Nanodimensional and Nanocrystalline Apatites and Other Calcium Orthophosphates in Biomedical Engineering, Biology and Medicine
Abstract
:1. Introduction
2. General Knowledge on Calcium Orthophosphates
| Ca/P ionic ratio | Compound | Chemical formula | Solubility at 25 °C, – log(Ks) | Solubility at 25 °C, g/L | pH stability range in aqueous solutions at 25 °C |
|---|---|---|---|---|---|
| 0.5 | Monocalcium phosphate monohydrate (MCPM) | Ca(H2PO4)2·H2O | 1.14 | ~18 | 0.0–2.0 |
| 0.5 | Monocalcium phosphate anhydrous (MCPA) | Ca(H2PO4)2 | 1.14 | ~17 | [c] |
| 1.0 | Dicalcium phosphate dihydrate (DCPD), mineral brushite | CaHPO4·2H2O | 6.59 | ~0.088 | 2.0–6.0 |
| 1.0 | Dicalcium phosphate anhydrous (DCPA), mineral monetite | CaHPO4 | 6.90 | ~0.048 | [c] |
| 1.33 | Octacalcium phosphate (OCP) | Ca8(HPO4)2(PO4)4·5H2O | 96.6 | ~0.0081 | 5.5–7.0 |
| 1.5 | α-Tricalcium phosphate (α-TCP) | α-Ca3(PO4)2 | 25.5 | ~0.0025 | [a] |
| 1.5 | β-Tricalcium phosphate (β-TCP) | β-Ca3(PO4)2 | 28.9 | ~0.0005 | [a] |
| 1.2–2.2 | Amorphous calcium phosphate (ACP) | CaxHy(PO4)z·nH2O, n = 3–4.5; 15–20% H2O | [b] | [b] | ~5–12 [d] |
| 1.5–1.67 | Calcium-deficient hydroxyapatite (CDHA)[e] | Ca10-x(HPO4)x(PO4)6-x(OH)2-x[f] (0 < x < 1) | ~85.1 | 0.0094 | 6.5–9.5 |
| 1.67 | Hydroxyapatite (HA) | Ca10(PO4)6(OH)2 | 116.8 | ~0.0003 | 9.5–12 |
| 1.67 | Fluorapatite (FA) | Ca10(PO4)6F2 | 120.0 | ~0.0002 | 7–12 |
| 2.0 | Tetracalcium phosphate (TTCP), mineral hilgenstockite | Ca4(PO4)2O | 38–44 | ~0.0007 | [a] |
3. General Information on “Nano”
4. The Micron- and Submicron-Sized Calcium Orthophosphates versus Nanodimensional Ones
5. Nanodimensional and Nanocrystalline Calcium Orthophosphates in Normal Calcified Tissues of Mammals
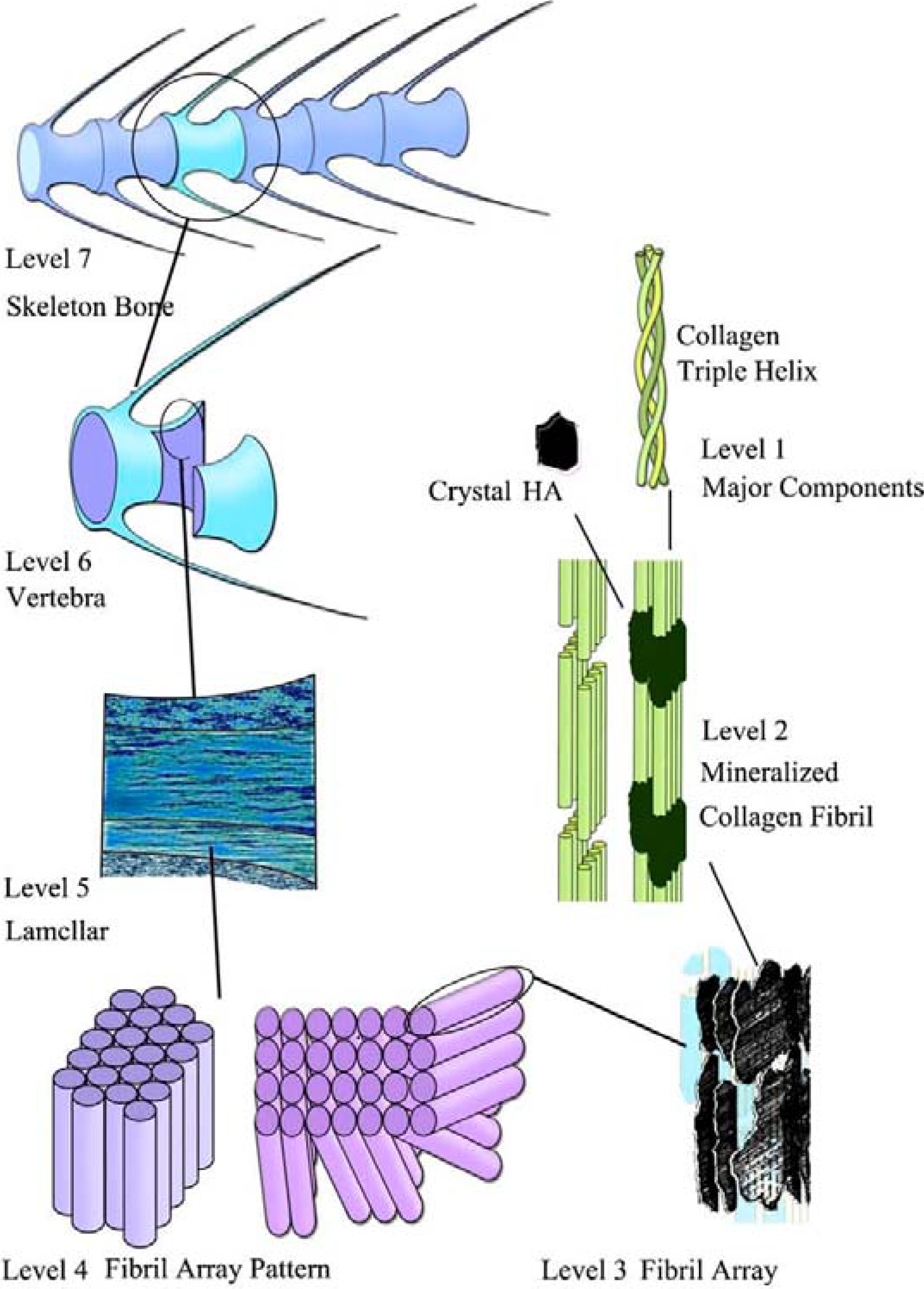
5.1. Bones
5.2. Teeth
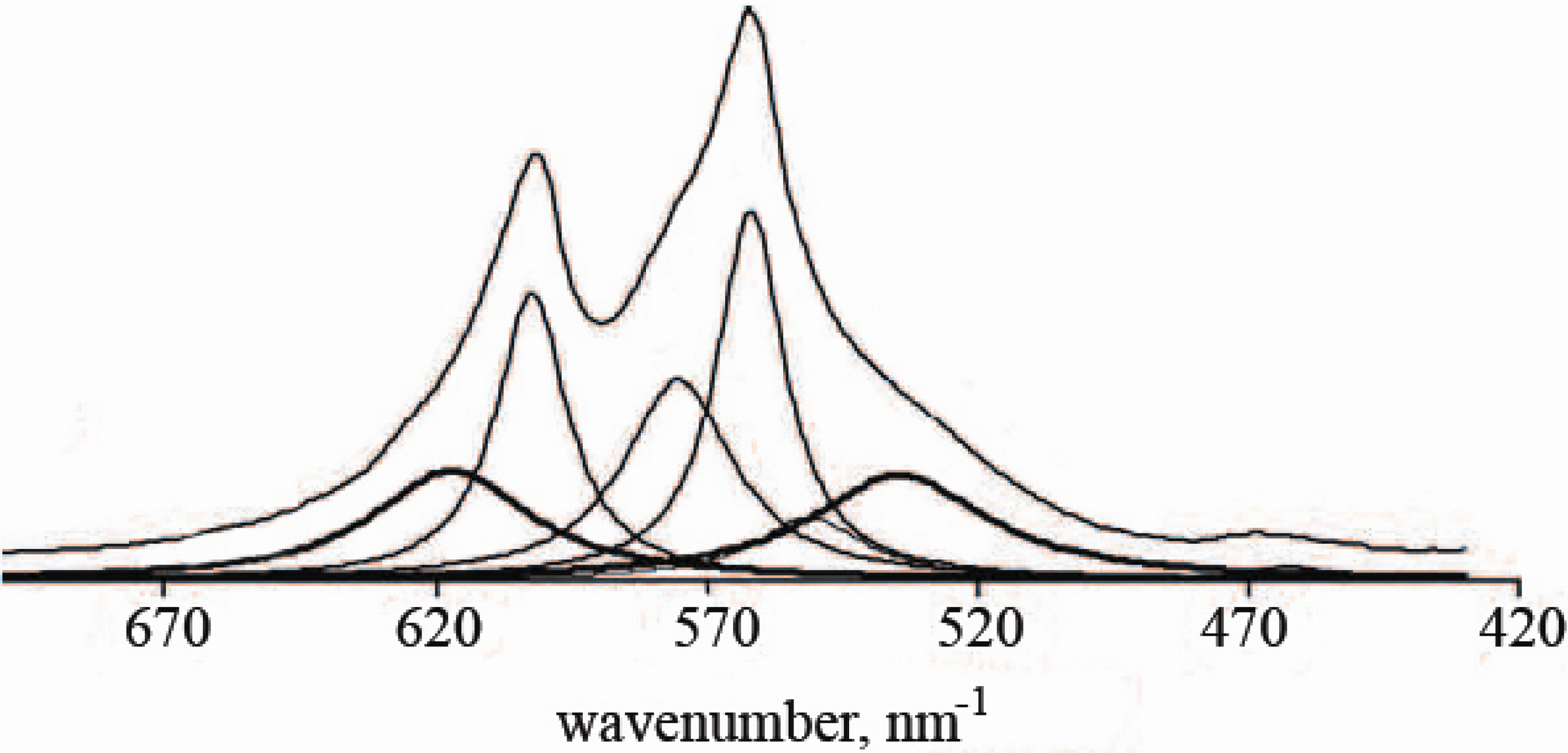
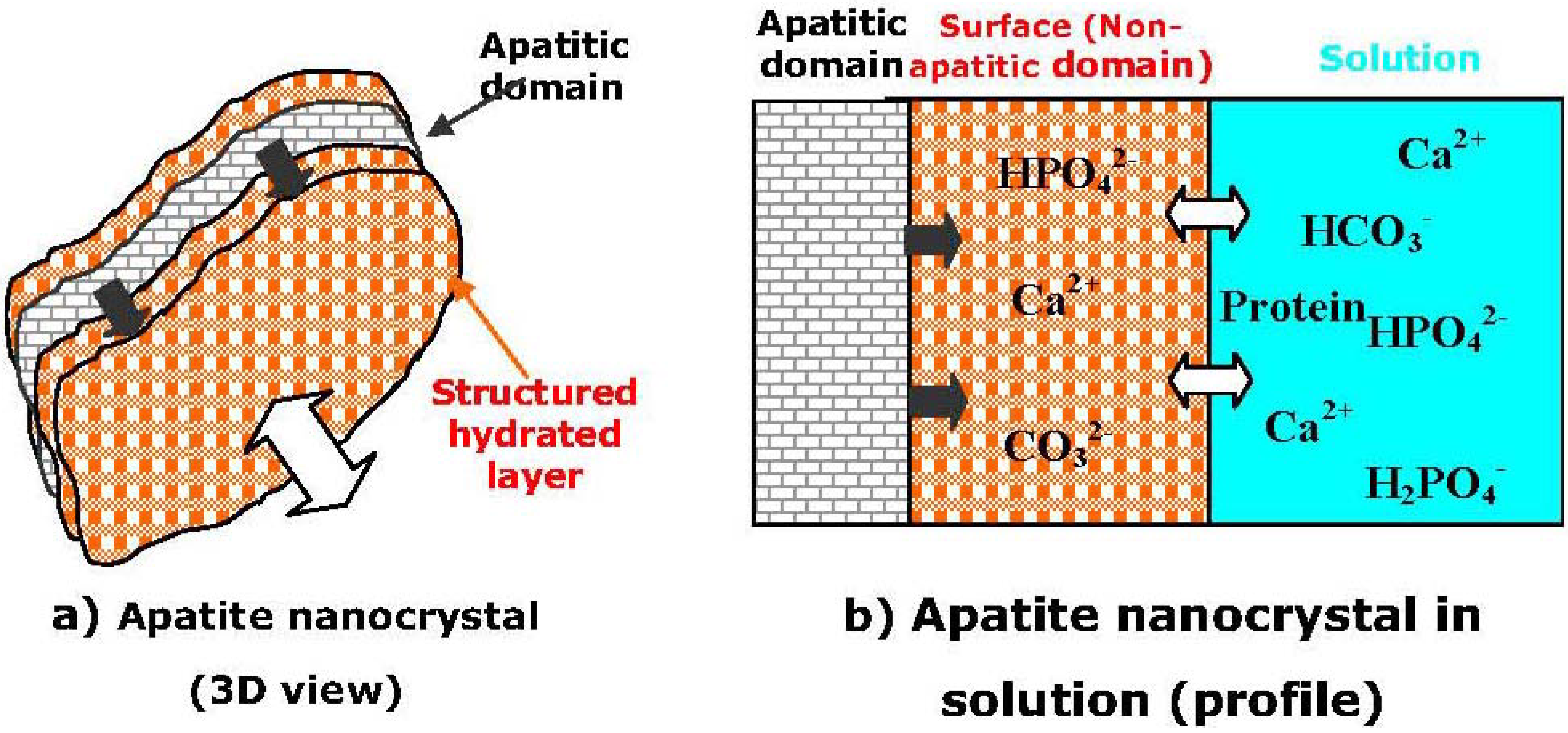
6. The Structure of the Nanodimensional and Nanocrystalline Apatites
7. Synthesis of the Nanodimensional and Nanocrystalline Calcium Orthophosphates
7.1. General Nanotechnological Approaches
7.2. Nanodimensional and Nanocrystalline Apatites
| Year | Process | Reference |
|---|---|---|
| 1995 | Synthesis of nanocrystalline HA (particle size ~20 nm) for the first time using calcium nitrate and diammonium hydrogen orthophosphate as precursors by solution spray dry method. | [368] |
| 2000 | Synthesis of biomimetic nanosized CDHA powders (~50 nm) at 37 °C and pH of 7.4 from calcium nitrate tetrahydrate and diammonium hydrogen orthophosphate salts in synthetic body fluid using a novel chemical precipitation technique. | [303] |
| 2002 | Preparation of nanosized HA particles and HA/chitosan nanocomposite. | [369] |
| 2002 | Direct precipitation from dilute calcium chloride and sodium orthophosphate solutions. | [370] |
| 2003 | Radio frequency plasma spray process employing fine spray dried HA powders (average size ~15 μm) as a feedstock. | [330] |
| 2003 | Sol-gel process using equimolar solutions of calcium nitrate and diammonium hydrogen orthophosphate dissolved in ethanol. | [297] |
| 2003 | Chemical precipitation through aqueous solutions of calcium chloride and ammonium hydrogen orthophosphate. | [371] |
| 2003 | Dry mechanochemical synthesis of hydroxyapatites from dicalcium phosphate dihydrate and calcium oxide: a kinetic study. | [323] |
| 2003 | Synthesis of nano-powders via sucrose-templated sol-gel method using calcium nitrate and diammonium hydrogen orthophosphate as precursor chemicals. | [372] |
| 2004 | Hydrolysis method of DCPD and CaCO3 by 2.5 M NaOH (aq). | [345] |
| 2004 | Citric acid sol-gel combustion process using calcium nitrate tetrahydrate, diammonium hydrogen orthophosphate and citric acid. | [373] |

7.3. Nanodimensional and Nanocrystalline TCP
7.4. Other Nanodimensional and Nanocrystalline Calcium Orthophosphates
7.5. Biomimetic Construction Using Calcium Orthophosphate Nanoparticles
8. Biomedical Applications of the Nanodimensional and Nanocrystalline Calcium Orthophosphates
8.1. Bone Repair

8.2. Nanodimensional and Nanocrystalline Calcium Orthophosphates and Bone-Related Cells

8.3. Dental Applications
8.4. Other Applications
9. Summary and Perspectives
- Consistency of the processing technologies;
- Optimization the structure and properties mimicking bones;
- Matching the strength of nanodimensional and nanocrystalline constructs with those of bones in order to provide a uniform distribution of stresses (load sharing);
- Optimizing bioresorption without comprising the mechanical properties;
- Assessing the inflammatory response to validate their biosafety.
