Abstract
Background: For decades, regenerative medicine and dentistry have been improved with new therapies and innovative clinical protocols. The aim of the present investigation was to evaluate through a critical review the recent innovations in the field of bone regeneration with a focus on the healing potentials and clinical protocols of bone substitutes combined with engineered constructs, growth factors and photobiomodulation applications. Methods: A Boolean systematic search was conducted by PubMed/Medline, PubMed/Central, Web of Science and Google scholar databases according to the PRISMA guidelines. Results: After the initial screening, a total of 304 papers were considered eligible for the qualitative synthesis. The articles included were categorized according to the main topics: alloplastic bone substitutes, autologous teeth derived substitutes, xenografts, platelet-derived concentrates, laser therapy, microbiota and bone metabolism and mesenchymal cells construct. Conclusions: The effectiveness of the present investigation showed that the use of biocompatible and bio-resorbable bone substitutes are related to the high-predictability of the bone regeneration protocols, while the oral microbiota and systemic health of the patient produce a clinical advantage for the long-term success of the regeneration procedures and implant-supported restorations. The use of growth factors is able to reduce the co-morbidity of the regenerative procedure ameliorating the post-operative healing phase. The LLLT is an adjuvant protocol to improve the soft and hard tissues response for bone regeneration treatment protocols.
1. Introduction
In recent years, the bone regeneration procedure for implant-supported rehabilitations gained increased predictability due to innovative biomaterials, new generation bone grafts and substitutes and novel adjuvant therapies able to increase the osseointegration, the new bone formation and substitution, promote the bone remodeling and decrease the post-operative co-mobility and healing period. In fact, the objective of bone regeneration protocols is determined by the long-term predictability and survival rate of the implant rehabilitation and the control of the patient’s general and local risks factors [1,2,3,4,5,6,7,8,9,10,11]. In terms of a general clinical evaluation of the patient, the presence of systemic disorders, neoplasms, chemotherapy and radiotherapies, the health of the gastrointestinal tract, systemic pH balance and the local release of metallic ions related to implant positioning could determine a considerable influence on the immune/metabolic system [12,13]. Moreover, the autologous tooth-derived graft materialinistration of drugs acting on vascularization and bone metabolism and the evidence of chronic infections could determine an increased risk of implant failure [14,15,16]. A recent review that evaluated a total of 120 clinical and radiographical prospective studies stated that the implant survival rate was 85% after 1 year and 78% after 10 years with a success rate of 81%. Age-related degenerative and periodontal diseases were visibly connected to a general degenerative metabolic state in conjunction with systemic dysbiosis involving the oral cavity and the intestinal compartment. These conditions represent the cause of an increased degree of loss and wear of both implants and prostheses. Moreover, the peri-implantitis could be found in patients with low standards of both oral hygiene and a high degree of dysbiosis with a high bacterial load and chronic inflammation, even in patients with a regular follow-up schedule. Dysbiosis has been associated with a pseudo-allergic state with alterations of immune responses and genes polymorphisms (SNPs) that regulate the expression of immuno-modulating and pro-inflammatory responses: IL-10, IL-6 TNF, IFN IL-1 and VDR (vitamin D metabolism). These alterations have been mainly observed in patients with implant rehabilitations with at least three or more units and also in patients with metabolic, cardiovascular, renal deficiency and diabetes comorbidities [17,18,19,20]. The need to develop new, more efficient materials and techniques for functional and aesthetic rehabilitations remains a priority for researchers in the dental field [21,22,23,24,25,26,27]. A biomaterial that is used as a bone substitute should possess certain qualitative criteria: biocompatibility, which represents the capability of providing osseointegration without causing inflammatory reactions [28,29,30,31,32], osteoconductivity, the natural properties that allow cell activity, reproduction and amplification, and at last osteoinductive properties, or to be capable of triggering the bio-chemical and modulating processes, so stem cells can differentiate into osteoblasts, osteoclasts and osteocytes and induce osteogenesis, which is related to the formation of a new bone matrix [1,33,34,35]. Moreover, osteoinductive biomaterials should be able to recruit progenitor cells (MCS) to the grafted site, induce the formation of osteoblasts by differentiating progenitor cells (MCS) in mature cells and eventually regenerate ectopic bone where there is no extraskeletal structure [36]. The prevalence of implant failure and wear has been related to the presence of inflammation and infections as a result of oral diseases, such as peri-implant and oral flora disorders/dysbiosis [37,38,39,40,41,42,43,44,45,46,47]. The biophysical and biochemical properties of biomaterials could influence the cellular responses, including the macro-topography, pore geometry and stiffness, surface chemistry, rate of degradation and presence of biomolecules, influence proliferation and differentiation to eventually give tissue regeneration [48,49]. Healing of bone tissue occurs as a result of coupling activity between osteoclasts and osteoblasts and stem cells with immune cells. The inflammatory response of the host body is important for activating biochemical signals that bring the immune cells to the implant region, although chronic inflammation may be the cause of the implant failure [50]. The materials used in bone regeneration are divided into four main groups according to the origin of the biomaterials: alloplastic grafts, autologous grafts, xenografts and allografts [51].
These bone substitutes are biocompatible and bioabsorbable, able to induce the formation of new bone and maintain the bone volume. However, the biocompatibility and the bioabsorbable/preservation ratio of bone volume need to be improved, through research, to obtain increasingly predictable and favorable results for rapid bone regeneration [52]. The aim of the present investigation was to evaluate through a critical systematic overview of the recent innovations in the field of bone regeneration of alloplastic bone substitutes, peripheral mesenchymal cells constructs, growth factors and photobiomodulation applications. The aim of the present review was to perform a systematic review of the recent innovations in the field of bone regeneration with a focus on the healing potentials and clinical protocols of bone substitutes combined with engineered constructs, growth factors and photobiomodulation applications.
2. Materials and Methods
2.1. Article Search Methodology
The present systematic search was conducted by PubMed/Medline, PubMed/Central, Web of Science and Google scholar according to the PRISMA guidelines [53]. The article search was performed according to an ad hoc combination of Boolean operators (AND, OR) with the keywords on the topics of the present review. The keyword searchline is presented in Table 1.

Table 1.
Summary of the electronic databases Boolean search strategy (PubMed/Medline, PubMed/Central, Web of Science; Google scholar). No limitation about the publication years has been considered.
2.2. Inclusion Criteria
For the present systematic search, the inclusion criteria were in vivo articles on human and animal studies in the field of cranio-maxillofacial bone regeneration that highlighted the characteristics of engineered bone constructs and combinations of growth factors and photobiomodulation applications.
2.3. Exclusion Criteria
The exclusion criteria considered for the descriptive analysis were, letter to the editor, articles written in non-English languages.
2.4. Paper Selection Process
The eligibility of the manuscripts for the descriptive review was performed independently by two reviewers evaluating the manuscript title and abstract. The full text was obtained and evaluated in this first stage if the abstract was unavailable. The papers not in line with the inclusion criteria were excluded from the analysis. The full text of the included manuscripts was collected and evaluated. The excluded articles were categorized according to the reasons for exclusion.
3. Results and Discussion
General Parameters
A total of 1448 articles were identified after the initial screening and a total of 304 papers were included for the qualitative synthesis (Figure 1).
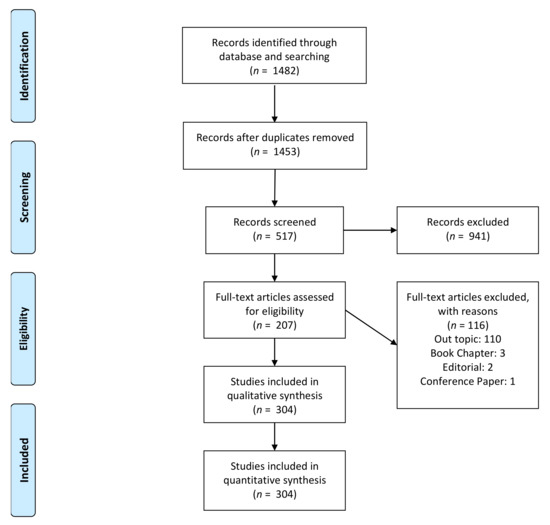
Figure 1.
PRISMA flowchart of the included articles.
4. Bone Substitutes and Graft
4.1. Alloplastic Grafts
Alloplastic bone grafts are synthetic biomaterials with no risks of antigenic reactions or transmission of various diseases. Many materials have been proposed as bone grafts containing calcium phosphate derivates with high biocompatibility. Calcium phosphate is similar to the inorganic components of human bones [54]. Hydroxyapatite (HA) Ca10(PO4)6(OH)2 is present in the human body, bones and teeth as an inorganic mineral, but in addition to the inorganic matrix; a consistent component of the human bone is the organic part that consists of type 1 proteins and collagen [55]. In a physiological environment, HA is not soluble; therefore, the formation of new bone occurs only through the reabsorption of these materials. The osteoclast activity is not optimal against the biphasic calcium phosphate (BCP) in 75% HA and 25% β-TCP. The solubility also influences the osteoclastic resorption pattern. The β-TCP has the highest solubility and HA the lowest, so the osteoclasts’ reabsorption of the biomaterial proceeded in the right proportion to the solubility of the substances, but this is not entirely accurate [56]. Zwingenberger et al. reported similarly to Yamada et al. that HA with HA/β-TCP 75/25% mix is not completely reabsorbed, but β-TCP has a higher solubility than HA/β-TPC 25/75% but HA/β-TPC 25/75% had better osteoclastic resorption [56,57]. Ortiz-Puigpelat et al. reported that HA/TCP 50% ratio is more appropriate in bone regeneration for the percentage of residual material and new newly formed bone after 12–24 weeks [58]. The hydroxyapatite (HA) and calcium tri-phosphate (TPC) are characterized by high compressive strength (statical forces) but are very fragile due to dynamic forces, so this feature limits their use in large bone defects [59]. In operative clinical practice, these defects are correlated to various causes, such as bone tumors, severe trauma or drugs abuse with an alteration in bone metabolism. In a pure form, HA and β-TCP have been widely used as biodegradable coatings. HA and β-TCP also prevent the formation of fibrotic tissue around the implants derived by the body’s immune response. This fibrotic tissue can also lead to implant failure [60,61]. The porosity of calcium phosphates is one of the factors that induce their poor initial mechanical property, but the porosity is able to influence the early fibro-vascularization of the graft and replace it with new bone [62]. Moreover, the scaffold pore size is able to affect the progression of osteogenesis. Small pores promote hypoxic conditions and induce osteochondral formation before osteogenesis occurs. On the other hand, larger scaffold pores allow vascularization, directly evoking the onset of osteogenesis [63,64]. The optimal pore diameter of bone substitutes should be between 0.2 and 0.5 mm [65,66], while Ghayer and Weber reported an optimal pore range between 0.7 and 1.2 mm with excellent results in healing cranial defects [67]. Another factor of these biomaterials for the new bone formation is the presence of micropores [68], while a submicron micropore structure <10 µm has been reported to accelerate the formation of new bone, and the quantity of these micropores improves the results [69]. Many studies are focused on compound forms or biphasic forms, thus improving the mechanical properties, solubility and integration of these biomaterials [59,60,70,71,72,73]. De Tullio et al. used bone replacement materials, such as calcium sulphate (CS) and nano-hydroxyapatite (NHA), in a comparative study to prevent a reduction in the alveolar ridge after tooth extraction [74]. After 5 months, the histomorphometric analysis showed that these biomaterials led to bone formation, but the combination of CS with NHA showed better results in the regeneration of new bone and in the number of residual graft particles [74]. Lin et al. reported on 51 patients that the HA/TCP+ collagen composite gave excellent results in preserving post-extraction alveolar bone [75]. Maji et al. in order to improve the mechanical properties, suggested gelatin-chitosan-β-TCP 30% with high porosity the GCT 30 scaffold. This scaffold has improved the mechanical properties showing high strength and compressive strength of the new bone up to 2.5 MPa, which is also the lower range of cancellous bone. The change in the percentage of β-TCP changes the absorption of proteins, and GCT 30 also has the ability to stimulate mesenchymal stem cells (MSCs) and transform them into osteoblasts, thus stimulating angiogenesis [76]. Afroze et al. proposed a different combination of HA with the addition of a fMWCNT 0.5 wt% multi-walled carbon nanotube. The study was carried out in vitro with the aim of improving the mechanical properties of HA without modifying its structure. In fact, the HA, which contains carbon, seems to have greater similarity with the inorganic phase of the bone [77]. The fMWCNT prevents the HA from decomposing into α-TCP and Ca2P2O7, and it promotes the porosity of the composite, which is essential for the growth of cells. This combination of HA with 0.5 wt% low dose fMWCNT is favorable for improving mechanical strength by approximately 317.5%, hardness by 172.4% and fracture strength by 237% [77]. This nanocomposite’s favorable application, as has been demonstrated, is when the bone will be a load-bearing support for implants [77]. Bone materials, such as β-TCP, have the ability to induce bone regeneration through the release of Ca ions [78]. Synthetic materials have high osteoconductive properties but no evidence of osteoinductivity [79]. Recently, a new synthetic biomaterial named Osopia has been suggested, in relation of its osteoinductive properties. This biomaterial is composed of the combination of HA and β-TCP to obtain medium resorption properties. The structure of the Osopia is extended in macropores with a submicronic surface. The submicronic surface structure promotes osteogenesis by regulating the transforming growth factor (β-TGF) pathway and thus inducing the differentiation of mesenchymal stem cell (MSC) [80]. The topographic/chemical characteristic of this biomaterial drives self-induction and consequently the differentiation of osteoblasts [80]. Chen et al. confirmed the possibility that a biphasic HA/TCP can induce ectopic bone in non-osseous sites and that this ability is closely related to the immune response that is caused by this material [81]. A new bio-scaffold called Compact Bio Bone Cells has recently been tested. Since this scaffold is composed of β-TCP, fibrin gel matrix and peripheral blood stem cells, it creates an imitation of the microenvironment of the bone tissue. The in vitro study showed that the Compact Bio Bone Cells had a comparable biodegradability rate to the bone regeneration rate, so at 7–12 days, cells resembling mature osteoblasts were highlighted. The presence of stem cells induces the vascularization of the region [82]. Even when stem cells are harvested from the pulp of the tooth, it is suggested to use them in bone regeneration. In combination with synthetic scaffolds, stem cells originating from the dental pulp have given excellent results in tissue neoformation in a shorter time [83]. The combination of TCP with platelet-rich plasma (PRF) has also been suggested in the case of fractures. This combination not only provides bone regeneration (resorption occurs at the same time as bone regeneration), but the presence of PRF aids in the healing of the positioning soft tissues [84].
The recent advances in reconstructive dentistry are oriented towards using bioactive glasses due to the increased potential bioactivity and biocompatibility for bone regeneration procedures [85]. Recent studies reported that the biocompatibility of these biomaterials is correlated with the silicate-derived percentage range between 45 and 52%, which represents an optimal equilibrium between the tissue tolerance and the osteogenesis capability of the graft [85,86,87,88,89]. The bioglasses-acting mechanism is produced by the local release of ions and the generation of amorphous calcium phosphates precipitates that are able to generate a local change of the pH levels and osmotic flows [90,91,92,93]. Due to the new bone formation properties, the bioglasses are able to interact with the grafting environment and modulate the activity of several osteogenetic factors, such as the alkaline phosphatase and bone morphogenetic proteins (BMP2).
4.2. Autologous Graft
The dental matrix has also been tested and used for a long time as a bone regeneration material [94,95]. After extraction, the tooth is considered a useless material and is eliminated, and for this reason, the use of this material has a low cost. The dental matrix contains HA and type 1, type 3 and type 5 collagen, and proteins are very similar to alveolar bone as they are both derived from the cells of the neural crest [55,96,97,98]. The hydroxyapatite present in the dental matrix has the same composition of HA as that present in bone, and for this reason, it is similar to the synthetic one [99]. The osteoconductive properties of tooth-derived materials are widely accepted by several authors [96,100,101]. In fact, the tooth can be considered the best natural scaffold. Comparing the dental matrix to HA/TCP, it is shown to be more biocompatible and bioactive [98,102]. Dentin is composed of inorganic material (65%) and organic matrix and water (35%). The inorganic part, HA [3Ca3 (PO4) 2Ca (OH)2], has crystals 10-times larger than those of bone (this is the biggest difference between these materials) and 300-times smaller than those of enamel [98,103]. The organic part is composed of 90% type 1 collagen and 10% non-collagenic proteins including growth factors (BMPs) and enzymes, such as alkalin and acid phosphatases and MMPs [98,103]. The presence of growth factors (GFs), as well as mesenchymal cells, is also found in the apical part of the wisdom teeth [104] and in the dental pulp in a considerable amount [105]. In 1965, Marshall R. Urist hypothesized the presence of proteins (BMP) in the bone matrix, and these proteins have the ability to induce ectopic bone [106,107]. BMPs play an important role in the differentiation of mesenchymal cells into osteoblasts [108], in addition to stimulating angiogenesis [109,110]. In 1991, Bessho et al. observed the presence of the bone morphogenic protein (BMP) in the dentin matrix [111]. Many researchers have focused on (BMPs) to evaluate the effectiveness of this low-molecular-weight glycoprotein [98,108,109,110,111,112,113,114,115]. In the BMP family, BMP-9 is considered the protein with the highest osteogenic potential. BMP-9 is capable of inducing the formation of new bone in critical defects by intervening in the differentiation of progenitor cells and in angiogenesis [110,112]. BMP-2 is also one of the strongest stimulants among growth factors. Its use has led to results comparable to those of autologous grafts in terms of bone volume and density and even reduced the risk of infection and the time of hospitalization [113]. It has been reported that bone repair could be produced by BMP-2, but this ability is dose-dependent [114], while a high dosage could give unwanted effects [115,116]. In the tooth matrix, the BMP is found in physiological quantities and therefore adequate for the patient. The discussion continues on how this material will be used—mineralized or demineralized. The tooth crushing technique is a tooth processing method that is proposed for use as an autologous bone graft. This technique was initially applied to the newly extracted wisdom tooth. The tooth was crushed with a bone mill and hammer without being made into a solution in order to retain the pulp. Six months after the surgery, radiological and clinical control showed that there was normal bone healing [117]. Other researchers also support the techniques with the tooth not transformed with acids, aiming to preserve the osteoinductive properties [118,119]. On the other hand, numerous studies evaluate the demineralized and granulated material as a bone graft. Woong et al. state that the demineralized dentin acts as a carrier for the BMP-2 contained within the dental structure, thus combining the properties of the scaffold with the cells of the BMP-2 [120]. After being treated with acids, the dentin releases Ca2+ ions, thus creating a porous graft that acts as a perfect scaffold. The porous structure will contribute not only to the circulation of proteins (BMP) but also to the positioning of the fibrovascular network, which will help osteogenesis [121]. Rijal et al. compared the mineralized tooth matrix (MDM) as a bone graft with the demineralized tooth matrix (DDM). Human teeth were treated, and the experiment was performed on rats. DDM gave positive results, allowing the formation of new bone, thus demonstrating the regenerative abilities of this autologous material. This study did not confirm the same for MDM; in fact, the mineralized tooth matrix fails to trigger the regeneration of new bone and takes longer to re-absorb. The authors express the need for a protocol for the demineralization of the tooth so that this material can maintain its osteoinductive and osteoconductive properties [121]. In a recent review of the dental graft by Gharupure and Bhatavadekar, they analyzed all the different protocols for using a tooth as a graft material and found that new bone was created around the graft material, but the dental bone graft was not fully absorbed and replaced with new bone. The amount of residual non-resorbed dental bone graft is approximately equal to that of bovine bone [122]. This study found a significant number of complications, such as the separation of the mineralized block of the scaffold in some cases, causing the loss of primary stability to the implant, lack of osseointegration in others and loss of marginal bone more than one millimeter after 5 years showed an increased risk of dehiscence. As many procedures are empirical and not really standardized, this leads the authors to conclude that a standardization is needed for the procedure of transforming the tooth into microparticles that will be used as a graft [122]. During the demineralization process, the dentinal tubules will turn into channels for the circulation and the release of proteins as they will become wider. The protocol used for the demineralization of the tooth is very important as it can also lead to the complete destruction of dentinal tubules [102]. Further, the technique uses six liquids in addition to a partially controlled demineralization. With this patent method, the disinfection of the dental matrix is allowed, giving, in the end, a graft of 0.4–0.8 mm, which is easy to handle and apply [98,123]. Minetti et al. evaluated the Tooth Transformer (TT), which performs the transformation of the tooth by also disinfecting the dental matrix. This procedure lasts 25 min and can be performed in the same session immediately after tooth avulsion. It is totally automatic, thus reducing the risk of human error. Koga et al. state that if the dental matrix is partially demineralized with particles around 500–1000 µm, it has greater regeneration potential than when it has been completely demineralized, as it preserves more growth factors that will intervene in osteogenesis [124]. Bono et al. Support the idea of using treated and demineralized teeth, confirming that the demineralization performed with TT increases the bioavailability of BMP-2. The protocol used includes six solutions that demineralize and sterilize the crushed tooth [125]. It turns out that they do not damage the microstructure of dentin and organic matrix, as has been stated in other studies [126,127], but they increase the availability of BMP-2 in the matrix [98,125]. Substances that determine too high a demineralization (substances that give a high demineralization) produce a graft material of dental origin with low osteogenic potential as they eliminate or decrease the proteins present in the tooth, including BMP-2 [98]. Bono et al. affirm that this slight demineralization of the tooth lowers (reduces) the content of Ca and P compared to the non-demineralized matrix, but at the same time, it increases the bioavailability of BMP-2 [125,128]. BMP-2 increases the activity of ALP (alkaline phosphatase), which leads to an increase in osteodifferentiation. To induce significant ALP activity, a minimum concentration of 12.5 ng/mL of BMP-2 is needed, and after treatment with TT, the concentration of BMP-2 in the dentin matrix is 22 ng/mL [98,128]. An evaluation through scanning electron microscopy has shown that the density, roughness and homogeneity of the autologous dental graft is relatively similar to that of autogenous cortical bone, with a surface containing both organic and mineralized material [129]. The technique with the autologous tooth elaborated with the Tooth Transformer has been tested in the alveolar socket preservation of the bone after the extraction of the teeth [98]. The authors state that the success of the implant after bone regeneration was 99.1%, and the time it took for bone healing to be ready for implant was four months. The demineralization and decontamination performed by the solution does not eliminate BMP-2 and collagen [130,131]. The same author continued his research by using the Tooth Transformer on sinus lift with the same technique on a demineralized and granulated tooth [98]. In this case, the implants were inserted after six months. In this study, no inflammatory reaction was observed around the graft, and the tooth material used as graft was perfectly integrated with the host tissue. Unlike other autologous grafts, the tooth matrix does not lose bone volume with the passage of months [132]. In large bone defects, there is the problem of the amount of grafting that is needed in these cases. Umebayashi et al. have suggested the use of autologous bone when the quantity of teeth is limited, which can also be mixed with other biomaterials [133]. The matrix of the autologous tooth was partially demineralized (APDDM) and used in combination with particulate cancellous and medullary bone (PCBM) in bilateral sinus lift and in anterior maxillary reconstruction. This combination showed the osteoinductive capacities of PBCM and the osteoconductivity of APDDM. The implant was performed after 3.5 months [133]. Another suggested combination was that with xenographic material (Bio-Oss), which gave positive results in bone regeneration, but compared with the dental matrix alone, this last one forms a greater amount of bone [134]. In any case, the dental matrix can be combined with other biomaterials in large bone defects, which provides very positive results [133,134,135,136]. From the physio-chemical side, the tooth can be considered a material similar to bone but with a higher mineralization. A completely demineralized or a mineralized tooth did not bring good results in bone regeneration. In fact, the decalcification serves to make the dentin more accessible to collagenolytic enzymes and also for the fact that demineralized surfaces are the most adherent for osteoblasts [98]. The use of Tooth Transformer is highly manageable and is totally automatic, with no risk of human error. The use of this machine offers shredding at low speed that allows for homogenous particles and more material to use. The protocol used here is the one that offers a ratio between Ca and P (1.70) that is closer to the natural ratio found in bone (1.67) and, moreover, preserves proteins in the dental matrix (Figure 2) [98].
Figure 2.
Synthesis of the biomaterials for bone regeneration.
