How Can Nanotechnology Help to Repair the Body? Advances in Cardiac, Skin, Bone, Cartilage and Nerve Tissue Regeneration
Abstract
:1. Introduction

2. Electrospinning
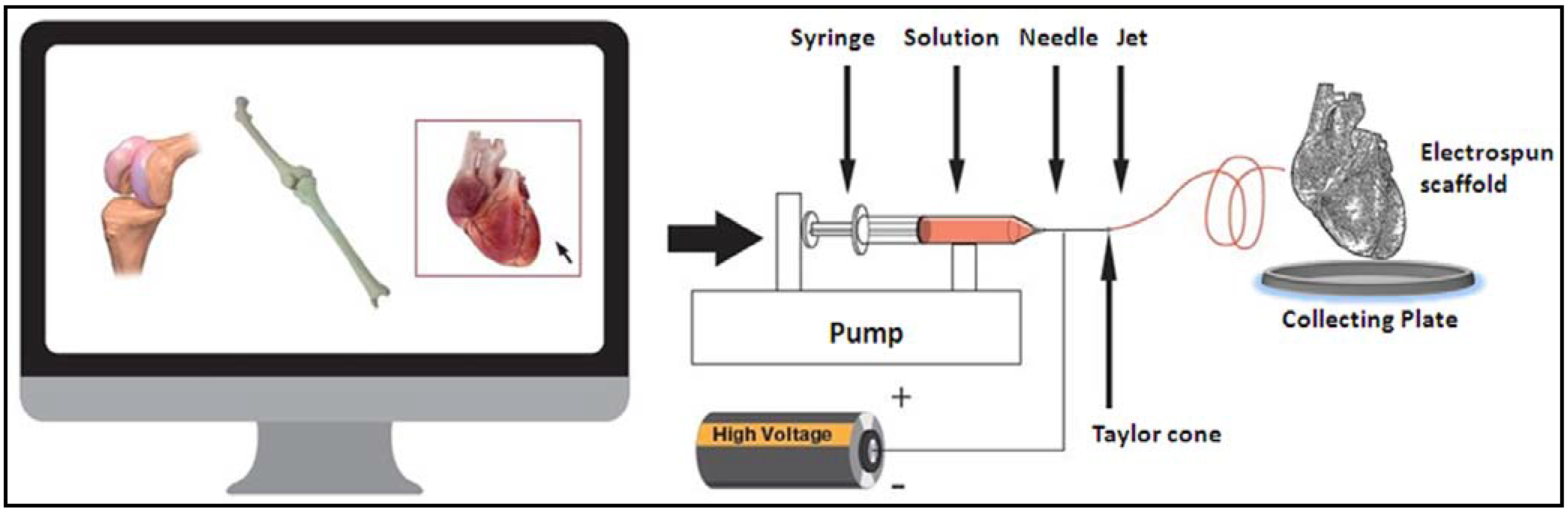
3. Skin Regeneration by Nanotechnological Approaches
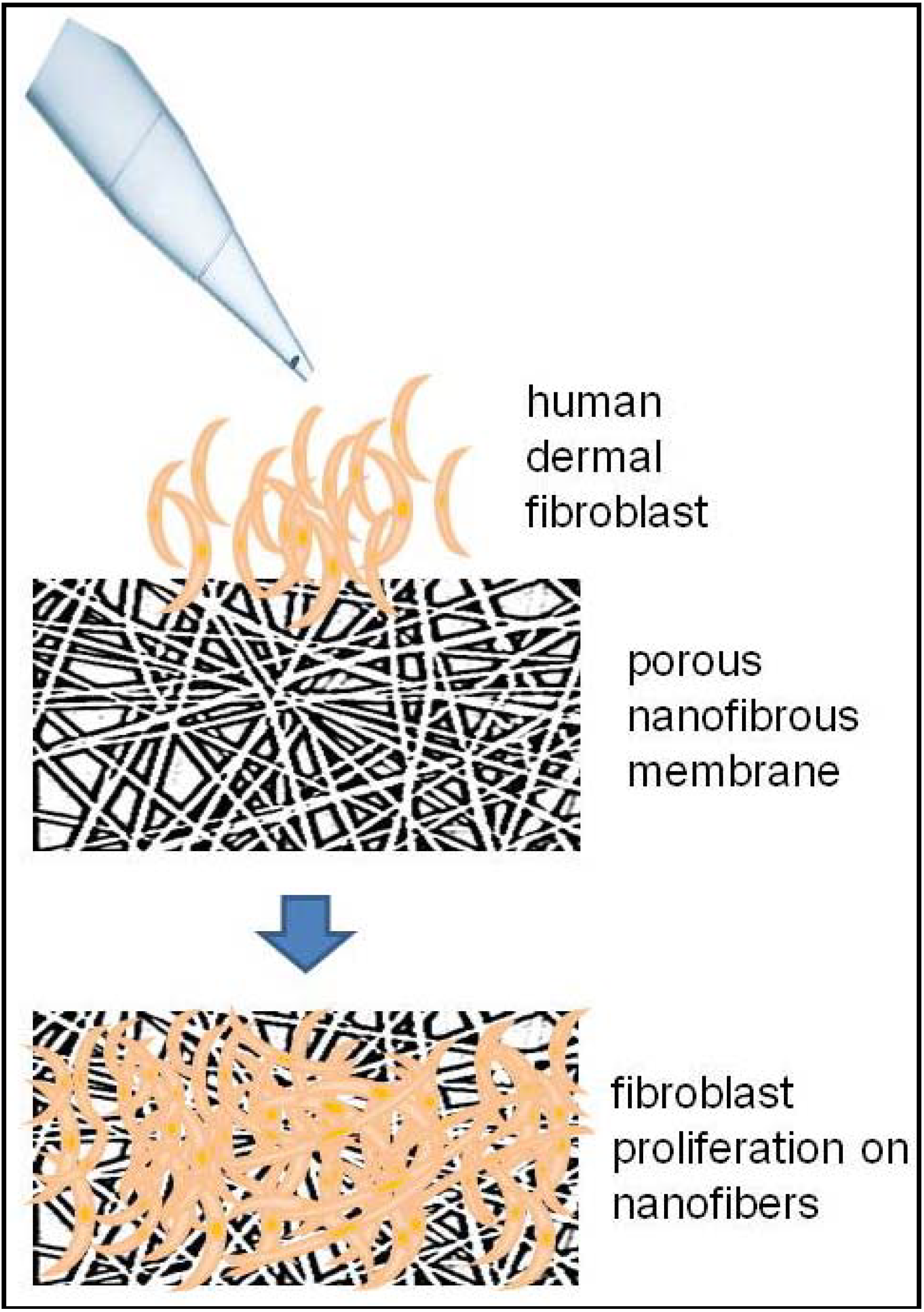

4. Nanotechnological Advances in Cartilage Repair
5. Applying Nanotechnology to Bone Reconstruction
6. Nanotechnology for Nerve Regeneration
7. Nanotecnology for Cardiac Tissue Regeneration
8. Clinical Trials
| ClinicalTrials.gov Identifier | Clinical trial name | Nanotechnology | Tissue | Status/Phase |
|---|---|---|---|---|
| NCT01539980 | Clinical Study on Silk Sericin Wound Dressing for Split-thickness Skin Graft Donor Sites Treatment | Device: Sericin scaffold | Skin | Phase 1 Phase 2 |
| NCT01108263 | Use of INTEGRA™ Flowable Wound Matrix to Manage Diabetic Foot Ulcers | INTEGRA™ Flowable Matrix (Collagen) | Skin | Phase 4 |
| NCT00317629 | Controlled Nitric Oxide-Releasing Patch Versus Meglumine Antimoniate in the Treatment of Cutaneous Leishmaniasis | Electrospinning-controlled nitric oxide releasing patch | Skin | Phase 3 |
| NCT00729716 | Comparison of BioCart™II With Microfracture for Treatment of Cartilage Defects of the Femoral Condyle | BioCart™II scaffold | Cartilage | Phase 2 |
| NCT01183637 | Evaluation of an Acellular Osteochondral Graft for Cartilage Lesions Pilot Trial (EAGLE Pilot) | bioresorbable scaffold | Bone/Cartilage | Phase 2 |
| NCT01218945 | Development of Bone Grafts Using Adipose-Derived Stem Cells and Different Scaffolds | Bone scaffold | Bone | recruiting participants |
| NCT01435434 | Mononucleotide Autologous Stem Cells and Demineralized Bone Matrix in the Treatment of Non-Union/Delayed Fractures | Ignite®ICS injectable scaffold | Bone | Not yet recruiting |
| NCT00948025 | A Comparative Post-Marketing Study of Commercially Available Peripheral Nerve Gap Repair Options (CHANGE) | Device: Hollow tube nerve conduit, synthetic or biosynthetic | Nerve | Active, not recruiting Phase 4 |
| NCT01573650 | Optimization of Peripheral Nerve Reconstruction: A Non-Inferiority Trial | Device: Fibrin Conduit | Nerve | not yet open for participant recruitment |
| NCT01270139 | Plasmonic Photothermal Therapy of Flow-Limiting Atherosclerotic Lesions With Silica–Gold Nanoparticles: a First-in-Man Study | Silica–gold nanoparticles. Iron bearing nanoparticles. | Heart | Has results Phase 1–2 |
| NCT00124943 | A Phase I/II Safety Trial of Intracoronary Administration of Systemic Nanoparticle Paclitaxel (ABI-007) for the Prevention of In-Stent Restenosis | Nanoparticle paclitaxel | Heart | Has results Phase 1–2 |
9. Conclusions
Acknowledgments
References
- de Mel, A.; Seifalian, A.M.; Birchall, M.A. Orchestrating cell/material interactions for tissue engineering of surgical implants. Macromol. Biosci. 2012, 12, 1010–1021. [Google Scholar] [CrossRef] [PubMed]
- Peran, M.; Garcia, M.A.; Lopez-Ruiz, E.; Bustamante, M.; Jimenez, G.; Madeddu, R.; Marchal, J.A. Functionalized nanostructures with application in regenerative medicine. Int. J. Mol. Sci. 2012, 13, 3847–3886. [Google Scholar] [CrossRef] [PubMed]
- Badylak, S.F.; Freytes, D.O.; Gilbert, T.W. Extracellular matrix as a biological scaffold material: Structure and function. Acta Biomater. 2009, 5, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Kakisis, J.D.; Liapis, C.D.; Breuer, C.; Sumpio, B.E. Artificial blood vessel: the Holy Grail of peripheral vascular surgery. J. Vasc. Surg. 2005, 41, 349–354. [Google Scholar] [CrossRef] [PubMed]
- Li, W.J.; Laurencin, C.T.; Caterson, E.J.; Tuan, R.S.; Ko, F.K. Electrospun nanofibrous structure: A novel scaffold for tissue engineering. J. Biomed. Mater. Res. 2002, 60, 613–621. [Google Scholar] [CrossRef] [PubMed]
- Liang, D.; Hsiao, B.S.; Chu, B. Functional electrospun nanofibrous scaffolds for biomedical applications. Adv. Drug Deliv. Rev. 2007, 59, 1392–1412. [Google Scholar] [CrossRef] [PubMed]
- Sen, C.K.; Gordillo, G.M.; Roy, S.; Kirsner, R.; Lambert, L.; Hunt, T.K.; Gottrup, F.; Gurtner, G.C.; Longaker, M.T. Human skin wounds: a major and snowballing threat to public health and the economy. Wound Repair Regen. 2009, 17, 763–771. [Google Scholar] [CrossRef] [PubMed]
- Clark, K.L. Nutritional considerations in joint health. Clin. Sports Med. 2007, 26, 101–118. [Google Scholar] [CrossRef] [PubMed]
- Viswanathan, H.N.; Curtis, J.R.; Yu, J.; White, J.; Stolshek, B.S.; Merinar, C.; Balasubramanian, A.; Kallich, J.D.; Adams, J.L.; Wade, S.W. Direct healthcare costs of osteoporosis-related fractures in managed care patients receiving pharmacological osteoporosis therapy. Appl. Health Econ. Health Policy 2012, 10, 163–173. [Google Scholar] [CrossRef]
