Use of Remdesivir in Patients Hospitalized for COVID-19 Pneumonia: Effect on the Hypoxic and Inflammatory State
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Patients’ Population
2.2. Treatment Protocols
2.3. Patients’ Management and Data Collection
2.4. Outcomes
2.5. Statistical Analysis
3. Results
3.1. Characteristics of the Study Groups
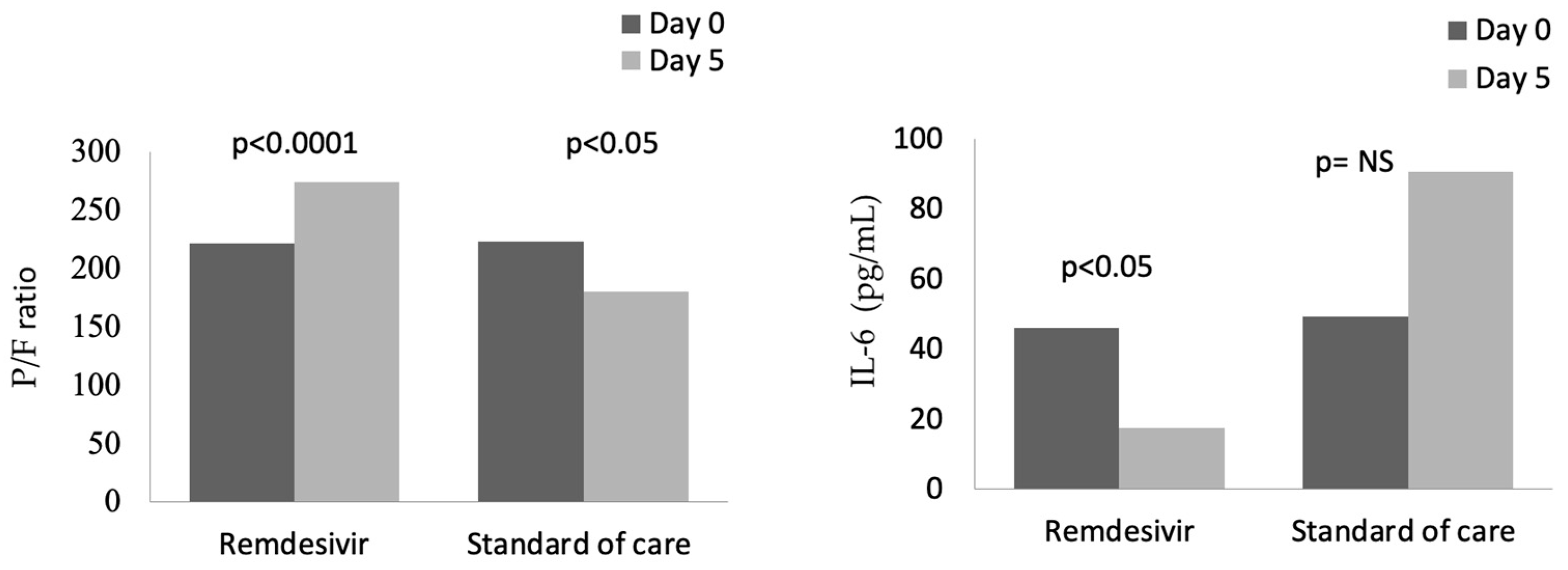
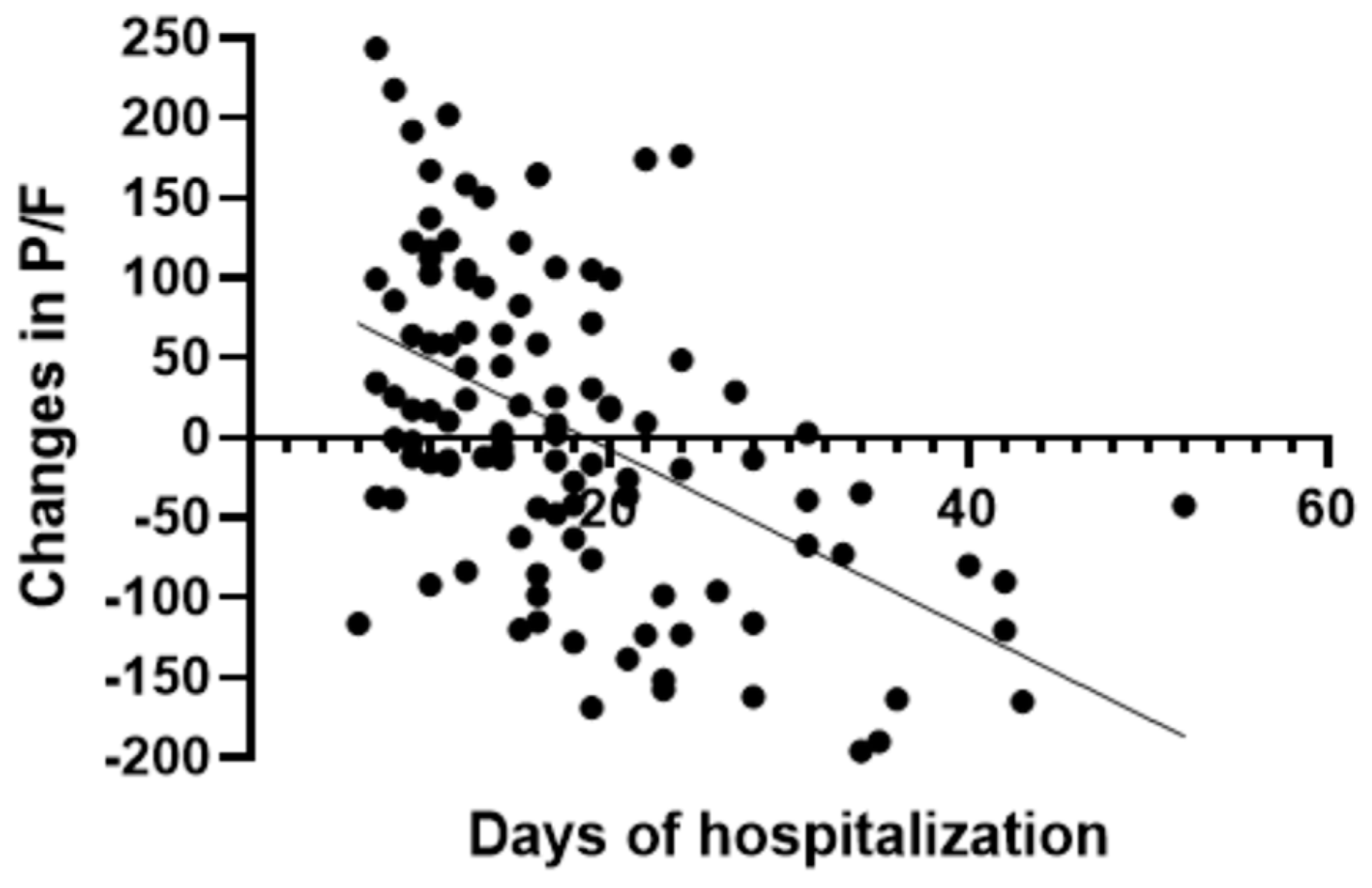
3.2. Effect of the Treatment with Remdesivir on the Hypoxic State and Disease Course
3.3. Effect of the Treatment with Remdesivir on the Inflammatory State
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Wang, H.; Paulson, K.R.; Pease, S.A.; Watson, S.; Comfort, H.; Zheng, P.; Aravkin, A.Y.; Bisignano, C.; Barber, R.M.; Alam, T.; et al. Estimating Excess Mortality Due to the COVID-19 Pandemic: A Systematic Analysis of COVID-19-Related Mortality, 2020–2021. Lancet 2022, 399, 1513–1536. [Google Scholar] [CrossRef]
- Team, F. Variation in the COVID-19 Infection–Fatality Ratio by Age, Time, and Geography during the Pre-Vaccine Era: A Systematic Analysis. Lancet 2022, 399, 1469–1488. [Google Scholar] [CrossRef]
- Aksak-Wąs, B.J.; Chober, D.; Serwin, K.; Scheibe, K.; Niścigorska-Olsen, J.; Niedźwiedź, A.; Dobrowolska, M.; Żybul, K.; Kubacka, M.; Zimoń, A.; et al. Remdesivir Reduces Mortality in Hemato-Oncology Patients with COVID-19. J. Inflamm. Res. 2022, 15, 4907–4920. [Google Scholar] [CrossRef] [PubMed]
- Niknam, Z.; Jafari, A.; Golchin, A.; Danesh Pouya, F.; Nemati, M.; Rezaei-Tavirani, M.; Rasmi, Y. Potential Therapeutic Options for COVID-19: An Update on Current Evidence. Eur. J. Med. Res. 2022, 27, 6. [Google Scholar] [CrossRef] [PubMed]
- Agostini, M.L.; Andres, E.L.; Sims, A.C.; Graham, R.L.; Sheahan, T.P.; Lu, X.; Smith, E.C.; Case, J.B.; Feng, J.Y.; Jordan, R.; et al. Coronavirus Susceptibility to the Antiviral Remdesivir (GS-5734) is Mediated by the Viral Polymerase and the Proofreading Exoribonuclease. mBio 2018, 9, 10-1128. [Google Scholar] [CrossRef]