10. Conclusions
11. Post-Conclusion Remarks
Acknowledgements
References and Notes
- Mann, S. Biomineralization Principles and Concepts in Bioinorganic Materials Chemistry; Oxford University Press: New York, USA, 2001; p. 216. [Google Scholar]
- Lowenstam, H.A.; Weiner, S. On Biomineralization; Oxford University Press: New York, USA, 1989; p. 324. [Google Scholar]
- Vallet-Regí, M.; González-Calbet, J.M. Calcium phosphates as substitution of bone tissues. Prog. Solid State Chem. 2004, 32, 1–31. [Google Scholar]
- Weiner, S.; Addadi, L. Design strategies in mineralized biological materials. J. Mater. Chem. 1997, 7, 689–702. [Google Scholar]
- Weiner, S.; Wagner, H.D. The material bone: structure-mechanical function relations. Ann. Rev. Mater. Sci. 1998, 28, 271–298. [Google Scholar]
- Pasteris, J.D.; Wopenka, B.; Valsami–Jones, E. Bone and tooth mineralization: why apatite? Elements 2008, 4, 97–104. [Google Scholar]
- Giachelli, C.M. Ectopic calcification: Gathering hard facts about soft tissue mineralization. Am. J. Pathol. 1999, 671, 671–675. [Google Scholar]
- Kirsch, T. Determinants of pathological mineralization: crystal deposition diseases. Curr. Opin. Rheumatol. 2006, 18, 174–180. [Google Scholar] [CrossRef]
- Christian, R.C.; Fitzpatrick, L.A. Vascular calcification. Curr. Opin. Nephrol. Hypertens. 1999, 8, 443–448. [Google Scholar] [CrossRef]
- Boskey, A. Bone mineral crystal size. Osteoporosis Int. 2003, 14 (Suppl. 5), S16S20; discussion S20–S21. [Google Scholar]
- Alivisatos, A.P. Enhanced: Naturally aligned nanocrystals. Science 2000, 289, 736–737. [Google Scholar]
- Narayan, R.J.; Kumta, P.N.; Sfeir, C.; Lee, D.H.; Choi, D.; Olton, D. Nanostructured ceramics in medical devices: applications and prospects. JOM 2004, 56, 38–43. [Google Scholar]
- Cai, Y.; Tang, R. Calcium phosphate nanoparticles in biomineralization and biomaterials. J. Mater. Chem. 2008, 18, 3775–3787. [Google Scholar]
- Ginebra, M.P.; Driessens, F.C.M.; Planell, J.A. Effect of the particle size on the micro and nanostructural features of a calcium phosphate cement: a kinetic analysis. Biomaterials 2004, 25, 3453–3462. [Google Scholar]
- Nanotechnology is an application of science and engineering at the nanoscale
- Karch, J.; Birringer, R.; Gleiter, H. Ceramics ductile at low temperature. Nature 1987, 330, 556–558. [Google Scholar] [CrossRef]
- Webster, T.J. Nanophase ceramics: The future of orthopedic and dental implant material. In Nanostructured Materials; Ying, J.Y., Ed.; Academic Press: New York, NY, USA, 2001; pp. 125–166. [Google Scholar]
- Tasker, L.H.; Sparey-Taylor, G.J.; Nokes, L.D. Applications of nanotechnology in orthopaedics. Clin. Orthop. Relat. Res. 2007, 456, 243–249. [Google Scholar] [CrossRef]
- Banfield, J.F.; Welch, S.A.; Zhang, H.; Ebert, T.T.; Penn, R.L. Aggregation–based crystal growth and microstructure development in natural iron oxyhydroxide biomineralization products. Science 2000, 289, 751–754. [Google Scholar]
- Cölfen, H. Bio-inspired mineralization using hydrophilic polymers. Top. Curr. Chem. 2007, 271, 1–77. [Google Scholar]
- Oaki, Y.; Imai, H. Nanoengineering in echinoderms: The emergence of morphology from nanobricks. Small 2005, 2, 66–70. [Google Scholar]
- Lee, S.H.; Shin, H. Matrices and scaffolds for delivery of bioactive molecules in bone and cartilage tissue engineering. Adv. Drug Delivery Rev. 2007, 59, 339–359. [Google Scholar] [CrossRef]
- Ben-Nissan, B. Nanoceramics in biomedical applications. MRS Bulletin 2004, 29, 28–32. [Google Scholar]
- Rehman, I. Nano bioceramics for biomedical and other applications. Mater. Technol. 2004, 19, 224–233. [Google Scholar]
- Driessens, F.C.M.; Boltong, M.G.; de Maeyer, E.A.P.; Wenz, R.; Nies, B.; Planell, J.A. The Ca/P range of nanoapatitic calcium phosphate cements. Biomaterials 2002, 23, 4011–4017. [Google Scholar]
- Doat, A.; Fanjul, M.; Pellé, F.; Hollande, E.; Lebugle, A. Europium-doped bioapatite: A new photostable biological probe, internalizable by human cells. Biomaterials 2003, 24, 3365–3371. [Google Scholar]
- Doat, A.; Pellé, F.; Gardant, N.; Lebugle, A. Synthesis of luminescent bioapatite nanoparticles for utilization as a biological probe. J. Solid State Chem. 2004, 177, 1179–1187. [Google Scholar] [CrossRef]
- Lebugle, A.; Pellé, F.; Charvillat, C.; Rousselot, I.; Chane-Ching, J.Y. Colloidal and monocrystalline Ln3+ doped apatite calcium phosphate as biocompatible fluorescent probes. Chem. Commun. 2006, 606–608. [Google Scholar]
- Mondejar, S.P.; Kovtun, A.; Epple, M. Lanthanide-doped calcium phosphate nanoparticles with high internal crystallinity and with a shell of DNA as fluorescent probes in cell experiments. J. Mater. Chem. 2007, 17, 4153–4159. [Google Scholar]
- Kalita, S.J.; Bhatt, H.A. Nanocrystalline hydroxyapatite doped with magnesium and zinc: Synthesis and characterization. Mater. Sci. Eng. C 2007, 27, 837–848. [Google Scholar] [CrossRef]
- Huang, J.; Jayasinghe, S.N.; Best, S.M.; Edirisinghe, M.J.; Brooks, R.A.; Rushton, N.; Bonfield, W. Novel deposition of nanosized silicon substituted hydroxyapatite by electrostatic spraying. J. Mater. Sci. Mater. Med. 2005, 16, 1137–1142. [Google Scholar] [CrossRef]
- Pon-On, W.; Meejoo, S.; Tang, I.M. Incorporation of iron into nano hydroxyapatite particles synthesized by the microwave process. Int. J. Nanosci. 2007, 6, 9–16. [Google Scholar] [CrossRef]
- Predoi, D.; Barsan, M.; Andronescu, E.; Vatasescu-Balcan, R.A.; Costache, M. Hydroxyapatite-iron oxide bioceramic prepared using nano–size powders. J. Optoelectronics Adv. Mater. 2007, 9, 3609–3613. [Google Scholar]
- Bakunova, N.V.; Fomin, A. S.; Fadeeva, I.V.; Barinov, S.M.; Shvorneva, L.I. Silicon-containing hydroxylapatite nanopowders. Russ. J. Inorg. Chem. 2007, 52, 1492–1497. [Google Scholar] [CrossRef]
- Miao, S.; Weng, W.; Cheng, K.; Du, P.; Shen, G.; Han, G. Preparation of nano-sized strontium containing tricalcium phosphate particles. Key Eng. Mater. 2007, 330–332, 263–266. [Google Scholar]
- Liu, Y.; Zhou, R.; Mo, A.; Chen, Z.; Wu, H. Synthesis and characterization of yttrium/hydroxyapatite nanoparticles. Key Eng. Mater. 2007, 330–332, 295–298. [Google Scholar]
- Wu, H.C.; Wang, T.W.; Sun, J.S.; Wang, W.H.; Lin, F.H. A novel biomagnetic nanoparticle based on hydroxyapatite. Nanotechnology 2007, 18, 165601:1–165601:9. [Google Scholar]
- Rameshbabu, N.; Kumar, T.S.S.; Prabhakar, T.G.; Sastry, V.S.; Murty, K.V.G.K.; Rao, K.P. Antibacterial nanosized silver substituted hydroxyapatite: Synthesis and characterization. J. Biomed. Mater. Res. A 2007, 80A, 581–591. [Google Scholar]
- Fujii, E.; Ohkubo, M.; Tsuru, K.; Hayakawa, S.; Osaka, A.; Kawabata, K.; Bonhomme, C.; Babonneau, F. Selective protein adsorption property and characterization of nano-crystalline zinc-containing hydroxyapatite. Acta Biomater. 2006, 2, 69–74. [Google Scholar] [CrossRef]
- Zhang, S.M.; Hu, W.; Zhou, W.; Li, J.; Liu, Y.H.; Qiu, Z.Y. Dialysis preparation of zinc-substituted nano-hydroxyapatite and its characterization. Key Eng. Mater. 2007, 330–332, 219–222. [Google Scholar]
- Pon-On, W.; Meejoo, S.; Tang, I.M. Substitution of manganese and iron into hydroxyapatite: Core/shell nanoparticles. Mater. Res. Bull. 2008, 43, 2137–2144. [Google Scholar] [CrossRef]
- Zou, C.; Weng, W.; Cheng, K.; Du, P.; Shen, G.; Han, G. Preparation of nanosized β-tricalcium phosphate particles with Zn substitution. J. Mater. Sci. Mater. Med. 2008, 19, 1133–1136. [Google Scholar] [CrossRef]
- Hwang, K.S.; Hwangbo, S.; Kim, J.T. Silver-doped calcium phosphate nanopowders prepared by electrostatic spraying. J. Nanoparticle Res. 2008, 10, 1337–1341. [Google Scholar] [CrossRef]
- Lee, D.; Sfeir, C.; Kumta, P.N. Novel in-situ synthesis and characterization of nanostructured magnesium substituted β-tricalcium phosphate (β-TCMP). Mater. Sci. Eng. C 2009, 29, 69–77. [Google Scholar] [CrossRef]
- Petchsang, N.; Pon-On, W.; Hodak, J.H.; Tang, I.M. Magnetic properties of Co-ferrite-doped hydroxyapatite nanoparticles having a core/shell structure. J. Magnetism Magnetic Mater. 2009, 321, 1990–1995. [Google Scholar] [CrossRef]
- Hou, C.H.; Hou, S.M.; Hsueh, Y.S.; Lin, J.; Wu, H.C.; Lin, F.H. The in vivo performance of biomagnetic hydroxyapatite nanoparticles in cancer hyperthermia therapy. Biomaterials 2009, 30, 3956–3960. [Google Scholar]
- Petchsang, N.; Pon-On, W.; Hodak, J.H.; Tang, I.M. Magnetic properties of Co-ferrite-doped hydroxyapatite nanoparticles having a core/shell structure. J. Magnetism Magnetic Mater. 2009, 321, 1990–1995. [Google Scholar] [CrossRef]
- Cacciotti, I.; Bianco, A.; Lombardi, M.; Montanaro, L. Mg-substituted hydroxyapatite nanopowders: Synthesis, thermal stability and sintering behaviour. J. Eur. Ceram. Soc. 2009, 29, 2969–2978. [Google Scholar] [CrossRef]
- Bianco, A.; Cacciotti, I.; Lombardi, M.; Montanaro, L. Si-substituted hydroxyapatite nanopowders: Synthesis, thermal stability and sinterability. Mater. Res. Bull. 2009, 44, 345–354. [Google Scholar] [CrossRef]
- Capuccini, C.; Torricelli, P.; Boanini, E.; Gazzano, M.; Giardino, R.; Bigi, A. Interaction of Sr-doped hydroxyapatite nanocrystals with osteoclast and osteoblast-like cells. J. Biomed. Mater. Res. A 2009, 89A, 594–600. [Google Scholar] [CrossRef]
- Hou, C.H.; Chen, C.W.; Hou, S.M.; Li, Y.T.; Lin, F.H. The fabrication and characterization of dicalcium phosphate dihydrate-modified magnetic nanoparticles and their performance in hyperthermia processes in vitro. Biomaterials 2009, 30, 4700–4707. [Google Scholar]
- Li, W.; Gao, L. Fabrication of Hap-ZrO2 (3Y) nano-composite by SPS. Biomaterials 2003, 24, 937–940. [Google Scholar]
- Wang, L.; Nemoto, R.; Senna, M. Microstructure and chemical states of hydroxyapatite/silk fibroin nanocomposites synthesized via a wet-mechanochemical route. J. Nanopart. Res. 2002, 4, 535–540. [Google Scholar] [CrossRef]
- Nemoto, R.; Wang, L.; Ikoma, T.; Tanaka, J.; Senna, M. Preferential alignment of hydroxyapatite crystallites in nanocomposites with chemically disintegrated silk fibroin. J. Nanopart. Res. 2004, 6, 259–265. [Google Scholar] [CrossRef]
- Fang, L.M.; Leng, Y.; Gao, P. Processing and mechanical properties of HA/UHMWPE nanocomposites. Biomaterials 2006, 27, 3701–3707. [Google Scholar]
- Sugawara, A.; Yamane, S.; Akiyoshi, K. Nanogel-templated mineralization: Polymer-calcium phosphate hybrid nanomaterials. Macromol. Rapid Commun. 2006, 27, 441–446. [Google Scholar] [CrossRef]
- Pushpakanth, S.; Srinivasan, B.; Sreedhar, B.; Sastry, T.P. An in situ approach to prepare nanorods of titania—hydroxyapatite (TiO2–HAp) nanocomposite by microwave hydrothermal technique. Mater. Chem. Phys. 2008, 107, 492–498. [Google Scholar] [CrossRef]
- Chang, M.C.; Ko, C.C.; Douglas, W.H. Preparation of hydroxyapatite-gelatin nanocomposite. Biomaterials 2003, 24, 2853–2862. [Google Scholar]
- Hao, J.; Liu, Y.; Zhou, S.; Li, Z.; Deng, X. Investigation of nanocomposites based on semi-interpenetrating network of [L-poly(ε-caprolactone)]/[net-poly(ε-caprolactone)] and hydroxyapatite nanocrystals. Biomaterials 2003, 24, 1531–1539. [Google Scholar]
- Deng, X.M.; Hao, J.Y.; Wang, C.S. Preparation and mechanical properties of nanocomposites of poly(D,L-lactide) with Ca-deficient hydroxyapatite nanocrystals. Biomaterials 2001, 22, 2867–2873. [Google Scholar]
- Hong, Z.; Zhang, P.; He, C.; Qiu, X.; Liu, A.; Chen, L.; Chena, X.; Jing, X. Nanocomposite of poly(L-lactide) and surface grafted hydroxyapatite: Mechanical properties and biocompatibility. Biomaterials 2005, 26, 6296–6304. [Google Scholar]
- Ramay, H.R.R.; Zhang, M. Biphasic calcium phosphate nanocomposite porous scaffolds for load-bearing bone tissue engineering. Biomaterials 2004, 25, 5171–5180. [Google Scholar]
- Cross, K.J.; Huq, N.L.; Palamara, J.E.; Perich, J.W.; Reynolds, E.C. Physicochemical characterization of casein phosphopeptide—amorphous calcium phosphate nanocomplexes. J. Biol. Chem. 2005, 280, 15362–15369. [Google Scholar]
- Murugan, R.; Ramakrishna, S. Development of nanocomposites for bone grafting. Comp. Sci. Tech. 2005, 65, 2385–2406. [Google Scholar]
- Liou, S.C.; Chen, S.Y.; Liu, D.M. Phase development and structural characterization of calcium phosphate ceramics—polyacrylic acid nanocomposites at room temperature in water-methanol mixtures. J. Mater. Sci. Mater. Med. 2004, 15, 1261–1266. [Google Scholar] [CrossRef]
- Sung, Y.M.; Shin, Y.K.; Ryu, J.J. Preparation of hydroxyapatite/zirconia bioceramic nanocomposites for orthopaedic and dental prosthesis applications. Nanotechnology 2007, 18, 065602:1–065602:6. [Google Scholar]
- Sreedhar, B.; Aparna, Y.; Sairam, M.; Hebalkar, N. Preparation and characterization of HAP / carboxymethyl chitosan nanocomposites. J. Appl. Polym. Sci. 2007, 105, 928–934. [Google Scholar] [CrossRef]
- Pramanik, N.; Biswas, S.K.; Pramanik, P. Synthesis and characterization of hydroxyl-apatite/poly(vinyl alcohol phosphate) nanocomposite biomaterials. Int. J. Appl. Ceram. Technol. 2008, 5, 20–28. [Google Scholar] [CrossRef]
- Li, X.; Chang, J. Preparation of bone-like apatite—collagen nanocomposites by a biomimetic process with phosphorylated collagen. J. Biomed. Mater. Res. A 2008, 85A, 293–300. [Google Scholar] [CrossRef]
- Ohsawa, H.; Ito, A.; Sogo, Y.; Yamazaki, A.; Ohno, T. Synthesis of albumin/DCP nano-composite particles. Key Eng. Mater. 2007, 330–332, 239–242. [Google Scholar]
- Degirmenbasi, N.; Kalyon, D.M.; Birinci, E. Biocomposites of nanohydroxyapatite with collagen and poly(vinyl alcohol). Colloids Surf. B 2006, 48, 42–49. [Google Scholar] [CrossRef]
- Zhang, X.; Li, Y.B.; Zuo, Y.; Lv, G.Y.; Mu, Y.H.; Li, H. Morphology, hydrogen-bonding and crystallinity of nano-hydroxyapatite/polyamide 66 biocomposites. Composites A 2007, 38, 843–848. [Google Scholar]
- Wei, J.; Li, Y.B.; Lau, K.T. Preparation and characterization of a nano apatite/polyamide6 bioactive composite. Composites B 2007, 38, 301–305. [Google Scholar]
- Wei, J.; Li, Y.B. Tissue engineering scaffold material of nano-apatite crystals and polyamide composite. Eur. Polym. J. 2004, 40, 509–515. [Google Scholar]
- Szaraniec, B.; Rosół, P.; Chłopek, J. Carbon composite material and polysulfone modified by nano-hydroxyapatite. e-Polymers 2005. no. 030. [Google Scholar]
- Pramanik, N.; Mohapatra, S.; Pramanik, P. Processing and properties of nano-hydroxyapatite (n-HAp)/poly(ethylene-co-acrylic acid) (EAA) composite using a phosphonic acid coupling agent for orthopedic applications. J. Am. Ceram. Soc. 2007, 90, 369–375. [Google Scholar] [CrossRef]
- Ren, Y.J.; Sun, X.D.; Cui, F.Z.; Wei, Y.T.; Cheng, Z.J.; Kong, X.D. Preparation and characterization of Antheraea pernyi silk fibroin based nanohydroxyapatite composites. J. Bioact. Compat. Polym. 2007, 22, 465–474. [Google Scholar] [CrossRef]
- Xu, H.H.K.; Sun, L.; Weir, M.D.; Takagi, S.; Chow, L.C.; Hockey, B. Effects of incorporating nanosized calcium phosphate particles on properties of whisker-reinforced dental composites. J. Biomed. Mater. Res. B Appl. Biomater. 2007, 81B, 116–125. [Google Scholar] [CrossRef]
- Liu, L.; Liu, J.; Wang, M.; Min, S.; Cai, Y.; Zhu, L.; Yao, J. Preparation and characterization of nano-hydroxyapatite/silk fibroin porous scaffolds. J. Biomater. Sci. Polymer Edn. 2008, 19, 325–338. [Google Scholar] [CrossRef]
- Xu, F.; Li, Y.B.; Deng, Y.; Xiong, J. Porous nano-hydroxyapatite/poly(vinyl alcohol) composite hydrogel as artificial cornea fringe: Characterization and evaluation in vitro. J. Biomater. Sci. Polymer Edn. 2008, 19, 431–439. [Google Scholar] [CrossRef]
- Huang, J.; Lin, Y.W.; Fu, X.W.; Best, S.M.; Brooks, R.A.; Rushton, N.; Bonfield, W. Development of nanosized hydroxyapatite reinforced composites for tissue engineering scaffolds. J. Mater. Sci. Mater. Med. 2007, 18, 2151–2157. [Google Scholar] [CrossRef]
- Yusong, P.; Dangsheng, X.; Xiaolin, C. Mechanical properties of nanohydroxyapatite reinforced poly(vinyl alcohol) gel composites as biomaterial. J. Mater. Sci. 2007, 42, 5129–5134. [Google Scholar]
- Deng, C.; Weng, J.; Lu, X.; Zhou, S.B.; Wan, J.X.; Qu, S.X.; Feng, B.; Li, X.H.; Cheng, Q.Y. Mechanism of ultrahigh elongation rate of poly(D, L-lactide)-matrix composite biomaterial containing nano-apatite fillers. Mater. Lett. 2008, 62, 607–610. [Google Scholar]
- Sundaraseelan, J.; Sastry, T.P. Fabrication of a biomimetic compound containing nano hydroxyapatite—demineralised bone matrix. J. Biomed. Nanotechnol. 2007, 3, 401–405. [Google Scholar] [CrossRef]
- Teng, S.; Chen, L.; Guo, Y.; Shi, J. Formation of nano-hydroxyapatite in gelatin droplets and the resulting porous composite microspheres. J. Inorg. Biochem. 2007, 101, 686–691. [Google Scholar] [CrossRef]
- Meng, Y.H.; Tang, C.Y.; Tsui, C.P.; Chen, D.Z. Fabrication and characterization of needle-like nano-HA and HA/MWNT composites. J. Mater. Sci. Mater. Med. 2008, 19, 75–81. [Google Scholar] [CrossRef]
- Dorozhkin, S.V. Calcium orthophosphate-based biocomposites and hybrid biomaterials. J. Mater. Sci. 2009, 44, 2343–2387. [Google Scholar]
- Dorozhkin, S.V. Calcium orthophosphates. J. Mater. Sci. 2007, 42, 1061–1095. [Google Scholar]
- Dorozhkin, S.V. Calcium orthophosphates in nature, biology and medicine. Materials 2009, 2, 399–498. [Google Scholar]
- Ong, J.L.; Chan, D.C.N. Hydroxyapatite and their use as coatings in dental implants: A review. Crit. Rev. Biomed. Eng. 1999, 28, 667–707. [Google Scholar]
- Davies, J.E. In vitro modeling of the bone/implant interface. Anat. Rec. 1996, 245, 426–445. [Google Scholar]
- Anselme, K. Osteoblast adhesion on biomaterials. Biomaterials 2000, 21, 667–681. [Google Scholar] [CrossRef]
- Suchanek, W.L.; Yoshimura, M. Processing and properties of hydroxyapatite-based biomaterials for use as hard tissue replacement implants. J. Mater. Res. 1998, 13, 94–117. [Google Scholar]
- Hench, L.L. Bioceramics: From a concept to clinics. J. Am. Ceram. Soc. 1991, 74, 1487–1510. [Google Scholar] [CrossRef]
- Hench, L.L. Bioceramics. J. Am. Ceram. Soc. 1998, 1705, 1705–1728. [Google Scholar]
- Gauthier, O.; Bouler, J.M.; Weiss, P.; Bosco, J.; Daculsi, G.; Aguado, E. Kinetic study of bone ingrowth and ceramic resorption associated with the implantation of different injectable calcium-phosphate bone substitutes. J. Biomed. Mater. Res. 1999, 47, 28–35. [Google Scholar]
- Hing, K.A.; Best, S.M.; Bonfield, W. Characterization of porous hydroxyapatite. J. Mater. Sci. Mater. Med. 1999, 10, 135–145. [Google Scholar]
- Carotenuto, G.; Spagnuolo, G.; Ambrosio, L.; Nicolais, L. Macroporous hydroxyapatite as alloplastic material for dental applications. J. Mater. Sci. Mater. Med. 1999, 10, 671–676. [Google Scholar] [CrossRef]
- LeGeros, R.Z. Calcium Phosphates in Oral Biology and Medicine; Karger: Basel, Switzerland, 1991; p. 210. [Google Scholar]
- Elliott, J.C. Structure and Chemistry of the Apatites and Other Calcium Orthophosphates; Elsevier: Amsterdam, The Netherlands, 1994; p. 404. [Google Scholar]
- Brown, P.W.; Constantz, B. (Eds.) Hydroxyapatite and Related Materials; CRC Press: Boca Raton, FL, USA, 1994; p. 343.
- Amjad, Z. (Ed.) Calcium Phosphates in Biological and Industrial Systems; Kluwer Academic Publishers: Boston, MA, USA, 1997; p. 529.
- Hughes, J.M.; Kohn, M.; Rakovan, J. (Eds.) Phosphates: Geochemical, Geobiological and Materials Importance; Mineralogical Society of America: Washington, D.C., USA, 2002.
- Chow, L.C.; Eanes, E.D. (Eds.) Octacalcium Phosphate; Karger: Basel, Switzerland, 2001; p. 168.
- Brès, E.; Hardouin, P. (Eds.) Les matériaux en phosphate de calcium. Aspects fondamentaux. / Calcium phosphate materials. Fundamentals; Sauramps Medical: Montpellier, France, 1998; p. 176.