- Jamison, D.T.; Breman, J.G.; Measham, A.R.; Alleyne, G.; Claeson, M.; Evans, D.B.; Jha, P.; Mills, A.; Musgrove, P. Priorities in Health; World Bank: Washington, DC, USA, 2006. [Google Scholar]
- Heidenreich, P.A.; Trogdon, J.G.; Khavjou, O.A.; Butler, J.; Dracup, K.; Ezekowitz, M.D.; Finkelstein, E.A.; Hong, Y.; Johnston, S.C.; Khera, A.; et al. Forecasting the future of cardiovascular disease in the United States: A policy statement from the American Heart Association. Circulation 2011, 123, 933–944. [Google Scholar] [CrossRef] [PubMed]
- Ramakrishna, S.; Fujihara, K.; Teo, W.E.; Lim, T.C.; Ma, Z. An Introduction to Electrospinning and Nanofibers; World Scientific Publishing Co.: Hackensack, NJ, USA, 2005. [Google Scholar]
- Pham, Q.P.; Sharma, U.; Mikos, A.G. Electrospinning of polymeric nanofibers for tissue engineering applications: a review. Tissue Eng. 2006, 12, 1197–1211. [Google Scholar] [CrossRef] [PubMed]
- Venugopal, J.; Ramakrishna, S. Applications of polymer nanofibers in biomedicine and biotechnology. Appl. Biochem. Biotechnol. 2005, 125, 147–158. [Google Scholar] [CrossRef] [PubMed]
- La Francesca, S. Nanotechnology and stem cell therapy for cardiovascular diseases: Potential applications. Methodist Debakey Cardiovasc. J. 2012, 8, 28–35. [Google Scholar]
- Mohamed, A.; Xing, M.M. Nanomaterials and nanotechnology for skin tissue engineering. Int. J. Burns Trauma 2012, 2, 29–41. [Google Scholar] [PubMed]
- Huang, S.; Fu, X. Naturally derived materials-based cell and drug delivery systems in skin regeneration. J. Control. Release 2010, 142, 149–159. [Google Scholar] [CrossRef] [PubMed]
- Stynes, G.; Kiroff, G.K.; Morrison, W.A.; Kirkland, M.A. Tissue compatibility of biomaterials: Benefits and problems of skin biointegration. ANZ J. Surg. 2008, 78, 654–659. [Google Scholar] [CrossRef] [PubMed]
- Liu, W.; Cao, Y.L. Application of scaffold materials in tissue reconstruction in immunocompetent mammals: Our experience and future requirements. Biomaterials 2007, 28, 5078–5086. [Google Scholar] [CrossRef] [PubMed]
- Tran, P.A.; Zhang, L.; Webster, T.J. Carbon nanofibers and carbon nanotubes in regenerative medicine. Adv. Drug Deliv. Rev. 2009, 61, 1097–1114. [Google Scholar] [CrossRef] [PubMed]
- Khil, M.S.; Cha, D.I.; Kim, H.Y.; Kim, I.S.; Bhattarai, N. Electrospun nanofibrous polyurethane membrane as wound dressing. J. Biomed. Mater. Res. B Appl. Biomater. 2003, 67, 675–679. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.C.; Su, C.H.; Chen, C.C. Water absorbing and antibacterial properties of N-isopropyl acrylamide grafted and collagen/chitosan immobilized polypropylene nonwoven fabric and its application on wound healing enhancement. J. Biomed. Mater. Res. A 2008, 84, 1006–1017. [Google Scholar] [CrossRef] [PubMed]
- van den Bogaerdt, A.J.; van Zuijlen, P.P.; van Galen, M.; Lamme, E.N.; Middelkoop, E. The suitability of cells from different tissues for use in tissue-engineered skin substitutes. Arch. Dermatol. Res. 2002, 294, 135–142. [Google Scholar]
- Ojeh, N.O.; Frame, J.D.; Navsaria, H.A. In vitro characterization of an artificial dermal scaffold. Tissue Eng. 2001, 7, 457–472. [Google Scholar] [CrossRef] [PubMed]
- Chandrasekaran, A.R.; Venugopal, J.; Sundarrajan, S.; Ramakrishna, S. Fabrication of a nanofibrous scaffold with improved bioactivity for culture of human dermal fibroblasts for skin regeneration. Biomed. Mater. 2011, 6, 015001:1–015001:10. [Google Scholar] [CrossRef]
- Venugopal, J.R.; Zhang, Y.; Ramakrishna, S. In vitro culture of human dermal fibroblasts on electrospun polycaprolactone collagen nanofibrous membrane. Artif. Organs 2006, 30, 440–446. [Google Scholar] [CrossRef] [PubMed]
- Jin, G.; Prabhakaran, M.P.; Ramakrishna, S. Stem cell differentiation to epidermal lineages on electrospun nanofibrous substrates for skin tissue engineering. Acta Biomater. 2011, 7, 3113–3122. [Google Scholar] [CrossRef] [PubMed]
- Tchemtchoua, V.T.; Atanasova, G.; Aqil, A.; Filee, P.; Garbacki, N.; Vanhooteghem, O.; Deroanne, C.; Noel, A.; Jerome, C.; Nusgens, B.; et al. Development of a chitosan nanofibrillar scaffold for skin repair and regeneration. Biomacromolecules 2011, 12, 3194–3204. [Google Scholar] [CrossRef] [PubMed]
- Lenz, G.; Mansson, P. Growth factors as pharmaceuticals. Pharm. Technol. 1991, 15, 34–38. [Google Scholar]
- Yang, Y.; Xia, T.; Chen, F.; Wei, W.; Liu, C.; He, S.; Li, X. Electrospun fibers with plasmid bFGF polyplex loadings promote skin wound healing in diabetic rats. Mol. Pharm. 2012, 9, 48–58. [Google Scholar] [CrossRef] [PubMed]