- Yokoyama, Y.; Briasoulis, A.; Takagi, H.; Kuno, T. Effect of Remdesivir on Patients with COVID-19: A Network Meta-Analysis of Randomized Control Trials. Virus Res. 2020, 288, 198137. [Google Scholar] [CrossRef] [PubMed]
- Beigel, J.H.; Tomashek, K.M.; Dodd, L.E.; Mehta, A.K.; Zingman, B.S.; Kalil, A.C.; Hohmann, E.; Chu, H.Y.; Luetkemeyer, A.; Kline, S.; et al. Remdesivir for the Treatment of COVID-19—Final Report. N. Engl. J. Med. 2020, 383, 1813–1826. [Google Scholar] [CrossRef]
- Spinner, C.D.; Gottlieb, R.L.; Criner, G.J.; Arribas López, J.R.; Cattelan, A.M.; Soriano Viladomiu, A.; Ogbuagu, O.; Malhotra, P.; Mullane, K.M.; Castagna, A.; et al. Effect of Remdesivir vs Standard Care on Clinical Status at 11 Days in Patients with Moderate COVID-19: A Randomized Clinical Trial. JAMA 2020, 324, 1048–1057. [Google Scholar] [CrossRef] [PubMed]
- Grundeis, F.; Ansems, K.; Dahms, K.; Thieme, V.; Metzendorf, M.I.; Skoetz, N.; Benstoem, C.; Mikolajewska, A.; Griesel, M.; Fichtner, F.; et al. Remdesivir for the Treatment of COVID-19. Cochrane Database Syst. Rev. 2023, 2023, CD014962. [Google Scholar] [CrossRef]
- Sellitto, C.; Corbi, G.; Bertini, N.; Ascione, T.; Costantino, M.; Scarpati, G.; Piazza, O.; Filippelli, A.; Conti, V.; Pagliano, P. Effect of Remdesivir on Mortality Rate and Clinical Status of COVID-19 Patients: A Systematic Review with Meta-Analysis. J. Chemother. 2022, 35, 383–396. [Google Scholar] [CrossRef]
- WHO Solidarity Trial Consortium. Repurposed Antiviral Drugs for COVID-19—Interim WHO Solidarity Trial Results. N. Engl. J. Med. 2021, 384, 497–511. [Google Scholar] [CrossRef]
- Wang, Y.; Zhang, D.; Du, G.; Du, R.; Zhao, J.; Jin, Y.; Fu, S.; Gao, L.; Cheng, Z.; Lu, Q.; et al. Remdesivir in Adults with Severe COVID-19: A Randomised, Double-Blind, Placebo-Controlled, Multicentre Trial. Lancet 2020, 395, 1569–1578. [Google Scholar] [CrossRef] [PubMed]
- Garibaldi, B.T.; Wang, K.; Robinson, M.L.; Zeger, S.L.; Bandeen-Roche, K.; Wang, M.C.; Alexander, G.C.; Gupta, A.; Bollinger, R.; Xu, Y. Comparison of Time to Clinical Improvement with vs without Remdesivir Treatment in Hospitalized Patients with COVID-19. JAMA Netw. Open 2021, 4, e213071. [Google Scholar] [CrossRef] [PubMed]