4.3. Xenografts Bone Substitutes
Xenotransplantation or bone derived from another species has been applied for many years as regenerative bone material. Their component is hydroxyapatite. Bone hydroxyapatite (BHA) is obtained naturally and has a lower cost than synthetic hydroxyapatite. The presence of ions, such as Na+ and CO3, seems to influence the molecular structure with lower porosity and thicker microstructure [137]. It has been shown that for bovine bone, the best results are obtained when it is used in particles with a diameter of 1.0–2.0 mm. These dimensions provide the best results in preserving bone volume compared to micro-sized particles [138]. The same result was accepted by Kon et al. for autologous bone, where larger particles (1.0–2.0 mm) give the best result in the formation of new bone and small particles tend to be absorbed more quickly [139]. Bovine-derived xenograft is one such material, which has been recognized as biocompatible with other animal and human organisms [140]. This material acts as a scaffold and promotes osteoblastic activity [141]. The microporous structure of bovine bone, which is considered similar to that of cancellous bone, allows this material to have osteoconductive properties [142]. The researchers demonstrated bone healing when they examined the bovine bone, and it was found that the bone is compact and mineralized and surrounds the bovine graft particles. The colonization of capillaries and newly formed cells is appreciated in Haversian canals [140,141,142]. Piattelli et al. used an inorganic bovine bone Bio-Oss for a maxillary sinus lift. After six months, the histomorphometric analysis showed that 30% of the samples selected for biopsy that were removed with a 4 mm drill under saline irrigation to a depth of 10 mm and examined by microscopy still contained Bio-Oss particles, but these particles were also observed after four years. The authors’ autologous tooth-derived graft material behaves like a scaffold an implant but has a very slow resorption [143]. However, other authors think that the slow reabsorption of this material serves as a source of mineralization [144,145]. In 2005, Sanchez et al. tested a combination of platelet-rich plasma (PRP) on dogs. In this study, they stated that the use of PRP in these animals did not give significant changes in bone regeneration [146]. More recent research has continued to combine Bio-Oss with platelet-rich fibrin PRF [147,148,149]. This combination is used in sinus lift, and the implant site was ready in 106 days, less than four months after surgery. The authors declare 100% success in bone regeneration following the Choukroun protocol [147]. The PRF has a dense and strong fibrin matrix, which is a great advantage over PRP. The PRP has also failed in other studies [150,151,152], but it should also be mentioned that the denomination of blood-derived products has often been confusing, but lately, everything has already been clarified, and their classification is made based on architecture of fibrin and cellular content [147,150,151,153,154,155,156,157,158,159,160]. Xenografts with CGF Growth Factor Concentrate is another suggested method. The authors used the Silfradent device to allow the CGF to penetrate the bone graft (to better allow fusion). Their technique in the augmentation of atrophic ridges gave excellent results; in just four months, mineralized bone was evident and ready for the implant procedure [161,162]. Continuing to try and improve osteoconductive properties, another study suggests combining Bio-Oss with BMP-2. To increase the building activity of this protein, rhBMP/Bio-Oss was coated with heparinized dopamine. The result showed that new bone formation began four weeks after surgery, while in week eight, there was a huge difference in the rate of bone formation between this study group and the group that was only used in the Bio-Oss graft [163]. Another combination tested is that between bovine bone Bio-Oss and autologous bone, but these two materials have differences in the time of absorption and have often not given good results in bone regeneration [164]. As xenografts are available in significant quantities, there are many studies focusing on these materials. A recent review on the use of bovine bone highlighted in the conclusions that 58% of cases failed in osseointegration, while 83% of these continued to have pain even after a long time. The main factor causing this complication is the body’s immune response to this material [165]. Therefore, for xenografts, the main antigen is the epitop alpha Gal, and to inhibit this antigen, the xenograft should be decellularized, and only then can it be used as a scaffold. However, the risk of an antigenic reaction will always be there, especially for bovine bone [165]. A new combination of bovine bone with type 1 atelocollagen has been recommended to minimize the antigenic reaction. Indeed, this combination is regarded as a new generation of xenografts. Atelocollagen has a low risk of antigenic reaction and inhibits bacterial activity. Additionally, unlike most xenografts, this combination of bovine bone graft with atelocollagen is totally resorbable [80]. Despite the treatment that xenograft undergoes, in 2007, Terry et al. highlighted the first case of bovine spongiform H-type encephalopathy related to bone reconstruction with bovine bone [166]. This means that the risk of transmitting diseases from one species to another exists.
5. Platelet Derivates and Growth Factors
From the peripheral blood, a platelet-rich autologous concentrate is collected, which is considered a “good healer” obtained in a non-invasive and rapid way [167], and when combined with other biomaterials, gives excellent results [168,169]. The first piastin concentrate has been called PRP and normally contains 0.5 × 1011 platelets for each unit. PRP does not have good mechanical properties. Before being activated, PRP is in liquid form [170]. This platelet concentrate releases growth factors and cytokines in a very short time and then reabsorbs in about 12–14 days. PRP has given the best results in combination with an autogenous graft compared to other materials used in bone regeneration [171]. However, the PRP gel in periodontology and dentoalveolar surgery has lost its use with the discovery of PRF, which has a lower cost and is easier to use [155]. The second-generation PRF encapsulates leukocytes, cytokines and, above all, growth factors in an autologous fibrin matrix. This PRF has been produced in the absence of anticoagulants, and for this reason, it is considered 100% autologous material that facilitates tissue regeneration by eliminating the transmission of diseases through the blood [172]. The fibrin matrix will act as a 3D scaffold in which cells and proteins will be captured. The cellular components of PRF are leukocytes, platelets, macrophages, granulocytes, neutrophils and erythrocytes. These cells play a fundamental role; in fact, platelets intervened in the first phase of healing in hemostasis with leukocytes, macrophages, granulocytes and neutrophils and participated in the anti-inflammatory phase. Platelets and macrophages release a large number of growth factors within 7–14 days, including platelet-derived growth factor (PDGF), transforming growth factor-β1 (TGF-β1), insulin-like growth factor (IGF) and vascular endothelial growth factor (VEGF) [150,151,155,156,157]. These bioactive molecules are able to further promote cell proliferation and bone remodeling [173,174]. The architecture of the fibrin matrix influences the trapping/release of GFs [156]. The cellular content and the fibrin matrix differentiate between the materials derived from the platelets because these are the elements that are involved in the regeneration and healing of the tissues. Therefore, it is necessary to recommend the use of this method of peripheral blood derivatives PRF associated with biomaterials [157]. When the use of PRF is included, the results indicate that osseointegration and bone regeneration takes place in a short time—only 106 days [147]. Currently, L-PRF as a component of the large PRF family has the potential to biostimulate bone regeneration and accelerate osseointegration [175]. The PRF does not induce new bone formation directly, but what all authors agree on is that PRF significantly improves early vascularization in bone grafts [147,150,151,155,156,157,176]. The PRF through the angiogenesis promoter (VEGF) induces the vascularization of the area and decreases the inflammatory reaction around the graft since it contains anti-inflammatory cytokines (IL-4) [177]. PRF improves soft tissue healing when in contact [178,179,180]. Indeed, some studies have come to the conclusion that PRF promotes and improves soft tissue regeneration more than hard tissue and therefore consider PRF to have slight potential in the GBR technique (guided bone regeneration). Excellent results have been obtained on soft tissues, even from the use of a mixture of ozolipoilein, which, in only 3–5 days, can heal small ulcers caused by radiation therapy cycles. This blend is also antibacterial and antifungal [181]. Instead, PRF significantly contributes to tissue healing through its antibacterial properties, especially against S. aureus and E. Coli. However, this is mostly expressed when a horizontal centrifuge is used to produce PRF [182]. The use of PRF as a membrane has produced effective results in both bone regeneration and soft tissue regeneration. This membrane can be obtained in a non-invasive way and is considered a protective barrier of newly formed tissues. For the patient, this method is very comfortable [183,184]. The PRF can be considered a very valid barrier membrane between the oral cavity and bone, with an easy and predictable preparation protocol and a well-defined structure with impressive mechanical properties, as reported by several authors [147,150,151,155,156,157,158,159,160,185]. A PRF membrane can also be used many hours after preparation as the release of PDGF continues to be high, as long as the membrane is properly prepared in a PRF box and stored under physiological conditions. The release of VEGF and β-TGF significantly increases in the first four hours, but then the amount of these growth factors does not show large differences between blood derivatives because GFs are mainly derived from leukocytes [186]. A new generation of blood products called CGF from Silfradent is produced without anticoagulants. The MEDIFUGE MF200 centrifuge that produces CGF is from Silfradent, has a special multi-speed centrifugation program, creates a gradual sinusoid (RPM) at various speeds and offers a large, high-density fibrin matrix rich in GFs [187]. This CGF is composed of three layers, a dense fibrin network and blood cells trapped within it, especially in the most outer part [188]. The first layer is called PPP and is a network of plasma proteins in which cells without a nucleus are found. These cells seem to have the typical appearance of erythrocytes. The second layer of CGF is much denser than the first and third layers. It is a fibrin network, in which cellular elements are trapped and collagen fibers are found where other corpuscular elements are captured. The CGF layer consists of three fragments: the upper white part, the lower red part and the buffycoat at the interface between the white and red part [187]. The third layer of RBC red blood cells appears to have a wider network of collagen fibers than the second layer, and coreless corpuscular elements, such as platelets, are found entangled in this network [188]. The CGF fibrin matrix is denser than PRF and has GFs present in it, such as TGF-β1 and VEGF, which are important in cell proliferation. The presence of these growth factors was also identified in the RBC layer. The CD34+ cells are trapped in the CGF matrix with a considerable number of them and have been found in both levels (CGF-RBC). The CGF appears to be more promising in tissue regeneration, as it promotes osteogenic cell differentiation and proliferation. Therefore, with the CGF, the activity of ALP [162,189] significantly increases. CGF also appears to be very promising in neural tissue regeneration. The controlled release of growth factors and cytokines from CGF influences cell differentiation and intervenes in the growth of neurons [190]. In conclusion, as a result, we have the PRP with a lower concentration of GFs compared to A-PRF or CGF. Advanced Platelet Fibrin (A-PRF) and Concentrated Growth Factors (CGFs) contain TGF-β1, VEGF, PDGF-BB, IL-1β and IL-6. Masuki et al. said that the main source of PRF growth factors is in the exudate and has a very low percentage of GFs found in the fibrin network [191]. However, Ehrenfestet al. suggest that exudate is not the most important part in platelet concentrates [159]. Kawaseet al. reported that even for PRP, which is in a liquid state, fibrin gel and thrombocyte aggregates, many more biological mechanisms will emerge [192,193]. This is also accepted from other studies [150,151,155,156,157,158]. An effective method used for bone reconstruction is the penetration of CGF into the Xenograft blocks with the method that uses the Round Up device from Silfradent [161,187]. The same method is also used with β-TCP, which shows that this combination significantly increases the release of certain growth factors, such as BMP-2 and BMP-7. Scientific evidence shows that calcium ions that are released by the dissolution of β-TCP influence the activation of platelets [150,151,155,156,157,158,159,160]. The Ca2+ ions stimulate the differentiation of osteoblasts and increase the stability of BMP-2. The same study reveals that CGF used alone instead of a combination increases the release of IGF-1 [194]. The release of growth factors is high in the first few days then starts to slow down. With the aim of overcoming one of the main limitations of PRF and its degradation, an in vitro study was conducted on Alb-PRF, an injectable biomaterial, produced by PRF in liquid form and PPP heated to 75 degrees Celsius in 10 min with a device called APAG [187,195,196,197]. Since PPP is composed of 60% albumin, its denaturation creates an organized and dense protein structure without cells. This combination with APAG has been shown in vitro to preserve the volume and prolong the reabsorption times, leading to that the conclusion that the release of growth factors can continue much longer than in the traditional PRF [187,196,197]. The Alb-PRF preserves its volume even after 21 days [198]; however, the Alb-PRF membrane loses the elasticity of the PRF membrane and becomes very fragile. To overcome this deficiency, the use of high-power laser pulses is suggested [199]. Laser irradiation is performed on a surface, leaving the inner part of the membrane intact. This method seems to stimulate and increase stability in the body and allows for better suturing/fixing of the membrane, thus optimizing the Alb-PRF [199]. Even with the albumin denatured with CGF, a solid and dense membrane of cells with nuclei is obtained. This Alb-CGF membrane is capable of releasing growth factors (VEGF, PDGF, FGF2) for seven days [195]. A comparative study was conducted on the preservation of the alveoli after extraction (socket preservation) using only Alb-CGF and allograft covered with albumin. This study demonstrates that radiographically and histologically, there was no significant difference between the two groups tested; thus, Alb-CGF is considered a promising biomaterial in tissue regeneration. In fact, the authors conclude that Alb-CGF gives the same results as a bone graft with allografts and albumin (sticky bone). This material is believed to be capable of immediate and prolonged release of growth factors [200]. Other studies have reported the effectiveness of CGF and PRF in osteogenesis in patients with systemic diseases. Systematic diseases are those that must be taken into consideration in particular for bone regeneration because, in these diseases, there is the need for a personalized protocol according to the underlying pathologies and the planning of the work to be carried out. The use of bisphosphonates in patients with osteoporosis reduces the production of BMP-2, while CGF or treatment with resveratrol combined with CGF instead promotes the production of BMP-2, and they have a positive role on osteoblasts in patients treated with bisphosphonates [150,151,155,156,157,158,159,160,201]. Bisphosphonates induce bone growth, but they alter bone turnover, decrease osteoclasts and significantly reduce vascularization in adult patients [202]. Moreover, in children and young patients, they are protected from this phenomenon [203]. Due to the apoptosis of endothelial cells, bisphosphonates decrease the number of endothelial progenitor cells, so both vascularization and neo-vascularization are reduced [204]. On the other hand, the use of CGF in combination with sodium orthosilicate has been shown in vitro to stimulate cell growth, proliferation and metabolic activity in several human cell lines, including fibroblasts, endothelial cells and osteoblasts [205], and that the use of growth factors, such as epidermal growth factor (EGF), may partially neutralize the effects of bisphosphonates on human oral keratinocytes and human umbilical cord endothelial cells via the EGFR/Akt/PI3K signaling pathway [206]. Diabetes is another very widespread systemic disease. Patients with diabetes have a noticeable reduction in the potential for healing and vascularization of the affected tissues. Durmuşlar et al. concluded that the use of PRF alone did not produce significant good results; only in combination with autologous bone does PRF induce bone formation in diabetic rats and significantly increase bone volume compared to the group where only autologous bone was used [207,208,209,210,211,212,213,214,215,216,217,218,219,220].
6. Biostimulation and Laser–Graft Interactions
In daily practice, the use of Lasers, Light Amplification by Stimulated Emission of Radiation (Table 2), is increasingly being applied. Its use leads to an operating field cleaner from blood and atraumatic work. Additionally, it significantly reduces pain and postoperative edema [221,222,223,224,225]. The use of lasers offers better aesthetic effects compared to other techniques since it does not leave an obvious scar, giving the part of the body where the intervention is performed an excellent restitutio ad integrum [221,222,223,224]. Photodynamics includes a photochemical and non-thermal biological interaction. Photobiomodulation (PBM), also known as low-level laser therapy (LLLT) [226], is a safe and non-invasive clinical method that, in most cases, uses red 600–700 nm and infrared 770–1200 nm light, with the aim of stimulating healing and reducing inflammation and pain [227]. The mechanism of action of the LLLT is based on the interaction between chromophores cells (especially the enzyme of the mitochondrial respiratory chain; cytochrome C oxidase) and laser light. The absorption of light by these chromosensors generates more energy (ATP) and, in addition, causes the modulation of the calcium level and an increase in the production of nitric oxide [227]. The LLLT has been recommended by the Multinational Association of Supportive Care in Cancer/International Society of OralOncology for the treatment of oral mucositis in adult cancer patients, but LLLT has been shown to reduce severe mucositis even in young cancer patients [228]. The use of low-intensity lasers has also given excellent results in many oral diseases [229]. In recurrent aphtosis and herpes simplex, it reduces pain and provides complete wound healing, and when combined with antibiotics, improves the condition of BRONJ/MRONJ patients by reducing clinical symptoms in hyposalivation or xerostomia. Therefore, LLLT is very effective in cell repair and increases secretion by stimulating the salivary glands. LLLT also reduces the symptoms of trigeminal neuralgia [230,231,232,233,234,235]. The use of LLLT has also spread widely in the field of periodontology and peri-implantology [236,237], but the effects that lead to the use of long-term laser on scaling and root planing (SRP), bacterial-subgingival reduction and sulcular debridement (laser curettage) appear to have no significant advantages over other methods [238]. However, the use of the laser gives excellent results on the surfaces of implants that have been attacked by peri-implantitis and have part of the fixture exposed in the oral cavity. The use of the laser decreases the microroughness and porosity of the implants, thus giving a more glossy surface, which prevents the adhesion of bacteria on smooth surfaces [225]. In their study, Pereira et al. reported that the use of the LLLT did not lead to any change in bone regeneration compared to the control group, but there was a noticeable difference in the interface between the implant and the bone, thus allowing for better osseointegration [239]. Grassi et al. reported that the use of LLLT promotes proliferation and differentiation by significantly increasing cell adhesion on the implant surface [216]. The ability to promote osseointegration and stimulate bone formation around the implant has also been confirmed by other authors in their research [240,241]. Other studies have also been developed to test the effect on mechanical strength that occurs during the use of the LLLT laser [242,243]. Maluf et al. tested two groups of mice: one group received laser therapy and the other did not. This study concluded that the group of mice that received laser irradiation had greater difficulties detaching the implant from the bone than the group that was not irradiated. A torque machine was used to measure the torque needed to detach the implant from the bone. The result showed that the group treated with laser had a resistance of 50% more than the other group without laser irradiation [242]. Other studies have used the LLLT laser to enhance osteoinductive properties in biomaterials that only possess osteoconduction [212,213,244,245,246]. For this purpose, the biphasic HA/TCP and bovine bone were tested as a scaffold. The groups to be tested were irradiated every 48 h for 13 days of 40 s per sector and, after 60 days, with a second intervention the endosseous implants were inserted. The results showed significant differences between the control group and the group tested 15 and 45 days after endosseous implantology. In this experiment, increased exposure of BMP-2 and osteocalcin was observed [213]. The authors concluded that the LLLT promotes osseointegration with a high expression of BMP2 and osteocalcin related to osteoblastic activity and that the force required to remove the implants could be compared with that of the implants inserted in autologous bone [213]. Another study that tested the use of LLLT on bovine bone (DBB) and biphasic HA/TCP led to the same conclusion. After 90 days in the irradiated group, there was bone augmentation, with an increase in the expression of BMP2, Osteocalcin (OCN), alkaline phosphates (ALP) and genes [212]. The LLLT laser is described as a promising therapy for stimulating osteoblastic activity and differentiation. Furthermore, it has been observed that LLLT improves the osteoconductive properties of these materials while maintaining the volume of the bone graft [212]. Other studies have used photobiomodulation to repair bone defects with bovine bone grafts. The irradiation began on the day of the surgery, and then seven other irradiations were performed every 48 h [244,245,246]. The use of LLLT in these studies led to a significant increase in the deposition of collagen in the first healing phase, as well as greater osteoblastic activity, rapid bone remediation with neo-formation of the Haversian system and regeneration of the cortex [244,245,246]. Another study, which lasted 12 months, used enamel matrix protein-derived (EMD) combined with laser LLLT in an intra-osseous defect. The radiation was performed after the surgery with a 4 J/cm2 diode laser for five minutes on each side of the defect in five days. The result showed that the use of LLLT improved the effect of EMD in the intra-bone defect [247]. The light-emitting diode (LED) is another promising alternative for tissue biostimulation. Unlike the LLLT, which emits coherent light, the LED has non-coherent light. The LED has a lower cost, is more manageable and does not carry the same risk to the eyes. The LED appears to have the same effects as the red light laser on the stimulation for the growth of pre-osteoblasts [217], promotes osteogenic differentiation and inhibits cell proliferation [248]. The application of the LED together with photosensitive substances has also led to excellent results in the osseointegration of implants inserted into bone diffusers and filled with biomaterials. After some time, the bone formed around the implants can be compared to autologous bone [249]. However, the use of LEDs is limited; for a small area when a high power density is required, it almost always requires the use of lasers [250]. Mergoni et al. conducted an in vitro 915 nm laser study on human osteoblasts. The treatment did not provide improved effects on cell proliferation and differentiation compared to the non-irradiated group but induced the formation of bone nodules by a considerable amount [219]. Instead, Jawad et al. concluded that decreasing the laser power increases osteoblastic cell differentiation and cell proliferation increases as the laser power increases. Thus, the cell proliferation of osteoblasts using a 940 n diode laser increased more when the irradiation power was 300 mW compared to 100 mW, while the expression of ALP and osteocalcin was, respectively, higher with the radiation at 100 mW and 200 mW compared to 300 Mw [220]. Barbosa et al., In their research, made a comparison between red light lasers and infrared lasers. They claim that the use of the infrared wavelength laser gives better results compared to the red wavelength laser, thus concluding that the bone healing process depends on the time and wavelength [251]. This result also agrees with the conclusions of Queiroga et al. [218] and Renno et al., which also confirm the fact that different cell lines respond differently to specific combinations of wavelengths and doses [252]. Tani et al. tested biomodulation with three different wavelengths: red light (635 nm), infrared light (808 nm) and LED (405 nm). The aim was to evaluate the differences in proliferation, adhesion and differentiation of pre-osteoblastic and human mesenchymal stomal (hMSC) cells [253]. Bone nodules (Ca2 deposition) were observed differently in both laser wavelengths from the radiation with LEDs. On human mesenchymal stromal cells, the 635 nm wavelength is capable of promoting osteogenic proliferation, adhesion and differentiation, while on osteoblasts, this wavelength does not have a significant effect on cell differentiation by questioning red light (the wavelengths) or the parameters used for radiation (0.5–1–2 J/cm2). Moreover, this study proposes the diode laser with a wavelength of 635 nm as an effective option to promote and stimulate bone regeneration [253]. On the other hand, Ghidini et al. concluded that red waves (645 nm) could penetrate to considerable depths [254]. All these data show that there is still a great deal of confusion on the working protocols for biomodulation. Many authors suggest that the use of LLLT fundamentally improves and accelerates the healing processes of newly formed tissues [208,209,210,211,212,213,214,218,219,220]. These conclusions have already necessitated a recommended and studied protocol of a guideline with irradiations and the type of laser prescribed by the World Association for Laser Therapy (WALT) on biomodulation, as its positive effects certainly cannot be denied [255].

Table 2.
Summary of the laser protocols for biomaterials osseointegration enhancement.
7. Microbiota in Tissue Repair Processes
Other factors come into play in bone and soft tissue metabolism. The crucial role of the intestinal microbiota in the regeneration process of our organisms is the subject of great study and debate. Several authors agree in asserting that the intestine as a whole is the place where basically any dysfunction begins, even before a symptom or pathological event is diagnosed or even evolved. The balance/imbalance between the constituent parts of the gut is known as symbiosis/dysbiosis, which accurately reflects systemic health. A healthy intestine is made up of the balanced presence of four Phila bacteria: Bacteroideti, Firmicutes, Actinobacteria, Proteobacteria and Verrucomicrobia. Ibacteroideti, and firmicutes represent the majority of the microbiota [256,257]. Over the past two decades, one of the most significant scientific discoveries has been the confirmation of the Neuro-Endocrine-Immune nature of the intestine, which as a single apparatus tends to perform an activity believed to be exclusive to the central nervous system (CNS), so much so that nowadays, it refers to the gut–brain axis. In fact, the two systems share anatomically and physiologically important multi-functionalities and have neurochemical, endocrine and immune significance that makes the intestine an autonomous system called the enteric nervous system (ENS), which is responsible for all gastrointestinal activities in full coordination with the CNS [258]. A further aspect that has been highlighted is the inter-communicative capacity of the two systems through a very complex network outlining a common clinical-pathological picture. In fact, many important pathologies tend to afflict the two systems in a one-to-one and constant way [259,260]. Within the intestine, the microbiome functions as a guarantor of the homeostasis of all the other systems of the organism, capable of producing 50 to 100 mmol/L per day of short-chain fatty acids (SCFA), such as acetic acid, propionic acid and butyric acid, which are the sources of energy for both the proper functioning of the complex cellular structure that makes up the intestinal epithelium and for the constant maintenance of the skeletal system [261,262,263,264]. The importance of SCFA among acetic acid, for example, is essential against infections, in regulating blood pressure and against the deposition of sclerotic plaque in the arterial walls. Butyric acid, for its part, acts as an inhibitor of inflammatory responses thanks to its immunomodulating properties, while propionic acid has been found vital in the prevention of obesity and diabetes 2 [261,262,263,264]. Furthermore, the intestinal system performs a “prompt delivery” function of vitamins, such as folic acid and the vitamin B2–12 complex, and at the same time, it allows the synthesis of vitamin K, which is involved in many physiological, metabolic and immunological activities and plays a fundamental role in the prohormone/vitamin D absorption mechanism, which is important for the homeostasis of the skeletal system and the formation of osteocytes, osteoblasts and osteoclasts [263,265]. The way in which this interaction takes place and the mechanism in which they carry out these processes reveals something that is revolutionizing the conventional thinking of contemporary medicine, for which we refer more and more often to the term epigenetics [266].
Epigenetic events are highly dynamic and change in response to the availability, quality and quantity of environmental insults both external and internal to the oral cavity. In this perspective, there is a tendency to have a substantially different perspective in which bacteria, viruses and fungi, which are also harmful and dangerous, are still indispensable for life. The results of the experiments conducted on germ-free (GF) mice confirmed that the shortage of gut microbiota was to be indicated as a functional cause of the severe deficiency of the immune system. GF animals were shown to have low levels of natural killer cells (NK), dendritic cells (DC), α/β + and γ/δ + T cell populations, which play an important role in defense and pathogenesis during inflammation and infection, particularly against some types of malignant neoplasms. Furthermore, the above experiments have unequivocally demonstrated that GF animals were particularly susceptible to frequent infections substantially due to the decline of angiogenin-4 (Ang4), a powerful antimicrobial molecule belonging to the class of microbiocidal proteins in Paneth cells [267,268].
Dysbiosis and Metabolic Disorders Related to the Bone Tissue Degenerative Processes
What is the connection between dysbiosis and the bone system? The conclusions revealed a different type of bacteria. In fact, patients suffering from osteopenia revealed an increase in the number of Firmicutes phyla with a reduced number of Bacteroidetes compared to patients in the control group; the genera Lachnoclostridium and Klebsiella, Gemmatimonadetes Chloroflexi and Synergistetes were detected to a high extent in both patients with osteoporosis and in those with osteopenia but were absent or very low in the control group; the control group showed a prevalence of Bacteroides, Faecalibacterium and Prevotella. Interestingly, Prevotella was in a constant presence in the osteoporosis group but very low in the osteopenia group [269,270,271,272].