- Tocco, I.; Zavan, B.; Bassetto, F.; Vindigni, V. Nanotechnology-based therapies for skin wound regeneration. J. Nanomater. 2012. [Google Scholar] [CrossRef]
- Ziv-Polat, O.; Topaz, M.; Brosh, T.; Margel, S. Enhancement of incisional wound healing by thrombin conjugated iron oxide nanoparticles. Biomaterials 2010, 31, 741–747. [Google Scholar] [CrossRef] [PubMed]
- Lopez-Ruiz, E.; Peran, M.; Cobo-Molinos, J.; Jimenez, G.; Picon, M.; Bustamante, M.; Arrebola, F.; Hernandez-Lamas, M.C.; Delgado-Martinez, A.D.; Montanez, E.; Marchal, J.A. Chondrocytes extract from patients with osteoarthritis induces chondrogenesis in infrapatellar fat pad-derived stem cells. Osteoarthr. Cartil. 2013, 21, 246–258. [Google Scholar] [CrossRef] [PubMed]
- Vinatier, C.; Bouffi, C.; Merceron, C.; Gordeladze, J.; Brondello, J.M.; Jorgensen, C.; Weiss, P.; Guicheux, J.; Noel, D. Cartilage tissue engineering: Towards a biomaterial-assisted mesenchymal stem cell therapy. Curr. Stem Cell Res. Ther. 2009, 4, 318–329. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.H.; Shin, H. Matrices and scaffolds for delivery of bioactive molecules in bone and cartilage tissue engineering. Adv. Drug Deliv. Rev. 2007, 59, 339–359. [Google Scholar] [CrossRef] [PubMed]
- Capito, R.M.; Spector, M. Scaffold-based articular cartilage repair. IEEE Eng. Med. Biol. Mag. 2003, 22, 42–50. [Google Scholar] [CrossRef] [PubMed]
- Alves da Silva, M.L.; Martins, A.; Costa-Pinto, A.R.; Costa, P.; Faria, S.; Gomes, M.; Reis, R.L.; Neves, N.M. Cartilage tissue engineering using electrospun PCL nanofiber meshes and MSCs. Biomacromolecules 2010, 11, 3228–3236. [Google Scholar]
- Dahl, J.P.; Caballero, M.; Pappa, A.K.; Madan, G.; Shockley, W.W.; van Aalst, J.A. Analysis of human auricular cartilage to guide tissue-engineered nanofiber-based chondrogenesis: Implications for microtia reconstruction. Otolaryngol. Head Neck Surg. 2011, 145, 915–923. [Google Scholar] [CrossRef] [PubMed]
- Coburn, J.M.; Gibson, M.; Monagle, S.; Patterson, Z.; Elisseeff, J.H. Bioinspired nanofibers support chondrogenesis for articular cartilage repair. Proc. Natl. Acad. Sci. USA 2012, 109, 10012–10017. [Google Scholar] [CrossRef] [PubMed]
- Shafiee, A.; Soleimani, M.; Chamheidari, G.A.; Seyedjafari, E.; Dodel, M.; Atashi, A.; Gheisari, Y. Electrospun nanofiber-based regeneration of cartilage enhanced by mesenchymal stem cells. J. Biomed. Mater. Res. A 2011, 99, 467–478. [Google Scholar] [CrossRef] [PubMed]
- Jung, Y.; Chung, Y.I.; Kim, S.H.; Tae, G.; Kim, Y.H.; Rhie, J.W. In situ chondrogenic differentiation of human adipose tissue-derived stem cells in a TGF-beta1 loaded fibrin-poly(lactide-caprolactone) nanoparticulate complex. Biomaterials 2009, 30, 4657–4664. [Google Scholar] [CrossRef] [PubMed]
- Park, J.S.; Yang, H.N.; Woo, D.G.; Jeon, S.Y.; Do, H.J.; Lim, H.Y.; Kim, J.H.; Park, K.H. Chondrogenesis of human mesenchymal stem cells mediated by the combination of SOX trio SOX5, 6, and 9 genes complexed with PEI-modified PLGA nanoparticles. Biomaterials 2011, 32, 3679–3688. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.H.; Park, J.S.; Yang, H.N.; Woo, D.G.; Jeon, S.Y.; Do, H.J.; Lim, H.Y.; Kim, J.M.; Park, K.H. The use of biodegradable PLGA nanoparticles to mediate SOX9 gene delivery in human mesenchymal stem cells (hMSCs) and induce chondrogenesis. Biomaterials 2011, 32, 268–278. [Google Scholar] [CrossRef] [PubMed]
- Jeon, S.Y.; Park, J.S.; Yang, H.N.; Woo, D.G.; Park, K.H. Co-delivery of SOX9 genes and anti-Cbfa-1 siRNA coated onto PLGA nanoparticles for chondrogenesis of human MSCs. Biomaterials 2012, 33, 4413–4423. [Google Scholar] [CrossRef] [PubMed]
- Park, J.S.; Yang, H.N.; Woo, D.G.; Chung, H.M.; Park, K.H. In vitro and in vivo chondrogenesis of rabbit bone marrow-derived stromal cells in fibrin matrix mixed with growth factor loaded in nanoparticles. Tissue Eng. A 2009, 15, 2163–2175. [Google Scholar] [CrossRef]
- Park, J.S.; Yang, H.N.; Woo, D.G.; Jeon, S.Y.; Park, K.H. Chondrogenesis of human mesenchymal stem cells in fibrin constructs evaluated in vitro and in nude mouse and rabbit defects models. Biomaterials 2011, 32, 1495–1507. [Google Scholar] [CrossRef] [PubMed]
- Na, K.; Kim, S.; Park, K.; Kim, K.; Woo, D.G.; Kwon, I.C.; Chung, H.M.; Park, K.H. Heparin/poly(l-lysine) nanoparticle-coated polymeric microspheres for stem-cell therapy. J. Am. Chem Soc. 2007, 129, 5788–5789. [Google Scholar] [CrossRef] [PubMed]
