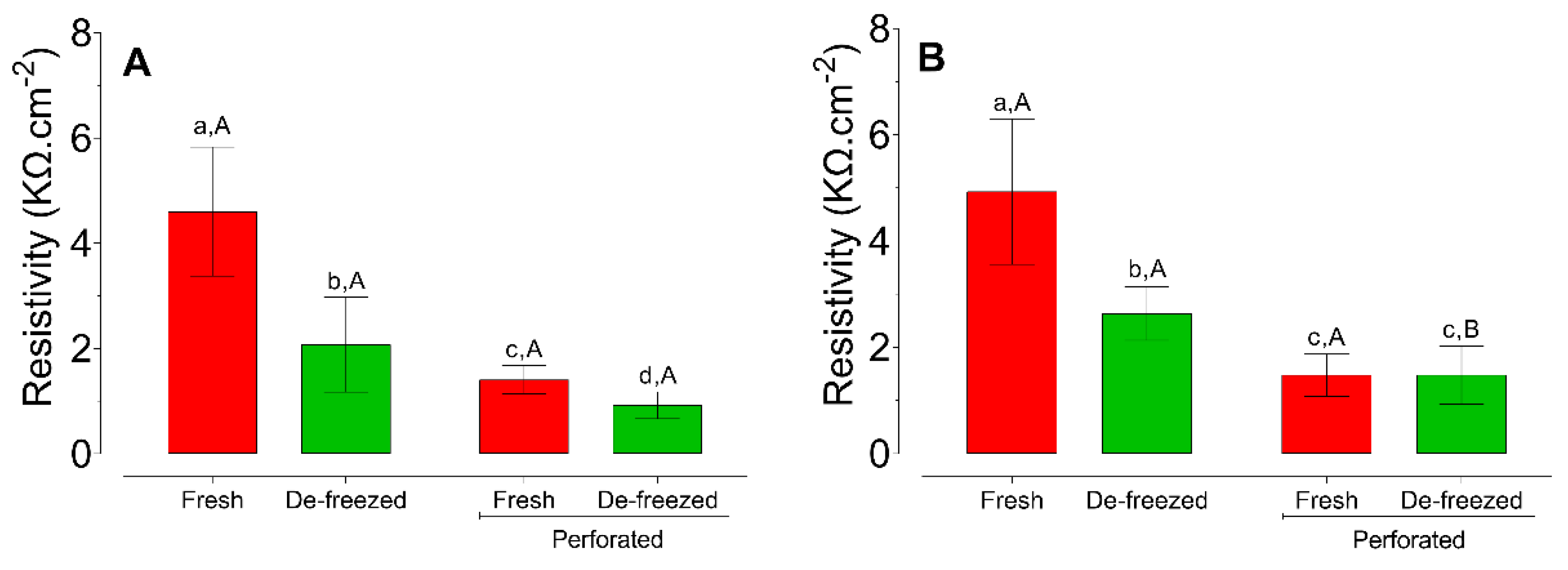
3.2. Electrical Resistivity
3.3. Permeation Assays
3.4. Correlation Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Shojaei, A.H. Buccal mucosa as a route for systemic drug delivery: A review. J. Pharm. Pharm. Sci. 1998, 1, 15–30. [Google Scholar]
- Morales, J.O.; McConville, J.T. Novel strategies for the buccal delivery of macromolecules. Drug Dev. Ind. Pharm. 2014, 40, 579–590. [Google Scholar] [CrossRef] [PubMed]
- Gleeson, J.P.; McCartney, F. Striving Towards the Perfect In Vitro Oral Drug Absorption Model. Trends Pharmacol. Sci. 2019, 40, 720–724. [Google Scholar] [CrossRef] [PubMed]
- Collins, L.M.; Dawes, C. The surface area of the adult human mouth and thickness of the salivary film covering the teeth and oral mucosa. J. Dent. Res. 1987, 66, 1300–1302. [Google Scholar] [CrossRef] [PubMed]
- Naumova, E.A.; Dierkes, T.; Sprang, J.; Arnold, W.H. The oral mucosal surface and blood vessels. Head Face Med. 2013, 9, 8. [Google Scholar] [CrossRef]
- Squier, C.A.; Kremer, M.J. Biology of oral mucosa and esophagus. J. Natl. Cancer Inst. Monogr. 2001, 29, 7–15. [Google Scholar] [CrossRef]
- Senel, S.; Hincal, A.A. Drug permeation enhancement via buccal route: Possibilities and limitations. J. Control Release 2001, 72, 133–144. [Google Scholar] [CrossRef]
- Hassan, N.; Ahad, A.; Ali, M.; Ali, J. Chemical permeation enhancers for transbuccal drug delivery. Expert Opin. Drug Deliv. 2010, 7, 97–112. [Google Scholar] [CrossRef]
- Anselmo, A.C.; Gokarn, Y.; Mitragotri, S. Non-invasive delivery strategies for biologics. Nat. Rev. Drug Discov. 2019, 18, 19–40. [Google Scholar] [CrossRef]
- Padula, C.; Pescina, S.; Nicoli, S.; Santi, P. New Insights on the Mechanism of Fatty Acids as Buccal Permeation Enhancers. Pharmaceutics 2018, 10, 201. [Google Scholar] [CrossRef]
- Food & Drug Administration. Transdermal and Topical Delivery Systems Product Development and Quality Considerations; U.S. Food & Drug Administration: White Oak, MD, USA, 2019. [Google Scholar]