In patients suffering from Crohn’s disease and ulcerative colitis, recent studies have confirmed the coexisting presence of osteoporosis, and the cause can be found in a chronic inflammatory state. One of the mechanisms involved seems to be related to the immune-mediated bone metabolism involving the RANKL axis (an activator of the NF receptor kappa B ligand NFκB-RANK), the osteoprotegerin (OPG) and the basic activation of the immune-receptor of the tyrosine (ITAM), all members belonging to the TNF super-family and all factors sharing the same androgen signaling pathway [269,270,271]. The chronic overexpression of pro-inflammatory interleukins determines inhibitory activity towards hormones, such as estrogen (E2), testosterone and progesterone, which play a key role in the formation, production and stabilization of such bone tissue. The decreased intake of these hormones triggers a vicious cycle of worsening the equilibrium state of the immune response and increasing the inflammatory quotient to almost block physiological bone turnover completely. This scenario is often found in women going through menopause and in men over 60 who present a physio-pathological picture that recalls the typical picture of many autoimmune syndromes and of different neoplastic forms [273,274,275]. The increase in phlogosis, the expression of inflammatory interleukins, such as interleukin 1α and 1β, IL-6, IL-11 and IL-17, also contributes to the decrease in the pH, which becomes peremptorily acidic and also contributes to slowing down the differentiation of mesenchymal cells from osteoblasts. In fact, it is well known that this process from MSCs to osteoblasts can only occur in an alkaline physiological environment. An interesting fact is the relationship between OPG and MSCs; both intervene in the regenerative phase by containing osteoclastogenesis precisely through their blocking action on RANK via RANKL. This ultimately explains how in a state of imbalance, determined both by a chronic inflammatory state and by the lack of male and female steroids, such as estrogen, testosterone and progesterone, the regenerative process of the bone tends to undergo a major arrest at the expense of remodeling activity on osteoclasts [276,277,278,279]. It is now known that not only intestinal dysbiosis but also oral bacteria, particularly periodontal bacteria, influence osteoporosis and bone loss. The oral microbiota plays an important role in many systematic conditions and vice versa [258,272,280,281,282,283,284]. Except for oral hygiene, which helps maintain the physiological state of saliva, a balanced diet and supplements of non-pathogenic microorganisms must be used to keep the oral microbiota in the normal range [285]. These non-pathogenic microorganisms are named probiota, and by interacting with the intestinal microbiota, have given good results in various conditions and pathologies [259,265,286,287,288,289,290].
8. Stem Cells Therapies for Regenerative and Translational Medicine
The direct use of stem cells requires a studied, planned approach and, above all, one that takes into account the general condition of the patient. For doctors, orthopedists and dentists, the use of pluripotent and multipotent stem cells, such as MSCs, constitute a superior quality method that exponentially improves the body’s regenerative capacity and ability. In fact, stem cells (SCs) are generally able not only to differentiate into new tissue but also coordinate, modulate and manage the entire chain of events of both repair and regenerative responses—just think of their role on M1 pro-inflammatory macrophages [291,292,293,294,295,296]. The M1s under pressure from MSCs trigger the recruitment of interleukins and pro-inflammatory cytokines involved in the first phase of the repair process, such as IL-1β, IL-2, IL-6, IL-17, TNFα and IFNγ, while M2 initiate recruitment in the second phase of anti-inflammatory interleukins, such as IL-10, IL-4 and IL-13, prostaglandin E2, oncostatin and bone morphogenetic protein 2 (BMP-2). This mechanism is of crucial importance, especially in the presence of the inhibitory effect of some autoimmune disorders on M2, in which the bone tissues are compromised and the regenerative process is completely blocked [297,298,299]. Preparing the laboratory procedures for bone regenerative therapy for SCs requires much more than a simple study centrifuge. The SCs are isolated and cultured in a sophisticated sterile cell culture laboratory by cell biologists, usually for a period ranging from a few days to two weeks. SCs can be obtained from different sources and can be both autologous and heterologous (from a donor). The main sources are peripheral blood (PB-SCs), bone marrow (BM-SCs), adipose tissue (AT-SCs), dental pulp (DP-SCs) or placenta (Pl-SCs), amniotic fluid (FA-MSCs) and umbilical cords (UCB-SCs). The efficacy of SCs from BM, AT, DP, UCB, Pl, FA or PB alone or in combination with bio-implants is a vast and expanding field of research and study. The information and data obtained are all in agreement in confirming the immuno-modulating and regenerative properties of SCs with evident improvements in anti-inflammatory, osteogenic and angiogenic activity. Part of this effect is surely due to the intrinsic ability of stem cells to secrete anti-inflammatory and angiogenic cytokines and growth factors, such as IL-10 and TGF-beta [297,298,299,300]. Peripheral blood has shown some advantages over other solutions for everything related to the use of PB-SCs for clinical purposes in vivo. From the peripheral blood, the cells are easy to harvest with a minimally invasive procedure in numbers and quantities readily available and with a low risk for any immunological reaction or rejection. Furthermore, PB-SCs do not require prolonged periods of in vitro culture, retain their multipotent capacity and remain substantially able to differentiate into different cellular phenotypes [297,298,299]. These cells were photographed with an electron microscope and then morphologically evaluated, and they were then tested and carefully characterized with the RT PCR method to identify the expression of genes such as Oct4, Sox2, OCN, Nestin, Nanog and DMP, all highly specific genes of pluripotent and multipotent SCs [297,298,299]; confirmations in this sense were then obtained with fluorescence analysis for the expression of genes such as TRA-1 and CD-44; flow-cytometric analysis then confirmed the trend in which both adherent and non-adherent mononuclear cells showed positivity with a panel of multipotency and pluripotency markers, such as CD44, CD73, CD90, CD133, CD34, CD45, CD14, Nestinand SSEA-3 and TRA-1, of NSCs. In addition, it was possible to perform a hormone quantification analysis from both female and male donors, and the results showed the presence of 14 hormones in the extracellular matrix component, the major ones being testosterone, estradiol, progesterone and cortisol. The isolated adherent and suspended mononuclear cells were able to maintain their plastic properties during in vitro culture while maintaining their ability to proliferate and differentiate when exposed to the appropriate culture medium [299]. The regenerative, restorative capacity of these SCs has been proven by multiple studies, especially in the area of the osteo-skeletal system. Recently, a study explored a new solution for osteo-regeneration at the level of the mandibular and maxillary bones with a resolution composed of the combination of β-TCP granules, autologous peripheral blood fibrin (hPB) and autologous peripheral blood stem cells [82]. The isolated PB-SCs were directly transferred and inserted into the previously constructed fibrin and β-TCP scaffolds. The β-TCP granules with diameters of 1 mm and 1–2.5 mm were embedded in a fibrin gel matrix and subsequently cultured with serum-free medium (SFM) for a period of 7–10 days. The compound was named compact bio-bone (CBB) [82]. In vivo CBB induced both horizontal (Table 1) and vertical (Table 2) growth, but the most important aspect was the quality and compactness of the new bone tissue, which revealed a formation of solid and compact tissue very similar to the structure of the original endogenous bone. The histological analyses carried out then, in fact, confirmed the presence and formation of new lamellar bone in excellent condition with the presence of osteocytic islets in lacunae and clusters of active osteoblasts in the production phase of a new matrix [82]. Understanding the tissue microenvironment in which you intend to perform an implant, a graft or simply inserting supports to facilitate bone fusion has certainly conditioned a new way of doing Regenerative Medicine, supported by in-depth studies on both the choice of elements and on the selection of innovative biomaterials to be used in the operating room. However, the use and continuous experimentation with new materials and new solutions had to deal not only with the vision of the mechanical properties of the tissue to be recovered or regenerated, be it bone, tendon or skin, but that of being fully compatible and similar with the part in which it is inserted keeping the surrounding structures intact [17,60,301]. An attempt was therefore made to broaden the overall vision by trying to identify the metabolic, genetic and decline conditions of the recipient because the failure of a specific implant or regeneration procedure also includes a broader and more careful analysis of the conditions that led to the process of degradation or rupture of a specific structure, such as bone [60,104,302]. In fact, a careful phase of tests and clinical evaluations was necessary, which must have the individual as its center in its complexity, and this epistemological attitude will therefore not only be focused on the quality of new and increasingly compatible bio-materials and inductive fabrics but will have to ignite a new perspective, on the importance of the physiological-molecular processes involved in the disease state intended as a progressive decline of the vital activities of the organism. Much remains to be learned about the close relationship between the microenvironment of bone tissue, the process of degenerative states and the patient’s external environment in order to evaluate a compatible and individualized treatment [14].
9. Bone Substitutes and Teeth Graft
Few studies evaluated the use of the autologous tooth in bone regeneration, where there is little evidence on the use of this biomaterial. Based on the properties that this material possesses and what it can offer in bone regeneration, there are great expectations in this regard (Table 3 and Table 4), but further studies are still needed [98,303].

Table 3.
Summary of the biomaterials and graft for sinus augmentation procedure.

Table 4.
Summary of the biomaterials and graftfor ridge preservation procedure. [T: Test; C; Control].
Calcium phosphate creates new bone faster than bovine bone [314,315], but they are also reabsorbed faster. The bovine bone preserves its volume for a long time by keeping the apex of the implant covered. The Calcium triphosphate (TCP) loses its volume, and the apex of the implant is exposed [307,310,311]. Yoko et al. believe that this loss of volume does not lead to any contraindication because this resorption is related to the length of the implant inside the sinus, and after three years, it is osteointegrated [311,312]. Oliveira et al., in a comparative study between TCP and inorganic bovine bone, stated that the implants have better primary stability in patients where only bovine bone was used [314]. For a different result, these materials can also be used combined together [316] or with blood derivatives PRF [160]; however, PRF improves the primary healing of soft tissues but does not give long-term benefits on hard tissues [305,317]. The use of the BMP morphogenic protein has given very promising results [318]. Although BMPs have a strong osteoinductive potential, used alone, they are very soluble and lose their properties. The combination with biomaterials serves as a carrier for BMPs. The BMP is found naturally in the dental matrix [98,111].
In the case of tooth extraction, a loss of approximately 30–60% in horizontal width and 10–20% in vertical length of the bone is expected after six months compared to the volume before tooth extraction [328]. Very few studies have been conducted on calcium triphosphate (TCP) in humans. This material resorbs completely, and the resorption time is rapid and fails to retain volume. It is often suggested to use it in the form of composites with a collagen matrix [75,329,330] or with calcium sulphate, which has given good results [327,331]. Compared to TCP, bovine bone preserves the volume longer because it has more graft residues, but it has less vital bone [331]. A rare case of a human autopsy was carried out five and a half years after the operation. The guided bone regeneration technique, GBR, was applied to the patient using biphasic calcium phosphate and autologous bone in contact with the implant and then using Bio-Oss bovine bone. The result of the autopsy shows that Bio-Oss had preserved the bone volume, but in the meantime, autologous bone with biphasic calcium phosphate had lost bone volume. The vestibular bone was concave, and recession of the mucosa was also seen [332]. Carmagnola et al. observed that the quality and quantity of bone added with the bovine graft was sufficient for the preservation of the alveolus and that the implantology and regenerative procedure was performed correctly [333]. However, the residues of the bovine graft remain for a long time without being reabsorbed, and consequently, there remains the suspicion that the implant at the time of contact with the bovine bone residues has osseointegration problems [334]. The dental matrix has a porous microstructure that promotes cell adhesion, blood circulation and slow resorption that guarantees correct osteoconduction, thus ensuring that the bone volume is preserved for longer [303]. Joshiet al. states that the autogenous tooth material has given good results compared to TCP while maintaining the length and width of the alveolar ridge after extractions [335]. In another analysis, the tooth material was found to be in close contact with the implant surface [336], making the dental matrix a promising biomaterial in preserving the alveolar ridge [98]. Kabir et al. removed the enamel and pulp from the tooth, making holes in it for use in critical defects. After four months, the new bone formed around the dentin graph and inside the pores was identified. This demineralized dentin microstructure showed osteoconductive and osteoinductive properties [337]. Schwarz et al. used autogenous teeth in an animal study for lateral alveolar ridge growth. The teeth were cleaned of cement, and the crown was cut. After endodontic treatment, the canal was filled with Ca(OH)2 in one group and the tooth was not treated endodontically in the other. Root dentin was used en bloc to fill the bone defect. To compare the results, they used the bone block obtained in the retromolar region. The authors concluded that the presence of dental pulp made no difference in bone regeneration compared to the endodontically treated group. The grafts are gradually reabsorbed to be replaced by homogenous bone intertwined with parallel fibers, and the dentinal block in this case has given good results for the lateral augmentation of alveolar bone followed by the subsequent positioning of the implants [338]. In the continuation of this experiment, Becker et al. reported that the dental block as a bone graft has a greater exposure and a higher failure rate than autologous bone [339]. Pohl et al. compared the dental block with the dentin particles for the lateral growth of the alveolar ridge. The authors state that the tooth material can be considered a good alternative in bone regeneration, but the dentinal block compared with the dentinal particles had distinct, clear bone margins and no macroscopic signs of bone remodeling, indicating very slow resorption [119]. Due to biocompatibility and bioactivity biomaterials of synthetic origin are widely used, but their study must be expanded in their compound form or with the combination of biomaterials or substances derived from macromolecules. Jack and Lemon state the need for these biologically derived substances [340]. For defects larger than two centimeters (>2 cm), it is recommended the use of bioactive molecules, such as growth factors, peptides of the extracellular matrix (EMC), and small molecules, such as Parathyroidhormone, Nel-like molecule-1 and LIM mineralization protein-1 [341]. Research has been developed for a long time to finalize and improve the mechanical properties and osteoinductivity of alloplasts. The combination of HA conf MWCNT 0.5% wt appears to be an appropriate combination as it improves mechanical strength and hardness; however, it remains a bio-scaffold with osteoconductive properties even though it has been claimed that this combination gives a scaffold with magnetic properties that will help to bring the growth factors into the implant site [77]. There are authors who give importance to osteoconductivity [342,343], but others think that poor osteoinductivity has often led to lower expectations in bone regeneration [175,344]. However, the third generation of bone grafting materials continues to develop more and more on the search for scaffolds capable of inducing cellular responses (Table 5 and Table 6) [60,345]. The use of human growth factors and stem cells together with biomaterials is believed to improve the osteoinductive properties of the scaffold [346]. Harwood et al. support the idea that the lack of growth factor secretion leads to delayed bone healing or even non-union with the host site [347]. Compact Bio Bone Cell increased osteoinductivity using stem cells [82].

Table 5.
Comparative summary of the main biomaterials’ properties.

Table 6.
Comparative summary of the healing characteristics of the bone substitutes (AB: autogenous bone; AP: alloplastic graft; XG: xenografts; DM: dentin matrix; NBR: New Bone Regeneration; RG: Residual Grafts; CT: Connective Tissue).
However, these bio-scaffolds have a high preparation cost. Synthetic HA and TCP need further studies to improve their mechanical and osteoinductive properties. The new alloplast osteoinductive Osopia seems to complete the three osteoinduction formation criteria, generating ectopic bone in the end. However, it is too early to discuss this biomaterial as further studies are needed to prove and determine its properties [80]. Calcifications of the bovine and dental matrix are considered, from the physiological point of view, as the most acceptable processes of HA production [348]. Bovine bone has a high resistance in the scaffolding, and its porosity allows cell circulation and the formation of angiogenesis. The reabsorption of this material remains very slow [143]. Xenografts do not have the ability to recruit or differentiate mesenchymal cells, so this biomaterial cannot produce ectopic bone. The increase in growth factors in this material has given positive results because xenografts are devoid of cells and proteins. The application of GFs has been extensively studied, and some of these are involved in the bone regeneration process, such as the BMP bone morphogenic protein [349]. The use of BMP-2 with other reconstructive materials recruits MSCs to improve differentiation in mature osteoblasts. When the BMP is used correctly, the regeneration of complex bone defects is possible, and BMP also reduces healing times [115], but these growth factors that participate in particular in osteogenic differentiation and cell interaction need to be explored in further studies because they are of great importance in bone regeneration [350]. Bracey et al. stated negative results using bovine bone as restorative material [165]. Out of ten cases considered, four of them failed in a period of 24 months. The etiology of this biomaterial is considered as a strong cause of the failures, and the immune response of the host body (anti-Gal antibody) led to the rejection of the implant because it is not possible to eliminate 100% alpha-Galepitop antigens. This review suggests using this biomaterial less and less [164]. The autologous graft remains the gold standard in bone regeneration [351], but due to the morbidity it causes and the limitation of the amount that we can obtain, studies continue to look for a replacement material [352,353]. Today, more and more attention is paid to autologous dentin grafts, which eliminate the risk of antigenicity [96]. An autologous tooth can be used by the same patient even after a long time from its avulsion, and the dental element can be preserved without additional liquids. Schmidt-Schultz and Schultz confirm that the tooth retains the inorganic matrix like the organic one even after hundreds of years [354]. If the dental matrix is processed in the right way, it has osteoinductive properties determined by the morphogenetic proteins BMPs, which are contained in physiological quantities in the tooth. The tooth crushed with Tooth Transformer (TT) seems to preserve these osteoinductive properties with a partial demineralization of the dental matrix without damaging its structure, offering a graft in 400–800 mm particles that are easy to handle during surgery [98,123,125,128,130,131,132,134]. The demineralized dental matrix has a faster resorption time than mineralized dentin as biodegradation is almost impossible for large particles with high crystalline. Small-sized HA crystals show the best osteoconduction effects [98,129,130,132]. In terms of comparing biomaterials, the healing time that each material takes is important, as it shows a great effect of new bone formation. Autogenic bone appears to be more effective in the first six months, but for a longer healing time, different materials achieve similar histomorphometric results between the various biomaterials. This means that when a surgeon has no time limit and can therefore wait more than six months for loading, can choose several alternatives, which give similar results to the autogenous bone, but the use of GFs and MSC in combination with other biomaterials increase and improve the healing rate [355].
10. Hyaluronic Acid and Bone Regeneration
Hyaluronic acid (Ha) is a natural extracellular matrix element that could be a promising component for the regenerative procedures for hard and soft tissues [356,357]. In literature, it was demonstrated that the Ha is able to improve cell adhesion, proliferation, and differentiation [358]. The treatment of the maxillary bone defects often requires a grafting approach with scaffold materials in order to restore the anatomy and the function of the damaged soft and hard tissues. In addition to the scaffold biocompatibility, the mechano-physical behavior, biodegradability and bioresorption represent a key factor for successful osteointegration [359]. The hyaluronic acid-based scaffold could play a broad role in improving the scaffold’s biological behavior and other implant materials [359]. Many different combinations of Ha-based biomaterials have been studied, such as Ha–bioglasses, Ha–metals, Ha–inorganic (calcium phosphate, Ha–hydroxyapatite) and organic grafts (polycaprolactone and poly-L-lactic acid) [360]. The principal advantages connected to the hyaluronic acid compounds are increased homogeneous and stable morphology, enhanced mineralization processes and material degradation [358]. Moreover, the hyaluronic acid-based biomaterials are available in the form of colloids, an injectable polymeric scaffold. In colloid form, the Ha crosslinking gradation could affect the mechanical behavior, the architectural characteristics and the material’s stability [361,362,363]. The colloids form could be used as drug carriers by incorporating osteogenic molecules, such as TGF-β, bone morphogenetic proteins and angiogenetic factors, such as VEGF, FGF, PDGF and chemotactic cytokines [364].
11. Conclusions
Numerous medical requirements in bone regeneration have made it possible for a wide range of materials. Studies continue in order to offer a product that meets the clinical needs of bone regeneration. To be used as bone substitutes, biomaterials must maintain the volume for a sufficient time until they are completely replaced by bone tissue and resist over time. None of the materials fully meet the requirements for any bone defect. This must be taken into consideration, and depending on the procedure and surgical needs of the bone defects, the materials must be chosen. The choice will be made based on the surgical problem to be treated, the clinical condition of the patient who may have comorbidities or hormonal-metabolic problems and also the needs related to the necessary regeneration time, the size of the defect, the opportunities that each country offers through bone banks and the economic and religious requirements of patients. An increasing amount of literature is focused on the recent applications of non-transfusional hemocomponents to enhance bone repair capability and the local response to tissue repair. These novel techniques could reduce the healing period of the alveolar bone defects. In particular, the use of specific growth factors and BMP in combination with different grafts could represent an advantageous approach to improve the new bone formation for a wide range of defects. The advantages deriving from the use of LLLT and lasers could produce different results depending on the frequency used and the type of regenerative intervention to be performed.
Author Contributions
Conceptualization, D.H., A.D.I., A.S., A.M.I., M.F., G.M.T. and F.L.; methodology, A.D.I., I.R.B., A.S., D.H., F.L., M.E.M. and A.M.; software, I.R.B., A.D.I., A.M.I. and G.D.; validation, F.I., F.L., A.M.I., M.E.M., A.M., D.H., I.R.B. and A.S.; formal analysis, A.M.I., F.L., A.S., G.D. and A.D.I.; investigation, G.M. (Giuseppina Malcangi), G.D., A.D.I., F.L., A.M.I., A.S. and F.I.; resources, A.M.I., G.D., A.D.I., F.I., I.R.B., G.M. (Grazia Marinelli) and G.M. (Giuseppina Malcangi); data curation, G.D., F.L., M.F., A.S., G.M. (Giuseppina Malcangi), G.M.T., M.F., F.I. and G.M. (Grazia Marinelli); writing—original draft preparation, A.D.I., A.M.I., G.D., A.S., G.M. (Giuseppina Malcangi), F.L. and F.I.; writing—review and editing, F.I., F.L., I.R.B., G.M. (Giuseppina Malcangi), A.S. and G.D.; visualization, F.L., A.S. and I.R.B.; supervision, G.M.T., I.R.B., F.I., A.D.I., A.S. and F.L.; project administration, F.I., G.D., G.M. (Giuseppina Malcangi), G.D., A.D.I. and A.M.I. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
All experimental data to support the findings of this study are available by contacting the corresponding author upon request. The authors have annotated the entire data building process and empirical techniques presented in the paper.
Acknowledgments
The authors declare no acknowledgement for the present research.
Conflicts of Interest
The authors declare no conflict of interest.