- Hsu, S.H.; Huang, T.B.; Cheng, S.J.; Weng, S.Y.; Tsai, C.L.; Tseng, C.S.; Chen, D.C.; Liu, T.Y.; Fu, K.Y.; Yen, B.L. Chondrogenesis from human placenta-derived mesenchymal stem cells in three-dimensional scaffolds for cartilage tissue engineering. Tissue Eng. A 2011, 17, 1549–1560. [Google Scholar] [CrossRef]
- Liu, L.; Wang, Y.; Guo, S.; Wang, Z.; Wang, W. Porous polycaprolactone/nanohydroxyapatite tissue engineering scaffolds fabricated by combining NaCl and PEG as co-porogens: structure, property, and chondrocyte-scaffold interaction in vitro. J. Biomed. Mater. Res. B Appl. Biomater. 2012, 100, 956–966. [Google Scholar] [CrossRef] [PubMed]
- Xue, D.; Zheng, Q.; Zong, C.; Li, Q.; Li, H.; Qian, S.; Zhang, B.; Yu, L.; Pan, Z. Osteochondral repair using porous poly(lactide-co-glycolide)/nano-hydroxyapatite hybrid scaffolds with undifferentiated mesenchymal stem cells in a rat model. J. Biomed. Mater. Res. A 2010, 94, 259–270. [Google Scholar] [CrossRef] [PubMed]
- Kon, E.; Delcogliano, M.; Filardo, G.; Busacca, M.; Di Martino, A.; Marcacci, M. Novel nano-composite multilayered biomaterial for osteochondral regeneration: A pilot clinical trial. Am. J. Sports Med. 2011, 39, 1180–1190. [Google Scholar] [CrossRef] [PubMed]
- Arrington, E.D.; Smith, W.J.; Chambers, H.G.; Bucknell, A.L.; Davino, N.A. Complications of iliac crest bone graft harvesting. Clin. Orthop. Relat. Res. 1996, 300–309. [Google Scholar]
- Giannoudis, P.V.; Dinopoulos, H.; Tsiridis, E. Bone substitutes: An update. Injury 2005, 36, S20–S27. [Google Scholar] [CrossRef] [PubMed]
- Miyazaki, M.; Tsumura, H.; Wang, J.C.; Alanay, A. An update on bone substitutes for spinal fusion. Eur. Spine J. 2009, 18, 783–799. [Google Scholar] [CrossRef] [PubMed]
- Kneser, U.; Schaefer, D.J.; Polykandriotis, E.; Horch, R.E. Tissue engineering of bone: The reconstructive surgeon’s point of view. J. Cell. Mol. Med. 2006, 10, 7–19. [Google Scholar] [CrossRef] [PubMed]
- Rho, J.Y.; Kuhn-Spearing, L.; Zioupos, P. Mechanical properties and the hierarchical structure of bone. Med. Eng. Phys. 1998, 20, 92–102. [Google Scholar] [CrossRef] [PubMed]
- Yoshimoto, H.; Shin, Y.M.; Terai, H.; Vacanti, J.P. A biodegradable nanofiber scaffold by electrospinning and its potential for bone tissue engineering. Biomaterials 2003, 24, 2077–2082. [Google Scholar] [CrossRef] [PubMed]
- Frohbergh, M.E.; Katsman, A.; Botta, G.P.; Lazarovici, P.; Schauer, C.L.; Wegst, U.G.; Lelkes, P.I. Electrospun hydroxyapatite-containing chitosan nanofibers crosslinked with genipin for bone tissue engineering. Biomaterials 2012, 33, 9167–9178. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.H.; Jeong, L.; Park, H.N.; Shin, S.Y.; Park, W.H.; Lee, S.C.; Kim, T.I.; Park, Y.J.; Seol, Y.J.; Lee, Y.M.; et al. Biological efficacy of silk fibroin nanofiber membranes for guided bone regeneration. J. Biotechnol. 2005, 120, 327–339. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, L.T.; Liao, S.; Chan, C.K.; Ramakrishna, S. Enhanced osteogenic differentiation with 3D electrospun nanofibrous scaffolds. Nanomedicine 2012, 7, 1561–1575. [Google Scholar] [CrossRef] [PubMed]
- Ravichandran, R.; Venugopal, J.R.; Sundarrajan, S.; Mukherjee, S.; Ramakrishna, S. Precipitation of nanohydroxyapatite on PLLA/PBLG/Collagen nanofibrous structures for the differentiation of adipose derived stem cells to osteogenic lineage. Biomaterials 2012, 33, 846–855. [Google Scholar] [CrossRef] [PubMed]
- Schofer, M.D.; Roessler, P.P.; Schaefer, J.; Theisen, C.; Schlimme, S.; Heverhagen, J.T.; Voelker, M.; Dersch, R.; Agarwal, S.; Fuchs-Winkelmann, S.; Paletta, J.R. Electrospun PLLA nanofiber scaffolds and their use in combination with BMP-2 for reconstruction of bone defects. PLoS One 2011, 6, e25462. [Google Scholar] [CrossRef] [PubMed]
- Schofer, M.D.; Tunnermann, L.; Kaiser, H.; Roessler, P.P.; Theisen, C.; Heverhagen, J.T.; Hering, J.; Voelker, M.; Agarwal, S.; Efe, T.; et al. Functionalisation of PLLA nanofiber scaffolds using a possible cooperative effect between collagen type I and BMP-2: Impact on colonization and bone formation in vivo. J. Mater. Sci. Mater. Med. 2012, 23, 2227–2233. [Google Scholar] [CrossRef] [PubMed]
- Dalby, M.J.; Gadegaard, N.; Curtis, A.S.; Oreffo, R.O. Nanotopographical control of human osteoprogenitor differentiation. Curr. Stem Cell Res. Ther. 2007, 2, 129–138. [Google Scholar] [CrossRef] [PubMed]
- Felice, P.; Pistilli, R.; Piattelli, M.; Soardi, E.; Corvino, V.; Esposito, M. Posterior atrophic jaws rehabilitated with prostheses supported by 5 × 5 mm implants with a novel nanostructured calcium-incorporated titanium surface or by longer implants in augmented bone. Preliminary results from a randomised controlled trial. Eur. J. Oral Implantol. 2012, 5, 149–161. [Google Scholar] [PubMed]