- Zerbit, J.; Detroit, M.; Chevret, S.; Pene, F.; Luyt, C.E.; Ghosn, J.; Eyvrard, F.; Martin-Blondel, G.; Sarton, B.; Clere-Jehl, R.; et al. Remdesivir for Patients Hospitalized with COVID-19 Severe Pneumonia: A National Cohort Study (Remdeco-19). J. Clin. Med. 2022, 11, 6545. [Google Scholar] [CrossRef] [PubMed]
- Sinatti, G.; Santini, S.J.; Tarantino, G.; Picchi, G.; Cosimini, B.; Ranfone, F.; Casano, N.; Zingaropoli, M.A.; Iapadre, N.; Bianconi, S.; et al. PaO2/FiO2 Ratio Forecasts COVID-19 Patients’ Outcome Regardless of Age: A Cross-Sectional, Monocentric Study. Intern. Emerg. Med. 2022, 17, 665–673. [Google Scholar] [CrossRef]
- Santus, P.; Radovanovic, D.; Saderi, L.; Marino, P.; Cogliati, C.; De Filippis, G.; Rizzi, M.; Franceschi, E.; Pini, S.; Giuliani, F.; et al. Severity of Respiratory Failure at Admission and In-Hospital Mortality in Patients with COVID-19: A Prospective Observational Multicentre Study. BMJ Open 2020, 10, e043651. [Google Scholar] [CrossRef]
- Ranieri, V.M.; Rubenfeld, G.D.; Thompson, B.T.; Ferguson, N.D.; Caldwell, E.; Fan, E.; Camporota, L.; Slutsky, A.S. Acute Respiratory Distress Syndrome: The Berlin Definition. JAMA 2012, 307, 2526–2533. [Google Scholar] [CrossRef] [PubMed]
- Crimi, C.; Noto, A.; Madotto, F.; Ippolito, M.; Nolasco, S.; Campisi, R.; De Vuono, S.; Fiorentino, G.; Pantazopoulos, I.; Chalkias, A.; et al. High-Flow Nasal Oxygen versus Conventional Oxygen Therapy in Patients with COVID-19 Pneumonia and Mild Hypoxaemia: A Randomised Controlled Trial. Thorax 2023, 78, 354–361. [Google Scholar] [CrossRef]
- Charlson, M.E.; Pompei, P.; Ales, K.L.; MacKenzie, C.R. A New Method of Classifying Prognostic Comorbidity in Longitudinal Studies: Development and Validation. J. Chronic Dis. 1987, 40, 373–383. [Google Scholar] [CrossRef]
- Bhimraj, A.; Morgan, R.L.; Shumaker, A.H.; Lavergne, V.; Baden, L.; Cheng, V.C.C.; Edwards, K.M.; Gandhi, R.; Muller, W.J.; O’Horo, J.C.; et al. Infectious Diseases Society of America Guidelines on the Treatment and Management of Patients with COVID-19. Clin. Infect. Dis. 2020, 27, ciaa478. [Google Scholar] [CrossRef]