- Franz-Montan, M.; Cereda, C.M.; Gaspari, A.; da Silva, C.M.; de Araújo, D.R.; Padula, C.; Santi, P.; Narvaes, E.; Novaes, P.D.; Groppo, F.C.; et al. Liposomal-benzocaine gel formulation: Correlation between in vitro assays and in vivo topical anesthesia in volunteers. J. Liposome Res. 2013, 23, 54–60. [Google Scholar] [CrossRef]
- Diaz Del Consuelo, I.; Pizzolato, G.P.; Falson, F.; Guy, R.H.; Jacques, Y. Evaluation of pig esophageal mucosa as a permeability barrier model for buccal tissue. J. Pharm. Sci. 2005, 94, 2777–2788. [Google Scholar] [CrossRef]
- Diaz-Del Consuelo, I.; Jacques, Y.; Pizzolato, G.P.; Guy, R.H.; Falson, F. Comparison of the lipid composition of porcine buccal and esophageal permeability barriers. Arch. Oral. Biol. 2005, 50, 981–987. [Google Scholar] [CrossRef]
- Kulkarni, U.; Mahalingam, R.; Pather, I.; Li, X.; Jasti, B. Porcine buccal mucosa as in vitro model: Effect of biological and experimental variables. J. Pharm. Sci. 2010, 99, 1265–1277. [Google Scholar] [CrossRef]
- Lesch, C.A.; Squier, C.A.; Cruchley, A.; Williams, D.M.; Speight, P. The permeability of human oral mucosa and skin to water. J. Dent. Res. 1989, 68, 1345–1349. [Google Scholar] [CrossRef]
- De Vries, M.E.; Boddé, H.E.; Verhoef, J.C.; Junginger, H.E. Developments in buccal drug delivery. Crit. Rev. Ther. Drug Carrier Syst. 1991, 8, 271–303. [Google Scholar]
- Amores, S.; Domenech, J.; Colom, H.; Calpena, A.C.; Clares, B.; Gimeno, A.; Lauroba, J. An improved cryopreservation method for porcine buccal mucosa in ex vivo drug permeation studies using Franz diffusion cells. Eur. J. Pharm. Sci. 2014, 60, 49–54. [Google Scholar] [CrossRef]
- Caon, T.; Simões, C.M. Effect of freezing and type of mucosa on ex vivo drug permeability parameters. AAPS PharmSciTech 2011, 12, 587–592. [Google Scholar] [CrossRef]