Abbreviations
| 3Ca3(PO4)2Ca(OH)2 | hydroxyapatitepurum |
| 3D | three-dimensional |
| ADM | autologous tooth-derived graft material |
| Alb-CGF | autologous albumin gel and concentrated growth factor |
| Alb-PRF | autologous albumin gel and platelet-rich fibrin |
| ALP | alkalin phosphatase |
| Ang4 | angiogenin-4 |
| APAG | activated plasma albumin gel |
| APDDM | autogenous partially demineralized dentin matrix |
| A-PRF | advanced platelet-rich fibrin |
| AT | adipose tissue |
| ATP | adenosine triphosphate |
| AT-SCs | adipose tissue-stem cells |
| BCP | biphasic calcium phosphate |
| bFGF | basic fibroblast growth factor |
| BHA | bone hydroxyapatite |
| BM | bone marrow |
| BMA | bone marrow aspirate |
| BMPs | bone morphogenetic proteins |
| BM-SCs | bone marrow-stem cells |
| BRONJ | bisphosphonate-related osteonecrosis of the jaw |
| Ca | calcium |
| Ca2+ | calcium ion |
| Ca2P2O7 | calcium pyrophosphate |
| Ca(OH)2 | calcium hydroxide |
| CBB | compact bio-bone |
| CD34 | encoded gene in human and other species |
| CG | control group |
| CGF® | concentrated growth factor |
| CNS | central nervous system |
| CO3(2−) | carbonate ion |
| CS | calcium sulphate |
| DBB | deproteinized bovine bone |
| DC | dendritic cells |
| DDM | demineralized dentin matrix |
| DMP | gene protein coding (dentin matrix acidic phosphoprotein) |
| E2 | estradiol |
| EGF | epidermal growth factor |
| EGFR/Akt/PI3K | epidermal growth factor receptor/protein kinase B/phosphatidylinositol-3-kinase |
| EMD | enamel matrix protein derived |
| ENS | enteric nervous system |
| FA | amniotic fluid |
| FA-MSCs | amniotic fluid-stem cells |
| fMWCNT | functionalized multi-walled carbon nanotube |
| GBR | guided bone regeneration |
| GCT 30 | gelatin-chitosan-β-TCP 30% |
| GF | germ free |
| GF | growth factor |
| HA | hydroxyapatite (Ca10(PO4)6(OH)2) |
| Ha | hyaluronic acid |
| HA/TCP | combination of hydroxyapatite with tricalcium phosphate |
| HL-BCB | vertical measurements from buccal cortical bone |
| hMSC | human mesenchymal stem cells |
| IFN | interferon |
| IFNγ | interferon gamma |
| IGF | insulin-like growth factor |
| IGFBP3 | insulin-like growth factor-binding protein 3 |
| IL-1 | interleukin-1 |
| ITAM | immunoreceptor tyrosine-based activation motif |
| LED | light-emitting diode |
| LLLT | low-level laser therapy |
| L-PRF | leukocyte platelet-rich fibrin |
| MCS | mesenchymal stem cell |
| MDM | mineralized dentin matrix |
| MMPs | matrix metalloproteinases |
| MRONJ | medication-related osteonecrosis of the jaw |
| MSFE | maxillary sinus floor elevation |
| Na+ | sodium ion |
| NHA | nano-hydroxyapatite |
| NK | natural killer |
| Oct4 | octamer-blinding transcription factor 4 |
| ONC | osteocalcin |
| OPG | osteoprotegerin |
| P | phosphorus |
| PB | peripheral blood |
| PBM | photobiomodulation |
| PB-SCs | peripheral-blood stem cells |
| PCBM | particulate cancellous bone and marrow |
| PDGF | platelet-derived growth factor |
| PDGF | platelet-derived growth factor |
| PDGF-BB | platelet-derived growth factor-BB |
| Pl | placenta |
| PLGA | poly(lactic-co-glycolic acid) |
| Pl-SCs | placenta-stem cells |
| PPP | platelet-poor plasma |
| PRF® | platelet-rich fibrin |
| PRP® | platelet-rich plasma |
| R.P.M | revolution per minute |
| RANK | receptor activator of nuclear factor kappa-B |
| RANKL | receptor activator of nuclear factor kappa-B ligand |
| RBC | red blood cells |
| rhBMP/Bio-Oss® | bovine bone as a carrier of recombinant human bone morphogenetic protein |
| RT PCR | reverse transcription polymerase chain reaction |
| SCFA | short chain fatty acids |
| SCs | stem cells |
| SEM | scanning electron microscope |
| SFM | serum-free media |
| Sox2 | sry-box-containing gene 2 |
| SRP | scaling and root planing |
| SSEA-3 | stage-specific embryonic antigen 3 |
| T α/β + e γ/δ + | cell population |
| T1 | tested group 1 |
| TCP | tricalcium phosphate |
| TG | test group |
| TGF | transforming growth factor |
| TGF-β1 | transforming growth factor-beta1 |
| TNF | tumor necrosis factor |
| TT® | tooth transformer |
| UCB | umbilical cord blood |
| UCB-SCs | umbilical cord blood |
| VDR | vitamin D receptor |
| VEGF | vascular endothelial growth factor |
| VL | vertical line, tooth’s axis |
| VL-BCB | horizontal measurements from buccal cortical bone |
| WALT | world association for laser therapy |
| α-TCP | alfa-tricalcium phosphate |
| β-TCP | beta-tricalcium phosphate |
| β-TGF | beta-transforming factor |
References
- Albrektsson, T.; Johansson, C. Osteoinduction, osteoconduction and osseointegration. Eur. Spine J. 2001, 10 (Suppl. 2), S96–S101. [Google Scholar] [CrossRef] [PubMed]
- Adell, R.; Lekholm, U.; Rockler, B.; Brånemark, P.I. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int. J. Oral. Surg. 1981, 10, 387–416. [Google Scholar] [CrossRef]
- Davies, J.E. Understanding Peri-Implant Endosseous Healing. J. Dent. Educ. 2003, 67, 932–949. [Google Scholar] [CrossRef] [PubMed]
- Brånemark, P.I. Osseointegration and its experimental background. J. Prosthet. Dent. 1983, 50, 399–410. [Google Scholar] [CrossRef]
- Tumedei, M.; Savadori, P.; Del Fabbro, M. Synthetic Blocks for Bone Regeneration: A Systematic Review and Meta-Analysis. Int. J. Mol. Sci. 2019, 20, 4221. [Google Scholar] [CrossRef] [PubMed]
- Comuzzi, L.; Tumedei, M.; Piattelli, A.; Iezzi, G. Short vs. Standard Length Cone Morse Connection Implants: An In Vitro Pilot Study in Low Density Polyurethane Foam. Symmetry 2019, 11, 1349. [Google Scholar] [CrossRef]
- Scarano, A.; Lorusso, F.; Orsini, T.; Morra, M.; Iviglia, G.; Valbonetti, L. Biomimetic Surfaces Coated with Covalently Immobilized Collagen Type I: An X-Ray Photoelectron Spectroscopy, Atomic Force Microscopy, Micro-CT and Histomorphometrical Study in Rabbits. Int. J. Mol. Sci. 2019, 20, 724. [Google Scholar] [CrossRef]
- Scarano, A.; Lorusso, F.; Staiti, G.; Sinjari, B.; Tampieri, A.; Mortellaro, C. Sinus Augmentation with Biomimetic Nanostructured Matrix: Tomographic, Radiological, Histological and Histomorphometrical Results after 6 Months in Humans. Front. Physiol. 2017, 8, 565. [Google Scholar] [CrossRef]
- Anitua, E.; Sánchez, M.; Nurden, A.T.; Nurden, P.; Orive, G.; Andía, I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol. 2006, 24, 227–234. [Google Scholar] [CrossRef]
- Vermesan, D.; Prejbeanu, R.; Poenaru, D.V.; Petrescu, H.; Apostol, E.; Inchingolo, F.; Dipalma, G.; Abbinante, A.; Caprio, M.; Potenza, M.A.; et al. Do intramedullary implants improve survival in elderly patients with trochanteric fractures? A retrospective study. Clin. Ter. 2015, 166, e140–e145. [Google Scholar] [CrossRef]
- Scarano, A.; Inchingolo, F.; Leo, L.; Buggea, C.; Crisante, A.; Lucchina, A.G.; Scogna, G. Bacterial adherence to silk and expanded polytatrafluorethilene sutures: An in vivo human study. J. Biol. Regul. Homeost. Agents 2021, 35, 205–210. [Google Scholar] [CrossRef] [PubMed]
- Gehrke, S.; Mazón, P.; Del Fabbro, M.; Tumedei, M.; Júnior, J.A.; Pérez-Díaz, L.; De Aza, P. Histological and Histomorphometric Analyses of Two Bovine Bone Blocks Implanted in Rabbit Calvaria. Symmetry 2019, 11, 641. [Google Scholar] [CrossRef]
- Comuzzi, L.; Tumedei, M.; Pontes, A.E.; Piattelli, A.; Iezzi, G. Primary Stability of Dental Implants in Low-Density (10 and 20 pcf) Polyurethane Foam Blocks: Conical vs Cylindrical Implants. Int. J. Environ. Res. Public Health 2020, 17, 2617. [Google Scholar] [CrossRef] [PubMed]
- Isacco, C.G.; Paduanelli, G.; Inchingolo, A.D.; Nguyen, K.C.D.; Inchingolo, A.M.; Pham, V.H.; Aityan, S.K.; Schiffman, M.; Tran, T.C.; Huynh, T.D.; et al. Bone decay and beyond: How can we approach it better. J. Biol. Regul. Homeost. Agents 2019, 33, 143–154. [Google Scholar]
- Castellanos-Cosano, L.; Rodriguez-Perez, A.; Spinato, S.; Wainwright, M.; Machuca-Portillo, G.; Serrera-Figallo, M.-A.; Torres-Lagares, D. Descriptive retrospective study analyzing relevant factors related to dental implant failure. Med. Oral Patol. Oral Y Cir. Bucal 2019, 24, e726–e738. [Google Scholar] [CrossRef]
- Isacco, C.G.; Inchingolo, A.D.; Cao, K.D.N.; Malcangi, G.; Paduanelli, G.; Hung, V.P.; Cong, T.T.; Bordea, I.R.; Scarano, A.; Laforgia, A.; et al. The bad relationship, osteo-decay and diabetes type 2 searching for a link: A literature review. J. Biol. Regul. Homeost. Agents 2021, 35, 253–269. [Google Scholar] [CrossRef]
- Ballini, A.; Dipalma, G.; Isacco, C.G.; Boccellino, M.; Di Domenico, M.; Santacroce, L.; Nguyễn, K.C.D.; Scacco, S.; Calvani, M.; Boddi, A.; et al. Oral Microbiota and Immune System Crosstalk: A Translational Research. Biology 2020, 9, 131. [Google Scholar] [CrossRef]
- Lorusso, F.; Postiglione, F.; Delvecchio, M.; Rapone, B.; Scarano, A. The impact of diabetes in implant oral rehabilitations: A bibliometric study and literature review. Acta Med. Mediterr. 2020, 36, 3333. [Google Scholar] [CrossRef]
- Scarano, A.; Lorusso, F.; Ravera, L.; Mortellaro, C.; Piattelli, A. Bone Regeneration in Iliac Crestal Defects: An Experimental Study on Sheep. BioMed Res. Int. 2016, 2016, 4086870. [Google Scholar] [CrossRef]
- Scarano, A.; Carinci, F.; Lorusso, F.; Festa, F.; Bevilacqua, L.; de Oliveira, P.S.; Maglione, M. Ultrasonic vs Drill Implant Site Preparation: Post-Operative Pain Measurement Through VAS, Swelling and Crestal Bone Remodeling: A Randomized Clinical Study. Materials 2018, 11, 2516. [Google Scholar] [CrossRef]
- Wisniewska, L.M.; Ehrenfest, D.M.D.; Galindo-Moreno, P.; Segovia, J.D.; Inchingolo, F.; Wang, H.-L.; Fernandes-Cruz, M. Molecular, Cellular and Pharmaceutical Aspects of Biomaterials in Dentistry and Oral and Maxillofacial Surgery. An Internationalization of Higher Education and Research Perspective. Curr. Pharm. Biotechnol. 2017, 18, 10–18. [Google Scholar] [CrossRef] [PubMed]
- Abdulghani, S.; Mitchell, G.R. Biomaterials for In Situ Tissue Regeneration: A Review. Biomolecules 2019, 9, 750. [Google Scholar] [CrossRef] [PubMed]
- Inchingolo, F.; Paduanelli, G.; De Oliveira, L.A.; Inchingolo, A.M.; Georgakopoulos, P.I.; Inchingolo, A.D.; Malcangi, G.; Athanasiou, E.; Fotopoulou, E.; Tsantis, S.; et al. Computer-based quantification of an atraumatic sinus augmentation technique using CBCT. J. Biol. Regul. Homeost. Agents 2019, 33, 31–39. [Google Scholar] [PubMed]
- Inchingolo, F.; Ballini, A.; Cagiano, R.; Inchingolo, A.D.; Serafini, M.; De Benedittis, M.; Cortelazzi, R.; Tatullo, M.; Marrelli, M.; Inchingolo, A.M.; et al. Immediately loaded dental implants bioactivated with platelet-rich plasma (PRP) placed in maxillary and mandibular region. Clin. Ter. 2015, 166, e146–e152. [Google Scholar] [CrossRef]
- Karakasli, K.; Erdur, E.A. The effect of platelet-rich fibrin (PRF) on maxillary incisor retraction rate. Angle Orthod. 2020, 91, 213–219. [Google Scholar] [CrossRef]
- Inchingolo, A.D.; Inchingolo, A.M.; Bordea, I.R.; Xhajanka, E.; Romeo, D.M.; Romeo, M.; Zappone, C.M.F.; Malcangi, G.; Scarano, A.; Lorusso, F.; et al. The Effectiveness of Osseodensification Drilling Protocol for Implant Site Osteotomy: A Systematic Review of the Literature and Meta-Analysis. Materials 2021, 14, 1147. [Google Scholar] [CrossRef]
- Datta, L.P.; Manchineella, S.; Govindaraju, T. Biomolecules-derived biomaterials. Biomaterials 2020, 230, 119633. [Google Scholar] [CrossRef]
- Munerato, M.S.; Biguetti, C.C.; da Silva, R.B.P.; da Silva, A.C.R.; Bacelar, A.C.Z.; da Silva, J.L.; Couto, M.C.R.; Duarte, M.A.H.; Santiago-Junior, J.F.; Bossini, P.S.; et al. Inflammatory response and macrophage polarization using different physicochemical biomaterials for oral and maxillofacial reconstruction. Mater. Sci. Eng. C Mater. Biol. Appl. 2020, 107, 110229. [Google Scholar] [CrossRef]
- Tumedei, M.; Piattelli, A.; Degidi, M.; Mangano, C.; Iezzi, G. A Narrative Review of the Histological and Histomorphometrical Evaluation of the Peri-Implant Bone in Loaded and Unloaded Dental Implants. A 30-Year Experience (1988–2018). Int. J. Environ. Res. Public Health 2020, 17, 2088. [Google Scholar] [CrossRef]
- Fanali, S.; Tumedei, M.; Pignatelli, P.; Inchingolo, F.; Pennacchietti, P.; Pace, G.; Piattelli, A. Implant primary stability with an osteocondensation drilling protocol in different density polyurethane blocks. Comput. Methods Biomech. Biomed. Eng. 2020, 24, 14–20. [Google Scholar] [CrossRef]
- Fujiwara, S.; Kato, S.; Bengazi, F.; Velez, J.U.; Tumedei, M.; Kotsu, M.; Botticelli, D. Healing at implants installed in osteotomies prepared either with a piezoelectric device or drills: An experimental study in dogs. Oral Maxillofac. Surg. 2020, 25, 65–73. [Google Scholar] [CrossRef] [PubMed]
- Kotsu, M.; Urbizo Velez, J.; Bengazi, F.; Tumedei, M.; Fujiwara, S.; Kato, S.; Botticelli, D. Healing at implants installed from ~70- to <10-Ncm insertion torques: An experimental study in dogs. Oral Maxillofac. Surg. 2020, 25, 55–64. [Google Scholar] [CrossRef] [PubMed]
- Scarano, A.; Lorusso, F.; Arcangelo, M.; D’Arcangelo, C.; Celletti, R.; de Oliveira, P.S. Lateral Sinus Floor Elevation Performed with Trapezoidal and Modified Triangular Flap Designs: A Randomized Pilot Study of Post-Operative Pain Using Thermal Infrared Imaging. Int. J. Environ. Res. Public Health 2018, 15, 1277. [Google Scholar] [CrossRef] [PubMed]
- Scarano, A.; de Oliveira, P.S.; Traini, T.; Lorusso, F. Sinus Membrane Elevation with Heterologous Cortical Lamina: A Randomized Study of a New Surgical Technique for Maxillary Sinus Floor Augmentation without Bone Graft. Materials 2018, 11, 1457. [Google Scholar] [CrossRef] [PubMed]
- Scarano, A.; Lorusso, F.; Di Cerbo, A.; Lucchina, A.G.; Carinci, F. Eradication of hairy mouth after oncological resection of the tongue and floor mouth using a diode laser 808 nm. Postoperative pain assessment using thermal infrared imaging. Lasers Surg. Med. 2019, 51, 516–521. [Google Scholar] [CrossRef]
- Miron, R.J.; Zhang, Y.F. Osteoinduction: A review of old concepts with new standards. J. Dent. Res. 2012, 91, 736–744. [Google Scholar] [CrossRef]
- Albrektsson, T.; Canullo, L.; Cochran, D.; Bruyn, H.D. “Peri-Implantitis”: A Complication of a Foreign Body or a Man-Made “Disease”. Facts and Fiction. Clin. Implant. Dent. Relat. Res. 2016, 18, 840–849. [Google Scholar] [CrossRef]
- Karl, M.; Albrektsson, T. Clinical Performance of Dental Implants with a Moderately Rough (TiUnite) Surface: A Meta-Analysis of Prospective Clinical Studies. Int. J. Oral Maxillofac. Implant. 2017, 32, 717–734. [Google Scholar] [CrossRef]
- Dewhirst, F.E.; Chen, T.; Izard, J.; Paster, B.J.; Tanner, A.C.R.; Yu, W.-H.; Lakshmanan, A.; Wade, W.G. The Human Oral Microbiome. J. Bacteriol. 2010, 192, 5002–5017. [Google Scholar] [CrossRef]
- Scarano, A.; Crincoli, V.; Di Benedetto, A.; Cozzolino, V.; Lorusso, F.; Vulpiani, M.P.; Grano, M.; Kalemaj, Z.; Mori, G.; Grassi, F.R. Bone Regeneration Induced by Bone Porcine Block with Bone Marrow Stromal Stem Cells in a Minipig Model of Mandibular “Critical Size” Defect. Stem Cells Int. 2017, 2017, 9082869. [Google Scholar] [CrossRef]
- Scarano, A.; Valbonetti, L.; Marchetti, M.; Lorusso, F.; Ceccarelli, M. Soft Tissue Augmentation of the Face With Autologous Platelet-Derived Growth Factors and Tricalcium Phosphate. Microtomography Evaluation of Mice. J. Craniofacial Surg. 2016, 27, 1212–1214. [Google Scholar] [CrossRef] [PubMed]
- Scarano, A.; Inchingolo, F.; Murmura, G.; Traini, T.; Piattelli, A.; Lorusso, F. Three-Dimensional Architecture and Mechanical Properties of Bovine Bone Mixed with Autologous Platelet Liquid, Blood, or Physiological Water: An In Vitro Study. Int. J. Mol. Sci. 2018, 19, 1230. [Google Scholar] [CrossRef] [PubMed]
- Scarano, A.; Sinjari, B.; Murmura, G.; Lorusso, F. Neurosensory Disturbance of the Inferior Alveolar Nerve After 3025 Implant Placements. Implant Dent. 2017, 26, 735–743. [Google Scholar] [CrossRef] [PubMed]
- Maglione, M.; Bevilacqua, L.; Dotto, F.; Costantinides, F.; Lorusso, F.; Scarano, A. Observational Study on the Preparation of the Implant Site with Piezosurgery vs. Drill: Comparison between the Two Methods in terms of Postoperative Pain, Surgical Times, and Operational Advantages. BioMed Res. Int. 2019, 2019, 8483658. [Google Scholar] [CrossRef]
- Scarano, A.; Lorusso, F.; Brucoli, M.; Lucchina, A.G.; Carinci, F.; Mortellaro, C. Upper Eyelid Blepharoplasty With Voltaic Arc Dermabrasion. J. Craniofacial Surg. 2018, 29, 2263–2266. [Google Scholar] [CrossRef]
- Scarano, A.; Murmura, G.; Vantaggiato, G.; Lauritano, D.; Silvestre-Rangil, J.; DI Cerbo, A.; Lorusso, F. Delayed expansion of atrophic mandible (deam): A case report. ORAL Implantol. 2017, 10, 190–196. [Google Scholar] [CrossRef]
- Lorusso, F.; Conte, R.; Inchingolo, F.; Festa, F.; Scarano, A. Survival Rate of Zygomatic Implants for Fixed Oral Maxillary Rehabilitations: A Systematic Review and Meta-Analysis Comparing Outcomes between Zygomatic and Regular Implants. Dent. J. 2021, 9, 38. [Google Scholar] [CrossRef]
- Place, E.S.; Evans, N.D.; Stevens, M.M. Complexity in biomaterials for tissue engineering. Nat. Mater. 2009, 8, 457–470. [Google Scholar] [CrossRef]
- Leipzig, N.D.; Shoichet, M.S. The effect of substrate stiffness on adult neural stem cell behavior. Biomaterials 2009, 30, 6867–6878. [Google Scholar] [CrossRef]
- Lee, J.; Byun, H.; Perikamana, S.K.M.; Lee, S.; Shin, H. Current Advances in Immunomodulatory Biomaterials for Bone Regeneration. Adv. Healthc. Mater. 2019, 8, 1801106. [Google Scholar] [CrossRef]
- Titsinides, S.; Agrogiannis, G.; Karatzas, T. Bone grafting materials in dentoalveolar reconstruction: A comprehensive review. Jpn. Dent. Sci. Rev. 2019, 55, 26–32. [Google Scholar] [CrossRef] [PubMed]
- Yamada, M.; Egusa, H. Current bone substitutes for implant dentistry. J. Prosthodont. Res. 2018, 62, 152–161. [Google Scholar] [CrossRef] [PubMed]
- Hutton, B.; Salanti, G.; Caldwell, D.M.; Chaimani, A.; Schmid, C.H.; Cameron, C.; Ioannidis, J.P.A.; Straus, S.; Thorlund, K.; Jansen, J.P.; et al. The PRISMA extension statement for reporting of systematic reviews incorporating network meta-analyses of health care interventions: Checklist and explanations. Ann. Intern. Med. 2015, 162, 777–784. [Google Scholar] [CrossRef] [PubMed]
- Giannoudis, P.V.; Dinopoulos, H.; Tsiridis, E. Bone substitutes: An update. Injury 2005, 36, S20–S27. [Google Scholar] [CrossRef]
- Habibah, T.U.; Salisbury, H.G. Hydroxyapatite Dental Material. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2020. [Google Scholar]
- Yamada, S.; Heymann, D.; Bouler, J.M.; Daculsi, G. Osteoclastic resorption of calcium phosphate ceramics with different hydroxyapatite/beta-tricalcium phosphate ratios. Biomaterials 1997, 18, 1037–1041. [Google Scholar] [CrossRef]
- Zwingenberger, S.; Nich, C.; Valladares, R.D.; Yao, Z.; Stiehler, M.; Goodman, S.B. Recommendations and considerations for the use of biologics in orthopedic surgery. BioDrugs 2012, 26, 245–256. [Google Scholar] [CrossRef]
- Ortiz-Puigpelat, O.; Elnayef, B.; Satorres-Nieto, M.; Gargallo-Albiol, J.; Hernández-Alfaro, F. Comparison of Three Biphasic Calcium Phosphate Block Substitutes: A Histologic and Histomorphometric Analysis in the Dog Mandible. Int. J. Periodontics Restor. Dent. 2019, 39, 315–323. [Google Scholar] [CrossRef] [PubMed]
- Prakasam, M.; Locs, J.; Salma-Ancane, K.; Loca, D.; Largeteau, A.; Berzina-Cimdina, L. Biodegradable Materials and Metallic Implants-A Review. J. Funct. Biomater. 2017, 8, 44. [Google Scholar] [CrossRef]
- Polo-Corrales, L.; Latorre-Esteves, M.; Ramirez-Vick, J.E. Scaffold Design for Bone Regeneration. J. Nanosci. Nanotechnol. 2014, 14, 15–56. [Google Scholar] [CrossRef]
- Saulacic, N.; Fujioka-Kobayashi, M.; Kimura, Y.; Bracher, A.I.; Zihlmann, C.; Lang, N.P. The effect of synthetic bone graft substitutes on bone formation in rabbit calvarial defects. J. Mater. Sci. Mater. Med. 2021, 32, 14. [Google Scholar] [CrossRef]
- Bhatt, R.A.; Rozental, T.D. Bone Graft Substitutes. Hand Clin. 2012, 28, 457–468. [Google Scholar] [CrossRef] [PubMed]
- Hutmacher, D.W.; Schantz, J.T.; Lam, C.X.F.; Tan, K.C.; Lim, T.C. State of the art and future directions of scaffold-based bone engineering from a biomaterials perspective. J. Tissue Eng. Regen. Med. 2007, 1, 245–260. [Google Scholar] [CrossRef] [PubMed]
- Nava, M.M.; Draghi, L.; Giordano, C.; Pietrabissa, R. The effect of scaffold pore size in cartilage tissue engineering. J. Appl. Biomater. Funct. Mater. 2016, 14, e223–e229. [Google Scholar] [CrossRef] [PubMed]
- Murphy, C.M.; Haugh, M.G.; O’Brien, F.J. The effect of mean pore size on cell attachment, proliferation and migration in collagen–glycosaminoglycan scaffolds for bone tissue engineering. Biomaterials 2010, 31, 461–466. [Google Scholar] [CrossRef] [PubMed]
- LeGeros, R.Z. Properties of Osteoconductive Biomaterials: Calcium Phosphates. Clin. Orthop. Relat. Res. 2002, 395, 81–98. [Google Scholar] [CrossRef]
- Ghayor, C.; Weber, F.E. Osteoconductive Microarchitecture of Bone Substitutes for Bone Regeneration Revisited. Front. Physiol. 2018, 9, 960. [Google Scholar] [CrossRef]
- Polak, S.J.; Levengood, S.K.L.; Wheeler, M.B.; Maki, A.J.; Clark, S.G.; Johnson, A.J.W. Analysis of the roles of microporosity and BMP-2 on multiple measures of bone regeneration and healing in calcium phosphate scaffolds. Acta Biomater. 2011, 7, 1760–1771. [Google Scholar] [CrossRef]
- Kakuta, A.; Tanaka, T.; Chazono, M.; Komaki, H.; Kitasato, S.; Inagaki, N.; Akiyama, S.; Marumo, K. Effects of micro-porosity and local BMP-2 administration on bioresorption of β-TCP and new bone formation. Biomater. Res. 2019, 23, 12. [Google Scholar] [CrossRef]
- Taktak, R.; Elghazel, A.; Bouaziz, J.; Charfi, S.; Keskes, H. Tricalcium phosphate-Fluorapatite as bone tissue engineering: Evaluation of bioactivity and biocompatibility. Mater. Sci. Eng. C Mater. Biol. Appl. 2018, 86, 121–128. [Google Scholar] [CrossRef]
- Da Silva Brum, I.; de Carvalho, J.J.; da Silva Pires, J.L.; de Carvalho, M.A.A.; Dos Santos, L.B.F.; Elias, C.N. Nanosized hydroxyapatite and β-tricalcium phosphate composite: Physico-chemical, cytotoxicity, morphological properties and in vivo trial. Sci. Rep. 2019, 9, 19602. [Google Scholar] [CrossRef]
- Ebrahimi, M.; Botelho, M.G.; Dorozhkin, S.V. Biphasic calcium phosphates bioceramics (HA/TCP): Concept, physicochemical properties and the impact of standardization of study protocols in biomaterials research. Mater. Sci. Eng. C 2017, 71, 1293–1312. [Google Scholar] [CrossRef] [PubMed]
- Fang, C.-H.; Lin, Y.-W.; Sun, J.-S.; Lin, F.-H. The chitosan/tri-calcium phosphate bio-composite bone cement promotes better osteo-integration: An in vitro and in vivo study. J. Orthop. Surg. Res. 2019, 14, 162. [Google Scholar] [CrossRef] [PubMed]
- De Tullio, I.; Caputi, S.; Perfetti, G.; Mavriqi, L.; Wismeijer, D.; Traini, T. A Human Clinical and Histomorphometrical Study on Different Resorbable and Non-Resorbable Bone Substitutes Used in Post-Extractive Sites. Preliminary Results. Materials 2019, 12, 2408. [Google Scholar] [CrossRef] [PubMed]
- Lin, H.K.; Pan, Y.H.; Salamanca, E.; Lin, Y.T.; Chang, W.J. Prevention of Bone Resorption by HA/β-TCP + Collagen Composite after Tooth Extraction: A Case Series. Int. J. Environ. Res. Public Health 2019, 16, 4616. [Google Scholar] [CrossRef]
- Maji, K.; Dasgupta, S.; Pramanik, K.; Bissoyi, A. Preparation and characterization of gelatin-chitosan-nanoβ-TCP based scaffold for orthopaedic application. Mater. Sci. Eng. C Mater. Biol. Appl. 2018, 86, 83–94. [Google Scholar] [CrossRef]
- Afroze, J.D.; Abden, M.J.; Islam, M.A. An efficient method to prepare magnetic hydroxyapatite-functionalized multi-walled carbon nanotubes nanocomposite for bone defects. Mater. Sci. Eng. C Mater. Biol. Appl. 2018, 86, 95–102. [Google Scholar] [CrossRef]
- Gao, P.; Zhang, H.; Liu, Y.; Fan, B.; Li, X.; Xiao, X.; Lan, P.; Li, M.; Geng, L.; Liu, D.; et al. Beta-tricalcium phosphate granules improve osteogenesis in vitro and establish innovative osteo-regenerators for bone tissue engineering in vivo. Sci. Rep. 2016, 6, 23367. [Google Scholar] [CrossRef]
- Bouler, J.M.; Pilet, P.; Gauthier, O.; Verron, E. Biphasic calcium phosphate ceramics for bone reconstruction: A review of biological response. Acta Biomater. 2017, 53, 1–12. [Google Scholar] [CrossRef]
- Miron, R.J.; Zhang, Y. Next-Generation Biomaterials for Bone & Periodontal Regeneration. Available online: http://www.quintpub.com/display_detail.php3?psku=B7963 (accessed on 30 October 2020).