- Meng, Y.; Irwin, D.M.; Shen, Y. Ecology of SARS-CoV-2 in the Post-Pandemic Era. Lancet Microbe 2022, 4, e208. [Google Scholar] [CrossRef] [PubMed]
- Booth, A.; Reed, A.B.; Ponzo, S.; Yassaee, A.; Aral, M.; Plans, D.; Labrique, A.; Mohan, D. Population Risk Factors for Severe Disease and Mortality in COVID-19: A Global Systematic Review and Meta-Analysis. PLoS ONE 2021, 16, e0247461. [Google Scholar] [CrossRef] [PubMed]
- Grasselli, G.; Zangrillo, A.; Zanella, A.; Antonelli, M.; Cabrini, L.; Castelli, A.; Cereda, D.; Coluccello, A.; Foti, G.; Fumagalli, R.; et al. Baseline Characteristics and Outcomes of 1591 Patients Infected with SARS-CoV-2 Admitted to ICUs of the Lombardy Region, Italy. JAMA 2020, 323, 1574–1581. [Google Scholar] [CrossRef] [PubMed]
- Barratt-Due, A.; Olsen, I.C.; Nezvalova-Henriksen, K.; Kåsine, T.; Lund-Johansen, F.; Hoel, H.; Holten, A.R.; Tveita, A.; Mathiessen, A.; Haugli, M.; et al. Evaluation of the Effects of Remdesivir and Hydroxychloroquine on Viral Clearance in COVID-19: A Randomized Trial. Ann. Intern. Med. 2021, 174, 1261–1269. [Google Scholar] [CrossRef]
- Simioli, F.; Nicoletta, C.; Valentino, M.R.; Martino, M.; Annunziata, A.; Carannante, N.; Di Micco, P.; Fiorentino, G. Remdesivir in Severe COVID-19 and Non-Invasive Ventilation: A Real-Life Experience. Healthcare 2021, 9, 1108. [Google Scholar] [CrossRef] [PubMed]
- Sarhan, R.M.; Harb, H.S.; Abou Warda, A.E.; Salem-Bekhit, M.M.; Shakeel, F.; Alzahrani, S.A.; Madney, Y.M.; Boshra, M.S. Efficacy of the Early Treatment with Tocilizumab-Hydroxychloroquine and Tocilizumab-Remdesivir in Severe COVID-19 Patients. J. Infect. Public Health 2022, 15, 116–122. [Google Scholar] [CrossRef]
- Rezagholizadeh, A.; Khiali, S.; Sarbakhsh, P.; Entezari-Maleki, T. Remdesivir for Treatment of COVID-19; an Updated Systematic Review and Meta-Analysis. Eur. J. Pharmacol. 2021, 897, 173926. [Google Scholar] [CrossRef]