- Kulkarni, U.; Mahalingam, R.; Pather, S.I.; Li, X.; Jasti, B. Porcine buccal mucosa as an in vitro model: Relative contribution of epithelium and connective tissue as permeability barriers. J. Pharm. Sci. 2009, 98, 471–483. [Google Scholar] [CrossRef]
- Franz-Montan, M.; Serpe, L.; Martinelli, C.C.; da Silva, C.B.; Santos, C.P.; Novaes, P.D.; Volpato, M.C.; De Paula, E.; Lopez, R.F.V.; Groppo, F.C. Evaluation of different pig oral mucosa sites as permeability barrier models for drug permeation studies. Eur. J. Pharm. Sci. 2016, 81, 52–59. [Google Scholar] [CrossRef]
- Kasting, G.B.; Bowman, L.A. Electrical analysis of fresh, excised human skin: A comparison with frozen skin. Pharm. Res. 1990, 7, 1141–1146. [Google Scholar] [CrossRef] [PubMed]
- Kasting, G.B.; Bowman, L.A. DC electrical properties of frozen, excised human skin. Pharm. Res. 1990, 7, 134–143. [Google Scholar] [CrossRef] [PubMed]
- Davies, D.J.; Ward, R.J.; Heylings, J.R. Multi-species assessment of electrical resistance as a skin integrity marker for in vitro percutaneous absorption studies. Toxicol. In Vitro 2004, 18, 351–358. [Google Scholar] [CrossRef]
- Zhang, Q.; Murawsky, M.; LaCount, T.; Kasting, G.B.; Li, S.K. Transepidermal water loss and skin conductance as barrier integrity tests. Toxicol. In Vitro 2018, 51, 129–135. [Google Scholar] [CrossRef]
- Fasano, W.J.; Manning, L.A.; Green, J.W. Rapid integrity assessment of rat and human epidermal membranes for in vitro dermal regulatory testing: Correlation of electrical resistance with tritiated water permeability. Toxicol. In Vitro 2002, 16, 731–740. [Google Scholar] [CrossRef]
- de Vries, M.E.; Boddk, H.E.; Verhoef, J.C.; Ponec, M.; Craane, W.I.H.M.; Junginger, H.E. Localization of the permeability barrier inside porcine buccal mucosa: A combined in vitro study of drug permeability, electrical resistance and tissue morphology. Int. J. Pharm. 1991, 76, 25–35. [Google Scholar] [CrossRef]