- Williams, D.F. The relationship between biomaterials and nanotechnology. Biomaterials 2008, 29, 1737–1738. [Google Scholar]
- Feynman, R.P. There’s plenty of room at the bottom. J. Microelectromechanical Systems 1992, 1, 60–66. [Google Scholar] [CrossRef]
- Strictly speaking, there are serious doubts that the term “nanomaterial” has a reasonable meaning. For example, let me cite Prof. David F. Williams, the Editor-in-Chief of Biomaterials: “… some words which have no rational basis whatsoever become part of everyday language so rapidly, even if so illogically, that it is impossible to reverse the process and their common use has to be accepted, or perhaps, accommodated. Nanomaterial is one such word, where I have argued that it should not exist, but accept that it does through common usage and have to recognise its existence [106]. The discussion about nanomaterial provides a hint of the analysis of a biomaterial that follows, since a prefix which is an indicator of scale cannot specify the integer that follows (in this case a material) unless that integer can be qualified by that scale. In other words, it is very clear what a nanometre is because nano means 10-9 and a metre is a measure of length. In the case of nanomaterial, what is it about the material that is 10-9. Is it the dimension of a crystal within the material, or of a grain boundary, a domain, or a molecule, or is it a parameter of a surface feature of the sample, or perhaps of the resistivity or thermal conductivity of the material. Clearly this is nonsense, but one has to accept that nanomaterials are here to stay, with even some journal titles containing the word.” [109, p. 5898, left column]
- Williams, D.F. On the nature of biomaterials. Biomaterials 2009, 30, 5897–5909. [Google Scholar]
- European Commission, Scientific Committee on Emerging and Newly Identified Health Risks (SCENIHR). Opinion on “the scientific aspects of the existing and proposed definitions relating to products of nanoscience and nanotechnologies”; Adopted Brussels: European Commission, 29 November 2007. [Google Scholar]
- Moriarty, P. Nanostructured materials. Rep. Prog. Phys. 2001, 64, 297–381. [Google Scholar] [CrossRef]
- Webster, T.J.; Ahn, E.S. Nanostructured biomaterials for tissue engineering bone. Adv. Biochem. Eng. Biotechnol. 2006, 103, 275–308. [Google Scholar]
- Streicher, R.M.; Schmidt, M.; Fiorito, S. Nanosurfaces and nanostructures for artificial orthopedic implants. Nanomedicine 2007, 2, 861–874. [Google Scholar]
- Havancsak, K. Nanotechnology at present and its promises in the future. Mater. Sci. Forum 2003, 414–415, 85–94. [Google Scholar]
- Duncan, R. Nanomedicines in action. Pharm. J. 2004, 273, 485–488. [Google Scholar]
- Liu, H.; Webster, T.J. Nanomedicine for implants: A review of studies and necessary experimental tools. Biomaterials 2007, 28, 354–369. [Google Scholar]
- Murugan, R.; Ramakrishna, S. Bioresorbable composite bone paste using polysaccharide based nano hydroxyapatite. Biomaterials 2004, 25, 3829–3835. [Google Scholar]
- Murugan, R.; Ramakrishna, S. Aqueous mediated synthesis of bioresorbable nanocrystalline hydroxyapatite. J. Cryst. Growth 2005, 274, 209–213. [Google Scholar]
- Li, G.; Huang, J.; Li, Y.; Zhang, R.; Deng, B.; Zhang, J.; Aoki, H. In vitro study on influence of a discrete nano-hydroxyapatite on leukemia P388 cell behavior. Biomed. Mater. Eng. 2007, 17, 321–327. [Google Scholar]
- Ganesan, K.; Kovtun, A.; Neumann, S.; Heumann, R.; Epple, M. Calcium phosphate nanoparticles: Colloidally stabilized and made fluorescent by a phosphate-functionalized porphyrin. J. Mater. Chem. 2008, 18, 3655–3661. [Google Scholar]
- Kim, H.W.; Kim, H.E. Nanofiber generation of hydroxyapatite and fluor-hydroxyapatite bioceramics. J. Biomed. Mater. Res. B Appl. Biomater. 2005, 77B, 323–328. [Google Scholar]
- Cihlar, J.; Castkova, K. Direct synthesis of nanocrystalline hydroxyapatite by hydrothermal hydrolysis of alkylphosphates. Monatshefte für Chemie 2002, 133, 761–771. [Google Scholar] [CrossRef]
- Lak, A.; Mazloumi, M.; Mohajerani, M.; Kajbafvala, A.; Zanganeh, S.; Arami, H.; Sadrnezhaad, S.K. Self-assembly of dandelion-like hydroxyapatite nanostructures via hydrothermal method. J. Am. Ceram. Soc. 2008, 91, 3292–3297. [Google Scholar] [CrossRef]
- Traykova, T.; Aparicio, C.; Ginebra, M.P.; Planell, J.A. Bioceramics as nanomaterials. Nanomedicine 2006, 1, 91–106. [Google Scholar]
- Grainger, D.W.; Castner, D.G. Nanobiomaterials and nanoanalysis: Opportunities for improving the science to benefit biomedical technologies. Adv. Mater. 2008, 20, 867–877. [Google Scholar]
- Nelson, K.G. The Kelvin equation and solubility of small particles. J. Pharmac. Sci. 1972, 61, 479–480. [Google Scholar] [CrossRef]
- Fan, C.; Chen, J.; Chen, Y.; Ji, J.; Teng, H.H. Relationship between solubility and solubility product: The roles of crystal sizes and crystallographic directions. Geochim. Cosmochim. Acta 2006, 70, 3820–3829. [Google Scholar] [CrossRef]
- Sato, M.; Webster, T.J. Nanobiotechnology: Implications for the future of nanotechnology in orthopedic applications. Expert Rev. Med. Dev. 2004, 1, 105–114. [Google Scholar] [CrossRef]
- Hahn, H. Unique features and properties of nanostructured materials. Adv. Eng. Mater. 2003, 5, 277–284. [Google Scholar] [CrossRef]
- Aronov, D.; Karlov, A.; Rosenman, G. Hydroxyapatite nanoceramics: Basic physical properties and biointerface modification. J. Eur. Ceram. Soc. 2007, 27, 4181–4186. [Google Scholar] [CrossRef]
- Ramsden, J.J.; Freeman, J. The nanoscale. Nanotechnol. Percept. 2009, 5, 3–25. [Google Scholar] [CrossRef]
- Rempel, A.A. Nanotechnologies. Properties and applications of nanostructured materials. Russ. Chem. Rev. 2007, 76, 435–461. [Google Scholar]
- Catledge, S.A.; Fries, M.D.; Vohra, Y.K.; Lacefield, W.R.; Lemons, J.E.; Woodard, S.; Venugopalan, R. Nanostructured ceramics for biomedical implants. J. Nanosci. Nanotechnol. 2002, 2, 1–20. [Google Scholar]
- Balasundarama, G.; Webster, T.J. A perspective on nanophase materials for orthopedic implant applications. J. Mater. Chem. 2006, 16, 3737–3745. [Google Scholar]
- Balasundarama, G.; Webster, T.J. Nanotechnology and biomaterials for orthopedic medical applications. Nanomedicine 2006, 1, 169–176. [Google Scholar]
- Padilla, S.; Izquierdo-Barba, I.; Vallet-Regí, M. High specific surface area in nanometric carbonated hydroxyapatite. Chem. Mater. 2008, 20, 5942–5944. [Google Scholar]
- Kalita, S.J.; Bhardwaj, A.; Bhatt, H.A. Nanocrystalline calcium phosphate ceramics in biomedical engineering. Mater. Sci. Eng. C 2007, 27, 441–449. [Google Scholar] [CrossRef]
- Mann, S. The study of biominerals by high resolution transmission electron microscopy. Scan. Electron. Microsc. 1986, Pt. 2, 393–413. [Google Scholar]
- Katsura, N. Nanospace theory for biomineralization. Dent. Jpn. Tokyo 1990, 27, 57–63. [Google Scholar]
- Cuisinier, F.J.G.; Voegel, J.C.; Yacaman, J.; Frank, R.M. Structure of initial crystals formed during human amelogenesis. J. Cryst. Growth 1992, 116, 314–318. [Google Scholar] [CrossRef]
- Cuisinier, F.J.G.; Steuer, P.; Senger, B.; Voegel, J.C.; Frank, R.M. Human amelogenesis: High resolution electron microscopy of nanometer–sized particles. Cell Tissue Res. 1993, 273, 175–182. [Google Scholar] [CrossRef]
- Brès, E.F.; Moebus, G.; Kleebe, H.J.; Pourroy, G.; Werkmann, J.; Ehret, G. High resolution electron microscopy study of amorphous calcium phosphate. J. Cryst. Growth 1993, 129, 149–162. [Google Scholar] [CrossRef]
- Layrolle, P.; Lebugle, A. Characterization and reactivity of nanosized calcium phosphate prepared in anhydrous ethanol. Chem. Mater. 1994, 6, 1996–2004. [Google Scholar]
- Cui, F.Z.; Wen, H.B.; Zhang, H.B.; Ma, C.L.; Li, H.D. Nanophase hydroxyapatite-like crystallites in natural ivory. J. Mater. Sci. Lett. 1994, 13, 1042–1044. [Google Scholar]
- Li, Y.B.; de Wijn, J.; Klein, C.P.A.T.; de Meer, S.V.; de Groot, K. Preparation and characterization of nanograde osteoapatite-like rod crystals. J. Mater. Sci. Mater. Med. 1994, 5, 252–255. [Google Scholar]
- Li, Y.B.; de Groot, K.; de Wijn, J.; Klein, C.P.A.T.; de Meer, S.V. Morphology and composition of nanograde calcium phosphate needle-like crystals formed by simple hydrothermal treatment. J. Mater. Sci. Mater. Med. 1994, 5, 326–331. [Google Scholar]
- Shirkhanzadeh, M. X-ray diffraction and Fourier transform infrared analysis of nanophase apatite coatings prepared by electrocrystallization. Nanostruct. Mater. 1994, 4, 677–684. [Google Scholar] [CrossRef]
- Webster, T.J.; Ergun, C.; Doremus, R.H.; Siegel, R.W.; Bizios, R. Specific proteins mediate enhanced osteoblast adhesion on nanophase ceramics. J. Biomed. Mater. Res. 2000, 51, 475–483. [Google Scholar]
- Chan, C.K.; Kumar, T.S.S.; Liao, S.; Murugan, R.; Ngiam, M.; Ramakrishnan, S. Biomimetic nanocomposites for bone graft applications. Nanomedicine 2006, 1, 177–188. [Google Scholar]
- Okada, M.; Furukawa, K.; Serizawa, T.; Yanagisawa, Y.; Tanaka, H.; Kawai, T.; Furuzono, T. Interfacial interactions between calcined hydroxyapatite nanocrystals and substrates. Langmuir 2009, 25, 6300–6306. [Google Scholar]
- Mikołajczyk, T.; Rabiej, S.; Bogun, M. Analysis of the structural parameters of polyacrylonitrile fibers containing nanohydroxyapatite. J. Appl. Polym. Sci. 2006, 101, 760–765. [Google Scholar] [CrossRef]
- There are both nanobiomaterials and nanostructured biomaterials, which should be differentiated from each other. Nanobiomaterials refer to individual molecular level biomaterials such as single proteins (are not considered in this review), while nanostructured biomaterials refer to any biomaterials whose structure or morphology can be engineered to get features with nanometer-scale dimensions [153]. This review is limited to calcium orthophosphate-based nanostructured biomaterials only
- Thomas, V.; Dean, D.R.; Vohra, Y.K. Nanostructured biomaterials for regenerative medicine. Curr. Nanosci. 2006, 2, 155–177. [Google Scholar] [CrossRef]
- LeGeros, R.Z. Biodegradation and bioresorption of calcium phosphate ceramics. Clin. Mater. 1993, 14, 65–88. [Google Scholar]
- Wang, J.; Shaw, L.L. Morphology-enhanced low-temperature sintering of nanocrystalline hydroxyapatite. Adv. Mater. 2007, 19, 2364–2369. [Google Scholar]
- Fomin, A.S.; Barinov, S.M.; Ievlev, V.M.; Smirnov, V.V.; Mikhailov, B.P.; Belonogov, E.K.; Drozdova, N.A. Nanocrystalline hydroxyapatite ceramics produced by low-temperature sintering after high-pressure treatment. Dokl. Chem. 2008, 418, 22–25. [Google Scholar]
- Drouet, C.; Bosc, F.; Banu, M.; Largeot, C.; Combes, C.; Dechambre, G.; Estournes, C.; Raimbeaux, G.; Rey, C. Nanocrystalline apatites: From powders to biomaterials. Powder Technol. 2009, 190, 118–122. [Google Scholar]
- Ramesh, S.; Tan, C.Y.; Bhaduri, S.B.; Teng, W.D.; Sopyan, I. Densification behaviour of nanocrystalline hydroxyapatite bioceramics. J. Mater. Process. Technol. 2008, 206, 221–230. [Google Scholar] [CrossRef]
- Skorokhod, V.V.; Solonin, S.M.; Dubok, V.A.; Kolomiets, L.L.; Katashinskii, V.P.; Shinkaruk, A.V. Pressing and sintering of nanosized hydroxyapatite powders. Powder Metall. Metal Ceram. 2008, 47, 518–524. [Google Scholar] [CrossRef]
- Sung, Y.M.; Lee, J.C.; Yang, J.W. Crystallization and sintering characteristics of chemically precipitated hydroxyapatite nanopowder. J. Cryst. Growth 2004, 262, 467–472. [Google Scholar] [CrossRef]
- Lin, K.; Chang, J.; Lu, J.; Wu, W.; Zeng, Y. Properties of β-Ca3(PO4)2 bioceramics prepared using nanosized powders. Ceram. Int. 2007, 33, 979–985. [Google Scholar]
- Tanaka, Y.; Hirata, Y.; Yoshinaka, R. Synthesis and characteristics of ultra-fine hydroxyapatite particles. J. Ceram. Proc. Res. 2003, 4, 197–201. [Google Scholar]
- Wang, J.; Shaw, L.L. Nanocrystalline hydroxyapatite with simultaneous enhancements in hardness and toughness. Biomaterials 2009, 30, 6565–6572. [Google Scholar]
- Stupp, S.I.; Ciegler, G.W. Organoapatites: Materials for artificial bone. I. Synthesis and microstructure. J. Biomed. Mater. Res. 1992, 26, 169–183. [Google Scholar]
- Webster, T.J.; Ergun, C.; Doremus, R.H.; Siegel, R.W.; Bizios, R. Enhanced osteoclast-like cell functions on nanophase ceramics. Biomaterials 2001, 22, 1327–1333. [Google Scholar]
- Huang, J.; Best, S.M.; Bonfield, W.; Brooks, R.A.; Rushton, N.; Jayasinghe, S.N.; Edirisinghe, M.J. In vitro assessment of the biological response to nanosized hydroxyapatite. J. Mater. Sci. Mater. Med. 2004, 15, 441–445. [Google Scholar] [CrossRef]
- Kim, H.W.; Kim, H.E.; Salih, V. Stimulation of osteoblast responses to biomimetic nanocomposites of gelatin-hydroxyapatite for tissue engineering scaffolds. Biomaterials 2005, 26, 5221–5230. [Google Scholar]
- Webster, T.J.; Siegel, R.W.; Bizios, R. Osteoblast adhesion on nanophase ceramics. Biomaterials 1999, 20, 1221–1227. [Google Scholar]
- Webster, T.J.; Ergun, C.; Doremus, R.H.; Siegel, R.W.; Bizios, R. Enhanced functions of osteoblast on nanophase ceramics. Biomaterials 2000, 21, 1803–1810. [Google Scholar] [CrossRef]
- Smith, I.O.; McCabe, L.R.; Baumann, M.J. MC3T3-E1 osteoblast attachment and proliferation on porous hydroxyapatite scaffolds fabricated with nanophase powder. Int. J. Nanomed. 2006, 1, 189–194. [Google Scholar] [CrossRef]
- Nelson, M.; Balasundaram, G.; Webster, T.J. Increased osteoblast adhesion on nanoparticulate crystalline hydroxyapatite functionalized with KRSR. Int. J. Nanomed. 2006, 1, 339–349. [Google Scholar]
- Liu, H.; Yazici, H.; Ergun, C.; Webster, T.J.; Bermek, H. An in vitro evaluation of the Ca/P ratio for the cytocompatibility of nano-to-micron particulate calcium phosphates for bone regeneration. Acta Biomater. 2008, 4, 1472–1479. [Google Scholar] [CrossRef]
- Sato, M.; Sambito, M.A.; Aslani, A.; Kalkhoran, N.M.; Slamovich, E.B.; Webster, T.J. Increased osteoblast functions on undoped and yttrium-doped nanocrystalline hydroxyapatite coatings on titanium. Biomaterials 2006, 27, 2358–2369. [Google Scholar]
- Thian, E.S.; Huang, J.; Best, S.M.; Barber, Z.H.; Brooks, R.A.; Rushton, N.; Bonfield, W. The response of osteoblasts to nanocrystalline silicon-substituted hydroxyapatite thin films. Biomaterials 2006, 27, 2692–2698. [Google Scholar]
- Palin, E.; Liu, H.; Webster, T.J. Mimicking the nanofeatures of bone increases bone-forming cell adhesion and proliferation. Nanotechnology 2005, 16, 1828–1835. [Google Scholar]
- Sun, W.; Chu, C.; Wang, J.; Zhao, H. Comparison of periodontal ligament cells responses to dense and nanophase hydroxyapatite. J. Mater. Sci. Mater. Med. 2007, 18, 677–683. [Google Scholar] [CrossRef]
- Ergun, C.; Liu, H.; Webster, T.J.; Olcay, E.; Yılmaz, Ş.; Sahin, F.C. Increased osteoblast adhesion on nanoparticulate calcium phosphates with higher Ca/P ratios. J. Biomed. Mater. Res. A 2008, 85A, 236–241. [Google Scholar]
- Lewandrowski, K.U.; Bondre, S.P.; Wise, D.L.; Trantolo, D.J. Enhanced bioactivity of a poly(propylene fumarate) bone graft substitute by augmentation with nano-hydroxyapatite. Biomed. Mater. Eng. 2003, 13, 115–124. [Google Scholar]
- Zhou, D.S.; Zhao, K.B.; Li, Y.; Cui, F.Z.; Lee, I.S. Repair of segmental defects with nano-hydroxyapatite/collagen/PLA composite combined with mesenchymal stem cells. J. Bioactive Compat. Polym. 2006, 21, 373–384. [Google Scholar] [CrossRef]
- Xu, Z.; Sun, J.; Changsheng, L.; Jie, W. Effect of hydroxyapatite nanoparticles of different concentrations on rat osteoblast. Mater. Sci. Forum 2009, 610–613, 1364–1369. [Google Scholar]
- Krut’ko, V.K.; Kulak, A.I.; Lesnikovich, L.A.; Trofimova, I.V.; Musskaya, O.N.; Zhavnerko, G.K.; Paribok, I.V. Influence of the dehydration procedure on the physicochemical properties of nanocrystalline hydroxylapatite xerogel. Russ. J. General Chem. 2007, 77, 336–342. [Google Scholar] [CrossRef]
- Severin, A.V.; Komarov, V.F.; Bozhevol’nov, V.E.; Melikhov, I.V. Morphological selection in suspensions of nanocrystalline hydroxylapatite leading to spheroidal aggregates. Russ. J. Inorg. Chem. 2005, 50, 72–77. [Google Scholar]
- Biggemann, D.; da Silva, M.H.P.; Rossi, A.M.; Ramirez, A.J. High-resolution transmission electron microscopy study of nanostructured hydroxyapatite. Microsc. Microanal. 2008, 14, 433–438. [Google Scholar] [CrossRef]
- Kester, M.; Heakal, Y.; Fox, T.; Sharma, A.; Robertson, G.P.; Morgan, T.T.; Altinoğlu, E.I.; Tabaković, A.; Parette, M.R.; Rouse, S.M.; Ruiz-Velasco, V.; Adair, J.H. Calcium phosphate nanocomposite particles for in vitro imaging and encapsulated chemotherapeutic drug delivery to cancer cells. Nano Lett. 2008, 8, 4116–4121. [Google Scholar]
- Welzel, T.; Meyer-Zaika, W.; Epple, M. Continuous preparation of functionalised calcium phosphate nanoparticles with adjustable crystallinity. Chem. Commun. 2004, 1204–1205. [Google Scholar]
- Nichols, H.L.; Zhang, N.; Zhang, J.; Shi, D.; Bhaduri, S.; Wen, X. Coating nanothickness degradable films on nanocrystalline hydroxyapatite particles to improve the bonding strength between nanohydroxyapatite and degradable polymer matrix. J. Biomed. Mater. Res. A 2007, 82A, 373–382. [Google Scholar] [CrossRef]
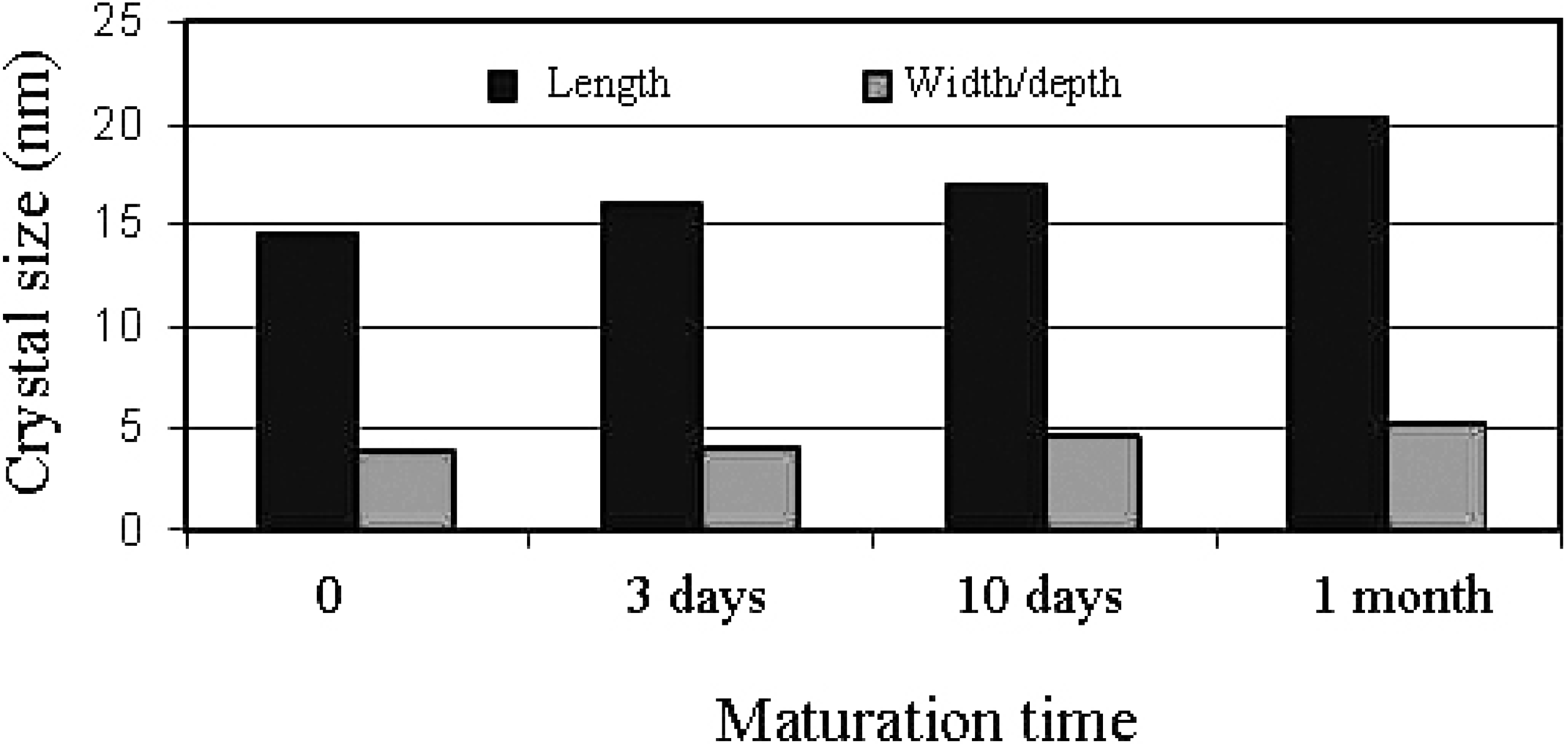
- Rey, C.; Hina, A.; Tofighi, A.; Glimcher, M.J. Maturation of poorly crystalline apatites: Chemical and structural aspects in vivo and in vitro. Cell Mater. 1995, 5, 345–356. [Google Scholar]
- Olszta, M.J.; Cheng, X.; Jee, S.S.; Kumar, R.; Kim, Y.Y.; Kaufmane, M.J.; Douglas, E.P.; Gower, L.B. Bone structure and formation: A new perspective. Mater. Sci. Eng. R 2007, 58, 77–116. [Google Scholar] [CrossRef]
- Cui, F.Z.; Li, Y.; Ge, J. Self-assembly of mineralized collagen composites. Mater. Sci. Eng. R 2007, 57, 1–27. [Google Scholar] [CrossRef]
- Meyers, M.A.; Chen, P.Y.; Lin, A.Y.M.; Seki, Y. Biological materials: Structure and mechanical properties. Prog. Mater. Sci. 2008, 53, 1–206. [Google Scholar] [CrossRef]
- Currey, J.D. Hierarchies in biomineral structures. Science 2005, 309, 253–254. [Google Scholar]
- Rubin, M.A.; Jasiuk, I.; Taylor, J.; Rubin, J.; Ganey, T.; Apkarian, R.P. TEM analysis of the nanostructure of normal and osteoporotic human trabecular bone. Bone 2003, 33, 270–282. [Google Scholar]
- Hartgerink, J.D.; Beniash, E.; Stupp, S.I. Self-assembly and mineralization of peptide-amphiphile nanofibers. Science 2001, 294, 1684–1688. [Google Scholar]
- Ji, B.; Gao, H. Elastic properties of nanocomposite structure of bone. Compos. Sci. Technol. 2006, 66, 1212–1218. [Google Scholar] [CrossRef]
- Wang, L.; Nancollas, G.H.; Henneman, Z.J.; Klein, E.; Weiner, S. Nanosized particles in bone and dissolution insensitivity of bone mineral. Biointerphases 2006, 1, 106–111. [Google Scholar]