- Chen, X.; Wang, M.; Chen, F.; Wang, J.; Li, X.; Liang, J.; Fan, Y.; Xiao, Y.; Zhang, X. Correlations between macrophage polarization and osteoinduction of porous calcium phosphate ceramics. Acta Biomater. 2020, 103, 318–332. [Google Scholar] [CrossRef]
- Isacco, C.G.; Nguyen, K.C.D.; Ballini, A.; Paduanelli, G.; Pham, V.H.; Aityan, S.K.; Schiffman, M.; Tran, T.C.; Huynh, T.D.; Filgueira, L.; et al. Innovative Scaffold Solution for Bone Regeneration Made of Beta-Tricalcium Phosphate Granules, Autologous Fibrin Fold, and Peripheral Blood Stem Cells. In Regenerative Medicine and Plastic Surgery: Skin and Soft Tissue, Bone, Cartilage, Muscle, Tendon and Nerves; Duscher, D., Shiffman, M.A., Eds.; Springer International Publishing: Cham, Switzerland, 2019; pp. 167–179. ISBN 978-3-030-19962-3. [Google Scholar]
- Lorusso, F.; Inchingolo, F.; Dipalma, G.; Postiglione, F.; Fulle, S.; Scarano, A. Synthetic Scaffold/Dental Pulp Stem Cell (DPSC) Tissue Engineering Constructs for Bone Defect Treatment: An Animal Studies Literature Review. Int. J. Mol. Sci. 2020, 21, 9765. [Google Scholar] [CrossRef]
- Szponder, T.; Wessely-Szponder, J.; Sobczyńska-Rak, A.; Żylińska, B.; Radzki, R.P.; Polkowska, I. Application of Platelet-rich Plasma and Tricalcium Phosphate in the Treatment of Comminuted Fractures in Animals. In Vivo 2018, 32, 1449–1455. [Google Scholar] [CrossRef] [PubMed]
- Cannio, M.; Bellucci, D.; Roether, J.A.; Boccaccini, D.N.; Cannillo, V. Bioactive Glass Applications: A Literature Review of Human Clinical Trials. Materials 2021, 14, 5440. [Google Scholar] [CrossRef] [PubMed]
- Rau, J.V.; Antoniac, I.; Cama, G.; Komlev, V.S.; Ravaglioli, A. Bioactive Materials for Bone Tissue Engineering. BioMed Res. Int. 2016, 2016, 3741428. [Google Scholar] [CrossRef] [PubMed]
- Eliaz, N.; Metoki, N. Calcium Phosphate Bioceramics: A Review of Their History, Structure, Properties, Coating Technologies and Biomedical Applications. Materials 2017, 10, 334. [Google Scholar] [CrossRef]
- Jones, J.R. Review of bioactive glass: From Hench to hybrids. Acta Biomater. 2013, 9, 4457–4486. [Google Scholar] [CrossRef]
- Antoniac, I.V. (Ed.) Handbook of Bioceramics and Biocomposites; Springer International Publishing: Cham, Switzerland, 2016; ISBN 978-3-319-12459-9. [Google Scholar]
- Maidaniuc, A.; Miculescu, F.; Voicu, S.I.; Andronescu, C.; Miculescu, M.; Matei, E.; Mocanu, A.C.; Pencea, I.; Csaki, I.; Machedon-Pisu, T.; et al. Induced wettability and surface-volume correlation of composition for bovine bone derived hydroxyapatite particles. Appl. Surf. Sci. 2018, 438, 158–166. [Google Scholar] [CrossRef]
- Miculescu, F.; Bojin, D.; Ciocan, L.T.; Antoniac, I.; Miculescu, M.; Miculescu, N. Experimental researches on biomaterial-tissue interface interactions. J. Optoelectron. Adv. Mater. 2007, 9, 3303–3306. [Google Scholar]
- Guazzo, R.; Gardin, C.; Bellin, G.; Sbricoli, L.; Ferroni, L.; Ludovichetti, F.S.; Piattelli, A.; Antoniac, I.; Bressan, E.; Zavan, B. Graphene-Based Nanomaterials for Tissue Engineering in the Dental Field. Nanomaterials 2018, 8, 349. [Google Scholar] [CrossRef]
- Miculescu, F.; Stan, G.E.; Ciocan, L.T.; Miculescu, M.; Berbecaru, A.; Antoniac, I. Cortical Bone as Resource for Producing Biomimetic Materials for Clinical Use. Dig. J. Nanomater. Biostruct. 2012, 7, 1667–1677. [Google Scholar]
- Ravindran, S.; George, A. Dentin Matrix Proteins in Bone Tissue Engineering. Adv. Exp. Med. Biol. 2015, 881, 129–142. [Google Scholar] [CrossRef]
- Hazballa, D.; Inchingolo, A.D.; Inchingolo, A.M.; Malcangi, G.; Santacroce, L.; Minetti, E.; Di Venere, D.; Limongelli, L.; Bordea, I.R.; Scarano, A.; et al. The effectiveness of autologous demineralized tooth graft for the bone ridge preservation: A systematic review of the literature. J. Biol. Regul. Homeost. Agents 2021, 35, 293–294. [Google Scholar] [CrossRef]
- Kim, Y.-K.; Lee, J.; Um, I.-W.; Kim, K.-W.; Murata, M.; Akazawa, T.; Mitsugi, M. Tooth-derived bone graft material. J. Korean Assoc. Oral Maxillofac. Surg. 2013, 39, 103–111. [Google Scholar] [CrossRef] [PubMed]
- Ramalingam, S.; Sundar, C.; Jansen, J.A.; Alghamdi, H. Chapter 1-Alveolar bone science: Structural characteristics and pathological changes. In Dental Implants and Bone Grafts; Alghamdi, H., Jansen, J., Eds.; Woodhead Publishing: Thorston, UK, 2020; pp. 1–22. ISBN 978-0-08-102478-2. [Google Scholar]
- Minetti, E.; Carasco, A.; Carasco, M.; Giacometti, E.; Ho, K.L.H.; Palermo, A.; Savadori, P.; Taschieri, S. Il Dente Come Materiale Da Innesto, 1st ed.; EDRA: Wood Buffalo, AB, Canada, 2020; Volume UNICO, ISBN 978-88-214-5353-3. [Google Scholar]
- Azariah, E.D.S.; Evangeline, A.; Chinnasami, R. Comparison of tooth derived hydroxyapatite with commercially pure hydroxyapatite. Int. J. Oral Maxillofac. Surg. 2017, 46, 365. [Google Scholar] [CrossRef]
- Min, B.; Song, J.S.; Kim, S.-O.; Kim, K.-M.; Park, W.S.; Lee, J.-H. Osteoconduction capacity of human deciduous and permanent teeth ash in a rat calvarial bone defect model. Cell Tissue Bank. 2015, 16, 361–369. [Google Scholar] [CrossRef]
- Wang, F.; Xie, C.; Ren, N.; Bai, S.; Zhao, Y. Human Freeze-dried Dentin Matrix as a Biologically Active Scaffold for Tooth Tissue Engineering. J. Endod. 2019, 45, 1321–1331. [Google Scholar] [CrossRef]
- Li, R.; Guo, W.; Yang, B.; Guo, L.; Sheng, L.; Chen, G.; Li, Y.; Zou, Q.; Xie, D.; An, X.; et al. Human treated dentin matrix as a natural scaffold for complete human dentin tissue regeneration. Biomaterials 2011, 32, 4525–4538. [Google Scholar] [CrossRef]
- Goldberg, M.; Kulkarni, A.B.; Young, M.; Boskey, A. Dentin structure composition and mineralization. Front. Biosci. 2011, E3, 711–735. [Google Scholar] [CrossRef]
- Cantore, S.; Ballini, A.; De Vito, D.; Martelli, F.S.; Georgakopoulos, I.; Almasri, M.; Dibello, V.; Altini, V.; Farronato, G.; Dipalma, G.; et al. Characterization of human apical papilla-derived stem cells. J. Biol. Regul. Homeost. Agents 2017, 31, 901–910. [Google Scholar]
- Campanella, V. Dental Stem Cells: Current research and future applications. Eur. J. Paediatr. Dent. 2018, 19, 257. [Google Scholar] [CrossRef]
- Urist, M.R. Bone: Formation by Autoinduction. Science 1965, 150, 893–899. [Google Scholar] [CrossRef]
- Urist, M.R.; Strates, B.S. Bone Morphogenetic Protein. J. Dent. Res. 1971, 50, 1392–1406. [Google Scholar] [CrossRef] [PubMed]
- Luu, H.H.; Song, W.-X.; Luo, X.; Manning, D.; Luo, J.; Deng, Z.-L.; Sharff, K.A.; Montag, A.G.; Haydon, R.C.; He, T.-C. Distinct roles of bone morphogenetic proteins in osteogenic differentiation of mesenchymal stem cells. J. Orthop. Res. 2007, 25, 665–677. [Google Scholar] [CrossRef] [PubMed]
- Chen, W.-C.; Chung, C.-H.; Lu, Y.-C.; Wu, M.-H.; Chou, P.-H.; Yen, J.-Y.; Lai, Y.-W.; Wang, G.-S.; Liu, S.-C.; Cheng, J.-K.; et al. BMP-2 induces angiogenesis by provoking integrin α6 expression in human endothelial progenitor cells. Biochem. Pharmacol. 2018, 150, 256–266. [Google Scholar] [CrossRef] [PubMed]
- Mostafa, S.; Pakvasa, M.; Coalson, E.; Zhu, A.; Alverdy, A.; Castillo, H.; Fan, J.; Li, A.; Feng, Y.; Wu, D.; et al. The wonders of BMP9: From mesenchymal stem cell differentiation, angiogenesis, neurogenesis, tumorigenesis, and metabolism to regenerative medicine. Genes Dis. 2019, 6, 201–223. [Google Scholar] [CrossRef]
- Bessho, K.; Tanaka, N.; Matsumoto, J.; Tagawa, T.; Murata, M. Human dentin-matrix-derived bone morphogenetic protein. J. Dent. Res. 1991, 70, 171–175. [Google Scholar] [CrossRef]
- Zhang, L.; Luo, Q.; Shu, Y.; Zeng, Z.; Huang, B.; Feng, Y.; Zhang, B.; Wang, X.; Lei, Y.; Ye, Z.; et al. Transcriptomic landscape regulated by the 14 types of bone morphogenetic proteins (BMPs) in lineage commitment and differentiation of mesenchymal stem cells (MSCs). Genes Dis. 2019, 6, 258–275. [Google Scholar] [CrossRef]
- Xiao, W.-L.; Jia, K.-N.; Yu, G.; Zhao, N. Outcomes of bone morphogenetic protein-2 and iliac cancellous bone transplantation on alveolar cleft bone grafting: A meta-analysis. J. Plast. Reconstr. Aesthet. Surg. 2020, 73, 1135–1142. [Google Scholar] [CrossRef]
- Zara, J.N.; Siu, R.K.; Zhang, X.; Shen, J.; Ngo, R.; Lee, M.; Li, W.; Chiang, M.; Chung, J.; Kwak, J.; et al. High doses of bone morphogenetic protein 2 induce structurally abnormal bone and inflammation in vivo. Tissue Eng. Part A 2011, 17, 1389–1399. [Google Scholar] [CrossRef]
- James, A.W.; LaChaud, G.; Shen, J.; Asatrian, G.; Nguyen, V.; Zhang, X.; Ting, K.; Soo, C. A Review of the Clinical Side Effects of Bone Morphogenetic Protein-2. Tissue Eng. Part B Rev. 2016, 22, 284–297. [Google Scholar] [CrossRef]
- Bal, Z.; Kushioka, J.; Kodama, J.; Kaito, T.; Yoshikawa, H.; Korkusuz, P.; Korkusuz, F. BMP and TGFβ use and release in bone regeneration. Turk. J. Med. Sci. 2020, 50, 1707–1722. [Google Scholar] [CrossRef]
- Arabadzhiev, I.; Maurer, P.; Stevao, E. Particulated wisdom teeth as an autologous bone substitute for grafting/filling material in bone defects: Case Report. J. Clin. Exp. Dent. 2020, 12, e424–e428. [Google Scholar] [CrossRef] [PubMed]
- Pohl, V.; Schuh, C.; Fischer, M.; Haas, R. A New Method Using Autogenous Impacted Third Molars for Sinus Augmentation to Enhance Implant Treatment: Case Series with Preliminary Results of an Open, Prospective Longitudinal Study. Int. J. Oral Maxillofac. Implant. 2016, 31, 622–630. [Google Scholar] [CrossRef] [PubMed]
- Pohl, V.; Pohl, S.; Sulzbacher, I.; Fuerhauser, R.; Mailath-Pokorny, G.; Haas, R. Alveolar Ridge Augmentation Using Dystopic Autogenous Tooth: 2-Year Results of an Open Prospective Study. Int. J. Oral Maxillofac. Implant. 2017, 32, 870–879. [Google Scholar] [CrossRef] [PubMed]
- Um, I.W. Demineralized Dentin Matrix (DDM) As a Carrier for Recombinant Human Bone Morphogenetic Proteins (rhBMP-2). Adv. Exp. Med. Biol. 2018, 1077, 487–499. [Google Scholar] [CrossRef]
- Rijal, G.; Shin, H.-I. Human tooth-derived biomaterial as a graft substitute for hard tissue regeneration. Regen. Med. 2017, 12, 263–273. [Google Scholar] [CrossRef]
- Gharpure, A.S.; Bhatavadekar, N.B. Clinical Efficacy of Tooth-Bone Graft: A Systematic Review and Risk of Bias Analysis of Randomized Control Trials and Observational Studies. Implant Dent. 2018, 27, 119–134. [Google Scholar] [CrossRef]
- Minetti, E.; Berardini, M.; Trisi, P. A New Tooth Processing Apparatus Allowing to Obtain Dentin Grafts for Bone Augmentation: The Tooth Transformer. Open Dent. J. 2019, 13, 6–14. [Google Scholar] [CrossRef]
- Koga, T.; Minamizato, T.; Kawai, Y.; Miura, K.I.T.; Nakatani, Y.; Sumita, Y.; Asahina, I. Bone Regeneration Using Dentin Matrix Depends on the Degree of Demineralization and Particle Size. PLoS ONE 2016, 11, e0147235. [Google Scholar] [CrossRef]
- Bono, N.; Tarsini, P.; Candiani, G. Demineralized dentin and enamel matrices as suitable substrates for bone regeneration. J. Appl. Biomater. Funct. Mater. 2017, 15, 236–243. [Google Scholar] [CrossRef]
- Kim, Y.-K.; Lee, J.; Kim, K.-W.; Um, I.-W.; Murata, M.; Ito, K. Analysis of Organic Components and Osteoinductivity in Autogenous Tooth Bone Graft Material. Maxillofac. Plast. Reconstr. Surg. 2013, 35, 353–359. [Google Scholar] [CrossRef]
- Hedenbjörk-Lager, A.; Hamberg, K.; Pääkkönen, V.; Tjäderhane, L.; Ericson, D. Collagen degradation and preservation of MMP-8 activity in human dentine matrix after demineralization. Arch. Oral Biol. 2016, 68, 66–72. [Google Scholar] [CrossRef] [PubMed]
- Bono, N.; Tarsini, P.; Candiani, G. BMP-2 and type I collagen preservation in human deciduous teeth after demineralization. J. Appl. Biomater. Funct. Mater. 2019, 17, 2280800018784230. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.-K.; Kim, S.-G.; Yun, P.-Y.; Yeo, I.-S.; Jin, S.-C.; Oh, J.-S.; Kim, H.-J.; Yu, S.-K.; Lee, S.-Y.; Kim, J.-S.; et al. Autogenous teeth used for bone grafting: A comparison with traditional grafting materials. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2014, 117, e39–e45. [Google Scholar] [CrossRef] [PubMed]
- Minetti, E.; Giacometti, E.; Gambardella, U.; Contessi, M.; Ballini, A.; Marenzi, G.; Celko, M.; Mastrangelo, F. Alveolar Socket Preservation with Different Autologous Graft Materials: Preliminary Results of a Multicenter Pilot Study in Human. Materials 2020, 13, 1153. [Google Scholar] [CrossRef] [PubMed]
- Minetti, E.; Palermo, A.; Ferrante, F.; Schmitz, J.H.; Ho, H.K.L.; Hann, S.N.D.; Giacometti, E.; Gambardella, U.; Contessi, M.; Celko, M.; et al. Autologous Tooth Graft after Endodontical Treated Used for Socket Preservation: A Multicenter Clinical Study. Appl. Sci. 2019, 9, 5396. [Google Scholar] [CrossRef]
- Minetti, E.; Palermo, A.; Contessi, M.; Gambardella, U.; Schmitz, J.H.; Giacometti, E.; Celko, M.; Trisi, P. Autologous tooth graft for maxillary sinus augmentation: A multicenter clinical study. Int. J. Growth Factors Stem Cells Dent. 2019, 2, 45. [Google Scholar] [CrossRef]
- Umebayashi, M.; Ohba, S.; Kurogi, T.; Noda, S.; Asahina, I. Full Regeneration of Maxillary Alveolar Bone Using Autogenous Partially Demineralized Dentin Matrix and Particulate Cancellous Bone and Marrow for Implant-Supported Full Arch Rehabilitation. J. Oral Implant. 2020, 46, 122–127. [Google Scholar] [CrossRef]
- Minetti, E.; Savadori, P.; Barlattani, A.; Franco, R.; Michele, M.; Gianfreda, F.; Bollero, P. Autologous tooth graft: A histological comparison between dentin mixed with xenograft and dentin alone grafts in socket preservation. J. Biol. Regul. Homeost. Agents 2019, 33, 189–197. [Google Scholar]
- Liu, X.; Li, Q.; Wang, F.; Wang, Z. Maxillary sinus floor augmentation and dental implant placement using dentin matrix protein-1 gene-modified bone marrow stromal cells mixed with deproteinized boving bone: A comparative study in beagles. Arch. Oral Biol. 2016, 64, 102–108. [Google Scholar] [CrossRef]
- Andrade, C.; Camino, J.; Nally, M.; Quirynen, M.; Martínez, B.; Pinto, N. Combining autologous particulate dentin, L-PRF, and fibrinogen to create a matrix for predictable ridge preservation: A pilot clinical study. Clin. Oral Investig. 2020, 24, 1151–1160. [Google Scholar] [CrossRef]
- Rincón-López, J.A.; Hermann-Muñoz, J.A.; Giraldo-Betancur, A.L.; De Vizcaya-Ruiz, A.; Alvarado-Orozco, J.M.; Muñoz-Saldaña, J. Synthesis, Characterization and In Vitro Study of Synthetic and Bovine-Derived Hydroxyapatite Ceramics: A Comparison. Materials 2018, 11, 333. [Google Scholar] [CrossRef] [PubMed]
- Testori, T.; Wallace, S.S.; Trisi, P.; Capelli, M.; Zuffetti, F.; Del Fabbro, M. Effect of xenograft (ABBM) particle size on vital bone formation following maxillary sinus augmentation: A multicenter, randomized, controlled, clinical histomorphometric trial. Int. J. Periodontics Restor. Dent. 2013, 33, 467–475. [Google Scholar] [CrossRef] [PubMed]
- Kon, K.; Shiota, M.; Ozeki, M.; Kasugai, S. The Effect of Graft Bone Particle Size on Bone Augmentation in a Rabbit Cranial Vertical Augmentation Model: A Microcomputed Tomography Study. Int. J. Oral Maxillofac. Implant. 2014, 29, 402–406. [Google Scholar] [CrossRef] [PubMed]
- Berglundh, T.; Lindhe, J. Healing around implants placed in bone defects treated with Bio-OssR. An experimental study in the dog. Clin. Oral Implant. Res. 1997, 8, 117–124. [Google Scholar] [CrossRef]
- Tapety, F.I.; Amizuka, N.; Uoshima, K.; Nomura, S.; Maeda, T. A histological evaluation of the involvement of Bio-Oss in osteoblastic differentiation and matrix synthesis. Clin. Oral Implant. Res. 2004, 15, 315–324. [Google Scholar] [CrossRef]
- Orsini, G.; Traini, T.; Scarano, A.; Degidi, M.; Perrotti, V.; Piccirilli, M.; Piattelli, A. Maxillary sinus augmentation with Bio-Oss particles: A light, scanning, and transmission electron microscopy study in man. J. Biomed. Mater. Res. Part B Appl. Biomater. 2005, 74, 448–457. [Google Scholar] [CrossRef]
- Piattelli, M.; Favero, G.A.; Scarano, A.; Orsini, G.; Piattelli, A. Bone reactions to anorganic bovine bone (Bio-Oss) used in sinus augmentation procedures: A histologic long-term report of 20 cases in humans. Int. J. Oral Maxillofac. Implant. 1999, 14, 835–840. [Google Scholar]
- Hofman, S.; Sidqui, M.; Abensur, D.; Valentini, P.; Missika, P. Effects of Laddec on the formation of calcified bone matrix in rat calvariae cells culture. Biomaterials 1999, 20, 1155–1166. [Google Scholar] [CrossRef]
- Artzi, Z.; Weinreb, M.; Givol, N.; Rohrer, M.D.; Nemcovsky, C.E.; Prasad, H.S.; Tal, H. Biomaterial Resorption Rate and Healing Site Morphology of Inorganic Bovine Bone and beta-Tricalcium Phosphate in the Canine: A 24-month Longitudinal Histologic Study and Morphometric Analysis. Int. J. Oral Maxillofac. Implant. 2004, 19, 357–368. [Google Scholar]
- Sánchez, A.; Eckert, S.; Sheridan, P.; Weaver, A. Influence of platelet-rich plasma added to xenogeneic bone grafts on bone mineral density associated with dental implants. Int. J. Oral Maxillofac. Implant. 2005, 20, 526–532. [Google Scholar]
- Tatullo, M.; Marrelli, M.; Cassetta, M.; Pacifici, A.; Stefanelli, L.V.; Scacco, S.; Dipalma, G.; Pacifici, L.; Inchingolo, F. Platelet Rich Fibrin (P.R.F.) in reconstructive surgery of atrophied maxillary bones: Clinical and histological evaluations. Int. J. Med. Sci. 2012, 9, 872–880. [Google Scholar] [CrossRef] [PubMed]
- Do Lago, E.S.; Ferreira, S.; Garcia, I.R.; Okamoto, R.; Mariano, R.C. Improvement of bone repair with l-PRF and bovine bone in calvaria of rats. histometric and immunohistochemical study. Clin. Oral Investig. 2020, 24, 1637–1650. [Google Scholar] [CrossRef]
- You, J.-S.; Kim, S.-G.; Oh, J.-S.; Kim, J.-S. Effects of Platelet-Derived Material (Platelet-Rich Fibrin) on Bone Regeneration. Implant Dent. 2019, 28, 244–255. [Google Scholar] [CrossRef] [PubMed]
- Dohan Ehrenfest, D.M.; Del Corso, M.; Diss, A.; Mouhyi, J.; Charrier, J.-B. Three-dimensional architecture and cell composition of a Choukroun’s platelet-rich fibrin clot and membrane. J. Periodontol. 2010, 81, 546–555. [Google Scholar] [CrossRef] [PubMed]
- Simonpieri, A.; Del Corso, M.; Vervelle, A.; Jimbo, R.; Inchingolo, F.; Sammartino, G.; Dohan Ehrenfest, D.M. Current knowledge and perspectives for the use of platelet-rich plasma (PRP) and platelet-rich fibrin (PRF) in oral and maxillofacial surgery part 2: Bone graft, implant and reconstructive surgery. Curr. Pharm. Biotechnol. 2012, 13, 1231–1256. [Google Scholar] [CrossRef] [PubMed]
- He, L.; Lin, Y.; Hu, X.; Zhang, Y.; Wu, H. A comparative study of platelet-rich fibrin (PRF) and platelet-rich plasma (PRP) on the effect of proliferation and differentiation of rat osteoblasts in vitro. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2009, 108, 707–713. [Google Scholar] [CrossRef] [PubMed]
- Dohan Ehrenfest, D.M.; Rasmusson, L.; Albrektsson, T. Classification of platelet concentrates: From pure platelet-rich plasma (P-PRP) to leucocyte- and platelet-rich fibrin (L-PRF). Trends Biotechnol. 2009, 27, 158–167. [Google Scholar] [CrossRef]
- Dohan Ehrenfest, D.M.; Bielecki, T.; Del Corso, M.; Inchingolo, F.; Sammartino, G. Shedding light in the controversial terminology for platelet-rich products: Platelet-rich plasma (PRP), platelet-rich fibrin (PRF), platelet-leukocyte gel (PLG), preparation rich in growth factors (PRGF), classification and commercialism. J. Biomed. Mater. Res. A 2010, 95, 1280–1282. [Google Scholar] [CrossRef]
- Del Corso, M.; Vervelle, A.; Simonpieri, A.; Jimbo, R.; Inchingolo, F.; Sammartino, G.; Dohan Ehrenfest, D.M. Current knowledge and perspectives for the use of platelet-rich plasma (PRP) and platelet-rich fibrin (PRF) in oral and maxillofacial surgery part 1: Periodontal and dentoalveolar surgery. Curr. Pharm. Biotechnol. 2012, 13, 1207–1230. [Google Scholar] [CrossRef]