- Cubayachi, C.; Couto, R.O.; de Gaitani, C.M.; Pedrazzi, V.; Freitas, O.; Lopez, R.F. Needle-free buccal anesthesia using iontophoresis and amino amide salts combined in a mucoadhesive formulation. Colloids Surf. B Biointerfaces 2015, 136, 1193–1201. [Google Scholar] [CrossRef]
- Abraham, S.; Heckenthaler, T.; Morgenstern, Y.; Kaufman, Y. Effect of Temperature on the Structure, Electrical Resistivity, and Charge Capacitance of Supported Lipid Bilayers. Langmuir 2019, 35, 8709–8715. [Google Scholar] [CrossRef]
- Diaz Del Consuelo, I.; Falson, F.; Guy, R.H.; Jacques, Y. Transport of fentanyl through pig buccal and esophageal epithelia in vitro: Influence of concentration and vehicle pH. Pharm. Res. 2005, 22, 1525–1529. [Google Scholar] [CrossRef] [PubMed]
- Majid, H.; Bartel, A.; Burckhardt, B.B. Development, validation and standardization of oromucosal ex-vivo permeation studies for implementation in quality-controlled environments. J. Pharm. Biomed. Anal 2021, 194, 113769. [Google Scholar] [CrossRef]
- European Food Safety Authority. Guidance on Dermal Absorption. EFSA J. 2012, 15, e04873. [Google Scholar]
- Franz-Montan, M.; Baroni, D.; Brunetto, G.; Sobral, V.R.; da Silva, C.M.; Venâncio, P.; Zago, P.W.; Saia Cereda, C.M.; Volpato, M.C.; Groppo, F.C.; et al. Liposomal lidocaine gel for topical use at the oral mucosa: Characterization, in vitro assays and in vivo anesthetic efficacy in humans. J. Liposome Res. 2015, 25, 11–19. [Google Scholar] [CrossRef]
- White, E.A.; Orazem, M.E.; Bunge, A.L. Characterization of damaged skin by impedance spectroscopy: Mechanical damage. Pharm. Res. 2013, 30, 2036–2049. [Google Scholar] [CrossRef] [PubMed]
- Praça, F.S.G.; Medina, W.S.G.; Eloy, J.O.; Petrilli, R.; Campos, P.M.; Ascenso, A.; Bentley, M.V.L. Evaluation of critical parameters for in vitro skin permeation and penetration studies using animal skin models. Eur. J. Pharm. Sci. 2018, 111, 121–132. [Google Scholar] [CrossRef]