- Beckerman, R.; Gori, A.; Jeyakumar, S.; Malin, J.J.; Paredes, R.; Póvoa, P.; Smith, N.J.; Teixeira-Pinto, A. Remdesivir for the Treatment of Patients Hospitalized with COVID-19 Receiving Supplemental Oxygen: A Targeted Literature Review and Meta-Analysis. Sci. Rep. 2022, 12, 9622. [Google Scholar] [CrossRef]
- Luo, X.; Zhou, W.; Yan, X.; Guo, T.; Wang, B.; Xia, H.; Ye, L.; Xiong, J.; Jiang, Z.; Liu, Y.; et al. Prognostic Value of C-Reactive Protein in Patients with Coronavirus 2019. Clin. Infect. Dis. 2020, 71, 2174–2179. [Google Scholar] [CrossRef]
- Akira, S.; Kishimoto, T. IL-6 and NF-IL6 in Acute-Phase Response and Viral Infection. Immunol. Rev. 1992, 127, 25–50. [Google Scholar] [CrossRef]
- Yin, J.X.; Agbana, Y.L.; Sun, Z.S.; Fei, S.W.; Zhao, H.Q.; Zhou, X.N.; Chen, J.H.; Kassegne, K. Increased Interleukin-6 is Associated with Long COVID-19: A Systematic Review and Meta-Analysis. Infect. Dis. Poverty 2023, 12, 43. [Google Scholar] [CrossRef] [PubMed]
- Marino, A.; Munafò, A.; Augello, E.; Bellanca, C.M.; Bonomo, C.; Ceccarelli, M.; Musso, N.; Cantarella, G.; Cacopardo, B.; Bernardini, R. Sarilumab Administration in COVID-19 Patients: Literature Review and Considerations. Infect. Dis. Rep. 2022, 14, 360–371. [Google Scholar] [CrossRef] [PubMed]
- Soy, M.; Keser, G.; Atagündüz, P.; Tabak, F.; Atagündüz, I.; Kayhan, S. Cytokine Storm in COVID-19: Pathogenesis and Overview of Anti-Inflammatory Agents Used in Treatment. Clin. Rheumatol. 2020, 39, 2085–2094. [Google Scholar] [CrossRef] [PubMed]
- Hsu, H.Y.; Yang, C.W.; Lee, Y.Z.; Lin, Y.L.; Chang, S.Y.; Yang, R.B.; Liang, J.J.; Chao, T.L.; Liao, C.C.; Kao, H.C.; et al. Remdesivir and Cyclosporine Synergistically Inhibit the Human Coronaviruses OC43 and SARS-CoV-2. Front. Pharmacol. 2021, 12, 2086. [Google Scholar] [CrossRef] [PubMed]
- Kalantar, K.; Ghamar Talepoor, A.; Eshkevar Vakili, M.; Karami, N.; Kalani, M.; Ghandehari, F.; Kabelitz, D.; Meri, S.; Moattari, A. Th-1, Th-2, Th-9, Th-17, Th-22 Type Cytokine Concentrations of Critical COVID-19 Patients after Treatment with Remdesivir. Immunobiology 2023, 228, 152378. [Google Scholar] [CrossRef] [PubMed]