- Dohan Ehrenfest, D.M.; Bielecki, T.; Jimbo, R.; Barbé, G.; Del Corso, M.; Inchingolo, F.; Sammartino, G. Do the fibrin architecture and leukocyte content influence the growth factor release of platelet concentrates? An evidence-based answer comparing a pure platelet-rich plasma (P-PRP) gel and a leukocyte- and platelet-rich fibrin (L-PRF). Curr. Pharm. Biotechnol. 2012, 13, 1145–1152. [Google Scholar] [CrossRef]
- Dohan Ehrenfest, D.M.; Bielecki, T.; Mishra, A.; Borzini, P.; Inchingolo, F.; Sammartino, G.; Rasmusson, L.; Everts, P.A. In search of a consensus terminology in the field of platelet concentrates for surgical use: Platelet-rich plasma (PRP), platelet-rich fibrin (PRF), fibrin gel polymerization and leukocytes. Curr. Pharm. Biotechnol. 2012, 13, 1131–1137. [Google Scholar] [CrossRef] [PubMed]
- Inchingolo, F.; Cantore, S.; Dipalma, G.; Georgakopoulos, I.; Almasri, M.; Gheno, E.; Motta, A.; Marrelli, M.; Farronato, D.; Ballini, A.; et al. Platelet rich fibrin in the management of medication-related osteonecrosis of the jaw: A clinical and histopathological evaluation. J. Biol. Regul. Homeost. Agents 2017, 31, 811–816. [Google Scholar] [PubMed]
- Ehrenfest, D.M.D.; Corso, M.D.; Inchingolo, F.; Charrier, J.-B. Selecting a relevant in vitro cell model for testing and comparing the effects of a Choukroun’s platelet-rich fibrin (PRF) membrane and a platelet-rich plasma (PRP) gel: Tricks and traps. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2010, 110, 409–411. [Google Scholar] [CrossRef] [PubMed]
- Inchingolo, F.; Tatullo, M.; Marrelli, M.; Inchingolo, A.M.; Scacco, S.; Inchingolo, A.D.; Dipalma, G.; Vermesan, D.; Abbinante, A.; Cagiano, R. Trial with Platelet-Rich Fibrin and Bio-Oss used as grafting materials in the treatment of the severe maxillar bone atrophy: Clinical and radiological evaluations. Eur. Rev. Med. Pharmacol. Sci. 2010, 14, 1075–1084. [Google Scholar]
- Gheno, E.; Palermo, A.; Rodella, L.F.; Buffoli, B. The effectiveness of the use of xenogeneic bone blocks mixed with autologous Concentrated Growth Factors (CGF) in bone regeneration techniques: A case series. J. Osseointegr. 2014, 6, 37–42. [Google Scholar] [CrossRef]
- Rodella, L.F.; Favero, G.; Boninsegna, R.; Buffoli, B.; Labanca, M.; Scarì, G.; Sacco, L.; Batani, T.; Rezzani, R. Growth factors, CD34 positive cells, and fibrin network analysis in concentrated growth factors fraction. Microsc. Res. Tech. 2011, 74, 772–777. [Google Scholar] [CrossRef]
- Huh, J.B.; Yang, J.J.; Choi, K.H.; Bae, J.H.; Lee, J.Y.; Kim, S.E.; Shin, S.-W. Effect of rhBMP-2 immobilized anorganic bovine bone matrix on bone regeneration. Int. J. Mol. Sci. 2015, 16, 16034. [Google Scholar] [CrossRef]
- Temmerman, A.; Cortellini, S.; Van Dessel, J.; De Greef, A.; Jacobs, R.; Dhondt, R.; Teughels, W.; Quirynen, M. Bovine-derived xenograft in combination with autogenous bone chips versus xenograft alone for the augmentation of bony dehiscences around oral implants: A randomized, controlled, split-mouth clinical trial. J. Clin. Periodontol. 2020, 47, 110–119. [Google Scholar] [CrossRef]
- Bracey, D.N.; Cignetti, N.E.; Jinnah, A.H.; Stone, A.V.; Gyr, B.M.; Whitlock, P.W.; Scott, A.T. Bone xenotransplantation: A review of the history, orthopedic clinical literature, and a single-center case series. Xenotransplantation 2020, 27, e12600. [Google Scholar] [CrossRef]
- Terry, L.A.; Jenkins, R.; Thorne, L.; Everest, S.J.; Chaplin, M.J.; Davis, L.A.; Stack, M.J. First case of H-type bovine spongiform encephalopathy identified in Great Britain. Vet. Rec. 2007, 160, 873–874. [Google Scholar] [CrossRef]
- Singh, G.; Kumari, B.; Grover, H.S.; Mahajan, A.; Jabeen, F.; Kumar, A. Application of Platelet Rich Fibrin, Platelet Rich Plasma, Plasma Rich Growth Factors in Different Fields of Dentistry: An Overview. J. Complementary Altern. Med. Res. 2020, 11, 12–23. [Google Scholar] [CrossRef]
- Isobe, K.; Watanebe, T.; Kawabata, H.; Kitamura, Y.; Okudera, T.; Okudera, H.; Uematsu, K.; Okuda, K.; Nakata, K.; Tanaka, T.; et al. Mechanical and degradation properties of advanced platelet-rich fibrin (A-PRF), concentrated growth factors (CGF), and platelet-poor plasma-derived fibrin (PPTF). Int. J. Implant Dent. 2017, 3, 17. [Google Scholar] [CrossRef] [PubMed]
- Inchingolo, F.; Tatullo, M.; Marrelli, M.; Inchingolo, A.M.; Inchingolo, A.D.; Dipalma, G.; Flace, P.; Girolamo, F.; Tarullo, A.; Laino, L.; et al. Regenerative surgery performed with platelet-rich plasma used in sinus lift elevation before dental implant surgery: An useful aid in healing and regeneration of bone tissue. Eur. Rev. Med. Pharmacol. Sci. 2012, 16, 1222–1226. [Google Scholar] [PubMed]
- Dohan Ehrenfest, D.M.; Andia, I.; Zumstein, M.A.; Zhang, C.-Q.; Pinto, N.R.; Bielecki, T. Classification of platelet concentrates (Platelet-Rich Plasma-PRP, Platelet-Rich Fibrin-PRF) for topical and infiltrative use in orthopedic and sports medicine: Current consensus, clinical implications and perspectives. Muscles Ligaments Tendons J. 2014, 4, 3–9. [Google Scholar] [CrossRef]
- Rocha, C.A.; Arantes, R.V.N.; Cestari, T.M.; Santos, P.S.; Assis, G.F.; Taga, R. Maxillary sinus lift response to platelet-rich plasma associated with autogenous bone, ceramic biphasic HA/β-TCP (70:30), or deproteinized bovine bone. Int. J. Implant Dent. 2020, 6, 79. [Google Scholar] [CrossRef]
- Srivastava, S.; Kalburgi, V.; Jain, K.; Modi, S.; Gupta, A.; Rajendra, R.S. Platelet-Rich Fibrin: Its Role in Advanced Surgical Dentistry-A Review. Int. J. Drug Res. Dent. Sci. 2020, 2, 16–22. [Google Scholar] [CrossRef]
- Choukroun, J.; Miron, R.J. Platelet Rich Fibrin: A Second-Generation Platelet Concentrate. In Platelet Rich Fibrin in Regenerative Dentistry: Biological Background and Clinical Indications; Miron, R.J., Choukroun, J., Eds.; John Wiley & Sons, Ltd: Oxford, UK, 2017; pp. 1–14. ISBN 978-1-119-40679-2. [Google Scholar]
- Fujioka-Kobayashi, M.; Miron, R.J. Biological Components of Platelet Rich Fibrin: Growth Factor Release and Cellular Activity. In Platelet Rich Fibrin in Regenerative Dentistry: Biological Background and Clinical Indications; Miron, R.J., Choukroun, J., Eds.; John Wiley & Sons, Ltd: Oxford, UK, 2017; pp. 15–31. ISBN 978-1-119-40679-2. [Google Scholar]
- Öncü, E.; Bayram, B.; Kantarcı, A.; Gülsever, S.; Alaaddinoğlu, E.-E. Posıtıve effect of platelet rich fibrin on osseointegration. Med. Oral Patol. Oral Cir. Bucal. 2016, 21, e601–e607. [Google Scholar] [CrossRef]
- Miron, R.J.; Pikos, M.A.; Zhang, Y.; Fretwurst, T. Guided Bone Regeneration with Platelet Rich Fibrin. In Platelet Rich Fibrin in Regenerative Dentistry: Biological Background and Clinical Indications; Miron, R.J., Choukroun, J., Eds.; John Wiley & Sons, Ltd.: Oxford, UK, 2017; pp. 159–183. ISBN 978-1-119-40679-2. [Google Scholar]
- Dohan, D.M.; Choukroun, J.; Diss, A.; Dohan, S.L.; Dohan, A.J.J.; Mouhyi, J.; Gogly, B. Platelet-rich fibrin (PRF): A second-generation platelet concentrate. Part III: Leucocyte activation: A new feature for platelet concentrates? Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2006, 101, e51–e55. [Google Scholar] [CrossRef]
- Barrientos, S.; Stojadinovic, O.; Golinko, M.S.; Brem, H.; Tomic-Canic, M. Growth factors and cytokines in wound healing. Wound Repair Regen. 2008, 16, 585–601. [Google Scholar] [CrossRef]
- Pitzurra, L.; Jansen, I.D.C.; de Vries, T.J.; Hoogenkamp, M.A.; Loos, B.G. Effects of L-PRF and A-PRF+ on periodontal fibroblasts in in vitro wound healing experiments. J. Periodontal Res. 2020, 55, 287–295. [Google Scholar] [CrossRef]
- Choukroun, J.; Diss, A.; Simonpieri, A.; Girard, M.-O.; Schoeffler, C.; Dohan, S.L.; Dohan, A.; Mouhyi, J.; Dohan, D.M. Platelet-rich fibrin (PRF): A second-generation platelet concentrate. Part IV: Clinical effects on tissue healing. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2006, 101, e56–e60. [Google Scholar] [CrossRef] [PubMed]
- Inchingolo, F.; Tarullo, A.; Cagiano, R.; Resta, G.; Dipalma, G.; Inchingolo, A.M.; Tarullo, A.; Scacco, S.; Marrelli, M.; Corti, L.; et al. Successful use of a topical mixture with ozolipoile in the treatment of actinic ulcers. Clin. Cosmet. Investig. Dermatol. 2015, 8, 147–150. [Google Scholar] [CrossRef] [PubMed]
- Feng, M.; Wang, Y.; Zhang, P.; Zhao, Q.; Yu, S.; Shen, K.; Miron, R.J.; Zhang, Y. Antibacterial effects of platelet-rich fibrin produced by horizontal centrifugation. Int. J. Oral Sci. 2020, 12, 32. [Google Scholar] [CrossRef] [PubMed]
- Toeroek, R.; Ehrenfest, D.M.D. The concept of Screw-Guided Bone Regeneration (S-GBR). Part 3: Fast Screw-Guided Bone Regeneration (FS-GBR) in the severely resorbed preimplant posterior mandible using allograft and Leukocyte-and Platelet-Rich Fibrin (L-PRF): A 4-year follow-up. POSEIDO J. 2013, 1, 93–100. [Google Scholar]
- Balčiūnaitė, A.; Rusilas, H.; Žilinskas, J. Use of platelet-rich fibrin versus connective tissue graft in treatment of gingival recessions: Literature review. Stomatologija 2020, 21, 58–64. [Google Scholar]
- Crisci, A.; Conte, A.; Crisci, M.; Cardillo, F. Second Generation Platelet Concentrates-L-PRF (Fibrin Rich in Platelets and Leukocytes) and Its Derivatives (A-PRF, I-PRF)-: Morphological Characteristics to be Used in Modern Regenerative Surgery. Experimental Research. J. Clin. Haematol. 2020, 1, 90–102. [Google Scholar]
- Ehrenfest, D.M.D. How to optimize the preparation of leukocyte- and platelet-rich fibrin (L-PRF, Choukroun’s technique) clots and membranes: Introducing the PRF Box. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2010, 110, 275–278. [Google Scholar] [CrossRef]
- Silfradent Srl-Medifuge MF 200: A Special Blood Separator for Tissue and Bone Regeneration, Platelets + Concentrated Growth Factors. Available online: https://www.infodent.com/showroom?op=rec&id=1879 (accessed on 20 December 2020).
- Bernardi, S.; Mummolo, S.; Tecco, S.; Continenza, M.; Marzo, G. Histological Characterization of Sacco’s Concentrated Growth Factors Membrane. Int. J. Morphol. 2017, 35, 114–119. [Google Scholar] [CrossRef]
- Zhang, L.; Ai, H. Concentrated growth factor promotes proliferation, osteogenic differentiation, and angiogenic potential of rabbit periosteum-derived cells in vitro. J. Orthop. Surg. Res. 2019, 14, 146. [Google Scholar] [CrossRef]
- Borsani, E.; Buffoli, B.; Bonazza, V.; Brunelli, G.; Monini, L.; Inchingolo, F.; Ballini, A.; Rezzani, R.; Rodella, L.F. In vitro effects of concentrated growth factors (CGF) on human SH-SY5Y neuronal cells. Eur. Rev. Med. Pharmacol Sci. 2020, 24, 304–314. [Google Scholar] [CrossRef]
- Masuki, H.; Okudera, T.; Watanebe, T.; Suzuki, M.; Nishiyama, K.; Okudera, H.; Nakata, K.; Uematsu, K.; Su, C.-Y.; Kawase, T. Growth factor and pro-inflammatory cytokine contents in platelet-rich plasma (PRP), plasma rich in growth factors (PRGF), advanced platelet-rich fibrin (A-PRF), and concentrated growth factors (CGF). Int. J. Implant Dent. 2016, 2, 19. [Google Scholar] [CrossRef] [PubMed]
- Kawase, T.; Okuda, K.; Wolff, L.F.; Yoshie, H. Platelet-Rich Plasma-Derived Fibrin Clot Formation Stimulates Collagen Synthesis in Periodontal Ligament and Osteoblastic Cells In Vitro. J. Periodontol. 2003, 74, 858–864. [Google Scholar] [CrossRef] [PubMed]
- Kawase, T.; Okuda, K.; Saito, Y.; Yoshie, H. In Vitro Evidence That the Biological Effects of Platelet-Rich Plasma on Periodontal Ligament Cells Is Not Mediated Solely by Constituent Transforming-Growth Factor-β or Platelet-Derived Growth Factor. J. Periodontol. 2005, 76, 760–767. [Google Scholar] [CrossRef] [PubMed]
- Bonazza, V.; Hajistilly, C.; Patel, D.; Patel, J.; Woo, R.; Cocchi, M.A.; Buffoli, B.; Lancini, D.; Gheno, E.; Rezzani, R.; et al. Growth Factors Release From Concentrated Growth Factors: Effect of β-Tricalcium Phosphate Addition. J. Craniofac. Surg. 2018, 29, 2291–2295. [Google Scholar] [CrossRef] [PubMed]
- Mourão, C.F.; Gheno, E.; Lourenço, E.; Barbosa, R.; Kurtzman, G.; Javid, K.; Mavropoulos, E.; Benedicenti, S.; Maia, M.; Machado, R.; et al. Characterization of a new membrane from concentrated growth factors associated with denaturized albumin (Alb-Cgf) for clinical applications: A preliminary study. Int. J. Growth Factors Stem Cells Dent. 2018, 1, 64–69. [Google Scholar] [CrossRef]
- Fujioka-Kobayashi, M.; Schaller, B.; De Almeida Barros Mourão, C.F.; Zhang, Y.; Sculean, A.; Miron, R.J. Biological characterization of an injectable platelet-rich fibrin mixture consisting of autologous albumin gel and liquid platelet-rich fibrin (Alb-PRF). Platelets 2020, 32, 74–81. [Google Scholar] [CrossRef]
- Palermo, A.; Ferrante, F.; Stanca, E.; Damiano, F.; Gnoni, A.; Batani, T.; Carluccio, M.A.; Demitri, C.; Siculella, L. Release of VEGF from Dental Implant Surface (IML® Implant) Coated with Concentrated Growth Factors (CGF) and the Liquid Phase of CGF (LPCGF): In Vitro Results and Future Expectations. Appl. Sci. 2019, 9, 2114. [Google Scholar] [CrossRef]
- Gheno, E.; Carlos Fernando de Almeida Barros, C.; de Mello-Machado, R.C.; Lourenço, E.S.; Miron, R.J.; Catarino, K.F.F.; Alves, A.T.; Alves, G.G.; Calasans-Maia, M.D. In vivo evaluation of the biocompatibility and biodegradation of a new denatured plasma membrane combined with liquid PRF (Alb-PRF). Platelets 2020, 32, 542–554. [Google Scholar] [CrossRef]
- De Almeida Barros, M.C.F.; Javid, K. New and improved platelet-rich fibrin membranes. Int. J. Growth Factors Stem Cells Dent. 2020, 3, 1. [Google Scholar] [CrossRef]
- Ayoub, A.H.; Belal, S.M.; Ramadan, O. Comparative Histologic and Radiographic Evaluation of Alveolar Ridge Preservation in Esthetic Zone Using Concentrated Growth Factors Associated with Denaturated Albumin (Alb-CGF) and Albumin Coated Bone Allograft. EC Dent. Sci. 2019, 18, 2221–2231. [Google Scholar]
- Borsani, E.; Bonazza, V.; Buffoli, B.; Nocini, P.F.; Albanese, M.; Zotti, F.; Inchingolo, F.; Rezzani, R.; Rodella, L.F. Beneficial Effects of Concentrated Growth Factors and Resveratrol on Human Osteoblasts In Vitro Treated with Bisphosphonates. Biomed Res. Int. 2018, 2018, 4597321. [Google Scholar] [CrossRef] [PubMed]
- Yifat, M.; Hila, E.; Avraham, H.; Inchingolo, F.; Mortellaro, C.; Peleg, O.; Mijiritsky, E. Histologic and Radiographic Characteristics of Bone Filler Under Bisphosphonates. J. Craniofacial Surg. 2019, 30, 1085–1088. [Google Scholar] [CrossRef] [PubMed]
- Contaldo, M.; Luzzi, V.; Ierardo, G.; Raimondo, E.; Boccellino, M.; Ferati, K.; Bexheti-Ferati, A.; Inchingolo, F.; Di Domenico, M.; Serpico, R.; et al. Bisphosphonate-related osteonecrosis of the jaws and dental surgery procedures in children and young people with osteogenesis imperfecta: A systematic review. J. Stomatol. Oral Maxillofac. Surg. 2020, 121, 556–562. [Google Scholar] [CrossRef] [PubMed]
- Ziebart, T.; Pabst, A.; Klein, M.O.; Kämmerer, P.; Gauss, L.; Brüllmann, D.; Al-Nawas, B.; Walter, C. Bisphosphonates: Restrictions for vasculogenesis and angiogenesis: Inhibition of cell function of endothelial progenitor cells and mature endothelial cells in vitro. Clin. Oral Investig. 2011, 15, 105–111. [Google Scholar] [CrossRef] [PubMed]
- Bonazza, V.; Borsani, E.; Buffoli, B.; Parolini, S.; Inchingolo, F.; Rezzani, R.; Rodella, L.F. In vitro treatment with concentrated growth factors (CGF) and sodium orthosilicate positively affects cell renewal in three different human cell lines: An in vitro approach for tissue regeneration. Cell Biol. Int. 2018, 42, 353–364. [Google Scholar] [CrossRef]
- Wang, Q.; Liu, J.; Guo, T.; Liu, D.; Pan, J. Epidermal Growth Factor Reverses the Inhibitory Effects of the Bisphosphonate, Zoledronic Acid, on Human Oral Keratinocytes and Human Vascular Endothelial Cells In Vitro via the Epidermal Growth Factor Receptor (EGFR)/Akt/Phosphoinositide 3-Kinase (PI3K) Signaling Pathway. Med. Sci. Monit. 2019, 25, 700–710. [Google Scholar] [CrossRef]
- Durmuşlar, M.C.; Ballı, U.; Öngöz Dede, F.; Bozkurt Doğan, Ş.; Mısır, A.F.; Barış, E.; Yılmaz, Z.; Çelik, H.H.; Vatansever, A. Evaluation of the effects of platelet-rich fibrin on bone regeneration in diabetic rabbits. J. Cranio-Maxillofac. Surg. 2016, 44, 126–133. [Google Scholar] [CrossRef]
- Nagata, M.J.H.; Santinoni, C.S.; Pola, N.M.; de Campos, N.; Messora, M.R.; Bomfim, S.R.M.; Ervolino, E.; Fucini, S.E.; Faleiros, P.L.; Garcia, V.G.; et al. Bone marrow aspirate combined with low-level laser therapy: A new therapeutic approach to enhance bone healing. J. Photochem. Photobiol. B Biol. 2013, 121, 6–14. [Google Scholar] [CrossRef]
- Garcia, V.G.; Sahyon, A.S.; Longo, M.; Fernandes, L.A.; Gualberto Junior, E.C.; Novaes, V.C.N.; Ervolino, E.; de Almeida, J.M.; Theodoro, L.H. Effect of LLLT on autogenous bone grafts in the repair of critical size defects in the calvaria of immunosuppressed rats. J. Cranio-Maxillofac. Surg. 2014, 42, 1196–1202. [Google Scholar] [CrossRef]
- Saygun, I.; Nizam, N.; Ural, A.U.; Serdar, M.A.; Avcu, F.; Tözüm, T.F. Low-Level Laser Irradiation Affects the Release of Basic Fibroblast Growth Factor (bFGF), Insulin-Like Growth Factor-I (IGF-I), and Receptor of IGF-I (IGFBP3) from Osteoblasts. Photomed. Laser Surg. 2012, 30, 149–154. [Google Scholar] [CrossRef]
- Cunha, M.J.S.; Esper, L.A.; Sbrana, M.C.; de Oliveira, P.G.F.P.; do Valle, A.L.; de Almeida, A.L.P.F. Effect of Low-Level Laser on Bone Defects Treated with Bovine or Autogenous Bone Grafts: In Vivo Study in Rat Calvaria. BioMed Res. Int. 2014, 2014, 104230. [Google Scholar] [CrossRef] [PubMed]
- De Oliveira, G.J.P.L.; Aroni, M.A.T.; Medeiros, M.C.; Marcantonio, E.; Marcantonio, R.A.C. Effect of low-level laser therapy on the healing of sites grafted with coagulum, deproteinized bovine bone, and biphasic ceramic made of hydroxyapatite and β-tricalcium phosphate. In vivo study in rats: Effect of lllt on bone grafted areas. Lasers Surg. Med. 2018, 50, 651–660. [Google Scholar] [CrossRef] [PubMed]
- De Oliveira, G.J.P.L.; Aroni, M.A.T.; Pinotti, F.E.; Marcantonio, E.; Marcantonio, R.A.C. Low-level laser therapy (LLLT) in sites grafted with osteoconductive bone substitutes improves osseointegration. Lasers Med. Sci. 2020, 35, 1519–1529. [Google Scholar] [CrossRef] [PubMed]
- De Martinez Gerbi, M.E.M.; Miranda, J.M.; de Arruda, J.A.A.; Moreno, L.M.M.; Carneiro, V.S.M.; Brasilino, N.C.; Menezes, R.F.; Brugnera Junior, A.; Pinheiro, A.L.B. Photobiomodulation Therapy in Bone Repair Associated with Bone Morphogenetic Proteins and Guided Bone Regeneration: A Histomorphometric Study. Photomed. Laser Surg. 2018, 36, 581–588. [Google Scholar] [CrossRef]
- Renno, A.C.M.; McDonnell, P.A.; Crovace, M.C.; Zanotto, E.D.; Laakso, L. Effect of 830 nm Laser Phototherapy on Osteoblasts Grown In Vitro on Biosilicate® Scaffolds. Photomed. Laser Surg. 2009, 28, 131–133. [Google Scholar] [CrossRef]
- Grassi, F.R.; Ciccolella, F.; D’Apolito, G.; Papa, F.; Iuso, A.; Salzo, A.E.; Trentadue, R.; Nardi, G.M.; Scivetti, M.; De Matteo, M.; et al. Effect of low-level laser irradiation on osteoblast proliferation and bone formation. J. Biol. Regul. Homeost. Agents 2011, 25, 603–614. [Google Scholar]
- Pagin, M.T.; de Oliveira, F.A.; Oliveira, R.C.; Sant’Ana, A.C.P.; de Rezende, M.L.R.; Greghi, S.L.A.; Damante, C.A. Laser and light-emitting diode effects on pre-osteoblast growth and differentiation. Lasers Med. Sci. 2014, 29, 55–59. [Google Scholar] [CrossRef]
- Queiroga, A.S.; Sousa, F.B.; Araújo, J.M.S.; Santos, S.D.; Sousa, C.D.S.; Quintans, T.C.; Almeida, T.P.; Nonaka, C.F.W.; Batista, L.V.; Limeira Junior, F.A. Evaluation of bone repair in the femur of rats submitted to laser therapy in different wavelengths: An image segmentation method of analysis. Laser Phys. 2008, 18, 1087–1091. [Google Scholar] [CrossRef]