- Higuchi, W.I.; Li, S.K.; Ghanem, A.H.; Zhu, H.; Song, Y. Mechanistic aspects of iontophoresis in human epidermal membrane. J. Control Release 1999, 62, 13–23. [Google Scholar] [CrossRef]
- Li, S.K.; Ghanem, A.H.; Peck, K.D.; Higuchi, W.I. Pore induction in human epidermal membrane during low to moderate voltage iontophoresis: A study using AC iontophoresis. J. Pharm. Sci. 1999, 88, 419–427. [Google Scholar] [CrossRef] [PubMed]
- Li, S.K.; Peck, K.D. Passive and iontophoretic transport through the skin polar pathway. Skin Pharmacol. Physiol. 2013, 26, 243–253. [Google Scholar] [CrossRef]
- Orchardson, R.; Cadden, S.W. Mastication and swallowing: 1. Functions, performance and mechanisms. Dent. Update 2009, 36, 327–337. [Google Scholar] [CrossRef]
- van Eyk, A.D.; van der Biijl, P. Comparative permeability of fresh and frozen/thawed porcine buccal mucosa towards various chemical markers. SADJ 2006, 61, 200–203. [Google Scholar]
- Kulkarni, U.D.; Mahalingam, R.; Li, X.; Pather, I.; Jasti, B. Effect of experimental temperature on the permeation of model diffusants across porcine buccal mucosa. AAPS Pharm. Sci. Tech. 2011, 12, 579–586. [Google Scholar] [CrossRef]
- do Couto, R.O.; Cubayachi, C.; Calefi, P.L.; Lopez, R.F.V.; Pedrazzi, V.; de Gaitani, C.M.; de Freitas, O. Combining amino amide salts in mucoadhesive films enhances needle-free buccal anesthesia in adults. J. Control Release 2017, 266, 205–215. [Google Scholar] [CrossRef]
- Serpe, L.; Jain, A.; Macedo, C.; Groppo, F.; Volpato, M.; Gill, H.; Franz-Montan, M. Influence of salivary washout on drug delivery to the oral cavity using coated microneedles: An in vitro evaluation. Eur. J. Pharm. Sci. 2016, 93, 215–223. [Google Scholar] [CrossRef]
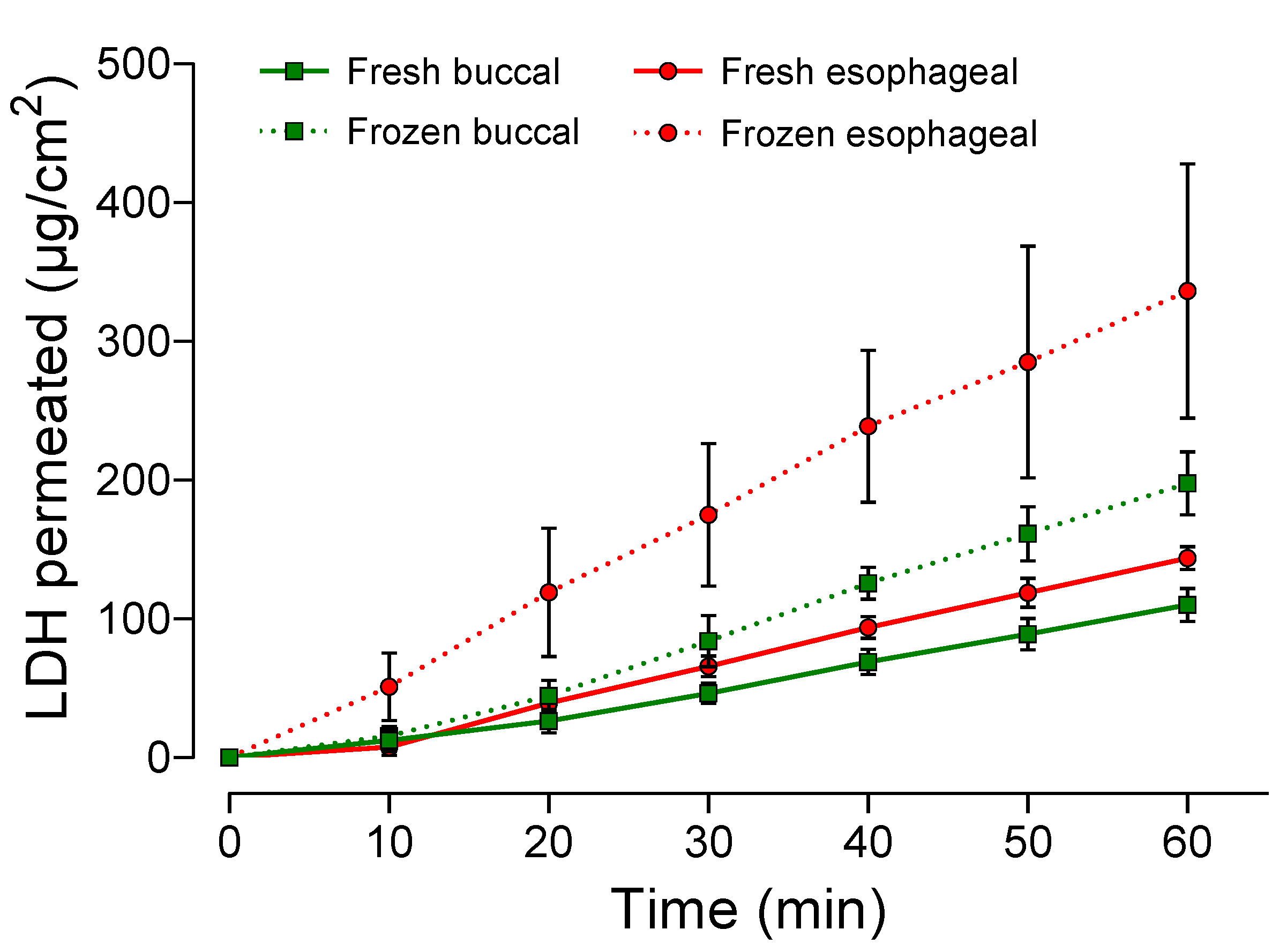
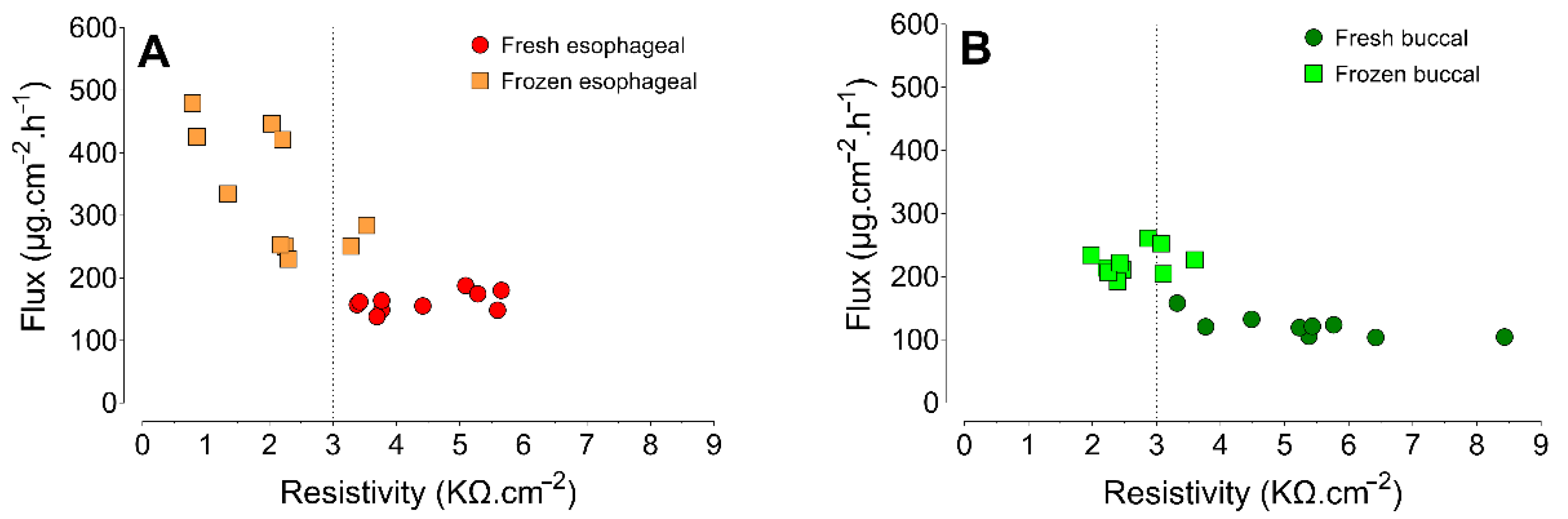
| Tissue | Jss (µg.cm−2.h−1) | EE * | Q1h (µg) | |
|---|---|---|---|---|
| Esophageal | Fresh | 161.6 ± 15.4 a | ---- | 254.3 ± 14.7 a |