- Peltola, T.; Jokinen, M.; Rahiala, H.; Patsi, M.; Heikkila, J.; Kangasniemi, I.; Yli-Urpo, A. Effect of aging time of sol on structure and in vitro calcium phosphate formation of sol-gel-derived titania films. J. Biomed. Mater. Res. 2000, 51, 200–208. [Google Scholar] [CrossRef] [PubMed]
- Wennerberg, A.; Frojd, V.; Olsson, M.; Nannmark, U.; Emanuelsson, L.; Johansson, P.; Josefsson, Y.; Kangasniemi, I.; Peltola, T.; Tirri, T.; et al. Nanoporous TiO(2) thin film on titanium oral implants for enhanced human soft tissue adhesion: a light and electron microscopy study. Clin. Implant. Dent. Relat. Res. 2011, 13, 184–196. [Google Scholar] [CrossRef] [PubMed]
- Rani, V.V.; Vinoth-Kumar, L.; Anitha, V.C.; Manzoor, K.; Deepthy, M.; Shantikumar, V.N. Osteointegration of titanium implant is sensitive to specific nanostructure morphology. Acta Biomater. 2012, 8, 1976–1989. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Gittens, R.A.; Song, R.; Tannenbaum, R.; Olivares-Navarrete, R.; Schwartz, Z.; Chen, H.; Boyan, B.D. Effects of structural properties of electrospun TiO2 nanofiber meshes on their osteogenic potential. Acta Biomater. 2012, 8, 878–885. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Chen, Y.; Rodriguez, J.; Fenniri, H.; Webster, T.J. Biomimetic helical rosette nanotubes and nanocrystalline hydroxyapatite coatings on titanium for improving orthopedic implants. Int. J. Nanomed. 2008, 3, 323–333. [Google Scholar]
- Sun, L.; Zhang, L.; Hemraz, U.D.; Fenniri, H.; Webster, T.J. Bioactive rosette nanotube-hydroxyapatite nanocomposites improve osteoblast functions. Tissue Eng. A 2012, 18, 1741–1750. [Google Scholar] [CrossRef]
- Sahithi, K.; Swetha, M.; Ramasamy, K.; Srinivasan, N.; Selvamurugan, N. Polymeric composites containing carbon nanotubes for bone tissue engineering. Int. J. Biol. Macromol. 2010, 46, 281–283. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Liu, H.; Niu, X.; Yu, B.; Fan, Y.; Feng, Q.; Cui, F.Z.; Watari, F. The use of carbon nanotubes to induce osteogenic differentiation of human adipose-derived MSCs in vitro and ectopic bone formation in vivo. Biomaterials 2012, 33, 4818–4827. [Google Scholar] [CrossRef] [PubMed]
- Dallari, D.; Savarino, L.; Albisinni, U.; Fornasari, P.; Ferruzzi, A.; Baldini, N.; Giannini, S. A prospective, randomised, controlled trial using a Mg-hydroxyapatite-demineralized bone matrix nanocomposite in tibial osteotomy. Biomaterials 2012, 33, 72–79. [Google Scholar] [CrossRef] [PubMed]
- Schwarz, F.; Sahm, N.; Bieling, K.; Becker, J. Surgical regenerative treatment of peri-implantitis lesions using a nanocrystalline hydroxyapatite or a natural bone mineral in combination with a collagen membrane: a four-year clinical follow-up report. J. Clin. Periodontol. 2009, 36, 807–814. [Google Scholar] [CrossRef] [PubMed]
- Tan, A.; Rajadas, J.; Seifalian, A.M. Biochemical engineering nerve conduits using peptide amphiphiles. J. Control. Release 2012, 163, 342–352. [Google Scholar] [CrossRef] [PubMed]
- Kehoe, S.; Zhang, X.F.; Boyd, D. Composition-property relationships for an experimental composite nerve guidance conduit: Evaluating cytotoxicity and initial tensile strength. J. Mater. Sci. Mater. Med. 2011, 22, 945–959. [Google Scholar] [CrossRef] [PubMed]
- Weber, R.A.; Breidenbach, W.C.; Brown, R.E.; Jabaley, M.E.; Mass, D.P. A randomized prospective study of polyglycolic acid conduits for digital nerve reconstruction in humans. Plast Reconstr. Surg. 2000, 106, 1036–1045; discussion 1046–1048. [Google Scholar] [CrossRef] [PubMed]
- Xiong, Y.; Zhu, J.X.; Fang, Z.Y.; Zeng, C.G.; Zhang, C.; Qi, G.L.; Li, M.H.; Zhang, W.; Quan, D.P.; Wan, J. Coseeded Schwann cells myelinate neurites from differentiated neural stem cells in neurotrophin-3-loaded PLGA carriers. Int. J. Nanomed. 2012, 7, 1977–1989. [Google Scholar] [CrossRef]
- de Boer, R.; Borntraeger, A.; Knight, A.M.; Hebert-Blouin, M.N.; Spinner, R.J.; Malessy, M.J.; Yaszemski, M.J.; Windebank, A.J. Short- and long-term peripheral nerve regeneration using a poly-lactic-co-glycolic-acid scaffold containing nerve growth factor and glial cell line-derived neurotrophic factor releasing microspheres. J. Biomed. Mater. Res. A 2012, 100, 2139–2146. [Google Scholar]
- Sasaki, R.; Aoki, S.; Yamato, M.; Uchiyama, H.; Wada, K.; Ogiuchi, H.; Okano, T.; Ando, T. PLGA artificial nerve conduits with dental pulp cells promote facial nerve regeneration. J. Tissue Eng. Regen. Med. 2011, 5, 823–830. [Google Scholar] [CrossRef] [PubMed]