- Hadi, J.M.; Mohammad, H.M.; Ahmed, A.Y.; Tofiq, S.S.; Abdalrahman, L.B.; Qasm, A.A.; Ameer, A.M. Investigation of Serum Ferritin for the Prediction of COVID-19 Severity and Mortality: A Cross-Sectional Study. Cureus 2022, 14, e31982. [Google Scholar] [CrossRef] [PubMed]
- Narazaki, M.; Kishimoto, T. The Two-Faced Cytokine IL-6 in Host Defense and Diseases. Int. J. Mol. Sci. 2018, 19, 3528. [Google Scholar] [CrossRef] [PubMed]
- Angamo, M.T.; Mohammed, M.A.; Peterson, G.M. Efficacy and Safety of Remdesivir in Hospitalised COVID-19 Patients: A Systematic Review and Meta-Analysis. Infection 2022, 50, 27–41. [Google Scholar] [CrossRef] [PubMed]
- Al-Abdouh, A.; Bizanti, A.; Barbarawi, M.; Jabri, A.; Kumar, A.; Fashanu, O.E.; Khan, S.U.; Zhao, D.; Antar, A.A.R.; Michos, E.D. Remdesivir for the Treatment of COVID-19: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Contemp. Clin. Trials 2021, 101, 106272. [Google Scholar] [CrossRef]
- Lee, T.C.; Murthy, S.; Del Corpo, O.; Senécal, J.; Butler-Laporte, G.; Sohani, Z.N.; Brophy, J.M.; McDonald, E.G. Remdesivir for the Treatment of COVID-19: A Systematic Review and Meta-Analysis. Clin. Microbiol. Infect. 2022, 28, 1203–1210. [Google Scholar] [CrossRef]
- Okoli, G.N.; Rabbani, R.; Copstein, L.; Al-Juboori, A.; Askin, N.; Abou-Setta, A.M. Remdesivir for Coronavirus Disease 2019 (COVID-19): A Systematic Review with Meta-Analysis and Trial Sequential Analysis of Randomized Controlled Trials. Infect. Dis. 2021, 53, 691–699. [Google Scholar] [CrossRef] [PubMed]
- Kajova, M.; Kekäläinen, E.; Anttila, V.J.; Paajanen, J. Successful Treatment with a Short Course of Remdesivir in a Case of Prolonged COVID-19 in a Lymphoma Patient. Infect. Dis. 2022, 54, 455–459. [Google Scholar] [CrossRef] [PubMed]
- Zampino, R.; Mele, F.; Florio, L.L.; Bertolino, L.; Andini, R.; Galdo, M.; De Rosa, R.; Corcione, A.; Durante-Mangoni, E. Liver Injury in Remdesivir-Treated COVID-19 Patients. Hepatol. Int. 2020, 14, 881. [Google Scholar] [CrossRef] [PubMed]