- Mergoni, G.; Vescovi, P.; Belletti, S.; Uggeri, J.; Nammour, S.; Gatti, R. Effects of 915 nm laser irradiation on human osteoblasts: A preliminary in vitro study. Lasers Med. Sci. 2018, 33, 1189–1195. [Google Scholar] [CrossRef]
- Jawad, M.M.; Husein, A.; Azlina, A.; Alam, M.K.; Hassan, R.; Shaari, R. Effect of 940 nm low-level laser therapy on osteogenesis in vitro. J. Biomed. Opt 2013, 18, 128001. [Google Scholar] [CrossRef]
- Inchingolo, F.; Tatullo, M.; Abenavoli, F.M.; Marrelli, M.; Inchingolo, A.D.; Inchingolo, A.M.; Dipalma, G. Comparison between traditional surgery, CO2 and Nd:Yag laser treatment for generalized gingival hyperplasia in Sturge-Weber syndrome: A retrospective study: Generalized gingival hyperplasia. J. Investig. Clin. Dent. 2010, 1, 85–89. [Google Scholar] [CrossRef] [PubMed]
- De Benedittis, M.; Petruzzi, M.; Pastore, L.; Inchingolo, F.; Serpico, R. Nd:YAG Laser for Gingivectomy in Sturge-Weber Syndrome. J. Oral Maxillofac. Surg. 2007, 65, 314–316. [Google Scholar] [CrossRef] [PubMed]
- Scarano, A.; Petrini, M.; Inchingolo, F.; Lorusso, F.; Amuso, D. A new technique for the treatment of nasal telangiectasia using atmospheric plasma (voltaic arc dermabrasion): Postoperative pain assessment by thermal infrared imaging. J. Cosmet. Dermatol. 2020, 19, 2912–2918. [Google Scholar] [CrossRef] [PubMed]
- Tarullo, A.; Laino, L.; Tarullo, A.; Inchingolo, F.; Flace, P.; Inchingolo, A.M.; Inchingolo, A.D.; Dipalma, G.; Podo Brunetti, S.; Cagiano, R. Use of a diode laser in an excisional biopsy of two spoonlike neoformations on the tongue tip. Acta Bio-Med. Atenei Parm. 2011, 82, 63–68. [Google Scholar]
- Scarano, A.; Lorusso, F.; Inchingolo, F.; Postiglione, F.; Petrini, M. The Effects of Erbium-Doped Yttrium Aluminum Garnet Laser (Er: YAG) Irradiation on Sandblasted and Acid-Etched (SLA) Titanium, an In Vitro Study. Materials 2020, 13, 4174. [Google Scholar] [CrossRef] [PubMed]
- Anders, J.J.; Lanzafame, R.J.; Arany, P.R. Low-Level Light/Laser Therapy Versus Photobiomodulation Therapy. Photomed. Laser Surg. 2015, 33, 183–184. [Google Scholar] [CrossRef]
- Hamblin, M.R. Mechanisms and applications of the anti-inflammatory effects of photobiomodulation. AIMS Biophys. 2017, 4, 337–361. [Google Scholar] [CrossRef]
- He, M.; Zhang, B.; Shen, N.; Wu, N.; Sun, J. A systematic review and meta-analysis of the effect of low-level laser therapy (LLLT) on chemotherapy-induced oral mucositis in pediatric and young patients. Eur. J. Pediatr. 2018, 177, 7–17. [Google Scholar] [CrossRef]
- Kalhori, K.A.M.; Vahdatinia, F.; Jamalpour, M.R.; Vescovi, P.; Fornaini, C.; Merigo, E.; Fekrazad, R. Photobiomodulation in Oral Medicine. Photobiomodulation Photomed. Laser Surg. 2019, 37, 837–861. [Google Scholar] [CrossRef]
- Vale, F.A.; Moreira, M.S.; de Almeida, F.C.S.; Ramalho, K.M. Low-level laser therapy in the treatment of recurrent aphthous ulcers: A systematic review. Sci. World J. 2015, 2015, 150412. [Google Scholar] [CrossRef]
- Honarmand, M.; Farhadmollashahi, L.; Vosoughirahbar, E. Comparing the effect of diode laser against acyclovir cream for the treatment of herpes labialis. J. Clin. Exp. Dent. 2017, 9, e729–e732. [Google Scholar] [CrossRef] [PubMed]
- Wibawa, A.; Sucharitakul, J.; Dansirikul, R.; Pisarnturakit, P.; Pisarnturakit, P.; Bhuridej, P.; Arirachakaran, P. Low-Level Laser Therapy to the Major Salivary Glands Increases Salivary Flow and MUC5B Protein Secretion in Diabetic Patients with Hyposalivation: A Preliminary Study. MSK 2018, 22, 14–21. [Google Scholar] [CrossRef]
- Falaki, F.; Nejat, A.H.; Dalirsani, Z. The Effect of Low-level Laser Therapy on Trigeminal Neuralgia: A Review of Literature. J. Dent. Res. Dent. Clin. Dent. Prospect. 2014, 8, 1–5. [Google Scholar] [CrossRef]
- Weber, J.B.B.; Camilotti, R.S.; Ponte, M.E. Efficacy of laser therapy in the management of bisphosphonate-related osteonecrosis of the jaw (BRONJ): A systematic review. Lasers Med. Sci. 2016, 31, 1261–1272. [Google Scholar] [CrossRef]
- Tenore, G.; Zimbalatti, A.; Rocchetti, F.; Graniero, F.; Gaglioti, D.; Mohsen, A.; Caputo, M.; Lollobrigida, M.; Lamazza, L.; De Biase, A.; et al. Management of Medication-Related Osteonecrosis of the Jaw (MRONJ) Using Leukocyte- and Platelet-Rich Fibrin (L-PRF) and Photobiomodulation: A Retrospective Study. J. Clin. Med. 2020, 9, 3505. [Google Scholar] [CrossRef] [PubMed]
- Gholami, L.; Asefi, S.; Hooshyarfard, A.; Sculean, A.; Romanos, G.E.; Aoki, A.; Fekrazad, R. Photobiomodulation in Periodontology and Implant Dentistry: Part 1. Photobiomodulation Photomed. Laser Surg. 2019, 37, 739–765. [Google Scholar] [CrossRef]
- Gholami, L.; Asefi, S.; Hooshyarfard, A.; Sculean, A.; Romanos, G.E.; Aoki, A.; Fekrazad, R. Photobiomodulation in Periodontology and Implant Dentistry: Part 2. Photobiomodulation Photomed. Laser Surg. 2019, 37, 766–783. [Google Scholar] [CrossRef]
- American Academy of Periodontology Statement on the Efficacy of Lasers in the Non-Surgical Treatment of Inflammatory Periodontal Disease. J. Periodontol. 2011, 82, 513–514. [CrossRef]
- Pereira, C.L.; Sallum, E.A.; Nociti, F.H.; Moreira, R.W.F. The effect of low-intensity laser therapy on bone healing around titanium implants: A histometric study in rabbits. Int. J. Oral Maxillofac. Implant. 2009, 24, 47–51. [Google Scholar]
- Mayer, L.; Gomes, F.V.; Carlsson, L.; Gerhardt-Oliveira, M. Histologic and Resonance Frequency Analysis of Peri-Implant Bone Healing After Low-Level Laser Therapy: An In Vivo Study. Int. J. Oral Maxillofac. Implant. 2015, 30, 1028–1035. [Google Scholar] [CrossRef]
- Jafarabadi, M.R.; Rouhi, G.; Kaka, G.; Sadraie, S.H.; Arum, J. The effects of photobiomodulation and low-amplitude high-frequency vibration on bone healing process: A comparative study. Lasers Med. Sci. 2016, 31, 1827–1836. [Google Scholar] [CrossRef] [PubMed]
- Maluf, A.P.; Maluf, R.P.; Brito, C.D.R.; França, F.M.G.; de Brito, R.B. Mechanical evaluation of the influence of low-level laser therapy in secondary stability of implants in mice shinbones. Lasers Med. Sci. 2010, 25, 693–698. [Google Scholar] [CrossRef] [PubMed]
- Boldrini, C.; de Almeida, J.M.; Fernandes, L.A.; Ribeiro, F.S.; Garcia, V.G.; Theodoro, L.H.; Pontes, A.E.F. Biomechanical effect of one session of low-level laser on the bone-titanium implant interface. Lasers Med. Sci. 2013, 28, 349–352. [Google Scholar] [CrossRef] [PubMed]
- Pinheiro, A.L.B.; Gerbi, M.E.M.; Ponzi, E.A.C.; Ramalho, L.M.P.; Marques, A.M.C.; Carvalho, C.M.; De Carneiro Santos, R.; Oliveira, P.C.; Nóia, M. Infrared Laser Light Further Improves Bone Healing When Associated with Bone Morphogenetic Proteins and Guided Bone Regeneration: An in Vivo Study in a Rodent Model. Photomed. Laser Surg. 2008, 26, 167–174. [Google Scholar] [CrossRef] [PubMed]
- Gerbi, M.E.M.; Pinheiro, A.L.B.; Marzola, C.; Limeira Júnior, F.D.A.; Ramalho, L.M.P.; Ponzi, E.A.C.; Soares, A.O.; Carvalho, L.C.B.; Lima, H.V.; Gonçalves, T.O. Assessment of bone repair associated with the use of organic bovine bone and membrane irradiated at 830 nm. Photomed. Laser Surg. 2005, 23, 382–388. [Google Scholar] [CrossRef]
- Márquez Martínez, M.E.; Pinheiro, A.L.B.; Ramalho, L.M.P. Effect of IR laser photobiomodulation on the repair of bone defects grafted with organic bovine bone. Lasers Med. Sci. 2008, 23, 313–317. [Google Scholar] [CrossRef]
- Ozcelik, O.; Haytac, M.C.; Seydaoglu, G. Enamel matrix derivative and low-level laser therapy in the treatment of intra-bony defects: A randomized placebo-controlled clinical trial: Emdogain with low-level laser. J. Clin. Periodontol. 2007, 35, 147–156. [Google Scholar] [CrossRef]
- Zhu, T.; Wu, Y.; Zhou, X.; Yang, Y.; Wang, Y. Irradiation by blue light-emitting diode enhances osteogenic differentiation in gingival mesenchymal stem cells in vitro. Lasers Med. Sci. 2019, 34, 1473–1481. [Google Scholar] [CrossRef]
- Faria, P.E.P.; Felipucci, D.N.B.; Simioni, A.R.; Primo, F.L.; Tedesco, A.C.; Salata, L.A. Effects of Photodynamic Process (PDP) in Implant Osseointegration: A Histologic and Histometric Study in Dogs: Photodynamic Process in Implant Osseointegration. Clin. Implant Dent. Relat. Res. 2015, 17, 879–890. [Google Scholar] [CrossRef]
- Stübinger, S.; Klämpfl, F.; Schmidt, M.; Zeilhofer, H.-F. (Eds.) Lasers in Oral and Maxillofacial Surgery; Springer International Publishing: Cham, Switzerland, 2020; ISBN 978-3-030-29603-2. [Google Scholar]
- Barbosa, D.; de Souza, R.A.; Xavier, M.; da Silva, F.F.; Arisawa, E.Â.L.; Villaverde, A.B. Effects of low-level laser therapy (LLLT) on bone repair in rats: Optical densitometry analysis. Lasers Med. Sci. 2013, 28, 651–656. [Google Scholar] [CrossRef]
- Renno, A.C.M.; McDonnell, P.A.; Parizotto, N.A.; Laakso, E.-L. The Effects of Laser Irradiation on Osteoblast and Osteosarcoma Cell Proliferation and Differentiation in Vitro. Photomed. Laser Surg. 2007, 25, 275–280. [Google Scholar] [CrossRef] [PubMed]
- Tani, A.; Chellini, F.; Giannelli, M.; Nosi, D.; Zecchi-Orlandini, S.; Sassoli, C. Red (635 nm), Near-Infrared (808 nm) and Violet-Blue (405 nm) Photobiomodulation Potentiality on Human Osteoblasts and Mesenchymal Stromal Cells: A Morphological and Molecular In Vitro Study. Int. J. Mol. Sci. 2018, 19, 1946. [Google Scholar] [CrossRef] [PubMed]
- Ghidini, G.; Sala, A.; Giovannacci, I.; Veneri, F.; Greco Lucchina, A.; Sala, R.; Vescovi, P. Absorption and diffusion of a 645 nm diode laser beam in the bone. An ex vivo study. J. Biol. Regul. Homeost. Agents 2019, 33, 137–141. [Google Scholar] [PubMed]
- Bjordal, J.M. Low Level Laser Therapy (LLLT) and World Association for Laser Therapy (WALT) Dosage Recommendations. Photomed. Laser Surg. 2012, 30, 61–62. [Google Scholar] [CrossRef] [PubMed]
- Pei, Z.; Bini, E.J.; Yang, L.; Zhou, M.; Francois, F.; Blaser, M.J. Bacterial biota in the human distal esophagus. Proc. Natl. Acad. Sci. USA 2004, 101, 4250–4255. [Google Scholar] [CrossRef] [PubMed]
- Inchingolo, F.; Dipalma, G.; Cirulli, N.; Cantore, S.; Saini, R.S.; Altini, V.; Santacroce, L.; Ballini, A.; Saini, R. Microbiological results of improvement in periodontal condition by administration of oral probiotics. J. Biol. Regul. Homeost. Agents 2018, 32, 1323–1328. [Google Scholar]
- Isacco, C.G.; Ballini, A.; De Vito, D.; Nguyen, K.C.D.; Cantore, S.; Bottalico, L.; Quagliuolo, L.; Boccellino, M.; Di Domenico, M.; Santacroce, L.; et al. Rebalance the oral microbiota as efficacy tool in endocrine, metabolic, and immune disorders. Endocr. Metab. Immune Disord. Drug Targets 2020, 21, 777–784. [Google Scholar] [CrossRef]
- Ballini, A.; Gnoni, A.; De Vito, D.; Dipalma, G.; Cantore, S.; Isacco, C.G.; Saini, R.; Santacroce, L.; Topi, S.; Scarano, A.; et al. Effect of probiotics on the occurrence of nutrition absorption capacities in healthy children: A randomized double-blinded placebo-controlled pilot study. Eur. Rev. Med. Pharmacol. Sci. 2019, 23, 8645–8657. [Google Scholar] [CrossRef]
- Cantore, S.; Ballini, A.; De Vito, D.; Abbinante, A.; Altini, V.; Dipalma, G.; Inchingolo, F.; Saini, R. Clinical results of improvement in periodontal condition by administration of oral probiotics. J. Biol. Regul. Homeost. Agents 2018, 32, 1329–1334. [Google Scholar]
- Larsbrink, J.; Rogers, T.E.; Hemsworth, G.R.; McKee, L.S.; Tauzin, A.S.; Spadiut, O.; Klinter, S.; Pudlo, N.A.; Urs, K.; Koropatkin, N.M.; et al. A discrete genetic locus confers xyloglucan metabolism in select human gut Bacteroidetes. Nature 2014, 506, 498–502. [Google Scholar] [CrossRef]
- Morowitz, M.J.; Denef, V.J.; Costello, E.K.; Thomas, B.C.; Poroyko, V.; Relman, D.A.; Banfield, J.F. Strain-resolved community genomic analysis of gut microbial colonization in a premature infant. Proc. Natl. Acad. Sci. USA 2011, 108, 1128–1133. [Google Scholar] [CrossRef] [PubMed]
- Wang, B.; Yao, M.; Lv, L.; Ling, Z.; Li, L. The Human Microbiota in Health and Disease. Engineering 2017, 3, 71–82. [Google Scholar] [CrossRef]
- Campanella, V.; Syed, J.; Santacroce, L.; Saini, R.; Ballini, A.; Inchingolo, F. Oral probiotics influence oral and respiratory tract infections in pediatric population: A randomized double-blinded placebo-controlled pilot study. Eur. Rev. Med. Pharmacol. Sci. 2018, 22, 8034–8041. [Google Scholar] [CrossRef] [PubMed]
- Signorini, L.; Ballini, A.; Arrigoni, R.; De Leonardis, F.; Saini, R.; Cantore, S.; De Vito, D.; Coscia, M.F.; Dipalma, G.; Santacroce, L.; et al. Evaluation of a nutraceutical product with probiotics, vitamin d, plus banaba leaf extracts (Lagerstroemia speciosa) in glycemic control. Endocr. Metab. Immune Disord. Drug Targets 2020, 21, 1356–1365. [Google Scholar] [CrossRef] [PubMed]
- Round, J.L.; Mazmanian, S.K. The gut microbiota shapes intestinal immune responses during health and disease. Nat. Rev. Immunol. 2009, 9, 313–323. [Google Scholar] [CrossRef]
- Reschner, A.; Hubert, P.; Delvenne, P.; Boniver, J.; Jacobs, N. Innate lymphocyte and dendritic cell cross-talk: A key factor in the regulation of the immune response. Clin. Exp. Immunol. 2008, 152, 219–226. [Google Scholar] [CrossRef]
- Haag, L.-M.; Siegmund, B. Intestinal Microbiota and the Innate Immune System—A Crosstalk in Crohn’s Disease Pathogenesis. Front. Immunol. 2015, 6, 489. [Google Scholar] [CrossRef]
- Wang, J.; Wang, Y.; Gao, W.; Wang, B.; Zhao, H.; Zeng, Y.; Ji, Y.; Hao, D. Diversity analysis of gut microbiota in osteoporosis and osteopenia patients. PeerJ 2017, 5, e3450. [Google Scholar] [CrossRef]
- Boyce, B.F.; Xing, L. The RANKL/RANK/OPG pathway. Curr. Osteoporos. Rep. 2007, 5, 98–104. [Google Scholar] [CrossRef]
- Park, J.H.; Lee, N.K.; Lee, S.Y. Current Understanding of RANK Signaling in Osteoclast Differentiation and Maturation. Mol. Cells 2017, 40, 706–713. [Google Scholar] [CrossRef]
- Contaldo, M.; Itro, A.; Lajolo, C.; Gioco, G.; Inchingolo, F.; Serpico, R. Overview on Osteoporosis, Periodontitis and Oral Dysbiosis: The Emerging Role of Oral Microbiota. Appl. Sci. 2020, 10, 6000. [Google Scholar] [CrossRef]
- Walsh, M.C.; Kim, N.; Kadono, Y.; Rho, J.; Lee, S.Y.; Lorenzo, J.; Choi, Y. Osteoimmunology: Interplay between the immune system and bone metabolism. Annu. Rev. Immunol. 2006, 24, 33–63. [Google Scholar] [CrossRef] [PubMed]
- Bernstein, C.N.; Leslie, W.D.; Leboff, M.S. AGA technical review on osteoporosis in gastrointestinal diseases. Gastroenterology 2003, 124, 795–841. [Google Scholar] [CrossRef] [PubMed]
- Yokota, K.; Sato, K.; Miyazaki, T.; Kitaura, H.; Kayama, H.; Miyoshi, F.; Araki, Y.; Akiyama, Y.; Takeda, K.; Mimura, T. Combination of Tumor Necrosis Factor α and Interleukin-6 Induces Mouse Osteoclast-like Cells With Bone Resorption Activity Both In Vitro and In Vivo. Arthritis Rheumatol. 2014, 66, 121–129. [Google Scholar] [CrossRef]
- Zhang, J.; Fu, Q.; Ren, Z.; Wang, Y.; Wang, C.; Shen, T.; Wang, G.; Wu, L. Changes of serum cytokines-related Th1/Th2/Th17 concentration in patients with postmenopausal osteoporosis. Gynecol. Endocrinol. 2015, 31, 183–190. [Google Scholar] [CrossRef]
- Boroń, D.; Agnieszka, S.-M.; Daniel, K.; Anna, B.; Adam, K. Polymorphism of interleukin-17 and its relation to mineral density of bones in perimenopausal women. Eur. J. Med. Res. 2014, 19, 69. [Google Scholar] [CrossRef]
- Vermesan, D.; Prejbeanu, R.; Haragus, H.; Poenaru, D.V.; Mioc, M.L.; Tatullo, M.; Abbinante, A.; Scacco, S.; Tarullo, A.; Inchingolo, F.; et al. Clinical relevance of altered bone immunopathology pathways around the elbow. Eur. Rev. Med. Pharmacol. Sci. 2014, 18, 2846–2850. [Google Scholar]
- Isacco, C.G.; Ballini, A.; Vito, D.D.; Inchingolo, A.M.; Cantore, S.; Paduanelli, G.; Nguyen, K.C.D.; Inchingolo, A.D.; Dipalma, G.; Inchingolo, F. Probiotics in Health and Immunity: A First Step toward Understanding the Importance of Microbiota System in Translational Medicine. Prebiotics Probiotics Potential Benefits Nutr. Health 2019, 1–18. [Google Scholar] [CrossRef]
- Santacroce, L.; Sardaro, N.; Topi, S.; Pettini, F.; Bottalico, L.; Cantore, S.; Cascella, G.; Del Prete, R.; Dipalma, G.; Inchingolo, F. The pivotal role of oral microbiota in health and disease. J. Biol. Regul. Homeost. Agents 2020, 34, 733–737. [Google Scholar] [CrossRef]
- Santacroce, L.; Charitos, I.A.; Ballini, A.; Inchingolo, F.; Luperto, P.; De Nitto, E.; Topi, S. The Human Respiratory System and its Microbiome at a Glimpse. Biology 2020, 9, 318. [Google Scholar] [CrossRef]
- Inchingolo, A.D.; Di Cosola, M.; Inchingolo, A.M.; Greco Lucchina, A.; Malcangi, G.; Pettini, F.; Scarano, A.; Bordea, I.R.; Hazballa, D.; Lorusso, F.; et al. Correlation between occlusal trauma and oral microbiota: A microbiological investigation. J. Biol. Regul. Homeost. Agents 2021, 35, 295–302. [Google Scholar] [CrossRef] [PubMed]
- Di Cosola, M.; Cazzolla, A.P.; Charitos, I.A.; Ballini, A.; Inchingolo, F.; Santacroce, L. Candida albicans and Oral Carcinogenesis. A Brief Review. J. Fungi 2021, 7, 476. [Google Scholar] [CrossRef] [PubMed]
- Contaldo, M.; Fusco, A.; Stiuso, P.; Lama, S.; Gravina, A.G.; Itro, A.; Federico, A.; Itro, A.; Dipalma, G.; Inchingolo, F.; et al. Oral Microbiota and Salivary Levels of Oral Pathogens in Gastro-Intestinal Diseases: Current Knowledge and Exploratory Study. Microorganisms 2021, 9, 1064. [Google Scholar] [CrossRef] [PubMed]
- Inchingolo, F.; Santacroce, L.; Cantore, S.; Ballini, A.; Del Prete, R.; Topi, S.; Saini, R.; Dipalma, G.; Arrigoni, R. Probiotics and EpiCor® in human health. J. Biol. Regul. Homeost. Agents 2019, 33, 1973–1979. [Google Scholar] [CrossRef] [PubMed]
- Pacifici, L.; Santacroce, L.; Dipalma, G.; Haxhirexha, K.; Topi, S.; Cantore, S.; Altini, V.; Pacifici, A.; De Vito, D.; Dds, F.; et al. Gender medicine: The impact of probiotics on male patients Clinical Trial. La Clin. Ter. 2021, 171, 8–15. [Google Scholar] [CrossRef]
- Ballini, A.; Signorini, L.; Inchingolo, A.D.; Saini, R.; Gnoni, A.; Scacco, S.; Cantore, S.; Dipalma, G.; Inchingolo, F.; Santacroce, L. Probiotics May Improve Serum Folate Availability in Pregnant Women: A Pilot Study. Open Access Maced. J. Med. Sci. 2020, 8, 1124–1130. [Google Scholar] [CrossRef]
- Ballini, A.; Santacroce, L.; Cantore, S.; Bottalico, L.; Dipalma, G.; Vito, D.D.; Saini, R.; Inchingolo, F. Probiotics Improve Urogenital Health in Women. Open Access Maced. J. Med. Sci. 2018, 6, 1845–1850. [Google Scholar] [CrossRef]
- Signorini, L.; De Leonardis, F.; Santacroce, L.; Haxhirexha, K.; Topi, S.; Fumarola, L.; Dipalma, G.; Coscia, M.F.; Inchingolo, F. Probiotics may modulate the impact of aging on adults. J. Biol. Regul. Homeost. Agents 2020, 34, 1601–1606. [Google Scholar] [CrossRef]
- Inchingolo, A.D.; Cazzolla, A.P.; Di Cosola, M.; Greco Lucchina, A.; Santacroce, L.; Charitos, I.A.; Topi, S.; Malcangi, G.; Hazballa, D.; Scarano, A.; et al. The integumentary system and its microbiota between health and disease. J. Biol. Regul. Homeost. Agents 2021, 35, 303–321. [Google Scholar] [CrossRef]
- Gargiulo, C.; van Pham, H.; Duy Huynh, T.; Vo Le Hoang, T.; Nguyen, K.; Shiffman, M.; Holterman, M.; Aityan, S.; Filgueira, L.; Agbo, J. Novel Therapeutic Strategy in the Treatment of Diabetes Type 2, the Use of Autologous Peripheral Blood Stem Cells in 15 Patients: Is There Any Relation with the Incretin-GLP-1/GIP Axis? J. Adv. Med. Med. Res. 2017, 20, 1–16. [Google Scholar] [CrossRef]
- Dohan Ehrenfest, D.M.; Del Corso, M.; Inchingolo, F.; Sammartino, G.; Charrier, J.-B. Platelet-rich plasma (PRP) and platelet-rich fibrin (PRF) in human cell cultures: Growth factor release and contradictory results. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2010, 110, 418–421. [Google Scholar] [CrossRef] [PubMed]