- Xue, C.; Hu, N.; Gu, Y.; Yang, Y.; Liu, Y.; Liu, J.; Ding, F.; Gu, X. Joint use of a chitosan/PLGA scaffold and MSCs to bridge an extra large gap in dog sciatic nerve. Neurorehabil. Neural Repair 2012, 26, 96–106. [Google Scholar] [CrossRef] [PubMed]
- Kang, K.N.; Kim da, Y.; Yoon, S.M.; Lee, J.Y.; Lee, B.N.; Kwon, J.S.; Seo, H.W.; Lee, I.W.; Shin, H.C.; Kim, Y.M.; et al. Tissue engineered regeneration of completely transected spinal cord using human mesenchymal stem cells. Biomaterials 2012, 33, 4828–4835. [Google Scholar] [CrossRef] [PubMed]
- Kehoe, S.; Zhang, X.F.; Boyd, D. FDA approved guidance conduits and wraps for peripheral nerve injury: A review of materials and efficacy. Injury 2012, 43, 553–572. [Google Scholar] [CrossRef] [PubMed]
- Meek, M.F.; Coert, J.H. Synthetic nerve guide implants in humans: A comprehensive survey. Neurosurgery 2007, 61, E1340. [Google Scholar] [CrossRef] [PubMed]
- Frattini, F.; Lopes, F.R.; Almeida, F.M.; Rodrigues, R.F.; Boldrini, L.C.; Tomaz, M.A.; Baptista, A.F.; Melo, P.A.; Martinez, A.M. Mesenchymal stem cells in a polycaprolactone conduit promote sciatic nerve regeneration and sensory neuron survival after nerve injury. Tissue Eng. A 2012, 18, 2030–2039. [Google Scholar] [CrossRef]
- Yu, W.; Zhao, W.; Zhu, C.; Zhang, X.; Ye, D.; Zhang, W.; Zhou, Y.; Jiang, X.; Zhang, Z. Sciatic nerve regeneration in rats by a promising electrospun collagen/poly(epsilon-caprolactone) nerve conduit with tailored degradation rate. BMC Neurosci. 2011. [Google Scholar] [CrossRef]
- Beniash, E.; Hartgerink, J.D.; Storrie, H.; Stendahl, J.C.; Stupp, S.I. Self-assembling peptide amphiphile nanofiber matrices for cell entrapment. Acta Biomater. 2005, 1, 387–397. [Google Scholar] [CrossRef] [PubMed]
- Liu, W.Q.; Martinez, J.A.; Durand, J.; Wildering, W.; Zochodne, D.W. RGD-mediated adhesive interactions are important for peripheral axon outgrowth in vivo. Neurobiol. Dis. 2009, 34, 11–22. [Google Scholar] [CrossRef] [PubMed]
- Taras, J.S.; Nanavati, V.; Steelman, P. Nerve conduits. J. Hand Ther. 2005, 18, 191–197. [Google Scholar] [CrossRef] [PubMed]
- Antoniadou, E.V.; Ahmad, R.K.; Jackman, R.B.; Seifalian, A.M. Next generation brain implant coatings and nerve regeneration via novel conductive nanocomposite development. Conf. Proc. IEEE Eng. Med. Biol. Soc. 2011. [Google Scholar] [CrossRef]
- Ibrahim, A.; Ohshima, H.; Allison, S.A.; Cottet, H. Determination of effective charge of small ions, polyelectrolytes and nanoparticles by capillary electrophoresis. J. Chromatogr. A 2012, 1247, 154–164. [Google Scholar] [CrossRef] [PubMed]
- Subramaniam, R.; Astot, C.; Juhlin, L.; Nilsson, C.; Ostin, A. Determination of S-2-(N,N-diisopropylaminoethyl)- and S-2-(N,N-diethylaminoethyl) methylphosphonothiolate, nerve agent markers, in water samples using strong anion-exchange disk extraction, in vial trimethylsilylation, and gas chromatography-mass spectrometry analysis. J. Chromatogr. A 2012, 1229, 86–94. [Google Scholar] [CrossRef] [PubMed]
- Kwon, O.S.; Park, S.J.; Lee, J.S.; Park, E.; Kim, T.; Park, H.W.; You, S.A.; Yoon, H.; Jang, J. Multidimensional conducting polymer nanotubes for ultrasensitive chemical nerve agent sensing. Nano Lett. 2012, 12, 2797–2802. [Google Scholar] [CrossRef] [PubMed]
- Tandon, V.; Zhang, B.; Radisic, M.; Murthy, S.K. Generation of tissue constructs for cardiovascular regenerative medicine: From cell procurement to scaffold design. Biotechnol. Adv. 2012. In Press. [Google Scholar]
- Prabhakaran, M.P.; Kai, D.; Ghasemi-Mobarakeh, L.; Ramakrishna, S. Electrospun biocomposite nanofibrous patch for cardiac tissue engineering. Biomed. Mater. 2011, 6, 055001:1–055001:12. [Google Scholar] [CrossRef]
- Kocher, A.A.; Schuster, M.D.; Szabolcs, M.J.; Takuma, S.; Burkhoff, D.; Wang, J.; Homma, S.; Edwards, N.M.; Itescu, S. Neovascularization of ischemic myocardium by human bone-marrow-derived angioblasts prevents cardiomyocyte apoptosis, reduces remodeling and improves cardiac function. Nat. Med. 2001, 7, 430–436. [Google Scholar] [CrossRef] [PubMed]
- Penn, M.S.; Francis, G.S.; Ellis, S.G.; Young, J.B.; McCarthy, P.M.; Topol, E.J. Autologous cell transplantation for the treatment of damaged myocardium. Prog. Cardiovasc. Dis. 2002, 45, 21–32. [Google Scholar] [CrossRef] [PubMed]
- Fuchs, S.; Kornowski, R.; Weisz, G.; Satler, L.F.; Smits, P.C.; Okubagzi, P.; Baffour, R.; Aggarwal, A.; Weissman, N.J.; Cerqueira, M.; et al. Safety and feasibility of transendocardial autologous bone marrow cell transplantation in patients with advanced heart disease. Am. J. Cardiol. 2006, 97, 823–829. [Google Scholar] [CrossRef] [PubMed]