- Gao, H.; Ji, B.; Jager, I.L.; Arz, E.; Fratzl, P. Materials become insensitive to flaws at nanoscale: Lessons from nature. Proc. Natl. Acad. Sci. USA 2003, 100, 5597–5660. [Google Scholar] [CrossRef]
- Gupta, H.S.; Seto, J.; Wagermaier, W.; Zaslansky, P.; Boesecke, P.; Fratzl, P. Cooperative deformation of mineral and collagen in bone at the nanoscale. Proc. Natl. Acad. Sci. USA 2006, 103, 17741–17746. [Google Scholar] [CrossRef]
- Currey, J.D. Bones: Structure and Mechanics; Princeton University Press: Princeton, NJ, USA, 2006; p. 456. [Google Scholar]
- Porter, A.E.; Nalla, R.K.; Minor, A.; Jinschek, J.R.; Kisielowski, C.; Radmilovic, V.; Kinney, J.H.; Tomsia, A.P.; Ritchie, R.O. A transmission electron microscopy study of mineralization in age-induced transparent dentin. Biomaterials 2005, 26, 7650–7660. [Google Scholar]
- Kirkham, J.; Brookes, S.J.; Shore, R.C.; Wood, S.R.; Smith, D.A.; Zhang, J.; Chen, H.; Robinson, C. Physico-chemical properties of crystal surfaces in matrix-mineral interactions during mammalian biomineralisation. Curr. Opin. Colloid Interf. Sci. 2002, 7, 124–132. [Google Scholar] [CrossRef]
- Daculsi, G.; Mentanteau, J.; Kerebel, L.M.; Mitre, D. Length and shape of enamel crystals. Calcif. Tissue Int. 1984, 36, 550–555. [Google Scholar] [CrossRef] [PubMed]
- Robinson, C.; Connell, S.; Kirkham, J.; Shorea, R.; Smith, A. Dental enamel—a biological ceramic: Regular substructures in enamel hydroxyapatite crystals revealed by atomic force microscopy. J. Mater. Chem. 2004, 14, 2242–2248. [Google Scholar]
- Chen, H.; Tang, Z.; Liu, J.; Sun, K.; Chang, S.R.; Peters, M.C.; Mansfield, J.F.; Czajka-Jakubowska, A.; Clarkson, B.H. Acellular synthesis of a human enamel-like microstructure. Adv. Mater. 2006, 18, 1846–1851. [Google Scholar]
- Chen, H.; Clarkson, B.H.; Sun, K.; Mansfield, J.F. Self-assembly of synthetic hydroxyapatite nanorods into an enamel prism-like structure. J. Colloid Interf. Sci. 2005, 288, 97–103. [Google Scholar] [CrossRef]
- Robinson, C. Self-oriented assembly of nano-apatite particles: A subunit mechanism for building biological mineral crystals. J. Dental Res. 2007, 86, 677–679. [Google Scholar]
- Cui, F.Z.; Ge, J. New observations of the hierarchical structure of human enamel, from nanoscale to microscale. J. Tissue Eng. Regen. Med. 2007, 1, 185–191. [Google Scholar]
- He, L.H.; Swain, M.V. Enamel—A “metallic-like” deformable biocomposite. J. Dent. 2007, 35, 431–437. [Google Scholar]
- Nelson, S.J. Wheeler’s Dental Anatomy, Physiology and Occlusion, 9th ed.; W.B. Saunders: Philadelphia, PA, USA, 2009; p. 368. [Google Scholar]
- Suvorova, E.I.; Buffat, P.A. Electron diffraction from micro- and nanoparticles of hydroxyapatite. J. Microscopy 1999, 196, 46–58. [Google Scholar]
- Panda, R.N.; Hsieh, M.F.; Chung, R.J.; Chin, T.S. X-ray diffractometry and X-ray photoelectron spectroscopy investigations of nanocrytalline hydroxyapatite synthesized by a hydroxide gel technique. Jpn. J. Appl. Phys. 2001, 40, 5030–5035. [Google Scholar] [CrossRef]
- Panda, R.N.; Hsieh, M.F.; Chung, R.J.; Chin, T.S. FTIR, XRD, SEM and solid state NMR investigations of carbonate-containing hydroxyapatite nano-particles synthesized by hydroxide-gel technique. J. Phys. Chem. Solids 2003, 64, 193–199. [Google Scholar] [CrossRef]
- Eichert, D.; Sfihi, H.; Combes, C.; Rey, C. Specific characteristics of wet nanocrystalline apatites. Consequences on biomaterials and bone tissue. Key Eng. Mater. 2004, 254–256, 927–930. [Google Scholar]
- Rey, C.; Combes, C.; Drouet, C.; Sfihi, H.; Barroug, A. Physico-chemical properties of nanocrystalline apatites: Implications for biominerals and biomaterials. Mater. Sci. Eng. C 2007, 27, 198–205. [Google Scholar] [CrossRef]
- Eichert, D.; Drouet, C.; Sfihi, H.; Rey, C.; Combes, C. Nanocrystalline apatite-based biomaterials: Synthesis, processing and characterization. In Biomaterials Research Advances; Kendall, J.B., Ed.; Nova Science Publishers, Inc.: Hauppauge, NY, USA, 2007; Chapter 5; pp. 93–143. [Google Scholar]
- Aronov, D.; Rosenman, G. Trap state spectroscopy studies and wettability modification of hydroxyapatite nanobioceramics. J. Appl. Phys. 2007, 101, 034701:1–034701:5. [Google Scholar]
- Jäger, C.; Welzel, T.; Meyer-Zaika, W.; Epple, M. A solid-state NMR investigation of the structure of nanocrystalline hydroxyapatite. Magn. Reson. Chem. 2006, 44, 573–580. [Google Scholar] [CrossRef]
- Isobe, T.; Nakamura, S.; Nemoto, R.; Senna, M.; Sfihi, H. Solid-state double nuclear magnetic resonance of calcium phosphate nanoparticules synthesized by wet-mechanochemical reaction. J. Phys. Chem. B 2002, 106, 5169–5176. [Google Scholar]
- Bertinetti, L.; Tampieri, A.; Landi, E.; Ducati, C.; Midgley, P.A.; Coluccia, S.; Martra, G. Surface structure, hydration, and cationic sites of nanohydroxyapatite: UHR-TEM, IR, and microgravimetric studies. J. Phys. Chem. C 2007, 111, 4027–4035. [Google Scholar]
- Bertinetti, L.; Tampieri, A.; Landi, E.; Bolis, V.; Busco, C.; Martra, G. Surface structure, hydration and cationic sites of nanohydroxyapatite. Key Eng. Mater. 2008, 361–363, 87–90. [Google Scholar]
- Bertinetti, L.; Drouet, C.; Combes, C.; Rey, C.; Tampieri, A.; Coluccia, S.; Martra, G. Surface characteristics of nanocrystalline apatites: Effect of Mg surface enrichment on morphology, surface hydration species, and cationic environments. Langmuir 2009, 25, 5647–5654. [Google Scholar]
- Gopi, D.; Indira, J.; Prakash, V.C.A.; Kavitha, L. Spectroscopic characterization of porous nanohydroxyapatite synthesized by a novel amino acid soft solution freezing method. Spectrochim. Acta A 2009, 74A, 282–284. [Google Scholar] [CrossRef]
- Rossi, A.M.; da Silva, M.H.P.; Ramirez, A.J.; Biggemann, D.; Caraballo, M.M.; Mascarenhas, Y.P.; Eon, J.G.; Moure, G.T. Structural properties of hydroxyapatite with particle size less than 10 nanometers. Key Eng. Mater. 2007, 330–332, 255–258. [Google Scholar]
- Ramirez, C.A.O.; Costa, A.M.; Bettini, J.; Ramirez, A.J.; da Silva, M.H.P.; Rossi, A.M. Structural properties of nanostructured carbonate apatites. Key Eng. Mater. 2009, 396–398, 611–614. [Google Scholar]
- Pasteris, J.D.; Wopenka, B.; Freeman, J.J.; Rogers, K.; Valsami-Jones, E.; van der Houten, J.A.M.; Silva, M.J. Lack of OH in nanocrystalline apatite as a function of degree of atomic order: Implications for bone and biomaterials. Biomaterials 2004, 25, 229–238. [Google Scholar]
- Zyman, Z.Z.; Epple, M.; Rokhmistrov, D.; Glushko, V. On impurities and the internal structure in precipitates occurring during the precipitation of nanocrystalline calcium phosphate. Mat. -wiss. u. Werkstofftech. 2009, 40, 297–301. [Google Scholar] [CrossRef]
- Cazalbou, S.; Combes, C.; Eichert, D.; Rey, C. Adaptative physico-chemistry of bio-related calcium phosphates. J. Mater. Chem. 2004, 14, 2148–2153. [Google Scholar]
- Eichert, D.; Salomé, M.; Banu, M.; Susini, J.; Rey, C. Preliminary characterization of calcium chemical environment in apatitic and non-apatitic calcium phosphates of biological interest by X-ray absorption spectroscopy. Spectrochim. Acta B 2005, 60B, 850–858. [Google Scholar] [CrossRef]
- Rosenman, G.; Aronov, D.; Oster, L.; Haddad, J.; Mezinskis, G.; Pavlovska, I.; Chaikina, M.; Karlov, A. Photoluminescence and surface photovoltage spectroscopy studies of hydroxyapatite nano-bio-ceramics. J. Luminescence 2007, 122–123, 936–938. [Google Scholar]
- Melikhov, I.V.; Teterin, Y.A.; Rudin, V.N.; Teterin, A.Y.; Maslakov, K.I.; Severin, A.V. An X-ray electron study of nanodisperse hydroxyapatite. Russ. J. Phys. Chem. A 2009, 83, 91–97. [Google Scholar] [CrossRef]
- Aronov, D.; Rosenman, G.; Karlov, A.; Shashkin, A. Wettability patterning of hydroxyapatite nanobioceramics induced by surface potential modification. Appl. Phys. Lett. 2006, 88, 163902:1–163902:3. [Google Scholar]
- Rau, J.V.; Generosi, A.; Ferro, D.; Minozzi, F.; Paci, B.; Albertini, V.R.; Dolci, G.; Barinov, S.M. In situ time-resolved X-ray diffraction study of evolution of nanohydroxyapatite particles in physiological solution. Mater. Sci. Eng. C 2009, 29, 1140–1143. [Google Scholar] [CrossRef]
- Arora, A. Ceramics in nanotech revolution. Adv. Eng. Mater. 2004, 6, 244–247. [Google Scholar] [CrossRef]
- Ioku, K.; Yoshimura, M. Stochiometric apatite fine single crystals by hydrothermal synthesis. Phosphorus Res. Bull. 1991, 1, 15–20. [Google Scholar]
- Chen, J.D.; Wang, Y.J.; Wei, K.; Zhang, S.H.; Shi, X.T. Self-organization of hydroxyapatite nanorods through oriented attachment. Biomaterials 2007, 28, 2275–2280. [Google Scholar]
- Guo, X.; Xiao, P.; Liu, J.; Shen, Z. Fabrication of nanostructured hydroxyapatite via hydrothermal synthesis and spark plasma sintering. J. Am. Ceram. Soc. 2004, 88, 1026–1029. [Google Scholar]
- Komarov, V.F.; Kibalchitz, V. Precipitation of apatite through highly saturated solutions. Moscow Univ. Bull. Chem. Dic. 1979, 2680–2685. [Google Scholar]
- Prakash, K.H.; Kumar, R.; Ooi, C.P.; Cheang, P.; Khor, K.A. Conductometric study of precursor compound formation during wet-chemical synthesis of nanocrystalline hydroxyapatite. J. Phys. Chem. B 2006, 110, 24457–24462. [Google Scholar]
- Tao, J.; Pan, H.; Wang, J.; Wu, J.; Wang, B.; Xu, X.; Tang, R. Evolution of amorphous calcium phosphate to hydroxyapatite probed by gold nanoparticles. J. Phys. Chem. C 2008, 112, 14929–14933. [Google Scholar]
- Chane-Ching, J.Y.; Lebugle, A.; Rousselot, I.; Pourpoint, A.; Pelle, F. Colloidal synthesis and characterization of monocrystalline apatite nanophosphors. J. Mater. Chem. 2007, 17, 2904–2913. [Google Scholar]
- Zyman, Z.Z.; Rokhmistrov, D.V.; Glushko, V.I. Structural and compositional features of amorphous calcium phosphate at the early stage of precipitation. J. Mater. Sci. Mater. Med. 2009, in press. [Google Scholar]
- Wei, M.; Ruys, A.J.; Milthorpe, B.K.; Sorrell, C.C. Solution ripening of hydroxyapatite nanoparticles: Effects on electrophoretic deposition. J. Biomed. Mater. Res. 1999, 45, 11–19. [Google Scholar]
- Zhu, X.; Eibl, O.; Berthold, C.; Scheideler, L.; Geis-Gerstorfer, J. Structural characterization of nanocrystalline hydroxyapatite and adhesion of pre-osteoblast cells. Nanotechnology 2006, 17, 2711–2721. [Google Scholar]
- Rusu, V.M.; Ng, C.H.; Wilke, M.; Tiersch, B.; Fratzl, P.; Peter, M.G. Size-controlled hydroxyapatite nanoparticles as self-organized organic–inorganic composite materials. Biomaterials 2005, 26, 5414–5426. [Google Scholar]
- Wang, Y.J.; Lai, C.; Wei, K.; Tang, S.Q. Influence of temperature, ripening time and cosurfactant on solvothermal synthesis of calcium phosphate nanobelts. Mater. Lett. 2005, 59, 1098–1104. [Google Scholar]
- Li, Y.B.; Li, D.; Weng, W. Preparation of nano carbonate-substituted hydroxyapatite from an amorphous precursor. Int. J. Appl. Ceram. Technol. 2008, 5, 442–448. [Google Scholar] [CrossRef]
- Zhang, S.; Gonsalves, K.E. Preparation and characterization of thermally stable nanohydroxyapatite. J. Mater. Sci. Mater. Med. 1997, 8, 25–28. [Google Scholar] [CrossRef]
- Ferraz, M.P.; Monteiro, F.J.; Manuel, C.M. Hydroxyapatite nanoparticles: A review of preparation methodologies. J. Appl. Biomater. Biomech. 2004, 2, 74–80. [Google Scholar]
- Ahn, E.S.; Gleason, N.J.; Nakahira, A.; Ying, J.Y. Nanostructure processing of hydroxyapatite-based bioceramics. Nano Lett. 2001, 1, 149–153. [Google Scholar]
- Mazelsky, R.; Hopkins, R.H.; Kramer, W.E. Czochralski–growth of calcium fluorophosphates. J. Cryst. Growth 1968, 3–4, 260–264. [Google Scholar]
- Loutts, G.B.; Chai, B.H.T. Growth of high-quality single crystals of FAP (Ca5(PO4)3F) and its isomorphs. Proc. SPIE Int. Soc. Optical Eng. 1993, 1863, 31–34. [Google Scholar]
- Siegel, R.W. Creating nanophase materials. Sci. Am. 1996, 275, 42–47. [Google Scholar]
- Hu, J.; Odom, T.W.; Lieber, C.M. Chemistry and physics in one dimension: Synthesis and properties of nanowires and nanotubes. Acc. Chem. Res. 1999, 32, 435–445. [Google Scholar]
- Schmidt, H.K. Nanoparticles for ceramic and nanocomposite processing. Mol. Cryst. Liq. Cryst. 2000, 353, 165–179. [Google Scholar] [CrossRef]
- Cushing, B.L.; Kolesnichenko, V.L.; O’Connor, C.J. Recent advances in the liquid-phase syntheses of inorganic nanoparticles. Chem. Rev. 2004, 104, 3893–3946. [Google Scholar]
- Wang, X.; Zhuang, J.; Peng, Q.; Li, Y. A general strategy for nanocrystal synthesis. Nature 2005, 437, 121–124. [Google Scholar]
- Mao, Y.; Park, T.J.; Zhang, F.; Zhou, H.; Wong, S.S. Environmentally friendly methodologies of nanostructure synthesis. Small 2007, 3, 1122–1139. [Google Scholar]
- Takagi, S.; Chow, L.C.; Ishikawa, K. Formation of hydroxyapatite in new calcium phosphate cements. Biomaterials 1998, 19, 1593–1599. [Google Scholar]
- Meejoo, S.; Maneeprakorn, W.; Winotai, P. Phase and thermal stability of nanocrystalline hydroxyapatite prepared via microwave heating. Thermochim. Acta 2006, 447, 115–120. [Google Scholar] [CrossRef]
- Kumta, P.; Sfeir, C.; Lee, D.H.; Olton, D.; Choi, D. Nanostructured calcium phosphates for biomedical applications: Novel synthesis and characterization. Acta Biomater. 2005, 1, 65–83. [Google Scholar] [CrossRef]
- Liou, S.C.; Chen, S.Y.; Lee, H.Y.; Bow, J.S. Structural characterization of nanosized calcium deficient apatite powders. Biomaterials 2004, 25, 189–196. [Google Scholar]
- Mollazadeh, S.; Javadpour, J.; Khavandi, A. In situ synthesis and characterization of nanosized hydroxyapatite in poly(vinyl alcohol) matrix. Ceram. Int. 2007, 33, 1579–1583. [Google Scholar]
- Bigi, A.; Boanini, E.; Gazzano, M.; Rubini, K.; Torricelli, P. Nanocrystalline hydroxyapatite—polyaspartate composites. Biomed. Mater. Eng. 2004, 14, 573–579. [Google Scholar]
- Chen, H.; Sun, K.; Tang, Z.; Law, R.V.; Mansfield, J.F.; Czajka-Jakubowska, A.; Clarkson, B.H. Synthesis of fluorapatite nanorods and nanowires by direct precipitation from solution. Cryst. Growth Des. 2006, 6, 1504–1508. [Google Scholar] [CrossRef]
- Kong, L.; Gao, Y.; Cao, W.; Gong, Y.; Zhao, N.; Zhang, X. Preparation and characterization of nano-hydroxyapatite/chitosan composite scaffolds. J. Biomed. Mater. Res. A 2005, 75A, 275–282. [Google Scholar] [CrossRef]
- Kong, L.; Gao, Y.; Lu, G.; Gong, Y.; Zhao, N.; Zhang, X. A study on the bioactivity of chitosan/nano-hydroxyapatite composite scaffolds for bone tissue engineering. Eur. Polym. J. 2006, 42, 3171–3179. [Google Scholar]
- Melikhov, I.V.; Komarov, V.F.; Severin, A.V.; Bozhevol’nov, V.E.; Rudin, V.N. Two-dimensional crystalline hydroxyapatite. Dokl. Phys. Chem. 2000, 373, 355–358. [Google Scholar]
- Zhao, Y.; Zhang, Y.; Ning, F.; Guo, D.; Xu, Z. Synthesis and cellular biocompatibility of two kinds of HAP with different nanocrystal morphology. J. Biomed. Mater. Res. B Appl. Biomater. 2007, 83B, 121–126. [Google Scholar] [CrossRef]
- Ganesan, K.; Epple, M. Calcium phosphate nanoparticles as nuclei for the preparation of colloidal calcium phytate. New J. Chem. 2008, 32, 1326–1330. [Google Scholar]
- Zhang, Y.; Lu, J. A simple method to tailor spherical nanocrystal hydroxyapatite at low temperature. J. Nanopart. Res. 2007, 9, 589–594. [Google Scholar] [CrossRef]
- Bouyer, E.; Gitzhofer, F.; Boulos, M.I. Morphological study of hydroxyapatite nanocrystal suspension. J. Mater. Sci. Mater. Med. 2000, 11, 523–531. [Google Scholar] [CrossRef]
- Wei, M.; Ruys, A.J.; Milthorpe, B.K.; Sorrell, C.C. Precipitation of hydroxyapatite nanoparticles: Effects of precipitation method on electrophoretic deposition. J. Mater. Sci. Mater. Med. 2005, 16, 319–324. [Google Scholar] [CrossRef]
- Liu, Y.; Hou, D.; Wang, G. A simple wet chemical synthesis and characterization of hydroxyapatite nanorods. Mater. Chem. Phys. 2004, 86, 69–73. [Google Scholar] [CrossRef]
- Mobasherpour, I.; Heshajin, M.S.; Kazemzadeh, A.; Zakeri, M. Synthesis of nanocrystalline hydroxyapatite by using precipitation method. J. Alloys Compd. 2007, 430, 330–333. [Google Scholar] [CrossRef]
- Phillips, M.J.; Darr, J.A.; Luklinska, Z.B.; Rehman, I. Synthesis and characterization of nanobiomaterials with potential osteological applications. J. Mater. Sci. Mater. Med. 2003, 14, 875–882. [Google Scholar] [CrossRef]
- Lee, S.J.; Yoon, Y.S.; Lee, M.H.; Oh, N.S. Nanosized hydroxyapatite powder synthesized from eggshell and phosphoric acid. J. Nanosci. Nanotechnol. 2007, 7, 4061–4064. [Google Scholar] [CrossRef]
- Monmaturapoj, N. Nanosize hydroxyapatite powders preparation by wet-chemical precipitation route. J. Metals Mater. Miner. 2008, 18, 15–20. [Google Scholar]
- Ramesh, S.; Tan, C.Y.; Sopyan, I.; Hamdi, M.; Teng, W.D. Consolidation of nanocrystalline hydroxyapatite powder. Sci. Technol. Adv. Mater. 2007, 8, 124–130. [Google Scholar] [CrossRef]
- Zhou, W.; Zhang, S.M.; Hu, W.; Qiu, Z.Y.; Liu, Y.H. Dialysis efficiency in rapid synthesis of nano-hydroxyapatite. Key Eng. Mater. 2007, 330–332, 211–214. [Google Scholar]
- Shi, H.B.; Zhong, H.; Liu, Y.; Gu, J.Y.; Yang, C.S. Effect of precipitation method on stoichiometry and morphology of hydroxyapatite nanoparticles. Key Eng. Mater. 2007, 330–332, 271–274. [Google Scholar]
- Monkawa, A.; Ikoma, T.; Yunoki, S.; Ohta, K.; Tanaka, J. Electrophoretic deposition of hydroxyapatite nanocrystal. Key Eng. Mater. 2006, 309–311, 643–646. [Google Scholar]
- Ong, H.T.; Loo, J.S.C.; Boey, F.Y.C.; Russell, S.J.; Ma, J.; Peng, K.W. Exploiting the high-affinity phosphonate—hydroxyapatite nanoparticle interaction for delivery of radiation and drugs. J. Nanopart. Res. 2008, 10, 141–150. [Google Scholar] [CrossRef]
- Silva, G.W.C.; Ma, L.; Hemmers, O.; Lindle, D. Micro-structural characterization of precipitation-synthesized fluorapatite nano-material by transmission electron microscopy using different sample preparation techniques. Micron 2008, 39, 269–274. [Google Scholar]
- Poinern, G.E.; Brundavanam, R.K.; Mondinos, N.; Jiang, Z.T. Synthesis and characterisation of nanohydroxyapatite using an ultrasound assisted method. Ultrason. Sonochem. 2009, 16, 469–474. [Google Scholar] [CrossRef]
- Doğan, Ö.; Öner, M. The influence of polymer architecture on nanosized hydroxyapatite precipitation. J. Nanosci. Nanotechnol. 2008, 8, 667–674. [Google Scholar]
- Loo, S.C.J.; Siew, Y.E.; Ho, S.; Boey, F.Y.C.; Ma, J. Synthesis and hydrothermal treatment of nanostructured hydroxyapatite of controllable sizes. J. Mater. Sci. Mater. Med. 2008, 19, 1389–1397. [Google Scholar] [CrossRef]
- Guo, X.; Gough, J.E.; Xiao, P.; Liu, J.; Shen, Z. Fabrication of nanostructured hydroxyapatite and analysis of human osteoblastic cellular response. J. Biomed. Mater. Res. A 2007, 82A, 1022–1032. [Google Scholar] [CrossRef]