| Frozen | 337.4 ± 96.3 b | 2.08 | 595.0 ± 162.3 b | |
| Buccal | Fresh | 120.9 ± 17.0 c | ---- | 194.8 ± 21.0 c |
| Frozen | 222.3 ± 21.7 d | 1.83 | 349.7 ± 40.1 d |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
de Araújo, J.S.M.; Volpato, M.C.; Muniz, B.V.; Xavier, G.G.A.; Martinelli, C.C.M.; Lopez, R.F.V.; Groppo, F.C.; Franz-Montan, M. Resistivity Technique for the Evaluation of the Integrity of Buccal and Esophageal Epithelium Mucosa for In Vitro Permeation Studies: Swine Buccal and Esophageal Mucosa Barrier Models. Pharmaceutics 2021, 13, 643. https://doi.org/10.3390/pharmaceutics13050643
de Araújo JSM, Volpato MC, Muniz BV, Xavier GGA, Martinelli CCM, Lopez RFV, Groppo FC, Franz-Montan M. Resistivity Technique for the Evaluation of the Integrity of Buccal and Esophageal Epithelium Mucosa for In Vitro Permeation Studies: Swine Buccal and Esophageal Mucosa Barrier Models. Pharmaceutics. 2021; 13(5):643. https://doi.org/10.3390/pharmaceutics13050643
Chicago/Turabian Stylede Araújo, Jaiza Samara Macena, Maria Cristina Volpato, Bruno Vilela Muniz, Gabriela Gama Augusto Xavier, Claudia Cristina Maia Martinelli, Renata Fonseca Vianna Lopez, Francisco Carlos Groppo, and Michelle Franz-Montan. 2021. "Resistivity Technique for the Evaluation of the Integrity of Buccal and Esophageal Epithelium Mucosa for In Vitro Permeation Studies: Swine Buccal and Esophageal Mucosa Barrier Models" Pharmaceutics 13, no. 5: 643. https://doi.org/10.3390/pharmaceutics13050643
APA Stylede Araújo, J. S. M., Volpato, M. C., Muniz, B. V., Xavier, G. G. A., Martinelli, C. C. M., Lopez, R. F. V., Groppo, F. C., & Franz-Montan, M. (2021). Resistivity Technique for the Evaluation of the Integrity of Buccal and Esophageal Epithelium Mucosa for In Vitro Permeation Studies: Swine Buccal and Esophageal Mucosa Barrier Models. Pharmaceutics, 13(5), 643. https://doi.org/10.3390/pharmaceutics13050643