| Item | Remdesivir (57) | Standard of Care (55) |
|---|---|---|
| Male sex (%) | 69.1% | 78.9% |
| Age (years) | 61.2 ± 10.8 | 63.4 ± 11.5 |
| Charlson Index Score | 2.4 ± 1.3 | 2.7 ±1.8 |
| BMI | 28.1 ± 5.4 | 28.2 ± 2.8 |
| P/F (mmHg) | 222 ± 62 | 223 ± 62 |
| PCO2 (mmHg) | 35.2 ± 6.5 | 34.2 ± 4.9 |
| RBC (×106/μL) | 4.6 ± 0.5 | 4.7 ± 0.7 |
| Hb (g/dL) | 13.8 ± 1.2 | 13.2 ± 2.2 |
| WBC (×103/μL) | 7.7 ± 3.4 | 8.2 ± 4.1 |
| PLT (×103/μL) | 242 ± 84 | 235 ± 94 |
| Neu (×103/μL) | 6.1 ± 3.4 | 6.7 ± 3.9 |
| Lym (×103/μL) | 1 ± 0.4 | 1.1 ± 0.6 |
| Mon (×103/μL) | 0.3 ± 0.5 | 0.3 ± 0.4 |
| Eos (×103/μL) | 0 ± 0 | 0 ± 0 |
| Bas (×103/μL) | 0.0 ± 0.2 | 0 ± 0 |
| CRP (mg/L) | 87.2 ± 61.3 | 90.2 ± 60.5 |
| Ferritin (ng/mL) | 624 ± 460 | 613 ± 426 |
| IL6 (pg/mL) | 45.9 ± 59.5 | 48.5 ± 48.7 |
| eGFR (mL/min/1.73 m2) | 86.5 ± 17.1 | 82.7 ± 25.9 |
| D-Dimer (μg/L) | 325 ± 292 | 389 ± 500 |
| AST (U/L) | 39.1 ± 19 | 34 ± 19.7 |
| ALT (U/L) | 38.2 ± 22.6 | 39 ± 48.8 |
| LDH (U/L) | 332 ± 114 | 336 ± 105 |
| PCT (ng/mL) | 0.1 ± 0.5 | 0.1 ± 0.4 |
| Remdesivir | Standard of Care | |||||
|---|---|---|---|---|---|---|
| Day 0 | Day 5 | p-Value | Day 0 | Day 5 | p-Value | |
| P/F (mmHg) | 222 ± 62 | 274 ± 97.4 | <0.0001 | 223 ± 62 | 183 ± 76 | 0.02 |
| RBC (×106/μL) | 4.6 ± 0.5 | 4.5 ± 0.6 | 0.28 | 4.7 ± 0.7 | 4.5 ± 0.7 | 0.09 |
| PLT (×103/μL) | 242 ± 84.8 | 357 ± 105 | <0.0001 | 235 ± 94.7 | 313 ± 106 | <0.0001 |
| Hb (g/dL) | 13.8 ± 1.2 | 15.4 ± 1.3 | 0.44 | 13.2 ± 2.1 | 12.6 ± 1.7 | <0.0001 |
| WBC (×103/μL) | 7.7 ± 3.4 | 9.6 ± 3.1 | <0.0001 | 8.2 ± 4.1 | 8.6 ± 3.1 | 0.4 |
| Neu (×103/μL) | 6.1 ± 3.4 | 6.1 ± 4.2 | <0.0001 | 6.7 ± 3.9 | 6.6 ± 2.8 | 0.91 |
| Lym (×103/μL) | 1 ± 0.4 | 1.5 ± 0.7 | <0.0001 | 1.1 ± 0.6 | 1.3 ± 0.7 | 0.09 |
| Mon (×103/μL) | 0.3 ± 0.5 | 0.6 ± 0.4 | <0.0001 | 0.3 ± 0.4 | 0.4 ± 0.5 | 0.22 |
| Eos (×103/μL) | 0 ± 0 | 0 ± 0 | 0.99 | 0 ± 0 | 0 ± 0 | 0.99 |
| Bas (×103/μL) | 0.0 ± 0.2 | 0 ± 0 | 0.32 | 0 ± 0 | 0 ± 0 | 0.99 |
| CRP (mg/L) | 87.2 ± 61.3 | 13.2 ± 26.3 | <0.0001 | 90.2 ± 60.5 | 33.1 ± 52 | <0.0001 |