- Safronova, T.V.; Putlyaev, V.I.; Sergeeva, A.I.; Kunenkov, E.V.; Tret’yakov, Y.D. Synthesis of nanocrystalline calcium hydroxyapatite from calcium saccharates and ammonium hydrogen phosphate. Dokl. Chem. 2009, 426, 118–123. [Google Scholar]
- Rodrigues, L.R.; Motisuke, M.; Zavaglia, C.A.C. Synthesis of nanostructured hydroxyapatite: A comparative study between sol-gel and aqueous solution precipitation. Key Eng. Mater. 2009, 396–398, 623–626. [Google Scholar]
- Chai, C.S.; Ben-Nissan, B. Bioactive nanocrystalline sol–gel hydroxyapatite coatings. J. Mater. Sci. Mater. Med. 1999, 10, 465–469. [Google Scholar] [CrossRef]
- Ben-Nissan, B.; Green, D.D.; Kannangara, G.S.K.; Chai, C.S.; Milev, A. 31P NMR studies of diethyl phosphite derived nanocrystalline hydroxyapatite. J. Sol-Gel Sci. Technol. 2001, 21, 27–37. [Google Scholar] [CrossRef]
- Ben-Nissan, B.; Choi, A.H. Sol-gel production of bioactive nanocoatings for medical applications. Part 1: An introduction. Nanomedicine 2006, 1, 311–319. [Google Scholar]
- Choi, A.H.; Ben-Nissan, B. Sol-gel production of bioactive nanocoatings for medical applications. Part 2: Current research and development. Nanomedicine 2007, 2, 51–61. [Google Scholar]
- Kim, T.S.; Kumta, P.N. Sol-gel synthesis and characterization of nanostructured hydroxyapatite powder. Mater. Sci. Eng. B 2004, 111, 232–236. [Google Scholar] [CrossRef]
- Rajabi-Zamani, A.H.; Behnamghader, A.; Kazemzadeh, A. Synthesis of nanocrystalline carbonated hydroxyapatite powder via nonalkoxide sol-gel method. Mater. Sci. Eng. C 2008, 28, 1326–1329. [Google Scholar] [CrossRef]
- Sopyan, I.; Toibah, A.R.; Natasha, A.N. Nanosized bioceramic hydroxyapatite powders via sol-gel method. Int. J. Mech. Mater. Eng. 2008, 3, 133–138. [Google Scholar]
- Yuan, Y.; Liu, C.; Zhang, Y.; Shan, X. Sol-gel auto-combustion synthesis of hydroxyapatite nanotubes array in porous alumina template. Mater. Chem. Phys. 2008, 112, 275–280. [Google Scholar] [CrossRef]
- Kuriakose, T.A.; Kalkura, S.N.; Palanichamy, M.; Arivuoli, D.; Dierks, K.; Bocelli, G.; Betzel, C. Synthesis of stoichiometric nano crystalline hydroxyapatite by ethanol-based sol-gel technique at low temperature. J. Cryst. Growth 2004, 263, 517–523. [Google Scholar] [CrossRef]
- Jahandideh, R.; Behnamghader, A.; Rangie, M.; Youzbashi, A.; Joughehdoust, S.; Tolouei, R. Sol-gel synthesis of FHA nanoparticles and CDHA agglomerates from a mixture with a nonstochiometric Ca/P ratio. Key Eng. Mater. 2009, 396–398, 607–610. [Google Scholar]
- Sanosh, K.P.; Chu, M.C.; Balakrishnan, A.; Lee, Y.J.; Kim, T.N.; Cho, S.J. Synthesis of nano hydroxyapatite powder that simulate teeth particle morphology and composition. Curr. Appl. Phys. 2009, 9, 1459–1462. [Google Scholar] [CrossRef]
- López-Macipe, A.; Gómez-Morales, J.; Rodríguez-Clemente, R. Nanosized hydroxyapatite precipitation from homogeneous calcium/citrate/phosphate solutions using microwave and conventional heating. Adv. Mater. 1998, 10, 49–53. [Google Scholar]
- Siddharthan, A.; Seshadri, S.K.; Kumar, T.S.S. Rapid synthesis of calcium deficient hydroxyapatite nanoparticles by microwave irradiation. Trends Biomater. Artif. Organs 2005, 18, 110–113. [Google Scholar]
- Li, B.; Wang, X.L.; Guo, B.; Xiao, Y.M.; Fan, H.S.; Zhang, X.D. Preparation and characterization of nano hydroxyapatite. Key Eng. Mater. 2007, 330–332, 235–238. [Google Scholar]
- Tas, A.C. Synthesis of biomimetic Ca-hydroxyapatite powders at 37°C in synthetic body fluids. Biomaterials 2000, 21, 1429–1438. [Google Scholar]
- Wu, Y.S.; Lee, Y.H.; Chang, H.C. Preparation and characteristics of nanosized carbonated apatite by urea addition with coprecipitation method. Mater. Sci. Eng. C 2009, 29, 237–241. [Google Scholar] [CrossRef]
- Kasahara, H.; Ogata, N.; Ogihara, T. Effect of starting solution on the formation of calcium phosphate nano particles by hydrothermal process. J. Ceram. Soc. Jpn. 2004, 112, 650–654. [Google Scholar] [CrossRef]
- Lemos, A.F.; Rocha, J.H.G.; Quaresma, S.S.F.; Kannana, S.; Oktar, F.N.; Agathopoulos, S.; Ferreira, J.M.F. Hydroxyapatite nano-powders produced hydrothermally from nacreous material. J. Eur. Ceram. Soc. 2006, 26, 3639–3646. [Google Scholar] [CrossRef]
- Chaudhry, A.A.; Haque, S.; Kellici, S.; Boldrin, P.; Rehman, I.; Khalid, F.A.; Darr, J.A. Instant nano-hydroxyapatite: A continuous and rapid hydrothermal synthesis. Chem. Commun. 2006, 2286–2288. [Google Scholar]
- Cao, M.; Wang, Y.; Guo, C.; Qi, Y.; Hu, C. Preparation of ultrahigh-aspect-ratio hydroxyapatite nanofibers in reverse micelles under hydrothermal conditions. Langmuir 2004, 20, 4784–4786. [Google Scholar]
- Jinlong, N. Hydrothermal synthesis of nano-crystalline hydroxyapatite. Key Eng. Mater. 2007, 330–332, 247–250. [Google Scholar]
- Ryu, I.Y.; Kim, D.J.; Han, J.S.; Lee, M.H. Influence of two-step sintering variables on phase stability of hydrothermally prepared HAp nano powders. Key Eng. Mater. 2008, 361–363, 91–94. [Google Scholar]
- Han, J.K.; Song, H.Y.; Saito, F.; Lee, B.T. Synthesis of high purity nanosized hydroxyapatite powder by microwave-hydrothermal method. Mater. Chem. Phys. 2006, 99, 235–239. [Google Scholar] [CrossRef]
- Suchanek, W.L.; Shuk, P.; Byrappa, K.; Riman, R.E.; TenHuisen, K.S.; Janas, V.F. Mechanochemical-hydrothermal synthesis of carbonated apatite powders at room temperature. Biomaterials 2002, 23, 699–710. [Google Scholar]
- Guo, X.; Xiao, P. Effects of solvents on properties of nanocrystalline hydroxyapatite produced from hydrothermal process. J. Eur. Ceram. Soc. 2006, 26, 3383–3391. [Google Scholar] [CrossRef]
- Xin, R.; Yu, K. Ultrastructure characterization of hydroxyapatite nanoparticles synthesized by EDTA–assisted hydrothermal method. J. Mater. Sci. 2009, 44, 4205–4209. [Google Scholar]
- Zhang, C.; Yang, J.; Quan, Z.; Yang, P.; Li, C.; Hou, Z.; Lin, J. Hydroxyapatite nano- and microcrystals with multiform morphologies: Controllable synthesis and luminescence properties. Cryst. Growth Des. 2009, 9, 2725–2733. [Google Scholar] [CrossRef]
- Zhang, H.B.; Zhou, K.C.; Li, Z.Y.; Huang, S.P. Plate-like hydroxyapatite nanoparticles synthesized by the hydrothermal method. J. Phys. Chem. Solids 2009, 70, 243–248. [Google Scholar] [CrossRef]
- Abdel-Aal, E.A.; El-Midany, A.A.; El-Shall, H. Mechanochemical-hydrothermal preparation of nano-crystallite hydroxyapatite using statistical design. Mater. Chem. Phys. 2008, 112, 202–207. [Google Scholar] [CrossRef]
- Sun, Y.; Guo, G.; Tao, D.; Wang, Z. Reverse microemulsion-directed synthesis of hydroxyapatite nanoparticles under hydrothermal conditions. J. Phys. Chem. Solids 2007, 68, 373–377. [Google Scholar] [CrossRef]
- Du, X.; Chu, Y.; Xing, S.; Dong, L. Hydrothermal synthesis of calcium hydroxyapatite nanorods in the presence of PVP. J. Mater. Sci. 2009, 44, 6273–6279. [Google Scholar]
- Rameshbabu, N.; Kumar, T.S.S.; Murugan, R.; Rao, K.P. Mechanochemical synthesis of nanocrystalline fluorinated hydroxyapatite. Int. J. Nanosci. 2005, 4, 643–649. [Google Scholar] [CrossRef]
- Yeong, K.C.B.; Wang, J.; Ng, S.C. Mechanochemical synthesis of nanocrystalline hydroxyapatite from CaO and CaHPO4. Biomaterials 2001, 22, 2705–2712. [Google Scholar]
- Coreno, J.A.; Coreno, O.A.; Cruz, R.J.J.; Rodriguez, C.C. Mechanochemical synthesis of nanocrystalline carbonate-substituted hydroxyapatite. Optical Mater. 2005, 27, 1281–1285. [Google Scholar]
- El Briak-BenAbdeslam, H.; Mochales, C.; Ginebra, M.P.; Nurit, J.; Planell, J.A.; Boudeville, P. Dry mechanochemical synthesis of hydroxyapatites from dicalcium phosphate dihydrate and calcium oxide: A kinetic study. J. Biomed. Mater. Res. A 2003, 67, 927–937. [Google Scholar] [CrossRef] [PubMed]
- Nakamura, S.; Isobe, T.; Senna, M. Hydroxyapatite nano sol prepared via a mechanochemical route. J. Nanopart. Res. 2001, 3, 57–61. [Google Scholar] [CrossRef]
- Nasiri-Tabrizi, B.; Honarmandi, P.; Ebrahimi-Kahrizsangi, R.; Honarmandi, P. Synthesis of nanosize single-crystal hydroxyapatite via mechanochemical method. Mater. Lett. 2009, 63, 543–546. [Google Scholar]
- Fathi, M.H.; Zahrani, E.M. Fabrication and characterization of fluoridated hydroxyapatite nanopowders via mechanical alloying. J. Alloys Compd. 2009, 475, 408–414. [Google Scholar] [CrossRef]
- Fathi, M.H.; Zahrani, E.M. Mechanical alloying synthesis and bioactivity evaluation of nanocrystalline fluoridated hydroxyapatite. J. Cryst. Growth 2009, 311, 1392–1403. [Google Scholar] [CrossRef]
- Silva, C.C.; Graça, M.P.F.; Valente, M.A.; Sombra, A.S.B. Crystallite size study of nanocrystalline hydroxyapatite and ceramic system with titanium oxide obtained by dry ball milling. J. Mater. Sci. 2007, 42, 3851–3855. [Google Scholar]
- Zahrani, E.M.; Fathi, M.H. The effect of high-energy ball milling parameters on the preparation and characterization of fluorapatite nanocrystalline powder. Ceram. Int. 2009, 35, 2311–2323. [Google Scholar]
- Xu, J.L.; Khor, K.A.; Dong, Z.L.; Gu, Y.W.; Kumar, R.; Cheang, P. Preparation and characterization of nanosized hydroxyapatite powders produced in a radio frequency (rf) thermal plasma. Mater. Sci. Eng. A 2004, 374, 101–108. [Google Scholar] [CrossRef]
- Xu, J.L.; Khor, K.A.; Kumar, R.; Cheang, P. RF induction plasma synthesized calcium phosphate nanoparticles. Key Eng. Mater. 2006, 309–311, 511–514. [Google Scholar]
- Ruksudjarit, A.; Pengpat, K.; Rujijanagul, G.; Tunkasiri, T. Synthesis and characterization of nanocrystalline hydroxyapatite from natural bovine bone. Curr. Appl. Phys. 2008, 8, 270–272. [Google Scholar] [CrossRef]
- Cho, J.S.; Kang, Y.C. Nano-sized hydroxyapatite powders prepared by flame spray pyrolysis. J. Alloys Compd. 2008, 464, 282–287. [Google Scholar] [CrossRef]
- Wang, X.; Zhuang, J.; Peng, Q.; Li, Y. Liquid-solid-solution synthesis of biomedical hydroxyapatite nanorods. Adv. Mater. 2006, 18, 2031–2034. [Google Scholar]
- Shirkhanzadeh, M. Direct formation of nanophase hydroxyapatite on cathodically polarized electrodes. J. Mater. Sci. Mater. Med. 1998, 9, 67–72. [Google Scholar] [CrossRef]
- Montalbert-Smith, R.; Palma, C.A.; Arias, J.D.; Montero, M.L. Formation of hydroxyapatite nanosized and other apatites by electrolysis process. Key Eng. Mater. 2009, 396–398, 579–582. [Google Scholar]
- Liu, J.; Li, K.; Wang, H.; Zhu, M.; Xu, H.; Yan, H. Self-assembly of hydroxyapatite nanostructures by microwave irradiation. Nanotechnology 2005, 16, 82–87. [Google Scholar]
- Rameshbabu, N.; Rao, K.P.; Kumar, T.S.S. Accelerated microwave processing of nanocrystalline hydroxyapatite. J. Mater. Sci. 2005, 40, 6319–6323. [Google Scholar]
- Ran, X.; Chen, J.; Ran, J.; Gou, L.; Zhang, X. Synthesis of nanosized carbonated hydroxyapatite under microwave irradiation. Key Eng. Mater. 2007, 330–332, 303–306. [Google Scholar]
- Siddharthan, A.; Seshadri, S.K.; Kumar, T.S.S. Microwave accelerated synthesis of nanosized calcium deficient hydroxyapatite. J. Mater. Sci. Mater. Med. 2004, 15, 1279–1284. [Google Scholar] [CrossRef]
- Krishna, D.S.R.; Siddharthan, A.; Seshadri, S.K.; Kumar, T.S.S. A novel route for synthesis of nanocrystalline hydroxyapatite from eggshell waste. J. Mater. Sci. Mater. Med. 2007, 18, 1735–1743. [Google Scholar] [CrossRef]
- Seo, D.S.; Hwang, K.H.; Lee, J.K. Nanostructured hydroxyapatite by microwave sintering. J. Nanosci. Nanotechnol. 2008, 8, 944–948. [Google Scholar] [CrossRef]
- Arami, H.; Mohajerani, M.; Mazloumi, M.; Khalifehzadeh, R.; Lak, A.; Sadrnezhaad, S.K. Rapid formation of hydroxyapatite nanostrips via microwave irradiation. J. Alloys Compd. 2009, 469, 391–394. [Google Scholar] [CrossRef]
- Rameshbabu, N.; Kumar, T.S.S.; Rao, K.P. Synthesis of nanocrystalline fluorinated hydroxyapatite by microwave processing and its in vitro dissolution study. Bull. Mater. Sci. 2006, 29, 611–615. [Google Scholar] [CrossRef]
- Shih, W.J.; Chen, Y.F.; Wang, M.C.; Hon, M.H. Crystal growth and morphology of the nanosized hydroxyapatite powders synthesized from CaHPO4·2H2O and CaCO3 by hydrolysis method. J. Cryst. Growth 2004, 270, 211–218. [Google Scholar] [CrossRef]
- Zhang, Y.; Lu, J. The transformation of single-crystal calcium phosphate ribbon-like fibres to hydroxyapatite spheres assembled from nanorods. Nanotechnology 2008, 19, 155608:1–155608:10. [Google Scholar]
- Furuichi, K.; Oaki, Y.; Imai, H. Preparation of nanotextured and nanofibrous hydroxyapatite through dicalcium phosphate with gelatin. Chem. Mater. 2006, 18, 229–234. [Google Scholar]
- Yoruç, A.B.H.; Koca, Y. Double step stirring: A novel method for precipitation of nano-sized hydroxyapatite powder. Digest J. Nanomater. Biostructures 2009, 4, 73–81. [Google Scholar]
- Furuzono, T.; Walsh, D.; Sato, K.; Sonoda, K.; Tanaka, J. Effect of reaction temperature on the morphology and size of hydroxyapatite nanoparticles in an emulsion system. J. Mater. Sci. Lett. 2001, 2, 111–114. [Google Scholar] [CrossRef]
- Wang, Y.J.; Lai, C.; Wei, K.; Chen, X.; Ding, Y.; Wang, Z.L. Investigations on the formation mechanism of hydroxyapatite synthesized by the solvothermal method. Nanotechnology 2006, 17, 4405–4412. [Google Scholar]
- Huang, J.; Jayasinghe, S.N.; Su, X.; Ahmad, Z.; Best, S.M.; Edirisinghe, M.J.; Brooks, R.A.; Rushton, N.; Bonfield, W. Electrostatic atomisation spraying: A novel deposition method for nano-sized hydroxyapatite. Key Eng. Mater. 2006, 309–311, 635–638. [Google Scholar]
- Hwang, K.S.; Kim, B.H. Preparation of calcium phosphate nano-powders prepared by sol-gel assisted-electrostatic spraying method. J. Mater. Sci. 2005, 40, 4665–4666. [Google Scholar]
- Uota, M.; Arakawa, H.; Kitamura, N.; Yoshimura, T.; Tanaka, J.; Kijima, T. Synthesis of high surface area hydroxyapatite nanoparticles by mixed surfactant-mediated approach. Langmuir 2005, 21, 4724–4728. [Google Scholar]
- Chu, M.; Liu, G. Preparation and characterization of hydroxyapatite/liposome core–shell nanocomposites. Nanotechnology 2005, 16, 1208–1212. [Google Scholar]
- Ye, F.; Guo, H.; Zhang, H. Biomimetic synthesis of oriented hydroxyapatite mediated by nonionic surfactants. Nanotechnology 2008, 19, 245605:1–245605:7. [Google Scholar]
- Han, Y.; Wang, X.; Li, S. A simple route to prepare stable hydroxyapatite nanoparticles suspension. J. Nanoparticle Res. 2009, 11, 1235–1240. [Google Scholar] [CrossRef]
- Tseng, Y.H.; Kuo, C.S.; Li, Y.Y.; Huang, C.P. Polymer-assisted synthesis of hydroxyapatite nanoparticle. Mater. Sci. Eng. C 2009, 29, 819–822. [Google Scholar] [CrossRef]
- Klinkaewnarong, J.; Swatsitang, E.; Maensiri, S. Nanocrystalline hydroxyapatite powders by a chitosan-polymer complex solution route: Synthesis and characterization. Solid State Sci. 2009, 11, 1023–1027. [Google Scholar] [CrossRef]
- Li, Y.; Li, D.; Xu, Z. Synthesis of hydroxyapatite nanorods assisted by Pluronics. J. Mater. Sci. 2009, 44, 1258–1263. [Google Scholar]
- Nayar, S.; Sinha, M.K.; Basu, D.; Sinha, A. Synthesis and sintering of biomimetic hydroxyapatite nanoparticles for biomedical applications. J. Mater. Sci. Mater. Med. 2006, 17, 1063–1068. [Google Scholar] [CrossRef]
- Tadic, D.; Veresov, A.; Putlayev, V.I.; Epple, M. In-vitro preparation of nanocrystalline calcium phosphates as bone substitution materials in surgery. Mat. -wiss. u. Werkstofftech. 2003, 34, 1048–1051. [Google Scholar] [CrossRef]
- Mhin, S.W.; Ryu, J.H.; Kim, K.M.; Park, G.S.; Ryu, H.W.; Shim, K.B.; Sasaki, T.; Koshizaki, N. Simple synthetic route for hydroxyapatite colloidal nanoparticles via a Nd:YAG laser ablation in liquid medium. Appl. Phys. A 2009, 96A, 435–440. [Google Scholar]
- Musaev, O.R.; Dusevich, V.; Wieliczka, D.M.; Wrobel, J.M.; Kruger, M.B. Nanoparticle fabrication of hydroxyapatite by laser ablation in water. J. Appl. Phys. 2008, 104, 084316:1–084316:5. [Google Scholar]
- Boutinguiza, M.; Lusquiños, F.; Riveiro, A.; Comesaña, R.; Pou, J. Hydroxylapatite nanoparticles obtained by fiber laser-induced fracture. Appl. Surf. Sci. 2009, 255, 5382–5385. [Google Scholar] [CrossRef]
- Zuo, Y.; Li, Y.B.; Wei, J.; Yan, Y. Influence of ethylene glycol on the formation of calcium phosphate nanocrystals. J. Mater. Sci. Technol. 2003, 19, 628–630. [Google Scholar]
- Barinov, S.M.; Belonogov, E.K.; Ievlev, V.M.; Kostyuchenko, A.V.; Putlyaev, V.I.; Tret’yakov, Y.D.; Smirnov, V.V.; Fadeeva, I.V. Synthesis of dense nanocrystalline hydroxyapatite films. Dokl. Phys. Chem. 2007, 412, 15–18. [Google Scholar] [CrossRef]
- Mello, A.; Mavropoulos, E.; Hong, Z.; Ketterson, J.B.; Rossi, A.M. Nanometer coatings of hydroxyapatite characterized by glancing-incidence X-ray diffraction. Key Eng. Mater. 2009, 396–398, 369–372. [Google Scholar]
- Luo, P.; Nieh, T.G. Synthesis of ultrafine hydroxyapatite particles by a spray dry method. Mater. Sci. Eng. C 1995, 3, 75–78. [Google Scholar] [CrossRef]
- Chen, F.; Wang, Z.C.; Chang, J.L. Preparation and characterization of nanosized hydroxyapatite particles and hydroxyapatite/chitosan nano-composite for use in biomedical materials. Mater. Lett. 2002, 57, 858–861. [Google Scholar]
- Sarig, S.; Kahana, F. Rapid formation of nanocrystalline apatite. J. Cryst. Growth 2002, 237–239, 55–59. [Google Scholar]
- Pang, Y.X.; Bao, X. Influence of temperature, ripening time and calcination on the morphology and crystallinity of hydroxyapatite nanoparticles. J. Eur. Ceram. Soc. 2003, 23, 1697–1704. [Google Scholar] [CrossRef]
- Bose, S.; Saha, S.K. Synthesis of hydroxyapatite nanopowders via sucrose-templated sol-gel method. J. Am. Ceram. Soc. 2003, 86, 1055–1057. [Google Scholar] [CrossRef]
- Han, Y.; Li, S.; Wang, X.; Chen, X. Synthesis and sintering of nanocrystalline hydroxyapatite powders by citric acid sol-gel combustion method. Mater. Res. Bull. 2004, 39, 25–32. [Google Scholar] [CrossRef]
- Leskiv, M.; Lagoa, A.L.C.; Urch, H.; Schwiertz, J.; da Piedade, M.E.M.; Epple, M. Energetics of calcium phosphate nanoparticle formation by the reaction of Ca(NO3)2 with (NH4)2HPO4. J. Phys. Chem. C 2009, 113, 5478–5484. [Google Scholar]
- Liu, D.M.; Yang, Q.; Troczynski, T.; Tseng, W.J. Structural evolution of sol-gel-derived hydroxyapatite. Biomaterials 2002, 23, 1679–1687. [Google Scholar]
- Liu, D.M.; Troczynski, T.; Tseng, W.J. Water-based sol-gel synthesis of hydroxyapatite: Process development. Biomaterials 2001, 22, 1721–1730. [Google Scholar]
- Wang, F.; Li, M.S.; Lu, Y.P.; Ge, S.S. Synthesis of nanocrystalline hydroxyapatite powders in stimulated body fluid. J. Mater. Sci. 2005, 40, 2073–2076. [Google Scholar]