- Ballini, A.; Cantore, S.; Farronato, D.; Cirulli, N.; Inchingolo, F.; Papa, F.; Malcangi, G.; Inchingolo, A.D.; Dipalma, G.; Sardaro, N.; et al. Periodontal Disease and Bone Pathogenesis: The Crosstalk between Cytokines and Porphyromonas Gingivalis. J. Biol. Regul. Homeost. Agents 2015, 29, 273–281. [Google Scholar] [PubMed]
- Cantore, S.; Mirgaldi, R.; Ballini, A.; Coscia, M.F.; Scacco, S.; Papa, F.; Inchingolo, F.; Dipalma, G.; De Vito, D. Cytokine Gene Polymorphisms Associate with Microbiogical Agents in Periodontal Disease: Our Experience. Int. J. Med. Sci. 2014, 11, 674–679. [Google Scholar] [CrossRef]
- Tatullo, M.; Gargiulo, I.C.; Dipalma, G.; Ballini, A.; Inchingolo, A.M.; Paduanelli, G.; Nguyen, C.; Dẳng, K.; Inchingolo, A.D.; Makeeva, I.; et al. Stem cells and regenerative medicine. In Translational Systems Medicine and Oral Disease; Sonis, S.T., Villa, A., Eds.; Academic Press: Cambridge, MA, USA, 2020; pp. 387–407. ISBN 978-0-12-813762-8. [Google Scholar]
- Dang, Q.T.; Huynh, T.D.; Inchingolo, F.; Dipalma, G.; Inchingolo, A.D.; Cantore, S.; Paduanelli, G.; Nguyen, K.C.D.; Ballini, A.; Isacco, C.G.; et al. Human Chondrocytes from Human Adipose Tissue-Derived Mesenchymal Stem Cells Seeded on a Dermal-Derived Collagen Matrix Sheet: Our Preliminary Results for a Ready to Go Biotechnological Cartilage Graft in Clinical Practice. Stem Cells Int. 2021, 2021, e6664697. [Google Scholar] [CrossRef] [PubMed]
- Wagner, W.; Wein, F.; Seckinger, A.; Frankhauser, M.; Wirkner, U.; Krause, U.; Blake, J.; Schwager, C.; Eckstein, V.; Ansorge, W.; et al. Comparative characteristics of mesenchymal stem cells from human bone marrow, adipose tissue, and umbilical cord blood. Exp. Hematol. 2005, 33, 1402–1416. [Google Scholar] [CrossRef] [PubMed]
- Ballini, A.; Cantore, S.; Scacco, S.; Perillo, L.; Scarano, A.; Aityan, S.; Contaldo, M.; Cd Nguyen, K.; Santacroce, L.; Syed, J.; et al. A comparative study on different stemness gene expression between dental pulp stem cells vs. dental bud stem cells. Eur. Rev. Med. Pharmacol. Sci. 2019, 23, 1626–1633. [Google Scholar] [CrossRef]
- Gargiulo, C.; Pham, V.H.; Thuy Hai, N.; Nguyen, K.C.D.; Phuc, P.V.; Abe, K.; Flores, V.; Shiffman, M. Isolation and Characterization of Multipotent and Pluripotent Stem Cells from Human Peripheral Blood. Stem Cell Discov. 2015, 05, 19–32. [Google Scholar] [CrossRef]
- Scarano, A.; Inchingolo, F.; Rapone, B.; Lucchina, A.G.; Qorri, E.; Lorusso, F. Role of Autologous Platelet Gel (APG) in Bone Healing: A Rabbit Study. Appl. Sci. 2021, 11, 395. [Google Scholar] [CrossRef]
- Inchingolo, F.; Martelli, F.S.; Gargiulo Isacco, C.; Borsani, E.; Cantore, S.; Corcioli, F.; Boddi, A.; Nguyễn, K.C.D.; De Vito, D.; Aityan, S.K.; et al. Chronic Periodontitis and Immunity, Towards the Implementation of a Personalized Medicine: A Translational Research on Gene Single Nucleotide Polymorphisms (SNPs) Linked to Chronic Oral Dysbiosis in 96 Caucasian Patients. Biomedicines 2020, 8, 115. [Google Scholar] [CrossRef]
- Gargiulo, C.; Hung, P.; Schifman, M. Innovative Concepts of Cell Therapy: Pluripotent and Multipotent Stem Cells and New Bio-Material Solution in Research and Clinical Application. Recent Patents Regen. Med. 2016, 5, 102–111. [Google Scholar] [CrossRef]
- Calvo-Guirado, J.L.; Montilla, A.B.; De Aza, P.N.; Fernández-Domínguez, M.; Gehrke, S.A.; Cegarra-Del Pino, P.; Mahesh, L.; Pelegrine, A.A.; Aragoneses, J.M.; de Val, J.E.M.-S. Particulated, Extracted Human Teeth Characterization by SEM–EDX Evaluation as a Biomaterial for Socket Preservation: An In Vitro Study. Materials 2019, 12, 380. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Wang, J.; Chen, F.; Feng, Y.; Xie, C.; Li, D. A reduced healing protocol for sinus floor elevation in a staged approach with deproteinized bovine bone mineral alone: A randomized controlled clinical trial of a 5-month healing in comparison to the 8-month healing. Clin. Implant. Dent. Relat. Res. 2020, 22, 281–291. [Google Scholar] [CrossRef] [PubMed]
- Younes, F.; Cosyn, J.; Bruyckere, T.D.; Cleymaet, R.; Eghbali, A. A 2-year prospective case series on volumetric changes, PROMs, and clinical outcomes following sinus floor elevation using deproteinized bovine bone mineral as filling material. Clin. Implant. Dent. Relat. Res. 2019, 21, 301–309. [Google Scholar] [CrossRef] [PubMed]
- Fouad, W.; Osman, A.; Atef, M.; Hakam, M. Guided maxillary sinus floor elevation using deproteinized bovine bone versus graftless Schneiderian membrane elevation with simultaneous implant placement: Randomized clinical trial. Clin. Implant. Dent. Relat. Res. 2018, 20, 424–433. [Google Scholar] [CrossRef] [PubMed]
- Mazzocco, F.; Lops, D.; Gobbato, L.; Lolato, A.; Romeo, E.; del Fabbro, M. Three-dimensional volume change of grafted bone in the maxillary sinus. Int. J. Oral Maxillofac. Implant. 2014, 29, 178–184. [Google Scholar] [CrossRef]
- Younes, F.; Eghbali, A.; De Troyer, S.; De Bruyckere, T.; Cleymaet, R.; Cosyn, J. Marginal and apical bone stability after staged sinus floor augmentation using bone condensing implants with variable-thread design: A two-dimensional analysis. Int. J. Oral Maxillofac. Surg. 2016, 45, 1135–1141. [Google Scholar] [CrossRef]
- Scarano, A. Maxillary Sinus Augmentation with Decellularized Bovine Compact Particles: A Radiological, Clinical, and Histologic Report of 4 Cases. Available online: https://www.hindawi.com/journals/bmri/2017/2594670/ (accessed on 11 October 2020).
- Olaechea, A.; Mendoza-Azpur, G.; O Valle, F.; Padial-Molina, M.; Martin-Morales, N.; Galindo-Moreno, P. Biphasic hydroxyapatite and ß-tricalcium phosphate biomaterial behavior in a case series of maxillary sinus augmentation in humans. Clin. Oral Implant. Res. 2019, 30, 336–343. [Google Scholar] [CrossRef]
- Okada, T.; Kanai, T.; Tachikawa, N.; Munakata, M.; Kasugai, S. Long-term radiographic assessment of maxillary sinus floor augmentation using beta-tricalcium phosphate: Analysis by cone-beam computed tomography. Int. J. Implant Dent. 2016, 2, 8. [Google Scholar] [CrossRef]
- Oba, Y.; Tachikawa, N.; Munakata, M.; Okada, T.; Kasugai, S. Evaluation of maxillary sinus floor augmentation with the crestal approach and beta-tricalcium phosphate: A cone-beam computed tomography 3- to 9-year follow-up. Int. J. Implant Dent. 2020, 6, 27. [Google Scholar] [CrossRef]
- Ohe, J.-Y.; Kim, G.-T.; Lee, J.-W.; Al Nawas, B.; Jung, J.; Kwon, Y.-D. Volume stability of hydroxyapatite and β-tricalcium phosphate biphasic bone graft material in maxillary sinus floor elevation: A radiographic study using 3D cone beam computed tomography. Clin. Oral Implant. Res. 2016, 27, 348–353. [Google Scholar] [CrossRef]
- Oliveira, G.; Pignaton, T.B.; Ferreira, C.E.A.; Peruzzo, L.C.; Marcantonio, E. New bone formation comparison in sinuses grafted with anorganic bovine bone and β-TCP. Clin. Oral Implant. Res. 2019, 30, 483. [Google Scholar] [CrossRef]
- Baranes, D.; Kurtzman, G.M. Biphasic Calcium Sulfate as an Alternative Grafting Material in Various Dental Applications. J. Oral Implantol. 2019, 45, 247–255. [Google Scholar] [CrossRef] [PubMed]
- Haugen, H.J.; Lyngstadaas, S.P.; Rossi, F.; Perale, G. Bone grafts: Which is the ideal biomaterial? J. Clin. Periodontol. 2019, 46, 92–102. [Google Scholar] [CrossRef] [PubMed]
- Meng, Y.; Huang, X.; Wu, M.; Yang, X.; Liu, Y. The Effect of Autologous Platelet Concentrates on Maxillary Sinus Augmentation: A Meta-Analysis of Randomized Controlled Trials and Systematic Review. Available online: https://www.hindawi.com/journals/bmri/2020/7589072/ (accessed on 4 October 2020).
- Ding, Y.; Wang, X. Long-Term Effects of Bone Morphogenetic Protein-2-Loaded Calcium Phosphate on Maxillary Sinus Lift Surgery for Delayed and Simultaneous Dental Implantation. J. Craniofac. Surg. 2018, 29, e58–e61. [Google Scholar] [CrossRef] [PubMed]
- Valdec, S.; Pasic, P.; Soltermann, A.; Thoma, D.; Stadlinger, B.; Rücker, M. Alveolar ridge preservation with autologous particulated dentin—a case series. Int. J. Implant. Dent. 2017, 3, 12. [Google Scholar] [CrossRef]
- Minetti, E.; Taschieri, S.; Corbella, S. Autologous Deciduous Tooth-Derived Material for Alveolar Ridge Preservation: A Clinical and Histological Case Report. Available online: https://www.hindawi.com/journals/crid/2020/2936878/ (accessed on 11 October 2020).
- Del Canto-Diaz, A.; de Elio-Oliveros, J.; del Canto-Diaz, M.; Alobera-Gracia, M.; del Canto-Pingarron, M.; Martinez-Gonzalez, J. Use of autologous tooth-derived graft material in the post-extraction dental socket. Pilot study. Med. Oral 2018, 24, e53–e60. [Google Scholar] [CrossRef]
- Al Qabbani, A.; Al Kawas, S.; Razak, N.H.A.; Al Bayatti, S.W.; Enezei, H.H.; Samsudin, A.R.; Ab Hamid, S.S. Three-Dimensional Radiological Assessment of Alveolar Bone Volume Preservation Using Bovine Bone Xenograft. J. Craniofacial Surg. 2018, 29, e203–e209. [Google Scholar] [CrossRef]
- Fischer, K.R.; Mühlemann, S.; Jung, R.E.; Friedmann, A.; Fickl, S. Dimensional Evaluation of Different Ridge Preservation Techniques with a Bovine Xenograft: A Randomized Controlled Clinical Trial. Int. J. Periodontics Restor. Dent. 2018, 38, 549–556. [Google Scholar] [CrossRef]
- Pang, C.; Ding, Y.; Zhou, H.; Qin, R.; Hou, R.; Zhang, G.; Hu, K. Alveolar Ridge Preservation With Deproteinized Bovine Bone Graft and Collagen Membrane and Delayed Implants. J. Craniofacial Surg. 2014, 25, 1698–1702. [Google Scholar] [CrossRef]
- Naenni, N.; Sapata, V.; Bienz, S.P.; Leventis, M.; Jung, R.E.; Hämmerle, C.H.F.; Thoma, D.S. Effect of flapless ridge preservation with two different alloplastic materials in sockets with buccal dehiscence defects-volumetric and linear changes. Clin. Oral Investig. 2018, 22, 2187–2197. [Google Scholar] [CrossRef]
- Ikawa, T.; Akizuki, T.; Matsuura, T.; Hoshi, S.; Ammar, S.A.; Kinoshita, A.; Oda, S.; Izumi, Y. Ridge Preservation After Tooth Extraction With Buccal Bone Plate Deficiency Using Tunnel Structured β-Tricalcium Phosphate Blocks: A 2-Month Histologic Pilot Study in Beagle Dogs. J. Periodontol. 2016, 87, 175–183. [Google Scholar] [CrossRef] [PubMed]
- Mayer, Y.; Zigdon-Giladi, H.; Machtei, E.E. Ridge Preservation Using Composite Alloplastic Materials: A Randomized Control Clinical and Histological Study in Humans. Clin. Implant. Dent. Relat. Res. 2016, 18, 1163–1170. [Google Scholar] [CrossRef] [PubMed]
- Tan, W.L.; Wong, T.L.T.; Wong, M.C.M.; Lang, N.P. A systematic review of post-extractional alveolar hard and soft tissue dimensional changes in humans. Clin. Oral Implant. Res. 2012, 23 (Suppl. 5), 1–21. [Google Scholar] [CrossRef] [PubMed]
- Hojo, S.; Bamba, N.; Kojima, K.; Kodama, T. Examination of β-TCP/collagen composite in bone defects without periosteum in dogs: A histological and cast model evaluation. Odontology 2020, 108, 578–587. [Google Scholar] [CrossRef]
- Kato, E.; Lemler, J.; Sakurai, K.; Yamada, M. Biodegradation property of beta-tricalcium phosphate-collagen composite in accordance with bone formation: A comparative study with Bio-Oss Collagen® in a rat critical-size defect model. Clin. Implant. Dent. Relat. Res. 2014, 16, 202–211. [Google Scholar] [CrossRef]
- Machtei, E.E.; Mayer, Y.; Horwitz, J.; Zigdon-Giladi, H. Prospective randomized controlled clinical trial to compare hard tissue changes following socket preservation using alloplasts, xenografts vs no grafting: Clinical and histological findings. Clin. Implant Dent. Relat. Res. 2019, 21, 14–20. [Google Scholar] [CrossRef]
- Cha, J.-K.; Sanz, M.; Jung, U.-W. Human Autopsy Study of Peri-implant Dehiscence Defects with Guided Bone Regeneration: A Case Report. Int. J. Periodontics Restor. Dent. 2019, 39, 517–524. [Google Scholar] [CrossRef]
- Carmagnola, D.; Adriaens, P.; Berglundh, T. Healing of human extraction sockets filled with Bio-Oss. Clin. Oral Implant. Res. 2003, 14, 137–143. [Google Scholar] [CrossRef]
- Guarnieri, R.; Belleggia, F.; DeVillier, P.; Testarelli, L. Histologic and Histomorphometric Analysis of Bone Regeneration with Bovine Grafting Material after 24 Months of Healing. A Case Report. J. Funct. Biomater. 2018, 9, 48. [Google Scholar] [CrossRef]
- Joshi, C.P.; Dani, N.H.; Khedkar, S.U. Alveolar ridge preservation using autogenous tooth graft versus beta-tricalcium phosphate alloplast: A randomized, controlled, prospective, clinical pilot study. J. Indian Soc. Periodontol. 2016, 20, 429–434. [Google Scholar] [CrossRef]
- Schwarz, F.; Mihatovic, I.; Golubovic, V.; Becker, J. Dentointegration of a titanium implant: A case report. Oral Maxillofac. Surg. 2013, 17, 235–241. [Google Scholar] [CrossRef] [PubMed]
- Kabir, M.A.; Murata, M.; Akazawa, T.; Kusano, K.; Yamada, K.; Ito, M. Evaluation of perforated demineralized dentin scaffold on bone regeneration in critical-size sheep iliac defects. Clin. Oral Implant. Res. 2017, 28, e227–e235. [Google Scholar] [CrossRef] [PubMed]
- Schwarz, F.; Golubovic, V.; Becker, K.; Mihatovic, I. Extracted tooth roots used for lateral alveolar ridge augmentation: A proof-of-concept study. J. Clin. Periodontol. 2016, 43, 345–353. [Google Scholar] [CrossRef] [PubMed]
- Becker, K.; Drescher, D.; Hönscheid, R.; Golubovic, V.; Mihatovic, I.; Schwarz, F. Biomechanical, micro-computed tomographic and immunohistochemical analysis of early osseous integration at titanium implants placed following lateral ridge augmentation using extracted tooth roots. Clin. Oral Implant. Res. 2017, 28, 334–340. [Google Scholar] [CrossRef] [PubMed]
- Lemons, J.E. Ceramics: Past, present, and future. Bone 1996, 19, S121–S128. [Google Scholar] [CrossRef]
- Ho-Shui-Ling, A.; Bolander, J.; Rustom, L.E.; Johnson, A.W.; Luyten, F.P.; Picart, C. Bone regeneration strategies: Engineered scaffolds, bioactive molecules and stem cells current stage and future perspectives. Biomaterials 2018, 180, 143–162. [Google Scholar] [CrossRef] [PubMed]
- Ghouse, S.; Reznikov, N.; Boughton, O.R.; Babu, S.; Ng, K.C.G.; Blunn, G.; Cobb, J.P.; Stevens, M.M.; Jeffers, J.R.T. The Design and In Vivo Testing of a Locally Stiffness-Matched Porous Scaffold. Appl. Mater. Today 2019, 15, 377–388. [Google Scholar] [CrossRef]
- Schlichting, K.; Schell, H.; Kleemann, R.; Schill, A.; Weiler, A.; Duda, G.; Epari, D. Influence of Scaffold Stiffness on Subchondral Bone and Subsequent Cartilage Regeneration in an Ovine Model of Osteochondral Defect Healing. Am. J. Sports Med. 2008, 36, 2379–2391. [Google Scholar] [CrossRef]
- Wang, W.; Yeung, K.W.K. Bone grafts and biomaterials substitutes for bone defect repair: A review. Bioact. Mater. 2017, 2, 224–247. [Google Scholar] [CrossRef]
- Li, S.; Tallia, F.; Mohammed, A.A.; Stevens, M.M.; Jones, J.R. Scaffold channel size influences stem cell differentiation pathway in 3-D printed silica hybrid scaffolds for cartilage regeneration. Biomater. Sci. 2020, 8, 4458–4466. [Google Scholar] [CrossRef]
- Fiorillo, L.; Cervino, G.; Galindo-Moreno, P.; Herford, A.S.; Spagnuolo, G.; Cicciù, M. Growth Factors in Oral Tissue Engineering: New Perspectives and Current Therapeutic Options. Available online: https://www.hindawi.com/journals/bmri/2021/8840598/ (accessed on 17 January 2021).
- Harwood, P.J.; Ferguson, D.O. (ii) An update on fracture healing and non-union. Orthop. Trauma 2015, 29, 228–242. [Google Scholar] [CrossRef]
- Agbeboh, N.I.; Oladele, I.O.; Daramola, O.O.; Adediran, A.A.; Olasukanmi, O.O.; Tanimola, M.O. Environmentally sustainable processes for the synthesis of hydroxyapatite. Heliyon 2020, 6, e03765. [Google Scholar] [CrossRef] [PubMed]
- Fisher, D.M.; Min-Leong Wong, J.; Crowley, C.S.; Khan, W. Preclinical and Clinical Studies on the Use of Growth Factors for Bone Repair: A Systematic Review. Curr. Stem Cell Res. Ther. 2013, 8, 260–268. [Google Scholar] [CrossRef] [PubMed]
- Tóth, F.; Gáll, J.M.; Tőzsér, J.; Hegedűs, C. Effect of inducible bone morphogenetic protein 2 expression on the osteogenic differentiation of dental pulp stem cells in vitro. Bone 2020, 132, 115214. [Google Scholar] [CrossRef] [PubMed]
- Schmitt, C.M.; Doering, H.; Schmidt, T.; Lutz, R.; Neukam, F.W.; Schlegel, K.A. Histological results after maxillary sinus augmentation with Straumann® BoneCeramic, Bio-Oss®, Puros®, and autologous bone. A randomized controlled clinical trial. Clin. Oral Implant. Res. 2013, 24, 576–585. [Google Scholar] [CrossRef] [PubMed]
- Schulhofer, S.D.; Oloff, L.M. Iliac crest donor site morbidity in foot and ankle surgery. J. Foot Ankle Surg. 1997, 36, 155–158. [Google Scholar] [CrossRef]
- Danesh-Sani, S.A.; Engebretson, S.P.; Janal, M.N. Histomorphometric results of different grafting materials and effect of healing time on bone maturation after sinus floor augmentation: A systematic review and meta-analysis. J. Periodont. Res. 2017, 52, 301–312. [Google Scholar] [CrossRef]
- Schmidt-Schultz, T.H.; Schultz, M. Intact growth factors are conserved in the extracellular matrix of ancient human bone and teeth: A storehouse for the study of human evolution in health and disease. Biol. Chem. 2005, 386, 767–776. [Google Scholar] [CrossRef]
- Al-Moraissi, E.A.; Alkhutari, A.S.; Abotaleb, B.; Altairi, N.H.; Del Fabbro, M. Do osteoconductive bone substitutes result in similar bone regeneration for maxillary sinus augmentation when compared to osteogenic and osteoinductive bone grafts? A systematic review and frequentist network meta-analysis. Int. J. Oral Maxillofac. Surg. 2020, 49, 107–120. [Google Scholar] [CrossRef]
- Zhai, P.; Peng, X.; Li, B.; Liu, Y.; Sun, H.; Li, X. The application of hyaluronic acid in bone regeneration. Int. J. Biol. Macromol. 2020, 151, 1224–1239. [Google Scholar] [CrossRef]
- Inchingolo, F.; Tatullo, M.; Abenavoli, F.M.; Marrelli, M.; Inchingolo, A.D.; Servili, A.; Inchingolo, A.M.; Dipalma, G. A hypothetical correlation between hyaluronic acid gel and development of cutaneous metaplastic synovial cyst. Head Face Med. 2010, 6, 13. [Google Scholar] [CrossRef] [PubMed]
- Niklason, L.E. Understanding the Extracellular Matrix to Enhance Stem Cell-Based Tissue Regeneration. Cell Stem Cell 2018, 22, 302–305. [Google Scholar] [CrossRef] [PubMed]
- Huang, L.; Cheng, Y.Y.; Koo, P.L.; Lee, K.M.; Qin, L.; Cheng, J.C.Y.; Kumta, S.M. The effect of hyaluronan on osteoblast proliferation and differentiation in rat calvarial-derived cell cultures. J. Biomed. Mater. Res. 2003, 66A, 880–884. [Google Scholar] [CrossRef] [PubMed]
- Kaczmarek, B.; Sionkowska, A.; Gołyńska, M.; Polkowska, I.; Szponder, T.; Nehrbass, D.; Osyczka, A.M. In vivo study on scaffolds based on chitosan, collagen, and hyaluronic acid with hydroxyapatite. Int. J. Biol. Macromol. 2018, 118, 938–944. [Google Scholar] [CrossRef]
- Scarano, A.; Puglia, F.; Cassese, R.; Mordente, I.; Amore, R.; Ferraro, G.; Sbarbati, A.; Lo Russo, F.; Lucchina, A.G.; Amuso, D. Hyaluronic acid fillers in lip augmentation procedure: A clinical and histological study. J. Biol. Regul. Homeost. Agents 2019, 33, 103–108. [Google Scholar]
- Scarano, A.; Amuso, D.; Amore, R.; Greco Lucchina, A.; Inchingolo, F.; Marchetti, M.; Lorusso, F. Malar augmentation with Hyaluronic acid enriched with glycine and proline: A clinical evaluation. J. Biol. Regul. Homeost. Agents 2021, 35, 187–194. [Google Scholar]
- Scarano, A.; Sbarbati, A.; Amore, R.; Iorio, E.L.; Ferraro, G.; Marchetti, M.; Amuso, D. The role of hyaluronic acid and amino acid against the aging of the human skin: A clinical and histological study. J. Cosmet. Dermatol. 2020, 20, 2296–2304. [Google Scholar] [CrossRef]
- Kim, M.H.; Kim, B.S.; Park, H.; Lee, J.; Park, W.H. Injectable methylcellulose hydrogel containing calcium phosphate nanoparticles for bone regeneration. Int. J. Biol. Macromol. 2018, 109, 57–64. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).