| Ferritin (ng/mL) | 624 ± 460 | 483 ± 399 | 0.01 | 613 ± 528 | 605 ± 394 | 0.79 |
| IL6 (pg/mL) | 45.9 ± 59.5 | 17.5 ± 62 | 0.01 | 49.1 ± 47.5 | 90.5 ± 225 | 0.12 |
| eGFR (mL/min/1.73 m2) | 86.5 ± 17.1 | 94.1 ± 14.3 | <0.0001 | 82.7 ± 25.9 | 92.9 ± 23.5 | 0.03 |
| D-Dimer (μg/L) | 325 ± 292 | 283 ± 206 | 0.26 | 389 ± 500 | 505 ± 614 | 0.7 |
| AST (U/L) | 39.1 ± 19 | 34.6 ± 17.1 | 0.15 | 34 ± 19.7 | 38.4 ± 27 | 0.4 |
| ALT (U/L) | 38.2 ± 22.7 | 64.1 ± 41 | <0.0001 | 39 ± 48.8 | 61.2 ± 60.1 | 0.06 |
| LDH (U/L) | 332 ± 114 | 304 ± 108 | 0.07 | 336 ± 105 | 299 ± 103 | 0.05 |
| Remdesivir (57) | Standard of Care (55) | p-Value | |
|---|---|---|---|
| Escalation to NIV/VMI, n. (%) | 15 (25.3) | 2 8 (49.1) | <0.05 |
| Days of hospitalization, n. | 15.3 ± 8.3 | 20.1 ± 8.8 | <0.05 |
| Admission to ICU, n. | 1 | 2 | |
| Death, n. | 0 | 1 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Libra, A.; Ciancio, N.; Sambataro, G.; Sciacca, E.; Muscato, G.; Marino, A.; Vancheri, C.; Spicuzza, L. Use of Remdesivir in Patients Hospitalized for COVID-19 Pneumonia: Effect on the Hypoxic and Inflammatory State. Viruses 2023, 15, 2101. https://doi.org/10.3390/v15102101
Libra A, Ciancio N, Sambataro G, Sciacca E, Muscato G, Marino A, Vancheri C, Spicuzza L. Use of Remdesivir in Patients Hospitalized for COVID-19 Pneumonia: Effect on the Hypoxic and Inflammatory State. Viruses. 2023; 15(10):2101. https://doi.org/10.3390/v15102101
Chicago/Turabian StyleLibra, Alessandro, Nicola Ciancio, Gianluca Sambataro, Enrico Sciacca, Giuseppe Muscato, Andrea Marino, Carlo Vancheri, and Lucia Spicuzza. 2023. "Use of Remdesivir in Patients Hospitalized for COVID-19 Pneumonia: Effect on the Hypoxic and Inflammatory State" Viruses 15, no. 10: 2101. https://doi.org/10.3390/v15102101
APA StyleLibra, A., Ciancio, N., Sambataro, G., Sciacca, E., Muscato, G., Marino, A., Vancheri, C., & Spicuzza, L. (2023). Use of Remdesivir in Patients Hospitalized for COVID-19 Pneumonia: Effect on the Hypoxic and Inflammatory State. Viruses, 15(10), 2101. https://doi.org/10.3390/v15102101