- Wang, J.; Shaw, L.L. Synthesis of high purity hydroxyapatite nanopowder via sol-gel combustion process. J. Mater. Sci. Mater. Med. 2009, 20, 1223–1227. [Google Scholar] [CrossRef]
- Varma, H.K.; Kalkura, S.N.; Sivakumar, R. Polymeric precursor route for the preparation of calcium phosphate compounds. Ceram. Int. 1998, 24, 467–470. [Google Scholar]
- Loher, S.; Stark, W.J.; Maciejewski, M.; Baiker, A.; Pratsinis, S.E.; Reichardt, D.; Maspero, F.; Krumeich, F.; Günther, D. Fluoro-apatite and calcium phosphate nanoparticles by flame synthesis. Chem. Mater. 2005, 17, 36–42. [Google Scholar]
- Trommer, R.M.; Santos, L.A.; Bergmann, C.P. Nanostructured hydroxyapatite powders produced by a flame-based technique. Mater. Sci. Eng. C 2009, 29, 1770–1775. [Google Scholar] [CrossRef]
- Chow, L.C.; Sun, L.; Hockey, B. Properties of nanostructured hydroxyapatite prepared by a spray drying technique. J. Res. Natl. Inst. Stand. Technol. 2004, 109, 543–551. [Google Scholar] [CrossRef]
- Li, J.; Chen, Y.P.; Yin, Y.; Yao, F.; Yao, K. Modulation of nano-hydroxyapatite size via formation on chitosan-gelatin network film in situ. Biomaterials 2007, 28, 781–790. [Google Scholar]
- Zhai, Y.; Cui, F.Z.; Wang, Y. Formation of nano hydroxyapatite on recombinant human like collagen fibrils. Curr. Appl. Phys. 2005, 5, 429–432. [Google Scholar] [CrossRef]
- Liou, S.C.; Chen, S.Y.; Liu, D.M. Synthesis and characterization of needlelike apatitic nanocomposite with controlled aspect ratios. Biomaterials 2003, 24, 3981–3988. [Google Scholar]
- Liou, S.C.; Chen, S.Y.; Liu, D.M. Manipulation of nanoneedle and nanosphere apatite/poly(acrylic acid) nanocomposites. J. Biomed. Mater. Res. B Appl. Biomater. 2005, 73B, 117–122. [Google Scholar] [CrossRef]
- Amjad, Z. Performance of polymeric additives as HA crystal growth inhibitors. Phosphorus Res. Bull. 1995, 5, 1–12. [Google Scholar] [CrossRef]
- Kamitahara, M.; Kawashita, M.; Kokubo, T.; Nakamura, T. Effect of polyacrylic acid on the apatite formation of a bioactive ceramic in a simulated body fluid: Fundamental examination of the possibility of obtaining bioactive glass-ionomer cements for orthopedic use. Biomaterials 2001, 22, 3191–3196. [Google Scholar]
- Wang, X.; Li, Y.; Wei, J.; de Groot, K. Development of biomimetic nano-hydroxyapatite/poly(hexamethylene adipamide) composites. Biomaterials 2002, 23, 4787–4791. [Google Scholar]
- Sinha, A.; Nayar, S.; Agrawak, A.C. Synthesis of nanosized and microporous precipitated hydroxyapatite in synthetic polymers and biopolymers. J. Am. Ceram. Soc. 2003, 86, 357–359. [Google Scholar] [CrossRef]
- Liao, S.; Watari, F.; Zhu, Y.; Uo, M.; Akasaka, T.; Wang, W.; Xu, G.; Cui, F. The degradation of the three layered nano-carbonated hydroxyapatite/collagen/PLGA composite membrane in vitro. Dental Mater. 2007, 23, 1120–1128. [Google Scholar]
- Gonzalez-McQuire, R.; Chane-Ching, J.Y.; Vignaud, E.; Lebugle, A.; Mann, S. Synthesis and characterization of amino acid-functionalized hydroxyapatite nanorods. J. Mater. Chem. 2004, 14, 2277–2281. [Google Scholar]
- Rosseeva, E.V.; Golovanova, O.A.; Frank-Kamenetskaya, O.V. The influence of amino acids on the formation of nanocrystalline hydroxyapatite. Glass Phys. Chem. 2007, 33, 283–286. [Google Scholar] [CrossRef]
- Zhan, J.; Tseng, Y.H.; Chan, J.C.C.; Mou, C.Y. Biomimetic formation of hydroxyapatite nanorods by a single-crystal-to-single-crystal transformation. Adv. Funct. Mater. 2005, 15, 2005–2010. [Google Scholar] [CrossRef]
- Xu, A.W.; Ma, Y.; Cölfen, H. Biomimetic mineralization. J. Mater. Chem. 2007, 17, 415–449. [Google Scholar]
- Lim, G.K.; Wang, J.; Ng, S.C.; Gan, L.M. Formation of nanocrystalline hydroxyapatite in nonionic surfactant emulsions. Langmuir 1999, 15, 7472–7477. [Google Scholar]
- Sun, Y.; Guo, G.; Wang, Z.; Guo, H. Synthesis of single-crystal HAP nanorods. Ceram. Int. 2006, 32, 951–954. [Google Scholar]
- Bose, S.; Saha, S.K. Synthesis and characterization of hydroxyapatite nanopowders by emulsion technique. Chem. Mater. 2003, 15, 4464–4469. [Google Scholar]
- Lai, C.; Tang, S.Q.; Wang, Y.J.; Wei, K. Formation of calcium phosphate nanoparticles in reverse microemulsions. Mater. Lett. 2005, 59, 210–214. [Google Scholar]
- Jiang, F.X.; Lu, X.Y.; Zhang, M.L.; Weng, J. Regulating size, morphology and dispersion of nano-crystallites of hydroxyapatite by pH value and temperature in microemulsion system. Key Eng. Mater. 2008, 361–363, 195–198. [Google Scholar]
- Sato, K.; Hotta, Y.; Nagaoka, T.; Yasuoka, M.; Watari, K. Agglomeration control of hydroxyapatite nano-crystals grown in phase-separated microenvironments. J. Mater. Sci. 2006, 41, 5424–5428. [Google Scholar]
- Li, H.; Zhu, M.Y.; Li, L.H.; Zhou, C.R. Processing of nanocrystalline hydroxyapatite particles via reverse microemulsions. J. Mater. Sci. 2008, 43, 384–389. [Google Scholar]
- Koetz, J.; Baier, J.; Kosmella, S. Formation of zinc sulfide and hydroxylapatite nanoparticles in polyelectrolyte-modified microemulsions. Colloid Polym. Sci. 2007, 285, 1719–1726. [Google Scholar]
- Wu, Y.; Bose, S. Nanocrystalline hydroxyapatite: Micelle templated synthesis and characterization. Langmuir 2005, 21, 3232–3234. [Google Scholar]
- Wei, K.; Lai, C.; Wang, Y. Solvothermal synthesis of calcium phosphate nanowires under different pH conditions. J. Macromolec. Sci. A 2006, 43A, 1531–1540. [Google Scholar]
- Lai, C.; Tang, S.Q.; Wang, Y.J.; Wei, K.; Zhang, S.Y. Insight into shape control mechanism of calcium phosphate nanopartiles in reverse micelles solution. Synth. React. Inorg. Met. Met. Org. Nano-Metal Chem. 2005, 35, 717–725. [Google Scholar]
- Shchukin, D.G.; Sukhorukov, G.B.; Möhwald, H. Biomimetic fabrication of nanoengineered hydroxyapatite/polyelectrolyte composite shell. Chem. Mater. 2003, 15, 3947–3950. [Google Scholar]
- Mateus, A.Y.P.; Ferraz, M.P.; Monteiro, F.J. Microspheres based on hydroxyapatite nanoparticles aggregates for bone regeneration. Key Eng. Mater. 2007, 330–332, 243–246. [Google Scholar]
- Cai, Y.; Liu, Y.; Yan, W.; Hu, Q.; Tao, J.; Zhang, M.; Shi, Z.; Tang, R. Role of hydroxyapatite nanoparticle size in bone cell proliferation. J. Mater. Chem. 2007, 17, 3780–3787. [Google Scholar]
- Quantum dots, first developed in the early 1980’s, are crystalline semi-conducting nanoparticles comprised of a metalloid crystalline core and a “cap” or “shell” that shields the core and renders the dots biologically compatible. They are used or being developed for use in electronics, biomedical imaging and surveillance
- Guo, Y.; Shi, D.; Lian, J.; Dong, Z.; Wang, W.; Cho, H.; Liu, G.; Wang, L.; Ewing, R.C. Quantum dot conjugated hydroxylapatite nanoparticles for in vivo imaging. Nanotechnology 2008, 19, 175102:1–175102:6. [Google Scholar]
- Liu, Q.; de Wijn, J.R.; de Groot, K.; van Blitterswijk, C.A. Surface modification of nano-apatite by grafting organic polymer. Biomaterials 1998, 19, 1067–1072. [Google Scholar]
- Palazzo, B.; Iafisco, M.; Laforgia, M.; Margiotta, N.; Natile, G.; Bianchi, C.L.; Walsh, D.; Mann, S.; Roveri, N. Biomimetic hydroxyapatite-drug nanocrystals as potential bone substitutes with antitumor drug delivery properties. Adv. Funct. Mater. 2007, 17, 2180–2188. [Google Scholar]
- Lee, H.J.; Choi, H.W.; Kim, K.J.; Lee, S.C. Modification of hydroxyapatite nanosurfaces for enhanced colloidal stability and improved interfacial adhesion in nanocomposites. Chem. Mater. 2006, 18, 5111–5118. [Google Scholar]
- Lee, S.C.; Choi, H.W.; Lee, H.J.; Kim, K.J.; Chang, J.H.; Kim, S.Y.; Choi, J.; Oh, K.S.; Jeong, Y.K. In-situ synthesis of reactive hydroxyapatite nanocrystals for a novel approach of surface grafting polymerization. J. Mater. Chem. 2007, 17, 174–180. [Google Scholar]
- Li, L.; Liu, Y.K.; Tao, J.H.; Zhang, M.; Pan, H.H.; Xu, X.R.; Tang, R.K. Surface modification of hydroxyapatite nanocrystallite by a small amount of terbium provides a biocompatible fluorescent probe. J. Phys. Chem. C 2008, 112, 12219–12224. [Google Scholar]
- Wang, W.; Shi, D.; Lian, J.; Guo, Y.; Liu, G.; Wang, L.; Ewing, R.C. Luminescent hydroxylapatite nanoparticles by surface functionalization. Appl. Phys. Lett. 2006, 89, 183106:1–183106:3. [Google Scholar]
- Bow, J.S.; Liou, S.C.; Chen, S.Y. Structural characterization of room-temperature synthesized nanosized β-tricalcium phosphate. Biomaterials 2004, 25, 3155–3161. [Google Scholar]
- Brunner, T.J.; Bohner, M.; Dora, C.; Gerber, C.; Stark, W.J. Comparison of amorphous TCP nanoparticles to micron-sized α-TCP as starting materials for calcium phosphate cements. J. Biomed. Mater. Res. B Appl. Biomater. 2007, 83B, 400–407. [Google Scholar]
- Brunner, T.J.; Grass, R.N.; Bohner, M.; Stark, W.J. Effect of particle size, crystal phase and crystallinity on the reactivity of tricalcium phosphate cements for bone reconstruction. J. Mater. Chem. 2007, 17, 4072–4078. [Google Scholar]
- Döbelin, N.; Brunner, T.J.; Stark, W.J.; Eggimann, M.; Fisch, M.; Bohner, M. Phase evolution of thermally treated amorphous tricalcium phosphate nanoparticles. Key Eng. Mater. 2009, 396–398, 595–598. [Google Scholar]
- Bohner, M.; Brunner, T.J.; Döbelin, N.; Tang, R.; Stark, W.J. Effect of thermal treatments on the reactivity of nanosized tricalcium phosphate powders. J. Mater. Chem. 2008, 18, 4460–4467. [Google Scholar]
- Liu, Y.H.; Zhang, S.M.; Liu, L.; Zhou, W.; Hu, W.; Li, J.; Qiu, Z.Y. Rapid wet synthesis of nano-sized β-TCP by using dialysis. Key Eng. Mater. 2007, 330–332, 199–202. [Google Scholar]
- Abdel-Fattah, W.I.; Reicha, F.M.; Elkhooly, T.A. Nano-beta-tricalcium phosphates synthesis and biodegradation: 1. Effect of microwave and SO42- ions on β-TCP synthesis and its characterization. Biomed. Mater. 2008, 3, 034121:1–034121:13. [Google Scholar]
- Sanosh, K.P.; Chu, M.C.; Balakrishnan, A.; Kim, T.N.; Cho, S.J. Sol-gel synthesis of pure nano sized β-tricalcium phosphate crystalline powders. Curr. Appl. Phys. 2010, 10, 68–71. [Google Scholar]
- Dasgupta, S.; Bandyopadhyay, A.; Bose, S. Reverse micelle-mediated synthesis of calcium phosphate nanocarriers for controlled release of bovine serum albumin. Acta Biomater. 2009, 5, 3112–3121. [Google Scholar]
- Choi, D.; Kumta, P.N. Mechano-chemical synthesis and characterization of nanostructured β-TCP powder. Mater. Sci. Eng. C 2007, 27, 377–381. [Google Scholar]
- Nikcevic, I.; Maravic, D.; Ignjatovic, N.; Mitric, M.; Makovec, D.; Uskokovic, D. The formation and characterization of nanocrystalline phases by mechanical milling of biphasic calcium phosphate/poly-L-lactide biocomposite. Mater. Transact. 2006, 47, 2980–2986. [Google Scholar]
- Cho, J.S.; Jung, D.S.; Han, J.M.; Kang, Y.C. Nano-sized α and β-TCP powders prepared by high temperature flame spray pyrolysis. Mater. Sci. Eng. C 2009, 29, 1288–1292. [Google Scholar]
- Jalota, S.; Tas, A.C.; Bhaduri, S.B. Microwave-assisted synthesis of calcium phosphate nanowhiskers. J. Mater. Res. 2004, 19, 1876–1881. [Google Scholar]
- Rameshbabu, N.; Rao, K.P. Microwave synthesis, characterization and in-vitro evaluation of nanostructured biphasic calcium phosphates. Curr. Appl. Phys. 2009, 9, S29–S31. [Google Scholar]
- Li, B.; Chen, X.; Guo, B.; Wang, X.; Fan, H.; Zhang, X. Fabrication and cellular biocompatibility of porous carbonated biphasic calcium phosphate ceramics with a nanostructure. Acta Biomater. 2009, 5, 134–143. [Google Scholar]
- Guha, A.K.; Singh, S.; Kumaresan, R.; Nayar, S.; Sinha, A. Mesenchymal cell response to nanosized biphasic calcium phosphate composites. Colloids Surf. B 2009, 73, 146–151. [Google Scholar]
- Layrolle, P.; Lebugle, A. Synthesis in pure ethanol and characterization of nanosized calcium phosphate fluoroapatite. Chem. Mater. 1996, 8, 134–144. [Google Scholar]
- Andres, C.; Sinani, V.; Lee, D.; Gun’ko, Y.; Kotov, N. Anisotropic calcium phosphate nanoparticles coated with 2-carboxyethylphosphonic acid. J. Mater. Chem. 2006, 16, 3964–3968. [Google Scholar]
- Shirkhanzadeh, M.; Sims, S. Immobilization of calcium phosphate nano-clusters into alkoxy-derived porous TiO2 coatings. J. Mater. Sci. Mater. Med. 1997, 8, 595–601. [Google Scholar]
- Schmidt, H.T.; Ostafin, A.E. Liposome directed growth of calcium phosphate nanoshells. Adv. Mater. 2002, 14, 532–535. [Google Scholar]
- Schmidt, H.T.; Gray, B.L.; Wingert, P.A.; Ostafin, A.E. Assembly of aqueous-cored calcium phosphate nanoparticles for drug delivery. Chem. Mater. 2004, 16, 4942–4947. [Google Scholar]
- Xu, H.H.K.; Sun, L.; Weir, M.D.; Antonucci, J.M.; Takagi, S.; Chow, L.C.; Peltz, M. Nano DCPA—whisker composites with high strength and Ca and PO4 release. J. Dent. Res. 2006, 85, 722–727. [Google Scholar]
- Xu, H.H.K.; Weir, M.D.; Sun, L.; Takagi, S.; Chow, L.C. Effects of calcium phosphate nanoparticles on Ca-PO4 composite. J. Dent. Res. 2007, 86, 378–383. [Google Scholar]
- Xu, H.H.K.; Weir, M.D.; Sun, L. Nanocomposites with Ca and PO4 release: Effects of reinforcement, dicalcium phosphate particle size and silanization. Dental Mater. 2007, 23, 1482–1491. [Google Scholar]
- Singh, S.; Bhardwaj, P.; Singh, V.; Aggarwal, S.; Mandal, U.K. Synthesis of nanocrystalline calcium phosphate in microemulsion—effect of nature of surfactants. J. Colloid Interf. Sci. 2008, 319, 322–329. [Google Scholar]
- Wals, D.; Mann, S. Chemical synthesis of microskeletal calcium phosphate in bicontinuous microemulsions. Chem. Mater. 1996, 8, 1944–1953. [Google Scholar]
- Urch, H.; Vallet-Regí, M.; Ruiz, L.; Gonzalez-Calbet, J.M.; Epple, M. Calcium phosphate nanoparticles with adjustable dispersability and crystallinity. J. Mater. Chem. 2009, 19, 2166–2171. [Google Scholar]
- Holt, C.; Wahlgren, N.M.; Drakenberg, T. Ability of a β-casein phosphopeptide to modulate the precipitation of calcium phosphate by forming amorphous dicalcium phosphate nanoclusters. Biochem. J. 1996, 314, 1035–1039. [Google Scholar]
- Holt, C.; Timmins, P.A.; Errington, N.; Leaver, J. A core-shell model of calcium phosphate nanoclusters stabilized by β-casein phosphopeptides, derived from sedimentation equilibrium and small-angle X-ray and neutron-scattering measurements. Eur. J. Biochem. 1998, 252, 73–78. [Google Scholar]
- Duan, B.; Wang, M.; Zhou, W.Y.; Cheung, W.L. Synthesis of Ca-P nanoparticles and fabrication of Ca-P/PHBV nanocomposite microspheres for bone tissue engineering applications. Appl. Surf. Sci. 2008, 255, 529–533. [Google Scholar]
- Hwang, K.S.; Jeon, K.O.; Jeon, Y.S.; Kim, B.H. Hydroxyapatite forming ability of electrostatic spray pyrolysis derived calcium phosphate nano powder. J. Mater. Sci. 2006, 41, 4159–4162. [Google Scholar]
- Hwang, K.S.; Jeon, K.O.; Jeon, Y.S.; Kim, B.H. Hydroxyapatite forming ability of electrostatic spray pyrolysis derived calcium phosphate nano powder. J. Mater. Sci. Mater. Med. 2007, 18, 619–622. [Google Scholar]
- Perkin, K.K.; Turner, J.L.; Wooley, K.L.; Mann, S. Fabrication of hybrid nanocapsules by calcium phosphate mineralization of shell cross-linked polymer micelles and nanocages. Nano Lett. 2005, 5, 1457–1461. [Google Scholar]
- Tjandra, W.; Ravi, P.; Yao, J.; Tam, K.C. Synthesis of hollow spherical calcium phosphate nanoparticles using polymeric nanotemplates. Nanotechnology 2006, 17, 5988–5994. [Google Scholar]
- Sadasivan, S.; Khushalani, D.; Mann, S. Synthesis of calcium phosphate nanofilaments in reverse micelles. Chem. Mater. 2005, 17, 2765–2770. [Google Scholar]
- Morgan, T.T.; Muddana, H.S.; Altinoglu, E.I.; Rouse, S.M.; Tabakovic, A.; Tabouillot, T.; Russin, T.J.; Butler, P.J.; Eklund, P.; Yun, J.K.; Kester, M.; Adair, J.H. Encapsulation of organic molecules in calcium phosphate nanocomposite particles for intracellular imaging and drug delivery. Nano Lett. 2008, 8, 4108–4115. [Google Scholar]
- Lai, C.; Wang, Y.J.; Wei, K. Nucleation kinetics of calcium phosphate nanoparticles in reverse micelle solution. Colloids Surf. A 2008, 315, 268–274. [Google Scholar]
- Socol, G.; Torricelli, P.; Bracci, B.; Iliescu, M.; Miroiu, F.; Bigi, A.; Werckmann, J.; Mihailescu, I.N. Biocompatible nanocrystalline octacalcium phosphate thin films obtained by pulsed laser deposition. Biomaterials 2004, 25, 2539–2545. [Google Scholar]
- Urch, H.; Franzka, S.; Dahlhaus, D.; Hartmann, N.; Hasselbrink, E.; Epple, M. Preparation of two-dimensionally patterned layers of functionalised calcium phosphate nanoparticles by laser direct writing. J. Mater. Chem. 2006, 16, 1798–1802. [Google Scholar]
- Sokolova, V.; Prymak, O.; Meyer-Zaika, W.; Cölfen, H.; Rehage, H.; Shukla, A.; Epple, M. Synthesis and characterization of DNA functionalized calcium phosphate nanoparticles. Mat. -wiss. u. Werkstofftech 2006, 37, 441–445. [Google Scholar]
- Muddana, H.S.; Morgan, T.T.; Adair, J.H.; Butler, P.J. Photophysics of Cy3-encapsulated calcium phosphate nanoparticles. Nano Letters 2009, 9, 1559–1566. [Google Scholar]
- Altinoğlu, E.I.; Russin, T.J.; Kaiser, J.M.; Barth, B.M.; Eklund, P.C.; Kester, M.; Adair, J.H. Near-infrared emitting fluorophore-doped calcium phosphate nanoparticles for in vivo imaging of human breast cancer. ACS Nano 2008, 2, 2075–2084. [Google Scholar]
- Schwiertz, J.; Wiehe, A.; Gräfe, S.; Gitter, B.; Epple, M. Calcium phosphate nanoparticles as efficient carriers for photodynamic therapy against cells and bacteria. Biomaterials 2009, 30, 3324–3331. [Google Scholar]
- Pan, L.; Li, Y.; Zou, C.; Weng, W.; Cheng, K.; Song, C.; Du, P.; Zhao, G.; Shen, G.; Wang, J.; Han, G. Surface modification of nanosized biphasic α-TCP/HA powders. Key Eng. Mater. 2007, 330–332, 223–226. [Google Scholar]
- Schwiertz, J.; Meyer-Zaika, W.; Ruiz-Gonzalez, L.; González-Calbet, J.M.; Vallet-Regí, M.; Epple, M. Calcium phosphate nanoparticles as templates for nanocapsules prepared by the layer-by-layer technique. J. Mater. Chem. 2008, 18, 3831–3834. [Google Scholar]
- Hayakawa, S.; Li, Y.; Tsuru, K.; Osaka, A.; Fujii, E.; Kawabata, K. Preparation of nanometer-scale rod array of hydroxyapatite crystal. Acta Biomater. 2009, 5, 2152–2160. [Google Scholar]
- Liao, S.S.; Cui, F.Z.; Zhang, W.; Feng, Q.L. Hierarchically biomimetic bone scaffold materials: Nano-HA/collagen/PLA composite. J. Biomed. Mater. Res. B Appl. Biomater. 2004, 69B, 158–165. [Google Scholar]
- Thomas, V.; Dean, D.R.; Jose, M.V.; Mathew, B.; Chowdhury, S.; Vohra, Y.K. Nanostructured biocomposite scaffolds based on collagen co-electrospun with nanohydroxyapatite. Biomacromolecules 2007, 8, 631–637. [Google Scholar]
- De Yoreo, J.J.; Vekilov, P.G. Principles of crystal nucleation and growth. Rev. Mineral. Geochem. 2003, 54, 57–93. [Google Scholar]
- Liao, S.; Xu, G.; Wang, W.; Watari, F.; Cui, F.; Ramakrishna, S.; Chan, C.K. Self-assembly of nano-hydroxyapatite on multi-walled carbon nanotubes. Acta Biomater. 2007, 3, 669–675. [Google Scholar]