- van Ramshorst, J.; Bax, J.J.; Beeres, S.L.; Dibbets-Schneider, P.; Roes, S.D.; Stokkel, M.P.; de Roos, A.; Fibbe, W.E.; Zwaginga, J.J.; Boersma, E.; et al. Intramyocardial bone marrow cell injection for chronic myocardial ischemia: a randomized controlled trial. JAMA 2009, 301, 1997–2004. [Google Scholar] [CrossRef] [PubMed]
- Tse, H.F.; Thambar, S.; Kwong, Y.L.; Rowlings, P.; Bellamy, G.; McCrohon, J.; Thomas, P.; Bastian, B.; Chan, J.K.; Lo, G.; et al. Prospective randomized trial of direct endomyocardial implantation of bone marrow cells for treatment of severe coronary artery diseases (PROTECT-CAD trial). Eur. Heart J. 2007, 28, 2998–3005. [Google Scholar] [CrossRef] [PubMed]
- Perin, E.C.; Silva, G.V.; Henry, T.D.; Cabreira-Hansen, M.G.; Moore, W.H.; Coulter, S.A.; Herlihy, J.P.; Fernandes, M.R.; Cheong, B.Y.; Flamm, S.D.; et al. A randomized study of transendocardial injection of autologous bone marrow mononuclear cells and cell function analysis in ischemic heart failure (FOCUS-HF). Am. Heart J. 2011, 161, 1078–1087. [Google Scholar] [CrossRef] [PubMed]
- Williams, A.R.; Trachtenberg, B.; Velazquez, D.L.; McNiece, I.; Altman, P.; Rouy, D.; Mendizabal, A.M.; Pattany, P.M.; Lopera, G.A.; Fishman, J.; et al. Intramyocardial stem cell injection in patients with ischemic cardiomyopathy: Functional recovery and reverse remodeling. Circ. Res. 2011, 108, 792–796. [Google Scholar] [CrossRef] [PubMed]
- Clifford, D.M.; Fisher, S.A.; Brunskill, S.J.; Doree, C.; Mathur, A.; Watt, S.; Martin-Rendon, E. Stem cell treatment for acute myocardial infarction. Cochrane Database Syst. Rev. 2012. [Google Scholar] [CrossRef]
- Shin, M.; Ishii, O.; Sueda, T.; Vacanti, J.P. Contractile cardiac grafts using a novel nanofibrous mesh. Biomaterials 2004, 25, 3717–3723. [Google Scholar] [CrossRef] [PubMed]
- Kai, D.; Prabhakaran, M.P.; Jin, G.; Ramakrishna, S. Guided orientation of cardiomyocytes on electrospun aligned nanofibers for cardiac tissue engineering. J. Biomed. Mater. Res. B Appl. Biomater. 2011, 98B, 379–386. [Google Scholar] [CrossRef] [PubMed]
- Mukherjee, S.; Gualandi, C.; Focarete, M.L.; Ravichandran, R.; Venugopal, J.R.; Raghunath, M.; Ramakrishna, S. Elastomeric electrospun scaffolds of poly(l-lactide-co-trimethylene carbonate) for myocardial tissue engineering. J. Mater. Sci. Mater. Med. 2011, 22, 1689–1699. [Google Scholar] [CrossRef] [PubMed]
- Prabhakaran, M.P.; Nair, A.S.; Kai, D.; Ramakrishna, S. Electrospun composite scaffolds containing poly(octanediol-co-citrate) for cardiac tissue engineering. Biopolymers 2012, 97, 529–538. [Google Scholar] [CrossRef] [PubMed]
- Gupta, M.K.; Walthall, J.M.; Venkataraman, R.; Crowder, S.W.; Jung, D.K.; Yu, S.S.; Feaster, T.K.; Wang, X.; Giorgio, T.D.; Hong, C.C.; Baudenbacher, F.J.; Hatzopoulos, A.K.; Sung, H.J. Combinatorial polymer electrospun matrices promote physiologically-relevant cardiomyogenic stem cell differentiation. PLoS One 2011, 6, e28935:1–e28935:12. [Google Scholar]
- Sreerekha, P.R.; Menon, D.; Nair, S.V.; Chennazhi, K.P. Fabrication of Electrospun Poly (Lactide-co-Glycolide)-Fibrin Multiscale Scaffold for Myocardial Regeneration In Vitro. Tissue Eng. A 2013, 19, 849–859. [Google Scholar] [CrossRef]
- Hussain, A.; Collins, G.; Yip, D.; Cho, C.H. Functional 3-D cardiac co-culture model using bioactive chitosan nanofiber scaffolds. Biotechnol. Bioeng. 2013, 110, 637–647. [Google Scholar] [CrossRef]
- Kim, D.H.; Kshitiz; Smith, R.R.; Kim, P.; Ahn, E.H.; Kim, H.N.; Marban, E.; Suh, K.Y.; Levchenko, A. Nanopatterned cardiac cell patches promote stem cell niche formation and myocardial regeneration. Integr. Biol. 2012, 4, 1019–1033. [Google Scholar] [CrossRef]
- Dvir, T.; Bauer, M.; Schroeder, A.; Tsui, J.H.; Anderson, D.G.; Langer, R.; Liao, R.; Kohane, D.S. Nanoparticles targeting the infarcted heart. Nano Lett. 2011, 11, 4411–4414. [Google Scholar] [CrossRef] [PubMed]
- Yang, X. Nano- and microparticle-based imaging of cardiovascular interventions: Overview. Radiology 2007, 243, 340–347. [Google Scholar] [CrossRef] [PubMed]
- Harel-Adar, T.; Ben Mordechai, T.; Amsalem, Y.; Feinberg, M.S.; Leor, J.; Cohen, S. Modulation of cardiac macrophages by phosphatidylserine-presenting liposomes improves infarct repair. Proc. Natl. Acad. Sci. USA 2011, 108, 1827–1832. [Google Scholar] [CrossRef] [PubMed]
- Scott, R.C.; Rosano, J.M.; Ivanov, Z.; Wang, B.; Chong, P.L.; Issekutz, A.C.; Crabbe, D.L.; Kiani, M.F. Targeting VEGF-encapsulated immunoliposomes to MI heart improves vascularity and cardiac function. FASEB J. 2009, 23, 3361–3367. [Google Scholar] [CrossRef] [PubMed]