- Penn, R.L.; Banfield, J.F. Imperfect oriented attachment: Dislocation generation in defect-free nanocrystals. Science 1998, 281, 969–971. [Google Scholar]
- Tao, J.; Pan, H.; Zeng, Y.; Xu, X.; Tang, R. Roles of amorphous calcium phosphate and biological additives in the assembly of hydroxyapatite nanoparticles. J. Phys. Chem. B 2007, 111, 13410–13418. [Google Scholar]
- Hing, K.A. Bone repair in the twenty-first century: Biology, chemistry or engineering? Philos. Trans. R. Soc. Lond. A 2004, 362, 2821–2850. [Google Scholar]
- Kokubo, T.; Kim, H.M.; Kawashita, M. Novel bioactive materials with different mechanical properties. Biomaterials 2003, 24, 2161–2175. [Google Scholar]
- Fu, J.M.; Miao, B.; Jia, L.H.; Lü, K.L. Nano-hydroxyapatite for repair of rabbit jaw bone defect: Bone mineral density analysis. J. Clin. Rehabil. Tissue Eng. Res. 2009, 13, 2387–2390. [Google Scholar]
- Barralet, J.E.; Lilley, K.J.; Grover, L.M.; Farrar, D.F.; Ansell, C.; Gbureck, U. Cements from nanocrystalline hydroxyapatite. J. Mater. Sci. Mater. Med. 2004, 15, 407–411. [Google Scholar]
- Lilley, K.J.; Gbureck, U.; Wright, A.J.; Farrar, D.F.; Barralet, J.E. Cement from nanocrystalline hydroxyapatite: Effect of calcium phosphate ratio. J. Mater. Sci. Mater. Med. 2005, 16, 1185–1190. [Google Scholar]
- Neira, I.S.; Kolen’ko, Y.V.; Lebedev, O.I.; van Tendeloo, G.; Gupta, H.S.; Matsushita, N.; Yoshimura, M.; Guitián, F. Rational synthesis of a nanocrystalline calcium phosphate cement exhibiting rapid conversion to hydroxyapatite. Mater. Sci. Eng. C 2009, 29, 2124–2132. [Google Scholar]
- Dorozhkin, S.V. Calcium orthophosphate cements for biomedical application. J. Mater. Sci. 2008, 43, 3028–3057. [Google Scholar]
- Dorozhkin, S.V. Calcium orthophosphate cements and concretes. Materials 2009, 2, 221–291. [Google Scholar]
- Fu, Q.; Zhou, N.; Huang, W.; Wang, D.; Zhang, L.; Li, H. Effects of nano HAP on biological and structural properties of glass bone cement. J. Biomed. Mater. Res. A 2005, 74A, 156–163. [Google Scholar]
- Strnadova, M.; Protivinsky, J.; Strnad, J.; Vejsicka, Z. Preparation of porous synthetic nanostructured HA scaffold. Key Eng. Mater. 2008, 361>–363, 211–214. [Google Scholar]
- Kim, J.Y.; Lee, J.W.; Lee, S.J.; Park, E.K.; Kim, S.Y.; Cho, D.W. Development of a bone scaffold using HA nanopowder and micro-stereolithography technology. Microelectronic Engineering 2007, 84, 1762–1765. [Google Scholar]
- Severin, A.V.; Komarov, V.F.; Bozhevol’nov, V.E.; Melikhov, I.V. Morphological selection in suspensions of nanocrystalline hydroxylapatite leading to spheroidal aggregates. Russ. J. Inorg. Chem. 2005, 50, 72–77. [Google Scholar]
- Krylova, I.V.; Ivanov, L.N.; Bozhevol’nov, V.E.; Severin, A.V. Self-organization processes and phase transitions in nanocrystalline hydroxyapatite according to exoemission data. Russ. J. Phys. Chem. A 2007, 81, 241–245. [Google Scholar]
- Veljovic, D.; Jokic, B.; Jankovic-Castvan, I.; Smiciklas, I.; Petrovic, R.; Janackovic, D. Sintering behaviour of nanosized HAP powder. Key Eng. Mater. 2007, 330>–332, 259–262. [Google Scholar]
- Zhang, F.; Lin, K.; Chang, J.; Lu, J.; Ning, C. Spark plasma sintering of macroporous calcium phosphate scaffolds from nanocrystalline powders. J. Eur. Ceram. Soc. 2008, 28, 539–545. [Google Scholar]
- Kutty, M.G.; Loertscher, J.; Bhaduri, S.; Bhaduri, S.B.; Tinga, W.R. Microwave sintering of nanocrystalline hydroxyapatite. Ceram. Eng. Sci. Proc. 2001, 22, 3–10. [Google Scholar]
- Vijayan, S.; Varma, H. Microwave sintering of nanosized hydroxyapatite powder compacts. Mater. Lett. 2002, 56, 827–831. [Google Scholar]
- Ramesh, S.; Tan, C.Y.; Bhaduri, S.B.; Teng, W.D. Rapid densification of nanocrystalline hydroxyapatite for biomedical applications. Ceram. Int. 2007, 33, 1363–1367. [Google Scholar]
- Okada, M.; Furuzono, T. Fabrication of high-dispersibility nanocrystals of calcined hydroxyapatite. J. Mater. Sci. 2006, 41, 6134–6137. [Google Scholar]
- Okada, M.; Furuzono, T. Nanosized ceramic particles of hydroxyapatite calcined with an anti-sintering agent. J. Nanosci. Nanotechnol. 2007, 7, 848–851. [Google Scholar]
- Okada, M.; Furuzono, T. Calcination of rod-like hydroxyapatite nanocrystals with an anti-sintering agent surrounding the crystals. J. Nanopart. Res. 2007, 9, 807–815. [Google Scholar]
- Müller-Mai, C.M.; Stupp, S.I.; Voigt, C.; Gross, U. Nanoapatite and organoapatite implants in bone: Histology and ultrastructure of the interface. J. Biomed. Mater. Res. 1995, 29, 9–18. [Google Scholar]
- Du, C.; Cui, F.Z.; Feng, Q.L.; Zhu, X.D.; de Groot, K. Tissue response to nano-hydroxyapatite/collagen composite implants in marrow cavity. J. Biomed. Mater. Res. 1998, 42, 540–548. [Google Scholar]
- Du, C.; Cui, F.Z.; Zhu, X.D.; de Groot, K. Three-dimensional nano-HAp/collagen matrix loading with osteogenic cells in organ culture. J. Biomed. Mater. Res. 1999, 44, 407–415. [Google Scholar]
- Paul, W.; Sharma, C.P. Nanoceramic matrices: Biomedical applications. Am. J. Biochem. Biotechnol. 2006, 2, 41–48. [Google Scholar]
- Huber, F.X.; McArthur, N.; Hillmeier, J.; Kock, H.J.; Baier, M.; Diwo, M.; Berger, I.; Meeder, P.J. Void filling of tibia compression fracture zones using a novel resorbable nanocrystalline hydroxyapatite paste in combination with a hydroxyapatite ceramic core: First clinical results. Arch. Orthop. Trauma Surg. 2006, 126, 533–540. [Google Scholar]
- Smeets, R.; Jelitte, G.; Heiland, M.; Kasaj, A.; Grosjean, M.; Riediger, D.; Yildirim, M.; Spiekermann, H.; Maciejewski, O. Hydroxylapatit-Knochenersatzmaterial (Ostim®) bei der Sinusbodenelevation. Schweiz Monatsschr. Zahnmed. 2008, 118, 203–208. [Google Scholar]
- Gerlach, K.L.; Niehues, D. Die Behandlung der Kieferzysten mit einem neuartigen nanopartikulären Hydroxylapatit. Mund Kiefer GesichtsChir. 2007, 11, 131–137. [Google Scholar]
- Schwarz, F.; Bieling, K.; Latz, T.; Nuesry, E.; Becker, J. Healing of intrabony periimplantitis defects following application of a nanocristalline hydroxyapatite (Ostim™) or a bovine-derived xenograft (Bio-Oss™) in combination with a collagen membrane (Bio-Gide™). A case series. J. Clin. Periodontol. 2006, 33, 491–499. [Google Scholar]
- Strietzel, F.P.; Reichart, P.A.; Graf, H.L. Lateral alveolar ridge augmentation using a synthetic nano-crystalline hydroxyapatite bone substitution material (Ostim®). Preliminary clinical and histological results. Clin. Oral Implants Res. 2007, 18, 743–751. [Google Scholar]
- Spies, C.; Schnürer, S.; Gotterbarm, T.; Breusch, S. Tierexperimentelle Untersuchung des Knochenersatzstoffs OstimTM im knöchernen Lager des Göttinger Miniaturschweins. Z. Orthop. Unfall. 2008, 146, 64–69. [Google Scholar]
- Thorwarth, M.; Schultze-Mosgau, S.; Kessler, P.; Wiltfang, J.; Schlegel, K.A. Bone regeneration in osseous defects using a resorbable nanoparticular hydroxyapatite. J. Oral Maxillofac. Surg. 2005, 63, 1626–1633. [Google Scholar]
- Brandt, J.; Henning, S.; Michler, G.; Schulz, M.; Bernstein, A. Nanocrystalline hydroxyapatite for bone repair. Key Eng. Mater. 2008, 361–, 35–38. [Google Scholar]
- Huber, F.X.; Hillmeier, J.; Herzog, L.; McArthur, N.; Kock, H.J.; Meeder, P.J. Open reduction and palmar plate-osteosynthesis in combination with a nanocrystalline hydroxyapatite spacer in the treatment of comminuted fractures of the distal radius. J. Hand Surg. (Brit.) 2006, 31B, 298–303. [Google Scholar]
- Huber, F.X.; Hillmeier, J.; McArthur, N.; Kock, H.J.; Meeder, P.J. The use of nanocrystalline hydroxyapatite for the reconstruction of calcaneal fractures: Preliminary results. J. Foot Ankle Surg. 2006, 45, 322–328. [Google Scholar]
- Laschke, M.W.; Witt, K.; Pohlemann, T.; Menger, M.D. Injectable nanocrystalline hydroxyapatite paste for bone substitution: In vivo analysis of biocompatibility and vascularization. J. Biomed. Mater. Res. B Appl. Biomater. 2007, 82B, 494–505. [Google Scholar]
- Spies, C.K.G.; Schnürer, S.; Gotterbarm, T.; Breusch, S. The efficacy of Biobon™ and Ostim™ within metaphyseal defects using the Göttinger Minipig. Arch. Orthop. Trauma Surg. 2009, 129, 979–988. [Google Scholar]
- Huber, F.X.; Belyaev, O.; Hillmeier, J.; Kock, H.J.; Huber, C.; Meeder, P.J.; Berger, I. First histological observations on the incorporation of a novel nanocrystalline hydroxyapatite paste OSTIM® in human cancellous bone. BMC Musculoskelet. Disord. 2006, 7, 50:1–50:14. [Google Scholar]
- Huber, F.X.; Berger, I.; McArthur, N.; Huber, C.; Kock, H.P.; Hillmeier, J.; Meeder, P.J. Evaluation of a novel nanocrystalline hydroxyapatite paste and a solid hydroxyapatite ceramic for the treatment of critical size bone defects (CSD) in rabbits. J. Mater. Sci. Mater. Med. 2008, 19, 33–38. [Google Scholar]
- Arts, J.J.C.; Verdonschot, N.; Schreurs, B.W.; Buma, P. The use of a bioresorbable nano-crystalline hydroxyapatite paste in acetabular bone impaction grafting. Biomaterials 2006, 27, 1110–1118. [Google Scholar]
- Zhang, W.; Liao, S.S.; Cui, F.Z. Hierarchical self-assembly of nano-fibrils in mineralized collagen. Chem. Mater. 2003, 15, 3221–3226. [Google Scholar]
- Li, X.; Huang, J.; Edirisinghe, M.J. Development of nano-hydroxyapatite coating by electrohydrodynamic atomization spraying. J. Mater. Sci. Mater. Med. 2008, 19, 1545–1551. [Google Scholar]
- Guo, L.; Li, H. Fabrication and characterization of thin nano-hydroxyapatite coatings on titanium. Surf. Coat. Technol. 2004, 185, 268–274. [Google Scholar]
- Thian, E.S.; Ahmad, Z.; Huang, J.; Edirisinghe, M.J.; Jayasinghe, S.N.; Ireland, D.C.; Brooks, R.A.; Rushton, N.; Bonfield, W.; Best, S.M. Electrosprayed nanoapatite: A new generation of bioactive material. Key Eng. Mater. 2008, 361–363, 597–600. [Google Scholar]
- Han, Y.; Xu, K.; Montay, G.; Fu, T.; Lu, J. Evaluation of nanostructured carbonated hydroxyapatite coatings formed by a hybrid process of plasma spraying and hydrothermal synthesis. J. Biomed. Mater. Res. 2002, 60, 511–516. [Google Scholar]
- Li, P. Biomimetic nano-apatite coating capable of promoting bone ingrowth. J. Biomed. Mater. Res. A 2003, 66A, 79–85. [Google Scholar]
- Mendes, V.C.; Moineddin, R.; Davies, J.E. The effect of discrete calcium phosphate nanocrystals on bone-bonding to titanium surfaces. Biomaterials 2007, 28, 4748–4755. [Google Scholar]
- Oh, S.H.; Finõnes, R.R.; Daraio, C.; Chen, L.H.; Jin, S. Growth of nano-scale hydroxyapatite using chemically treated titanium oxide nanotubes. Biomaterials 2005, 26, 4938–4943. [Google Scholar]
- Ma, J.; Wong, H.; Kong, L.B.; Peng, K.W. Biomimetic processing of nanocrystallite bioactive apatite coating on titanium. Nanotechnology 2003, 14, 619–623. [Google Scholar]
- Gu, Y.W.; Tay, B.Y.; Lim, C.S.; Yong, M.S. Nanocrystallite apatite formation and its growth kinetics on chemically treated porous NiTi. Nanotechnology 2006, 17, 2212–2218. [Google Scholar]
- Hu, R.; Lin, C.J.; Shi, H.Y. A novel ordered nano hydroxyapatite coating electrochemically deposited on titanium substrate. J. Biomed. Mater. Res. A 2007, 80A, 687–692. [Google Scholar]
- Bigi, A.; Boanini, E.; Bracci, B.; Facchini, A.; Panzavolta, S.; Segatti, F.; Sturba, L. Nanocrystalline hydroxyapatite coatings on titanium: A new fast biomimetic method. Biomaterials 2005, 26, 4085–4089. [Google Scholar]
- Narayanan, R.; Seshadri, S.K.; Kwon, T.Y.; Kim, K.H. Electrochemical nano-grained calcium phosphate coatings on Ti-6Al-4V for biomaterial applications. Scripta Mater. 2007, 56, 229–232. [Google Scholar]
- Thian, E.S.; Huang, J.; Best, S.M.; Barber, Z.H.; Bonfield, W. Nanostructured apatite coatings for rapid bone repair. Key Eng. Mater. 2006, 309–311, 519–522. [Google Scholar]
- Cai, X.; Gong, P.; Man, Y.; Chen, Z.; He, G. The construction and characterization of nano-FHA bioceramic coating on titanium surface. Key Eng. Mater. 2007, 330–332, 333–336. [Google Scholar]
- Citterio, H.; Jakani, S.; Benmarouane, A.; Millet, P.; Lodini, A. Nano-hydroxyapatite coatings on titanium substrates. Finite element analysis of process and experimental plasma thermal sprayed coatings. Key Eng. Mater. 2008, 361–363, 745–748. [Google Scholar]
- Lee, S.H.; Kim, H.E.; Kim, H.W. Nanosized hydroxyapatite coatings on Ti substrate with TiO2 buffer layer by e-beam deposition. J. Am. Ceram. Soc. 2007, 90, 50–56. [Google Scholar]
- Nishimura, I.; Huang, Y.; Butz, F.; Ogawa, T.; Lin, A.; Wang, C.J. Discrete deposition of hydroxyapatite nanoparticles on a titanium implant with predisposing substrate microtopography accelerated osseointegration. Nanotechnology 2007, 18, 245101:1–245101:9. [Google Scholar]
- Narayanan, R.; Kwon, T.Y.; Kim, K.H. Preparation and characteristics of nano-grained calcium phosphate coatings on titanium from ultrasonated bath at acidic pH. J. Biomed. Mater. Res. B Appl. Biomater. 2008, 85B, 231–239. [Google Scholar]
- Hahn, B.D.; Park, D.S.; Choi, J.J.; Ryu, J.; Yoon, W.H.; Kim, K.H.; Park, C.; Kim, H.E. Dense nanostructured hydroxyapatite coating on titanium by aerosol deposition. J. Am. Ceram. Soc. 2009, 92, 683–687. [Google Scholar]
- Narayanan, R.; Kwon, T.Y.; Kim, K.H. Direct nanocrystalline hydroxyapatite formation on titanium from ultrasonated electrochemical bath at physiological pH. Mater. Sci. Eng. C 2008, 28, 1265–1270. [Google Scholar]
- Yousefpour, M.; Afshar, A.; Yang, X.; Li, X.; Yang, B.; Wu, Y.; Chen, J.; Zhang, X. Nano-crystalline growth of electrochemically deposited apatite coating on pure titanium. J. Electroanal. Chem. 2006, 589, 96–105. [Google Scholar]
- Mendes, V.C.; Moineddin, R.; Davies, J.E. Discrete calcium phosphate nanocrystalline deposition enhances osteoconduction on titanium-based implant surfaces. J. Biomed. Mater. Res. A 2009, 90A, 577–585. [Google Scholar]
- Yang, Y.; Kim, K.H.; Ong, J.L. A review on calcium phosphate coatings produced using a sputtering process—an alternative to plasma spraying. Biomaterials 2005, 26, 327–337. [Google Scholar]
- Nies, B.; Rößler, S.; Reinstorf, A. Formation of nano hydroxyapatite—a straightforward way to bioactivate bone implant surfaces. Int. J. Mat. Res. (formerly Z. Metallkd.) 2007, 98, 630–636. [Google Scholar]
- Jalota, S.; Bhaduri, S.B.; Tas, A.C. Effect of carbonate content and buffer type on calcium phosphate formation in SBF solutions. J. Mater. Sci. Mater. Med. 2006, 17, 697–707. [Google Scholar]
- Chen, F.; Lam, W.M.; Lin, C.J.; Qiu, G.X.; Wu, Z.H.; Luk, K.D.K.; Lu, W.W. Biocompatibility of electrophoretical deposition of nanostructured hydroxyapatite coating on roughen titanium surface: In vitro evaluation using mesenchymal stem cells. J. Biomed. Mater. Res. B Appl. Biomater. 2007, 82B, 183–191. [Google Scholar]
- Thian, E.S.; Ahmad, Z.; Huang, J.; Edirisinghe, M.J.; Jayasinghe, S.N.; Ireland, D.C.; Brooks, R.A.; Rushton, N.; Bonfield, W.; Best, S.M. The role of electrosprayed nanoapatites in guiding osteoblast behaviour. Biomaterials 2008, 29, 1833–1843. [Google Scholar]
- Bigi, A.; Nicoli-Aldini, N.; Bracci, B.; Zavan, B.; Boanini, E.; Sbaiz, F.; Panzavolta, S.; Zorzato, G.; Giardino, R.; Facchini, A.; Abatangelo, G.; Cortivo, R. In vitro culture of mesenchymal cells onto nanocrystalline hydroxyapatite coated Ti13Nb13Zr alloy. J. Biomed. Mater. Res. A 2007, 82A, 213–221. [Google Scholar]
- Bigi, A.; Fini, M.; Bracci, B.; Boanini, E.; Torricelli, P.; Giavaresi, G.; Aldini, N.N.; Facchini, A.; Sbaiz, F.; Giardino, R. The response of bone to nanocrystalline hydroxyapatite-coated Ti13Nb11Zr alloy in an animal model. Biomaterials 2008, 29, 1730–1736. [Google Scholar]
- Thian, E.S.; Huang, J.; Ahmad, Z.; Edirisinghe, M.J.; Jayasinghe, S.N.; Ireland, D.C.; Brooks, R.A.; Rushton, N.; Best, S.M.; Bonfield, W. Influence of nanohydroxyapatite patterns deposited by electrohydrodynamic spraying on osteoblast response. J. Biomed. Mater. Res. A 2008, 85A, 188–194. [Google Scholar]
- Furuzono, T.; Masuda, M.; Okada, M.; Yasuda, S.; Kadono, H.; Tanaka, R.; Miyatake, K. Increase in cell adhesiveness on a poly(ethylene terephthalate) fabric by sintered hydroxyapatite nanocrystal coating in the development of an artificial blood vessel. ASAIO J. 2006, 52, 315–320. [Google Scholar]
- Yanagida, H.; Okada, M.; Masuda, M.; Ueki, M.; Narama, I.; Kitao, S.; Koyama, Y.; Furuzono, T.; Takakuda, K. Cell adhesion and tissue response to hydroxyapatite nanocrystal-coated poly(L-lactic acid) fabric. J. Biosci. Bioengin. 2009, 108, 235–243. [Google Scholar]
- Li, X.; Huang, J.; Edirisinghe, M.J. Development of template-assisted electrohydrodynamic atomization spraying for nanoHA patterning. Key Eng. Mater. 2008, 361–363, 585–588. [Google Scholar]
- Shi, Z.L.; Huang, X.; Cai, Y.R.; Tang, R.K.; Yang, D.S. Size effect of hydroxyapatite nanoparticles on proliferation and apoptosis of osteoblast-like cells. Acta Biomater. 2009, 5, 338–345. [Google Scholar]
- Liu, Y.; Wang, G.; Cai, Y.; Ji, H.; Zhou, G.; Zhao, X.; Tang, R.; Zhang, M. In vitro effects of nanophase hydroxyapatite particles on proliferation and osteogenic differentiation of bone marrow-derived mesenchymal stem cells. J. Biomed. Mater. Res. A 2009, 15, 1083–1091. [Google Scholar]
- Zhu, X.; Eibl, O.; Scheideler, L.; Geis-Gerstorfer, J. Characterization of nano hydroxyapatite/collagen surfaces and cellular behaviors. J. Biomed. Mater. Res. A 2006, 79A, 114–127. [Google Scholar]
- Wang, H.; Li, Y.; Zuo, Y.; Li, J.; Ma, S.; Cheng, L. Biocompatibility and osteogenesis of biomimetic nano-hydroxyapatite/polyamide composite scaffolds for bone tissue engineering. Biomaterials 2007, 28, 3338–3348. [Google Scholar]
- Zhang, Y.F.; Cheng, X.R.; Chen, Y.; Shi, B.; Chen, X.H.; Xu, D.X.; Ke, J. Three-dimensional nanohydroxyapatite/chitosan scaffolds as potential tissue engineered periodontal tissue. J. Biomater. Appl. 2007, 21, 333–349. [Google Scholar]
- Huang, Y.X.; Ren, J.; Chen, C.; Ren, T.B.; Zhou, X.Y. Preparation and properties of poly(lactide-co-glycolide) (PLGA) / nano-hydroxyapatite (NHA) scaffolds by thermally induced phase separation and rabbit mscs culture on scaffolds. J. Biomater. Appl. 2008, 22, 409–432. [Google Scholar]
- Thian, E.S.; Ahmad, Z.; Huang, J.; Edirisinghe, M.J.; Jayasinghe, S.N.; Ireland, D.C.; Brooks, R.A.; Rushton, N.; Bonfield, W.; Best, S.M. Bioactivity of nanoapatite produced by electrohydrodynamic atomization. J. Bionanosci. 2007, 1, 60–63. [Google Scholar]
- Pezzatini, S.; Solito, R.; Morbidelli, L.; Lamponi, S.; Boanini, E.; Bigi, A.; Ziche, M. The effect of hydroxyapatite nanocrystals on microvascular endothelial cell viability and functions. J. Biomed. Mater. Res. A 2006, 76A, 656–663. [Google Scholar]