- Huang, G.; Rahimtoola, S.H. Prosthetic heart valve. Circulation 2011, 123, 2602–2605. [Google Scholar] [CrossRef] [PubMed]
- Flanagan, T.C.; Sachweh, J.S.; Frese, J.; Schnoring, H.; Gronloh, N.; Koch, S.; Tolba, R.H.; Schmitz-Rode, T.; Jockenhoevel, S. In vivo remodeling and structural characterization of fibrin-based tissue-engineered heart valves in the adult sheep model. Tissue Eng. A 2009, 15, 2965–2976. [Google Scholar] [CrossRef]
- Kalfa, D.; Bel, A.; Chen-Tournoux, A.; Della Martina, A.; Rochereau, P.; Coz, C.; Bellamy, V.; Bensalah, M.; Vanneaux, V.; Lecourt, S.; et al. A polydioxanone electrospun valved patch to replace the right ventricular outflow tract in a growing lamb model. Biomaterials 2010, 31, 4056–4063. [Google Scholar] [CrossRef] [PubMed]
- Aleksieva, G.; Hollweck, T.; Thierfelder, N.; Haas, U.; Koenig, F.; Fano, C.; Dauner, M.; Wintermantel, E.; Reichart, B.; Schmitz, C.; Akra, B. Use of a special bioreactor for the cultivation of a new flexible polyurethane scaffold for aortic valve tissue engineering. Biomed. Eng. Online 2012, 11, 92. [Google Scholar] [CrossRef] [PubMed]
- Martin, I.; Wendt, D.; Heberer, M. The role of bioreactors in tissue engineering. Trends Biotechnol. 2004, 22, 80–86. [Google Scholar] [CrossRef] [PubMed]
- Mol, A.; Smits, A.I.; Bouten, C.V.; Baaijens, F.P. Tissue engineering of heart valves: advances and current challenges. Expert Rev. Med. Devices 2009, 6, 259–275. [Google Scholar] [CrossRef] [PubMed]
- Winter, P.M.; Neubauer, A.M.; Caruthers, S.D.; Harris, T.D.; Robertson, J.D.; Williams, T.A.; Schmieder, A.H.; Hu, G.; Allen, J.S.; Lacy, E.K.; et al. Endothelial alpha(v)beta3 integrin-targeted fumagillin nanoparticles inhibit angiogenesis in atherosclerosis. Arterioscler. Thromb. Vasc. Biol. 2006, 26, 2103–2109. [Google Scholar] [CrossRef] [PubMed]
- Winter, P.M.; Caruthers, S.D.; Zhang, H.; Williams, T.A.; Wickline, S.A.; Lanza, G.M. Antiangiogenic synergism of integrin-targeted fumagillin nanoparticles and atorvastatin in atherosclerosis. JACC Cardiovasc. Imaging 2008, 1, 624–634. [Google Scholar] [CrossRef] [PubMed]
- Peters, D.; Kastantin, M.; Kotamraju, V.R.; Karmali, P.P.; Gujraty, K.; Tirrell, M.; Ruoslahti, E. Targeting atherosclerosis by using modular, multifunctional micelles. Proc. Natl. Acad. Sci. USA 2009, 106, 9815–9819. [Google Scholar] [CrossRef] [PubMed]
- Sharma, G.; She, Z.G.; Valenta, D.T.; Stallcup, W.B.; Smith, J.W. Targeting of Macrophage Foam Cells in Atherosclerotic Plaque Using Oligonucleotide-Functionalized Nanoparticles. Nano Life 2010, 1, 207–214. [Google Scholar] [CrossRef] [PubMed]
- Ji, J.; Ji, S.Y.; Yang, J.A.; He, X.; Yang, X.H.; Ling, W.P.; Chen, X.L. Ultrasound-targeted transfection of tissue-type plasminogen activator gene carried by albumin nanoparticles to dog myocardium to prevent thrombosis after heart mechanical valve replacement. Int. J. Nanomed. 2012, 7, 2911–2919. [Google Scholar] [CrossRef]
- Acharya, G.; Hopkins, R.A.; Lee, C.H. Advanced polymeric matrix for valvular complications. J. Biomed. Mater. Res. A 2012, 100, 1151–1159. [Google Scholar] [CrossRef] [PubMed]
- U.S. Food and Drug Administration. The FDA’s Drug Review Process: Ensuring Drugs Are Safe and Effective. Avaliable online: http://www.fda.gov/drugs/resourcesforyou/consumers/ucm143534.htm (aceessed on 25 March 2013).
- ClinicalTrials Home Page. Avaliable online: http://www.clinicaltrials.gov/ (aceessed on 25 March 2013).
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Perán, M.; García, M.A.; Lopez-Ruiz, E.; Jiménez, G.; Marchal, J.A. How Can Nanotechnology Help to Repair the Body? Advances in Cardiac, Skin, Bone, Cartilage and Nerve Tissue Regeneration. Materials 2013, 6, 1333-1359. https://doi.org/10.3390/ma6041333
Perán M, García MA, Lopez-Ruiz E, Jiménez G, Marchal JA. How Can Nanotechnology Help to Repair the Body? Advances in Cardiac, Skin, Bone, Cartilage and Nerve Tissue Regeneration. Materials. 2013; 6(4):1333-1359. https://doi.org/10.3390/ma6041333
Chicago/Turabian StylePerán, Macarena, María Angel García, Elena Lopez-Ruiz, Gema Jiménez, and Juan Antonio Marchal. 2013. "How Can Nanotechnology Help to Repair the Body? Advances in Cardiac, Skin, Bone, Cartilage and Nerve Tissue Regeneration" Materials 6, no. 4: 1333-1359. https://doi.org/10.3390/ma6041333
APA StylePerán, M., García, M. A., Lopez-Ruiz, E., Jiménez, G., & Marchal, J. A. (2013). How Can Nanotechnology Help to Repair the Body? Advances in Cardiac, Skin, Bone, Cartilage and Nerve Tissue Regeneration. Materials, 6(4), 1333-1359. https://doi.org/10.3390/ma6041333