- Pezzatini, S.; Morbidelli, L.; Solito, R.; Paccagnini, E.; Boanini, E.; Bigi, A.; Ziche, M. Nanostructured HA crystals up-regulate FGF-2 expression and activity in microvascular endothelium promoting angiogenesis. Bone 2007, 41, 523–534. [Google Scholar]
- Hu, Q.; Tan, Z.; Liu, Y.; Tao, J.; Cai, Y.; Zhang, M.; Pan, H.; Xu, X.; Tang, R. Effect of crystallinity of calcium phosphate nanoparticles on adhesion, proliferation, and differentiation of bone marrow mesenchymal stem cells. J. Mater. Chem. 2007, 17, 4690–4698. [Google Scholar]
- Balasundaram, G.; Sato, M.; Webster, T.J. Using hydroxyapatite nanoparticles and decreased crystallinity to promote osteoblast adhesion similar to functionalizing with RGD. Biomaterials 2006, 27, 2798–2805. [Google Scholar]
- Stevens, M.M.; George, J.H. Exploring and engineering the cell surface interface. Science 2005, 310, 1135–1138. [Google Scholar]
- Martínez, E.; Engel, E.; Planell, J.A.; Samitier, J. Effects of artificial micro- and nano-structured surfaces on cell behaviour. Annals Anat. 2009, 191, 126–135. [Google Scholar]
- Lee, D.H.; Han, J.S.; Yang, J.H.; Lee, J.B. MC3T3-E1 cell response to pure titanium, zirconia and nano-hydroxyapatite. Int. J. Modern Phys. B 2009, 23, 1535–1540. [Google Scholar]
- Onuma, K.; Yamagishi, K.; Oyane, A. Nucleation and growth of hydroxyapatite nanocrystals for nondestructive repair of early caries lesions. J. Cryst. Growth 2005, 282, 199–207. [Google Scholar]
- Roveri, N.; Battistella, E.; Bianchi, C.L.; Foltran, I.; Foresti, E.; Iafisco, M.; Lelli, M.; Naldoni, A.; Palazzo, B.; Rimondini, L. Surface enamel remineralization: Biomimetic apatite nanocrystals and fluoride ions different effects. J. Nanomater 2009, 746383:1–746383:9. [Google Scholar]
- Lv, K.; Zhang, J.; Meng, X.; Li, X. Remineralization effect of the nano-HA toothpaste on artificial caries. Key Eng. Mater. 2007, 330–332, 267–270. [Google Scholar]
- Jeong, S.H.; Jang, S.O.; Kim, K.N.; Kwon, H.K.; Park, Y.D.; Kim, B.I. Remineralization potential of new toothpaste containing nano-hydroxyapatite. Key Eng. Mater. 2006, 309–311, 537–540. [Google Scholar]
- Kim, B.I.; Jeong, S.H.; Jang, S.O.; Kim, K.N.; Kwon, H.K.; Park, Y.D. Tooth whitening effect of toothpastes containing nano-hydroxyapatite. Key Eng. Mater. 2006, 309–311, 541–544. [Google Scholar]
- Kim, M.Y.; Kwon, H.K.; Choi, C.H.; Kim, B.I. Combined effects of nano-hydroxyapatite and NaF on remineralization of early caries lesion. Key Eng. Mater. 2007, 330–332, 1347–1350. [Google Scholar]
- Lee, H.J.; Min, J.H.; Choi, C.H.; Kwon, H.G.; Kim, B.I. Remineralization potential of sports drink containing nano-sized hydroxyapatite. Key Eng. Mater. 2007, 330–332, 275–278. [Google Scholar]
- Hong, Y.W.; Kim, J.H.; Lee, B.H.; Lee, Y.K.; Choi, B.J.; Lee, J.H.; Choi, H.J. The effect of nano-sized β-tricalcium phosphate on remineralization in glass ionomer dental luting cement. Key Eng. Mater. 2008, 361–363, 861–864. [Google Scholar]
- Li, L.; Pan, H.H.; Tao, J.H.; Xu, X.R.; Mao, C.Y.; Gu, X.H.; Tang, R.K. Repair of enamel by using hydroxyapatite nanoparticles as the building blocks. J. Mater. Chem. 2008, 18, 4079–4084. [Google Scholar]
- Meng, X.; Lv, K.; Zhang, J.; Qu, D. Caries inhibitory activity of the nano-HA in vitro. Key Eng. Mater. 2007, 330–332, 251–254. [Google Scholar]
- Li, B.G.; Wang, J.P.; Zhao, Z.Y.; Sui, Y.F.; Zhang, Y.X. Mineralizing of nano-hydroxyapatite powders on artificial caries. Rare Metal. Mat. Eng. 2007, 36, 128–130. [Google Scholar]
- Borum, L.; Wilson, O.C. Surface modification of hydroxyapatite. Part II. Silica. Biomaterials 2003, 24, 3681–3688. [Google Scholar]
- Lee, H.J.; Kim, S.E.; Choi, H.W.; Kim, C.W.; Kim, K.J.; Lee, S.C. The effect of surface-modified nano-hydroxyapatite on biocompatibility of poly(ε-caprolactone)/hydroxyapatite nanocomposites. Eur. Polym. J. 2007, 43, 1602–1608. [Google Scholar]
- Wilson, O.C.; Hull, J.R. Surface modification of nanophase hydroxyapatite with chitosan. Mater. Sci. Eng. C 2008, 28, 434–437. [Google Scholar]
- Liao, J.G.; Wang, X.J.; Zuo, Y.; Zhang, L.; Wen, J.Q.; Li, Y.B. Surface modification of nano-hydroxyapatite with silane agent. J. Inorg. Mater. 2008, 23, 145–149. [Google Scholar]
- Fu, H.; Hu, Y.; McNelis, T.; Hollinger, J.O. A calcium phosphate-based gene delivery system. J. Biomed. Mater. Res. A 2005, 74A, 40–48. [Google Scholar]
- Liu, T.Y.; Chen, S.Y.; Liu, D.M.; Liou, S.C. On the study of BSA-loaded calcium-deficient hydroxyapatite nano-carriers for controlled drug delivery. J. Control. Release 2005, 107, 112–121. [Google Scholar]
- Barroug, A.; Kuhn, L.T.; Gerstenfeld, L.C.; Glimcher, M.J. Interactions of cisplatin with calcium phosphate nanoparticles: In vitro controlled adsorption and release. J. Orthop. Res. 2004, 22, 703–708. [Google Scholar]
- Cheng, X.G.; Kuhn, L.T. Chemotherapy drug delivery from calcium phosphate nanoparticles. Int. J. Nanomed. 2007, 2, 667–674. [Google Scholar]
- Maitra, A. Calcium phosphate nanoparticles: Second-generation nonviral vectors in gene therapy. Expert Rev. Mol. Diagn. 2005, 5, 893–905. [Google Scholar]
- Yang, X.C.; Walboomers, X.F.; van den Dolder, J.; Yang, F.; Bian, Z.; Fan, M.W.; Jansen, J.A. Non-viral bone morphogenetic protein 2 transfection of rat dental pulp stem cells using calcium phosphate nanoparticles as carriers. Tissue Eng. A 2008, 14, 71–81. [Google Scholar]
- Bauer, I.W.; Li, S.P.; Han, Y.C.; Yuan, L.; Yin, M.Z. Internalization of hydroxyapatite nanoparticles in liver cancer cells. J. Mater. Sci. Mater. Med. 2008, 19, 1091–1095. [Google Scholar]
- Altinoǧlu, E.I.; Adair, J.H. Calcium phosphate nanocomposite particles: A safer and more effective alternative to conventional chemotherapy? Future Oncol. 2009, 5, 279–281. [Google Scholar]
- Joyappa, D.H.; Kumar, C.A.; Banumathi, N.; Reddy, G.R.; Suryanarayana, V.V.S. Calcium phosphate nanoparticle prepared with foot and mouth disease virus P1-3CD gene construct protects mice and guinea pigs against the challenge virus. Veter. Microbiol. 2009, 139, 58–66. [Google Scholar]
- Dreesen, I.A.J.; Lüchinger, N.A.; Stark, W.J.; Fussenegger, M. Tricalcium phosphate nanoparticles enable rapid purification, increase transduction kinetics, and modify the tropism of mammalian viruses. Biotechnol. Bioengin. 2009, 102, 1197–1208. [Google Scholar]
- Chu, T.C.; He, Q.; Potter, D.E. Biodegradable calcium phosphate nanoparticlesas a new vehicle for delivery of a potential ocular hypotensive agent. J. Ocular Pharmacol. Therapeutics 2002, 18, 507–514. [Google Scholar]
- Paul, W.; Sharma, C.P. Porous hydroxyapatite nanoparticles for intestinal delivery of insulin. Trends Biomater. Artif. Organs 2001, 14, 37–38. [Google Scholar]
- Victor, S.P.; Kumar, T.S.S. Tailoring calcium-deficient hydroxyapatite nanocarriers for enhanced release of antibiotics. J. Biomed. Nanotechnol. 2008, 4, 203–209. [Google Scholar]
- Kilian, O.; Alt, V.; Heiss, C.; Jonuleit, T.; Dingeldein, E.; Flesch, I.; Fidorra, U.; Wenisch, S.; Schnettler, R. New blood vessel formation and expression of VEGF receptors after implantation of platelet growth factor-enriched biodegradable nanocrystalline hydroxyapatite. Growth Factors 2005, 23, 125–133. [Google Scholar]
- Jordan, M.; Schallhorn, A.; Wurm, F.M. Transfecting mammalian cells: Optimization of critical parameters affecting calcium-phosphate precipitate formation. Nucleic Acids Res. 1996, 24, 596–601. [Google Scholar]
- Sokolova, V.V.; Epple, M. Inorganic nanoparticles as carriers of nucleic acids into cells. Angew. Chem. Int. Ed. 2008, 47, 1382–1395. [Google Scholar]
- Liu, T.; Tang, A.; Zhang, G.Y.; Chen, Y.X.; Zhang, J.Y.; Peng, S.S.; Cai, Z.M. Calcium phosphate nanoparticles as a novel nonviral vector for efficient transfection of DNA in cancer gene therapy. Cancer Biother. Radiopharm. 2005, 20, 141–149. [Google Scholar]
- Czupryna, J.; Tsourkas, A. Suicide gene delivery by calcium phosphate nanoparticles. A novel method of targeted therapy for gastric cancer. Cancer Biol. Ther. 2006, 5, 1691–1692. [Google Scholar]
- Olton, D.; Li, J.; Wilson, M.E.; Rogers, T.; Close, J.; Huang, L.; Kumta, P.N.; Sfeir, C. Nanostructured calcium phosphates (NanoCaPs) for non-viral gene delivery: Influence of the synthesis parameters on transfection efficiency. Biomaterials 2007, 28, 1267–1279. [Google Scholar]
- Bisht, S.; Bhakta, G.; Mitra, S.; Maitra, A. pDNA loaded calcium phosphate nanoparticles: Highly efficient non-viral vector for gene delivery. Int. J. Pharm. 2005, 288, 157–168. [Google Scholar]
- Chowdhury, E.H.; Akaike, T. A bio-recognition device developed onto nano-crystals of carbonate apatite for cell-targeted gene delivery. Biotechnol. Bioeng. 2005, 90, 414–421. [Google Scholar]
- Bisht, S.; Chattopadhyay, D.; Maitra, A. Intraperitoneal administration of calcium phosphate nanoparticles encapsulating pSVβgal elicits immune response to encoded protein. J. Biomed. Nanotechnol. 2006, 2, 229–238. [Google Scholar]
- Zhu, S.H.; Huang, B.Y.; Zhou, K.C.; Huang, S.P.; Liu, F.; Li, Y.M.; Xue, Z.G.; Long, Z.G. Hydroxyapatite nanoparticles as a novel gene carrier. J. Nanopart. Res. 2004, 6, 307–311. [Google Scholar]
- Chowdhury, E.H.; Kutsuzawa, K.; Akaike, T. Designing smart nano-apatite composites: The emerging era of non-viral gene delivery. Gene Ther. Mol. Biol. 2005, 9, 301–316. [Google Scholar]
- Chowdhury, E.H.; Maruyama, A.; Kano, A.; Nagaoka, M.; Kotaka, M.; Hirose, S.; Kunou, M.; Akaike, T. pH-sensing nano-crystals of carbonate apatite: Effects on intracellular delivery and release of DNA for efficient expression into mammalian cells. Gene 2006, 376, 87–94. [Google Scholar]
- Chowdhury, E.H. pH-sensitive nano-crystals of carbonate apatite for smart and cell-specific transgene delivery. Expert Opin. Drug Deliv. 2007, 4, 193–196. [Google Scholar]
- Chowdhury, E.H.; Akaike, T. High performance DNA nano-carriers of carbonate apatite: Multiple factors in regulation of particle synthesis and transfection efficiency. Int. J. Nanomed. 2007, 2, 101–106. [Google Scholar]
- Pedraza, C.E.; Bassett, D.C.; McKee, M.D.; Nelea, V.; Gbureck, U.; Barralet, J.E. The importance of particle size and DNA condensation salt for calcium phosphate nanoparticle transfection. Biomaterials 2008, 29, 3384–3392. [Google Scholar]
- Welzel, T.; Radtke, I.; Meyer-Zaika, W.; Heumann, R.; Epple, M. Transfection of cells with custom-made calcium phosphate nanoparticles coated with DNA. J. Mater. Chem. 2004, 14, 2213–2217. [Google Scholar]
- Sokolova, V.V.; Radtke, I.; Heumann, R.; Epple, M. Effective transfection of cells with multi-shell calcium phosphate-DNA nanoparticles. Biomaterials 2006, 27, 3147–3153. [Google Scholar]
- Sokolova, V.V.; Kovtun, A.; Heumann, R.; Epple, M. Tracking the pathway of calcium phosphate/DNA nanoparticles during cell transfection by incorporation of red-fluorescing tetramethylrhodamine isothiocyanate-bovine serum albumin into these nanoparticles. J. Biol. Inorg. Chem. 2007, 12, 174–179. [Google Scholar]
- Sokolova, V.V.; Kovtun, A.; Prymak, O.; Meyer-Zaika, W.; Kubareva, E.A.; Romanova, E.A.; Oretskaya, T.S.; Heumann, R.; Epple, M. Functionalisation of calcium phosphate nanoparticles by oligonucleotides and their application for gene silencing. J. Mater. Chem. 2007, 17, 721–727. [Google Scholar]
- Neumann, S.; Kovtun, A.; Dietzel, I.D.; Epple, M.; Heumann, R. The use of size-defined DNA-functionalized calcium phosphate nanoparticles to minimise intracellular calcium disturbance during transfection. Biomaterials 2009, 30, 6794–6802. [Google Scholar]
- Kovtun, A.; Heumann, R.; Epple, M. Calcium phosphate nanoparticles for the transfection of cells. Bio-Med. Mater. Eng. 2009, 19, 241–247. [Google Scholar]
- Roy, I.; Mitra, S.; Maitra, A.; Mozumdar, S. Calcium phosphate nanoparticles as novel non-viral vectors for targeted gene delivery. Int. J. Pharm. 2003, 250, 25–33. [Google Scholar]
- Kakizawa, Y.; Kataoka, K. Block copolymer self-assembly into monodispersive nanoparticles with hybrid core of antisense DNA and calcium phosphate. Langmuir 2002, 18, 4539–4543. [Google Scholar]
- He, Q.; Mitchell, A.R.; Johnson, S.L.; Wagner-Bartak, C.; Morcol, T.; Bell, S.J.D. Calcium phosphate nanoparticle adjuvant. Clin. Diagn. Lab. Immunol. 2000, 7, 899–903. [Google Scholar]
- He, Q.; Mitchell, A.R.; Morcol, T.; Bell, S.J.D. Calcium phosphate nanoparticles induce mucosal immunity and protection against herpes simplex virus type 2. Clin. Diagn. Lab. Immunol. 2002, 9, 1021–1024. [Google Scholar]
- Liu, Z.S.; Tang, S.L.; Ai, Z.L. Effects of hydroxyapatite nanoparticles on proliferation and apoptosis of human hepatoma BEL-7402 cells. World J. Gastroenterol. 2003, 9, 1968–1971. [Google Scholar]
- Sun, J.; Ding, T. P53 reaction to apoptosis induced by hydroxyapatite nanoparticles in rat macrophages. J. Biomed. Mater. Res. A 2009, 88A, 673–679. [Google Scholar]
- Allen, T.M.; Cullis, P.R. Drug delivery systems: Entering the mainstream. Science 2004, 303, 1818–1822. [Google Scholar]
- Schmidt, H.T.; Kroczynski, M.; Maddox, J.; Chen, Y.; Josephs, R.; Ostafin, A.E.J. Antibody-conjugated soybean oil-filled calcium phosphate nanoshells for targeted delivery of hydrophobic molecules. Microencapsulation 2006, 23, 769–781. [Google Scholar]
- Ferraz, M.P.; Mateus, A.Y.; Sousa, J.C.; Monteiro, F.J. Nanohydroxyapatite microspheres as delivery system for antibiotics: Release kinetics, antimicrobial activity, and interaction with osteoblasts. J. Biomed. Mater. Res. A 2007, 81A, 994–1004. [Google Scholar]
- Cai, Y.; Pan, H.; Xu, X.; Hu, Q.; Li, L.; Tang, R. Ultrasonic controlled morphology transformation of hollow calcium phosphate nanospheres: A smart and biocompatible drug release system. Chem. Mater. 2007, 19, 3081–3083. [Google Scholar]
- Zhou, W.Y.; Wang, M.; Cheung, W.L.; Guo, B.C.; Jia, D.M. Synthesis of carbonated hydroxyapatite nanospheres through nanoemulsion. J. Mater. Sci. Mater. Med. 2008, 19, 103–110. [Google Scholar]
- Wingert, P.A.; Mizukami, H.; Ostafin, A.E. Enhanced chemiluminescent resonance energy transfer in hollow calcium phosphate nanoreactors and the detection of hydrogen peroxide. Nanotechnology 2007, 18, 295707:1–295707:7. [Google Scholar]
- Yih, T.C.; Al-Fandi, M. Engineered nanoparticles as precise drug delivery systems. J. Cell. Biochem. 2006, 97, 1184–1190. [Google Scholar]
- Celotti, G.; Tampieri, A.; Sprio, S.; Landi, E.; Bertinetti, L.; Martra, G.; Ducati, C. Crystallinity in apatites: How can a truly disordered fraction be distinguished from nanosize crystalline domains? J. Mater. Sci. Mater. Med. 2006, 17, 1079–1087. [Google Scholar]
- Christenson, E.M.; Anseth, K.S.; van den Beucken, J.J.J.P.; Chan, C.K.; Ercan, B.; Jansen, J.A.; Laurencin, C.T.; Li, W.J.; Murugan, R.; Nair, L.S.; Ramakrishna, S.; Tuan, R.S.; Webster, T.J.; Mikos, A.G. Nanobiomaterial applications in orthopedics. J. Orthop. Res. 2007, 25, 11–22. [Google Scholar]
- Schmidt, S.M.; Moran, K.A.; Kent, A.M.T.; Slosar, J.L.; Webber, M.J.; McCready, M.J.; Deering, C.; Veranth, J.M.; Ostafin, A. Uptake of calcium phosphate nanoshells by osteoblasts and their effect on growth and differentiation. J. Biomed. Mater. Res. A 2008, 87A, 418–428. [Google Scholar]
- Powell, M.C.; Kanarek, M.S. Nanomaterials health effects—Part 1: Background and current knowledge. Wisconsin Med. J. 2006, 105, 16–20. [Google Scholar]
- Powell, M.C.; Kanarek, M.S. Nanomaterials health effects—Part 2: Uncertainties and recommendations for the future. Wisconsin Med. J. 2006, 105, 18–23. [Google Scholar]
- Motskin, M.; Wright, D.M.; Muller, K.; Kyle, N.; Gard, T.G.; Porter, A.E.; Skepper, J.N. Hydroxyapatite nano and microparticles: Correlation of particle properties with cytotoxicity and biostability. Biomaterials 2009, 30, 3307–3317. [Google Scholar]
- Bionanotechnologies are modeled after biological substances and structures, or combine nanomaterials with biological substances. They include materials such as biochips, drug release systems, nanofibers, hybrid nanobiodevices, molecular electronics and biomimetics (synthetic genes, proteins and viruses) [627]
- Moghimi, S.J.; Hunter, A.C.; Murray, J.C. Nanomedicine: Current status and future prospects. FASEB J. 2005, 19, 311–330. [Google Scholar]
- Xu, H.H.K.; Weir, M.D.; Simon, C.G. Injectable and strong nano-apatite scaffolds for cell/growth factor delivery and bone regeneration. Dental Mater. 2008, 24, 1212–1222. [Google Scholar]
- Watari, F.; Abe, S.; Tamura, K.; Uo, M.; Yokoyama, A.; Totsuka, Y. Internal diffusion of micro/nanoparticles inside body. Key Eng. Mater. 2008, 361–363, 95–98. [Google Scholar]
- Oberdorster, G.; Oberdorster, E.; Oberdorster, J. Nanotoxicology: An emerging discipline evolving from studies of ultrafine particles. Environ. Health Perspect. 2005, 113, 823–839. [Google Scholar]
- Nel, A.; Xia, T.; Mädler, L.; Li, N. Toxic potential of materials at the nanolevel. Science 2006, 311, 622–627. [Google Scholar]
- Jahnen-Dechent, W.; Simon, U. Function follows form: Shape complementarity and nanoparticle toxicity. Nanomedicine 2008, 3, 601–603. [Google Scholar]
- Singh, N.; Manshian, B.; Jenkins, G.J.S.; Griffiths, S.M.; Williams, P.M.; Maffeis, T.G.G.; Wright, C.J.; Doak, S.H. NanoGenotoxicology: The DNA damaging potential of engineered nanomaterials. Biomaterials 2009, 30, 3891–3914. [Google Scholar]
- Dhawan, A.; Sharma, V.; Parmar, D. Nanomaterials: A challenge for toxicologists. Nanotoxicology 2009, 3, 1–9. [Google Scholar]
- Dwivedi, P.D.; Misra, A.; Shanker, R.; Das, M. Are nanomaterials a threat to the immune system? Nanotoxicology 2009, 3, 19–26. [Google Scholar]
© 2009 by the authors; licensee Molecular Diversity Preservation International, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Dorozhkin, S.V. Nanodimensional and Nanocrystalline Apatites and Other Calcium Orthophosphates in Biomedical Engineering, Biology and Medicine. Materials 2009, 2, 1975-2045. https://doi.org/10.3390/ma2041975
Dorozhkin SV. Nanodimensional and Nanocrystalline Apatites and Other Calcium Orthophosphates in Biomedical Engineering, Biology and Medicine. Materials. 2009; 2(4):1975-2045. https://doi.org/10.3390/ma2041975
Chicago/Turabian StyleDorozhkin, Sergey V. 2009. "Nanodimensional and Nanocrystalline Apatites and Other Calcium Orthophosphates in Biomedical Engineering, Biology and Medicine" Materials 2, no. 4: 1975-2045. https://doi.org/10.3390/ma2041975
APA StyleDorozhkin, S. V. (2009). Nanodimensional and Nanocrystalline Apatites and Other Calcium Orthophosphates in Biomedical Engineering, Biology and Medicine. Materials, 2(4), 1975-2045. https://doi.org/10.3390/ma2041975




